Back to Journals » Journal of Multidisciplinary Healthcare » Volume 15
The Magnitude of Anxiety and Depressive Symptoms Among Tuberculosis Patients in Community Health Centers Setting During the Peak of COVID-19 Pandemic
Authors Sunjaya DK , Paskaria C , Pramayanti M, Herawati DMD , Parwati I
Received 22 January 2022
Accepted for publication 31 March 2022
Published 8 April 2022 Volume 2022:15 Pages 755—764
DOI https://doi.org/10.2147/JMDH.S359530
Checked for plagiarism Yes
Review by Single anonymous peer review
Peer reviewer comments 6
Editor who approved publication: Dr Scott Fraser
Deni Kurniadi Sunjaya,1 Cindra Paskaria,2 Meisera Pramayanti,1 Dewi Marhaeni Diah Herawati,1 Ida Parwati3
1Department of Public Health, Faculty of Medicine, Universitas Padjadjaran, Bandung, Indonesia; 2Department of Public Health, Faculty of Medicine, Maranatha Christian University, Bandung, Indonesia; 3Department of Clinical Pathology, Faculty of Medicine, Universitas Padjadjaran, Bandung, Indonesia
Correspondence: Deni Kurniadi Sunjaya, Faculty of Medicine, Universitas Padjadjaran, Jalan Eyckman No. 38, Bandung, Indonesia, Tel +62 82218893543, Email [email protected]
Background: Mental health problems can occur in patients with chronic diseases such as tuberculosis, and the stress of a pandemic exacerbates the condition. The study aims to explore the magnitude of anxiety and depressive symptoms in tuberculosis (TB) patients in community health centers (CHCs) settings during the COVID-19 pandemic.
Methods: The study design was quantitative and cross-sectional. Subjects were TB patients who were recruited from TB services by doctors in CHCs. TB patients (n=74) were screened for anxiety and depressive symptoms over 4 months. Screening results are uploaded on a cloud-based digital platform and analyzed. Non-TB patients, as a comparison, were recruited and screened from the same cloud-based digital platform (n=245) during the same period. Analysis was carried out using Rasch modeling for data transformation. Data was analyzed then for frequency distribution for both groups and the logistic binaries to measure the burden of the mixed anxiety and depressive symptoms among the TB patient age’s sub-group.
Results: In both groups, there were 48.9% of mild, moderate, and severe categories of anxiety and 63.9% of depressive symptoms. In the TB-patients group, anxiety occurred at 48.7%, of which 23% were in the moderate and severe categories, compared to 13.4% for non-TB patients. Depressive symptoms were present in 71.6% of the TB patient group, of which 28.4% were in the moderate and severe categories, compared to 15.5% of non-TB patients. TB patients aged less than 20 years experienced moderate–severe anxiety with depressive symptoms simultaneously (mixed) as much as 16.3% or 4.6 times more than those aged over 20 years (p< 0.05).
Conclusion: Moderate and severe anxiety and depressive symptoms were shown higher in the TB patients’ group. Adolescents with TB are more susceptible to mental and emotional disorders.
Keywords: tuberculosis, pandemic COVID-19, mental health screening, patient-centered, primary health care
Introduction
In 2021, Indonesia had the third-highest prevalence of TB in the world after India and China.1 Only 46% of registered TB patients have successful treatment. Older patients are associated with poor TB treatment, due to management difficulties, drug resistance, and can be transmitted over time.2
Chronic and complex treatment of TB disease can lead to mental emotional and other psychiatric disorders in TB patients.3,4 TB is treated for 6 months with many drugs to be taken. Mental disorders can lead to poor drug adherence and low treatment success.5 In addition, they are also a driver of multidrug-resistant TB (MDR-TB) and death.6,7 Depression is associated with disability, poor quality of life, treatment failure, and death.8,9 Depression may pose a risk of not achieving the final TB strategy.8
Psychiatric problems often occur in patients who suffer from chronic diseases.10–12 Lung disease is a chronic disease that is strongly associated with psychiatric disorders,13 such as tuberculosis, Chronic Obstructive Pulmonary Disease (COPD),14 and asthma.15 Previous studies have shown that TB patients have a higher prevalence of anxiety and depression than general patients.16,17 The mental problems that occur are included anxiety and depression.18
The COVID-19 pandemic is affecting the mental health of global communities such as China, Spain, Italy, Iran, the USA, Turkey, Nepal, and Denmark. In these countries, there is an increase in symptoms of anxiety, depression, post-traumatic stress disorder, psychological stress and varying stress.19 The COVID-19 pandemic has also affected mental health in countries such as America, Asia, and Europe, where Poland and Pakistan have the highest scores on anxiety, depression, and stress compared to Vietnam.20,21
Indonesia experienced the highest pressure of the COVID-19 pandemic period from June to August 2021. This peak of the wave of COVID-19 in 2021 has caused service disruption as experienced in 2020 as well.22 On the other hand, the pandemic causes psychological stress that can result in mental and emotional disorders for the public in general.23 Thus, there were multiple psychological burdens for the TB patient due to treatment, service processes,24 and the pandemic situation. Some of the burdens are anxiety and depressive symptoms. The tuberculosis program and services as an essential service must continue, so there will be no hindrance to achieving the zero TB agenda in the year 2035.
Improving the quality of TB programs and services with a patient-centered approach has long been recommended by WHO.25 Patient-centered care is carried out holistically, where service is not only provided for physical aspects but the mental health aspects as well.26 However, the practice of treatment in health care facilities is still fragmented. TB cases are not treated adequately and mental health is not given attention in the TB program.27,28 Tuberculosis services are an essential program in primary health care. Therefore, integrating tuberculosis and mental health care can reduce costs, improve the quality of care and patient life, and ultimately save lives.29
In Indonesia today, almost no health workers at CHCs perform procedures for mental health diagnosis in TB patients. Whereas, the detection of mental and emotional disorders is very necessary for the practice of treating TB patients. The study aimed to explore the magnitude of anxiety and depressive symptoms in TB patients during the COVID-19 pandemic. The results of the study are used for policy development on improving the strength and resilience of the TB program, especially in primary health care.
Materials and Methods
Study Context
Indonesia has a population of 270 million people with an estimated 824,000 TB cases, but only 393,323 cases were notified in 2020. This research is under umbrella research, namely the development of District Based Public Private Mix Tuberculosis (DPPM TB), placed in Purwakarta District with a population of 956,057 people (the year 2020). The research was conducted on the ongoing health care system. The number of TB patients was notified at 1920 patients (2021) from the estimated 2289 cases. A total of 964 cases (50.18%) were treated and reported by Community Health Center (CHC), namely Puskesmas: 256 cases (13.33%); by Government Hospitals: 697 cases (36.28%); by private hospitals, while private primary health care facilities had not reported TB cases yet.
Research Design
The research design is quantitative with operational research and a cross-sectional approach. Researchers have been developed an online mental health screening (cloud-based platform) in the umbrella research to facilitate doctors/health facilities, especially for Primary Health Care (PHC) facilities (CHC and private PHC). The cloud-based screening aimed to detect the presence of mental and emotional disorders in TB patients.
As operational research, doctors in primary health services are given a mental health refreshing program and training on the use of mental health screening instruments (anxiety and depressive symptoms) first, including private doctors being involved in the program. They are offered to improve services for TB patients by conducting mental health screening for holistic care practice.
Observation of mental and emotional disorders, where anxiety and depressive symptoms as measured variables,30 was carried out for 4 months in TB patients who visited CHCs. Screening is only done once for one patient. Then the data in this group were compared with data in the group of non-TB patients in the same period and using the same online mental health screening.
Subject
Subjects were TB patients who visited CHC in Purwakarta District in daily practice. The selection was based on convenience sampling. The comparison subjects were non-TB patients who were being screened for mental health through the same digital platform. Inclusion criteria were those who were willing to be involved in this study. Cases with incomplete screening data were excluded.
Data Collection
The instruments used are the Zung Anxiety Scale (20 items) and the CESD R-10 (10 items).31 Validity, reliability, and uni-dimensionality of instruments are shown in Table 1. These instruments are stored on a digital platform and can be used by doctors or health professionals in need. Data collection was carried out for 4 months from July to October in the year 2021 when the wave of COVID-19 was at its peak. TB patient was asked for their involvement in the study and got informed consent. CHC doctors screened TB patients directly during service. Then measurement results on the digital screening platform were saved anonymously. Data analysis was carried out by the researcher using the Rasch model and returned in the form of the anxiety and depressive symptoms status output to the examining doctor, still through the screening platform.
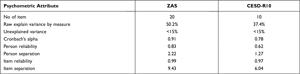 |
Table 1 Psychometric Attribute of the Instrument (n=319) |
During the same period, screening for mental and emotional disorders in the general population is being collected through the same platform. This group is referred to as non-TB patients. We use this group as a comparison. Participants who were successfully recruited during this period were 74 TB patients and 245 non-TB patients.
Data Analysis
Data analysis was carried out by first transforming the ordinal data of all items on each instrument using Rasch modeling (Winsteps application) so that numerical data was obtained from each participant for both anxiety and depressive symptoms status. The numerical data is then categorized based on the mean and standard deviation.
Further analysis was carried out by categorizing the categories of concern, namely moderate and severe. Both become one category (moderate and severe), while the rest (mild and None) become another category, for each instrument. Moderate and severe anxiety and depressive symptoms were analyzed based on gender and age. For the age variable, the concern that arises is the adolescent patient (< 20 years). The tool used is SPSS version 20.
In the population of TB patients, data were identified for those exposed to both anxiety and depression symptoms (mix) and made to the new category. Then a comparison was made between the subgroups of TB patients aged less than 20 years and the older subgroups. Data were reanalyzed using the logistic binary.
Ethical Considerations
This research is following the Declaration of Helsinki and has obtained ethical approval from the Universitas Padjadjaran Ethical Committee No 005/ UN6.KEP/EC/2021 and 723/UN6.KEP/EC/2021. Informed consent was obtained from all subjects before participating in this study, and informants were registered under pseudonyms.
Results
Anxiety
In both TB patient and non-TB patient groups (n=319), there were 48.9% of participants with anxiety in all categories (mild, moderate, and severe). When compared percentage by group, severe anxiety was present in 5.4% of TB patients and 1.6% of non-TB patients. Meanwhile, moderate anxiety was present in 17.6% of TB patients and 11.8% of non-TB patients (Figure 1).
 |
Figure 1 Anxiety in TB patients and non-TB patients group. |
Thus, there is 48.7% anxiety in the TB patient group; where 23% of the 74 tuberculosis patients experienced moderate and severe anxiety. The proportion of moderate and severe anxiety almost doubled in the TB patient group compared to the non-TB patient group.
Depressive Symptoms
For all groups (n=319), 63.9% of participants with depressive symptoms were found in all categories. When compared percentage by group, severe depressive symptoms were present in 2.7% of TB patients and 1.6% of non-TB patients. Meanwhile, moderate depressive symptoms were present in 25.7% of TB patients and 13.9% of non-TB patients (Figure 2).
 |
Figure 2 Depressive symptoms in TB patients and non-TB patients group. |
Thus, there are 71.6% experiencing depressive symptoms; where 28.4% of the 74 tuberculosis patients experienced moderate and severe depressive symptoms. Similar to the situation of anxiety, the proportion of depressive symptoms almost double in the TB patient group compared to the non-TB patient group.
Anxiety and Depressive Symptoms by Gender and Age in TB Patients Group
Exploration carried out in the group of TB patients showed a slightly higher percentage of moderate and severe anxiety in female patients (Table 2). Based on the age group, moderate and severe anxiety was 16.3% in those younger than 20 years old; moderate and severe depressive symptoms were 20.3% in those younger than 20 years old. This situation is more than 2 times that of TB patients older than 20 years old.
 |
Table 2 Mental and Emotional Disorder by Gender and Age (n=74) |
The Mix of Anxiety Along with Depressive Symptoms in TB Patients
There were as many as 14.9% of TB patients exposed to moderate-severe of anxiety along with depressive symptoms. There were 21.6% who got only one of either the moderate-severe anxiety or depressive symptoms. Thus, there are as many as 36.5% of TB patients require attention from the mental and emotional aspects.
Furthermore, as much as 8.1% of the double burden of moderate-severe anxiety with depressive symptoms occurred in female patients which is more than in male patients. For single disorder (anxiety or depressive symptoms), female patients also showed more than men (12.2%).
Exposure to both moderate-severe of anxiety with depressive symptoms occurred more than doubled in patients under 20 years (10.8%) compared to those aged over 20 years (4.1%). A total of 14.9% of patients aged <20 years who had one symptom, more than doubled compared to those aged over 20 years.
This age group under 20 years attracts attention for further analysis. As seen in Table 3, we compared patients who had these multiple psychological burdens (anxiety with depressive symptoms) with those who had only one burden (mild only plus None). The results of the analysis showed that there were TB patients aged less than 20 years who experienced moderate-severe anxiety along with depressive symptoms as much as 4 to 5 times significantly more than those aged more than 20 years.
 |
Table 3 Odds Ratio of Mix Burden of Anxiety with Depressive Symptoms in Adolescent TB Patients |
Discussion
This inquiry has reached two main points, the first is mental suffering in tuberculosis patients, and the second is related to the problem of adolescent TB patients. First, the results showed that the percentage of anxiety and depressive symptoms in tuberculosis patients was higher than that of non-tuberculosis patients. This result is similar to the research of Shen et al and Balaji et al.16,17 This finding is in line with Wang who states that TB patients are very susceptible to mental disorders such as anxiety and depressive symptoms due to long-term treatment and side effects of anti-TB drugs and the effects of TB recurrence.32
The results of this study showed that the percentage of anxiety in TB patients was 48.7%. It is a little bit higher than those of Ambaw et al stated that the prevalence of TB in Ethiopia was 41.5%.33 However, this result was different from the study of Yilmaz et al, who stated that the prevalence of anxiety in Turkey was 26% lower.34 This difference may be due to differences in data collection tools and sample sizes.
The percentage of depressive symptoms in TB patients from the results of this study was 71.6%. This result is higher than studies conducted in India (49–54%)35 and Africa (57%),33 while in Turkey it is higher than India and Africa, 60.5%.34 The high percentage of depressive symptoms in TB patients in the study is probably because the research was conducted when Indonesia was experiencing the peak of the COVID-19 pandemic in 2021.
The percentage of moderate and severe anxiety results of this study showed that women (16.3%) were greater than men (6.8%). This finding is similar to the opinion of Theron et al and van den Heuvel et al, who said that psychological distress was more common in female TB patients.36,37
Second, the results showed that TB patients aged less than 20 years experienced moderate-severe anxiety and depressive symptoms 4.6 times more than those aged over 20 years. These results are different from studies conducted by previous researchers who said that older patients had greater depressive symptoms than younger people.38,39 This difference is since adolescence is a period that susceptible to tuberculosis.40 Adolescence is a developmental age characterized by biological and social changes.41 Or, is the increased stressor (the peak of the pandemic) leaving adolescents susceptible and increasing mental and emotional burden?
Exposure to the COVID-19 pandemic causes high levels of anxiety and depressive symptoms in adolescents.42 This is similar to the results of Chao’s research which says that adolescent mental health increases when facing the COVID-19 pandemic.43 This result is also in line with the opinion of Wang et al, who state that young age increases the risk of depression in TB patients, due to social pressure and feelings of shame about being diagnosed with TB.32 Stigmatization of TB patients still occurs in the community.
Therefore, it is very important in providing health services to tuberculosis patients to pay attention to the mental and emotional state of young patients. So that young patients affected by TB can recover quickly and not fall into a prolonged mental disorder that will eventually aggravate the TB disease they suffer. The patient is seen as a unique individual and should not be generalized. Thus, a patient-centered approach is needed in the treatment of TB.
The COVID-19 pandemic is associated with changes in adolescent mental health such as anxiety and depression.42,43 The results of this study indicate that anxiety and depressive symptoms in adolescent TB patients during the COVID-19 pandemic were higher than in those who did not suffer from TB.
Adolescent TB patients are susceptible to mental disorders. Identifying risk factors and developing treatment to reduce mental disorders in TB patients is beneficial in controlling the disease better and stopping its spread to others and reducing cases of TB drug resistance.44 Anxiety and depression are factors that can affect patient compliance and well-being.44 Furthermore it can be associated with suicidal ideation.45
The suffering of both adolescent and general TB patients does not stop at the magnitude of mental health disorders. The COVID-19 pandemic has disrupted essential services and TB patients are often neglected. Services are very limited, doctors often treat minimally, to reduce the risk of exposure. Thus, the examination of mental health disorders is often neglected as well.
This was also happening in the case of psychiatric patients, only the most severe psychiatric patients were receiving care. The reduction in psychiatric emergency department admission during the pandemic was associated with more severe psychopathologies.46 The peak of the pandemic and disruption of services add to the severity of mental disorders in psychiatric patients, thus requiring a new approach and continuous intervention.47 As a reflection of these two studies, it is necessary to strengthen awareness of TB patients who have mental disorders and take real action on TB programs and services.
Holistic services in the tuberculosis treatment program must be carried out consistently. Holistic services do not only treat TB disease but also treat the patient’s mental health. There is comorbidity between TB and mental illness, therefore the treatment of TB patients should be integral to the treatment of depression and anxiety. This is in accordance with the WHO end TB strategy 2015–2035.25
Healthcare providers and professionals need to emphasize a patient-centered approach to TB treatment. On the other hand, National TB Programs (NTPs) need to implement a comprehensive patient-centered policy at the national level. Patient-centered is one of the efforts to strengthen PHC, where TB management is mostly carried out at this level.
Tuberculosis treatment programs need to include screening procedures for mental and emotional disorders. Screening can be used to identify patients who require further psychosocial assessment, support, and treatment so that patients are expected to have a better response to anti-TB treatment.32
In areas with limited mental health specialists, online mental health screening is a very useful tool to help doctors and other health professionals identify mental and emotional disorders. Doctors, then, can selectively treat people with severe mental and emotional disorders. PHC handled by non-specialist professionals need to be assisted with cloud-based screening instruments to strengthen the system and patient-centered approach. One of the interesting tools for a rapid assessment of mental health is the Patient Health Questionnaire-9 (PHQ-9). It has been validated for depression screening in PHC in high- and low-income countries.48
Several hospitals in Singapore have launched an online educational psychotherapy program using Cognitive Behavior Therapy.49 CBT can reduce adaptive coping behaviors and self-blame by increasing the ability to manage stress. This platform can be a peer tool for patients to support and strengthen each other during the COVID-19 pandemic.49
Limitations and Strength of This Study
Data is derived from convenience sampling, not randomized, so it needs to be considered in the interpretation of inference results. Because this research is limited to one district, it can only be generalized to the district. The research needs to be scaled up to the national level even if the pandemic had passed its peak. However, it can be used as an indication to pay more attention to the patient’s approach as a unique individual (patient-centered).
Screening in this study is not purposed for diagnosis. Management and treatment of the patient are then carried out by the doctor. Screening using this questionnaire can be inaccurate, therefore structured clinical interviews and functional neuroimaging can be used as gold standards.50–52
The cloud-based screening carried out in this study can help health workers in areas with limited mental health expertise, and expand the reach and coverage of mental health services for TB programs. This study succeeded in capturing the mental health phenomenon in tuberculosis patients at a rare moment when the peak of the pandemic wave occurred.
Conclusion
TB patients, at the peak period of the Covid-19 pandemic wave at the study site, experienced higher mental health disorders than non-TB patients. TB patients less than 20 years of age are more susceptible to moderate-severe mix anxiety and depressive syndrome than older patients. Mental health multiple burdens can occur in forms other than pandemic events and can have an impact on young TB patients. The patient-centered approach needs to be emphasized in holistic TB patient care. Patient management is not only limited to physical aspects but also mental, social, and spiritual. NTP has to implement patient-centered policies to address TB missing cases for achieving zero TB in 2035. The government needs to develop a model for strengthening and resilience of primary health care as well as national and local health systems.
Acknowledgments
The authors would like to thank LPDP (Indonesia Endowment Fund for Education), the Ministry of Economics as a research funder; the District Health Office of Purwakarta, along with all CHCs who have facilitated and collaborated in this research, and Screenout.id for data collection facilitation.
Funding
This study was funded by LPDP, Ministry of Economics. The funder had a limited role in the conduct of the study and did not interfere with the objectivity of the study.
Disclosure
All authors have no financial interests or conflicts of interest for this study/work.
References
1. World Health Organization. Global Tuberculosis Report 2021. Geneva: World Health Organization; 2021.
2. Arlinda D, Indah RM, Yulianto A, et al. Poor tuberculosis treatment outcomes associated with older age, previous treatment, HIV and drug resistance at seven hospitals in Indonesia. J Penelitian Dan Pengembangan Pelayanan Kesehatan. 2020;4(2):61–68. doi:10.22435/jpppk.v4i2.3698
3. Duko B, Gebeyehu A, Ayano G. Prevalence and correlates of depression and anxiety among patients with tuberculosis at Wolaita Sodo University Hospital and Sodo Health Center, Wolaita Sodo, South Ethiopia, cross-sectional study. BMC Psychiatry. 2015;15:214. doi:10.1186/s12888-015-0598-3
4. Husain MO, Dearman SP, Chaudhry IB, et al. The relationship between anxiety, depression and illness perception in tuberculosis patients in Pakistan. Clin Pract Epidemiol Ment Health. 2008;4:4. doi:10.1186/1745-0179-4-4
5. Katon W, Schulberg H. Epidemiology of depression in primary care. Gen Hosp Psychiatry. 1992;14:237–247. doi:10.1016/0163-8343(92)
6. Koyanagi A, Vancampfort D, Carvalho A, et al. Depression comorbid with tuberculosis and its impact on health status: a cross-sectional analysis of community-based data from 48 low- and middle-income countries. BMC Med. 2017;15(1):209. doi:10.1186/s12916-017-0975-5
7. Sweetland AC, Oquendo MA, Wickramaratne P, et al. Depression: a silent driver of the global tuberculosis epidemic. World Psychiatry. 2014;13:325–326. doi:10.1002/wps.20134
8. Sweetland AC, Kritski A, Oquendo MA, et al. Addressing the tuberculosis- depression syndemic to end the tuberculosis epidemic. Int J Tuberc Lung Dis. 2017;21:852–861. doi:10.5588/ijtld.16.0584
9. Ambaw F, Mayston R, Hanlon C, et al. Impact of untreated depression on tuberculosis treatment outcomes, disability, and quality of life in Ethiopia: a cohort study. WHO Bull. 2018;96:243–255.
10. Cassano P, Fava M. Depression and public health: an overview. J Psychosomatic Res. 2002;53:849–857. doi:10.1016/S0022-3999(02
11. Bystritsky A, Khalsa SS, Cameron ME, et al. Current Diagnosis and treatment of anxiety disorders. J Formul Manage. 2013;38:30–57.
12. Tee CA, Salido EO, Reyes PWC, et al. Psychological state and associated factors during the 2019 Coronavirus Disease (COVID-19) pandemic among Filipinos with rheumatoid arthritis or systemic lupus erythematosus. Rheumatol Res Rev. 2020;12:215–222.
13. Wells KB, Golding J, Burnam MA. Psychiatric disorder in a sample of the general population with and without chronic medical conditions. Am J Psychiatry. 1988;145:976–981.
14. Zhang MWB, Ho RCM, Cheung MWL, et al. Prevalence of depressive symptoms in patients with chronic obstructive pulmonary disease: a systematic review, meta-analysis and meta-regression. Gen Hosp Psychiatry. 2011;33(3):217–223. doi:10.1016/j.genhosppsych.2011.03.009
15. Lu Y, Mak -K-K, van Bever HPS, et al. Prevalence of anxiety and depressive symptoms in adolescent with asthma: a meta-analysis and meta-regression. Pediatr Allergy Immunol. 2012;23(8):707–715. doi:10.1111/pai.12000
16. Shen TC, Wang CY, Lin CL, et al. People with tuberculosis are associated with a subsequent risk of depression. Eur J Int Med. 2014;25:936–940. doi:10.1016/j.ejim.2014.10.006
17. Balaji AL, Abhishekh HA, Kumar NC, et al. Depression in patients with pulmonary tuberculosis in a tertiary care general hospital. Asian J Psychiatry. 2013;6:251–252. doi:10.1016/j.ajp.2012.12.017
18. Ige OM, Lasebikan VO. Prevalence of depression in tuberculosis patients in comparison with non-tuberculosis family contacts visiting the DOTS clinic in a Nigerian tertiary care hospital and its correlation with disease pattern. Ment Health Fam Med. 2011;8:235–241.
19. Xiong J, Lipsitz O, Nasri F, et al. Impact of COVID-19 pandemic on mental health in the general population: a systematic review. J Affect Disord. 2020;277:55–64. doi:10.1016/j.jad.2020.08.001
20. Wang C, Chudzicka-Czupala A, Tee ML, et al. A chain mediation model on COVID-19 symptoms and mental health outcomes in Americans, Asians and Europeans. Sci Rep. 2021;11:6481. doi:10.1038/s41598-021-85943-7
21. Wang C, Tee M, Roy AE, et al. The impact of COVID-19 pandemic on physical and mental health of Asians: a study of seven middle-income countries in Asia. PLoS One. 2021;16(2):e0246824. doi:10.1371/journal.pone.0246824
22. WHO. COVID-10 continues to disrupt essential health services in 90% of countries; 2021. Available from: https://www.who.int/news/item/23-04-2021-COVID-19-continues-to-disrupt-essential-health-services-in-90-of-countries.
23. Salari N, Hosseinian-Far A, Jalali R, et al. Prevalence of stress, anxiety, depression among the general population during the COVID-19 pandemic: a systematic review and meta-analysis. Global Health. 2020;16:57. doi:10.1186/s12992-020-00589-w
24. Di Gennaro F, Gualano G, Timelli L, et al. Increase in tuberculosis diagnostic delay during first wave of the COVID-19 pandemic: data from an Italian infectious disease referral hospital. Antibiotics. 2021;10(3):272. doi:10.3390/antibiotics10030272
25. World Health Organization. Implementing the End TB Strategy: The Essentials. Geneva: World Health Organization; 2015.
26. Grigoryan Z, Truzyan N, Musheghyan L, et al. A qualitative assessment of people-centeredness of inpatient tuberculosis treatment services in Armenia. J Tubercul Res. 2021;9:184–196. doi:10.4236/jtr.2021.93017
27. Agarwal N, Sarthi P. The necessity of psychological interventions to improve compliance with tuberculosis treatment and reduce psychological distress. J Fam Med Prim Care. 2020;9(8):4174–4180. doi:10.4103/jfmpc.jfmpc_1404_20
28. Dong X, Zhao L, Sun T, et al. Prevalence of depressive symptoms and associated factors among internal migrants with tuberculosis: a cross-sectional study in China. Am J Trop Med Hyg. 2020;102(1):31–35. doi:10.4269/ajtmh.19-0542
29. Sweetland AC, Jaramillo E, Wainberg ML, et al. Tuberculosis: an opportunity to integrate mental health services in primary care in low-resource settings. Lancet Psychiatry. 2018;5(12):952–954. doi:10.1016/S2215-0366(18)30347-X
30. Sunjaya DK, Herawati DMD, Siregar AY, et al. Depressive, anxiety, and burnout symptoms on health care personnel at a month after COVID-19 outbreak in Indonesia. BMC Public Health. 2021;21:227. doi:10.1186/s12889-021-10299-6
31. Sunjaya DK, Sumintono B, Gunawan E, et al. On line mental health survey for addressing psychosocial condition during the COVID-19 pandemic in Indonesia: instrument evaluation. Psychol Res Behav Manag. 2022;15:161–170. doi:10.2147/PRBM.S347386
32. Wang X-B, Li X-L, Zhang Q, et al. A survey of anxiety and depressive symptoms in pulmonary tuberculosis patients with and without tracheobronchial tuberculosis. Front Psy. 2018;9:308. doi:10.3389/fpsyt.2018.00308
33. Ambaw F, Mayston R, Hanlon C, et al. Depression among patients with tuberculosis: determinants, course and impact on pathways to care and treatment outcomes in a primary care setting in southern Ethiopia‐A study protocol. BMJ Open. 2015;5:e007653. doi:10.1136/bmjopen-2015-007653
34. Yilmaz A, Dedeli O. Assessment of anxiety, depression, loneliness and stigmatization in patients with tuberculosis. Acta Paul Enferm. 2016;29(5):549–557. doi:10.1590/1982-0194201600076
35. Theron G, Peter J, Zijenah L, et al. Psychological distress and its relationship with non-adherence to TB treatment: a multicentre study. BMC Infect Dis. 2015;15:253. doi:10.1186/s12879-015-0964-2
36. van den Heuvel L, Chishinga N, Kinyanda E, et al. Frequency and correlates of anxiety and mood disorders among TB- and HIV-infected Zambians. AIDS Care. 2013;25(12):1527–1535. doi:10.1080/09540121.2013.793263
37. Adem A, Tesfaye M, Adem M. The prevalence and pattern of depression in patients with tuberculosis on follow-up at Jimma University Specialized Hospital and Jimma Health Center. Med Sci. 2014;3:955–968. doi:10.5455/medscience.2013.02.8097
38. Yohannes K, Mokona H, Abebe L, et al. Prevalence of depressive symptoms and associated factors among patients with tuberculosis attending public health institution in Gede’o zone, South Ethiopia. BMC Public Health. 2020;20:1702. doi:10.1186/s12889-020-09794-z
39. Ige OM, Lasebikan VO. Prevalence of depression in tuberculosis patients in comparison with non-tuberculosis family contacts visiting the DOTS clinic in a Nigerian tertiary care hospital and its correlation with disease pattern. Ment Health Fam Med. 2011;8(4):235.
40. Snow KJ, Cruz AT, Seddon JA, et al. Adolescent tuberculosis. Lancet Child Adolesc Health. 2020;4(1):68–79. doi:10.1016/S2352-4642(19)30337-2
41. Patton GC, Viner R. Pubertal transitions in health. Lancet. 2007;369:1130–1139. doi:10.1016/S0140-6736(07)60366-3
42. Octavius GS, Silviani FR, Lesmandjaya A, et al. Impact of COVID-19 on adolescents’ mental health: a systematic review. Middle East Curr Psychiatry. 2020;27:72–80. doi:10.1186/s43045-020-00075-4
43. Cao W, Fang Z, Hou G, et al. The psychological impact of the COVID-19 epidemic on college students in China. Psychiatry Res. 2020;287:112934. doi:10.1016/j.psychres.2020.112934
44. Lara-Espinosa JV, Hernandez-Pando R. Psychiatric problems in pulmonary tuberculosis: depression and anxiety. J Tubercul Res. 2021;9:31–50. doi:10.4236/jtr.2021.91003
45. Chytas V, Costanza A, Piguet V, Cedraschi C, Bondolfi G. Demoralization and meaning in life in suicidal ideation: a role for patients suffering from chronic pain? Rev Med Suisse. 2019;15(656):1282–1285.
46. Ambrosetti J, Macheret L, Folliet A, et al. Impact of the COVID-19 pandemic on psychiatric admissions to a large Swiss emergency department: an observational study. Int J Environ Res Public Health. 2021;18(3):1174. doi:10.3390/ijerph18031174
47. Hao F, Tan W, Jiang L, et al. Do psychiatric experience more psychiatric symptoms during COVID-19 pandemic and lockdown? A case-control study with service and research implications for immunopsychiatry. Brain Behav Immun. 2020;87:100–106. doi:10.1016/j.bbi.2020.04.069
48. Costantini L, Pasquarella C, Odone A, et al. Screening for depression in primary care with Patient Health Questionnaire-9(PHQ-9): a systematic review. J Affect Disord. 2021;279:473–483. doi:10.1016/j.jad.2020.09.131
49. Ho CS, Chee CY, Ho RC. Mental health strategies to combat the psychological impact of coronavirus disease 2019 (COVID-19) beyond paranoia and panic. Ann Acad Med Singap. 2020;16(49):155–160.
50. Ho RC, Sharma VK, Tan BYQ, et al. Comparison of brain activation patterns during olfactory stimuli between recovered COVID-19 patients and healthy controls: a functional near-infrared spectroscopy (fNIRS) study. Brain Sci. 2021;11(8):968. doi:10.3390/brainsci11080968
51. Husain SF, Tang TB, Yu R, et al. Cortical hemodynamic response measured by functional near infrared spectroscopy during a verbal fluency task in patients with major depression and borderline personality disorder. EbioMedicine. 2020;51:102586. doi:10.1016/j.ebiom.2019.11.047
52. Ho CSH, Lim LJH, Lim AQ, et al. Diagnostic and predictive applications of functional near-infrared spectroscopy for major depressive disorder: a systematic review. Front Psychiatry. 2020;11:378. doi:10.3389/fpsyt.2020.00378
 © 2022 The Author(s). This work is published and licensed by Dove Medical Press Limited. The
full terms of this license are available at https://www.dovepress.com/terms.php
and incorporate the Creative Commons Attribution
- Non Commercial (unported, v3.0) License.
By accessing the work you hereby accept the Terms. Non-commercial uses of the work are permitted
without any further permission from Dove Medical Press Limited, provided the work is properly
attributed. For permission for commercial use of this work, please see paragraphs 4.2 and 5 of our Terms.
© 2022 The Author(s). This work is published and licensed by Dove Medical Press Limited. The
full terms of this license are available at https://www.dovepress.com/terms.php
and incorporate the Creative Commons Attribution
- Non Commercial (unported, v3.0) License.
By accessing the work you hereby accept the Terms. Non-commercial uses of the work are permitted
without any further permission from Dove Medical Press Limited, provided the work is properly
attributed. For permission for commercial use of this work, please see paragraphs 4.2 and 5 of our Terms.
