Back to Journals » Drug Design, Development and Therapy » Volume 16
Nintedanib Treatment After Ovulation is an Effective Therapeutic Strategy for the Alleviation of Ovarian Hyperstimulation Syndrome (OHSS) in a Mouse Model
Authors Jiang S , Li W , Zhao X, Chen L , Kuang Y
Received 29 November 2021
Accepted for publication 4 February 2022
Published 18 February 2022 Volume 2022:16 Pages 397—411
DOI https://doi.org/10.2147/DDDT.S351292
Checked for plagiarism Yes
Review by Single anonymous peer review
Peer reviewer comments 2
Editor who approved publication: Prof. Dr. Tin Wui Wong
Shutian Jiang,* Wenzhi Li,* Xinxi Zhao, Li Chen, Yanping Kuang
Department of Assisted Reproduction, Shanghai Ninth People’s Hospital, Shanghai Jiaotong University School of Medicine, Shanghai, People’s Republic of China
*These authors contributed equally to this work
Correspondence: Yanping Kuang; Wenzhi Li, Email [email protected]; [email protected]
Purpose: Ovarian hyperstimulation syndrome (OHSS) is a serious complication of controlled ovarian hyperstimulation. In this study, we hope to explore whether nintedanib, a tyrosine kinase inhibitor, can inhibit OHSS by blocking signaling of vascular endothelial growth factor in a mouse model. Considering that nintedanib been approved for the treatment of some diseases. We believe that nintedanib has important potential in the treatment of OHSS.
Methods: Female ICR mice aged 6– 8 weeks with similar initial weights were used to establish the OHSS model. At 12 and 24 hours after human chorionic gonadotropin (hCG) trigger, we administered nintedanib by subcutaneous injection and analyzed the OHSS-related physiological characteristics and biochemical indices of the model mice within 48 hours after hCG-trigger.
Results: Nintedanib significantly alleviated the symptoms of OHSS after hCG-trigger compared with those of OHSS group (weight change, P < 0.0001; ovarian weight, P < 0.0001, peritoneal exudation level, P < 0.01). Further investigation proved that the corpus luteum (number, P < 0.001; diameter, P < 0.0001) and luteal vessel (P < 0.0001) development were inhibited in the nintedanib administration group. Then, the vascular permeability test showed that the capillary bleeding points (P < 0.0001) were also significantly reduced in nintedanib administration group. Gene expression tests demonstrated that the intercellular connection-related genes expression in the nintedanib administration group was similar to that in the no-OHSS induced group. Further detection of coagulation and thrombosis indices indicated that the nintedanib administration in the OHSS model did not increase the risk of thrombosis or bleeding.
Conclusion: Our study demonstrated that nintedanib can alleviate and manage the symptoms of OHSS in a mouse model. These findings identify a feasible scheme for the prevention and treatment of OHSS in clinical practice in the future. Moreover, since the scheme can be implemented after ovulation, it will not cause potential adverse effects on gametogenesis, fertilization or embryonic development.
Keywords: ovarian hyperstimulation syndrome, vascular endothelial growth factor, nintedanib, tyrosine kinase inhibitor, vascular permeability
Introduction
Ovarian hyperstimulation syndrome (OHSS) is a serious complication that may occur in the process of controlled ovarian hyperstimulation.1,2 To date, the mechanism of OHSS is not fully understood, but its pathogenesis as follows. During the follicular phase, multiple follicles develop simultaneously with the application of ovulation-stimulating drugs. Then, after ovulation/oocyte retrieval, extensive luteinization occurs in the ovaries and the large amount of newly generated corpus luteum will lead to ovarian enlargement and secretion of a series of substances, including estrogen, progesterone and vascular growth factors (eg, vascular endothelial growth factor, VEGF),2,3 which promoting the proliferation of vessels in the corpus luteum and increasing the permeability of local capillaries.4 As a result, body fluid “leaks” and accumulates in the third space, clinically manifesting as a decrease in blood volume and multiple system failure (renal, hepatic, respiratory and circulatory dysfunctions), which may potentially develop into a life-threatening condition.2,4,5 Therefore, how to prevent the occurrence of OHSS and find an effective treatment for OHSS is important in the field of assisted reproduction.
At present, there is a set of methods to prevent the occurrence of OHSS in clinical practice, mainly including the reduction in hCG dose when trigger,6 a “freeze-all” strategy for patients at high risk of OHSS,7 and tapering or ceasing gonadotropin administration when multiple follicles develop and estradiol rises severely.8 In addition, some drugs have been applied to prevent OHSS, such as metformin, clarithromycin, oxytocin and cabergoline in recent years.9–12 The latter, a dopamine agonist that acts as a vascular permeability inhibitor, has been used clinically to reduce the incidence of moderate to severe OHSS. However, despite various methods to prevent OHSS, the effect is still limited, and occasionally, a few cases of OHSS inevitably and unpredictably occur.2,5,6,8 For OHSS that has occurred, most of the available measures are symptomatic relief and supportive treatment.1,2,5,13–15 These treatments are of little benefit, and the final recovery of the disease depends on its self-limitation.
Early studies have found that there are many cytokines and growth factors (including tumor necrosis factor/TNF, VEGF and interleukins: IL-2, IL-6, IL-8, IL-10, IL-18, etc.) in the peritoneal effusion of patients with OHSS,16,17 among which VEGF is considered to play a key role in the occurrence of OHSS.18 For direct intervention of VEGF expression, the main method is to block the synthesis of VEGF by drugs (including adding kisspeptin-10, inhibiting transforming growth factor/TGFβ1 or vasopressin).19–22 However, such a strategy often requires additional administration during ovarian stimulation. This process may affect the development of follicles and the genetic safety of gametes. Another strategy is drug intervention after ovulation/oocyte retrieval, which aims to block the effect of synthesized VEGF and other cytokines on downstream receptors, mainly including blocking the binding of VEGF and VEGFR by antibodies,18 inhibiting the phosphorylation of the VEGF receptor and blocking its downstream pathway of increasing permeability. It has been reported that SU5416 can inhibit angiogenesis and vascular permeability by inhibiting the phosphorylation of VEGFR2 in an OHSS model.23 However, because it might lead to severe vomiting and intravascular embolism, this drug failed to be developed for subsequent clinical application for OHSS.24,25
Nintedanib is a drug that has been approved for the clinical treatment of pulmonary fibrosis, systemic sclerosis-associated interstitial lung disease and non-small cell lung cancer.26–28 It is a broad-spectrum and powerful tyrosine kinase inhibitor targeting vascular endothelial growth factor receptors (VEGFRs), fibroblast growth factor receptors (FGFRs) and platelet-derived growth factor receptors (PDGFRs). The corresponding cytokines of these three receptors play an important role in promoting angiogenesis.26–29 Moreover, compared with other kinds of TKIs, such as SU5416, nintedanib results in a very low risk of bleeding in application, and more importantly, it does not show a correlation with thrombosis.30–32 Therefore, in this study, we intervened in disease progression by administering nintedanib to a mouse model of OHSS to explore the possibility of this drug in the treatment of OHSS. The results showed that the application of nintedanib after ovulation in the OHSS model could effectively inhibit the enlargement of the ovary, the proliferation of corpus luteum vessels and the increase in vascular permeability. These results suggest that nintedanib may be a potential effective drug in the prevention and treatment of OHSS.
Materials and Methods
Induction of Ovulation Under General/OHSS Conditions and Nintedanib Treatment
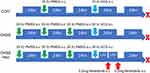
The 6-week-old ICR female mice with similar body weight (201, Vital River, China) were divided into the controlled ovarian hyperstimulation (COH), ovarian hyperstimulation syndrome (OHSS) and ovarian hyperstimulation syndrome with nintedanib administration (OHSS + Nin) groups. Based on the ovarian stimulation protocol in the reported literatures,33,34 we developed a modified OHSS mouse model to achieve more stable phenotypic characteristics. In detail, for the COH group, 10 international unit (IU) of pregnant horse serum gonadotropin (PMSG, 110914564, Sansheng Biological Technology, China) dissolved in saline was subcutaneously injected. Forty-eight hours later, 10 IU of human chorionic gonadotropins (hCG, 110911282, Sansheng Biological Technology, China) dissolved in saline was subcutaneously injected. For the OHSS group, 20 IU of PMSG dissolved in saline was subcutaneously injected every day for three consecutive days, with an interval of 24 hours. Then, after 24 hours, 30 IU of hCG dissolved in saline was subcutaneously injected. For the OHSS + Nin group, induction of ovulation was the same as that in the OHSS group. After 12 hours and 24 hours of hCG injection, 0.2 mL of nintedanib (S1010, Selleck, US) suspension (added in sequence and fully mixed with each solvent: 10% ~10 mg/mL nintedanib in DMSO, 40% PEG300, 5% Tween-80, 45% saline) was subcutaneously injected.
Detection of Typical OHSS Symptoms (Body Weight Change and Ovarian Weight, Peritoneal Effusion Level)
For body weight change, mice were marked with ear tags, before weighing the mice were anesthetized with isoflurane, their body weight was measured within 1-hour before hCG-trigger and 48-hour after hCG-trigger, then the weight change of each mouse was obtained by subtracting the previous data from the latter data. For the ovary weight, after the mice were sacrificed, the ovaries were removed, and the nonspecific tissues were pruned. Then, the excess water was removed, and the weight was measured on a precision balance. For peritoneal effusion level, the mice were anesthetized and injected with 0.1 mL of 5 mM Evan’s blue dye (A602025, Sangon, China) through the tail vein. One hour later, 3 mL of saline was injected intraperitoneally, and the abdomen was gently and carefully massaged for 1 minute. Then, the peritoneal fluid was carefully obtained and added to an ELISA plate. Then, the absorbance value was detected at 450 nm by a microplate reader (F50, Tecan, Switzerland).
Serum Hormone and Growth Factor Detection
After anesthesia, the tail vein of the mice was carefully cut off, the blood was repeatedly massaged and squeezed to drip into the collecting tube, and then, it was allowed to stand at room temperature for 1 hour. After initial blood coagulation, the supernatant was centrifuged at 350 rcf for 10 minutes. Then, mouse VEGF-A (D721156, Sangon, China)/progesterone (D751044, Sangon, China)/estradiol (D741005, Sangon, China) ELISA kits were used.
HE Staining and Immunohistochemistry
After the mice were sacrificed, the ovaries were removed and placed in 4% paraformaldehyde (PFA) overnight at room temperature. Next, the Leica automatic immunohistochemistry system was used to generate the slides. Then, the antibodies (VEGF-A antibody, ab1316, Abcam, US/CD31 antibody, ab182981, Abcam, US) were incubated with the slides, followed by staining with hematoxylin-eosin (HE). The thickness of the sections was 8 μm.
Determination of Vascular Permeability
As reported in the literature,35 after anesthesia, fluorescently labeled Ricinus communis agglutinin I (RCA I, L32478, Invitrogen, US) and Lycopersicon esculentum lectin (LEL, L32471, Invitrogen, US) were injected into mice via the tail vein. One hour later, the mice were perfused with saline containing 1% PFA, and the ovary/mesentery-small intestine tissue was removed and quickly cooled in liquid nitrogen. Then, the tissues were sectioned on a frozen section machine and observed under an Olympus confocal microscope. The thickness of the sections was 10 μm.
Gene Expression Detection and Analysis
After the mice were sacrificed, the ovarian tissue was removed, cleaned, and quickly frozen in liquid nitrogen. The subsequent base construction and sequencing work were completely based on the Illumina HiSeq-2500 system. Data extraction and analysis were carried out according to the literature description. All the original sequencing data can be obtained from the Gene Expression Omnibus (GEO) under accession number GSE183346.
Coagulation and D-D Dimer Detection
After anesthesia, the eyeballs of the mice were removed for blood collection, and the obtained blood was mixed with 2.5% sodium citrate at a ratio of 9:1. After standing at room temperature for half an hour, the samples were centrifuged at 2000 g for 10 minutes, and the plasma supernatant was carefully collected. Subsequently, the coagulation- and thrombus-related indices PT, APTT, TT, FIB and D-D dimer were detected by a coagulation analyzer (CS-5100, Sysmex, China).
Unilateral Ovariectomy in Mice
Twelve hours after triggering by hCG, the mice were anesthetized. Then, the abdomen was opened up, and one of the two ovaries was pulled out for each mouse. In the experimental group, mice with OHSS underwent unilateral ovariectomy. Moreover, in the COH group and OHSS group (control groups), the ovaries of the mice were just pulled out for confirmation and then placed back intact. Then, in both groups, the abdomen was closed by fine stitching for later observation.
Statistical Methods
Statistical analysis was carried out using SPSS 24.0 statistical software. The results are expressed as the mean ± standard error of the mean (X ± SD). One-way ANOVA is used for comparison among three groups. Dunnett's test is used for comparison between control and experimental groups, P < 0.05 was considered statistically significant. Bonferroni test is used for comparison between experimental groups, P < 0.016 was considered statistically significant in Bonferroni test of three groups. All quantifiable results are integrated in Table S1.
Results
Nintedanib Treatment After Ovulation Alleviates OHSS Symptoms in a Mouse Model
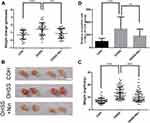
First, we evaluated the typical OHSS characteristics of the mouse model with different processing strategies (Figure 1). We found that compared with that of the COH group (0.74 ± 0.59 g, n=32), the weight change of the mice from hCG-trigger to 48h after trigger in the OHSS group (1.45 ± 0.83 g, n=45) increased, while the weight of the mice in the OHSS+Nin group (0.90 ± 0.62 g, n=44) treated with nintedanib did not change significantly (Figure 2A). Then, we compared the ovarian weight, which presented a more notable difference (Figure 2B and C). Compared with that of the COH group (7.26 ± 2.14 mg, n=64), the ovarian weight of the OHSS group (13.57 ± 4.67 mg, n=90) was obviously increased. However, in the OHSS+Nin group (10.35 ± 4.21 mg, n=88), nintedanib treatment apparently alleviated the enlargement of the ovaries. A phenotype similar to that of the OHSS + Nin group was also observed in the OHSS mice with unilateral ovariectomy. Twelve hours after the hCG trigger, we resected one side of the ovary and then sewed up the incision (Figure S1A). Then, similar changes in mouse body weight and ovarian weight were detected at the same observation time point as mentioned above (Figure S1B–D).
To directly prove whether there was a significant increase in vascular leakage, we used intravenous injection of Evans blue and collected the peritoneal exudate 30 minutes later, after which the content of Evans blue was detected by spectrophotometer (Figure 2D). The results showed that the content of Evans blue in the OHSS group (295.90 ± 189.20%, n=28) was significantly higher than that in the COH group (100.00 ± 46.30%, n=26), and there were obvious differences among individual mice. However, the content of Evans blue in the peritoneal exudate of the OHSS+Nin group (186.90 ± 106.70%, n=31), which was treated with nintedanib after ovulation, decreased dramatically.
Nintedanib Inhibited Corpus Luteum Development by Reducing Ovarian Vascular Density
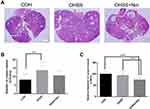
To further observe the effect of nintedanib-induced vascular density reduction on the corpus luteum and ovary after ovulation, we sacrificed the mice and collected the ovaries 2 days post-hCG trigger. Then, we determined the number and diameter of the corpus luteum with HE staining (Figure 3A). We found that the OHSS group (13.80 ± 4.87, n=15) had the highest mean number of corpora lutea per slide. Moreover, although the OHSS + Nin group (10.60 ± 2.61, n=15) had a higher mean luteal number than the control group (8.13 ± 3.42, n=15), this value was significantly lower than that of the OHSS group (Figure 3B). Further comparing the diameter of the corpus luteum, we found that there was no significant difference in this parameter between the COH group (100.00 ± 14.42%, n=45) and the OHSS group (94.64 ± 16.48%, n=64), but the mean luteal diameter of the OHSS + Nin group (74.58 ± 12.49%, n=44) was significantly smaller than that of the other two groups (Figure 3C).
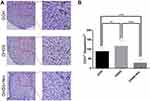
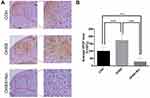
Considering that nintedanib is a broad-spectrum inhibitor of VEGFR/PDGFR/FGFR, it can effectively inhibit angiogenesis. We measured the level and distribution of CD31 (PECAM1), which is a well-known vascular marker, in the corpus luteum two days post-hCG trigger by immunohistochemistry (Figure 4A). Then, we discovered that compared with that of the COH group (88.58 ± 20.80, n=20), the number of CD31+ vessels in the OHSS group (116.50 ± 31.86, n=23) was distinctively increased, while the number of CD31+ vessels in the OHSS + Nin group (27.88 ± 19.43, n=24) was significantly lower than that in the OHSS group (Figure 4B).
Disturbed Luteal Function Was Accompanied by Decreased VEGF Levels
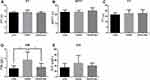
We also evaluated the function of the corpus luteum by measuring the serum estradiol, progesterone and VEGF levels of the mice in different periods. We found that estrogen levels were less affected by nintedanib treatment after the hCG trigger. Since the regimen was the same between the OHSS group and the OHSS + Nin group before trigger, the estradiol value of the two groups remained similar in the follicular phase, while after the trigger, the estradiol level of the OHSS + Nin group (Day 3: 23.00 ± 4.86 pg/mL, n=6; Day 4: 22.83 ± 3.87 pg/mL, n=6) was slightly lower than that of the OHSS group (Day 3: 25.67 ± 3.88 pg/mL, n=6; Day 4: 25.00 ± 4.29 pg/mL, n=6), with both of these groups maintaining levels higher than the COH group (Day 3: 13.33 ± 5.16 pg/mL, n=6; Day 4: 16.33 ± 4.23 pg/mL, n=6) (Figure 5A). However, with nintedanib treatment, although the progesterone level of the OHSS + Nin group (Day 3: 45.00 ± 9.59 ng/mL, n=6; Day 4: 38.67 ± 5.47 ng/mL, n=6) was still higher than that of the COH group (Day 3: 35.67 ± 4.97 ng/mL, n=6; Day 4: 34.33 ± 5.50 ng/mL, n=6), it clearly decreased after the initial rise following the hCG trigger compared with the continuing rising trend of the OHSS group (Day 3: 63.33 ± 13.76 ng/mL, n=6; Day 4: 67.83 ± 13.70 ng/mL, n=6) (Figure 5B). The level of VEGF in serum was similar to that of progesterone. After nintedanib treatment, although the VEGF level of the OHSS + Nin group (Day 3: 43.00 ± 4.94 pg/mL, n=6; Day 4: 47.50 ± 6.57 pg/mL, n=6) was higher than that of the COH group (Day 3: 37.83 ± 3.76 pg/mL, n=6; Day 4: 43.17 ± 5.91 pg/mL, n=6), the value and increase rate were apparently lower than those of the OHSS group (Day 3: 48.17 ± 5.04 pg/mL, n=6; Day 4: 62.83 ± 12.66 pg/mL, n=6) (Figure 5C).
To further assess whether luteal function was influenced by nintedanib in the OHSS + Nin group, we detected the level of VEGF in the corpus luteum 2 days post-hCG trigger by immunohistochemistry (Figure 6A). The results demonstrated that compared with that in the OHSS group (173.70 ± 40.55%, n=23), the expression of VEGF in the corpus luteum in the OHSS + Nin group decreased significantly (27.84 ± 24.73%, n=24) and was much lower than that in the COH group (100.00 ± 27.20%, n=19) (Figure 6B).
Changes in Peritoneal Vascular Permeability and Cell-Cell Adhesion-Related Gene Expression
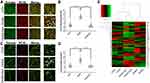
A decrease in VEGF levels will also reduce vascular permeability. To intuitively observe the changes in vascular permeability, we intravenously injected FITC-labeled Lycopersicon esculentum lectin (FITC-LEL, vascular endothelial marker) and DyLight594-labeled Ricinus communis agglutinin I (DL594-RCA I, serum albumin marker) into the mice 2 days post hCG-trigger. One hour later, we collected the ovaries and mesentery-small intestine segments to observe them with frozen sections and fluorescence (Figure 7A–D). The results showed that in ovaries, the number of vascular exudation points of the OHSS group (12.44 ± 2.36, n=18) was significantly greater than that of the COH group (2.35 ± 2.25, n=20), while the exudation points of the OHSS + Nin group (1.524 ± 2.06, n=21) were significantly reduced (Figure 7B); in the mesentery-small intestine segments, the vascular exudation points of surface capillaries of the small intestine showed the same trend as ovarian capillaries: compared with that of the COH group (1.85 ± 2.16, n=20), the exudation point in the OHSS group (6.80 ± 2.24, n=20) increased significantly, while the exudation level in the OHSS + Nin group (1.24 ± 1.70, n=21) decreased (Figure 7D).
To further illustrate the inhibitory effect of nintedanib treatment on luteal vascular permeability, we detected gene expression in whole ovarian tissue 2 days post-hCG triggering by high-throughput sequencing (Figure 7E, Table S2). The results showed that intercellular adhesion-related genes were one of the main differentially expressed gene clusters among the groups. Compared with those of the OHSS group, the expression characteristics of the OHSS + Nin group were more similar to those in the COH group.
The Risk of Coagulation and Thrombosis Did Not Increase Significantly with the Administration of Nintedanib
It has been reported that the application of TKIs may increase the risk of bleeding and thrombosis, and OHSS itself has certain characteristics of hypercoagulability. Therefore, we detected indices related to coagulation and thrombosis (Figure 8). In terms of coagulation-related indices, prothrombin time (PT), activated partial thromboplastin time (APTT) and thrombin time (TT) were not significantly different among the three groups. For fibrinogen (FIB), the OHSS group (3.70 ± 1.72 g/L, n=16) showed a higher level, while the COH group (1.79 ± 0.60 g/L, n=14) and the OHSS + Nin group (2.11 ± 0.80 g/L, n=16) showed a relatively lower level. In terms of thrombus-related indices, although the level of D-D dimer in the OHSS group (50.00 ± 27.81 μg/L, n=16) was relatively high, there was no significant difference compared with the COH (33.57 ± 14.99 μg/L, n=14) and OHSS + Nin groups (40.63 ± 9.29 μg/L, n=16).
Discussion
OHSS is a kind of iatrogenic complication that occasionally occurs after ovarian stimulation. However, the dominant therapeutic schedule of OHSS remains symptomatic and supportive treatment at present, and preventive measures have limited effects, resulting in many patients inevitably suffering from OHSS.5,14,16,18,36 In the current study, we established a mouse model of OHSS using PMSG and hCG. We found that the OHSS symptoms were significantly alleviated with the use of nintedanib, including weight gain, ovarian enlargement and increase in peritoneal vascular permeability. Meanwhile, it was observed that the corpus luteum development as well as the luteal secretory function in OHSS mice with nintedanib treatment were obviously inhibited. Additionally, it was demonstrated that the intercellular adhesion-related genes were markedly differentially expressed among groups.
Initially, we used subcutaneous injection of nintedanib twice, at 12 hours and 24 hours after the hCG trigger in the OHSS mouse model (Figure 1). Then, we found that this strategy could effectively inhibit the weight gain and ovarian enlargement of mice. Among these parameters, weight may be affected by many factors, with its change relatively not obvious. However, considering the substantial sample size, it can still reflect the exudation and retention of body fluid to some extent (Figure 2A). Ovarian enlargement is one of the typical pathological features of OHSS and mainly represents the continuous development of the corpus luteum and local tissue edema. Notably, in the OHSS + Nin group treated with nintedanib, the ovarian weight and size did not seem to increase significantly after ovulation (Figure 2B and C), which suggested that the development of the corpus luteum and the accompanying exudation might be inhibited by nintedanib. It thus appears that the symptoms of OHSS are relieved with the use of nintedanib, probably as a consequence of a weakening in VEGF downstream effects. This phenomenon is similar to what we observed in the mouse model of unilateral ovariectomy after ovulation. Weight gain and ovarian enlargement in OHSS were strongly inhibited by resection of one side of the ovary, indicating that the production of VEGF mainly comes from ovaries and a reduction in VEGF production can alleviate vascular proliferation of the other ovary and inhibit the occurrence of OHSS (Figure S1).
Then, we evaluated the number and diameter of the corpus luteum in HE-stained sections. Compared with those of the OHSS group, the number and diameter of the corpus luteum in the OHSS + Nin group decreased significantly (Figure 3). This result demonstrated that the luteal development of the OHSS + Nin group was indeed inhibited. Considering that the ovulation induction plan before hCG triggering was the same in the OHSS group and the OHSS + Nin group, together with the inhibitory effect of nintedanib on angiogenesis, we inferred that the inhibition of luteal development in the OHSS + Nin group was due to the inhibition of luteal vascular development by nintedanib. Therefore, we observed the expression and distribution of total CD31 in the corpus luteum by immunohistochemical staining (Figure 4). The results showed that compared with that of the OHSS group, the density of luteal vessels in the OHSS + Nin group decreased significantly. This result indicated that the impaired development of the corpus luteum is caused by the inhibition of corpus luteum angiogenesis. Abnormal development is often accompanied by abnormal function. Therefore, we measured the serum levels of estradiol, progesterone and VEGF in the model mice at different time points (Figure 5). The levels of serum progesterone and VEGF in the OHSS group increased continuously after ovulation, while in the OHSS + Nin group, VEGF increased much slower, and progesterone levels showed a downward trend (Figure 5B and C). Further immunohistochemical staining of VEGF also showed that the level of VEGF in the OHSS + Nin group was significantly lower than that in the OHSS group (Figure 6). All of these results illustrated that the luteal synthesis function in the OHSS + Nin group, including the secretion of hormones and growth factors, was weaker than that in the OHSS group. The development of the corpus luteum depends on vascular proliferation induced by VEGF, and the functional corpus luteum is the main source of VEGF. Therefore, we conclude that nintedanib treatment interferes with the initial interaction between VEGF and VEGFR in the corpus luteum, which leads to the inhibition of luteal vascular proliferation and abnormal luteal development. As a result, the synthesis of sexual hormones and growth factors (progesterone, VEGF, etc.) is impaired. In this manner, the “positive feedback” mechanism of luteal development is disrupted.
In addition, we used vein injection of Evans blue to detect the peritoneal exudation level of mice (Figure 2D). After a period of intravenous injection, the Evans blue content of the exudate in the abdominal cavity can represent the change in local vascular permeability. The results showed that compared with the high level of Evans blue in the OHSS group, the level of Evans blue in the peritoneal fluid of the OHSS + Nin group was significantly lower, although it was still higher than that of the COH group. This result suggested that the increase in vascular permeability induced by OHSS might be inhibited by nintedanib treatment. To further explore whether changes in vascular permeability occur widely in the abdominal cavity, we labeled endothelial cells and blood cells with tomato agglutinin and Ricinus communis agglutinin, respectively, by tail iv administration and then observed the in-situ permeability of the corpus luteum and intestinal surface capillaries by frozen sectioning (Figure 7A–D). The results showed that in the OHSS + Nin group, the number of exudation points in both the corpus luteum and intestinal surface capillaries was less than that in the OHSS group. This result reveals that the permeability of capillaries in the whole abdominal environment is affected by the upregulation of VEGF expression induced by OHSS levels, and the application of nintedanib can inhibit this change.
Moreover, the global gene expression analysis of ovarian tissue showed that the expression characteristics of genes related to intercellular adhesion and association in the OHSS + Nin group were closer to those in the COH group, while the expression of the corresponding genes in the OHSS group was significantly different (Figure 7E). This finding suggests that nintedanib can indeed reduce the increase in peritoneal capillary permeability induced by OHSS. Combined with the abovementioned results (the development of the corpus luteum and the synthesis of hormones and growth factors were affected by nintedanib), we believe that nintedanib treatment can reduce the increase in corpus luteum vascular permeability by blocking the development of the corpus luteum and the secretion of VEGF and other signaling molecules.
It has been reported that TKI treatment may lead to an increased risk of both thrombosis and bleeding.31 Among these drugs, nintedanib is considered to have little risk of thrombosis and only a very low risk of bleeding.30–32 Due to the body fluid loss caused by OHSS, the patient’s blood is generally in a hypercoagulable state.1,14 Therefore, the bleeding risk of nintedanib is further reduced in the context of the hypercoagulable state of OHSS itself. To comprehensively evaluate the two risks, we tested coagulation- and thrombosis-related indices of mouse models after using nintedanib (Figure 8). The results showed that FIB increased significantly in the OHSS group compared with the COH group and the OHSS + Nin group. The corresponding D-D dimer also increased in the OHSS group, but without a significant difference compared with the other two groups. Since these two indicators both reflect thrombotic risk, the results confirmed the hypercoagulable state of OHSS and that nintedanib treatment in OHSS do not increase the risk of thrombosis. For the indices of APTT, PT and TT, all of which represent the bleeding risk, there was no significant difference observed among the three groups, with the indices of the OHSS + Nin group much closer to those in the COH group. This result suggests that the use of nintedanib does not increase the risk of bleeding in the OHSS mouse model. In addition to the low risk of thrombosis and bleeding of the drug itself, we speculate from the following two perspectives to explain the results. On the one hand, the use of nintedanib alleviates the symptoms of OHSS, thus reducing the loss of body fluid and avoiding the occurrence of blood hypercoagulability. On the other hand, the treatment of OHSS is generally a relatively short process, while the side effects of nintedanib reported in the literature are for the treatment of other diseases, with long-term and high-dose drug utilization characteristics.30–32,37 Therefore, we believe that the use of nintedanib in OHSS can avoid the risks related to coagulation and bleeding. Moreover, according to the literature reports, after stopping the use of TKIs, the capillary system of the corresponding tissue can be quickly restored and reconstructed, which suggests that the use of this kind of drug should not affect the structure and function of the ovary in the future.37
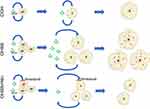
In conclusion, we found that nintedanib, a broad-spectrum angiogenesis inhibitor, can directly block the effect of VEGF on VEGFR through the action of TKIs; moreover, nintedanib can inhibit the proliferation of corpus luteum vessels, thus destroying the development of the corpus luteum and the secretion of VEGF. Both of these factors can reduce the vascular permeability increase induced by VEGF to alleviate the severity of OHSS symptoms (Figure 9). In addition, no serious side effects, such as thrombosis and bleeding, were observed in the treatment of OHSS with nintedanib. Considering that current treatment schemes, such as cabergoline, are not fully applicable to all cases and that nintedanib is a more direct and powerful VEGF signal blocker that can be used after ovulation, our results may provide a new idea for the treatment of OHSS without affecting the ovulation stimulation process, oocyte quality, embryonic development or gamete safety. Undeniably, the application of nintedanib has limitations. Since the scheme dramatically blocks the development of the corpus luteum and reduces luteal function, it is not suitable for fresh embryo transfer cycles. However, taking its potential therapeutic value into account, we think nintedanib is worthy of consideration among patients at high risk of OHSS in “freeze-all” COH cycles.
Abbreviations
COH, Controlled ovarian hyperstimulation; FGFR, Fibroblast growth factor receptor; GEO, Gene Expression Omnibus; GnRH, Gonadotropin-releasing hormone; GnRH-A, Gonadotropin-releasing hormone agonist; hCG, Human chorionic gonadotropin; HE, Hematoxylin-eosin; IU, International unit; LEL, Lycopersicon esculentum lectin; LH, Luteinizing hormone; Nin, Nintedanib; OHSS, Ovarian hyperstimulation syndrome; PDGFR, Platelet-derived growth factor receptors; PMSG, Pregnant horse serum gonadotropin; RCA I, Ricinus communis agglutinin I; TGFβ1, Transforming growth factor 1; TKI, Tyrosine kinase inhibitors; TNF, Tumor necrosis factor; VEGF, Vascular endothelial growth factor; VEGFR, Vascular endothelial growth factor receptor; E2, Estradiol; P4, Progesterone; CD31, PECAM1; SD, Standard deviation; PT, Prothrombin time; APTT, Activated partial thromboplastin time; TT, Thrombin time; FIB, Fibrinogen; D-D, D-D dimer.
Data Sharing Statement
The raw data supporting the conclusions of this article will be made available by the authors, without undue reservation. Contact E-mail [email protected] (Wenzhi Li).
Ethics Approval and Consent to Participate
All animal experiments were conducted in accordance with the Guide for the Care and Use of Animals for Research Purposes. The protocol for mouse embryo operation was approved by the Institutional Animal Care and Use Committee and Internal Review Board of Shanghai Jiaotong University School of Medicine (Approval number: SH9H-2021-A167-SB).
Consent for Publication
All authors declare their agreement to publish this article.
Acknowledgments
We thank the Clinical laboratory department and Pathology department of Shanghai Ninth People’s Hospital, Shanghai Jiao Tong University School of Medicine for providing the platform and the convenience of performing experiments. Shutian Jiang and Wenzhi Li are co-first authors for this study. Wenzhi Li and Yanping Kuang are co-senior authors for this study.
Funding
This work was supported by the National Natural Science Foundation of China (81901478) and the Fundamental Research Program Funding of Ninth People’s Hospital affiliated to Shanghai Jiao Tong University School of Medicine (JYZZ084B).
Disclosure
The authors report no conflicts of interest in this work.
References
1. Delvigne A, Rozenberg S. Epidemiology and prevention of ovarian hyperstimulation syndrome (OHSS): a review. Hum Reprod Update. 2002;8(6):559–577. doi:10.1093/humupd/8.6.559
2. Humaidan P, Nelson SM, Devroey P, et al. Ovarian hyperstimulation syndrome: review and new classification criteria for reporting in clinical trials. Hum Reprod. 2016;31(9):1997–2004. doi:10.1093/humrep/dew149
3. Morris RS, Wong IL, Do YS, et al. The pathophysiology of ovarian hyperstimulation syndrome (OHSS). A proposal role of the ovarian derived prorenin to angiotensin cascade (ODPAC). Adv Exp Med Biol. 1995;377:391–398.
4. Soares SR, Gomez R, Simon C, Garcia-Velasco JA, Pellicer A. Targeting the vascular endothelial growth factor system to prevent ovarian hyperstimulation syndrome. Hum Reprod Update. 2008;14(4):321–333. doi:10.1093/humupd/dmn008
5. Fiedler K, Ezcurra D. Predicting and preventing ovarian hyperstimulation syndrome (OHSS): the need for individualized not standardized treatment. Reprod Biol Endocrinol. 2012;10:32. doi:10.1186/1477-7827-10-32
6. Ioannidou PG, Bosdou JK, Lainas GT, Lainas TG, Grimbizis GF, Kolibianakis EM. How frequent is severe ovarian hyperstimulation syndrome after GnRH agonist triggering in high-risk women? A systematic review and meta-analysis. Reprod Biomed Online. 2020;42:635–650. doi:10.1016/j.rbmo.2020.11.008
7. Kalinderis M, Kalinderi K, Srivastava G, Homburg R. When should we freeze embryos? Current data for fresh and frozen embryo replacement IVF cycles. Reprod Sci. 2021;28:3061–3072. doi:10.1007/s43032-021-00628-w
8. D’Angelo A, Amso NN, Hassan R. Coasting (withholding gonadotrophins) for preventing ovarian hyperstimulation syndrome. Cochrane Database Syst Rev. 2017;5:CD002811. doi:10.1002/14651858.CD002811.pub4
9. Moll E, van der Veen F, van Wely M. The role of metformin in polycystic ovary syndrome: a systematic review. Hum Reprod Update. 2007;13(6):527–537. doi:10.1093/humupd/dmm026
10. Tang H, Mourad S, Zhai SD, Hart RJ. Dopamine agonists for preventing ovarian hyperstimulation syndrome. Cochrane Database Syst Rev. 2016;11:CD008605. doi:10.1002/14651858.CD008605.pub3
11. Atilgan R, Pala S, Yavuzkir S, Baspinar M, Yilmaz M, Ilhan N. What is the impact of short- and long-term supplementation of either cabergoline or clarithromycin on resolving rat ovarian hyperstimulation syndrome (OHSS) model? J Obstet Gynaecol. 2019;39(5):687–694. doi:10.1080/01443615.2018.1563774
12. Hortu I, Karadadas E, Ozceltik G, et al. Oxytocin and cabergoline alleviate ovarian hyperstimulation syndrome (OHSS) by suppressing vascular endothelial growth factor (VEGF) in an experimental model. Arch Gynecol Obstet. 2021;303(4):1099–1108. doi:10.1007/s00404-020-05855-1
13. Al-Inany HG. Human albumin is effective in prevention of severe OHSS. Acta Obstet Gynecol Scand. 2001;80(10):878–882. doi:10.1080/791200640
14. Delvigne A, Rozenberg S. Review of clinical course and treatment of ovarian hyperstimulation syndrome (OHSS). Hum Reprod Update. 2003;9(1):77–96. doi:10.1093/humupd/dmg005
15. Aboulghar M. Prediction of ovarian hyperstimulation syndrome (OHSS). Estradiol level has an important role in the prediction of OHSS. Hum Reprod. 2003;18(6):1140–1141. doi:10.1093/humrep/deg208
16. Alper MM, Smith LP, Sills ES. Ovarian hyperstimulation syndrome: current views on pathophysiology, risk factors, prevention, and management. J Exp Clin Assist Reprod. 2009;6:3.
17. Rizk B, Aboulghar M, Smitz J, Ron-El R. The role of vascular endothelial growth factor and interleukins in the pathogenesis of severe ovarian hyperstimulation syndrome. Hum Reprod Update. 1997;3(3):255–266. doi:10.1093/humupd/3.3.255
18. McClure N, Healy DL, Rogers PA, et al. Vascular endothelial growth factor as capillary permeability agent in ovarian hyperstimulation syndrome. Lancet. 1994;344(8917):235–236. doi:10.1016/S0140-6736(94)93001-5
19. Fang L, Li Y, Wang S, et al. TGF-beta1 induces VEGF expression in human granulosa-lutein cells: a potential mechanism for the pathogenesis of ovarian hyperstimulation syndrome. Exp Mol Med. 2020;52(3):450–460. doi:10.1038/s12276-020-0396-y
20. Evbuomwan IO, Davison JM, Baylis PH, Murdoch AP. Altered osmotic thresholds for arginine vasopressin secretion and thirst during superovulation and in the ovarian hyperstimulation syndrome (OHSS): relevance to the pathophysiology of OHSS. Fertil Steril. 2001;75(5):933–941. doi:10.1016/S0015-0282(01)01704-6
21. Zhai J, Liu J, Zhao S, et al. Kisspeptin-10 inhibits OHSS by suppressing VEGF secretion. Reproduction. 2017;154(4):355–362. doi:10.1530/REP-17-0268
22. Cenksoy C, Cenksoy PO, Erdem O, Sancak B, Gursoy R. A potential novel strategy, inhibition of vasopressin-induced VEGF secretion by relcovaptan, for decreasing the incidence of ovarian hyperstimulation syndrome in the hyperstimulated rat model. Eur J Obstet Gynecol Reprod Biol. 2014;174:86–90. doi:10.1016/j.ejogrb.2013.12.001
23. Gomez R, Simon C, Remohi J, Pellicer A. Vascular endothelial growth factor receptor-2 activation induces vascular permeability in hyperstimulated rats, and this effect is prevented by receptor blockade. Endocrinology. 2002;143(11):4339–4348. doi:10.1210/en.2002-220204
24. Heymach JV, Desai J, Manola J, et al. Phase II study of the antiangiogenic agent SU5416 in patients with advanced soft tissue sarcomas. Clin Cancer Res. 2004;10(17):5732–5740. doi:10.1158/1078-0432.CCR-04-0157
25. Hoff PM, Wolff RA, Bogaard K, Waldrum S, Abbruzzese JL. A phase I study of escalating doses of the tyrosine kinase inhibitor semaxanib (SU5416) in combination with irinotecan in patients with advanced colorectal carcinoma. Jpn J Clin Oncol. 2006;36(2):100–103. doi:10.1093/jjco/hyi229
26. Wollin L, Wex E, Pautsch A, et al. Mode of action of nintedanib in the treatment of idiopathic pulmonary fibrosis. Eur Respir J. 2015;45(5):1434–1445. doi:10.1183/09031936.00174914
27. Wollin L, Distler JHW, Redente EF, et al. Potential of nintedanib in treatment of progressive fibrosing interstitial lung diseases. Eur Respir J. 2019;54(3):1900161. doi:10.1183/13993003.00161-2019
28. Shiratori T, Tanaka H, Tabe C, et al. Effect of nintedanib on non-small cell lung cancer in a patient with idiopathic pulmonary fibrosis: a case report and literature review. Thorac Cancer. 2020;11(6):1720–1723. doi:10.1111/1759-7714.13437
29. Lamb YN. Nintedanib: a review in fibrotic interstitial lung diseases. Drugs. 2021;81(5):575–586. doi:10.1007/s40265-021-01487-0
30. Watson N, Al-Samkari H. Thrombotic and bleeding risk of angiogenesis inhibitors in patients with and without malignancy. J Thromb Haemost. 2021;19(8):1852–1863. doi:10.1111/jth.15354
31. Liu B, Ding F, Zhang D, Wei GH. Risk of venous and arterial thromboembolic events associated with VEGFR-TKIs: a meta-analysis. Cancer Chemother Pharmacol. 2017;80(3):487–495. doi:10.1007/s00280-017-3386-6
32. Totzeck M, Mincu RI, Mrotzek S, Schadendorf D, Rassaf T. Cardiovascular diseases in patients receiving small molecules with anti-vascular endothelial growth factor activity: a meta-analysis of approximately 29,000 cancer patients. Eur J Prev Cardiol. 2018;25(5):482–494. doi:10.1177/2047487318755193
33. Wei LH, Chou CH, Chen MW, et al. The role of IL-6 trans-signaling in vascular leakage: implications for ovarian hyperstimulation syndrome in a murine model. J Clin Endocrinol Metab. 2013;98(3):E472–E484. doi:10.1210/jc.2012-3462
34. Fainaru O, Hornstein MD, Folkman J. Doxycycline inhibits vascular leakage and prevents ovarian hyperstimulation syndrome in a murine model. Fertil Steril. 2009;92(5):1701–1705. doi:10.1016/j.fertnstert.2008.08.129
35. Goddard LM, Murphy TJ, Org T, et al. Progesterone receptor in the vascular endothelium triggers physiological uterine permeability preimplantation. Cell. 2014;156(3):549–562. doi:10.1016/j.cell.2013.12.025
36. Pala S, Atilgan R, Ozkan ZS, et al. Effect of varying doses of tamoxifen on ovarian histopathology, serum VEGF, and endothelin 1 levels in ovarian hyperstimulation syndrome: an experimental study. Drug Des Devel Ther. 2015;9:1761–1766. doi:10.2147/DDDT.S75266
37. Kamba T, McDonald DM. Mechanisms of adverse effects of anti-VEGF therapy for cancer. Br J Cancer. 2007;96(12):1788–1795. doi:10.1038/sj.bjc.6603813
 © 2022 The Author(s). This work is published and licensed by Dove Medical Press Limited. The
full terms of this license are available at https://www.dovepress.com/terms.php
and incorporate the Creative Commons Attribution
- Non Commercial (unported, v3.0) License.
By accessing the work you hereby accept the Terms. Non-commercial uses of the work are permitted
without any further permission from Dove Medical Press Limited, provided the work is properly
attributed. For permission for commercial use of this work, please see paragraphs 4.2 and 5 of our Terms.
© 2022 The Author(s). This work is published and licensed by Dove Medical Press Limited. The
full terms of this license are available at https://www.dovepress.com/terms.php
and incorporate the Creative Commons Attribution
- Non Commercial (unported, v3.0) License.
By accessing the work you hereby accept the Terms. Non-commercial uses of the work are permitted
without any further permission from Dove Medical Press Limited, provided the work is properly
attributed. For permission for commercial use of this work, please see paragraphs 4.2 and 5 of our Terms.