Back to Journals » Nature and Science of Sleep » Volume 12
The Relationship of Sleep Duration with Ethnicity and Chronic Disease in a Canadian General Population Cohort
Authors Singh M , Hall KA, Reynolds A , Palmer LJ , Mukherjee S
Received 11 August 2019
Accepted for publication 2 April 2020
Published 15 April 2020 Volume 2020:12 Pages 239—251
DOI https://doi.org/10.2147/NSS.S226834
Checked for plagiarism Yes
Review by Single anonymous peer review
Peer reviewer comments 3
Editor who approved publication: Dr Steven A Shea
Mandeep Singh,1– 3 Kelly A Hall,4 Amy Reynolds,5 Lyle J Palmer,4,* Sutapa Mukherjee6,7,*
1Department of Anesthesiology and Pain Management, Women’s College Hospital, Toronto, Canada; 2Department of Anaesthesiology and Pain Management, Toronto Western Hospital, University Health Network, Toronto, Canada; 3Toronto Sleep and Pulmonary Centre, Toronto, Canada; 4School of Public Health, University of Adelaide, Adelaide, SA, Australia; 5Appleton Institute, CQ University Australia, Wayville, SA, Australia; 6Respiratory and Sleep Services, Southern Adelaide Local Health Network, Adelaide, SA, Australia; 7Adelaide Institute for Sleep Health, Flinders University, Adelaide, SA, Australia
*These authors contributed equally to this work
Correspondence: Sutapa Mukherjee
Adelaide Institute for Sleep Health, Flinders University, Adelaide, SA, Australia
Tel +61 8 8201 7925
Email [email protected]
Study Objectives: Sleep duration is an important marker of sleep quality and overall sleep health. Both too little and too much sleep are associated with poorer health outcomes. We hypothesized that ethnicity-specific differences in sleep duration exist.
Methods: This cross-sectional study utilized questionnaire data from the Ontario Health Study (OHS), a multi-ethnic population-based cohort of Canadian adult residents aged 18 to 99 years, who provided medical, socio-demographic, and sleep information. Generalised linear models were used to investigate the association of sleep duration with ethnicity.
Results: The study sample consisted of 143,307 adults (60.4% women). The sample was multi-ethnic, including self-identified Aboriginal, Arab, Black, Chinese, Filipino, Hispanic, Japanese, Korean, Mixed (> 1 ethnicity), South Asian, South-East Asian, West Asian, and White ethnicities. Univariate analyses found that mean sleep duration compared to the White reference group (7.34 hours) was shorter in the Filipino (6.93 hours, 25 min less), Black (6.96 hours, 23 min less), Japanese (7.02 hours, 19 min less), Chinese (7.23 hours, 7 min less), and Mixed (7.27 hours, 4 min less) groups (all P< 0.001). Mean sleep duration was shorter in men (7.25 hours) compared to women (7.37 hours) in the cohort as a whole (P< 0.001), and in all ethnic groups (P< 0.001). Multivariate analyses, adjusted for a wide range of potential risk factors, and analysis of sleep duration as a categorical variable (“short”, “average”, and “long” sleepers) confirmed these relationships. Both sleep duration and ethnicity were independent significant predictors of a range of physician-diagnosed morbidities including diabetes, stroke, and depression.
Conclusion: Important differences exist in sleep duration between ethnic groups and may contribute to observed health disparities. Our results highlight the need for ethnicity-specific targeted education on the importance of prioritizing sleep for good health, and the need to account appropriately for ethnicity in future epidemiological, clinical, and translational research into sleep and related conditions.
Keywords: sleep health, sleep duration, ethnicity, population health, health disparity
Plain Language Summary
Sleep that is too short or too long in duration is an important marker of sleep quality, general health, and chronic disease risk. Little is known regarding the inter-relationship of ethnic background with sleep duration. We studied a large, population-based, multi-ethnic sample of adults (aged at least 18 years) from Canada - the Ontario Health Study - in order to address this question. We found significant differences in self-reported average sleep duration by ethnic group. Subjects in all ethnic groups were, on average, either at the lower end or below recommended guidelines for healthy sleep. Average sleep duration was highest in White adults, and lowest in Black and Filipino adults. Differences in sleep duration, especially short sleep, were highly correlated with an increased risk of poor health outcomes, and may contribute to observed health disparities amongst ethnic groups. Further research is needed to investigate the factors that contribute to ethnicity-specific variations in sleep duration.
Introduction
Sleep is essential for good health.1 Sleep habits are influenced by social, behavioural, environmental, and genetic factors, and impact sleep quality, timing, and duration. Sleep duration has been investigated in numerous studies, is commonly obtained by self-report, and is generally defined by the average number of hours of sleep (including naps) in a 24-hour period. Extremes of sleep duration (short and long) are associated with adverse health outcomes, including increased risk of cardiovascular disease (CVD)2,3 and diabetes,4,5 and poor self-rated general health.6 There is some evidence of an association between variation in sleep duration and all-cause mortality,7–9 and emerging evidence of an interactive association between obstructive sleep apnoea and short sleep duration and the development of hypertension.10 Current recommendations are that adults sleep between 7 and 9 hours per night for good health.1,11 However, it is clear that in many industrialized countries average sleep duration has declined over the past 50 years, due in part to longer work schedules and increased screen time.2 There is growing concern that adults are becoming systematically sleep deprived.12 This is illustrated by recent prevalence estimates of sleep duration among adolescents which suggest that 60% of adolescents in developed countries are sleep deprived (<8 hours sleep per night).13 These findings are problematic for both current and future generations and suggest that sleep disorders and concomitant adverse health outcomes such as hypertension, diabetes, and poor general health will continue to rise. Identifying correlates of poor sleep in the population is consequently important, in order to inform public policy and interventions.
There are well-documented gender-based differences in sleep duration,14 with sleep duration and quality generally found to be higher in women than men.15 This may be due to an increased biological need for slow wave sleep in women.16 The National Sleep Foundation poll of 1007 respondents from the United States found significant differences in sleep duration related to ethnicity.12 African Americans reported the lowest average weekday sleep duration (6 hours, 14 minutes) compared to White Americans (6 hours, 52 minutes), Asians (6 hours 48 minutes), and Hispanics (6 hours, 34 minutes). Another study from the US showed that African Americans demonstrated more variation in habitual sleep time than White Americans.17 However, there are few such studies globally. Up to 30% of the Canadian adult population have been estimated to have insufficient sleep based on data from the Canadian Health Measures Survey data (n=10,976 individuals).18 Poor quality and reduced duration of sleep thus appear to be common in Canada, although the limited information available adversely impacts the ability to intervene and manage sleep problems in the community.
Ontario is the most populous province of Canada with a large multi-ethnic population.19 The capital city, Toronto, is among the most ethnically diverse cities in the world.20 Ontario thus provides a rich sampling frame to investigate whether differences in ethnicity might be associated with variation in sleep duration. The Ontario Health Study (OHS) is a population-based cohort of adults resident in Ontario. Using cross-sectional baseline questionnaire data, we evaluated variation in self-reported sleep duration by gender and ethnicity among participants in the OHS. We hypothesized that, independent of other risk factors, self-reported sleep duration would be associated with ethnicity. Ours is the largest research study to date to report the inter-relationships among sleep duration and ethnicity.
Methods
Study Design
The OHS is a population-based cohort study comprising a large, ethnically diverse sample from the province of Ontario, Canada.21 The current study was based upon the self-reported data collected at baseline recruitment from adult (≥18 years) residents of Ontario using a comprehensive web-based questionnaire. Data collected included: health-related behaviour, personal medical history, education history, socio-demographic characteristics, and health service utilization. Data provided as part of this study were collected from study participants between September 29, 2010 and April 29, 2013. Institutional review ethics board approval was obtained (Women’s College Hospital REB#2013-0010-E). Informed consent was obtained from all participants. The sampling frame was all adults aged 18 years and above and resident in the province of Ontario. Online recruitment and measurement were used to enrol large numbers of adult participants at low marginal cost from a broad cross-section of Ontario society. The recruitment of participants at baseline was supported by extensive province-wide advertising in various media, including radio, print and television in addition to online media. Incentive programs were also employed in order to encourage participation.
Questionnaire Data
All questions asked (with the exception of current age and sex) had the additional possible answers of “don’t know” and “prefer not to answer.”
Sleep History
Self-reported sleep duration was recorded based on the response to the question: “On average, how many hours per day do you usually sleep, including naps?” The response was recorded as a continuous variable in hours and minutes. Sleep quality was determined by the response to the question: “How often do you have trouble going to sleep or staying asleep?” Possible responses were: “never”, “part of the time”, “some of the time”, “most of the time”, or “all of the time”.
Ethnicity
Ethnicity was recorded as a positive answer to at least one of the following options: “Aboriginal” (eg, First Nations, Métis, Inuit), “Arab” (eg, Egypt, Iraq, Jordan, Lebanon), “Black” (African or Caribbean descent), “Chinese”, “Filipino”, “Japanese”, “Korean”, “Latin American/Hispanic”, “South Asian” (eg, India, Sri Lanka, Pakistan, Bangladesh), “Southeast Asian” (eg, Malaysia, Indonesia, Vietnam, Cambodia, Laos), “West Asian” (eg, Turkey, Iran, Afghanistan), or “White” (European ancestry). Where more than one ethnicity was recorded, ethnicity was defined as “Mixed”.
Socio-Demographic Variables and Morbidities
Current age and gender were reported by all participants. Nativity was recorded as the answer to the question “Were you born in Canada?”. The number of years spent resident in Canada was recorded as the answer to the question “How old were you when you first came to Canada to live?” Body mass index (BMI; kg/m2) was calculated using self-reported height and weight. Morbidities of participants were self-reported physician diagnosed conditions (ie, “Has a doctor ever told you that you had any of the following conditions?”). Conditions reported included: high blood pressure (hypertension), blood glucose disorder (high blood glucose/sugar), diabetes (gestational, type 1, or type 2), high cholesterol, depression, stroke, sleep apnoea, and cardiovascular conditions (heart disease and myocardial infarction). Additionally, self-reported general health perception was evaluated (ie, “How would you rate your general health?”) on an ordinal scale from 1 (poor) to 5 (excellent). Geographic residential status (rural or urban, according to Canada Post designations), household income (ie, “What is the approximate total household income (from all sources) before taxes last year?”, with categorical responses: 1= < $10,000, 2=$10,000–$24,999, 3=$25,000–$49,999, 4=$50,000–$74,999, 5=$75,000–$99,999, 6=$100,000–$149,999, 7=$150,000–$199,999, 8= >$200,000), education level (ie, “What is the highest level of education you have completed?”, with responses: 1=none, 2=elementary, 3=high school, 4=trade, 5=diploma, 6=certificate, 7=bachelor’s, 8=graduate degree), current working status (i.e, “Which of the following best describes your working schedule in your current job?, with responses 1=regular daytime shift, 2=regular evening shift, 3=regular night shift, 4=rotating shift, 5=split shift, 6=irregular schedule/on call), smoking status (ie, “Have you ever smoked at least 100 cigarettes in your life?”, with yes or no responses). Physical activity was recorded based on International Physical Activity Questionnaire (IPAQ) activity score is included as “Total met/min/week”,22 based on the response to questions, “During the last 7 days, on how many days did you do vigorous physical activities like heavy lifting, digging, aerobics or fast bicycling?’, “During the last 7 days, on how many days did you do moderate physical activities like carrying light loads, bicycling at a regular pace or doubles tennis?” or “During the last 7 days, on how many days did you walk for at least 10 minutes at a time?”. The IPAQ sedentary score was calculated as “Total sitting mins/week”, based on question, “During the last 7 days, on how much time did you spend sitting on a weekday?”. Alcohol consumption (ie, “On average, over the last year, how often did you drink alcohol?”, with responses 0=never, 1=less than monthly, 2=about once a month, 3=two to three times a month, 4=once a week, 5=two to three times a week, 6=four to five times a week, 7=six to seven times a week) and binge drinking behaviour (ie, “During the past 12 months, how often did you have five or more drinks at the same sitting or occasion?”, with responses 0=never, 1=1 to 5 times a year, 2=6 to 11 times a year, 3=about once a month, 4=2 to 3 times a month, 5=once a week, 6=2 to 3 times a week, 7=4 to 5 times a week, 8=6 to 7 times a week) were also recorded.
Statistical Analysis
Data were analysed using the R statistical software (Version 3.5.1)23 Descriptive statistics used mean and standard deviation for continuous variables, and frequencies and percentages for categorical variables. To investigate the association of ethnic category and sex with sleep duration, multivariate generalized linear models24 were fitted. The principal outcome was continuous sleep duration in minutes. Potential covariates investigated in multivariate modelling included: age, nativity (born in Canada or born elsewhere); years spent resident in Canada; body mass index (BMI), general health perception, physician diagnosis of morbidities (high blood pressure [hypertension], high blood glucose, diabetes [gestational, type 1, or type 2], high cholesterol level, depression, stroke, sleep apnoea, cardiovascular conditions [heart disease and previous myocardial infarction], total physical activity (IPAQ score), tobacco smoke exposure, alcohol consumption, binge drinking, highest education level, residential location (rural/urban), employment status, total household income, and current shift worker.
Quadratic terms for age and BMI were investigated in order to account for non-linear association of these variables with sleep duration. Interaction terms for sex:ethnicity, age:ethnicity, and sex:age were investigated.
Secondary analyses were performed on sleep duration as a categorical variable to enable comparison with previous studies7 and with the current recommendations of 7–9 hours of sleep per day from the National Sleep Foundation25 and American Thoracic Society.1 Sleep duration was categorized as: “short sleep” (<7 hours), “average sleep” (7 to 9 hours), or “long sleep” (>9 hours). Univariate analyses were conducted to investigate the association of ethnic category and categorical sleep duration using a Chi-square test of independence. Multivariate analyses were conducted by fitting a multinomial logistic regression model with principal explanatory variables ethnicity (categorical) and sex (binary).
In order to fully assess the clinical implications of the current study, secondary analyses were performed to investigate the univariate and multivariate associations (logistic regression) of the morbidity outcomes investigated with (a) ethnicity and (b) sleep duration.
Questions answered as “Prefer not to answer” or “Do not know” were coded as missing. All P-values were two-tailed.
Results
The final study population consisted of 143,307 participants with complete data on sleep duration, ethnicity, age, sex and residential location. Of these, 87,357 (61.0%) had missing values in one or more other variables.
Demographic Characteristics
Table 1 describes the demographic characteristics of the cohort. Compared to Statistics Canada Census data from 2011,26 there was a higher percentage of women in the OHS cohort and participants were older than the general population. In the OHS cohort, there was an overrepresentation of participants of “White” ancestry (79% vs 74% in the 2011 Census data). All other ethnic groups were slightly underrepresented in the OHS; however, the overall pattern of distribution was similar to that of the Census data (Table 1). A total of 8.3% of participants reported more than one ethnicity and were classified as “Mixed” ethnicity, in contrast to the 2011 Census data where only 0.8% reported more than 1 ethnicity. Of the study sample, approximately 20% of the cohort belonged to ethnic minorities of which Chinese (3.8%), South Asian (3.4%) and Black (1.4%) ethnicities formed the majority (Table 1). All other ethnicity minority groups (Aboriginal, Arab, East-Asian, Filipino, Japanese, Korean, Hispanic, South-East Asian and West Asian) each formed <1% of the cohort.
 |
Table 1 Demographic Characteristics of the OHS Cohort Compared to the Ontario General Population Using Statistics Canada 2011 Census Data |
Sleep Duration as a Continuous Outcome
Table 2 summarizes the distribution of average sleep duration stratified by gender and ethnicity. Univariate analyses indicated that average sleep duration varied significantly between ethnic groups in the cohort as a whole and in men and women separately (all P<0.001). Women reported sleeping longer on average than men across all ethnic groups, with the longest average sleep times observed in West Asian women (Table 2; 7.49 hours, SD 1.44). For women, the shortest average sleep durations were observed in Filipino (6.99 hours, SD 1.19), Black (6.99 hours, SD1.44), and Japanese participants (7.08, SD 0.98). Similarly, Filipino (6.82 hours, SD 1.08), Black (6.91 hours, SD 1.33) and Japanese men (6.94 hours, SD 1.14) reported the shortest sleep durations.
 |
Table 2 Average Sleep Duration by Gender and Ethnicity (in Hours) |
Multivariate linear models (Table 3) fitted to mean sleep duration in the entire cohort confirmed the univariate observations. Independently significant covariates included in the final multivariate model were: age, age2, BMI, measures of physical activity (IPAQ), location (urban/rural), general health perception, household income, current employment, highest education level, shift work status, alcohol intake, frequency of binge drinking, diagnosed stroke and high blood glucose, trouble sleeping, nativity, and years resident in Canada.
 |
Table 3 Association of Ethnicity with Mean Sleep Duration (in Minutes): Final Linear Regression Model, Adjusted for Significant Covariates |
After adjustment for extensive demographic and risk factors, estimated average sleep duration was significantly shorter (P<0.001) in Black, Chinese, Filipino, Japanese, and mixed ethnicity participants compared to White participants (Table 3). Similarly, Korean (P=0.01) and South Asian (P=0.05) participants had significantly shorter sleep duration than White participants (Table 3). Sleep duration for the Aboriginal, Arab, Hispanic, and West Asian ethnic groups did not significantly differ either from each other or from the White reference category. Multivariate analysis estimated that on average men slept less than women (P<0.001). There was evidence of a significant interactions between sex:age (P<0.001) and sex:ethnicity (P=0.034) but not age:ethnicity (P=0.969); the effects of both age and ethnicity were greater in men.
Sleep Duration as a Categorical Outcome
Univariate analysis of sleep duration as a categorical variable produced consistent results for men and women (Table 4), with a high proportion of short sleepers (sleep duration <7 hours) in those of Filipino (51% men, 44% women), Black (46% men, 44% women), and Japanese (41% men, 31% women) ancestry. The ethnic group with the highest proportion of long sleepers (sleep duration >9 hours) was the Aboriginal group (men 7.2%, women 8%) (Table 4). West Asian (7%) and Black (5%) women had high proportions of long sleepers; Korean men had a high proportion (6.8%) of long sleepers.
 |
Table 4 Sleep Duration as a Categorical Variable by Gender and Ethnicity |
Multivariate logistic models (Table 5) fitted to categorical sleep duration confirmed the univariate associations. Relative to the White reference groups, the prevalence of short sleeping was significantly more common in all ethnic groups except for Hispanics. Short sleeping was common in the Filipino (OR=3.00, 95% CI=2.59 to 3.47), Black (OR=2.51, 95% CI=2.26 to 2.78), and Southeast Asian (OR=1.69, 95% CI=1.39 to 2.06) ethnic groups, consistent with the data in Table 3. Long sleepers were most prevalent in the Aboriginal (OR=2.04, 95% CI=1.57 to 2.66), West Asian (OR=1.81, 955 CI=1.24 to 2.66), Korean (OR=1.77, 95% CI=1.09 to 2.88), and Black (OR=1.53, 95% CI=1.20 to 1.96) ethnic groups (Table 5). Independently significant covariates included in the final multivariate model were: sex, age, BMI, nativity, and years resident in Canada.
 |
Table 5 The Association of Ethnicity with Sleep Duration (Short or Long): Multinomial Logistic Regression Comparing Short (<7 Hours) and Long (>9 Hours) to Average (7–9 Hours) Sleep Time* |
The Association of Morbidity Outcomes with Ethnicity and Sleep Duration
The prevalence of morbidities differed significantly between ethnic groups (all P <0.001) (Table 6). Physician diagnosed high blood glucose, diabetes, heart disease, myocardial infarction, stroke, depression, sleep apnoea, and poor general health perception were all most prevalent in participants of Aboriginal descent (Table 6). The proportion of participants reporting a diagnosis of high cholesterol level was highest amongst participants of Japanese followed by those of Arab, Aboriginal, and White descent. Hypertension was most prevalent amongst Japanese participants, followed by the Aboriginal, White and Black ethnic groups (Table 6). Multivariate logistic models (analyses not shown) confirmed the univariate associations; after adjustment for many other risk factors including sleep duration, ethnicity was independently associated with risk of self-reported high blood pressure, high blood glucose, diabetes, high cholesterol levels, depression, stroke, OSA (all P<0.001), and heart disease (P=0.028).
 |
Table 6 Characteristics of the Study Sample by Ethnicity |
Univariate analyses suggested that higher average sleep duration was associated with physician diagnosed depression and stroke (all P<0.001; Table 6). Conversely, lower average sleep duration was associated with physician diagnosed hypertension, high cholesterol levels, and sleep apnoea (all P<0.001; Table 6). Average sleep duration was highest for those with both the best and worst perceptions of general health (P<0.001; data not shown). Multivariate logistic models (analysis not shown) confirmed the univariate associations; after adjustment for many other risk factors including ethnicity, longer sleep duration (continuous covariate) was independently associated with an increased risk of physician diagnosed: high blood glucose (OR=1.05, 95% CI=1.02 to 1.08, P<0.001), diabetes (OR=1.03, 95% CI=1.01 to 1.06, P=0.016), high cholesterol levels (OR=1.05, 95% CI=1.03 to 1.07, P<0.001), depression (OR=1.21, 95% CI=1.18 to 1.23, P<0.001), and stroke (OR=1.10, 95% CI=1.03 to 1.16, P=0.002). Similarly, shorter sleep duration (continuous covariate) was independently associated with an increased risk of physician diagnosed OSA (OR=0.96, 95% CI=0.93 to 0.98, P=0.002).
Ethnicity and Sleep Quality
Self-reported sleep quality was associated with a linear trend in average sleep duration; poorer sleep was associated with decreasing sleep duration (P<0.001; data not shown) Troubled sleep differed significantly by ethnicity (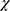 248=1794.2, P<0.001) (Table 7). Aboriginal participants reported experiencing the most trouble sleeping compared to other ethnic groups, with over 25% of participants reporting troubled sleep most or all of the time. Approximately 6% of Chinese participants reported experiencing trouble sleeping most or all of the time, compared to 10% of Filipino, Japanese, South Asian, West Asian or Korean participants; 12% of Hispanic participants, 14% of Arab and Black participants, 21% of Mixed participants, 17% of White participants, and 9% of South-East Asian participants (Table 7).
248=1794.2, P<0.001) (Table 7). Aboriginal participants reported experiencing the most trouble sleeping compared to other ethnic groups, with over 25% of participants reporting troubled sleep most or all of the time. Approximately 6% of Chinese participants reported experiencing trouble sleeping most or all of the time, compared to 10% of Filipino, Japanese, South Asian, West Asian or Korean participants; 12% of Hispanic participants, 14% of Arab and Black participants, 21% of Mixed participants, 17% of White participants, and 9% of South-East Asian participants (Table 7).
 |
Table 7 Distribution of “Trouble Sleeping” Question by Ethnicity* |
Discussion
Principal Findings
We have conducted the largest research study to date that has examined ethnic differences in sleep duration in a general adult population sample. We report significant ethnic differences in sleep duration that were further modified by sex. In our study, mean sleep duration was shorter in Filipino, Black, Japanese, Chinese, and Mixed participants compared to participants of White origin. We found that women on average sleep longer than men in all ethnic groups, consistent with previous findings.14 We have further demonstrated the independent associations of sleep duration and ethnicity with a number of important morbidities: depression, diabetes, high cholesterol levels, heart disease, stroke, sleep apnoea, and perception of general health (Table 6).
Strengths and Weaknesses of the Current Study
The ethnicity related differences in self-reported sleep duration were independent of a large range of socioeconomic, environmental, and biological risk factors. The modulating effect of sex was apparent in the multivariate models. However, the effect sizes and odds ratios observed in our study were of modest magnitude, suggesting that biological, environmental/cultural, and/or psychosocial factors16,27-29 other than ethnicity also play a role in determining average sleep duration. In addition, differences between the White ethnic group and the Chinese (7 min less than White) and Mixed (4 min less than White; Table 2) groups were small and may not be clinically significant.
A strength of the current study is the large and ethnically diverse population-based sample available from the OHS and the use of standardized data capture in the form of an online questionnaire that ensured internal validity. Our study is both substantially larger than all previous published studies - the next largest study was of 29,818 adults17 - and considered a far more heterogenous and ethnically diverse sample of adults, which increases generalizability to other populations. Ethnic diversity related to ongoing immigration and admixture is an increasingly relevant characteristic of industrialized societies such as Canada and other Organization for Economic Cooperation and Development (OECD) nations and has been under-investigated apropos sleep.
The limitations of our study primarily relate to the cross-sectional study design, to potential selection and reporting biases, and potential confounding factors. Although more robust than many “conventionally” recruited epidemiology cohorts, the OHS is not a perfectly representative sample of the general adult population of Ontario. Uniquely for a large cohort study at the time all data were collected using an online questionnaire. The available evidence suggests that responses to online questionnaires are comparable in accuracy to questionnaires administered in person or self-reported on paper.30 It is possible that our recruitment strategy may have encouraged participants more proficient in use of the internet or with better internet access to participate, thus affecting the external validity of the study and limiting the generalizability of the findings. However, comparison to Ontario census data (Table 1) suggested that a robust sample broadly representative of the general population of Ontario was collected, making this unlikely. Objective measurements of sleep duration and morbidities were not collected, which may contribute to lack of precision in the outcome data. However, there is evidence that self-reported history of physician-diagnosed chronic health conditions can have high specificity and sensitivity.31,32 Only self-reported items were used (with no use of standardized questionnaires or objective measurements of sleep duration or morbidities) which may contribute to recall and assessment bias. Another limitation is that the one question on sleep duration requested the subject to include nap time. The current study thus cannot discriminate between individuals with excessive daytime sleepiness or those with poor sleep hygiene due to split sleep times, and cannot, therefore, be directly compared to previous studies that asked questions on nocturnal sleep duration.
It has been observed that comparison of objective measures of sleep duration (actigraphy and polysomnography) and self-reported sleep duration leads to an overestimation of sleep time for subjective recall of sleep duration.33,34 In addition, the cross-sectional design of the study does not account for variability in sleep duration and timing between weekdays and weekends, or seasonally.35,36 Future research will thus be needed in order to explore these relationships.
A possible explanation for the observed differences in sleep duration between ethnic groups may be potential “confounding” due to disparity in socio-economic position among ethnic groups, as socio-economic position differs by ethnicity (ie, inequality)29 and has been previously associated with reduced sleep duration and quality.37,38 Note that this is not true confounding, as socio-economic factors cannot cause ethnicity. The effect of socioeconomic status (eg, the clustering of education level, rural/urban residential location, employment status or household income), across ethnic groups may be particularly important and influential as it may emphasize differences within Whites and between average-to-high socioeconomic status Whites and all other ethnic groups, potentially regardless of SES.39,40
Health disparities among different ethnic minorities are similarly “confounded” by differences in psychosocial factors such as stress, self-esteem, mental illness, access to health care, neighbourhood characteristics (crime, safety, air pollution, noise) which can all disrupt normal physiological functioning including sleep.14 However, we found significant differences in sleep duration in multivariate analysis after controlling for many of these variables (Tables 3 and 5), suggesting that the associations are robust. It is possible that more sensitive indicators of neighbourhood stress and disruption are required41 and may explain some of the disparity in sleep duration in the cohort.
Comparison to Previous Studies
Our findings should be considered in the context of previous studies in both Canadian and other populations exploring sleep duration and ethnicity. Prior literature on sleep duration has been largely based on data from populations of predominantly European ancestry.42 The Canadian population, particularly that of Ontario, is ethnically diverse and hence advantageous to study because of the relatively large proportion of visible minorities with sufficient cases to meaningfully explore ethnic differences in sleep. Differences in sleep duration among the largest ethnic groups in the US (White, Black and Hispanic groups) have been identified.29,42 However, there is a dearth of data on sleep duration in other ethnic minorities. There is also no obvious explanation for the differences in sleep duration observed.
The 2010 General Social Survey (GSS)43 reported mean sleep duration in a small sample (n=15,390) of the general Canadian population (aged 15 years and over) to be 8 hours 18 mins. In contrast, the crude estimate of mean sleep duration in the OHS (aged 18 years and over) was almost 1 hour less (7 hours 21 mins in the entire cohort). These differences could reflect differences in age distribution, sampling biases, and/or a more accurate estimate in the much larger OHS sample.
Our findings are consistent with the many prior studies that have documented the close and potentially causal relationships of both sleep duration and ethnicity with a range of morbidities,44–46 including cardio-metabolic outcomes,47–50 hypertension,51,52 stroke,53,54 and depression.55,56 Our findings and those of prior studies highlight the potential clinical impact of ethnicity-driven short and long sleep duration. Despite Canada being a high-immigration country and non-Western immigrants’ having systematically higher morbidity than ethnic White Canadians, no national strategy targeting immigrants’ health has been implemented. Future research should emphasize a life-course perspective and include the children of immigrants.
Clinical Implications
Sleep duration has been consistently shown to be an independent predictor of health.1,11 Consistent with previous research, sleep duration was associated a range of important physician-diagnosed clinical outcomes in our study, including depression44 and stroke44 (long sleep duration), and hypertension,45 hypercholesterolemia46 and sleep apnea47,48 (short sleep duration). Almost all adults sampled in the current study were on the lower range or below accepted norms for healthy sleep.1,11 This finding is even more striking given the known tendency of self-report to overestimate sleep duration.34 Important differences exist in self-reported mean sleep duration between ethnicities and may contribute to ethnic group differences in the prevalence of sleep disorders and other chronic diseases. To the best of our knowledge, there are no published guidelines regarding the threshold for “clinical significance” in sleep duration in the general population. Using RCTs of pharmacotherapy in insomnia patients as a guide,57 a “clinically significant” difference in total sleep duration can be as little as 8–10 minutes. However, we feel that a difference of at least 20 minutes total sleep duration is a more reasonable threshold for “clinical significance”. Our study reaches this threshold for the Black, Filipino, and Japanese ethnic groups relative to the White reference group (Table 4). Measures to increase sleep duration in ethnic minority populations may help to reduce ethnic health inequalities. Our results highlight the need for gender- and ethnicity-specific targeted education on the importance of prioritizing sleep for overall health, and the need to account appropriately for ethnicity in future clinical and translational research into sleep and related conditions. Further study and elucidation of the factors involved in determining differences in sleep duration among different ethnic groups is warranted.
Conclusion
Poor sleep has an impact on general health and lifestyle and is also associated with increased morbidity. On average, Canadian adults are sleep restricted or at the lower end of recommended guidelines for healthy sleep. We found that significant ethnic differences exist for self-reported sleep duration among residents of Ontario, and that both ethnicity and sleep duration were independent risk factors for common chronic diseases. Further research is warranted to investigate the possible factors that contribute to the shorter sleep duration observed in certain ethnic groups and in men, and to implement strategies to improve sleep duration and sleep quality in the Canadian and other populations.
Acknowledgments
We thank Woganee Filate for technical assistance. We also thank the participants in the Ontario Health Study.
Disclosure
Financial disclosure: This work was supported by the Ontario Institute for Cancer Research; Cancer Care Ontario; Public Health Ontario and the Canadian Partnership Against Cancer. Amy Reynolds reports financial reimbursement from Sealy Australia to provide expert scientific commentary on findings of the Sealy Global Sleep Census. The authors report no other conflicts of interest in this work.
Non-financial disclosure: The data used for this research was made available by the Ontario Health Study with the financial support from the Canadian Partnership Against Cancer, Health Canada and the Ontario Institute for Cancer Research. The views expressed herein represent the views of the authors and do not necessarily represent the views of Health Canada or the Government of Ontario.
References
1. Mukherjee S, Patel SR, Kales SN, et al. An official American Thoracic Society statement: the importance of healthy sleep. Recommendations and future priorities. Am J Respir Crit Care Med. 2015;191(12):1450–1458. doi:10.1164/rccm.201504-0767ST
2. Gallicchio L, Kalesan B. Sleep duration and mortality: a systematic review and meta-analysis. J Sleep Res. 2009;18(2):148–158. doi:10.1111/j.1365-2869.2008.00732.x
3. Liu Y, Wheaton AG, Chapman DP, Croft JB. Sleep duration and chronic diseases among U.S. adults age 45 years and older: evidence from the 2010 behavioral risk factor surveillance system. Sleep. 2013;36(10):1421–1427. doi:10.5665/sleep.3028
4. Zizi F, Pandey A, Murrray-Bachmann R, et al. Race/ethnicity, sleep duration, and diabetes mellitus: analysis of the National Health Interview Survey. Am J Med. 2012;125(2):162–167. doi:10.1016/j.amjmed.2011.08.020
5. Gangwisch JE, Heymsfield SB, Boden-Albala B, et al. Sleep duration as a risk factor for diabetes incidence in a large U.S. sample. Sleep. 2007;30(12):1667–1673. doi:10.1093/sleep/30.12.1667
6. Kim JH, Kim KR, Cho KH, Yoo KB, Kwon JA, Park EC. The association between sleep duration and self-rated health in the Korean general population. J Clin Sleep Med. 2013;9(10):1057–1064. doi:10.5664/jcsm.3082
7. Cappuccio FP, D’Elia L, Strazzullo P, Miller MA. Sleep duration and all-cause mortality: a systematic review and meta-analysis of prospective studies. Sleep. 2010;33(5):585–592. doi:10.1093/sleep/33.5.585
8. Gangwisch JE, Heymsfield SB, Boden-Albala B, et al. Sleep duration associated with mortality in elderly, but not middle-aged, adults in a large US sample. Sleep. 2008;31(8):1087–1096.
9. Cai H, Shu X-O, Xiang Y-B, et al. Sleep duration and mortality: a prospective study of 113,138 middle-aged and elderly Chinese men and women. Sleep. 2015;38(4):529–536. doi:10.5665/sleep.4564
10. Priou P, Le Vaillant M, Meslier N, et al. Cumulative association of obstructive sleep apnea severity and short sleep duration with the risk for hypertension. PLoS One. 2014;9(12):e115666. doi:10.1371/journal.pone.0115666
11. Watson NF, Badr MS, Belenky G, et al. Recommended amount of sleep for a healthy adult: a joint consensus statement of the American Academy of Sleep Medicine and Sleep Research Society. Sleep. 2015;38(6):843–844. doi:10.5665/sleep.4716
12. National Sleep Foundation. Summary Findings of Sleep in America; Sleep and Ethnicity; 2010.
13. Hale L, Guan S. Screen time and sleep among school-aged children and adolescents: a systematic literature review. Sleep Med Rev. 2015;21:50–58. doi:10.1016/j.smrv.2014.07.007
14. Knutson KL. Sociodemographic and cultural determinants of sleep deficiency: implications for cardiometabolic disease risk. Soc Sci Med. 2013;79:7–15. doi:10.1016/j.socscimed.2012.05.002
15. Lauderdale DS, Knutson KL, Yan LL, et al. Objectively measured sleep characteristics among early-middle-aged adults: the CARDIA study. Am J Epidemiol. 2006;164(1):5–16. doi:10.1093/aje/kwj199
16. Redline S, Kirchner HL, Quan SF, Gottlieb DJ, Kapur V, Newman A. The effects of age, sex, ethnicity, and sleep-disordered breathing on sleep architecture. Arch Intern Med. 2004;164(4):406–418. doi:10.1001/archinte.164.4.406
17. Nunes J, Jean-Louis G, Zizi F, et al. Sleep duration among black and white Americans: results of the National Health Interview Survey. J Natl Med Assoc. 2008;100(3):317–322. doi:10.1016/S0027-9684(15)31244-X
18. Chaput JP, Wong SL, Michaud I. Duration and quality of sleep among Canadians aged 18 to 79. Health Rep. 2017;28(9):28–33.
19. Statistics Canada. Visual census. 2006 Census. Ottawa; 2010. Available from: http://www12.statcan.gc.ca/census-recensement/2006/dp-pd/fs-fi/index.cfm?Lang=ENG&TOPIC_ID=11&PRCODE=35.
20. Statistics Canada. Canada’s Ethnocultural Mosaic, 2006 Census; 2008.
21. Ontario Health Study. Available from: https://ontariohealthstudy.ca.
22. Craig CL, Marshall AL, Sjostrom M, et al. International physical activity questionnaire: 12-country reliability and validity. Med Sci Sports Exerc. 2003;35(8):1381–1395. doi:10.1249/01.MSS.0000078924.61453.FB
23. Ihaka R, Gentleman R. R: a language for data analysis and graphics. J Comput Graph Stat. 1996;5:299–314.
24. McCullagh PNJ. Generalized Linear Models. Chapman and Hall; 1989.
25. Hirshkowitz M, Whiton K, Albert SM, et al. National Sleep Foundation’s updated sleep duration recommendations: final report. Sleep Health. 2015;1(4):233–243. doi:10.1016/j.sleh.2015.10.004
26. Statistics Canada. National Household Survey Profile, Ontario; 2011.
27. Dijk DJ, Beersma DG, Bloem GM. Sex differences in the sleep EEG of young adults: visual scoring and spectral analysis. Sleep. 1989;12(6):500–507. doi:10.1093/sleep/12.6.500
28. Walsemann KM, Ailshire JA, Fisk CE, Brown LL. Do gender and racial/ethnic disparities in sleep duration emerge in early adulthood? Evidence from a longitudinal study of U.S. adults. Sleep Med. 2017;36:133–140. doi:10.1016/j.sleep.2017.03.031
29. Adenekan B, Pandey A, McKenzie S, Zizi F, Casimir GJ, Jean-Louis G. Sleep in America: role of racial/ethnic differences. Sleep Med Rev. 2013;17(4):255–262. doi:10.1016/j.smrv.2012.07.002
30. Campbell N, Ali F, Finlay AY, Salek SS. Equivalence of electronic and paper-based patient-reported outcome measures. Qual Life Res. 2015;24(8):1949–1961. doi:10.1007/s11136-015-0937-3
31. Oksanen T, Kivimaki M, Pentti J, Virtanen M, Klaukka T, Vahtera J. Self-report as an indicator of incident disease. Ann Epidemiol. 2010;20(7):547–554. doi:10.1016/j.annepidem.2010.03.017
32. Okura Y, Urban LH, Mahoney DW, Jacobsen SJ, Rodeheffer RJ. Agreement between self-report questionnaires and medical record data was substantial for diabetes, hypertension, myocardial infarction and stroke but not for heart failure. J Clin Epidemiol. 2004;57(10):1096–1103. doi:10.1016/j.jclinepi.2004.04.005
33. Kurina LM, McClintock MK, Chen JH, Waite LJ, Thisted RA, Lauderdale DS. Sleep duration and all-cause mortality: a critical review of measurement and associations. Ann Epidemiol. 2013;23(6):361–370. doi:10.1016/j.annepidem.2013.03.015
34. Cespedes EM, Hu FB, Redline S, et al. Comparison of Self-Reported Sleep Duration With Actigraphy: results From the Hispanic Community Health Study/Study of Latinos Sueno Ancillary Study. Am J Epidemiol. 2016;183(6):561–573. doi:10.1093/aje/kwv251
35. Roenneberg T, Allebrandt KV, Merrow M, Vetter C. Social jetlag and obesity. Curr Biol. 2012;22(10):939–943. doi:10.1016/j.cub.2012.03.038
36. Kasper S, Wehr TA, Bartko JJ, Gaist PA, Rosenthal NE. Epidemiological findings of seasonal changes in mood and behavior. A telephone survey of Montgomery County, Maryland. Arch Gen Psychiatry. 1989;46(9):823–833.
37. Stamatakis KA, Kaplan GA, Roberts RE. Short sleep duration across income, education, and race/ethnic groups: population prevalence and growing disparities during 34 years of follow-up. Ann Epidemiol. 2007;17(12):948–955. doi:10.1016/j.annepidem.2007.07.096
38. Geroldi C, Frisoni GB, Rozzini R, De Leo D, Trabucchi M. Principal lifetime occupation and sleep quality in the elderly. Gerontology. 1996;42(3):163–169. doi:10.1159/000213788
39. Puckrein GA, Egan BM, Howard G. Social and medical determinants of cardiometabolic health: the big picture. Ethn Dis. 2015;25(4):521–524. doi:10.18865/ed.25.4.521
40. Wi CI, St Sauver JL, Jacobson DJ, et al. Ethnicity, socioeconomic status, and health disparities in a mixed rural-urban US Community-Olmsted County, Minnesota. Mayo Clin Proc. 2016;91(5):612–622. doi:10.1016/j.mayocp.2016.02.011
41. Johnson DA, Thorpe RJ, McGrath JA, Jackson WB, Jackson CL. Black-White Differences in Housing Type and Sleep Duration as Well as Sleep Difficulties in the United States. Int J Environ Res Public Health. 2018;15(4):564. doi:10.3390/ijerph15040564
42. Loredo JS, Soler X, Bardwell W, Ancoli-Israel S, Dimsdale JE, Palinkas LA. Sleep health in U.S. Hispanic population. Sleep. 2010;33(7):962–967. doi:10.1093/sleep/33.7.962
43. Statistics Canada. General Social Survey-2010 Overview of the Time Use of Canadians. 2010. Available from: https://www150.statcan.gc.ca/n1/pub/89-647-x/89-647-x2011001-eng.htm.
44. Itani O, Jike M, Watanabe N, Kaneita Y. Short sleep duration and health outcomes: a systematic review, meta-analysis, and meta-regression. Sleep Med. 2017;32:246–256. doi:10.1016/j.sleep.2016.08.006
45. Jervelund SS, Malik S, Ahlmark N, Villadsen SF, Nielsen A, Vitus K. Morbidity self-perceived health and mortality among non-western immigrants and their descendants in Denmark in a life phase perspective. J Immigr Minor Health. 2017;19(2):448–476. doi:10.1007/s10903-016-0347-9
46. Jike M, Itani O, Watanabe N, Buysse DJ, Kaneita Y. Long sleep duration and health outcomes: A systematic review, meta-analysis and meta-regression. Sleep Med Rev. 2018;39:25–36. doi:10.1016/j.smrv.2017.06.011
47. Cappuccio FP, Miller MA. Sleep and cardio-metabolic disease. Curr Cardiol Rep. 2017;19(11):110. doi:10.1007/s11886-017-0916-0
48. Graham G. Disparities in cardiovascular disease risk in the United States. Curr Cardiol Rev. 2015;11(3):238–245. doi:10.2174/1573403X11666141122220003
49. Gazzola K, Reeskamp L, van den Born BJ. Ethnicity, lipids and cardiovascular disease. Curr Opin Lipidol. 2017;28(3):225–230. doi:10.1097/MOL.0000000000000412
50. St-Onge MP, Grandner MA, Brown D, et al. Sleep duration and quality: impact on lifestyle behaviors and cardiometabolic health: a scientific statement from the American Heart Association. Circulation. 2016;134(18):e367–e386. doi:10.1161/CIR.0000000000000444
51. Modesti PA, Reboldi G, Cappuccio FP, et al. Panethnic differences in blood pressure in Europe: a systematic review and meta-analysis. PLoS One. 2016;11(1):e0147601. doi:10.1371/journal.pone.0147601
52. Wang Y, Mei H, Jiang YR, et al. Relationship between duration of sleep and hypertension in adults: a meta-analysis. J Clin Sleep Med. 2015;11(9):1047–1056. doi:10.5664/jcsm.5024
53. Boehme AK, Esenwa C, Elkind MS. stroke risk factors, genetics, and prevention. Circ Res. 2017;120(3):472–495. doi:10.1161/CIRCRESAHA.116.308398
54. McDermott M, Brown DL, Chervin RD. Sleep disorders and the risk of stroke. Expert Rev Neurother. 2018;18(7):523–531. doi:10.1080/14737175.2018.1489239
55. Zhai L, Zhang H, Zhang D. Sleep duration and depression among adults: a meta-analysis of prospective studies. Depress Anxiety. 2015;32(9):664–670. doi:10.1002/da.22386
56. Patil PA, Porche MV, Shippen NA, Dallenbach NT, Fortuna LR. Which girls, which boys? The intersectional risk for depression by race and ethnicity, and gender in the U.S. Clin Psychol Rev. 2018;66:51–68. doi:10.1016/j.cpr.2017.12.003
57. Elie R, Ruther E, Farr I, Emilien G, Salinas E. Sleep latency is shortened during 4 weeks of treatment with zaleplon, a novel nonbenzodiazepine hypnotic. Zaleplon clinical study group. J Clin Psychiatry. 1999;60(8):536–544. doi:10.4088/JCP.v60n0806
 © 2020 The Author(s). This work is published and licensed by Dove Medical Press Limited. The full terms of this license are available at https://www.dovepress.com/terms.php and incorporate the Creative Commons Attribution - Non Commercial (unported, v3.0) License.
By accessing the work you hereby accept the Terms. Non-commercial uses of the work are permitted without any further permission from Dove Medical Press Limited, provided the work is properly attributed. For permission for commercial use of this work, please see paragraphs 4.2 and 5 of our Terms.
© 2020 The Author(s). This work is published and licensed by Dove Medical Press Limited. The full terms of this license are available at https://www.dovepress.com/terms.php and incorporate the Creative Commons Attribution - Non Commercial (unported, v3.0) License.
By accessing the work you hereby accept the Terms. Non-commercial uses of the work are permitted without any further permission from Dove Medical Press Limited, provided the work is properly attributed. For permission for commercial use of this work, please see paragraphs 4.2 and 5 of our Terms.
