Back to Journals » OncoTargets and Therapy » Volume 12
A Retrospective Analysis: A Novel Index Predicts Survival and Risk-Stratification for Bone Destruction in 419 Newly Diagnosed Multiple Myelomas
Authors Jin Y, Shang Y, Liu H , Ding L, Tong X, Tu H, Yuan G, Zhou F
Received 29 August 2019
Accepted for publication 22 October 2019
Published 3 December 2019 Volume 2019:12 Pages 10587—10596
DOI https://doi.org/10.2147/OTT.S229122
Checked for plagiarism Yes
Review by Single anonymous peer review
Peer reviewer comments 2
Editor who approved publication: Prof. Dr. Takuya Aoki
Yanxia Jin,1,2 Yufeng Shang,1 Hailing Liu,3 Lu Ding,1 Xiqin Tong,1 Honglei Tu,1 Guolin Yuan,4 Fuling Zhou1,5
1Department of Hematology, Zhongnan Hospital, Wuhan University, Wuhan, Hubei 430071, People’s Republic of China; 2Hubei Key Laboratory of Edible Wild Plants Conservation and Utilization, Hubei Normal University, Huangshi, Hubei 435002, People’s Republic of China; 3Department of Clinical Hematology, Second Affiliated Hospital, Medical School of Xi’an Jiaotong University, Xi’an, Shaanxi 710004, People’s Republic of China; 4Department of Hematology, Xiangyang Central Hospital, The Affiliated Hospital of Hubei University of Arts and Science, Xiangyang, Hubei 441021, People’s Republic of China; 5Key Laboratory of Tumor Biological Behavior of Hubei Province, Zhongnan Hospital, Wuhan University, Wuhan, Hubei 430071, People’s Republic of China
Correspondence: Fuling Zhou
Department of Hematology, Zhongnan Hospital, Wuhan University, No. 169 Donghu Road, Wuchang District, Wuhan 430071, People’s Republic of China
Tel +8618986265580
Email [email protected]
Objective: Multiple myeloma (MM) patients with bone destruction are difficult to restore, so it is of great clinical significance to further explore the factors affecting MM bone destruction.
Methods and results: This study retrospectively analyzed 419 cases with MM. Multiple linear regression analysis showed that those MM patients with a higher concentration of Ca2+ in serum, higher positive rate of CD138 immuno-phenotype and advanced in stage with 13q34 deletion in cytogenetics would be more prone to bone destruction, while total bile acid (TBA) and kappa chain isotope negatively correlated with bone destruction in MM patients. The Kaplan–Meier analysis indicated that Ca2+, serum β2-microglobulin (β2-MG), hemoglobin (HGB), creatinine (CREA), uric acid (UA) and age correlated with the survival of bone destruction in MM patients. Cox regression analysis further showed that the independent prognostic factors of β2-MG and CREA had a higher risk for early mortality in bone destruction patients. Moreover, an index was calculated based on β2-MG and globulin (GLB) to white blood cell (WBC) ratio to predict the poor survival of bone destruction patients.
Conclusion: We provide a novel marker to predict the prognosis of myeloma patients using routine examination method instead of bone marrow aspiration, and provide a reference for clinical evaluation.
Keywords: multiple myeloma, bone destruction, prediction index, prognosis
Introduction
Multiple myeloma (MM) is a malignant clonal proliferation of plasma cell predominantly located in bone marrow, which affects the hematopoiesis in the bone marrow. MM is mainly characterized by hypercalcemia, renal dysfunction, anemia and multiple bone destruction (CRAB) in the clinic.1 The mortality of MM has increased in recent years.2,3 Nowadays, some new drugs, such as the immunomodulatory drug thalidomide, lenalidomide, proteasome inhibitor bortezomib, as well as high-dose therapy/autologous stem cell transplantation,4,5 have been introduced for treatment of MM patients, which seems to have improved the life quality of MM patients and significantly prolonged survival time.6 The 5-year survival rate has been improved as a result of more effective treatment options available.7 However, currently, multiple myeloma is still an incurable disease, and patients with minimal residual disease are prone to relapse, with fatal outcomes for most patients in the advanced stages.
Multiple myeloma bone destruction is a common and devastating complication of MM due to the majority of patients with destructive bony lesions, leading to bone pain, pathologic fractures, mobility issues and other clinical manifestations. Increased osteoclastogenesis with suppressed osteoblastic activity is the main mechanism in the development of myeloma bone destruction.8,9 The activated bone destruction factors and lack of bone formation factors are found to be involved in the pathogenesis of myeloma bone destruction, such as receptor activator of nuclear factor kappa-B ligand (RANKL),10 osteoprotegerin (OPG) system (RANKL/OPG) and Wnt/DKK1 pathway.11–13 The relative level of RANKL/OPG is a key factor of osteogenesis and osteoclast balance.14 Overexpression of Dickkopf-1 (DKK1) in myeloma cells is associated with the degree of lytic bone disease.15 DKK1 directly promotes the decrease of RANKL and OPG, which leads to the increase of osteoclast formation.16
There are some therapeutic approaches for targeting OC pathways or OB pathways,17,18 such as anti-DKK1, TGF-β inhibitors and cytotherapy. We previously reported a novel multiepitope vaccine from MMSA-1 and DKK1 for MM immunotherapy.19 BTZ is a first-in-class proteasome inhibitor that primarily targets the constitutive proteasome subunit b5 of the 26S proteasome20 to induce myeloma cell apoptosis and directly change the activity of osteoblast by decreasing RANKL and DKK-1 levels in the sera of myeloma patients.21 Despite so many progresses, MM patients with bone destruction are difficult to restore, which is one of the major problems for the treatment of multiple myeloma. Therefore, further in-depth study of the characteristics of myeloma bone destruction will help us to find more effective methods to treat multiple myeloma bone disease and to improve the prognosis and prolong survival period of patients.
In this study, the factors correlated with bone destruction and the factors affecting survival and prognosis of myeloma bone destruction were analyzed by a retrospective study.
Materials and Methods
Patients
A total number of 419 patients with newly diagnosed multiple myeloma were collected between April 2000 and July 2016, of which 224 patients were from Zhongnan Hospital of Wuhan University, 108 patients were from Xiangyang Central Hospital and 87 cases were from Second Affiliated Hospital of Xi’an Jiaotong University. Both studies were conducted in accordance with the Declaration of Helsinki and approved by the institution’s Research Ethics Board of Zhongnan Hospital of Wuhan University and Xiangyang Central Hospital and Second Affiliated Hospital of Xi’an Jiaotong University. Informed consent was obtained from all patients. Patients were diagnosed according to the WHO diagnosis for the myeloma disease by standard morphologic and cytochemical examinations of peripheral blood and marrow smears, and flow cytometry of marrow, and fluorescence in situ hybridization (FISH) on plasma cells extracted from bone marrow to determine specific chromosomal abnormalities in MM patients, including translocation, deletion or amplification.22,23 The hybridization signals were evaluated and photographed digitally by photomicrography. All patients had image examinations including X-ray, computed tomographic (CT) scan imaging or positron emission tomography-computed tomography (PET-CT) of the whole body to determine if there was bone destruction.24 For the MM cases, we also documented the date of diagnosis and the stage of MM according to the ISS and IMWG risk stratification at diagnosis.25,26
Data Collection and Prognosis Evaluation
Data were collected from the electronic patient record without any clinical intervention in this retrospective study. Clinical dates include basic characteristics of patients, such as age, gender, and performance status (PS), which were evaluated based on the Eastern Cooperative Oncology Group scale (ECOG)27 and laboratory examination, such as complete blood count, liver and kidney function, erythrocyte sedimentation rate and image examinations. The laboratory features were evaluated and the standards were defined as follows: abnormal white blood cell (WBC < 4 ×109 g/l or >10 ×109 g/l), abnormal platelet (PLT <100 ×109 g/l or >300 ×109 g/l), anemia (HGB≤ 100 g/L) and erythrocyte sedimentation rate increase fast (ESR >30 mm/h), elevated alkaline phosphatase (ALP >150 U/I), elevated lactate dehydrogenase (LDH >250 U/l), elevated serum β2-microglobulin (β2-MG ≥3.5 mg/l), hypercalcaemia (calcium ≥2.75 mmo1/L),28 elevated urine β2-microglobulin (β2-MG ≥650 μg/l), hepatorenal insufficiency (creatinine ≥177 μmol/l, UA>420 μmol/l), hypoalbuminemia (albumin <35 g/l) and higher immunoglobulin (IgG ≥35 g/l, IgA ≥20 g/l).29,30 In addition to the above data, it also includes information on some characteristics of multiple myeloma.
The evaluation of prognosis mainly included overall survival (OS). OS was defined as the time from diagnosis to last follow-up or death resulting from any cause. Follow-up of patients not experiencing any of these events was censored at the date of the last contact.
Statistical Analysis
Patient characteristics were summarized using descriptive statistics, such as mean, median and range for quantitative variables and frequencies for qualitative variables. Data were expressed as means ± standard deviations or median (range). A comparison between categorical variables was made by the chi-square analysis with the Pearson test. The parametric t-test with independent samples was used to compare the mean of variables between patients without bone destruction and with bone destruction. The correlation was analyzed using bivariate correlation analysis by Pearson test (r). In the multivariate analysis, factors associated with bone destruction were determined by a binary logistic regression model with forward stepwise. The survival analysis was evaluated according to the Kaplan–Meier method with the two-sided log-rank test.31 Univariate analysis by chi-square analysis with Pearson test was used to evaluate the odds ratios (OR) and 95% CI. Multivariate analysis by the Cox proportional hazards regression model (Omnibus test of model coefficients, likelihood ratio test) with forward stepwise was used to estimate hazard ratios (HR) and 95% CI.28 The constructed ROC curves and the AUC were analyzed, the combined index of β2-MG, GLB and WBC was performed using binary logistic regression by calculating the new probability, and acquiring the new ROC and AUC value.
In all statistical analyses, a p value less than 0.05 was considered as statistically significant. Calculations were performed using IBM SPSS statistics software (version 24.0).
Results
Clinical Characteristics of Patients with Multiple Myeloma
The retrospective study included 419 patients diagnosed with multiple myeloma. There were 131 patients without multiple myeloma bone destruction and 288 patients with multiple myeloma bone destruction at the time of diagnosis. The clinical characteristics of the included participants are summarized in Table 1. In the without bone destruction group, 67 patients (51.1%) were male with median age 63 years (range 43–85) at diagnosis, while in the bone destruction group, the median age at diagnosis was 62 years (range 31–86), and 176 patients (61.1%) were male. The survival of patients with bone destruction or without bone destruction was analyzed by Cox regression model analysis (p=0.001), which indicated that MM patients with bone destruction has lower survival compared to MM patients without bone destruction (Figure 1).
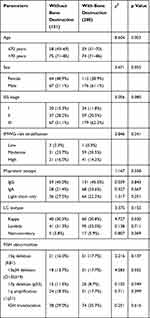 |
Table 1 Baseline Characteristics in 419 Cases of MM Patients |
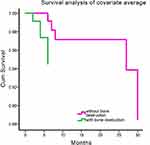 |
Figure 1 Survival curves of MM patients with bone destruction and without bone destruction. |
Analysis of the Correlated Factors to Multiple Myeloma Bone Destruction
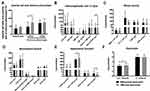
The chi-square test was performed to analyze the clinical characteristics of age, sex, ISS stage, IMWG risk stratification, M-protein isotype, light chain isotype and FISH abnormalities in 419 cases. The results show that age ≥70 years (p=0.003), serum kappa light chain (p=0.030) and 13q34 deletion (p=0.032) have a significant difference between MM patients with without bone destruction and with bone destruction. We focused on different factors involved in bone destruction by comparing the mean of variates in this retrospective study. Two independent samples parametric t-test showed that uric acid (p=0.002), total bile acid (p=0.016), Ca2+ (p=0.005), serum kappa chain isotope (p=0.036) and positive rate of CD138 immuno-phenotype (p=0.011) have significant differences between patients without bone destruction and with bone destruction. The other factors have no statistical difference in this current cohort including chi-square analysis (Figure 2).
Univariate analysis indicated that Ca2+ (p=0.011), ISS stage (p=0.049) and 13q34 deletion (p=0.032), and positive rate of CD138 immuno-phenotype (p=0.011) positively correlated with bone destruction, while TBA (p=0.006) and kappa chain isotope (p=0.030) negatively correlated with bone destruction in MM patients. Multivariate analysis further determined that 13q34 deletion (p=0.019) and positive rate of CD138 immuno-phenotype (p=0.014) were independent factors associated with bone destruction (Table 2). The cutoff value of the positive rate of CD138 immunophenotype is 75.00% based on the ROC curve, with a sensitivity of 64.9% at a specificity of 92.30% (Fig. S1).
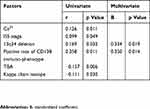 |
Table 2 Factors Associated with Bone Destruction in MM by Univariate and Multivariate Analysis |
The Survival Analysis of Multiple Myeloma Bone Destruction
The Kaplan–Meier with two-sided log-rank test was used to analyze the factors affecting survival in multiple myeloma. The results showed that Ca2+ (p=0.001), serum β2-microglobulin (p=0.001), hemoglobin (p=0.009), creatinine (p<0.001), uric acid (p=0.002) and age (p=0.024) have a marked difference in correlation with survival of multiple myeloma (Table 3). It is suggested that the Ca2+ (≥2.75 mmol/l), serum β2-microglobulin (≥3.5 mg/l), hemoglobin (≤100 g/l), creatinine (≥177 μmol/l), uric acid (>420 μmol/l) and age (>70 years) were correlated with poor survival in multiple myeloma. Cox regression analysis showed that serum β2-microglobulin and creatinine were independent factors for the prediction of the survival of MM (Table 4). The curves of hazard ratios for β2-MG and CREA are shown in Fig. S2.
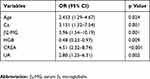 |
Table 3 Predictors of Overall Survival in MM for the Current Cohort |
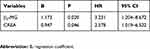 |
Table 4 Cox Analysis of the Hazard Ratios in MM for the Current Cohort |
In multiple myeloma bone destruction group, the Ca2+ (p=0.001), serum β2-microglobulin (p=0.001), hemoglobin (p=0.009), creatinine (p<0.001), uric acid (p=0.001) and age (p=0.017) have a significant difference in correlation with survival of multiple myeloma bone disease (Figure 3). It was indicated that the hypercalcemia, elevated serum β2-microglobulin, anemia, renal insufficiency and advanced age were correlated with poor survival in multiple myeloma bone destruction.
A Novel Index Predicts the Survival of Bone Destruction in MM Patients
The level of serum β2-MG reflects the tumor mass and is now considered a standard measure of the tumor burden,32 for example, serum β2-MG was a powerful prognostic factor in malignant lymphomas.33 For MM, serum β2-MG levels correlate with the ISS stage. Serum GLB was also an important factor for MM and white blood cell counts were associated with inflammation and immune, so we combined the three factors for further analysis. Interestingly, a novel index was defined as follows: β2-MG×GLB/WBC, where β2-MG and globulin in serum levels and white blood cell counts, respectively. The cutoff value of β2-MG×GLB/WBC is defined as 52.78 based on the ROC curve, with a sensitivity of 51.70% at a specificity of 75.30%. β2-MG×GLB/WBC could improve the diagnostic performance for bone destruction from MM patients (Figure 4A and Table 5). Moreover, combined β2-MG, GLB and WBC could improve the prediction value for bone destruction patients (Figure 4B and Table 5). This combined index can significantly predict the overall survival of bone destruction patients (Figure 4C) and as an independent factor for high-risk evaluation (Table 5).
 |
Table 5 Predictive Value of Index (β2-MG, GLB and WBC) in Bone Destruction of MM Patients |
Discussion
Multiple myeloma bone destruction is characterized by bone marrow infiltration with clonal plasma cells, which results in lytic lesions in the bones. Although RANKL/OPG and DKK1 pathways play important roles in bone destruction, which support that myeloma bone disease is a multifactorial disease, the molecular mechanism of multiple myeloma bone destruction caused is uncertain and needs to be further studied.8,34 Studies have shown that bone marrow microenvironment is close to the growth of myeloma cells, and their interaction plays an important role in the occurrence of myeloma bone destruction and even causes a vicious cycle of tumor development and bone destruction.11 Many cytokines are involved in the occurrence of myeloma bone destruction, such as RANKL, M-CSF and IL-6, whose interaction further stimulates tumor proliferation and bone damage and directly impacts on the clinical manifestation and prognosis of the disease.35
In this study, we found that hyperuricemia and increased total bile acid (TBA) have a statistical difference between patients with myeloma bone destruction and without bone lesions. That hepatic and renal were involved in multiple myeloma are frequently found due to plasma cell infiltration. Renal insufficiency is one of the clinical characteristics of MM, while the clinical manifestation of liver disease in multiple myeloma was quite uncommon, but abnormal liver functions were common in multiple myeloma.36 The expression of bile acids may be associated with bone destruction. Studies have shown that antagonist of bile acid receptor suppressed the RANKL-induced NF-kappa B activation pathway by inhibiting I kappa kinase (IKK); moreover, this effect is related to the suppression of osteoclastogenesis induced by RANKL or by multiple myeloma cells,37 which can be explained why total bile acid was related to myeloma bone destruction.
Deletion of 13q is an adverse prognostic factor in newly diagnosed MM,38,39 and in this study, we found D13S319 as an independent factor had a significant difference between MM patients with bone destruction and without bone destruction. We also know that p53 gene is correlated with poor prognosis in above 10% of newly diagnosed MM patients,40 and 1q21 gene amplification has significantly worsened poor prognosis in multiple myeloma patients.41 However, in our study, there were no significant differences correlated with survival between MM patients with bone destruction and without bone destruction, which may be associated with hypodiploidy in MM patients42; thus further research is needed to explore the mechanism about bone destruction in MM.
Despite the mean of many variates have no difference between without bone destruction and with bone destruction patients, many variates affected the overall survival of patients. The survival analysis showed that the factors Ca2+, serum β2-MG, HGB, CREA, UA and age have a marked difference in correlation with the survival of multiple myeloma and patients with bone destruction (Figure 3).
Importantly, this study found the effect of independent prognostic factor β2-MG on early mortality and high risk for bone destruction patients, which supports the result of β2-MG considered as a standard measure of the tumor burden.32 Fetal serum β2-MG correlates with kidney injury.43 In MM, the level of serum β2-MG is considered essential for ISS stage and clinical management.44 Globulin (GLB) levels correlate with MM diagnosis and therapy. White blood cell (WBC) count including leukocyte and neutrophil reflects the inflammation response, and T lymphocytes, B lymphocytes, macrophages and natural killer cells reflect the immune function,45,46 which closely associated with tumor development. We found an index β2-MG×GLB/WBC can improve the diagnostic performance for bone destruction from MM patients, and combined β2-MG, GLB and WBC could improve the prediction value and significantly predict the overall survival of bone destruction patients. It suggests that a combination of β2-MG, GLB and WBC as a marker reflects the balance between myeloma and immune response, which enables better understanding of the role of β2-MG, GLB and WBC in myeloma and will help illustrate the association between cancer and immunity in the clinic. β2-MG, GLB and WBC can be detected by peripheral blood routine examination, which can reduce the pain of additional invasive examination in MM patients. In addition, according to the index, the abnormality of the results can quickly attract the attention of clinicians, and thus the progress of the disease can be detected early and the prognosis of the patients can be predicted, which had an important significance for clinical guide. To sum up, this will be a novel index to predict the prognosis of myeloma patients using routine examination method instead of bone marrow aspiration.
In conclusion, for MM patients, those with a higher concentration of Ca2+ in serum, higher positive rate of CD138 immuno-phenotype and advanced in stage with 13q34 deletion in cytogenetics would more prone to bone destruction. Hypercalcemia, elevated serum β2-MG, anemia, renal insufficiency, elevated UA and advanced in years were correlated with poor survival and high risk in bone destruction of multiple myeloma. Combined β2-MG, GLB and WBC significantly predict prognosis of bone destruction patients, which will be an important significance for clinical guide.
Statement of Ethics
All procedures performed in studies involving human participants were in accordance with the ethical standards of the institutional research committee and with the 1964 Helsinki declaration. Written informed consent was received from all patients before inclusion in the study and information was collected from the electronic patient records.
Acknowledgements
The authors would thank the patients from Zhongnan Hospital of Wuhan University, Xiangyang Central Hospital and Second Affiliated Hospital of Xi’an Jiaotong University who participated in the study. An abstract of this paper was presented as a poster section at the Sixteenth National Academic Conference on Experimental Hematology (October 20-22, 2017, Fuzhou, China).
Author Contributions
All authors contributed to data analysis, drafting and revising the article, gave final approval of the version to be published and agreed to be accountable for all aspects of the work.
Disclosure
The authors report no conflicts of interest in this work.
References
1. Talamo G, Farooq U, Zangari M, et al. Beyond the CRAB symptoms: a study of presenting clinical manifestations of multiple myeloma. Clin Lymphoma Myeloma Leuk. 2010;10(6):464–468. doi:10.3816/CLML.2010.n.080
2. Mehta GR, Suhail F, Haddad RY, Zalzaleh G, Lerma EV. Multiple myeloma. Dis Mon. 2014;60(10):483–488. doi:10.1016/j.disamonth.2014.08.002
3. Walz S, Stickel JS, Kowalewski DJ, et al. The antigenic landscape of multiple myeloma: mass spectrometry (re)defines targets for T-cell-based immunotherapy. Blood. 2015;126(10):1203–1213. doi:10.1182/blood-2015-04-640532
4. Kumar SK, Rajkumar SV, Dispenzieri A, et al. Improved survival in multiple myeloma and the impact of novel therapies. Blood. 2008;111(5):2516–2520. doi:10.1182/blood-2007-10-116129
5. Palumbo A, Anderson K. Multiple myeloma. N Engl J Med. 2011;364(11):1046–1060. doi:10.1056/NEJMra1011442
6. Cherry BM, Korde N, Kwok M, Roschewski M, Landgren O. Evolving therapeutic paradigms for multiple myeloma: back to the future. Leuk Lymphoma. 2013;54(3):451–463. doi:10.3109/10428194.2012.717277
7. Brenner H, Gondos A, Pulte D. Recent major improvement in long-term survival of younger patients with multiple myeloma. Blood. 2008;111(5):2521–2526. doi:10.1182/blood-2007-08-104984
8. Qiao M, Wu D, Carey M, Zhou X, Zhang L. Multi-scale agent-based multiple myeloma cancer modeling and the related study of the balance between osteoclasts and osteoblasts. PLoS One. 2015;10(12):e0143206. doi:10.1371/journal.pone.0143206
9. Silbermann R, Roodman GD. Myeloma bone disease: pathophysiology and management. J Bone Oncol. 2013;2(2):59–69. doi:10.1016/j.jbo.2013.04.001
10. Giuliani N, Colla S, Sala R, et al. Human myeloma cells stimulate the receptor activator of nuclear factor-kappa B ligand (RANKL) in T lymphocytes: a potential role in multiple myeloma bone disease. Blood. 2002;100(13):4615–4621. doi:10.1182/blood-2002-04-1121
11. Delgado-Calle J, Anderson J, Cregor MD, et al. Bidirectional notch signaling and osteocyte-derived factors in the bone marrow microenvironment promote tumor cell proliferation and bone destruction in multiple myeloma. Cancer Res. 2016;76(5):1089–1100. doi:10.1158/0008-5472.CAN-15-1703
12. Golden D, Saria EA, Hansen MF. Regulation of osteoblast migration involving receptor activator of nuclear factor-kappa B (RANK) signaling. J Cell Physiol. 2015;230(12):2951–2960. doi:10.1002/jcp.25024
13. Hameed A, Brady JJ, Dowling P, Clynes M, O’Gorman P. Bone disease in multiple myeloma: pathophysiology and management. Cancer Growth Metastasis. 2014;7:33–42. doi:10.4137/CGM.S16817
14. Johnson DC, Weinhold N, Mitchell J, et al. Genetic factors influencing the risk of multiple myeloma bone disease. Leukemia. 2016;30(4):883–888. doi:10.1038/leu.2015.342
15. Haaber J, Abildgaard N, Knudsen LM, et al. Myeloma cell expression of 10 candidate genes for osteolytic bone disease. Only overexpression of DKK1 correlates with clinical bone involvement at diagnosis. Br J Haematol. 2008;140(1):25–35. doi:10.1111/j.1365-2141.2007.06871.x
16. Zhou F, Meng S, Song H, Claret FX. Dickkopf-1 is a key regulator of myeloma bone disease: opportunities and challenges for therapeutic intervention. Blood Rev. 2013;27(6):261–267. doi:10.1016/j.blre.2013.08.002
17. Longo V, Brunetti O, D’Oronzo S, Dammacco F, Silvestris F. Therapeutic approaches to myeloma bone disease: an evolving story. Cancer Treat Rev. 2012;38(6):787–797. doi:10.1016/j.ctrv.2012.03.004
18. Terpos E, Kastritis E, Dimopoulos MA. Prevention and treatment of myeloma bone disease. Curr Hematol Malig Rep. 2012;7(4):249–257. doi:10.1007/s11899-012-0135-0
19. Lu C, Meng S, Jin Y, et al. A novel multi-epitope vaccine from MMSA-1 and DKK1 for multiple myeloma immunotherapy. Br J Haematol. 2017. doi:10.1111/bjh.14686
20. Nooka AK, Kastritis E, Dimopoulos MA, Lonial S. Treatment options for relapsed and refractory multiple myeloma. Blood. 2015;125(20):3085–3099. doi:10.1182/blood-2014-11-568923
21. Terpos E, Heath DJ, Rahemtulla A, et al. Bortezomib reduces serum dickkopf-1 and receptor activator of nuclear factor-kappaB ligand concentrations and normalises indices of bone remodelling in patients with relapsed multiple myeloma. Br J Haematol. 2006;135(5):688–692. doi:10.1111/j.1365-2141.2006.06356.x
22. Paiva B, Chandia M, Vidriales MB, et al. Multiparameter flow cytometry for staging of solitary bone plasmacytoma: new criteria for risk of progression to myeloma. Blood. 2014;124(8):1300–1303. doi:10.1182/blood-2014-04-567909
23. Rajkumar SV, Dimopoulos MA, Palumbo A, et al. International Myeloma Working Group updated criteria for the diagnosis of multiple myeloma. Lancet Oncol. 2014;15(12):e538–e548. doi:10.1016/S1470-2045(14)70442-5
24. Zamagni E, Cavo M. The role of imaging techniques in the management of multiple myeloma. Br J Haematol. 2012;159(5):499–513. doi:10.1111/bjh.12007
25. Greipp PR, San Miguel J, Durie BG, et al. International staging system for multiple myeloma. J Clin Oncol. 2005;23(15):3412–3420. doi:10.1200/JCO.2005.04.242
26. Mikhael JR, Dingli D, Roy V, et al. Management of newly diagnosed symptomatic multiple myeloma: updated Mayo Stratification of Myeloma and Risk-Adapted Therapy (mSMART) consensus guidelines 2013. Mayo Clinic Proc. 2013;88(4):360–376. doi:10.1016/j.mayocp.2013.01.019
27. Oken MM, Creech RH, Tormey DC, et al. Toxicity and response criteria of the Eastern Cooperative Oncology Group. Am J Clin Oncol. 1982;5(6):649–655.
28. Muchtar E, Gatt ME, Rouvio O, et al. Efficacy and safety of salvage therapy using Carfilzomib for relapsed or refractory multiple myeloma patients: a multicentre retrospective observational study. Br J Haematol. 2016;172(1):89–96. doi:10.1111/bjh.13799
29. Rajkumar SV. Updated diagnostic criteria and staging system for multiple myeloma. Am Soc Clin Oncol Educ Book. 2016;35:e418–423. doi:10.1200/EDBK_159009
30. Rajkumar SV. Evolving diagnostic criteria for multiple myeloma. Hematology Am Soc Hematol Educ Program. 2015;2015:272–278. doi:10.1182/asheducation-2015.1.272
31. Kuo KH, Callum JL, Panzarella T, et al. A retrospective observational study of leucoreductive strategies to manage patients with acute myeloid leukaemia presenting with hyperleucocytosis. Br J Haematol. 2015;168(3):384–394. doi:10.1111/bjh.13146
32. Anderson KC, Alsina M, Atanackovic D, et al. Multiple Myeloma, Version 2.2016: clinical practice guidelines in oncology. J Natl Compr Canc Netw. 2015;13(11):1398–1435. doi:10.6004/jnccn.2015.0167
33. Yoo C, Yoon DH, Suh C. Serum beta-2 microglobulin in malignant lymphomas: an old but powerful prognostic factor. Blood Res. 2014;49(3):148–153. doi:10.5045/br.2014.49.3.148
34. Delgado-Calle J, Bellido T, Roodman GD. Role of osteocytes in multiple myeloma bone disease. Curr Opin Support Palliat Care. 2014;8(4):407–413. doi:10.1097/SPC.0000000000000090
35. Ji B, Genever PG, Patton RJ, Fagan MJ. Mathematical modelling of the pathogenesis of multiple myeloma-induced bone disease. Int J Numer Method Biomed Eng. 2014;30(11):1085–1102. doi:10.1002/cnm.v30.11
36. Poudel B, Mittal A, Shrestha R, Farooqui MS, Yadav NK, Shukla PS. Liver involvement in multiple myeloma: a hospital based retrospective study. Asian Pac J Cancer Prev. 2012;13(5):2153–2155. doi:10.7314/APJCP.2012.13.5.2153
37. Ichikawa H, Aggarwal BB. Guggulsterone inhibits osteoclastogenesis induced by receptor activator of nuclear factor-kappaB ligand and by tumor cells by suppressing nuclear factor-kappaB activation. Clin Cancer Res. 2006;12(2):662–668. doi:10.1158/1078-0432.CCR-05-1749
38. Fonseca R, Harrington D, Oken MM, et al. Biological and prognostic significance of interphase fluorescence in situ hybridization detection of chromosome 13 abnormalities (delta13) in multiple myeloma: an eastern cooperative oncology group study. Cancer Res. 2002;62(3):715–720.
39. Facon T, Avet-Loiseau H, Guillerm G, et al. Chromosome 13 abnormalities identified by FISH analysis and serum beta2-microglobulin produce a powerful myeloma staging system for patients receiving high-dose therapy. Blood. 2001;97(6):1566–1571. doi:10.1182/blood.V97.6.1566
40. Teoh PJ, Chung TH, Sebastian S, et al. p53 haploinsufficiency and functional abnormalities in multiple myeloma. Leukemia. 2014;28(10):2066–2074. doi:10.1038/leu.2014.102
41. Grzasko N, Hus M, Pluta A, et al. Additional genetic abnormalities significantly worsen poor prognosis associated with 1q21 amplification in multiple myeloma patients. Hematol Oncol. 2013;31(1):41–48. doi:10.1002/hon.v31.1
42. Smadja NV, Bastard C, Brigaudeau C, Leroux D, Fruchart C, Groupe Francais de Cytogenetique H. Hypodiploidy is a major prognostic factor in multiple myeloma. Blood. 2001;98(7):2229–2238. doi:10.1182/blood.V98.7.2229
43. Luton D, Delezoide AL, Leguy MC, et al. Foetal serum but not urinary beta2-microglobulin correlates with histological injury to the kidney. Clin Biochem. 2013;46(15):1607–1610. doi:10.1016/j.clinbiochem.2013.04.017
44. Munshi NC, Anderson KC, Bergsagel PL, et al. Consensus recommendations for risk stratification in multiple myeloma: report of the International Myeloma Workshop Consensus Panel 2. Blood. 2011;117(18):4696–4700. doi:10.1182/blood-2010-10-300970
45. Kounis NG, Soufras GD, Tsigkas G, Hahalis G. White blood cell counts, leukocyte ratios, and eosinophils as inflammatory markers in patients with coronary artery disease. Clin Appl Thromb Hemost. 2015;21(2):139–143. doi:10.1177/1076029614531449
46. Yuksel OH, Verit A, Sahin A, Urkmez A, Uruc F. White blood cell counts and neutrophil to lymphocyte ratio in the diagnosis of testicular cancer: a simple secondary serum tumor marker. Int Braz J Urol. 2016;42(1):53–59. doi:10.1590/S1677-5538.IBJU.2014.0593
 © 2019 The Author(s). This work is published and licensed by Dove Medical Press Limited. The full terms of this license are available at https://www.dovepress.com/terms.php and incorporate the Creative Commons Attribution - Non Commercial (unported, v3.0) License.
By accessing the work you hereby accept the Terms. Non-commercial uses of the work are permitted without any further permission from Dove Medical Press Limited, provided the work is properly attributed. For permission for commercial use of this work, please see paragraphs 4.2 and 5 of our Terms.
© 2019 The Author(s). This work is published and licensed by Dove Medical Press Limited. The full terms of this license are available at https://www.dovepress.com/terms.php and incorporate the Creative Commons Attribution - Non Commercial (unported, v3.0) License.
By accessing the work you hereby accept the Terms. Non-commercial uses of the work are permitted without any further permission from Dove Medical Press Limited, provided the work is properly attributed. For permission for commercial use of this work, please see paragraphs 4.2 and 5 of our Terms.