Back to Journals » Nutrition and Dietary Supplements » Volume 12
Health Benefits of a Vegan Diet: Current Insights
Authors Radnitz C, Ni J, Dennis D, Cerrito B
Received 12 October 2019
Accepted for publication 23 March 2020
Published 12 May 2020 Volume 2020:12 Pages 57—85
DOI https://doi.org/10.2147/NDS.S191793
Checked for plagiarism Yes
Review by Single anonymous peer review
Peer reviewer comments 3
Editor who approved publication: Dr Gary Johanning
Video abstract of "Health benefits of a vegan diet" [ID 191793].
Views: 1231
Cynthia Radnitz, Jingwen Ni, Danielle Dennis, Brianna Cerrito
School of Psychology, Fairleigh Dickinson University, Teaneck, NJ, USA
Correspondence: Cynthia Radnitz
School of Psychology, Fairleigh Dickinson University, 1000 River Road., Teaneck, NJ, USA
Tel +1 (201) 692-2306
Fax +1 (201) 692-2304
Email [email protected]
Abstract: To assess the health benefits of a vegan diet, observational studies of diabetes (non-insulin dependent; NIDDM), cancer, mortality, gut microbiota, hypertension, lipids, and overweight were examined. Utilizing PRISMA items to identify articles and assess their quality for inclusion, 44 studies were screened into the review. In two separate studies, vegans did not have a reduced risk of diagnosis of “any” cancer, nor of specific cancers when the effects of BMI were adjusted. When data were aggregated, there was a reduced risk of any cancer. Vegans had lower total cholesterol and LDL-C levels compared to omnivores, and in some cases other dietary groups. In the US, there was a reduced risk of a diagnosis of NIDDM and in Western countries, vegans had lower BMI. Research support for reduced risk of diagnosis of female cancers, improved mortality rates, lower blood pressure, lower triglycerides, and a healthier microbiome for vegans compared to omnivores was inconsistent. There was no evidence that reduced specific cancer incidence rates were lower in vegans although inadequate sample sizes had hampered these analyses. In vegans, HDL-C levels were either lower or not significantly different from omnivores. Geographic location was a strong moderator with the most compelling evidence for the health advantages of a vegan diet coming from the US, whereas in Taiwan, India and Vietnam, there was much less evidence of its benefit. In some instances, sex moderated the association between adopting the diet and health outcomes. Adherence, specific content of the diet, and dietary comparison groups utilized in studies may also affect results. Although a vegan diet is associated with some health benefits, the level of support for the benefit varied according to the health outcome being measured, with evidence emerging that BMI is an important mediator and geography and to a lesser extent sex are important moderators.
Keywords: vegan, vegetarian, health
Introduction
In 1944, members of the Vegetarian Society in the United Kingdom first coined the term “vegan.”1 Veganism is defined as “ … the practice of dispensing with all products derived wholly or partly from animals.”2 Hence, people identifying as vegan avoid eating meat, poultry, fish, eggs or dairy foods. Although veganism extends beyond food choices, as many adopted the diet, its health benefits began to be investigated.
A review of the health benefits of a vegan diet is timely. One previous review3 was published eleven years ago. Recently there have been more focused reviews and meta-analyses (eg, Yokoyama et al4), but a more expansive analysis has not been performed.
Because addressing the health benefits of a vegan diet is a broad topic, further delineation of the parameters of this review was necessary. First, we chose to focus on observational studies (cohort, case control and cross-sectional designs) rather than clinical trials. Second, we decided to forego reviewing the nutrient deficiencies that can result from a poorly planned vegan diet as these have been described elsewhere.5 Beyond addressing diet benefits, health conditions and medical/nutritional indicators of health problems were selected based on there being sufficient literature to merit inclusion. Furthermore, if findings from included studies showed those following a vegan diet had worse outcomes than those following other diets, these results were reported.
The specific areas targeted in this review are the following: non-insulin dependent diabetes mellitus (NIDDM), cancers, mortality, gut microbiome, hypertension (blood pressure), lipids (cholesterol), and overweight (body mass index (BMI)).
Methodology
In line with recommendations for reviewing studies within a broad topic area, we adopted a semi-systematic approach.6 We utilized methods outlined in the Preferred Reporting Items for Systematic Reviews and Meta-Analyses (PRISMA)7,8 to identify, evaluate and ultimately select studies for inclusion. Furthermore, we reported in Table 1–7 characteristics of studies in the review including location, cohort, design, sample description, sex, mean age, results/follow-up, adjustment and effect size. However, as the topic areas were diverse (eg, cancer, NIDDM), we could not extract uniform data across topics. Additionally, we included well-conducted meta-analyses and other systematic analyses and reviews in our discussion of findings as this work is informative.
 |
Table 1 NIDDM |
 |
Table 2 Cancer |
 |
Table 3 Mortality |
 |
Table 4 Gut Microbiome |
 |
Table 5 Hypertension |
 |  |  |  |  |  |  |
Table 6 Lipids |
 |  |  |  |
Table 7 Overweight |
Eligibility criteria for inclusion were the following: 1) English language, 2) Human participants, 3) Focused on health benefits of a vegan diet (see above for specific areas), 4) Inclusion of both vegans and an appropriate comparison group, 5) Age of participants was 18 or older, 6) Vegan diet was defined as consuming fish, meat, poultry, dairy or eggs no more than once monthly, 7) On vegan diet at least 3 weeks, 8) Cohort, cross-sectional or case-controlled design, 9) Dependent variables were well-defined health outcomes, and 10) Full-text article (not just abstract) published in peer-reviewed journals. Exclusion criteria were 1) Vegans combined with another group for study 2) Other diet (eg, vegetarian), and 3) Lack of between-group parametric tests.
Search Plan and Identification of Studies
A systematic search of Pubmed, Cochrane Central Register of Controlled Trials, MEDLINE, and MEDLINE PLUS was performed on June 24, 2019. Then, reference lists of articles with relevant topic areas were reviewed to search for additional studies that were appropriate. In addition, articles published in the first issue of a new journal focused on studies of plant-based diets were considered for the review. The search terms used to locate studies were: “plant-based” OR “vegan” AND “mortality” OR “death” OR “risk assessment” OR “heart disease” OR “cardiovascular” OR “cardiovascular disease” OR “stroke*” OR “cerebrovascular disease” OR “statin*” OR “cancer*” OR “tumor” OR “diabet*” OR “TRD” OR “DT2” OR “cholester*” OR “gut microbiome” OR “gut bacteria” OR “body mass index” OR “bmi” OR “bariatric surgery” OR “obesity” OR “overweight” OR “gastric banding” OR “hypertension” OR “blood pressure increase” OR “atrial fibrillation”.
Study Selection
Results from searches of the databases were combined yielding a total of 3,105 (see Figure 1) published articles. After removal of duplicates (N=207), the remaining 2,898 articles were screened to determine if they met inclusion criteria, using a systematic inspection of article title, abstract, and if necessary, full text. From this screening, an additional 2,826 articles were excluded based on abstract and title review. After full-text review, an additional 32 articles were excluded. Specifically, 26 studies were excluded for not measuring a target outcome, 1 study was excluded for using children as participants, 1 study was excluded for not being an original study, 2 studies were excluded for having no control group, and 2 were excluded because the sample was comprised of both vegetarians and vegans. A review of the reference sections of screened-in articles and other sources revealed additional 20 articles, yielding a total of 60 studies undergoing quality assessment.
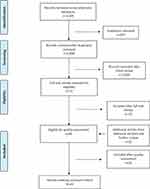 |
Figure 1 Search outcomes. |
No case–control studies were selected to undergo evaluation. To assess the methodological rigor of screened in studies, all were rated using the Newcastle-Ottawa Quality Assessment Scale (NOS)9 for either 1) cohort or 2) cross-sectional designs.10 Both scales are widely used in systematic reviews and have strong psychometric support. Each study was assessed independently by two raters, and any rating disagreement was settled by discussion and consensus. Ratings of “Fair” or “Good” from both raters were required for inclusion. From those assessments, 16 articles were removed for failing quality assessment (see Supplementary Table).
A total of 44 studies were screened into the review (See Table 1–7). As some studies reported multiple outcomes, they may appear in more than one table. Effect sizes were computed for studies that provided standard deviations or standard errors of the mean. To facilitate comparisons between studies in Tables, the following abbreviations were used: VG=vegan; VEG=vegetarian or ovo-lacto vegetarian; PESC=pescatarian, pesco-vegetarian or “fisheater;” OMN=omnivore, non-vegetarian or “meateater.”
Results
Diabetes. Studies investigating the relationship between diabetes and a vegan diet have focused on NIDDM. Four observational studies11–14 were published between 2009 and 2019 (see Table 1). Two US studies reported data from the same cohort of participants,11,12 with a total of 60,903 participants in the first study and 49,140 of those individuals also in the second study, conducted two years later. The cases of NIDDM and Insulin-Dependent Diabetes Mellitus (IDDM) found during the first assessment were removed from the follow-up analyses. In these two studies, vegans were less likely to develop NIDDM than omnivores, but not other comparison groups, when controlling for BMI. In a UK study, compared to omnivores there was no significantly lower risk for incidence of NIDDM when BMI was controlled although there was a significantly lower risk of NIDDM in vegans when BMI was not controlled.13 However, an Indian study reported no significant reduction in risk for vegans and other dietary groups.14
Cancers. Three observational studies of cancer risk in dietary groups were included in the review (see Table 2).15–17 They were published between 2012 and 2016 and included 7,198 vegans, 38,028 vegetarians, 15,446 pescatarians, 3,885 semivegetarians and 66,204 omnivores for a total of 130,761 participants. Tantamango-Bartley et al15 and Penniecook-Sawyers et al17 reported different data from a cohort of participants where there was substantial overlap with the 44,674 female participants in the Tantamango-Bartley et al15 study included in the Penniecook-Sawyers et al17 study, although the latter study included data from more US states (48 vs 38 in the Tantamango-Bartley et al study).
Two cohort studies examined whether overall cancer diagnosis rates were related to the type of diet that individuals consume.15,16 According to Tantamango-Bartley et al,15 once several factors were controlled for including but not limited to BMI, education, smoking, and menopause, there was no significant difference in cancer incidence between vegans and omnivores in both genders combined and for female-specific cancers. In a similar vein, Key et al16 reported a 14% lower risk of any cancer diagnosis in vegans compared to omnivores, but it was not a statistically significant reduction. However, when BMI was not a covariate, there was a specific risk reduction for “any” cancer and for female cancers. There was no significant risk reduction in the incidence of other specific diseases (colorectal, breast, or prostate cancer). Confirming the Key et al16 finding for breast cancer incidence, Penniecook-Sawyers et al17 also found a lower risk of breast cancer in vegans that was not statistically significant.
Mortality. The 3 articles reporting mortality rates in dietary groups included several cohort studies (see Table 3). 18–20 They were published between 1999 and 2016. One report included data from the EPIC-Oxford Study,18 one included data from the Adventist Health Study-2,19 and one included data from four cohorts (Adventist Mortality Study, Health Food Shoppers Study, Heidelberg Study Cohort, Oxford Vegetarian Study Cohort).20 The total sample size was 199,913 observations (mean age=50.81), including 8,529 vegans, 53,790 omnivores, 18,085 pescatarians, 25,205 semi-vegetarians (including 21,174 low meat omnivores), and 62,538 vegetarians. Participants from the Oxford Vegetarian Study (11,047) were included in both Key et al20 and Appleby et al.18
In the majority of comparisons between vegans and other dietary groups, no significant differences in mortality risk were found. In a UK study,18 and one combining data from five studies,20 the death rate hazard ratio (HR) for vegans compared to omnivores was not significantly different for malignant cancer (stomach cancer, colorectal cancer, lung cancer, breast cancer, and prostate cancer), ischemic heart disease, cardiovascular disease, cerebrovascular disease, diseases of the respiratory system, other causes and all causes.18–20 However, in a US study using an omnivore comparison group, vegans had a significantly lower death rate HR from other causes (excluding heart disease, cardiovascular disease, and cancer).19 Moreover, for men, vegans’ death rate HR (from all causes, ischemic heart disease, and cardiovascular disease) was significantly lower compared to omnivores.
Gut Microbiome. The gut microbiome consists of various commensal microbial species (thought to be >500) in the gastrointestinal tract including bacteria, viruses, archaea, and eukaryotic microbes.21,22 It has been increasingly studied due to its link to diseases, such as cardiovascular disease, inflammatory bowel disease, and infections (eg, clostridium difficile). Research has found positive effects of a plant-based diet on the microbiome, and, in turn, on disease.23
Four cross-sectional studies (see Table 4)24–27 assessed the gut microbiota of 754 participants (total). In European studies significantly lower microbial counts of the Bacteroides fragilis group and the mesophilic/thermophilic LAB loads (on MRS agar)24 and of the Bacteroides spp., Bifidobacterium spp., Escherichia coli and Enterobacteriaceae spp. groups as well as lower stool pH25 were found in vegan fecal microbiota compared to omnivores. Contrary to these findings, a US study found neither a difference in the gut microbiota between vegans and omnivores nor an association between higher consumption of fermentable substrate and higher levels of fecal short-chain fatty acids. The only reported significant finding was a healthier metabolome for vegans compared to omnivores.26 Similarly, Ruengsomwong et al27 compared several Thai vegetarian groups including a small vegan sample and found no significant differences in the genus and species of their microbiotas.
Hypertension. Hypertension is a risk factor for cardiovascular and cerebrovascular diseases.28 The 11 included articles29–39 reporting blood pressure data in vegans and other dietary groups were published between 1987 and 2018 (see Table 5). Data from large cohorts were reported in five studies, including the Adventist Health Study-2 (N=1),38 EPIC-Oxford (N=1),33 UK Biobank (N=1),31 German Vegan Study (N=1),35 and MJ Health Screening (N=1).39 The total sample size was 478,218 (mean age=55.5 years), including 3,399 vegans, 448,412 omnivores 14,936 vegetarians and 11,402 pescatarians, and 69 partial (semi) vegetarians.
In US studies, vegans had lower systolic blood pressure (SBP) and diastolic blood pressure (DBP) compared to omnivores,36,38 although no significant differences in blood pressure were found between vegans, vegetarians, and partial vegetarians.32,38 The majority of the remaining comparisons (across several studies)29,30,32–35 found no significant differences in blood pressure between vegans and other dietary groups with the following exceptions: 1) 2 studies reported significantly lower SBP in vegans compared to omnivores,34,37 2) 1 study found higher DPB in vegans than omnivores37 and another reported higher DBP in vegan men than omnivore men,29 and 3) among white participants, one study found in women significantly lower SBP (vegans versus omnivore) and DBP (vegans versus omnivores and vegetarians) and in men significantly lower SBP (vegans versus omnivores and vegetarians) and DBP (vegans versus all other dietary groups).31
Lipids. High serum low-density lipoprotein (LDL-C) cholesterol is a leading risk factor for several diseases, including stroke, coronary heart disease, and myocardial infarction.28 Observational studies (N=18; see Table 6),29,30,32,34–37,39–49 comparing cholesterol levels among dietary groups were published between 1978 and 2016 included a total of 149,838 participants, comprised of vegans (n=4,299), vegetarians (n=5,933), pescatarians (n=2,398), and omnivores (n=137,208). Most studies (N=11) found that total cholesterol (TC) was significantly lower in vegans compared to omnivores,30,36,37,41,44,45,47–49 vegetarians,32 and moderate vegans (animal products < 5% diet).35 Only one study reported no difference in TC in vegans compared to omnivores.34 In most studies, LDL-C was found to be significantly lower, in vegans compared to omnivores,36,40,41,43,46,47,49 with one showing lower levels in pescatarians49(women) and another in vegetarians.32
High-density lipoprotein (HDL-C) levels were lower in vegan groups across studies,32,43-45 with subgroup analyses showing significantly lower HDL-C in vegan women.44 Shang et al42 found that compared to vegans, omnivores and pescatarians were at reduced risk of developing low HDL-C. At the same time, other research reported no significant differences in HDL-C levels between vegans and other diet groups.34,36,40,41
Several studies reported that vegans had significantly lower triglycerides compared to omnivores30,34,36,48 and vegetarians.32 Other research found no difference in triglycerides in vegans compared to omnivores,37,41,44,46,47 or higher triglycerides in vegans compared to omnivores.39,43,44
Overweight. In studies, overweight is typically assessed using BMI, which is calculated by dividing weight in kilograms by height in meters squared. Individuals with a BMI between 25 and 29.9 are considered overweight, while those with a BMI equal to or greater than 30 are considered obese.50
The 18 observational studies11,14,30,31,35,36,39,48,51–60 were published between 1978 and 2018 (see Table 7). In 12 articles, data from larger studies were reported, including EPIC-Oxford (N=4),53,56,58,60 Adventist Health Study-2 (N=3),11,55,57 Indian’s Third National Family Health Survey (N=1),14 German Vegan Study (N=1),35 Swedish Mammography Cohort (N=1),52 MJ Health Screening (N=1)39 and UK Biobank (N=1).31 Including only the most recent reports, the total sample size for these studies was 808,079, including 12,853 vegans, 92,381 vegetarians, 12,781 semi-vegetarians, 28,152 pescatarians, and 661,912 omnivores.
In US studies, vegans had significantly lower BMI than omnivores, vegetarians, pescatarians, and semi-vegetarians.11,36,51,55,57 The BMI of Canadian vegans was not significantly different from that of vegetarians but was significantly lower than that of Canadian omnivores.59
In the UK, vegans had significantly lower BMI than omnivores, regardless of sex.31,48,53,56,58 One study60 found the BMI of vegans was significantly lower than that of vegetarians and was not significantly different from that of pescatarians. Further, weight gain over 5 years was significantly less in vegan compared to omnivore women, but this difference was not observed in men.58 However, when white men were selected for analysis, BMIs for vegans were significantly lower than those of all other diet groups.31
In India, diet groups had similar BMI profiles.14 The percentage of vegans that were overweight did not significantly differ from that of pescatarians, semi-vegetarians, and omnivores, but was significantly lower compared to vegetarians and lacto-vegetarians. The same pattern of results was found in comparisons of obesity rates with the exception that the percentage of vegans who were obese did not significantly differ from the percentage of vegetarians who were obese.
The mean BMI of Swedish vegans did not differ from those of vegetarians and semi-vegetarians, but was significantly lower than that of omnivores.52 Taiwanese vegans had significantly lower BMIs than omnivores, with each additional year of following a vegan diet lowering the risk of obesity.39 No significant differences were found in the BMIs of Vietnamese54 and Nigerian30 vegans versus omnivores.
Discussion
Based on a review of this literature, several health benefits of a vegan diet were identified. Compared to omnivores, vegans were less likely to be diagnosed with NIDDM in the US11,12 but not India.14 There was reduced mortality risk for all vegans (other causes) and male vegans (all causes, ischemic heart disease, cardiovascular disease) in the US19 but not UK18 or in a larger study combining data from multiple cohorts.20 Vegans were at reduced risk for incidence of “any” cancer15,16 (US and UK) and of female cancers15 (US), but only when analyses were not adjusted for BMI.
Mean blood pressure was lower in vegans compared to omnivores from the US,36,38 whereas in other locales there were mixed findings for analyses of SBP and DBP. Similarly, compared to omnivores, vegans’ BMIs were significantly lower in some countries (eg, US,11,36,51,55,57 Sweden,52 Canada,59 Taiwan39) but not others (eg, India,14 Nigeria,30 Vietnam54). The majority of observational studies found superior lipid profiles (except HDL-C and triglycerides) in vegans compared to other diet groups.30,31,37,46-49 However, observational studies of the vegan microbiome reported mixed results.24–27
Significantly lower rates of NIDDM were found for vegans versus omnivores in two large-scale North American studies.11,12 Although not reported in Table 1, when BMI was not included as a covariate, in the US, vegans were less likely to be diagnosed with NIDDM compared to all dietary groups, suggesting that BMI is an important mediator for the analyses of vegans versus vegetarians and pescatarians. Similarly, in a UK study, vegans’ risk of NIDDM was significantly less than omnivores’, but only when there was no BMI adjustment.13 These results are consistent with other research reporting an average diabetes risk reduction of 47–78% in vegans.61 However, adopting a vegan diet did not result in a significant difference in diabetes rates in a large Indian study.14 Agrawal et al14 surmise that the lack of reduced relative risk for their vegan sample compared to the advantage reported for US vegan diabetics was due to 1) the belief among Indians that consuming ghee was permitted on a vegan diet, 2) the consumption of more refined rice by Indian vegans, or 3) reverse causality with some diabetics adopting a vegan diet to better manage their disease. It is unclear whether cultural and socio-economic factors affect diet content and whether other intersecting factors (eg, diabetics choosing a vegan diet to manage symptoms), in turn, affect diet-related prevalence of NIDDM.
Two seminal studies of vegan and omnivore diets provided evidence that a vegan diet decreases "any" cancer risk, but only when the effects of BMI are not partialled out, with the implication being that it is an important mediator.15,16 However, in a recent meta-analysis,62 when the results of these studies were aggregated, there was a significant risk reduction for vegans even when BMI was covaried, because of the larger sample size of the combined studies. However, there was no support that a vegan diet offered protection against diagnosis of most specific cancers with the exception of female-specific cancers, but only when BMI was not a covariate.15 Relatively few studies have investigated the link between veganism and cancer probably due to the low prevalence of vegan cancers in the population when this research was conducted.63
For both sexes together, vegans’ mortality rate for causes other than heart disease, cardiovascular disease and cancer was significantly lower than that of omnivores in a US study19 but not significantly different in a UK study,18 and combined analysis of five data sets.20 In the Orlich et al study, men’s death rates were significantly lower in vegans from all causes, ischemic heart disease and cardiovascular disease.19 Dinu et al62 found a benefit in mortality rates for vegans considered together with vegetarians, but not for vegans alone. However, they did not break down their analysis by sex. It is unclear why, despite the many health benefits of a vegan diet (eg, reduced risk of NIDDM and cancer ("any"), lower TC and LDL cholesterol, and lower BMI), there was not more evidence for a mortality advantage. One possibility is that the relatively advanced health care systems in the countries where this research was conducted were able to effectively treat diseases, therefore delaying mortality in sick people.18 Insufficient sample size representing the vegan population is also partly responsible for the sparseness of this evidence.20
Investigations of the microbiome of vegans and omnivores have reported mixed results. Two cross-sectional studies of vegans and omnivores reported a comparatively favorable profile for the gut microbiota in the vegan sample, suggesting potential positive effects on fecal flora of a vegan diet.24,25 At the same time, a fecal analysis examining the gut make-up of individuals following different vegetarian diets did not reveal significant differences.27 However, the Ruengsomwong et al sample of vegans was small (n=3). Similarly, in US urban vegans, the microbiome was not significantly different from that of omnivores, but there were significant differences in their plasma metabolome.26 Specifically, in the plasma metabolome of vegans, compared to omnivores there were more numerous bacterial metabolites and fewer amino acid metabolites, differences associated with improved health outcomes such as increases in beneficial bacterially generated metabolites (eg, equol) and reductions in harmful metabolites like trimethylamine. The authors note that gut microbiota affected the make-up of the plasma metabolome to a greater extent in vegans than in omnivores and that environmental differences can affect gut microbiota, an observation that is in line with the geographic differences in findings described in these articles.
Compared to omnivores, the lower mean SBPs and DBPs in vegans were found in US studies.36,38 Moreover, vegans’ SBP and DBP levels did not significantly differ from those of vegetarians, semi-vegetarians, and pescatarians. In the remainder of the research, there were no significant blood pressure differences in comparisons of vegans to other dietary groups29,30,32–35 with only a few exceptions.29,31,34,37 Other considerations may have impacted these results, for example that persons with hypertension routinely take medications to lower their blood pressures. Indeed, examination of means for dietary groups revealed that most were well within normotensive ranges.
The large majority of observational studies found more favorable lipid profiles in vegans than in omnivores and other comparison groups.30,36,37,41,45-49 These findings are consistent with results from a recent meta-analysis assessing the relationship between lipids and vegetarian diets.4 There is a strong relationship between high levels of TC and LDL-C and intake of saturated fat, which in the human omnivore diet is derived predominantly from animal sources.64
The varied results for triglycerides may be explained by geographic differences. Vegans had higher triglyceride levels in studies conducted in Taiwan whereas other research showed they had either lower levels or levels that were not significantly different. In trying to explain this discrepancy, Shang et al42 note that the omnivore diet in Taiwan differs from the typical Western diet in that there are more plant foods, no dairy and lesser quantities of other animal-derived foods. This finding is consistent with a meta-analysis of vegan diets and cardio-metabolic risk factors that also found a different pattern of results in some Taiwan studies.65
The results for HDL-C levels were also mixed, with studies reporting either less favorable levels for vegans or non-significant differences. Low HDL-C and high triglycerides have been considered components of metabolic syndrome and independent risk factors for cardiovascular disease.43 However, other research has cast doubt on this relationship with respect to HDL-C4 as interventions66 and genetic variants67 that increase HDL-C do not reduce coronary heart disease risk. As later follow-up analyses showed no associations, Chiu et al39 proposed that poorer triglycerides and HDL-C in vegetarians and vegans may be due to “reverse causation”, in which individuals with medical conditions switch to a vegetarian diet in order to improve their health.
Vegans had lower BMI or overweight/obesity rates than omnivores in some countries (eg, US,11,36,51,55,57 Sweden,52 Canada,59 Taiwan39), but these differences were not found in other countries (eg, India,14 Nigeria,30 Vietnam54). In the Nigerian study,30 there were only 8 vegans, so that comparison was likely insufficiently powered. The Vietnamese study54 assessed vegan Buddhist nuns and matched controls. In both groups, the mean BMI was 24, well within the normal range. The larger US studies in this review did not report average BMI of their female participants. However, in the US, the BMI of the average adult woman is 26.5,68 which is in the overweight range. The data for the Indian sample14 were divided according to weight status category (eg, underweight, overweight, obese) and the proportions in each following different diets were compared. Across diet categories, the percentage of individuals who were overweight or obese was small by Western standards, ranging from 10% in pescatarians (11.5% in vegans) to 16.2% in lacto-vegetarians. Considering these results and those of the other observational studies that were reviewed, compared to an omnivore diet consuming a vegan diet appears to provide some protection against overweight in non-Asian countries, possibly because obesity is more prevalent in these locations. In terms of the differences between vegans versus vegetarians, semi-vegetarians, and pescatarians, the results were inconsistent.
An important finding from this review was that demographic variables moderated the relationship between consuming a vegan diet and some outcomes. For example, in a US study, there were sex differences in mortality (from all causes, ischemic heart disease and cardiovascular disease) with male vegans reporting significantly lower rates than their omnivore counterparts while there was not a significant difference in female mortality rates.19 In the UK, vegan white women had lower SBP and DBP than omnivore white women and lower DBP than vegetarian white women. Vegan white men had lower SBP and DBP than their vegetarian and omnivore counterparts, with DBP also lower than all other white male dietary groups. Geographic location exerted a moderating effect, with the most wide-ranging evidence for the health benefits of a vegan diet coming from the US. In American studies there were lower rates of NIDDM compared to omnivores;11,12 reduced incidence of “any” and female cancer relative to omnivores when data were aggregated with UK data;15 decreased “other cause” mortality risk in men, as well as reduced mortality risk due to cardiovascular disease, coronary heart disease, and all cause compared to omnivores;19 significantly lower SBP and DBP compared to omnivores,36 but not vegetarians;32,38 superior lipid profiles to both vegetarians32 and omnivores;36,38 and significantly lower BMI compared to omnivores.11,36,51,55,57 In the UK, the evidence was still strong but not as extensive as in the US. In UK studies, compared to omnivores, vegans had reduced risk of “any” cancer when data were aggregated with US data;16 decreased TC and LDL-C;29,40,45,48,49 and significantly lower BMI.48,53,56,60 In the UK, there was evidence for BMI mediating the relationship between vegan diet choice and reduced incidence of NIDDM.13 The evidence for lower blood pressure in vegans versus omnivores was mixed.29,33,34 However, in Asian countries, there was less evidence for the health advantages of a vegan diet.43,65 In India, the proportion of overweight and obese vegans did not significantly differ from the proportion of overweight and obese omnivores and pescatarians, but were significantly lower than the corresponding percentages of lacto-vegetarians.14 Of interest, compared to vegans, Indian lacto-vegetarians also had a lower risk of NIDDM, despite having a higher risk of overweight and obesity. In Taiwan, there was a lower risk of high SBP and high DBP in vegans compared to omnivores,39 although in a small study vegan nuns had higher DBP than omnivore nuns.37 However, lipid profiles for vegans in Taiwan did not compare as favorably to their omnivore counterparts with most studies showing significantly worse HDL-C39,42–44 and triglycerides43,44 for Taiwanese vegans with only a few comparisons showing an advantage for TC37,43,44 and LDL-C39,43 while others reported non-significant differences.43,44 In one Taiwanese study, vegans had a significantly reduced risk of overweight.39 However, in one study from Vietnam,69 there was no significant difference in BMIs between vegan and omnivore nuns although the sample size was relatively small.
As to why these discrepancies in results exist, there are several possible explanations. We screened in more studies from the US and UK, so the relative dearth of evidence in Asian countries may be due, in part, to less research that was screened into our review or that may not have been performed at all. Other possibilities include regional differences in cuisine (the typical foods consumed on both vegan and omnivore diets), and international disparities in obesity rates, socio-economic statuses or other religious and/or cultural factors. Regardless of the reason, the evidence for the benefits of a vegan diet was strongest in the US, less strong in the UK, and weakest in Asian countries.
Other important causal factors related to how the reviewed studies were conducted may have affected results. The healthfulness of the vegan diet can make a difference in outcome for both cardiovascular disease70 and NIDDM.71 For free-living vegans, the reason for choosing the diet (eg, health, concern for animals) may be associated with diet quality.72 Individuals citing health as their primary reason for adopting a vegan diet reported consuming fewer sweets and more fruit whereas those citing concern for animals as the primary reason reported greater intake of soy, foods containing vitamin D and vitamin supplements (D and B12). Geographic location is also an important consideration as vegans in the US (Adventist 2) reported consuming more fiber and vitamin C than their British counterparts (EPIC-Oxford).19 These results suggest that evaluating how the content of vegan diets affects outcomes is an important area for further research.
An important mediator that affected outcomes was BMI. In several studies, results were reported both with and without BMI as a covariate. In our Tables, we only listed results that were adjusted for BMI. However, in studies of NIDDM and cancer, inclusion of BMI as a covariate not only made a difference in the results of individual studies, but also affected the aggregate research that was reviewed. Adjustment for BMI in studies of NIDDM affected the overall pattern of results in that US vegans were no longer at reduced risk of NIDDM compared to vegetarians and pescatarians.11,12 However, even with adjustment for BMI, vegans’ risk of NIDDM was less than that of omnivores, suggesting that following a vegan diet did affect diabetes risk independent of BMI in the US. In the UK, adopting a vegan versus omnivore diet significantly reduced the risk of NIDDM only when the effects of BMI were not covaried.13 For cancers, in each of the two studies that were reviewed, adjustment for BMI in analyses shifted the pattern of the results such that reduced risk of any cancer for vegans compared to omnivores was no longer significant.15,16 However, a meta-analysis that statistically aggregated that data showed, that even with the inclusion of BMI, there was a reduced risk of any cancer in vegans.62 Aggregating the data functioned to increase the sample size and consequently shrink the confidence interval so that the analysis was significant.
Dietary adherence is not always measured in observational studies, so the extent to which vegans adhere to their diets is largely unknown. Self-identified vegans (127 for ethical reasons and 80 for health reasons) reported mean numbers of diet violations since beginning their diets, 3.22 ± 6 for ethical vegans and 16 ± 63.8 for health vegans.73 As statistics for duration on their respective diets were not reported, adherence was difficult to assess. Nonetheless, low violation estimates suggest an overall high adherence rate. Regardless, the extent to which adherence is important to health outcomes is unclear. One study compared highly restrictive to more moderate vegans and with one exception (TC) reported non-significant differences (in blood pressure, BMI and some lipid measures35). However, other research suggests that level of adherence to a plant-based diet can make a difference in lowering insulin resistance and in risk of both diagnosis of pre-diabetes and NIDDM.74
One final consideration that can affect the outcome is the dietary group that was selected for comparison to vegans. In a tally of results listed in our tables, the majority of the significant findings were obtained in comparisons of vegans to omnivores (47.2% of total vegan-omnivore comparisons). There were fewer significant findings when comparing vegans to vegetarians (20% of total vegan-vegetarian comparisons), pescatarians (12.5% of total vegan-pescatarian comparisons) and semi-vegetarians (2.5% of total vegan-semi-vegetarian comparisons). This is not surprising considering that an omnivore diet is more discrepant from a vegan diet than either vegetarian or pescatarian diets. The relatively small number of favorable comparisons for vegan versus semi-vegetarian diets was largely driven by the large number of null findings comparing these two groups on measures of mortality. Regardless, this survey of findings is consistent with the idea that there is more research support for the benefits of a vegan diet when it is compared to an omnivore diet (as opposed to other vegetarian/pescatarian diets).
Several limitations to this review should be acknowledged. First, although adjustment for potential confounders was one criterion for judging a study’s inclusion, there may have been other confounders that were not addressed (eg, medication usage). Second, several of our included studies reported multiple outcomes. Consequently, the conclusions for some of the outcomes were based, at least in part, on data from the same participants. Third, to evaluate research in the aggregate and facilitate comparisons, dietary groups with different names but similar definitions were given uniform names (eg, meat-eaters were called omnivores). There may have been small differences across studies in how these groups were defined, although there is inevitably some diversity in food choices among people following common diets. Fourth, because these studies investigated free-living vegans, the amount of time that individuals practiced the diet was not uniform and varied both within and across studies. Fifth, although an attempt was made to cover diverse outcomes in this review; there were some areas that were omitted. For example, we did not review studies of mental health outcomes and we excluded studies of children on vegan diets. Sixth, because the health benefits of a vegan diet is a broad topic, we were limited in the extent to which we could cover each medical condition or nutritional status. Seventh, because we used scores on the NOS scales to evaluate study quality, there may have been some studies that were excluded, not because they were poorly executed but because they did not report sufficient detail to score high enough to be screened into the review.
Conclusion
To summarize, there was strong evidence that free-living vegans were less likely than omnivores to develop NIDDM (in the US). Vegans had reduced TC and LDL-C levels, and lower BMIs (in non-Asian locales) compared to omnivores, and in some cases, other dietary groups.
There was evidence that when the effects of BMI were not covaried or when results were aggregated across studies, vegans were less likely than omnivores to develop cancer (all cause). Similarly, there was evidence that BMI mediated the relationship between vegan vs omnivore diet status and development of NIDDM in the UK and between vegan vs vegetarian and pescatarian diet status and development of NIDDM in the US.
There was inconsistent evidence that a vegan diet reduced risk of diagnosis of female cancers and improved mortality rates. There was also mixed evidence that vegans had lower triglycerides and blood pressure, and healthier microbiota.
Finally, we found no evidence that vegans were at reduced risk of developing most specific cancers. Further, in Indian vegans, there was not a reduced probability of overweight, obesity, or NIDDM. Moreover, the preponderance of evidence showed lower HDL-C in vegans compared to omnivores or no significant differences.
Evidence supporting the health benefits of a vegan diet was strongest in the US and weaker in Asian countries. As the number of vegans increases worldwide, there is a need for additional studies of the diet’s protective and therapeutic effects, the pathways through which it exerts them, and the role of moderators and other causal factors in how they are manifested.
Acknowledgments
The authors wish to acknowledge the assistance of Ilana Brodzki, Rachel Concha, Mira Tesla, and Robert McGrath.
Disclosure
The authors report no conflicts of interest in this work.
References
1. Leneman L. No animal food: the road to Veganism in Britain, 1909–1944. Soc Anim. 1999;7(2):219–228. doi:10.1163/156853099X00095
2. Definition of Veganism. the Vegan society. Available from: https://www.vegansociety.com/go-vegan/definition-veganism.
3. Craig WJ. Health effects of vegan diets. Am J Clin Nutr. 2009;89(5):1627–1633. doi:10.3945/ajcn.2009.26736N.Am
4. Yokoyama Y, Levin SM, Barnard ND. Association between plant-based diets and plasma lipids: a systematic review and meta-analysis. Nutr Rev. 2017;75(9):683–698. doi:10.1093/nutrit/nux030
5. Melina V, Craig W, Levin S. Position of the academy of nutrition and dietetics: vegetarian Diets. J Acad Nutr Diet. 2016;116(12):1970–1980. doi:10.1016/j.jand.2016.09.025
6. Snyder H. Literature review as a research methodology: an overview and guidelines. J Bus Res. 2019;104:333–339. doi:10.1016/j.jbusres.2019.07.039
7. Harms M. The Equator network and the PRISMA statement for the reporting of systematic reviews and meta-analyses. Physiotherapy. 2009;95(4):237–240. doi:10.1016/j.physio.2009.10.001
8. Liberati A, Altman DG, Tetzlaff J, et al. The PRISMA statement for reporting systematic reviews and meta-analyses of studies that evaluate healthcare interventions: explanation and elaboration. BMJ. 2009;339(jul21 1):b2700–b2700. doi:10.1136/bmj.b2700
9. Stang A. Critical evaluation of the Newcastle-Ottawa scale for the assessment of the quality of nonrandomized studies in meta-analyses. Eur J Epidemiol. 2010;25(9):603–605. doi:10.1007/s10654-010-9491-z
10. Herzog R, Alvarez-Pasquin MJ, Diaz C, Del Barrio JL, Estrada JM, Gil A. Are healthcare workers’ intentions to vaccinate related to their knowledge, beliefs and attitudes? A systematic review. BMC Public Health. 2013;13(154). doi:10.1186/1471-2458-13-154
11. Tonstad S, Butler T, Yan R, et al. Type of vegetarian diet, body weight, and prevalence of type 2 diabetes. Diabetes Care. 2009;32(5):791–796. doi:10.2337/dc08-1886
12. Tonstad S, Stewart K, Oda K, Batech M, Herring RP, Fraser GE. Vegetarian diets and incidence of diabetes in the Adventist Health Study-2. Nutr Metab Cardiovasc Dis. 2013;23(4):292–299. doi:10.1016/j.numecd.2011.07.004
13. Papier K, Appleby PN, Fensom GK, et al. Vegetarian diets and risk of hospitalisation or death with diabetes in British adults: results from the EPIC-Oxford Study. Nutr Diabetes. 2019;9(8). doi:10.1038/s41387-019-0074-0
14. Agrawal S, Millett CJ, Dhillon PK, Subramanian S, Ebrahim S. Type of vegetarian diet, obesity and diabetes in adult Indian population. Nutr J. 2014;13(1). doi:10.1186/1475-2891-13-89
15. Tantamango-bartley Y, Jaceldo-siegl K, Fan J, Fraser G. Vegetarian diets and the incidence of cancer in a low-risk population. Cancer Epidemiol Biomarkers Prev. 2013;22(2):286–294. doi:10.1158/1055-9965.EPI-12-1060
16. Key TJ, Appleby PN, Crowe FL, Bradbury KE, Schmidt JA, Travis RC. Cancer in British vegetarians: updated analyses of 4998 incident cancers in a cohort of 32,491 meat eaters, 8612 fish eaters, 18,298 vegetarians, and 2246 vegans. Am J Clin Nutr. 2014;100(SUPPL. 1):378–385. doi:10.3945/ajcn.113.071266
17. Penniecook-sawyers JA, Jaceldo-siegl K, Fan J, et al. Vegetarian dietary patterns and the risk of breast cancer in a low-risk population. Br J Nutr. 2016;115(10):1790–1797. doi:10.1017/S0007114516000751
18. Appleby PN, Crowe FL, Bradbury KE, Travis RC, Key TJ. Mortality in vegetarians and comparable nonvegetarians in the United Kingdom. Am J Clin Nutr. 2016;103(1):218–230. doi:10.3945/ajcn.115.119461
19. Orlich MJ, Singh PN, Sabaté J, et al. Vegetarian dietary patterns and mortality in adventist health study 2. JAMA Intern Med. 2013;173(13):1230–1238. doi:10.1001/jamainternmed.2013.6473
20. Key TJ, Fraser GE, Thorogood M, et al. Mortality in vegetarians and nonvegetarians: detailed findings from a collaborative analysis of 5 prospective studies. Am J Clin Nutr. 1999;70(3 SUPPL):516–524. doi:10.1093/ajcn/70.3.516s
21. Shreiner AB, Kao JY, Young VB. The gut microbiome in health and in disease. Curr Opin Gastroenterol. 2015;31(1):69–75. doi:10.1097/MOG.0000000000000139
22. Cox A, West NP, Cripps AW. Obesity, inflammation, and the gut microbiota. Lancet Diabetes Endocrinol. 2015;3(3):207–215. doi:10.1016/S2213-8587(14)70134-2
23. Glick-Bauer M, Yeh M. The health advantage of a vegan diet: exploring the gut microbiota connection. Nutrients. 2014;6(11):4822–4838. doi:10.3390/nu6114822
24. Ferrocino I, Di Cagno R, De Angelis M, et al. Fecal microbiota in healthy subjects following omnivore, vegetarian and vegan diets: culturable populations and rRNA DGGE profiling. PLoS One. 2015;10(6):1–16. doi:10.1371/journal.pone.0128669
25. Zimmer J, Lange B, Frick JS, et al. A vegan or vegetarian diet substantially alters the human colonic faecal microbiota. Eur J Clin Nutr. 2012;66(1):53–60. doi:10.1038/ejcn.2011.141
26. Wu GD, Compher C, Chen EZ, et al. Comparative metabolomics in vegans and omnivores reveal constraints on diet-dependent gut microbiota metabolite production. Gut. 2016;65(1):63–72. doi:10.1136/gutjnl-2014-308209.Comparative
27. Ruengsomwong S, La-ongkham O, Jiang J, Wannissorn B, Nakayama J, Nitisinpraser S. Microbial community of healthy Thai vegetarians and non-vegetarians, their core gut microbiota and pathogens risk. J Microbiol Biotechnol. 2016;26(10):1723–1735. doi:10.4014/jmb.1603.03057
28. Guilbert JJ. The world health report 2002 - Reducing risks, promoting healthy life [2]. Educ Heal. 2003;16(2):230.doi:10.1080/1357628031000116808
29. Sanders TAB, Key TJ. Blood pressure, plasma renin activity and aldosterone concentrations in Vegans and Omnivore controls. Hum Nutr Appl Nutr. 1987;41A:204–211.
30. Famodu AA, Osilesi O, Makinde YO, Osonuga OA. Blood pressure and blood lipid levels among vegetarian, semi- vegetarian, and non-vegetarian native Africans. Clin Biochem. 1998;31(7):545–549. doi:10.1016/S0009-9120(98)00067-8
31. Tong T, Key TJ, Sobieki JG, Bradbury K. Anthropometric and physiologic characteristics in white and British Indian vegetarians and nonvegetarians in the UK Biobank. Am J Clin Nutr. 2018;107(6):909–920. doi:10.1093/ajcn/nqy042
32. Toohey ML, Harris MA, Melby CL, Williams DW, Foster G, Schmidt WD. Cardiovascular disease risk factors are lower in african-american vegans compared to lacto-ovo-vegetarians. J Am Coll Nutr. 1998;17(5):425–434. doi:10.1080/07315724.1998.10718789
33. Appleby PN, Davey GK, Key TJ. Hypertension and blood pressure among meat eaters, fish eaters, vegetarians and vegans in EPIC–Oxford. Public Health Nutr. 2002;5(5):645–654. doi:10.1079/phn2002332
34. Goff LM, Bell JD, So PW, Dornhorst A, Frost GS. Veganism and its relationship with insulin resistance and intramyocellular lipid. Eur J Clin Nutr. 2005;59(2):291–298. doi:10.1038/sj.ejcn.1602076
35. Waldmann A, Koschizke JW, Leitzmann C, Hahn A. German vegan study: diet, life-style factors, and cardiovascular risk profile. Ann Nutr Metab. 2005;49(6):366–372. doi:10.1159/000088888
36. Fontana L, Meyer TE, Klein S, Holloszy JO. Long-term low-calorie low-protein vegan diet and endurance exercise are associated with low cardiometabolic risk. Rejuvenation Res. 2007;10(2):225–234. doi:10.1089/rej.2006.0529
37. Lin CK, Lin DJ, Yen CH, et al. Comparison of renal function and other health outcomes in vegetarians versus omnivores in Taiwan. J Heal Popul Nutr. 2010;28(5):470–475. doi:10.3329/jhpn.v28i5.6155
38. Pettersen BJ, Anousheh R, Fan J, Jaceldo-siegl K, Fraser GE. Vegetarian diets and blood pressure among white subjects: results from the Adventist Health Study-2 (AHS-2). Public Health Nutr. 2012;15(10):1909–1916. doi:10.1017/S1368980011003454
39. Chiu YF, Hsu CC, Chiu THT, et al. Cross-sectional and longitudinal comparisons of metabolic profiles between vegetarian and non-vegetarian subjects: a matched cohort study. Br J Nutr. 2015;114(8):1313–1320. doi:10.1017/S0007114515002937
40. Thomas HV, Davey GK, Key TJ. Oestradiol and sex hormone-binding globulin in premenopausal and post-menopausal meat-eaters, vegetarians and vegans. Br J Cancer. 1999;80(9):1470–1475. doi:10.1038/sj.bjc.6690546
41. Vinagre JC, Vinagre CG, Pozzi FS, Slywitch E, Maranhão RC. Metabolism of triglyceride-rich lipoproteins and transfer of lipids to high-density lipoproteins (HDL) in vegan and omnivore subjects. Nutr Metab Cardiovasc Dis. 2013;23(1):61–67. doi:10.1016/j.numecd.2011.02.011
42. Shang P, Shu Z, Wang Y, et al. Veganism does not reduce the risk of the metabolic syndrome in a taiwanese cohort. Asia Pac J Clin Nutr. 2011;20(3):404–410.
43. Jian ZH, Chiang YC, Lung CC, et al. Vegetarian diet and cholesterol and TAG levels by gender. Public Health Nutr. 2014;18(4):721–726. doi:10.1017/S1368980014000883
44. Huang YW, Jian ZH, Chang HC, et al. Vegan diet and blood lipid profiles: a cross-sectional study of pre and postmenopausal women. BMC Womens Health. 2014;14(1):2–7. doi:10.1186/1472-6874-14-55
45. Bradbury KE, Crowe FL, Appleby PN, Schmidt JA, Travis RC, Key TJ. Serum concentrations of cholesterol, apolipoprotein A-I, and apolipoprotein B in a total of 1 694 meat-eaters, fish-eaters, vegetarians, and vegans. Eur J Clin Nutr. 2014;68(2):178–183. doi:10.1038/ejcn.2013.248
46. Elorinne AL, Alfthan G, Erlund I, et al. Food and nutrient intake and nutritional status of Finnish vegans and non-vegetarians. PLoS One. 2016;11(2):1–14. doi:10.1371/journal.pone.0148235
47. Kuchta A, Ebiedzińska AL, Fijałkowski M, et al. Impact of plant-based diet on lipid risk factors for atherosclerosis. Cardiol J. 2016;23(2):141–148. doi:10.5603/CJ.a2016.0002
48. Sanders TAB, Ellis FR, Dickerson JWT. Studies of vegans: the fatty acid composition of plasma choline phosphoglycerides, erythrocytes, adipose tissue, and breast milk, and some indicators of susceptibility to ischemic heart disease in vegans and omnivore controls. Am J Clin Nutr. 1978;31(5):805–813. doi:10.1093/ajcn/31.5.805
49. Thorogood M, Roe L, McPherson K, Mann J. Dietary intake and plasma lipid levels: lessons from a study of the diet of health conscious groups. Br Med J. 1990;300(6735):1297–1301. doi:10.1136/bmj.300.6735.1297
50. National Heart Lung and Blood Institute, National Institutes of Health (NIH) National Heart, Lung, and Blood Institute N. Clinical Guidelines on the Identification, Evaluation, and Treatment of Overweight and Obesity in Adults. The Evidence Report, NIH Publication No. 98-4083.; 1998. doi:10.1001/jama.2012.39
51. Fontana L, Shew JL, Holloszy JO, Villareal DT. Low bone mass in subjects on a long-term raw vegetarian diet. Arch Intern Med. 2005;165(6):684–689. doi:10.1001/archinte.165.6.684
52. Newby PK, Tucker KL, Wolk A. Risk of overweight and obesity among semivegetarian, lactovegetarian, and vegan women. Am J Clin Nutr. 2005;81(6):1267–1274. doi:10.1093/ajcn/81.6.1267
53. Rosell MS, Lloyd-Wright Z, Appleby PN, Sanders TAB, Allen NE, Key TJ. Long-chain n-3 polyunsaturated fatty acids in plasma in British meat-eating, vegetarian, and vegan men. Am J Clin Nutr. 2005;82(2):327–334. doi:10.1093/ajcn/82.2.327
54. Ho-Pham LT, Nguyen PLT, Le TTTA, et al. Veganism, bone mineral density, and body composition: a study in Buddhist nuns. Osteoporos Int. 2009;20(12):2087–2093. doi:10.1007/s00198-009-0916-z
55. Rizzo NS, Jaceldo-Siegl K, Sabate J, Fraser GE. Nutrient profiles of vegetarian and nonvegetarian dietary patterns. J Acad Nutr Diet. 2013;113(12):1610–1619. doi:10.1016/j.jand.2013.06.349
56. Schmidt JA, Crowe FL, Appleby PN, Key TJ, Travis RC. Serum uric acid concentrations in meat eaters, fish eaters, vegetarians and vegans: a cross-sectional analysis in the EPIC-Oxford Cohort. PLoS One. 2013;8(2). doi:10.1371/journal.pone.0056339
57. Tonstad S, Nathan E, Oda K, et al. Prevalence of hyperthyroidism acc. Public health nutr. 2015;18(June2001):1482–1487. doi:10.1017/S1368980014002183.
58. Rosell M, Appleby P, Spencer E, Key T. Weight gain over 5 years in 21 966 meat-eating, fish-eating, vegetarian, and vegan men and women in EPIC-Oxford. Int J Obes. 2006;30(9):1389–1396. doi:10.1038/sj.ijo.0803305
59. Barr SI, Prior JC, Janelle KC, Lentle BC. Spinal bone mineral density in premenopausal vegetarian and nonvegetarian women: cross-sectional and prospective comparisons. J Am Diet Assoc. 1998;98(7):760–765. doi:10.1016/S0002-8223(98)00172-2
60. Spencer EA, Appleby PN, Davey GK, Key TJ. Diet and body mass index in 38 000 EPIC-Oxford meat-eaters, fish-eaters, vegetarians and vegans. Int J Obes. 2003;27(6):728–734. doi:10.1038/sj.ijo.0802300
61. Le LT, Sabate J. Beyond meatless, the health effects of vegan diets: findings from the adventist cohorts. Nutrients. 2014;6(6):2131–2147. doi:10.3390/nu6062131
62. Dinu M, Abbate R, Franco G, Casini A, Sofi F. Vegetarian, vegan diets and multiple health outcomes: a systematic review with meta-analysis of observational studies. Crit Rev Food Sci Nutr. 2017;57(17):3640–3649. doi:10.1080/10408398.2016.1138447
63. Lanou A, Svenson B. Reduced cancer risk in vegetarians: an analysis of recent reports. Cancer Manag Res. 2011;3:1–8.
64. Mattson FH, Grundy SM. Comparison of effects of dietary saturated, monounsaturated, and polyunsaturated fatty acids on plasma lipids and lipoproteins in man. J Lipid Res. 1985;26(2):194–202.
65. Benatar JR, Stewart RAH. Cardiometabolic risk factors in vegans; A meta-analysis of observational studies. PLoS One. 2018;13(12):1–23. doi:10.1371/journal.pone.0209086
66. Keene D, Price C, Shun-Shin MJ, Francis DP. Effect on cardiovascular risk of high density lipoprotein targeted drug treatments niacin, fibrates, and CETP inhibitors: metaanalysis of randomised controlled trials including 117,411 patients. BMJ. 2014;349(jul18 2):4379. doi:10.1136/bmj.g4379
67. Frikke-Schmidt R, Nordestgaard BG, Stene MC. Association of loss-of-function mutations in the ABCA1 gene with high-density lipoprotein cholesterol levels and risk of ischemic heart disease. J Am Med Assoc. 2008;299(21):2524–2532. doi:10.1001/jama.299.21.2524
68. Healthy weight, overweight, and obesity among U.S. adults. National Health and Nutrition Examination Survey. Available from: https://www.cdc.gov/nchs/data/nhanes/databriefs/adultweight.pdf.
69. Walls HL, Peeters A, Son PT, et al. Prevalence of underweight, overweight and obesity in urban Hanoi, Vietnam. Asia Pac J Clin Nutr. 2009;18(2):234–239.
70. Hemler E, Hu FB. Plant-based diets for cardiovascular disease prevention: all plant foods are not created equal. Curr Atheroscler Rep. 2019;21:18. doi:10.1007/s11883-019-0779-5
71. Qian F, Liu G, Hu FB, Bhupathiraju SN, Sun Q. Association between plant-based dietary patterns and risk of type 2 diabetes a systematic review and meta-analysis. JAMA Intern Med. 2019;179(10):1335–1344. doi:10.1001/jamainternmed.2019.2195
72. Radnitz C, Beezhold B, DiMatteo J. Investigation of lifestyle choices of individuals following a vegan diet for health and ethical reasons. Appetite. 2015;90:31–36. doi:10.1016/j.appet.2015.02.026
73. Rothgerber H. Can you have your meat and eat it too? Conscientious omnivores, vegetarians, and adherence to diet. Appetite. 2015;84:196–203. doi:10.1016/j.appet.2014.10.012
74. Chen Z, Zuurmond MG, Van der Schaft N, Nano J, Wijinhoven HAH, Ikram MA. Plant versus animal based diets and insulin resistance, prediabetes and type 2 diabetes: the Rotterdam Study. Eur J Epidemiol. 2018;33(9). doi:10.1007/s10654-018-0414-
 © 2020 The Author(s). This work is published and licensed by Dove Medical Press Limited. The full terms of this license are available at https://www.dovepress.com/terms.php and incorporate the Creative Commons Attribution - Non Commercial (unported, v3.0) License.
By accessing the work you hereby accept the Terms. Non-commercial uses of the work are permitted without any further permission from Dove Medical Press Limited, provided the work is properly attributed. For permission for commercial use of this work, please see paragraphs 4.2 and 5 of our Terms.
© 2020 The Author(s). This work is published and licensed by Dove Medical Press Limited. The full terms of this license are available at https://www.dovepress.com/terms.php and incorporate the Creative Commons Attribution - Non Commercial (unported, v3.0) License.
By accessing the work you hereby accept the Terms. Non-commercial uses of the work are permitted without any further permission from Dove Medical Press Limited, provided the work is properly attributed. For permission for commercial use of this work, please see paragraphs 4.2 and 5 of our Terms.
