Back to Journals » International Journal of General Medicine » Volume 13
Voluntary Blood Donation Knowledge, Attitudes, and Practices in Central Ethiopia
Authors Beyene GA
Received 15 January 2020
Accepted for publication 20 February 2020
Published 4 March 2020 Volume 2020:13 Pages 67—76
DOI https://doi.org/10.2147/IJGM.S246138
Checked for plagiarism Yes
Review by Single anonymous peer review
Peer reviewer comments 2
Editor who approved publication: Dr Scott Fraser
Girma Alemayehu Beyene
Department of Public Health, College of Health Science and Medicine, Wolkite University, Wolkite, Ethiopia
Correspondence: Girma Alemayehu Beyene
Department of Public Health, College of Health Science and Medicine, Wolkite University, Wolkite PO Box 07, Ethiopia
Tel +251911056495
Email [email protected]
Background: Increasing the availability of safe blood is a major challenge in developing countries. Given the scant amount of community-based data in Africa, this study examines the knowledge, attitudes, and practices of blood donation of Ethiopian adults.
Methods: A cross-sectional study was conducted on 421 adult residents of Adama town using face-to-face interviews with translated questionnaires. Knowledge and attitude levels were assessed using a set of questions and those who answered above mean for knowledge and attitude questions were categorized as above-average knowledge level and favorable attitude, respectively. The data were coded and entered into EPI Info™ version 7, transferred to SPSS version 25 for cleaning and analysis. All variables with p< 0.25 in the bivariable analysis were examined as candidate variables in the multivariable logistic regression models.
Results: Less than half, 47% (95% CI: 42– 52%) of the study participants have above-average knowledge level about blood donation and 48% (95% CI: 43– 53%) have favorable attitudes towards blood donation. Only 17% (95% CI: 13– 21%) of study participants ever donated blood of which 14.6% of them donated for replacement and less than 2% (1.95%) are voluntary donors. Younger age of 18– 25 AOR: 95% CI: 3.40 (1.30, 12.43), having good knowledge AOR: 95% CI: 2.21 (1.26, 3.89) and favorable attitude AOR: 95% CI: 10.25 (4.90, 21.44) were factors independently associated with blood donation practice.
Conclusion: The level of blood donation practiced in the study area is low. Low knowledge and poor attitudes are independent predictors of low inclination to donate, so awareness creation and improving attitudes in blood donation campaigns, particularly among older people is necessary to increase voluntary blood donation.
Keywords: blood donation, voluntary, knowledge, attitude, practice, health services, Africa, epidemiology
Introduction
Blood donation is a gift of life that improves health and reduces premature mortality but many patients in need of blood transfusion do not have timely access to safe blood. An adequate and sustainable supply of safe blood can be assured by non-remunerated voluntary and unpaid blood donors as the rate of transfusion transmissible infection is lowest among them. However, in developing countries, there is a great challenge of availing safe and adequate blood.1,2
Globally, around 112.5 million units of donated blood are collected every year. Nearly half of these are collected in high-income countries and the average blood donation rate is more than 9 times greater in high-income countries than in low-income countries. Particularly, Sub-Saharan Africa faces great challenges not only in the shortage of blood but also in the safety of blood.3,4
The World Health Organization (WHO) urged all countries to obtain their blood supplies from voluntary, non-remunerated donors by the year 2020. However, 40 countries in Africa have donation rates of less than the WHO threshold level of 1% which is required to meet the most basic blood requirements. Many countries in Sub-Saharan Africa, still unable to meet the minimum need for blood transfusions from all sources combined.4–7
According to a report from the Ethiopian Ministry of Health, Ethiopia collected 223,000 units of blood in 2019/20, meeting only 22% of its need as per the standard of the World Health Organization. Studies conducted in different parts of Ethiopia have reported lifetime blood donation rates ranging from 18.4% to 26.4% among the general public and relatively higher rate among students and healthcare professionals ranging from 23.6% to 32.6% although the majority of the studies showed high levels of knowledge and favorable attitudes.8–12 Studies from the Middle East and South Asia have reported much higher lifetime blood donation levels ranging from 43.4% to 61.2% and very high knowledge and attitude levels.13–17
Lack of information and understanding about the need and process of blood donation, inadequate knowledge regarding the benefit of blood donation, misconceptions and perceived negative health effects caused by donation, and negative attitudes are the most frequently revealed reasons that discourage individuals from donating blood.17,18 Therefore, improving the level of knowledge and attitude towards blood donation in the community is essential to ensure safe and adequate blood supply.19,20
Limited studies have described the level of knowledge, attitude, and practice of voluntary blood donation in developing countries and Ethiopia, even those few studies were conducted among students and healthcare professionals using only quantitative methods.11,21-23 No study is available in our setting and this study tried to fill the knowledge gap by conducting the survey in a community setting and also supplementing the finding with some open-ended questions so as to understand community perception about blood donation.
Therefore, the aim of this study is to explore the knowledge, attitudes and practice towards voluntary blood donation and associated factors among adults in Adama town. The finding of the study will be used as a baseline to evaluate the effectiveness of an intervention we are planning to implement which will reduce misconceptions and misunderstanding, improve knowledge, and enable people to donate blood voluntarily and regularly.
Materials and Methods
Study Area and Period
The study was conducted in Adama town, Oromia regional state, central Ethiopia, 99-km Southeast of the national capital, Addis Ababa. According to the Ethiopian central statistics agency, 2017 projected total population of Adama town is 355,475 of which 174,089 are males and 181,386 are females.24 The town is organized into six sub-cities and 18 kebeles (lowest administrative unit in Ethiopia). The study was conducted from May to June 2019.
Study Design and Population
Community-based cross-sectional study design was used. All adults aged 18 to 65 years residing in the town for at least 6 months were the source population.
Exclusion Criteria
Study participants who had a serious illness and unable to communicate during the data collection period were excluded from the study.
Sample Size
The sample size was determined using Epi Info 7 ™ StatCalc25 functions for population survey taking the prevalence of favorable attitude (52.5%) for blood donation from a previous study19 which gave the largest sample size. Using 95% CI and a 5% margin of error and considering a 10% non-response rate, the sample size was found to be 421.
Sampling Technique and Procedures
The multistage sampling technique was used with sub-cities as primary sampling units (PSU) and kebeles (the lowest administrative unit in Ethiopia) within selected sub-cities as the secondary sampling units (SSU). From the six sub-cities of the town, three sub-cities (namely Dabe, Aba Geda and Denbela) were selected by simple random sampling techniques using lottery method and two kebeles from each of the selected sub-cities were selected randomly. Households were selected proportionally from the selected kebeles using a systematic sampling technique. The sampling interval (K) value was calculated for each selected kebele dividing the total households of kebele to their corresponding proportional sample size calculated for each kebele (Figure 1).
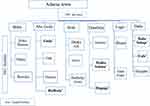 |
Figure 1 Sampling procedures for study on voluntary blood donation knowledge, attitudes, and practices in Central Ethiopia. |
Data Collection Techniques and Procedures
Data were collected by face-to-face interviews using a structured and semi-structured pre-tested questionnaire developed after an extensive review of related literature.8,10,11,14,21–23,26-29 The questionnaire was first prepared in English and translated to Amharic, then translated back to English by another person to check for its consistency. The questionnaire had four sections comprising: socio-demographic factors, eight knowledge questions, six attitude questions, and five practice questions. Additionally, open-ended questions were also used to understand the perceptions and feelings of the study participants about blood donation. Three diploma nurses and two Public health professionals were recruited and trained as data collectors and supervisors, respectively.
Donation is considered voluntary and non-remunerated if the person gives blood with his/her own free will and receives no payment for it, either in cash or kind which could be considered a substitute for money. Replacement donation is when it is required for a member of a family or when someone donates blood with an intention to replace the blood their family member has received. In order to measure knowledge level, multiple questions were used which includes minimum criteria for donating blood, possible health benefit and risk of blood donation, number of patients benefiting from a single unit of donated blood, the volume of blood collected in single donation, minimum interval of blood donation, best source of blood donors. Those who scored mean and above for knowledge questions were categorized as having above-average knowledge level, otherwise poor knowledge level.12 The attitude was measured using six questions regarding the general perception about blood donation, intention and willingness to donate blood in the future. The result was dichotomized based on mean score, those who scored above mean for attitude questions were labeled as having a favorable attitude, otherwise unfavorable attitude.19 Those who donated blood at least once in their lifetime were labeled as practicing blood donation.11
Data Management and Analysis
The training was given for the data collectors and supervisors, all completed questionnaires were reviewed and cross-checked for completeness and consistency by the supervisors and all the necessary feedback was given to the data collectors immediately. Data documentation sheet was prepared and used to make data entry form in Epi Info 7 and additionally, the check commands were applied in order to restrict out of range and illegal values. After data were coded and entered into EPI Info ™ version 7, then transferred to Statistical Package for Social Science (SPSS) version 25 for cleaning and analysis. Frequencies and percentages for categorical variables and means and standard deviations for numerical variables were computed and results were presented using tables and narratives. Correlation between knowledge score, attitude score and practice score were done. Binary logistic regression analysis was used to examine the association between the independent variables and the dependent variable. All variables with p-value <0.25 in the bivariable analysis were entered into the final multiple logistic regression model to identify variables independently associated with blood donation. Multivariable logistic regression (backward stepwise likelihood ratio method) was conducted to select factors independently associated with blood donation. The significance of the adjusted Odds Ratio (AOR) was declared at p-value <0.05 and confidence intervals.
Results
Socio-Demographic Characteristic of Respondents
From the total sample size of 421 approached, 410 of them accepted to participate in the study, making a response rate of 97.4%. The minimum and maximum age of respondents were 18 years and 59 years, mean ± standard deviation (SD) of the age of respondents were (31.92 ± 8.17). The majority (41%) of respondents were in the age group of 26–35 years. Among the study participants, 50.5% of them were males and the remaining 49.5% of them were females. More than seven in 10 (71.7%) of respondents were married and more than third (37.6%) of study participants were followers of orthodox religion. Regarding the educational status majority (37.3%) of them attained secondary education followed by those who have a diploma or above (29.3%) (Table 1).
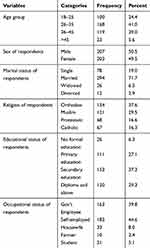 |
Table 1 Sociodemographic Characteristics of Respondents for Study on Voluntary Blood Donation Knowledge, Attitudes, and Practices in Central Ethiopia, 2019 (n = 410) |
Level of Knowledge About Blood Donation
All the study participants know to be in good general health as minimum criteria for blood donation. However, only two-third of them knew the weight and age limit criteria for donating blood. Understanding about the health benefits of donating blood is very limited as only 6.8% of the study participants knew the availability of free medical checkup just by donating blood. Only 10% of the study participants knew the possibility of donating blood every 3 months. More than half (53.2%) of the study participants perceive replacement donation as the best source of blood and only 16.1% knew voluntary blood donation as the best source of blood. Generally, less than half, 47% (95% CI: 42–52%) of the study participants have above-average knowledge levels about blood donation (Table 2). There is no statistically significant correlation between the knowledge score and age of the respondents (r= 0.019, p= 0.704).
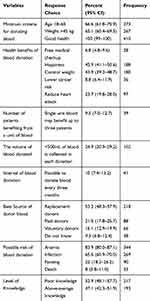 |
Table 2 Blood Donation Knowledge Levels Among Ethiopian Adults, 2019 (n = 410) |
The Attitude of Respondents About Blood Donation
Nearly half (48.5%) of the study participants perceive blood donation as a good idea and 45.9% of them think as neutral and only 5.6% of the participants think of blood donation as a bad thing to do. Two-thirds (66.1%) of the study participants think people should donate blood for their relatives or someone close to them, only 21.5% think people should donate blood for anyone in need. Only two-fifth (39.8%) of the study participants are willing to donate blood in the future. However, four in five (79.8%) % of them intended to donate for their relatives whenever needed and only 28 (17.2%) of them intended to donate voluntarily. Less than half, 48% (95% CI: 43–53%) of the study participants have a favorable attitude towards blood donation (Table 3).
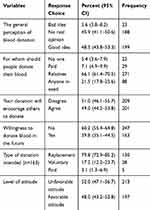 |
Table 3 Blood Donation Attitude Levels Among Ethiopian Adults, 2019 (n = 410) |
There is a weak but statistically significant correlation between knowledge and attitude scores of the study participants (r= 0.116, p= 0.019). However, there is no statistically significant correlation between attitude score and age of the respondents (r= −0.056, p= 0.262).
The Practice of Blood Donation
Only 70 of the study participants (17.1%: 95% CI: 13–21%) ever donated blood in their lifetime, from which 14.6% of them donated as a replacement for blood their relatives received. Among seven whoever donated blood, six (85.7%) of them donated for replacement for the blood their family member or someone close to them received previously and less than 2% (1.95%) of study participants or 11.5% of those who ever donated blood, donated their blood voluntarily to be used by anyone in need. The common reasons mentioned for not donating blood includes no one asked for, inaccessibility of the service, fear of pain, fear of anemia, fear the sight of blood (Table 4). There is positive statistically significant correlation between attitude and practice score (r= 0.331, p= 0.000), knowledge and practice scores of the study participants (r= 0.225, p= 0.000).
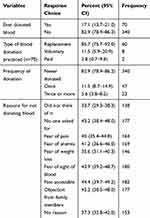 |
Table 4 Blood Donation Practice Among Ethiopian Adults, 2019 (n = 410) |
Factors Associated with the Practice of Blood Donation
Variables with p-value <0.25 in bivariable analysis were selected and entered into the final multiple logistic regression model to identify variables independently associated with blood donation practice.
In multivariable analysis using multiple logistic regression, a young age, having good knowledge and favorable attitude were found to be independently and significantly associated with blood donation practice. After controlling for other independent factors, the study participants who are the younger age group of 18–25 years were more than three times likely to donate blood as compared to those older ages of more than 45 years (AOR: 3.40; 95% CI: 1.30, 12.43).
Controlling other independent factors study participants who have above-average knowledge level about blood donation were more than two times more likely to donate blood as compared to those having poor knowledge (AOR: 2.21; 95% CI: 1.26, 3.89).
Having a favorable attitude was found to be significantly associated with blood donation practice. Those who have favorable attitudes were more than 10 times more likely to donate blood compared to those having unfavorable attitudes (AOR: 10.25; 95% CI: 4.90, 21.44) (Table 5).
 |
Table 5 Factors Associated with the Practice of Blood Donation in Adama Town, 2019 |
There is a diversity of opinions regarding blood donation. Some of the study participants were in favor of blood donation describing how valuable blood is in saving lives, especially during emergency situations. However, other respondents had expressed great misunderstandings about blood donations (eg, need for donors and recipients to have blood relationships, beliefs of having “not enough” blood for oneself, suspicions of a black market) that made them disinclined to donate blood.
Discussion
This study analyzed the level of knowledge, attitude, the practice of blood donation and associated factors at the community level. The finding of the study revealed less than half of the study participants have above-average knowledge level about blood donation, which was consistent with other related community-based studies conducted in Harar town, Eastern Ethiopia where 43.55% of the study participants had good knowledge level about voluntary blood donation.8 However, the result was lower than the study conducted in Aman sub-city, Southwest Ethiopia and Riyadh city, Saudi Arabia where 76% and 78% of respondents had good knowledge about blood donation, respectively. The possible explanation for the discrepancy might be due to the difference in measurement of knowledge level and the difference in the study setting.9,15
Knowledge of study participants on the health benefits of donating blood is very limited, most of them think blood donation benefits only the patient who receives the blood. Only 6.8% of them know they will have free medical checkups, 8.8% knew they will reduce their risk of cancer and 23.7% knew their risk of experiencing a heart attack is reduced as a result of their blood donation. Educating potential donors about health benefits of donating blood, the volume of blood donated and the number of patients benefiting from a single unit of blood donated is very important to improve knowledge about blood donation and hence increase voluntary blood donation.30–32
In this study, less than half (48%) of the study participants have a favorable attitude towards blood donation, as two-third of participants thought they are expected to donate blood only for their relatives. This finding is consistent with the study conducted in Ambo town, Ethiopia where 47.4% of study participants have a positive attitude for blood donation,12 but higher than the study conducted in Harar, Eastern Ethiopia where 32.9% of participants have a positive attitude towards voluntary blood donation.8 The possible explanation for the discrepancy might be due to the difference in the time period in which the study was conducted.
Finding of this study revealed only 17.1% of study participants ever donated blood in their lifetime, which is consistent to the study conducted in Gondar town, Northern Ethiopia and lower than the study conducted in Aman sub-city, West Ethiopia.9,10 However, the rate of voluntary donation is very low as the majority of them donated for replacement purposes, which have its’ own risk. Even though replacing blood in order to get blood from blood bank is not required in our setting, most of the time peoples are donating with the intention to replace blood given for their loved ones. However, the public should be encouraged to donate blood voluntarily and regularly so as to get safe and reliable blood.
Common reasons reported for not donating blood includes no one asked for, not accessible, fear of pain, fear of anemia, fear of weight loss and the fear sight of blood, which is consistent with the study conducted in Eastern Ethiopia, India and Saudi.8,13,16,33 This indicated most reasons peoples fail to donate blood are just misconceptions that could be cleared with appropriate health information and campaign in approaching those potential blood donors. Had blood donation service been more accessible, and appropriate methods used to approach potential donors, the rate of blood donation would have been improved. Health system and health care providers should act on making blood bank service more accessible and should approach potential donors so as to increase the rate of voluntary blood donation.
In this study, from the sociodemographic factors being the young age group of 18–25 years was significantly associated with blood donation practice. This indicated targeting our intervention to older adults would increase the rate of blood donation practice and generate a future pool of regular donors. Furthermore, using younger adults as an advocate for blood donation campaign and engaging them in awareness creation and risk reduction intervention in the community would improve voluntary blood donation.
In multivariable analysis using multiple logistic regression good knowledge and favorable attitude were found to be independently and significantly associated with blood donation practice. This is consistent with comparable studies conducted so far. Our intervention to increase blood donation practice should focus on clearing misconceptions and irrational fear, hence improving the knowledge level of adults and also increasing accessibility of blood bank service and approaching potential donors is essential.
As limitations of the study, the response of the participants might be influenced by social desirability bias, which refers to the tendency of study participants to give socially desirable responses instead of indicating answers that are reflective of their true practice. Respondents who were not donating blood may falsely report they have donated blood as blood donation is socially desired behavior.
Conclusions
The level of knowledge, attitude, and practice of voluntary blood donation are low in the study setting. Knowledge and attitude levels are an independent and significant predictors of blood donation. In order to improve the knowledge and attitude of blood donation comprehensive health information is needed on eligibility criteria for donating blood, health benefits and risks of donating blood, volume of blood donated, number of patients benefiting from single unit of blood donated and importance of blood in saving lives, improving health and wellbeing of the community.
Since most reasons people fail to donate blood are inaccessibility of the service, unreasonable fear and misunderstanding, government and related stakeholders aiming to improve health services should make blood bank service more accessible, health care providers should clear misconceptions with appropriate health information and organizing a well-planned campaign in approaching the potential blood donors.
Abbreviations
AOR, adjusted odds ratio; CI, confidence interval; COR, crude odds ratio; IRB, Institutional Review Board; KAP, knowledge, attitude and practice; PSU, primary sampling unit; SD, standard deviation; SPSS, Statistical Package for Social Science; SSU, secondary sampling unit; WHO, World Health Organization.
Ethical Approval and Consent to Participate
Ethical approval and support letter were obtained from the Institutional Review Board (IRB) of Wolkite University (Ref. No: RCSUIL/110/018) and the Adama town health office before the data collection process started. Verbal informed consent from participants was acceptable and approved by the IRB of Wolkite University and Adama town health office. All the study participants were informed about the aim and purpose of the study, the importance of their participation and verbal informed consent was obtained. Also, the study subjects were informed their right to skip questions or questions that they don’t want to answer partly or fully and to stop the interviewing process at any time if they want to do so and withdraw from the study.
Consent for Publication
Not applicable
Data Sharing Statement
The datasets used and/or analyzed during the current study are available from the corresponding author on reasonable request.
Acknowledgments
I would like to acknowledge the study participants, data collectors, and supervisors who participated in the study. I’m very grateful for my family for their ever-increasing support and encouragement.
Disclosure
The author reports no conflicts of interest in this work.
References
1. World Health Organization. 10 facts on blood transfusion 2017. Available from: http://www.who.int/features/factfiles/blood_transfusion/en/.
2. World Health Organization. WHO calls for increase in voluntary blood donors to save millions of lives 2018. Available from: http://www.who.int/news-room/headlines/10-06-2015-who-calls-for-increase-in-voluntary-blood-donors-to-save-millions-of-lives.
3. World Health Organization. Blood safety and availability 2017. [Available from: http://www.who.int/en/news-room/fact-sheets/detail/blood-safety-and-availability.
4. World Health Organization W. Global Consultation: 100% Voluntary Non–Remunerated Donation of Blood and Blood Components. Melbourne, Australia; 2009. Available from: https://www.who.int/bloodsafety/ReportGlobalConsultation2009onVNRBD.pdf?ua=1.
5. World Health Organization & International Federation of Red Cross and Red Crescent Societies. (2010). Towards 100% Voluntary Blood Donation: A global framework for action. Available from: https://apps.who.int/iris/bitstream/handle/10665/44359/9789241599696_eng.pdf.
6. World Health Organization W. Standards for Blood Banks/Blood Centres and Transfusion Services; 2016.
7. World Health Organization, editor. Blood Donation Success Stories from Countries. World Blood Donor Day - 14 June 2012. Available from: https://www.who.int/worldblooddonorday/media/success_story/en/.
8. Urgesa K, Hassen N, Seyoum A. Knowledge, attitude, and practice regarding voluntary blood donation among adult residents of Harar town, Eastern Ethiopia: a community-based study. J Blood Med. 2017;8:13–20. doi:10.2147/JBM.S121460
9. Mulatu K, Hailu T, Yegezu A, Tena B. Assessment of knowledge, attitude and practice on blood donation in Aman Sub City Residents, South West, Ethiopia, 2015. Health Sci J. 2017;11:1. doi:10.21767/1791-809X
10. Melku M, Terefe B, Asrie F, et al. Knowledge, attitude, and practice of adult population towards blood donation in Gondar Town, Northwest Ethiopia: a community based cross-sectional study. J Blood Transfus. 2016;2016:7949862.
11. Bantayehu D. Knowledge, attitude, and practice of voluntary blood donation and associated factors among health care providers in Addis Ababa health Facilities, Ethiopia. Occup Med Health Affairs. 2014;3:4.
12. Nigatu A, Demissie DB. Knowledge, attitude and practice on voluntary blood donation and associated factors among Ambo University regular students, Ambo Town, Ethiopia. J Community Med Health Educ. 2014;4:315.
13. Meinia SK, Kumar Y, Meinia A, Singh G, Dutt N. A study to assess the knowledge, attitude, and practices about voluntary blood donation amongst the undergraduate medical students in Solan, North India. Int J Med Sci Publ Health. 2016;5(12):2550–2554. doi:10.5455/ijmsph.
14. Alfouzan N. Knowledge. Attitudes, and Motivations towards Blood Donation among King AbdulazizMedical City Population. International Journal of Family Medicine; 2014.
15. Almutairi SH, Almalaq AA, Albalawi YM, Aloufi RM, Al-Mutairi MR, Albiek AF. Assessment of Knowledge, Attitude and Practice (KAP) of Saudi Adult toward Blood Donation in Riyadh City, 2017. Egypt J Hosp Med. 2018;70(3):507–510. doi:10.12816/0043497
16. Alam M, Masalmeh BED. Knowledge, attitudes and practices regarding blood donation among the Saudi population. Saudi Med J. 2004;25(3):318–321.
17. Waheed U, Azmaat M, Zaheer HA. Knowledge, attitude and practices towards blood donation in Pakistan: a nationwide survey. Hematol Transf Int J. 2015;1:4. doi:10.15406/htij.2015.01.00018
18. Zanin TZ, Hersey DP, Cone DC, Agrawal P. Tapping into a vital resource: understanding the motivators and barriers to blood donation in Sub-Saharan Africa. Afr J Emergency Med. 2016;6:70–79. doi:10.1016/j.afjem.2016.02.003
19. Jemberu YA, Esmael A, Ahmed KY. Knowledge, attitude and practice towards blood donation and associated factors among adults in Debre Markos town, Northwest Ethiopia. BMC Hematol. 2016;16:23. doi:10.1186/s12878-016-0062-8
20. Lownik E, Riley E, Konstenius T, Riley W, McCullough J. Knowledge, attitudes and practices surveys of blood donation in developing countries. Vox Sang. 2012;103(1):64–74. doi:10.1111/vox.2012.103.issue-1
21. Elias E, WilhellmussMauka PRN, Damian DJ, Mahande J, Msuya SE. Knowledge, Attitudes, Practices, and Factors Associated with Voluntary Blood Donation Among University Students in Kilimanjaro, Tanzania. 2016. Available from: http://dx.doi.org/10.1155/2016/8546803.
22. Ahmed Z, Zafar M, Khan AA, Anjum MU, Siddique MA. Knowledge, attitude and practices about blood donation among undergraduate medical students in Karachi. Infect Dis Ther. 2014;2:2.
23. Benedict N, Usimenahon A, Alexander NI, Isi A. Knowledge, attitude and practice of voluntary blood donation among physicians in a tertiary health facility of a developing country. J Blood Disord Transf. 2012;3:1. doi:10.4172/2155-9864.1000117
24. Federal Democratic Republic of Ethiopia Central Statistical Agency CE. Population Projection of Ethiopia for All Regions at Wereda Level from 2014–2017; 2013. Available from: http://www.csa.gov.et/index.php/ehioinfo-internal%3Fdownload%3D724:population-projection.
25. Centers for Disease Control and Prevention C. Epi Info™, a Database and Statistics Program for Public Health Professionals. Atlanta, GA: CDC; 2011.
26. Devi HS, Laishram J, Elangbam V. Knowledge, Attitude and Practice (KAP) of Blood Safety and Donation. Indian Medical Gazette; 2012.
27. Salaudeen AG. Knowledge and behavior towards voluntary blood donation among students of a tertiary institution in Nigeria. Niger J Clin Pract. 2011;14(3):303–307. doi:10.4103/1119-3077.86773
28. Gilani I, Kayani ZA, Atique M. Knowledge, attitude and practices (KAP) regarding blood donation prevalent in medical and paramedical personnel. J Coll Phys Surg Pak. 2007;17(8):473–476. doi:10.82007/JCPSP.473476
29. Sabu KM, Remya A, Binu VS, Vivek R. Knowledge, attitude and practice on blood donation among health science students in a University campus, South India. Online J Health Allied Sci. 2011;10:2.
30. Meyers DG, Strickland D, Maloley PA, Seburg J, Wilson JE, McManus BF. Possible association of a reduction in cardiovascular events with blood donation. Heart. 1997;78(2):188–193. doi:10.1136/hrt.78.2.188
31. Bmrs. Health benefits of donating blood 2018. Available from: https://www.brmsonline.com/blog/wellness/healthcare/2018/benefits-of-blood-donation.
32. Yunce M, Erdamar H, Bayram NA, Gok S. One more health benefit of blood donation: reduces acute-phase reactants, oxidants and increases antioxidant capacity. J Basic Clin Physiol Pharmacol. 2016;27(6):653–657. doi:10.1515/jbcpp-2015-0111
33. UMA S, ARUN R, ARUMUGAM P. The knowledge, attitude and practice towards blood donation among voluntary blood donors in Chennai, India. J Clin Diagn Res. 2013;7(6):1043–1046. doi:10.7860/JCDR/2013/4851.3033
 © 2020 The Author(s). This work is published and licensed by Dove Medical Press Limited. The
full terms of this license are available at https://www.dovepress.com/terms.php
and incorporate the Creative Commons Attribution
- Non Commercial (unported, v3.0) License.
By accessing the work you hereby accept the Terms. Non-commercial uses of the work are permitted
without any further permission from Dove Medical Press Limited, provided the work is properly
attributed. For permission for commercial use of this work, please see paragraphs 4.2 and 5 of our Terms.
© 2020 The Author(s). This work is published and licensed by Dove Medical Press Limited. The
full terms of this license are available at https://www.dovepress.com/terms.php
and incorporate the Creative Commons Attribution
- Non Commercial (unported, v3.0) License.
By accessing the work you hereby accept the Terms. Non-commercial uses of the work are permitted
without any further permission from Dove Medical Press Limited, provided the work is properly
attributed. For permission for commercial use of this work, please see paragraphs 4.2 and 5 of our Terms.
