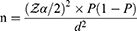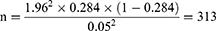Back to Journals » Diabetes, Metabolic Syndrome and Obesity » Volume 15
Self-Care Practice and Associated Factors Among Patients with Type 2 Diabetes Mellitus at a Referral Hospital in Northern Ethiopia – A Mixed Methods Study
Authors Zewdie S , Moges G , Andargie A , Habte BM
Received 20 May 2022
Accepted for publication 22 September 2022
Published 6 October 2022 Volume 2022:15 Pages 3081—3091
DOI https://doi.org/10.2147/DMSO.S373449
Checked for plagiarism Yes
Review by Single anonymous peer review
Peer reviewer comments 2
Editor who approved publication: Prof. Dr. Muthuswamy Balasubramanyam
Segenet Zewdie,1 Getachew Moges,1 Assefa Andargie,2 Bruck Messele Habte3
1Department of Pharmacy, College of Medicine and Health Sciences, Wollo University, Dessie, Ethiopia; 2School of Public Health, College of Medicine and Health Sciences, Wollo University, Dessie, Ethiopia; 3School of Pharmacy, College of Health Sciences, Addis Ababa University, Addis Ababa, Ethiopia
Correspondence: Bruck Messele Habte, School of Pharmacy, College of Health Sciences, Addis Ababa University, P. O. Box 9086, Addis Ababa, Ethiopia, Tel +251 911 626356, Email [email protected]
Introduction: Diabetes self-care is important to maintain optimal glycemic control and prevent debilitating and costly complications. Diabetes self-care may be improved through the identification of individual and group barriers to regimen adherence and subsequent development of specific plans to overcome these barriers. This study assessed the self-care practice and associated factors among type 2 diabetes patients attending their treatment at Dessie Referral Hospital, Dessie, North-Eastern Ethiopia.
Methods: The study employed parallel mixed methods design which followed a cross-sectional interview and in-depth interview methods, respectively, from September to October 2019. The collected data were subjected to descriptive and inferential analysis for the quantitative part and a thematic analysis for the qualitative part.
Results: A total of 328 type 2 diabetes patients participated in the study of which 50.3% reported good self-care practice. Being in the age category of 60– 69 years old (AOR = 0.334, 95% CI (0.135, 0.951)), being ≥ 70 years old (AOR = 0.359, 95% CI (0.135, 0.951)), having complications (AOR = 1.956, 95% CI (1.172, 3.262)), having co-morbidity (AOR = 0.443, 95% CI (0.262, 0.749)) and diabetes education (AOR = 2.684, 95% CI (1.633, 4.412)) were significantly associated with good diabetes self-care. Accessibility, social support, knowledge and beliefs and diabetes-related morbidities were identified as barriers to diabetes self-care by the patients.
Conclusion: The findings from this study revealed that only half of the type 2 diabetes patients who participated in this study reported good self-care practice. Different factors, including diabetes education, were significantly associated with good diabetes self-care according to the quantitative study. This was supported by the findings from the qualitative part and thus the recommendation to strengthen diabetes health education to patients and their families.
Keywords: type 2 diabetes mellitus, barriers to self-care practice, diabetes education, mixed methods study, Ethiopia
Introduction
Diabetes mellitus (DM) is one of the rapidly growing health problems of the 21st century. The International Diabetes Federation (IDF) reported that an estimated 537 million people, ie, 10.5%of adults aged 20–79 years, globally live with DM. This figure will increase to 643 million adults by 2030 and 783 million by 2045 according to the 2021 edition of IDF Diabetes Atlas. In Africa, more than 24 Rmillion people live with DM and this figure is expected to increase by 129% to 55 million in 2045. Ethiopia is among the top five countries in Africa with regard to the number of people with DM. According to the latest IDF Atlas, 1.9 million people live with DM in 2021 which is a 36% increase compared to a decade back. About 26,448 adults aged 20–79 years old are reported to have died in relation to DM in Ethiopia in 2021.1
Diabetes self-care (DSC) is a critical factor to keep the disease under control and reduce premature death. About 95% of this care, including self-monitoring of blood glucose, nutrition, physical activity, adherence to medication and foot care is usually carried out by the affected individual or their families.2 DSC is positively associated with good glycemic control, reduced DM-related complications, and improved quality of life. DM patients have been shown to make a significant impact on the prognosis of their disease by participating in their care.3,4 Different factors affect patients with DM and their families’ ability to practice self-care activities including access to health care, communication with health-care providers, patient characteristics, psychosocial adjustment (like stress, depression and distress), and education or behavioral support tailored to individual/family needs.3
There are a few studies conducted on DSC practice and associated factors in Ethiopia. Accordingly, the prevalence of good DSC practice in Ethiopia ranges from 25.5% to 76.8%5,6 indicating a significant variation across studies. However, none of these studies used mixed method and went further to explore some of these factors like payment type and counseling regarding DMSCA that influence DSC. Moreover, the factors identified in previous studies were not consistent from study to study. Hence, this study aimed at assessing DSC practice and associated factors as well as the barriers as perceived by the patients.
Methods
The study was conducted at Dessie Referral Hospital DM Clinic from 20 September to 20 October 2019. The hospital is located in Amhara regional state about 401 km northeast of the Ethiopian capital, Addis Ababa. The study employed a concurrent mixed-methods approach. For the quantitative part, an institution-based cross-sectional study was employed to determine the DSC practice and its associated factors whereas, a descriptive qualitative design7 was employed to explore barriers to DM self-care.
Participants’ Recruitment
All adults (aged 18 years and above) type 2 DM patients attending the DM clinic and were accessible during the time of data collection in the hospital were eligible to participate in the study. However, DM patients who had hearing and speech problems, and those with severe illness were excluded. A total of 344 DM patients participated in the quantitative study by using single population formula.
where
n = the required sample size.
Zα/2=the standard normal distribution score at (100-α) confidence level which is 1.96 for 95% confidence level.
P = the population proportion which is taken 28.4% in a similar study conducted in Bahir Dar.8
d = the margin of error for the population proportion, taken to be 0.05
Adding 10% non-response rate the total sample size becomes 344.
The number of participants for the qualitative interview were 13 type 2 DM patients determined by information saturation.
Participants were approached when they came to the hospital for their monthly follow-up. After patients were identified as type 2 DM from their card, they were selected using systematic sampling at every other patient. On average 25 patients come to follow up per day. Based on this, 12 patients were selected for interview. The first respondent was selected by using a lottery method from the first two patients who arrived at the hospital on the start date of data collection. Participants for the qualitative interview were selected purposively from among the quantitative study participants considering their sex, age, time of their diagnosis and the recommendations of health-care professionals working at the DM clinic.
Data Collection Procedure
The quantitative data were collected through an exit interview using a semi-structured Amharic language questionnaire (Supplementary File-English version data collection tools) which took 30 days. The questionnaire consists of 6 parts which included socio-demographic characteristics (like sex, age, marital status, educational level) diabetes history, medical history, diabetes knowledge test (DKT2), social support, and summary of diabetes self-care activities (SDSCA). The DKT2 questionnaire contains 23 items on areas of diet, glucose control, DM treatment, exercise, foot care, and complications.9 However, only 13 items were selected which were deemed appropriate for the Ethiopian context. The DSC practice was evaluated by self-reported revised SDSCA scale. The tool consists of a core set of 11 items along with the expanded list of 14 additional questions. The scale measures the frequency of self-care activities in the last 7 days on a general and specific diet, physical activity, blood glucose testing, foot care, and medication. The SDSCA is the most widely used self-report instrument for measuring DM self-management in adults.10 This study used only 13-items of the tool to consider the Ethiopian context. As to the social support part, six items were used for this study that was adapted from the Social Support Assessment Tool.11 All the tools were pre-tested and their reliability and validity assessed before the actual data collection.
Two trained BSc nurses were employed to collect quantitative data which on average took 35 minutes to complete. The qualitative data, which on average took 50 minutes to complete, was collected using Amharic language interview guide prepared to explore the barriers of DSC by the first author (Supplementary File-English version data collection tools) which took five days. The interview was audio-recorded along with note-taking so as not to miss out on the interview data.
Diabetes self-care practice includes a range of activities including self-monitoring of blood glucose, eating a low-saturated-fat diet, physical exercise, adherence to recommended medication, and checking one’s feet.10 It is measured by taking respondents’ report on the frequency with which they performed various activities over the previous 7 days. The mean score of each participant was calculated for the five domains by summing the frequency with which they performed each activity domain and divided by the number of questions of each domain. When the domain-specific mean score was summed up and divided by the total number of participants, it provides a domain-specific overall mean score. Then the domain-specific DSC practice was categorized as good if a participant has a mean score of greater than or equal to the overall domain-specific mean score and poor if it is below the domain-specific mean score. The overall DSC practice was measured by computing the overall mean DSC score. It was calculated by summing up the mean scores (the sum of the frequencies divided by the total number of questions in all domains) for each individual divided by the total number of participants. Using the overall mean score, which was 3.93 days, the level of DSC practice was categorized as good or poor practice.
Knowledge of DM was defined as awareness of participants regarding DM. The median score, which was found to be 6, was used to classify the knowledge level of participants. Good knowledge was defined as score greater than or equal to the median score (≥6) and Poor knowledge was measured as score below the median score (<6).
Social support was about whether the participant has any one around to help him/her when needed. Using a 6-item Likert scale questionnaire scored from 1 to 5, a participant may have a minimum of 6 and a maximum of 30 sum scores. Then the median score was used to determine whether a participant has good or poor social support. Good social support was defined as score of greater than or equal to the median score (≥17) and poor social support refers to score below the median score (<17).
Data Analysis
Following completion of the data collection, questionnaires were checked for completeness and consistency, and data were entered using Epi Data version 4.6.0.0, then transferred to SPSS version 25 for analysis. After checking for missing values, outliers, and distributions, descriptive statistics like frequencies, percentages and other summary measures were computed and presented in texts, tables and graphs. Binary logistic regression was used to measure the association between independent variables and DSC. Those variables with a p-value of below 0.2 in the bivariate analysis were fitted to multiple logistic regression and variables with a p-value of below 0.05 were considered statistically significant factors. Finally, the crude and adjusted odds ratios with the respective 95% confidence intervals were reported and interpreted. The audio recorded qualitative data was first transcribed verbatim, and then translated to the English language by the first author. The data was then analyzed manually using thematic analysis method. Codes and categories emerged that facilitated interpretation. Finally, the findings were reported in textual narrations and quotations as a supplement to the quantitative findings.
Results
Socio-Demographic Characteristics
A total of 328 Type 2 DM patients provided valid responses out of the 344 approached resulting in 95% response rate. From all participants, 55.2% were females and 28.4% were in the age category 50–59 years with a mean age of 55±11.9 years. About 63.1% respondents were married and 72.6% were urban residents. The occupation of 40.9% participants were privately employed and 31.7% of the participants cannot read and write (see Table 1).
 |
Table 1 Socio-Demographic Characteristics of Type 2 Diabetes Patients in Dessie Referral Hospital, 2019 (n = 328) |
Diabetes Care and History
The mean duration of DM was 7 years with SD of ±5.7 years. 48.5% respondents had DM duration between 1 and 5 years, 82% study participants had no family history of DM, and 75.3% respondents took oral hypoglycemic agents. Of all participants, 47.3% had DM-related complications and 43% had other comorbidities. Nearly 37.8% patients got DM education in different ways, 17.4% individuals were members of the Ethiopian Diabetes Association, and 68.6% participants got counseling services related to DSC from health-care professionals. A total of 45.7% participants got DM care through the out-of-pocket payment scheme (see Table 2).
 |
Table 2 DM Care and History of DM Patients at Dessie Referral Hospital, 2019 (n = 328) |
Diabetes Knowledge and Social Support
A total of 55.2% participants had good DM knowledge and the same percentage of respondents had good social support (see Table 3).
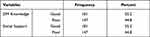 |
Table 3 Knowledge and Social Support Status of DM Patients at Dessie Referral Hospital, 2019 (n = 328) |
Diabetes Self-Care Practice
The findings revealed that 54.9% and 39.3% of the respondents, respectively, had good diet adherence and exercise practice, respectively, for the last seven days which was less than the 82.3% who reported good adherence to their medication regimens. The overall self-care practice was found to be good amongst 50.3% of the study participants (Figure 1).
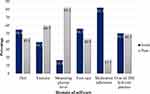 |
Figure 1 Self-care practice of DM patients at Dessie Referral Hospital, 2019 (n = 328). |
Factors Associated with Diabetes Self Care Practice
Lower levels of DSC practice were associated with higher age levels, 60–69 years (AOR 0.334, 95% CI 0.135, 0.823), age ≥70 years (AOR 0.359, 95% CI 0.135, 0.951), having other comorbid conditions (AOR 0.443, 95% CI 0.262, 0.749) and DM-related complications (AOR 1.956, 95% CI 1.172–3.262). On the other hand, higher levels of DSC practice were associated with getting DM education (AOR 2.684 95% CI1.633–4.412) at p-value <0.05. There was no evidence, however, that employment status, occupation type, educational level, having glucometer at home for self-monitoring of blood glucose, being a member of diabetic association and payment type were significantly associated with type 2 diabetes patients' self-care practice (see Table 4).
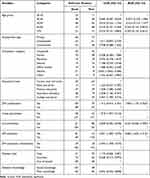 |
Table 4 Factors Associated with Overall Diabetes Self-Care Practice in Dessie Referral Hospital, 2019 (n = 328) |
Barriers to Diabetes Self Care Practice
A total of 13 DM patients participated in the qualitative interview study. The participants’ age ranged from 33 to 75 years, with about half being male. Their duration of diagnosis ranged from 1 to 25 years. With regard to their medication regimen, twelve participants were on oral hypoglycemic agents, while the remaining was on insulin.
The major barriers to DSC practice that were identified include accessibility issues both geographic and financial affordability, lack of social or family support, having diabetes-related complications and other co-morbid conditions, limited awareness towards diabetes self-care and lack of self-control.
Accessibility Issues
Most of the participants lived in the rural parts of the country where fruits and vegetables are scarcely produced and also had meager income. Some of the participants thus described how they cannot eat fruits and vegetables even once in a week.
I get to eat fruits and vegetables rarely when my families go to market…there are no fruits and vegetables in our village. (70 years, male)
Social Support Issues
Lack of social support was expressed in the form of absence to remind them to take or help in purchasing their medications and not sharing in household chores which were identified as barriers to diabetes self-care practice by some participants.
Sometimes, I forget to take my medications and took when I remember them. This is because there is no one around to remind me to take my medication… Furthermore, I had finished my medication yesterday and I told my husband to buy from the nearby pharmacy, but he refused to buy as he is careless towards me. Eventually, I missed the night dose. (45 years, female)
Diabetes-Related Morbidities
Some participants also cited diabetes-related complications and other comorbid conditions as barriers from engaging in their daily physical exercises.
My exercise habit is not good. In addition to my diabetes, I also have kidney disease… because of this I felt ill when I tried to walk. (58 years, female)
The participants further mentioned stress, anxiety and fatigue as reasons to forget taking their medication.
Sometimes I forgot my DM medication at the regular time and take it as I remember…my sickness has made me stressful. (64 years, female)
The participants also explained issues related to loss of their appetite as a barrier to adhere to the recommended diet.
When I lost my appetite, I took a soft drink to boost my appetite. (65 years, female)
Sometimes I lose my appetite, at that time I miss my breakfast and take large amount of food at lunchtime. (45 years, female)
Knowledge and Beliefs
Patients’ knowledge and beliefs and lack of self-control were also mentioned as barriers to DSC. Lack of awareness regarding the DSC components such as exercise, diet, foot care and blood glucose monitoring and not appreciating the importance of adhering to these elements were expressed by the patients.
I believe that exercise have no contribution in controlling blood glucose level, rather it is advised for patients with hypertension. (40 years, male)
The doctors did not tell me the importance of fruits and vegetables for DM patients. Until now, I have not eaten fruits and vegetables because I was afraid it will increase my blood glucose level. (58 years, female)
I didn’t check the inside part of my foot frequently because it has no wound. (60 years, male)
On the other hand, lack of self-control was identified by the respondents as a barrier for diabetes self-care.
I like fatty meat rather than red meat, and so I usually eat fatty meat. (45 years, female)
Discussions
The study findings revealed that only half of the DM patients included in the study had a good overall self-care practice. This proportion was apparently similar to those who demonstrated good DM knowledge. The findings also demonstrated significant positive association between those who got DM education and higher levels of DSC practice. The qualitative component likewise supported these findings whereby participants expressed lack of awareness regarding the DSC components such as diet and exercise.
The findings with regard to the overall self-care practice were similar to studies reported from Ethiopian regions West Shoa Zone,12 Jimma13 and Benishangul Gumuz.14 Whereas, it is higher than studies conducted at Tigray Region (Ayder hospital) (25.5%),5 Central zone of Tigray (37.3%)15 and Bahir Dar (28.4%).8 On the other hand, a higher good self-care practice was reported from Debre Tabor, Ethiopia (63.1%).16
Good DM knowledge was associated with good overall self-care practice although it was not statistically significant. This finding is similar to the findings from other local studies13,16,17 as well as studies reporting from other parts of the globe.18,19 These studies cite about knowledge deficiencies, inconsistent information sources and at times “misconceptions” with regard to the details of recommendations regarding appropriate diets and physical exercises. The recommendations in this regard are for appropriate, culturally appropriate and cost-effective interventions that address the knowledge deficits and misconceptions.
On the other hand, the study findings revealed that attending diabetes education was significantly associated with good DSC practice similar to studies reported from other parts of the country.14–16 This finding is further supported by the qualitative finding, in which lack of awareness regarding the recommended DSC practice elements was identified as a barrier. The need to strengthen existing education programs and exploration of innovative education programs to improve patients’ knowledge on the recommended treatment regimens, their self-care practices and ultimately their health outcomes is unarguable.19,20 Due consideration also has also to be made to ensure the validity of existing educational programs as there are literature reports of a program from a Middle Eastern country that was suboptimal and not addressing specific patient needs.21
It was also apparent from the study findings that there were positive significant associations between DM patients who had complications and a good self-care practice similar to findings from other studies including local ones.22,23 The low risk perception of complications among DM patients may make them reluctant to practice recommended self-care. This phenomenon may also be the basis to have a group diabetes education program where patients are able to share experiences, where those who have not yet experienced such complications may be able to have first-hand experiences from those who have.
In fact, peer education programs have been demonstrated to be a viable option to improve self-care practices and health outcomes.19,24 Such diabetes peer groups were described to serve as, “platforms to interact and share information of self-management of diabetes” according to a qualitative study reported from an African setting.25 The idea of peer support program is in fact not new to the Ethiopian healthcare system. There are reports of the use of “health development army” and “women development army” in both the urban and rural areas to serve as a community engagement platform for health-related issues as part of the health extension package – considered as the pillar of the country’s primary healthcare system. In this case, women who have received special training would be actively engaged so as to train other women and the community members on different health topics.26 Thus, the use of peer support which is not new to the Ethiopian healthcare system may be an idea for future intervention study to assess the feasibility and cost-effectiveness.
The Strengths and Limitations of the Study
This study used a standardized validated questionnaire albeit with omissions of a few items to measure self-care practice and knowledge level, which allowed the finding to be comparable with previous studies. Furthermore, we used a mixed methods approach which enabled us to identify factors related to diabetes self-care practice quantitatively and subjectively perceived barriers qualitatively. Self-care practice was determined through self-report which may be liable to recall and social desirability bias. In addition, due to the very nature of cross-sectional design, the temporal relationship between the factors and the outcome cannot be ascertained.
Practical Implications
The low level of overall self-care practice is worrying and needs the attention of health practitioners and policy makers. Strengthening existing DM education programs is of critical importance. In addition to strengthening the existing programs, it is worth exploring alternative and cost-effective programs such as the peer support programs that can improve the self-care practices and health outcomes.
Conclusions
Our study findings revealed poor diabetes self-care practices in about half of the study participants which are bound to lead to worsening of their health conditions. The self-care practices have been shown to have benefited from access to diabetes education which is indicative of the need to strengthen such educational programs and explore innovative ways to address patient needs.
Abbreviations
DM, Diabetes Mellitus; DSC, Diabetes Self-care; IDF, International Diabetes Federation; SDSCA, Summary of Diabetes Self-care Activities.
Data Sharing Statement
The tools that were used for both the quantitative and qualitative parts of the study are included as additional files. The datasets that were generated during the current study are not publicly available due to reasons of confidentiality and anonymity.
Ethical Approval and Consent to Participate
The study was done in accordance with the principles of the Declaration of Helsinki. Ethical approval was obtained from Research Ethics Committee of the College of Medicine and Health Sciences, Wollo University (CMHS/013/519/12) that was followed by permissions from the administrator of the study hospital prior to starting data collection. Oral informed consents were obtained using pre-prepared information and consent form from all participants before the data collection. This consent process which used plain language and was also approved by the Research Ethics Committee of Wollo University (CMHS/013/519/12) involved information about the purpose of the study, procedures to be followed, confidentiality issues, anticipated benefits and harms/discomforts that participation in the study entails including possible publication of anonymized responses, and the voluntary nature of the participation with the full right to refuse and withdraw their participation at any time. The oral consent process is customary in the study setting for such type of observational studies where majority of the population have low educational status and tries to avoid written consents and signatures which may be considered “risky”.
Acknowledgments
The authors acknowledge the data collectors for their devotion in collecting the data. Furthermore, they wish to express their appreciation to the study participants for their keen and honest response. The authors also would like to acknowledge the Michigan Diabetes Research Center (MDRC), University of Michigan Medical School, which was supported by Grant Number P30DK020572 (MDRC) from the National Institute of Diabetes and Digestive and Kidney Diseases for permitting use of the DKT2 and the Oregon Research Institute for permitting use of the SDSCA survey instruments, respectively.
Author Contributions
All authors made a significant contribution to the work reported, whether that is in the conception, study design, execution, acquisition of data, analysis and interpretation, or in all these areas; took part in drafting, revising or critically reviewing the article; gave final approval of the version to be published; have agreed on the journal to which the article has been submitted; and agree to be accountable for all aspects of the work.
Funding
The source of funding which was part of the graduate study of the first author was Wollo University.
Disclosure
The authors declare that they have no competing interests.
References
1. International Diabetes Federation. IDF Diabetes Atlas 10th edition. International Diabetes Federation; 2021. Available from: https://diabetesatlas.org/idfawp/resource-files/2021/07/IDF_Atlas_10th_Edition_2021.pdf.
2. Anderson R, Funnell M, Butler P, Arnold M, Fitzgerald J, Feste C. Patient empowerment. Results of a randomized controlled trial. Diabetes Care. 1995;18:943–949. doi:10.2337/diacare.18.7.943
3. Whittemore R, Vilar-compte M, La Cerda SD, et al. Challenges to diabetes self-management for adults with type 2 diabetes in low- resource settings in Mexico City: a qualitative descriptive study. Int J Equity Health. 2019;18(133):1–10. doi:10.1186/s12939-019-1035-x
4. Shrivastava S, Shrivastava R, Saurabh P, Ramasamy J. Role of self-care in management of diabetes mellitus. J Diabetes Metab Disord. 2013;12(14):1–5. doi:10.1186/2251-6581-12-14
5. Niguse H, Belay G, Fisseha G, Desale T, Gebremedhn G. Self-care related knowledge, attitude, practice and associated factors among patients with diabetes in Ayder Comprehensive Specialized Hospital, North Ethiopia. BMC Res Notes. 2019;12(34):1–7. doi:10.1186/s13104-019-4072-z
6. Addisu Y, Eshete A, Hailu E. Assessment of diabetic patient perception on diabetic disease and self-care practice in Dilla University Referral Hospital, South Ethiopia. Metab Syndr. 2015;3:4. doi:10.4172/2167-0943.1000166
7. Colorafi KJ, Evans B. Qualitative descriptive methods in health science research. Heal Environ Res Des J. 2016;9(4):16–25. doi:10.1177/1937586715614171
8. Abate TW, Tareke M, Tirfie M. Self ‑ care practices and associated factors among diabetes patients attending the outpatient department in Bahir Dar, Northwest Ethiopia. BMC Res Notes. 2018;11(800):4–8. doi:10.1186/s13104-018-3874-8
9. Fitzgerald JT, Funnell MM, Anderson RM, et al. Validation of the revised brief Diabetes Knowledge Test (DKT2). Diabetes Educ. 2016;42(2):178–187. doi:10.1177/0145721715624968
10. Toobert DJ, Hampson SE, Glasgow RE. The summary of diabetes self-care activities measure: results from 7 studies and a revised scale. Diabetes Care. 2000;23(7):943–950. doi:10.2337/diacare.23.7.943
11. La Clinica de La Raza. Social support. Social support assessment tool; 2005. Available from: http://www.diabetesinitiative.org/resources/topics/documents/8-LAC-SocialSupportToolEnglish_web.pdf.
12. Gurmu Y, Gela D, Aga F. Factors associated with self-care practice among adult diabetes patients in West Shoa Zone, Oromia Regional State, Ethiopia. BMC Health Serv Res. 2018;18(732):4–11. doi:10.1186/s12913-018-3448-4
13. Kassahun T, Gesesew H, Mwanri L, Eshetie T. Diabetes related knowledge, self-care behaviours and adherence to medications among diabetic patients in Southwest Ethiopia: a cross-sectional survey. BMC Endocr Disord. 2016;16(28). doi:10.1186/s12902-016-0114-x
14. Chali SW, Salih MH, Abate AT. Self - care practice and associated factors among diabetes mellitus patients on follow up in Benishangul Gumuz Regional State Public Hospitals, Western Ethiopia: a cross‑sectional study. BMC Res Notes. 2018;11(833):1–8. doi:10.1186/s13104-018-3939-8
15. Mariye T, Tasew H, Teklay G, Gerensea H, Daba W. Magnitude of diabetes self‑care practice and associated factors among type two adult diabetic patients following at public Hospitals in central zone, Tigray Region, Ethiopia, 2017. BMC Res Notes. 2018;11(380):1–6. doi:10.1186/s13104-018-3489-0
16. Tiruneh SA, Ayele AA, Emiru YK, Tegegn HG. Factors influencing diabetes self-care practice among type 2 diabetes patients attending diabetic care follow up at an Ethiopian General Hospital, 2018. J Diabetes Metab Disord. 2019;18:199–206. doi:10.1007/s40200-019-00408-z
17. Ayele AA, Emiru YK, Tiruneh SA, Ayele BA, Gebremariam AD, Tegegn HG. Level of adherence to dietary recommendations and barriers among type 2 diabetic patients: a cross-sectional study in an Ethiopian hospital. Clin Diabetes Endocrinol. 2018;4(1):1–7. doi:10.1186/s40842-018-0070-7
18. Mphwanthe G, Carolan M, Earnesty D, Weatherspoon L. Perceived barriers and facilitators to diet and physical activity among adults diagnosed with type 2 diabetes in Malawi. Glob Public Health. 2020;16(3):469–484. doi:10.1080/17441692.2020.1805784
19. Sohal T, Sohal P, King-Shier KM, Khan NA, Barengo NC. Barriers and facilitators for type-2 diabetes management in south asians: a systematic review. PLoS One. 2015;10(9):1–15. doi:10.1371/journal.pone.0136202
20. Tan JP, Cheng KKF, Siah RCJ. A systematic review and meta-analysis on the effectiveness of education on medication adherence for patients with hypertension, hyperlipidaemia and diabetes. J Adv Nurs. 2019;75(11):2478–2494. doi:10.1111/jan.14025
21. Aloudah NM, Scott NW, Aljadhey HS, Araujo-Soares V, Alrubeaan KA, Watson MC. Medication adherence among patients with type 2 diabetes: a mixed methods study. PLoS One. 2018;13(12):1–18. doi:10.1371/journal.pone.0207583
22. Van Puffelen AL, Heijmans MJWM, Rijken M, Rutten GEHM, Schellevis FG. Illness perceptions and self-care behaviours in the first years of living with type 2 diabetes; does the presence of complications matter? Psychol Health. 2015;37–41. doi:10.1080/08870446.2015.1045511
23. Ayele BH, Mengesha MM, Tesfa T. Predictors of self-care activities of outpatient diabetic residents in Harar and Dire Dawa: a hospital-based cross-sectional study. SAGE Open Med. 2019;7:1–10. doi:10.1177/2050312119865646
24. Yin J, Wong R, Au S, et al. Effects of providing peer support on diabetes management in people with type 2 diabetes. Ann Fam Med. 2015;13:S42–S49. doi:10.1370/afm.1853
25. Mphwanthe G, Weatherspoon D, Kalimbira A, Weatherspoon L. Non-dietary factors associated with glycemic status among adults diagnosed with type 2 diabetes mellitus in Malawi. Soc Work Public Heal. 2020;35(6):380–391. doi:10.1080/19371918.2020.1785367
26. Ethiopian Federal Ministry of Health. Annual Performance Report 2012. Vol. 1. Ethiopian Federal Ministry of Health; 2020.
 © 2022 The Author(s). This work is published and licensed by Dove Medical Press Limited. The
full terms of this license are available at https://www.dovepress.com/terms.php
and incorporate the Creative Commons Attribution
- Non Commercial (unported, v3.0) License.
By accessing the work you hereby accept the Terms. Non-commercial uses of the work are permitted
without any further permission from Dove Medical Press Limited, provided the work is properly
attributed. For permission for commercial use of this work, please see paragraphs 4.2 and 5 of our Terms.
© 2022 The Author(s). This work is published and licensed by Dove Medical Press Limited. The
full terms of this license are available at https://www.dovepress.com/terms.php
and incorporate the Creative Commons Attribution
- Non Commercial (unported, v3.0) License.
By accessing the work you hereby accept the Terms. Non-commercial uses of the work are permitted
without any further permission from Dove Medical Press Limited, provided the work is properly
attributed. For permission for commercial use of this work, please see paragraphs 4.2 and 5 of our Terms.