Back to Journals » Advances in Medical Education and Practice » Volume 10
Academic detailing as a method of continuing medical education
Authors Dyrkorn R , Langaas HC , Giverhaug T, Espnes KA , Rowett D, Spigset O
Received 20 February 2019
Accepted for publication 18 July 2019
Published 30 August 2019 Volume 2019:10 Pages 717—725
DOI https://doi.org/10.2147/AMEP.S206073
Checked for plagiarism Yes
Review by Single anonymous peer review
Peer reviewer comments 2
Editor who approved publication: Dr Md Anwarul Azim Majumder
Roar Dyrkorn,1 Harald Christian Langaas,2 Trude Giverhaug,3 Ketil Arne Espnes,1 Debra Rowett,4 Olav Spigset1,5
1Department of Clinical Pharmacology, St. Olav University Hospital, Trondheim, Norway; 2Regional Medicines Information and Pharmacovigilance Centre (RELIS), Department of Clinical Pharmacology, St. Olav University Hospital, Trondheim, Norway; 3Regional Medicines Information and Pharmacovigilance Centre (RELIS), University Hospital of North-norway, Tromsoe, North-Norway; 4Repatriation General Hospital, School of Pharmacy and Medical Sciences, University of South Australia, Adelaide, South Australia, Australia; 5Department of Clinical and Molecular Medicine, Norwegian University of Science and Technology, Trondheim, Norway
Correspondence: Roar Dyrkorn
Department of Clinical Pharmacology, St. Olav University Hospital, 7006 Trondheim, Norway
Email [email protected]
Introduction: Academic detailing is an interactive educational outreach to prescribers to present unbiased, non-commercial, evidence-based information, mostly about medications, with the goal of improving patient care. Academic detailing in Norway is an approach for providing continuing medical education to general practitioners (GPs). The basis of academic detailing is a one-to-one discussion between a trained health professional (the academic detailer) and the GP at the GP’s workplace.
Method: Our first campaign was named “Better use of non-steroidal anti-inflammatory drugs (NSAIDs)”, which aim was to reduce the use of diclofenac due to the risk of serious cardiovascular adverse events. At the same time we advised the GPs to use naproxen as the drug of choice if an NSAID was needed. We did a one-to-one intervention in two cities, where a trained academic detailer met the GP during office hours. A total of 247 GPs were invited to participate and 213 visits (86%) were completed. This article reviews the theoretical framework underlying the method and describes the development and implementation of academic detailing to GPs in Norway.
Results: More than 90% the participating GPs considered academic detailing a suitable method for providing up-to-date evidence-based, manufacturer-independent information, and nearly all would most likely or probably welcome another visit. After the intervention there was a reduction of diclofenac prescribing of 16% and 18%, respectively, in the two cities.
Conclusion: We consider that academic detailing is a suitable method to bring the best available evidence to the point at which care is delivered, to achieve the best for the patients. According to the Norwegian GPs’ evaluation, it is a key supplement to other methods of continuing medical education. To have maximum impact, it is important that academic detailing is practiced according to the consensus that has evolved in the USA and Australia.
Keywords: academic detailing, educational outreach visits, general practitioners, general practice, quality improvement
Introduction
It is virtually impossible for general practitioners (GPs) to be fully updated on all guidelines for all existing therapies. Several methods are used to obtain new and updated information, including congress participations, courses and seminars, group meetings with peers and self-studies. In 1983, Jerry Avorn and Stephen Soumerai published two articles in which they introduced a new method for providing evidence-based manufacturer-independent information for GPs, termed Academic detailing (AD).1,2 Since then the method has been used in several countries, especially Australia, USA and Canada3–7 as a strategy to enhance prescription decisions in general practice. However, the use of AD in Europe is minimal.
The basis of AD as defined in this article is a face-to-face discussion by a trained health professional, usually termed academic detailer (or clinical facilitator), in a one-to-one setting in the prescriber’s workplace during office hours. As a behaviour change intervention, one-to-one visits have shown to be more effective than group meetings with peer discussions.6–12 The term AD has also been used to describe other approaches as group meetings and small seminars.13–15 Both one-to-one visits and group meetings have advantages and disadvantages, as shown in Table 1.
 |
Table 1 Advantages and disadvantages with academic detailing versus group meetings as methods for changing drug prescribing practices among general practitioners (GPs) |
We searched PubMed and Embase after publications describing AD in Europe. We identified a total of 62 articles, but only 7 (11%) of those described a method were the prescriber was visited in a one-to-one setting. Thus, the use of the term AD is not unambiguous. We agree with bodies such as The Society for Academic Continuing Medical Education14 that the term AD should be reserved for one-to-one meetings as described and that studies should more clearly define the method used.
The steps of AD described in 1983 still form the basis of AD today1,2,13 (Box 1). The aim of this article is to review the theoretical framework underlying the method and to describe the development and implementation of academic detailing to GPs in Norway.
Method
Theoretical framework
For successful AD it is of crucial importance that the academic detailers are trained both in the method of AD and the best available evidence in the specific therapeutic area to be presented. This training allows the academic detailers to build necessary background and communication skills to engage in a collaborative dialog with the GP, to assess the GP’s needs and at the same time be aware of the GP’s attitudes, beliefs and values. The academic detailer is specifically trained to use open questions in the dialog. For example; “What is your experience in dealing with patients in this area?”, “Which adverse events do you see as the most common when using this medication?”, “How do you deal with this adverse event?”. Thus, information can be tailored on an individual basis. In the training, the academic detailer also practices communication skills, such as minimal enablers, to encourage a two-way conversation and reflecting skills, making sure that the academic detailer understands the views being expressed by the GP in the ongoing dialog.
Influencing professional behaviour change is complex and is increasingly being studied to better understand how to optimize the effectiveness of an intervention in different contexts and reduce the evidence-to-practice gap among GPs in a cost-effective manner. AD is influenced by social marketing theory,13 transtheoretical models of behaviour change and social cognitive theory. Figure 1, from the book Drug Utilization Research: Methods and Applications, highlights the complexity of practice change. For example, while it is recognized that guidelines alone may not affect professional behaviour change, they can be a component or part of the process from contemplation, awareness rising and knowledge building to reflection and rehearsal. These processes overlap in real life and are necessary for skill development and creation of motivation for change. The model helps to provide a theoretical basis and understanding of the relationship between multiple events across time that influence behavioural changes including medication use. In Figure 1, AD is placed under “Skill development” but it also has a place under “Motivation” and under “Reinforcement” when the GP is revisited.
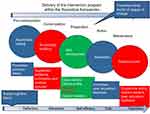 |
Figure 1 The complexity of practice change and the underlying theoretical frameworks. Academic detailing is placed under “Skill development” but it also has a place under “Motivation” and under “Reinforcement” when the general practitioner is revisited. Data f rom Elseviers M et al drug utilization research: methods and applications, Wiley-Blackwell, 2016, page 474. With permission from Wiley-Blackwell.16 |
When designing an AD campaign, updated evidence from internationally acknowledged sources should be gathered and reviewed by a group of professionals in the field, a priori key messages should be determined and educational material should be developed.
Academic detailing in Norway
The Department of Clinical Pharmacology and the Regional Medicines Information and Pharmacovigilance Center (RELIS) in Trondheim have been offering group education and participated in educational outreach visits to GPs over many years,17,18 typically during lunch hours or as half-day or full-day courses. Although group meetings are an efficient method to reach many GPs within a short period of time, this kind of education has limited impact.19 In addition, there are many potential disruptions, for example participants coming in or leaving the lunchroom during the session, checking e-mails and answering phone calls. Some key differences between AD and group meetings are presented in Table 1.
We wanted to implement AD in primary care in Norway, and received funding from the Norwegian Ministry of Health to perform a study in two cities, Tromsoe and Trondheim. Medical doctors (specialists in clinical pharmacology and junior doctors) and pharmacists employed at the Department of Clinical Pharmacology and RELIS were trained to be academic detailers. The training was undertaken over three days by an experienced AD teacher from The Drug and Therapeutic Information Service (DATIS) in Adelaide, Australia, following the same model as the courses in Australia. Education and training are crucial to ensure that the academic detailers have the competence to conduct an updating visit to maximize the impact of AD.14,15,20 To carry out a successful updating visit open questions is essential to facilitate the dialog11,21 - the academic detailer must continuously assess the clinician’s individual needs throughout the discussion. The academic detailers were trained to present a topic consistently while meeting the needs of individual GPs together with how to respond to questions. At the conclusion of the seminar the participants were filmed performing an AD visit to a local GP who was engaged to participate in the training. The film was used by the academic detailers for self-reflection, eg to consider body language and general attitude.
The first campaign was named “Better use of non-steroidal anti-inflammatory drugs (NSAIDs)”. In 2013, the European Medicines Agency (EMA)22 and the Norwegian Medicines Agency23 published new safety advice for diclofenac based on an increased risk for cardiovascular disease. Nevertheless, diclofenac continued to be the most frequently prescribed NSAID in Norway. We therefore concluded that prescription of NSAIDs would be a suitable topic for AD.
First, we carried out a literature search in the PubMed and Embase databases to identify the most recently updated knowledge in the area. A group of clinical pharmacologists, pharmacists, GPs, a nephrologist and a geriatrician worked together to distil the most important knowledge for the AD brochure. The distilled evidence-based material was presented in a four-page brochure. The most important content was broken down to 4–5 key messages, which were outlined on the front page of the brochure, while the rest of the brochure was used to provide the evidence behind the key messages, background information and reference citations. By such a procedure, a guideline of 50–200 pages can be condensed to present the most important aspects of a therapeutic guideline in a visually engaging format during the course of a relatively short updating visit.
The impact of the campaign was evaluated using data from the Norwegian Prescription Database (NorPD)24 covering a period of 12 months before and after the intervention. Prescription data was analysed with interrupted time series analysis. Full results of these analyses are published elsewhere.25
In most of the available literature there is no specification of the time frame for an AD visit. In Norway we chose to use 20 mins for the visit, as this is the time interval used for an ordinary patient consultation in general practice. Actual mean time for the visits in our campaign was 24 mins. When the visits took longer than the planned 20 mins, it was initiated by the GP, usually by asking further questions. In a few cases, the visit lasted considerably longer, up to 60 mins. In contrast, the shortest visit was only 10 mins. It all depended on the interest of the GP and the willingness to engage in the dialog. All GPs did engage to some degree, but most of them also wanted us to be able to finish the documentation of our key messages within the scheduled time frame of 20 mins.
After the one-to-one visit the academic detailer documented information about who was visited, duration of the visit, whether the whole brochure was presented or not, whether the GP seemed interested in the topic, and whether the GP suggested future topics of interest. If the academic detailer had been unable to answer specific questions during the visit, he or she brought the question back to the center to review the literature and/or discuss it with the team. Thereafter the answer was forwarded to the GP either by phone or by e-mail. Irrespective of any questions, the GP’s e-mail address was registered in order to send an evaluation form after the visit.
When revisiting a GP with a new campaign, key messages from the previous visit would be repeated as a reinforcement.
AD in Norway is solely an updating service. We do not examine the GP’s actual practice data, but give the GP an opportunity to reflect on whether his/her own practice is in accordance with the best available evidence, and make a change if needed. All GPs in the two cities were offered a visit, regardless of their prescribing pattern. The life cycle of a Norwegian AD program is presented in Figure 2.
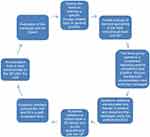 |
Figure 2 The life cycle of the academic detailing program in Norway. |
Results
Our campaign was named “Better use of non-steroidal anti-inflammatory drugs (NSAIDs)”, which advised GPs to reduce the use of diclofenac due to increased risk of serious cardiovascular adverse events, and at the same time we advised the GPs to use naproxen as drug of choice if an NSAID was needed, as naproxen has a more advantageous cardiovascular adverse event profile.26 In addition, we advised the GPs to generally avoid NSAIDs in the elderly.
The campaign took place between March and May 2015. A total of 247 GPs were invited to participate and 213 visits (86%) were completed. All participating GPs received an electronic questionnaire by e-mail to evaluate the visit. Of the 213 GPs visited, 169 (79%) completed the questionnaire. As this evaluation did not involve any patients, approval from an Ethical Committee was not needed according to Norwegian legislation. The principal results from the evaluation are shown in Table 2.
 |
Table 2 Norwegian general practitioners’ evaluation of the academic detailing campaign (n=213) |
Post-intervention prescribing effects were quite immediate and showed statistically significant results with a reduction of diclofenac prescribing of 16% and 18%, respectively, in the two cities where the campaign was carried out, relative to the rest of the country.25 The results are depicted in detail in Figures 3 and 4 where the changes in the prescription of diclofenac and naproxen in the two study cities are compared with the rest of the country. Full results of these analyses are published elsewhere.25
 |
Figure 3 Actual and modelled prescription of diclofenac 12 months before and after the academic detailing campaign (vertical dashed line) targeting general practitioners in the cities of Trondheim (A) and Tromsoe (B), compared with the rest of Norway. Reproduced under the terms of the creative commons attribution 4.0 international licence (http://creativecommons.org/licenses/by/4.0/); Langaas HC, Hurley E, Dyrkorn R, Spigset O. Effectiveness of an academic detailing intervention in primary care on the prescribing of non-steroidal anti-inflammatory drugs. Eur J Clin Pharmacol. 2019;75(4):577–86.25 |
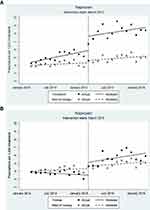 |
Figure 4 Actual and modelled prescription of naproxen 12 months before and after the academic detailing campaign (vertical dashed line) targeting general practitioners in the cities of Trondheim (A) and Tromsoe (B), compared with the rest of Norway. (Reproduced under the terms of the creative commons attribution 4.0 international licence (http://creativecommons.org/licenses/by/4.0/)). Langaas HC, Hurley E, Dyrkorn R, Spigset O. Effectiveness of an academic detailing intervention in primary care on the prescribing of non-steroidal anti-inflammatory drugs. Eur J Clin Pharmacol. 2019;75(4):577–86.25 |
Discussion
The key findings in this study was that post-intervention prescribing showed a reduction of diclofenac prescribing of 16–18% and that 90% of the participating GPs considered academic detailing a suitable method for keeping them up-to-date and 98% would probably or most probably welcome another visit. These numbers are about the same as those found in a study from France.27 The GPs were also very satisfied with the chosen visit duration of 20 mins. This is in accordance with our own experience indicating that 20 mins generally is sufficient to discuss the key messages, present the background documentation and, most importantly, to ensure that the academic detailer engages in a dialog with the GP. Some visits take longer and some shorter time, as individual needs and the eagerness to discuss and oppose differs between GPs. The time used is shorter than in other countries. In Australia the average appointment time booked is 30 mins and the average time used is 38 mins (unpublished data, Drug and Therapeutics Information Service). Van Hoof et al found that the time frame was about 60 mins in their review article on Characteristics of Academic Detailing.14
As we now have started new campaigns in other therapeutic areas, we have experienced that when visiting a GP for a second time, repeating and discussing key messages from the previous visit, some of the GPs are willing to share whether they have changed their practice. They had most often not proceeded through all the stages of changes, but instead moved straight to action. We believe that the main reason for this swift response is the trust and credibility towards the academic detailer and the synthesized practical material. This process is referred to as “cognitive debiasing”28 and is a heuristic or short-cut approach for clinical decision making, and can possibly explain the immediate prescribing changes after the intervention. This outcome presupposes a high awareness for the AD service providers to ensure that the program content is reliable and up-to-date, and that the academic detailer is well trained in presenting the clinical content correctly. Another factor could be the simple message presented in the NSAID campaign; prescribing another drug within the same class and with the same therapeutic effect which is not particularly complicated to perform for the GP in the clinical setting.
Independence from commercial interests as well as from the health authorities was emphasized by many of the GPs as a factor that increased credibility. Even though our campaign was funded by a public grant our organization developed the materials independently and was perceived as independent by most of the GPs. Others have also shown that users of AD highly appreciate its educational value and, due to their positive experience with AD, tend to view information from other sources and other forms of continuing medical education more critically.29 In a study from Belgium, the GPs concluded that the visits were a credible and interesting way of receiving continuing medical education and that they both enhanced their knowledge and increased their reflections on their own prescribing behaviour.30 That the service is free for the GP and that the GP does not have to leave the office eliminates the need for travel and minimizes any loss of income for the GP.
Conclusion
AD as a method is gradually expanding to new countries and is well suited for professional updating among GPs. Several studies have shown that AD is the most effective method to ignite motivation for behavioural change among GPs.6–8,12,19,29 The method is based on encouragement and reflection to achieve voluntary action, rather than coercion or enforcement. It brings the best available evidence to the point at which care is delivered and can be tailored to meet the individual needs of the doctors, to achieve the best for their patients. According to the Norwegian GPs’ evaluation it is a key supplement to other methods of professional updating. In order to evaluate the method even more thoroughly, we agree with bodies such as The Society for Academic Continuing Medical Education,14 and strongly recommend that future studies should more clearly define and explain the specific method used, and that the term AD should be reserved for one-to-one meetings.
Key message
- Several studies have shown that academic detailing is the most effective method to ignite motivation for behavioural change among general practitioners.
- We have developed and implemented the method in Norway.
- According to the general practitioners’ evaluation academic detailing is a welcome activity and a key supplement to other methods of professional updating.
Ethical requirement
As this evaluation did not involve any patients, approval from an Ethical Committee was not needed according to Norwegian legislation. Participating GPs enrolled themselves after an invitation letter and analysis were done with depersonalized data.
Aknowlegdements
We thank all participating academic detailers for their dedication and enthusiasm. The study received funding from the Norwegian Ministry of Health
Author contributions
All authors contributed to data analysis, drafting or revising the article, gave final approval of the version to be published, and agree to be accountable for all aspects of the work.
Disclosure
Mr Harald Christian Langaas reports grants from Norwegian Directorate of Health, during the conduct of the study. The authors report no other conflicts of interest in this work.
 |
References
1. Avorn J, Soumerai SB. Improving drug-therapy decisions through educational outreach. A randomized controlled trial of academically based “detailing”. N Engl J Med. 1983;308(24):1457–1463. doi:10.1056/NEJM198306163082406
2. Avorn J, Soumerai SB. A new approach to reducing suboptimal drug use. JAMA. 1983;250(13):1752–1753.
3. May FW, Rowett DS, Gilbert AL, McNeece JI, Hurley E. Outcomes of an educational-outreach service for community medical practitioners: non-steroidal anti-inflammatory drugs. Med J Aust. 1999;170(10):471–474.
4. Shankar PR, Jha N, Piryani RM, Bajracharya O, Shrestha R, Thapa HS. Academic detailing. Kathmandu Univ Med J (KUMJ). 2010;8(29):126–134.
5. Costa J, Almeida-Brasil CC, Lemos LL, et al. Brazilian guideline for academic detailing: a need to improve health care. Value Health. 2015;18(7):A854. doi:10.1016/j.jval.2015.09.451
6. Figueiras A, Sastre I, Tato F, et al. One-to-one versus group sessions to improve prescription in primary care: a pragmatic randomized controlled trial. Med Care. 2001;39(2):158–167.
7. van Eijk ME, Avorn J, Porsius AJ, de Boer A. Reducing prescribing of highly anticholinergic antidepressants for elderly people: randomised trial of group versus individual academic detailing. BMJ. 2001;322(7287):654–657. doi:10.1136/bmj.322.7287.654
8. Freemantle N, Nazareth I, Eccles M, Wood J, Haines A. Evidence-based outReach t. A randomised controlled trial of the effect of educational outreach by community pharmacists on prescribing in UK general practice. Br J Gen Pract. 2002;52(477):290–295.
9. O’Brien MA, Rogers S, Jamtvedt G, et al. Educational outreach visits: effects on professional practice and health care outcomes. Cochrane Database Syst Rev. 2007;4:CD000409.
10. Bloom BS. Effects of continuing medical education on improving physician clinical care and patient health: a review of systematic reviews. Int J Technol Assess Health Care. 2005;21(3):380–385.
11. Satterlee WG, Eggers RG, Grimes DA. Effective medical education: insights from the cochrane library. Obstet Gynecol Surv. 2008;63(5):329–333. doi:10.1097/OGX.0b013e31816ff661
12. Bounthavong M, Harvey MA, Wells DL, et al. Trends in naloxone prescriptions prescribed after implementation of a national academic detailing service in the veterans health administration: a preliminary analysis. J Am Pharm Assoc (2003). 2017;57(2S):S68–S72. doi:10.1016/j.japh.2016.11.003
13. Soumerai SB, Avorn J. Principles of educational outreach (‘academic detailing’) to improve clinical decision making. JAMA. 1990;263(4):549–556.
14. Van Hoof TJ, Harrison LG, Miller NE, Pappas MS, Fischer MA. Characteristics of academic detailing: results of a literature review. Am Health Drug Benefits. 2015;8(8):414–422.
15. Yeh JS, Van Hoof TJ, Fischer MA. Key features of academic detailing: development of an expert consensus using the delphi method. Am Health Drug Benefits. 2016;9(1):42–50.
16. Elseviers M, Wettermark B, Almarsdottir AB et al, editors. Drug Utilization Research: Methods and Applications. West Sussex: Wiley-Blackwell, 2016; p 474.
17. Dyrkorn R, Gjelstad S, Espnes KA, Lindbaek M. Peer academic detailing on use of antibiotics in acute respiratory tract infections. A controlled study in an urban Norwegian out-of-hours service. Scand J Prim Health Care. 2016;34(2):180–185. doi:10.3109/02813432.2016.1163035
18. Gjelstad S, Fetveit A, Straand J, Dalen I, Rognstad S, Lindbaek M. Can antibiotic prescriptions in respiratory tract infections be improved? A cluster-randomized educational intervention in general practice–the prescription peer academic detailing (Rx-PAD) study [NCT00272155]. BMC Health Serv Res. 2006;6:75. doi:10.1186/1472-6963-6-75
19. Simon SR, Majumdar SR, Prosser LA, et al. Group versus individual academic detailing to improve the use of antihypertensive medications in primary care: a cluster-randomized controlled trial. Am J Med. 2005;118(5):521–528. doi:10.1016/j.amjmed.2004.12.023
20. Morrow RW, Tattelman E, Purcell JM, King J, Fordis M. Academic peer detailing-the preparation and experience of detailers involved in a project to disseminate a comparative effectiveness module. J Contin Educ Health Prof. 2016;36(2):123–126. doi:10.1097/CEH.0000000000000067
21. Soumerai SB. Principles and uses of academic detailing to improve the management of psychiatric disorders. Int J Psychiatry Med. 1998;28(1):81–96. doi:10.2190/BTCA-Q06P-MGCQ-R0L5
22. European Medicines Agency (28.06.2013) New safety advice for diclofenac – cMDh endorses PRAC recommendation 2013 Available from: https://www.ema.europa.eu/.
23. Statens legemiddelverk (25.06.2013) Nye anbefalinger for diklofenak: NOMA; 2013 Available from: https://legemiddelverket.no.
24. Norwegian Prescription Database: Norwegian Prescription Database; 2019 Available from: http://www.norpd.no/.
25. Langaas HC, Hurley E, Dyrkorn R, Spigset O. Effectiveness of an academic detailing intervention in primary care on the prescribing of non-steroidal anti-inflammatory drugs. Eur J Clin Pharmacol. 2019;75(4):577–586. doi:10.1007/s00228-018-02611-y
26. Coxib, traditional NTC, Bhala N, Emberson J, Merhi A, et al. Vascular and upper gastrointestinal effects of non-steroidal anti-inflammatory drugs: meta-analyses of individual participant data from randomised trials. Lancet. 2013;382(9894):769–779. doi:10.1016/S0140-6736(13)60900-9
27. Bruno-Bazureault P, Touboul P, Hofliger P, et al. [Peer visits to community-based general practitioners and pediatricians as part of the “antibiotics only when necessary” campaign in the alpes-maritimes district. Methodology, feasibility, and interest]. Presse Med. 2006;35(5 Pt 1):749–754.
28. Croskerry P, Singhal G, Mamede S. Cognitive debiasing 2: impediments to and strategies for change. BMJ Qual Saf. 2013;22(Suppl 2):ii65–ii72. doi:10.1136/bmjqs-2012-001713
29. Allen M, Ferrier S, O’Connor N, Fleming I. Family physicians’ perceptions of academic detailing: a quantitative and qualitative study. BMC Med Educ. 2007;7:36. doi:10.1186/1472-6920-7-36
30. Anthierens S, Verhoeven V, Schmitz O, Coenen S. Academic detailers’ and general practitioners’ views and experiences of their academic detailing visits to improve the quality of analgesic use: process evaluation alongside a pragmatic cluster randomized controlled trial. BMC Health Serv Res. 2017;17(1):841. doi:10.1186/s12913-017-2797-8
 © 2019 The Author(s). This work is published and licensed by Dove Medical Press Limited. The full terms of this license are available at https://www.dovepress.com/terms.php and incorporate the Creative Commons Attribution - Non Commercial (unported, v3.0) License.
By accessing the work you hereby accept the Terms. Non-commercial uses of the work are permitted without any further permission from Dove Medical Press Limited, provided the work is properly attributed. For permission for commercial use of this work, please see paragraphs 4.2 and 5 of our Terms.
© 2019 The Author(s). This work is published and licensed by Dove Medical Press Limited. The full terms of this license are available at https://www.dovepress.com/terms.php and incorporate the Creative Commons Attribution - Non Commercial (unported, v3.0) License.
By accessing the work you hereby accept the Terms. Non-commercial uses of the work are permitted without any further permission from Dove Medical Press Limited, provided the work is properly attributed. For permission for commercial use of this work, please see paragraphs 4.2 and 5 of our Terms.
