Back to Journals » Diabetes, Metabolic Syndrome and Obesity » Volume 15
The Importance of Patient and Family Engagement, the Needs for Self-Monitoring of Blood Glucose (SMBG) – Our Perspectives Learned Through a Story of SMBG Assistive Devices Made by a Husband of the Patient with Diabetes
Authors Kimura M , Toyoda M , Saito N, Takahashi M, Isozumi K, Kato E, Kawanami D , Fukagawa M
Received 1 March 2022
Accepted for publication 13 May 2022
Published 25 May 2022 Volume 2022:15 Pages 1627—1638
DOI https://doi.org/10.2147/DMSO.S363762
Checked for plagiarism Yes
Review by Single anonymous peer review
Peer reviewer comments 2
Editor who approved publication: Prof. Dr. Juei-Tang Cheng
Moritsugu Kimura,1 Masao Toyoda,1 Nobumichi Saito,1 Makiko Takahashi,1 Konomi Isozumi,1 Eri Kato,2 Daiji Kawanami,3 Masafumi Fukagawa1
1Division of Nephrology, Endocrinology and Metabolism, Department of Internal Medicine, Tokai University School of Medicine, Isehara, Kanagawa, Japan; 2Seichi Clinic, Isehara, Kanagawa, Japan; 3Department of Endocrinology and Diabetes Mellitus, Fukuoka University School of Medicine, Fukuoka, Japan
Correspondence: Moritsugu Kimura, Division of Nephrology, Endocrinology and Metabolism, Department of Internal Medicine, Tokai University School of Medicine, Isehara, Kanagawa, Japan, Tel +81-463-93-1121 (ext. 2490), Fax +81-463-91-3350, Email [email protected]
Abstract: Despite some negative reports regarding the need for the self-monitoring of blood glucose (SMBG), including the issue of cost-effectiveness, there are still many users, and in diabetes treatment, which is largely dependent on the patient’s self-care, SMBG remains an important tool in establishing such self-care habits, with several reports supporting this notion. In addition, devices are needed to assist in SMBG for patients with diabetes who have difficulty performing SMBG, such as the elderly or those with visual impairment. In current diabetes care, it is reported that patient-centered care that respects the preferences, needs, and values of individual patients and personalized care that consider the characteristics and comorbidities of each patient are important. Through a case study of a patient with diabetes who had difficulty performing SMBG due to visual impairment, we learned of the needs of SMBG and its assistive devices and the importance of patient and family engagement with emphasis on patient-centered and personalized care. We herein report what we learned through this case in the form of perspectives. Through this report, we hope that medical professionals involved in diabetes care will learn of the importance and needs of these issues and apply them to their actual clinical practice.
Keywords: patient-centered care, personalized care, patient and family engagement, self-monitoring of blood glucose, SMBG assistive devices, diabetes
Graphical Abstract:
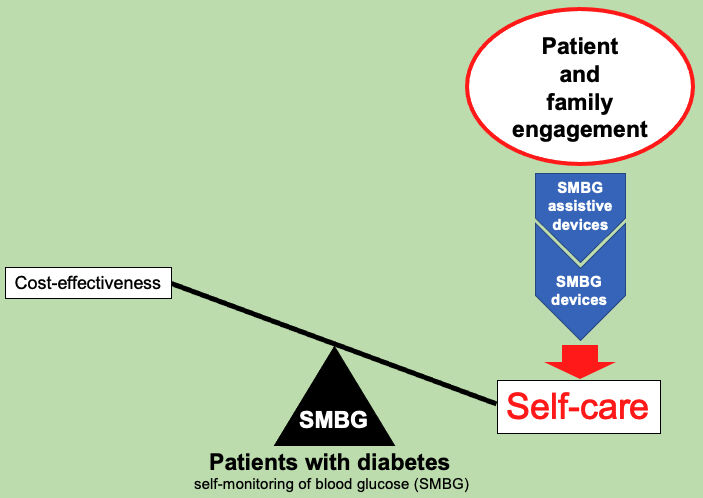
Introduction
Currently in Japan, medical insurance covers the use of self-monitoring blood glucose (SMBG) only for patients on insulin and Glucagon like peptide-1 receptor agonists and pregnant women with abnormal glucose metabolism.1 Even with the widespread use of new self-monitoring devices, such as intermittently scanned continuous glucose monitoring (isCGM), there are still many SMBG users. The American Diabetes Association (ADA) guidelines recognize even for patients using less frequent insulin injections, SMBG may help guide treatment decisions as part of a broad educational program.2 And it has advantages in not only checking hypoglycemia and hyperglycemia but also assessing physical activity and diet, motivating self-management, and building a close relationship with the attending physician.3 On the other hand, the elderly, visually impaired, and hypersensitive patients may have difficulty performing SMBG due to pain at the time of puncture and the complexity of the measurement operation, and several assistive devices are sometimes used as accessories in Japan (Figure 1A–C). However, there are cases where SMBG cannot be performed with existing SMBG assistive devices, so adequate self-care has not yet been achieved.
As medical care becomes more sophisticated and complex, the success or failure of treatment for chronic diseases, such as diabetes, largely depends on the patient’s self-care, and patients and their families are important members of the medical team. It is therefore important to foster patient and family engagement, wherein the patient and their family members participate in various aspects of medical care, performing medical care together with the patient’s doctors.4 In addition, the ADA and European Association for the Study of Diabetes (EASD) published a basic policy concerning the treatment of type 2 diabetes (T2D) in 2012. It advocates a patient-centered approach, which
respects the preferences, needs, and values of the individual patient, provides care that is responsive to those preferences and needs, and ensures that patient values guide all clinical decisions.5,6
In addition, the importance of personalized care that takes into account the characteristics and comorbidities of each patient are important in the field of diabetes has been recently reported, as the use of personalized medicine in patients with T2D should improve medication adherence, patient satisfaction, and quality of life, reduce diabetes distress, and improve physical health.7
In this study, we report our perspectives on the importance of patient and family engagement, the needs for SMBG the need for SMBG and its assistive devices engagement in diabetes care, using a story as a resource.
Case Presentation
The patient was a 47-year-old woman with a chief complaint of vision loss. Regarding her family history, her mother had T2D. The patient was a homemaker. When she had been pregnant with her first son at 25 years old and her second son at 27 years old, high blood glucose levels had been noted, but diabetes had not been diagnosed, and she never underwent a physical examination or hospital visit. At 47 years old, she became aware of decreased visual acuity in her left eye in May X. In June X, she became aware of decreased visual acuity in her right eye, and in July X, her decreased visual acuity worsened, so her husband recommended that she visit the Department of Ophthalmology of Tokai University School of Medicine.
On visiting the ophthalmology department, she was diagnosed with bilateral proliferative diabetic retinopathy and tractional retinal detachment, and she was referred to a diabetologist at the same university on the same day. She had never been weighed on a daily basis, so her weight fluctuations were unknown, and she had never been on a diet. She was not aware of any symptoms, such as thirst, polydipsia, or polyuria.
At the time of consultation, her height was 153 cm, her weight was 66 kg, her body mass index (BMI) was 28 kg/m2. Her arterial blood pressure was 190/103mmHg, pulse rate was 83 bpm (regular), respiration rate was 16/min, body temperature was 36.0 °C, and consciousness was lucid. A decreased Achilles tendon reflex was observed.
Laboratory tests at consultation showed a fasting blood glucose level of 242 mg/dl and HbA1c of 10.3%, indicating poor blood glucose control. Urinary ketone bodies were positive, but there was no metabolic acidosis, and anti-GAD (glutamic acid decarboxylase) antibodies were negative. As a result, the patient was diagnosed with hypertension, and diabetic ketosis due to T2D.
To manage her diabetic ketosis, SMBG guidance and insulin therapy were started. For her hypertension, salt restriction to 6 g/day and the antihypertensive drug olmesartan medoxomil were started. Regarding the eye disease, it was decided that she would undergo surgery once her blood glucose levels stabilized. Due to the patient’s strong request that she could not be hospitalized because of the need to take care of her cat and the considerable mental and physical burden she would sustain, we decided to treat her as an outpatient instead of hospitalizing her.
Since it was difficult to learn the SMBG technique due to poor vision, we prepared ready-made SMBG assistive devices made of rubber bands and plastic (Figure 1A–C). Unfortunately, the ready-made SMBG assistive devices were complicated to operate and SMBG could not be performed, making it difficult to continue insulin therapy in the outpatient hospital. We made the recommendation again that she be hospitalized, but she still refused. For diabetic ketosis, SMBG instruction and insulin therapy were started, but the patient had difficulty learning the SMBG with general technique instruction due to poor vision and other factors, and SMBG could not be performed well, and her blood glucose level remained unstable. The lack of results increased the anxiety and frustration of the patient and her family day by day. However, the medical staff tried to create an atmosphere where the patient and family could participate in the treatment as much as possible while giving priority to the patient’s requests. The staff continued to treat the patients at outpatient visits every one to two weeks, but at the outpatient clinic on week X+4, many readings of blood glucose levels were noted in the SMBG notes. This turned out to not be a false reading but instead the result of the patient’s husband, who worked in manufacturing, creating a less complicated SMBG aid that the patient could operate alone. Thereafter, whenever the patient’s husband visited the outpatient hospital with the patient, the husband brought the SMBG assistive device with him. Each day, the SMBG assistive devices became more hygienic, safer, and more adaptable to various finger sizes. The first SMBG assistive device was made of wood by the manufacturer, the patient’s husband (Figure 2A). The second SMBG assistive device was made of ABS (acrylonitrile-butadiene-styrene) resin with an antibacterial effect by the patient’s husband (Figure 2B). The third SMBG assistive device was made of ABS resin with an antibacterial effect for safety by the patient’s husband (Figure 2C). After the third SMBG assistive device, it’s device made of ABS resin with an antibacterial effect continued to improve, and various types and sizes of SMBG assistive devices were made (Figure 2D).
As a result of being able to measure blood glucose levels smoothly with the SMBG assistive device, the patient herself became more positive about the treatment and paid more attention to her daily life, including diet, and her blood glucose levels stabilized. Laser therapy and vitrectomy were performed for bilateral proliferative diabetic retinopathy and tractional retinal detachment, and 10 months after the visit, the visual acuity of the right eye recovered from 0.04 to 0.06 and that of the left eye from 0.01 to 0.4. In addition, the SMBG assistive devices created by her husband brought her, her family, and medical professionals closer together, allowing patient to avoid being subjected to excessive physical and bodily stress. The patient, family, and medical professionals are now able to practice medicine in a good relationship. With strict dietary control and increased daily biological activity in attention to her eyes, insulin was not increased beyond insulin aspart (2-2-2 units), insulin degludec (4-0-0 units), and good glycemic control could be continued.
After one year, the need for insulin was eliminated and insulin was discontinued. We recommended that the patient discontinue SMBG, as her insurance would not continue to cover the monitoring due her cessation of insulin. However, as the patient and her husband desired to do so, she continued to perform SMBG at her own expense. Since withdrawing from insulin, she has maintained her HbA1c level in the 6% range for several years with no oral medication, only diet and exercise therapy. She has said that she was able to continue self-management of her diabetes by checking her blood glucose levels via SMBG, which she measures occasionally. Her husband and the medical staff continued to develop SMBG assistive devices for patients who were having trouble performing SMBG on their own. As a result, a medical device company producing SMBG assist devices asked for our help in developing a new SMBG assist device, and after testing more than 200 prototypes (Figure 3), a new type of SMBG assistive device is now available for patients who wish to have it as an accessory to SMBG (Figure 4).
Problems with SMBG
Some reports have described different views concerning the need for SMBG, and support for SMBG is mixed.8 Randomized trials of SMBG in non-insulin-treated T2D say that it does not affect glycemic control, that the effects of SMBG are not long-lasting, and that the cost-effectiveness of reducing diabetes-related complications may be low.9–11 It has also been reported that the Society of General Internal Medicine (SGIM) does not recommend SMBG in such patients.12
Furthermore, some reports suggest that clinicians’ attitudes toward SMBG play an important role in the frequency of monitoring and that the option for discontinuation should be discussed with the patient.12,14 Among the poor, SMBG adherence reportedly does not correlate with achieving glycemic targets, imposing a significant cost burden on the healthcare system.15 The main reasons for not performing SMBG frequently include a lack of time, not remembering, and self-consciousness, underscoring the need to increase support for SMBG implementation and successful behavior change in patients.16,17 Unlike assisted monitoring of blood glucose (AMBG), which is performed by healthcare professionals and other caregivers for patients with diabetes, SMBG is not a self-monitoring measure per se but is often performed by the patient.18 However, as patients age, their family members or home care givers may need to support them, and similar measures are needed to prevent infections, which is a problem with AMBG. Although the current general principle of SMBG involves collecting blood by inserting a needle into the finger, applying it to a reagent strip, and reading it with an automated device, new technologies are now being evaluated to achieve painless and accurate next-generation glucose monitoring for diabetes mellitus and to meaningfully shape the glucose self-monitoring device market. In addition, a number of organizations are making attempts to significantly improve the health status of people suffering from diabetes.19
The quality and usability of SMBG devices are continuously improving. However, due to the complicated operations required, SMBG may not be able to be performed by the elderly, visually impaired, or hypersensitive patients, due to the pain during puncture and difficulty performing measurements.
About SMBG Assistive Devices
SMBG is essential for the self-management of diabetes, and the reliability of SMBG measurements depends largely on how the measurer prepares and performs the measurement.20,21 Innovative technologies have led to the emergence of high-quality SMBG systems with a variety of user-friendly features, such as shorter measurement times, smaller blood draws, and painless lancing devices, and have been reported to reduce the risk of mishandling and improve usability by changing the SMBG operating procedure.22–26
However, we have seen many cases in clinical practice where SMBG is difficult to perform, and although some manufacturers have developed their own assistive devices, we have not seen many instances where these devices are effectively used.26 In addition, to our knowledge, there are few articles related to SMBG assistive devices, and most of the few that exist are from the same institution in Japan concerning elderly patients with diabetes. The authors developed an SMBG device suitable for the elderly and reported the need for SMBG assistive devices in an aging society and the need for educational methods to support the implementation of SMBG in elderly diabetic patients.27–31 Their report is believed to be the first describing the difficulties of SMBG implementation based on patient observation.31 However, their assistive device is precise but complex, mainly targeting the elderly, and is unlikely to still be used by many patients.
Need for SMBG
In Japan, the use of SMBG is still mostly managed by medical institutions specializing in diabetes care, but overseas, SMBG is recommended for primary care physicians due to its importance in patient self-management. It has been recognized as an essential prerequisite for the successful management and treatment of diabetes in various guidelines.1,7 Furthermore, with the widespread use of new self-monitoring instruments, such as isCGM, many type 1 and 2 diabetic patients and their care teams are likely to rely on isCGM as an important tool in diabetes management.32 However, the need for continued SMBG testing reportedly remains important for all isCGM users.33 Regarding the effectiveness of SMBG, the ADA guidelines have reported its usefulness in improving diabetes self-management and pharmacotherapy. In addition to checking for hypoglycemia and hyperglycemia, SMBG has been reported to be effective in assessing physical activity and diet, motivating self-management, building a close relationship with the patient’s physician, being effective in non-insulin users, influencing the number of times SMBG is performed on glycemic control, serving as an educational and therapeutic tool for patients, and potentially reducing annual medical costs.1–3,34–37
Effective Use of SMBG
Effective use of SMBG can lead to outcomes that promote self-management and empowerment, form a reasonable basis for a partnership between the patient and the healthcare team, and may even enable patients to achieve good glycemic control and reduce the risk of diabetes-related complications.38–44 In order to use SMBG effectively, it is important to identify how and why SMBG is performed in practice.42,45,46 A personalized understanding is reportedly needed to advise diabetic patients on how SMBG can be optimized, as patients with diabetes who are receiving insulin therapy do not necessarily self-monitor with the explicit goal of improving their long-term glycemic control.47 Furthermore, patients with diabetes need to be able to perform smooth blood glucose monitoring and have the ability and confidence to interpret the results of self-monitored blood glucose levels; however, patients often lack formal SMBG training.48,49 For these practices to support patients’ self-monitoring, it is necessary to develop a patient and family engagement approach to healthcare that includes patients and their families and is conducted in good relationship with healthcare providers.
Patient and Family Engagement with Emphasis on Patient-Centered and Personalized Care
In the 21st century, medical care has become more sophisticated and complex, and the number of patients with multiple comorbidities has increased. With increasing specialization, the continuity of treatment and care is fragmented, and the patient is the only one involved in the entire treatment process. When there are multiple treatment options, it is difficult for physicians to decide which one is best for the patient in the midst of diversifying needs. The success or failure of a treatment for a chronic disease, such as diabetes, depends largely on the patient’s self-care. In this context, the idea that “patients are important members of the medical team and are responsible for creating medical care together” and that involving patients and their families in various medical processes is essential for 21st century medicine has evolved.4
There are multiple definitions of patient-centered medicine.50–56 Among these, Carman et al’s definition,“patient-centered care is the active collaboration of patients, families, agents, and healthcare providers at various levels of healthcare, ie direct care, hospital system development and governance, and health policy, to improve the quality and safety of healthcare,” is often cited.4,50
The importance of patient-centered care is highlighted in the basic policy for the treatment of T2D published by the ADA and EASD in 2012. It advocates a patient-centered approach, which
respects the preferences, needs, and values of the individual patient, provides care that is responsive to those preferences and needs, and ensures that patient values guide all clinical decisions.5,6
There is also a recent report that the use of personalized approach in the management of T2D patients can reduce the costs and failures associated with algorithmic “one-size-fits-all” approaches, predict disease progression, improve response to diabetes medications, reduce the development of diabetes-related complications, and ultimately improve medication adherence, patient satisfaction, quality of life, diabetes distress, and physical health by using personalized approach for T2D patients.7 These cares should be the basic principle of healthcare for patients with all chronic diseases. In addition, regarding patient decision-making, patient involvement in medical decision making is reportedly a basic principle of evidence-based medicine, and in clinical practice, it is necessary to understand the extent to which patients wish to be involved and to consider treatment options.57,58 In the shared decision-making approach, it is useful for clinicians and patients to discuss the situation in order to reach a consensus regarding the treatment plan.59,60
Patient engagement is the active collaboration of patients, their families, their representatives, and healthcare providers at various levels of healthcare (ie direct medical care, hospital system development and governance, and healthcare policy) to improve the quality and safety of healthcare. Patient engagement is expected to not only improve the patient experience and satisfaction, treatment adherence, and treatment outcomes but also to strengthen trust between patients and healthcare providers, improve job satisfaction for healthcare providers, and reduce burnout and turnover among healthcare providers.54,61–66 If patients proactively participate in their own treatment, unnecessary hospitalizations and emergency room visits will be reduced, the length of hospital stay will be shortened, and as a result, healthcare costs will be reduced, which is seen as an important issue in healthcare policy.4 In addition, as the population ages and the number of patients with chronic diseases increases, the role of the family will become even more important, so the term “ patient and family engagement” is often used instead of “patient engagement”.67
Discussion
The case we presented here is a rare example of a patient who was successfully treated for severe diabetes mellitus and diabetic complications without unnecessary financial burden of hospitalization due to enhanced self-care by SMBG through the practice of patient-centered or personalized care and patient and family engagement.
As mentioned in “Problems with SMBG” above, the need to consider cost-effectiveness and patients’ intentions has led to several issues regarding the duration of SMBG use, the involvement of healthcare providers, and measurement methods.16–23 One of them states that,
A survey of patients showed that many of those who responded that SMBG improves their QOL would discontinue monitoring if their physician told them it could be discontinued. Considering the costs associated with SMBG, primary care physicians should reevaluate the benefits of SMBG for patients and discontinue it if possible It should be discontinued if possible.22
However, SMBG has long been proven necessary for diabetes self-management.1,2,8–14 Furthermore, considering the importance of patient and family engagement, a reassessment of the patient’s self-care status and the benefits of SMBG should not be determined solely by the primary care physician but should instead involve the patient, their family, and all participating healthcare providers.
In the case presented here, although physicians urged the patient to discontinue SMBG, the patient and her family continued to engage in SMBG at their own expense, not covered by medical insurance, of their own volition. The patient is now doing well with self-management thanks to the effects of SMBG. The amount of out-of-pocket expenses for insulin, SMBG equipment varies depending on the medical situation in each country, so it is difficult to strictly compare and evaluate the cost-effectiveness between Japan and other countries. Of course, it is important to be aware of cost-effectiveness in medical treatment. However, whether or not the cost of SMBG is commensurate with its effectiveness will be judged based on how patients feel about the cost-effectiveness and whether or not they are able to maintain good control of their blood glucose levels, ie the evaluation will be left up to individual patients, their personal feelings, and their management status.
In addition, considering that self-care is greatly influenced by the patient’s preference, need, and values, it is extremely important to consider patients (and families) with emphasis on patient-centered and personalized care. Such patient and family engagement with emphasis on patient-centered and personalized care is important for inducing behavioral changes in patients and generating the following effects of SMBG on diabetes management: 1) accurate assessments of the physical activity and diet, 2) increased motivation for self-management, 3) establishment of a close relationship with the attending physician, 4) improved efficacy in non-insulin users, 5) increased impact of the number of SMBG sessions on glycemic control, 6) establishment of a role as an educational and therapeutic tool for patients, and 7) increased potential to reduce annual medical costs.4,8,10–13 The present reported case is a good example of these roles of SMBG in action. Heeding the patient’s request that she could not be hospitalized because she needed to take care of her cat, the medical staff prioritized the patient’s wishes and tried to create an atmosphere where the patient and her family could participate in the treatment as much as possible. As a result, the patient’s family became involved in her medical care by crafting SMBG assistive devices, and the patient was able to perform SMBG by herself. Regarding point 3, the SMBG assistive devices made by her husband brought the patient, her family, and the medical staff closer together, and regarding points 5 and 6, frequent blood glucose monitoring showed that SMBG is an important tool for adjusting the number of insulin units. Regarding point 4, the fact that the patient was able to be weaned off insulin and maintained good glycemic control without medication for several years highlights the effectiveness of SMBG in insulin non-users, and regarding point 7, although the patient had to bear the financial burden of SMBG at her own expense, this medical cost was less than that of insulin use and thus a worthwhile investment.
We and the patient’s husband continued to work together to create SMBG assistive devices for patients who were having trouble with SMBG, and as a result, these aids have been distributed as accessories for SMBG (Figure 4). While the quality and ease of use of SMBG equipment has improved over the years, the elderly, visually impaired, and hypersensitive patients may still be unable to perform SMBG due to pain at the time of puncture or difficulty in performing measurements and manipulation, so SMBG assistive devices are important tools for building a stable self-care system with emphasis on patient-centered and personalized care. To utilize this important tool for self-care, it is necessary for medical professionals to recognize that SMBG is an important tool to support self-management by creating behavioral changes in patients through patient and family engagement with emphasis on patient-centered and personalized care, taking into consideration patients’ preferences, needs, and values. Patients must be made aware that SMBG is an important tool to support self-management. It is also an important point that empirical studies using isCGM and multiple subjects and followed over time are needed to show that SMBG and SMBG assistive devices are indeed truly useful for many patients with diabetes. The SMBG assistive device developed in this study, while taking hygiene issues into consideration, has begun to be used effectively for not only guiding needle puncture but also helping those who are unable to squeeze out enough blood from the puncture site. However, there has been no specific evaluation of the effectiveness of this aid and no verification of its issues. The patient’s husband is still working on creating a better SMBG assistive device, and we maintain hope that this device will be re-evaluated in the future, with even better SMBG assistive devices to be developed to meet the needs of patients.
Conclusion
As medical care becomes more sophisticated and complex, the success or failure of treatment in diabetes largely depends on the patient’s self-care. In order to make SMBG, which is an important tool for maintaining self-care, effective in diabetes treatment, it is important to foster patient and family engagement with emphasis on patient-centered and personalized care, ie taking into consideration patients’ preferences, needs, values, characteristics, and comorbidities. In addition, SMBG assistive devices are important tools for aiding the elderly, visually impaired, and hypersensitive patients in establishing a stable self-care system.
We hope that, based on these findings, many medical professionals involved in diabetes care will be reminded of these needs and importance and apply our observations to actual clinical practice.
Ethical Approval
This case report has been prepared in accordance with the ethical principles of the Declaration of Helsinki and conforms to the ICMJE guidelines for appropriate anonymization.
Consent
We have obtained written consent from the patient to submit this manuscript to an academic journal using the Patient Consent Form (provided by the Taylor & Francis Group, of which Dove Medical Press is a member). Our institution does not require Institutional Review Board approval for publication of a case report.
Acknowledgments
We would like to thank Yoritomo Tamura, the patient’s husband, who played a central role in the design of the assistive device, and Roche DC Japan K.K. for their cooperation in designing the device and increasing its production, and Hiromi Tsuzukibashi, Masaki Hoshino for their sympathy with the need to create SMBG assistive devices.
Author Contributions
All authors made a significant contribution to the work reported, whether that is in the conception, study design, execution, acquisition of data, analysis and interpretation, or in all these areas; took part in drafting, revising or critically reviewing the article; gave final approval of the version to be published; have agreed on the journal to which the article has been submitted; and agree to be accountable for all aspects of the work.
Disclosure
Masafumi Fukagawa reports grants and/or personal fees from Kyowa Kirin and Astra Zeneca, outside the submitted work. The authors declare no other conflicts of interest in this work.
References
1. Leminen A, Tykkyläinen M, Laatikainen T. Self-monitoring induced savings on type 2 diabetes patients’travel and healthcare costs. Int J Med Inform. 2018;115:120–127. doi:10.1016/j.ijmedinf.2018.04.012
2. Chamberlain JJ, Doyle-Delgado K, Peterson L, Skolnik N. Diabetes technology: review of the 2019 American Diabetes Association Standards of Medical Care in diabetes. Ann Intern Med. 2019;171(6):415–420. doi:10.7326/M19-1638
3. Takeda A. Diabetes: advances in diagnosis and treatment, use of blood glucose self-monitoring. J Jpn Soc Int Med. 2009;98(4):761–767. in Japanese. doi:10.2169/naika.98.761
4. Komatsu Y. Patient engagement will change the way medicine is practiced -A paradigm shift in 21st century medicine-. J Res Soc Econ Life. 2019;59(2):56–80. in Japanese.
5. Inzucchi SE, Bergenstal RM, Buse JB, et al. Management of hyperglycemia in Type 2 diabetes: a patient-centered approach: position statement of the American Diabetes Association (ADA) and the European Association for the Study of Diabetes (EASD). Diabetes Care. 2012;35(6):1364–1379. doi:10.2337/dc12-0413
6. Institute of Medicine (US) Committee on Quality of Health Care in America. Crossing the Quality Chasm: A New Health System for the 21st Century. Washington (DC): National Academies Press (US); 2001. doi:10.17226/10027
7. Williams DM, Jones H, Stephens JW. Personalized Type 2 diabetes management: an update on recent advances and recommendations. Diabetes Metab Syndr Obes. 2022;15:281–295. doi:10.2147/DMSO.S331654
8. Havele SA, Pfoh ER, Yan C, Misra-Hebert AD, Le P, Rothberg MB. Physicians’ views of self-monitoring of blood glucose in patients with type 2 diabetes not on insulin. Ann Fam Med. 2018;16(4):349–352. doi:10.1370/afm.2244
9. Young LA, Buse JB, Weaver MA, et al. Glucose self-monitoring in non-insulin-treated patients with type 2 diabetes in primary care settings: a randomized trial. JAMA Internal Med. 2017;177(7):920–929. doi:10.1001/jamainternmed.2017.1233
10. Malanda UL, Welschen LMC, Riphagen II, Dekker JM, Nijpels G, Bot SDM. Self-monitoring of blood glucose in patients with type 2 diabetes mellitus who are not using insulin. Cochrane Database Syst Rev. 2012;1:CD005060. doi:10.1002/14651858.CD005060.pub3
11. Cameron C, Coyle D, Ur E, Klarenbach S. Cost-effectiveness of self-monitoring of blood glucose in patients with type 2 diabetes mellitus managed without insulin. CMAJ. 2010;182(1):28–34. doi:10.1503/cmaj.090765
12. SGIM. Daily home finger glucose testing | Choosing Wisely. Available from: https://www.choosingwisely.org/clinician-lists/society-general-internal-medicine-daily-home-finger-glucose-testing-type-2-diabetes-mellitus/.
13. Polonsky WH, Fisher L, Hessler D, Edelman SV. A survey of blood glucose monitoring in patients with type 2 diabetes: are recommendations from health care professionals being followed? Curr Med Res Opin. 2011;27(suppl 3):31–37. doi:10.1185/03007995.2011.599838
14. Pfoh ER, Linfielld D, Speaker SL, et al. Patient perspectives on self-monitoring of blood glucose when not using insulin: a cross-sectional survey. J Gen Intern Med. 2021. doi:10.1007/s11606-021-07047-2
15. Yi WM, Jones EM, Hansen BK, Vora J. The impact of self-monitoring blood glucose adherence on glycemic goal attainment in an indigent population, with pharmacy assistance. P T. 2019;44(9):554–559.
16. Mostrom P, Ahlen E, Imberg H, Hansson PO, Lind M. Adherence of self-monitoring of blood glucose in persons with type 1 diabetes in Sweden. BMJ Open Diabetes Res Care. 2017;5(1):e000342. doi:10.1136/bmjdrc-2016-000342
17. Du Y, Dennis B, Rhodes SL, et al. Technology-assisted self-monitoring of lifestyle behaviors and health indicators in diabetes: qualitative study. JMIR Diabetes. 2020;5(3):e21183. doi:10.2196/21183
18. Klonoff DC, Perz JF. Assisted monitoring of blood glucose: special safety needs for a new paradigm in testing glucose. J Diabetes Sci Technol. 2010;4(5):1027–1031. doi:10.1177/193229681000400501
19. Markey report. Diabetes self-monitoring devices in low- and middle-income countries. Available from: https://www.finddx.org/wp-content/uploads/2021/10/Market-Report_Self-monitoring-Devices-in-LMICs.pdf.
20. Skeie S, Thue G, Nerhus K, Sandberg S. Instruments for self-monitoring of blood glucose: comparisons of testing quality achieved by patients and a technician. Clin Chem. 2002;48(7):994–1003. doi:10.1093/clinchem/48.7.994
21. Muller U, Hammerlein A, Casper A, Schulz M. Evaluation der Durchführung von Glukoseselbstkontrollen in Apotheken (EDGAr). Diabetes Stoffwechsel Herz. 2006;15(4):9–17.
22. Fruhstorfer H, Schmelzeisen-Redeker G, Weiss T. Capillary blood sampling: relation between lancet diameter, lancing pain and blood volume. Eur J Pain. 1999;3(3):283–286. doi:10.1053/eujp.1999.0132
23. Fruhstorfer H, Schmelzeisen-Redeker G, Weiss T. Capillary blood volume and pain intensity depend on lancet penetration. Diabetes Care. 2000;23(4):562–563. doi:10.2337/diacare.23.4.562
24. Hones J, Müller P, Surridge N. The technology behind glucose meters: test strips. Diabetes Technol Ther. 2008;10:10–26. doi:10.1089/dia.2008.0005
25. Westhoff A, Jendricke N, Haug C, Freckmann G. Schmerzempfinden an Finger und Handballen bei Verwendung verschiedener Blutzuckermesssysteme. Diabetologie Stoffwechsel. 2010;5:120. doi:10.1055/s-0030-1253848
26. Freckmann G, Schmid C, Ruhland K, Baumstark A, Haug C. Integrated self-monitoring of blood glucose system: handling step analysis. J Diabetes Sci Technol. 2012;6(4):938–946. doi:10.1177/193229681200600427
27. Oe M, Nagai S, Ikeda M, et al. Difficulties of the introduction of self-monitoring of blood glucose in elderly diabetic patients. JNSE. 2015;2(3):164–173.
28. Arai R, Murayama R, Oe M, et al. Blood collection assistance device for self-monitoring blood glucose in elderly patients with diabetes. JNSE. 2016;3(2):86–92.
29. Abe-Doi M, Oe M, Murayama R, et al. Development of an automatic puncturing and sampling system for a self-monitoring blood glucose device. Diabetes Technol Ther. 2017;19(11):651–659. doi:10.1089/dia.2017.0163
30. Abe-Doi M, Oe M, Murayama R, Zushi Y, Tanabe H, Sanada H. Impact of squeezing condition to obtain sufficient blood volume for self-monitoring of blood glucose using an automatic puncturing and sampling system. J Diabetes Sci Technol. 2018;12(5):1041–1044. doi:10.1177/1932296818771108
31. Oe M, Koike N, Tobe H, et al. Difficulties of self-monitoring blood glucose in the aged with diabetes: an analysis based on observations of self-monitoring blood glucose procedures. JNSE. 2020;7:141–148.
32. Carlson AL, Mullen DM, Bergenstal RM. Clinical use of continuous glucose monitoring in adults with Type 2 diabetes. Diabetes Technol Ther. 2017;19(S2):4–11. doi:10.1089/dia.2017.0024
33. Reddy M, Oliver N. Self-monitoring of blood glucose requirements with the use of intermittently scanned continuous glucose monitoring: a follow-up analysis using real-life data. Diabetes Technol Ther. 2021;23(5):392–396. doi:10.1089/dia.2020.0477
34. Sia HK, Kor CT, Tu ST, Liao PY, Wang JY. Self-monitoring of blood glucose in association with glycemic control in newly diagnosed non-insulin-treated diabetes patients: a retrospective cohort study. Sci Rep. 2021;11(1):1176. doi:10.1038/s41598-021-81024-x
35. Welschen LMC, Bloemendal E, Nijpels G, et al. Self-monitoring of blood glucose in patients with type 2 diabetes who are not using insulin: a systematic review. Diabetes Care. 2005;28(6):1510–1517. doi:10.2337/diacare.28.6.1510
36. Ziegler R, Heidtmann B, Hilgard D, et al. Frequency of SMBG correlates with HbA1c and acute complications in children and adolescents with type 1 diabetes. Pediatr Diabetes. 2011;12(1):11–17. doi:10.1111/j.1399-5448.2010.00650.x
37. Gracia TR, Lobo NGT, Duran A, Hervada R, Pascual ALC. Structured SMBG in early management of T2DM: contributions from the St Carlos study. World J Diabetes. 2014;5(4):471–481. doi:10.4239/wjd.v5.i4.471
38. International Diabetes Federation. Guideline on self-monitoring of blood glucose in non-insulin treated type 2 diabetes. Available from: http://www.idf.org/webdata/docs/SMBG_EN2.pdf.
39. Ryden L, Rydén L, Grant PJ, et al. ESC Guidelines on dia- betes, pre-diabetes, and cardiovascular diseases developed in collaboration with the EASD: the Task Force on diabetes, pre- diabetes, and cardiovascular diseases of the European Society of Cardiology (ESC) and developed in collaboration with the European Association for the Study of Diabetes (EASD). Eur Heart J. 2013;34(39):3035–3087. doi:10.1093/eurheartj/eht108
40. Investigators OT, Gerstein H, Yusuf S, Riddle MC, Ryden L, Bosch J. Rationale, design, and base- line characteristics for a large international trial of cardio- vascular disease prevention in people with dysglycemia: the ORIGIN trial (Outcome Reduction with an Initial Glargine INtervention). Am Heart J. 2008;155(1):
41. Nathan DM, Genuth S, Lachin J, et al; Diabetes Control and Complications Trial Research Group. The effect of intensive treatment of diabetes on the develop- ment and progression of long-term complications in insulin- dependent diabetes mellitus. N Engl J Med. 1993;329:977–986. doi:10.1056/NEJM199309303291401
42. Writing Team for the Diabetes Control and Complications Trial/ Epidemiology of Diabetes Interventions and Complications Research Group. Effect of intensive therapy on the micro- vascular complications of type 1 diabetes mellitus. JAMA. 2002;287(19):2563–2569. doi:10.1001/jama.287.19.2563
43. Schnell O, Amann-Zalan I, Jelsovsky Z, et al. Changes in A1C levels are significantly associated with changes in levels of the cardiovascular risk biomarker hs-CRP: results from SteP study. Diabetes Care. 2013;36(7):2084–2089. doi:10.2337/dc12-1711
44. Duckworth W, Abraira C, Moritz T. Glucose control and vascular complications in veterans with type 2 diabetes. N Engl J Med. 2009;360:129–139. doi:10.1016/j.jvs.2009.02.026
45. Klonoff DC, Blonde L, Cembrowski G, et al. Consensus report: the current role of self-monitoring of blood glucose in non-insulin-treated type 2 diabetes. J Diabetes Sci Technol. 2011;5(6):1529–1548. doi:10.1177/193229681100500630
46. Schnell O, Alawi H, Battelino T, et al. The role of self-monitoring of blood glucose in glucagon-like peptide-1-based treatment approaches: a European expert recommendation. J Diabetes Sci Technol. 2012;6(3):665–673. doi:10.1177/193229681200600323
47. Cameron D, Harris F, Evans JMM. Self-monitoring of blood glucose in insulin-treated diabetes: a multicase study. BMJ Open Diab Res Care. 2018;6(1):e000538. doi:10.1136/bmjdrc-2018-000538
48. Austin MM. The two skill sets of self-monitoring of blood glucose education: the operational and the interpretive. Diabetes Spectr. 2013;26(2):83–90. doi:10.2337/diaspect.26.2.83
49. Deshmukh V, Deshmukh C. Achieving good glycaemic control-effective use of self monitoring of blood glucose (SMBG). J Indian Med Assoc. 2012;110(3):161–163.
50. Carman KL, Dardess P, Maurer M, et al. Patient and family engagement: a framework for understanding the elements and developing interventions and policies. Health Aff. 2013;32(2):223–231. doi:10.1377/hlthaff.2012.1133
51. Maurer M, Dardess P, Carman KL, Frazier K, Smeeding L. Guide to patient and family engagement: environmental scan report AHRQ publication No.12-0042-EF. Rockville, MD: Agency for Healthcare Research and Quality. Available from: https://www.ahrq.gov/research/findings/final-reports/ptfamilyscan/index.html.
52. World Health Organization. Patient engagement: technical series on safer primary care; 2016. Available from: https://apps.who.int/iris/bitstream/handle/10665/252269/9789241511629-eng.pdf?sequence=1.
53. American Hospital Association. Engaging health care users: a framework for healthy individuals and communities. Chicago, IL: American Hospital Association; 2013 Available from: https://www.wsha.org/wp-content/uploads/engagement_AHA_Engaging_Health_Care_Users.pdf.
54. Minniti M, Abraham M. Essential allies—Patient, resident, and family advisors: a guide for staff liaisons. Bethesda, MD: Institute for Patient- and Family-Centered Care; 2013.
55. Coulter A. Engaging Patients in Healthcare. Maidenhead, UK: Open University Press; 2011.
56. Ontario’s patient engagement framework creating a strong culture of patient engagement to support high quality health care. Healthcare Quality. Queen’s Printer for Ontario; 2017.
57. Mullan RJ, Montori VM, Shah ND, et al. The diabetes mellitus medication choice decision aid: a randomized trial. Arch Intern Med. 2009;169(17):1560–1568. doi:10.1001/archinternmed.2009.293
58. Guyatt GH, Haynes RB, Jaeschke RZ, et al; Evidence-Based Medicine Working Group. Users’ Guides to the Medical Literature: XXV. Evidence-based medicine: principles for applying the Users’ Guides to patient care. JAMA. 2000;284(10):1290–1296. doi:10.1001/jama.284.10.1290
59. Tsapas A, Matthews DR. N of 1 trials in diabetes: making individual therapeutic decisions. Diabetologia. 2008;51(6):921–925. doi:10.1007/s00125-008-0983-2
60. Shah ND, Mullan RJ, Breslin M, Yawn BP, Ting HH, Montori VM. Translating comparative effectiveness into practice: the case of diabetes medications. Med Care. 2010;48(6 Suppl):153–158. doi:10.1097/MLR.0b013e3181d5956c
61. Frosch DL, Rincon D, Ochoa S, Mangione CM. Activating seniors to improve chronic disease care: results from a pilot intervention study. J Am Geriatr Soc. 2010;58(8):1496–1503. doi:10.1111/j.1532-5415.2010.02980.x
62. Stamp KD, Dunbar SB, Clark PC, et al. Family partner intervention influences self-care confidence and treatment self-regulation in patients with heart failure. Eur J Cardiovasc Nurs. 2016;15(5):317–327. doi:10.1177/1474515115572047
63. Strom JL, Egede LE. The impact of social support on outcomes in adult patients with type 2 diabetes: a systematic review. Curr Diab Rep. 2012;12(6):769–781. doi:10.1007/s11892-012-0317-0
64. Coulmont M, Roy C, Dumas L. Does the Planetree patient-centered approach to care pay off?: a cost-benefit analysis. Health Care Manag. 2013;32(1):87–95. doi:10.1097/HCM.0b013e31827edbfe
65. Gazelle G, Liebschutz JM, Riess H. Physician burnout: coaching a way out. J Gen Inter Med. 2015;30(4):508–513. doi:10.1007/s11606-014-3144-y
66. Nelson KM, Helfrich C, Sun H, et al. Implementation of the patient-centered medical home in the Veterans Health Administration: associations with patient satisfaction, quality of care, staff burnout, and hospital and emergency department use. JAMA Inter Med. 2014;174(8):1350–1358. doi:10.1001/jamainternmed.2014.2488
67. Cene CW, Johnson BH, Wells N, Beverly B, Davis R, Turchi R. A Narrative review of patient and family engagement: the “Foundation” of the medical home. Med Care. 2016;54(7):697–705. doi:10.1097/MLR.0000000000000548
 © 2022 The Author(s). This work is published and licensed by Dove Medical Press Limited. The full terms of this license are available at https://www.dovepress.com/terms.php and incorporate the Creative Commons Attribution - Non Commercial (unported, v3.0) License.
By accessing the work you hereby accept the Terms. Non-commercial uses of the work are permitted without any further permission from Dove Medical Press Limited, provided the work is properly attributed. For permission for commercial use of this work, please see paragraphs 4.2 and 5 of our Terms.
© 2022 The Author(s). This work is published and licensed by Dove Medical Press Limited. The full terms of this license are available at https://www.dovepress.com/terms.php and incorporate the Creative Commons Attribution - Non Commercial (unported, v3.0) License.
By accessing the work you hereby accept the Terms. Non-commercial uses of the work are permitted without any further permission from Dove Medical Press Limited, provided the work is properly attributed. For permission for commercial use of this work, please see paragraphs 4.2 and 5 of our Terms.




