Back to Journals » Clinical, Cosmetic and Investigational Dermatology » Volume 17
Knowledge, Attitudes and Practices Towards Psoriasis Among Patients and Their Family Members
Authors Zhang X, Du H, Liu X, Liu L, Zhang T
Received 13 December 2023
Accepted for publication 31 March 2024
Published 3 April 2024 Volume 2024:17 Pages 769—782
DOI https://doi.org/10.2147/CCID.S454798
Checked for plagiarism Yes
Review by Single anonymous peer review
Peer reviewer comments 2
Editor who approved publication: Dr Jeffrey Weinberg
Xiaolan Zhang, Hongyang Du, Xiaoxiao Liu, Luyao Liu, Tingwei Zhang
Department of Dermatology, The First Affiliated Hospital of JinZhou Medical University, Jinzhou, 121001, People’s Republic of China
Correspondence: Xiaolan Zhang, Department of Dermatology, The First Affiliated Hospital of JinZhou Medical University, Jinzhou, 121001, People’s Republic of China, Tel +86-13840698157, Email [email protected]
Purpose: KAP studies serve to enhance health consciousness and furnish foundational data for appraising, strategizing, and enacting disease management and prejudice eradication initiatives. There remains a dearth of published studies elucidating the dimensions of knowledge, attitudes, and practices among psoriasis patients in China. To investigate the knowledge, attitudes and practices (KAP) towards psoriasis among patients and their family members in Northern China.
Methods: This web-based, cross-sectional study was conducted among psoriasis patients and their family members through a self-administered questionnaire.
Results: Among patients (n=260), their mean KAP scores were 9.76± 5.69 (range: 0– 19), 35.64± 11.48 (range: 14– 70), and 56.73± 10.98 (range: 16– 80), respectively. Among family members (n=237), their mean KAP scores were 11.93± 5.34 (range: 0– 19), 35.80± 4.34 (range: 8– 40), and 37.04± 4.38 (range: 8– 40), respectively. Structural equation modeling (SEM) analysis for patients indicated significant and negative path relations between knowledge and attitudes (β=− 2.271, P< 0.001), and between knowledge and practice (β=− 0.398, P< 0.001). Extended SEM analysis, which divides knowledge into K1, K2, and K3 parts, showed negative path relations between K3 and attitude (β=− 1.300, P=0.002), between attitude and practice (β=− 0.634, P< 0.001). Moreover, SEM for family members showed positive path relations between knowledge and attitude (β=1.536, P< 0.001), between attitude and practice (β=0.682, P< 0.001).
Conclusion: Patients in Northern China demonstrated insufficient knowledge, negative attitude, and proactive practice, while their family members had insufficient knowledge, positive attitude, and proactive practice toward psoriasis. It is recommended to implement educational interventions addressing knowledge gaps among patients and families.
Keywords: knowledge, attitude, practice, psoriasis, patients and family members, questionnaire, cross-sectional study
Introduction
Psoriasis, an enduring inflammatory skin disease typified by erythematous squamous plaques, impacts roughly 2% of populations in Europe and North America.1 Despite its prevalence, the etiological underpinnings of the disease remain enigmatic, with antecedent infections, specific medications, and psychological and physiological stressors constituting potential contributors to its manifestation.2 Furthermore, deficient social connections can precipitate issues encompassing emotional distress.3 Notably, individuals with psoriatic lesions evident in conspicuously visible regions like the face, scalp, and dorsal hand surface often grapple with heightened stigmatization compared to those afflicted with alternate dermatological conditions, consequently encountering diminished social support networks.4 Psoriasis is commonly associated with significant impairment of quality of life (QoL).5 A cross-sectional study reported that 8.5% of patients exhibited symptoms of depression, while 16.9% demonstrated symptoms of anxiety.6 Depression can exacerbate the recurrence of psoriasis and deteriorate the quality of life of patients, potentially leading to suicide and other grave outcomes.7
The psychological ramifications of psoriasis have demonstrated an impact that reverberates beyond the confines of the patient’s experience, influencing the well-being of their family members as well.8 Those in the familial sphere of patients with psoriasis contend with an array of challenges, encompassing concerns regarding the patient’s future, apprehension regarding potential side effects of employed medications, increased domestic responsibilities due to the presence of scales and residue resulting from topical treatments, and constraints on their social and recreational pursuits. Notably, these issues may hold lesser relevance for family members of individuals grappling with skin conditions distinct from psoriasis, such as acne or benign cutaneous lesions.
The Knowledge, Attitude, and Practice (KAP) framework constitutes a structured survey approach widely employed in health promotion endeavors.9 KAP studies serve to enhance health consciousness and furnish foundational data for appraising, strategizing, and enacting disease management and prejudice eradication initiatives. Insufficient awareness, unfavorable attitudes, and apprehensions regarding disclosing their condition due to concerns over discrimination stand as pivotal obstacles in addressing the adverse psychological ramifications of psoriasis and bolstering patients’ adherence to treatment regimens. While research has examined the influence of stigmatizing behaviors on psoriasis patients, there remains a dearth of published studies elucidating the dimensions of knowledge, attitudes, and practices among psoriasis patients. Previous inquiries underscore the deleterious impact of stigmatization and social isolation experienced by psoriasis patients and their familial circles, manifesting as amplified propensities toward depression and anxiety, ultimately contributing to a diminished health-related quality of life.10,11 Therefore, this study aims to investigate the knowledge, attitudes and practices towards psoriasis among patients with psoriasis and their family members in Northern China.
Materials and Methods
Study Design and Participants
This cross-sectional study was conducted at The First Affiliated Hospital of Jinzhou Medical University among patients with psoriasis and their family members between October 2022 and April 2023. Inclusion criteria: 1) patients diagnosed with psoriasis and their corresponding family members; 2) individuals aged ≥ 18 years; and 3) voluntary engagement in the study. Exclusion criteria were individuals with psychiatric disorders and those manifesting behavioral disorders. This study was approved by the Ethics Committee for New Technology and New Projects of the First Affiliated Hospital of Jinzhou Medical University (2022015), and informed consent was obtained from all participants.
Questionnaires
Two questionnaires were developed for patients and their respective family members, drawing from established literature12,13 and “Human Health 8th edition of Dermatology textbook. 139–142”, and subsequently refined based on feedback from two associate chief physicians specializing in dermatovenereology. A pilot study was conducted involving 23 patients and 22 family members. The Cronbach’s α coefficients for the patients’ and family members’ questionnaires were 0.889 and 0.902, respectively, indicating robust internal consistency within both sets of questionnaires.
Both the patient and family member questionnaires were developed in the Chinese language, each encompassing four dimensions. The patient questionnaire comprised 70 items, distributed as 19 for sociodemographic characteristics, 20 for knowledge, 14 for attitudes, and 17 for practices. In the knowledge section, correct responses were scored 1 point, while incorrect or unclear responses received 0 points; notably, a decoy question (K4) was included to identify inattentive responses and was not scored. This rendered the knowledge section theoretically ranging from 0 to 19 points. Attitudes and practices were predominantly evaluated using a five-point Likert scale, reflecting the degree of positivity. For instance, items A11 and A13 were scored from strongly agree (5 points) to strongly disagree (1 point), with the remaining items reverse scored, resulting in a potential score range of 14 to 70 points for attitudes. Within the practices section, items were scored from 5 points (very conformance) to 1 point (very non-conformance), except for P14 and P15, which were reverse scored, leading to a theoretical score span of 16 to 80 points. The questionnaire for family member encompass 70 items, included 14 items for sociodemographic characteristics, 20 for knowledge, 8 for attitudes, and 8 for practices. The scoring methodology for knowledge was consistent with the patient questionnaire. Similar to the patient questionnaire, attitudes and practices were evaluated through a five-point Likert scale, reflecting degrees of positivity, with item A4 scored from strongly agree (5 points) to strongly disagree (1 point), and the remaining items reverse scored, yielding a possible score range of 8 to 40 points for attitudes. Within the practices dimension, items were scored from 5 points (very conformance) to 1 point (very non- conformance), resulting in a theoretical score range of 8 to 40 points. Attainment of 70% or more of the total theoretical score for knowledge, attitudes, and practices was construed as indicative of “sufficient knowledge”, “positive attitudes”, and “proactive practices”.
Participants were enlisted through diverse avenues including WeChat groups, dermatology clinics outreach, promotional platforms within Jinzhou Medical University, and routine psoriasis seminars. The data collection process employed a combination of paper-based questionnaires, the online questionnaire platform “Sojump (https://www.wjx.cn/)” and telephone consultations. Healthcare professionals engaged in the study undertook responsibilities such as verifying patient-specific details, overseeing the endorsement of commitment letters, and addressing any operational or content-related inquiries during the response process. Questionnaires featuring conflicting responses to decoy questions, conspicuous logical inconsistencies, such as an improbable age of 5 years, or exhibiting identical patterns of option selection were deemed invalid and excluded from analysis.
Statistical Analysis
Stata 17.0 (Stata Corporation, College Station, TX, USA) and SPSS 20.0 (IBM Corp., Armonk, NY, USA) were used for statistical analysis. Continuous variables were expressed using mean ± standard deviations (SD), Student’s t-tests was used for comparisons between two groups, and ANOVA for comparisons between multiple groups. Categorical variables were expressed as n (%). Structural equation modelling (SEM) was used to test the hypotheses that (H1) knowledge has a direct effect on Attitudes; (H2) knowledge has a direct effect on Practices; and (H3) knowledge has an indirect effect on Practices via its effect on Attitudes. Two-sided P<0.05 was considered statistically significant.
Results
Initially, a total of 327 patients completed the questionnaire. However, 9 questionnaires were excluded due to contradictory logic or selecting the same option multiple times, leaving a total of 318 valid questionnaires (97.25%). Similarly, a total of 327 patients’ family members completed the questionnaire. Among them, 90 questionnaires were excluded for similar reasons, resulting in 237 valid questionnaires (72.48%). As a result, patients (n=318) and their family members (n=237) who were affected by psoriasis were included in the final analysis. Among patients, 117 (45.00%) were male, 81 (31.15%) were aged between 18 and 35 years, 216 (83.08%) identified as Han ethnicity. Among their family members, 67 (28.27%) were male, the mean age was 40.46±12.06 years, 195 (82.28%) identified as Han ethnicity. The mean scores of patients were 9.76±5.69 (knowledge, possible range: 0–19), 35.64±11.48 (attitudes, possible range: 14–70), and 56.73±10.98 (practices, possible range: 16–80). The mean scores of their family members were 11.93±5.34 (knowledge, possible range: 0–19), 35.80±4.34 (attitudes, possible range: 8–40), and 37.04±4.38 (practices, possible range: 8–40). In patients, knowledge scores were significantly varied in the type of medical insurance, duration since diagnosis, type of psoriasis, underlying diseases, family history of psoriasis (all p<0.05). Attitude scores were significantly varied in the type of medical insurance, type of psoriasis, underlying diseases (all p<0.05). Practice scores were significantly varied in the type of medical insurance and underlying diseases (both p<0.05). In family members, knowledge scores were significantly varied in the education, medical insurance, smoking status (all p<0.05). Attitude scores were significantly varied in smoking and drinking alcohol or not (both p<0.05). Practice scores were significantly varied in drinking alcohol status (p<0.05) (Table 1).
 |
Table 1 Demographic Information of Patients and Families |
The correctness rates for knowledge items related to psoriasis among patients and family members. Among the top three knowledge items with relative high correctness rates for the two populations were: “Psoriasis is a chronic inflammatory skin disease” (K1.1) with a correctness rate of 67.31% for patients and 81.86% for family members, “Psoriasis is an immune-related disease” (K1.3) with a correctness rate of 70.38% for patients and 80.59% for family members, and “The use of skin moisturizers is very important for patients with psoriasis” (K3.2) with a correctness rate of 63.46% for patients and 75.95% for family members. Conversely, the three items with relative low correctness rates for patients and family members were: “Psoriasis is associated with genetic factors” (K1.4) with a correctness rate of 50.00% for patients and 56.54% for family members, “Some drugs such as propranolol and ibuprofen can trigger an onset of psoriasis” (K3.3) with a correctness rate of 29.23% for patients and 36.71% for family members, and “The internal medications used to treat psoriasis, such as methotrexate and retinoids, may cause some damage to the body over a long period of time” (K3.4) with a correctness rate of 25.38% for patients and 60.34% for family members (Table S1).
In the attitudes dimension, among the patients, a significant proportion reported experiencing psychological stress (127, 48.85%) and concerns about the hereditary nature of psoriasis (133, 51.15%). Many participants expressed fears regarding the impact of psoriasis on their relationships and social interactions, with 94 (36.15%) being afraid of its effect on marriage, and 106 (40.77%) feeling embarrassed or uncomfortable in social occasions. Additionally, a considerable number of patients (92, 35.38%) expressed concerns about how others perceive them due to psoriasis. On the other hand, lower agreement rates were observed regarding the impact of psoriasis on self-image and behavior, such as becoming more introverted (71, 27.31%) and feeling overlooked by others (68, 26.15%). Among family members, a significant majority (190, 80.17%) strongly agreed that patients with psoriasis experience considerable psychological stress and require more care and support. Additionally, a substantial number of respondents understood and empathized if their family member becomes grumpy and irritable after diagnosis (160, 67.51%), and they agreed that if their member becomes introverted due to psoriasis, they should offer encouragement and support (188, 79.32%). However, a noteworthy proportion of family members expressed worry about potential psoriasis transmission, leading them to avoid close contact with the affected member (100, 42.19%) (Table S2).
In the practices dimension, a significant proportion of patients (121, 46.54%) reported always or completely complying with the prescribed order of administration of topical medication. Furthermore, a considerable number (113, 43.46%) chose appropriate clothing according to their skin condition. Additionally, many patients sought regular psychological counseling (77, 29.62%) and actively engaged with other psoriasis patients in sharing treatment experiences (80, 30.77%). However, certain behaviors saw lower levels of compliance, such as refusing internal medications prescribed by doctors (46, 17.69%), avoiding physical contact with others (84, 32.31%), and losing friends or jobs due to psoriasis (48, 18.46%). A significant majority of family members reported always or completely complying with supervising the patient’s regular follow-ups (182, 76.79%), medical check-ups (169, 71.31%), and assisting with the administration of topical medication (178, 75.11%) if needed. Additionally, many family members monitored the patient’s avoidance of smoking and alcohol (184, 77.64%) and provided care and frequent encouragement to the patient (184, 77.64%). Moreover, a considerable number of family members actively intervened if they saw the patient using informal medication (176, 74.26%) and encouraged them to join groups of psoriasis patients for increased communication (163, 68.78%). Furthermore, family members engaged in learning about psoriasis (158, 66.67%) to better support the patient’s condition (Table S3).
The SEM analysis of patients indicated significant and negative path relations between knowledge and attitudes (β=−1.985, P<0.001), as well as between knowledge and practice (β=−0.470, P<0.001), and between attitude and practice (β=−1.001, P<0.001) (Figure 1, Table 2, and Table S4). Additionally, extended SEM analysis of patients, which divides knowledge into three parts (K1, K2, and K3), showed negative path relations between K3 and attitude (β=−1.300, P=0.002), as well as between attitude and practice (β=−0.634, P<0.001) (Figure 2, Table 3, and Table S5). The SEM analysis of family members showed positive path relations between knowledge and attitude (β=1.084, P<0.001), and between attitude and practice (β=1.223, P<0.001), while negative path relations between knowledge and practice (β=−0.383, P<0.001) (Figure 3, Table 4, and Table S6). The extended SEM analysis of family members indicated positive path relations between attitude and practice (β=0.565, P<0.001) (Figure 4, Table 5, and Table S7).
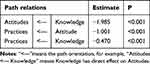 |
Table 2 SEM for Patients |
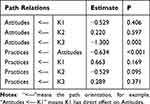 |
Table 3 Extended SEM for Patients |
 |
Table 4 SEM for Families |
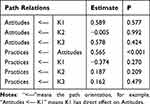 |
Table 5 Extended SEM for Families |
 |
Figure 1 SEM for patients. |
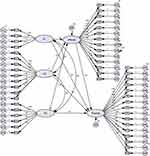 |
Figure 2 Extended SEM for patients. |
 |
Figure 3 SEM for families. |
 |
Figure 4 Extended SEM for families. |
Discussion
This study suggested that patients in Northern China demonstrated insufficient knowledge, negative attitude, and proactive practice, while their family members had insufficient knowledge, positive attitude, and proactive practice toward psoriasis. To improve disease management, it is recommended to implement educational interventions for patients and their families to address knowledge gaps. Additionally, providing psychosocial support and counseling to patients with negative attitudes could enhance their well-being. Emphasizing and reinforcing positive practices among patients and their families might contribute to better treatment outcomes and more patient-centered care.
The findings of this study highlighted that a significant portion of participants accurately grasped key facets of psoriasis, encompassing its chronic inflammatory nature and immune-related factors. However, evident knowledge gaps were identified, particularly concerning genetic elements, medication-induced triggers, and potential long-term effects of treatments. This underscores the urgency for focused educational interventions to address these gaps, with healthcare practitioners taking the lead in disseminating precise information to patients and their families.14 By offering educational resources, workshops, and interactive sessions, a deeper understanding can be fostered, ensuring that patients and families are well-informed about the condition.15,16 Aligning with the study’s emphasis on tackling knowledge gaps, it is imperative for healthcare practitioners to craft evidence-based educational interventions that specifically target areas of misunderstanding.17,18
The research findings underscore the significant psychological impact of psoriasis on both patients and their family members. Patients commonly experienced psychological stress and harbored concerns about the potential hereditary transmission of the condition.19,20 Meanwhile, family members exhibited a profound comprehension of the emotional toll inflicted upon patients. However, the study also brought to light certain misconceptions, exemplified by the avoidance of close contact due to a fear of disease transmission. Addressing these attitudes necessitates fostering open communication channels between patients, their families, and healthcare providers. Cultivating empathy, dispelling misconceptions, and nurturing a supportive environment are crucial steps in alleviating the emotional burden entailed by psoriasis.21,22 The study’s findings accentuate the imperative for comprehensive psychosocial support systems aimed at tackling the emotional challenges associated with psoriasis. The integration of interventions designed to enhance patient and family attitudes, such as cognitive-behavioral therapy and participation in support groups, has been shown to yield noteworthy benefits in reducing distress and enhancing overall quality of life.23–25
The study elucidated commendable practices, such as the consistent adherence to prescribed topical medications and active engagement in seeking psychological counseling. Nevertheless, instances of non-compliance were also evident, encompassing the refusal of internal medications and the avoidance of physical contact. Enhancing these practices demands a multi-pronged approach. Healthcare practitioners should concentrate on refining the lines of communication between patients and doctors to effectively address concerns and rectify misconceptions surrounding various treatments.26,27 Moreover, the inclusion of family members in the treatment regimen can wield a positive influence on patient adherence. This inclusion might encompass educating family members on the significance of treatment adherence, accentuating their supportive role, and cultivating an environment conducive to sustained compliance.28
A noteworthy observation is the consistency in the questions related to the “K” dimension across both patient and family member questionnaires, yet a contrasting positive effect in the SEM results for family members. This intriguing phenomenon warrants in-depth exploration to discern potential reasons behind this positivity among family members, despite the shared questionnaire content. Possible explanations might include variations in interpretation, emotional involvement, or familial support dynamics.29,30 Furthermore, the recognition that external factors, encompassing the environment and personnel, can influence and disrupt certain patient attitudes and practices, leading to negative effects, underscores the intricate interplay between individuals and their surroundings.31
In addition, the observed negative path relations between KAP towards psoriasis among patients and their family members may be attributed to a multifaceted interplay of factors. Limited understanding and misinformation about psoriasis can lead to the development of negative attitudes, while the visible nature of the condition can result in stigmatization and discriminatory practices.32,33 Media and cultural influences further shape these perceptions.34–36 Addressing these issues through evidence-based education, destigmatization efforts, and challenging stereotypes is essential for promoting a more empathetic and informed society, ultimately improving the experiences of individuals living with psoriasis and their family members.
Based on the results of this study, it is recommended that comprehensive improvement measures be taken to address the disparities in KAP among psoriasis patients and their family members in Northern China. Initially, gender-sensitive health education programs should be developed to bridge the gap in knowledge acquisition and attitudes between male and female patients, particularly aiming to enhance the knowledge level and positive attitudes of female patients. Subsequently, targeted support and intervention measures should be designed for patients with different employment statuses and income levels, especially providing financial assistance and health education to low-income and unemployed patients to facilitate their access to treatment and improve their lifestyles. Additionally, integrated care plans should be offered to patients with comorbidities, focusing on the management of psoriasis and other potential diseases concurrently. The role of family members in patient education and care should also be strengthened, leveraging the positive influence of family on patients’ attitudes and practices, and encouraging family support and participation. Furthermore, the promotion of community support groups and patient mutual aid groups is essential, providing a platform for patients and families to share experiences and support each other. Moreover, in the holistic treatment approach for psoriasis patients with comorbidities, the development of new drugs is paramount, particularly those targeting key molecules in the pathogenesis. Such drug development efforts not only aid in reducing the risks associated with polypharmacy and drug interactions but also improve patient compliance to treatment, wellbeing, and quality of life.37
Strengths and Limitations
This study had limitations. The cross-sectional design precludes the establishment of causal relationships, limiting the ability to discern temporal dynamics. The study’s single-site setting and potential sampling bias compromise the generalizability of findings. Reliance on self-reported data introduces recall and social desirability biases, potentially influencing response accuracy. Moreover, the absence of comprehensive confounding variable control and validated measurement tools may confound the observed associations. Despite these limitations, this study contributes to the sparse literature on psoriasis KAP in China, highlighting the urgent need for targeted educational interventions. By revealing specific gaps in knowledge and attitudes, as well as the proactive practices among patients and their families, this research lays a foundational base for developing strategies aimed at improving disease management and reducing stigma.
Conclusion
Patients in Northern China demonstrated insufficient knowledge, negative attitude, and proactive practice, while their family members had insufficient knowledge, positive attitude, and proactive practice toward psoriasis. Healthcare professionals should focus on addressing the interrelated aspects of knowledge, attitudes, and practices through targeted interventions to improve clinical outcomes and provide patient-centered care.
Data Sharing Statement
The data underlying this article are available in the article and in its online Supplementary Material.
Ethics Approval and Informed Consent
This study was approved by the Ethics Committee for New Technology and New Projects of the First Affiliated Hospital of Jinzhou Medical University (2022015), and informed consent was obtained from all participants. We confirmed that our study complied with the Declaration of Helsinki.
Acknowledgments
We greatly appreciate all the members of the dermatology department in the First Affiliated Hospital of Jinzhou Medical University.
Author Contributions
All authors made a significant contribution to the work reported, whether that is in the conception, study design, execution, acquisition of data, analysis and interpretation, or in all these areas; took part in drafting, revising or critically reviewing the article; gave final approval of the version to be published; have agreed on the journal to which the article has been submitted; and agree to be accountable for all aspects of the work.
Funding
This work was supported by the Doctoral Scientific Research Foundation of Liaoning Province (grant number: 2022-BS-326).
Disclosure
The author(s) report no conflicts of interest in this work.
References
1. Boehncke WH, Schön MP. Psoriasis. Lancet. 2015;386(9997):983–994. doi:10.1016/S0140-6736(14)61909-7
2. Kamiya K, Kishimoto M, Sugai J, Komine M, Ohtsuki M. Risk factors for the development of psoriasis. Int J Mol Sci. 2019;20(18):4347. doi:10.3390/ijms20184347
3. Zhang H, Yang Z, Tang K, Sun Q, Jin H. Stigmatization in patients with psoriasis: a mini review. Front Immunol. 2021;12:715839. doi:10.3389/fimmu.2021.715839
4. Hrehorów E, Salomon J, Matusiak L, Reich A, Szepietowski JC. Patients with psoriasis feel stigmatized. Acta Derm Venereol. 2012;92(1):67–72. doi:10.2340/00015555-1193
5. Esposito M, Campanati A, Giunta A, et al. Dimethyl fumarate’s effectiveness and safety in psoriasis: a real-life experience during the COVID-19 pandemic. Dermatol Ther. 2022;12(3):671–681. doi:10.1007/s13555-022-00684-3
6. Bakar RS, Jaapar SZS, Azmi AF, Aun YC. Depression and anxiety among patients with psoriasis: a correlation with quality of life and associated factors. J Taibah Univ Med Sci. 2021;16(4):491–496. doi:10.1016/j.jtumed.2021.02.008
7. Zhou L, Wu Z, Li Y, et al. Brief maternal separation promotes resilience to anxiety-like and depressive-like behaviors in female C57BL/6J offspring with imiquimod-induced psoriasis. Brain Sci. 2022;12(9):1250. doi:10.3390/brainsci12091250
8. Eghlileb AM, Davies EE, Finlay AY. Psoriasis has a major secondary impact on the lives of family members and partners. Br J Dermatol. 2007;156(6):1245–1250. doi:10.1111/j.1365-2133.2007.07881.x
9. Yumiya Y, Ohba T, Murakami M, et al. User-guided design of a digital tool for health promotion and radiation protection: results from an internet needs survey. Int J Environ Res Public Health. 2021;18(22):12007. doi:10.3390/ijerph182212007
10. Jankowiak B, Kowalewska B, Krajewska-Kułak E, Khvorik DF. Stigmatization and quality of life in patients with psoriasis. Dermatol Ther. 2020;10(2):285–296. doi:10.1007/s13555-020-00363-1
11. Łakuta P, Marcinkiewicz K, Bergler-Czop B, Brzezińska-Wcisło L. How does stigma affect people with psoriasis? Postepy Dermatol Alergol. 2017;34(1):36–41. doi:10.5114/pdia.2016.62286
12. Menter A, Korman NJ, Elmets CA, et al. Guidelines of care for the management of psoriasis and psoriatic arthritis: section 6. Guidelines of care for the treatment of psoriasis and psoriatic arthritis: case-based presentations and evidence-based conclusions. J Am Acad Dermatol. 2011;65(1):137–174. doi:10.1016/j.jaad.2010.11.055
13. Menter A, Strober BE, Kaplan DH, et al. Joint AAD-NPF guidelines of care for the management and treatment of psoriasis with biologics. J Am Acad Dermatol. 2019;80(4):1029–1072. doi:10.1016/j.jaad.2018.11.057
14. Hur S, Lee J, Kim T, et al. An automated fast healthcare interoperability resources-based 12-lead electrocardiogram mobile alert system for suspected acute coronary syndrome. Yonsei Med J. 2020;61(5):416–422. doi:10.3349/ymj.2020.61.5.416
15. Grauman Å, Viberg Johansson J, Falahee M, Veldwijk J. Public perceptions of myocardial infarction: do illness perceptions predict preferences for health check results. Prev Med Rep. 2022;26:101683. doi:10.1016/j.pmedr.2021.101683
16. Yang T, Tan T, Yang J, et al. The impact of using three-dimensional printed liver models for patient education. J Int Med Res. 2018;46(4):1570–1578. doi:10.1177/0300060518755267
17. Irazusta-Garmendia A, Orpí E, Bach-Faig A, González Svatetz CA. Food sustainability knowledge, attitudes, and dietary habits among students and professionals of the health sciences. Nutrients. 2023;15(9):2064. doi:10.3390/nu15092064
18. Jaarsma T, Hill L, Bayes-Genis A, et al. Self-care of heart failure patients: practical management recommendations from the Heart Failure Association of the European Society of Cardiology. Eur J Heart Fail. 2021;23(1):157–174. doi:10.1002/ejhf.2008
19. Burger B, Sagiorato RN, Cavenaghi I, Rodrigues HG. Abnormalities of sphingolipids metabolic pathways in the pathogenesis of psoriasis. Metabolites. 2023;13(2):291. doi:10.3390/metabo13020291
20. Subedi S, Gong Y, Chen Y, Shi Y. Infliximab and biosimilar infliximab in psoriasis: efficacy, loss of efficacy, and adverse events. Drug Des Devel Ther. 2019;13:2491–2502. doi:10.2147/DDDT.S200147
21. October TW, Dizon ZB, Arnold RM, Rosenberg AR. Characteristics of physician empathetic statements during pediatric intensive care conferences with family members: a qualitative study. JAMA Network Open. 2018;1(3):e180351. doi:10.1001/jamanetworkopen.2018.0351
22. Xie J, Yang H, Xia X, Yu S. The influence of medical professional knowledge on empathy for pain: evidence from fNIRS. Front Psychol. 2018;9:1089. doi:10.3389/fpsyg.2018.01089
23. Birnie KA, Noel M, Chambers CT, Uman LS, Parker JA. Psychological interventions for needle-related procedural pain and distress in children and adolescents. Cochrane Database Syst Rev. 2018;10(10):Cd005179. doi:10.1002/14651858.CD005179.pub4
24. Judd-Glossy L, Ariefdjohan M, Ketzer J, et al. Considering the value of online support groups for colorectal conditions: perspectives from caregivers and adult patients. Pediatr Surg Int. 2022;38(1):31–42. doi:10.1007/s00383-021-05021-x
25. Padgaonkar NT, Phuong Uy J, DePasque S, Galván A, Peris TS. Neural correlates of emotional reactivity and regulation in youth with and without anxiety. Depress Anxiety. 2021;38(8):804–815. doi:10.1002/da.23154
26. Bowers SP, Clare K, Hagerty L, et al. Predicting 1-year mortality among patients with decompensated cirrhosis: results of a multicentre evaluation of the Bristol Prognostic Score. BMJ Open Gastroenterol. 2022;9(1):1465. doi:10.1136/bmjgast-2021-000822
27. Guo X, Chen S, Zhang X, Ju X, Wang X. Exploring patients’ intentions for continuous usage of mHealth services: elaboration-likelihood perspective study. JMIR mHealth uHealth. 2020;8(4):e17258. doi:10.2196/17258
28. Sultana J, Sutradhar I, Rahman MJ, et al. An uninformed decision-making process for cesarean section: a qualitative exploratory study among the slum residents of Dhaka City, Bangladesh. Int J Environ Res Public Health. 2022;19(3):1465. doi:10.3390/ijerph19031465
29. Steijvers LC, Brinkhues S, Tilburg TGV, et al. Changes in structure and function of social networks of independently living middle-aged and older adults in diverse sociodemographic subgroups during the COVID-19 pandemic: a longitudinal study. BMC Public Health. 2022;22(1):2253. doi:10.1186/s12889-022-14500-2
30. Wu Q, Zhu P, Liu X, et al. The impact of family function on mental health status in patient with inflammatory bowel disease: the mediating role of self-esteem. Front Psychiatry. 2022;13:1007318. doi:10.3389/fpsyt.2022.1007318
31. Buljac-Samardzic M, Clark MA, van Exel NJA, van Wijngaarden JDH. Patients as team members: factors affecting involvement in treatment decisions from the perspective of patients with a chronic condition. Health Expect. 2022;25(1):138–148. doi:10.1111/hex.13358
32. Papp KA, Gooderham M, Beecker J, et al. Rationale, objectives and design of PURE, a prospective registry of patients with moderate to severe chronic plaque psoriasis in Canada and Latin America. BMC Dermatol. 2019;19(1):9. doi:10.1186/s12895-019-0087-3
33. Piraccini BM, Starace M, Toft A. Early visible improvements during K101-03 treatment: an open-label multicenter clinical investigation in patients with onychomycosis and/or nail psoriasis. Dermatology. 2017;233(2–3):178–183. doi:10.1159/000478257
34. Coombs NC, Campbell DG, Caringi J. A qualitative study of rural healthcare providers’ views of social, cultural, and programmatic barriers to healthcare access. BMC Health Serv Res. 2022;22(1):438. doi:10.1186/s12913-022-07829-2
35. de Macêdo PFC, Nepomuceno CMM, Dos Santos NS, et al. Weight stigma in the COVID-19 pandemic: a scoping review. J Eat Disord. 2022;10(1):44. doi:10.1186/s40337-022-00563-4
36. Teng F, Shi J, Wang X, Chen Z. The association between COVID-19-related wellbeing with materialism and perceived threat. Int J Environ Res Public Health. 2022;19(2):912. doi:10.3390/ijerph19020912
37. Camela E, Potestio L, Fabbrocini G, Pallotta S, Megna M. The holistic approach to psoriasis patients with comorbidities: the role of investigational drugs. Expert Opin Investig Drugs. 2023;32(6):537–552. doi:10.1080/13543784.2023.2219387
 © 2024 The Author(s). This work is published and licensed by Dove Medical Press Limited. The
full terms of this license are available at https://www.dovepress.com/terms.php
and incorporate the Creative Commons Attribution
- Non Commercial (unported, v3.0) License.
By accessing the work you hereby accept the Terms. Non-commercial uses of the work are permitted
without any further permission from Dove Medical Press Limited, provided the work is properly
attributed. For permission for commercial use of this work, please see paragraphs 4.2 and 5 of our Terms.
© 2024 The Author(s). This work is published and licensed by Dove Medical Press Limited. The
full terms of this license are available at https://www.dovepress.com/terms.php
and incorporate the Creative Commons Attribution
- Non Commercial (unported, v3.0) License.
By accessing the work you hereby accept the Terms. Non-commercial uses of the work are permitted
without any further permission from Dove Medical Press Limited, provided the work is properly
attributed. For permission for commercial use of this work, please see paragraphs 4.2 and 5 of our Terms.
Recommended articles
Managing Pain in Low Resource Settings: Healthcare Professionals’ Knowledge, Attitude and Practice Regarding Pain Management in Western Nepal
Thapa P, KC B, Lee SWH, Dujaili JA, Gyawali S, Mohamed Ibrahim MI, Alrasheedy AA
Journal of Pain Research 2022, 15:1587-1599
Published Date: 2 June 2022
Knowledge, Attitudes, and Practices Regarding Ergonomic Hazards Among Healthcare Workers in a Saudi Government Hospital

ALHazim SS, Al-Otaibi ST, Herzallah NH
Journal of Multidisciplinary Healthcare 2022, 15:1771-1778
Published Date: 24 August 2022
Self-Medication Prevalence and Factors Associated with Knowledge and Attitude Towards Self-Medication Among Undergraduate Health Science Students at GAMBY Medical and Business College, Bahir Dar, Ethiopia
Siraj EA, Yayehrad AT, Kassaw AT, Kassahun D, Solomon E, Abdela H, Gizachew G, Awoke E
Patient Preference and Adherence 2022, 16:3157-3172
Published Date: 5 December 2022
Knowledge, Attitudes and Practices Toward Physical Literacy Among the College Students During COVID-19 School Closure
Ma C, Yue M, Zhu X
Journal of Multidisciplinary Healthcare 2024, 17:1629-1640
Published Date: 15 April 2024
Knowledge, Attitude and Practice of Radiologists Regarding Artificial Intelligence in Medical Imaging
Huang W, Li Y, Bao Z, Ye J, Xia W, Lv Y, Lu J, Wang C, Zhu X
Journal of Multidisciplinary Healthcare 2024, 17:3109-3119
Published Date: 4 July 2024
