Back to Journals » Advances in Medical Education and Practice » Volume 8
Innovative curriculum for second-year Harvard-MIT medical students: practicing communication skills with volunteer patients giving immediate feedback
Authors Ali NB, Pelletier SR, Shields HM
Received 20 February 2017
Accepted for publication 20 April 2017
Published 19 May 2017 Volume 2017:8 Pages 337—345
DOI https://doi.org/10.2147/AMEP.S135172
Checked for plagiarism Yes
Review by Single anonymous peer review
Peer reviewer comments 4
Editor who approved publication: Dr Md Anwarul Azim Majumder
Nadaa B Ali,1 Stephen R Pelletier,2 Helen M Shields1
1Department of Medicine, Brigham and Women’s Hospital, 2Center for Evaluation, Harvard Medical School, Boston, MA, USA
Purpose: Medical students are expected to develop excellent communication skills. The purpose of our study was to create an innovative communication skills exercise using real volunteer patients and physician co-teachers for students to practice communication skills while receiving immediate feedback.
Method: This is a mixed methods study where second-year medical students participated in the communication skills exercise with real patients and physician co-teachers giving immediate feedback. Clinical scenarios reflected the patients’ actual experiences. Students acted out roles as physicians. Physicians co-taught with the patients and gave immediate feedback to students. Students completed an anonymous written survey at the end of the exercise. Qualitative and quantitative responses were recorded. Student feedback from the 2014 surveys was used to modify the teaching designs to increase active role play opportunities by having only two students in each group and doubling the number of stations with real patients.
Results: Students rated the overall exercise and the utility of patient volunteers in learning how to communicate on a Likert scale of 1–5, where in this medical school traditionally 1 is excellent and 5 is poor. In 2014, the exercises were rated with a mean score of 1.47 (SD 0.621). In 2015, the exercises were rated with a mean score of 1.03 (SD 0.62). In 2016, the exercises were rated with a mean score of 1.27 (SD 0.52). ANOVA analysis (p=0.002) and Bonferroni corrections indicate a statistically significant difference between combined mean scores of the exercise in 2014 and 2015 (p=0.001). No difference was shown between 2014 and 2016 or 2015 and 2016.
Conclusions: Medical students rated practicing communication skills with real patient volunteers and physician co-teachers giving immediate feedback in their preclinical years very highly. Student feedback indicated that they preferred active roles and increased opportunities to practice their communication skills.
Keywords: communication skills, real volunteer patients, immediate feedback, medical students, innovative curriculum, undergraduate medical education
Introduction
Excellent communication skills are required to provide high-quality, patient-centered care.1 Historically, the focus in medical training has been on acquiring knowledge and mastering practical skills. Less attention has been focused on developing the humanistic side of physicians.2 However, studies have shown that good communication between physicians and patients can increase patient satisfaction, medication adherence, and health-related outcomes.3–8 Patients are less likely to sue physicians who spend more time talking to them.9 Due to the Affordable Care Act, reimbursements are also becoming increasingly linked to healthcare outcomes, rather than fee for service.10
The specific aims for this communication skills exercise were to 1) provide preclinical medical students early opportunities to practice their communication skills with volunteer patients and physician co-teachers, 2) receive immediate feedback from patients and physicians on verbal and nonverbal communication skills, 3) expose students to different communication styles, and 4) recognize effective strategies for difficult conversations.
This study investigates the utility and value of practicing communication skills with real patient volunteers and physician co-teachers by medical students in the preclinical years.
Methods
The communications skills exercise was created for second-year Harvard-Massachusetts Institute of Technology (MIT) Health Sciences and Technology (HST) students in the MD program as part of the Introduction to Clinical Medicine (ICM) HST 200 Course. This is a mixed methods study; students gave both qualitative and quantitative feedback. Many of the HST students have a background in engineering and basic science and will pursue both a PhD and an MD. They are required to complete the 4-month long ICM course prior to beginning their third-year medical clerkships.
This research was reviewed and deemed exempt by the Harvard Faculty of Medicine Institutional Review Board Office, IRB16-1934, under the regulations of HHS.gov 45 CFR 46.101 (b) (1) and (2). Participation was voluntary, and the board did not require that written informed consent be obtained.
Volunteer patients were recruited to teach communication skills from the Brigham and Women’s Hospital Volunteer Patient Teaching Corps.11 Clinical scenarios were customized with each patient’s feedback to reflect the patient’s actual medical experience. Scenarios ranged from delivering difficult news, goals of care discussions, medical mistakes, organ donation to a close relative, and communicating with a frustrated family member of an elderly patient with a massive hemorrhagic stroke (see Box 1 for a case example).
  | Box 1 Case example. |
Faculty and resident physicians were invited to co-teach the communication skills exercise with the volunteer patients. A mandatory 1-hour faculty development session was required for physicians. Patients were met individually to review the logistics and timing of the exercise and their individual scenarios. In addition, both patients and physician co-teachers were trained to give students immediate feedback on communication skills.
Patients and physician co-teachers met for 30 minutes prior to each exercise to become acquainted with each other and agree upon the unique teaching points from his or her case. Patients were reimbursed for parking at the hospital or given free parking at the medical school garage. Patients and physician co-teachers were provided with water and light snacks during the exercise but did not otherwise receive monetary compensation for face-to-face teaching time.
The exercise was held in a medical school clinical skills area that had ambulatory patient clinic rooms with examining tables, sinks, rolling chairs, and patient chairs. Prior to beginning the exercise, students were emailed a brief description of the exercise including the learning objectives, goals, and lesson plan (Table 1). At the beginning of the exercise, the students were welcomed and given instructions. Goals and objectives were reviewed. Students were reminded that the goal was to practice their communication skills.
  | Table 1 Communication skills exercise: objectives and goals for second year medical students |
In 2014, a total of 32 HST students were randomly divided into two groups. Group A participated in the 90-minute exercise near the end of the ICM course in week 11; and Group B participated in week 12. Each group was further divided into teams of four students. After a brief orientation to the exercise, students rotated through four clinical scenarios, lasting 18 minutes each. The clinical scenario was taped to the door for the students to read prior to entering the room and also available on a clip board for reference during the role play. In 2014, week 11 Group A, we assigned each of the four students to one of the following roles: doctor 1, doctor 2, time keeper, and scribe. Doctors 1 and 2 each had 5 minutes to role play, followed by 8 minutes for debriefing and feedback.
In 2014, after anonymous student feedback from the 16 students in Group A, the exercise was modified to give each of the 16 students in Group B in week 12 an active role in the exercise. The passive roles of timekeeper and scribe were deleted. In each team of four students in Group B, students 3 and 4 were made consultants who could be called on by their peers for advice. Similar to Group A, students in Group B role-played the part of the doctor, patients gave direct feedback on communication skills, and physician teachers supplemented observations and gave recommendations on strategies for communication. Before moving on to the next case, the student team identified one key take home point from the discussion.
In 2015, the ICM program leadership moved the exercise to earlier in the ICM course based on students’ request for an earlier time in the ICM course; course directors increased the time for the exercise from 90 to 150 minutes based on student feedback. A total of 30 HST students were randomly divided into two groups of 15 and 15 students. They participated in the exercise in weeks 4 and 5 of the ICM course. Each group was divided into teams of two students. The number of cases was doubled based on student feedback requesting increased opportunities to practice communication skills. In 2015, students rotated through eight clinical scenarios, lasting 15 minutes each. Both students had 5 minutes to role play followed by a 5-minute discussion with the patient and physician co-teachers giving immediate feedback and advice on communication skills.
In 2016, 30 students (two groups of 14 and 16 students) participated in the exercise. Based on student feedback from 2015, course directors further expanded the time for the exercise to 180 minutes, with 5 minutes for introduction and 15 minutes for conclusion. The exercise occurred during weeks 4 and 9 of the 2016 ICM course due to a snow storm delaying week 5’s exercise. Students were given 4 minutes each to role play in seven total cases. The debriefing time for each case was increased to 6 minutes.
At the end of each exercise, students were asked to complete an anonymous paper evaluation. Participation was voluntary. Informed consent was not required. The survey asked each student to rate the overall exercise and the usefulness of real patient volunteers giving immediate feedback on communication skills. The scoring system was based on a Likert scale of 1–5, with 1 being excellent and 5 being poor. This Likert scale is the traditional one for this medical school; lower numbers indicate a better evaluation. In one case, the accuracy of the scored evaluation form given to the statistician was questioned by the authors. In this case in 2014, the student’s verbatim comment was that the exercise was “excellent” but gave it a numerical score of 5 or poor. It was thought to be an inadvertent scoring error on the part of the student whose comments reflected an excellent rating of 1. This score was changed by NBA and HMS with the approval of the statistician SRP. In 2015, one student only answered the first question about the overall rating of the exercise but did not rate the utility of the patients. The data set reflects this missing piece of data from 2015.
At the end of the anonymous paper survey, students were invited to write three things that they liked best about the exercise along with three things that they would like to change.
After surveys were completed and turned face down, students participated in a collective reflection with the patients and physician co-teachers. Students shared their take home points and identified important and effective communication skills. They learned more about each patient and the patient’s motivation for teaching medical students. The collective debriefing was not recorded, transcribed, or analyzed.
Results
Faculty and patient co-teacher characteristics
In 2014, there were four patients and four physicians (one faculty and three residents) in each exercise. Patients’ ages ranged from 35 to 80 years old with two women and two men. In 2015, there were eight patients, ranging from 48 to 85 years old. Group A in week 11 had six women and two men; and Group B in week 12 had five women and three men. Eight physicians (two faculty and six residents) participated in each exercise. In 2016, there were eight patients; ages ranged from 22 to 83 years old with six women and two men in each exercise. Eight physicians (four faculty and four residents) participated in each exercise.
Anonymous survey results
In 2014 (n=32), 2015 (n=30), and 2016 (n=30), all of the students (n=92) completed an anonymous paper survey at the end of each exercise before engaging in a collective reflection. The survey asked each student to rate the overall exercise and the usefulness of real patient volunteers giving immediate feedback on communication skills.
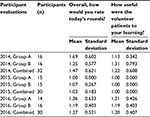
Students rated the overall exercise and the utility of patient volunteers on a Likert scale of 1–5, with 1 being excellent (Table 2). In 2014, Group A rated the overall exercise with a mean score of 1.69±0.602 SD. After the roles of time keeper and scribe were eliminated, the students in Group B rated the overall exercise with a mean score of 1.25±0.577 SD. In 2014, the two exercises combined were rated with a mean score of 1.47±0.621 SD. The utility of patient volunteers in 2014 received a mean score of 1.13±0.342 SD by Group A and 1.31±0.793 SD by Group B; the combined mean score for the utility of the patients was 1.22±0.608 SD.
In 2015, the students actively participated in each case in teams of two rather than four, and the number of cases was doubled. The two exercises combined were rated with a mean score of 1.03±0.62 SD with Group A rating the exercise with a mean score of 1.00±0.000 SD and Group B with a score of 1.07±0.267 SD. The 2015 combined score for the utility of patient volunteers was 1.00±0.000 SD.
In 2016, the length of the exercise was further increased with more time allotted for debriefing in small groups. The exercise was rated with a mean score of 1.36±0.633 SD by Group A and 1.19±0.403 SD by Group B; the combined mean score for the exercise was 1.27±0.521. The utility of patient volunteers received a mean score of 1.21±0.426 SD by Group A and 1.19±0.403 SD by Group B; the 2016 combined score for the overall utility of patient volunteers was 1.20±0.407 SD.
Parametric tests such as one-way analysis of variance and Bonferroni corrections were used to analyze the Likert scale responses. However, due to the limited value of means to describe ordinal data, frequency distributions of responses are included in Table 3.12,13
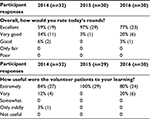  | Table 3 Communication skills exercise: distribution of responses |
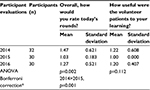
In Table 4, ANOVA analysis (p=0.002) and Bonferroni corrections indicate a statistically significant difference between the combined mean scores of the exercise between 2014 and 2015 (p=0.001), but no significant difference between 2014 and 2016 or 2015 and 2016. There was no statistically significant difference in the mean scores for the utility of patient volunteers. To determine if the class of 2015 graded courses more favorably compared to the classes of 2014 and 2016, all HST course grades from the classes of 2014, 2015 and 2016 were evaluated. The class of 2015 did not stand out as “unique” in its grading characteristics after careful review.
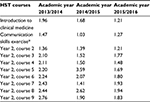
The overall ICM course was rated excellent to very good from 2014 to 2016 (Table 5). Compared with the other second-year courses for HST students at Harvard Medical School, the ICM course is rated very highly. Within this course, the communication skills exercise was rated as excellent.
Representative, verbatim, and anonymous student comments are listed below
What did you like best about today’s session?
2014
Real patients, great cases, felt real
Quick, rapid feedback, many interactions
Real patients, as opposed to role play/actors
Practice with difficult but common situations, small group setting for both participation and observation, having take home points
Have actual patients with real stories to talk about, dealing with difficult situations that we don’t often talk about, having immediate feedback
Very different experience, very real experiences, very positive and helpful feedback, good amount of timing
Diversity of patients’ experience; focus on communication, not diagnosis; preceptors taking care of patient and discussed how they actually handled the situation
Immediate feedback from physician, class, patient; real patients; HST has very little discussion regarding these types of issues, so this session was fantastic
Great
Real cases, timed interactions, supervised by doctors
The patients, summarizing take home points with preceptor and patients, getting to do many roles
Talking to patients in different situations; role playing different situations
The patient’s advice was wonderful
Real patients, not models
Scenarios were real-life, patient experiences; group size; variety of scenarios and roles
I love the feedback at the end
Good feedback from colleagues, preceptors, and especially patients
2015
Feedback from patients was super helpful
Immediate feedback, high stress scenarios are good to practice, very friendly patients
I was able to receive very useful critique about my communication skills which will help me tremendously to improve
Actual practice talking to real patients, real-time feedback, focus more on the art than the science
Real patients with their actual conditions; getting feedback from patients
Time for feedback, directly from patients; having to synthesize 1 take away point from each situation; variety in scenarios
Immediate feedback; incredible patients who were able to teach us so much
Hands on interaction; honest and immediate feedback
2016
Having real patients share their stories; having a physician in the room; having two back to back sessions
Doctors providing constructive feedback
Patients telling their own story is a wonderful way to have genuine feeling
The take home points sheet! I now have concrete, personal things to improve
These were real patients telling their own real stories. Great learning too!
Doing it in pairs. Seeing a partner and doing it myself improved what I learned
Patients gave clear and honest feedback
Even in similar types of situations (examples, medical mistakes), patients reacted so differently
Would you change anything about today’s session?
2014
Nothing
Let’s do this more often; the best preceptors solicited feedback from everyone in the group – was helpful to hear everyone
Decide whether we should do small talk before conversation. It was common feedback but didn’t feel feasible in 5 minutes.
More elaboration about role play setting
Not so much of a time constraint – really quick to talk about some issues
More of these sessions – one is not enough
Follow-up session is probably not necessary; scribe is not necessary
More time; 3–5 minutes was not enough – maybe do a full day or half-day session
More time per patient
More time
More stations; such a great exercise – we should do more!
Make it longer; have all of us participate with every patient (go twice)
Smaller groups would make more productive/negative feedback easier
Doing the exercise in partners was great; I learned a lot by watching
2015
More time would be helpful, even if it meant less patients
More stressful scenarios – death/terminal diagnosis; more hostile/unfriendly patients to practice that in a controlled environment
Perhaps, a great diversity of patients; the two cancer cases were somewhat similar.
Be more critical; we can handle it
More time to get advice from clinicians
Have people change partners to see other people’s communication styles
Maybe slightly more time to debrief
More time in between to reflect and prepare
2016
Having more time to debrief; having more sessions like this regularly
Fewer cases before the final debrief
Giving a little more time to reflect at the very end
Fewer patients and more time
Put in some social and ethnically complicated issues (example, patients with sexist, racist views)
Perhaps reading cases before class would be helpful
Discussion
This study is the first to use real patients as volunteer co-teachers with physicians for medical students to practice communication skills during preclinical years in medical school. This curriculum creates an opportunity for students to engage with real patients in a memorable way because the cases used for training are based on the actual experiences of each patient.
Students rated real patient teachers and the overall exercise as highly useful and effective. Because the patients helped create the cases based on real-life experiences, the exercise was expected to be high yield. Students reported that they gained a tremendous amount from the exercise; they particularly enjoyed the real patients, immediate feedback, and multiple opportunities to practice. It is important that medical students practice communication skills as evidence shows that perceptions of good communication between patients and physicians improve patient satisfaction.3–8 In addition, patients want autonomy and a role in determination of their medical care; physicians need to be able to understand the goals and needs of patients.14,15
Prior studies showed that effective communication skills can be learned.16–20 For example, Roter et al21 analyzed audiotapes of physicians interacting with real and standardized patients after a communication skills training program. They found that trained physicians were more likely to use the behaviors taught and “scored higher on clinical proficiency with simulated patients.”21
In 1999, the Association of American Medical Colleges (AAMC) made effective communication with patients and families a major learning objective for medical schools.22 In 2001, the Institute of Medicine (IOM) issued the Crossing the Quality Chasm report that emphasized the importance of taking patient’s values and preferences into account to provide high quality, patient-centered care.23 Effective and collaborative communication skills increases patient satisfaction and improves health related outcomes.3–8
The American Academy on Physician and Patient’s Conference on Education and Evaluation of Competence in Communication and Interpersonal Skills issued the Kalamazoo II Report in 2002 that defined communication as “performance of specific tasks and behaviors such as obtaining a medical history, explaining a diagnosis and prognosis, giving therapeutic instructions, and counseling.”24
In an effort to improve communication training, residency and medical program leadership began sharing ideas and identifying ways to evaluate students prior to matriculation.24 Standardized patients, actors trained to assess certain physician skills, have become a common means of assessing skills in pre-clinical years. Standardized patients are able to reliably score physician skills with minimal variability between scores.25
In 2014, the AAMC released guidelines to evaluate students with qualitative feedback on observable, concrete skills (also known as entrustable professional activities [EPAs]) using longitudinal and repeated assessments.26 Many medical schools are reassessing curricula and adapting the EPA rubric. This communications exercise is one way in which medical schools may begin introducing students to real patients, giving them opportunities for communication skills’ development, providing repetitive and longitudinal qualitative feedback, and assessing students’ preparedness for residency.
In this study, real patients were the most highly rated part of the exercise. The overall quality of the exercise improved with feedback and immediate implementation of changes. For example, in 2014 Group A, each student had an opportunity to actively communicate in only 50% of the clinical scenarios. In Group A, in the 2014 exercises, the students were in teams of four, with only two students taking an active role. The other two students were asked to keep time and/or act as a scribe. Immediate student feedback indicated that students preferred the active doctor roles throughout the exercise. Given that feedback, the exercise design was immediately revised to give every student an active role at every station. In Group B of 2014, two students acted as doctors, while the other two students played the roles of consultants and gave feedback to the student doctors. In 2015 and 2016, based on qualitative student feedback, the number of clinical scenarios was doubled, and each student had an opportunity to actively communicate in 100% of the clinical scenarios. The overall rating of the exercise improved significantly from 2014 to 2015.
The exercise was purposely not graded to allow students to take risks and try different communication styles. Students received immediate verbal feedback from the patient and physician co-teachers; the goal of the feedback was to enhance personal growth and verbal and nonverbal communication behaviors. Because the patients and scenarios were real, this exercise was a high yield activity that allowed students to practice communication skills and connect with patients. Themes from cases were repeated more than once (e.g., two patients who experienced medical mistakes and two patients who had to receive news about a serious diagnosis participated). Repetition and immediate feedback gave students the opportunity to improve during the exercise.
The strengths of the study are three years of evaluations with almost total capture of the anonymous medical student responses, the uniformly high scores for the utility of volunteer patients in the exercise, and the willingness of all the patients to return to teach communication skills to the students.
Limitations of the study include the absence of both objective data (clerkship evaluations) and subjective data (graduation questionnaire) showing improvement in communication skills during the clinical years. It is unknown whether increased practice in this exercise will result in a lasting impact on communication skills throughout the clinical years. An additional limitation is that patients and physician co-teachers were not surveyed. Therefore, the study reflects the unilateral perspective of the medical students. Next steps include performing outcomes research on the medical students during clinical years to show whether this communication skills exercise in the preclinical years has an impact on their clinical performance and communication skills with actual patients in the hospital. In the future, graduation questionnaires will be analyzed for students’ perception of the quality of communication skills training during preclinical medical school training.
Ventres and Frankel defined the connection between physicians and patients as “shared presence” or “a trust that facilitates healing.”27 In this exercise, students have the opportunity to hear the patient narrative and actively connect with patients on a deeper level. Experiential learning is one way to increase empathy and improve patient–doctor communication.28
Volunteer patients were introduced to the Brigham and Women’s Hospital in 2013 and began co-teaching with physicians in 2014.11 This exercise demonstrates a valuable role for real patients to teach medical students during the formative preclinical years.
Conclusions
Excellent communication between patients and physicians is needed to deliver patient-centered care and improve patient satisfaction.5,15 As the educational paradigm shifts to assessing students based on observable skills longitudinally, medical schools will need more opportunities for students to practice communication skills and receive immediate feedback.26 In this study, medical students highly rated practicing communication skills with real patient volunteers in the preclinical years.>
Acknowledgements
We thank Wolfram Goessling, MD, PhD, Director of Harvard-MIT Health Sciences and Technology Program at HMS; Program Coordinators Lindsay Clinton, Patricia Cunningham, and Rachel Lucier for their encouragement and expert support. We are deeply grateful to the following Patient and Physician co-teachers: Christine J. Chung, MD; Hamed Nayeb-Hashemi, MD; Derek Monette, MD; Doris Bunte; Theresa Fay; Jason Figueiredo; Deborah Murray; Kenneth Murray; Louise Quynn; Brian Weir; Edward Barnes, MD, MPH; Jennifer Nayor, MD; Alison Goldin, MD, MPH; Kevin Sullivan, MD; Joseph Feuerstein, MD; Alison Schulman, MD; Sarah Post, MD; Viswatej Avutu, MD; Joanne Goldstein, JD; William Gladue; Gail Tsimprea, PhD; Norton Fishman, DMD; Menno Verhave, MD; Julia Blum Caton, MD; Martha Jurchak, RN, PhD; Vatche Tchekmedyian, MD, MEd; Elihu Schimmel, MD; Edith Schimmel; Carol Fishman; Luke Johnson; Margaret Merrill; and Nan Lin for their outstanding commitment to medical education.
The Harvard-MIT Health Sciences and Technology Program at HMS and Brigham and Women’s Division of Medical Communications provided water bottles and parking for the patients and physicians.
The initial data from this study were presented as a poster at Harvard Medical School’s Medical Education Day,29 and as an oral presentation at the 2015 Regional Society for General Internal Medicine Meeting.30
Author contributions
Dr. NB Ali and Dr. HM Shields designed the study and communication skills exercise. They recruited patients and physician teachers, wrote the cases, with each patient editing his/hers, and held faculty development sessions in addition to teaching in the exercises. Dr. SR Pelletier performed the statistical analysis. All three authors were heavily involved in writing this manuscript. All authors gave final approval of the version to be published, and agree to be accountable for all aspects of the work
Disclosure
The authors report no conflicts of interest in this work.
References
Epstein RM, Franks P, Fiscella K, et al. Measuring patient-centered communication in patient-physician consultations: theoretical and practical issues. Soc Sci Med. 2005;61(7):1516–1528. | ||
Novack DH, Epstein RM, Paulsen RH. Toward creating physician-healers: fostering medical students’ self-awareness, personal growth, and well-being. Acad Med. 1999;74(5):516–520. | ||
Schoenthaler A, Chaplin WF, Allegrante JP, et al. Provider communication effects (sic) medication adherence in hypertensive African Americans. Patient Educ Couns. 2009;75(2):185–191. | ||
Schoenthaler AM, Schwartz BS, Wood C, Stewart WF. Patient and physician factors associated with adherence to diabetes medications. Diabetes Educ. 2012;38(3):397–408. | ||
Heisler M, Bouknight RR, Hayward RA, Smith DM, Kerr EA. The relative importance of physician communication, participatory decision making, and patient understanding in diabetes self-management. J Gen Intern Med. 2002;17(4):243–252. | ||
Kafetsios K, Anagnostopoulos F, Lempesis E, Valindra A. Doctors’ emotion regulation and patient satisfaction: a social-functional perspective. Health Commun. 2014;29(2):205–214. | ||
Bredart A, Bouleuc C, Dolbeault S. Doctor-patient communication and satisfaction with care in oncology. Curr Opin Oncol. 2005;17(4):351–354. | ||
Al Shahrani A, Baraja M. Patient satisfaction and it’s (sic) relation to diabetic control in a primary care setting. J Family Med Prim Care. 2014;3(1):5–11. | ||
Levinson W, Roter DL, Mullooly JP, Dull VT, Frankel RM. Physician-patient communication. The relationship with malpractice claims among primary care physicians and surgeons. JAMA. 1997;277(7):553–559. | ||
Levinson W, Lesser CS, Epstein RM. Developing physician communication skills for patient-centered care. Health Aff (Millwood). 2010;29(7):1310–1318. | ||
Drazen JM, Shields HM, Loscalzo J. A division of medical communications in an academic medical center’s department of medicine. Acad Med. 2014;89(12):1623–1629. | ||
Sullivan GM, Artino AR Jr. Analyzing and interpreting data from Likert-type scales. J Grad Med Educ. 2013;5(4):541–542. | ||
Norman G. Likert scales, levels of measurement and the “laws” of statistics. Adv Health Sci Educ Theory Pract. 2010;15(5):625–632. | ||
Carman KL, Maurer M, Mangrum R, et al. Understanding an informed public’s views on the role of evidence in making health care decisions. Health Aff (Millwood). 2016;35(4):566–574.. | ||
Look Through Patients’ Eyes to Improve the Delivery of Care. Hosp Case Manag. 2016;24(7):94, 99. | ||
Bachmann C, Barzel A, Roschlaub S, Ehrhardt M, Scherer M. Can a brief two-hour interdisciplinary communication skills training be successful in undergraduate medical education? Patient Educ Couns. 2013;93(2):298–305. | ||
Moore PM, Rivera Mercado S, Grez Artigues M, Lawrie TA. Communication skills training for healthcare professionals working with people who have cancer. Cochrane Database Syst Rev. 2013(3):CD003751. | ||
Joyce BL, Scher E, Steenbergh T, Voutt-Goos MJ. Development of an institutional resident curriculum in communication skills. J Grad Med Educ. 2011;3(4):524–528. | ||
Yedidia MJ, Gillespie CC, Kachur E, et al. Effect of communications training on medical student performance. JAMA. 2003;290(9):1157–1165. | ||
Cinar O, Ak M, Sutcigil L, et al. Communication skills training for emergency medicine residents. Eur J Emerg Med. 2012;19(1):9–13. | ||
Roter DL, Hall JA, Kern DE, Barker LR, Cole KA, Roca RP. Improving physicians’ interviewing skills and reducing patients’ emotional distress. A randomized clinical trial. Arch Intern Med. 1995;155(17):1877–1884. | ||
Association of American Medical Colleges. Medical School Objectives Project. Contemporary Issues in Medicine: Communication in Medicine. Washington DC: Association of American Medical Colleges; 1999. | ||
Institute of Medicine, Committee on Quality of Health Care in America. Crossing the Quality Chasm: A New Health System for the 21st Century. Washington DC: Institute of Medicine; 2001. | ||
Duffy FD, Gordon GH, Whelan G, et al. Assessing competence in communication and interpersonal skills: the Kalamazoo II report. Acad Med. 2004;79(6):495–507. | ||
Srinivasan M, Franks P, Meredith LS, Fiscella K, Epstein RM, Kravitz RL. Connoisseurs of care? Unannounced standardized patients’ ratings of physicians. Med Care. 2006;44(12):1092–1098. | ||
Brown DR, Warren JB, Hyderi A, et al. Finding a Path to Entrustment in Undergraduate Medical Education: A Progress Report From the AAMC Core Entrustable Professional Activities for Entering Residency Entrustment Concept Group. Acad Med. Available from: http://journals.lww.com/academicmedicine/Abstract/publishahead/Finding_a_Path_to_Entrustment_in_Undergraduate.98300.aspx. Accessed May 3, 2017. | ||
Ventres WB, Frankel RM. Shared presence in physician-patient communication: a graphic representation. Fam Syst Health. 2015;33(3):270–279. | ||
Klitzman R. Improving education on doctor-patient relationships and communication: lessons from doctors who become patients. Acad Med. 2006;81(5):447–453. | ||
Ali NB, Chung CJ, Nayeb-Hashemi H, Monette D, Pelletier SR, Shields HM. Innovative curriculum for second-year Harvard-MIT medical students: practicing communication skills with volunteer patients giving immediate feedback. Poster presentation at: Harvard Medical School’s Medical Education Day, October 28, 2014; Boston, MA, USA. | ||
Ali NB, Chung CJ, Nayeb-Hashemi H, Monette D, Pelletier SR, Shields HM. Innovative curriculum for second-year Harvard-MIT medical students: practicing communication skills with volunteer patients giving immediate feedback. Oral presentation at: 2015 Regional Society for General Internal Medicine Meeting, March 27, 2015; Boston, MA, USA. |
 © 2017 The Author(s). This work is published and licensed by Dove Medical Press Limited. The full terms of this license are available at https://www.dovepress.com/terms.php and incorporate the Creative Commons Attribution - Non Commercial (unported, v3.0) License.
By accessing the work you hereby accept the Terms. Non-commercial uses of the work are permitted without any further permission from Dove Medical Press Limited, provided the work is properly attributed. For permission for commercial use of this work, please see paragraphs 4.2 and 5 of our Terms.
© 2017 The Author(s). This work is published and licensed by Dove Medical Press Limited. The full terms of this license are available at https://www.dovepress.com/terms.php and incorporate the Creative Commons Attribution - Non Commercial (unported, v3.0) License.
By accessing the work you hereby accept the Terms. Non-commercial uses of the work are permitted without any further permission from Dove Medical Press Limited, provided the work is properly attributed. For permission for commercial use of this work, please see paragraphs 4.2 and 5 of our Terms.