Back to Journals » Nature and Science of Sleep » Volume 14
Structural Model of Napping Motivation Among Chinese College Students Based on Self-Rating: Evidence from an Exploratory Factor Analysis
Authors Du J, Wang Y , Xu S, Huang Y, Zhang R, Xiao L, Xu J, Wang H, Su T, Tang Y
Received 16 November 2021
Accepted for publication 13 April 2022
Published 2 May 2022 Volume 2022:14 Pages 843—853
DOI https://doi.org/10.2147/NSS.S349013
Checked for plagiarism Yes
Review by Single anonymous peer review
Peer reviewer comments 3
Editor who approved publication: Prof. Dr. Ahmed BaHammam
Jing Du, Yajing Wang, Shuyu Xu, Yujia Huang, Ruike Zhang, Lei Xiao, Jingzhou Xu, Hao Wang, Tong Su, Yunxiang Tang
Department of Medical Psychology, Naval Medical University, Shanghai, People’s Republic of China
Correspondence: Tong Su; Yunxiang Tang, Department of Psychology, Naval Medical University, Shanghai, People’s Republic of China, Email [email protected]; [email protected]
Purpose: Previous epidemiological and psychological studies have assessed the effects of napping on individual performance and health. However, these studies did not distinguish between spontaneous and passive napping due to sleep disorders. Therefore, this study aimed to explore the potential motivation for napping among Chinese college students and to assess the relationship between different nap motivations and sleep.
Patients and Methods: This cross-sectional study was conducted at a university in Shanghai in March 2021 using convenience sampling. A total of 564 Chinese college students with self-reported napping habits participated in this study. Exploratory factor analysis (EFA) was employed to analyze 34 self-rated motivations for napping to derive a potential structural model of napping motivation. Correlation and multiple linear regression analyses were performed to determine the influence of nap motivation on sleep behavior.
Results: Chinese college students mainly take naps to reduce fatigue, usually in the form of frequent and long naps (6.25 ± 1.24 days; 64.62 ± 23.70 min). A structural model of nap motivation named the I-DREAM model was proposed, consisting of six factors: restorative, induced, mindful, appetitive, dysregulative, and exercise naps. There were also sex differences in nap motivation, as women preferred restorative naps and appetitive naps, while men preferred exercise naps (p < 0.01, p < 0.05). Furthermore, there was a significant correlation between nap motivation on nap duration, frequency and nighttime sleep quality (R2= 2.70– 18.9%).
Conclusion: The proposed I-DREAM model implies that there are population differences in napping motivation. Different motivations also have different relationships with napping patterns and nighttime sleep. In understanding the relationship between naps and health status, nap motivation may be an extremely important influencing factor.
Keywords: nap, sleep quality, Chinese college student, exploratory factor analysis
Introduction
The impermanent decline in alertness and performance during the afternoon, known as post-lunch dip, is thought to be the result of daytime sleepiness.1–3 The introduction of naps is a practical countermeasure to overcome daytime sleepiness, which has been reported to significantly influence alertness, cognitive performance, decision-making, and social interactions in humans.4–7 In fact, napping for 10–45 minutes after lunch has been verified to promote afternoon performance to varying degrees, including learning ability, memory, executive function, and vigilance.8–10
Despite all the benefits of naps, naps are not widely accepted as a form of sleep, and cultural norms vary widely.11 The afternoon propensity for sleep is recognized in North American and Northern European cultures, with approximately 41–74% of healthy American adults choosing to nap at least once a week.12–14 However, it is also viewed by some as a nuisance, with excessive napping leading to sleep inertia, which is associated with confusion, lethargy, and cognitive deficits; therefore, naps are often labelled as “afternoon blahs”.15,16 In addition, napping is associated with increased potential long-term health risks and lower quality of sleep at night.17–19 In fact, whether napping is good or bad for individuals must take into account factors such as nap frequency, nap duration and nap motivation, as they may lead to different nap patterns and thus to different nap consequences.20,21
The motivations for napping vary between individuals, which can lead to different napping patterns and play a key role in the post-napping effect.21 Several previous studies have attempted to classify nappers in various ways, such as napping frequency, daytime sleepiness, or sleep duration.22–24 The most recognized classification of nappers separates individuals into one of three categories: restorative nappers (replenishing the length of nighttime sleep); prophylactic nappers (preventing insufficient nighttime sleep); and appetitive nappers (enjoyment and relaxation from napping).20 In general, people who nap for voluntary purposes, such as appetitive nappers, have a higher possibility of gaining benefits from napping.25 In contrast, restorative nappers, often have chronic comorbidities or sleep disorders, prompting them to nap unconsciously and frequently. In fact, a study by Leng et al, found that voluntary napping and napping as underlying pathological outcomes have different health effects.18
Previous studies have tended to categorize nappers by asking about their motivations, without a standardized instrument, and with a one-sided view of napper classification. Recently, Duggan et al performed the first statistical quantification of napping motivation and proposed a DREAM (dysregulative, restorative, emotional, appetitive, and mindful) model to classify nappers.21 Further, Duggan et al listed 29 motivations for napping and asked participants to determine whether each motivation for napping was consistent with their own situation by “yes” or “no”. The model is shown in Figure 1. However, the polarization of dichotomous variables may have obscured some non-dominant nap motivations. This is because in practice, motivation for a behavior is assessed more often using indicators of continuity, such as propensity.
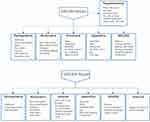 |
Figure 1 Comparison of items in the DREAM model and the I-DREAM model. |
It is also unclear whether the DREAM model is applicable to the Chinese college student population. In China, it is widely accepted that an afternoon nap is a healthy activity that supplements nighttime sleep, and approximately 88% of people usually take a nap.17,26 Among them, college students in China have the highest nap prevalence among various populations, thus understanding the underlying motivations for napping among those who nap more frequently is warranted.4,27 Furthermore, whether this frequent afternoon sleep is just a habit, a sign of laziness, or has some biological significance for Chinese college students, or what they hope to gain from it, remains unclear.28,29
Therefore, this study was designed to create a new tool to explore the nap motivation of Chinese college students. By analyzing the relationship between nap motivation, nap duration, nap frequency, and sleep quality, we can begin to understand the nap patterns corresponding to different nap motivations and their impact on sleep quality.
Materials and Methods
Participants
This cross-sectional study was conducted at a military university in Shanghai in March 2021 using convenience sampling. The survey began at the beginning of the spring semester and was designed to exclude course and exam stress. Consent and survey responses were anonymously recorded via an online link (https://www.wjx.cn/). The survey took approximately 15 min to complete. In total, 564 healthy college students completed the questionnaire. However, 64 students were excluded from the subsequent analysis. The specific reasons for exclusion included: (a) unclear age (N=5); (b) not filling out the questionnaire according to the requirements (N=9); (c) abnormal sleep efficiency, which was greater than or equal to 150% in the sleep efficiency from the Pittsburgh Sleep Quality Index (PSQI) (N=3); (d) abnormal nap duration, which claimed to have napping habits, filled in negative or zero nap duration (N=8); (e) individuals with abnormal motivation scores of naps, the proportion of the same number of nap motivation scores reached 85% (N=39). The final sample size was 500, resulting in an effective response rate of 88.65% (M age = 20.11, SD=1.13, range[16,24]; 50.8% women). The research was carried out in accordance with the Helsinki Declaration as revised in 1989, and was approved by the Ethics Committee of Naval Medical University. The participants provided electronic informed consent and were financially compensated for their time.
Study Measures
Demographic Characteristics
A self-designed demographic characteristics questionnaire was used to investigate age, sex, and grade. Grades were divided into lower grades (1–2 years in school) and upper grades (3 years in school or greater). In addition, exercise habits and past napping habits were investigated and categorized as yes (≥3 per week) or no (< 3 per week).
Nap
Napping behavior was assessed using a self-rating questionnaire, and all questions required the participants to answer based on their self-situation in the past month. Participants were asked, “When did you start your nap” (not bedtime) and “When did you wake up from your nap” and the difference in time was taken as the nap duration. It should be noted that naps at times other than after lunch, such as napping in class, were not included in the nap duration for this study. In addition, they were asked, “How many days a week do you nap” as the frequency of napping. Typically, when the number of naps per week is three or more, the individual is considered a habitual napper; otherwise, they are considered a non-habitual napper.20 Finally, participants rated their level of fatigue before and after napping using a 5-point scale (0=extremely alert, 2=neither alert nor sleepy, 4=extremely sleepy).
Nap Motivation
Duggan et al proposed the DREAM model of nap motivation, which contains 29 nap motivations distributed across five dimensions: dysregulative, restorative, emotional, appetitive, and mindful.21 We added five nap motivations to the DREAM model by searching through the previous literature related to napping among Chinese college students and conducting relevant pre-interviews with the intended survey group to compose a list of 34 nap motivation items. The original and added entries for the nap motive are shown in Figure 1. Participants were asked to read each nap motivation in detail and select a number from 0–100, representing their propensity to nap because of that motivation, which was called the endorsement rate. A higher score indicates a higher propensity. Considering that participants’ motivation for napping was not unique, nap motivation was scored independently.
Sleep Quality
Sleep quality was assessed using the PSQI, a self-administered scale that includes 19 items consisting of the following seven dimensions: subjective sleep quality, sleep latency, sleep duration, sleep efficiency, sleep disturbances, use of sleep medications, and daytime dysfunction.30 Each dimension is scored from 0–3, and the total PSQI score ranges from 0–21. A higher score indicates poorer sleep. The PSQI had good internal consistency among Chinese college students (Cronbach’s α=0.84), and the retest reliability of the total score was 0.81.31,32
Statistical Analysis
Descriptive statistics were calculated first, and visual examinations for potential outliers were prioritized before statistical processing. Categorical data are presented as numbers and percentages (eg, sex, major, grade, exercise habits, napping habits, pre-nap fatigue, and 30 min post-nap fatigue), and continuous data are presented as mean and standard deviations (eg, age, nap duration, nap frequency, and PSQI score). T-tests were applied to compare the differences in nap duration, frequency, and sleep quality among all classification variables. The mean score for each nap motivation was calculated as the endorsement rate for that population on that motivation, with the frequency distribution listed in Table 1.
 |
Table 1 Exploratory Factor Analysis of Nap Motivation Structure |
To probe the potential structure of nap motivation, exploratory factor analysis (EFA) was employed to analyze the motivation score data for naps. Kaiser-Meyer-Olkin (KMO) and Bartlett’s test of sphericity (Bartlett’s) were applied to evaluate the applicability of EFA for 34 items.33 The KMO should be greater than 0.60 and is considered ideal if greater than 0.90.34 The data was required to be spherical, Bartlett’s p<0.05. Because of the possible correlation between nap motives, we used promax oblique rotation (ie, individuals may endorse multiple nap motives,21 and these motives may be interrelated), which is advantageous for interrelated items. Next, we selected the number of retained factors using the compound approach: 1) eigenvalues >1; and 2) visual inspection of Cattell’s scree plot. After checking the factor loadings and commonality, three types of items were excluded: 1) if the commonality was less than 0.3; 2) if the absolute value of factor loading was less than 0.4; and 3) if the difference in the absolute value of the load of multiple factors was less than 0.3. When an item was removed, the analysis was repeated until none of the items met the above exclusion criteria.
Reliability and validity tests were conducted for the remaining entries, and the results indicated that the questionnaire had high internal consistency (Cronbach’s α=0.88) and acceptable test–retest reliability (r=0.57). The KMO values were satisfactory (KMO=0.88, Bartlett’s p<0.05) with significant sphericity test results.
Nap preference scores were calculated for each participant by summing the item scores assigned to each factor, which indicated the participants’ internal drivers of napping. A t-test was used to determine whether nap motivation differed by sex and past habits. Spearman correlation analysis was used to determine the relationship between the nap preference scores to evaluate whether individuals napped for multiple motivations. Pearson correlation analysis was used to assess the relationship between nap preference scores and age, pre-nap fatigue, 30 min post-nap fatigue, and sleep variables. Finally, to further determine the effect of nap motivation on sleep variables, multiple linear regressions were applied to assess the relationship between nap preference scores and sleep variables, with nap duration, nap frequency, and PSQI score as the dependent variables and nap preference as the independent variable.21
A two-tailed p<0.05 was considered statistically significant. All statistical analyses were performed using SPSS 23.0 (IBM Corp., Armonk, N.Y., USA) for Windows.
Results
Descriptive Statistics
Most participants tended to take naps, with 97.8% reported napping more than three times a week (N=489), 63.4% reported napping every day (N=317), and only 0.004% reported napping 0 times per week (N=2). On average, participants napped almost every day (6.25±1.24 day), with each nap lasting approximately an hour (64.62±23.70 min). Participants reported that napping reduced their subjective feelings of fatigue (pre-nap fatigue M=2.59 vs 30 min post-nap fatigue M=1.47). Compared to men, women had shorter and more frequent naps, poorer sleep quality, higher pre-nap fatigue, and higher 30-minute post-nap fatigue. Participants in the upper grades had greater 30-minute post-nap fatigue and poorer sleep quality. Non-exercisers also showed poorer nighttime sleep, higher pre-nap fatigue, and greater 30-minute post-nap fatigue, and those who had napped in the past reported more frequent naps (see Table 2).
 |
Table 2 Statistical Description of Sleep and Nap |
Participants showed variability in the endorsement rate for nap motivation. Most participants reported that napping reduced their subjective fatigue, so the most recognized motivations for napping were: “I want to reduce fatigue and regain my energy” (M=72.54), followed by, “I thought it would make me feel good, I think naps are beneficial” (M=70.37), and “I have the habit of taking a nap” (M=68.40). The three least frequently reported motivations were, “I was drowsy from the drugs” (M=5.46), “I have to work a shift” (M=8.56), and, “I had slept too much the day before and my sleep rhythm was out of whack” (M=8.71) (see Table 1).
Exploratory Factor Analysis of Nap Motivation
Exploratory factor analysis reduced the 34 motivations for napping to interpretable factors. Nine items were eliminated because factor loading, and commonality fell short of the requirement. The factor analysis obtained 25 items distributed across six factors with eigenvalues > 1.0 (KMO=0.88, Bartlett’s p<0.05), and six factors explained up to 68.02% of the variance (see Table 1). Finally, according to the meaning of the included items, nap motivation can be grouped into six factors: restorative, induced, mindful, appetitive, dysregulative, and exercise.
Relationship Between Nap Preference Scores and Demographic Variables
Nap preference scores were calculated by summing the item scores assigned to each factor. The results of the correlation analysis between the nap preference scores are presented in Table 3. As expected, a significant correlation was found between nap preference scores, apart from dysregulative and induced napping unrelated to appetitive napping, revealing that individuals tended to sustain multiple motivations for napping (p<0.01).
 |
Table 3 Correlation Analysis Between Nap Preference Score and Various Variables |
We also investigated whether nap preference scores varied with age, finding that restorative, appetitive, and induced napping were associated with higher age (p<0.01, p<0.05). We also found that there were sex differences in appetitive naps and exercise naps (p<0.01, p<0.05). Interestingly, appetitive naps were preferred by women, whereas exercise naps were preferred by men. In terms of grade level, the upper grades preferred restorative and appetitive naps over the lower grades. Participants who exercised regularly were expected to recover from a nap (p<0.01). However, the function of napping was viewed as restoring sleep restriction by those who used to be non-habitual nappers, and instead a means of enjoyment by those who used to be habitual nappers (p<0.01).
Correlation of Nap Preference Scores with Sleep Variables
Correlational analysis indicated a tendency to choose mindful naps and exercise naps for longer nap durations (p<0.05), while those who chose mindful and appetitive naps napped more frequently (p<0.01, p<0.05). Those who chose restorative, induced, and dysregulative naps indicated poorer sleep quality (p<0.05). Restorative, appetitive, and mindful napping resulted in higher pre-nap fatigue (p<0.01, p<0.05). Mindfulness and appetite napping were significantly correlated with a reduction in fatigue after napping (p<0.01).
Multiple Linear Regression Analysis Among Nap Preference Scores, Nap Duration, Nap Frequency, and Sleep Quality
As shown in Table 4, three multiple linear regression analyses were conducted to further explain the variance in sleep status (eg, nap duration, frequency, and sleep quality) observed among nap preference scores. The results of all three regression models were significant, and motivations for napping explained between 2.70–18.9% of the variance in the sleep variables. In all models, mindfulness (β=0.14, p<0.05) and exercise napping (β=0.11, p<0.05) were positively associated with nap duration, while restorative napping was negatively associated with nap duration (β=−0.14, p<0.05). Appetitive napping was positively associated with nap frequency (β=0.38, p<0.01). Restorative napping was positively associated with PSQI scores (β=0.50, p<0.01), whereas exercise napping was negatively associated with PSQI scores (β=−0.13, p<0.01). Restorative nappers had poorer sleep quality than exercise-motivated nappers, corresponding to the items included in the reported factors.
 |
Table 4 Multiple Linear Regression Analysis of Nap Preference Score and Sleep Variables |
Discussion
Based on the participants’ self-ratings of nap motivation, we propose a structural model of napping motivation for Chinese college students, consisting of six factors: restorative nap factor (naps to restore or prevent sleep loss at night), induced nap factor (naps are induced by environmental or external factors), mindful nap factor (naps to restore cognition and reduce fatigue), appetitive nap factor (naps due to enjoyment), dysregulative nap factor (naps due to dysbalanced sleep rhythms), and exercise nap factor (naps to restore energy or prepare for physical exertion). In this study, we replaced the “emotional factor” in the DREAM model with the “exercise factor” and added an “induced factor”, so it was named the I-DREAM model.
In partial agreement with previous studies, four motivations of the I-DREAM model, namely restorative, mindful, appetitive, and dysregulative, have been reported.21 This implies that the motivational processes of napping are partially similar in study populations from different countries. Although similarities in nomenclature exist, our factor analysis of the Chinese college student population indicates that there are differences in the entries included in the same categories.
In contrast to the DREAM model, on the dysregulative factor, the results of our factor analysis of Chinese college students concluded that “illness” and “experience pain” motivations to nap cannot be included within this factor, or even any of the factors within the overall model. In addition, we included exercise-related motivation for napping as a separate factor from the dysregulative factor, named the ” exercise factor”. This is a novel finding among the Chinese college student population, and the appearance of the exercise napping factor may be attributed to the fact that our survey group was a student population with few illness-related problems. Moreover, the educational process of Chinese college students usually includes physical education exams, and daily physical exercise is very common among them. Therefore, napping becomes a common way for them to regain physical fitness, which could explain the high frequency of napping in the Chinese college student population.
Furthermore, we found that in addition to the exercise napping factor, there exists an additional category of napping factors that has been largely unmentioned and ignored in the literature: the induced napping factor. The five items included in the induced napping factor were not included in the original napping motivation structure and were derived from the open-ended questions asked by Chinese college students. The motivations for napping included in this factor are usually diet, temperature, or other objective circumstances that lead individuals to choose to nap. In China, a high-carbohydrate diet, high midday temperatures, establishment of a lunch break, and herding behavior due to large nap groups all contribute to the occurrence of napping.15,35 These factors are unique and, in China, tied to inherent cultural, dietary, and lifestyle habits.
Finally, another napping motivation, the emotional nap factor, has been previously reported, but this was not confirmed in this survey. Motivation for napping from the emotional factor was excluded when checking the factor loadings in the exploratory factor analysis, possibly because the distribution of the emotional nap items was so extreme that it was impossible to classify it as a single factor. In short, the distinctions between what is included in the I-DREAM model and the DREAM model imply that there may be differences in motivation for napping among different types of people, which suggests that it is necessary to consider differences in nap motivation and lifestyle in future studies exploring nap-related behaviors.
The duration and frequency of naps have been controversial topics in the field of previous epidemiological and psychological research. Some studies suggest that napping for longer than 30 min creates sleep inertia and impairs cognitive performance, while others suggest that longer naps are better.36,37 The results of this study may suggest some new ideas for this controversy, as different nap motivations may need to be matched with appropriate nap duration and nap frequency to achieve the desired effect, otherwise, it may have a negative impact on human performance. The napping preference score was calculated to assess participants’ propensity to motivation for each nap factor and then to explore the relationship between nap motivation factors and nap duration and frequency. We found that naps with different motivations exhibited similar patterns (duration or frequency). It is worth noting that differences in napping motivation have caused diverging studies that have explored the effects of napping behavior on individual performance. Therefore, future studies that further control for nap motivation may help us better understand the impact of nap duration and frequency on individuals.
Another critical finding of this research is that different nap motivations are associated with different patterns of napping and different sleep quality. Napping is not a sleep disorder, but its presence may be a symptom of underlying sleep disorders that cause excessive daytime sleepiness, such as sleep apnea syndrome and circadian sleep disorders.38 However, some studies have suggested that napping improves nighttime sleep quality. Therefore, we believe that it is difficult to draw clear conclusions when discussing the effects of napping on sleep or health, if the motivation for napping is ignored.
As the survey population napped very frequently, the nap motivation model proposed in this study is more applicable to habitual nappers than to non-habitual nappers in the Chinese college student population. This may limit the possible generalization of the nap motivation model to nonhabitual nappers in the Chinese college student population. However, napping is common among Chinese college students, with approximately 89% of the college student population reporting that they nap regularly. Nevertheless, the napping habits of the group being studied should be considered when using the nap motivation model.
To the best of our knowledge, this study is the first to investigate nap motivation among Chinese college students using a continuous self-rating method, which provided detailed information about their motivation for napping compared to the dichotomous self-rating method.
The present study has some limitations that should be acknowledged. First, this study was conducted at only one university in Shanghai, China, and the findings revealed a large group of habitual nappers, which may not allow the nap motivation model to be generalizable to nonhabitual nappers in other regions. Second, the design of the cross-sectional study prevented us from drawing firm conclusions about the causal relationships between the factors of the nap motivation model and other sleep variables. Therefore, longitudinal studies are necessary for exploring the temporal variability and structural stability of motivational structures. Third, the incomplete information from the survey of the study population and the lack of specific controls for pre-survey nighttime sleep may have introduced confounding factors in the interpretation of the results. Finally, the simplicity of the single structural analysis method may have limited the results of the nap motivation model in Chinese college students. Notably, the latent class model (LCA) is an innovative statistical method based on factor analysis. Therefore, the integration and mutual validation of various methods may be a reliable and effective way to explore the structure of nap motivation in the future. In conclusion, expanding the population sample and survey indicators and simplifying the survey methods are worthy of further consideration in future studies.
Conclusion
Our study found that Chinese college students mainly took naps to reduce fatigue, usually in the form of frequent and long naps. We propose a structural model of napping motivation for Chinese college students based on self-rated motivations for napping, consisting of six factors: restorative naps, induced naps, mindful naps, appetitive naps, dysregulative naps, and exercise naps. The various nap motives showed similar patterns, and some nap motives were associated with underlying sleep problems. Our findings can be used by future researchers to determine the effects of nap duration and frequency on behavioral performance, as well as provide earlier identification and intervention for those at risk of potentially unhealthy sleep.
Data Sharing Statement
Data supporting the findings presented in the current study will be available from the corresponding author upon request.
Acknowledgments
Thanks to all the participants who provided support and the professors who provided guidance for this study.
Funding
This work was supported by Thirteenth Five-Year Army Key Discipline Professional Construction Project Support (2020SZxx) and Key Scientific and Research Projects of Logistics in PLA (20BJZ09)
Disclosure
The authors declare that they have no competing interests.
References
1. Monk TH. The post-lunch dip in performance. Clin Sports Med. 2005;24(2):e15–e23. doi:10.1016/j.csm.2004.12.002
2. Lim J, Dinges DF. Sleep deprivation and vigilant attention. Ann N Y Acad Sci. 2008;1129(1):305–322. doi:10.1196/annals.1417.002
3. Owens DS, Macdonald I, Tucker P, et al. Diurnal variations in the mood and performance of highly practised young women living under strictly controlled conditions. Br J Psychol. 2000;91(Pt 1):41–60. doi:10.1348/000712600161664
4. Mantua J, Spencer RMC. Exploring the nap paradox: are mid-day sleep bouts a friend or foe? Sleep Med. 2017;37:88–97. doi:10.1016/j.sleep.2017.01.019
5. Faraut B, Andrillon T, Vecchierini MF, Leger D. Napping: a public health issue. From epidemiological to laboratory studies. Sleep Med Rev. 2017;35:85–100. doi:10.1016/j.smrv.2016.09.002
6. Ficca G, Axelsson J, Mollicone DJ, Muto V, Vitiello MV. Naps, cognition and performance. Sleep Med Rev. 2010;14(4):249–258. doi:10.1016/j.smrv.2009.09.005
7. Chen Q, Ru T, Yang M, et al. Effects of afternoon nap deprivation on adult habitual nappers’ inhibition functions. Biomed Res Int. 2018;2018:5702646. doi:10.1155/2018/5702646
8. Lau EY, Wong ML, Lau KN, Hui FW, Tseng CH. Rapid-Eye-Movement-Sleep (REM) associated enhancement of working memory performance after a daytime nap. PLoS One. 2015;10(5):e0125752. doi:10.1371/journal.pone.0125752
9. Daaloul H, Souissi N, Davenne D. Effects of napping on alertness, cognitive, and physical outcomes of karate athletes. Med Sci Sports Exerc. 2019;51(2):338–345. doi:10.1249/MSS.0000000000001786
10. Ru T, Chen Q, You J, Zhou G. Effects of a short midday nap on habitual nappers’ alertness, mood and mental performance across cognitive domains. J Sleep Res. 2019;28(3):e12638. doi:10.1111/jsr.12638
11. Dinges DF, Orne MT, Whitehouse WG, Orne EC. Temporal placement of a nap for alertness: contributions of circadian phase and prior wakefulness. Sleep. 1987;10(4):313–329.
12. McDevitt EA, Alaynick WA, Mednick SC. The effect of nap frequency on daytime sleep architecture. Physiol Behav. 2012;107(1):40–44. doi:10.1016/j.physbeh.2012.05.021
13. Pilcher JJ, Ginter DR, Sadowsky B. Sleep quality versus sleep quantity: relationships between sleep and measures of health, well-being and sleepiness in college students. J Psychosom Res. 1997;42(6):583–596. doi:10.1016/S0022-3999(97)00004-4
14. Knutson K. Sleep and pain: summary of the 2015 Sleep in America Poll. Sleep Health. 2015;1(2):85. doi:10.1016/j.sleh.2015.03.006
15. Dhand R, Sohal H. Good sleep, bad sleep! The role of daytime naps in healthy adults. Curr Opin Pulm Med. 2006;12(6):379–382. doi:10.1097/01.mcp.0000245703.92311.d0
16. Hilditch CJ, Centofanti SA, Dorrian J, Banks S. A 30-minute, but not a 10-minute nighttime nap is associated with sleep inertia. Sleep. 2016;39(3):675–685. doi:10.5665/sleep.5550
17. Lan TY, Lan TH, Wen CP, Lin YH, Chuang YL. Nighttime sleep, Chinese afternoon nap, and mortality in the elderly. Sleep. 2007;30(9):1105–1110. doi:10.1093/sleep/30.9.1105
18. Leng Y, Wainwright NW, Cappuccio FP, et al. Daytime napping and the risk of all-cause and cause-specific mortality: a 13-year follow-up of a British population. Am J Epidemiol. 2014;179(9):1115–1124. doi:10.1093/aje/kwu036
19. Naska A, Oikonomou E, Trichopoulou A, Psaltopoulou T, Trichopoulos D. Siesta in healthy adults and coronary mortality in the general population. Arch Intern Med. 2007;167(3):296–301. doi:10.1001/archinte.167.3.296
20. Milner CE, Cote KA. Benefits of napping in healthy adults: impact of nap length, time of day, age, and experience with napping. J Sleep Res. 2009;18(2):272–281. doi:10.1111/j.1365-2869.2008.00718.x
21. Duggan KA, McDevitt EA, Whitehurst LN, Mednick SC. To nap, perchance to DREAM: a factor analysis of college students’ self-reported reasons for napping. Behav Sleep Med. 2018;16(2):135–153. doi:10.1080/15402002.2016.1178115
22. Milner CE, Fogel SM, Cote KA. Habitual napping moderates motor performance improvements following a short daytime nap. Biol Psychol. 2006;73(2):141–156. doi:10.1016/j.biopsycho.2006.01.015
23. Macchi MM, Boulos Z, Ranney T, Simmons L, Campbell SS. Effects of an afternoon nap on nighttime alertness and performance in long-haul drivers. Accid Anal Prev. 2002;34(6):825–834. doi:10.1016/S0001-4575(01)00089-6
24. Vela-Bueno A, Fernandez-Mendoza J, Olavarrieta-Bernardino S, et al. Sleep and behavioral correlates of napping among young adults: a survey of first-year university students in Madrid, Spain. J Am Coll Health. 2008;57(2):150–158. doi:10.3200/JACH.57.2.150-158
25. Evans FJ, Cook MR, Cohen HD, Orne EC, Orne MT. Appetitive and replacement naps: EEG and behavior. Science. 1977;197(4304):687–689. doi:10.1126/science.17922
26. Liao JQ. A review of studies on napping at home and abroad. Human Ergonomics. 1999;80(4):42–47.
27. Liao JQ, Xu QZ, Yuan ZY, Wu T, Li ZH. The prevalence of napping in China and analysis of its causes. Hum Ergon. 2000;83(2):
28. Owens JF, Buysse DJ, Hall M, et al. Napping, nighttime sleep, and cardiovascular risk factors in mid-life adults. J Clin Sleep Med. 2010;6(4):330–335. doi:10.5664/jcsm.27873
29. Foley DJ, Vitiello MV, Bliwise DL, Ancoli-Israel S, Monjan AA, Walsh JK. Frequent napping is associated with excessive daytime sleepiness, depression, pain, and nocturia in older adults: findings from the National Sleep Foundation ‘2003 sleep in America’ Poll. Am J Geriatr Psychiatry. 2007;15(4):344–350. doi:10.1097/01.JGP.0000249385.50101.67
30. Buysse DJ, Reynolds CF
31. Zheng B, Li M, Wang KL, Lv J. Analysis of the reliability and validity of the Chinese version of Pittsburgh sleep quality index among medical college students. J Peking Univ. 2016;48(3):424–428.
32. Liu XC, Tang MQ, Hu L, et al. Reliability and validity study of the Pittsburgh Sleep Quality Index. Chin J Psychiatry. 1996;29(2):103–107.
33. Beard MT, Edwards K, Marshall D, Johnson MN. Research methodology: part II, essentials of factor analysis. ABNF J. 1995;6(4):107–112.
34. Al-Balhan EM, Khabbache H, Watfa A, Re TS, Zerbetto R, Bragazzi NL. Psychometric evaluation of the Arabic version of the nomophobia questionnaire: confirmatory and exploratory factor analysis - implications from a pilot study in Kuwait among university students. Psychol Res Behav Manag. 2018;11:471–482. doi:10.2147/PRBM.S169918
35. Lai ML, Li AQ, Wang QP. A review on the effects of dietary protein and carbohydrates on sleep. Food Sci. 2021;166:1–12.
36. Furihata R, Kaneita Y, Jike M, Ohida T, Uchiyama M. Napping and associated factors: a Japanese nationwide general population survey. Sleep Med. 2016;20:72–79. doi:10.1016/j.sleep.2015.12.006
37. Hsouna H, Boukhris O, Abdessalem R, et al. Effect of different nap opportunity durations on short-term maximal performance, attention, feelings, muscle soreness, fatigue, stress and sleep. Physiol Behav. 2019;211:112673. doi:10.1016/j.physbeh.2019.112673
38. Garbarino S. Excessive daytime sleepiness in obstructive sleep apnea: implications for driving licenses. Sleep Breath. 2020;24(1):37–47. doi:10.1007/s11325-019-01903-6
 © 2022 The Author(s). This work is published and licensed by Dove Medical Press Limited. The full terms of this license are available at https://www.dovepress.com/terms.php and incorporate the Creative Commons Attribution - Non Commercial (unported, v3.0) License.
By accessing the work you hereby accept the Terms. Non-commercial uses of the work are permitted without any further permission from Dove Medical Press Limited, provided the work is properly attributed. For permission for commercial use of this work, please see paragraphs 4.2 and 5 of our Terms.
© 2022 The Author(s). This work is published and licensed by Dove Medical Press Limited. The full terms of this license are available at https://www.dovepress.com/terms.php and incorporate the Creative Commons Attribution - Non Commercial (unported, v3.0) License.
By accessing the work you hereby accept the Terms. Non-commercial uses of the work are permitted without any further permission from Dove Medical Press Limited, provided the work is properly attributed. For permission for commercial use of this work, please see paragraphs 4.2 and 5 of our Terms.
