Back to Journals » Journal of Inflammation Research » Volume 14
The Pulsatile Modification Improves Hemodynamics and Attenuates Inflammatory Responses in Extracorporeal Membrane Oxygenation
Authors Li G , Zeng J, Liu Z, Zhang Y, Fan X
Received 20 November 2020
Accepted for publication 25 February 2021
Published 12 April 2021 Volume 2021:14 Pages 1357—1364
DOI https://doi.org/10.2147/JIR.S292543
Checked for plagiarism Yes
Review by Single anonymous peer review
Peer reviewer comments 3
Editor who approved publication: Professor Ning Quan
Guanhua Li,1,2 Jianfeng Zeng,3 Zhaoyuan Liu,4 Yu Zhang,5,* Xiaoping Fan6,*
1Department of Cardiovascular Surgery, Sun Yat-sen Memorial Hospital, Sun Yat-sen University, Guangzhou, 510120, People’s Republic of China; 2Department of Cardiovascular Surgery, Guangdong Cardiovascular Institute, Guangdong Provincial Key Laboratory of South China Structural Heart Disease, Guangdong General Hospital, Guangdong Academy of Medical Sciences, Guangzhou, 510080, People’s Republic of China; 3Department of Anesthesiology, Sun Yat-sen Memorial Hospital, Sun Yat-sen University, Guangzhou, 510120, People’s Republic of China; 4Department of Hepatobiliary Surgery, Second Affiliated Hospital of Guangzhou Medical University, Guangzhou, 510260, People’s Republic of China; 5Department of Pathology, Guangdong Provincial Hospital of Chinese Medicine, The Second Affiliated Hospital of Guangzhou University of Chinese Medicine, Guangzhou, 510120, People’s Republic of China; 6Department of Cardiovascular Surgery, Guangdong Provincial Hospital of Chinese Medicine, The Second Affiliated Hospital of Guangzhou University of Chinese Medicine, Guangzhou, 510006, People’s Republic of China
*These authors contributed equally to this work
Correspondence: Xiaoping Fan
Department of Cardiovascular Surgery, Guangdong Provincial Hospital of Chinese Medicine, The Second Affiliated Hospital of Guangzhou University of Chinese Medicine, No. 55, Neihuan Xi Road, Panyu District, Guangzhou, 510006, People’s Republic of China
Tel/Fax +86 20-81887233
Email [email protected]
Yu Zhang
Department of Pathology, Guangdong Provincial Hospital of Chinese Medicine, The Second Affiliated Hospital of Guangzhou University of Chinese Medicine, No. 111, Dade Road, Guangzhou, 510120, People’s Republic of China
Tel/Fax +86 20-81887233
Email [email protected]
Background: COVID-19 is still a worldwide pandemic and extracorporeal membrane oxygenation (ECMO) is vital for extremely critical COVID-19 patients. Pulsatile flow impacts greatly on organ function and microcirculation, however, the effects of pulsatile flow on hemodynamics and inflammatory responses during ECMO are unknown. An in vivo study was launched aiming at comparing the two perfusion modes in ECMO.
Methods: Fourteen beagles were randomly allocated into two groups: the pulsatile group (n=7) and the non-pulsatile group (n=7). ECMO was conducted using the i-Cor system for 24 hours. Hemodynamic parameters including surplus hemodynamic energy (SHE), energy equivalent pressure (EEP), oxygenator pressure drop (OPD), and circuit pressure drop (CPD) were monitored. To assess inflammatory responses during ECMO, levels of tumor necrosis factor-α (TNF-α), interleukin-1β (IL-1β), IL-6, IL-8, and transforming growth factor-β 1 (TGF-β 1) were measured.
Results: EEP and SHE were markedly higher in pulsatile circuits when compared with the conventional circuits. Between-group differences in both OPD and CPD reached statistical significance. Significant decreases in TNF-α were seen in animals treated with pulsatile flows at 2 hours, 12 hours, and 24 hours as well as a decrease in IL-1β at 24 hours during ECMO. The TGF-β 1 levels were significantly higher in pulsatile circuits from 2 hours to 24 hours. The changes in IL-6 and IL-8 levels were insignificant.
Conclusion: The modification of pulsatility in ECMO generates more hemodynamic energies and attenuates inflammatory responses as compared to the conventional non-pulsatile ECMO.
Keywords: pulsatile flow, extracorporeal membrane oxygenation, inflammatory response, COVID-19
Introduction
COVID-19, caused by the SARS-CoV-2 outbreak at the end of 2019, is still a worldwide pandemic and has infected more than 11 billion people. Most COVID-19 patients manifest moderate symptoms and recover rapidly, however, approximately 14% of COVID-19 patients develop severe respiratory failure,1 which requires mechanical ventilation or even extracorporeal membrane oxygenation (ECMO) support, with relatively high mortality.2 ECMO serves as a life-supporting method and is essentially important in managing those lethal COVID-19 cases,3 yet the overall survival rate for extracorporeal life support progresses slowly over the years.4 One important reason for this tardiness is the imperfection of ECMO components, for which technical optimization is imperative.
Flow pattern (pulsatile or non-pulsatile) may influence greatly on vital organ function during mechanical circulatory support.5,6 It has been reported that pulsatile perfusion during extracorporeal circulation lowers the rate of in-hospital mortality in patients undergoing open-heart surgeries as compared with non-pulsatile perfusion.7 It has been broadly acknowledged that pulsatile flow in mechanical circulatory support offers biomimetic hemodynamic energy to more effectively maintain microcirculation,8 like energy equivalent pressure (EEP) and surplus hemodynamic energy (SHE).9 Moreover, studies on tissue microcirculation have confirmed that pulsatile flow alleviates systemic inflammatory responses,5 and we had proved previously that pulsatile perfusion also improves vascular oxidative status as it upregulates the expression of nitric oxide.9 However, there is no pulsatile ECMO device feasible for patients and how pulsatile flow affects inflammatory responses during ECMO remains unknown.
Unlike the cardiopulmonary bypass, ECMO is a longer life-supporting system for which enhanced surplus energy to microcirculation may be more necessary. Therefore, translational studies are essential to determine the safety, efficacy, and potential benefits of pulsatile flow in ECMO. Ündar`s group constructed a pulsatile in-vitro ECMO, which enhances surplus hemodynamic energy to microcirculation.10 The i-Cor system, a product from the Xenios AG, was firstly applied in European countries, consisting of a diagonal blood pump that enables fast switching of both continuous non-pulsatile flow and pulsatile flow.11,12 We had recently established an investigated ECMO circuit comprised of the i-Cor diagonal pump, a membrane oxygenator, and the tubing sets in animal models. An in vivo study was launched to compare the effects on hemodynamics and inflammatory responses between non-pulsatile flow and pulsatile flow in ECMO.
Methods
Ethical approval (Reference number: SYSU-IACUC-2020-B0402) was obtained before the study was carried out. The Institutional Animal Care and Use Committee of Sun Yat-sen Memorial Hospital approved our experimental protocol, which was made according to the Guide for the Care and Use of Laboratory Animals, revised and established in 1985 by the National Institute of Health of the United States. This study was reported in compliance with the ARRIVE guidelines 2.0.13
ECMO Circuit Setup
As shown in Figure 1, the experimental ECMO circuit was composed of the i-Cor system (Xenious AG, Heilbronn, Germany), including a console and an i-Cor diagonal pump, the Medos Hilite 2400LT membrane oxygenator (Medos Medizintechnik AG, Stolberg, Germany), and the ECMO tubing sets. The oxygen (O2)/airflow was maintained in the ranges of arterial partial pressure of oxygen (PaO2) from 10.0 kilopascal (kPa) to 16.0 kPa, and arterial partial pressure of carbon dioxide (PaCO2) from 4.0 kPa to 6.0 kPa, respectively, as suggested elsewhere.12 The blood flow rate was initiated at 1 liter/minute (L/min) before ECMO commencement. Switching of pulsatile or non-pulsatile flow can be done by the i-Cor system with a fixed blood flow rate. Adjustment of the pump rotation speed can be triggered by the electrocardiogram (ECG), according to which pulsatile flows were running in a parallel manner (1:1) on condition that heart rates stayed below 100 beats/min. Intravenous verapamil (1.5 mg) was used if tachycardia (heart rate higher than 120 beats/min) occurred to maintain the parallel pulsatile flow.
 |
Figure 1 The investigated V-A ECMO circuits. Abbreviation: V-A ECMO, venous-arterial extracorporeal membrane oxygenation. |
Animal Models and Surgery
Fourteen beagles weighing 9.5 kg to 10.5 kg were prepared for experiments and were purchased from the Laboratory Animal Center of the South Medical University (Guangzhou, China). Propofol (2.0 mg/kg intravenous), pentobarbital (30.0 mg/kg intravenous), and morphine (0.1 mg/kg intravenous) were pre-medicated for inducing general anesthesia. Each animal was then orotracheally intubated in a supine position, with isoflurane (0.5% to 2.0%) inhaled and fentanyl (150 μg/kg, intravenous) administered to maintain anesthesia intra-operatively. A cervical incision was made, with the right internal jugular vein (RIJV) and right common carotid artery (RCCA) carefully dissected. An initial bolus (100 U/kg) of unfractionated heparin was used before cannulation. An activated clotting time (ACT) from 180 to 240 seconds was held and regularly supervised in each experimental circuit. The maintenance dose of heparin was 10 to 50 U/kg/hour. We smoothly cannulated the RCCA and RIJV with the 6-French (Fr) and 8-Fr cannulas (Medtronic Inc., Minneapolis, MN, USA), respectively. To achieve a cardiac output above 80 mL/kg/min, all venous-arterial (V-A) ECMO circuits were maintained with a pump flow rate ranging from 80 to 100 mL/kg/min and with a pump speed from 2500 to 3000 RPM during the experiment. After a-24-hour-observation, the circuit was weaned off and the cannulas were removed. The animals were then extubated with stable hemodynamics.
Hemodynamic Assessment
Flow rate and pressures were measured by flow sensors and pressure transducers. At each experiment, pressure drops were calculated by the following formulas as suggested by Ündar`s group:10
Oxygenator pressure drop (OPD)=pre-oxygenator pressure – post-oxygenator pressure;
Circuit pressure drop (CPD)=pre-oxygenator pressure – pre-clamp pressure.
Shepard`s principle was applied to quantitatively estimate the hemodynamic energies induced by pulsatile flow as we described previously,9 and these parameters were calculated:
EEP=ʃQpdt/ʃQdt, where Q represents the blood flow (mL/second), p stands for the instant arterial pressure (mmHg), and t is the time (second);
SHE=1332 (EEP − MAP) (ergs/cm3), where mean arterial pressure is abbreviated as MAP.
Blood Chemistry and Cytokine Measurements
Blood samples were drawn before surgery and at different time-points after ECMO. Blood cell count, lactic acid level, and ACT were detected routinely, while arterial blood gas was determined by the i-STAT analyzer. Blood samples were collected and injected into the Ethylene Diamine Tetraacetic Acid (EDTA) anticoagulant tube. These specimens were then centrifuged at 4000 revolutions per minute (RPM) at 4 degrees centigrade for 10 min and the plasma was accrued. We processed each sample within 4 hours after collection. Cytokines were measured at baseline, 2 hours, 6 hours, 12 hours, and 24 hours during ECMO, using the enzyme-linked immunosorbent assay (ELISA). ELISA kits for plasma free hemoglobin (PFH), tissue growth factor-β1 (TGF-β1), human tumor necrosis factor-alpha (TNF-α), interleukin-1β (IL-1β), IL-6, and IL-8 (BD Biosciences, San Jose, CA, USA) were used based on their instructions.
Statistics
We carried out statistical analyses with version 16.0 of the IBM SPSS Statistics software (SPSS Inc., Chicago, IL, USA). Each continuous variable in this study was expressed in terms of mean±standard deviation (SD). To estimate between-group differences, the Student`s t-test, as well as the Tukey-Kremer procedure was applied. The central comparison was the group (pulsatile versus non-pulsatile), based on the assumption that between-group alterations in hemodynamics and cytokines were similar. To compare between-group differences over time, the multiple linear regression model was used, with repeated measures analysis of variance (ANOVA) applied to manage these data, which were cytokine levels at different time-points in different groups. Each hypothesis in this study was two-sided and p-values below 0.05 were deemed as a level of statistical significance.
Results
Perioperative Data and Complications
Each animal was managed with a 10% Glucose solution of 200 mL and 200 mL normal saline during ECMO. No blood transfusion was received. No continuous vasopressors and inotropes were used during the experiment. The systolic pressure was maintained from 45 to 80 mmHg, with a heart rate ranging from 70 to 110 beats/min. The ventilation was supported with tidal volume at 8 mL/kg perioperatively, and a respiratory rate of 30 breaths/min was preserved under positive end-expiratory pressure of 4 cm H2O.
All circuits went smoothly within 24 hours. No premature termination of the ECMO circuit occurred in our study. No hemorrhagic complication was noted. In terms of hemodynamic complications, most circuits went smoothly, except for two cases of hypotension (systolic pressure below 20 mmHg) in the pulsatile group, and they were easily reversed by phenylephrine shots. One case in the non-pulsatile group had supraventricular tachycardia intermittently during ECMO, and it was properly managed by propranolol. Inadequate anticoagulation was observed in one animal in the pulsatile group, and the target ACT was obtained with additional heparin added. As no clots were identified in this circuit, this case was still included in data analyses.
Hematological Parameters
Baseline hematological parameters between groups were similar (Table 1). ACT levels and hematocrit were similar between the two groups during ECMO. Lactic acid values slightly increased in both groups, however, no significant between-group difference was observed. There were decreases over time regarding the level of hemoglobin and platelets, on the contrary, the white blood cell records raised during ECMO. Nonetheless, marked between-group differences were absent in terms of main blood components.
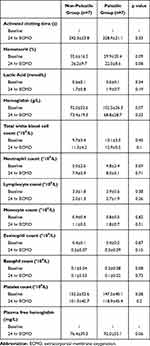 |
Table 1 Hematological Variables of the Experimental ECMO Circuits |
There were no statistically remarkable between-group alterations demonstrated concerning the white blood cell subpopulations, however, the neutrophil proportion was modestly higher in conventional circuits when compared with pulsatile circuits after 24 hours of observation (69.9% versus 62.0%). Plasma free hemoglobins presented a remarkable increase in pulsatile circuits after 24 hours comparing non-pulsatile circuits, however, statistical significance was not reached (92.0±55.1 mg/L versus 76.4±39.3, p=0.06).
Hemodynamic Variables
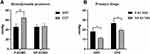
The alterations of MAPs were similar between the two groups, but higher levels of EEP were noted in animals under pulsatile circuits, where the EEPs were significantly higher than MAPs (Table 2, Figure 2A). The pulsatile circuits had significantly higher OPD and CPD than did the conventional circuits (Figure 2B). For the hemodynamic energy, more SHE was produced by the pulsatile flow than by the non-pulsatile flow according to Shepard`s model (Table 2).
 |
Table 2 Hemodynamic Data of the Experimental ECMO Circuits |
Cytokines
Blood concentrations of biomarkers associated with pro-inflammatory and anti-inflammatory responses were illustrated in Table 3. Significant decreases in TNF-α were seen in pulsatile flow at 2 hours, 12 hours, and 24 hours during ECMO. There was also a decrease in IL-1β in the pulsatility-treated circuits at 24 hours. TGF-β1, an anti-inflammatory factor, was significantly higher in animals exposed to pulsatile flow from 2 hours during ECMO than in animals exposed to non-pulsatile flow. No remarkable alterations were noted in other pro-inflammatory biomarkers, including IL-6 and IL-8.
 |
Table 3 Cytokines Changes in the ECMO Circuits |
Discussion
In the present work, the investigated ECMO circuits were categorized into the pulsatile or non-pulsatile mode. We have shown that pulsatility generates more hemodynamic energies and alleviates inflammatory responses during ECMO. The pulsatile ECMO has apparent benefits in hemodynamics in that pulsatility provides extra-energy effects and pulse stimulus.
The initiation of ECMO is relevant to prompt activation of inflammatory responses. Hence, the establishment of ECMO in critically ill COVID-19 patients may complicate the situation of septic shock and multiple organ failure, for which hyperinflammatory state and evident elevation of cytokines are common.14–16 The mechanisms for ECMO-induced inflammation involve the blood-device interaction, triggering the immune system. Cytokines and chemokines are all crucial to this pathophysiology and are associated with clinical outcomes during ECMO.17,18 On the other hand, microcirculatory malperfusion by the non-physiologic flow also results in the accumulation of inflammatory mediators. Our findings are consistent with other studies,19,20 and the pulsatile circuits had constantly higher EEPs and SHEs, which are vital to the microcirculatory perfusion. With the augmentation for microcirculation perfusion, the hyperinflammatory state is thus improved. Using an ex-vivo model, Wang et al21 found no alterations were presented regarding pro-inflammatory cytokines among the investigated group. An explanation for these conflicting results is the huge disparities between interactions on the “silent” blood components and impacts on the “active” immune system in different investigated models.
There are some other advantages which have been suggested by other researchers. Ostadal’s group12 compared the two modes of perfusion in porcine models of cardiogenic shock, and they found that the pulsatile flow preserved left ventricular function by elevating the coronary blood flow. Their system was electrocardiogram-synchronized, allowing for pulsatility during diastole, which was analogous to the concept of an intra-aortic balloon pump (IABP). Focusing on inflammatory responses related to ECMO, we used relatively healthy animals rather than animals with compromised heart or lung function, which might introduce biases. Other investigators also revealed that ECMO under pulsatile mode reduces priming volume and is associated with lower risks for tubing rupture, spallation, leakage, and embolization.10
The provision of pulsatility in the centrifugal pump and roller pump is typically difficult. Relatively few diagonal pumps are available. The i-Cor system was overall friendly to use. It had no difficulty in priming and switched conveniently between the continuous and pulsatile flow. Of note, a constant flow rate is recommended to keep the same flow rate if you switch continuous flow to pulsatile flow. Pressures at the outlet should be supervised and alerts should be taken for clots, leakage, and cannula kinking or migration. Cannulas must be secured to avoid bleeding around the insertion site, particularly in the pulsatile flow which slight shaking of the cannula will frequently take place. If tachycardia (heart rate above 150 beats/minute) is confronted, switching the 1:1 assisting mode to 1:2 will bring about better pulsatility, similar to the IABP protocols. Other recent examples that generate pulsatility for ECMO were the Medos Deltastream DP3 system (Medos Medizintechnik AG, USA)10 and the K-Beat system designed by Inamori’s group.22
The in vivo nature of our work surely presents certain limitations. Only healthy animals on ECMO for a relatively short duration were investigated. Hence, neither changes in cytokine levels in bronchoalveolar lavage, nor lung histological injuries were evaluated. Given the relatively small body weight of the experimental animals to model the pathophysiology of ECMO in infants, our data should still be validated in larger animal models. The pathophysiology of inflammation is a complicated process, involving an army of cytokines and chemokines, however, only a limited number of these biomarkers were measured in the present study. The investigators were non-blinded to the presence of pulsatility in this study. All these limitations prevent us from modeling inflammatory changes in real-world practice. Nevertheless, the hemodynamics, as well as ECMO-induced inflammation is easily neglected by clinicians, hence, translational investigations from bench to bedside are required.
The molecular mechanisms for pulsatile flow are still poorly acknowledged. Previously we also launched a bioinformatics analysis to figure out some underlying mechanisms for the pulsatility in ventricular assisting devices at the molecular level, and five hub genes strongly relevant to inflammation were identified, including CCL2, CX3CR1, CD163, TLR7, and SERPINE1.23 Prospective studies should assess more thoroughly how pulsatile flow acts on genetics. The inflammation activation is also closely interrelated with other pathophysiological processes like endothelial activation, coagulation, trauma, and so on. How pulsatility impacts these pathophysiological processes is still unclear and merits further investigations. Overall, future ECMO design will require an option of pulsatility. Either patients with cardiogenic shock or patients with severe COVID-19 usually receive ECMO for weeks or even months, a device allowing for more effective microcirculatory perfusion with less inflammatory responses is therefore optimal. These are crucial as ECMO techniques progress and become especially imperative amid the COVID-19 pandemic.
Conclusion
The i-Cor system is feasible to generate biomimetic pulsatile flow in our animal models on V-A ECMO. Most circuits went uneventfully, except for two cases of hypotension in the pulsatile group. Our findings demonstrated that the pulsatile modification in ECMO generates higher hemodynamic energies including SHE and EEP when compared with the traditional ECMO. The pulsatile circuits show declines in TNF-α and IL-1β, together with an increase in TGF-β1, suggesting that the pulsatility attenuates inflammatory responses during ECMO. Further studies are required to validate and refresh our results.
Funding
This study was supported by grants from the Traditional Chinese Medicine Bureau of Guangdong Province (Grant No. 20212071), National Natural Science Funds of China (Grant No. 82000081 and 81900285), Science and Technology Program of Guangzhou, China (Grant No. 202002030317), Medical Scientific Research Foundation of Guangdong Province of China (Grant No. A2021433), and Guangdong Basic and Applied Basic Research Foundation (Grant No. 2020A15150101242 and 2021A1515010280).
Disclosure
All authors declare no conflicts of interest.
References
1. Wu Z, McGoogan JM. Characteristics of and important lessons from the coronavirus disease 2019 (COVID-19) outbreak in China: summary of a Report of 72 314 cases from the Chinese center for disease control and prevention. JAMA. 2020;323(13):1239–1242. doi:10.1001/jama.2020.2648
2. Guan WJ, Ni ZY, Hu Y, et al. Clinical characteristics of coronavirus disease 2019 in China. N Engl J Med. 2020;382(18):1708–1720. doi:10.1056/NEJMoa2002032
3. Kowalewski M, Fina D, Słomka A, et al. COVID-19 and ECMO: the interplay between coagulation and inflammation-a narrative review. Crit Care. 2020;24(1):205. doi:10.1186/s13054-020-02925-3
4. Matteucci M, Fina D, Jiritano F, et al. The use of extracorporeal membrane oxygenation in the setting of postinfarction mechanical complications: outcome analysis of the extracorporeal life support organization registry. Interact Cardiovasc Thorac Surg. 2020;31(3):369–374. doi:10.1093/icvts/ivaa108
5. Salameh A, Kühne L, Grassl M, et al. Protective effects of pulsatile flow during cardiopulmonary bypass. Ann Thorac Surg. 2015;99(1):192–199. doi:10.1016/j.athoracsur.2014.07.070
6. Borulu F, Hanedan MO, Coşkun C, Emir İ, Mataraci İ. Investigation of the effect of pulsatile and nonpulsatile flow on kidney in coronary surgery with NIRS. Heart Surg Forum. 2020;23(4):E401–e6. doi:10.1532/hsf.2341
7. Sunagawa G, Koprivanac M, Karimov JH, Moazami N, Fukamachi K. Is a pulse absolutely necessary during cardiopulmonary bypass? Expert Rev Med Devices. 2017;14(1):27–35. doi:10.1080/17434440.2017.1265445
8. Kadiroğulları E, Sen O, Gode S, et al. Effect of pulsatile cardiopulmonary bypass in adult heart surgery. Heart Surg Forum. 2020;23(3):E258–e63. doi:10.1532/hsf.2857
9. Li G, Jiang W, Zhang Y, et al. The outcome of pediatric patients undergoing congenital cardiac surgery under pulsatile cardiopulmonary bypass in different frequencies. Ther Clin Risk Manag. 2018;14:1553–1561. doi:10.2147/TCRM.S170642
10. Wang S, Kunselman AR, Clark JB, Ündar A. In vitro hemodynamic evaluation of a novel pulsatile extracorporeal life support system: impact of perfusion modes and circuit components on energy loss. Artif Organs. 2015;39(1):59–66. doi:10.1111/aor.12430
11. Fleck T, Benk C, Klemm R, et al. First serial in vivo results of mechanical circulatory support in children with a new diagonal pump. Eur J Cardiothorac Surg. 2013;44(5):828–835. doi:10.1093/ejcts/ezt427
12. Ostadal P, Mlcek M, Gorhan H, et al. Electrocardiogram-synchronized pulsatile extracorporeal life support preserves left ventricular function and coronary flow in a porcine model of cardiogenic shock. PLoS One. 2018;13(4):e0196321. doi:10.1371/journal.pone.0196321
13. Percie Du Sert N, Hurst V, Ahluwalia A, et al. The ARRIVE guidelines 2.0: updated guidelines for reporting animal research. PLoS Biol. 2020;18(7):e3000410. doi:10.1371/journal.pbio.3000410
14. Chousterman BG, Swirski FK, Weber GF. Cytokine storm and sepsis disease pathogenesis. Semin Immunopathol. 2017;39(5):517–528. doi:10.1007/s00281-017-0639-8
15. Veras FP, Pontelli MC, Silva CM, et al. SARS-CoV-2-triggered neutrophil extracellular traps mediate COVID-19 pathology. J Exp Med. 2020;217(12). doi:10.1084/jem.20201129.
16. Conti P, Caraffa A, Gallenga CE, et al. Coronavirus-19 (SARS-CoV-2) induces acute severe lung inflammation via IL-1 causing cytokine storm in COVID-19: a promising inhibitory strategy. J Biol Regul Homeost Agents. 2020;34(6).
17. Hong TH, Kuo SW, Hu FC, et al. Do interleukin-10 and superoxide ions predict outcomes of cardiac extracorporeal membrane oxygenation patients? Antioxid Redox Signal. 2014;20(1):60–68. doi:10.1089/ars.2013.5427
18. Risnes I, Wagner K, Ueland T, Mollnes T, Aukrust P, Svennevig J. Interleukin-6 may predict survival in extracorporeal membrane oxygenation treatment. Perfusion. 2008;23(3):173–178. doi:10.1177/0267659108097882
19. Cremers B, Link A, Werner C, et al. Pulsatile venoarterial perfusion using a novel synchronized cardiac assist device augments coronary artery blood flow during ventricular fibrillation. Artif Organs. 2015;39(1):77–82. doi:10.1111/aor.12413
20. Wang S, Izer JM, Clark JB, et al. In vivo hemodynamic performance evaluation of novel electrocardiogram-synchronized pulsatile and nonpulsatile extracorporeal life support systems in an adult swine model. Artif Organs. 2015;39(7):E90–E101. doi:10.1111/aor.12482
21. Wang S, Krawiec C, Patel S, et al. Laboratory evaluation of hemolysis and systemic inflammatory response in neonatal nonpulsatile and pulsatile extracorporeal life support systems. Artif Organs. 2015;39(9):774–781. doi:10.1111/aor.12466
22. Fujii Y, Akamatsu N, Yamasaki Y, et al. Development of a pulsatile flow-generating circulatory assist device (K-Beat) for use with veno-arterial extracorporeal membrane oxygenation in a Pig Model Study. Biology. 2020;9(6):121. doi:10.3390/biology9060121
23. Li G, Chen Z, Zhang Y, Wu Z, Zheng J. Effects of left ventricular assist device on heart failure patients: a bioinformatics analysis. Artif Organs. 2020;44(6):577–583. doi:10.1111/aor.13627
 © 2021 The Author(s). This work is published and licensed by Dove Medical Press Limited. The full terms of this license are available at https://www.dovepress.com/terms.php and incorporate the Creative Commons Attribution - Non Commercial (unported, v3.0) License.
By accessing the work you hereby accept the Terms. Non-commercial uses of the work are permitted without any further permission from Dove Medical Press Limited, provided the work is properly attributed. For permission for commercial use of this work, please see paragraphs 4.2 and 5 of our Terms.
© 2021 The Author(s). This work is published and licensed by Dove Medical Press Limited. The full terms of this license are available at https://www.dovepress.com/terms.php and incorporate the Creative Commons Attribution - Non Commercial (unported, v3.0) License.
By accessing the work you hereby accept the Terms. Non-commercial uses of the work are permitted without any further permission from Dove Medical Press Limited, provided the work is properly attributed. For permission for commercial use of this work, please see paragraphs 4.2 and 5 of our Terms.