Back to Journals » International Journal of General Medicine » Volume 14
The Effectiveness of the Supine Position in Managing Inferior Breaks in Rhegmatogenous Retinal Detachment After Vitrectomy with Gas Tamponade
Received 9 February 2021
Accepted for publication 9 March 2021
Published 1 April 2021 Volume 2021:14 Pages 1179—1184
DOI https://doi.org/10.2147/IJGM.S306006
Checked for plagiarism Yes
Review by Single anonymous peer review
Peer reviewer comments 3
Editor who approved publication: Dr Scott Fraser
Qiong Huang, Yang Cheng
Department of Ophthalmology, Union Hospital, Tongji Medical College, Huazhong University of Science and Technology, Wuhan, Hubei, 430022, People’s Republic of China
Correspondence: Yang Cheng
Department of Ophthalmology, Union Hospital, Tongji Medical College, Huazhong University of Science and Technology, 1277 Jiefang Ave, Jianghan District, Wuhan, Hubei, 430022, People’s Republic of China
Tel +86 027 85726533
Email [email protected]
Objective: This study aims to determine whether the supine position is effective for the management of inferior peripheral breaks after pars plana vitrectomy with gas tamponade.
Methods: A total of 29 patients (29 eyes) with acute rhegmatogenous retinal detachment and causative peripheral inferior breaks, located between the four o’clock and eight o’clock positions, underwent pars plana vitrectomy with gas tamponade. These patients maintained a face-up supine position for at least six hours each day for 14 days postoperatively. The alternate lateral position was used for the remaining hours, depending on the distribution of the retinal breaks.
Results: The final retinal reattachment rate was 100%, and the visual acuity improvement rate was 100% postoperatively, with no recurrence during the one-year follow up. No patients suffered from any sight-threatening complications. Of the 16 patients with preoperatively clear lenses, 3 were documented to have a cataract during their three-month postoperative follow up. Four patients were documented to have increased intraocular pressure, which was controllable during the early postoperative days.
Conclusion: Postoperative pars plana vitrectomy and gas tamponade in the supine position is effective for managing primary rhegmatogenous retinal detachment with causative breaks between the four o’clock and eight o’clock positions.
Keywords: rhegmatogenous retinal detachment, inferior breaks, supine position, pars plana vitrectomy, gas tamponade
Introduction
Pars plana vitrectomy (PPV) has gained popularity for the treatment of primary rhegmatogenous retinal detachment (RRD) and offers the possibility of removing the vitreoretinal traction, performing the complete drainage of subretinal fluid, and treating retinal breaks. Inferior retinal detachments associated with inferior breaks continue to present a challenging condition to be managed by PPV,1–7 and PPV with gas tamponade is generally indicated for retinal breaks that involve the superior hours of the clock. It has been recognized that strict postoperative prone positioning is essential for tamponade for inferior breaks. However, it remains difficult and uncomfortable for many patients to be appropriately positioned after surgery owing to medical, physical, or social conditions. Another inherent problem is the difficulty in maintaining a direct tamponade on inferior breaks for at least eight days of using gases.8
Recently, more surgeons have focused on determining how postoperative positions affect the outcomes of PPV in RRD due to inferior breaks. In a short-term retrospective study, Ajlan et al reported that patients with uncomplicated RRD due to inferior breaks who underwent PPV, 360° endolaser, 15% C3F8 gas, and limited (24-hour) prone positioning did not exhibit a statistically significant difference in anatomical outcome when compared with one-week postoperative prone positioning.9 Chen et al reported that the primary retinal reattachment rate of PPV with gas tamponade in an adjustable postoperative position (alternating upright or lateral recumbent position) was as high as in the traditional strict face-down position.10 Lin et al confirmed the safety and efficacy of the adjustable postoperative position after PPV for RRD under more complicated conditions.11 Shiraki et al reported that positioning without the use of a strict prone position did not decrease the success rate of the vitrectomy performed to treat RRDs, and that the supine or the lateral position appeared to be associated with a higher reattachment rate in inferior retinal breaks.12
The aim of the present prospective study is to determine whether the supine position is effective for the management of inferior peripheral breaks after PPV with gas tamponade.
Materials and Methods
The present prospective study adhered to the tenets of the Declaration of Helsinki and was approved by the Institutional Review Board of the Union Hospital Affiliated to the Tongji Medical College, Huazhong University of Science and Technology. A total of 29 consecutive acute RRD patients (29 eyes), who had peripheral inferior breaks from January 2014 to January 2016, were included in the study. Acute RRD was classified as a short duration of symptoms (<7 days). An inferior break was defined as a horseshoe tear present between the 4 o’clock and 8 o’clock positions. Exclusion criteria included previous retinal detachment surgery or vitrectomy, proliferative vitreoretinopathy (PVR) of grade C or greater, and giant retinal tears. The preoperative data collected included the age, gender, best corrected visual acuity, location and number of retinal breaks, and retinal detachment field of the patients. All patients underwent a slit-lamp examination, including biomicroscopy of the cornea; lens; vitreous; and retina, and indirect ophthalmicroscopy. In addition, intraocular pressure (IOP) was measured.
All patients underwent PPV immediately upon admission, and a standard 3-port, 23-gauge transconjunctival PPV was performed under local anesthesia by one surgeon (Y. Cheng) using a wide-angle viewing system. After the removal of the core vitreous, the posterior hyaloid was removed by active suction using a vitreous cutter. The vitreous traction on all retinal tears was carefully relieved, followed by peripheral trimming with 360-degree indentation. A thorough fluid–air exchange was performed via the most accessible retinal break, with perfluorocarbon liquids as adjuncts. The breaks were all treated with endolaser, and indentation was applied on the far peripheral breaks. A gas–air exchange was then performed with C3F8. Postoperatively, all patients were placed in the face-up supine position with no pillow under the head for at least six hours each day for 14 days. The alternate lateral position was used for the remaining hours, depending on the distribution of the retinal breaks.
Postoperatively, the best corrected visual acuities, retinal statuses, and complications were recorded for all patients. These patients were followed up and assessed during their postoperative visits at 1, 7, and 14 days and at 1, 3, 6, and 12 months.
Results
This technique was employed for 29 patients, 18 males and 11 females aged 52.4 ± 4.2 years old, with RRD and inferior breaks. The freshly detached retinae showed good mobility and were level PVR-B or PVR-A. There were 14 patients with one tear, 10 patients with two tears, and 5 patients with three tears. No patients had four or more tears. Among the 15 patients with multiple tears, there were 8 patients with tears located in the same quadrant and 7 patients with tears located in both the temporal inferior and nasal inferior quadrants. The mean number of inferior retinal breaks was 1.68 ± 0.76 on each eye, and the average number of quadrants of the retina involved in the detachment was 1.52 ± 0.69. The best corrected visual acuity varied from counting finger to 80/200. Of these patients, 11 patients had macular involved detachment, and 18 patients had macular attachment. The distances of the breaks from the ora serrata were less than four PDs, which was confirmed during PPV.
All patients improved postoperatively, and the best corrected visual acuity varied from counting finger to 120/200, and the primary anatomic success rate was 100%. No recurring retinal detachment was documented at the 12-month postoperative visits. None of these patients suffered from any sight-threatening complications, such as choroidal hemorrhage.
Of the 16 patients with preoperatively clear lenses, 3 patients were documented to have a cataract during their three-month postoperative follow-up. In addition, four patients were documented to have increased IOP during the early postoperative days (<7 days), which was reduced to normal by using a combination of topical brimonidine, bemeprostaglandin, and timolol. We observed an IOP peak on the third day after vitrectomy, and the elevated IOP was 28–35 mmHg. During the follow-up visit on day 14, the IOPs were below 15 mmHg, and the topical IOP reducers were stopped. Subsequently, the IOPs remained normal.
Case Attached
A 45-year male with RRD and causative inferior breaks underwent PPV with air tamponade. This patient was photocoagulated on the retinal breaks. However, inferior retinal detachment still developed (Figure 1). The patient was placed in the face-up supine position (with no pillow under the head) or the alternate left recumbent position for 14 days postoperatively. On the 14th day, a small air bubble still existed in the vitreous cavity, but the retina remained attached (Figure 2).
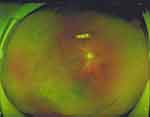 |
Figure 1 The inferior retinal detachment with causative inferior breaks and multiple peripheral breaks that have been photocoagulated. |
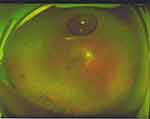 |
Figure 2 Retinal attachment on the 14th day postoperatively, with a small air bubble present in the vitreous cavity. |
Discussion
RRD with inferior breaks has been shown to have worse results when compared with RRD with superior breaks. Therefore, this remains a surgical challenge for intraocular gas tamponade. Goto et al compared the anatomic success between the repair of an RRD with superior breaks and the repair of an RRD with inferior breaks by performing a primary vitrectomy using the same gas. In their study, the primary attachment rate was 80% for inferior breaks and 98% for superior breaks.1 Heimann et al carried out a retrospective study on 53 patients with RRD, and the primary attachment rate was 64%, with a 50% re-detachment rate in the group with inferior breaks.2 According to the literature, the primary success rate is 76.9%–93.3%, and the final success rate is 95%–100%.1,3–7
There are two main reasons for the challenges in PPV when treating RRD due to inferior breaks. First, is the difficulty in completely shaving the inferior peripheral vitreous, especially in phakic eyes. Second, is the difficulty with conventional intraocular tamponade agents that produce a direct tamponade effect on the inferior breaks.13
To improve the success rate of PPV, different options have been proposed, such as combining PPV with scleral buckle; the use of long-acting tamponade, silicone oil, and heavy silicone oil; and strict positioning during the postoperative period. Since PPV and gas tamponade can be safely used to treat RRD with causative inferior breaks, silicone oil tamponade and the use of heavy silicone oil were excluded when treating the patients in the present study. In addition, reports show that severe visual loss occurs after using silicone oil, and the visual loss is associated with a significant reduction in inner retinal thickness, indicating neuronal cell loss in the macular area as a possible explanation.14 There is also a need for a second operation to extract the oil.
A scleral buckle was not used in combination with the vitrectomy, which is usually used in the presence of inferior retinal breaks or PVR, since the scleral buckle is more technically demanding and has the following associated complications: exposure, refractive change, diplopia, and risk of anterior segment ischemia.15 Several studies have revealed that PPV and gas tamponade without a scleral buckle can be safely used to treat RRD with inferior breaks.16–18 A small case series in a study conducted by Tanner et al revealed that buckling could be avoided in patients with inferior breaks.16 A study conducted by Sharma et al revealed that acceptable success rates could be achieved without scleral buckling when repairing RRD with inferior breaks using PPV and gas tamponade.17 A study conducted by Wickham et al also revealed that vitrectomy and gas, without the application of a scleral buckle, may be used to safely treat inferior break retinal detachments.18
The forces of retinal detachment and reattachment were further described by Machemer in 1984.19 It was shown that three factors are required to achieve retinal reattachment: relief of traction, alteration of intraocular currents, and chorioretinal adhesion. All these conditions can be addressed by using PPV and gas tamponade. Vitrectomy, especially under a wide-angle viewing system and scleral indentation, can enhance the peripheral vitreous traction relief. The alteration of intraocular currents can be achieved using an intraocular large gas tamponade, especially with good vitreous clearance. The key point to achieve chorioretinal adhesion, in addition to completing the subretinal fluid drainage and endolaser diode retinopexy, is to keep the breaks dry, which can be achieved by maintaining the contact of these breaks with the gas for enough time postoperatively.
In a pilot study of primary pseudophakic RRD with inferior breaks repaired with PPV alone, Martínez-Castillo reported an intravitreal volume of air in the range 90%–60% at the first 24-hour postoperative visit, and retinal breaks located between the five o’clock and seven o’clock positions were not tamponade after the first six hours postoperatively.3,4 They also reported that the postoperative volume of the tamponade agent in pseudophakic RRD was reduced with PPV and gas or air tamponade. In addition, they found that merely 14.4% of patients presented with a vitreous cavity filled to 90% or more, and that 81.6% of inferior retinal breaks located between the five o’clock and seven o’clock positions were not located within the limits of the gas bubble on the first and third days postoperatively.8 In their study, they emphasized the role of subretinal fluid drainage and the sealing of the edges of the inferior retinal breaks on laser retinopexy, thereby reducing the need for the gas bubble to cover the retinal breaks in the early postoperative period.
According to Machemer,20 the rationale for using a tamponade agent is that the surface tension of the tamponade agent permits the absorption of subretinal fluid, which keeps the retina attached for the first two weeks after laser retinopexy until a chorioretinal scar develops. The hypothesis was that the patient should be kept in the supine position. Therefore, the patients in the present study were placed in the face-up supine position for at least six hours each day for 14 days postoperatively, and the alternate lateral position was used for the remaining hours, depending on the distribution of the retinal breaks. In this position, the inferior retina breaks can be optimally tamponaded (Figure 3) and kept dry for a sufficient amount of time postoperatively to ensure retinal reattachment.
In the present study, all the patients improved postoperatively, and the primary retinal attachment rate was 100% at the 12-month follow-up. In addition, none of these patients suffered from serious complications. Of the 16 patients with a clear lens preoperatively, three developed a cataract three months postoperatively. These patients later underwent cataract surgery. There was no change at the one-year follow up in the lenses of the other 13 patients with preoperatively clear lenses or the 13 patients with initial mild opacity. This requires further study. Different rates of cataract progression (18.8%–51.8%) have been reported,21,22 which may be due to the increase in retrolental oxygen levels and the inhibition of the diffusion of nutrients impeding lens metabolism.23 The risk factors include the duration of the exposure of the lens to gas, the patient’s age, and the magnitude of the vitreous removal. It has been suggested that patients should avoid the supine position to decrease the contact between the lens and the gas. However, similar results were found when comparing the prone and the supine position.24 Previous studies25 have mentioned that supine positioning after PPV with gas tamponade is not suitable for phakia eyes, assuming that a much higher buoyancy in gas tamponaded eyes will lead to the formation of irreversible, progressive lens opacity. Another concern is pupillary block glaucoma or gas translocation to the anterior chamber due to fragile zonules of Zinn. However, no such adverse complications occurred in the current study.
In addition, 4 of the 29 patients (13.7%) suffered from increased IOP, which was controllable. An increase in IOP was reported in up to 58.9% of patients after vitrectomy with expandable gas administration for retinal detachment. The risk factors included high gas concentrations, advanced patient age, and concomitant circumferential scleral buckling.23 The rate of increase in IOP was low, and the increase occurred in the early days post-vitrectomy. This was controllable using topical antihypertensive medications. Although IOP elevation is a common complication of vitrectomy and gas tamponade that we believe is related to the expansion of the gas, the IOP returns to normal during the later follow ups when the gas volume decreases. These results are supported by earlier studies that showed that, in the majority of cases, IOP elevation is transient, with the highest mean values occurring 2–4 h postoperatively and lasting for up to one week after surgery.26
The limitations of this study include the retrospective, non-randomized design and the relatively small sample size. It needs to be validated by a larger cohort. Also, it should be emphasized that careful case selection is needed for success, including fresh and uncomplicated RRD with peripheral inferior breaks, the absence of posterior breaks, and PVR of grade C or greater. Meticulous vitreoretinal surgical techniques are also needed, including thorough vitreous clearance and complete fluid drainage, while avoiding iatrogenic tears.
It could be hypothesized that an area for future study is developing methods to achieve immediate intraoperative chorioretinal adhesion around the retinal breaks and to reduce the time needed for chorioretinal scar formation after retinopexy, thereby improving surgical results.
In conclusion, PPV and gas tamponade, with patients in the supine position postoperatively, is effective for managing primary RRD with causative breaks between the four o’clock and eight o’clock positions.
Ethics Approval and Consent to Participate
This study was conducted with approval from the Ethics Committee of Union Hospital, Tongji Medical College, Huazhong University of Science and Technology. This study was conducted in accordance with the Declaration of Helsinki. Written informed consent was obtained from all participants.
Funding
There is no funding to report.
Disclosure
The authors declare that they have no competing interests.
References
1. Goto T, Nakagomi T, Iijima H. A comparison of the anatomic successes of primary vitrectomy for rhegmatogenous retinal detachment with superior and inferior breaks. Acta Ophthalmol. 2013;91:552–556. doi:10.1111/j.1755-3768.2012.02455.x
2. Heimann H, Bornfeld N, Friedrichs W, et al. Primary vitrectomy without scleral buckling for rhegmatogenous retinal detachment. Graefes Arch Clin Exp Ophthalmol. 1996;234:561–568. doi:10.1007/BF00448800
3. Martínez-Castillo V, Verdugo A, Boixadera A, García-Arumí J, Corcóstegui B. Management of inferior breaks in pseudophakic rhegmatogenous retinal detachment with pars plana vitrectomy and air. Arch Ophthalmol. 2005;123:1078–1081. doi:10.1001/archopht.123.8.1078
4. Martínez-Castillo V, Boixadera A, Verdugo A, García-Arumí J. Pars plana vitrectomy alone for the management of inferior breaks in pseudophakic retinal detachment without facedown position. Ophthalmology. 2005;112:1222–1226. doi:10.1016/j.ophtha.2004.12.046
5. Tan HS, Oberstein SY, Mura M, Bijl HM. Air versus gas tamponade in retinal detachment surgery. Br J Ophthalmol. 2013;97:80–82. doi:10.1136/bjophthalmol-2012-302140
6. Hwang JF, Chen SN, Lin CJ. Treatment of inferior rhegmatogenous retinal detachment by pneumatic retinopexy technique. Retina. 2011;31:257–261. doi:10.1097/IAE.0b013e3181e586f9
7. Yee KM, Sebag J. Long-term results of office-based pneumatic retinopexy using pure air. Br J Ophthalmol. 2011;95:1728–1730. doi:10.1136/bjophthalmol-2011-300114
8. Martínez-Castillo VJ, García-Arumí J, Boixadera A. Pars plana vitrectomy alone for the management of pseudophakic rhegmatogenous retinal detachment with only inferior breaks. Ophthalmology. 2016;123:1563–1569. doi:10.1016/j.ophtha.2016.03.032
9. Ajlan R, Isenberg J, Cordahi G, Duval R, Olivier S, Rezende F. Primary rhegmatogenous retinal detachment with inferior retinal breaks postoperative prone positioning results: 1 day versus 7 days. Int J Retina Vitreous. 2017;3:47. doi:10.1186/s40942-017-0100-0
10. Chen X, Yan Y, Hong L, Zhu L. A comparison of strict face-down positioning with adjustable positioning after pars plana vitrectomy and gas tamponade for rhegmatogenous retinal detachment. Retina. 2015;35:892–898. doi:10.1097/IAE.0000000000000413
11. Lin Z, Sun JT, Wu RH, Moonasar N, Zhou YH. The safety and efficacy of adjustable postoperative position after pars plana vitrectomy for rhegmatogenous retinal detachment. J Ophthalmol. 2017;2017:5760173. doi:10.1155/2017/5760173
12. Shiraki N, Sakimoto S, Sakaguchi H, Nishida K, Nishida K, Kamei M. Vitrectomy without prone positioning for rhegmatogenous retinal detachments in eyes with inferior retinal breaks. PLoS One. 2018;13:e0191531. doi:10.1371/journal.pone.0191531
13. Dell’Omo R, Barca F, Tan HS, Bijl HM, Oberstein SY, Mura M. Pars plana vitrectomy for the repair of primary, inferior rhegmatogenous retinal detachment associated to inferior breaks. A comparison of a 25-gauge versus a 20-gauge system. Graefes Arch Clin Exp Ophthalmol. 2013;251:485–490. doi:10.1007/s00417-012-2059-8
14. Christensen UC, la Cour M. Visual loss after use of intraocular silicone oil associated with thinning of inner retinal layers. Acta Ophthalmol. 2012;90(8):733–737. doi:10.1111/j.1755-3768.2011.02248.x
15. Papakostas TD, Vavvas D. Postoperative complications of scleral buckling. Semin Ophthalmol. 2018;33(1):70–74. doi:10.1080/08820538.2017.1353816
16. Tanner V, Minihan M, Williamson T. Management of inferior retinal breaks during pars plana vitrectomy for retinal detachment. Br J Ophthalmol. 2001;85:480–482. doi:10.1136/bjo.85.4.480
17. Sharma A, Grigoropoulos V, Williamson TH. Management of primary rhegmatogenous retinal detachment with inferior breaks. Br J Ophthalmol. 2004;88:1372–1375. doi:10.1136/bjo.2003.041350
18. Wickham L, Connor M, Aylward GW. Vitrectomy and gas for inferior break retinal detachments: are the results comparable to vitrectomy, gas, and scleral buckle? Br J Ophthalmol. 2004;88:1376–1379. doi:10.1136/bjo.2004.043687
19. Machemer R. The importance of fluid absorption, traction, intraocular currents, and chorioretinal scars in the therapy of rhegmatogenous retinal detachments. XLI Edward Jackson memorial lecture. Am J Ophthalmol. 1984;98:681–693. doi:10.1016/0002-9394(84)90682-2
20. Machemer R, Buettner H, Norton EW, Parel JM. Vitrectomy: a pars plana approach. Trans Am Acad Ophthalmol Otolaryngol. 1971;75:813–820.
21. Jackson TL, Donachie PHJ, Sparrow JM, Johnston RL. United Kingdom National Ophthalmology Database study of vitreoretinal surgery: report 2, macular hole. Ophthalmology. 2013;120:629–634. doi:10.1016/j.ophtha.2012.09.003
22. Singh S, Byanju R, Pradhan S, Lamichhane G. Retrospective study on outcome of macular hole surgery. Nepal J Ophthalmol. 2016;8:139–143. doi:10.3126/nepjoph.v8i2.17002
23. Kanclerz P, Grzybowski A. Complications associated with the use of expandable gases in vitrectomy. J Ophthalmol. 2018;2018:8606494. doi:10.1155/2018/8606494
24. Otsuka K, Imai H, Miki A, Nakamura M. Impact of postoperative positioning on the outcome of pars plana vitrectomy with gas tamponade for primary rhegmatogenous retinal detachment: comparison between supine and prone positioning. Acta Ophthalmol. 2018;96:e189–e194. doi:10.1111/aos.13482
25. Abdelkader AME, Abouelkheir HY. Supine positioning after vitrectomy for rhegmatogenous retinal detachments with inferior retinal breaks. Int J Retina Vitreous. 2020;6:41. doi:10.1186/s40942-020-00247-8
26. Chen CJ. Glaucoma after macular hole surgery. Ophthalmology. 1998;105:94–99. doi:10.1016/S0161-6420(98)91470-1
 © 2021 The Author(s). This work is published and licensed by Dove Medical Press Limited. The full terms of this license are available at https://www.dovepress.com/terms.php and incorporate the Creative Commons Attribution - Non Commercial (unported, v3.0) License.
By accessing the work you hereby accept the Terms. Non-commercial uses of the work are permitted without any further permission from Dove Medical Press Limited, provided the work is properly attributed. For permission for commercial use of this work, please see paragraphs 4.2 and 5 of our Terms.
© 2021 The Author(s). This work is published and licensed by Dove Medical Press Limited. The full terms of this license are available at https://www.dovepress.com/terms.php and incorporate the Creative Commons Attribution - Non Commercial (unported, v3.0) License.
By accessing the work you hereby accept the Terms. Non-commercial uses of the work are permitted without any further permission from Dove Medical Press Limited, provided the work is properly attributed. For permission for commercial use of this work, please see paragraphs 4.2 and 5 of our Terms.

