Back to Journals » Biologics: Targets and Therapy » Volume 16
Biosimilars in Pediatric IBD: Updated Considerations for Disease Management
Authors Dipasquale V , Cucinotta U , Romano C
Received 18 March 2022
Accepted for publication 3 June 2022
Published 13 June 2022 Volume 2022:16 Pages 57—66
DOI https://doi.org/10.2147/BTT.S367032
Checked for plagiarism Yes
Review by Single anonymous peer review
Peer reviewer comments 2
Editor who approved publication: Dr Doris Benbrook
Valeria Dipasquale, Ugo Cucinotta, Claudio Romano
Pediatric Gastroenterology and Cystic Fibrosis Unit, Department of Human Pathology in Adulthood and Childhood “G. Barresi”, University of Messina, Messina, Italy
Correspondence: Valeria Dipasquale, Pediatric Gastroenterology and Cystic Fibrosis Unit, Department of Human Pathology in Adulthood and Childhood “G. Barresi”, University of Messina, Via Consolare Valeria 1, Messina, 98124, Italy, Tel +390902212918, Email [email protected]
Abstract: Biologic drugs have significantly modified the pharmacological management of several chronic conditions, including inflammatory bowel diseases (IBD). By contrast, in the last two decades, biologics have been associated with increased direct medical costs. As patents for the reference drugs have expired, the development and commercialization of biosimilars through abbreviated licensing pathways represented an affordable alternative in patients fulfilling the indication for biologics. A growing body of evidence, first in adults and then in the pediatric age group too, has provided reassuring data in terms of efficacy and safety of biosimilars both in naïve patients and in those previously on reference drugs who had to switch to the biosimilar. This review summarizes the currently available evidence for biosimilar use in IBD, with a focus on pediatric IBD. The most common practical approaches to biosimilar use in the pediatric clinical settings are also discussed.
Keywords: anti-TNF, CT-P13, Crohn’s disease, ulcerative colitis, inflammatory bowel disease, children
Introduction
Inflammatory bowel diseases (IBDs), which include Crohn’s disease (CD), ulcerative colitis (UC), and inflammatory bowel disease unclassified (IBD-U), are chronic, life-long diseases that affect the gastrointestinal tract and have relapsing-remitting behavior.1,2 Traditionally, broad-spectrum anti-inflammatory medications such as amino-salicylates and steroids, as well as immunosuppressive agents including thiopurines or methotrexate, have been used in treatment.3,4 Over the last few decades, the prevalence of IBD has risen exponentially in developed nations, both in children and adults, creating the opportunity for novel therapeutic approaches.5,6 The introduction of monoclonal antibodies directed against tumor necrosis factor-α (TNF-α), an inflammatory cytokine produced by activated macrophages, T lymphocytes, and natural killer cells, has significantly changed the management and outcome of IBDs and has become a core component of the pharmacological treatment for these diseases.3,4 However, these drugs are expensive and constitute a major source of healthcare spending for IBD patients.7 The patent on the reference anti-TNF-α infliximab (IFX) expired in 2013, allowing companies to commercialize its biosimilar. Biosimilars are a major topic of interest in terms of lowering the financial burden of certain chronic diseases, including IBD.8 The present study aims to provide an in-depth overview of the key aspects of biosimilar use in IBD, with an updated focus on their use in pediatric IBD.
Biologic Therapies in IBD
Biologic drugs are monoclonal antibodies that target specific cytokines implicated in the inflammatory cascade, such as TNF-α or small molecules like integrins or interleukin 12 and 23, which can be produced by living cells, blood, or plasma, or produced using recombinant DNA and controlled gene expression technologies.9 The binding and neutralization of TNF-α, both soluble and transmembrane, is the most recognized mechanism of action of these drugs, but other possible mechanisms of action have emerged as having a potential role in IBD (Figure 1). The majority of them have been demonstrated to be comparable between the reference anti-TNF-α drugs (infliximab, IFX; adalimumab, ADA) and their respective first biosimilars (CT-P13 and ABP 501, respectively).10
 |
Figure 1 Key mechanisms of action of anti-TNF agents in inflammatory bowel diseases. TNF, tumor necrosis factor; Ck, cytokine. |
The medical management of IBD was significantly changed by the introduction of these molecules, with the first being the anti-TNF-α IFX, which received the Food and Drug Administration (FDA) approval for CD in 1998. Since that time, other anti-TNF-α molecules, including adalimumab and golimumab, have been licensed for use in both adults and children (Table 1). In children, the anti-TNF-α reference drugs currently available to treat IBD are represented by IFX (Remicade, Janssen) and ADA (Humira, AbbVie).3,4 Biologic treatment is increasingly considered as a key component of the medical management of both adult and pediatric IBDs. In various clinical trials and real-world studies, its efficacy has been proven in terms of induction and maintenance of remission, steroid-sparing effects, mucosal healing, higher quality of life, and lower rates of admissions and surgery.11–14 In pediatric CD patients, anti-TNF-α therapy is indicated for induction and maintenance of remission in cases of severe active disease despite immunomodulator treatment (step-up therapy). In pediatric UC patients, IFX should be considered in chronically active or steroid-dependent disease, uncontrolled by mesalamine and thiopurines, for both induction and maintenance of remission.4 ADA could be considered for those who initially respond but then lose response or are intolerant to IFX.4 In new-onset patients with a high risk of a complicated disease course, as well as extraintestinal manifestations and/or fistulizing perianal CD, anti-TNF-α therapy is recommended as first-line treatment (top-down strategy).3,4,15,16 The good efficacy and safety profile of biologic drugs, along with growing confidence in their utilization, have progressively supported the top-down strategy and/or longer duration of treatment.3,4
 |
Table 1 Mechanisms of Actions and Indications of EMA Approved Biologics for IBD |
Biosimilars in the Management of Pediatric IBD
The relatively high costs of anti-TNF-α agents, combined with the impending or actual expiration of patents for several biologic drugs, has resulted in the development of “highly similar” versions of the reference product known as “biosimilars,” which are viewed as important tools for controlling costs and increasing access to biologic drugs.17,18 In pediatric IBD clinical practice, biosimilars may be used in some situations (Table 2).
 |
Table 2 Clinical Settings for Biosimilar Use in Pediatric IBD |
What are Biosimilars Made of?
As defined by the FDA, a biosimilar is highly similar to an existing FDA-approved reference product in terms of safety, purity, and potency (safety and effectiveness).19 According to the World Health Organization (WHO), a biosimilar consists of a “biotherapeutic product which is similar in terms of quality, safety, and efficacy to an already licensed reference biotherapeutic product”.20 The regulatory process for a biosimilar worldwide is centered on showing biosimilarity between the biosimilar and the reference drug in terms of structural and functional characteristics, biological property (bioactivity), and immunogenicity. It is worth noting that the regulatory process is not intended to “independently establish the safety and efficacy of the proposed product,”19 because it has already been proven for the originator. A four-step approach is used to perform the similarity evaluation, which includes preclinical molecular, structural, and functional analytic studies, as well as clinical pharmacokinetic, pharmacodynamic, effectiveness, safety, and immunogenicity data in humans. Comparative efficacy trials in humans may not be required if there is strong evidence that pharmacokinetic or pharmacodynamic results well match the biosimilar and the originator drug.19,21,22 The final approval of biosimilars is then based on shortened licensing pathways in which data “extrapolation” across all indications of the reference product is accomplished without any need for clinical studies and even though the biosimilar has not been formally analyzed in all indications or populations of the originator.23–25 Extrapolation of molecules in the same class with the same mechanism of action from adults to children or across indications is prevalent in clinical practice when there is insufficient supporting evidence or when clinical studies are underway.23–25 Nonetheless, known mechanisms of action (for example, TNF-α inhibition) in different diseases may not result in the same clinical efficacy.26 As previously mentioned, the anti-TNF-α reference drugs currently available to treat pediatric IBD patients are represented by IFX and ADA. The expiry of the patent on Remicade in 2013 allowed its biosimilars to be marketed. The first biosimilar of IFX to be approved by the regulatory agencies was CT-P13, in 2013 by the European Medicine Agency (EMA) and in 2016 by the FDA.27,28 The approval of CT-P13 in both adult and pediatric IBD patients was based on extrapolation. The clinical testing of biosimilar IFX in rheumatologic diseases revealed evidence of comparability in terms of pharmacokinetics, safety, and efficacy between the reference and biosimilar IFX.29,30 CT-P13 biosimilars are marketed under a variety of brand names, including Remsima (Celltrion, Incheon, South Korea) and Inflectra (Hospira, Lake Forest, IL, USA). Other biosimilars of IFX were marketed, such as SB2, also known as Flixabi (Samsung Bioepis, Incheon, Republic of Korea) and Renflexis (Merck, Kenilworth, NJ), and PF-06438179, also known as Zessly (Sandoz GmbH). There are currently seven authorized IFX biosimilars and ten approved ADA biosimilars (Table 3). To date, no biosimilars exist for the anti-integrins vedolizumab and natalizumab or the anti-interleukin 12/23 ustekinumab, while clinical trials for new biologics in the class and biosimilars to these reference drugs are ongoing.31,32
 |
Table 3 Currently Approved Biosimilars for IBD in Europe and US |
Which Evidence Exists for Biosimilars in the Pediatric Setting?
Studies evaluating the efficacy and safety of biosimilars in IBD have primarily been conducted among adult patients.33–37 The European Crohn’s and Colitis Organization (ECCO) guidelines stated that the efficacy and safety of CT-P13 are comparable with its reference product, both in patients who are naïve to IFX or have been switched to CT-P13.17 A recent randomized, multicenter, double-blind trial showed non-inferiority of CT-P13 to IFX in 220 adult patients with active CD.33 Data on the effectiveness and safety of biosimilars in pediatric IBD is steadily increasing.38 The European Society of Pediatric Gastroenterology, Hepatology and Nutrition (ESPGHAN) Pediatric IBD Porto Group stated that CT-P13 can be considered as a reliable alternative to the reference drug for remission induction and maintenance in children with IBD who are candidates for IFX treatment.26 Available pediatric studies have suggested that biosimilar IFX and the reference drug have comparable efficacy, safety, and immunogenicity, even after switching (Table 4).39–47 However, these studies are observational and limited by their small sample size and the varying lengths of follow-up in individual patients.
 |
Table 4 Studies Investigating the Use of CT-P13 in Pediatric IBD |
To date, no study has been done to evaluate the efficacy and safety of an ADA biosimilar in pediatric IBD. There is also no pediatric data on the use of biosimilars in children who have had a secondary loss of response or adverse event to the originator. A secondary loss of response to a biologic is a common situation in which a patient has a sufficient response when the medication is commenced but then has either a subsequent declining response (symptoms reappear before the next dose) or a full flare at any moment before the next dose.48 An adult study investigated the cross-reactivity of antibodies to IFX (ATI) to IFX biosimilar (infliximab-dyyb) in 125 IBD patients and found that serum samples from all the patients with positive ATI to the originator cross-reacted to the biosimilar, whereas none of the patients with negative ATI showed cross-reactivity.49 The ATI titers for the reference drug and infliximab-dyyb were thoroughly correlated and demonstrated similar functional competition for and suppression of drug binding to TNF-α.49 It does not appear to be advisable to use a biosimilar to a reference drug in patients who have experienced a secondary loss of response or adverse reaction to the originator, as it appears unlikely that patients with non-response to the originator drug benefit from a biosimilar trial, and an increased risk of complications mediated by ATI may occur. On the other hand, biosimilars can be subjected to the same established tests for therapeutic drug monitoring and ATI as the reference drug.
Which are the Main Concerns Regarding the Use of Biosimilars for Pediatric IBD?
The major concern in the pediatric population is the issue of interchangeability and automatic or non-medical switching. “Automatic therapeutic substitution” refers to the automatic substitution of a prescribed medicine for an equivalent one, usually without prior communication with the prescriber.50 “Non-medical switching” refers to the practice of switching a prescribed drug to a comparable drug, which is typically done by insurance companies and is often motivated by financial benefit.51 A recent systematic review looked at the non-medical switching of originator IFX to an IFX biosimilar in adult IBD patients. They were included 44 different studies in total, including three randomized controlled trials, 40 observational trials, and one case series.52 The authors concluded that non-medical switching from originator to biosimilar was safe and had no negative impact on efficacy, safety, or immunogenicity. However, only three small randomized controlled trials were included in this analysis, with observational cohort studies predominating. The American College of Rheumatology’s position statement on biosimilars stated that safety in adults does not guarantee safety in children.53 A recent research study expressed worry about the absence of long-term data on the immunogenicity of biosimilars in pediatric IBD.54 The authors urge that the FDA not presume interchangeability is achievable in this cohort until long-term trial evidence is available. The ESPGHAN Pediatric IBD Porto Group issued its first position statement on the use of biosimilars in pediatric IBD in 2015.55 The authors cautioned against extrapolating clinical results from adult studies to children with IBD.56 The following were the key points from this statement: (i) physicians’ willingness to accept FDA approval of biosimilars based on extrapolation; (ii) physicians’ concerns about immunogenicity and loss of response when switching from a reference biologic to a biosimilar and inversely; (iii) the need for the FDA to collaborate with interested parties (insurance and patients) to try to educate physicians and patients about biosimilars; and (iv) shared decision-making and transparency between the FDA and interested parties (insurance and patients). Following the release of new safety data, an updated ESPGHAN position statement in 2019 claimed that switching from the originator IFX to CT-P13 was safe and well-tolerated in children, better if in clinical remission and after at least three induction infusions.26 Importantly, multiple switches between the originator and biosimilars or between different biosimilars are not yet recommended in pediatric patients with IBD due to a lack of sufficient interchangeability data.26 IBD experts also recommended additional studies in this population of patients, including long-term follow-up and post-marketing surveillance of the efficacy, safety, and immunogenicity of biosimilars if delivered to young patients.26
Knowledge on Biosimilar Use
The state of knowledge on biosimilar experiences in IBD is limited. In 2013, a survey by ECCO showed that a minority of IBD experts were aware and confident about the benefits and issues of biosimilars. In a later survey promoted by ECCO, they were reported fewer concerns and more confidence about biosimilar use in clinical practice.57,58 A more recent web survey revealed that pediatric IBD experts in Italy have a good level of knowledge on biosimilar use advantages, disadvantages, costs, and traceability.59 The increasing confidence in biosimilar use may be linked to the growing post-marketing studies and the dissemination of real-world data. Patient education is also an important aspect of the acceptance of biosimilar treatment. Morris et al60 have recently demonstrated the successful application of a quality improvement approach to boost biosimilar use from 1% to 96% in intravenous anti-TNF-α naïve pediatric patients. This was achieved through substantial provider and patient education and expediting the prior authorization process for all inpatient and outpatient biosimilar starters.60 Patient and provider education is even more essential when considering a switch from the originator to its biosimilar because of the existence of the so-called “nocebo effect”.61 The “nocebo effect” arises when the expectation of side effects leads to the occurrence of those symptoms, which can occur when patients move from brand-name to generic medications.61 As a result, generic drugs are frequently associated with significantly higher patient reporting of side effects and treatment non-adherence. This “nocebo effect” may also occur in patients who switch from biologic drugs to biosimilars.62 Physicians can help to reduce the “nocebo effect” with biosimilars through (i) clear communication and positive framing (for instance, “the great majority of patients have a good tolerance to this treatment”), (ii) an authorized concealment approach (for instance, for milder side effects, or asking whether they would prefer to be informed about these side effects or not), and (iii) involvement of (older) patients in the decision-making process.61 The effects of positive framing have been seen in a study enrolling patients receiving the opioid painkiller remifentanil, where positive treatment expectations significantly boosted remifentanil’s analgesic effectiveness.63 However, the insurance demand to switch a patient from the originator to its biosimilar often comes with insufficient notification to allow for information and reassurance.61
Impact of Biosimilars on Costs
The basic principle underlying the development of biosimilars is healthcare systems’ expectation that these molecules will reduce the financial burden of biologic therapy, hence boosting access to these treatments and allowing for more intensive treatment regimens when clinically indicated.64 Although biosimilar prices vary across Europe,65 they are at least 15–45% less expensive than the originator biologics.66 The potential for cost reductions varies between biologic classes depending on sales, competition, and the timing of biosimilar launches. Together with monoclonal antibody antineoplastics and insulin, they account for more than 60% of the expected savings (Figure 2).67 The price evolution of off-patent biologics and biosimilars is rapid across Europe, with reductions on certain biosimilars reaching up to 80%.65 In Europe, most biologics are off-patent and biosimilars are available for clinical use. The extrapolation process, which minimizes the number of clinical studies required for biosimilar approval and hence lowers costs, is primarily responsible for the cost savings associated with the usage of biosimilars. A study by Jha et al68 estimated a 1-year cumulative cost savings for the usage of Remsima in six autoimmune indications (including CD and UC) for five countries (Belgium, Germany, Italy, Netherlands, UK), projecting an annual cost saving of €2.89 million in Belgium (10% discount scenario) to €33.80 million in Germany (30% discount scenario). Some pediatric studies reported a comparison of costs between reference IFX and CT-P13.41,42,44 Overall, considerable cost reductions from using biosimilar IFX based on estimated and averaged local procurement rates were reported. Richmond et al41 reported an average 38% cost reduction per vial from the originator to the biosimilar Remsima over 12 weeks and around £47,800 (€57,000) of savings for the total number of infusions. In another study, the cost-saving for the total number of infusions was around £875 000 (€998 526) over a year.42 Cost savings from biosimilars can be used to increase patient access to biologic therapy. The hypothetical budget impact study by Jha et al68 has computed that 250 to 2602 additional patients can be treated with the money saved from biosimilars.
 |
Figure 2 Potential cost reductions across biologic classes. |
Conclusion
Available pediatric studies confirm that the IFX biosimilar is as effective and safe as the reference drug, whilst simultaneously reducing the cost of treating IBD versus the originator. Cost reduction is considered the most important advantage of biosimilars. By lowering overall treatment costs while maintaining a high level of patient care, the use of biosimilars represents a chance to drastically cut healthcare costs and enhance patient access to biologic therapies. In recent years, biosimilars of anti-TNF-α have been increasingly used, even in pediatrics. Most IBD experts have reported increasing awareness of the advantages, efficacy, and safety of biosimilars in pediatric IBD. Clear communication, proper education, and patient reassurance appear to be associated with a reduced “nocebo effect” and are therefore needed to overcome the remaining barriers to effective switching in both pediatric and adult IBD patients. Additionally, currently available studies do not report any major issues with the immunogenicity of biosimilars. Further prospective, randomized-controlled trials are needed to support the validity of these studies, including the biosimilars of ADA for which data are currently lacking.
Abbreviations
ADA, adalimumab; ATI, antibodies to infliximab; CD, Crohn’s disease; ECCO, European Crohn’s and Colitis Organization; EMA, European Medicine Agency; FDA, Food and Drug Administration; IBD-U, inflammatory bowel disease unclassified; IBD, inflammatory bowel disease; IFX, infliximab; SIGENP, Italian Society of Pediatric Gastroenterology, Hepatology and Nutrition; TNF-α, tumor necrosis factor-α; UC, ulcerative colitis; WHO, World Health Organization.
Disclosure
The authors report no conflicts of interest in this work.
References
1. Ungaro R, Mehandru S, Allen PB, Peyrin-Biroulet L, Colombel JF. Ulcerative colitis. Lancet. 2017;2017(389):1756–1770.
2. Torres J, Mehandru S, Colombel JF, Peyrin-Biroulet L. Crohn’s disease. Lancet. 2017;389(389):1741–1755.
3. Van Rheenen PF, Aloi M, Assa A, et al. The medical management of paediatric Crohn’s disease: an ECCO-ESPGHAN guideline update. J Crohns Colitis. 2020. doi:10.1093/ecco-jcc/jjaa161
4. Turner D, Ruemmele FM, Orlanski-Meyer E, et al. Management of paediatric ulcerative colitis, part 1: ambulatory care—an evidence-based guideline from European Crohn’s and Colitis Organization and European Society of paediatric gastroenterology, hepatology and nutrition. J Pediatr Gastroenterol Nutr. 2018;67:257–291. doi:10.1097/MPG.0000000000002035
5. Burisch J, Jess T, Martinato M, Lakatos PL; ECCO -EpiCom. The burden of inflammatory bowel disease in Europe. J Crohns Colitis. 2013;7:322–337. doi:10.1016/j.crohns.2013.01.010
6. Alatab S, Sepanlou SG, Ikuta K; GBD 2017 Inflammatory Bowel Disease Collaborators. The global, regional, and national burden of inflammatory bowel disease in 195 countries and territories, 1990–2017: a systematic analysis for the Global Burden of Disease Study 2017. Lancet Gastroenterol Hepatol. 2020;5:17–30. doi:10.1016/S2468-1253(19)30333-4
7. Click B, Lopez R, Arrigain S, Schold J, Regueiro M, Rizk M. Shifting cost-drivers of health care expenditures in inflammatory bowel disease. Inflamm Bowel Dis. 2020;26:1268–1275. doi:10.1093/ibd/izz256
8. Bhat S, Limdi JK, Cross RK, Farraye FA. Does similarity breed contempt? A review of the use of biosimilars in inflammatory bowel disease. Dig Dis Sci. 2021;66:2513–2532. doi:10.1007/s10620-021-07114-y
9. Laharie D, Salzmann M, Boubekeur H, et al. Predictors of response to infliximab in luminal Crohn’s disease. Gastroenterol. Clin Biol. 2005;29:145–149.
10. Ben-Horin S, Vande Casteele N, Schreiber S, Lakatos PL. Biosimilars in inflammatory bowel disease: facts and fears of extrapolation. Clin Gastroenterol Hepatol. 2016;14(12):1685–1696.
11. REACH Study Group; Hyams J, Crandall W, Kugathasan S, et al. Induction and maintenance infliximab therapy for the treatment of moderate-to-severe Crohn’s disease in children. Gastroenterology. 2007;132:863–873. doi:10.1053/j.gastro.2006.12.003
12. T72 Study Group; Hyams J, Damaraju L, Blank M, et al. Induction and maintenance therapy with infliximab for children with moderate to severe ulcerative colitis. Clin Gastroenterol Hepatol. 2012;10:391–399. doi:10.1016/j.cgh.2011.11.026
13. Faubion WA, Dubinsky M, Ruemmele FM, et al. Long-term efficacy and safety of Adalimumab in pediatric patients with Crohn’s disease. Inflamm Bowel Dis. 2017;23:453–460. doi:10.1097/MIB.0000000000001021
14. Croft NM, Faubion WA Jr, Kugathasan S, et al. Efficacy and safety of Adalimumab in paediatric patients with moderate-to-severe ulcerative colitis (ENVISION I): a randomised, controlled, Phase 3 study. Lancet Gastroenterol Hepatol. 2021;6:616–627. doi:10.1016/S2468-1253(21)00142-4
15. Harbord M, Annese V, Vavricka SR, et al. The first European evidence-based consensus on extra-intestinal manifestations in inflammatory bowel disease. J Crohns Colitis. 2016;10:239–254. doi:10.1093/ecco-jcc/jjv213
16. van Rheenen H, van Rheenen PF. Long-term efficacy of anti-tumor necrosis factor agents in pediatric luminal Crohn’s disease: a systematic review of real-world evidence studies. Pediatr Gastroenterol Hepatol Nutr. 2020;23:121–131. doi:10.5223/pghn.2020.23.2.121
17. Danese S, Gomollon F; Governing Board and Operational Board of ECCO. ECCO position statement: the use of biosimilar medicines in the treatment of inflammatory bowel disease (IBD). J Crohns Colitis. 2013;7:586–589. doi:10.1016/j.crohns.2013.03.011
18. Gherghescu I, Delgado-Charro MB. The biosimilar landscape: an overview of regulatory approvals by the EMA and FDA. Pharmaceutics. 2020;13:48. doi:10.3390/pharmaceutics13010048
19. FDA. Biosimilar development, review, and approval. Available from: https://www.fda.gov/drugs/biosimilars/biosimilar-development-review-and-approval.
20. World Health Organization. Guidelines on Evaluation of Similar Biotherapeutic Products (Sbps), Expert Committee on Biological Standardization, Geneva, 19 to 23 October 2009. Geneva: World Health Organization; 2009.
21. FDA. Guidance on Scientific Considerations in Demonstrating Biosimilarity to a Reference Product. Silver Spring: The United States Food and Drug Administration; 2015.
22. Chow SC, Song F, Bai H. Analytical similarity assessment in biosimilar studies. AAPS J. 2016;18:670–677. doi:10.1208/s12248-016-9882-5
23. Alten R, Cronstein BN. Clinical trial development for biosimilars. Semin Arthritis Rheum. 2015;44:S2–S8. doi:10.1016/j.semarthrit.2015.04.002
24. Vande Casteele N, Sandborn WJ. IBD: indication extrapolation for anti-TNF biosimilars. Nat Rev Gastroenterol Hepatol. 2015;12:373–374. doi:10.1038/nrgastro.2015.104
25. Weise M, Kurki P, Wolff-Holz E, Bielsky MC, Schneider CK. Biosimilars: the science of extrapolation. Blood. 2014;124:3191–3196. doi:10.1182/blood-2014-06-583617
26. de Ridder L, Assa A, Bronsky J, et al. Use of biosimilars in pediatric inflammatory bowel disease: an updated position statement of the pediatric IBD Porto Group of ESPGHAN. J Pediatr Gastroenterol Nutr. 2019;68:144–153. doi:10.1097/MPG.0000000000002141
27. Organization site European Medicines Agency. Committee for medicinal products for human use (CHMP). Assessment report: inflectra (infliximab); 2013. Available from: http://www.ema.europa.eu/docs/en_GB/document_library/EPAR_-_Public_assessment_report/human/002778/WC500151490.pdf.
28. Organization site World Health Organization. Expert committee on biological standardization Geneva, 17 to 20 October 2017. Report on a Collaborative Study for Proposed 1st International Standard for Infliximab. 2017. Available from: http://www.who.int/biologicals/expert_committee/BS2323_Infliximab_ECBS_2017_V.6.1.pdf.
29. Park W, Hrycaj P, Jeka S, et al. A randomised, double-blind, multicentre, parallel-group, prospective study comparing the pharmacokinetics, safety, and efficacy of CT-P13 and innovator infliximab in patients with ankylosing spondylitis: the PLANETAS study. Ann Rheum Dis. 2013;72:1605–1612.
30. Yoo DH, Hrycaj P, Miranda P, et al. A randomised, double-blind, parallel-group study to demonstrate equivalence in efficacy and safety of CT-P13 compared with innovator infliximab when coadministered with methotrexate in patients with active rheumatoid arthritis: the PLANETRA study. Ann Rheum Dis. 2013;72:1613–1620.
31. Vedolizumab Biosimilar-Research Grade [ICH4035]-ichorbio. Available from: https://ichor.bio/product/vedolizumabbiosimilar-research-grade-ich4035/.
32. SAMSUNG BIOEPIS. Initiates phase 1 clinical trial for SB17, proposed biosimilar to stelara (ustekinumab). Available from: https://www.samsungbioepis.com/en/newsroom/newsroomView.do?idx=221¤tPage=1.
33. Ye BD, Pesegova M, Alexeeva O, et al. Efficacy and safety of biosimilar CT-P13 compared with originator infliximab in patients with active Crohn’s disease: an international, randomised, double-blind, phase 3 non-inferiority study. Lancet. 2019;393:1699–1707. doi:10.1016/S0140-6736(18)32196-2
34. Komaki Y, Yamada A, Komaki F, Micic D, Ido A, Sakuraba A. Systematic review with meta-analysis: the efficacy and safety of CT-P13, a biosimilar of anti-tumour necrosis factor-α agent (infliximab), in inflammatory bowel diseases. Aliment Pharmacol Ther. 2017;45:1043–1057. doi:10.1111/apt.13990
35. Farkas K, Rutka M, Bálint A, et al. Efficacy of the new infliximab biosimilar CT-P13 induction therapy in Crohn’s disease and ulcerative colitis - experiences from a single center. Expert Opin Biol Ther. 2015;15:1257–1262. doi:10.1517/14712598.2015.1064893
36. Gecse KB, Lovász BD, Farkas K, et al. Efficacy and safety of the biosimilar infliximab CT-P13 treatment in inflammatory bowel diseases: a prospective, multicentre, nationwide cohort. J Crohns Colitis. 2016;10:133–140. doi:10.1093/ecco-jcc/jjv220
37. Jahnsen J, Detlie T, Vatn S, Ricanek P. Biosimilar infliximab (CT-P13) in the treatment of inflammatory bowel disease: a Norwegian observational study. Expert Rev Gastroenterol Hepatol. 2015;9:45–52. doi:10.1586/17474124.2015.1091308
38. Dipasquale V, Romano C. Biosimilar infliximab in paediatric inflammatory bowel disease: efficacy, immunogenicity and safety. J Clin Pharm Ther. 2020;45:1228–1234. doi:10.1111/jcpt.13239
39. Sieczkowska-Golub J, Meglicka M, Plocek A, et al. Induction therapy with biosimilar infliximab in children with Crohn disease. J Pediatr Gastroenterol Nutr. 2017;65:285–288. doi:10.1097/MPG.0000000000001643
40. Richmond L, Curtis L, Garrick V, et al. Biosimilar infliximab use in paediatric IBD. Arch Dis Child. 2018;103:89–91. doi:10.1136/archdischild-2017-313404
41. Chanchlani N, Mortier K, Williams LJ, et al. Use of infliximab biosimilar versus originator in a pediatric United Kingdom inflammatory bowel disease induction cohort. J Pediatr Gastroenterol Nutr. 2018;67:513–519. doi:10.1097/MPG.0000000000002011
42. Nikkonen A, Kolho K. Infliximab and its biosimilar produced similar first-year therapy outcomes in patients with inflammatory bowel disease. Acta Paediatr. 2020;109:836–841. doi:10.1111/apa.15026
43. Sieczkowska J, Jarzębicka D, Banaszkiewicz A, et al. Switching between infliximab originator and biosimilar in paediatric patients with inflammatory bowel disease. Preliminary observations. J Crohns Colitis. 2016;10:127–132. doi:10.1093/ecco-jcc/jjv233
44. Kang B, Lee Y, Lee K, Choi YO, Choe YH. Long-term outcomes after switching to CT-P13 in pediatric-onset inflammatory bowel disease: a single-center prospective observational study. Inflamm Bowel Dis. 2018;24:607–616. doi:10.1093/ibd/izx047
45. Gervais L, McLean LL, Wilson ML, et al. Switching from originator to biosimilar infliximab in paediatric inflammatory bowel disease is feasible and uneventful. J Pediatr Gastroenterol Nutr. 2018;67:745–748. doi:10.1097/MPG.0000000000002091
46. van Hoeve K, Dreesen E, Hoffman I, et al. Efficacy, pharmacokinetics, and immunogenicity is not affected by switching from infliximab originator to a biosimilar in pediatric patients with inflammatory bowel disease. Ther Drug Monit. 2019;41:317–324. doi:10.1097/FTD.0000000000000601
47. Cheon JH, Nah S, Kang HW, et al. Infliximab biosimilar CT-P13 observational studies for rheumatoid arthritis, inflammatory bowel diseases, and ankylosing spondylitis: pooled analysis of long-term safety and effectiveness. Adv Ther. 2021;38:4366–4387. doi:10.1007/s12325-021-01834-3
48. Roda G, Jharap B, Neeraj N, Colombel JF. Loss of response to anti-tnfs: definition, epidemiology, and management. Clin Transl Gastroenterol. 2016;7:e135. doi:10.1038/ctg.2015.63
49. Ben-Horin S, Yavzori M, Benhar I, et al. Cross-immunogenicity: antibodies to infliximab in Remicade-treated patients with IBD similarly recognise the biosimilar Remsima. Gut. 2016;65:1132–1138. doi:10.1136/gutjnl-2015-309290
50. Glaholt S, Hayes GL, Wisniewski CS. Evaluation of discharge medication orders following automatic therapeutic substitution of commonly exchanged drug classes. P&t. 2014;39:267–277.
51. Nguyen E, Weeda ER, Sobieraj DM, Bookhart BK, Piech CT, Coleman CI. Impact of non-medical switching on clinical and economic outcomes, resource utilization and medication-taking behavior: a systematic literature review. Curr Med Res Opin. 2016;32:1281–1290. doi:10.1185/03007995.2016.1170673
52. Bernard EJ, Fedorak RN, Jairath V. Systematic review: non-medical switching of infliximab to CT-P13 in inflammatory bowel disease. Dig Dis Sci. 2020;65:2354–2372. doi:10.1007/s10620-019-06036-0
53. ACR releases new position statement on biosimilars: encourages strict oversight, scientific study & physician involvement; 2015. https://www.rheumatology.org/About-Us/Newsroom/PressReleases/ID/33#::text=ATLANTA%20%E2%80%94%20The%20American%20College%20of,in%20patients%20with%20rheumatic%20disease.&text=The%20need%20for%20rigorous%20clinical,with%20or%20iginal%20biologic%20drugs.
54. Patel D, Park KT. The path of interchangeability of biosimilars in pediatric inflammatory bowel disease: quality before cost-savings. J Pediatr Gastroenterol Nutr. 2017;65:134–136. doi:10.1097/MPG.0000000000001572
55. de Ridder L, Waterman M, Turner D, et al. Use of biosimilars in paediatric inflammatory bowel disease: a position statement of the ESPGHAN paediatric IBD Porto Group. J Pediatr Gastroenterol Nutr. 2015;61:503–508. doi:10.1097/MPG.0000000000000903
56. Crohn’s and colitis foundation of America position statement: biosimilars. Available from: https://www.naspghan.org/files/documents/pdfs/advocacy/2016/Biosimilar%20Position%20Statement%20-%20NASPGHAN%20endorsed%20.pdf.
57. Danese S, Fiorino G, Michetti P. Viewpoint: knowledge and viewpoints on biosimilar monoclonal antibodies among members of the European Crohn’s and Colitis Organization. J Crohns Colitis. 2014;8:1548–1550. doi:10.1016/j.crohns.2014.06.007
58. Danese S, Fiorino G, Michetti P. Changes in biosimilar knowledge among European Crohn’s Colitis Organization [ECCO] members: an updated survey. J Crohns Colitis. 2016;10:1362–1365. doi:10.1093/ecco-jcc/jjw090
59. Dipasquale V, Martinelli M, Aloi M, et al. Real-life use of biosimilars in pediatric inflammatory bowel disease: a nation-wide web survey on behalf of the SIGENP IBD Working Group. Paediatr Drugs. 2022;24:57–62. doi:10.1007/s40272-021-00486-8
60. Morris GA, McNicol M, Boyle B, et al. Increasing biosimilar utilization at a pediatric inflammatory bowel disease center and associated cost savings: show me the money. Inflamm Bowel Dis. 2021;28:531–538.
61. Gecse KB, Cumming F, D’Haens G. Biosimilars for inflammatory bowel disease: how can healthcare professionals help address patients’ concerns? Expert Rev Gastroenterol Hepatol. 2019;13:143–155. doi:10.1080/17474124.2019.1553617
62. Rezk MF, Pieper B. Treatment outcomes with biosimilars: be aware of the nocebo effect. Rheumatol Ther. 2017;4:209–218. doi:10.1007/s40744-017-0085-z
63. Bingel U, Wanigasekera V, Wiech K, et al. The effect of treatment expectation on drug efficacy: imaging the analgesic benefit of the opioid remifentanil. Sci Transl Med. 2011;3:70ra14. doi:10.1126/scitranslmed.3001244
64. Dutta B, Huys I, Vulto AG, Simoens S. Identifying key benefits in European off-patent biologics and biosimilar markets: it is not only about price! BioDrugs. 2020;34:159–170. doi:10.1007/s40259-019-00395-w
65. Heredia E, Ribeiro A. Discount offered by first and subsequent biosimilars in the US, EU and LATAM: impact trends of originator starting price, market dynamics and regulations. Value Health. 2018;21(Suppl.1):S103–4. doi:10.1016/j.jval.2018.04.700
66. Moorkens E, Vulto AG, Huys I, et al. Policies for biosimilar uptake in Europe: an overview. PLoS One. 2017;12:e0190147. doi:10.1371/journal.pone.0190147
67. Mulcahy AW, Predmore Z, Mattke S; RAND Corporation. The cost savings potential of biosimilar drugs in the United States. Available from: https://www.rand.org/content/dam/rand/pubs/perspectives/PE100/PE127/RAND_PE127.pdf.
68. Jha A, Upton A, Dunlop WC, Akehurst R. The budget impact of biosimilar infliximab (Remsima®) for the treatment of autoimmune diseases in five European countries. Adv Ther. 2015;32:742–756. doi:10.1007/s12325-015-0233-1
 © 2022 The Author(s). This work is published and licensed by Dove Medical Press Limited. The
full terms of this license are available at https://www.dovepress.com/terms.php
and incorporate the Creative Commons Attribution
- Non Commercial (unported, v3.0) License.
By accessing the work you hereby accept the Terms. Non-commercial uses of the work are permitted
without any further permission from Dove Medical Press Limited, provided the work is properly
attributed. For permission for commercial use of this work, please see paragraphs 4.2 and 5 of our Terms.
© 2022 The Author(s). This work is published and licensed by Dove Medical Press Limited. The
full terms of this license are available at https://www.dovepress.com/terms.php
and incorporate the Creative Commons Attribution
- Non Commercial (unported, v3.0) License.
By accessing the work you hereby accept the Terms. Non-commercial uses of the work are permitted
without any further permission from Dove Medical Press Limited, provided the work is properly
attributed. For permission for commercial use of this work, please see paragraphs 4.2 and 5 of our Terms.
Recommended articles
Atypical Forms of Pyoderma Gangrenosum in Inflammatory Bowel Disease: Report of Four Cases and Literature Review
Martinelli VF, Martinelli Barbosa P, Dantas de Oliveira LS, Melo LALV, Casa Nova JM, Brito CAA
International Medical Case Reports Journal 2022, 15:449-456
Published Date: 26 August 2022
A Literature Review of Ozanimod Therapy in Inflammatory Bowel Disease: From Concept to Practical Application
Becher N, Swaminath A, Sultan K
Therapeutics and Clinical Risk Management 2022, 18:913-927
Published Date: 8 September 2022
A Review on Inflammatory Bowel Diseases: Recent Molecular Pathophysiology Advances
Abdulla M, Mohammed N
Biologics: Targets and Therapy 2022, 16:129-140
Published Date: 12 September 2022
The Association Between Inflammatory Bowel Disease and Exposure to Tobacco Smoking: A Case-Control Study in Qatar
Abdallah B, Arif M, Al-Malki M, Hourani R, Al-Maadeed T, Khodr N, Al-Kuwari G, Al-Siddiqi M, Kane T, Chivese T
International Journal of General Medicine 2023, 16:233-242
Published Date: 21 January 2023
Stem Cell Therapy in Inflammatory Bowel Disease: A Review of Achievements and Challenges
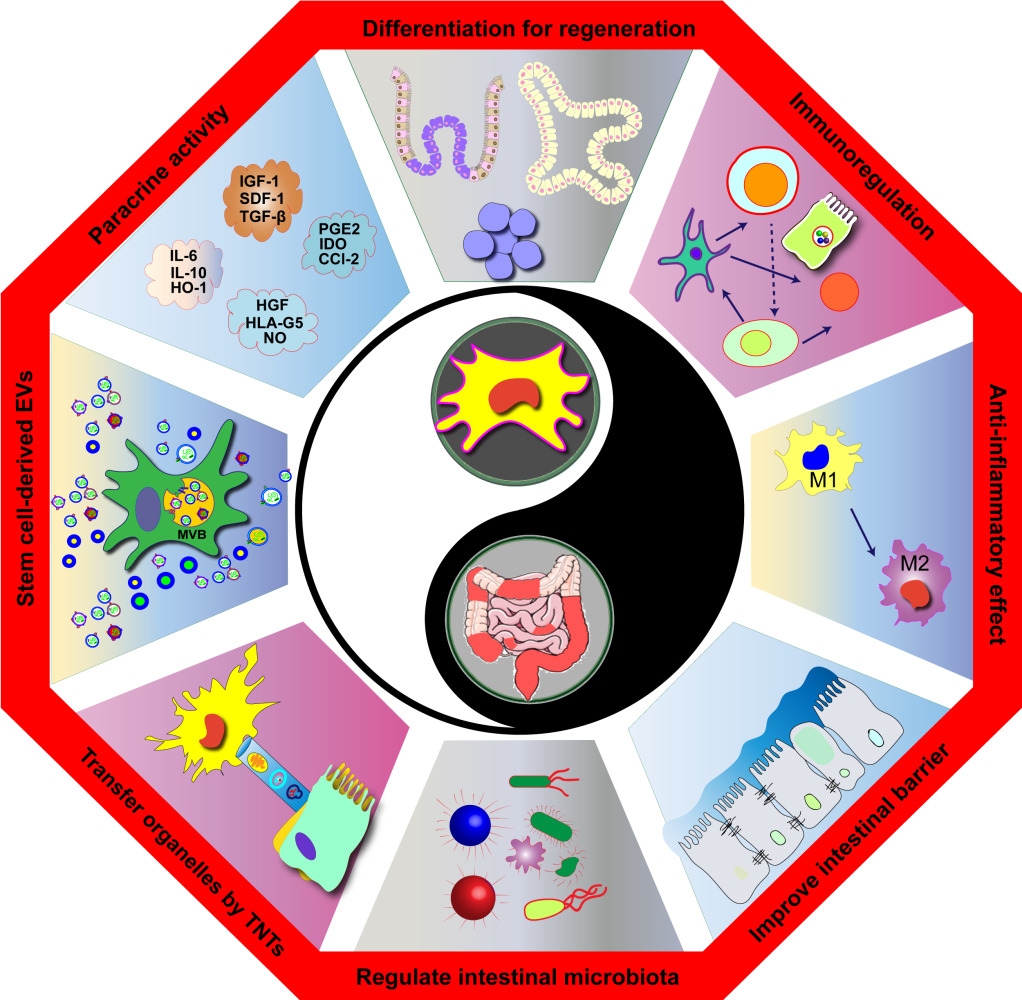
Tian CM, Zhang Y, Yang MF, Xu HM, Zhu MZ, Yao J, Wang LS, Liang YJ, Li DF
Journal of Inflammation Research 2023, 16:2089-2119
Published Date: 16 May 2023
