Back to Journals » Nutrition and Dietary Supplements » Volume 10
Role of nutrients in metabolic syndrome: a 2017 update
Authors Kern HJ, Mitmesser SH
Received 12 August 2017
Accepted for publication 7 December 2017
Published 28 February 2018 Volume 2018:10 Pages 13—26
DOI https://doi.org/10.2147/NDS.S148987
Checked for plagiarism Yes
Review by Single anonymous peer review
Peer reviewer comments 4
Editor who approved publication: Dr Chandrika J Piyathilake
Hua J Kern, Susan Hazels Mitmesser
The Nature’s Bounty Co., Ronkonkoma, NY, USA
Abstract: Metabolic syndrome (MetS) and its associated chronic disorders including cardiovascular disease and type 2 diabetes are public health concerns in the USA and worldwide. “Good health is an investment in economic growth,” and nutrition is one of the recommended preventive measures to manage these chronic diseases. However, it is unclear whether and to what extent nutrients could be beneficial to the improvement of MetS. To help answer this question, we performed a literature review of the emerging human data on single nutrients and MetS: PubMed was searched from January 1, 2005 to June 12, 2017, using a combination of the following keywords: “nutrient” OR “vitamin” OR “mineral” OR “nutraceutical” AND “metabolic syndrome.” The summary of literature comprises macronutrients (proteins/amino acids, fatty acids, fibers, and sugar), micronutrients (antioxidant vitamins, vitamin D, folate, magnesium, and chromium), polyphenols (flavonoids, resveratrol, isoflavones, and chlorogenic acid), and other compounds (α-lipoic acid, benfotiamine, fucoxanthin, policosanol, and stanols). Bearing a holistic approach in mind, we also highlighted select lifestyle factors that may contribute to MetS (such as circadian rhythm and nutrition in early life). Observational studies have generated positive evidence supporting the beneficial role of numerous nutrients in MetS. Although the results of some clinical trials are consistent with the observational data, causality is not always clear or consistent across trials. Both nutrition and health are complex and dynamic systems with a hierarchical nature. When we design confirmatory trials to investigate nutrient(s) and MetS, instead of the traditional “single-nutrient” concept, it is worth considering a holistic approach to integrate groups or classes of nutrients, lifestyle influencers (ie, diet and physical activity), and population relevance (ie, healthy, at-risk, or diseased).
Keywords: nutrient, metabolic syndrome, obesity, hypertension, dyslipidemia, insulin resistance
Introduction
Metabolic syndrome (MetS) is a constellation of interrelated metabolic abnormalities that are major risk factors for the development of cardiovascular disease (CVD) and type 2 diabetes mellitus (T2DM). There are various definitions of MetS (eg, World Health Organization, the International Diabetes Federation, and the US National Cholesterol Education Program’s Adult Treatment Panel III [NCEP/ATP III]).1 The most widely used definition (from the NCEP/ATP III) is defined as the presence of three or more of the following metabolic disorders: central obesity (waist circumference: ≥102 cm for men, ≥88 cm for women), dyslipidemia (high-density lipoprotein cholesterol [HDL]: <40 mg/dL for men, <50 mg/dL for women; or triglycerides [TGs] ≥150 mg/dL), hypertension (systolic/diastolic blood pressure ≥130/85 mmHg), and insulin resistance (elevated fasting blood glucose ≥110 mg/dL).2
MetS and its associated chronic diseases are public health concerns in the USA and worldwide. About 34% of US adults have MetS,3 and 9.3% of the US population (29.1 million) are diabetic.6 MetS is associated with an increase in risks of developing CVD and T2DM over the next 5–10 years.4 Each year, one in every four deaths among Americans is attributed to heart disease, totaling about 610,000 deaths annually.5 The annual combined cost (direct and indirect expenditures) of CVD (hypertension, heart disease, and stroke) and diabetes in the USA was $650 billion in 2003 and is projected to be $1.96 trillion by 2023.7 Prevention and early management of MetS may help manage these disease burdens and the associated health care cost worldwide.
“Good health is an investment in economic growth,”7 and nutrition is one of the recommended preventive measures to help manage chronic morbidities.8 However, it is unclear whether and to what extent single nutrients could be beneficial to MetS. To help address this question, we reviewed relevant literature in the past decade and summarize emerging human data for single nutrients’ influence on MetS in this review.
Literature search methods
We searched PubMed from January 1, 2005 to June 12, 2017, by using a combination of the following keywords: “nutrient” OR “vitamin” OR “mineral” OR “nutraceutical” AND “metabolic syndrome.” Table S1 summarizes the reviews, systematic reviews, and meta-analyses of human data published in English.
The focus of this review is on the specific role of individual nutrients in the prevention or treatment of MetS among US adults. In the section of “Literature summary/Discussion,” individual nutrients are grouped into one of the following four categories: macronutrients, micronutrients, polyphenols, and other compounds. Specific dietary patterns, food groups, gene/drug–nutrient interactions, biochemical/molecular mechanism, or pediatric studies are not included in the present review.
Literature summary/discussion
Figure 1 summarizes the literature data on key nutrients and MetS parameters
Macronutrients
Proteins/amino acids
A review of human acute feeding trials and relevant meta-analyses concludes that, compared with lower-protein diets, higher-protein energy-restriction diets containing 1.2–1.6 g protein/kg/day improve appetite, weight management (eg, loss of fat mass while maintaining lean muscle), and some cardiometabolic risk factors (eg, lowering fasting TGs) over a short term (<1 year).9,10 The long-term data (≥1 year) are less consistent primarily due to discrepant dietary compliance, but there is persistent evidence supporting the benefits of increased protein consumption on weight maintenance.9,10 Hypothesized mechanisms of action include an increase in thermogenesis and metabolic rate and a modest satiety effect after the consumption of protein-rich meals.9,10
Certain amino acids including glutamine derivatives, alanine and arginine, may influence pancreatic β-cell function (eg, insulin secretion), but the mechanism is not completely understood.11 Human studies report that consumption of dairy products rich in branched-chain amino acids (BCAAs; leucine, isoleucine, and valine) or whey/casein protein is associated with improved diabetic parameters (eg, fasting insulin levels) among obese and T2DM individuals.11,12
When human subjects with hypercholesterolemia consumed lupin protein (25 g/day) with a mixed diet for 28 days, their plasma levels of total cholesterol (TC), TGs, and low-density lipoprotein cholesterol (LDL) decreased.2 Animal or in vitro data have reported benefits of peptides (synthesized or extracted from dietary proteins) for lipid metabolism, but human data are limited.
Fatty acids
According to recent evidence, saturated and trans fatty acids have deleterious influences on metabolic health.4,13–15 In contrast, unsaturated fatty acids including monounsaturated fatty acids and omega-3/omega-6 polyunsaturated fatty acids (PUFA) improve metabolic parameters (eg, blood pressure, lipid profile, glycemic control, and insulin sensitivity). 4,13–15 Diets rich in conjugated linoleic acid (CLA), in particular the cis-9 trans-11-CLA isomer, have been shown to improve the markers of metabolic and insulin sensitivity in adipose tissue and liver, indicating a potential benefit for metabolic health.15 It is important to note that these benefits are linked to the consumption of the dietary components as part of a specific diet, suggesting a need for human studies to confirm the benefit of single nutrients.13 In addition, more data are needed to define the optimal composition of dietary fatty acids (eg, amount and type) to which metabolic health will be affected.4
The Japanese have the highest intake of omega-3 fatty acids in the world. Even in this population, omega-3 and omega-6 fatty acids have been reported to provide some protection against cardiac and major coronary events.16 Based on evidence from randomized controlled trials (RCTs), the American Heart Association concluded that omega-3 fatty acids have been demonstrated to reduce the risks of CVD events in patients with coronary artery diseases.14 While there is little direct evidence that omega-3 PUFA supplementation affects insulin sensitivity in humans, epidemiological studies found that habitual fish intake is associated with the reduced incidence of T2DM.15
Fiber
Observational data indicate an inverse relationship between dietary fiber intake (from cereals and whole grain) and body weight/diabetes/CVD.14 According to a meta-analysis of six prospective studies, an increase in whole grain consumption by two servings per day may reduce the risk of diabetes by 21%.14 Fiber is commonly classified as soluble or insoluble, based on its solubility in water. Soluble dietary fiber is associated with improved glycemic control and insulin sensitivity in both diabetic and healthy subjects, generally attributable to its viscous properties. It, however, does not appear to reduce the risk of T2DM.14 In contrast, insoluble fiber reduces the risk of diabetes, even though it has negligible influence on postprandial glucose levels.14
Sugar
Sugar-sweetened beverages (SSBs) contain caloric sweeteners such as sucrose, high-fructose corn syrup, or fruit juice concentrates and are the primary source of added sugar in the US diet.17 A meta-analysis pooled data from 11 prospective cohort studies and included 19,431 participants for MetS (5,803 cases) and 310,819 for T2DM (15,043 cases). Compared with individuals who rarely consume SSB (none or <1 serving/month), those who consumed one to two servings per day were at a higher risk of developing MetS (relative risk [RR] =1.20; 95% confidence interval [CI] =1.02–1.42) and T2DM (RR =1.26; 95% CI =1.12–1.41).17 In addition, a longitudinal cohort followed >88,000 women for 24 years and found that consumption of ≥2 SSBs/day was associated with a 35% increased risk for coronary heart disease compared with infrequent consumers (RR =1.35; 95% CI =1.1–1.7).17 A number of prospective cohort studies have also reported positive associations between SSB consumption and incidence of hypertension.17
In response to convincing evidence linking SSBs to metabolic disorders, organizations such as the American Heart Association have called for reducing the consumption of SSBs. In addition, the US Food and Drug Administration (US FDA) announced new food-labeling rules stating that the content of added sugar must be called out on food labels in the near future. Low-energy sweeteners are emerging as a potential replacement for traditional sugar. In vivo human studies have extensively studied the influence of this group on metabolic health and indicate inconsistent evidence linking low-energy sweeteners to unfavorable metabolic changes (eg, increased appetite, altered glucose homeostasis, or blood pressure).18
Micronutrients
Antioxidant vitamins
Systemic inflammation and oxidative stress are core mechanisms connecting energy overload and obesity to insulin resistance and consequent metabolic disorders.14,19 Antioxidant compounds can modulate oxidative stress and potentially prevent health complications that are associated with oxidative damage.19 As an example, vitamin A in the form of retinol not only influences immune function, but can also reverse chronic inflammation by reducing the level of adipocytokines according to in vitro and in vivo data.20 Animal data indicate retinol-binding protein (RBP4; the transport protein for retinol) concentrations are inversely related to insulin sensitivity. Furthermore, obese or diabetic individuals are found to have increased serum levels of RBP4.20
Epidemiological studies have found that diets rich in antioxidants (such as vitamin C, vitamin E, and β-carotene) have advantageous effects on glucose metabolism and the prevention of diabetes19 and are associated with a reduced risk of CVD.16 Observational data further suggest that higher dietary intake or supplementation of antioxidants (vitamins A, C, and E, folic acid, niacin, β-carotene, selenium, and zinc) reduces CVD-related mortalities and morbidities over a minimum of 2-year intervention.16 Furthermore, natural forms of these vitamins may be more efficacious than synthetic forms.14,21 However, RCTs indicate mixed results regarding the role of any single antioxidant or a combination of antioxidants in metabolic health.14,21
Vitamin D
T2DM is associated with systemic inflammation, impaired insulin secretion, and insulin resistance.20 Experimental data indicate that vitamin D improves pancreatic function through the induction of insulin synthesis in the islet cells, stimulating the expression of insulin receptors, regulating calcium influx into pancreatic β cells, and inhibiting the generation of proinflammatory cytokines to decrease systemic inflammation.20 It is estimated that 25%–57% of US adults and 1 billion people worldwide are vitamin D-insufficient or vitamin D-deficient,22 with ethnic minorities having higher prevalence of vitamin D insufficiency compared with Caucasian counterparts.23
Many observational data (including US National Health and Nutrition Examination Survey [NHANES]) have reported that vitamin D status (dietary intake and blood concentrations) is inversely related to the risk or prevalence of MetS, hypertension, obesity, T2DM, and CVD.16,20,22–26 A meta-analysis pooled data from 18 prospective studies with a total sample size of 210,107 participants (15,899 metabolic events) and a median follow-up of 10 years (range =3–22 years). Compared with individuals with the lowest baseline vitamin D level (bottom third), those with the highest baseline vitamin D status (top third) were at a lower risk of developing MetS (RR =0.86; 95% CI =0.80–0.92) and T2DM (RR =0.81; 95% CI =0.71–0.92).25,27 Similarly, another meta-analysis of observational and clinical trials concluded an inverse association between vitamin D status, calcium or dairy intake, and the prevalence or incidence of MetS/T2DM (odds ratios [ORs] comparing highest to lowest 25-hydroxyvitamin D [25(OH)D]: 0.36 [95% CI =0.16–0.80] for T2DM prevalence and 0.82 [95% CI =0.72–0.93] for T2DM incidence; ORs for highest vs lowest calcium/diary intake: 0.71 [95% CI =0.57–0.89] for MetS prevalence and 0.86 [95% CI =0.79–0.93] for MetS incidence).28 Furthermore, a meta-analysis of 16 cross-sectional studies reported an increment of 25 nmol/L blood 25(OH)D to be associated with a risk reduction of 13% for MetS among adults aged ≥18 years (OR =0.87; 95% CI =0.83–0.92).29 It should be noted that this inverse association does not appear to be significant in cohort or nested case–control studies (n=2), suggesting that more longitudinal and RCT data are needed to confirm causality.29
The benefits of vitamin D supplementation on MetS and related medical conditions are not conclusive. For combined vitamin D and calcium supplementation, intervention trials suggest a benefit only in high-risk populations (eg, with glucose intolerance).28 Vitamin D supplementation among high-risk individuals is reported to reduce the incidence of T2DM, indicating a protective role against diabetes.28 However, results from RCTs have not shown consistent clinical improvement when supplemented with vitamin D, which may be due to a small sample size, an inappropriate vitamin D dose, baseline vitamin D status inconsistency, gene polymorphism (eg, related to vitamin D receptor), and/or poor compliance.20,30,31 Therefore, vitamin D supplementation is not recommended for the prevention or treatment of diabetes due to insufficient evidence.31 Well-designed intervention trials targeting generally healthy and at-risk populations are needed to confirm causality.27,31
Folate and Biotin
Epidemiological data have linked folate deficiency to an increased risk and incidence of CVD. Furthermore, serum folate levels appear to be lower among overweight or obese people, indicating a relationship between folate status and adiposity.32 However, temporal and causal associations remain uncertain. Future studies focusing on populations with low folate status and folate supplementation as the primary prevention measures are recommended.
A potential synergy between biotin and folic acid in repressing proinflammatory cytokines has been reported in some cell culture experiments.20 Relevant human data are currently lacking.
Magnesium
Magnesium is the fourth most abundant essential mineral in the body and is involved in >300 metabolic reactions, including protein/DNA/RNA synthesis, cellular energy production, and cell growth and reproduction.33 There is evidence indicating the effective use of magnesium in the treatment of certain medical conditions, including eclampsia, preeclampsia, migraine, severe asthma, and constipation.33
A recent meta-analysis of 34 RCTs (2,028 participants) revealed magnesium supplementation at a median dose of 368 mg/day for a median duration of 3 months to be associated with a reduction of 2 mmHg (95% CI =0.43–3.58) and 1.78 mmHg (95% CI =0.73–2.82) in systolic and diastolic blood pressure, respectively,34 suggesting an anti-hypertensive effect with magnesium supplementation.
Diabetic patients appear to have a higher incidence of hypomagnesaemia than nondiabetics (14%–48% vs 3%–15%, respectively),35 and epidemiological data suggest an inverse correlation between a magnesium-rich diet and fasting insulin level and risk of diabetes.14,36 In a recent meta-analysis of 13 prospective cohort studies (536,318 subjects and 24,516 diabetes cases), magnesium intake was inversely correlated to the risk of T2DM (RR =0.78; 95% CI =0.73 –0.84) in a dose–response manner.39 Magnesium supplementation has been demonstrated to improve insulin sensitivity and metabolic control among people with T2DM or insulin resistance in a few RCTs.35,36
Dietary magnesium intakes and serum levels are inversely associated with the risk of CVD and all-cause mortality according to observational data and a meta-analysis of 19 prospective studies (532,979 participants).35 Cross-sectional and prospective studies also report that low urinary magnesium excretion, an indicator of dietary magnesium intake, is associated with a higher risk of developing hypertension and CVD.35 However, clinical trials have not confirmed such beneficial effects of magnesium supplementation.35 In addition, observational data indicate an inverse association between magnesium status and the risk of MetS among adults, but this potential benefit needs further investigation.33–37
Chromium
Trivalent chromium is the form found in foods and nutrient supplements, with chromium picolinate considered the most stable and bioavailable supplemental form in the market.38 It is difficult to assess the intakes of chromium from food sources partially due to the lack of standardized analytical methods, and chromium dietary intake data are currently not available in standard databases (eg, NHANES).38
Individuals with diabetes are found to have lower tissue levels of chromium than nondiabetic controls, with low circulating chromium being associated with the incidence of T2DM.38 Clinical trials have shown that chromium supplementation improves glycemic control in patients with diabetes, but this benefit is not found in other trials.14 Given limited and controversial data to date, the American Diabetes Association and US FDA have concluded the evidence for the benefit of chromium supplementation in individuals with diabetes as inconclusive.14,38
Polyphenols
Flavonoids
Flavonoids are polyphenols commonly found in fruits, vegetables, legumes, herbs, and tea and have been examined for their anti-inflammatory and antioxidant properties. Prospective studies indicate that the intake of flavonoids is inversely associated with CVD incidence or mortality.14 Similarly, a systematic review confers favorable benefits of foods rich in flavonoids, including cocoa, chocolate, red wine, grapes, or black tea on CVD parameters (eg, reduced blood pressure and improved endothelial function).14
Resveratrol
Resveratrol is a polyphenol found in a variety of fruits (eg, grapes, berries, and plums) and may have a beneficial effect on cardiovascular health via its antioxidant properties and regulation of nitric oxide concentrations in the body.16 Consumption of resveratrol at both 10 and 100 mg/day has been linked to decreased LDL and improved endothelial cell function.21 Recently, a favorable effect of trans-resveratrol on glucose homeostasis has been reported at a dose of 150 mg/day over a 1-month intervention period, indicating a potential benefit on insulin sensitivity.19 In animal studies, resveratrol has also been shown to decrease fat mass via inhibiting adipocyte differentiation and lipid accumulation and to improve energy efficiency via the regulation of brown fat tissue activity.39 However, human data are needed to further explore the influence of resveratrol on weight management.
Isoflavones
Isoflavones from soy are a class of phytoestrogens that can mimic the effects of estradiol.14 Animal studies have shown that soy and phytoestrogens reduce adiposity and improve insulin sensitivity, but human data are limited and inconclusive.14
Chlorogenic acid (CGA)
Also known as 5-O-caffeoylquinic acid, is one of the main polyphenols that is widely distributed in foods including apples, coffee beans, and carrots. This ingredient and its derived compounds have been extensively evaluated both in in vivo and in human studies for its role in the prevention and treatment of MetS and its associated disorders.40 As described below in detail, these data have revealed beneficial effects on weight management, T2DM, and hypertension when supplemented with pure CGA or CGA-rich foods/supplements. 1) Consumption of Coffee Slender (45 mg CGA/g) for 12 weeks significantly reduced weight by 5.4 kg among overweight subjects.40 A CGA-rich beverage (329 mg CGA/185 mL) was reported to increase postprandial energy expenditure and fat utilization after 4 weeks of daily consumption among healthy men;40 2) a review summarizing findings from five human trials demonstrated a positive impact of CGA-rich foods and supplements or pure CGA on diabetic parameters (eg, glucose absorption).40 Consumption of caffeinated (40 mg CGA/g) and decaffeinated coffee (30 mg CGAs/g) decreased glucose-dependent insulinotropic polypeptide, indicating a lowered rate of glucose absorption in the intestine. Coffee Slender (45 mg CGA/g) reduced glucose absorption by 6.9% among healthy subjects. Similar benefits on plasma glucose and area under the curve were observed for a CGA-rich extract from decaffeinated green coffee bean (13.9% CGA dry weight) among healthy subjects with the highest postprandial glucose levels. Emulin™ (a patented blend of CGA, myricetin, and quercetin) was reported to lower the glycemic impact of foods among subjects with T2DM; and 3) the anti-hypertension properties of pure CGA and CGA-rich green coffee extract have been investigated in subjects with and without mild hypertension. A health benefit has been reported in these human studies, including a reduction in systolic/diastolic blood pressure and improved endothelial function measured by continuous flow-mediated dilation.40
Other compounds
α-Lipoic acid
The supplementation of α-lipoic acid (a naturally occurring antioxidant) has been shown to increase insulin sensitivity among diabetics by 18%–20% and improve acute symptoms and disease progression of diabetic neuropathy.14
Benfotiamine
Benfotiamine is a lipophilic derivative of thiamine (vitamin B1) and can increase plasma concentrations of thiamine five times higher than an equivalent dose of thiamine.20 In clinical trials, benfotiamine has been demonstrated to prevent vascular endothelial dysfunction and oxidative stress and improve polyneuropathy among diabetic patients.20
Fucoxanthin
Fucoxanthin is a natural carotenoid found in certain types of brown algae, including Undaria pinnatifida (Wakame), Saccharina japonica (Makonbu), and Sargassum fulvellum (Hondawara).41 It cannot be converted to vitamin A in the body and is a potent antioxidant.41 Fucoxanthin acts by downregulating adipokine secretion that is associated with inflammation in white adipose tissue (WAT) and upregulating glucose transporter 4 that is associated with insulin resistance in skeletal muscle under diabetic conditions.41 Animal data indicate that fucoxanthin may reduce excess abdominal fat by inducing the expression of uncoupling protein 1 and thus upregulate thermogenesis in abdominal WAT.41 In a clinical trial, obese women with a mean body weight of 100 kg were administered 2.4 mg/day of fucoxanthin for 16 weeks and showed a significant increase in resting energy expenditure and a reduction in body weight, waist circumference, body and liver fat content, and serum triacylglycerol levels.41
Policosanol
Policosanol is an extract from sugarcane wax and has been shown to significantly reduce LDL cholesterol.16 It has been reported that policosanol reduced LDL by 17% among patients who did not reach their LDL target at the maximum dose of statin or with a combination therapy.16 In a recent meta-analysis of 11 human RCTs, a specific combination of natural compounds (policosanol, berberine, red yeast rice extract, folic acid, coenzyme Q10, and astaxanthin) was supplemented to examine the benefit on the lipid profile among 3,924 hypercholesterolemic patients. This combination of compounds was reported to significantly reduce all lipid parameters (TC, HDL, LDL, and TG) compared with control.42
Stanols
Stanols, also known as plant sterols, have been shown to decrease LDL cholesterol by reducing the uptake of cholesterol in the gastrointestinal tract; an optimal intake of ~2000 mg stanols daily is expected to decrease LDL by 6%–20%.16
Lifestyle factors
Although the focus of this review is single nutrients, we highlight a few lifestyle factors that may influence or “program” the development of MetS.
Circadian rhythm
According to a review of human and animal data, circadian disruption is associated with metabolic disorders.43 As illustrated in night-shift workers and those with jetlag, desynchronization between the light-regulated central clock, located in the hypothalamic suprachiasmatic nucleus, and nutrient-responsive peripheral clock can contribute to unfavorable health outcomes (including obesity, T2DM, and CVD).43 The influence of dietary components (eg, a high-fat diet and polyphenols) on tissue-specific peripheral clock responses has been investigated using animal, in vitro, and in vivo models, suggesting that feeding is a modulator of the internal circadian clock.43 Further human studies are needed to clarify which nutrients can influence and how they can influence the circadian rhythm toward advantageous metabolic outcomes.43
Nutrition in early life
Epidemiological studies have demonstrated that nutrition in early life is associated with MetS, obesity, and diabetes later in adulthood; this is known as the theory of “developmental origins of health and disease” proposed by Barker in the early 1990s.44–47 Both maternal undernutrition and overnutrition during pregnancy are correlated with suboptimal infant birth weight (underweight or overweight), altered postnatal growth (eg, rapid catch-up growth among low–birth-weight infants), and an increased risk of adulthood obesity and MetS.44–46 Low birth weight is associated with reduced fetal and adulthood muscle mass and consequently increased risks of MetS, T2DM, and CVD later in life. This is in part due to the fact that skeletal muscle is critical to maintaining resting energy expenditure and whole-body insulin sensitivity.48 In addition, childhood infection and growth restriction may contribute to future metabolic and CVDs, possibly due to caloric deficit and infection-related inflammation.49
Although weaning and the introduction of complementary feeding can influence the future health of infants, the relationship between the timing of complementary feeding and the risk of metabolic disorders later in life remains unclear.50 However, what is clear is that overconsumption of high-calorie beverages during infancy is associated with childhood obesity.50 The addition of salt during infancy may also increase the risk of hypertension later in life, as it may stimulate the development of a preference for salty taste and subsequent high intake of salt.50 Although there is evidence showing improved blood pressure among infants who received fish oil supplementation,50 there is limited literature about the long-term effects of long-chain omega-3 PUFA during weaning on cardiovascular health.50
Conclusion
Observational studies have generated positive evidence for the beneficial role of numerous nutrients in MetS. The underlying mechanisms include modulation of systemic inflammation, oxidative stress, pancreatic functions, energy absorption/production/utilization, and genetic programming in early life. Although results of some clinical trials are consistent with the findings from observational data, causality remains inconclusive due to either overall contradicting data or an inability to repeat findings or compare findings due to variance in dose, population, and clinical end points.
Both nutrition and health are complex and dynamic systems with a hierarchical nature. Nutrients are essential for health, but they do not work in isolation. When we, as nutrition scientists, design confirmatory intervention trials for nutrients and metabolic health, instead of the traditional “single-nutrient” concept, it is worth considering a holistic and interdisciplinary approach to integrate nutrients, lifestyle factors (eg, dietary patterns, physical activity, and circadian rhythm), early risk exposure (eg, in uterus and infancy), and population relevance (eg, healthy, at-risk, or diseased).
Acknowledgment
An abstract of this paper was presented at “The 2017 Experimental Biology Conference” as a poster presentation. Thereafter, the abstract was published in the FASEB Journal (available from: http://www.fasebj.org/content/31/1_Supplement/789.10.short).
Disclosure
HJK is an employee of the Nature’s Bounty Co. SHM was an employee of the Nature’s Bounty Co. when the work was performed. The authors report no other conflicts of interest in this work.
References
McCullough AJ. Epidemiology of the metabolic syndrome in the USA. J Dig Dis. 2011;12(5):333–340. | ||
Udenigwe CC, Rouvinen-Watt K. The role of food peptides in lipid metabolism during dyslipidemia and associated health conditions. Int J Mol Sci. 2015;16(5):9303–9313. | ||
Ervin RB. Prevalence of metabolic syndrome among adults 20 years of age and over, by sex, age, race and ethnicity, and body mass index: United States, 2003–2006. National Health Statistics Reports; no 13. Hyattsville, MD: National Center for Health Statistics. 2009. | ||
Phillips CM. Nutrigenetics and metabolic disease: current status and implications for personalised nutrition. Nutrients. 2013;5(1):32–57. | ||
Writing Group Members; Mozzafarian D, Benjamin EJ, et al. Heart Disease And Stroke Statistics-2016 Update: a report from the American Heart Association. Circulation. 2016;133:e38–e360. | ||
Centers for Disease Control and Prevention. National Diabetes Statistics Report 2014. Atlanta, GA: Centers for Disease Control and Prevention,US Department of Health and Human Services. 2017. | ||
DeVol R, Bedroussian A. Research report: an unhealthy America: the economic burden of chronic disease. Santa Monica CA: Milken Institute. 2017. Available at: http://www.milkeninstitute.org/publications/view/321. | ||
Brenseke B, Prater MR, Bahamonde J, Gutierrez JC. Current thoughts on maternal nutrition and fetal programming of the metabolic syndrome. J Pregnancy. 2013;2013:368461. | ||
Leidy HJ, Clifton PM, Astrup A, et al. The role of protein in weight loss and maintenance. Am J Clin Nutr. 2015; 101 (Suppl):1320S–9S. | ||
Keller U. Dietary proteins in obesity and in diabetes. Int J Vitam Nutr Res. 2011;81(2–3): 125–133. | ||
Newsholme P, Cruzat V, Arfuso F, Keane K. Nutrient regulation of insulin secretion and action. J Endocrinol. 2014;221(3):R105–R120. | ||
Dugan CE, Fernandez ML. Effects of dairy on metabolic syndrome parameters: a review. Yale J Biol Med. 2014;87(2):135–147. | ||
Calton EK, James AP, Pannu PK, Soares MJ. Certain dietary patterns are beneficial for the metabolic syndrome: reviewing the evidence. Nutr Res. 2014;34(7):559–568. | ||
Davi G, Santilli F, Patrono C. Nutraceuticals in diabetes and metabolic syndrome. Cardiovasc Ther. 2010;28(4):216–226. | ||
Roche HM. Fatty acids and the metabolic syndrome. Proc Nutr Soc. 2005;64(1):23–29. | ||
Whayne TF Jr, Maulik N. Nutrition and the healthy heart with an exercise boost. Can J Physiol Pharmacol. 2012;90(8):967–976. | ||
Malik P, Popkin BM, Bray GA, Després JP, Willett WC, Hu FB. Sugar-sweetened beverages and risk of metabolic syndrome and type 2 diabetes: a meta-analysis. Diabetes Care. 2010;33(11):2477–2483. | ||
Renwick AG, Molinary SV. Sweet-taste receptors, low-energy sweeteners, glucose absorption and insulin release. Br J Nutr. 2010;104:1415–1420. | ||
Avignon A, Hokayem M, Bisbal C, Lambert K. Dietary antioxidants: do they have a role to play in the ongoing fight against abnormal glucose metabolism? Nutrition. 2012;28(7–8):715–721. | ||
Dakshinamurti K. Vitamins and their derivatives in the prevention and treatment of metabolic syndrome diseases (diabetes). Can J Physiol Pharmacol. 2015;93(5):355–362. | ||
Xu YJ, Tappia PS, Neki NS, Dhalla NS. Prevention of diabetes-induced cardiovascular complications upon treatment with antioxidants. Heart Fail Rev. 2014;19(1):113–121. | ||
Makariou S, Liberopoulos EN, Elisaf M, Challa A. Novel roles of vitamin D in disease: what is new in 2011? Eur J Intern Med. 2011;22(4):355–362. | ||
Renzaho AM, Halliday JA, Nowson C. Vitamin D, obesity, and obesity-related chronic disease among ethnic minorities: a systematic review. Nutrition. 2011;27(9):868–879. | ||
Cosenso-Martin LN, Vilela-Martin JF. Is there an association between vitamin D and hypertension? Recent Pat Cardiovasc Drug Discov. 2011;6(2):140–147. | ||
Penckofer S, Kouba J, Wallis DE, Emanuele MA. Vitamin D and diabetes: let the sunshine in. Diabetes Educ. 2008;34(6):939–940, 942, 944 passim. | ||
Mozos I, Marginean O. Links between vitamin D deficiency and cardiovascular diseases. Biomed Res Int. 2015;2015:109275. | ||
Khan H, Kunutsor S, Franco OH, Chowdhury R. Vitamin D, type 2 diabetes and other metabolic outcomes: a systematic review and meta-analysis of prospective studies. Proc Nutr Soc. 2013;72(1):89–97. | ||
Pittas AG, Lau J, Hu FB, Dawson-Hughes B. The role of vitamin D and calcium in type 2 diabetes. A systematic review and meta-analysis. J Clin Endocrinol Metab. 2007;92(6):2017–2029. | ||
Ju SY, Jeong HS, Kim DH. Blood vitamin D status and metabolic syndrome in the general adult population: a dose-response meta-analysis. J Clin Endocrinol Metab. 2014;99(3):1053–1063. | ||
Barengolts E. Vitamin D role and use in prediabetes. Endocr Pract. 2010;16(3):476–485. | ||
Garbossa SG, Folli F. Vitamin D, sub-inflammation and insulin resistance: a window on a potential role for the interaction between bone and glucose metabolism. Rev Endocr Metab Disord 2017;18:243–258. | ||
da Silva RP, Kelly KB, Al Rajabi A, Jacobs RL. Novel insights on interactions between folate and lipid metabolism. Biofactors. 2014;40(3):277–283. | ||
Guerrera MP, Volpe SL, Mao JJ. Therapeutic uses of magnesium. Am Fam Physician. 2009;80(2):157–162. | ||
Zhang X, Li Y, Del Gobbo LC, et al. Effects of magnesium supplementation on blood pressure-a meta-analysis of randomized double-blind placebo-controlled trials. Hypertension. 2016;68(2):324–333. | ||
Floege J. Magnesium in CKD: more than a calcification inhibitor? J Nephrol. 2015;28(3):269–277. | ||
Volpe SL. Magnesium, the metabolic syndrome, insulin resistance, and type 2 diabetes mellitus. Crit Rev Food Sci Nutr. 2008;48(3):293–300. | ||
He K, Song Y, Belin RJ, Chen Y. Magnesium intake and the metabolic syndrome: epidemiologic evidence to date. J Cardiometab Syndr. 2006;1(5):351–355. | ||
Hummel M, Standl E, Schnell O. Chromium in metabolic and cardiovascular disease. Horm Metab Res. 2007;39(10):743–751. | ||
Azhar Y, Parmar A, Miller CN, Samuels JS, Rayalam S. Phytochemicals as novel agents for the induction of browning in white adipose tissue. Nutr Metab (Lond). 2016;13:89. | ||
Santana-Galvez J, Cisneros-Zevallos L, Jacobo-Velazquez DA. Chlorogenic acid: recent advances on its dual role as a food additive and a nutraceutical against metabolic syndrome. Molecules. 2017;22(3):pii:E358. | ||
Maeda H. Nutraceutical effects of fucoxanthin for obesity and diabetes therapy: a review. J Oleo Sci. 2015;64(2):125–132. | ||
Millan J, Cicero AFG, Torres F, Anguera A. Effects of a nutraceutical combination containing berberine (BRB), policosanol, and red yeast rice (RYR), on lipid profile in hypercholesterolemic patients: a meta-analysis of randomized controlled trials. Clin Investig Arterioscler. 2016;28(4):178–187. | ||
Ribas-Latre A, Eckel-Mahan K. Interdependence of nutrient metabolism and the circadian clock system: importance for metabolic health. Mol Metab. 2016;5(3):133–152. | ||
Desai M, Jellyman JK, Ross MG. Epigenomics, gestational programming and risk of metabolic syndrome. Int J Obes (Lond). 2015;39(4):633–641. | ||
Tarrade A, Panchenko P, Junien C, Gabory A. Placental contribution to nutritional programming of health and diseases: epigenetics and sexual dimorphism. J Exp Biol. 2015;218(Pt 1):50–58. | ||
Brenseke B, Prater MR, Bahamonde J, Gutierrez JC. Current thoughts on maternal nutrition and fetal programming of the metabolic syndrome. J Pregnancy. 2013;2013:368461. | ||
Knip M, Akerblom HK. Early nutrition and later diabetes risk. Adv Exp Med Biol. 2005;569:142–150. | ||
Brown LD. Endocrine regulation of fetal skeletal muscle growth: impact on future metabolic health. J Endocrinol. 2014;221(2):R13–R29. | ||
DeBoer MD, Lima AA, Oría RB, et al. Early childhood growth failure and the developmental origins of adult disease: do enteric infections and malnutrition increase risk for the metabolic syndrome? Nutr Rev. 2012;70(11):642–653. | ||
Alvisi P, Brusa S, Alboresi S, et al. Recommendations on complementary feeding for healthy, full-term infants. Ital J Pediatr. 2015;41:36. |
Supplementary material
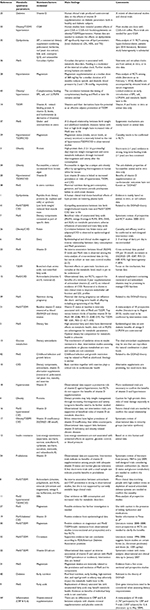
Table S1 Summary of reviews and meta-analyses (2005–2017)
References
Udenigwe CC, Rouvinen-Watt K. The role of food peptides in lipid metabolism during dyslipidemia and associated health conditions. Int J Mol Sci 2015; 16(5):9303–9313. | ||
Phillips, CM. Nutrigenetics and metabolic disease: current status and implications for personalised nutrition. Nutrients 2013; 5(1):32–57. | ||
Leidy HJ, Clifton PM, Astrup A, Wycherley TP, Westerterp-Plantenga MS, Luscombe-Marsh ND, Woods SC, Mattes RD. The role of protein in weight loss and maintenance. Am J Clin Nutrition 2015; 101 (Suppl):1320S-9S. | ||
Keller U. Dietary proteins in obesity and in diabetes. Int J Vitam Nutr Res 2011; 81(2–3):125–133. | ||
Newsholme P, Cruzat V, Arfuso F, Keane K. Nutrient regulation of insulin secretion and action. J Endocrinol 2014; 221(3): R105–120. | ||
Dugan CE, Fernandez ML. Effects of dairy on metabolic syndrome parameters: a review. Yale J Biol Med 2014; 87(2):135–147. | ||
Calton EK, James AP, Pannu PK, Soares MJ. Certain dietary patterns are beneficial for the metabolic syndrome: reviewing the evidence. Nutr Res 2014; 34(7):559–568. | ||
Davi G, Santilli F, Patrono C. Nutraceuticals in diabetes and metabolic syndrome. Cardiovasc Ther 2010; 28(4):216–226. | ||
Roche HM. Fatty acids and the metabolic syndrome. Proc Nutr Soc 2005; 64(1):23–29. | ||
Whayne TF Jr., Maulik N. Nutrition and the healthy heart with an exercise boost. Can J Physiol Pharmacol 2012; 90(8):967–976. | ||
Malik P, Popkin BM, Bray GA, Després JP, Willett WC, Hu FB. Sugar-sweetened beverages and risk of metabolic syndrome and type 2 diabetes: a meta-analysis. Diabetes Care 2010; 33(11):2477–83. | ||
Renwick AG, Molinary SV. Sweet-taste receptors, low-energy sweeteners, glucose absorption and insulin release. British Journal of Nutrition 2010; 104:1415–1420. | ||
Avignon A, Hokayem M, Bisbal C, Lambert K. Dietary antioxidants: Do they have a role to play in the ongoing fight against abnormal glucose metabolism? Nutrition 2012; 28(7–8):715–721. | ||
Dakshinamurti, K.Vitamins and their derivatives in the prevention and treatment of metabolic syndrome diseases (diabetes). Can J Physiol Pharmacol 2015; 93(5):355–362. | ||
Xu YJ, Tappia PS, Neki NS, Dhalla NS. Prevention of diabetes-induced cardiovascular complications upon treatment with antioxidants. Heart Fail Rev 2014; 19(1):113–121. | ||
Makariou S, Liberopoulos EN, Elisaf M, Challa A. Novel roles of vitamin D in disease: what is new in 2011? Eur J Intern Med 2011; 22(4):355–362. | ||
Renzaho AM, Halliday JA, Nowson C. Vitamin D, obesity, and obesity-related chronic disease among ethnic minorities: a systematic review. Nutrition 2011; 27(9):868–879. | ||
Cosenso-Martin LN, Vilela-Martin JF. Is there an association between vitamin D and hypertension? Recent Pat Cardiovasc Drug Discov 2011; 6(2):140–147. | ||
Penckofer S, Kouba J, Wallis DE, Emanuele MA. Vitamin D and diabetes: let the sunshine in. Diabetes Educ 2008; 34(6):939–940, 942, 944 passim. | ||
Mozos I, Marginean O. Links between Vitamin D Deficiency and Cardiovascular Diseases. Biomed Res Int 2015:109275. | ||
Khan H, Kunutsor S, Franco OH, Chowdhury R. Vitamin D, type 2 diabetes and other metabolic outcomes: a systematic review and meta-analysis of prospective studies. Proc Nutr Soc 2013; 72(1):89–97. | ||
Pittas AG, Lau J, Hu FB, Dawson-Hughes B. The role of vitamin D and calcium in type 2 diabetes. A systematic review and meta-analysis. J Clin Endocrinol Metab 2007; 92(6):2017–2029. | ||
Ju SY, Jeong HS, Kim DH. Blood vitamin D status and metabolic syndrome in the general adult population: a dose-response meta-analysis. J Clin Endocrinol Metab 2014; 99(3):1053–1063. | ||
Barengolts E. Vitamin D role and use in prediabetes. Endocr Pract 2010; 16(3):476–485. | ||
Garbossa SG, Folli F. Vitamin D, sub-inflammation and insulin resistance: a window on a potential role for the interaction between bone and glucose metabolism. Rev Endocr Metab Disord 2017;18:243–258. | ||
da Silva RP, Kelly KB, Al Rajabi A, Jacobs RL. Novel insights on interactions between folate and lipid metabolism. Biofactors 2014; 40(3):277–283. | ||
Guerrera MP, Volpe SL, Mao JJ. Therapeutic uses of magnesium. Am Fam Physician 2009. 80(2):157–162. | ||
Zhang X, Li Y, Del Gobbo LC, Rosanoff A, Wang J, Zhang W, Song Y. Effects of magnesium supplementation on blood pressure-a meta-analysis of randomized double-blind placebo-controlled trials. Hypertension 2016; 68. | ||
Floege J. Magnesium in CKD: more than a calcification inhibitor? J Nephrol 2015; 28(3):269–277. | ||
Volpe SL. Magnesium, the metabolic syndrome, insulin resistance, and type 2 diabetes mellitus. Crit Rev Food Sci Nutr 2008; 48(3):293–300. | ||
He K, Song Y, Belin RJ, Chen Y. Magnesium intake and the metabolic syndrome: epidemiologic evidence to date. J Cardiometab Syndr 2006; 1(5):351–355. | ||
Hummel M, Standl E, Schnell O. Chromium in metabolic and cardiovascular disease. Horm Metab Res 2007; 39(10):743–751. | ||
Santana-Galvez J, Cisneros-Zevallos L, Jacobo-Velazquez DA. Chlorogenic acid: recent advances on its dual role as a food additive and a nutraceutical agaist metabolic syndrome. Molecules 2017; 22:358. | ||
Maeda H. Nutraceutical effects of fucoxanthin for obesity and diabetes therapy: a review. J Oleo Sci 2015; 64(2):125–132. | ||
Millan J, Cicero AFG, Torres F, Anguera A. Effects of a nutraceutical combination containing berberine (BRB), policosanol, and red yeast rice (RYR), on lipid profile in hypercholesterolemic patients: a meta-analysis of randomized controlled trials. Clin Investig Arteriosclero 2016; 28 (4):178–187. | ||
Ribas-Latre A, Eckel-Mahan K. Interdependence of nutrient metabolism and the circadian clock system: Importance for metabolic health. Mol Metab 2016; 5(3):133–152. | ||
Desai M, Jellyman JK, Ross MG. Epigenomics, gestational programming and risk of metabolic syndrome. Int J Obes (Lond) 2015; 39(4):633–641. | ||
Tarrade A, Panchenko P, Junien C, Gabory A. Placental contribution to nutritional programming of health and diseases: epigenetics and sexual dimorphism. J Exp Biol 2015; 218(Pt 1):50–58. | ||
Brenseke B, Prater MR, Bahamonde J, Gutierrez JC. Current thoughts on maternal nutrition and fetal programming of the metabolic syndrome. J Pregnancy 2013:368461. | ||
Knip M, Akerblom HK.Early nutrition and later diabetes risk. Adv Exp Med Biol 2005; 569:142–150. | ||
Brown LD. Endocrine regulation of fetal skeletal muscle growth: impact on future metabolic health. J Endocrinol 2014; 221(2): R13–29. | ||
DeBoer MD, Lima AA, Oría RB, Scharf RJ, Moore SR, Luna MA, Guerrant RL. Early childhood growth failure and the developmental origins of adult disease: do enteric infections and malnutrition increase risk for the metabolic syndrome? Nutr Rev 2012; 70(11):642–653. | ||
Alvisi P, Brusa S, Alboresi S, Amarri S, Bottau P, Cavagni G, Corradini B, Landi L, Loroni L, Marani M, et al. Recommendations on complementary feeding for healthy, full-term infants. Ital J Pediatr 2015; 41:36. | ||
Sun, C. H., et al. (2011). The effect of vitamin-mineral supplementation on CRP and IL-6: a systemic review and meta-analysis of randomised controlled trials. Nutr Metab Cardiovasc Dis. 21(8):576–583. (Not referenced in the paper) |
 © 2018 The Author(s). This work is published and licensed by Dove Medical Press Limited. The full terms of this license are available at https://www.dovepress.com/terms.php and incorporate the Creative Commons Attribution - Non Commercial (unported, v3.0) License.
By accessing the work you hereby accept the Terms. Non-commercial uses of the work are permitted without any further permission from Dove Medical Press Limited, provided the work is properly attributed. For permission for commercial use of this work, please see paragraphs 4.2 and 5 of our Terms.
© 2018 The Author(s). This work is published and licensed by Dove Medical Press Limited. The full terms of this license are available at https://www.dovepress.com/terms.php and incorporate the Creative Commons Attribution - Non Commercial (unported, v3.0) License.
By accessing the work you hereby accept the Terms. Non-commercial uses of the work are permitted without any further permission from Dove Medical Press Limited, provided the work is properly attributed. For permission for commercial use of this work, please see paragraphs 4.2 and 5 of our Terms.