Back to Journals » International Journal of Chronic Obstructive Pulmonary Disease » Volume 15
Serum Levels of Autoantibodies Against Extracellular Antigens and Neutrophil Granule Proteins Increase in Patients with COPD Compared to Non-COPD Smokers
Authors Ma A, Wen L, Yin J, Hu Y, Yue X, Li J, Dong X, Gupta Y , Ludwig RJ , Krauss-Etschmann S , Riemekasten G, Petersen F, Yu X
Received 24 October 2019
Accepted for publication 9 January 2020
Published 29 January 2020 Volume 2020:15 Pages 189—200
DOI https://doi.org/10.2147/COPD.S235903
Checked for plagiarism Yes
Review by Single anonymous peer review
Peer reviewer comments 3
Editor who approved publication: Dr Richard Russell
Aiping Ma,1,* Lifang Wen,2,* Junping Yin,3 Yi Hu,4 Xiaoyang Yue,3 Jiurong Li,1 Xiaoru Dong,2 Yask Gupta,5 Ralf J Ludwig,5 Susanne Krauss-Etschmann,3,6 Gabriela Riemekasten,7 Frank Petersen,3 Xinhua Yu2,3
1Department of Respiratory Medicine, The First Affiliated Hospital, School of Medicine, Xiamen University, Xiamen, People’s Republic of China; 2Xiamen-Borstel Joint Laboratory of Autoimmunity, The Medical College of Xiamen University; 3Priority Area Asthma and Allergy, Research Center Borstel, Airway Research Center North (ARCN), Members of the German Center for Lung Research (DZL), Borstel, Germany; 4Department of Clinical Laboratory, The First Affiliated Hospital, School of Medicine, Xiamen University, Xiamen, People’s Republic of China; 5Lübeck Institute of Experimental Dermatology, University of Lübeck, Lübeck, Germany; 6Institute for Experimental Medicine, Christian-Albrechts-Universitaetzu Kiel, Kiel, Germany; 7Department of Rheumatology, University of Lübeck, Lübeck 23538, Germany
*These authors contributed equally to this work
Correspondence: Xinhua Yu
Priority Area Asthma and Allergy, Research Center Borstel, Borstel 23845, Germany
Tel +49 453 7188 2520
Email [email protected]
Background: Chronic obstructive pulmonary disease (COPD) is a highly prevalent disease leading to irreversible airflow limitation and is characterized by chronic pulmonary inflammation, obstructive bronchiolitis and emphysema. Etiologically, COPD is mediated by toxic gases and particles, eg, cigarette smoke, while the pathogenesis of the disease is largely unknown. Several lines of evidence indicate a link between COPD and autoimmunity but comprehensive studies are lacking.
Methods: By using a protein microarray assaying more than 19,000 human proteins we determined in this study the autoantibody profiles of COPD and non-COPD smokers. The discovery cohort included 5 COPD patients under acute exacerbation (AECOPD) and 5 age- and gender-matched non-COPD smokers. One putative candidate autoantibody, anti-lactoferrin IgG, was further investigated by using immunoblotting with a large validation cohort containing 124 healthy controls, 92 patients with AECOPD and 52 patients with stable COPD.
Results: We show that i) autoantigens targeted by autoantibodies with higher titers in COPD patients were enriched in extracellular regions, while those with lower titers in COPD patients were enriched in intracellular compartments. ii) levels of IgG autoantibodies against many neutrophil granule proteins were significantly higher in COPD patients than in non-COPD smokers. Furthermore, increased levels of anti-lactoferrin antibodies in COPD patients were confirmed in a cohort with a large number of samples.
Conclusion: The comprehensive autoantibody profiles from COPD patients established in this study demonstrated for the first time a shift in the cellular localization of antigens targeted by autoantibodies in COPD.
Keywords: chronic obstructive pulmonary disease, autoimmunity, autoantibody profile, neutrophil granule proteins, lactoferrin
Introduction
Chronic obstructive pulmonary disease (COPD) is a disease characterized by persistent pulmonary inflammation, obstruction of the small airways (obstructive bronchiolitis) and structural changes of the alveoli (emphysema).1 Patients with COPD suffer from a progressive airflow limitation and develop symptoms such as wheezing, coughing, chest tightness and shortness of breath.1 Currently, COPD is a major public health problem, affecting more than 300 million people worldwide and leading to millions of death annually.2 Although it is widely accepted that COPD is triggered by inhaled toxic gases and particles, the pathogenesis of COPD remains largely unclear.1,3 Cigarette smoking (CS) is the major etiologic factor for COPD,4,5 with more than 80% patients with COPD being smokers.5 However, the prevalence of COPD even after many years of smoking is only around 50%,6 suggesting that the susceptibility to smoking-induced COPD varies considerably among smoking persons. Therefore, exploring the biological differences between patients with COPD and non-COPD smokers could help to better understand the pathogenesis of the disease and to delineate novel therapeutic targets.
Smoke-induced immune responses play an essential role in the development of COPD.4,7,8 On the one hand, it is widely believed that innate immunity is the leading actor in the early development of pulmonary changes in the disease and its animal models.8–12 One the other hand, there is accumulating evidence that adaptive immunity plays a role in the chronic phase of COPD. For example, it has been shown that smoke cessation does not attenuate the pulmonary inflammation once COPD,13,14 suggesting a memory adaptive immune response to non-cigarette antigens. In addition, COPD patients are featured by well-organized lymphoid follicles around small airways and lung parenchyma,15–17 which also implicates a role of adaptive immunity in the disease.
Among smoke-induced adaptive immune responses, autoimmunity is a putative candidate which has been suggested to be associated with COPD.18 Since 2007, when Lee et al reported that emphysema is characterized by the presence of autoimmune responses against elastin,19 a large body of evidence has been accumulated for an association of autoimmunity with COPD.20 It has been shown that autoantibodies against lung tissue 21,22 or single pulmonary cell types, such as epithelial and endothelial cells 21,23–25 are highly prevalent in sera of patients with COPD. In addition, COPD patients with more severe disease show a higher prevalence of anti-tissue antibodies,22,26 suggesting an association of anti-tissue antibodies with the severity of COPD. In line with observations made in humans, animal models for COPD also support a role of autoantibodies in the pathogenesis of COPD, especially in those with emphysema. For example, Taraseviciene-Stewart and colleagues reported that immunization with human umbilical vein endothelial cells (HUVECs) induces antibodies against epithelial cells and emphysema in rats,27 suggesting a role of autoimmunity against the epithelium in COPD.
Encouraged by the association between autoimmunity and COPD, many studies aimed to identify autoantigens with potential relevance for the development of the disease. These include autoantibodies against extracellular matrix proteins, intracellular proteins of pulmonary epithelial or endothelial, neo-autoantigens, immune molecules and further autoantigens that are found in common autoimmune diseases. However, the presence of autoantibodies against those defined antigens is not always consistent among different studies.20 These studies are frequently limited by the very low number of autoantigens included in their analysis. As a consequence, the whole landscape of autoantibodies in COPD remained unexplored in these approaches and disease-relevant autoantigens may have been missed.
The presence of natural autoantibodies of both IgG and IgM classes in sera is a normal phenomenon in humans and animals,28–30 implying that those autoantibodies might play a physiological role in maintaining tissue homeostasis. Therefore, it is conceivable that autoantibody profiles might change from physiological condition to pathological condition, e.g. from non-COPD smokers to COPD patients. In this study, we therefore aimed to determine the difference in autoantibody profiles between patients with COPD and non-COPD smokers. To reach this aim, we performed a proteome-wide screening of autoantibodies of both IgG and IgM subclasses by using protein microarrays with more than 19,000 full-length human proteins in a small cohort of COPD patients and non-COPD smokers. Deregulated autoantibodies were then validated in a large cohort of COPD patients using patients with asthma as disease controls.
Materials and Methods
Subjects
COPD was defined and categorized according to the Global Initiative for Chronic Obstructive Lung Disease (GOLD) guidelines.31 Pulmonary function tests were performed using Master Screen (Erich Jaeger GmbH) and included post-bronchodilator FEV1, FVC, FEV1/FVC ratio, TLC, RV and inspiratory capacity (IC). Lung function measurements were expressed as percentage of predicted values. Tests were performed according to the American Thoracic Society/European Respiratory Society guidelines.31 Because this study was focused on COPD-related autoimmunity, we excluded patients who showed any of the following conditions: other chronic lung diseases (e.g. bronchiectasis, cystic fibrosis, or idiopathic pulmonary fibrosis), heart failure, autoimmune disease, lung cancer or metastatic cancer, HIV/AIDS, or chronic oral prednisone use. The presence of emphysema was assessed by using high resolution computed tomography (HRCT) of the chest.32 Patients with asthma were included when fulfilling the diagnostic criteria according to the guideline proposed the Global Initiative for Asthma.33 The normal control group was composed of healthy subjects who received an annual routine physical examination. All subjects were recruited from the First Affiliated Hospital of Xiamen University. This study was conducted in accordance with the Helsinki declaration. This project was approved by the Ethics Committee of the First Affiliated Hospital of Xiamen University (approval No. 5210-07/03/2018). Written informed consent was obtained from COPD patients and healthy volunteers.
Preparation of Serum Samples
Blood samples were collected from all subjects with BD Vacutainer Plus Plastic tubes which were coated with silicone and micronized silica particles to accelerate clotting. Samples were then centrifuged at 1500 x g for 15 min at room temperature, and supernatants were aliquoted and immediately stored at –80°C for further evaluation.
Detection of Autoantibodies Using a Human Proteome Microarray
A human proteome microarray (HuProtTM v3.0, CDI Labs, Mayaguez, PR) that contains over 19,000 recombinant human full-length proteins in duplicates was used to profile serum autoantibodies.34 Briefly, arrays were blocked with 1% BSA at 4 oC for 3 h and probed with a total of 5 mL of diluted serum sample (1:200 diluted in Tris-buffered saline containing 0.1% Tween 20 detergent (TBS-T)) at room temperature for 1 h. The microarray was then washed with 1× TBS-T and probed with Cy3-labeled anti-human IgG and Cy5-labeled anti-human IgM at room temperature for 1 h. Finally, arrays were washed with TBS-T, dried in a Slide Washer (CapitalBio Inc., Beijing, China) at room temperature, and then scanned in a GenePix 4200A (Molecular Devices, Sunnyvale, CA). Signal intensities were measured by using GenePix Pro 6.0 Software (Molecular Devices, Sunnyvale, CA). The median foreground and background intensities for each spot on the protein microarrays were obtained, and the raw intensity for each spot was defined as the difference between foreground and background median intensity.
Analysis of Autoantibody Profiles
All data analysis of protein microarray was performed using R Studio (version 3.4.4). Background correction and quantile normalization of all expression files were performed by using LIMMA (Linear Models for Microarray Data) package.35 Differentially expressed autoantibodies between COPD patients and non-COPD smokers were identified according to the following criteria i) fold change (FC) more than 1.5 (logFC ± 0.585), ii) p value less than 0.05, and iii) absolute difference in signal intensity more than 100.36 Redundancy in differentially expressed autoantibodies was removed by a homology search. Two-dimensional hierarchical cluster analysis was performed with differentially expressed autoantibodies using LIMMA package. The enrichment analysis of Gene Ontology (GO) was performed as previously described 37 by using Database for Annotation, Visualization and Integrated Discovery (DAVID, v6.8) software.38 Multiple-testing adjustment was performed via false discovery rate estimation. STRING database (version 11.0) and Cytoscape software platform were used for the construction of co-expression network of differentially expressed autoantibodies.
Immunoblotting Analysis
Immunoblotting was used to quantify the levels of IgG autoantibodies against lactoferrin. Briefly, lactoferrin (Sigma, USA) was resolved by 10% SDS-polyacrylamide gel electrophoresis (SDS-PAGE) and transferred onto a polyvinylidene difluoride (PVDF) membrane. After incubation with the individual sera (1:100 diluted) at 4°C overnight, the membrane was incubated with DyLightTM 680-labeled goat anti-human IgG at room temperature for 1h. Finally, the membrane was scanned by Odyssey® CLx (LI-COR, Germany), and fluorescence signals were quantified using Image Studio Lite 5.2 analysis software. A mixture of several serum samples used as an internal control was applied on each membrane to make samples from different membrane comparable. Signal intensities of all samples were normalized to that of the internal control, and the normalized signals were used for further analysis.
Statistical Analyses
Apart from microarray analysis, all other statistical analyses were performed with GraphPad Prism statistical software (GraphPad Software Inc., version 5.01, La Jolla, CA, USA). The Kolmogorov–Smirnov normality test was performed to analyze if quantitative variables were normally distributed. To calculate the P values, quantitative data in normal distribution were compared using the Student’s t-test; otherwise, the Mann–Whitney U-test was used. Pearson correlation was performed to determine the correlation between autoantibodies and disease-related phenotypes. P<0.05 was considered as statistically significant.
Results
Differentially Expressed Autoantibodies Between COPD Patients and Non-COPD Smokers
For the detection of autoantibody profiles, we recruited 5 male COPD patients ranging from 67 to 82 years in age who were current smokers with 10 to 20 cigarettes per day since 30 to 50 years (Table 1). All 5 patients had severe COPD with GOLD grade III and emphysema and were admitted to the hospital because they experienced an acute exacerbation. Five male non-COPD smokers were recruited as controls, with comparable age, smoking history and numbers of cigarettes smoked per day (Table 1). Serum samples from 5 COPD patients with acute exacerbation (AECOPD) and 5 non-COPD smokers were used for the detection of autoantibody profiles using protein microarray. Normalization of signal intensities of 10 HuProtTM v3.0 microarrays was performed to make them comparable to each other (Supplementary Figure 1). The microarray data were deposited into Gene Expression Omnibus: https://www.ncbi.nlm.nih.gov/geo/info/linking.html, with an accession number of GSE133096. Principal component analysis (PCA) with the normalized data demonstrated that the IgG autoantibodies, but not IgM autoantibodies, distinguished COPD patients from non-COPD smokers (Supplementary Figure 2). Using the predefined selection criteria (FC>1.5, p<0.05, and difference>100), we identified 546 IgG autoantibodies (252 with higher titer and 294 with lower titer in COPD) that were differentially expressed between COPD patients and non-COPD smokers (Supplementary Table 1 and Figure 1A and B). In addition, 527 differentially expressed IgM autoantibodies (167 with higher titer and 360 with lower titer in COPD) were identified between the two groups (Supplementary Table 2 and Figure 1A and B). However, when a multiple-testing adjustment was performed via false discovery rate (FDR) estimation, none of the differences determined between experimental groups remained significant. Two-dimensional hierarchical cluster analysis of differentially expressed IgG autoantibodies (Figure 1C) and IgM autoantibodies (Figure 1D) identified multiple subset clusters based on the similarity of autoantibody patterns.
 |
Table 1 Demographic and Clinical Status of Patients with COPD and Non-COPD Smokers Used for the Detection of Autoantibody Profiles |
Interestingly, autoantibodies against many neutrophil granule proteins were differentially expressed between COPD patients and non-COPD smokers (Table 2). Among 103 neutrophil specific granule proteins proposed by Rorvig and colleagues,39 levels of IgG autoantibodies against 8 of them were higher in COPD patients than in non-COPD patients, including cathepsin H (CTSH), alpha-L-fucosidase (FUCA2), LTF, matrix metallopeptidase 9 (MMP9), plasminogen activator, urokinase receptor (PLAUR), proteinase 3 (PRTN3), tissue inhibitor of metalloproteinases 2 (TIMP2) and TNF superfamily member 14 (TNFSF14). In addition, levels of IgM autoantibodies against vanin 1 (VNN1) and neutrophil elastase (ELANE) were higher, while levels of IgM autoantibodies against arginase 1 (ARG1) were lower in COPD patients than in non-COPD smokers.
 |
Table 2 Differentially Expressed Autoantibodies Against Neutrophil Granule Proteins in COPD Patients Compared to Non-COPD Smokers |
Since several autoantibodies including those against elastin, aggrecan, cytokeratin 18, cytokeratin 19, CD80, β2-microglobulin and collagen I, II and IV have already been suggested to be upregulated in COPD,19,22,40–43 we evaluated the expression of those autoantibodies in our samples. All those autoantigens were presented on the microarray, but no significant difference was observed for any of those autoantibodies between COPD patients and non-COPD smokers (Supplementary Table 3).
Functional Grouping and Network Analysis of Differentially Expressed Autoantibodies
To explore functional annotations for the differentially expressed autoantibodies, the biological processes, cellular components and molecular function of their autoantigens were analyzed using GO enrichment analysis (Figure 2, Supplementary Tables 4 and 5). According to their cellular positions, autoantigens targeted by IgG autoantibodies with higher titers in COPD patients were enriched in the extracellular region, while those targeted by IgG autoantibodies with lower titers in COPD patients were enriched in intracellular region.
With regards to differentially expressed IgM autoantibodies, autoantigens targeted by autoantibodies with higher titers in COPD patients were enriched in the nucleus and functionally related to the regulation of smooth muscle contraction. By contrast, those targeted by IgM autoantibodies with lower titers in COPD patients were enriched in cytosol, cytoplasm and nucleoplasm, and they were functionally related to L-methionine biosynthetic process from methylthioadenosine, endosomal transport, negative regulation of apoptotic process, cell-cell adhesion, protein binding, transcription coactivator activity and signaling adaptor activity.
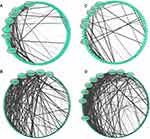
To further characterize the differentially expressed autoantibodies, we determined their functional connections by using network analysis. As shown in Figure 3, several neutrophil granule proteins such as MMP9, TIMP2 and ELANE were on the lists of top 5 connected autoantigens targeted by differentially expressed autoantibodies (Supplementary Tables 6 and 7)
Validation of the Association of Anti-Lactoferrin IgG with COPD
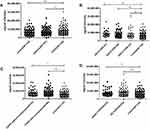
For the validation of COPD-associated autoantibodies, we recruited 144 COPD patients, including 92 patients with COPD with acute exacerbation (AECOPD) and 52 patients with stable COPD, 101 patients with asthma as a disease control, and 124 healthy controls including smokers and non-smokers (Table 3). Given that neutrophils play an important role in the pathogenesis of COPD 4,7 and the current study demonstrated that IgG autoantibodies against multiple neutrophil-specific autoantigens were upregulated in COPD patients than in non-COPD smokers, we selected autoantibodies against LTF which have been demonstrated to be presented in multiple autoimmune diseases 44–46 for validation. Using immunoblotting, we quantified the expression of IgG autoantibodies against LTF in sera of patients and controls (Supplementary Figure 3). As shown in Figure 4A, COPD patients showed significantly higher levels of IgG autoantibodies against LTF than both healthy control and patients with asthma. When COPD patients were divided into subgroups according to the GOLD stages, levels of anti-LTF IgG were significantly higher in all subgroups of COPD patients compared with healthy controls (Figure 4B). Moreover, when stratifying COPD patients according to the presence or absence of emphysema, both groups were characterized by significantly higher levels of anti-LTF IgG than healthy controls. This difference was however more pronounced in emphysematic patients (Figure 4C). Finally, a corresponding effect was seen also when COPD patients were subgrouped into AECOPD and stable COPD. Both subgroups showed significantly higher levels of anti-LTF IgG as compared to healthy controls (Figure 4D).
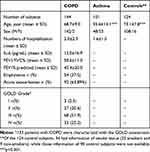 |
Table 3 Demographic and Clinical Status of COPD Patients and Controls Used for the Validation of Differentially Expressed Autoantibodies |
In addition, correlated analysis demonstrated that levels of anti-LTF IgG were not correlated with sub-phenotypes of COPD including lung function, GOLD grade, number of hospitalizations, levels of IL-6 or body mass index (BMI). (Supplementary Figure 4)
Therefore, these results validated the higher levels of IgG autoantibodies against LTF in patients with COPD than in healthy controls and patients with asthma.
Discussion
Although it is well known that COPD is associated with the formation of autoantibodies, the landscape of autoimmunity in the disease is still unknown. Using a protein microarray containing more than 19,000 proteins, the current study for the first time generated comprehensive autoantibody profiles from patients with COPD and non-COPD smokers. Compared to non-COPD smokers, patients with COPD were characterized by a distinct autoantibody profile, whose predicted autoantigens differed considerably in terms of cellular location and biological function. Furthermore, with a large number of samples, we validated the upregulation of anti-LTF IgG in patients with COPD compared with healthy control and patients with asthma.
Interestingly, numbers of autoantibodies with higher titers in COPD patients than in non-COPD smokers were similar to those with lower titers, which is in contrast to the idea that COPD is associated only with a strong general increase in autoimmunity. Although unexpected at first glance, this observation is not surprising as it has been shown that healthy subjects can have even more autoantibodies to some antigens than patients suffering from various diseases including autoimmune diseases such as multiple sclerosis.30 Therefore, these findings suggest that the association of COPD with autoimmunity is more due to a change in the profile of autoantibodies than to a simple general shift in self-reactivity.
The current study demonstrates that autoantigens targeted by IgG autoantibodies with high titers in COPD patients were enriched in extracellular regions, while those of IgG autoantibodies with lower titers were enriched in intracellular compartments such as cytoplasm and nucleus. Thus, low levels of IgG autoantibodies against intracellular antigens in COPD patients might disturb tissue homeostasis. This notion is further supported by the finding that levels of IgM autoantibodies against intracellular antigens were also lower in COPD patients than in non-COPD smokers. It has been suggested that in healthy subjects one of the main functions of natural autoantibodies, especially those against intracellular antigens, is to clean cell debris and thus to maintain tissue homeostasis.30,47 In addition, due to the difference in accessibility to autoantigens, autoantibodies against extracellular antigens are more likely to be pathogenic than those against intracellular antigens, which is best exemplified by neurological paraneoplastic syndrome.48,49 Thus, high levels of IgG autoantibodies against extracellular antigens in COPD patients might increase the possibility of autoantibody-mediated pathogenic changes, which, however, needs to be further investigated.
Maybe the most interesting result from this study is that IgG autoantibodies against many neutrophil granule proteins are upregulated in COPD patients. Among 103 neutrophil-specific granule proteins proposed by Rorvig and colleagues,39 levels of IgG autoantibodies against 8 of them were higher in COPD patients than in non-COPD smokers, including CTSH, FUCA2, LTF, MMP9, PLAUR, PRTN3, TIMP2 and TNFSF14. In sharp contrast, levels of IgG autoantibodies against none of the 103 neutrophil granule proteins were lower in COPD patients. This drastic discrepancy suggests that there are stronger autoimmune responses against neutrophil granule proteins in patients with COPD than non-COPD smokers. It is well known that neutrophil-derived proteases released via degranulation are key mediators of tissue damage in COPD.50 In addition, some molecules involved in the recruitment and activation of neutrophils have been shown to play an important role in the development of experimental COPD.11,51,52 Therefore, it is conceivable that neutrophil degranulation in the lung during disease manifestation provides granule proteins as autoantigens, which enhances the corresponding autoimmune responses.
One of the main functions of natural autoantibodies in healthy subjects is to neutralize target antigens, which is best exemplified by autoantibodies against cytokines.53 An interesting question is whether autoantibodies against neutrophil granule proteins, e.g. proteases involved in tissue destruction in the pathogenesis of COPD, are functional and thus regulate the development of the disease. With a large number of samples, the current study confirmed the higher levels of autoantibodies against LTF in COPD, but the levels of anti-LTF antibodies were not associated with any disease phenotypes of the disease, suggesting that the anti-LTF antibodies have no strong effect on the development of COPD. However, high levels of autoantibodies against three neutrophil proteases including MMP9, CTSH and PRTN3 and one protease inhibitor, TIMP2, might be interesting candidates, which need to be elucidated in the future.
Previously, many autoantibodies such as anti-extracellular matrix proteins, anti-cytokeratins, anti-immune molecules antibodies have been suggested to associate with COPD and some of them have been shown to correlate with disease phenotypes,19,22,40–43 suggesting that those autoantibodies might contribute to the development of the disease. However, such associations have not been confirmed by others 45,54–57 and were also not observed in our study using microarray data analysis. These findings support the notion that those potential candidate autoantibodies might be not relevant for COPD.
Although our results provide an idea of the autoantibody landscape in COPD patients and non-COPD smokers, some limitations in this study have to be mentioned. First, the number of samples used for the microarray screening is very small, which might lead to false-positive and false-negative results. For example, among hundreds of differentially expressed autoantibodies identified between COPD patients and non-COPD smoker controls, none of them remains significant after multiple-testing adjustment. This suggests that differentially expressed autoantibodies identified in the discovery cohort of the current study might be false positives and thus need to be validated in another cohort. Second, only one member of the group of differentially expressed autoantibodies has been selected for validation with a large number of samples. Third, all five COPD patients recruited for the microarray screening are under acute exacerbation. Since acute exacerbation is often caused by bacterial or viral infections that will stimulate immune system,58 the differences in autoantibody profiles between those COPD patients and non-COPD smokers are not only associated with the disease but also related to acute exacerbation. Finally, this study lacks experimental evidence for a role of those increased autoantibodies in the development of COPD. Further cellular or animal experiments are required in the future to clarify this issue.
In conclusion, this study for the first time determined autoantibody profiles of COPD patients and non-COPD smokers. It provides a landscape of the autoimmunity in these two related groups, which sheds new light on the pathogenesis of smoke-induced COPD.
Acknowledgments
This work was supported by the National Natural Science Foundation of China (No.81600048) and by the Deutsche Forschungsgemeinschaft: Research Training Group “Modulation of Autoimmunity” (GRK1727), Cluster of Excellence “Inflammation at Interfaces” (EXC 306) and Bundesministerium für Bildung und Forschung via the German Center for Lung Research (DZL).
Author Contributions
All authors contributed to data analysis, drafting or revising the article, gave final approval of the version to be published, and agree.
Disclosure
During the last 3 years, RJL has received research funding from MiltenyiBiotec, Biogen, Biotest, Almirall, True North Therapeutics, UCB Pharma, ArgenX, TxCell, Topadur, Incyte and Admirx and fees for consulting or speaking from ArgenX, Immunogenetics, Novartis and Lilly. The authors report no other conflicts of interest in this work.
References
1. Hogg JC, Timens W. The pathology of chronic obstructive pulmonary disease. Annu Rev Pathol. 2009;4:435–459. doi:10.1146/annurev.pathol.4.110807.092145
2. Global Burden of Disease Study 2013 Collaborators. Global, regional, and national incidence, prevalence, and years lived with disability for 301 acute and chronic diseases and injuries in 188 countries, 1990–2013: a systematic analysis for the Global Burden of Disease Study 2013. Lancet. 2015;386(9995):743–800. doi:10.1016/S0140-6736(15)60692-4
3. Tuder RM, Petrache I. Pathogenesis of chronic obstructive pulmonary disease. J Clin Invest. 2012;122(8):2749–2755. doi:10.1172/JCI60324
4. Caramori G, Casolari P, Barczyk A, Durham AL, Di SA, Adcock I. COPD immunopathology. Semin Immunopathol. 2016;38(4):497–515. doi:10.1007/s00281-016-0561-5
5. Terzikhan N, Verhamme KM, Hofman A, Stricker BH, Brusselle GG, Lahousse L. Prevalence and incidence of COPD in smokers and non-smokers: the Rotterdam Study. Eur J Epidemiol. 2016;31(8):785–792. doi:10.1007/s10654-016-0132-z
6. Lundback B, Lindberg A, Lindstrom M, et al. Not 15 but 50% of smokers develop COPD?–Report from the Obstructive Lung Disease in Northern Sweden Studies. Respir Med. 2003;97(2):115–122. doi:10.1053/rmed.2003.1446
7. Brusselle GG, Joos GF, Bracke KR. New insights into the immunology of chronic obstructive pulmonary disease. Lancet. 2011;378(9795):1015–1026. doi:10.1016/S0140-6736(11)60988-4
8. Shaykhiev R, Crystal RG. Innate immunity and chronic obstructive pulmonary disease: a mini-review. Gerontology. 2013;59(6):481–489. doi:10.1159/000354173
9. De CG, Lunghi B, Bartalesi B, et al. Severe Reduction in Number and Function of Peripheral T Cells Does Not Afford Protection toward Emphysema and Bronchial Remodeling Induced in Mice by Cigarette Smoke. Am J Pathol. 2016;186(7):1814–1824. doi:10.1016/j.ajpath.2016.03.002
10. De CG, Bartalesi B, Cavarra E, Balzano E, Lungarella G, Lucattelli M. Ongoing lung inflammation and disease progression in mice after smoking cessation: beneficial effects of formyl-peptide receptor blockade. Am J Pathol. 2018;188(10):2195–2206. doi:10.1016/j.ajpath.2018.06.010
11. Dunne AE, Kawamatawong T, Fenwick PS, et al. Direct inhibitory effect of the PDE4 inhibitor roflumilast on neutrophil migration in chronic obstructive pulmonary disease. Am J Respir Cell Mol Biol. 2019;60(4):445–453. doi:10.1165/rcmb.2018-0065OC
12. Fessler MB. Drugging the mighty neutrophil in chronic obstructive pulmonary disease. Am J Respir Cell Mol Biol. 2019;60(4):382–383. doi:10.1165/rcmb.2018-0370ED
13. Gamble E, Grootendorst DC, Hattotuwa K, et al. Airway mucosal inflammation in COPD is similar in smokers and ex-smokers: a pooled analysis. Eur Respir J. 2007;30(3):467–471. doi:10.1183/09031936.00013006
14. Rutgers SR, Postma DS, Ten Hacken NH, et al. Ongoing airway inflammation in patients with COPD who do not currently smoke. Thorax. 2000;55(1):12–18. doi:10.1136/thorax.55.1.12
15. Brusselle GG, Demoor T, Bracke KR, Brandsma CA, Timens W. Lymphoid follicles in (very) severe COPD: beneficial or harmful? Eur Respir J. 2009;34(1):219–230. doi:10.1183/09031936.00150208
16. Hogg JC, Chu F, Utokaparch S, et al. The nature of small-airway obstruction in chronic obstructive pulmonary disease. N Engl J Med. 2004;350(26):2645–2653. doi:10.1056/NEJMoa032158
17. Seys LJ, Verhamme FM, Schinwald A, et al. Role of B cell-activating factor in chronic obstructive pulmonary disease. Am J Respir Crit Care Med. 2015;192(6):706–718. doi:10.1164/rccm.201501-0103OC
18. Caramori G, Ruggeri P, Di SA, et al. Autoimmunity and COPD: clinical Implications. Chest. 2018;153(6):1424–1431. doi:10.1016/j.chest.2017.10.033
19. Lee SH, Goswami S, Grudo A, et al. Antielastin autoimmunity in tobacco smoking-induced emphysema. Nat Med. 2007;13(5):567–569. doi:10.1038/nm1583
20. Wen L, Krauss-Etschmann S, Petersen F, Yu X. Autoantibodies in chronic obstructive pulmonary disease. Front Immunol. 2018;9:66. doi:10.3389/fimmu.2018.00066
21. Feghali-Bostwick CA, Gadgil AS, Otterbein LE, et al. Autoantibodies in patients with chronic obstructive pulmonary disease. Am J Respir Crit Care Med. 2008;177(2):156–163. doi:10.1164/rccm.200701-014OC
22. Packard TA, Li QZ, Cosgrove GP, Bowler RP, Cambier JC. COPD is associated with production of autoantibodies to a broad spectrum of self-antigens, correlative with disease phenotype. Immunol Res. 2013;55(1–3):48–57. doi:10.1007/s12026-012-8347-x
23. Cheng G, Zhang N, Wang Y, Rui J, Yin X, Cui T. Antibodies of IgG, IgA and IgM against human bronchial epithelial cell in patients with chronic obstructive pulmonary disease. Clin Lab. 2016;62(6):1101–1108. doi:10.7754/Clin.Lab.2015.151020
24. Karayama M, Inui N, Suda T, Nakamura Y, Nakamura H, Chida K. Antiendothelial cell antibodies in patients with COPD. Chest. 2010;138(6):1303–1308. doi:10.1378/chest.10-0863
25. Kirkham PA, Caramori G, Casolari P, et al. Oxidative stress-induced antibodies to carbonyl-modified protein correlate with severity of chronic obstructive pulmonary disease. Am J Respir Crit Care Med. 2011;184(7):796–802. doi:10.1164/rccm.201010-1605OC
26. Nunez B, Sauleda J, Anto JM, et al. Anti-tissue antibodies are related to lung function in chronic obstructive pulmonary disease. Am J Respir Crit Care Med. 2011;183(8):1025–1031. doi:10.1164/rccm.201001-0029OC
27. Taraseviciene-Stewart L, Scerbavicius R, Choe KH, et al. An animal model of autoimmune emphysema. Am J Respir Crit Care Med. 2005;171(7):734–742. doi:10.1164/rccm.200409-1275OC
28. Cabral-Marques O, Marques A, Giil LM, et al. GPCR-specific autoantibody signatures are associated with physiological and pathological immune homeostasis. Nat Commun. 2018;9(1):5224. doi:10.1038/s41467-018-07598-9
29. Madi A, Hecht I, Bransburg-Zabary S, et al. Organization of the autoantibody repertoire in healthy newborns and adults revealed by system level informatics of antigen microarray data. Proc Natl Acad Sci U S A. 2009;106(34):14484–14489. doi:10.1073/pnas.0901528106
30. Nagele EP, Han M, Acharya NK, DeMarshall C, Kosciuk MC, Nagele RG. Natural IgG autoantibodies are abundant and ubiquitous in human sera, and their number is influenced by age, gender, and disease. PLoS One. 2013;8(4):e60726. doi:10.1371/journal.pone.0060726
31. Vogelmeier CF, Criner GJ, Martinez FJ, et al. Global strategy for the diagnosis, management, and prevention of chronic obstructive lung disease 2017 report. GOLD executive summary. Am J Respir Crit Care Med. 2017;195(5):557–582. doi:10.1164/rccm.201701-0218PP
32. Haruna A, Muro S, Nakano Y, et al. CT scan findings of emphysema predict mortality in COPD. Chest. 2010;138(3):635–640. doi:10.1378/chest.09-2836
33. Bateman ED, Hurd SS, Barnes PJ, et al..Global strategy for asthma management and prevention: GINA executive summary. Eur Respir J.2008;31:143–178. doi:10.1183/09031936.00138707
34. Gowen MF, Giles KM, Simpson D, et al. Baseline antibody profiles predict toxicity in melanoma patients treated with immune checkpoint inhibitors. J Transl Med. 2018;16(1):82. doi:10.1186/s12967-018-1452-4
35. Smyth GK. Linear models and empirical bayes methods for assessing differential expression in microarray experiments. Stat Appl Genet Mol Biol. 2004;3:Article3. doi:10.2202/1544-6115.1027
36. Li C, Hung WW. Model-based analysis of oligonucleotide arrays: model validation, design issues and standard error application. Genome Biol. 2001;2(8):RESEARCH0032.
37. Yin J, Zheng J, Deng F, et al. Gene Expression profiling of lacrimal glands identifies the ectopic expression of MHC II on glandular cells as a presymptomatic feature in a mouse model of primary sjogren’s syndrome. Front Immunol. 2018;9:2362. doi:10.3389/fimmu.2018.02362
38. Huang D, Sherman BT, Lempicki RA. Bioinformatics enrichment tools: paths toward the comprehensive functional analysis of large gene lists. Nucleic Acids Res. 2009;37(1):1–13. doi:10.1093/nar/gkn923
39. Rorvig S, Ostergaard O, Heegaard NH, Borregaard N. Proteome profiling of human neutrophil granule subsets, secretory vesicles, and cell membrane: correlation with transcriptome profiling of neutrophil precursors. J Leukoc Biol. 2013;94(4):711–721. doi:10.1189/jlb.1212619
40. Cherneva RV, Georgiev OB, Petrova DS, et al. The role of small heat-shock protein alphaB-crystalline (HspB5) in COPD pathogenesis. Int J Chron Obstruct Pulmon Dis. 2012;7:633–640. doi:10.2147/COPD.S34929
41. Kuo YB, Chang CA, Wu YK, et al. Identification and clinical association of anti-cytokeratin 18 autoantibody in COPD. Immunol Lett. 2010;128(2):131–136. doi:10.1016/j.imlet.2009.12.017
42. Luo XM, Liu XY, Tang JH, et al. Autoantibodies against CD80 in patients with COPD. Clin Transl Immunol. 2016;5(10):e103. doi:10.1038/cti.2016.57
43. Xiong Y, Gao S, Luo G, et al. Increased circulating autoantibodies levels of IgG, IgA, IgM against cytokeratin 18 and cytokeratin 19 in chronic obstructive pulmonary disease. Arch Med Res. 2017;48(1):79–87. doi:10.1016/j.arcmed.2017.01.007
44. Esaguy N, Freitas PM, Aguas AP. Anti-lactoferrin autoantibodies in rheumatoid arthritis. Clin Exp Rheumatol. 1993;11(5):581–582.
45. Greene CM, Low TB, O’Neill SJ, McElvaney NG. Anti-proline-glycine-proline or antielastin autoantibodies are not evident in chronic inflammatory lung disease. Am J Respir Crit Care Med. 2010;181(1):31–35. doi:10.1164/rccm.200904-0545OC
46. Nassberger L, Hultquist R, Sturfelt G. Occurrence of anti-lactoferrin antibodies in patients with systemic lupus erythematosus, hydralazine-induced lupus, and rheumatoid arthritis. Scand J Rheumatol. 1994;23(4):206–210. doi:10.3109/03009749409103062
47. Avrameas S, Selmi C. Natural autoantibodies in the physiology and pathophysiology of the immune system. J Autoimmun. 2013;41:46–49. doi:10.1016/j.jaut.2013.01.006
48. Dalmau J, Graus F. Antibody-mediated encephalitis. N Engl J Med. 2018;378(9):840–851. doi:10.1056/NEJMra1708712
49. Hoftberger R, Rosenfeld MR, Dalmau J. Update on neurological paraneoplastic syndromes. Curr Opin Oncol. 2015;27(6):489–495. doi:10.1097/CCO.0000000000000222
50. Hoenderdos K, Condliffe A. The neutrophil in chronic obstructive pulmonary disease. Am J Respir Cell Mol Biol. 2013;48(5):531–539. doi:10.1165/rcmb.2012-0492TR
51. Cardini S, Dalli J, Fineschi S, Perretti M, Lungarella G, Lucattelli M. Genetic ablation of the fpr1 gene confers protection from smoking-induced lung emphysema in mice. Am J Respir Cell Mol Biol. 2012;47(3):332–339. doi:10.1165/rcmb.2012-0036OC
52. Cicko S, Lucattelli M, Muller T, et al. Purinergic receptor inhibition prevents the development of smoke-induced lung injury and emphysema. J Immunol. 2010;185(1):688–697. doi:10.4049/jimmunol.0904042
53. Vincent T, Plawecki M, Goulabchand R, Guilpain P, Eliaou JF. Emerging clinical phenotypes associated with anti-cytokine autoantibodies. Autoimmun Rev. 2015;14(6):528–535. doi:10.1016/j.autrev.2015.01.015
54. Brandsma CA, Kerstjens HA, Geerlings M, et al. The search for autoantibodies against elastin, collagen and decorin in COPD. Eur Respir J. 2011;37(5):1289–1292. doi:10.1183/09031936.00116710
55. Cottin V, Fabien N, Khouatra C, Moreira A, Cordier JF. Anti-elastin autoantibodies are not present in combined pulmonary fibrosis and emphysema. Eur Respir J. 2009;33(1):219–221. doi:10.1183/09031936.00140208
56. Daffa NI, Tighe PJ, Corne JM, Fairclough LC, Todd I. Natural and disease-specific autoantibodies in chronic obstructive pulmonary disease. Clin Exp Immunol. 2015;180(1):155–163. doi:10.1111/cei.v180.1
57. Rinaldi M, Lehouck A, Heulens N, et al. Antielastin B-cell and T-cell immunity in patients with chronic obstructive pulmonary disease. Thorax. 2012;67(8):694–700. doi:10.1136/thoraxjnl-2011-200690
58. Viniol C, Vogelmeier CF. Exacerbations of COPD. Eur Respir Rev. 2018;27:147. doi:10.1183/16000617.0103-2017
 © 2020 The Author(s). This work is published and licensed by Dove Medical Press Limited. The full terms of this license are available at https://www.dovepress.com/terms.php and incorporate the Creative Commons Attribution - Non Commercial (unported, v3.0) License.
By accessing the work you hereby accept the Terms. Non-commercial uses of the work are permitted without any further permission from Dove Medical Press Limited, provided the work is properly attributed. For permission for commercial use of this work, please see paragraphs 4.2 and 5 of our Terms.
© 2020 The Author(s). This work is published and licensed by Dove Medical Press Limited. The full terms of this license are available at https://www.dovepress.com/terms.php and incorporate the Creative Commons Attribution - Non Commercial (unported, v3.0) License.
By accessing the work you hereby accept the Terms. Non-commercial uses of the work are permitted without any further permission from Dove Medical Press Limited, provided the work is properly attributed. For permission for commercial use of this work, please see paragraphs 4.2 and 5 of our Terms.