Back to Journals » Clinical Epidemiology » Volume 12
Three Quarters of People with SARS-CoV-2 Infection are Asymptomatic: Analysis of English Household Survey Data
Authors Petersen I , Phillips A
Received 13 August 2020
Accepted for publication 25 September 2020
Published 8 October 2020 Volume 2020:12 Pages 1039—1043
DOI https://doi.org/10.2147/CLEP.S276825
Checked for plagiarism Yes
Review by Single anonymous peer review
Peer reviewer comments 2
Editor who approved publication: Professor Henrik Sørensen
Irene Petersen,1,2 Andrew Phillips3
1Research Department of Primary Care and Population Health, University College London, London, UK; 2Department of Clinical Epidemiology, Aarhus University Hospital, Aarhus, Denmark; 3Institute for Global Health, University College London, London, UK
Correspondence: Irene Petersen
Research Department of Primary Care and Population Health, University College London, Rowland Hill St., London NW3 2PF, UK
Tel +44 020 801 68032
Email [email protected]
Background: To reduce transmission of SARS-CoV-2, it is important to identify those who are infectious. However, little is known about what proportion of infectious people are asymptomatic and potential “silent” transmitters. We evaluated the value of COVID-19 symptoms as a marker for SARS-CoV-2 infection from a representative English survey.
Methods: We used data from the Office for National Statistics Coronavirus (COVID-19) Infection Survey pilot study. We estimated sensitivity, specificity, the proportion of asymptomatic cases (1 – sensitivity), positive predictive value (PPV) and negative predictive value (NPV) of COVID-19 symptoms as a marker of infection using results of the SARS-CoV-2 test as the “gold standard”.
Results: In total, there were 36,061 individuals with a SARS-CoV-2 test between 26 April and 27 June 2020. Of these, 625 (1.7%) reported symptoms on the day of the test. There were 115 (0.32%) with a positive SARS-CoV-2 test result. Of the 115, there were 27 (23.5%) who were symptomatic and 88 (76.5%) who were asymptomatic on the day of the test. Focusing on those with specific symptoms (cough, and/or fever, and/or loss of taste/smell), there were 158 (0.43%) with such symptoms on the day of the test. Of the 115 with a positive SARS-CoV-2, there were 16 (13.9%) reporting symptoms. In contrast, 99 (86.1%) did not report specific symptoms on the day of the test. The PPV for all symptoms was 4.3% and for the specific symptoms 10.1%. The specificity and NPV of symptoms were above 98%.
Conclusion: COVID-19 symptoms are poor markers of SARS-CoV-2. Thus, 76.5% of this random sample who tested positive reported no symptoms, and 86.1% reported none of those specific to COVID-19. A more widespread testing programme is necessary to capture “silent” transmission and potentially prevent and reduce future outbreaks.
Keywords: COVID-19 symptoms, SARS-CoV-2, sensitivity, asymptomatic SARS-CoV-2
Introduction
A major component of the strategy to suppress SARS-CoV-2 transmission is to advise those with symptoms of COVID-19 to self-isolate. However, there are several reports suggesting that not all individuals with a positive SARS-CoV-2 RNA test result have symptoms.1–7 The proportion of asymptomatic cases varies substantially between studies and settings.8 For example, among 262 confirmed cases admitted to hospitals in Beijing 13 (5%) were asymptomatic. In contrast, reports from a small village in Italy suggest that up to 40–75% were asymptomatic.6,9 A study of 13,000 residents in Iceland found 43 out of 100 with a positive SARS-CoV-2 test were asymptomatic.7 There are also several reports of asymptomatic children,4,10,11 but many reports of asymptomatic cases are from selective and relatively small study samples.8
In this analysis of data from a large representative study by the English Office for National Statistics we aimed to understand the value of COVID-19 symptoms as a marker for SARS-CoV-2 infection. We estimated the sensitivity, specificity, positive and negative predictive values of COVID-19 symptoms for SARS-CoV-2 infections as well as the proportion of asymptomatic cases (1 – sensitivity). These basic epidemiological estimates may help to inform the needed scale of future SARS-CoV-2 test programmes.
Methods
Data Source
The Office for National Statistics Coronavirus (COVID-19) Infection Survey pilot is a household survey of private households in England, excluding people living in care homes, other communal establishments and hospitals. The sample for the survey is drawn mainly from the Annual Population Survey (APS). Further information on the survey is available on the study website.12
The survey is ongoing, but for this study, we used data collected in the period 26 April and 27 June 2020 and reported in the statistical bulletin on 9 July 2020 (July edition of the dataset released on 7 July).13 Thus, we used information on the number of individuals with and without symptoms testing positive for SARS-CoV-2 (Table 10 in the dataset)14 and the number of individuals with and without specific symptoms (cough, and/or fever, and/or loss of taste/smell) testing positive for SARS-CoV-2 (Table 11 in the dataset).14
We use the SARS-CoV-2 test results as a proxy for presence of SARS-CoV-2 infection. It is estimated that the sensitivity of the SARS-CoV-2 test used in this survey is between 85% and 95% and the specificity is above 95%.15 The sensitivity is a measures of how often the SARS-CoV-2 test correctly identifies those who had the virus. Specificity measures how often the COVID-19 test correctly identifies those who did not have the virus.
Data Sharing
The data are available under the open government licence.14,16
Analysis
We estimated the sensitivity, specificity, and positive and negative predictive values of COVID-19 symptoms as a marker of infection by using the results of the SARS-CoV-2 test as the “gold standard”. We calculated the proportion among positive test cases who were asymptomatic on the day of the test as: 1 – sensitivity.
The sensitivity was estimated as the number of individuals with COVID19 symptoms who had a positive test (A) over the total number of individuals with a positive test (A + B) (Table 1).
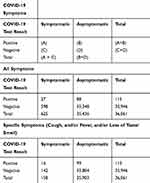 |
Table 1 Individuals Reporting Any Symptoms on the Day of the Test and COVID-19 Test Results |
The specificity was estimated as the number of individuals with a negative test and without symptoms (D) over the total number of individuals with a negative test (C+ D) (Table 1).
The positive predictive value was estimated as the number of individuals with COVID19 symptoms who had a positive test (A) over the total number of individuals with symptoms (A + C) (Table 1).
The negative predictive value was estimated as the number of individuals with no COVID19 symptoms who had a negative test (D) over the total number of individual with no symptoms (B + D) (Table 1).
All analyses were performed in Stata version 16.
Ethics
The Office for National Statistics Coronavirus (COVID-19) Infection Survey has obtained approval by South Central – Berkshire B Research Ethics Committee (20/SC/0195).
Results
In total, there were 36,061 individuals who had a SARS-CoV-2 test between 26 April and 27 June 2020. Of these, there were 625 (1.7%) who reported symptoms on the day of the test. There were 115 (0.32%) with a positive SARS-CoV-2 test result (Table 1). Of the 115, there were 27 (23.5%) who were symptomatic and 88 (76.5%) who were asymptomatic on the day of the test (Tables 1 and 2).
Focusing on those who had specific symptoms (cough, and/or fever, and/or loss of taste/smell) there were 158 (0.43%) who had such symptoms on the day of the test. Of the 115 with a positive SARS-CoV-2, there were 16 (13.9%) who reported such symptoms. In contrast, 99 (86.1%) did not report specific symptoms on the day of the test (Table 2).
The positive predictive value (PPV) for symptoms was 4.3% while the PPV for specific symptoms was 10.1% (Table 2). The specificity and negative predictive values (NPV) were above 98% (Table 2).
Discussion
Overall, 115 (0.32%) of the sample tested positive for SARS-CoV-2. There were less than 2% who reported any symptoms indicative of COVID-19 and less than 0.5% who reported specific symptoms on the day of the test. The results of our study suggest that COVID-19 symptoms are a relatively poor marker of SARS-CoV-2 infection. Thus, 76.5% of those tested positive reported no symptoms and 86% reported none of the specific COVID-19 symptoms on the day of the test.
To our knowledge, the Office for National Statistics Coronavirus (COVID-19) Infection Survey pilot is the largest population survey carried out to date including information on the association between COVID-19 symptoms and SARS-CoV-2 test results.8 The study sample is approximately representative of the English population outside care homes, other communal establishments and hospital settings. Information on COVID-19 symptoms was reported before results of the SARS-CoV-2 test were known and therefore not subject to recall bias.
An assumption behind our interpretation is that test specificity of SARS-CoV-2 test is very close to 100%. A test with specificity of 99.9% conducted in 36,061 people without SARS-CoV-2 infection would be expected to lead to 36 false-positive tests. Thus, there is scope for over-estimating the number of people with SARS-CoV-2 and this might be part of the reason for the high proportion of positive tests we observed to be in people without symptoms. Confirmation of positive test results is important for avoiding bias in prevalence estimates in such surveys.
Several studies have highlighted a proportion of individuals testing positive for SARS-CoV-2 are asymptomatic.1–6,8,9 However, the prevalence of asymptomatic cases varies substantially, possibly due to the sampling and the settings of the study.8 The findings from our analyses suggest that asymptomatic cases of COVID-19 were widespread in the UK in Spring 2020. Similar findings were observed from smaller community samples Italy where 42% of the individuals testing positive were asymptomatic6 and on Iceland where 43% of the participants who tested positive reported having no symptoms, although symptoms may have developed later in some of them.7 A study of 126 residents in a nursing facility in the US suggested 39% of those who tested positive were asymptomatic.1 There has been some debate as to whether children and young people were less susceptible to SARS-CoV-2 and/or more likely to be asymptomatic than adults.11 Unfortunately, we did not have access to age-stratified data and therefore unable to evaluate this question in further detail.
As the prevalence of SARS-CoV-2 positive tests was low (0.32%), it is not surprising that the positive predictive value (PPV) of COVID-19 symptoms also was low. However, it is worth noting that the PPV for specific symptoms is more than twice as high as for the non-specific symptoms (10.1% (5.9% to 15.9%) vs 4.3% (2.9% to 6.2%)). On the other hand, the specificity of the symptoms was high consistent with the majority of people without SARS-CoV-2 infection being asymptomatic at any point in time. However, this may change in periods where there is overlap between SARS-CoV-2 infections and other respiratory infections eg, in the influenza season.
Our findings have implications for ongoing and future SARS-CoV-2 test programmes. The fact that up to 86% of those who tested positive were asymptomatic on the day of a positive SARS-CoV-2 test results calls for a change to future testing strategies. In order to capture “silent” transmission and potentially prevent future outbreaks test programmes should involve frequent and widespread SARS-CoV-2 testing of all individuals, not just symptomatic cases at least in high-risk settings or specific locations. Thus, a strategy has been proposed for suppressing SARS-CoV-2 transmission which involves frequent and widespread testing which is regardless of presence of symptoms.17 Such a strategy is feasible with the development of simpler tests that produce rapid results at low cost, accepting some loss of sensitivity.18
Conclusions
COVID-19 symptoms are poor marker of SARS-CoV-2 infection. Thus, 76.5% of those who tested positive reported no symptoms and 86.1% reported none of the specific COVID-19 symptoms on the day of the test. It is likely to be necessary to set up test programmes involving frequent and widespread SARS-CoV-2 testing of all individuals, at least where there are recent cases, and certainly in high-risk setting, for example, care homes, hospitals, or specific industries in order to capture “silent” transmission and potentially prevent future outbreaks. It may be important for testing programs used to estimate prevalence for surveillance purposes to consider test specificity of SARS-CoV-2 tests and confirmation of positive cases where the person is asymptomatic.
Author Contributions
All authors made a significant contribution to the work reported, whether that is in the conception, study design, execution, acquisition of data, analysis, and interpretation, or in all these areas; took part in drafting, revising, or critically reviewing the article; gave final approval of the version to be published; have agreed on the journal to which the article has been submitted; and agree to be accountable for all aspects of the work.
Funding
This research did not receive any specific grant from funding agencies in the public, commercial, or not-for-profit sectors.
Disclosure
The authors report no conflicts of interest for this work.
References
1. Patel MC, Chaisson LH, Borgetti S, et al. Asymptomatic SARS-CoV-2 infection and COVID-19 mortality during an outbreak investigation in a skilled nursing facility. Clin Infect Dis. 2020. doi:10.1093/cid/ciaa763
2. Kimball A, Hatfield KM, Arons M, et al. Asymptomatic and presymptomatic SARS-CoV-2 infections in residents of a long-term care skilled nursing facility - King County, Washington. MMWR Morb Mortal Wkly Rep. 2020;69(13):377–381. doi:10.15585/mmwr.mm6913e1
3. Mizumoto K, Kagaya K, Zarebski A, Chowell G. Estimating the asymptomatic proportion of coronavirus disease 2019 (COVID-19) cases on board the diamond princess cruise ship, Yokohama, Japan, 2020. Euro Surveill Bull Eur Sur Mal Transm Eur Commun Dis Bull. 2020;25. doi:10.2807/1560-7917.ES.2020.25.10.2000180.
4. Kam K-Q, Yung CF, Cui L, et al. A well infant with coronavirus disease 2019 (COVID-19) with high viral load. Clin Infect Dis. 2020;71(15):847–849. doi:10.1093/cid/ciaa201
5. Roxby AC, Greninger AL, Hatfield KM, et al. Detection of SARS-CoV-2 among residents and staff members of an independent and assisted living community for older adults - Seattle, Washington, 2020. MMWR Morb Mortal Wkly Rep. 2020;69(14):416–418. doi:10.15585/mmwr.mm6914e2
6. Imperial College COVID-19 Response Team, Lavezzo E, Franchin E, Ciavarella C, et al. Suppression of a SARS-CoV-2 outbreak in the Italian municipality of Vo. Nature. 2020;584(7821):425–429. doi:10.1038/s41586-020-2488-1.
7. Gudbjartsson DF, Helgason A, Jonsson H, et al. Spread of SARS-CoV-2 in the Icelandic population. N Engl J Med. 2020;382(24):2302–2315. doi:10.1056/NEJMoa2006100
8. Oran DP, Topol EJ. Prevalence of asymptomatic SARS-CoV-2 infection: a narrative review. Ann Intern Med. 2020;173(5):362–367. doi:10.7326/M20-3012
9. Day M. Covid-19: identifying and isolating asymptomatic people helped eliminate virus in Italian village. BMJ. 2020;m1165. doi:10.1136/bmj.m1165
10. Qiu H, Wu J, Hong L, Luo Y, Song Q, Chen D. Clinical and epidemiological features of 36 children with coronavirus disease 2019 (COVID-19) in Zhejiang, China: an observational cohort study. Lancet Infect Dis. 2020;20(6):689–696. doi:10.1016/S1473-3099(20)30198-5
11. Mehta NS, Mytton OT, Mullins EWS, et al. SARS-CoV-2 (COVID-19): what do we know about children? A systematic review. Clin Infect Dis. 2020. doi:10.1093/cid/ciaa556
12. Coronavirus (COVID-19) infection survey pilot - office for national statistics. Available from: https://www.ons.gov.uk/peoplepopulationandcommunity/healthandsocialcare/conditionsanddiseases/bulletins/coronaviruscovid19infectionsurveypilot/2july2020#covid-19-infection-survey-data.
13. Coronavirus (COVID-19) infections in the community in England - office for national statistics. Available from: https://www.ons.gov.uk/peoplepopulationandcommunity/healthandsocialcare/conditionsanddiseases/bulletins/coronaviruscovid19infectionsurveypilot/england9july2020.
14. Coronavirus (COVID-19) infection survey - office for national statistics. Available from: https://www.ons.gov.uk/peoplepopulationandcommunity/healthandsocialcare/conditionsanddiseases/datasets/coronaviruscovid19infectionsinthecommunityinengland.
15. COVID-19 infection survey (pilot): methods and further information - office for national statistics. Available from: https://www.ons.gov.uk/peoplepopulationandcommunity/healthandsocialcare/conditionsanddiseases/methodologies/covid19infectionsurveypilotmethodsandfurtherinformation#sensitivity-and-specificity-analysis.
16. Open government licence. Available from: http://www.nationalarchives.gov.uk/doc/open-government-licence/version/3/.
17. Peto J, Alwan NA, Godfrey KM, et al. Universal weekly testing as the UK COVID-19 lockdown exit strategy. Lancet. 2020;395(10234):1420–1421. doi:10.1016/S0140-6736(20)30936-3
18. Larremore DB, Wilder B, Lester E, et al. Test sensitivity is secondary to frequency and turnaround time for COVID-19 surveillance. Infect Dis. 2020. doi:10.1101/2020.06.22.20136309
 © 2020 The Author(s). This work is published and licensed by Dove Medical Press Limited. The full terms of this license are available at https://www.dovepress.com/terms.php and incorporate the Creative Commons Attribution - Non Commercial (unported, v3.0) License.
By accessing the work you hereby accept the Terms. Non-commercial uses of the work are permitted without any further permission from Dove Medical Press Limited, provided the work is properly attributed. For permission for commercial use of this work, please see paragraphs 4.2 and 5 of our Terms.
© 2020 The Author(s). This work is published and licensed by Dove Medical Press Limited. The full terms of this license are available at https://www.dovepress.com/terms.php and incorporate the Creative Commons Attribution - Non Commercial (unported, v3.0) License.
By accessing the work you hereby accept the Terms. Non-commercial uses of the work are permitted without any further permission from Dove Medical Press Limited, provided the work is properly attributed. For permission for commercial use of this work, please see paragraphs 4.2 and 5 of our Terms.

