Back to Journals » Journal of Multidisciplinary Healthcare » Volume 13
The “Ideal” Clinical Supervision Environment in Nursing and Allied Health
Authors King C, Edlington T, Williams B
Received 21 November 2019
Accepted for publication 22 December 2019
Published 17 February 2020 Volume 2020:13 Pages 187—196
DOI https://doi.org/10.2147/JMDH.S239559
Checked for plagiarism Yes
Review by Single anonymous peer review
Peer reviewer comments 2
Editor who approved publication: Dr Scott Fraser
Christine King, 1 Tanya Edlington, 2 Brett Williams 1
1Department of Community Emergency Health and Paramedic Practice, Monash University, Melbourne, VIC, Australia; 2The Conversation Clinic Pty Ltd, Melbourne, VIC, Australia
Correspondence: Brett Williams
Department of Community Emergency Health and Paramedic Practice, Monash University, Melbourne, VIC, Australia
Tel +61 49 904 4283
Email [email protected]
Background: The importance of effective clinical supervision for emerging clinicians is well recognised, not only for practice preparation, but also for reducing future attrition rates. Also recognised are the challenges faced by both students and supervisors during the supervision experience. This study aimed to identify the qualities of the “ideal” clinical supervision environment from the perspective of clinical supervisors from both nursing and allied health.
Design: A qualitative study using an interview method based on action research.
Methods: The convergent interview method was used with 20 clinical supervisors and educators from nursing and allied health across Victoria. Interviews were recorded and data analysis occurred at the end of each pair of interviews to develop deeper questions in line with the method.
Results: 12 major themes emerged as “ideal” qualities with a range of suggestions on how these can be achieved.
Conclusion: The “ideal” qualities can be used in assessing and improving current contexts, as well as designing new clinical supervision processes, models, programs and guidelines or policies. The convergent interview method allowed for deeper level analysis than previous research.
Keywords: clinical supervision, clinical placement, health educators, nursing, allied health personnel
Introduction
Clinical supervision is essential in practice preparation in clinical settings. It develops the professional values, identity, and competency of emerging clinicians while also offering professional development opportunities for experienced clinicians and reductions in stress and burn-out.8,27,33,47 Although there is no universally accepted definition, clinical supervision generally means
a process that seeks to create an environment in which participants have an opportunity to evaluate, reflect and develop their own clinical practice and provide a support system for one another.50
In healthcare, clinical supervisees receive increased attention due to continued high attrition rates globally among nurses.13 Although slow to catch on in Australia, clinical supervision is widely considered critical to the transition from student nurse to graduate staff nurse, and the quality of those transition experiences influence retention.18,21,37 Other healthcare professions, such as physiotherapists, are also reported as having high attrition rates in Australia and ceasing clinical practice early because of various reasons such as family, burnout, or work-related musculoskeletal disorders.35 Health Workforce Australia25 also reports high attrition rates of Speech Pathologists because of high caseloads, rationing of services, and lack of autonomy and career pathways suggesting
high attrition and high levels of part-time work impact on workforce supply and capacity, including the number of experienced practitioners able to provide more complex speech pathology services, as well as training capacity – both in terms of clinical supervision and academic/research activity.
The literature mostly highlights the challenges faced by nursing students during clinical supervision. Beck and Srivastava6 conducted a study with undergraduate nursing students on their level and source of stress by identifying their level of physiological and psychological health. They found that one main cause of stress was the atmosphere created by the clinical facilitator. Given that this study did not focus on the clinical environment, but on the students’ entire undergraduate experience, this finding is of great concern. Beck,5 later researched nursing students’ initial experiences in the clinical area and showed that nurses often experienced pervading anxiety, feeling abandoned, reality shock, feeling incompetent, and questioned their career choice. The literature identifies a whole range of other stressors and anxiety that nurses experience during clinical placements.20 In a study by two Australian universities to explore speech pathology student perceptions of clinical placements, one shared theme by both international and domestic students was that “the relationship that students develop with their clinical educator on placement was considered crucial and influenced their perception of the placement’s success”.2
Literature on the challenges faced by supervisors is more limited. Two key documents produced by Health Workforce Australia,26 and Department of Health, Victoria,49 highlight that the supervisor is responsible for many facets of clinical learning and culture within organisations, such as: managing conflict, professionalism, self-awareness, feedback, active listening, empathy, performance management, professional development, and management of psychological risk. Browning10 also emphasises the challenges faced by clinical supervisors when the need for “difficult” conversations arises. Research suggests that interventions for such challenges are often under-represented.36
Cummins13 believed it is important to identify whether clinical supervision is simply a system to ensure an effective workforce or a system that will empower nurses to realise their vision. She advocates for the latter, and calls for the improvement of existing support structures such as mentorship. Given that clinical supervisors and students face challenges it makes sense to focus on clinical supervision education for all involved.
Clinical supervision needs to be seen not only as an educational activity but also as a relationship.27 It is through this ongoing relationship where a range of facilitative and evaluative activities provide mutual benefits for supervisors and supervisees.3,41 Aston and Molassiotis1 evaluated the supervision environment and suggest that both supervisors and students require preparation for successful implementation of clinical supervision. Elliot20 suggested that although nursing education has been university-based for many years in Australia, the use of the clinical environment as a learning or teaching experience is yet to be maximised. More recent literature has shown a greater emphasis on learning and teaching within this environment; however, improvements are still recommended.46 Our research aims to contribute to this maximisation by finding the qualities of the “ideal” clinical supervision environment, as perceived by nurses and other allied healthcare clinical supervisors and educators in Victoria, Australia.
Method
Design
This study was part of a larger research project called: “The use of DVD simulations to teach effective communication to clinical supervisors”.51 The study involved nurses and other allied healthcare supervisors across Victoria and used a qualitative action-research-based method known as Convergent Interviewing.14 This method is based on undertaking cycles of paired interviews and after each pair of interviews, the interviewee tests for convergent information and explores divergent information (Figure 1). Subsequent questions arising from the analysis after each pair of interviews come from the participants’ data analysis. In this process, emergent and deeper levels of understanding (complexity) are possible, which is difficult with traditional interview methods. Through this deeper level of questioning, themes emerge from the data that form the basis of the results. This method assumes that the interviewer (an outsider) lacks knowledge compared to the interviewees (insiders) about the situation, so is not well equipped to develop a list of prior interview questions. The method also has a secondary benefit of shared learning and ownership, as participants recognise that this deeper level of questioning could only emerge through such a process, and perceive that the interviewer is genuinely listening.30
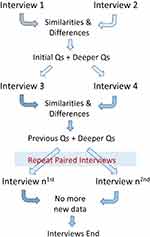 |
Figure 1 Convergent interviewing method. |
Participants
Study participation invitations were sent to 117 clinical supervisors who were participants of nine previously held “difficult conversations” workshops.51 Approximately 40 people responded with their availability. The number of interviews was dependent upon when “saturation of ideas/knowledge” was reached from the interviewer’s perspective, and this was reached at 20 interviews. That is, the last pair of interviews were interview 19 and 20. The 20 interviewees were selected based on their availability. Where participants’ availability coincided, the first to respond was provided at that time. Selection also had to ensure a cross-section of the attendees and this was achieved using the demographic data from the workshops. Each interview took approximately 45 mins.
Procedures
Interviews were carried out by telephone and typed into a word document by the interviewer during the interview. They were also recorded, so that the interviewer could go back and insert or check any parts that were missed immediately after the interview. The broad question used to explore interviewee perspectives of the “ideal” clinical supervision environment was: “Can you describe what the ‘ideal’ clinical supervision environment might look like and what key features would it have?” In line with the convergent interview process, subsequent questions that emerged through the process were asked after the initial broad question.
Data Analysis
As convergent interviewing requires a level of analysis throughout the interview process, after each pair of interviews, the interviewer spent approximately two hours examining the data to construct new additional questions to confirm, disconfirm, and explore at a deeper level. Time to do this analysis had to be factored into the interview schedule. The convergence of the data led to themes being identified along the way. Once the interviews were complete, the interviewer listed these themes, referring back to the data to check assumptions, explore further the depth for each of the themes, and distil interviewee quotes that represented the key points for each emergent theme.
Ethics
Ethics approval was obtained for the project from the Monash University Human Research Ethics Committee (MUHREC).
Results
Participant Demographics
Twenty health professionals took part in the convergent interviewing process. Ten were nurses (one clinical educator), eight were in allied health (five speech pathologists, two physiotherapists, one community support worker) and two were in medicine. Two participants were from the private sector and 18 from the public sector. Eight participants identified as being metropolitan based, eight as regionally based, and two as rural based. No participants identified as being remote. Eighteen of the 20 participants indicated that they had some previous form of training in clinical supervision, with eight indicating formal qualifications in clinical supervision. When asked which type of clinical supervision they provided, it was determined that eight were in one-on-one and multiple student supervision; five were in one-on-one, multiple student and team supervision; two were in each of multiple student, team, and multiple and team; and one participant was in only one-on-one supervision. Table 1 shows the participants’ years of experience in the health sector and as a clinical supervisor.
 |
Table 1 Participant Experience with the Health Sector and as a Clinical Supervisor |
Emergent Themes
A total of 12 major themes emerged from the broad question: “Can you describe what the ‘ideal’ clinical supervision environment might look like and what key features would it have?” and subsequent emergent questions. As the question asked interviewees their perceptions of clinical supervision, then the findings of this study are based on the interviewees own definition of clinical supervision. These themes are described below.
Theme 1: The “Ideal” Environment Would Learn from Students and Clinical Supervisors “Best” and “Worst” Clinical Supervision Experiences
Interviewees highlighted the importance of learning from experience and identified what they perceived as the “best” and “worst” aspects of their clinical supervision experiences. Five “best” aspects were identified including: (i) a formal structure of supervision (including formalised feedback), (ii) students and supervisors both being clear about assessment expectations, (iii) having a learning approach rather than a pass or fail approach, (iv) working with motivated students, and (v) an interactive learning approach with constant communication rather than a teaching approach. One interviewee also stated that having both a junior supervisor and a senior supervisor was beneficial for a student to gain a range of perspectives from their clinical placement.
A range of “worst” aspects were identified including (i) a supervisor having too many students for the context they were in, (ii) a clinical educator not hearing about a poor relationship between a student and supervisor until something has gone wrong, (iii) when assessment is open for debate and a student does not agree with their marking, (iv) when a university pushes for a student to pass even though a clinical supervisor has failed them, (v) when a supervisor does not know what a student can and cannot do, (vi) when a student is paired with a supervisor that does not want them, (vii) when there is no time for feedback, (viii) the short amount of time you have to get to know a student, and (viii) the fact that it is difficult for a student who is there infrequently to follow through with a patient. The difficulties faced by students on placement in accessing information technology (IT) was also highlighted as a “worst” aspect. This was usually referring to students on limited time-frames; however, some mentioned it for longer placements in remote areas.
Theme 2: The “Ideal” Environment Would Enable Students to Move Between Group Supervision and One-on-One Supervision
The value of students working in groups was identified as a key component of an “ideal” clinical supervision model as students could learn from each other, provide peer support, and gain a better picture of what is happening through multiple perceptions. The value of students working one-on-one with supervisors was also emphasised, with the main benefit being the depth and disclosure that was made possible in a one-on-one relationship. Situation and context were seen as the main determinants of how group and one-on-one processes were incorporated and all interviewees recognised the benefits of having both.
The “ideal” group size for home visits in the community services context and small private establishments such as physiotherapy, speech pathology, or allied health clinics was considered to be 2 to 1. In a hospital context, a ratio of 1 to 8 was seen as too difficult for preceptors, with recommendations of a ratio of 1 to 4 (possibly 6) for “non-challenging” students and a ratio of 1 to 2 for “challenging” students. The ideal group size suggested for in-patient wards was 4 to 1; however, a number of interviewees suggested that a ratio of 8 to 2 would be “ideal” as students then receive the benefits of the different perspectives offered by two supervisors, as well as experiencing different communication styles and modelling behaviour. The major benefit of this team nursing concept was consistency for everyone involved and being able to address the human side of clinical practice. An additional benefit was for students to experience the progression of patients over time.
Theme 3: The “Ideal” Environment Would Ensure That Students and Preceptors Were Well Prepared Prior to Placement
Most interviewees discussed the need for student preparation improvement prior to clinical placement, suggesting 2–3 days of teaching, either before, or in the initial days of clinical placement. Problems discussed were the lack of knowledge that students had about their placement in general, skills in reflection that focus on performance, and the basics of an oral exam. As one interviewee explained
There often needs to be some teaching and this is something that we are not very good at. We have to tick them off on self-reflection, but we never actually teach it. There is a feeling that we are being sent unprepared students … so there is some resentment about teaching it to them on placement.
Also suggested was the involvement of someone from the university to assist in teaching these skills during these 2–3 days. The preceptors’ preparation was also questioned by interviewees. Two main issues were preceptors’ knowledge of what students at different levels can and cannot do, and understanding the differences in assessment requirements of students at different levels. The lack of training to improve preceptor preparation was the main concern.
Theme 4: The “Ideal” Environment Would Have a Clinical Educator Supporting Students and Supervisors Based in the Placement Organisation, and in the Case with Nursing, a Clinical Educator on Every Ward
In terms of clinical supervision within hospitals, the “ideal” model was suggested to have a clinical educator in every ward. This was recognised as being extremely beneficial by interviewees that were currently working with this model, and by interviewees working with other models. There were two main benefits mentioned to this model, one being that staff are busy and need support from a person focused on clinical education, and the second being that a clinical educator on a ward can have a good relationship with both preceptors and students, and can gain feedback from students about preceptors and vice versa. This provides an alternative perspective when the need arises. Thirdly, an alternative model suggested by some interviewees was to have a clinical educator assigned to a group of students. The other benefit with a clinical educator on every ward is that they can work with undergraduate and postgraduate students, as well as nurses all the time. Other professions also mentioned having a clinical educator based within their organisation to work with all student placements and be responsible for reporting. It was suggested that this would enable clinical supervisors in these organisations to focus on the learning component of supervision rather than administrative tasks, and take on more students.
Theme 5: The “Ideal” Environment Would Ensure More Awareness of the Different Tasks and Time Required for Clinical Supervision and What This Means for Busy Settings and Funding
In this study, the majority of interviewees felt that blaming lack of time as a reason for poor supervision was a poor excuse or “cop out.” Interviewees stated that in the medical setting, approximately 20% of a clinician’s time is allocated to non-clinical duties, including supervision, student support, and administration, so lack of time is not really the issue. In addition, they felt that most clinicians had the attitude now that if the issue or feedback is important enough, they will make time. As one interviewee stated, “I always make time … if someone needs feedback … then they need feedback … and the sooner the better.” Only a few interviewees felt that more time would be beneficial but acknowledged that the real issue was their own time management. A number of interviewees did however acknowledge that time for supervision was sometimes a juggling act. The size of the organisation, its attitude towards clinical supervision, and the type of profession, were all seen to influence whether or not clinical supervision was supported and/or funded. For example, as one allied health interviewee explained
We are in a big health network so it accepted that you take time out to do that … but others have no funding in smaller groups … where you have all OTs [occupational therapists] or all speechies. [speech pathologists]
Theme 6: The “Ideal” Environment Would Ensure Students Did Not Face Any Surprises During Their Clinical Appraisal
Many of the interviewees stated that in a clinical appraisal, a clinical supervisor should “ensure there are no surprises” and never use an appraisal to introduce something that a student does not already know. Interviewees suggested that the best way to do this was for the supervisor to give feedback as early as possible if they have a concern, ideally on the same day, and then set a goal with the student on what to do next time. This feedback could be either informal or formal, and had to be decided upon given the situation. Interviewees believed that by addressing issues sooner, more “difficult” conversations were less likely later. Other suggestions included an “expectations” document which maps out week-to-week where students should be and checking and asking questions along the way. Most standard clinical supervision guidelines distinguish between the role of clinical supervision (i.e., support and reflection) and the role of the individual performance appraisal. Some interviewees expressed that although it was “ideal” to ensure there were no surprises, that in reality this was not always possible. For example,
You have to be flexible … you can’t really ensure no surprises … the majority of my job is done in the community … so I try and give students the heads up … I would have discussed my concerns before the mid assessment form but they often don’t take it on board unless it is in writing.
Theme 7: The “Ideal” Environment Would Place a Large Emphasis on Clinical Supervisors and Educator’s Role Modelling the Behaviours They Want to See in Their Students
Clinical supervisors and educators modelling the behaviours they want to see in their students were also seen as “ideal”. Suggested behaviours included being professional, listening, clear and concise communication, achieving what you say you are going to achieve, integrity, being genuine, and addressing issues as they arise. As one interviewee stated
You have to be a role model … never tell someone something you can’t achieve … I will be back in half an hour to debrief … and then not follow through … be genuine with students … forming a therapeutic relationship with the student is important so they feel comfortable … the same that we do with patients.
Theme 8: The “Ideal” Environment Would Have Students Skilled in Reflection and Feedback Before They Began, or at the Beginning of, Their Clinical Placement
The importance of students having skills in reflection and feedback was mentioned by all interviewees, no matter their profession or what clinical supervision model they were working with. It was also stated by many interviewees that students could describe a clinical session but not actually reflect on it. Engaging in reflective practice was seen as a skill that must be learned, requiring both practical knowledge on how to practise it, as well as a structure to follow. In general, interviewees agreed that students were ill-prepared to engage in reflection. In addition, supervisors were expected to tick the reflection box on assessment forms even though they did not really see evidence of student reflection.
Theme 9: The “Ideal” Environment Would Use a Strengths-Based Approach with Students
Three interviewees used the label of a “strengths-based approach” and many others used descriptions that reflected this approach (e.g. identify what is going well, encouraging students to do more of it, and build on those). Also highlighted was the need for supervisors to truly believe that students do have strengths, resources, and the capacity to improve their skills, and then provide them the support systems to do this.
Theme 10: The “Ideal” Environment Would Include a More Effective Relationship Between the University and the Placement Organisation
Interviewees perceived that universities differed in how effective they are in terms of creating the “ideal” clinical supervision environment. The names of a couple of universities came up repeatedly as being “ideal” in terms of the support they provided, the involvement they had, and how students were prepared for placement. Few universities were seen as having little or no involvement during placement, providing inadequate support, and/or producing unprepared students with no knowledge about their placement, expectations and role. The majority of universities were between these two extremes and the relationship was described as “good” if the organisation could easily alert the university about any problems. All but one interviewee stated that when there was a very serious issue, most universities did “produce the goods” and provided adequate support. In all cases, interviewees gave actual examples to back up their claims.
The majority of interviewees thought that universities should be more involved with placement visits suggesting more hands-on support, telephone conferences, case studies of anonymous students, greater availability for discussions, and on-site visits. Occasional face-to-face meetings or solely online interactions were felt to be inadequate. In general, interviewees felt that supervision should be a three-way relationship between university staff, students, and supervisors, and not just students and supervisors. Perhaps, not surprisingly, a geographic component appeared to mediate the level of a university’s involvement in clinical supervision. As one interviewee noted
We deal with 4 universities … geographically it can be hard. We have more involvement when a university is closer to us … but if they are far away … we don’t see them … and sometimes don’t hear from them … out of sight, out of mind.
Theme 11: The “Ideal” Environment Would Reduce Tensions Between University Staff and Clinical Supervisors About Passing Students
Interviewees expressed concern that universities are under some amount of pressure to pass students, and when clinical supervisors feel a student is not ready to be passed, tensions arise. As one interviewee put it, “Universities push people through even [in spite of] poor assessments.” Another interviewee noted, “If you say you have a concern, the uni will be informed … and then they will get in touch and then they contact us and then they ask – what are you going to do to make them pass!?” There was a general view that the pressure to pass students resulted in a lack of attention to the placement site, how assessment was carried out, and the supervisor. One interviewee was candidly shocked by the lack of university involvement and believed that this lack of involvement resulted in supervisors being unclear about the university’s requirements. Some interviewees suggested that a solution would involve the university having someone who had a deeper understanding of what was required being based at the hospital or university to oversee students.
Theme 12: The “Ideal” Environment Would Include Universities Providing Relevant Information About Students Prior to Placement
Several interviewees noted the lack of information about students before they arrive on-site. This information could serve as a “heads-up” concerning potential challenges or instances in which extra support for a student might be warranted. One interviewee described a recent event where, “if we had known the past history we would have been able to manage the student better” where the student just had someone close to them die and they would have chosen not to put them in the emergency ward. Another interviewee also explained that a student struggling academically may be more likely to struggle during a placement as well. One interviewee noted, “To be ideal it would be good to have a bit of information on these students before they come, for example, any cultural/linguistic issues or written language skills.” Such information could help determine placements and overall approaches to management. However, one interviewee also noted that although there would be benefits to having this information, there is also the potential that it could bias the assessment of students.
Discussion
This study enabled the identification of a variety of qualities of the “ideal” clinical supervision environment and these findings can be compared with other research. For example, having both group and one on one supervision is supported in the literature. Evidence favouring only group supervisions is very limited and the main benefit distinguishing group from individual supervision is the opportunity for peer interaction and support.22 As with our study, research also shows that the most satisfying preceptorship model as perceived among nursing placements is one that involves intensive mentoring rather than increasing students’ independence.40 In terms of student preparation at the onset of placement, Windsor52 stated that adequate preparation has been credited with “making all the difference in the world”.52 Elliot suggests that preparation can include being familiar with assessment tasks, knowing who the clinical facilitator will be, having priority setting and problem-solving skills, or reading the institution’s policies, and can be carried out prior to clinical placement.
Most of the literature tends to assume that students are prepared by the university but face additional challenges in spite of this preparation. Our study found that there was a perceived lack of student preparation; however, this could be inflated by what one interviewee described as the mismatch between student and supervisor expectations of the supervisory experience. If this is the case, then the students being perceived as unprepared make sense. However, the lack of, and need for, effective training of preceptors has also been noted in relation to the quality experience of students.24
Contrary to this study that found that interviewees believed lack of time was an excuse to addressing issues during clinical supervision, lack of time and busy workloads has been identified in many studies as a barrier to effective clinical supervision.12,15,29 Reid-Searl and Happell43 stated that the research shows that supervision really suffers in clinical setting that are extremely busy, hectic, and super-charged, such as emergency rooms. Given the alarming frequency and seriousness of medication errors, it is in these extremely busy environments where the closest supervision is required, but time pressures detract from quality supervision.32,44
Clinical supervisors need to provide essential knowledge, skills, support and encouragement to students and the placement organisation has to navigate and coordinate student semester breaks and the overall schedule of the preceptors.9,11 Failure to deal with these challenges has eroded the quality of the experience into a “tick-the-box” paperwork exercise that leaves all parties feeling fatigued and unfulfilled.9 The literature highlights the importance of participants receiving recognition for their work as the role of the preceptor is often seen as an additional task to a full-time workload.23,28,48
Social Learning Theory (SLT) upholds role modelling as an effective way to modify an observer’s behaviour because people tend to adopt the practices of exemplary models and compare their own performance relative to the model.4 Donaldson and Carter16 studied role modelling in the nursing clinical education context, finding that “good” role models have a tremendous influence in developing both student competence and confidence. Our study had similar findings. Another study found that both students and faculty staff perceived that ‘being or not being a good role model was the most critical characteristic differentiating the good from the less desirable clinical teacher”.39
The personal qualities of an effective supervisor that were mentioned by interviewees in our study are also echoed in the literature. For example, a good supervisor is one that has confidence in their own approach, is well organised, and knows how to deal with conflicts.27,31 Driscoll17 described some of the personal qualities in supervisors that lead to excellence in supervision as the ability to read and track the emotional content of the relationship; lessening the traditional structural power differential by explicitly being open to mutual discussion and learning; active and attentive listening to the supervisee; effective inquiry techniques that facilitate learning; and the ability to both give feedback and be open to receiving it as well. From the student’s perspective, such qualities as helpfulness, empathy, humour, flexibility, dependability, enthusiasm, respect, and a commitment to teaching novices are all desirable in a supervisor.23
Reflective practice has long been used in education to stimulate critical thinking and enhance problem-solving, and more recently has made its way into the fields of supervision and counselling.7,45 Clinical supervisors and students having good reflection skills were also seen as important in our study. Whether it occurs during practice or afterwards, the aim of reflection is a deeper analysis of what is or has occurred in order to make sense of it and subsequently make changes to one’s practice in order to improve it. Many have called for specific training in it as a vital pathway for professional development.38,42,53 Senediak46 offered several example questions that supervisors might use to stimulate reflection among supervisees and suggests that “critical enquiry into one’s own practice to examine and refine clinical work is a skill that supervisees most often need to learn.”
In addition to reflective practice, a strength-based approach was also identified as important in our study. A strength-based approach has a longer tradition of application in social work practice and more recently in mental health practice. In the clinical health area, however, a strength-based approach is applied at an individual level, rather than being recognised as a core principle or common practice. Edwards19 noted that strengths-based clinical supervision has strong roots in Positive Psychology. He notes that one of the easiest and most effective ways of introducing this concept is to have supervisors and supervisees tell each other a story about themselves when they were at their very best in clinical practice, to bring forward each person’s ability to do well.
Perceiving clinical supervision as a tri-partite model between the student, the university and the placement organisation was an unanticipated theme that emerged from our study. McKellar & Graham34 also found this to be important when they conducted a review of the elements of quality in clinical placements. In their review they found one enabler to be effective communication and collaboration between students, academic institutions, and placement sites to ensure adequate placement preparation.
Limitations
This study has a number of limitations. First, participants who took part in the convergent interviews were selected as a cross-section of a larger group that took part in a “difficult conversations” workshop, rather than a cross-section of clinical supervisors in Victoria, per se. However, there were no exclusion criteria used to select participants for the “difficult conversations” workshop, and therefore we would hope that participants were representative of the wider population of clinical supervisors. A second limitation was only conducting one series of convergent interviews. Although this allowed for multi-professional issues to be explored where participants could comment on clinical supervision in general, as well as their own and others' context, conducting a series of interviews with each profession would have enabled a greater depth of understanding on the “ideal” environment for each profession. The latter however, in isolation, would have been limited in allowing cross context and interface issues to surface.
Conclusion
The findings of this study, represented as themes, suggest many “ideal” qualities when it comes to the clinical supervision environment. These can be used in assessing and improving current contexts, as well as designing new clinical supervision processes, models, programs and guidelines or policies. Learning from experience, enhancing students’ reflection and feedback skills, supervisor role modelling, both group and one-on-one supervision, the presence of clinical educators, strength-based approaches, being more aware of time requirements, and perceiving supervision as a tri-partite relationship, all show promise in enhancing the clinical supervision experience.
The emergent and inquiry-based nature of convergent interviewing allowed for more in-depth understanding than many previous studies, such as the issue of lack of time and its influence on clinical supervision. It also enabled some surprises to emerge, such as the importance and nature of the relationship between the university, the placement organisation, and the student; and the different types of support needed from the university prior, during and after placement. This is a research area that is currently very limited and provides opportunities for further research.
Having multi-professional participants was also beneficial to bring out similarities and differences in clinical supervision between the professions, as well as contextual issues. As interviewees shared their experiences, not only in Victoria, but from other states in Australia (and internationally), interviews provided a rich source of data of the “state of play” of clinical supervision in Australia, in so far as it would be safe to say that the effectiveness of, and approaches to, clinical supervision are extremely varied and diverse, where both failing and best practice case studies abound.
Acknowledgments
We like to thank and acknowledge the generous funding provided by the Department of Health, Victorian Government. We would also like to thank the clinical supervisors from nursing and allied health care that offered their time to take part in our interviews.
Disclosure
The authors report no conflicts of interest in this work.
References
1. Aston L, Molassiotis A. Supervising and supporting student nurses in clinical placements: the peer support initiative. Nurse Educ Today. 2003;23:202–210. doi:10.1016/S0260-6917(02)00215-0
2. Attrill S, Lincoln M, McAllister S. International students in speech-language pathology clinical education placements: perceptions of experience and competency development. Int J Speech Lang Pathol. 2015;17(3):11. doi:10.3109/17549507.2015.1016109
3. Bambling M, King R. The effect of clinical supervision on the development of counsellor competency. Psychother Aust. 2000;6(1):58–63.
4. Bandura A. Self-efficacy: toward a unifying approach of behavior change. Psychol Rev. 1977;84(2):191–215. doi:10.1037/0033-295X.84.2.191
5. Beck CT. Nursing students’ initial clinical experience: a phenomenological study. Int J Nurs Stud. 1993;30(6):489–497. doi:10.1016/0020-7489(93)90020-U
6. Beck DL, Srivastava R. Perceived level and sources of stress in baccalaureate nursing students. J Nurs Educ. 1991;30(3):127–133. doi:10.3928/0148-4834-19910301-08
7. Belton V, Gould H, Scott J. Developing the reflective practitioner: designing an undergraduate class. Interfaces. 2006;36(2):150–164. doi:10.1287/inte.1050.0175
8. Bernard J, Goodyear R. Fundamentals of Clinical Supervision.
9. Brennan A. Preceptorship. Is tt a workable concept? Nurs Stand. 1993;7(52):34–36. doi:10.7748/ns.7.52.34.s40
10. Browning DM, Meyer EC, Truog RD, et al. Difficult conversations in health care: cultivating relational learning to address the hidden curriculum. Acad Med. 2007;82:905–913. doi:10.1097/ACM.0b013e31812f77b9
11. Chickerella BG, Lutz WJ. Professional nurturance: preceptorships for undergraduate nursing students. Am J Nurs. 1981;81(1):107–109. doi:10.2307/3462542
12. Chilvers R, Ramsey S. Implementing a clinical supervision programme for nurses in a hospice setting. Int J Palliat Nurs. 2009;15(12):615–619. doi:10.12968/ijpn.2009.15.12.45866
13. Cummins A. Clinical supervision: the way forward? A review of the literature. Nurse Educ Pract. 2009;9(3):215–220. doi:10.1016/j.nepr.2008.10.009
14. Dick B. What can grounded theorists and action researchers learn from each other? In: Bryant A, Charmaz K, editors. The SAGE Handbook of Grounded Theory. Sage: Thousand Oaks, CA; 2007:398–416.
15. Dilworth S, Higgins I, Parker V, Kelly B, Turner J Examining clinical supervision as a mechanism for changes in practice: a research protocol. J Adv Nurs. 2013;70(2):421–430. doi:10.1111/jan.12211
16. Donaldson JH, Carter D. The value of role modelling: perceptions of undergraduate and diploma nursing (adult) students. Nurse Educ Pract. 2005;5:353–359. doi:10.1016/j.nepr.2005.05.006
17. Driscoll J. Reflective Practice in Nursing.
18. Duchscher JEB. Out in the real world: newly graduate nurses in acute-care speak out. J Nurs Admin. 2001;31(9):426–439. doi:10.1097/00005110-200109000-00009
19. Edwards JK. Strengths-Based Supervision in Clinical Practice. Thousand Oaks, CA: Sage; 2013.
20. Elliot M. The clinical environment: a source of stress for undergraduate nurses. J Adv Nurs. 2002;20(1):34–38.
21. Ewens A. Changes in nursing identities: supporting a successful transition. J Nurs Manag. 2003;11(4):224–228. doi:10.1046/j.1365-2834.2003.00405.x
22. Francke AL, de Graff FM. The effects of group supervision of nurses: a systematic literature review. Int J Nurs Stud. 2012;49(9):1165–1179. doi:10.1016/j.ijnurstu.2011.11.012
23. Greenberg M, Colombraro G, DeBlasio J, Dolan J, Rich ER. Rewarding preceptors: a cost effective model. Nurse Educ. 2001;26(3):114–116. doi:10.1097/00006223-200105000-00009
24. Happell B. A model of preceptorship in nursing: reflecting the complex functions of the role. Nurs Educ Perspect. 2009;30(6):372–376.
25. Health Workforce Australia. Australia’s Health Workforce Series – Speech Pathologists in Focus. 2014.
26. Health Workforce Australia. National Clinical Supervision Skills Initiative Evaluation Strategy. Adelaide, South Australia; 2013.
27. Holloway E. Clinical Supervision: A Systems Approach. Thousand Oaks, CA: Sage; 1995.
28. Jackson M. A preceptor incentive program: rewarding staff nurses for mentorship. Am J Nurs. 2001;101(6):24a–24e. doi:10.1097/00000446-200106000-00031
29. Kenny A, Allenby A. Implementing clinical supervision for Australian rural nurses. Nurse Educ Pract. 2013;13(3):165–169. doi:10.1016/j.nepr.2012.08.009
30. King CA. Systemic Process for Facilitating Social Learning: Challenging the Legacy, in Department of Rural Development Studies. Ultuna, Uppsala, Sweden: Swedish University of Agricultural Sciences; 2000.
31. Mantzorou M. Preceptorship in nursing education: is it a viable alternative method for clinical teaching? ICUs Nurs Web J. 2004;19:1–10.
32. Maxfield D. Silence Kills: The Seven Crucial Conversations for Healthcare. VitalSmarts and AACN; 2005.
33. McCarron RH, Eade J, Delmage E. The experience of clinical supervision for nurses and healthcare assistants in a secure adolescent service: affective service improvement. Psychiatric Mental Health Nurs. 2018;25(3):145–156. doi:10.1111/jpm.12447
34. McKellar L, Graham K. A review of the literature to inform a best-practice clinical supervision model for midwifery students in Australia. Nurse Educ Pract. 2017;24:92–98. doi:10.1016/j.nepr.2016.05.002
35. McPhail S, Waite M. Physical activity and health-related quality of life among physiotherapists: a cross sectional survey in an Australian hospital and health service. J Occup Med Toxicol. 2014;9(1):9. doi:10.1186/1745-6673-9-1
36. Meyer EC, Sellers DE, Browning DM, et al. Difficult conversations: improving communication skills and relational abilities in health care. Pediatr Crit Care Med. 2009;10:352–359. doi:10.1097/PCC.0b013e3181a3183a
37. Mills JE, Francis KL, Bonner A. Mentoring, clinical supervision and preceptoring: clarifying the conceptual definitions for Australian rural nurses. A review of the literature. Rural Remote Health. 2005;5(3):1–10.
38. Moffett L. Directed self-reflection protocols in supervision. Train Educ Prof Psychol. 2009;3(2):78–83. doi:10.1037/a0014384
39. Mogan J, Knox JE. Characteristics of ‘best’ and ‘worst’ clinical teachers as perceived by university nursing faculty and students. J Adv Nurs. 1987;12(3):331–337. doi:10.1111/jan.1987.12.issue-3
40. Omer TY, Suliman WA, Thomas L, et al. Perception of nursing students to two models of preceptorship in clinical training. Nurse Educ Pract. 2013;13(3):155–160. doi:10.1016/j.nepr.2013.02.003
41. Ramos-Sánchez L, Esnil E, Goodwin A, et al. Negative supervisory events: effects on supervision and supervisory alliance. Prof Psychol Res Pr. 2002;33(2):197–202. doi:10.1037/0735-7028.33.2.197
42. Regan P. Reflective practice: how far, how deep? Reflective Pract. 2008;9(2):219–229. doi:10.1080/14623940802005616
43. Reid-Searl K, Happell B. Factors influencing the supervision of nursing students administering medication: the registered nurse perspective. Collegian. 2011;18(4):139–146. doi:10.1016/j.colegn.2011.05.003
44. Richardson J, McKie J. Reducing the Incidence of Adverse Events in Australian Hospitals: An Expert Panel Evaluation of Some Proposals. Victoria: Monash University; 2007.
45. Ronnestad MH, Ladany N. The impact of psychotherapy training: introduction to the special section. Psychother Res. 2006;16(3):261–267. doi:10.1080/10503300600612241
46. Senediak C. A Reflective Practice Model of Clinical Supervision. In Advances in Clinical Supervision Conference. Sydney, Australia: The New South Wales Institute of Psychiatry; 2013.
47. Simpson‐Southward C, Waller G, Hardy GE. How do we know what makes for “best practice” in clinical supervision for psychological therapists? A content analysis of supervisory models and approaches. Clin Psychol Psychother. 2017;24(6):1228–1234. doi:10.1002/cpp.2084
48. Stone C, Rowles C. What rewards do clinical preceptors in nursing think are important? J Nurses Staff Dev. 2002;18(3):162–166. doi:10.1097/00124645-200205000-00010
49. The Best Practice Clinical Learning Environment Framework: Quality Clinical Education in Victoria. Melbourne, Victoria: Department of Health, Victoria; 2013.
50. White E, Roche M. A selective review of mental health nursing in New South Wales, Australia, in relation to clinical supervision. Int J Ment Health Nurs. 2006;15(3):209–219. doi:10.1111/inm.2006.15.issue-3
51. Williams B, King C, Edlington T. Overcoming difficult conversations in clinical supervision. J Healthc Leadersh. 2016;8:31–40. doi:10.2147/JHL.S96592
52. Windsor A. Nursing students’ perceptions of clinical experience. J Nurs Educ. 1987;26(4):150–154.
53. Wright J. F. Griffiths, Reflective practice at a distance: using technology in counselling supervision. Reflective Practice. Int Multidiscip Perspect. 2010;11(5):693–703. doi:10.1080/14623943.2010.516986
 © 2020 The Author(s). This work is published and licensed by Dove Medical Press Limited. The full terms of this license are available at https://www.dovepress.com/terms.php and incorporate the Creative Commons Attribution - Non Commercial (unported, v3.0) License.
By accessing the work you hereby accept the Terms. Non-commercial uses of the work are permitted without any further permission from Dove Medical Press Limited, provided the work is properly attributed. For permission for commercial use of this work, please see paragraphs 4.2 and 5 of our Terms.
© 2020 The Author(s). This work is published and licensed by Dove Medical Press Limited. The full terms of this license are available at https://www.dovepress.com/terms.php and incorporate the Creative Commons Attribution - Non Commercial (unported, v3.0) License.
By accessing the work you hereby accept the Terms. Non-commercial uses of the work are permitted without any further permission from Dove Medical Press Limited, provided the work is properly attributed. For permission for commercial use of this work, please see paragraphs 4.2 and 5 of our Terms.
