Back to Journals » Clinical Ophthalmology » Volume 10
Use of the phaco tip technique for lens cleavage and removal during cataract surgery
Authors Masuda Y, Oki K, Iwaki H, Okamoto T, Tsuneoka H
Received 19 July 2016
Accepted for publication 3 September 2016
Published 6 October 2016 Volume 2016:10 Pages 1925—1929
DOI https://doi.org/10.2147/OPTH.S117588
Checked for plagiarism Yes
Review by Single anonymous peer review
Peer reviewer comments 2
Editor who approved publication: Dr Scott Fraser
Supplementary video "Use of the phaco tip technique for lens cleavage and removal"
Views: 247377
Yoichiro Masuda,1 Kotaro Oki,2 Hisaharu Iwaki,3 Toshinori Okamoto,1 Hiroshi Tsuneoka4
1Department of Ophthalmology, Jikei University Katsushika Medical Center, 2Oki Eye Surgery Center, 3Iwaki Eye Clinic, 4Department of Ophthalmology, Jikei University School of Medicine, Tokyo, Japan
Abstract: Use of the phaco tip technique for lens cleavage and removal does not require manual hydrodissection using a syringe and cannula, or cortical removal using an irrigation/aspiration tip. The phaco tip is the only surgical instrument required for this technique. Its advantages include maintaining a stable intraocular pressure during cortical cleaving hydrodissection and lens removal, which includes the cortex.
Keywords: cataract surgery, hydrodissection, capsular block syndrome, FLACS, Dewey tip
A Letter to the Editor has been received and published for this article.
Introduction
Normal surgical procedures for cataract removal require lens cortical–capsular cleavage (hydrodissection) using a syringe and cannula, lens nucleus removal using a phacoemulsification tip (phaco tip), and lens cortical removal using an irrigation/aspiration tip (I/A tip). Therefore, this requires the insertion and withdrawal of three different surgical instruments in order to complete these three surgical stages. As a result, this can lead to an increased risk of the collapse of the eye. Multiple studies that have examined manual hydrodissection and hydrodissection-related complications have reported that there is a significant increase in the intraocular pressure (IOP) during the procedures.1–7 Furthermore, when using femtosecond laser-assisted cataract surgery (FLACS), it has been reported that there is a manual hydrodissection induced capsular block syndrome because of the expansion of the endocapsular volume by the laser-induced intracapsular gas and cortical changes.8 Based on these findings, it is suggested that the use of a single instrument for all the three cataract surgical stages would likely improve stability of the IOP during hydrodissection and lens removal, including the cortex. Moreover, it is also likely that the number of complications would be reduced, as the use of a single instrument would also keep the safety irrigation IOP from the phaco tip sleeve which limit is the bottle-height dependent hydrostatic pressure, thereby helping to avoid an excessively high IOP and disturbance of the eye.9,10 In the present article, we describe a novel method that only uses the phaco tip for lens cleavage and removal.
Surgical technique
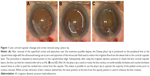
After completion of the initial steps of cataract surgery (incision; 2.7 mm, ophthalmic viscosurgical device injection, and continuous curvilinear capsulorhexis [CCC]), a Dewey phaco tip (0.9 mm diameter; MicroSurgical Technology, Inc., Redmond, WA, USA) with a microsleeve (Alcon Laboratories, Inc., Fort Worth, TX, USA) is inserted into the anterior chamber. When using the phaco tip technique for lens cleavage and removal, once the superficial cortex and epinucleus have been removed to the maximum possible degree, the Dewey phaco tip is positioned on the peripheral lens at the capsulorrhexis edge using zero ultrasound energy. Aspiration of the intraocular fluid is then performed to induce irrigation flow from the sleeve hole to the cortical–capsular layer (Figure 1A). By repeating this procedure at several points on the capsulorhexis edge, the irrigation dynamic pressure cleaves the cortical–capsular layers of the lens, which makes it possible to rotate the lens (which is referred to as the irrigation dynamic pressure hydrodissection [iH]). In this stage, a Constellation Vision System (Alcon Laboratories, Inc.) is used that contains a Dewey phaco tip with a microsleeve. The phacoemulsification parameters are set as follows: vacuum system, Venturi pump; vacuum pressure, 200 mmHg; irrigation pressure, 50 cm H2O; and ultrasound power, zero.
The same parameters are utilized during the second stage of surgery, with the phaco tip used to rotate the lens nucleus circumferentially clockwise and counterclockwise (Figure 1B and C) several times in order to peel the residual lens cortex from the capsule. Consequently, this makes it possible to use the phaco tip to aspirate the majority of the peeled cortex prior to removal of the nucleus.
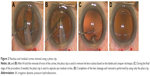
After cortical–capsular cleavage and removal of most of the cortex, the lens nucleus is removed during the third stage of surgery using the phaco tip, with the procedure based on the divide and conquer technique (Figure 2A and B).11 During the final stage of the procedure, if needed, any residual cortex is aspirated using the phaco tip (Figure 2C) followed by removal of the entire lens via the use of only the phaco tip (Figure 2D). In order to prevent damage to the capsule when aspirating the cortex using the Dewey phaco tip: 1) we aspirated only the cortex by peeling it from the capsule, and thus did not aspirate the capsule and 2) as the posterior capsule is easily absorbed by phaco tip in cases with Wieger’s ligament disturbance, infusion misdirection syndrome, etc., we aspirated the residual cortex after intraocular lens implantation using the I/A tip. Video S1 presents the technique in detail. Subsequently, the posterior chamber intraocular lens is implanted in the bag and the procedure is concluded as per the normal surgical procedure.
Discussion
In the current study, only a phaco tip was used for lens cleavage and removal during the phacoemulsification surgeries utilized for the cortical–capsular cleavage, and cortex and nucleus removal. The unique point of this technique is that it removes the cortex in parallel with the iH, which is carried out prior to the lens nucleus phacoemulsification. As the cortical capsular connection adhesive strength affects the time of the iH, the procedure tends to be faster in cases with a harder versus a softer nucleus. As the Dewey tip has a smooth edge that does not cause rupture of the capsule due to attachment, tip placement on the posterior capsule is considered to be safe in cases that have residual cortex after the nucleus removal (Figure 3).12,13 This technique is also unique as it uses a circumferential nucleus rotation approach after the cortical–capsular cleavage. This weakens the lens cortical–capsular adhesive strength, which makes it possible to remove the majority of the cortex prior to the removal of the nucleus. As the aspiration opening of the phaco tip is larger than that of the I/A tip and the phaco tip can easily absorb the posterior capsule in situations in which there is no tension from the nucleus, in the past, the phaco tip has been previously considered to be unsuitable for cortical removal after the removal of the nucleus. In contrast to the common phacoemulsification approach, our technique can overcome this issue by aspirating the cortex prior to removal of the nucleus. Thus, the cortex can be removed without any absorption of the capsule, as the nucleus stretches the capsule centrifugally. Modern phacoemulsification machines provide stable irrigation pressure in the endocapsular space, which makes it possible to avoid the risk for capsular tears when removing the nucleus without the residual cortex.
The cause of capsular block syndrome has been considered to be due to the CCC block by the lens nucleus and the pressure of the trapped irrigation that occurs between the lens nucleus and the posterior capsule. Due to the development of this high pressure, posterior capsule rupture can be elicited during manual hydrodissection. With our technique, however, the cortical removal in parallel with the iH produces space for flow passage around the CCC, thereby contributing to the avoidance of the CCC block during the hydrodissection. In cases undergoing FLACS, it is very important to reduce the intracapsular gas prior to hydrodissection in order to avoid these high-pressure complications. Thus, when the cortical and intracapsular gas removal is performed in parallel with iH, it ensures that FLACS can be performed safely compared to manual hydrodissection.
When using the phaco tip technique for lens cleavage and removal, it is not necessary to perform manual hydrodissection using a syringe and cannula or cortical removal using an I/A tip. Moreover, avoiding the use of multiple surgical instruments and bottle height-dependent maximum irrigation pressure promotes a stable IOP during hydrodissection and lens removal, including the cortex. In addition, the cortical and/or intracapsular gas removal in parallel with iH also contributes to the avoidance of capsular block syndrome. As this approach may be a beneficial option for phacoemulsification surgery, further studies that examine the safety and efficacy of the technique in various other types of cataract cases will need to be undertaken.
Disclosure
The authors report no conflicts of interest in this work.
References
Khng C, Packer M, Fine IH, Hoffman RS, Moreira FB. Intraocular pressure during phacoemulsification. J Cataract Refract Surg. 2006;32(2):301–308. | ||
Hurvitz LM. Posterior capsular rupture at hydrodissection (letter). J Cataract Refract Surg. 1991;17(6):866. | ||
Ota I, Miyake S, Miyake K. Dislocation of the lens nucleus into the vitreous cavity after standard hydrodissection. Am J Ophthalmol. 1996;121(6):706–708. | ||
Miyake K, Ota I, Ichihashi S, Miyake S, Tanaka Y, Terasaki H. New classification of the capsular block syndrome. J Cataract Refract Surg. 1998;24(9):1230–1234. | ||
Yoeh R, Theng J. Capsular block syndrome and pseudoexpulsive hemorrhage. J Cataract Refract Surg. 2000;26(8):1082–1084. | ||
Kawasaki S, Suzuki T, Yamaguchi M, et al. Disruption of the posterior chamber-anterior hyaloid membrane barrier during phacoemulsification and aspiration as revealed by contrast-enhanced magnetic resonance imaging. Arch Ophthalmol. 2009;127(4):465–470. | ||
Kawasaki S, Tasaka Y, Suzuki T, et al. Influence of elevated intraocular pressure on the posterior chamber-anterior hyaloid membrane barrier during cataract operations. Arch Ophthalmol. 2011;129(6):751–757. | ||
Roberts TV, Sutton G, Lawless MA, Jindal-Bali S, Hodge C. Capsular block syndrome associated with femtosecond laser-assisted cataract surgery. J Cataract Refract Surg. 2011;37(11):2068–2070. | ||
Eriksson A, Koranyi G, Sereqard S, Philipson B. Risk of acute suprachoroidal hemorrhage with phacoemulsification. J Cataract Refract Surg. 1998;24(6):793–800. | ||
Matsuo K. [Surgical outcomes of non-hydrodissection phacoemulsification and aspiration: removal of the lens fiber cell layer]. Jpn J Ophthalm Surg. 2008;32:97–102. Japanese. | ||
Gimbel HV. Divide and conquer nucleofractis phacoemulsification: development and variations. J Cataract Refract Surg. 1991;17(3):281–291. | ||
Meyer JJ, Kuo AF, Olson RJ. The risk of capsular breakage from phacoemulsification needle contact with the lens capsule: a laboratory study. Am J Ophthalmol. 2010;149(6):882–886. | ||
Dewey S. Ultrasonic polishing of the posterior capsule with the Dewey radius tip. Tech Ophthalmol. 2006;4(4):139–148. |
Supplementary material
Video S1 Use of the phaco tip technique for lens cleavage and removal.
 © 2016 The Author(s). This work is published and licensed by Dove Medical Press Limited. The full terms of this license are available at https://www.dovepress.com/terms.php and incorporate the Creative Commons Attribution - Non Commercial (unported, v3.0) License.
By accessing the work you hereby accept the Terms. Non-commercial uses of the work are permitted without any further permission from Dove Medical Press Limited, provided the work is properly attributed. For permission for commercial use of this work, please see paragraphs 4.2 and 5 of our Terms.
© 2016 The Author(s). This work is published and licensed by Dove Medical Press Limited. The full terms of this license are available at https://www.dovepress.com/terms.php and incorporate the Creative Commons Attribution - Non Commercial (unported, v3.0) License.
By accessing the work you hereby accept the Terms. Non-commercial uses of the work are permitted without any further permission from Dove Medical Press Limited, provided the work is properly attributed. For permission for commercial use of this work, please see paragraphs 4.2 and 5 of our Terms.