Back to Journals » Advances in Medical Education and Practice » Volume 7
Proposed learning strategies of medical students in a clinical rotation in obstetrics and gynecology: a descriptive study
Received 8 March 2016
Accepted for publication 2 May 2016
Published 10 August 2016 Volume 2016:7 Pages 489—496
DOI https://doi.org/10.2147/AMEP.S108008
Checked for plagiarism Yes
Review by Single anonymous peer review
Peer reviewer comments 3
Editor who approved publication: Dr Md Anwarul Azim Majumder
Richard P Deane, Deirdre J Murphy
Department of Obstetrics and Gynecology, Trinity College Dublin, University of Dublin, Coombe Women & Infants University Hospital, Dublin, Republic of Ireland
Background: Medical students face many challenges when learning within clinical environments. How students plan to use their time and engage with learning opportunities is therefore critical, as it may be possible to highlight strategies that optimize the learning experience at an early stage in the rotation. The aim of the study was to describe the learning drivers and proposed learning strategies of medical students for a clinical rotation in obstetrics and gynecology.
Methods: A descriptive study of personal learning plans completed by students at the start of their clinical rotation in obstetrics and gynecology was undertaken. Data relating to students’ learning strategies were obtained from the personal learning plans completed by students. Quantitative and qualitative analyses were used.
Results: The desire to obtain a good examination result was the most significant reason why the rotation was important to students (n=67/71, 94%). Students struggled to create a specific and practical learning outcome relevant to their career interest. Target scores of students were significantly higher than their reported typical scores (P<0.01). Textbooks were rated as likely to be the most helpful learning resource during the rotation. Bedside tutorials were rated as likely to be the most useful learning activity and small group learning activities were rated as likely to be more useful than lectures. Most students intended to study the course material linked to their clinical program rather than the classroom-based tutorial program.
Conclusion: The main learning driver for medical students was academic achievement, and the proposed learning strategy favored by medical students was linking their study plans to clinical activities. Medical educators should consider strategies that foster more intrinsic drivers of student learning and more student-oriented learning resources and activities.
Keywords: academic performance, clinical learning environment, learning activities, learning plan, undergraduate
Previous letter has been published
Further letter has been published
Introduction
Learning in clinical environments is highly valued by medical students and their teachers.1 However, it is challenging and clinical teachers may underestimate the difficulties facing medical students.2 Medical curricula have evolved considerably with the introduction of new initiatives, for example, student electives.3 However, there has been a gradual reduction in the time available for many clinical rotations, including obstetrics and gynecology (OBGYN).4,5 Given the challenging nature of the clinical learning environment and shortened clinical rotations, students may only realize the most effective learning strategies at a late stage in the rotation, often beyond the point of remedy. Students’ perceptions of how best to learn during their clinical rotations have therefore become increasingly important. There has been little research into the mindset of students commencing clinical rotations. For medical educators, gaining an insight into these perceptions is relevant as it may be possible to highlight strategies that optimize the student learning experience at an early stage in the rotation.
The aim of the study was to describe the learning drivers and proposed learning strategies of medical students for a clinical rotation in OBGYN. The following research questions were addressed: Why is the rotation important to students? Can students create learning outcomes relevant to their future careers? What academic goals do students wish to achieve? What learning resources do students rate as likely to be most helpful? What learning activities do students rate as likely to be most helpful? How do students plan to study the course material?
Methods
Study setting
The study was conducted by the Department of OBGYN, Trinity College, University of Dublin based at the Coombe Women & Infants University Hospital. The undergraduate program in OBGYN is conducted in the penultimate year of a 5-year degree course in medicine and is 8 weeks in duration. There are four rotations during each academic year with ∼40 students in each rotation. For students undertaking the rotation, it is their first exposure to clinical OBGYN. The program consists of a combination of clinical and classroom-based learning activities. Students are assessed using a combination of written assessments (50 single best answer questions [20%] and six short answer questions [20%]) and practical assessments (eleven station objective structured clinical examination [20%] and a long case clinical examination [40%]). Criterion referenced standard setting is applied to each component of the examination. Raw scores are then converted to a standardized grading system used by the university. Students require an overall score of 50% to pass the examination and 60% to obtain a distinction. Scores above 70% and below 40% are rare. OBGYN is assessed as an individual subject and students must pass the examination in order to proceed into the final year.
Study design
This was a descriptive study of personal learning plans (PLPs) completed by students at the start of their clinical rotation in OBGYN. The PLPs were part of a separate cluster randomized control trial (RCT) evaluating the impact of a PLP supported by an induction meeting in undergraduate OBGYN that was conducted over a full academic year (2012–2013), which has been published previously.6 The intervention was the creation of a PLP by the medical student supported through an individual “one-to-one” induction education meeting between the student and an academic staff member during the first 2 weeks of the rotation. The purpose of the induction meeting was to support the creation of the PLP. Each student was asked to complete the PLP in advance of the induction meeting and the PLP created by the student was reviewed at the meeting. At the end of the induction meeting, each student had completed a PLP for the clinical rotation. The control group received a group presentation on how to optimize their learning experience during the rotation (but not a PLP or induction meeting). Institutional research ethics committee approval for the study was obtained (Trinity College Dublin Research Ethics Committee, approval October 2012).
Personal learning plan
The PLP was developed using Association for Medical Education in Europe guidance on the use of PLPs.7 The PLP contained a combination of open and closed questions. The PLP was an eight-page booklet divided into six sections (an example page is shown in Figure 1), as follows:
- Part 1 (importance of the OBGYN rotation) aimed to identify the main factors motivating students to learn during the rotation by asking them to reflect on the importance of the OBGYN rotation and rate a number of reasons commonly cited by students for undertaking the rotation, and add any additional reasons.
- Part 2 (relevance of the OBGYN rotation for future careers) aimed to provide relevance of the OBGYN rotation to their future careers by identifying their career interests and asking them to formulate a specific and practical learning outcome to be achieved during the OBGYN rotation that would be beneficial in their future careers.
- Part 3 (academic targets) aimed to define a specific academic target for students by asking them to consider their typical self-reported academic performance and the summary of grades distributions from the previous year.
- Part 4 (learning resources) aimed to ensure that students had identified their main learning resource by rating a series of commonly used resources during the rotation.
- Part 5 (learning activities) aimed to highlight strategies to maximize learning in the clinical learning environment and encourage student attendance by providing information on the positive impact of attendance on academic performance.
- Part 6 (study schedule) aimed to identify a strategy for learning during the rotation by asking students to create a study plan documenting the topics to be covered each week.
  | Figure 1 Page from personal learning plan booklet. |
Participants
Students who consented to participate in the intervention group of the previously described RCT were included in this study.6 For the RCT, each rotation during the year was defined as a separate cluster. Rotations 2 and 3 were selected for intervention (the PLP and induction meeting) and rotations 1 and 4 were selected for the control (group presentation without a PLP). All students within rotations 2 and 3 were invited to participate in the intervention. These students were supplied with a written information leaflet in advance of the rotation and given an explanatory presentation on the first day of the rotation. Analysis of the PLPs submitted by students formed part of this consent process. All students who provided written informed consent to participate were supplied with a blank PLP to complete and a date and time for their individual “one-to-one” induction meeting.
Data collection
Data relating to students’ learning strategies were obtained from the PLPs completed by the students prior to the induction meeting. At the induction meeting, the supervisor made a photocopy of each PLP and returned the original copy to the student. Data relating to student demographics (sex, age, country of origin) and previous end-of-year failure were obtained from departmental records. Previous end-of-year failure refers to failure in any of the end-of-year examinations during the student’s preceding 3 years on the medical course. A staff member separate from the research team coded all data before analysis (including the PLPs) to ensure confidentiality.
Data analysis
Descriptive statistics were used to summarize the student population and academic performance. The learning plans were analyzed using quantitative and qualitative analysis. Likert scales were characterized as ordinal scales and summarized using descriptive statistics. Students answering “don’t know” to any question were excluded from calculations of the mean and standard deviation. Qualitative data of free text comments within the learning plans were analyzed using content analysis. ATLAS.ti version 7 (Berlin, Germany) was used to assist content analysis. Codes for common themes were generated, and through a series of iterations, common themes were identified. A paired samples t-test was used to compare academic goals, that is, target scores, typical scores, and actual scores. Statistical Package for the Social Sciences version 22 (SPSS Inc., IBM Corporation, Armonk, NY, USA) was used for statistical analysis.
Results
Participant profile
Of the 73 students invited to participate in the study, 71 students (97%) consented and completed a PLP. Table 1 provides a summary of the demographic profile of these students.
  | Table 1 Student demographics |
Importance of the OBGYN rotation for students
Table 2 outlines student ratings of different reasons why the rotation may be important to them. Students rated the need for academic achievement as the most important reason. In addition, ten students listed other reasons: the personal relevance of OBGYN (three students), the application of OBGYN for a career in pediatrics (three students), the ability to provide OBGYN care in developing world settings (two students) and emergency settings (one student), and the lack of teaching of OBGYN during the earlier years of the course (one student).
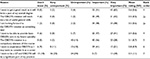  | Table 2 Importance of the OBGYN rotation to students Note: =, Joint. Abbreviations: GP, general practitioner; OBGYN, obstetrics and gynecology; SD, standard deviation. |
Relevance of OBGYN rotation to the student’s future career
Only 12 students (n=12/71, 17%) were planning on pursuing a career in OBGYN (Table 3). Of these students, only three students (n=3/12, 25%) were male. The majority of students defined a learning outcome related to their future career (n=52/71, 73.2%). Content analysis of these learning outcomes produced the following observations:
- Learning outcomes were generally generic and focused, for the most part, on history-taking and examination skills.
- Example: “Get very proficient with history taking skills and my examination skills,” student 17.
- Some wanted to use the rotation to further their communications skills.
- Example: “Demonstrate proficiency in case and topic presentation. Have awareness of verbal and non-verbal communication skills,” student 29.
- Although some students related their career aspirations to learning outcomes, the learning outcomes themselves were nonspecific.
  | Table 3 Student career plans |
Example: “I would like to understand birthing injuries etc. as these are very relevant in pediatrics. I find female health interesting and would like to understand more of hormonal influences,” student 19.
The majority of students defined a strategy to achieve their learning outcome (n=51/71, 71.8%). Content analysis of these learning outcomes produced the following observations:
- Most students identified attendance and participation or practice as their strategy.
Example 1: “Attend all the clinics, theatre, tutorials etc. plus read around the topic as much as possible,” student 15.
Example 2: “Practice. Study and read journals. Participate in surgery, clinics and labour ward. Watch videos – very helpful for me,” student 21.
Academic goals
The mean reported typical score (the score that the student usually achieves during his/her preceding years as reported by the student) was 61.0%±6.2% (range 50 to 70), the mean target score (the score the student was aiming to achieve as reported by the student) was 64.1%±4.4% (range 55 to 70). The mean difference between typical scores and target scores was +3.2%±4.7% (range −10 to +15) and was significant (P=0.000) (Figure 2). The majority of students (n=59/71, 83.1%) responded to a question asking them to define a “successful” rotation. The main divide was between students who defined success through academic achievement (n=30/71, 42.3%) and clinical competence (n=29/71, 40.8%). Only three students mentioned personal interest or enjoyment (n=3/71, 4.2%).
- Example (academic achievement): “I am results orientated so if I achieve my target academic achievement (ie, an honor),” student 51.
- Example (clinical competence): “I feel confident in managing the common presentations in OBGYN,” student 71.
- Example (personal interest or enjoyment): “Still interested in OBGYN by the end of the rotation,” student 25.
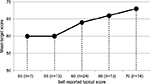  | Figure 2 Typical scores compared to mean target scores. |
Learning resources
Table 4 outlines student ratings of common learning resources used in OBGYN. Textbooks were rated as likely to be the most helpful learning activity during the rotation. All students opted to use the traditional textbook as their “primary” resource supplemented by information gathered at tutorials and clinical activities. In addition, students cited the following e-learning resources: Wikipedia (n=11), Medscape (n=6), YouTube (n=3), Google (n=2), Up-to-date (n=2), Geeky Medics (n=1), National Institute for Clinical Excellence (NICE) Guidelines (n=1), Royal College of Obstetricians and Gynaecologists (RCOG) Guidelines (n=1), Pubmed (n=1), One 2 One OBSGYN iphone app (n=1), and Medical Doctor (MD) Consult (n=1).
  | Table 4 Mean rating scores by students for the helpfulness of various learning resources and learning activities Note: =, Joint. Abbreviations: OBGYN, obstetrics and gynecology; SD, standard deviation. |
Learning activities
Table 4 outlines student ratings of common learning activities used in OBGYN. Students rated clinical activities with supervision higher than other clinical activities and small group tutorials higher than lectures.
Study strategies
In contrast to the other parts of the PLP, only 44 students (n=44/71, 62%) completed the study schedule within the PLP in advance of the induction meeting. The majority of students (n=38/44, 86%) created study schedules linked with their weekly clinical activities rather than the classroom-based lecture program (n=6/44, 14%). Students planned to use handwritten notes only (n=35/68, 52%), computer-typed notes only (n=5/68, 7%), the learning resource directly (n=4/68, 6%), or a combination of these approaches (n=24/68, 35%). A small number of students mentioned the use of study groups (n=2).
Discussion
Principal findings
The desire to obtain a good examination result was the most significant reason why the rotation was important to students. Students struggled to create a specific and practical learning outcome relevant to their career interest. Target scores of students were significantly higher than their reported typical scores. Textbooks were rated as likely to be the most helpful learning resource during the rotation. Bedside tutorials were rated as likely to be the most useful learning activity and small group learning activities were rated as likely to be more useful than lectures. Most students intended to study the course material linked to their clinical program rather than the classroom-based tutorial program.
Learning drivers
Motivation is a continuum of intrinsic motivation (ie, for personal interest) at one end of the spectrum, and extrinsic motivation (ie, to obtain a reward or to avoid a loss) and amotivation (ie, no motivation) at the other end of the spectrum.8 As a person matures from pedagogy to andragogy, motivation shifts from extrinsic to intrinsic.9 While recognizing the critical role of extrinsic motivation in achievement, medical educators hope instinctively that their students are fundamentally intrinsically motivated.10,11 In this study, students who rated achieving a good result highly, were unable to create a learning outcome relevant to their future career, and wanted to perform better academically than their typical performance. The main motivators for students were therefore extrinsic rather than intrinsic and students viewed their learning in terms of short-term academic success rather than long-term clinical application. This may reflect the pressure on medical students to succeed academically in order to secure postgraduate posts as rankings are used to select candidates for these posts in Ireland and the UK.12 Although there will always be a need for extrinsic motivators, these findings suggest that medical educators should consider strategies of fostering more intrinsic drivers of student learning.
Proposed learning strategies
Clinical teaching, defined as teaching in the presence of a patient, is considered an enormously beneficial “active” learning process for medical students.1 However, medical educators are concerned over the gradual decline in clinical teaching.13,14 Some students struggle in adapting to learn within the clinical learning environment and become overwhelmed.2 In this study, most students intended to study the course material linked to their clinical activities rather than the classroom-based lecture program. In relation to clinical activities, students expected activities focused toward themselves (eg, bedside tutorials) to be more useful than less focused activities (eg, operating theater). The finding that students intended to link learning strategies to clinical experience is desirable. However, a concern with this approach is the potential for patchy and haphazard coverage of the curriculum. The low rating of less student-focused learning activities (eg, ward work) suggests the inability of some students to self-direct their learning in clinical settings. Medical educators should continue to encourage students to link their learning to their clinical experiences. However, medical educators should also provide students with learning resources to allow students to complete the relevant theoretical topics alongside their clinical activities, for example, e-learning modules.
Strengths
In this study, the focus was on students’ perspectives at the start of a clinical rotation in OBGYN. Students undertaking this rotation have already completed a full year of clinical rotations in medicine and surgery. This enhanced the findings, as they were based on real previous experiences of learning in clinical environments. The high completion rate of the PLP ensured more representative findings. The fact that the PLP was supported by an induction meeting encouraged its completion by students.
Limitations
The study did not evaluate whether students actually used the proposed strategies during their rotation and the effect of these strategies on their learning. However, the aim of the study was to gain an insight into the students’ mindset at the start of a clinical rotation. Students may have completed the learning plan at any stage before their meeting, as the learning plan was collected as part of the induction meeting, although all meetings were held within the first 10 days. Some of the findings may be limited to the specialty of OBGYN. For example, the identification of academic success as the most important aspect of the rotation may not be replicated in specialties that are perceived as more mainstream. Given that the study was conducted at a single institution, the generalizability of some of the findings may be limited.
Implications for academic practice and future research
This study has identified a number of students’ perceptions regarding their learning during a clinical rotation that are of concern, for example, the low rating of self-directed learning on wards. Medical educators should consider these perceptions carefully and potential strategies to address them, for example, the enhancement of self-directed learning skills. In addition, medical educators should also consider strategies to encourage more intrinsic drivers of student learning. Future research should evaluate the actual strategies employed by students during the rotation and an enhanced PLP based on these strategies. As this study describes findings in relation to a specific specialty in a single institution, it would be important to establish if similar findings exist in other specialties and institutions.
Conclusion
The main learning driver for medical students was academic achievement, and the proposed learning strategy favored by medical students was linking their study plans to clinical activities. Medical educators should consider strategies that foster more intrinsic drivers of student learning and more student-oriented learning resources and activities.
Acknowledgments
We wish to acknowledge the many medical students who generously gave their time to participate in this study. We are indebted to Prof Patricia Crowley, Professor of Obstetrics and Gynaecology, and Ms Cristina Boccado, Executive Officer, Department of OBGYN, Trinity College Dublin, for their support of this study. We are grateful to Prof Martina Hennessy, Director of Undergraduate Teaching and Learning, Trinity College Dublin, for her advice and support.
Author contributions
All authors contributed toward data analysis, drafting, and critically revising the paper, and agreed to be accountable for all aspects of the work.
Disclosure
The authors report no conflicts of interest in this work.
References
Ramani S, Leinster S. AMEE guide No. 34: Teaching in the clinical environment. Med Teach. 2008;30(4):347–364. | ||
O’Brien B, Cooke M, Irby DM. Perceptions and attributions of third-year student struggles in clerkships: do students and clerkship directors agree? Acad Med. 2007;82(10):970–978. | ||
Riley SC. Student Selected Components (SSCs): AMEE guide no 46. Med Teach. 2009;31(10):885–894. | ||
Edwards RK, Davis JD, Kellner KR. Effect of obstetrics-gynecology clerkship duration on medical student examination performance. Obstet Gynecol. 2000;95(1):160–162. | ||
Higham J. Current themes in the teaching of obstetrics and gynaecology in the United Kingdom. Med Teach. 2006;28(6):495–496. | ||
Deane RP, Murphy DJ. Impact of a personal learning plan supported by an induction meeting on academic performance in undergraduate obstetrics and gynaecology: a cluster randomised controlled trial. BMC Med Educ. 2015;15(1):43. | ||
Challis M. AMEE medical education guide no. 19: Personal learning plans. Med Teach. 2000;22(3):225–236. | ||
Kusurkar RA, Ten Cate TJ, Van Asperen M, Croiset G. Motivation as an independent and a dependent variable in medical education: a review of the literature. Med Teach. 2011;33(5):e242–e262. | ||
Knowles M. The Adult Learner: A Neglected Species. Houston, TX: Gulf Publishing; 1978. | ||
Kusurkar RA, Croiset G, Mann KV, Custers E, Ten Cate O. Have motivation theories guided the development and reform of medical education curricula? A review of the literature. Acad Med. 2012;87(6):735–743. | ||
Kusurkar RA, Croiset G, Ten Cate TJ. Twelve tips to stimulate intrinsic motivation in students through autonomy-supportive classroom teaching derived from self-determination theory. Med Teach. 2011;33(12):978–982. | ||
Foundation Programme, Applicants Handbook 2016 [Internet]. The Foundation Programme; 2015. Available from: http://www.foundationprogramme.nhs.uk/pages/home. Accessed June 16, 2016. | ||
Salam A, Halizah Siraj H, Mohamad N, Das S, Yousuf R. Bedside teaching in undergraduate medical education: issues, strategies, and new models for better preparation of new generation doctors. Iran J Med Sci. 2011;36(1):1–6. | ||
Qureshi Z. Back to the bedside: the role of bedside teaching in the modern era. Perspect Med Educ. 2014;3(2):69–72. Available from: http://link.springer.com/10.1007/s40037-014-0111-6. |
 © 2016 The Author(s). This work is published and licensed by Dove Medical Press Limited. The full terms of this license are available at https://www.dovepress.com/terms.php and incorporate the Creative Commons Attribution - Non Commercial (unported, v3.0) License.
By accessing the work you hereby accept the Terms. Non-commercial uses of the work are permitted without any further permission from Dove Medical Press Limited, provided the work is properly attributed. For permission for commercial use of this work, please see paragraphs 4.2 and 5 of our Terms.
© 2016 The Author(s). This work is published and licensed by Dove Medical Press Limited. The full terms of this license are available at https://www.dovepress.com/terms.php and incorporate the Creative Commons Attribution - Non Commercial (unported, v3.0) License.
By accessing the work you hereby accept the Terms. Non-commercial uses of the work are permitted without any further permission from Dove Medical Press Limited, provided the work is properly attributed. For permission for commercial use of this work, please see paragraphs 4.2 and 5 of our Terms.
