Back to Journals » Journal of Multidisciplinary Healthcare » Volume 15
The Stress of Leprosy as a Mediator of the Relationship Between Coping Resources, Coping Strategies, and Psychological Well-Being in Persons Affected by Leprosy. The Structural Equation Models Through a Correlation Study
Authors Listiawan MY , Sigit Prakoeswa CR, Alinda MD, Kusumaputra BH, Hartanto F , Nasir A , Yusuf A
Received 17 July 2022
Accepted for publication 8 September 2022
Published 29 September 2022 Volume 2022:15 Pages 2189—2202
DOI https://doi.org/10.2147/JMDH.S382723
Checked for plagiarism Yes
Review by Single anonymous peer review
Peer reviewer comments 2
Editor who approved publication: Dr Scott Fraser
Muhammad Yulianto Listiawan,1 Cita Rosita Sigit Prakoeswa,1 Medhi Denisa Alinda,1 Bagus Haryo Kusumaputra,1 Felix Hartanto,1 Abd Nasir,2,3 Ah Yusuf3
1Faculty of Medicine, Airlangga University, Surabaya, Indonesia; 2Faculty of Vocational Studies, Airlangga University, Surabaya, Indonesia; 3Faculty of Nursing, Airlangga University, Surabaya, Indonesia
Correspondence: Muhammad Yulianto Listiawan, Email [email protected]
Intoduction: Psychological strength plays an important role in reducing stress due to leprosy because leprosy can cause physical, psychological, and social problems. For that reason, this study aims to investigate the relationship between coping sources, coping strategies, and psychological well-being through leprosy stress.
Methods: This research instrument uses a stress perception scale, coping sources, coping strategies, and psychological well-being scale to collect data from 125 participants consisting of women (33.60%) and men 66.40%. The test analysis in this study uses SmartPLS through structural equation modeling to prove the correlation.
Results: The results of the SEM test indicate that there is a negative relationship between coping resources and leprosy stress, with a coefficient value of (− 0.380), p-value of (0.000) < 0.05, and a positive relationship is obtained with psychological well-being with the coefficient value of (0.427), p-value of (0.000) < 0.05. Meanwhile, the SEM test shows a negative relationship between coping strategies and stress of leprosy, with the coefficient of (− 0.566), p-value of (0.000) < 0.05, and a positive relationship is obtained with psychological well-being (0.355), p-value of (0.000) < 0.05. Furthermore, on psychological well-being, stress shows a negative relationship, with the coefficient of (− 0.212), p-value of (0.002).
Discussion: Exploration of important coping sources is done to weaken the power of leprosy as a stressor and the use of effective coping strategies is needed to solve physical, psychological, and social problems for “People Affected by Leprosy”, and simultaneously these two attributes are used to achieve prosperity. psychological. better.
Keywords: stress leprosy, coping resources, coping strategies, psychological well-being
Introduction
Potential discrimination against Persons affected by leprosy because of deformities and disabilities that are visible prevents them from being actively involved in social interactions, thus having a wide impact on their life processes.1 Based on the Weekly epidemiological record report, the completion rate of treatment for Persons affected by leprosy, Type Multi Basiler is 88.3%, and Type Pause Basiler is 93.8%. Meanwhile in Indonesia, completion of treatment for the Multi-Bacillary type was 86.7%, and for the Pause, Basiler type was 87.5% with 419 recurrences and 425 returning to treatment2 For this reason, the Indonesian government has implemented many measures to reduce morbidity and disability in leprosy, such as MDT drug treatment, early detection of leprosy, household contact checks, and epidemiological surveillance. Leprosy has spread globally and currently, no drug can prevent the occurrence of leprosy reactions as the initial cause of disability,3 as well as the difficulty of controlling stigma and discrimination,4 and this situation has a significant impact on economic, social, and psychological.5
Meanwhile, the label of leprosy which more dominantly affects mental and emotional than the dangers of the disease itself, makes Persons affected by leprosy withdraw from the association in society.6 Besides, stigma and discrimination by the community add to the burden of suffering.7 This stressful atmosphere has a negative impact on the pattern of life in society and socio-economics8 so that factors related to mental-emotional protection and daily functioning are important to identify. The focus of mental health services to protect and prevent individuals from psychological disorders is an important force in ensuring the psychological well-being of people with leprosy. Therefore, to deal with mental pressure both from oneself and from the community, focus on individual fighting power is the dominant factor to avoid the mental burden. In this domain, coping resources9 and coping strategies10,11 as a protective factor in helping to prevent emotional mental disorders will be very effective against the negative effects of leprosy.
Research that evaluates the impact of leprosy from a mental health perspective usually focuses on emotional mental disorders,12 and focuses on indicators of a healthy psychological outlook, such as coping resources,13 coping strategy,14 and psychological well-being,15 which are very effective for developing better mental health. In this case, analyzing the influence of leprosy stress and psychological well-being as psychological forces can provide important information about how a person can survive mentally and emotionally while suffering from leprosy with the risks faced throughout his life. This is why protective factors related to how to deal with stressful situations due to leprosy must be observed, not just mental-emotional disorders causes. Regarding the pressure due to leprosy, although there have been many reports of previous research on the use of coping resources and coping strategies as a protective factor or psychological well-being as emotional and mental parameters, however, there are still no reports on this study from the perspective of the individual “Persons Affected by Leprosy”.
Stress Due to Leprosy
Maybe only “Persons Affected by Leprosy” is shunned by the community even though there are many other chronic infectious diseases, because this disease is seen as a curse, unclean, and a recompense from God for his actions.16 As for him, the burden of depression and anxiety is part of their daily life.17 For this reason, it is inevitable that stressful situations are experienced by people with leprosy, because the effects caused by leprosy can affect the emotional mentality of the sufferer and his family.12 However, stress can also be a source of motivation that leads individuals to take protective action to seek medical help in dealing with stressful situations,18,19 and this is also done by “Person affected by leprosy”.20 However, the uncertainty surrounding the risk of permanent disability due to leprosy reactions that occur before, during, and after treatment, Persons Affected by Leprosy experience prolonged mental stress, which affects their well-being of them and their families,21 and this is always related to the chosen coping strategy.22 For individuals who do not have physical problems, they may feel optimistic and very flexible in using coping because they have taken a number of very strategic steps in dealing with their problems.23 However, it could be that the stressor inspires individuals to use various coping strategies because they have prepared various alternative coping sources and set realistic goals.
Coping Resources as a Protective Factor in Preventing the Occurrence of Leprosy Stress
The source of coping is one of the elements of positive psychology and is an important instrument that can be proven as a protector in preventing mental stress for chronic diseases,24 where this may also apply to stress due to leprosy. Coping resources are a very important initial capital for developing coping strategies for problem-solving efforts in ensuring psychological well-being, and this involves the availability of personal and environmental resources.25 Based on the stress resource conservation model, that the size of a person’s resources to deal with stressors is the most important factor in predicting the amount of perceived stress.26 Meanwhile, Lazarus & Folkman (1984) made it clear through the view of transactional stress, that the instability between the need to deal with stressors and the available resources can trigger stress, and this makes excessive demands to cope with stressors so that it can burden personal resources.27
As long as the perception of the label “Persons Affected by Leprosy” cannot be separated in personal life and the environment, the application of individual coping resources is less effective, while the risk of severity due to leprosy can increase.3 This is why coping resources can be considered as an important component for PWL to overcome fear, anxiety, depression, increase self-esteem, and stress due to leprosy. The results of studies that report that the use of coping resources helps to create effective stress management strategies and adjustment to stressful situations can support this view.28 Besides, coping resources have a positive relationship with life satisfaction,27 all of which are indicators of better psychological well-being. Furthermore, it has also been reported that coping resources not only protect a person against stress attacks but can also be used as an assessment of certain situations and predict coping behavior.29 Following this reasoning, strong coping resources are most likely associated with stressful situations of leprosy.
Coping Strategies as Facilitators in Preventing the Psychological Distress of Leprosy
Coping strategies are cognitive and behavioral responses that are used as facilitators to control the side effects of stressful situations.30 From this perspective, individuals with multiple coping strategies, have high flexibility, so it is very beneficial and is likely to be able to modify stress to a lesser extent, so that several of the available coping strategies provide different benefits and roles, depending on the nature, type, and quality of the stressor.31 Thus, having several coping strategies can be used as a security guarantee for the happiness of those who have many stressors. And the leprosy label has encouraged people with leprosy to choose the various alternative of coping related to various fields such as self-care, environmental care, and nutritional needs,32 maintain social relations,1 medication regimen adherence,33 and stress management.34 Furthermore, if the development of new modes of behavior is considered as a goal of protection against leprosy, then coping strategies will be an important attribute when trying to achieve that goal. An important aspect of coping strategies is that people with leprosy can create a happy emotional atmosphere, especially when facilitated by strong personal resilience,35 improved quality of life36 and psychological resilience.37 Thus, naturally, a person may have a strong desire to identify various coping strategies and apply new modes of behavior for leprosy healing that motivate the person to do better now and in the future. The findings in this study, that there is a positive relationship between coping strategies and coping resources, especially when in a stressful environment, support this view.25 Likewise, the intervention program of leprosy treatment is used as an effective coping strategy to reduce psychological symptoms and their recovery.20 When these findings are taken as a whole, coping strategies can be considered to play a protective role in stimulating better mental health and overcoming the psychological problems caused by leprosy.
Psychological Well-Being for Better Mental Health
Prosperous individuals are those who are relatively stressed and have better mental health status but stressful situations due to leprosy can affect their psychological well-being.38 The more pleasant experiences they have, the more happiness they will get in life. Thus, they will feel a feeling of well-being, which becomes a guarantee for their happiness. But, leprosy keeps them from feeling happy and prosperous.39 Thus, the stressful conditions due to leprosy will reduce happiness among individuals and have an impact on their mental condition. Several studies report that leprosy causes psychological disorders.17,40 Along with this, positive psychology-based intervention programs have been found to reduce stressful conditions and increase happiness.41–43 This finding supports the notion that a stressful situation will have a negative correlation with psychological well-being. In addition, factors that are considered to prevent stressful situations for leprosy, such as coping resources9 and coping strategies,44,45 have a positive correlation effect with psychological well-being.
Thus, two hypotheses (Hs) were determined based on the research above; (H1) the relationship between coping strategies and psychological well-being through stress leprosy and (H2) the relationship between coping strategies and psychological well-being through stress leprosy.
Methods
Participants and Procedures
Participants and procedures
Data were obtained from participants who were treated in the Leprosy Poly Room at the “Dr. Sutomo” Surabaya, using the convenience sampling method using IBMSPSS Statistics version 20, conducted between March 2021 to June 2021. The research sample was “Persons Affected by Leprosy”, consisting of 42 (33.60%) women and 83 (66.40%)) men. The mean age of participants > 15 years was 122 participants (97.60%), and <15 years were 3 (2.40%) participants. Regarding marital status, 65 (52%) participants were married, and 60 (48%) participants were unmarried. In addition, based on employment status, 65 (52%) participants worked and 60 (48%) participants did not work. Meanwhile, based on the incidence of leprosy reactions, once as many as 63 (50.40%) participants, twice as many as 14 (11.20%) participants, three times as many as 12 (9.60%) participants, four times as many as 15 (12.00) %) %) participants, five times as many as 12 (9.60%) participants, and more than 5 times as many as 9 (7.20%) participants, and the details can be seen in Table 1.
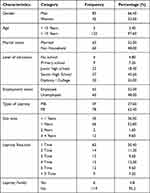 |
Table 1 Results of the Analysis of Respondents Characteristics |
Questionnaires were given to people with leprosy in paper and pencil format in Indonesian. Written informed consent and signatures were obtained from participants after the researcher provided brief information about the study. Written informed consent was also obtained from child participants who were represented and signed by parents. Next, participants completed a four-step anonymous self-report to avoid response bias. Because the questionnaire is anonymous, individual participants cannot be identified.
The researchers explained that participants could withdraw from the study whenever they wanted. Each participant takes approximately 15 to 20 minutes to complete all questionnaires.
Measurement
Psychological Well-Being
Psychological well-being was measured using the psychological well-being scale of leprosy which consisted of 18 items. The psychological well-being scale from CD Ryff was used as a development of this psychological well-being scale.46 Psychological well-being scale responses to leprosy were made on a 4-point Likert scale (1 = strongly disagree and 4 = strongly agree). Higher scores indicate better psychological well-being. This psychological well-being scale has been developed according to the Turkish version. The total variance explained was 68% and factor loadings ranged from 0.30 to 0.94. Internal consistencies varied between 0.87 and 0.96 and test-retest reliability coefficients ranged between 0.78 and 0.97.47 In this study, the researcher developed the psychological well-being scale from CD Ryff in the Indonesian version for data collection.
Leprosy Stress
Stress was measured using a leprosy stress scale consisting of 14 items as a result of the development of the perceived stress scale48 experienced by leprosy patients during the past month. The response to the leprosy stress scale was made on a 5-point Likert scale (0 = never and 4 = very often). Higher scores indicate stronger stress. This perceived stress scale has been developed according to the Iranian version, and the results of Confirmatory Factor Analysis (CFA) show that the data is acceptable with the two-factor model (Perceived Helplessness and Perceived Self-Efficacy) PSS-10 (v2 /df = 2.58, CFI = 0.96; RMSEA = 0.081 and SRMR = 0.061), and in this study, the perceived stress scale has a Cronbach’s α value of 0.842.49 In this study, the researcher developed the perceived stress scale in the Indonesian version for data collection.
Coping Resources
Coping resources were measured using the scale of the coping resources for leprosy as a result of the development of the coping resources inventory for stress50 designed to expand personal resources in dealing with stress. The coping resources scale was made on a 4-point Likert scale (1 = strongly disagree and 4 = strongly agree). Higher scores indicate broader coping resources. This coping resources scale has been adopted and developed according to the Iranian version, and in this study, the coping resources inventory for stress has an acceptable reliability coefficient value, with a Cronbach’s α of 0.79, a Mean of 42.93, and SD of 11.72.51 In this study, the researcher developed the coping resources inventory for stress in the Indonesian version for data collection.
Coping Strategies
Coping strategies were measured using a coping strategies scale consisting of 15 items. Coping Strategies Inventory Short-Form (CSI-SF)52 was used as the development of the leprosy coping strategies scale. The response to the coping strategies scale was made on a 4-point Likert scale (1 = strongly disagree and 4 = strongly agree). Higher scores indicate better coping strategies. This coping strategies scale has been identified based on a systematic review related to the reliability and validity of the coping strategy inventory-short form applied to hemodialysis patients in 13 countries in the Department of Epidemiology, School of Public Health, University of Michigan, Ann Arbor, MI, United States in which the results was Comparative Fit Index (CFI) ≥0.90; Goodness of Fit Index (GFI) ≥0.90; Standardized Root Mean Square Residual (SRMR) 0.08; and a root mean square error of approximation (RMSEA) ≤ 0.08, whereas good internal consistency (α = 0.56–0.80).53 In this study, the researcher developed the Coping Strategies Inventory Short-Form (CSI-SF) in the Indonesian version for data collection.
Statistical Analysis
Descriptive data for each variable which includes data on coping sources, coping strategies, psychological well-being, and stress of leprosy were tested using descriptive statistical analysis (mean and standard deviation) using IBMSPSS Statistics version 20. While the analysis of the relationship test of coping sources, coping strategies, and psychological well-being through leprosy stress, used SEM (Structural Equation Modeling) analysis with Smart-PLS (Partial Least Square). The first time the researcher assesses whether each latent variable is represented by its indicator. The structural model is then tested using the maximum likelihood estimate in Smart-PLS if the measurement model turns out to be significant. The index of covariance structure analysis recommended by Hu, Li-tze and Bentler, Peter M. (1999) was used to evaluate the overall fit of the model with the data.54
First: The researcher started the observation through structural equation modeling by evaluating the outer model to determine the value of cross loading, evaluating construct reliability, and evaluating construct validity. The cross-loading value is used to evaluate how strong the indicator value in the latent variable is against the indicator value in other latent variables. While the evaluation of construct reliability and evaluation of construct validity were used to determine the reliability of the instrument. Evaluation of construct validity and reliability follows Krabbe PFM’s (2017) suggestion by calculating convergent validity, namely calculating the Average Variance Extracted (AVE) value while evaluating construct reliability by calculating Cronbach’s Alpha value and Composite Reliability value.55
Second: Researchers observe the Inner model through hypothesis testing to determine the effect of independent variables on the dependent variable so that direct and indirect relationships between variables are known. Hypothesis testing in this study was conducted to determine the relationship between coping sources, coping strategies, and psychological well-being through stress of leprosy.
Third: Through the bootstrap procedure, the researcher calculated the R-Square value to calculate how strong the contribution of the independent variable was to the dependent variable,56 namely to determine the significance of the effect of coping resources, coping strategies on leprosy stress, and to determine the significance of the influence of coping resources, coping strategies, leprosy stress on psychological well-being.
Ethical Approval
The study procedure was in accordance with the Declaration of Helsinki and was approved by the Dr. Sutomo Hospital Health Research Ethics Committee with the number: 0168/KEPK/III/2021 (March 30, 2021).
Results
Descriptive Statistics of Variables
Table 2 shows that respondents’ perceptions of the variables have a good average and standard deviation, including the coping resources variable with cognitive dimensions (2.8053–0.71246), social (2.8128–0.71335), emotional (2 0.7560–0.73949), spiritual (2.7360–0.74210), and physical (2.7880–0.74396). Besides, the result regarding coping strategies variables with dimensions of resourcefulness and focus is 2.8608–0.75870, physical and persistent is 2.9030–0.83335, positive and knowledge-based is 2.8680–0.82585, and warning processing is 2 0.8907–0.84524. Respondents’ perceptions of the leprosy stress variable have an average and standard deviation (2.6664–0.47951), while the results concerning psychological well-being variable on the autonomy dimension is 2.9714–0.99491, environmental mastery is 2.8536–0.77326, personal growth is 2.8190–0.74865, positive relationship with others is 2.8366–0.74832, and purpose in life is 2.7754–0.76619.
 |
Table 2 Description of Research Variables |
Structural Equation Modeling
The results of this structural equation modeling test show the results of the evaluation of the outer model, inner model, and the contribution of the independent variable to the dependent variable.
Evaluation of Outer Models
The Outer Model Evaluation Scheme involves cross-loading values and the construction of Validity and Reliability, each of which has been described in Figure 1 as follows.
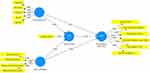 |
Figure 1 Outer Model Construct. |
Value of loading and cross loading
The results of the analysis show that the loading factor value of coping resources which includes cognitive, emotional, physical, social, and spiritual is between (0.959–0.981) > 0.5, and the loading factor value of coping strategies which include Alert processing, Physical and fixed, Positive and knowing-based, Resourceful and focused is about between (0.962–0.982) > 0.5, the loading factor value of psychological well-being which includes The Autonomy, The Environmental Mastery, The Personal Growth, The Positive Relations with Others, The Purpose in Life, The Self-Acceptance, is between (0.941–0.977) > 0.5, and the loading factor value of stress leprosy is (1000) > 0.05. Thus, all indicators that support the variable coping resources, coping strategies, psychological well-being, and leprosy stress are good, and the indicator that gives the biggest contribution to measuring Coping Resources is Social (0.981). Then the indicator that gives the biggest contribution to measuring Coping Strategies is Positive and knowledge-based (0.982), and the indicator that gives the biggest contribution to measuring Psychological Well-Being is Personal Growth (0.977). Meanwhile, overall the indicators of each variable, produce a loading value that is greater than the loading indicator value on other variables, this shows that from the discriminant validity test, each indicator can measure the latent variable that has conformity with the indicator. seen in Table 3
 |
Table 3 Value of Loading and Cross Loading |
Construct reliability and validity
The results of the reliability and construct validity test resulted in the Coping Resources values being Cronbach’s Alpha (0.983 > 0.5), Composite Reliability (0.987 > 0.7) and Average Variance Extracted (0.938) > 0.6. The values of the coping strategies are Cronbach’s Alpha (0.979 > 0.5), Composite Reliability (0.984 > 0.7) and Average Variance Extracted (0.940 > 0.6). Values of Psychological Well-being are Cronbach’s Alpha (0.980 > 0.5), Composite Reliability (0.983 > 0.7) and Average Variance Extracted (0.908 > 0.6). While the value of stress leprosy is Cronbach’s Alpha (1000 > 0.5), Composite Reliability (1000 > 0.7) and Average Variance Extracted (1000 > 0.6). Thus the results of the reliability and validity tests on all variables showed very adequate or marginal results. Further details can be seen in Table 4
 |
Table 4 Construct Reliability and Validity |
Evaluation of Inner Models
In general, the Evaluation of Inner Models can be explained in Figure 2 as follows. While the results of the detailed evaluation of the Inner Models are based on the goodness of fit evaluation stages based on hypothesis testing, the results have direct and indirect relationships.
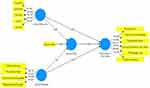 |
Figure 2 Inner Model Construct. |
The results of this analysis have reported that the value of the relationship between Coping Resources and Leprosy Stress is the value of Coefficients (−0.389), T Statistics (5.081 > 1.96), and P values (0.000 < 0.05). The value of the relationship between Coping Resources and Psychological Well-being is the value of Coefficients (0.426), T Statistics (4.481> 1.96), and P values (0.000 <0.05). The value of the relationship between Coping Strategies and Leprosy Stress is the coefficient value (−0.556), T Statistics (7.347 > 1.96), P values (0.000 < 0.05). The value of the relationship between Coping Strategies and Psychological Well-being is the value of Coefficients (0.350), T Statistics (4.502 > 1.96), P values (0.000 < 0.05). The value of the relationship between Leprosy stress and Psychological Well-being is the coefficient value (−0.219), T Statistics (3.068 > 1.96), P values (0.002 < 0.05). And this indicates that all independent variables are directly related to the dependent variable, which can then be seen in Table 3. Meanwhile, The test results report that the value of the indirect relationship between Coping Resources and Psychological Well-being through Leprosy Stress is the value of Coefficient (0.085), T Statistics (2.709 > 1.96), P values (0.007 < 0.05), which indicates that Coping Resources have a direct relationship with Psychological Well-being through leprosy stress. While the value of the indirect relationship between Coping strategies and Psychological Well-being through Leprosy Stress is the value of Coefficient (0.122), T Statistics (2.701 > 1.96), and P values (0.007 < 0.05), which indicates that Coping Strategies have a relationship directly with Psychological Well-being through stress leprosy, and the detail can be seen in Table 5.
 |
Table 5 Hypothesis Testing Results |
The Contribution of the Independent Variable to the Dependent Variable
The results of the analysis show that the value of the Leprosy stress variable is R Square (0.825), which indicates that Leprosy stress is influenced by coping resources and coping strategies by 82.5%. In addition, the value of the Psychological Well-being variable is R Square (0.897), which indicates that Psychological Well-being is influenced by coping resources, coping strategies, and leprosy stress by 89.7%. More details can be seen in Table 6
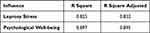 |
Table 6 R Square |
Discussion
Coping resources and coping strategies are protective factors in preventing the development of mental disorders, and these have a positive relationship with improving psychological well-being.57 As a result, coping resources and coping strategies are considered as protective factors that prevent psycho-emotional disorders that may arise from the stress of leprosy. Because leprosy stress can change psychological well-being and has a close relationship with coping resources and coping strategies to be chosen, while coping resources and coping strategies are always related to psychological well-being, in this study researchers examine the relationship between coping resources, coping strategies, and psychological well-being through the stress of leprosy. The first finding suggests that leprosy stress partially facilitates the relationship between coping resources and psychological well-being in favor of H1. The findings of this study as in other findings related to stressful situations due to chronic illness, increased coping resources make a positive contribution to psychological problems.58,59
It has also been reported that positive psychological interventions can relieve depression for the purpose of improving subjective well-being and psychological well-being.60–62 For this reason, too, in preventing the development of a stress response to leprosy (which is a chronic disease), coping resources are an important instrument for protecting the psychological well-being of “Person affected by leprosy”. It is very possible, that while infected with leprosy, the individual has developed symptoms related to psychological distress such as stress, anxiety, fear, and depression,39,63,64 and this all greatly affects their mental well-being.21 This is why the use and improvement of coping resources have been developed in other places where stress reduction and pressure are severe. The practice of increasing resources to overcome problems in the workplace that is set in the form of theory-based training and workshops in increasing psychosocial coping resources can cope with work stress to support their mental health.65 It is the same with workers who experience stress due to intimidation.66 Thus, the finding here that increased coping resources are used to improve mental health by decreasing stress response can be said to be a feature similar to the findings of previous studies. Confidence to recover from illness, increased ability and willingness to interact with other people and the environment, strong personality, high self-confidence, and a strong desire to solve problems are forms of coping resources that exist in every individual and can use to solve problems through the selection of effective coping strategies, and this is also what “Persons Affected by Leprosy” must do to maintain their well-being.
The second finding shows that coping strategies have a relationship with psychological well-being through leprosy stress, strongly supporting H2. This indicates that people who have several coping strategies in solving problems will experience low leprosy stress, so they can protect their psychological well-being. Like the experience experienced by people infected with leprosy, it has caused post-traumatic stress disorder (PTSD).67 Several studies that have reported the power of coping strategies in reducing stress to ensure psychological well-being are very supportive in this study.68 Besides, coping strategies have a positive relationship with sources of stress and other common psychological disorders.69 In addition, interventions directed at developing coping strategies have been effective in reducing the development of psychological disorders.35,70 On the other hand, coping strategies have a positive relationship with feelings of well-being,71 psychological well-being,72 as well as subjective well-being,73 This is because coping strategies are alternative methods for understanding coping and adjustment.31 So the findings here that emergent coping strategies to improve mental health in general and psychological well-being in particular, by reducing stress can be said to exhibit similar features to the findings of previous studies.
Finally, coping resources and coping strategies, with low-stress levels in leprosy patients as facilitators, have been shown to predict better levels of psychological well-being. Therefore, by using resources and coping strategies, people with leprosy can help protect their mental health from the stress of leprosy. And the findings of this study, have confirmed what has been successfully practiced elsewhere in Indonesia by Lusli et al through their work on rights-based peer counseling of and by people who have experienced leprosy.74 This approach argues that resources and coping strategies are psychological strengths to support the self-integrity of lepers and are not used for people who have psychological disorders. In other words, developing psychological strength is a strategic step for people who are prone to mental stress and also improves well-being,43 so that, coping resources13,65 and coping strategies70,72,75,76 can predict better psychological well-being. Thus, positive psychology-based leprosy treatment approaches such as exploring the source of coping and strengthening the use of effective coping strategies in addition to providing leprosy treatment services need to be developed in the future by health service providers such as doctors, nurses, nutritionists, and other health workers, so that they feel comfortable in undergoing the treatment program to completion to achieve optimal healing.
Conclusion
Overcoming leprosy is very important to do because it has caused psychosocial problems and has an impact on physical, emotional, and social. Therefore, it is now a very important thing to pay attention to. In connection with this, the results of this study indicate that coping resources and coping strategies contribute as a buffer for better mental health so this is always associated with a decrease in leprosy stress and an increase in psychological well-being. Moreover, individuals who have extensive coping resources and many coping strategies are possible to use alternative flexible coping sources to cope with the stress of leprosy and ensure their well-being. Their experience of leprosy stress can be handled adaptively on a practical level and as a result, they can feel better psychological well-being.
Data Sharing Statement
All data generated or analysed during this study are included in this published article.
Ethical Approval
The study procedure was in accordance with the Declaration of Helsinki and was approved by the Dr. Sutomo Hospital Health Research Ethics Committee with the number: 0168/KEPK/III/2021. All participants were given informed consent and were informed that they could withdraw at any time from the study.
Acknowledgments
The author would like to thank Leprosy patients and those around them, for sharing their experiences. We would also like to express our gratitude to the administrators at the institution who have assisted and supported this research.
Author Contributions
All authors made a significant contribution to the work reported, whether that is in the conception, study design, execution, acquisition of data, analysis and interpretation, or in all these areas; took part in drafting, revising or critically reviewing the article; gave final approval of the version to be published; have agreed on the journal to which the article has been submitted; and agree to be accountable for all aspects of the work. All authors critically revised the article, give final approval for the submission of the article, and agree to be responsible for all aspects of the work in ensuring that questions related to the accuracy or integrity of each part of the work are properly researched and resolved.
Funding
This research did not receive any specific grant from funding agencies in the public, commercial, or not for- profit sectors.
Disclosure
The authors report no conflicts of interest in relation to this work.
References
1. Marahatta SB, Amatya R, Adhikari S, et al. Perceived stigma of leprosy among community members and health care providers in Lalitpur district of Nepal: a qualitative study. PLoS One. 2018;13(12):1–13. doi:10.1371/journal.pone.0209676
2. World Health Organization. Global leprosy (Hansen disease) update, 2020: impact of COVID-19 on global leprosy control. Wky Epidemiol Rec. 2021;2021(36):421–444.
3. Scollard DM, Martelli CMT, Stefani MMA, et al. Risk factors for leprosy reactions in three endemic countries. Am J Trop Med Hyg. 2015;92(1):108–114. doi:10.4269/ajtmh.13-0221
4. Lusli M, Zweekhorst MBM, Miranda-Galarza B, et al. Dealing with stigma: experiences of persons affected by disabilities and leprosy. Biomed Res Int. 2015;2015:1–9. doi:10.1155/2015/261329
5. Pescarini JM, Strina A, Nery JS, et al. Socioeconomic risk markers of leprosy in high-burden countries: a systematic review and meta-analysis. PLoS Negl Trop Dis. 2018;12:1–20.
6. Sottie CA, Darkey J. Living with stigma: voices from the Cured Lepers’ village in Ghana. Soc Work Health Care. 2019;58(2):151–165. doi:10.1080/00981389.2018.1526842
7. Sardana K, Ananta K. Leprosy stigma & the relevance of emergent therapeutic options. Indian J Med Res. 2020;517–520. doi:10.4103/ijmr.IJMR
8. Van’T Noordende AT, Lisam S, Ruthindartri P, et al. Leprosy perceptions and knowledge in endemic districts in India and Indonesia: differences and commonalities. PLoS Negl Trop Dis. 2021;15(1):1–19. doi:10.1371/journal.pntd.0009031
9. Correia JC, Golay A, Lachat S, et al. “If you will counsel properly with love, they will listen”: a qualitative analysis of leprosy affected patients’ educational needs and caregiver perceptions in Nepal. PLoS One. 2019;14(2):1–15. doi:10.1371/journal.pone.0210955
10. Bakare AT, Yusuf AJ, Habib ZG, Obembe A. Anxiety and depression: a study of people with leprosy in Sokoto, North-Western Nigeria. J Psychiatry. 2015;s1. doi:10.4172/2378-5756.S1-004
11. Yusuf A, Aditya RS, Yunitasari E, Aziz AN, Solikhah FK. Experience of persons affected by leprosy in facing psychosocial problems: a qualitative method. Syst Rev Pharm. 2020;11(7):219–223.
12. Nasir A, Yusuf A, Listiawan MY, Harianto S, Huda N. adaptive strategy of women ` s leprosy in Indonesia psychic experience of women with leprosy in living a community life. Sys Rev Pharm. 2020;11(10):306–312.
13. Taylor SE, Stanton AL. Coping Resources, Coping Processes, and Mental Health. Annu Rev Clin Psychol. 2007;3(1):377–401. doi:10.1146/annurev.clinpsy.3.022806.091520
14. Macía P, Barranco M, Gorbeña S, Álvarez-Fuentes E, Iraurgi I. Resilience and coping strategies in relation to mental health outcomes in people with cancer. PLoS One. 2021;16(5):e0252075. doi:10.1371/journal.pone.0252075
15. Weiss LA, Westerhof GJ, Bohlmeijer ET. Can we increase psychological well-being? The effects of interventions on psychological well-being: a meta-analysis of randomized controlled trials. PLoS One. 2016;26:1–16. doi:10.1371/journal.pone.0158092
16. Gracino ME, Mendes B, Garbelin MV, Nishi V, Silva D. Leprosy: a systematic review Leprosy: a systematic review. Int J Dermatology Sci. 2020;2:8–21.
17. Govindasamy K, Jacob I, Solomon RM, Darlong J. Burden of depression and anxiety among leprosy affected and associated factors — a cross sectional study from India. PLoS Negl Trop Dis. 2021;1–12. doi:10.1371/journal.pntd.0009030
18. Gulliver A, Griffiths KM, Christensen H. Perceived barriers and facilitators to mental health help-seeking in young people: a systematic review. BMC Psychiatry. 2010;10(1):113. doi:10.1186/1471-244X-10-113
19. Kantor V, Knefel M, Lueger-Schuster B. Perceived barriers and facilitators of mental health service utilization in adult trauma survivors: a systematic review. Clin Psychol Rev. 2017;52:52–68. doi:10.1016/j.cpr.2016.12.001
20. Susanti IA, Mahardita NGP, Alfianto R, Sujana IM, Siswoyo ST, Susanto T. Social stigma, adherence to medication and motivation for healing: a cross-sectional study of leprosy patients at Jember Public Health Center, Indonesia. J Taibah Univ Med Sci. 2018;13(1):97–102. doi:10.1016/j.jtumed.2017.06.006
21. Somar P, Waltz M, van Brakel W. The impact of leprosy on the mental wellbeing of leprosy-affected persons and their family members – a systematic review. Glob Ment Heal. 2020;7. doi:10.1017/gmh.2020.3
22. Khanna D, De WG, Antonio L, et al. Improving treatment outcomes for leprosy in Pernambuco, Brazil: a qualitative study exploring the experiences and perceptions of retreatment patients and their carers. BMC Infect Dis. 2021;21:1–19. doi:10.1186/s12879-020-05706-z
23. Hanssen MM, Vancleef LMG, Vlaeyen JWS, Hayes AF, Schouten EGW, Peters ML. Optimism, motivational coping and well-being: evidence supporting the importance of flexible goal adjustment. J Happiness Stud. 2015;16(6):1525–1537. doi:10.1007/s10902-014-9572-x
24. Panjwani AA, Revenson TA. Coping with Chronic Illness. In: The Wiley Encyclopedia of Health Psychology.
25. Callan VJ, Terry DJ, Schweitzer R. Coping resources, coping strategies and adjustment to organizational change: direct or buffering effects? Empl Adjust to Organ Chang. 1994;8(4):372–383. doi:10.1080/02678379408256543
26. Hobfoll SE. Conservation of resources: a new attempt at conceptualizing stress. Am Psychol. 1989;44(3):513–524. doi:10.1037/0003-066X.44.3.513
27. Matheny KB, Roque-tovar BE, Curlette WL. Perceived stress, coping resources, and life satisfaction among U. S. and Mexican college students: a cross-cultural study. An Psicol. 2008;24:49–57.
28. Fredrickson BL, Cohn MA, Coffey KA, Pek J, Finkel SM. Open hearts build lives: positive emotions, induced through loving-kindness meditation, build consequential personal resources. J Pers Soc Psychol. 2008;95:1045–1062. doi:10.1037/a0013262
29. Zhang J, Cui M, Wang W, et al. The coexistence of coping resources and specific coping styles in stress: evidence from full information item bifactor analysis. PLoS One. 2014;9(5). doi:10.1371/journal.pone.0096451
30. Kim JH, Shim Y, Choi I, Choi E. The role of coping strategies in maintaining well-being during the COVID-19 Outbreak in South Korea. Soc Psychol Personal Sci. 2021. doi:10.1177/1948550621990595
31. Heffer T, Willoughby T. A count of coping strategies: a longitudinal study investigating an alternative method to understanding coping and adjustment. PLoS One. 2017;12:1–16.
32. Ramona F, Prakoeswa S, Ilhami AZ, et al. Correlation analysis between household hygiene and sanitation and nutritional status and female leprosy in Gresik regency. Dermatol Res Pract. 2020;2020. doi:10.1155/2020/4379825
33. Bezerra K, Jaime J, Leite G, et al. Knowledge of the patients regarding leprosy and adherence to treatment. Brazilian J Infect Dis. 2012;16(5):472–475. doi:10.1016/j.bjid.2012.04.002
34. Margaeta KL, Kusnanto Yulis SD. Knowledge, self effi cacy and stress in patient with leprosy through implementation of support group using adaptation theory. J Ners. 2014;9:49–58. doi:10.20473/jn.v9i1.2965
35. Smith MM, Saklofske DH, Keefer KV, Tremblay PF. Coping strategies and psychological outcomes: the moderating effects of personal resiliency. J Psychol. 2016;150:318–332. doi:10.1080/00223980.2015.1036828
36. Gattino S, De PN, Rollero C. The influence of coping strategies on quality of life from a gender perspective. Appl Res Qual Life. 2014. doi:10.1007/s11482-014-9348-9
37. Booth JW, Neill JT. Coping strategies and the development of psychological resilience. J Outdoor Environ Educ. 2017;20(1):47–54. doi:10.1007/BF03401002
38. Revenson T, Hoyt MA. Chronic illness and mental health. Encycl Mental Health. 2018. doi:10.1016/B978-0-12-397045-9.00151-8
39. van Dorst MM, van Netten WJ, Waltz MM, et al. Depression and mental wellbeing in people affected by leprosy in southern Nepal. Glob Health Action. 2020;13:1815275. doi:10.1080/16549716.2020.1815275
40. Xiong M, Wang X, Su T, Yang B, Li M, Zheng D. Relationship between psychological health and quality of life of people affected by leprosy in the community in Guangdong province, China: a cross-sectional study. BMC Public Health. 2019;19(1):1–8. doi:10.1186/s12889-019-6672-x
41. Ebrahimi N, Bahari F, Zare-Bahramabadi M. The effectiveness of group logo therapy on the hope among the leukemic patients. Iran J Cancer Prev. 2014;7(1):9–16.
42. Mohammadi F, Fard FD, Heidari H. Effectiveness of Logo Therapy in Hope of Life in the Women Depression. Procedia Soc Behav Sci. 2014;159:643–646. doi:10.1016/j.sbspro.2014.12.440
43. Joshanloo LLHAPM, Passmore H-A, Joshanloo M. in a culturally ‑ diverse university: boosting happiness and reducing fear. J Happiness Stud. 2019;20(4):1141–1162. doi:10.1007/s10902-018-9993-z
44. Rao S. Perspectives on the impact of stigma in leprosy: strategies to improve access to health care. Res Rep Trop Med. 2015;49. doi:10.2147/rrtm.s55903
45. Neelmani B, Premal D, Rao PSS, John AS. Enhancing counselling strategies for leprosy patients through the Participation Scale. Lepr Rev. 2013;84(3):199–208. doi:10.47276/lr.84.3.199
46. Ryff CD, Keyes CLM. The structure of psychological well-being revisited. J Pers Soc Psychol. 1995;69(4):719–727. doi:10.1037/0022-3514.69.4.719
47. Akin A. The scales of psychological well-being: a study of validity and reliability. Educ Sci Theory Pract. 2008;8:741–750.
48. Cohen S, Kamarck T, Mermelstein R. Stress A global measure of perceived stress. J Health Soc Behav. 2012;24(4):385–396. doi:10.2307/2136404
49. Maroufizadeh S, Foroudifard F, Navid B, Ezabadi Z, Sobati B. The perceived stress scale (PSS-10) in women experiencing infertility: a reliability and validity study. Middle East Fertil Soc J. 2018;3. doi:10.1016/j.mefs.2018.02.003
50. Matheny K, Aycock D, Curlette W, Junker G. The coping resources inventory for stress: a measure of perceived resourcefulness*. J Clin Psychol. 2003;59:1261–1277. doi:10.1002/jclp.10219
51. Chinaveh M. The examination of reliability and validity of coping responses inventory among Iranian students. Procedia Soc Behav Sci. 2013;84:607–614. doi:10.1016/j.sbspro.2013.06.612
52. Addison CC, Campbell-jenkins BW, Sarpong DF, et al. Psychometric Evaluation of a Coping Strategies Inventory Short-Form (CSI-SF) in the Jackson heart study cohort. Int J Environ Res Public Health. 2007;4(4):289–295. doi:10.3390/ijerph200704040004
53. Speyer E, Morgenstern H, Hayashino Y, Kerr PG, Rayner H. Reliability and validity of the coping strategy inventory-short form applied to hemodialysis patients in 13 countries: results from the dialysis outcomes and practice patterns study. J Psychosom Res. 2021;91:12–19. doi:10.1016/j.jpsychores.2016.08.015
54. Hu L, Bentler PM. Cutoff criteria for fit indexes in covariance structure analysis: conventional criteria versus new alternatives. Struct Equ Model. 1999;6(1):1–55. doi:10.1080/10705519909540118
55. Krabbe PFM. Validity. Meas Heal Heal Status. 2017;113–134. doi:10.1016/b978-0-12-801504-9.00007-6
56. Mavridis D, Moustaki I, Knott M. Goodness-of-Fit Measures for Latent Variable Models for Binary Data. Vol. 1. Elsevier B.V; 2007. doi:10.1016/B978-044452044-9/50010-0
57. Saxon L, Makhashvili N, Chikovani I, et al. Coping strategies and mental health outcomes of conflict-affected persons in the Republic of Georgia. Epidemiol Psychiatr Sci. 2017;26(3):276–286. doi:10.1017/S2045796016000019
58. Warner CB, Restorick A, Jeanblanc AB, Adams KB. Coping resources, loneliness, and depressive symptoms of older women with chronic Illness. J Appl Gerontol. 2019;38:295–322. doi:10.1177/0733464816687218
59. Wheaton B. Personal and psychiatric stress, coping resources, symptoms: an investigation of interactive models. J Health Soc Behav. 2015;24(3):208–229.
60. Hendriks T, Dijkstra MS, Hassankhan A, de Jong J, Bohlmeijer E. The Efficacy of Multicomponent Positive Psychology Interventions: A Meta-Analysis. Manuscript submitted for publication; 2019. doi:10.1007/s10902-019-00082-1
61. Bolier L, Haverman M, Westerhof GJ, Riper H, Smit F, Bohlmeijer E. Positive psychology interventions: a meta-analysis of randomized controlled studies. BMC Public Health. 2013;13(1):1. doi:10.1186/1471-2458-13-119
62. Cohn MA, Francisco S, Moskowitz JT. Positive affect interventions to reduce stress; 2016.
63. Ramasamy S, Panneerselvam S, Govindharaj P, Kumar A, Nayak R. Progressive muscle relaxation technique on anxiety and depression among persons affected by leprosy. J Exerc Rehabil. 2018;14(3):375–381. doi:10.12965/jer.1836158.079
64. George R, George MR, Alphonsa R. Effectiveness of bibliotherapy on stress among patients with Hansen ’ s disease. IJSR. 2019:10–12. DOI:10.13140/RG.2.2.34295.68009
65. Heaney CA, Price RH, Rafferty J. Increasing coping resources at wmk a field experiment to increase social support, improve work team fmctiolliag, and enhance employee mental health. J Organ Behav. 1995;16:335–352. doi:10.1002/job.4030160405
66. Brande W, Baillien E, Witte H, Elst T, Godderis L. The role of work stressors, coping strategies and coping resources in the process of workplace bullying: a systematic review and development of a comprehensive model. Aggress Violent Behav. 2016. doi:10.1016/j.avb.2016.06.004
67. Singh GP. Psychosocial aspects of Hansen’s disease (leprosy). Indian Dermatol Online J. 2012;3(3):166–170. doi:10.4103/2229-5178.101811
68. Regehr C, Glancy D, Pitts A. Interventions to reduce stress in university students: a review and. J Affect Disord. 2013;148(1):1–11. doi:10.1016/j.jad.2012.11.026
69. Bamuhair SS, Farhan A, Althubaiti A, Agha S, Rahman S, Ibrahim NO. Sources of stress and coping strategies among undergraduate medical students enrolled in a problem-based learning curriculum. Depression. 2015;20:33.
70. Ukeh MI, Salawu HA. The impact of coping strategies on psychological well-being among students of federal University, Lafia, Nigeria. J Psychol Psychother. 2018;8:5. doi:10.4172/2161-0487.1000349
71. Mele C, Mayordomo-rodrı T. Coping Strategies as Predictors of Well-Being in Youth Adult Coping Strategies as Predictors of Well-Being in Youth Adult. Soc Indic Res. 2015. doi:10.1007/s11205-014-0689-4
72. Freire C, Del M, Ferradás M, Valle A, Núñez JC, Vallejo G. Profiles of psychological well-being and coping strategies among university students. Front Psychol. 2016;7:1–11. doi:10.3389/fpsyg.2016.01554
73. Fischer R, Scheunemann J, Moritz S. Coping strategies and subjective well‑being: context matters. J Happiness Stud. 2021;22:3413–3434. doi:10.1007/s10902-021-00372-7
74. Lusli M, Peters R, van Brakel W, et al. The impact of a rights-based counselling intervention to reduce stigma in people affected by leprosy in Indonesia. PLoS Negl Trop Dis. 2016;10:12. doi:10.1371/journal.pntd.0005088
75. Kumar R. Resilience, psychological well-being, and coping strategies in medical students. Indian J Psychiatry Nur. 2019;16:92. doi:10.4103/IOPN.IOPN_22_19
76. Carnicer JG, Calderón C. Coping strategies and psychological well-being among teacher education students: coping and well-being in students. Eur J. 2018;28(4):1127–1140. doi:10.1007/sl0212-012-0158-x
 © 2022 The Author(s). This work is published and licensed by Dove Medical Press Limited. The
full terms of this license are available at https://www.dovepress.com/terms.php
and incorporate the Creative Commons Attribution
- Non Commercial (unported, v3.0) License.
By accessing the work you hereby accept the Terms. Non-commercial uses of the work are permitted
without any further permission from Dove Medical Press Limited, provided the work is properly
attributed. For permission for commercial use of this work, please see paragraphs 4.2 and 5 of our Terms.
© 2022 The Author(s). This work is published and licensed by Dove Medical Press Limited. The
full terms of this license are available at https://www.dovepress.com/terms.php
and incorporate the Creative Commons Attribution
- Non Commercial (unported, v3.0) License.
By accessing the work you hereby accept the Terms. Non-commercial uses of the work are permitted
without any further permission from Dove Medical Press Limited, provided the work is properly
attributed. For permission for commercial use of this work, please see paragraphs 4.2 and 5 of our Terms.
