Back to Journals » Clinical Ophthalmology » Volume 17
Prevalence and Factors Associated with Suicidal Ideation Among Older People with Visual Impairments Attending an Eye Center During the COVID-19 Pandemic: A Hospital-Based Cross-Sectional Study
Authors Tantirattanakulchai P , Hounnaklang N , Pongsachareonnont PF , Khambhiphant B, Win N , Tepjan S
Received 29 December 2022
Accepted for publication 16 March 2023
Published 19 March 2023 Volume 2023:17 Pages 917—930
DOI https://doi.org/10.2147/OPTH.S403003
Checked for plagiarism Yes
Review by Single anonymous peer review
Peer reviewer comments 2
Editor who approved publication: Dr Scott Fraser
Pankaew Tantirattanakulchai,1 Nuchanad Hounnaklang,1 Pear Ferreira Pongsachareonnont,2,3 Bharkbhum Khambhiphant,4 Nanda Win,1 Suchon Tepjan5
1College of Public Health Sciences, Chulalongkorn University, Bangkok, Thailand; 2Center of Excellence in Retina, Faculty of Medicine, Chulalongkorn University, Bangkok, Thailand; 3King Chulalongkorn Memorial Hospital, Bangkok, Thailand; 4Department of Ophthalmology, Faculty of Medicine, Chulalongkorn University, Bangkok, Thailand; 5VOICES-Thailand Foundation, Chiang Mai, Thailand
Correspondence: Nuchanad Hounnaklang, College of Public Health Sciences, Chulalongkorn University, Institute Building 2-3, Soi Chulalongkorn 62, Phyathai Road, Pathumwan, Bangkok, 10330, Thailand, Tel +66 2218 8205, Fax +66 2255 6046, Email [email protected]
Purpose: To evaluate the prevalence of suicidal ideation and associated factors among older people with visual impairments attending an eye center during the COVID-19 pandemic.
Patients and Methods: A total of 314 older people aged 60 and above with visual impairments who attended an eye center were included in this study. This was a hospital-based cross-sectional study conducted from February to July, 2022. Data were collected in person. Suicidal ideation was measured using the Columbia–Suicide Severity Rating Scale (C-SSRS). Multivariable logistic regression analysis was used to explore associations between related factors and suicidal ideation.
Results: Of 314 older people with visual impairments, the prevalence of suicidal ideation was 32.5%. Suicidal ideation was independently associated with diabetic retinopathy (adjusted odds ratio (AOR)=2.4, 95% confidence interval (CI): 1.0– 5.8; p=0.038) and depression (AOR=6.3, 95% CI: 3.5– 11.2; p< 0.001).
Conclusion: This study found a relatively high prevalence of suicidal ideation among older people with visual impairments. There was also a significant association between depression and suicidal ideation among these individuals. Visual impairments can lead to negative émotions. This underscores the importance of addressing the mental health needs of older individuals with visual impairments, including suicide prevention efforts tailored to their needs. Ophthalmologists should be equipped with the skills necessary to identify the early signs of suicidal ideation and refer patients to mental healthcare specialists for appropriate treatment.
Keywords: older people, visual impairment, suicidal ideation, depression, COVID-19
Introduction
The World Health Organization officially declared the novel coronavirus disease (COVID- 19) outbreak a global pandemic on 11 March 2020.1 The COVID-19 pandemic has had a significant impact on people’s lives, influencing their behaviors and physical and mental health. The pandemic has resulted in social isolation, restrictions on physical and social contact, fear of illness, and the loss of loved ones.2 It has been well documented that quarantines and self-isolation can worsen anxiety, depression, loneliness, and insomnia, and even lead to suicidal behavior.3 The COVID-19 pandemic and its resulting shutdowns have presented numerous challenges to patients with visual impairments who are seeking eye care, particularly in emergency situations and at healthcare facilities that are unable to provide services.4
The growing and aging of the global population has resulted in an increased number of individuals with moderate or severe visual impairment. Visual impairment among older people is a significant health concern, as normal eye function declines and the risk of developing eye-related diseases or conditions increases with age. Previous research has shown that age is the most significant predictor of blindness and visual impairment.5,6
The high prevalence of visual impairment among older people and has become a significant public health issue.7,8 There are at least 2.2 billion people with visual impairments globally, with the majority being over 50 years old.9 The 2000 US Census estimated that 0.78% of older Americans were blind and an additional 1.98% Americans had low vision.10 Previous population-based cross-sectional studies have reported an overall estimated prevalence of visual impairment of 2.14%, and an overall estimated prevalence of blindness of 0.68%.11
In a study from the English Longitudinal Study of Ageing, 11.9% of a representative sample of older men and women in England had poor overall eyesight and 8.6% had poor eyesight up close.12 Moreover, a cross-sectional analysis of a dataset of registered patients aged 65 years and above in Scotland, UK reported a prevalence of visual impairment of 1.8%.13
According to the World Health Organization, the prevalence of visual impairment was 5.5% in China, 5.3% in India, and 4.8% in Southeast Asia.14 A study using data from the 2010 Thailand National Census found that the prevalence of blindness, severe visual impairment, and moderate visual impairment among individuals over 50 years old was 0.6%, 1.3%, and 12.6%, respectively.15
Visual impairment, including blindness, has a significant economic impact. According to the 2017 Global Burden of Disease (GBD), visual impairment ranked as the third leading cause of disability-adjusted life years. Previous research has estimated that the global financial burden of visual impairment ranged from US$ 0.1 billion in Honduras to as much as US$ 16.5 billion in the United States. These costs are largely due to productivity losses and the impact of visual impairment on employment.16,17
Visual impairment and blindness can have a significant impact on mental health and societal burden. Visual impairment has been linked to an increased risk of developing depressive symptoms and can lead to a variety of negative physical and psychological health effects, including social function and quality of life.18,19 These negative effects can include reduced morale, depression, social isolation, reduced self-esteem, diminished emotional security, lower levels of social interaction, and an increased risk of suicide.20,21 Visual problems are common among those over 60 years of age, and the rate of suicide and suicidal ideation increases with age.22,23
Suicide is a tragic event that affects families, communities, and entire countries, and has long-lasting effects on those who are left behind. Suicide is a leading cause of death and disability worldwide, and can occur at any stage of life.24 Suicidal ideation is an uncommon engrossment with thoughts of suicide.25 Suicide has become a major public health concern among people who are visually impaired. A previous study illustrated that visual impairment has a direct effect on suicide20 and the mortality rate of visually impaired people has increased raised significantly.26 The estimated incidence visually impaired people who committed suicide was 28.3.20
Studies have shown that older people who are visually impaired have a higher risk of suicidal ideation than those without a visual impairment.23,27 Suicidal ideation is also often associated with demographics, socioeconomic status, living conditions, health risk behaviors, chronic illness, adverse life events, social support, quality of life, and depression.28,29
Depression is the most common risk factor for suicide.30 Older adults with depression have a higher prevalence of suicidal ideation. More severe depression has been associated with increased suicidal ideation.31
Although many studies have investigated depression in older adults with visual impairments, few have focused on the suicidality of this group. This study aimed to evaluate the prevalence of suicidal ideation and associated factors among older people with visual impairments who attended an eye center during the COVID-19 pandemic.
Materials and Methods
Study Design, Period and Setting
A hospital-based cross-sectional study was conducted in person from February and July 2022 at the eye center of King Chulalongkorn Memorial Hospital in Bangkok, Thailand.
Study Participants and Eligibility Criteria
Study participants were older people aged 60 and above with visual impairments who attended the eye center during the data collection period. Inclusion criteria were ophthalmic patients with a Snellen visual acuity worse than 6/12 (20/40) in their best eye. Patients were Thai native speakers, willing to participate in the study, and were able to provide informed consent. Patients with auditory deficits and dementia were excluded.
Of the 325 patients who volunteered to participate in this study, 7 patients were excluded due to auditory deficits and 4 patients were excluded due to dementia. There were no additional drop-outs before participants completed all measures.
Measures
Socio-Demographic Characteristics
Participants were asked to report their socio-demographic characteristics (age, religion, education level, monthly income) and health status (eye diseases, duration of having eye diseases, physical illnesses, smoking, alcohol consumption, and prior COVID-19 infection).
Center for Epidemiological Studies-Depression (CES-D) Scale
The Center for Epidemiological Studies-Depression (CES-D) scale in Thai32 used in this study included a 20-item metric for assessing depression symptoms. Study participants were invited to provide information concerning how often they had experienced depression symptoms during the previous week. Answers were reported using a 4-point Likert scale from 0–3, where 0 indicated rarely or never and 3 indicated almost all the time. CES-D scores are rated from 0 to 60, with a cut-off point at 16. The Cronbach’s α of this metric was 0.89.
Columbia–Suicide Severity Rating Scale (C-SSRS)
The Columbia–Suicide Severity Rating Scale (C-SSRS) in Thai33 was used to assess suicidal ideation. The C-SSRS included a 5-item (1. wish to be dead, 2. non-specific active suicidal thoughts, 3. active suicidal ideation without any methods (not planned) without an intent to act, 4. active suicidal ideation with some intent to act, without a specific plan and 5. active suicidal ideation with a specific plan and an intent to act) with binary answers (yes/no). Score ranged from 0 and 5. Participants with scores greater than 0 were considered to have suicidal ideation. The Cronbach’s α of this metric was 0.84.
Statistical Analysis
Data were assessed using Statistical Package for the Social Sciences version 28.0. A descriptive analysis was performed to evaluate the characteristics of older people with impaired vision and to determine the extent to which suicidal ideation occurred. The relationships between related factors and suicidal ideation were evaluated using bivariate logistic regression. A multivariable logistic regression model was created using those variables whose p-value measured <0.2 in the bivariate regression. A p-value of less than 0.05 was considered statistically significant, and an AOR (adjusted odds ratio) was calculated with a 95% confidence interval (CI).34–37
Post hoc analysis was used to investigate interactions between diabetic retinopathy and depression. C-SSRS was utilized as a dichotomous variable. Post hoc analysis was used to investigate which individual items were more commonly endorsed by the depressed group vs the non-depressed group, and which individual items were more commonly endorsed by those with vs without diabetic retinopathy.
Results
Socio-Demographic Characteristics of the Study Participants
A total of 314 older people with visual impairment were included in this study, of whom the prevalence of suicidal ideation was 32.5%. Participant ages ranged from 60 and 96 years, with a mean age of 71.42 years (SD 7.83). The majority of participants were female (58.6%), Buddhist (94.3%), married (50.6%), had a primary school degree education (44.3%), and had no income (38.5%) (Table 1).
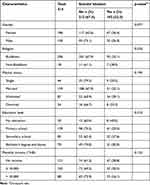 |
Table 1 Socio-Demographic Characteristics of Older People with Visual Impairments Attending an Eye Center During the COVID-19 Pandemic (n=314) |
Clinical Characteristics of the Study Participants
Most of participants had no macular degeneration (61.8%), had cataracts (59.6%), did not have diabetic retinopathy (74.2%) or glaucoma (79.9%), had eye disease for 2–5 years (38.5%), did not have diabetes (57.3%) hypertension (67.8%), or kidney disease (90.4%), were non-smokers (72.6%) and non-drinkers (64.3%), had no history of COVID-19 infection (88.2%), and were not depressed (68.2%) (Table 2).
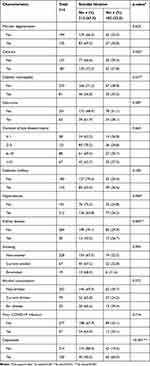 |
Table 2 Clinical Characteristics of Older People with Visual Impairments Attending an Eye Center During the COVID-19 Pandemic (n=314) |
Factor Associated with Suicidal Ideation Among the Study Participants
In the bivariable logistic regression analysis, participants with cataracts were 0.5 times more likely to have suicidal ideation compared with those without cataracts (OR= 0.5, 95% CI: 0.36–0.95). Participants with diabetic retinopathy were 1.8 times more likely to have suicidal ideation compared with those without diabetic retinopathy (OR= 1.8, 95% CI: 1.11–3.18). Participants with hypertension were 1.7 times more likely to have suicidal ideation compared with those without hypertension (OR= 1.7, 95% CI: 1.01–2.92). Participants with kidney disease were 3.0 times more likely to have suicidal ideation compared with those without kidney disease (OR= 3.0, 95% CI: 1.42–6.58). Participants with depression were 6.1 times more likely to have suicidal ideation compared with those without depression (OR= 6.1, 95% CI: 3.54–10.36) (Table 3).
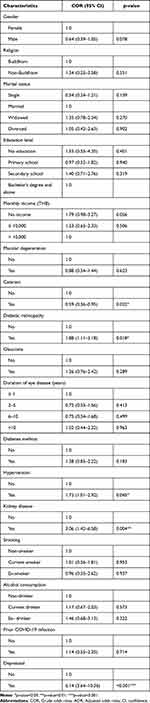 |
Table 3 Bivariate Logistic Regression of Factors Associated with Suicidal Ideation in Older People with Visual Impairment Attending an Eye Center During the COVID-19 Pandemic |
In the multivariable logistic regression analysis, after adjusting for cataracts, hypertension, and kidney disease, participants with diabetic retinopathy were 2.4 times more likely to have suicidal ideation compared with those without diabetic retinopathy (AOR= 2.4, 95% CI: 1.05–5.85). Moreover, depressed participants were 6.3 times more likely to be at risk of suicidal ideation than those without depression (AOR= 6.3, 95% CI: 3.56–11.28) (Table 4).
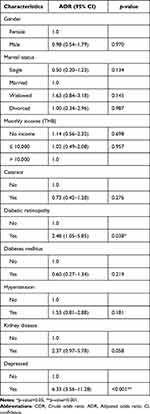 |
Table 4 Multivariable Binary Logistic Regression of Factors Associated with Suicidal Ideation in Older People with Visual Impairments Attending an Eye Center During the COVID-19 Pandemic |
Post Hoc Logistic Regression Analysis
The interaction effect between diabetic retinopathy and depression was found to be 7.1 times more likely to have suicidal ideation than those without diabetic retinopathy and depression (OR=7.1, 95% CI: 2.91–12.53).
According to the Columbia–Suicide Severity Rating Scale (C-SSRS), The interactions between diabetic retinopathy and depression impacted the participant’s wish to be dead (OR=7.1, 95% CI: 2.91–17.53), non-specific active suicidal thoughts (OR=4.2, 95% CI: 1.83–9.80); active suicidal ideation without any methods (not planned) without intent to act (OR=5.4, 95% CI: 2.27–13.02) and active suicidal ideation with some intent to act, without a specific plan (OR=4.7, 95% CI: 1.56–14.66).
Diabetic retinopathy alone was found to impact the participant’s wish to be dead (OR=1.8, 95% CI: 1.11–3.18) and active suicidal ideation with a specific plan and intent (OR=7.5, 95% CI: 1.44–39.97).
Depression was found to impact the participant’s wish to be dead (OR=6.1, 95% CI: 3.64–10.36); non-specific active suicidal thoughts; (OR=5.3, 95% CI: 32.83–10.14); active suicidal ideation with any methods (not planned) without an intent to act (OR=5.9, 95% CI: 2.83–12.32), and active suicidal ideation with some intent to act, without a specific plan (OR=12.4, 95% CI: 3.50–43.97) (Table 5).
 |
Table 5 Post Hoc Logistic Regression Analysis |
Discussion
This study identified the risk factors for suicidal ideation in older people with visual impairments who attended an eye center in Bangkok, Thailand during the COVID-19 pandemic. Our findings indicated that diabetic retinopathy is associated with suicidal ideation. Moreover, depression significantly increased the risk of having suicidal ideation.
Our findings indicate that one-third of older people with visual impairments (32.5%) experienced suicidal ideation. This result was higher than figures reported by a produced in the United States from 2015 and 2019,38 England’s 2014 Adult Psychiatric Morbidity Survey,39 and data from Mexico, India, Ghana, and Russia between 2007 and 2010,27 which reported rates of 9.0%, 7.9%, 7.6%, 6.7%, 4.0%, and 2.7%, respectively.
Based on population-based surveys performed over the past 8 years, the prevalence of suicidal ideation lies between 7.9% and 9.0%.38,39 However, a survey of older adults over the past 15 years found that this prevalence lies between 2.7% and 7.6%.27 It is highly possible that our increased rates were because this hospital-based survey was primarily performed on an older adult population.
Retinitis pigmentosa is a leading cause of visual impairment and blindness. The suicidal ideation rate among patients with retinitis pigmentosa is 38.5%, which is higher than the findings of our study.40 Further, the prevalence of suicide ideation found in our study was lower than the rate of 50.5% reported by a study conducted in Finland on suicide among visually impaired people aged 65 years and older.26
It is well established from different population-based studies that visual impairment is associated with increased mortality. Different levels of visual impairment may lead to psychological changes that over time increase the risk of death.41 When compared to patients with low or moderate levels of visual impairment, those severe visual impairment and blindness were more likely to develop suicidal ideation (1.8, 1.5, and 1.7 times, respectively). Diabetic retinopathy is a common complication of diabetes mellitus and is a major cause of vision loss in elderly people. One-third of people with diabetes have diabetic retinopathy. The most relevant risk factors for the development of diabetic retinopathy are disease duration, poor glycemic control, and the presence of hypertension.42 Our study found that the proportion of patients with diabetes mellitus who had diabetic retinopathy was 59.7%.
Previous works have verified the high prevalence and negative effects of depression in patients with diabetic retinopathy.43 We found that the proportion of patients with diabetic retinopathy who had depression was 33.3%.
In light of interaction between diabetic retinopathy and depression, it can be clarified that both diabetic retinopathy and depression impact suicidal ideation. Visual loss in patients with diabetic retinopathy is significantly related to depression. The progression of diabetic retinopathy can also lead to depression, whereas depressive symptoms often worsen diabetic retinopathy.43 Comorbid depression in patients with diabetic retinopathy aggravates retinopathy and increases the financial burden on the patient, the majority of whom were non-income earners. Interestingly, fear of blindness and the potential adverse effects of diabetic retinopathy treatment can lead to depression and suicidal ideation.44
Our study found that 43.2% of patients with diabetic retinopathy experienced suicidal ideation. After adjusting for covariates, patients with diabetic retinopathy were 2.4 times more likely to be at risk of suicidal ideation than those without diabetic retinopathy. Furthermore, patients with both diabetic retinopathy and depression were 7.1 times more likely to have suicidal ideation than those without diabetic retinopathy and depression.
Given its increased prevalence in the aging population, suicide among older people has become a major global problem.45 After controlling for gender, marital status, monthly income, cataract, diabetic retinopathy, diabetes mellitus, hypertension, and kidney disease, we found that older people with impaired vision and depression were 6.3 times more likely to have suicidal ideation than those without depression. This finding is supported by a previous work that found that depression was a key contributor to suicidal ideation in the older adults.46
The COVID-19 pandemic has led to a significant loss of human life worldwide and poses an unprecedented challenge to public health. It has increased suffering, damaged the economy, disrupted the lives of billions of people globally, and had a major impact on health, economics, the environment, and society.47
According to “Coronavirus disease 2019 (COVID-19) WHO Thailand Situation Report in February 2022”, Bangkok continues to report a higher number of COVID cases each day. The average number of new COVID-19 cases reported per day in Bangkok over the past week was 27% higher than that of the week prior. The number of cases reported on 9 February 2022 was the highest since 20 September 2021.
The number of patients with COVID-19 skyrocketed during the study period. The governor issued a statement limiting gatherings of more than 5 people, enforced strict legal measures by communicable disease officials under the Communicable Diseases Act 2015, and ordered the public to refrain from performing non-essential activities. Organizers could request to cancel or postpone events. These measures were to make it possible to control the outbreak.
Infections continue to rise in both industrial facilities and educational institutions. New disease strains also increase spread. Some individuals who were infected during the first wave were reinfected. Schools have also opened for on-site instruction, allowing for more school children to become infected and spread COVID-19 to their family. The disease control and disease prevention measure enforcement period has been extended, and all types of entertainment venues, including pubs, bars, and karaoke shops nationwide are to remain closed during this period.
People are continually infected with COVID-19. Consequently, the study setting, King Chulalongkorn Memorial Hospital, Bangkok, Thailand reduced its outpatient services by 50%. All patients were screened for COVID-19, and patient visitation was restricted for all wards.
Older people with visual impairments may have a higher risk of suicidal ideation and behavior due to other factors, such as unemployment, cognitive problems, depression, anxiety, stress, sleep problems, mobility limitations, loneliness, lack of social participation, disability and poor self-related health.27,48 Some older people adapt to visual loss by adopting a resilient attitude and positive coping skills. However, others struggle to accept and adapt to their visual loss and are at risk of depression. A previous study reported that depression is the most important factor associated with suicidal ideation among older people.45 In line with these findings, a previous study focusing on suicide in the older people found that having a visual impairment and a history of major depression increased the risk of suicide.49 In contrast, supportive relationships with family members have been shown to have a positive influence on those with visual impairments, and can help to improve their adaptation to visual loss, increase their life satisfaction, and reduce depressive symptoms.16
Further studies should focus on variables that affect the mental health, and well-being of older people with visual impairments. These may include qualitative investigations to identify ways to prevent the risk factors discussed in this paper from leading to suicidal ideation. It is also important to promote interventions that can reduce the incidence of suicidal ideation among older people with visual impairments who are from different cultural and socioeconomic backgrounds. Comparative studies set in the community and in different clinical contexts may also provide valuable insights.
In terms of public health policy and practice, caregivers should be encouraged to employ screening tools to identify depression and suicidal ideation at an early stage. This can allow caregivers to assist patients by discussing the significant risk factors for suicidal ideation and implement preventive measures and coping strategies. Given the pandemic’s negative impact on mental health, it is important for governments to prioritize care for older people who have already experienced suffering or emotional harm.
This study has a number of limitations that must be taken into consideration. First, a cross-sectional study design was used to infer the nature of the association between predictor variables and suicidal ideation. Second, this study only collected hospital-based data, and is not likely to be representative of the overall visually impaired population. Third, only a small proportion of individuals with visual impairments were included in the present study. The present study also has some notable strengths. Its most prominent benefit is that it provides new evidence supporting the interaction between diabetic retinopathy, depression, and suicidal ideation among older people with visual impairments. This relationship is important to consider when implementing health policies and designing public health interventions for the visually impaired.
Conclusion
This study demonstrates the association between associated factors and suicidal ideation in older people who are visually impaired. Suicidal ideation represents severe distress and is therefore a symptom that must be recognized and acted upon. Ophthalmologists must be able to recognize the early signs of suicidal ideation and be able to refer at risk patients to mental healthcare specialists. Management strategies may include frequent counseling and learning programs designed to support emotional health. These interventions may also focus on the different causes of visual impairment on suicide ideation, such as neurologic, renal, and cardiovascular disease. This approach is necessary to improve the mental health of older patients and to reduce the risk of suicidal ideation. Family members, friends, and other caregivers often play a vital role in providing physical, emotional, and social support for those with visual impairment.
Although Thailand has a universal health coverage (UHC) for vision healthcare, only 30% of elderly people with blinding cataracts and severely poor vision who have undergone the surgery receive support. The UHC supports the cost of surgery for senile cataracts by providing a lump sum payment, but if the cost of the treatment exceeds that specified amount, the patient must bear this burden themselves. There is also support for the treatment of diabetic retinopathy in the form of a lump sum payment of approximately $115 per person per year in addition to coverage of the additional cost of laser treatment. Thailand requires that patients with diabetes mellitus have an eye examination at least once a year.50 Although there are policies that support the provision of services for elderly patients with eye diseases, few undergo surgery. Access to eye care services is also limited as ophthalmologists are mainly available at tertiary hospitals. Future government policy should raise awareness among this group and encourage them to use available services more frequently. There should also be a review of the costs of care for those with a low income, which can further compound the effects of vision loss on depression and suicidal ideation.
Data Sharing Statement
Data is available upon request to the corresponding author.
Ethics Approval
This study was approved by the Institutional Review Board (IRB) for Human Research at the Faculty of Medicine of Chulalongkorn University (COA No.1638/2021). In addition to protecting participant identities and maintaining confidentiality, written informed consent was obtained from all participants before the interview. This study was performed in accordance with the principles stated in the Declaration of Helsinki.
Acknowledgments
The authors would like to acknowledge the 100th Anniversary Chulalongkorn University Fund for Doctoral Scholarship and the 90th Anniversary Chulalongkorn University Fund (Ratchadapiseksomphot Endowment Fund) for supporting this study. I am also grateful to Ms. Reberta Adele Steer Huthart for her kind support during this study.
Disclosure
The authors report no conflicts of interest in this work.
References
1. World Health Organization. Statement on the second meeting of the International Health Regulations (2005) Emergency Committee regarding the outbreak of novel coronavirus (2019-nCoV). Geneva, Switzerland: World Health Organisation; 2020. Available from: https://www.who.int/news-room/detail/30-01-2020-statement-on-The-second-meeting-of-The-international-health-regulations-(2005)-emergency-committee-regarding-The-outbreak-of-novel-coronavirus-(2019-ncov.
2. Wang C, Pan R, Wan X, et al. Immediate psychological responses and associated factors during the initial stage of the 2019 coronavirus disease (COVID-19) epidemic among the general population in China. Int J Environ Res Public Health. 2020;17(5):1729. doi:10.3390/ijerph17051729
3. Silișteanu SC, Totan M, Antonescu OR, et al. The impact of COVID-19 on behavior and physical and mental health of Romanian college students. Medicina. 2022;58(2):246. doi:10.3390/medicina58020246
4. Shalaby WS, Odayappan A, Venkatesh R, et al. The impact of COVID-19 on individuals across the spectrum of visual impairment. Am J Ophthalmol. 2021;227:53–65. doi:10.1016/j.ajo.2021.03.016
5. GBD 2019 Blindness and Vision Impairment Collaborators, Vision Loss Expert Group of the Global Burden of Disease Study. Causes of blindness and vision impairment in 2020 and trends over 30 years, and prevalence of avoidable blindness in relation to VISION 2020: the Right to Sight: an analysis for the Global Burden of Disease Study. Lancet Glob Health. 2021;9(2):e144–e160. doi:10.1016/S2214-109X(20)30489-7
6. Loh KY, Ogle J. Age related visual impairment in the elderly. Med J Malaysia. 2004;59(4):562–568.
7. Jones GC, Rovner BW, Crews JE, et al. Effects of depressive symptoms on health behavior practices among older adults with vision loss. Rehabil Psychol. 2009;54(2):164–172. doi:10.1037/a0015910
8. Ribeiro MV, Hasten-Reiter Júnior HN, Ribeiro EA, et al. Association between visual impairment and depression in the elderly: a systematic review. Arq Bras Oftalmol. 2015;78(3):197–201. doi:10.5935/0004-2749.20150051
9. World Health Organization. Blindness and vision impairment; 2021. Available from: https://www.who.int/news-room/fact-sheets/detail/blindness-and-visual-impairment.
10. Congdon N, O’Colmain B, Klaver CC, et al.; Eye Diseases Prevalence Research Group. Causes and prevalence of visual impairment among adults in the United States. Arch Ophthalmol. 2004;122(4):477–485. doi:10.1001/archopht.122.4.477
11. Varma R, Vajaranant TS, Burkemper B, et al. Visual impairment and blindness in adults in the United States: demographic and geographic variations from 2015 to 2050. JAMA Ophthalmol. 2016;134(7):802–809. doi:10.1001/jamaophthalmol.2016
12. Jackson SE, Hackett RA, Pardhan S, et al. Association of perceived discrimination with emotional well-being in older adults with visual impairment. JAMA Ophthalmol. 2019;137(7):825–832. doi:10.1001/jamaophthalmol.2019.1230
13. Court H, McLean G, Guthrie B, et al. Visual impairment is associated with physical and mental comorbidities in older adults: a cross-sectional study. BMC Med. 2014;12:181. doi:10.1186/s12916-014-0181-7
14. World Health Organization, Regional Office for South-East Asia. 2012 Situation analysis of vision 2020 in the WHO South-East Asia Region. WHO Regional Office for South-East Asia; 2020.
15. Isipradit S, Sirimaharaj M, Charukamnoetkanok P, et al. The first rapid assessment of avoidable blindness (RAAB) in Thailand. PLoS One. 2014;9(12):e114245. doi:10.1371/journal.pone.0114245
16. World Health Organization. World report on vision. Geneva: World Health Organization; 2019. Available from: who.int.
17. Eckert KA, Carter MJ, Lansingh VC, et al. A simple method for estimating the economic cost of productivity loss due to blindness and moderate to severe visual impairment. Ophthalmic Epidemiol. 2015;22(5):349–355. doi:10.3109/09286586.2015.1066394
18. Fischer ME, Cruickshanks KJ, Klein BEK, et al. Multiple sensory impairment and quality of life. Ophthalmic Epidemiol. 2009;16(6):346–353. doi:10.3109/09286580903312236
19. van der Aa HP, Comijs HC, Penninx BW, et al. Major depressive and anxiety disorders in visually impaired older adults. Invest Ophthalmol Vis Sci. 2015;56(2):849–854. doi:10.1167/iovs.14-15848
20. Lam BL, Christ SL, Lee DJ, et al. Reported visual impairment and risk of suicide: the 1986–1996 national health interview surveys. Arch Ophthalmol. 2008;126(7):975–980. doi:10.1001/archopht.126.7.975
21. Branch LG, Horowitz A, Carr C. The implications for everyday life of incident self-reported visual decline among people over age 65 living in the community. Gerontologist. 1989;29(3):359–365. doi:10.1093/geront/29.3.359
22. Shah A, Bhat R, Zarate-Escudero S, et al. Suicide rates in five-year age-bands after the age of 60 years: the international landscape. Aging Ment Health. 2016;20(2):131–138. doi:10.1080/13607863.2015.1055552
23. Smith M, Cui R, Odom JV, et al. Giving support and suicidal ideation in older adults with vision-related diagnoses. Clin Gerontol. 2020;43(1):17–23. doi:10.1080/07317115.2019.1659465
24. World Health Organization. Suicide; 2021. Available from: https://www.who.int/news-room/fact-sheets/detail/suicide.
25. World Health Organization. MB26.A suicidal ideation; 2023. Available from: https://icd.who.int/browse11/l-m/en#/http://id.who.int/icd/entity/778734771.
26. Meyer-Rochow VB, Hakko H, Ojamo M, et al. Suicides in visually impaired persons: a nation-wide register-linked study from Finland based on thirty years of data. PLoS One. 2015;10(10):e0141583. doi:10.1371/journal.pone.0141583
27. Smith L, Shin JI, Barnett Y, et al. Association of objective visual impairment with suicidal ideation and suicide attempts among adults aged ≥50 years in low/middle-income countries. Br J Ophthalmol. 2022;106(11):1610–1616. doi:10.1136/bjophthalmol-2021-318864
28. Naicker KGN, Zeng Y, Senthilselvan A, et al. Social, demographic, and health outcomes in the 10 years following adolescent depression. J Adolesc Health. 2013;52(5):533–538. doi:10.1016/j.jadohealth.2012.12.016
29. Gong Y, Zhang L, Wang Z, et al. Pathway analysis of risk factors for severe suicidal ideation: a survey in rural China. Can J Public Health. 2011;102(6):472–475. doi:10.1007/BF03404203
30. Lee SU, Roh S, Kim YE, et al. Impact of disability status on suicide risks in South Korea: analysis of National Health Insurance cohort data from 2003 to 2013. Disabil Health J. 2017;10(1):123–130. doi:10.1016/j.dhjo.2016.06.008
31. Ponte C, Almeida V, Fernandes L. Suicidal ideation, depression and quality of life in the elderly: study in a gerontopsychiatric consultation. Span J Psychol. 2014;17:E14. doi:10.1017/sjp.2014.15
32. Trangkasombat U, Larpboonsarp V, Havanond P. CES-D as a screen for depression in adolescents. J Psychiatr Assoc Thailand. 1997;42(1):2–13.
33. Posner K, Brent D, Lucas C, et al. The Columbia-Suicide Severity Rating Scale (C-SSRS); 2009. Available from: https://cssrs.columbia.edu/the-columbia-scale-c-ssrs/translations/.
34. Bezabih L, Abebe TW, Fite RO. Prevalence and factors associated with childhood visual impairment in Ethiopia. Clin Ophthalmol. 2017;11:1941–1948. doi:10.2147/OPTH.S135011
35. Bursac Z, Gauss CH, Williams DK, et al. Purposeful selection of variables in logistic regression. Source Code Biol Med. 2008;3(17):1–8. doi:10.1186/1751-0473-3-17
36. Robert BB, Afifi AA. Comparison of stopping rules in forward “stepwise” regression. J Am Stat Assoc. 1997;72(357):46–53. doi:10.1080/01621459.1977.10479905
37. Mickey RM, Greenland S. The impact of confounder selection criteria on effect estimation. Am J Epidemiol. 1989;129(1):125–137. doi:10.1093/oxfordjournals.aje.a115101
38. Lee OE, Park D, Park J. Association of vision impairment with suicide ideation, plans, and attempts among adults in the United States. J Clin Psychol. 2022;78(11):2197–2213. doi:10.1002/jclp.23437
39. Khurana M, Shoham N, Cooper C, et al. Association between sensory impairment and suicidal ideation and attempt: a cross-sectional analysis of nationally representative English household data. BMJ Open. 2021;11(2):e043179. doi:10.1136/bmjopen-2020-043179
40. Kim S, Shin DW, An AR, et al. Mental health of people with retinitis pigmentosa. Optom Vis Sci. 2013;90(5):488–493. doi:10.1097/OPX.0b013e31828dee0a
41. Freeman EE, Egleston BL, West SK, et al. Visual acuity change and mortality in older adults. Invest Ophthalmol Vis Sci. 2005;46(11):4040–4045. doi:10.1167/iovs.05-0687
42. Wong TY, Cheung CM, Larsen M, et al. Diabetic retinopathy. Nat Rev Dis Primers. 2016;2:16012. doi:10.1038/nrdp.2016.12
43. Chen X, Lu L. Depression in diabetic retinopathy: a review and recommendation for psychiatric management. Psychosomatics. 2016;57(5):465–471. doi:10.1016/j.psym.2016.04.003
44. Rajeshkannan S, Yenuganti VV, Solomon MAT, et al. Association of visual impairment with suicidal ideation and suicide attempts: a systematic review and meta-analysis. Indian J Psychol Med. 2022:02537176221087124. doi:10.1177/02537176221087124
45. Kim Y, Kwak Y, Kim JS. The association between suicide ideation and sensory impairment among elderly Koreans. Aging Ment Health. 2015;19(7):658–665. doi:10.1080/13607863.2014.989812
46. Kim BJ, Kihl T. Suicidal ideation associated with depression and social support: a survey-based analysis of older adults in South Korea. BMC Psychiatry. 2021;21(1):409. doi:10.1186/s12888-021-03423-8
47. Mofijur M, Fattah IMR, Alam MA, et al. Impact of COVID-19 on the social, economic, environmental and energy domains: lessons learnt from a global pandemic. Sustain Prod Consum. 2021;26:343–359. doi:10.1016/j.spc.2020.10.016
48. Cabello M, Miret M, Ayuso-Mateos JL, et al. Cross-national prevalence and factors associated with suicide ideation and attempts in older and young-and-middle age people. Aging Ment Health. 2020;24(9):1533–1542. doi:10.1080/13607863.2019.1603284
49. Waern M, Rubenowitz E, Runeson B, et al. Burden of illness and suicide in elderly people: case-control study. BMJ. 2002;324(7350):1355. doi:10.1136/bmj.324.7350.1355
50. Olarn R, Suchada C. Increasing access to cataract services in vulnerable populations (elderly) District 2. Health Systems Research Institute (HSRI); 2018. Available from: https://kb.hsri.or.th/dspace/handle/11228/4985.
 © 2023 The Author(s). This work is published and licensed by Dove Medical Press Limited. The
full terms of this license are available at https://www.dovepress.com/terms.php
and incorporate the Creative Commons Attribution
- Non Commercial (unported, v3.0) License.
By accessing the work you hereby accept the Terms. Non-commercial uses of the work are permitted
without any further permission from Dove Medical Press Limited, provided the work is properly
attributed. For permission for commercial use of this work, please see paragraphs 4.2 and 5 of our Terms.
© 2023 The Author(s). This work is published and licensed by Dove Medical Press Limited. The
full terms of this license are available at https://www.dovepress.com/terms.php
and incorporate the Creative Commons Attribution
- Non Commercial (unported, v3.0) License.
By accessing the work you hereby accept the Terms. Non-commercial uses of the work are permitted
without any further permission from Dove Medical Press Limited, provided the work is properly
attributed. For permission for commercial use of this work, please see paragraphs 4.2 and 5 of our Terms.
Recommended articles
Physical Activity, Dietary Habits and Factors Associated with Depression Among Medical Students of Sindh, Pakistan, During the COVID-19 Pandemic
Khidri FF, Riaz H, Bhatti U, Shahani KA, Kamran Ali F, Effendi S, Rani K, Chohan MN
Psychology Research and Behavior Management 2022, 15:1311-1323
Published Date: 25 May 2022
Psychological Impact of COVID-19 on Doctors and Medical Students of Punjab, Pakistan: A Logistic Regression Analysis
Junaid Tahir M, Tariq W, Anas Tahseen Asar M, Irfan Malik M, Kamal Akhtar F, Malik M, Akhtar Q, Abbasher Hussien Mohamed Ahmed K, Talha Awan M, Ullah K, Asghar MS
Journal of Multidisciplinary Healthcare 2022, 15:1297-1308
Published Date: 8 June 2022
Factors Affecting the Psychological Well-Being of Health Care Workers During the COVID-19 Crisis
Alharthi MH, Alshomrani AT, Bazaid K, Sonpol HMA, Ibrahim IAE, Alashkar AM
Psychology Research and Behavior Management 2022, 15:1931-1942
Published Date: 28 July 2022
Resilience and Depressive Symptoms Mediated Pathways from Social Support to Suicidal Ideation Among Undergraduates During the COVID-19 Campus Lockdown in China
Zhang X, Liu X, Mi Y, Wang W, Xu H
Psychology Research and Behavior Management 2022, 15:2291-2301
Published Date: 23 August 2022
Pre- and Post-Pandemic (COVID-19) Mental Health of International Students: Data from a Longitudinal Study
Jamshaid S, Bahadar N, Jamshed K, Rashid M, Imran Afzal M, Tian L, Umar M, Feng X, Khan I, Zong M
Psychology Research and Behavior Management 2023, 16:431-446
Published Date: 15 February 2023
