Back to Journals » ClinicoEconomics and Outcomes Research » Volume 14
Health-care Workers’ Willingness to Pay for COVID-19 Vaccines in Eastern Ethiopia: Using Contingent Valuation Method
Authors Merga BT , Ayana GM , Negash B, Alemu A, Abdurke M , Abdu A , Balis B , Bekana M, Fekadu G , Raru TB
Received 4 February 2022
Accepted for publication 9 May 2022
Published 19 May 2022 Volume 2022:14 Pages 395—404
DOI https://doi.org/10.2147/CEOR.S361199
Checked for plagiarism Yes
Review by Single anonymous peer review
Peer reviewer comments 4
Editor who approved publication: Dr Samer Hamidi
Bedasa Taye Merga,1 Galana Mamo Ayana,1 Belay Negash,1 Addisu Alemu,1 Mohammed Abdurke,2 Ahmedmenewer Abdu,3 Bikila Balis,2 Miressa Bekana,4 Gelana Fekadu,2 Temam Beshir Raru1
1School of Public Health, College of Health and Medical Sciences, Haramaya University, Harar, Ethiopia; 2School of Nursing and Midwifery, College of Health and Medical Sciences, Haramaya University, Harar, Ethiopia; 3Department of Laboratory Science, College of Health and Medical Sciences, Haramaya University, Harar, Ethiopia; 4School of Medicine, College of Health and Medical Sciences, Haramaya University, Harar, Ethiopia
Correspondence: Galana Mamo Ayana, School of Public Health, College of Health and Medical Sciences, Haramaya University, P.O.Box: 235, Harar, Ethiopia, Email [email protected] Bedasa Taye Merga, School of Public Health, College of Health and Medical Sciences, Haramaya University, P.O.Box: 235, Harar, Ethiopia, Email [email protected]
Background: Health-care workers (HCWs) are among the highest risk groups for COVID-19 infection. The vaccine is found to be vital for HCWs, their household contacts, and their patients to protect against COVID-19 infection and maintain the safety of health systems. The actual willingness to pay for COVID-19 vaccination and associated factors remain uncertain among health-care workers in Ethiopia. Therefore, studying health-care workers’ willingness to pay (WTP) for COVID-19 vaccination helps to have an insight on valuation of the vaccine.
Methods: Institution-based cross-sectional study was conducted among 403 randomly selected health-care workers working in health facilities in eastern Ethiopia from February 3 to March 20, 2021. Pretested structured questionnaire was used to collect data. Binary logistic regression analysis was fitted to test the associations between outcome and explanatory variables. A p-value of < 0.05 with 95% confidence interval was used to declare statistical significance.
Results: The magnitude of willingness to pay for a COVID-19 vaccine was 42.8%. The median amounts of money respondents willing to pay was 400 ETB (US$ 10.04). Sex (male, AOR = 2.33; 95% CI: 1.39, 3.93), monthly income (> 7000 ETB, AOR = 1.22; 95% CI: 1.11, 2.51), affordability (AOR = 1.99; 95% CI: 1.18, 3.35), fear of side effects (AOR = 3.75; 95% CI: 2.13, 6.60), support vaccinations (AOR = 2.97; 95% CI: 1.65, 5.35), the likelihood of getting COVID-19 infection (AOR = 2.11; 95% CI: 1.26, 3.52) were independent determinants of WTP for a COVID-19 vaccine.
Conclusion: Health-care workers’ willingness to pay for COVID-19 vaccination was found to be low. Detailed health education and training about COVID-19 vaccines are required regarding their side effects, and efficacy to make an informed decision to enhance the willingness to pay for the vaccine. Moreover, the government should consider providing COVID vaccines free of charge for low-income groups and at an affordable price for those who could pay.
Keywords: COVID-19, vaccine, health workers, willingness to pay, Ethiopia
Introduction
Coronavirus disease 2019 (COVID-19) epidemic started from Wuhan city of China towards the end of December 2019 and since then spread rapidly to all the countries of the world.1 It causes a range of human respiratory tract infections varying from mild cold to severe respiratory distress syndrome.2 COVID-19 pandemic has continued causing severe diseases and economic burdens around the world.3 Among many others, health-care workers (HCW) face an infectious outbreak in the front line by exposing themselves to a substantial risk of contracting the infection and developing mental health problems.4,5 The increased susceptibility, morbidity, and mortality among the healthcare workers have further worsened the already strained health system, and consequently, worsened the fight against the pandemic.6,7
Several public health measures have been tried in the fight against the disease, including the promotion of universal precaution, drugs and vaccinations.4,8–10 Ethiopia introduced COVID-19 vaccination on March 13, 2021, and several vaccines (e.g. Johnson & Johnson, AstraZeneca, Pfizer, Sinopharm, Sinovac) have been made available.11 As of April 10, 2022, a total of 29,411,822 vaccine doses have been administered in Ethiopia which is <10% of the total population.12 A narrative review mapping global COVID-19 vaccine acceptance rates indicated low vaccine acceptance rates (48.4%) among health-care workers in Ethiopia compared with other African countries, and high acceptance rate (92%) among general population in Ethiopia.13
The vaccine is vital for HCWs, their household contacts, and their patients to protect against COVID-19 infection and maintain the safety of health systems.14 Studies have consistently shown that health-care workers offer guidance on vaccine recommendations and help combat misinformation, confusion, and ignorance about the risks and benefits of vaccination to the public.15 However, absolute HCW support for vaccines should not be taken for granted. A recent study conducted in France found that 43% of health practitioners did not recommend vaccines to key demographic groups, and carried strong perceptions of vaccine risk based on decades-old societal controversies.16 Acceptance and willingness to pay for COVID-19 vaccines can be affected by factors such as vaccine effectiveness, safety and side effects.17 Sex, age, level of education and adherence to safety measures are associated with willingness to vaccinate.18
Willingness to pay (WTP) is an indicator of the monetary value that people would consider paying for a product or service.19 In the current context this term refers to the amount of money a person is ready to pay in exchange for COVID-19 vaccinations to avoid losses or reduce health risks for themselves and their contacts.20 Willingness to pay is related to vaccine characteristics such as vaccine’s effectiveness and side effects, and socio-demographic factors such as sex, marital status, religion, education, employment status, income, or ability to pay.21 To estimate the WTP, the contingent valuation approach was adopted. This method has been used to estimate WTP for many hypothetical vaccines such as against dengue,22–24 Zika,25,26 HIV,27 rabies,28 and COVID-19.29
Evidence regarding the willingness to pay for COVID-19 vaccines among HCWs has paramount importance to ensure its acceptance and valuing that in turn result in positive outcomes for the largest community acceptance and willingness to pay. Therefore, the study assessed health-care workers’ willingness to pay (WTP) for COVID-19 vaccination in eastern Ethiopia. Moreover, the study estimated the average amount of money health-care workers will be willing to pay for the vaccine. This may form the basis for projecting subsidization of the vaccine to ensure universal access.
Methods
Study Design, Period, and Settings
Institution-based cross-sectional study was conducted among health-care workers in Harari region public health facilities, Eastern Ethiopia from February 3 to March 20, 2021. Harar, the capital of Harari region is located 526 km away from Addis Ababa to the east. There are five hospitals (four public and one private), eight health centers, and 20 health posts in the region providing services to more than 5.2 million people around Harar and neighboring regions such as Dire Dawa administrative council, Oromia, and Somali regions.
Populations
In this study, the source populations were all health-care professionals working in Harari region public health facilities. The study population was all health-care professionals working at selected hospitals and health centers. All health-care professionals who are working in Harari region were included.
Sample Size and Sampling Procedure
Sample size was calculated by using single population proportion formula assuming p = 0.5, since there is no prior study done in the study area, q = (1-p), critical value at 95% confidence limit (z) =1.96, margin of error (d) = 0.05, sample size (n) = (zα2)2pq/d2 = (1.96)2 (0.5) (0.5)/ (0.05)2, n = 384. By considering 5% non-response rate, the final sample was calculated to be 403. Out of four public hospitals and 8 health centers found in the region, 2 public hospitals and 5 health centers were selected using a lottery method. Then, based on the number of health-care workers (HCWs) in the selected health facilities, the total calculated sample size was proportionally allocated to each facility. Then the samples were selected from the list of health-care workers in the respective facility using simple random sampling.
Variables in the Study
The dependent variable of the study was willingness to pay for COVID-19 vaccination. Before asking about willingness to pay for COVID-19 vaccine, each participant was presented with a detailed standard COVID-19 vaccine scenario after consenting. The real amount of premium that they were willing to pay for COVID-19 vaccine was assessed using Double Bounded Dichotomous Choice Variant scenario on the contingent valuation method.
Explanatory Variables
The explanatory variables were socio-demographic characteristics (age, sex, marital status, educational status, monthly income, type of profession, family size), self-reported health status, existence of chronic disease, fear of side effects of the COVID-19 vaccine, concern about vaccine efficacy, support vaccine, affordability of the vaccine.
Data Collection Procedures
Data were collected using self-administered questionnaire. A pretest was conducted on 40 health-care workers from unselected health facilities to validate the questionnaire. Ten graduating class students participated in the data collection, while five public health professionals were involved as supervisors. Two days training was provided for both data collectors and supervisors mainly on how to approach the study participants, the objectives and relevance of the study. The questionnaires were prepared in English language. On average each interview took 20 minutes. No incentives were used to promote participation.
Eliciting Willingness to Pay
This study estimated WTP using contingent valuation methods. Contingent valuation is a survey-based economic technique for the valuation of non-market resources, typically the survey asks how much money people would be willing to pay (or willing to accept) to get the proposed services.30 The respondents were told about a hypothetical COVID-19 vaccine with typical attributes based on common features of a vaccine. The question was:
suppose that a vaccine for COVID-19 was developed that assured 95% effective in a year. Suppose that there are no adverse effects. The bid vector (initial bid = 400 ETB) was obtained from a pretest study of 40 individuals who expressed their WTP for a vaccine in an open-ended format. Would you be willing to pay 400 ETB for getting vaccinated?
If the respondent replied “yes” to this question, after that, similar questions with the price of 800 ETB, then 1600 ETB were asked. If the respondent answered “no” to the initial question (400 ETB), they were asked the same question with a price at 200 ETB, then 100 ETB. A participant who refused to pay at the lowest bid (i.e. 100 ETB) was considered not willing to pay. We used double-bound dichotomous choice and bidding game approach to elicit WTP amount for COVID-19.
Statistical Analysis
The data were entered using EpiData version 3.1 and exported to SPSS 24.0 for analysis. Descriptive statistics were presented using percentages, mean and standard deviations. Variables with a p-value of <0.25 in the bivariable analysis were entered into the multivariable analysis. Both crude odds ratio (COR) and adjusted odds ratios (AOR) with a 95% confidence interval were estimated to show the strength of associations. Finally, a p-value of <0.05 in the multivariable logistic regression analysis was used to identify factors significantly associated with the willingness to pay for COVID-19 vaccine.
Ethical Statement
An ethical clearance was received from Haramaya University College of Health and Medical Sciences Institutional Health Research Ethical Review Committee (IHERC). Informed, voluntary, written, and signed consent was obtained from each study participants before commencing the study. No personal identifier information was collected and confidentiality of the information obtained from the respondents was assured. Data were collected under strict adherence to WHO recommended COVID-19 prevention standards for all data collectors, supervisors, and study participants. This study complies with the Declaration of Helsinki.
Results
Socio-Demographic Characteristics of the Study Participants
From a total of 403 approached health-care workers, 348 (86.3% response rate) completed the questionnaire. More than half (54.6%) of them were males. The mean age of the respondents was 29.4± 6.8, majority (43.1%) were in the age group of 26–30 years. Majority of the respondents (56.6%) have work experiences of less than or equal to five years. Two out five respondents had monthly income of 7000 ETB (Ethiopian birr) (see Table 1).
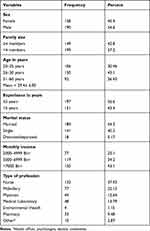 |
Table 1 Socio-Demographic Characteristics of Study Participants, Ethiopia, 2021 (n = 348) |
Perceptions About COVID-19 Vaccine
The majority (63.5%) of the health-care workers supported the COVID-19 vaccine. More than half (54.6%) of the respondents reported that the vaccine is not affordable in terms of its price. About 52.9% and 56% of the respondents have a concern on the side effects and its efficacy, respectively (see Table 2).
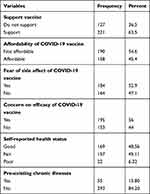 |
Table 2 Vaccine-Related Factors for Willingness to Pay for COVID-19 Vaccine, February, 2021, Harar, Ethiopia (n=348) |
Willingness to Pay for COVID-19 Vaccine
Altogether 149 (42.8%) of participants showed WTP for a COVID-19 vaccine (95% CI: 37.68%, 48.1%). The median amounts of money respondents were willing to pay were 400 ETB (US$10.04, using the average exchange rate between February 3 and March 20, 2021). Of the 149 respondents willing to pay, 63 (42.28%) were willing to pay the initial bid amount of 400 ETB. Of these, 14 (9.4%) participants who were willing to pay the initial bid were also willing to pay the first higher bid of 800 ETB, and 15 (10.1%) who were willing to pay the first higher bid were also willing to pay the second higher bid of 1600 ETB. Of total respondents who were not willing to pay the initial bid, 35 (23.49%) were willing to pay the first lower bid of 200 ETB, 51 (34.22%) who were not willing to pay the first lower bid were willing to pay 100 ETB.
Determinants of WTP for COVID-19 Vaccines
In multivariable analysis sex, monthly income, affordability, fear of side effects, support vaccinations, perceived chance of getting COVID-19 infection were independent determinants of WTP for COVID-19 vaccine.
The odds of willingness to pay for a COVID vaccine was 2.33 times higher among males compared with female respondents (AOR = 2.33; 95% CI: 1.39, 3.93). The odds of willingness to pay for a COVID vaccine was 1.22 times higher among respondents whose monthly income were >7000 ETB compared with those whose monthly incomes were 2000–4999 ETB (AOR = 1.22; 95% CI: 1.11, 2.51). The odds of willingness to pay for a COVID vaccine was 1.99 times higher among respondents who perceive the vaccine as affordable compared with those who perceive the vaccine as unaffordable (AOR = 1.99; 95% CI: 1.18, 3.35).
The odds of willingness to pay for a COVID vaccine was 3.75 times higher among respondents who did not fear side effects of the vaccine compared with those who feared side effects of the vaccine (AOR = 3.75; 95% CI: 2.13, 6.60). The odds of willingness to pay for a COVID vaccine was 2.97 times higher among respondents who support the vaccine compared with those who did not support the vaccine (AOR = 2.97; 95% CI: 1.65, 5.35). The odds of willingness to pay for a COVID vaccine was 2.11 times higher among respondents whose self-reported chance of getting COVID-19 infection was ‘‘likely’’ compared with those whose self-reported chance of getting COVID-19 infection was ‘’unlikely’’ (AOR = 2.11; 95% CI: 1.26, 3.52) (Table 3).
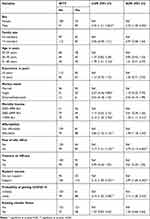 |
Table 3 Determinants of WTP for COVID 19 Vaccine Among Health-Care Workers in Harari Region Public Health Facilities, Eastern Ethiopia, 2021 |
Discussion
More than two-fifths (42.8%) of the health-care workers were willing to pay for a COVID-19 vaccine. This finding is in the range of results from eight surveys conducted among health-care workers (doctors and nurses) with vaccine acceptance rates ranging from 27.7% in the Democratic Republic of the Congo to 78.1% in Israel.31 Contrary to the expectation of high acceptance rate and willingness to pay among health-care workers, this study disclosed a significantly low figure which calls for health-care authorities to increase the COVID-19 vaccine acceptance by health-care workers.
The median amounts of money respondents were willing to pay were 400 ETB (US$10.04 by average exchange rate between February 3 and March 20, 2021). Similar studies estimated significantly higher WTP values. For example, the mean WTP for a COVID-19 vaccine was US$57.2 and US$30.66 in Indonesia and Malaysia, respectively.32,33 A study from Kenya also showed higher values of willingness to pay with estimates of individuals’ mean WTP for the vaccine ranging from USD 49.81 to USD 68.25 (depending on vaccine characteristics).34 This discrepancy may be attributed to the fact that the average income of health-care workers in Ethiopia is relatively low.
Our findings depict that male HCWs were more willing to pay for the vaccine compared with the female respondents. In line with this finding study evidence from other countries suggested that female respondents were less willing to accept COVID-19 vaccines.35–38 In spite of their crucial role regarding childhood vaccination it is unclear why female health-care workers are less willing to pay for the vaccine. Affordability of the vaccine was also found to be significantly associated with willingness to pay for COVID-19 vaccines. Health-care workers who perceived the COVID-19 vaccine as affordable were more likely to pay for the vaccine. This means that a higher price will reduce individuals’ willingness to pay and demand for a vaccine.
Income was found to be an independent determinant of willingness to pay for COVID-19 vaccines. Health-care workers with a higher income were more likely to pay for a vaccine. Other studies from Chile and Kenya support our finding.29,34,39 The demand for health-care service in preventive and non-threatening condition is income sensitive, and the demand and willingness to pay for vaccine is directly related to the income level. This implies that the government should consider providing the vaccine free of charge for low-income groups and allow those with higher incomes to acquire the vaccine through the private sector by paying.
Fear of the vaccine side effects were found to be significantly associated with willingness to pay for the vaccine. The higher the perceived risk of vaccine-associated adverse effects, the lower the demand for vaccination is. Studies revealed that vaccine-related factors such as vaccine effectiveness, safety and side effects were identified as determinants for acceptance of and willingness to pay for vaccines.17,39,40 This implies the need to give detailed information regarding vaccine safety and inviting witnesses who had previously experienced COVID-19 vaccinations to give reassurance to those with fear of side effects.
Respondents who supported the vaccine were more willing to pay for COVID-19 vaccines. Previously conducted studies revealed that it is commonly observed at different times that some individuals might be misinformed about the vaccines and may protest the vaccine-based interventions.41,42 This implies that those who do not consider the vaccine to be important will not get vaccinated and they will be less willing to pay for the vaccine. Therefore, the health-care workers should be provided with detailed information about the importance and protective capacity of COVID-19 vaccines.
Perceived probability of getting COVID-19 infection was found to be an independent determinant of HCWs’ willingness to pay for COVID-19 vaccines. Health-care workers who reported their probability of getting COVID-19 infection as ‘‘likely’’ were more willing to pay for COVID-19 vaccines. This finding is in line with studies from Malaysia and Indonesia that individuals’ risk perception influences their acceptance and willingness to pay for vaccines.43,44 The Health Belief model proposes that the decision to vaccinate is a function of perceived susceptibility to and severity of disease as well as concern about vaccine benefits and risks.17,45
Lack of generalizability to the general population should also be noted since the study was institution-based and focused on a specific population. Furthermore, though a contingency valuation method is widely used to assess WTP, some authors hypothesize that biases can be introduced by the respondent’s lack of understanding of the contingent market.46 Moreover, establishing causal relationship between outcome and response variables may not be possible due to the cross-sectional nature of the study. Therefore, the findings of this study should be interpreted in light of the above-mentioned limitations.
Conclusions
Health-care workers’ willingness to pay for COVID-19 vaccination was found to be low. The median willingness to pay of HCWs was 400 ETB (US$10.04), considering a contingent valuation model (CVM) in double dichotomous format. Sex, income, affordability of the vaccine, fear of side effects, support for the vaccine, and perceived probability of acquiring COVID-19 infection were factors significantly associated with WTP for a COVID-19 vaccine.
Detailed health education and training about COVID-19 vaccines are required for sufficiency of information regarding their side effects, and efficacy to make informed decisions to enhance the willingness to pay for a COVID-19 vaccine. Moreover, the government should consider vaccine price subsidies in order to attain adequately high vaccination coverage.
Data Sharing Statement
Data that support the findings are available from the corresponding author on reasonable request.
Acknowledgments
The authors would like to thank Haramaya University College of Health and Medical Sciences for providing the opportunity to conduct this study and for intellectual and technical support throughout the work. We are also grateful to study participants, data collectors, and supervisors who were involved in the survey.
Author Contributions
All authors contributed to conception and design of the study, acquisition of data, data analysis and interpretation, drafting and revising the manuscript, agreed on the journal to which the article would be submitted, gave their final approval for submission and the version to be published, and agreed to be accountable for all aspects of the work.
Funding
No external funding was received.
Disclosure
The authors declared that they have no conflicts of interest for this work.
References
1. Wu F, Zhao S, Yu B, et al. A new coronavirus associated with human respiratory disease in China. Nature. 2020;579(7798):265–269. doi:10.1038/s41586-020-2008-3
2. Umakanthan S, Sahu P, Ranade AV, et al. Origin, transmission, diagnosis and management of coronavirus disease 2019 (COVID-19). Postgrad Med J. 2020;96(1142):753–758. doi:10.1136/postgradmedj-2020-138234
3. Chan JF-W, Yuan S, Kok K-H, et al. A familial cluster of pneumonia associated with the 2019 novel coronavirus indicating person-to-person transmission: a study of a family cluster. Lancet. 2020;395(10223):514–523. doi:10.1016/S0140-6736(20)30154-9
4. Suryavanshi N, Kadam A, Dhumal G, et al. Mental health and quality of life among healthcare professionals during the COVID‐19 pandemic in India. Brain Behav. 2020;10(11):e01837. doi:10.1002/brb3.1837
5. Serrano-Ripoll MJ, Meneses-Echavez JF, Ricci-Cabello I, et al. Impact of viral epidemic outbreaks on mental health of healthcare workers: a rapid systematic review and meta-analysis. J Affect Disord. 2020;277:347–357. doi:10.1016/j.jad.2020.08.034
6. Akande-Sholabi W, Adebisi YA. The impact of COVID-19 pandemic on medicine security in Africa: Nigeria as a case study. Pan Afr Med J. 2020;35(Suppl 2):54. doi:10.11604/pamj.supp.2020.35.2.23671
7. Abikoye TM. Collateral damage: the impact of the COVID-19 pandemic on the care of a patient with tuberculous neuroretinitis in Lagos, Nigeria. Pan Afr Med J. 2020;35(Suppl 2):664. doi:10.11604/pamj.supp.2020.35.2.24691
8. World Health Organization. Rational Use of Personal Protective Equipment for Coronavirus Disease ( COVID-19): Interim Guidance, 27 February 2020. World Health Organization; 2020.
9. Polack FP, Thomas SJ, Kitchin N, et al. Safety and efficacy of the BNT162b2 mRNA Covid-19 vaccine. N Eng J Med. 2020;383(27):2603–2615. doi:10.1056/NEJMoa2034577
10. Umakanthan S, Chauhan A, Gupta MM, Sahu PK, Bukelo MM, Chattu VK. COVID-19 pandemic containment in the Caribbean Region: a review of case-management and public health strategies. AIMS Public Health. 2021;8(4):665. doi:10.3934/publichealth.2021053
11. Yilma D, Mohammed R, Getahun Abdela S, et al. COVID‐19 vaccine acceptability among health care workers in Ethiopia: do we practice what we preach? Tropical Med Int Health. 2022;27(4):418–425. doi:10.1111/tmi.13742
12. WHO. Ethiopia: WHO Coronavirus Disease (COVID-19) Dashboard With Vaccination Data 2022. Available from: https://covid19.who.int/region/afro/country/et.
13. Sallam M, Al-Sanafi M, Sallam M, Global A. Map of COVID-19 Vaccine Acceptance Rates per Country: an Updated Concise Narrative Review. J Multidiscip Healthc. 2022;15:21. doi:10.2147/JMDH.S347669
14. Lazarus JV, Ratzan SC, Palayew A, et al. A global survey of potential acceptance of a COVID-19 vaccine. Nat Med. 2021;27(2):225–228. doi:10.1038/s41591-020-1124-9
15. MacDonald NE, Dubé E. Unpacking vaccine hesitancy among healthcare providers. EBioMedicine. 2015;2(8):792. doi:10.1016/j.ebiom.2015.06.028
16. Verger P, Fressard L, Collange F, et al. Vaccine hesitancy among general practitioners and its determinants during controversies: a national cross-sectional survey in France. EBioMedicine. 2015;2(8):891–897. doi:10.1016/j.ebiom.2015.06.018
17. Sadique MZ, Devlin N, Edmunds WJ, Parkin D. The effect of perceived risks on the demand for vaccination: results from a discrete choice experiment. PLoS One. 2013;8(2):e54149. doi:10.1371/journal.pone.0054149
18. Umakanthan S, Lawrence S. Predictors of COVID-19 vaccine hesitancy in Germany: a cross-sectional, population-based study. Postgrad Med J. 2022. doi:10.1136/postgradmedj-2021-141365
19. Berghea F, Berghea CE, Abobului M, Vlad VM. Willingness to Pay for a for a Potential Vaccine Against SARS-CoV-2/COVID-19 Among Adult Persons. 2020.
20. Culyer AJ. Encyclopedia of Health Economics. Newnes; 2014.
21. Deal K, Marshall D, Dabrowski D, Charter A, Bukoski M, Moayyedi P. Assessing the value of symptom relief for patients with gastroesophageal reflux disease treatment: willingness to pay using a discrete choice experiment. Value Health. 2013;16(4):588–598. doi:10.1016/j.jval.2013.01.007
22. Palanca-Tan R. The demand for a dengue vaccine: a contingent valuation survey in Metro Manila. Vaccine. 2008;26(7):914–923. doi:10.1016/j.vaccine.2007.12.011
23. Yeo HY, Shafie AA. The acceptance and willingness to pay (WTP) for hypothetical dengue vaccine in Penang, Malaysia: a contingent valuation study. Cost Effectiveness Resource Allocation. 2018;16(1):1–10. doi:10.1186/s12962-018-0163-2
24. Nguyen LH, Tran BX, Do CD, et al. Feasibility and willingness to pay for dengue vaccine in the threat of dengue fever outbreaks in Vietnam. Patient Prefer Adherence. 2018;12:1917. doi:10.2147/PPA.S178444
25. Muniz Junior RL, Godói IP, Reis EA, et al. Consumer willingness to pay for a hypothetical Zika vaccine in Brazil and the implications. Expert Rev Pharmacoecon Outcomes Res. 2019;19(4):473–482. doi:10.1080/14737167.2019.1552136
26. Harapan H, Mudatsir M, Yufika A, et al. Community acceptance and willingness-to-pay for a hypothetical Zika vaccine: a cross-sectional study in Indonesia. Vaccine. 2019;37(11):1398–1406. doi:10.1016/j.vaccine.2019.01.062
27. Bishai D, Pariyo G, Ainsworth M, Hill K. Determinants of personal demand for an AIDS vaccine in Uganda: contingent valuation survey. Bull World Health Organ. 2004;82:652–660.
28. Birhane MG, Miranda MEG, Dyer JL, Blanton JD, Recuenco S. Willingness to pay for dog rabies vaccine and registration in Ilocos Norte, Philippines (2012). PLoS Negl Trop Dis. 2016;10(3):e0004486. doi:10.1371/journal.pntd.0004486
29. García LY, Cerda AA. Contingent assessment of the COVID-19 vaccine. Vaccine. 2020;38(34):5424–5429. doi:10.1016/j.vaccine.2020.06.068
30. Nunes PALD. Contingent Valuation Method; 2022. Available from: http://www.coastalwiki.org/wiki/Contingent_Valuation_Method.
31. Sallam M. COVID-19 vaccine hesitancy worldwide: a concise systematic review of vaccine acceptance rates. Vaccines. 2021;9(2):160. doi:10.3390/vaccines9020160
32. Harapan H, Wagner AL, Yufika A, et al. Willingness-to-pay for a COVID-19 vaccine and its associated determinants in Indonesia. Hum Vaccin Immunother. 2020;16(12):3074–3080. doi:10.1080/21645515.2020.1819741
33. Wong LP, Alias H, Wong P-F, Lee HY, AbuBakar S. The use of the health belief model to assess predictors of intent to receive the COVID-19 vaccine and willingness to pay. Hum Vaccin Immunother. 2020;16(9):2204–2214. doi:10.1080/21645515.2020.1790279
34. Carpio CE, Sarasty O, Hudson D, Macharia A, Shibia M. The demand for a COVID-19 vaccine in Africa: evidence from Kenya. 2020.
35. Peretti-Watel P, Seror V, Cortaredona S, et al. A future vaccination campaign against COVID-19 at risk of vaccine hesitancy and politicisation. Lancet Infect Dis. 2020;20(7):769–770. doi:10.1016/S1473-3099(20)30426-6
36. Alley SJ, Stanton R, Browne M, et al. As the pandemic progresses, how does willingness to vaccinate against cOVID-19 evolve? Int J Environ Res Public Health. 2021;18(2):797. doi:10.3390/ijerph18020797
37. Sarasty O, Carpio CE, Hudson D, Guerrero-Ochoa PA, Borja I. The demand for a COVID-19 vaccine in Ecuador. Vaccine. 2020;38(51):8090–8098. doi:10.1016/j.vaccine.2020.11.013
38. Catma S, Varol S. Willingness to Pay for a Hypothetical COVID-19 Vaccine in the United States: a Contingent Valuation Approach. Vaccines. 2021;9(4):318. doi:10.3390/vaccines9040318
39. Cerda AA, García LY. Willingness to Pay for a COVID-19 Vaccine. Appl Health Econ Health Policy. 2021;19(3):343–351. doi:10.1007/s40258-021-00644-6
40. Wagner AL, Boulton ML, Sun X, et al. Perceptions of measles, pneumonia, and meningitis vaccines among caregivers in Shanghai, China, and the health belief model: a cross-sectional study. BMC Pediatr. 2017;17(1):1–9. doi:10.1186/s12887-017-0900-2
41. Hussain A, Ali S, Ahmed M, Hussain S. The anti-vaccination movement: a regression in modern medicine. Cureus. 2018;10(7):65.
42. Ransing R, Dashi E, Rehman S, Chepure A, Mehta V, Kundadak GK. COVID-19 anti-vaccine movement and mental health: challenges and A way forward. Asian J Psychiatr. 2021;58:102614. doi:10.1016/j.ajp.2021.102614
43. Rajamoorthy Y, Radam A, Taib NM, et al. Willingness to pay for hepatitis B vaccination in Selangor, Malaysia: a cross-sectional household survey. PLoS One. 2019;14(4):e0215125. doi:10.1371/journal.pone.0215125
44. Harapan H, Wagner AL, Yufika A, et al. Acceptance of a COVID-19 vaccine in Southeast Asia: a cross-sectional study in Indonesia. Front Public Health. 2020;2:8.
45. Meszaros JR, Asch DA, Baron J, Hershey JC, Kunreuther H, Schwartz-Buzaglo J. Cognitive processes and the decisions of some parents to forego pertussis vaccination for their children. J Clin Epidemiol. 1996;49(6):697–703. doi:10.1016/0895-4356(96)00007-8
46. Hausman J. Contingent valuation: from dubious to hopeless. J Economic Perspectives. 2012;26(4):43–56. doi:10.1257/jep.26.4.43
 © 2022 The Author(s). This work is published and licensed by Dove Medical Press Limited. The full terms of this license are available at https://www.dovepress.com/terms.php and incorporate the Creative Commons Attribution - Non Commercial (unported, v3.0) License.
By accessing the work you hereby accept the Terms. Non-commercial uses of the work are permitted without any further permission from Dove Medical Press Limited, provided the work is properly attributed. For permission for commercial use of this work, please see paragraphs 4.2 and 5 of our Terms.
© 2022 The Author(s). This work is published and licensed by Dove Medical Press Limited. The full terms of this license are available at https://www.dovepress.com/terms.php and incorporate the Creative Commons Attribution - Non Commercial (unported, v3.0) License.
By accessing the work you hereby accept the Terms. Non-commercial uses of the work are permitted without any further permission from Dove Medical Press Limited, provided the work is properly attributed. For permission for commercial use of this work, please see paragraphs 4.2 and 5 of our Terms.
