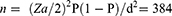Back to Journals » Infection and Drug Resistance » Volume 14
Seroprevalence of Hepatitis B Virus and Associated Factors Among Female Sex Workers Using Respondent-Driven Sampling in Hawassa City, Ethiopia
Authors Daka D , Hailemeskel G, Fenta DA
Received 2 August 2021
Accepted for publication 5 October 2021
Published 20 October 2021 Volume 2021:14 Pages 4301—4311
DOI https://doi.org/10.2147/IDR.S332333
Checked for plagiarism Yes
Review by Single anonymous peer review
Peer reviewer comments 2
Editor who approved publication: Prof. Dr. Héctor Mora-Montes
Deresse Daka,1,2 Getahun Hailemeskel,1,2 Demissie Assegu Fenta2
1School of Medical Laboratory Science, College of Medicine and Health Science, Hawassa University, Hawassa, Sidama, Ethiopia; 2Department of Medical Laboratory, Comprehensive Specialized Hospital, College of Medicine and Health Science Hawassa University, Hawassa, Sidama, Ethiopia
Correspondence: Demissie Assegu Fenta
School of Medical Laboratory Science, College of Medicine and Health Science, Hawassa University, P. O. Box: 1560, Hawassa, Sidama, Ethiopia
Tel +251 911 02 01 89
Fax +251 462 12 21 22
Email [email protected]
Background: Female sex workers (FSWs) are a marginalized group having limited healthcare access and poor-quality care. Inevitably, they are vulnerable to sexually transmitted infections including hepatitis B virus. It is one of the most serious and major public health problems, with an increased risk of transmission and acquisition of the infection. Hence, this study was aimed to assess the prevalence and associated factors of HBV infection among FSWs in southern Ethiopia.
Methods: A cross-sectional study was conducted from November to February 2019 at Hawassa city among ISHDO confidential clinics among 383 FSWs using respondent-driven consecutive sampling techniques to select study participants using a standardized questionnaire. The blood samples were collected to detect viral surface antigen using ELISA. Data were entered into SPSS version 21. Descriptive and logistic regression analysis was used.
Results: The overall prevalence of HBV was 35 (9.2%) (95% CI=6.3– 12.1). Among 381 FSWs, 249 (65.4%) of them had stayed for 2– 5 years in sexual work. A total of 240 (63%) of them used condoms consistently during sexual practice. In multivariate analysis, FSWs who did not use a condom during sexual practice were 6-times more at risk than those who used a condom (AOR=6.38, CI=2.04– 18.51). Condom breakage (AOR=2.10, CI=1.95– 4.65), use of stimulants (AOR=3.25, CI=1.59– 18.63), history of STI (AOR=2.15, CI=1.02– 6.93), and genital ulcer (AOR=4.64, CI=1.31– 11.35), number of sexual partners (AOR=3.25, CI=1.59– 7.47), sex during menses (AOR=5.85, CI=1.29– 21.44), sexual assault (AOR=2.93, CI=1.23– 9.01), sharp material sharing (AOR=4.98, CI=1.34– 10.95), and history of abortion (AOR=2.46, CI=1.18– 12.19) were statistically associated with HBV infection.
Conclusion: The prevalence of HBV infection in this study was relatively high compared to the general population. Factors like sociodemographic, behavioral, and previous information were associated with HBV infection. There is a need for ongoing screening of this high-risk population to inform planning for vaccination and preventive measures.
Keywords: hepatitis B virus, female sex workers, Hawassa, Ethiopia
Introduction
Hepatitis B virus (HBV) is a DNA virus belonging to the Hepadnaviridae family.1,2 Despite the availability of a safe and effective vaccine against hepatitis B infection for over two decades now, the overall burden of the disease remains enormous with over 2 billion people infected worldwide and approximately 1 million deaths occuring annually from HBV-related illness.1,3 According to the WHO report, over 240 and 150 million people are infected with chronic liver disease due to HBV and HCV, respectively.1
Hepatitis B virus (HBV) is endemic in sub-Saharan Africa and, despite the introduction of universal hepatitis B vaccination and effective antiviral therapy, the estimated overall seroprevalence of hepatitis B surface antigen remains high, at 6.1%.4
Hepatitis B virus (HBV) prevalence is highest in an adult population of the Western Pacific Region and Africa, where it is 6.2% and 6.1%, respectively.4,5 The prevalence of HBV infection among the general population of the Eastern Mediterranean Region, South-East Asia, Europe, and the Americas was 3.3%, 2.0%, 1.6%, and 0.7%, respectively.5 It is mentioned that Africa is one of the continents with the highest prevalence of HBV, with Ethiopia being a member of this continent and sharing the burden.1
Hepatitis B Virus (HBV) is usually transmitted through exposure to infected blood and various body fluids (saliva, menstrual, vaginal, and seminal fluids) and recycling of needles and syringes either in healthcare settings or along with persons who inject drugs. Furthermore, the infection can arise during medical, surgical, and dental procedures, through tattooing, or through the utilization of razors and related objects that are contaminated with infected blood.5
The prevalence of HBV among female sex workers in different studies conducted in African countries has been revealed as 4.2% in the Republic of Congo,6 17.1% in Nigeria,7 18.2% in Burkina Faso,8 4% in South Africa,9 and 2.5% in Ruanda.10 From limited studies in Ethiopia, the highest prevalences were reported from Gondar (28.9%),11 Mekelle (6%),12 and Dessie (13.1%).13 In other developed countries such as Brazil,14 China,15 Thailand,16 and India17 the prevalence of HBV among Female sex workers (FSWs) was 23.6%, 10.7%, 11.4%, and 3.6%, respectively.
Different factors are associated with female sex workers acquiring HBV, like workplace associated factors, inconsistent condom use, substance, and drug use,12 economic factors, marital interruption, low educational status, and unsafe alcohol use, and co-infection with other sexually transmitted infections, which are common factors associated with HBV infection.9
Sex work remains an important contributor to HBV and HIV transmission within early, advanced, and regressing epidemics in sub-Saharan Africa, and its social and behavioral factors play an important role in the transmission of these diseases.5 FSWs are more prone to HBV and other STIs as well as transmitting them to the public through their clients as they are often in a poor position to negotiate safe sex because of social, economic, cultural, and legal factors.18
In sub-Saharan Africa, FSWs constitute one of the high-risk groups for HBV and STI acquisition and transmission. This is because sex workers have numerous sex partners and engage in unprotected sex and other forms of sex that cause contact with body fluids of a partner who may be infected with HBV.19
According to 2019 EDHS data, this is a stable, low-level, generalized epidemic with marked regional variations driven by most at-risk populations (MARPs). However, urban areas and females are more affected than rural areas and males.20 Small towns are also becoming hot spots and can potentially bridge further the spread of the HIV and HBV epidemic to rural settings by such population groups. Across the country, FSW carries a disproportionate burden of HIV and HBV.20 A study conducted in Gondar and Mekelle among FSWs showed that the prevalence of HBV was 28.9% and 16%, respectively.11,12 These findings were greater than findings from the Ethiopian general population (9%),21 the adult population in southwest Ethiopia (9%),22 and from a health professional in Gondar (4.52%),23 which provides evidence that HBV infection is more prevalent among sex workers than the other population group.
Therefore, this study was planned to determine the prevalence of Hepatitis B virus infection and its predisposing factors among FSWs in one of the hot spot cities of Ethiopia – Hawassa. It could be important to emphasize the need for strengthening intervention strategies that address the risk and the marginalized group to stop the link or spread of HBV to the community through them and their sexual partners by designing vaccination schedules.
Materials and Methods
Study Area
This study was conducted in Sidama regional state of Hawassa City in one of the nongovernmental institutions founded to support marginalized populations to give integrated services on Health Development (ISHDO) project confidential clinic. Hawassa city is the central town of the regional state located 270 km from Addis Ababa at the shores of Lake Hawassa in the Great Rift Valley area of southern Ethiopia. It is known by its diverse cultural constituents, socio-economic benefit, and as a good tourist destination and recreational city, with a total population of 302,000 according to the Worldometer report of 2021.24
Study Design, Period, and Population
A cross-sectional study design was employed among adolescent and young adult female sex workers from November 31, 2019 to February 30, 2019, who are living in Hawassa city working as commercial sex workers for at least 3 months and registered in the nongovernmental institutions founded to support marginalized populations to give integrated services on Health Development (ISHDO) project confidential clinic were selected and included in the study.
A single population proportion formula was used to estimate the sample size, following the assumption to consider: 95% confidence interval (Zα/2=1:96), 50% proportion was taken due to limited data about HBV among FSWs in the area and nearby localities, and 5% margin of error.
A total of 384 female sex workers were included from eight sub-cities and from all kebeles who were pre-registered in the registration book. They were selected using a simple random sampling method by using assigned ex-sex workers, namely: “Demand creator” and preregistered FSWs to bring their counterparts by moving from home to home and brought to this special clinic were participated.
Female sex workers registered in the non-governmental institutions, founded to support marginalized populations to give an integrated service on Health Development (ISHDO) project confidential clinic, were included in the study. We have considered and defined women as FSWs when they are living and commercializing sex for the last 3 months in Hawassa City. Female sex workers with age greater than or equal to 15 years old and willing to participate in this study were included, but those FSWs with apparent mental or physical illness that limit them from an interview and those who are not available during the study period were excluded.
Specimen Collection
A simple random sampling technique was used to select 384 study participants during the study period. Before the actual data collection, we studied the average number of FSWs registered in the clinic. Then, the number of study participants who were going to be included in the study each day was allocated.
Data Collection Methods
After obtaining informed and written consent, a standardized questionnaire was used to collect the sociodemographic, behavioral, and other predisposing variables that are associated with the dependent variable. Venous blood (5 mL) was drawn under aseptic conditions by trained data collectors. The sample was labeled and processed by centrifugation at 3,500 rpm for 5 minutes to obtain the serum and stored at −20°C in a refrigerator until it was tested. HBsAg was detected from serum samples by using the AiDTM antibody sandwich HBsAg ELISA method (WANTAI HBV diagnostics AiDTM HBsAg ELISA). The test was conducted following the manufacturer’s instructions and the microplates read at a wavelength of 450 nm using the Enzyme-linked immune assay (ELISA) reader. The presence or absence of HBsAg was determined by relating the absorbance of the unknown sample to the cut-off value.
Statistical Analysis
Data were cleaned and checked and entered into SPSS version 21 for analysis. The data were analyzed using a descriptive summary using frequencies, appropriate summary tables, and cross tabs, and relevant information was summarized to present the results. Bivariate logistic regression analysis was performed to identify the factors associated with HBV infection. Variables having a P-value of <0.2 in bivariate analysis were eligible for multivariate logistic regression analysis to control potential confounding factors. A P-value of less than 0.05 is considered as statistically significant.
Result
Demographic and Socio-Economic Conditions
Of the 384 female sex workers who agreed to participate in the study, three of them were excluded because of incomplete information from the questionnaire and also were not recruited for blood sample collection. For the remaining 381 FSWs, 45.7% of the participants were within the age group of 20–24 years, with the mean and standard deviation age of the study subjects being 22.63±4.3 years. The median age was 22 and the range was 16–40 years. In total, 370 (97.1%) were single and 11 (2.9%) were previously married. Among the 381 FSWs, 242 (63.5%) of the respondents were from urban areas. According to their educational level, 306 (80.3%) of the study participants had attended formal education. More than 35% of the study participants have a monthly income within the range of 1,501–3,000 Ethiopian Birr (Table 1).
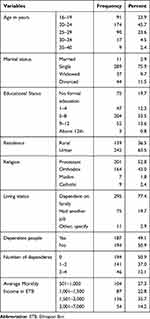 |
Table 1 Socio-Demographic Characteristics of Female Sex Workers at Hawassa City, Southern Ethiopia, 2019 (n=381) |
Sexual and Behavioral Characteristics of Female Commercial Sex Workers
The overall prevalence of FSWs who were tested for HBV using ELISA in the current study was 35 (9.2%). Among the 381 FSWs, 249 (65.4%) of them stayed for 2–5 years in sexual work. Also, 240 (63%) of them used condoms consistently during sexual practice and 308 (80.8%) had a habit of alcohol consumption. One hundred (26.2%) of them had a history of STI infection and 103 (27%) of FSWs had a steady partner. The majority of 287 (73.3%) of the study subjects used the vagina for sexual intercourse while 39 (10.2%) of them had both anal and vaginal intercourse, 55 (14.4%) used both oral and vaginal sexual practice. A total of 243 (63.8%) of the participants used injectable drugs and other stimulants to initiate their sexual desire (Table 2).
 |
Table 2 Sexual Behavior of Female Sex Workers at Hawassa, Southern Ethiopia, 2019 (n=381) |
Factors Associated with HBV Among Female Commercial Sex Workers
Many different variables were assessed for the presence or absence of an association between HBV and FSWs using both bivariate and multivariate logistic regression models. The bivariate analysis was computed independently, and we have used a cut-off P-value of 0.2 to recruit and analyze the variables in the multivariate model.
In the multivariate logistic regression model, condom use, condom breakage, use of stimulants, duration on sex work, history of STI, history of genital ulcer, the number of sexual partners, sex during menses, sexual assault, common use of sharp material, and the history of abortion had a significant association with HBV infection at a P-value<0.05 (Table 3).
 |
Table 3 Factors Associated with HBV Among Females Sex Workers at Hawassa City, Southern Ethiopia, 2019 (n=381) |
In multivariate logistic regression analysis, FSWs who did not use condoms commonly during sexual practice were more significantly associated with acquiring HBV (AOR=6.38, CI=2.04–18.51), while condom breakage (AOR=2.10, CI=1.95–4.65), use of stimulants (AOR=3.25, CI=1.59–18.63), history of STI (AOR=2.15, CI=1.02–6.93), history of genital ulcer (AOR=4.64, CI=1.31–11.35), number of clients seen per day (AOR=3.25, CI=1.59–7.47), sex during menses (AOR=5.85, CI=1.29–21.44), sexual assault (AOR=2.93, CI=1.23–9.01), sharp material sharing (AOR=4.98, CI=1.34–10.95), and history of abortion (AOR=2.46, CI=1.18–12.19) were also statistically associated with HBV infection. Factors such as age, marital status, residence, alcohol consumption, and dependent size were not significantly associated with HBV infection among FSWs in the current study (Table 3).
Ethics Approval and Consent to Participate
Ethical approval was obtained from Hawassa University Institutional Review Board (IRB) under the reference number of Ref.No IRB/026/2010 signed by the chairperson of Dr. Ayalew Astateke on December 21, 2018 and was conducted in accordance with the Declaration of Helsinki for human subjects. In this study we secured consent instead of assent in participants under the age of 18 years according to the Ethiopian National research Ethics review guideline, because early sexual practice and marriage is common in the study area, and a permission letter was obtained from the Southern Nation, Nationality, and People Regional Health Bureau to the respective health institutions. Written informed consent was obtained from each participant before data collection. After informing each respondent about the aim and purpose of the study, participants were asked for their voluntary participation. Those respondents were assured that they could withdraw from the study at any time if they felt unhappy. They were also informed that all data obtained from them would be kept confidential by using codes instead of any personal identifiers.
Discussion
Ethiopia has been classified as an HBV endemic zone.25 Although this classification gives a fair picture of the global HBV endemicity, it fails to take into account the variability of the disease within various population groups.25 Also, most information on HBV prevalence in Ethiopia is available from blood donors and pregnant women.26 In this study, the prevalence of an HBsAg marker (indicating HBV infection) among female sex workers at integrated services on Health Development project confidential clinic Hawassa was 9.2% (95% CI=6.3–12.1%).
This prevalence is higher than in many other population groups studied in Ethiopia. This is critical, owing to the fact that this group has a greater probability of transmitting and maintaining the virus in the community.
This finding was lower than the studies reported from Gondar, Ethiopia (11.9%),27 Nigeria (17.1%),28 Cameroon (36%),29 Argentina (14.4%),30 Shanghai, China (12.3%),31 and in two different studies in Brazil (17.1%32 and 23.1%).33 The current finding was higher than the studies conducted in Mekelle, Ethiopia (6%),34 Iran (1.2%),35 Rwanda (2.5%),36 Congo (7.3%),37 Italy (3.5%),38 Venezuela (3.8%),39 and Afghanistan (6.54%).40 This difference might be due to the difference between diagnostic tools, sample size, and differences in socio-demographic and socio-economic environments. Furthermore, the difference in the prevalence estimates is also likely to be influenced by stigma and discrimination and also study settings.
Compared to the prevalence general population (6%)34 it can be assumed that CSWs were more likely to have a high prevalence (9.2%) of HBV in this study. Comparing this study results with the general population indicates that there is less emphasis on this group of the population.
Regarding the prevalence of HBV according to age group of FSWs, the highest prevalence (16; 45.7%) was accounted for within the age group of 20–24 years. But, this finding was not statistically significant (P>0.05), which is inconsistent with a study conducted in Nigeria.28 On the other hand, similar findings to the current study were reported from Dessie, Ethiopia13 and Burkina Faso.8 The possible reasons may be the early onset of sexual intercourse, which represents an increased risk for sexually transmitted infections.
In this study, educational status, marital status, monthly income, vaccination, and alcohol consumption were not statistically significantly associated with HBV, similar to other studies conducted in three Afghan cities among FSWs41 in Mekelle among commercial sex workers34 and in Tehran, Iran, among FSWs.42
Sexual intercourse during menses is statistically associated with acquiring HBV infection in sex workers (AOR=5.85, 95% CI=1.29–21.44), FSW who have a history of abortion (AOR=2.46, 95% CI=1.18–12.19) and a genital ulcer (AOR=4.64, 95% CI=1.31–11.35) were 24- and 46-times more risk full than those who have not a history of abortion and genital ulcer. Similar findings were reported from Mekelle, Ethiopia,34 Brazil,43 and Nigeria.28
Sexual assault was 12-times more exposed for acquiring HBV (AOR=2.93, 95% CI=1.23–9.01); similar findings were reported from Iran41 and Nigeria.28 The number of sexual partners (AOR=3.25, 95% CI=1.59–7.47), the duration on sex work (AOR=1.84, 95% CI=1.33–2.14), and condom use (AOR=6.38, 95% CI=2.04–18.51). A similar finding was reported from Mexico.44 The possible explanation may be that multiple clients produce greater vulnerability to risks for low adherence to the use of condoms in all sexual relations.
Limitations of the current study were due to significant difficulties encountered in attempting to recruit the needed sample size from the FSWs population. Female sex workers in Ethiopia are mainly street-based, which makes it quite tough and threatening to reach them. A follow-up study with a larger sample size with a longitudinal study in the different study areas is worthwhile to add to the literature.
Conclusion
Despite the limitations in difficulties encountered in attempting to recruit the study participants, the prevalence of HBV infection among FSWs was relatively high compared to the general population in the current study. Furthermore, different factors like sociodemographic, behavioral, clinical, and previous history-related information have been also assessed for the presence of association with HBV infection. Condom use, history of genital ulcer, sexes during menses, sexual assault, history of abortion, number of sexual partners, duration of sex work, and sharing of sharp material were highly associated with HBV infection among female sex workers. Meanwhile, they are at a higher risk of acquiring HBV infection, as indicated above due to high-risk behaviors of sex practice and lack of successful HBV immunization evidence. Preparedness should be initiated to prevent the potential risk of HBV infection. Since they can be a source of infection for the community, first, a mass screening activity or a longitudinal survey study on FSWs should be done. Then, a preventive approach or vaccination schedule and appropriate treatment scheme for HBV should be developed.
Finally, the government, non-governmental organizations, civic society, and religious institutions should work together to alleviate the problem by counseling and recruiting them on other productive job sectors that are found in the country, and other large-scale studies indicating other HBV markers should be conducted for the future.
Abbreviations
ISHDO, integrated services on Health development; HBV, hepatitis B virus; HBsAg, Hepatitis B surface antigen; FSW, Female sex workers; STIs, sexually transmitted infections; AOR, Adjusted odds ratio; COR, crude odds ratio; WHO, World Health Organization.
Data Sharing Statement
The datasets used and/or analyzed during the current study are available from the corresponding author on reasonable request.
Acknowledgments
We are grateful to Hawassa University for its technical and financial support. We would also like to thank the Integrated Service on Health and Development Organization (ISHDO) for their permission and guidance to undertake this research in their organization. Finally, we also thank all participants of the study.
Author Contributions
All authors made substantial contributions to the conception and design, acquisition of data, or analysis and interpretation of data; took part in drafting the article or revising it critically for important intellectual content; agreed to submit to the current journal; gave final approval of the version to be published; and agree to be accountable for all aspects of the work.
Funding
This study was supported by Hawassa University, College of Medicine and Health Sciences. The support included payment for data collectors and the purchase of materials and supplies required for the study. The support did not include designing the study, analysis, interpretation of data, manuscript preparation, and publications.
Disclosure
The authors declare that they have no conflicts of interest both on the work and financial interest or another conflict of interest statement.
References
1. Hwang EW, Cheung R. Global epidemiology of hepatitis B virus (HBV) infection. N Am J Med Sci (Boston). 2011;4(1):7.
2. World Health Organization. World Health Statistics 2013: A Wealth of Information on Global Public Health. World Health Organization; 2013.
3. Akani C, Ojule A, Opurum H, Ejilemele A. Sero-prevalence of hepatitis B surface antigen (HBsAg) in pregnant women in Port Harcourt, Nigeria. Niger Postgrad Med J. 2005;12(4):266–270.
4. Spearman C, Afihene M, Ally R, Apica B, Awuku Y, Cunha L. Hepatitis B in sub-Saharan Africa: strategies to achieve the 2030 elimination targets. Lancet Gastroenterol Hepatol. 2017;2(12):900–909. doi:10.1016/S2468-1253(17)30295-9
5. Scorgie F, Chersich MF, Ntaganira I, Gerbase A, Lule F, Lo Y-R. Socio-demographic characteristics and behavioral risk factors of female sex workers in sub-Saharan Africa: a systematic review. AIDS Behav. 2012;16(4):920–933. doi:10.1007/s10461-011-9985-z
6. Niama FR, Bongolo NCL, Mayengue PI, et al. A study on HIV, Syphilis, and Hepatitis B and C virus infections among female sex workers in the Republic Of Congo. Archiv Public Health. 2017;75(1):1–8. doi:10.1186/s13690-017-0189-5
7. Forbi JC, Onyemauwa N, Gyar S, Oyeleye A, Entonu P, Agwale S. High prevalence of hepatitis B virus among female sex workers in Nigeria. Revista Do Instituto De Med Trop De São Paulo. 2008;50(4):219–221. doi:10.1590/S0036-46652008000400006
8. Ouedraogo HG, Kouanda S, Goodman S, et al. Hepatitis B, C and delta viruses’ infections and correlate factors among female sex workers in Burkina Faso, West-Africa. Open Virol J. 2019;13(1):9–17. doi:10.2174/1874357901913010009
9. Scheibe A, Young K, Versfeld A, et al. Hepatitis B, hepatitis C, and HIV prevalence and related sexual and substance use risk practices among key populations who access HIV prevention, treatment, and related services in South Africa: findings from a seven-city cross-sectional survey (2017). BMC Infect Dis. 2020;20(1):1–15. doi:10.1186/s12879-020-05359-y
10. Mutagoma M, Nyirazinyoye L, Sebuhoro D, Riedel DJ, Ntaganira J. Syphilis and HIV prevalence and associated factors to their co-infection, hepatitis B and hepatitis C viruses prevalence among female sex workers in Rwanda. BMC Infect Dis. 2017;17(1):1–9. doi:10.1186/s12879-017-2625-0
11. Moges F, Kebede Y, Kassu A, et al. Seroprevalence of HIV, hepatitis B infections and syphilis among street dwellers in Gondar city, Northwest Ethiopia. Ethiop J Health Dev. 2006;20(3):136–205.
12. Bugssa G, Dessalegn B, Dimtsu B, Berhane Y. Prevalence and factors associated with HIV and hepatitis B virus infections among female commercial sex workers in Mekelle, Ethiopia: cross-sectional study. Int J Pharm Sci Res. 2015;6(1):135.
13. Metaferia Y, Ali A, Eshetu S, Gebretsadik D, Mishra N. Seroprevalence and associated factors of human immunodeficiency virus, treponema pallidum, hepatitis B virus, and hepatitis C virus among female sex workers in Dessie City, Northeast Ethiopia. Biomed Res Int. 2021;2021:1–13. doi:10.1155/2021/6650333
14. Passos ADC, Figueiredo JFDC, Martinelli ADLC. Hepatitis B among female sex workers in Ribeirão Preto – São Paulo, Brazil. Rev Bras Epidemiol. 2007;10:517–524. doi:10.1590/S1415-790X2007000400010
15. Su S, Chow EP, Muessig KE, et al. Sustained high prevalence of viral hepatitis and sexually transmissible infections among female sex workers in China: a systematic review and meta-analysis. BMC Infect Dis. 2015;16(1):1–10. doi:10.1186/s12879-015-1322-0
16. Hongjaisee S, Khamduang W, Sripan P, et al.Prevalence and factors associated with hepatitis B and D virus infections among migrant sex workers in Chiangmai, Thailand: a cross-sectional study. Int J Infect Dis. 2019;100(2020):247–254.
17. Risbud SM, Basu S, Kulkarni S, et al. Prevalence and incidence of hepatitis B virus infection in STD clinic attendees in Pune, India. Sex Transm Infect. 2002;78:169–173. doi:10.1136/sti.78.3.169
18. Remple VP, Patrick DM, Johnston C, Tyndall MW, Jolly AM. Clients of indoor commercial sex workers: heterogeneity in patronage patterns and implications for HIV and STI propagation through sexual networks. Sex Transm Dis. 2007;34(10):754–760. doi:10.1097/01.olq.0000261327.78674.cb
19. Lawan U, Abubakar S, Ahmed A. Risk perceptions, prevention and treatment-seeking for sexually transmitted infections and HIV/AIDS among female sex workers in Kano, Nigeria. Afr J Reprod Health. 2012;16:61–67.
20. Central statistical agency (CSA)[Ethiopia] and ICF. Ethiopia demographic and health survey, Addis Ababa, Ethiopia and Calverton, Maryland, USA. 2016.
21. Gebreselassie L. Prevalence of specific markers of viral hepatitis A and B among an Ethiopian population. Bull World Health Organ. 1983;61(6):991.
22. Belay AS, Abateneh DD, Yehualashet SS, Kebede KM. Hepatitis B virus infection and associated factors among adults in Southwest Ethiopia: community-based cross-sectional study. Int J Gen Med. 2020;13:323. doi:10.2147/IJGM.S259375
23. Gebremariam AA, Tsegaye AT, Shiferaw YF, Reta MM, Getaneh A. Seroprevalence of hepatitis B virus and associated factors among health professionals in University of Gondar Hospital, Northwest Ethiopia. Adv Prev Med. 2019;2019:1–5. doi:10.1155/2019/7136763
24. Review WP. Ethiopia population 2021. Woldometer report. 2021.
25. WHO. Global Policy Report on the Prevention and Control of Viral Hepatitis: In WHO Member States. Geneva: WHO; 2013.
26. Tegegne DDK, Tegbaru B, Tegbaru B, et al. Seroprevalence and transmission of Hepatitis B virus among delivering women and their newborn in selected health facilities, Addis Ababa, Ethiopia: a cross-sectional study. BMC Res Notes. 2014;7(1):2–7. doi:10.1186/1756-0500-7-239
27. Moges F, Kebede Y, Kassu A, et al. Seroprevalence of HIV, Hepatitis B infections and Syphilis among street dwellers in Gondar city, Northwest Ethiopia. Ethiop J Health Dev. 2006;20. doi:10.4314/ejhd.v20i3.46836
28. Forbi JC, Onyemauwa N, Gyar SD, Oyeleye AO, Entonu P, Agwale SM. High prevalence of hepatitis B virus among female sex workers in Nigeria. Rev Inst Med Trop S Paulo. 2008;50:219–221.
29. PEPFAR. Cameroon operational plan report. 2011.
30. María A, Pando CB, Bibini M, et al. Prevalence of HIV and other Sexually transmitted infections among female commercial sex workers in Argentina. Am J Trop Med Hyg. 2006;74:233–238. doi:10.4269/ajtmh.2006.74.233
31. Zhang TYY, Yu F, Yu F, et al. Kaposi’s sarcoma-associated herpesvirus infection among female sex workers and general population women in Shanghai, China: a cross-sectional study. BMC Infect Dis. 2014;14:58. doi:10.1186/1471-2334-14-58
32. Matos MA, França DD, Carneiro MA, et al. Viral hepatitis in female sex workers using the respondent-driven sampling. Rev Saude Publica. 2017; 51:65.
33. Schuelter-Trevisol F, Custodio G, Silva ACBD, Oliveira MBD, Wolfart A, Trevisol DJ. HIV, hepatitis B and C, and syphilis prevalence and coinfection among sex workers in Southern Brazil. Revista Da Sociedade Brasileira Trop. 2013;46:493–497. doi:10.1590/0037-8682-1364-2013
34. Bugssa G, Dessalegn B, Dimtsu B, Berhane Y. Prevalence and factors associated with HIV and Hepatitis B virus infection among female commercial sex workers in Mekelle, Ethiopia: cross-sectional study. IJPSR. 2015;6:135–146.
35. Moayedi-Nia S, Esmaeeli Djavid G, Esmaeeli Djavid G, et al. HIV, HCV, HBV, HSV, and syphilis prevalence among female sex workers in Tehran, Iran, by using respondent-driven sampling. AIDS Care. 2016;28:487–490. doi:10.1080/09540121.2015.1109582
36. Mutagoma MNL, Sebuhoro D, Sebuhoro D, et al. Syphilis and HIV prevalence and associated factors to their co-infection, hepatitis B and hepatitis C viruses prevalence among female sex workers in Rwanda. BMC Infect Dis. 2017;17:525.
37. Niama FR, Bongolo NC, Mayengue PI, et al.A study on HIV, Syphilis, and hepatitis B and C virus infections among female sex workers in the Republic of Congo BMC. Archiv Public Health. 2017; 75.
38. Monica Zermiani CM, Rimondo C, Rimondo C, et al. Prevalence of sexually transmitted diseases and hepatitis C in a survey of female sex workers in the North-East of Italy. Open AIDS J. 2012;6:60–64. doi:10.2174/1874613601206010060
39. Camejo MI, Diaz M. Prevalence of hepatitis B, hepatitis C, and syphilis in female sex workers in Venezuela. Rev Saúde Publica. 2003;37:339–344.
40. Catherine S, Todd AN, Mohammad R, et al. HIV, hepatitis B, and hepatitis C prevalence and associated risk behaviors among female sex workers in three Afghan Cities. AIDS. 2010;24:S69–S75. doi:10.1097/01.aids.0000386736.25296.8d
41. Todd CS, Nasir A, Stanekzai MR, et al. HIV, hepatitis B, and hepatitis C prevalence and associated risk behaviors among female sex workers in three Afghan cities. AIDS (London, England). 2010;24(2):S69.
42. Nasirian M, Kianersi S, Hoseini SG, et al. Prevalence of sexually transmitted infections and their risk factors among female sex workers in Isfahan, Iran: a cross-sectional study. JIAPAC. 2017;16(6):608–614. doi:10.1177/2325957417732836
43. Matos MA, França DD, Carneiro MA, et al. Viral hepatitis in female sex workers using the respondent-driven sampling. Rev Saude Publica. 2017;51:65.
44. Juárez-Figueroa LU, Conde-Glez C, Conde-Glez C, et al. Low prevalence of hepatitis B markers among Mexican female sex workers. Sex Transm. 1998;74:448–450. doi:10.1136/sti.74.6.448
 © 2021 The Author(s). This work is published and licensed by Dove Medical Press Limited. The
full terms of this license are available at https://www.dovepress.com/terms.php
and incorporate the Creative Commons Attribution
- Non Commercial (unported, v3.0) License.
By accessing the work you hereby accept the Terms. Non-commercial uses of the work are permitted
without any further permission from Dove Medical Press Limited, provided the work is properly
attributed. For permission for commercial use of this work, please see paragraphs 4.2 and 5 of our Terms.
© 2021 The Author(s). This work is published and licensed by Dove Medical Press Limited. The
full terms of this license are available at https://www.dovepress.com/terms.php
and incorporate the Creative Commons Attribution
- Non Commercial (unported, v3.0) License.
By accessing the work you hereby accept the Terms. Non-commercial uses of the work are permitted
without any further permission from Dove Medical Press Limited, provided the work is properly
attributed. For permission for commercial use of this work, please see paragraphs 4.2 and 5 of our Terms.