Back to Journals » Patient Related Outcome Measures » Volume 10
Validation study of the Parkinson’s Fatigue Scale in advanced Parkinson’s disease
Authors Martinez-Martin P , Wetmore JB , Arbelo JM, Catalán MJ , Valldeoriola F, Rodriguez-Blazquez C
Received 26 November 2018
Accepted for publication 12 March 2019
Published 17 April 2019 Volume 2019:10 Pages 141—152
DOI https://doi.org/10.2147/PROM.S196042
Checked for plagiarism Yes
Review by Single anonymous peer review
Peer reviewer comments 2
Editor who approved publication: Dr Robert Howland
Pablo Martinez-Martin,1,2 John B Wetmore,1 José Matías Arbelo,3 María José Catalán,4 Francesc Valldeoriola,5 Carmen Rodriguez-Blazquez1,2
1National Center of Epidemiology, Carlos III Institute of Health, Madrid, Spain; 2Center for Networked Biomedical Research in Neurodegenerative Diseases (CIBERNED), Carlos III Institute of Health, Madrid, Spain; 3Movement Disorders Unit, Hospital Universitario Insular de Gran Canaria, Las Palmas de Gran Canaria, Spain; 4Department of Neurology, Hospital Clínico San Carlos, Madrid, Spain; 5Department of Neurology, Hospital Clínico de Barcelona, Barcelona, Spain
Purpose: To validate the Parkinson’s Fatigue Scale (PFS-16) in advanced Parkinson Disease (APD) patients using the scale’s Spanish version.
Patients and methods: In a clinical study for Levodopa-Carbidopa Intestinal Gel (LCIG), 59 patients were assessed over six months using the PFS-16 and other instruments. The psychometric properties of the PFS-16 were then analyzed.
Results: Patients (60.7% men) were aged 68.02±7.43 years. PD duration was 12.57±5.97 years. Median Hoehn and Yahr (HY) stage of patients in “on” was 2 (range: 1–4). There were excellent data quality and acceptability for the PFS-16 as a whole, except for moderate-to-high ceiling effects in its items. Two factors explained 67% of the variance, yet parallel analysis demonstrated the unidimensional nature of the PFS-16, whose internal consistency was satisfactory (Cronbach’s alpha=0.93; item homogeneity coefficient=0.19, and item total-corrected correlations=0.50–0.84). PFS-16 total score showed moderate-to-high correlations with fatigue-specific questions within clinical tools, namely item 20 of the Beck Depression Inventory (rS=0.65) and item 4 of the Non-Motor Symptoms Scale (rS=0.33). Weak-to-moderate correlations were observed between the PFS-16 and measures of anxiety, depression, apathy, and quality of life. There were no significant differences in PFS-16 total scores when grouped by age, sex, time from diagnosis, HY, and CGI-S. After treatment with LCIG, the relative change in PFS-16 total score was −17.6% and the effect size (Cohen’s d) was 0.92. Moderate correlations between changes in the PFS-16 and several other clinical tools were also found.
Conclusion: In APD patients, the PFS-16 showed satisfactory acceptability, internal consistency, construct validity, and responsiveness.
Keywords: Parkinson’s disease, fatigue, Parkinson’s Fatigue Scale, PFS-16, advanced Parkinson’s disease, psychometric properties
Plain language summary
Causing deterioration of patient health and quality of life, fatigue is a prominent symptom of Parkinson’s disease (PD). Measuring this symptom is relevant to the management of the disease, but doctors can only know about the presence and severity of fatigue through patients’ reporting. The Parkinson’s disease Fatigue Scale-16 items (PFS-16) was designed as self-applied scale (“patient-reported outcome,” PRO) to measure and monitor the course of fatigue in a valid and reliable manner. The PFS-16 showed satisfactory metric properties and has been recommended for use in PD by a task force of the Movement Disorder Society.
The PFS-16 was developed for English-speaking populations, and it was validated in a cohort of PD patients. Translation, cross-cultural adaptation, and validation analyses are needed to make a PRO available to populations other than the one in which it was originally developed. As a result, researchers must explore and establish the equivalence between multiple versions of a clinical rating scale.
In the present study, the measurement properties of the PFS-16 were analyzed in a group of Spanish PD patients who were considered to have “advanced PD” and needed treatment with levodopa-carbidopa intestinal gel (LCIG). The characteristics of this sample made it convenient to check how the scale performs in this specific population, rather than in the general PD population. Using the methodology and statistical analyses relevant to this goal, the authors demonstrated that the PFS-16 performs as a feasible, reliable, valid, and sensitive measure of fatigue in advanced PD patients.
Introduction
While fatigue has been shown to affect 7–45% of the general population,1–3 this crippling non-motor symptom is estimated to affect 33–58% of patients with Parkinson’s disease (PD).4–7 However, figures in some studies can be biased due to the challenging nature of defining this disorder.7,8 Even though there is no standardized definition of fatigue, despite its inclusion among the diagnostic criteria for both depression and anxiety in the Diagnostic and Statistical Manual of Mental Disorders, fifth edition,7,9,10 specific criteria for diagnosing fatigue in PD have recently been proposed.8
Although frequently confounded with depression and excessive sleepiness, fatigue has been shown to be related to anxiety, apathy, motor impairment, pain, and cognitive deficits, leading to drastic decreases in the health-related quality of life (QoL) of patients with PD.8,11–14 Suggesting that it could be treated by increasing brain levels of serotonin and dopamine, fatigue has been linked both to the reduced serotonergic function in the basal ganglia and limbic areas of the brain and to the dopamine deficiency characteristic of PD.7,15,16 Yet, even though insights exist into its pathophysiology, fatigue is often overlooked and underdiagnosed in PD.17
There are many generic rating scales to assess fatigue; however, the Parkinson’s Fatigue Scale (PFS-16) is the only PD-specific scale.18 This patient-based, 16-item scale assesses the presence and severity of fatigue in PD patients, captures the physical aspects of fatigue and its impact on activities of daily living, and purposefully excludes fatigue’s mental aspects. In previous studies, it has shown satisfactory internal consistency, stability, and construct validity,18–24 and is recommended by the Movement Disorder Society Task Force.25
Using its Spanish version, this study presents the first attempt to both validate the PFS-16 in patients with advanced PD (APD) and present data about responsiveness after a pharmacologic intervention.
Material and methods
Design
The ADEQUA study (ClinicalTrials.gov Identifier: NCT02289729) focused on the treatment of APD using levodopa-carbidopa intestinal gel (LCIG). The data for the present study are derived from this national, multi-center study.26
Patients
Patients were included in the ADEQUA study for LCIG treatment by their neurologists if they were aged ≥18 years and had advanced levodopa-responsive PD with at least 2 hrs of daily “Off” time or 2 hrs of daily dyskinesia that could not be controlled by conventional treatment options. Participants were also required to be free from severe cognitive deterioration (Mini-Mental State Examination score ≥26).27
If patients did not meet all inclusion criteria, were not compatible with LCIG treatment according to the drug fact sheet, or did not display appropriate cognitive functioning (Mini-Mental State Examination score <26), they were excluded from the study.
The estimated sample size to achieve the objectives of the ADEQUA study was a minimum of 60 patients. This sample was recruited from November 2014 to April 2016 from several hospitals throughout Spain. A minimal sample of 50 patients was deemed acceptable for the validation study.28
Assessments
Demographic data for sex, age, ethnicity, marital status, employment, education, time from PD diagnosis, and current treatment were collected.
The Parkinson’s Fatigue Scale is a 16-question inventory used to screen for the presence and severity of fatigue in PD patients over the past two weeks. Each item ranges between one (“strongly disagree”) and five (“strongly agree”). While there are three ways to calculate the total score for this clinical instrument,29 the method chosen for the present study was summing all the items because evidence suggests that the dichotomized scoring of the PFS-16 limits the precision and accuracy of this tool.30
Besides the PFS-16, patients were assessed in the “on” state during this study with the following instruments:
Unified Parkinson’s Disease Rating Scale (UPDRS)31 parts III (motor examination) and IV (therapy complications). Part III is composed of 14 items, but there are 27 scores as each item assesses multiple parts of the body. Each score ranges from from 0 (normal) to 4 (severe), and the total score can be between 0 and 108. Part IV includes 11 items (four for dyskinesias, four for fluctuations, and 3 items for other complications), with some items scoring from 0 to 4 and others 0 (no) to 1 (yes). The total score for Part IV ranges from 0 to 23.
Schwab and England Scale (S&E).32 This frequently used, 11-stage scale evaluates the ability to complete activities of daily living in PD patients and meets “recommended” criteria for use in PD.33 Scores range from 0% (completely dependent with vegetative dysfunction, bedridden) to 100% (completely independent, essentially normal).
Hoehn and Yahr (HY).34 This five-level classification system ranks the stages of a patient’s disease progression from one (“unilateral involvement only usually with minimal or no functional disability”) to five (“confinement to bed or wheelchair unless aided”).
Non-motor Symptoms Scale (NMSS).35 The NMSS is a 30-item instrument used to evaluate the burden of non-motor symptoms in PD. This scale is divided into nine domains: cardiovascular, sleep/fatigue, mood/apathy, perceptual problems/hallucinations, attention/memory, gastrointestinal tract, urinary function, sexual function, and miscellaneous.
Clinical Global Impression–Severity Scale (CGI-S).36 This is a generic, seven-point scale used to rate the severity of a patient’s disease state at a given time. This scale ranges from one (“normal/not at all ill”) to seven (“among the most extremely ill patients”).
Beck Anxiety Inventory (BAI).37 Using 21 items, the BAI determines the severity of anxiety over the past week. The total score is calculated by summing the items, which are scored from zero (“not at all”) to three (“severely – it bothered me a lot”). More severe anxiety symptoms are indicated by higher scores.
Beck Depression Inventory II (BDI-II).38 Also composed of 21 items that are scored from zero to three, this inventory measures the severity of depression over the past three weeks. Its total score is calculated by summing the patient’s responses to each item. More severe depressive symptoms are expressed with higher BDI-II scores.
Apathy Scale (AS).39 This 14-question instrument screens and assesses the severity of apathy in PD patients over the past four weeks. Each question is scored from zero (“not at all”) to three (“a lot”), and the total score is calculated by adding the scores from questions 1–8 to the inverse scores from questions 9–14. According to the AS developers, the cutoff score for apathy is 13/14.39
Parkinson’s Disease Questionnaire-39 items (PDQ-39).40 This patient-completed assessment determines the impact of PD on QoL. It consists of 39 questions separated into eight domains: mobility, activities of daily living, emotional well-being, stigma, social support, cognitions, communication, and bodily discomfort.
Zarit Burden Interview (ZBI).41 The ZBI assesses the burden experienced by caregivers of dependent persons with various medical disorders, and it has been validated for caregivers of PD patients.42 This 22-item inventory is scored from one (“never/nothing”) to five (“almost always/extremely”), and its total score is calculated by summing the responses to represent a caregiver’s overall burden.
Levodopa equivalent daily dose (LEDD) was calculated for each patient according to Tomlinson et al43.
Ethical issues
The study was conducted in accordance with the Declaration of Helsinki and with standard operating procedures that guaranteed compliance with Good Clinical Practice, as described in the ICH guidelines. The study was evaluated by the Spanish Agency of Medicines and Medical Devices, and it was approved by the Spanish Autonomous Communities and the Ethics Committees of the participant hospitals. Patients signed their informed consent before inclusion in the study.
Data analysis
Data were anonymized and sent to the National Center Epidemiology at the Carlos III Institute of Health in Madrid, Spain, for analysis. Using the Shapiro-Francia test, it was determined that non-parametric statistics were required for this analysis. Descriptive statistics (measures of central tendency and frequency percentages) were applied to socio-demographic, historical, and evaluative data.
For each item of the PFS-16 and its total score, statistics regarding data quality and acceptability were calculated. These statistics included the percentage of computable scale scores, mean, median, standard deviation, skewness, minimum and maximum values, and floor and ceiling effects. To consider data quality and acceptability satisfactory, missing data should comprise <5% of the data set,44 all possible scores should be observed in the sample, the mean and median of the scale total score should be close (difference of <10% of maximum possible score),45 floor and ceiling effect should be <15%,46 and the skewness values for both items and total score should range from −1 to +1.47
An exploratory factor analysis based on polychoric correlations (due to the non-normality of data according to Mardia’s test) and robust unweighted least squares for factor extraction was performed. Bartlett’s sphericity test and Kaiser-Meyer-Olkin statistic were applied to determine the sample adequacy. In addition, an optimal implementation of parallel analysis for determining the number of dimensions was carried out.
Using Cronbach’s alpha, corrected item-total correlation, and item homogeneity, internal consistency was analyzed. Standard values used for these statistics are: Cronbach’s alpha >0.70,48 corrected item-total correlation ≥0.30,47 and item homogeneity coefficient ≥0.15.49
Convergent validity of the PFS-16 total score with the domains and total scores of the other instruments used in this study was assessed using Spearman’s rank correlation coefficients (rS). Coefficient values of 0.30 to 0.59 were deemed moderate correlations, and values ≥0.60 were deemed high correlations.50
To analyze the differences between groups of sex, age, time from diagnosis, HY stage, and CGI-S in reference to PFS-16 total score, Mann-Whitney and Kruskal-Wallis tests were applied. Significant differences were determined using the magnitude of difference and p-values.51
PFS-16 responsiveness was analyzed using data from baseline and follow-up 6±0.5 months later. The magnitude of difference, relative change (percentage of change), standard error of the difference (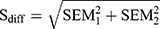 ),52 and effect size for paired samples data53 were applied. Cohen’s d of 0.20–0.49, 0.50–0.79, and ≥80 were considered weak, moderate, and strong, respectively.54 The relationship between changes in PFS-16 total score and the total scores of the other instruments utilized in this study were assessed using Spearman’s rank correlation coefficients.
),52 and effect size for paired samples data53 were applied. Cohen’s d of 0.20–0.49, 0.50–0.79, and ≥80 were considered weak, moderate, and strong, respectively.54 The relationship between changes in PFS-16 total score and the total scores of the other instruments utilized in this study were assessed using Spearman’s rank correlation coefficients.
This data analysis was carried out according to the Consensus‐based standards for the selection of health measurement instruments (COSMIN)55,56 using IBM SPSS (Version 24).
Results
The baseline characteristics of the sample are described in Table 1. In Table 2, the descriptive statistics for the applied measures are summarized.
 | Table 1 Clinical and socio-demographic characteristics of patients at baseline |
 | Table 2 Descriptive statistics of measures in the study |
Two patients (3.3%) were excluded from the analysis due to a lack of responses on the PFS-16; the reasons for this lack of response are unknown. In the remaining sample, 0.31% of the data was missing, but these values were imputed using the mean of the patient’s observed values. Disregarding PFS-16 item 3, in which no patient chose a score of 1, all possible scores were observed in the sample. Item standard deviation ranged from 0.82 to 1.31, floor effects stayed within the standard range for all items, and there were moderate-to-high ceiling effects for most items. Almost all values remained within the accepted range of skewness or were marginally outside (up to an excess of |0.55| points). The PFS-16 total score had a mean and standard deviation of 58.71±12.43, a median of 61.0, a range of 18 to 78, negligible floor and ceiling effects of 1.7% each, and skewness of −0.84 (Table 3).
 | Table 3 Acceptability data of the Parkinson’s Fatigue Scale |
The exploratory factor analysis showed two factors explaining 67% of the variance (Bartlett’s statistic, p=0.00001; Kaiser-Meyer-Olkin test =0.87). The first factor (57.7% of the variance) of the unrotated matrix included all items of the scale, with loads ≥0.58, and the parallel analysis advised considering only one dimension.
Cronbach’s alpha was 0.93, and item homogeneity was 0.19; both were greater than the minimum accepted values of 0.70 and 0.15, respectively. Similarly, all corrected item-total correlations were greater than the standard value of 0.30 (Table 4).
 | Table 4 Corrected item-total correlations |
In terms of convergent validity, the PFS-16 showed a strong correlation with item 20 of the BDI-II (“tiredness or fatigue,” rS=0.65) and a moderate correlation with item 4 of the NMSS (fatigue or lack of energy, rS=0.33). Furthermore, it had moderate correlations with the BAI (rS=0.30), BDI-II (rS=0.48), and PDQ-39 summary index (rS=0.36) and a weak correlation with the AS (rS=0.26). Regarding the PDQ-39 domains, the PFS-16 had moderate correlations with social support (rS=0.31), cognitions (rS=0.35), and communication (rS=0.32) and weak ones with the rest (rS=0.10–0.29). However, the PFS-16 was not significantly correlated with the other measures in the study, including LEDD (Table 5). When considering groups categorized by age (≤60, 61–70, ≥71 years), sex, marital status, education level, time from diagnosis (<10, 10–15, >15 years), HY, and CGI-S, there were no significant differences in PFS-16 total score among them. There was a significant difference between retired patients (79%) and the combination of other employment status (21%; Table 1): 56.74±12.46 vs 66.25±9.28 (Mann-Whitney test, p=0.01).
 | Table 5 Correlation between the Parkinson Fatigue Scale and other measures |
After treatment, significant improvements in the conditions assessed by the clinical measures applied in this study are apparent, except the social support domain of the PDQ-39 and the ZBI (Table 6).
 | Table 6 Differences in assessments between baseline and follow-up |
The standard error of the difference between baseline-follow-up on PFS-16 total score over this 6-month period was 4.3, the relative change was −17.6%, and the effect size was 0.92. Correlations between the changes in the other assessments and the PFS-16 were generally weak or lesser, except for BDI (rS=0.58); NMSS domain 3: mood/apathy (rS=0.49) and total score (rS=0.38); and PDQ-39 mobility (rS=0.57), emotional well-being (rS=0.44), cognitions (rS=0.30), bodily discomfort (rS=0.47), and total score (rS=0.60).
Discussion
The PFS-16 has already been validated in several countries;18–24 however, this study presents the first attempt to validate the scale in APD patients using the Spanish version.
In this study, data quality was considered acceptable, as only two patients were excluded due to a lack of data and because imputation needed to be applied to only 0.3% of the data. However, other studies reported no missing data (Table 7).19,21,22 This difference could be related to the advanced condition of patients in the present study, although other reasons are plausible.
 | Table 7 Summary of the clinimetric attributes explored for the PFS-16* |
Almost all possible values were observed in the sample (except for a score of 1 on item 3), and the relationship between the mean, median, and closeness of item standard deviations were consistent throughout, as was observed in other studies.20,21
While the floor effects remained within the standard range for all items, the ceiling effect was moderate-to-high for most and the skewness values slightly exceeded the standard range in several items. However, the PFS-16 total score displayed negligible floor and ceiling effects and a skewness value within the standard range (Table 3). Therefore, it can be concluded that the scale contains appropriate feasibility and acceptability – a finding consistent with previous validation studies (Table 7).19–21
In agreement with the confirmatory analysis of previous studies,18,22,23 our exploratory factor analysis showed results compatible with the unidimensional nature of the PFS-16, including the amount of variance explained (67% vs 64%).
Furthermore, as measured by Cronbach’s alpha, the internal consistency for the scale in our study (0.93) was in line with those found in previous studies.18–24 Similarly, corrected item-total correlations (Table 4) overlap previous findings.20–23 Item homogeneity (rS=0.19) was found to satisfy the accepted value of ≥0.15, indicating sufficient association among the items.19,22 As a whole, our results demonstrate adequate scaling assumptions and internal consistency for the PFS-16 in APD.
Like Hagell et al49 and others,21,22 we found a weak correlation between the PFS-16 and UPDRS III and IV, whereas a moderate correlation was obtained by other researchers.19,23
Since our analysis, to our knowledge, was the first to be conducted using a sample of APD patients using the PFS-16 and AS, it is challenging the draw conclusions from these results. While significant associations have been found between apathy and fatigue in some studies,57–61 our study and others have shown a loose relationship between these two non-motor symptoms, which are separate disorders (Table 5).8,17,62,63
Nonetheless, the PFS-16 did moderately correlate with BAI and BDI-II, suggesting that fatigue is related to anxiety and depression in PD patients. The highest correlation was found between the PFS-16 and BDI-II item 20, which directly inquired about tiredness and fatigue. In other studies, low-to-high correlations were found between the PFS-16 and depression measures,19–22 and similar findings are observed between the fatigue scale and anxiety assessments.19,21,22 As a whole, these findings suggests that PFS-16 does not discriminate between pure symptoms of fatigue and disorders like anxiety and depression.
Furthermore, the PFS-16 was moderately correlated with item 4 of the NMSS (rS=0.33), which directly asked about fatigue or lack of energy. A measure of daytime sleepiness was not included, and this deficit is recognized as a limitation in the present study due to the potential overlap between fatigue and sleepiness.
Prior research has shown that anxiety, depression, and fatigue are negatively associated with QoL and are extensively-comorbid non-motor symptoms of PD.6,13,64,65 As such, our study found a moderate correlation between PFS-16 and PDQ-39 summary index and with its domains of social support, cognitions, and communication, suggesting an association of these factors with fatigue’s effect on QoL in APD. Other studies have found a moderate or close relationship between PFS-16 and QoL measures,22,24,66,67
We found that sex, age, education level, time from diagnosis, HY, LEDD, and CGI-S were not related to the presence or severity of fatigue – findings shared with other studies and indicative of a weak discriminant validity of the scale for these groupings.19–23,58 Marital status showed no significant differences in the PFS-16 total score. A significant difference was found between retired and other employment status, but the meaning of this finding is uncertain given the diversity of situations included in the latter group and its small size.
With an acceptable precision value, a strong effect size, and a sizable percentage of relative change, the PFS-16 demonstrated satisfactory performance and reliability following longitudinal analysis. Specifically, this can be derived from the standard error of the difference value, which was around one-third of the baseline standard deviation.
Longitudinal analysis even showed weak-to-moderate correlations with changes in several of the clinical assessments applied in this study – namely, BDI-II; NMSS domain 3 and total score; and PDQ-39 total score and its domains of mobility, emotional well-being, cognitions, and bodily discomfort. This would suggest a potential relationship between the improvement of fatigue and these other aspects. It was also found that, following LCIG treatment, PFS-16 total score was significantly lower (four times the SED; a large effect size) – a finding consistent with another clinical trial that found improvement of physical fatigue with levodopa.15
This study has, at least, two relevant limitations: the relatively small sample size and the use of data from a study not designed for the validation of the PFS-16. Nonetheless, it provides information on the responsiveness of this scale and its performance in a scenario not previously explored (APD).
Conclusions
Fatigue is a disabling non-motor symptom of PD that severely deteriorates patients’ ability and QoL. Therefore, it is necessary to have valid clinical tools to assess fatigue in PD. The present study found that the Spanish version of PFS-16, as a whole, possesses satisfactory acceptability, reliability, construct validity, and responsiveness in the assessment of physical fatigue in patients with APD.
Abbreviation list
APD, Advanced Parkinson’s disease; AS, Apathy scale; BAI, Beck Anxiety Inventory; BDI-II, Beck Depression Inventory-II; LCIG, Levodopa-Carbidopa Intestinal Gel; CGI-S, Clinical Global Impression–Severity; HY, Hoehn & Yahr stage; LEDD, Levodopa equivalent daily dose; NMSS, Non-Motor Symptoms Scale; PD, Parkinson’s disease; PDQ-39, Parkinson’s Disease Questionnaire-39 items; PFS-16, Parkinson’s Fatigue Scale; QoL, Health-related quality of lifep; S&E, Schwab and England Scale; UPDRS, Unified Parkinson’s Disease Rating Scale; ZBI, Zarit Burden Inventory.
Data sharing statement
The datasets generated and/or analyzed during the current study are available from the corresponding author on reasonable request.
Acknowledgments
The authors would like to acknowledge the members of the ADEQUA Study Group responsible for recruitment in the clinical centers: Virgen de las Nieves Hospital: Francisco Escamilla Sevilla; Torrecárdenas Hospital: Jesús Olivares; Burgos Hospital Center: Esther Cubo; Arquitecto Marcide Hospital: Diego Santos; Son Espases Hospital: Bárbara Vives; Puerta del Mar Hospital: Miguel Moya, Raúl Espinosa Rosso; Santa Creu i Sant Pau Hospital: Berta Pascual; Vall d’Hebron Hospital: Oriol de Fabregues; Valladolid Hospital: Javier Marco; Elche General Hospital: María Álvarez, Eric Freire; La Fe Hospital: Irene Martínez; Santa Lucía Hospital: Juan José Soria; Navarra Hospital Center: Pedro Luis Clavero, Icíar Gastón; San Pedro Alcántara Hospital: Gonzalo Gámez-Leyva, Montserrat Gómez; Bellvitge Hospital: Matilde Calopa; Parc Taulí Hospital: Tania Delgado.
Author contributions
The persons in the list of authors of this manuscript meet the following requirements:
- They did substantial contributions to conception and design, data acquisition, or data analysis and interpretation;
- They drafted the article or critically revised it for important intellectual content;
- They gave their final approval of the version to be published; and
- They agree to be accountable for all aspects of the work in ensuring that questions related to the accuracy or integrity of the work are appropriately investigated and resolved.
Disclosure
P. Martinez-Martin received honoraria from Editorial Viguera for lecturing in courses; International Parkinson and Movement Disorder Society for management of the Program on Rating Scales; Air Liquide, HM Hospitales de Madrid, and Zambon for advice in clinic epidemiological studies; license fee payments for the King’s Parkinson’s Disease Pain scale; and grant from the International Parkinson and Movement Disorder Society to attend the congress of the society in 2017. J.M. Arbelo González has received honoraria from AbbVie, Zambon, Bial, and Teva. M. J. Catalán has received honoraria for speaking services and research from AbbVie Laboratories and Merz. F. Valldeoriola has received honoraria for speaking services and advisory boards from AbbVie, Zambon, Teva, Medtronic, and Boston Scientific. The authors report no other conflicts of interest in this work.
References
1. Lewis G, Wessely S. The epidemiology of fatigue: more questions than answers. J Epidemiol Community Health. 1992;46(2):92–97.
2. Kant IJ, Bültmann U, Schröer KA, Beurskens AJ, Van Amelsvoort LG, Swaen GM. An epidemiological approach to study fatigue in the working population: the Maastricht Cohort Study. Occup Environ Med. 2003;60(Suppl 1):i32–i39.
3. Stadje R, Dornieden K, Baum E, et al. The differential diagnosis of tiredness: a systematic review. BMC Fam Pract. 2016;17(1):147. doi:10.1186/s12875-016-0545-5
4. Karlsen K, Larsen JP, Tandberg E, Jørgensen K. Fatigue in patients with Parkinson’s disease. Mov Disord. 1999;14(2):237–241.
5. Friedman JH, Friedman H. Fatigue in Parkinson’s disease: a nine‐year follow‐up. Mov Disord. 2001;16(6):1120–1122.
6. Shulman LM, Taback RL, Bean J, Weiner WJ. Comorbidity of the nonmotor symptoms of Parkinson’s disease. Mov Disord. 2001;16(3):507–510.
7. Herlofson K, Kluger BM. Fatigue in Parkinson’s disease. J Neurol Sci. 2017;374:38–41. doi:10.1016/j.jns.2016.12.061
8. Kluger BM, Herlofson K, Chou KL, et al. Parkinson’s disease-related fatigue: a case definition and recommendations for clinical research. Mov Disord. 2016;31(5):625–631. doi:10.1002/mds.26511
9.
10. Grace J, Mendelsohn A, Friedman JH. A comparison of fatigue measures in Parkinson’s disease. Parkinsonism Relat Disord. 2007;13(7):443–445. doi:10.1016/j.parkreldis.2006.09.001
11. Rochester L, Hetherington V, Jones D, et al. Attending to the task: interference effects of functional tasks on walking in Parkinson’s disease and the roles of cognition, depression, fatigue, and balance. Arch Phys Med Rehabil. 2004;85(10):1578–1585.
12. Hagell P, Brundin L. Towards an understanding of fatigue in Parkinson disease. J Neurol Neurosurg Psychiatry. 2009;80(5):489–492. doi:10.1136/jnnp.2008.159772
13. Martinez‐Martin P, Rodriguez‐Blazquez C, Kurtis MM, Chaudhuri K. The impact of non‐motor symptoms on health‐related quality of life of patients with Parkinson’s disease. Mov Disord. 2011;26(3):399–406. doi:10.1002/mds.23462
14. Dogan VB, Koksal A, Dirican A, Baybas S, Dirican A, Dogan GB. Independent effect of fatigue on health-related quality of life in patients with idiopathic Parkinson’s disease. Neurol Sci. 2015;36(12):2221–2226. doi:10.1007/s10072-015-2340-9
15. Lou JS, Kearns G, Benice T, Oken B, Sexton G, Nutt J. Levodopa improves physical fatigue in Parkinson’s disease: a double‐blind, placebo‐controlled, crossover study. Mov Disord. 2003;18(10):1108–1114. doi:10.1002/mds.10505
16. Pavese N, Metta V, Bose SK, Chaudhuri KR, Brooks DJ. Fatigue in Parkinson’s disease is linked to striatal and limbic serotonergic dysfunction. Brain. 2010;133(11):3434–3443. doi:10.1093/brain/awq268
17. Friedman JH, Brown RG, Comella C, et al. Fatigue in Parkinson’s disease: a review. Mov Disord. 2007;22(3):297–308. doi:10.1002/mds.21240
18. Brown RG, Dittner A, Findley L, Wessely SC. The Parkinson fatigue scale. Parkinsonism Relat Disord. 2005;11(1):49–55. doi:10.1016/j.parkreldis.2004.07.007
19. Kummer A, Scalzo P, Cardoso F, Teixeira AL. Evaluation of fatigue in Parkinson’s disease using the Brazilian version of Parkinson’s Fatigue Scale. Acta Neurol Scand. 2011;123(2):130–136. doi:10.1111/j.1600-0404.2010.01364.x
20. Hagell P, Rosblom T, Pålhagen S. A Swedish version of the 16‐item Parkinson Fatigue Scale (PFS‐16). Acta Neurol Scand. 2012;125(4):288–292. doi:10.1111/j.1600-0404.2011.01560.x
21. Fu R, Cui SS, Du JJ, et al. Validation of the Parkinson Fatigue Scale in Chinese Parkinson’s disease patients. Brain Behav. 2017;7(6):e00712. doi:10.1002/brb3.712
22. Ozturk EA, Kocer BG, Umay E, Cakci A. Cross-cultural adaptation and psychometric evaluations of the Turkish version of Parkinson Fatigue Scale. Qual Life Res. 2018;27(10):2719–2730. doi:10.1007/s11136-018-1907-3
23. Çilga G, Genç A, Çolakoğlu BD, Kahraman T. Turkish adaptation of Parkinson fatigue scale and investigating its psychometric properties. Int J Rehabil Res. 2019;42(1):20–25. doi:10.1097/MRR.0000000000000314
24. Dagklis IE, Tsantaki E, Kazis D, et al. The Parkinson fatigue scale: an evaluation of its validity and reliability in Greek Parkinson’s disease patients. Neurol Sci. 2019. doi:10.1007/s10072-018-3695-5
25. Friedman JH, Alves G, Hagell P, et al. Fatigue rating scales critique and recommendations by the Movement Disorders Society task force on rating scales for Parkinson’s disease. Mov Disord. 2010;25(7):805–822. doi:10.1002/mds.22989
26. Valldeoriola F, Catalab MJ, Escamilla-Sevilla F, et al. Study on patient‐ and caregiver‐reported symptoms and outcomes with levodopa‐carbidopa intestinal gel for the treatment of advanced Parkinson’s Disease. ADEQUA Study. Mov Disord. 2018;33(Suppl 2):S120.
27. Dubois B, Burn D, Goetz C, et al. Diagnostic procedures for Parkinson’s disease dementia: recommendations from the movement disorder society task force. Mov Disord. 2007;22(16):2314–2324. doi:10.1002/mds.21844
28. Terwee CB, Bot SD, de Boer MR, et al. Quality criteria were proposed for measurement properties of health status questionnaires. J Clin Epidemiol. 2007;60(1):34–42. doi:10.1016/j.jclinepi.2006.03.012
29. Martinez-Martin P, Rodriguez-Blazquez C, Forjaz MJ, Kurtis MM, Skorvanek M. Measurement of nonmotor symptoms in clinical practice. Intern Rev Neurobiol. 2017;133:291–345.
30. Nilsson MH, Bladh S, Hagell P. Fatigue in Parkinson’s disease: measurement properties of a generic and a condition-specific rating scale. J Pain Symptom Manage. 2013;46(5):737–746. doi:10.1016/j.jpainsymman.2012.11.004
31. Fahn S, Elton RL. Members of the UPDRS Development Committee. Unified Parkinson’s Disease Rating Scale. In: Fahn S, Marsden CD, Calne DB, Goldstein M, editors. Recent Developments in Parkinson’s Disease. Vol. 2. Florham Park: Macmillan Healthcare Information; 1987:153–164.
32. Schwab J, England A. Projection technique for evaluating surgery in Parkinson’s disease. In: Gillingham F, Donaldson M, editors. Third Symposium on Parkinson’s Disease. Vol. 232. Edinburgh: Livingston; 1969:152–157.
33. Shulman LM, Armstrong M, Ellis T, et al. Disability rating scales in Parkinson’s disease: critique and recommendations. Mov Disord. 2016;31(10):1455–1465. doi:10.1002/mds.26649
34. Hoehn MM, Yahr MD. Parkinsonism: onset, progression and mortality. Neurology. 1967;17(5):427–442.
35. Chaudhuri KR, Martinez‐Martin P, Brown RG, et al. The metric properties of a novel non‐motor symptoms scale for Parkinson’s disease: results from an international pilot study. Mov Disord. 2007;22(13):1901–1911. doi:10.1002/mds.21596
36. Busner J, Targum SD. The clinical global impressions scale: applying a research tool in clinical practice. Psychiatry (Edgmont). 2007;4(7):28–37.
37. Beck AT, Epstein N, Brown G, Steer RA. An inventory for measuring clinical anxiety: psychometric properties. J Consult Clin Psychol. 1988;56(6):893–897.
38. Beck AT, Steer RA, Brown GK. Manual for the Beck Depression Inventory-II. San Antonio, TX: Psychological Corporation; 1996.
39. Starkstein SE, Mayberg HS, Preziosi T, Andrezejewski P, Leiguarda R, Robinson RG. Reliability, validity, and clinical correlates of apathy in Parkinson’s disease. J Neuropsychiatry Clin Neurosci. 1992;4(2):134–139. doi:10.1176/jnp.4.2.134
40. Peto V, Jenkinson C, Fitzpatrick R, Greenhall R. The development and validation of a short measure of functioning and well being for individuals with Parkinson’s disease. Qual Life Res. 1995;4(3):241–248.
41. Zarit SH, Orr NK, Zarit JM. The Hidden Victims of Alzheimer’s Disease: Families under Stress. New York: New York University Press; 1985.
42. Martínez-Martín P, Forjaz MJ, Frades-Payo B, et al. Caregiver burden in Parkinson’s disease. Mov Disord. 2007;22(7):924–931. doi:10.1002/mds.21355
43. Tomlinson CL, Stowe R, Patel S, Rick C, Gray R, Clarke CE. Systematic review of levodopa dose equivalency reporting in Parkinson’s disease. Mov Disord. 2010;25(15):2649–2653. doi:10.1002/mds.23429
44. Smith SC, Lamping DL, Banarjee S, et al. Measurement of health-related quality of life for people with dementia: development of a new instrument (DEMQOL) and an evaluation of current methodology. Health Technol Assess. 2005;9(10):16–19. doi:10.3310/hta9100
45. Martinez-Martin P, Rodriguez-Blazquez C, Abe K, et al. International study on the psychometric attributes of the non-motor symptoms scale in Parkinson disease. Neurology. 2009;73(19):1584–1591. doi:10.1212/WNL.0b013e3181c0d416
46. McHorney CA, Tarlov AR. Individual-patient monitoring in clinical practice: are available health status surveys adequate? Qual Life Res. 1995;4(4):293–307. doi:10.1007/BF01593882
47. Hobart JC, Riazi A, Lamping DL, Fitzpatrick R, Thompson AJ. Improving the evaluation of therapeutic interventions in multiple sclerosis: development of a patient-based measure of outcome. Health Technol Assess. 2004;8(9):7–10. doi:10.3310/hta8090
48.
49. Clark LA, Watson D. Constructing validity: basic issues in objective scale development. Psychol Assessm. 1995;7:309–319. doi:10.1037/1040-3590.7.3.309
50. Fisk JD, Brown MG, Sketris IS, Metz LM, Murray TJ, Stadnyk KJ. A comparison of health utility measures for the evaluation of multiple sclerosis treatments. J Neurol Neurosurg Psychiatry. 2005;76(1):58–63. doi:10.1136/jnnp.2003.017897
51. Fayers PM, Machin D. Quality of Life: Assessment, Analysis and Interpretation. New Jersey: John Wiley & Sons; 2000:72–90.
52. Fitzpatrick R, Norquist JM, Jenkinson C. Distribution-based criteria for change in health-related quality of life in Parkinson’s disease. J Clin Epidemiol. 2004;57(1):40–44. doi:10.1016/j.jclinepi.2003.07.003
53. Cohen J. Statistical Power Analysis for the Behavioral Sciences.
54. Crosby RD, Kolotkin RL, Williams GR. Defining clinically meaningful change in health-related quality of life. J Clin Epidemiol. 2003;56(5):395–407.
55. Mokkink LB, Terwee CB, Patrick DL, et al. The COSMIN checklist for assessing the methodological quality of studies on measurement properties of health status measurement instruments: an international Delphi study. Qual Life Res. 2010;19(4):539–549. doi:10.1007/s11136-010-9606-8
56. Mokkink LB, Terwee CB, Knol DL, et al. The COSMIN checklist for evaluating the methodological quality of studies on measurement properties: a clarification of its content. BMC Med Res Methodol. 2010;10:22. doi:10.1186/1471-2288-10-22
57. Miwa H, Miwa T. Fatigue in patients with Parkinson’s disease: impact on quality of life. Intern Med. 2011;50(15):1553–1558.
58. Sáez-Francàs N, Hernández-Vara J, Corominas Roso M, Alegre Martín J, Casas Brugué M. The association of apathy with central fatigue perception in patients with Parkinson’s disease. Behav Neurosci. 2013;127(2):237–244. doi:10.1037/a0031531
59. Nodel M, Yakhno N, Medvedeva A, Kulikov M. Apathy in Parkinson’s disease. Front Biol. 2014;9(4):324–331. doi:10.1007/s11515-014-1322-2
60. Cochrane GD, Rizvi S, Abrantes AM, Crabtree B, Cahill J, Friedman JH. The association between fatigue and apathy in patients with either Parkinson’s disease or multiple sclerosis. Parkinsonism Relat Disord. 2015;21(9):1093–1095. doi:10.1016/j.parkreldis.2015.07.007
61. Siciliano M, Trojano L, De Micco R, et al. Motor, behavioural, and cognitive correlates of fatigue in early, de novo Parkinson disease patients. Parkinsonism Relat Disord. 2017;45:63–68. doi:10.1016/j.parkreldis.2017.10.004
62. Ongre SO, Larsen JP, Tysnes OB, Herlofson K. Fatigue in early Parkinson’s disease: the Norwegian ParkWest study. Eur J Neurol. 2017;24(1):105–111. doi:10.1111/ene.13161
63. Aarsland D, Marsh L, Schrag A. Neuropsychiatric symptoms in Parkinson’s disease. Mov Disord. 2009;24(15):2175–2186. doi:10.1002/mds.22589
64. Schrag A, Jahanshahi M, Quinn N. What contributes to quality of life in patients with Parkinson’s disease? J Neurol, Neurosurg Psychiatry. 2000;69(3):308–312. doi:10.1136/jnnp.69.3.308
65. Barone P, Antonini A, Colosimo C, et al. The PRIAMO study: a multicenter assessment of nonmotor symptoms and their impact on quality of life in Parkinson’s disease. Mov Disord. 2009;24(11):1641–1649. doi:10.1002/mds.22643
66. Okuma Y, Kamei S, Morita A, et al. Fatigue in Japanese patients with Parkinson’s disease: a study using Parkinson fatigue scale. Mov Disord. 2009;24(13):1977–1983. doi:10.1002/mds.22731
67. Stocchi F, Abbruzzese G, Ceravolo R, et al. Prevalence of fatigue in Parkinson disease and its clinical correlates. Neurology. 2014;83(3):215–220. doi:10.1212/WNL.0000000000000587
 © 2019 The Author(s). This work is published and licensed by Dove Medical Press Limited. The full terms of this license are available at https://www.dovepress.com/terms.php and incorporate the Creative Commons Attribution - Non Commercial (unported, v3.0) License.
By accessing the work you hereby accept the Terms. Non-commercial uses of the work are permitted without any further permission from Dove Medical Press Limited, provided the work is properly attributed. For permission for commercial use of this work, please see paragraphs 4.2 and 5 of our Terms.
© 2019 The Author(s). This work is published and licensed by Dove Medical Press Limited. The full terms of this license are available at https://www.dovepress.com/terms.php and incorporate the Creative Commons Attribution - Non Commercial (unported, v3.0) License.
By accessing the work you hereby accept the Terms. Non-commercial uses of the work are permitted without any further permission from Dove Medical Press Limited, provided the work is properly attributed. For permission for commercial use of this work, please see paragraphs 4.2 and 5 of our Terms.
