Back to Journals » Journal of Pain Research » Volume 13
Ten kilohertz SCS for Treatment of Chronic Upper Extremity Pain (UEP): Results from Prospective Observational Study
Authors Burgher A, Kosek P, Surrett S, Rosen SM, Bromberg T, Gulve A , Kansal A, Wu P, McRoberts WP , Udeshi A , Esposito M, Gliner BE , Maneshi M, Rotte A , Subbaroyan J
Received 25 August 2020
Accepted for publication 10 October 2020
Published 10 November 2020 Volume 2020:13 Pages 2837—2851
DOI https://doi.org/10.2147/JPR.S278661
Checked for plagiarism Yes
Review by Single anonymous peer review
Peer reviewer comments 2
Editor who approved publication: Professor Robert B. Raffa
Abram Burgher,1 Peter Kosek,2 Steven Surrett,3 Steven M Rosen,4 Todd Bromberg,4 Ashish Gulve,5 Anu Kansal,5 Paul Wu,6 W Porter McRoberts,6 Ashish Udeshi,7 Michael Esposito,7 Bradford E Gliner,8 Mona Maneshi,8 Anand Rotte,8 Jeyakumar Subbaroyan8
1Hope Research Institute, Phoenix, AZ, USA; 2Oregon Neurosurgery, Eugene, OR, USA; 3Oregon Medical Group, Eugene, OR, USA; 4Delaware Valley Spine and Pain, Trevose, PA, USA; 5The James Cook University Hospital, Middlesbrough, UK; 6Holy Cross Hospital, Inc., Ft, Lauderdale, FL, USA; 7Florida Pain Institute, Merritt Island, FL, USA; 8Nevro Corp., Redwood City, CA, USA
Correspondence: Anand Rotte
Nevro Corp., 1800 Bridge Parkway, Redwood City, CA 94065, USA
Email [email protected]
Background: Chronic upper extremity pain (UEP) has complex etiologies and is often disabling. It has been shown that 10 kHz SCS can provide paresthesia-free and durable pain relief in multiple pain types and improve the quality of life of patients.
Objective: To gain additional evidence on the safety and effectiveness of 10 kHz SCS for the treatment of chronic UEP.
Study Design: It was a prospective, multicenter, and observational study. The study was registered on ClinicalTrials.gov prospectively (clinical trial identifier: NCT02703818).
Setting: Multicenter.
Patients, Intervention and Main Outcomes: A total of 43 subjects with chronic UEP of ≥ 5 cm (on a 0– 10 cm visual analog scale; VAS) underwent a trial of 10 kHz SCS, and subjects with ≥ 40% pain relief received a permanent implant. All subjects had upper limb pain at baseline, while some had concomitant shoulder or neck pain. Subject outcomes were assessed for 12 months, and the primary outcome was the responder rate (percentage of subjects experiencing ≥ 50% pain relief from baseline) at three months.
Results: Thirty-eight subjects successfully completed the trial (88.3% success rate), 33 received permanent implants (five withdrew consent), and 32 had device activation (per protocol population). There were no paresthesias or uncomfortable changes in stimulation related to changes in posture during the study and there were no neurological deficits. Responder rates at 12 months for upper limb, shoulder, and neck pain in per protocol population (N=32) were 78.1%, 85.2%, and 75.0%, respectively. At 12 months, 84.4% of subjects were satisfied or very satisfied with 10 kHz SCS, and 38.7% either reduced or eliminated opioid usage.
Conclusion: This study further supports the effectiveness of 10 kHz SCS for chronic UEP treatment and documents the safety profile of the therapy.
Clinical Trial Identifier: NCT02703818.
Keywords: 10 kHz SCS, VAS, upper extremity pain, shoulder and upper limb pain
Introduction
Cervical spine disorders that cause pain in the upper extremities are frequently disabling and costly to treat.1,2 In the absence of neurological compromise, upper extremity pain (UEP) patients are typically managed with conservative care including physiotherapy or minimally invasive therapies such as epidural injections. If not effective, or when neurological sequelae indicate, surgical procedures including foraminotomy, and anterior or posterior cervical discectomy with or without fusion may be indicated. For specific etiologies, neurosurgical procedures such as lesioning of the dorsal root ganglia or entry zone may be considered.
Spinal cord stimulation (SCS) is a minimally invasive, reversible therapy that, in patients with previous lumbar spine surgery, was shown to provide greater reduction in leg pain compared to re-operation.3 Decades of clinical research suggests that SCS is a safe and effective option for certain types of pain that are refractory to conservative therapies.3–6 However, evidence in the literature supporting the use of traditional SCS to treat UEP is limited to small prospective studies, retrospective case reports and case series.7–9 Moreover, traditional SCS is often accompanied by the uncomfortable paresthesias that may be exacerbated by head, neck, and upper limb position and movement.
Ten kilohertz SCS is known to provide paresthesia-independent pain relief and its efficacy has been demonstrated in different types of chronic pain conditions including low back and leg pain, nonsurgical back pain and complex regional pain syndrome (CRPS).10–13 Thus, the positional variation that compromises UEP relief with traditional SCS may be eliminated with 10 kHz SCS. However, SCS devices including 10 kHz SCS can have procedural/surgical complications such as infection, cellulitis, abscess, fever, sepsis, bleeding, cerebrospinal fluid leak, hematoma, seroma or thrombosis, epidural hemorrhage, impaired or inadequate wound healing, wound dehiscence and in rare instances spinal cord compression, nerve, nerve root, or spinal cord injury, paralysis and death. Ten kilohertz SCS was previously shown to provide pain relief and improve quality of life in patients with UEP in a small retrospective chart review.14 Recently, two prospective single arm studies reported the efficacy of 10 kHz SCS in patients with upper limb and neck pain.15,16 Upper limb pain relief recorded in these studies was 62% and 79% and the corresponding responder rate was 77% and 89%, whereas neck pain relief was 86% and 74% and the corresponding responder rate was 85% and 95%, respectively. The objective of this prospective, multicenter, observational study was to gain additional effectiveness data of 10 kHz SCS for the treatment of chronic, intractable pain of the upper extremities. Along with safety and pain relief assessments, the study also reports data from overall quality of life assessments, patient satisfaction and changes in opioid medication usage.
Materials and Methods
Ethics Statement
The investigational protocol (20152890) and informed consent forms were reviewed and approved by an Institutional Review Board in the US (Western Institutional Review Board) and ethics committee in the UK in January 2016, prior to patient enrollment. All aspects of the study were conducted in accordance with the Declaration of Helsinki and national, federal and local laws of pertinent regulatory authorities. The protocol was listed on ClinicalTrials.gov (NCT02703818) in January 2016 and was conducted as per STROBE guidelines.
Study Design and Patient Population
This was a prospective, postmarket, observational, multicenter study designed to provide evidence on the safety and effectiveness of 10 kHz SCS in subjects with chronic, intractable pain of the upper extremities (upper limbs with or without concomitant neck or shoulder pain). Outcomes were assessed via standardized tests.
Subjects with chronic UEP, affiliated with or referred to the clinical sites, who were identified by the study investigators as candidates for SCS therapy, were recruited from multiple centers in the US5 and UK.1 Subjects who signed informed consent were assessed for eligibility based on the inclusion and exclusion criteria.
Key inclusion criteria were chronic, intractable UEP (visual analog scale, VAS ≥5 out of 10 cm) in adults aged 18 years and up, refractory to conservative therapy for a minimum of three months (previous conservative treatments included pain medications, physical therapy, spinal injections, pharmacological, and behavioral treatment); appropriate candidate for surgical procedures; and stable neurological status and pain medication (Box 1).
Major exclusion criteria were confounding pain in other areas (eg fibromyalgia, chronic headache); mechanical spine instability or significant cervical stenosis; active disruptive psychological or psychiatric disorder or other known condition significant enough to impact perception of pain (Box 2).
 |
Box 1 Inclusion Criteria |
 |
Box 2 Exclusion Criteria |
Procedures
Enrolled subjects who met all of the inclusion criteria and none of the exclusion criteria underwent a trial stimulation with 10 kHz SCS (Senza System, Nevro Corp., Redwood City, CA, USA). Two octopolar leads (contact length: 3 mm; inter-electrode distance: 5 mm; lead materials: electrodes: Pt-Ir, platinum-iridium) were placed in the epidural space spanning C2–C7 cervical spine (entry from T2–T8) along the radiological/anatomical midline of the cervical spine to deliver the therapy (Figure 1). For selecting the optimal stimulation parameters and location during the trial, a simple bipole sweep was performed rostrocaudally along the lead. Starting at the most rostral (distal) pair of contacts, bipole stimulation at 10 kHz and 30 µs was applied. Perception threshold testing was performed up to 5.0 mA. Initial and maximum amplitudes were developed over time as the stimulation thresholds were unknown at the start of the study. Amplitude was initially set at 0.6 or 0.9 mA and increased up to 2.1 or 2.5. If the subject did not achieve sufficient pain relief, amplitude was increased. If the amplitude reached the sensation threshold or 2.5 mA and the bipole location did not provide sufficient pain relief, the next set of bipoles were tested until the subject reported at least 40% pain relief or all possible bipoles had been tested. Subjects who experienced at least 40% reduction in their upper extremity pain during the trial compared to baseline were eligible for permanent device implantation with 10 kHz SCS (Senza System, Nevro Corp.). Lower pain relief (40%) was allowed during the trial primarily because the duration of the trial in many cases was expected to be not enough to fully optimize the therapy. IMPAACT guidelines suggest that 30% pain relief is clinically meaningful,17 so 40% cutoff was chosen during the trial only, as a reasonable screening criterion. However, ≥50% pain relief was required to be considered as a responder for therapy at follow-up assessment.
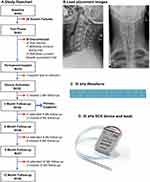 |
Figure 1 Study design; (A) study flowchart; (B) lead placement; (C) 10 kHz Waveform; (D) 10 kHz SCS device and leads. |
At the end of the trial, leads were removed, and subjects did not receive further stimulation until permanent implant of the SCS device. For the permanent implant, two leads were placed anatomically at approximately the same vertebral level as in the trial, anchored and then connected to an implantable pulse generator (IPG) placed in the subject’s flank. Stimulation was delivered with a fixed waveform at 10 kHz frequency, 30 μs pulse width, and amplitudes adjusted to maximize the subject’s pain relief, typically 0.3–1.2 mA. Choice of leads, contacts and vertebral level has been described previously.15 Briefly, the majority of the subjects had staggered octopolar leads placed midline in the cervical epidural space with the most cephalad lead at top of C2 and second lead at mid-C2 vertebrae. A single bipole over the C3–C4 disc was identified as the most effective “sweet spot” in most subjects.
Assessments were performed at one, three, six, and 12 months after permanent implant through regular follow-up visits. Study protocol allowed programming adjustments throughout the follow-up period. As described previously, programming was usually done in a cephalad to caudad bipole search pattern starting at the tip of the most cephalad lead.15 This continued caudally, crossing to the second lead as needed until a positive response was obtained. After achieving a positive response in pain reduction, effort was made to get optimal relief by altering (increasing or decreasing) the amplitude. Before moving to the next amplitude or new bipole, a typical wait time of eight hours was allowed.15 Median time to reach ≥50% pain relief was three days during the trial and five days during the permanent implant phase.15 During the study, 10 subjects with a permanently implanted device made 20 unscheduled visits for reprogramming and the median of the number of programming sessions in the study was two (max, 4; min, 0).
Intent-to-Treat (ITT) and per Protocol (PP) Analysis Populations
The ITT population was defined as all subjects who were intended for a trial stimulation with 10 kHz SCS (43 subjects). PP population was defined as those ITT subjects who received an IPG implant (after completing a successful screening trial), had their device activated, and completed at least three months of follow-up (32 subjects). Safety results are presented for all ITT subjects, while efficacy results are reported for PP subjects, which closely reflects clinical practice.
Data Collection and Statistics
Data were collected by independent clinic personnel from the study subjects and recorded in case report forms (CRFs) during prespecified follow-up assessments. The collected data was monitored and transferred into data listings using SAS 9.4 program and then into Excel™ spreadsheets by the sponsor’s team according to ICH-GCP, ISO14155 and 21 CFR 11 guidelines. Researchers from the sponsor institution were also responsible for the data analysis and presentation. Considering the study sample size (Supplementary Digital Content. Methods 1) and the fact that data did not always have a normal distribution (determined by goodness of fit test using Excel), descriptive analysis of continuous variables included median and lower-higher quartiles (Q1–Q3). Categorical variables were reported as counts and percentages. All the outcomes (Supplementary Digital Content. Methods 2) were analyzed longitudinally and missing data was estimated using “last observation carried forward” (LOCF) approach.18 Rationale for choosing LOCF approach is discussed in Supplementary Digital Content. Methods 3. All the statistical analysis was performed using Excel. Two-tailed paired t-test was used for comparing two groups and a p-value <0.05 was considered as significant.
Results
Study Population
Flow of subjects in the study is detailed in Supplementary Digital Content. Results 1. Briefly, out of 43 trial subjects, 38 (88.3%) had ≥40% relief in UEP (Figure 1). Of the 38 subjects who were eligible to receive permanent implant, five withdrew consent despite successful trial due to reasons including denial of insurance coverage. The remaining 33 subjects received a permanent implant and one had a device explanted before activation due to infection. Among the 32 PP subjects with upper limb pain, 24 (75.0%) who also had concomitant neck pain (baseline VAS score of ≥5.0 cm) were included in the neck pain subset and 27 (84.4%) who also had concomitant shoulder pain (baseline VAS score of ≥5 cm) were included in the shoulder pain subset.
Demographics
Baseline demographics and clinical characteristics of the PP population are shown in Table 1. Briefly, median age of the subjects at the time of enrollment was 47.0 years (range: 27.0–70.0), 65.6% were female and the median time since diagnosis was 9.6 years (range: 1.0–30.0). At baseline, median pain VAS score was 8.0 cm for upper limbs, 8.8 cm for neck, and 8.3 cm for shoulder. Opioids were used by 96.9% of subjects.
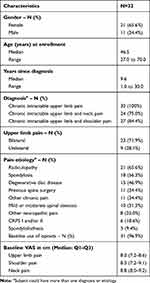 |
Table 1 Baseline Demographics and Clinical Characteristics for PP Subjects |
Safety
For the ITT population, there were no stimulation-related neurological deficits reported. There were no paresthesias or uncomfortable changes in stimulation related to changes in posture during the study. Neurological assessments of 30 subjects who completed the 12-month visit showed “no change” in neurological function in 29 subjects (96.7%) and “improvement” in neurological function in 1 subject (3.3%) compared to baseline.
There were eight study-related adverse events (AEs). Six procedure-related AEs occurring in four subjects included hematoma, headache, implant site infection, medical device site hemorrhage, musculoskeletal pain, and pain in extremity (one each). All the procedure-related AEs except headache occurred during the permanent implant phase. All but one AE resolved without any sequalae by study completion. The ongoing AE was mild procedure-related (as judged by the investigator) musculoskeletal pain in the right shoulder, which was treated conservatively using Diclofenac Sodium (Voltaren) 1% transdermal gel, PRN. This subject decided to continue the therapy and declined explant. Two AEs categorized as possibly related to stimulation/therapy occurring in two subjects included headache and unilateral pain in the extremity, both resolved with reprogramming (one each). There were two procedure-related serious adverse events (SAEs) occurring in one subject, which occurred after permanent implant, a hematoma at the site of surgery and an implant site infection, which resulted in explant of the device. Both were resolved without sequelae following aspiration of the wound and prophylactic antibiotic treatment.
Pain Relief
Baseline median VAS scores of 8.0, 8.8, and 8.3 cm for upper limb, neck, and shoulder pain, respectively, were significantly reduced to 1.0, 1.3, and 1.2 cm at the three-month assessment (p=7.2×10−15, 4.6×10−9, 1.6×10−11 respectively compared to baseline). At 12 months, median VAS scores were significantly reduced to 1.2, 1.2, and 1.4 cm for upper limb, neck, and shoulder pain, respectively (Figure 2A; p=1.4×10−15, 6.8×10−10, 4.2×10−11 respectively compared to baseline). Pain relief in individual subjects for upper limb, neck, and shoulder at 12 months compared to baseline is reported in Figure 2B, C, and D, respectively. Median percentage pain relief at three months compared to baseline was 88.0% for upper limb, 87.5% for neck and 87.6% for shoulder. Pain reductions were maintained through follow-ups and median pain reduction at 12 months compared to baseline was 86.2% for upper limb, 85.7% for neck and 86.3% for shoulder.
Responder Rates
In the PP population, responder rate at three-months was 81.3% (N=26/32), 77.8% (N=21/27) and 70.8% (N=17/24) for upper limb, shoulder and neck pain, respectively, which sustained through the 12-month follow-up period (Figure 2E).
Remitter Rates
Subjects with VAS scores ≤3 cm for six months at the time of follow-up assessments were defined as remitters.19 Remitter rate in PP population at 12 months was 78.1% (N=25/32), 77.8% (N=21/27) and 62.5% (N=15/24) for upper limb, shoulder and neck pain respectively (Figure 2F).
Short Form McGill Pain Questionnaire
Ten kilohertz SCS therapy resulted in significant improvement (p=2.1×10−7, p=1.4×10−8, p=8.4×10−7, p=1.1×10−6, p=8.6×10−9) in all components of SF-MPQ scores including “continuous pain”, “intermittent pain”, “neuropathic pain”, ‘affective descriptors’ and “total score” at three months, which further improved at 12 months (Figure 3).
 |
Figure 3 Reduction in SF-MPQ scores with 10 kHz SCS; Data shown includes median (Q1–Q3) at indicated assessment times. |
Improvement in Disability and Quality of Life
Compared to baseline, pain disability index (PDI) score significantly improved (p=1.4×10−7) by 32.0 points (3.4× minimum clinically important difference, MCID) at three months. Similarly, disabilities of the arm, shoulder and hand (QuickDASH) score significantly improved (p=1.5×10−8) by 40.9 points and global assessment of functioning (GAF) score significantly improved (p=1.2×10−6) by 20.0 points at three months compared to baseline. At 12-month endpoint, PDI score improved by 30.5 points, Quick-DASH by 36.4 points, and GAF by 19.5 points (Figure 4A–C). The 12-item Short Form Health Survey (SF-12) PCS subscale scores significantly improved (p=2.7×10−6) by 12.3 points and SF-12 MCS subscale improved significantly (p=0.004) by 6.8 points at 12-month endpoint assessment (Figure 4D).
At three months, subjects reporting global impression of change (GIC)s “a great deal better”, “better”, or “moderately better” were 75.0% (N=24/32), which was sustained at 12-month assessment (Figure 5A and B). Similarly, clinicians reporting GIC as “a great deal better”, “better”, or “moderately better” were 71.9% (N=23/32) at three months, which increased to 78.1% (N=25/32) at the 12-month endpoint assessment (Figure 5C and D).
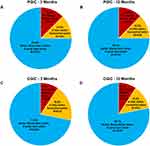 |
Figure 5 Patient and physician global impression of change with 10 kHz SCS; (A–B) PGIC at three months and 12 months, (C–D) CGIC at three months and 12 months. |
Sleep
Ten kilohertz SCS treatment reduced scores for all the three questions of the three-item pain and sleep questionnaire (PSQ-3), including how often subjects have trouble falling asleep due to pain, how often they are awakened due to pain in the night, and how often they are awakened due to pain in the morning (Supplementary Digital Content. Table S1). Global PSQ-3 score was significantly reduced (p=7.8×10−7) from 25.1 at baseline to 8.6 at three months (16.5 reduction). The impact of pain on sleep continued to decrease over the study period, with a global score of 5.5 at 12 months (Figure 6A).
Satisfaction
At three months, 75.0% (N=24/32) of the subjects reported being “satisfied” or “very satisfied” with 10 kHz SCS, which increased to 84.4% (N=27/32) at 12 months (Figure 6B).
Medication Usage
At baseline, 31 subjects in the PP (96.9%) were taking an opioid medication (Table 1) and dose information was available from 24 (75.0%) subjects. At three months, three subjects eliminated opioids, seven subjects decreased their opioid dose, 14 subjects had no change in opioid use and four subjects increased their opioid dose. At 12 months, three subjects eliminated opioids, nine subjects decreased their opioid dose, 11 subjects had no change in opioid use and five subjects increased their opioid dose. One subject who was not taking opioids at baseline, was taking opioids at 15 morphine milligram equivalents (MME) dose at 12 months. Altogether, in subjects who increased their opioid dose at 12 months, the increase ranged between 5 and 30 MME, with an average increase of 18 MME compared to baseline. Interestingly, subjects who increased their opioids to over 60 MME at 12 months (N=2) were nonresponders (≥50% reduction) and did not even have clinically relevant pain reduction (≥30% reduction). Out of the remaining three subjects, one subject increased opioids by 5 MME after six-month follow-up, one increased by 25 MME and the third subject, who was not taking opioids at baseline increased opioids by 60 MME at three-month follow-up and then decreased the dose to 15 MME at six- and 12-month follow-up. All these three subjects were responders at 12-month follow-up.
Overall, the difference in mean opioid dose between baseline (81.8 MME) and three months (77.2 MME) was not statistically significant (p=0.49). However, the difference reached statistical significance at 12 months (61.0 MME, p=0.04).
Discussion
People with moderate to severe UEP have difficulties in maintaining their lifestyle, exercise, sleep, performing household chores and social activities.20 This study suggests 10 kHz SCS provides safe, substantial, and sustained pain relief in subjects with chronic UEP, along with clinically meaningful improvement in disability, functioning, and sleep.
A single case of possible, therapy-related extremity pain was reported by an investigator in this study. This was mild and transient, resolving after reprogramming and is consistent with recent prospective studies.15,16 Subjects were managed with reprogramming in all cases and did not require explant of the device. Similarly, AEs were without any neurological symptom changes and all device-related AEs were manageable (resolved after reprogramming). More importantly, despite positioning leads at C2–C7 vertebral level, there were no cases of lead migration that required lead repositioning in the current study or in the previous prospective studies.15,19 Previous retrospective studies using 10 kHz SCS for upper limb and/or neck pain also reported no cases or low rates of lead migration.21–23 Lead migration is among the most concerning complications reported in prospective studies of cervical lead placement for management of pain.7,24–27 A systematic literature review of outcomes in patients with cervical SCS documented the rates for hardware malfunction (17.8%), lead migration (13.9%), lead fracture (6.7%), pain over implant site (4.4%) and infection (2.2%).28 The AE rates reported in this study and in the previous studies evaluating 10 kHz SCS for upper limb and neck pain treatment compare favorably with the published literature and further support the safety of this therapy. Loss of efficacy and uncomfortable paresthesia are two common manifestations of lead migration and require revision surgery and/or explant of the device. However, because 10 kHz SCS is paresthesia-free, most cases of lead migration manifesting as decreased efficacy can be managed through reprogramming and very few cases require revision surgery or explant.21 Indeed, the rate of explant due to loss of efficacy is comparatively low with 10 kHz SCS29,30 and only one out of over 200 patients from six prospective and retrospective studies (including the current study) required an explant for loss of efficacy.15,16,21–23
Evidence for use of SCS in UEP is available from prospective studies testing traditional SCS and dorsal nerve root stimulation (DNRS) for upper limb and/or neck pain.26–28 Pain relief, responder rate, and remitter rates observed in the current study are substantial, sustained, and comparable to 10 kHz SCS studies for treating chronic back and/or leg pain, such as randomized controlled trials, long-term retrospective evaluations, real-world data10,26–29,31–33 and an investigational 10 kHz SCS study for treating upper limb and neck pain.15 Interestingly, outcomes improved over time and responses at 12 months were better than three months. While the improvement in efficacy at later time points could have been due to programming changes, data from a recently published upper limb and neck pain study showed that the number of programming sessions in fact decreased from three months to 12 months.15
Consistent with previous findings in patients with back and leg pain, results at three and 12 months revealed that 10 kHz SCS improved all components of the SF-MPQ including affective descriptors, disability scores (PDI and QuickDASH), and quality of life scales such as SF-12, GIC and satisfaction. Results from the current study indicate that 10 kHz SCS helps subjects with UEP with continuous improvement in their sleep, reaching an approximately 20-point improvement in PSQ-3 scores at 12-month endpoint. It is an interesting finding considering that about 40% of subjects either reduced or eliminated and 20% subjects increased their opioid dose at 12-months. As opioids are known to interfere with sleep, further investigation is needed to understand whether improvement in sleep was due to decrease in opioid usage or because of direct effects of 10 kHz SCS on sleep. Current findings on PSQ-3 scores and changes in opioid medication are similar to results from previously reported 10 kHz SCS studies in chronic back and leg pain and retrospective analysis of real-world data.10,11,29,33,34
Durable and differentiated outcomes seen with 10 kHz SCS treatment may be attributed to its unique mechanism of action.35–42 Using in vivo and ex vivo electrophysiological approaches, Lee et al reported that unlike low-intensity (sub-sensory threshold) 1 kHz and 5 kHz SCS, 10 kHz SCS selectively activated inhibitory interneurons in the spinal dorsal horn (DH) and proposed that low-intensity 10 kHz SCS provided paresthesia-free pain relief possibly by activating the inhibitory interneurons without activating dorsal column fibers.35 Researchers from Chang Gung Memorial Hospital, Taiwan used spared nerve injury (SNI)-induced neuropathic pain model in rats and showed that 10 kHz SCS significantly reduced SNI-induced mechanical hyperalgesia compared to sham stimulation group.36 The study also showed significant reduction in activation of inflammatory kinases ERK1, ERK2, JNK1 and p38 in the dorsal root ganglia and the spinal DH in 10 kHz SCS group compared to sham stimulation group. Recently, the differences in mechanism of action between 10 kHz SCS and 40–60 Hz paresthesia-based SCS was studied using 10-channel electroencephalogram (EEG) measurements in patients.40 Authors of the study recorded EEG changes in response to stimulation ON and OFF in chronic pain patients (four women, five men) during SCS surgery and demonstrated a unique shift in peak frequency from theta to alpha rhythms in 10 kHz SCS group. Authors further showed a positive correlation between improvement in Oswestry disability index (ODI) scores and alpha/theta peak power ratio in frontal and somatosensory regions. Another study used resting stage functional magnetic resonance imaging (fMRI) to study brain connectome patterns in FBSS patients implanted with 10 kHz SCS device and demonstrated increased connectivity between the anterior insula (affective salience network) and regions of the frontoparietal network and the central executive network.41 Authors of the fMRI study followed-up with another study to test structural volumetric changes in chosen regions of interest of brain in patients with 10 kHz SCS implants and documented significant decreases in left and right hippocampus volume over time, which correlated with reduction in back pain intensity.42 Taken together, the findings demonstrate 10 kHz SCS treatment is associated with unique objective physiological responses and sustained pain relief.
Rationale for Choosing Lower Pain Relief Cutoff
A lower pain relief cutoff (≥40%) during the trial phase was chosen in the study over conventional cutoff (≥50%) mainly because the duration of the trial was typically less than seven days. We anticipated that, in some subjects, we may not be able to program the optimal stimulation parameters to get the ≥50% pain relief during the trial period. As the main objective of the study was to understand the efficacy of 10 kHz SCS over 12 months, we used a comparatively lower cutoff, which was higher than the clinically meaningful change (≥30% reduction).17 Two out of 33 subjects who received a permanent implant had >40% and <50% pain relief during the trial. One subject who had reported less than standard ≥50% pain relief during the trial reported sustained pain relief after permanent implant and improvements in other outcomes. The second subject achieved standard pain relief after one month of treatment with 10 kHz SCS but reported loss of pain relief at later time points. The study does not recommend using lower than 50% pain relief as a cutoff during the trial period normal clinical practice and does not propose that using a longer trial period (>7 days) is required for best outcomes.
Additional discussion on rationale for inclusion and exclusion criteria and the rationale for using subjects at follow-up visits for the efficacy analysis are presented in the Supplementary Digital Content. Discussion 1 and 2, respectively.
Limitations
This study was a pragmatic, postmarket, observational design intended to provide information on safety and efficacy to clinicians for counseling patients on the use of 10 kHz SCS in the treatment of refractory upper extremity pain. As is the case in all such studies, without an appropriate randomized comparator arm there is an increased potential for various biases and confounding treatment influences to affect the results. Thus, any clinical decision making should carefully include consideration of these limitations. In addition, the findings are not universally generalizable to all patients with UEP and the demographics and various etiologies reported herein warrant careful inspection. Patient selection and treatment followed commercial standard of care at the individual sites and hence minimal selection bias, consistent with “real-world” practice was expected. Lack of a control group was partly addressed by comparing our findings with published results on the efficacy of 10 kHz SCS from previous randomized controlled trials or real-world retrospective review.29,31,32 The findings from the current study encourages additional studies to address more scientific objectives.
Conclusion
To summarize, this study provides evidence that 10 kHz SCS produces sustained and substantial pain relief in subjects with chronic, intractable pain of the upper extremities. Moreover, clinically meaningful improvement in functioning and sleep, and decrease in disability were observed. Further studies with appropriate design and sample size could confirm the efficacy of 10 kHz SCS for UEP.
Data Sharing Statement
All the relevant de-identified data in this study has been included in the manuscript as part of the results. Authors cannot share the raw data from the patients due to privacy concerns.
Acknowledgments
We thank Ms Ami Shah, clinical consultant at Nevro for assistance with data analysis and Dr Madhuri Bhandaru for help with preparation of illustrations.
Funding
The study was sponsored by Nevro Corp.
Disclosure
Dr Kosek received research grants from Boston Scientific and Nevro Corp. Dr Rosen is a consultant to and received research grants from Flowonix, Saluda Medical, Biotronik, Medtronic, and Nevro. Dr Bromberg is a consultant and investor in Nevro and Mudjala. He also reports clinical educator/speakership from Medtronic, outside the submitted work. Dr Gulve is a consultant to Nevro Corp., Saluda Medical and received research grants from Boston Scientific, Abbott, Medtronic, and Mainstay Medical. Dr Esposito is a consultant to Nevro Corp., Abbott, Boston Scientific, Flowonix, and Vertiflex. Dr McRoberts is a consultant to Abbott. Dr Rotte is an employee of Nevro Corp. Mr Gliner was an employee of Nevro Corp. at the time the study was conducted and is now an independent consultant, Seattle, WA, USA. Dr Maneshi was an employee of Nevro Corp. at the time the study was conducted and is now affiliated with Abbott, Sunnyvale, CA, USA. Dr Subbaroyan was an employee of Nevro Corp. at the time the study was conducted and received stock options from Nevro Corp. He is now affiliated with GTX Medical, New York, NY, USA. The authors report no other conflicts of interest in this work.
References
1. Cote P, Cassidy JD, Carroll L. The Saskatchewan Health and Back Pain Survey. The prevalence of neck pain and related disability in Saskatchewan adults. Spine. 1998;23(15):1689–1698. doi:10.1097/00007632-199808010-00015
2. Makela M, Heliovaara M, Sievers K, Impivaara O, Knekt P, Aromaa A. Prevalence, determinants, and consequences of chronic neck pain in Finland. Am J Epidemiol. 1991;134(11):1356–1367. doi:10.1093/oxfordjournals.aje.a116038
3. North RB, Kidd DH, Petrucci L, Dorsi MJ. Spinal cord stimulation electrode design: a prospective, randomized, controlled trial comparing percutaneous with laminectomy electrodes: part II-clinical outcomes. Neurosurgery. 2005;57(5):990–996.
4. North RB, Kidd DH, Olin J, Sieracki JM, Boulay M. Spinal cord stimulation with interleaved pulses: a randomized, controlled trial. Neuromodulation. 2007;10(4):349–357.
5. Foletti A, Durrer A, Buchser E. Neurostimulation technology for the treatment of chronic pain: a focus on spinal cord stimulation. Expert Rev Med Devices. 2007;4(2):201–214.
6. Oakley JC. Spinal Cord Stimulation in Axial Low Back Pain: solving the Dilemma. Pain Medicine. 2006;7:S58–S63.
7. Chivukula S, Tempel ZJ, Weiner GM, et al. Cervical and cervicomedullary spinal cord stimulation for chronic pain: efficacy and outcomes. Clin Neurol Neurosurg. 2014;127:33–41.
8. Penn DL, Zussman BM, Wu C, Sharan AD. Anterograde revision of cervical spinal cord stimulator paddle electrode: a case report. Neuromodulation. 2012;15(6):581–584.
9. Vallejo R, Kramer J, Benyamin R. Neuromodulation of the cervical spinal cord in the treatment of chronic intractable neck and upper extremity pain: a case series and review of the literature. Pain Physician. 2007;10(2):305–311.
10. Al-Kaisy A, Van Buyten J-P, Smet I, Palmisani S, Pang D, Smith T. Sustained Effectiveness of 10 kHz High-Frequency Spinal Cord Stimulation for Patients with Chronic, Low Back Pain: 24-Month Results of a Prospective Multicenter Study. Pain Medicine. 2014;15(3):347–354. doi:10.1111/pme.12294
11. Al-Kaisy A, Palmisani S, Smith TE, et al. Long-Term Improvements in Chronic Axial Low Back Pain Patients Without Previous Spinal Surgery: A Cohort Analysis of 10-kHz High-Frequency Spinal Cord Stimulation over 36 Months. Pain Med. 2018;19(6):1219–1226. doi:10.1093/pm/pnx237
12. Gill JS, Asgerally A, Simopoulos TT. High-Frequency Spinal Cord Stimulation at 10 kHz for the Treatment of Complex Regional Pain Syndrome: A Case Series of Patients With or Without Previous Spinal Cord Stimulator Implantation. Pain Pract. 2019;19(3):289–294. doi:10.1111/papr.12739
13. De Carolis G, Paroli M, Tollapi L, et al. Paresthesia-Independence: an Assessment of Technical Factors Related to 10 kHz Paresthesia-Free Spinal Cord Stimulation. Pain Physician. 2017;20(4):331–341.
14. Al-Kaisy A, Palmisani S, Smith T, Harris S, Pang D. The Use of 10-Kilohertz Spinal Cord Stimulation in a Cohort of Patients With Chronic Neuropathic Limb Pain Refractory to Medical Management. Neuromodulation. 2015;18(1):18–23. doi:10.1111/ner.12237
15. Amirdelfan K, Vallejo R, Benyamin R, et al. High-Frequency Spinal Cord Stimulation at 10 kHz for the Treatment of Combined Neck and Arm Pain: results From a Prospective Multicenter Study. Neurosurgery. 2020;87(2):176–185. doi:10.1093/neuros/nyz495
16. Verrills P, Salmon J, Russo M, Gliner B, Barnard A, Caraway D. 10 kHz spinal cord stimulation for chronic upper limb and neck pain: australian experience. Eur Spine J. 2020. doi:10.1007/s00586-020-06480-x
17. Dworkin RH, Turk DC, Wyrwich KW, et al. Interpreting the clinical importance of treatment outcomes in chronic pain clinical trials: IMMPACT recommendations. J Pain. 2008;9(2):105–121. doi:10.1016/j.jpain.2007.09.005
18. Dziura JD, Post LA, Zhao Q, Fu Z, Peduzzi P. Strategies for dealing with missing data in clinical trials: from design to analysis. Yale J Biol Med. 2013;86(3):343–358.
19. Amirdelfan K, Gliner BE, Kapural L, et al. A proposed definition of remission from chronic pain, based on retrospective evaluation of 24-month outcomes with spinal cord stimulation. Postgrad Med. 2019;131(4):278–286. doi:10.1080/00325481.2019.1592401
20. Gummesson C, Atroshi I, Ekdahl C, Johnsson R, Ornstein E. Chronic upper extremity pain and co-occurring symptoms in a general population. Arthritis Rheum. 2003;49(5):697–702. doi:10.1002/art.11386
21. El Majdoub F, Neudorfer C, Richter R, Schieferdecker S, Maarouf M. 10 kHz cervical SCS for chronic neck and upper limb pain: 12 months’ results. Ann Clin Transl Neurol. 2019;6(11):2223–2229. doi:10.1002/acn3.50915
22. Sayed D, Salmon J, Khan T, et al. <p>Retrospective Analysis of Real-World Outcomes of 10 kHz SCS in Patients with Upper Limb and Neck Pain. J Pain Res. 2020;Volume 13(13):1441–1448. doi:10.2147/JPR.S257071
23. Russo M, Verrills P, Mitchell B, Salmon J, Barnard A, Santarelli D. High Frequency Spinal Cord Stimulation at 10 kHz for the Treatment of Chronic Pain: 6-Month Australian Clinical Experience. Pain Physician. 2016;19(4):267–280.
24. Chan AK, Winkler EA, Jacques L. Rate of perioperative neurological complications after surgery for cervical spinal cord stimulation. J Neurosurg Spine. 2016;25(1):31–38. doi:10.3171/2015.10.SPINE15670
25. Forouzanfar T, Kemler MA, Weber WE, Kessels AG, van Kleef M. Spinal cord stimulation in complex regional pain syndrome: cervical and lumbar devices are comparably effective. Br J Anaesth. 2004;92(3):348–353. doi:10.1093/bja/aeh072
26. Haider S, Owusu-Sarpong S, Peris Celda M, et al. A Single Center Prospective Observational Study of Outcomes With Tonic Cervical Spinal Cord Stimulation. Neuromodulation. 2017;20(3):263–268. doi:10.1111/ner.12483
27. Levine AB, Parrent AG, MacDougall KW. Cervical Spinal Cord and Dorsal Nerve Root Stimulation for Neuropathic Upper Limb Pain. Can J Neurol Sci. 2017;44(1):83–89. doi:10.1017/cjn.2016.294
28. Deer TR, Skaribas IM, Haider N, et al. Effectiveness of cervical spinal cord stimulation for the management of chronic pain. Neuromodulation. 2014;17(3):265–271. doi:10.1111/ner.12119
29. Stauss T, El Majdoub F, Sayed D, et al. A multicenter real-world review of 10 kHz SCS outcomes for treatment of chronic trunk and/or limb pain. Ann Clin Transl Neurol. 2019;6(3):496–507.
30. Al-Kaisy A, Royds J, Al-Kaisy O, et al. Explant rates of electrical neuromodulation devices in 1177 patients in a single center over an 11-year period. Reg Anesth Pain Med. 2020.
31. Kapural L, Yu C, Doust MW, et al. Novel 10-kHz High-frequency Therapy (HF10 Therapy) Is Superior to Traditional Low-frequency Spinal Cord Stimulation for the Treatment of Chronic Back and Leg PainThe SENZA-RCT Randomized Controlled Trial. Anesthesiology. 2015;123(4):851–860.
32. Kapural L, Yu C, Doust MW, et al. Comparison of 10-kHz High-Frequency and Traditional Low-Frequency Spinal Cord Stimulation for the Treatment of Chronic Back and Leg Pain: 24-Month Results From a Multicenter, Randomized, Controlled Pivotal Trial. Neurosurgery. 2016;79(5):667–677.
33. Amirdelfan K, Yu C, Doust MW, et al. Long-term quality of life improvement for chronic intractable back and leg pain patients using spinal cord stimulation: 12-month results from the SENZA-RCT. Qual Life Res. 2018;27(8):2035–2044.
34. Van Buyten JP, Al-Kaisy A, Smet I, Palmisani S, Smith T. High-frequency spinal cord stimulation for the treatment of chronic back pain patients: results of a prospective multicenter European clinical study. Neuromodulation. 2013;16(1):59–65.
35. Lee KY, Bae C, Lee D, et al. Low-intensity, Kilohertz Frequency Spinal Cord Stimulation Differently Affects Excitatory and Inhibitory Neurons in the Rodent Superficial Dorsal Horn. Neuroscience. 2020;428:132–139.
36. Liao WT, Tseng CC, Wu CH, Lin CR. Early high-frequency spinal cord stimulation treatment inhibited the activation of spinal mitogen-activated protein kinases and ameliorated spared nerve injury-induced neuropathic pain in rats. Neurosci Lett. 2020;721:134763.
37. Zannou AL, Khadka N, FallahRad M, Truong DQ, Kopell BH, Bikson M. Tissue Temperature Increases by a 10 kHz Spinal Cord Stimulation System: phantom and Bioheat Model. Neuromodulation. 2019;25.
38. Caraway DL, Bradley K. Response to: “Tissue Temperature Increases by a 10 kHz Spinal Cord Stimulation System: phantom and Bioheat Model”. Neuromodulation. 2019;22(8):986–987.
39. Khadka N, Bikson M. Response to the Letter to the Editor by Caraway et al. on “Tissue Temperature Increases by a 10 kHz Spinal Cord Stimulation System: phantom and Bioheat Model”. Neuromodulation. 2019;22(8):988.
40. Telkes L, Hancu M, Paniccioli S, et al. Differences in EEG patterns between tonic and high frequency spinal cord stimulation in chronic pain patients. Clin Neurophysiol. 2020;131(8):1731–1740.
41. De Groote S, De Jaeger M, Van Schuerbeek P, et al. Functional magnetic resonance imaging: cerebral function alterations in subthreshold and suprathreshold spinal cord stimulation. J Pain Res. 2018;11:2517–2526.
42. De Groote S, Goudman L, Linderoth B, et al. A Regions of Interest Voxel-Based Morphometry Study of the Human Brain During High-Frequency Spinal Cord Stimulation in Patients With Failed Back Surgery Syndrome. Pain Pract. 2020;1:457.
 © 2020 The Author(s). This work is published and licensed by Dove Medical Press Limited. The full terms of this license are available at https://www.dovepress.com/terms.php and incorporate the Creative Commons Attribution - Non Commercial (unported, v3.0) License.
By accessing the work you hereby accept the Terms. Non-commercial uses of the work are permitted without any further permission from Dove Medical Press Limited, provided the work is properly attributed. For permission for commercial use of this work, please see paragraphs 4.2 and 5 of our Terms.
© 2020 The Author(s). This work is published and licensed by Dove Medical Press Limited. The full terms of this license are available at https://www.dovepress.com/terms.php and incorporate the Creative Commons Attribution - Non Commercial (unported, v3.0) License.
By accessing the work you hereby accept the Terms. Non-commercial uses of the work are permitted without any further permission from Dove Medical Press Limited, provided the work is properly attributed. For permission for commercial use of this work, please see paragraphs 4.2 and 5 of our Terms.



