Back to Journals » Advances in Medical Education and Practice » Volume 11
Medical Students’ Perception of Their Education and Training to Cope with Future Market Trends
Authors Iesa MAM
Received 5 October 2019
Accepted for publication 9 February 2020
Published 25 March 2020 Volume 2020:11 Pages 237—243
DOI https://doi.org/10.2147/AMEP.S233494
Checked for plagiarism Yes
Review by Single anonymous peer review
Peer reviewer comments 2
Editor who approved publication: Prof. Dr. Balakrishnan Nair
This paper has been retracted.
Mohamed Abdelrahman Mohamed Iesa
Department of Physiology, Faculty of Medicine, Umm Al-Qura University, Al Qunfudhah, Makkah, Saudi Arabia
Correspondence: Mohamed Abdelrahman Mohamed Iesa
Department of Physiology, Faculty of Medicine, Umm Al-Qura University, P.O. Box: 715, Al Qunfudhah, Makkah, Saudi Arabia
Tel +966 538832384
Fax +966 177461197
Email [email protected]
Purpose: Medical studies is a very diverse field of education that seeks to prepare students for a rapidly evolving healthcare market. This study presents the findings of a survey about the perception of medical students about whether they receive training in professionalism and management skills and whether their education prepares them to face the evolving market trends.
Methods: This was a qualitative study that used descriptive data obtained via an online survey conducted among medical students via WhatsApp. The sample included 500 students from 10 medical schools across the UK. The survey was divided into three parts: The first part contained questions related to professionalism and the training they received at the basic level. The second part contained questions about management and leadership training for the medical field and whether the students thought it was important for their future. The last part contained questions about whether the students thought that their level of education was competitive enough to ensure their survival in the face of future market trends.
Results: Most students (77%) thought that training in leadership and management skills was necessary to prepare them for the future market, and 68% felt that they were not receiving satisfactory training in leadership and management skills. The students also felt that they need to be taught more about the market and its various changing features. Finally, the majority (62%) of the students felt that their courses did not focus on social and professional skills.
Conclusion: The findings from the survey indicate that there is a clear need for courses on professionalism and management among medical students and that institutes need to keep up with these emerging needs in terms of training.
Keywords: professionalism, management skills, qualitative study, team work, elements of professionalism
Introduction
Public health has become an important topic of debate all over the world, and this has resulted in continuous research and improvements in this field. Most countries around the world have an exclusive department of health that focuses on consistent work on bringing about improvements in healthcare services. Since it is a rather complex field that involves many players, there are a lot of factors that come into play.1–3 In this regard, an important topic to consider is the perception of students in the medical field, since eventually, these students will set the standards for the medical profession in the market.3,4 Therefore, there are a number of studies that mainly focus on students’ views about professionalism in the medical field.
There are certain beliefs, values, and priorities that are directly associated with medical professionals that students of the field take with them from the institution, while at the same time, they also have their own set of beliefs, values, and priorities, which is often defined as a “hidden curriculum.”5 The point of inquiry then is whether the characteristics, feelings, and requirements of the understudies (or the hidden curriculum) are in agreement with those of the establishments.6 Another interesting point of inquiry is patient autonomy, which has received some coverage in the media. Additionally, the internet has provided the public with greater access to information about the health profession.7,8 Understudies’ perspective of medicinal experts could be influenced by their impression or view of this calling, based on their experiences with individuals that they are in contact with.9,10 Students’ perspective of experts, which is largely based on their experiences with individuals, may differ from their perspective on treatment, which would be based on wider experiences and multi-person perspectives: that is, the correct treatment would be based on scientific and clinical evidence, whereas the ideal treatment would also take into consideration the patient’s values and preferences and the physician’s judgment.11 Students’ perspectives are based on their experiences with experts, their own set of values, and their expectations of what an expert ought to be.12 Thus, professionalism is viewed by students as an acquired state, and not a trait that one possesses, as environmental factors contribute more than biological ones to their development over time.12
Students are often confused about their perceptions of the medical field, and there is not enough previous research to provide a clear picture of the impact of their perceptions on future market trends.13,14 In one of the few studies that have explored this topic, students of the first year were investigated,15 and the results were rather different from those obtained for final-year students at medical institutes.16 The latter report found that students in their senior years view the medical profession from a more vocational perspective.17,18 There are a number of relevant reports that have investigated the different perspectives of medical students in different case scenarios. The present study also seeks to explore medical students’ perspectives of the field, but it pays special attention to the impact of social media, competition between medical professionals worldwide, and the importance of evolving medical technology as a tool for learning and gaining evidence-based knowledge. Below, the findings from relevant published studies are presented.
Background Studies
In a cross-sectional research conducted in 2015–2016, questionnaires were distributed to almost 2349 students in their final year via an online platform. The survey included 10 medical schools from the UK, and the questions were based on the current perception of the medical students and their interests and attitudes towards professionalism and leadership in their field.19 Another reported20 survey also included self-rated questions on the students’ perception of their competence in the current medical market and whether they were being taught the skills that can help them become proficient medical professionals.20 According to another study,21 only 7.9% of the students reported that they were being trained to develop the necessary managerial and leadership skills that can help them become good-quality medical professionals. Although professionalism is very important in the medical field, students seem to feel that they are not being properly trained for their future as professionals in the medical field.22,23 According to the majority of students, another important teaching point is decision-making ability, which is an important skill for clinicians, especially in critical situations.24,25 Students were also of the opinion that they needed leadership, management, and professionalism courses in order to keep up with future market trends.26–28 Undoubtedly, competition is always on the increase, and students need to keep up with the changing market trends in order to ensure that their career progresses and they are ready to face their future responsibilities.29
Recent developments in the world, especially in medical curricula, have led to the introduction of various technological tools in teaching.34 A number of these technological developments have been highly beneficial to the medical field.35 Therefore, it is important for students to acquire the skills required for using such tools.36 However, several studies have suggested that medical students in the UK are willing to enhance their technical and leadership skills, but they are not provided with the proper resources they need to do so.30,31 Further, it appears that medical students are expected to focus mostly on gaining theoretical knowledge, but as a result, certain fundamental aspects of the practice are neglected.32,33 Another consequence is that these medical students, who have sound theoretical knowledge, lack other basic practical skills.32,33 If this situation does not change, such poor training and neglect of the students’ needs could critically affect the medical field in the future.
Medical curricula often undergo changes with regard to the teaching of different fields of medical sciences on account of developments that occur globally.37 Some researchers are of the opinion that certain fields of healthcare are assigned more importance than others in the initial training of doctors.26 Further, it has been pointed out that irrespective of the importance assigned to healthcare courses, none of them have been able to keep up with rapidly changing trends in the market and community that have occurred as a result of technological changes.38,39 To date, there have been no objective studies on the perceived relevance of these different courses to the field of medical sciences or their influence on the future from the viewpoint of medical students.40–42 However, one study did investigate the perception of medical students at Cardiff and Paris about the importance of different courses in the medical field, with the help of an attitude analysis questionnaire.43 The study included students who were in the final stages of their studies (and were about to graduate) and were looking forward to their professional life. The results reflect the attitudes of students from varied geopolitical and cultural backgrounds who were at all stages of their medical course and reflect their professional perspectives about the state of medical education in their own region and the scope for the future. The findings pointed to the need for standard medical practices that are tailored to different cultural backgrounds.
Thus, the findings of the relevant studies so far indicate that only a minority of medical students feel that they are receiving training for the necessary leadership and managerial skills they need. They also feel that decision-making skill was an important subject that should be taught as part of their course. Further, the studies so far indicate that there is too much focus on gaining theoretical knowledge and not enough attention to basic practical skills that are required in the field. Finally, the importance of equipping students to learn the use of rapidly evolving technological tools was also pointed out.
Objective
The aim of the present study is to analyze medical students’ views about training in professionalism, leadership, and management skills, and whether they think that their education prepares them for future market trends.
Experimental Design
An online survey was conducted on final-year students from 10 different medical schools in the UK. The survey collected descriptive data, as this study is a qualitative one. The questionnaires were distributed online via WhatsApp to final-year medical students. A total of 500 graduates from the 10 medical schools were sampled. The questionnaire used has been tested and validated by the American board of internal medicine (ABIM) and is accepted as a standard tool for assessing professionalism. The students were expected to respond to the questions with the use of a Likert scale. The questionnaire was divided into three parts that focused on a different aspect of medical studies. The first part contained questions related to professionalism and the training they received at the basic level. The second part contained questions about management and leadership training for the medical field and whether the students thought it was important for their future. The last part contained questions about whether the students thought that their level of education was competitive enough to ensure their survival in the face of future market trends (Figure 1). This qualitative method was apt for understanding the specific research topics. There was some clash of opinions with regard to certain questions; however, the results are based on the opinions of the majority of the participants.
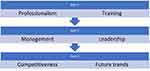 |
Figure 1 Survey design for the research. |
Results
The results of the survey indicate that 74% of the students believe that their education and learning is advanced enough to deal with future competition (Table 1), while 68% believe that they are not being taught management and leadership skills in a satisfactory way (Table 2). Further, 77% of the participants think that acquiring management and leadership skills is essential for medical professionals to cope with future market trends (Table 3). The students also think that improving the quality of medical institutes and modifying the subjects being taught can help them to learn more about the market environment. In particular, 78% of the students strongly agree that there is a need for courses that focus exclusively on management, professionalism, and leadership for medical students. Further, 62% of the student disagree with the statement that their courses are sufficient to enhance their social and professional skills. Overall, the findings from the survey indicate that although institutes are aware that medical students do not receive sufficient preparation to directly enter the market, the institutes make very few changes in their courses to provide their students with the management and leadership skills required to enter a competitive market.
 |
Table 1 Part 1 of the Survey (Professionalism and Training) |
 |
Table 2 Part 2 of the Survey (Management and Leadership) |
 |
Table 3 Part 3 of the Survey (Competitiveness and Future Trends) |
Discussion
Currently, the healthcare market is changing rapidly and becoming more complex, since the demands of the market cannot be fulfilled by a single platform or a single expert or group of experts. In this scenario, efficient sharing of information between institutions has gained importance, especially since few changes are being made in the courses and educational strategies of these institutes.1,4 The expansion of educational options, as well as the escalating rate of competition in the current market, mandates greater scrutiny of the true effectiveness of medical institutions in educating future medical professionals,16 and this is what the current study set out to do.
The technological advances of this era have led to rapid diversifications in the field of medical sciences, but the perceptions of medical students are not being honed according to future market needs.44 Although students are aware of these changes and of the need to change their perception of their profession, they require the appropriate guidance and training to help them keep up with the trends. The majority of the students (77%) in the current survey were of the opinion that training in leadership and management skills was necessary to prepare them for the future market, and 68% felt that they were not receiving satisfactory training in leadership and management skills. Thus, the findings indicate that There are various factors that highly impact the future market, such as an increase in healthcare costs, personalization of medical treatment, advances in technology, focus on medical tourism, patient satisfaction, and the ability of professionals to deal with patients.33,43 There is a definite need for exclusive training for medical students in order to help them understand these variables and their impact on the future market, so that they can become competent medical professionals in the future.25 Such training is expected to also enhance the quality of services, and therefore, eventually contribute to economic growth.29 The students surveyed in the present study also felt that they need to be taught more about the market and its various changing features.
According to some published studies, 22,38, medical schools are adopting courses on social and professional skills across different countries because new graduates from medical schools have been found to struggle with these skills. These medical schools acknowledge that while they provide education which ensures that the students gain the essential healthcare knowledge required to work as a professional in the market, it is essential to teach the students such skills as well. In the current study, the majority (62%) of the students felt that their courses did not focus on these skills.
Conclusion
Based on the findings of the survey conducted, the present research concludes that the market trends in the medical field are evolving constantly, and students need to be trained so they can cope with these changes. In particular, the findings highlight the importance of courses on professionalism and management as these courses can help medical students to survive and thrive in a competitive market.
Ethical Considerations
All other ethical considerations for web-based questionnaires were considered.45
Acknowledgments
This study would have been not possible without the committed support of my student Dr. Oliver Whingston. My special thanks go to my colleagues Dr. Emad Hussein, Hani Eisa, and Hamed AL Redaisy.
Disclosure
The author reports no conflicts of interest in this work.
References
1. Von Fragstein M, Silverman J, Cushing A, Quilligan S, Salisbury H, Wiskin C. UK Council for Clinical Communication Skills Teaching in Undergraduate Medical Education. UK consensus statement on the content of communication curricula in undergraduate medical education. Med Educ. 2008;42(11):1100–1107. doi:10.1111/med.2008.42.issue-11
2. Varkey P, Peloquin J, Reed D, Lindor K, Harris I. Leadership curriculum in undergraduate medical education: a study of student and faculty perspectives. Med Teach. 2009;31(3):244–250. doi:10.1080/01421590802144278
3. Twine FW. Outsourcing the Womb: Race, Class and Gestational Surrogacy in a Global Market. Routledge; March 27, 2015.
4. Thomas PA, Kern DE, Hughes MT, Chen BY, editors. Curriculum Development for Medical Education: A Six-Step Approach. JHU Press; January 29, 2016.
5. Telio S, Ajjawi R, Regehr G. The “educational alliance” as a framework for reconceptualizing feedback in medical education. Acad Med. 2015;90(5):609–614. doi:10.1097/ACM.0000000000000560
6. Swanwick T. Understanding medical education. Understanding Med Educ. 2013:1–6.
7. Sun Z, Wang S, Barnes SR. Understanding congestion in China’s medical market: an incentive structure perspective. Health Policy Plan. 2015;31(3):390–403. doi:10.1093/heapol/czv062
8. Straus CM, Webb EM, Kondo KL, et al. Medical student radiology education: summary and recommendations from a national survey of medical school and radiology department leadership. J Am Coll Radiol. 2014;11(6):606–610. doi:10.1016/j.jacr.2014.01.012
9. Steinert Y, Naismith L, Mann K. Faculty development initiatives designed to promote leadership in medical education. A BEME systematic review: BEME Guide No. 19. Med Teach. 2012;34(6):483–503. doi:10.3109/0142159X.2012.680937
10. Sevigny EL, Pacula RL, Heaton P. The effects of medical marijuana laws on potency. Int J Drug Policy. 2014;25(2):308–319. doi:10.1016/j.drugpo.2014.01.003
11. Quince TA, Parker RA, Wood DF, Benson JA. Stability of empathy among undergraduate medical students: a longitudinal study at one UK medical school. BMC Med Educ. 2011;11(1):90. doi:10.1186/1472-6920-11-90
12. Quince T, Abbas M, Murugesu S, et al. Leadership and management in the undergraduate medical curriculum: a qualitative study of students’ attitudes and opinions at one UK medical school. BMJ Open. 2014;4(6):e005353. doi:10.1136/bmjopen-2014-005353
13. Palmer EJ, Devitt PG. Assessment of higher order cognitive skills in undergraduate education: modified essay or multiple choice questions? Research paper. BMC Med Educ. 2007;7(1):49. doi:10.1186/1472-6920-7-49
14. Osmani SS. Effective leadership–the way to excellence in health professions education. Med Teach. 2013;35(11):956–958. doi:10.3109/0142159X.2013.818629
15. Morse LC, Babcock DL, Murthy M. Managing Engineering and Technology. Pearson; September 10, 2014.
16. Miles S, Leinster SJ. Medical students’ perceptions of their educational environment: expected versus actual perceptions. Med Educ. 2007;41(3):265–272. doi:10.1111/med.2007.41.issue-3
17. McGaghie WC, Issenberg SB, Cohen ME, Barsuk JH, Wayne DB. Does simulation-based medical education with deliberate practice yield better results than traditional clinical education? A meta-analytic comparative review of the evidence. Acad Med. 2011;86(6):706. doi:10.1097/ACM.0b013e318217e119
18. Lynch* R, Baines P. Strategy development in UK higher education: towards resource‐based competitive advantages. J Higher Educ Policy Manage. 2004;26(2):171–187. doi:10.1080/1360080042000218249
19. Lunt N, Horsfall D, Smith R, Exworthy M, Hanefeld J, Mannion R. Market size, market share and market strategy: three myths of medical tourism. Policy Politics. 2014;42(4):597–614. doi:10.1332/030557312X655918
20. Lempp H, Seale C. The hidden curriculum in undergraduate medical education: qualitative study of medical students’ perceptions of teaching. BMJ. 2004;329(7469):770–773. doi:10.1136/bmj.329.7469.770
21. Könings KD, Brand‐Gruwel S, Van Merriënboer JJ. Towards more powerful learning environments through combining the perspectives of designers, teachers, and students. Br J Educ Psychol. 2005;75(4):645–660. doi:10.1348/000709905X43616
22. Kamphuis C, Barsom E, Schijven M, Christoph N. Augmented reality in medical education? Perspect Med Educ. 2014;3(4):300–311. doi:10.1007/s40037-013-0107-7
23. Inglesby TV, Dennis DT, Henderson DA, et al. Plague as a biological weapon: medical and public health management. JAMA. 2000;283(17):2281–2290. doi:10.1001/jama.283.17.2281
24. Huda N, Yousuf S. Career preference of final year medical students of Ziauddin Medical University. Educ Health. 2006;19(3):345–353. doi:10.1080/13576280600984087
25. Hren D, Lukić IK, Marušić A, et al. Teaching research methodology in medical schools: students’ attitudes towards and knowledge about science. Med Educ. 2004;38(1):81–86. doi:10.1111/med.2004.38.issue-1
26. Howe A, Campion P, Searle J, Smith H. New perspectives—approaches to medical education at four new UK medical schools. BMJ. 2004;329(7461):327–331. doi:10.1136/bmj.329.7461.327
27. Houlden RL, Raja JB, Collier CP, Clark AF, Waugh JM. Medical students’ perceptions of an undergraduate research elective. Med Teach. 2004;26(7):659–661. doi:10.1080/01421590400019542
28. Horsburgh M, Lamdin R, Williamson E. Multiprofessional learning: the attitudes of medical, nursing and pharmacy students to shared learning. Med Educ. 2001;35(9):876–883. doi:10.1046/j.1365-2923.2001.00959.x
29. Holmboe ES. Realizing the promise of competency-based medical education. Acad Med. 2015;90(4):411–413. doi:10.1097/ACM.0000000000000515
30. Hoffman SJ, Rosenfield D, Gilbert JH, Oandasan IF. Student leadership in interprofessional education: benefits, challenges and implications for educators, researchers and policymakers. Med Educ. 2008;42(7):654–661. doi:10.1111/j.1365-2923.2008.03042.x
31. Goldacre MJ, Turner G, Lambert TW. Variation by medical school in career choices of UK graduates of 1999 and 2000. Med Educ. 2004;38(3):249–258. doi:10.1046/j.1365-2923.2004.01763.x
32. Funnell MM, Brown TL, Childs BP, et al. National standards for diabetes self-management education. Diabetes Care. 2009;32(Supplement 1):S87–S94. doi:10.2337/dc09-S087
33. Feudtner C, Christakis DA, Christakis NA. Do clinical clerks suffer ethical erosion? Students’ perceptions of their ethical environment and personal development. Acad Med. 1994;69(8):670–679. doi:10.1097/00001888-199408000-00017
34. Ende J. Feedback in clinical medical education. JAMA. 1983;250(6):777–781. doi:10.1001/jama.1983.03340060055026
35. Dunne F, McAleer S, Roff S. Assessment of the undergraduate medical education environment in a large UK medical school. Health Educ J. 2006;65(2):149–158. doi:10.1177/001789690606500205
36. Denis JL, van Gestel N. Medical doctors in healthcare leadership: theoretical and practical challenges. BMC Health Serv Res. 2016;16(2):158. doi:10.1186/s12913-016-1392-8
37. Davis DA, Thomson MA, Oxman AD, Haynes RB. Changing physician performance: a systematic review of the effect of continuing medical education strategies. JAMA. 1995;274(9):700–705. doi:10.1001/jama.1995.03530090032018
38. Cutler JL, Alspector SL, Harding KJ, Wright LL, Graham MJ. Medical students’ perceptions of psychiatry as a career choice. Acad Psychiatry. 2006;30(2):144–149. doi:10.1176/appi.ap.30.2.144
39. Curran VR, Sharpe D, Forristall J, Flynn K. Attitudes of health sciences students towards interprofessional teamwork and education. Learn Health Social Care. 2008;7(3):146–156. doi:10.1111/lhs.2008.7.issue-3
40. Cruess RL, Cruess SR, Boudreau JD, Snell L, Steinert Y. Reframing medical education to support professional identity formation. Acad Med. 2014;89(11):1446–1451. doi:10.1097/ACM.0000000000000427
41. Connell MT, Pascoe JM. Undergraduate medical education for the 21st century: leadership and teamwork. Family Med Kansas City. 2004;36(1; SUPP):S51–S56.
42. Çitaku F, Violato C, Beran T, Donnon T, Hecker K, Cawthorpe D. Leadership competencies for medical education and healthcare professions: population-based study. BMJ Open. 2012;2(2):e000812. doi:10.1136/bmjopen-2012-000812
43. Benbassat J. Role modeling in medical education: the importance of a reflective imitation. Acad Med. 2014;89(4):550. doi:10.1097/ACM.0000000000000189
44. Barrows HS, Tamblyn RM. Problem-Based Learning: An Approach to Medical Education. UK: Springer Publishing Company; March 1980.
45. Fox J, Murray C, Warm A. Conducting research using web-based questionnaires: practical, methodological, and ethical considerations. Int J Social Res Methodol, 2003;6(2):167–180. doi:10.1080/13645570210142883
 © 2020 The Author(s). This work is published and licensed by Dove Medical Press Limited. The full terms of this license are available at https://www.dovepress.com/terms.php and incorporate the Creative Commons Attribution - Non Commercial (unported, v3.0) License.
By accessing the work you hereby accept the Terms. Non-commercial uses of the work are permitted without any further permission from Dove Medical Press Limited, provided the work is properly attributed. For permission for commercial use of this work, please see paragraphs 4.2 and 5 of our Terms.
© 2020 The Author(s). This work is published and licensed by Dove Medical Press Limited. The full terms of this license are available at https://www.dovepress.com/terms.php and incorporate the Creative Commons Attribution - Non Commercial (unported, v3.0) License.
By accessing the work you hereby accept the Terms. Non-commercial uses of the work are permitted without any further permission from Dove Medical Press Limited, provided the work is properly attributed. For permission for commercial use of this work, please see paragraphs 4.2 and 5 of our Terms.
