Back to Journals » Cancer Management and Research » Volume 12
Central Venous Catheter Insertion in Colorectal Cancer Patients, PICC or PC?
Received 18 February 2020
Accepted for publication 22 June 2020
Published 14 July 2020 Volume 2020:12 Pages 5813—5818
DOI https://doi.org/10.2147/CMAR.S250410
Checked for plagiarism Yes
Review by Single anonymous peer review
Peer reviewer comments 2
Editor who approved publication: Professor Harikrishna Nakshatri
Lijuan Yin, Jinhua Li
Center of Oncology, Jiangsu Province Hospital, Nanjing, People’s Republic of China
Correspondence: Jinhua Li Email [email protected]
Purpose: Central venous catheters (CVCs) have been demonstrated as a feasible method for chemotherapy delivery in colorectal cancer patients. The objective of our study was to explore the preference of colorectal cancer patients (89%) in our institution for port catheters (PCs) through comparing the costs and complications between peripherally inserted central venous catheters (PICCs) and PCs.
Methods: Overall, 777 colorectal cancer patients (89%) were eligible for central venous catheter (CVC) insertions from January 1, 2017, to January 1, 2019. We retrospectively compared the costs and complications following the introduction of PICCs and PCs in the infusion of intravenous chemotherapy agents in patients with colorectal cancer.
Results: A total of 773 colorectal patients were enrolled. The total cost of PICC and PC was US $436.20 and US $976, respectively. The complication rate was higher in the PICC compared with the PC group (45% versus 4%, P < 0.001). The late complication rate of the two groups was particularly pronounced (52% versus 7%, p < 0.001). The incidence rate of total complications, that were developed in patients, with and without hemostatic prophylaxis, was 0.7% versus 5.7% (p < 0.001).
Conclusion: Port devices are associated with higher costs but fewer complications, compared to PICC in patients with colorectal cancer.
Keywords: central venous catheter, CVC, colorectal cancer, port catheter, PC, peripherally inserted central venous catheter, PICC, complication, cost
Introduction
Central venous catheters (CVCs) have become mandatory for the delivery of therapies in cancer patients. Chemotherapy of colorectal cancer (CRC) has significantly advanced with the development of FOLFOX (5-FU, oxaliplatin and leucovorin), FOLFIRI (irinotecan,5-FU and leucovorin), and the combination of oral anticancer agents, such as capecitabine. In the last 2 years, chemotherapy that was used to treat 874 colorectal cancer patients, who were hospitalized in our department. To reduce risks during chemotherapy, central venous catheters (CVCs) have been replaced by port catheters (PC) and peripherally inserted central catheters (PICC), which are convenient routes for chemotherapy administration.1 PICC usage shows the lowest procedure-related risk of severe adverse events (eg, hemothorax), because it can be inserted from the peripheral vein and without requiring surgical procedures. Moreover, it can be performed by trained nurses.2,3 On the other hand, PC has the advantage of inexistence of a visible external line, with no risk of pulling and impairment of patients’ quality of life. However, both types of catheters have limitations, including the high cost of invasive insertion, port removal and weekly maintenance. A fixed type of CVC for routine use in patients’ colorectal cancer therapies cannot be recommended without adequate evidence. Costs could also serve as an important factor in decision making. This secondary analysis mainly focused on investigating the complication rates, that were recorded within the 6-month period following catheters’ insertion, and the incidence rates of early and late complications. These were divided into early (<30 days) and late (>30 days) complications starting from the day of the first implantation.4 This study is one of the few reports that compared the estimated additional costs and complications of applying PICC and PC in drugs delivery to colorectal cancer patients in China, and that explored whether the 89% of the patients that used these delivery systems made the right choice.
Methods
Search Strategy
For this study, we considered colorectal patients who were hospitalized from January 1, 2017 to January 1, 2019, when a CVC was inserted. Comparisons of additional costs and related complications were made between colorectal patients with PCs and PICCs.
Detailed data on patients were collected by the principal investigator from all colorectal cancer patients’ medical records. The registered patient characteristics included age, gender, catheter type, vein choice, use of ultrasound, hemostatic and laboratory results, such as partial thromboplastin time (PTT), platelets’ count, use of Tranexamic acid, date of CVC insertion and removal, reason for CVC insertion and removal, and the incidence of complications related to CVC insertion and usage. Patients were fully informed on all potential issues associated with the use of PCs and PICCs, including information on the quality of life, costs and potential complications. The study was approved by Jiangsu Province People’s Hospital Ethical Committee. All enrolled patients were informed of the purpose of the study and signed informed consent forms were obtained.
Selection Criteria
Overall, 789 colorectal cancer patients were evaluated. Patients were excluded from the study if their platelet count was less than 20,000/mm, had an international normalized ratio (INR) that was higher than 2, or had sepsis, or severe behavioral problems, which would make CVC insertion more difficult. CVCs were maintained by experienced nursing staff, who changed the dressing at the insertion sites and the caps connected with the catheters. The PICC was flushed with a 10mL of 0.9% saline solution after administration of medication, followed by 5 mL heparinized saline solution (100IU/mL). When the PC was not in use, it was flushed with 5mL of heparinized saline (50IU/mL) every 4 weeks. CVCs care guidelines have been as congruent as possible in our institute. Chest radiography was used to ensure the correct location (the superior vena cava-right atrial junction) of the catheter tip.
Early complications included hemothorax, pneumothorax, excessive bleeding at the insertion site, accidental arterial puncture, cardiac arrhythmia, and pericardial and brachial plexus injuries.5 Late complications included catheter dysfunction, catheter-related blood stream infection (CRBSI), rupture, catheter allergy, extravasation, migration or embolization, drop out of the Huber needle, CVC-associated eczema, catheter-related thrombosis, local skin/tunnel infection, port inversion and “pinch-off” syndrome.6,7
The total cost included costs of catheters’ insertion, maintenance, and associated treatment complications. Medical costs over the 6-month period, that started from the day of catheters’ insertion, were recorded for each patient. Insertion costs also included costs of drugs, devices, and operational procedures. The charges for drugs and devices were based on manufacturers’ prices that were applied during the study. Operational costs were fixed by the National Administration for Commodity Prices. The maintenance costs were estimated based on the charges for CVCs’ connector changes, dressing and monthly flushing of the catheters. The costs of treatment complications were obtained through the analysis of related overall costs for each case. The costs associated with Maintenance and complications were calculated based on the CVC total usage time and all recorded complications. Cost estimates were converted from Chinese yuan to US dollars at a conversion rate of 7:1.
Statistical Analysis
Statistical variables were compared using the chi-squared test or Fisher’s exact test, while the Student’s t-test was used for comparing normally distributed parametric data and the Mann–Whitney U-test for non-parametric skewed data. A p-value of <0.05 was considered statistically significant. All analyses and figures were performed using the SPSS software version 21.0; SPSS Inc. (IBM Corp, Armonk, NY, USA).
Results
A total of 777 colorectal cancer patients were eligible for this study, which included 69 with PICC and 698 with PC. The basilica vein was used for PICC, and 4 PICCs were excluded due to 1 cephalic vein puncture and 3 brachial vein punctures (Table 1). The PICC and PC both used Brand silicon single-lumen catheters that were inserted with a modified Seldinger technique. All PICC lines were inserted using ultrasound guidance. The PC systems were inserted through the axillary vein without ultrasound guidance and fixed at the chest wall. In addition to the use of ultrasound, the laterality of CVC insertion is also shown in Table 1: 65% of PICCs in the left arm and 96% of PCs on the right side.
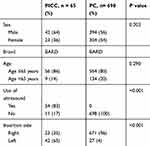 |
Table 1 Characteristics of Study Groups |
We analyzed the early and late complication rates during the 6-month period of catheter implantation. Our study did not take into account factors, such as the duration of chemotherapy cycles or patients’ death. The most common complications for patients with CVC include hematoma, arteriovenous fistula, arterial puncture, pneumothorax, and nerve injury. The cannulation success rate was 92~95% on the first pass.
Early complications occurred in 5 (7%) patients with PICCs and in 22 (3%) patients with PCs (p=0.377). In the PICC group, these complications included 2 cases of insertion site wound bleeding, 1 case of arterial puncture and 2 cases of ecchymoma. In the PC group, ecchymoma was observed in 15 patients, arterial puncture in 3 patients, and PC insertion site wound bleeding in 4 patients. Despite these complications, all cannulations were successfully completed. The late complication and total complication rates were higher in the PICC group compared to the PC group with 45% versus 4% (p < 0.001) and 52% versus 7%, respectively (p<0.001) (Table 2). Ruptures of the catheter devices occurred in 2 patients with PICCs and 3 clinically significant CRBSI were recorded, with 1 in the PICC group and 2 in the PC group, one of whom required a PC replacement and one PC case was kept with antibiotics treatment. A total of 3 patients (0.39%) underwent CVCs permanent removal due to complications. Two patients who received PICCs had complications that were due to CRBSI and occlusion, while the other patient with PC underwent premature PC removal due to CRBSI.
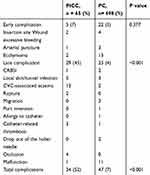 |
Table 2 Early and Late Complications Stratified by PICC and PC |
In contrast with other charges, the amount of medical expenses was variable and mainly dependent on the patient medical insurance (government and/or new rural medical insurance). In China, compensations for PICC insertion can be reimbursed up to 50% of the total incurred medical costs which depend on the type of medical insurance. However, the costs of PC insertion are excluded from insurance coverage. Patients who are implanted with PCs must pay for the total insertion costs. With a social medical insurance, the patient pays US $874 for a PC insertion and US $292.60 for a PICC insertion. The monthly compensation mean for the maintenance costs of PICC is US $60.4 versus US $30 for PC. The mean cost of treatment complications for PICC is US $78.3 versus US $48 for PC. The removal costs for PICCs and PCs are US $4.9 versus US $24, respectively, regardless of the type of medical insurance (Table 3).
 |
Table 3 Summary of Costs Calculated by PICC versus PC |
Discussion
Many cancer patients require CVCs for a safe and effective delivery of chemotherapeutic drugs. At our hospital, 2131 PICC and PC devices were placed in 3180 cancer patients over a two-year period, from 2017 to 2019. A total of 777 devices were inserted in 874 CRC patients. Metastatic and advanced CRCs are usually treated with continuous infusions of 5-FU using CVCs. Home chemotherapy has been carried out more often since the approval of FOLFIRI and FOLFOX. Consequently, complications involving CVCs and 5-FU pumps more frequent.8 In comparison to patients with PICC lines, those with PCs demonstrated lower incidence rates of overall complications (7% versus 52%, p < 0.001) and late complications (4% versus 45%, p<0.001). Among the late complications in the PICC group, the rate of CVC-associated eczema reached 45%. Most complications (85%) occurred outside the -hospital, due to incompliance with the nurses’ instructions. Only 15% of patients with CVC-associated eczema used dressing for sensitive skin, especially in summer. Unlike PICCs, PCs do not require dressing after needles’ extraction; thus, the incidence of CVC-associate eczema in the PC group is only 0.29%. Furthermore, additional hospital visits are required for patients with PICC as they require frequent dressing changes. PICC and PC insertion procedures were performed in a sterile room and by experienced clinicians who were trained and certified. When performed under strict sterile conditions and under radiological guidance, PICC insertions demonstrated higher insertion success rates and lower procedure related complications, especially with late complications, such as thrombosis or CRBSI. For convenience, 23 patients (35%) preferred the placement of PICCs in the upper left arm rather than the upper right arm. These were performed despite informing the patients that PICC insertions on the right have lower rates of related complications.9
As a common complication of CVCs, infection is the major cause of their removal.10 The results of our study (66%) were similar to the previous reports, where we found that 1.5% of PICCs’ implantations had CRBSI, which was slightly higher than the 1.1% CRBSI rate in previous studies.11 Therefore, we evaluated the economic and clinical impacts of catheter-related complications in China. As one of the most significant catheter-related complications, CRBSI is associated with high additional costs. The relationship between hospitalization costs and length was analyzed in previous studies.12–16 In this study, the cost of CRBSI treatments and the second replacements for PICC and PC were US $551.4 versus US $1346, respectively. Except for catheter removal, antibiotic therapy should be another option if the patient has no clinical signs of sepsis.
In some studies on CVCs, the symptomatic deep venous thrombosis rates were up to 9.3% in adults.17 In our study, 4 cases of catheter-related thrombosis were confirmed by doppler ultrasound connected with clinical symptoms of venous thrombosis which required anticoagulation treatment. All 3 (4.6%) cases of catheter-related thrombosis in patients with PICC were diagnosed as upper extremity deep venous thrombosis (UEDVT) by vascular ultrasound. It is worth mentioning that a study on PICCs implantation in tumor patients has shown that the incidence of UEDVT ranges from 4% to 50%.18,19 All twelve cases of CVCs’ malfunction did not render the line ineffective, such as the impossibility of injection and/or aspiration, but had made them difficult. According to the“Catheter Injection and Aspiration” (CINAS) classification scheme, we scored 6 2IN1ASI catheters’ malfunctions, 4 IN2ASI catheters’ malfunctions and 2 catheters with a IN2AS2 malfunction. CINAS is designed to describe the function of the catheter and to distinguish patients with good catheters’ function from the terms “injection” and “aspiration”.20
Another common complication was occlusion. One out of four cases of PICC occlusion was removed due to the failure of intravenous thrombolysis with urokinase, and that was removed under radiological guidance. Several studies confirmed that the occurrence rates of catheter malposition and re-implantation without ultrasound guidance were approximately 1.9–2.3%.21–24 Ideally, the tip of the catheter should terminate in the SVC upstream of the right atrium. In our study, only 2 cases in the PC group were mispositioned and the tip of the catheter was located in the right atrium, which showed adaptation to higher blood flow velocity, but was associated with a higher risk of cardiac complications such as cardiac tamponade and atrial thrombosis.25,26 Bleeding rates of 0.5–1.6% were shown to be associated with CVC insertion and tranexamic acid (TA) has been shown to clearly reduce excessive bleeding at the wound insertion site27,28 and the occurrence rate of hematoma and excessive bleeding from insertion site in the PC group (0.7% versus 4%, p=0.003) and (0 versus 1.3%, p=0.032). Although there are no definite conclusions in our study as to whether tranexamic acid will increase the risk of catheter-related thrombosis (p=0.426), Chornenki NLJ, Um KJ demonstrated that tranexamic acid does not increase the risk of thrombosis, and the occurrence of arterial thrombosis has been reduced since the introduction of TA.29,30 In our study, 401 patients with PC devices (57%), who accepted hemostatic prophylaxis, just after the insertion, had fewer complications compared to those without hemostatic prophylaxis (0.7% versus 5.7%, p < 0.001) (Table 4). During the period of our study, the mean of additional cost of hemostatic infusion was $4.6.
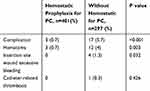 |
Table 4 All Complications Recorded for Patients Prescribing Hemostatic Prophylaxis or Not? |
In this study, we compared the relative cost-effectiveness of using PICCs and PCs. With the exception of the monthly mean of maintenance costs, the monthly mean of therapeutic complications costs, device insertion and removal, the overall cost for patients with a PCs were all higher compared to those of patients with PICCs. As the maintenance cost increased over time, the total cost of a PC will be lower than that of a PICC and without any insurance. However, the yearly overall cost of a PC is twice the cost of a PICC when compensation from medical insurance is considered.
There were some limitations, such as lifestyle issues relating to CVC that were not sufficiently explored in our study. We also aimed at ruling out all factors that may affect the incidence of complications, due to the retrospective nature of the study. For instance, random grouping may not be possible, which results in minor biases and requires additional studies.
Conclusion
In conclusion, PCs have greater costs than PICC, but have less complication rates, especially for patients with medical insurance. In our institution, 698 PCs were inserted in 777 colorectal cancer patients (89%). PCs increase convenience and lower complication rates suggest that these devices are safe tools for drugs delivery in colorectal cancer patients. This evidence may form a good basis for optimal CPs decisions.
Abbreviations
CVCs, central venous catheters; PICC, peripherally inserted central venous catheter; SVC, superior vena cava; PC, port catheter; CRC, chemotherapy for colorectal cancer; PTT, partial thromboplastin time; UEDVT, upper extremity deep venous thrombosis; INR, international normalized ratio.
Acknowledgments
The authors thank Ruixu and Juanwu, employees from Center of Oncology, Jiangsu Province Hospital, Nanjing, China.
Disclosure
The authors report no conflicts of interest in this work.
References
1. Lyon SM, Given M, Marshall NL. Interventional radiology in the provision and maintenance of long-term central venous access. J Med Imaging Radiat Oncol. 2008;52(1):10–17. doi:10.1111/j.1440-1673.2007.01904.x
2. Cotogni P, Pittiruti M. Focus on peripherally inserted central catheters in critically ill patients. World J Crit Care Med. 2014;3(4):80–94. doi:10.5492/wjccm.v3.i4.80
3. Mueller JT, Wright AJ, Fedraw LA, et al. Standardizing central line safety: lessons learned for physician leaders. Am J Med Qual. 2013;29:191–199. doi:10.1177/1062860613494752
4. Moureau N, Poole S, Murdock MA, et al. Central venous catheters in home infusion care: outcomes analysis in 50,470 patients. J Vasc Interv Radiol. 2002;13(10):1009–1016. doi:10.1016/S1051-0443(07)61865-X
5. Kurul S, Saip P, Aydin T. Totally implantable venous-access ports: local problems and extravasation injury. Lancet Oncol. 2002;3(11):684–692. doi:10.1016/S1470-2045(02)00905-1
6. Schulmeister L. Management of non-infectious central venous access device complications. Semin Oncol Nurs. 2010;26(2):132–141. doi:10.1016/j.soncn.2010.02.003
7. Jordan K, Behlendorf T, Surov A, et al. Venous access ports: frequency and management of complications in oncology patients. Onkologie. 2008;31(7):404–410. doi:10.1159/000140451
8. Petrioli R, Pascucci A, Francini E, et al. Neurotoxicity of FOLFOX-4 as adjuvant treatment for patients with colon and gastric cancer: a randomized study of two different schedules of oxaliplatin. Cancer Chemother Pharmacol. 2008;61(1):105–111. doi:10.1007/s00280-007-0454-3
9. Tesselaar ME, Ouwerkerk J, Nooy MA, et al. Risk factors for catheter-related thrombosis in cancer patients. Eur J Cancer. 2004;40(15):2253–2259. doi:10.1016/j.ejca.2004.06.023
10. Kim JS, Holtom P, Vigen C. Reduction of catheter-related bloodstream infections through the use of a central venous line bundle: epidemiologic and economic consequences. Am J Infect Control. 2011;39(8):640–646. doi:10.1016/j.ajic.2010.11.005
11. Cotogni P, Barbero C, Garrino C, et al. Peripherally inserted central catheters in non-hospitalized cancer patients: 5-year results of a prospective study. Support Care Cancer. 2015;23(2):403–409. doi:10.1007/s00520-014-2387-9
12. Blot SI, Depuydt P, Annemans L, et al. Clinical and economic outcomes in critically ill patients with nosocomial catheter-related bloodstream infections. Clin Infect Dis. 2005;41(11):1591–1598. doi:10.1086/497833
13. Dimick JB, Pelz RK, Consunji R, et al. Increased resource use associated with catheter-related bloodstream infection in the surgical intensive care unit. Arch Surg. 2001;136(2):229–234. doi:10.1001/archsurg.136.2.229
14. Leistner R, Hirsemann E, Bloch A, et al. Costs and prolonged length of stay of central venous catheter-associated bloodstream infections (CVC BSI): a matched prospective cohort study. Infection. 2014;42(1):31–36. doi:10.1007/s15010-013-0494-z
15. Pittet D, Tarara D, Wenzel RP. Nosocomial bloodstream infection in critically ill patients. Excess length of stay, extra costs, and attributable mortality. JAMA. 1994;271(20):1598–1601. doi:10.1001/jama.1994.03510440058033
16. Warren DK, Quadir WW, Hollenbeak CS, et al. Attributable cost of catheter-associated bloodstream infections among intensive care patients in a nonteaching hospital. Crit Care Med. 2006;34(8):2084–2089. doi:10.1097/01.CCM.0000227648.15804.2D
17. Beckers MM, Ruven HJ, Seldenrijk CA, et al. Risk of thrombosis and infections of central venous catheters and totally implanted access ports in patients treated for cancer. Thromb Res. 2010;125(4):318–321. doi:10.1016/j.thromres.2009.06.008
18. Liu Y, Gao Y, Wei L, et al. Peripherally inserted central catheter thrombosis incidence and risk factors in cancer patients: a double-center prospective investigation. Ther Clin Risk Manag. 2015;11:153–160. doi:10.2147/TCRM.S73379
19. Tabatabaie O, Kasumova GG, Eskander MF, et al. Totally implantable venous access devices: a review of complications and management strategies. Am J Clin Oncol. 2017;40(1):94–105. doi:10.1097/COC.0000000000000361
20. Goossens GA, De Waele Y, Jerome M, et al. Diagnostic accuracy of the catheter injection and aspiration (CINAS) classification for assessing the function of totally implantable venous access devices. Support Care Cancer. 2016;24(2):755–761. doi:10.1007/s00520-015-2839-x
21. Ku YH, Kuo PH, Tsai YF, et al. Port-A-Cath implantation using percutaneous puncture without guidance. Ann Surg Oncol. 2009;16(3):729–734. doi:10.1245/s10434-008-0224-4
22. Lin CP, Wang YC, Lin FS, et al. Ultrasound-assisted percutaneous catheterization of the axillary vein for totally implantable venous access device. Eur J Surg Oncol. 2011;37(5):448–451. doi:10.1016/j.ejso.2011.01.026
23. Lee JH, Bahk JH, Ryu HG, et al. Comparison of the bedside central venous catheter placement techniques: landmark vs electrocardiogram guidance. Br J Anaesth. 2009;102(5):662–666. doi:10.1093/bja/aep046
24. LaBella G, Kerlakian G, Muck P, et al. Port-A-Cath placement without the aid of fluoroscopy or localizing devices: a community hospital series. Cancer J. 2005;11(2):157–159. doi:10.1097/00130404-200503000-00012
25. Collier PE, Goodman GB. Cardiac tamponade caused by central venous catheter perforation of the heart: a preventable complication. J Am Coll Surg. 1995;181(5):459–463.
26. Darling JC, Newell SJ, Mohamdee O, Uzun O, Cullinane CJ, Dear PR. Central venous catheter tip in the right atrium: a risk factor for neonatal cardiac tamponade. J Perinatol. 2001;21(7):461–464. doi:10.1038/sj.jp.7210541
27. Eisen LA, Narasimhan M, Berger JS, et al. Mechanical complications of central venous catheters. J Intensive Care Med. 2006;21(1):40–46. doi:10.1177/0885066605280884
28. Ker K, Edwards P, Perel P, et al. Effect of tranexamic acid on surgical bleeding: systematic review and cumulative metaanalysis. BMJ. 2012;344:e3054. doi:10.1136/bmj.e3054
29. Chornenki N, Um KJ, Mendoza PA, et al. Risk of venous and arterial thrombosis in non-surgical patients receiving systemic tranexamic acid: a systematic review and meta-analysis. Thromb Res. 2019;179:81–86. doi:10.1016/j.thromres.2019.05.003
30. Godier A, Roberts I, Hunt BJ. Tranexamic acid: less bleeding and less thrombosis? Crit Care. 2012;16(3):135. doi:10.1186/cc11374
 © 2020 The Author(s). This work is published and licensed by Dove Medical Press Limited. The full terms of this license are available at https://www.dovepress.com/terms.php and incorporate the Creative Commons Attribution - Non Commercial (unported, v3.0) License.
By accessing the work you hereby accept the Terms. Non-commercial uses of the work are permitted without any further permission from Dove Medical Press Limited, provided the work is properly attributed. For permission for commercial use of this work, please see paragraphs 4.2 and 5 of our Terms.
© 2020 The Author(s). This work is published and licensed by Dove Medical Press Limited. The full terms of this license are available at https://www.dovepress.com/terms.php and incorporate the Creative Commons Attribution - Non Commercial (unported, v3.0) License.
By accessing the work you hereby accept the Terms. Non-commercial uses of the work are permitted without any further permission from Dove Medical Press Limited, provided the work is properly attributed. For permission for commercial use of this work, please see paragraphs 4.2 and 5 of our Terms.
