Back to Journals » Infection and Drug Resistance » Volume 11
Risk factors for infectious complications following transrectal ultrasound-guided prostate biopsy
Authors Wu YP, Li XD, Ke ZB, Chen SH, Chen PZ, Wei Y , Huang JB, Sun XL, Xue XY , Zheng QS, Xu N
Received 14 April 2018
Accepted for publication 6 June 2018
Published 17 September 2018 Volume 2018:11 Pages 1491—1497
DOI https://doi.org/10.2147/IDR.S171162
Checked for plagiarism Yes
Review by Single anonymous peer review
Peer reviewer comments 2
Editor who approved publication: Professor Suresh Antony
Yu-Peng Wu,* Xiao-Dong Li,* Zhi-Bin Ke,* Shao-Hao Chen, Ping-Zhou Chen, Yong Wei, Jin-Bei Huang, Xiong-Lin Sun, Xue-Yi Xue, Qing-Shui Zheng, Ning Xu
Department of Urology, The First Affiliated Hospital of Fujian Medical University, Fuzhou, China
*These authors contributed equally to this work
Objective: To explore risk factors of infectious complications following transrectal ultrasound-guided prostate biopsy (TRUSPB).
Methods: We retrospectively analyzed 1,203 patients with suspected prostate cancer who underwent TRUSPB at our center between December 2012 and December 2016. Demographics, clinical characteristics, and data regarding complications were collected, and then univariate and multivariate logistic regression analyses were used to identify independent risk factors for infectious complications after prostate biopsy.
Results: Multivariate logistic analysis demonstrated that body mass index (BMI) (OR=2.339, 95% CI 2.029–2.697, P<0.001), history of diabetes (OR=2.203, 95% CI 1.090–4.455, P=0.028), and preoperative catheterization (OR=2.303, 95% CI 1.119–4.737, P=0.023) were risk factors for infection after prostate biopsy. The area under the receiver operating characteristics curve for infectious complications was 0.930 (95% CI 0.907–0.953, P<0.001). BMI=28.196 kg/m2 was the best cut-off threshold for predicting infection after TRUSPB.
Conclusion: BMI >28.196 kg/m2, history of diabetes, and preoperative catheterization are independent risk factors for infection after prostate biopsy.
Keywords: body mass index, diabetes mellitus, preoperative catheterization, infectious complications, transrectal ultrasound-guided prostate biopsy
Introduction
Prostate cancer remains the second leading cause of cancer-related death for American men.1 Prostate cancer incidence rates are rising yearly; in China, >100,000 new patients are diagnosed with prostate cancer annually,2 making it the seventh most common cancer in 2011 and an important healthcare issue. It has been reported that prostate cancer incidence rates increased nearly 6-fold between 1973 and 2009 in eastern China (from 2.12/100,000 to 12.96/100,000). In addition, the disease-specific mortality of prostate cancer has increased more than 3-fold. However, few studies have focused on infections after prostate biopsy in Chinese men.
Currently, transrectal ultrasound-guided prostate biopsy (TRUSPB) is the gold standard for obtaining pathological specimens to diagnose prostate cancer;3 however, complications following TRUSPB vary widely and include hematuria, hematospermia, infection, pain, rectal bleeding, urinary retention, lower urinary tract symptoms, erectile dysfunction, and mortality.4 It has been reported that minor complications such as bleeding and pain are frequent,5 but worryingly, infectious complications that may lead to death have increased over time.6,7 Infectious complications after TRUSPB are reported in up to 6% of patients,6–8 and a previous study showed that the hospitalization rate of patients who developed infectious complications ranges from 0% to 6.3%.4 Chiang et al9 studied 3,694 Chinese prostate cancer patients and revealed that the rate of complications after prostate biopsy was 1.98%. A retrospective study10 from China that included 1,130 patients who underwent prostate biopsy demonstrated that the overall infectious complications rate was 4.25% after prostate biopsy. These infectious complications included 26 (2.30%) cases of urinary tract infection, 22 (1.95%) cases of fever, but no cases of sepsis. A 10-year single-center study11 in southern China that included 1,526 patients who underwent prostate biopsy revealed that the percentage of patients who developed febrile infection was 2.2%.
The use of prophylactic antibiotics plays an important role in reducing complications following prostate biopsy. However, drug choice and treatment course are variable in different Chinese hospitals.12 Qiao et al12 studied a Chinese population and reported that 500 mg oral levofloxacin once daily for 3 days could prevent infections after prostate biopsy. Notwithstanding, quinolones remain the most active agent against the bacteria in prostate and feces, and are commonly used to treat urinary tract infections.9 An 8-year single-center study reported that levofloxacin remained effective and was superior to pipemidic acid-based prophylactic antibiotics. Wang et al13 demonstrated that quinolones can be used postoperatively as routine antibiotics, and also revealed that carbapenems or teicoplanin can be used for patients with sepsis.
The risk factors for infectious complications after TRUSPB remain controversial. Several studies have demonstrated that recent hospitalization (<1 month prior to TRUSPB), comorbidities (particularly diabetes), history of urinary infections, history of antibiotic use, and year of biopsy were significantly associated with rates of infectious complications after TRUSPB.8,14,15 This retrospective study aimed to more precisely explore risk factors of infectious complications following TRUSPB.
Methods
Patients
This study was approved by the Ethics Committee of the First Affiliated Hospital of Fujian Medical University (Fuzhou, China). All patients signed informed consent forms. We retrospectively analyzed 1,252 patients with suspected prostate cancer between December 2012 and December 2016 at the First Affiliated Hospital of Fujian Medical University. We excluded 49 patients who did not meet the inclusion criteria, and the remaining 1,203 patients who underwent TRUSPB formed the study cohort. All patients underwent digital rectal examination, serum prostate-specific antigen (PSA) testing, Doppler ultrasonography, and MRI.
Indications for TRUSPB were patients with a suspicious finding on digital rectal examination, Doppler ultrasonography, and/or MRI,16 as well as a PSA >10 ng/mL.17 Patients with PSA 4–10 ng/mL, a free/total PSA ratio of <0.16,17 or PSA density >0.15 ng/mL/mL18 were also included. However, 17 patients with blood coagulation disorders and coagulation function that could not be corrected, 13 patients with alteration of the urinary tract due to infection within 1 month of TRUSPB, five patients with severe organ dysfunction, eight patients with acute prostatitis, and six patients with anal stenosis were excluded from the study.
The definition of febrile urinary tract infections was as follows: fever (≥38.3°C), leukocytes in urine sediment, and tenderness of the prostate during digital rectal examination.19,20 Fever was defined as body temperature ≥38.3°C, and infectious complications were defined as body temperature ≥38.3°C accompanied by urinary tract infection symptoms.19,20 Urinary tract infection symptoms were defined as the presence of chilliness, frequency, urgency, and dysuria. Sepsis was defined as the presence of clinically or microbiologically documented infection in conjunction with systemic inflammatory response syndrome.11,19,20
TRUSPB
A pre-biopsy enema using glycerin or saline solution was performed 1 hour before the procedure. Patients were instructed to take 200 mg ciprofloxacin 1 hour before TRUSPB, and then 250 mg ciprofloxacin every 12 hours after TRUSPB.21 All TRUSPB procedures were performed by the same senior urologist under the guidance of color Doppler ultrasonography (Acuson Aspen; Siemens, Erlangen, Germany) with an 18-gage biopsy gun (Max-Core; BARD, Covington, GA, USA). All patients were placed in the left lateral decubitus position with knees and hips flexed and underwent a 12-core biopsy protocol, including six parasagittally and six laterally targeted cores covering the base, mid-zones, and apex.21
Statistical analysis
All data were analyzed using SPSS version 18.0 software (SPSS, Chicago, IL, USA). Numerical data that were normally distributed are represented as mean ± SD. Non-parametric numerical data are expressed as median (range) and were analyzed using the Kruskal–Wallis test. Categorical data were analyzed by Pearson’s chi-squared test and Fisher’s test. Univariate and multivariate logistic regression analyses were used to determine risk factors for infectious complications. Receiver operating characteristics (ROC) curves were used to evaluate the diagnostic accuracy of the BMI for infection after prostate biopsy. The Youden index (J), defined as the maximum vertical distance between the ROC curve and the diagonal line, serves as another global measure of overall diagnostic accuracy and can be used to choose the optimal cut-off point.22 The Youden index (J) was calculated using the following formula23: J=(sensitivity + specificity)−1. The highest value of J was assumed to be the best cut-off point. Thus, the Youden index was used to determine the cut-off threshold for infectious complications. P<0.05 was considered significant for all tests.
Results
In total, 1,203 patients were enrolled in this study after 49 were excluded. The overall complications after prostate biopsy are shown in Table 1. Infectious symptoms were observed within 1 week of prostate biopsy in 99 patients. Patients who developed fever20 (≥38.3°C) after prostate biopsy were hospitalized and treated with third-generation cephalosporins or quinolones. The eight patients who developed sepsis were treated with carbapenem and teicoplanin. Blood and urine cultures showed that the pathogen was Escherichia coli (E. coli). There were no mortalities.
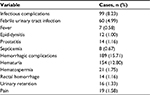  | Table 1 Overview of complications following prostate biopsy |
Patients were then divided into two groups: the infection group (99 patients) and the non-infection group (1,104 patients). Univariate analysis demonstrated that there was no significant relationship between the two groups in terms of age, hypertension, cerebrovascular accident, anticoagulant agents, secondary biopsy, history of transurethral resection of the prostate, pre-biopsy total PSA, prostate volume, core biopsy volume, or pathology. However, there were significant differences between the two arms in terms of BMI, history of diabetes, chronic prostatitis, preoperative catheterization, and history of urinary infection (P<0.05) (Table 2). Multivariate logistic regression analysis demonstrated that BMI, history of diabetes, and preoperative catheterization were risk factors for infection after TRUSPB (Table 3). The area under the ROC curve for infectious complications was 0.930 (95% CI 0.907–0.953, P<0.001). BMI=28.196 kg/m2 was the best cut-off threshold for predicting infection after TRUSPB.
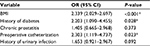  | Table 3 Multivariate logistic regression analysis of risk factors for infection after prostate biopsy (n=1203) Note: *P<0.05. Abbreviation: BMI, body mas index. |
Among the 99 patients with infections after prostate biopsy, 98 had blood cultures and 99 had urine cultures. These results demonstrated that 48 patients had positive blood cultures and 61 had positive urine cultures. Among the 109 positive cultures (blood or urine), E. coli was the most frequent pathogen (n=98, 89.9%), followed by Klebsiella (n=8, 7.34%), and Bacteroides fragilis (n=3, 2.75%). Quinolone resistance was observed in 72 (66.06%) cultures (Table 4).
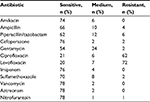  | Table 4 Antibiotic susceptibility in patients who underwent blood or urine cultures |
Discussion
While complications following TRUSPB are common, infectious complications are some of the most severe that face this patient population.4 Mortality after TRUSPB is extremely rare, and most reported deaths are caused by septic shock.24 Batura and Gopal Rao25 reported that ~2.15%–3.6% of patients who underwent TRUSPB in England and Wales were readmitted with infectious complications. Simsir et al26 showed that there was a 3.06% chance of sepsis after TRUSPB, while Wagenlehner et al27 reported that 3.5% of patients had febrile urinary infections and 3.1% required hospitalization after TRUSPB. Carignan et al8 reported that chronic obstructive pulmonary disease, diabetes, and recent hospitalization were risk factors for infectious complications, while Simsir et al26 reported that diabetes, benign prostatic hyperplasia, the presence of a catheter, more biopsy cores, and repeat biopsies were also associated with infectious complications after TRUSPB.
To the best of our knowledge, most studies investigating infections after prostate biopsy have been based on patients from North America and Europe.28,29 The genetic and physiological characteristics of Chinese men are significantly different from those of Western populations; however, studies pertinent to Chinese patients are lacking.11 Chiang et al9 studied a total of 3,694 Chinese patients and revealed that the rate of complications after prostate biopsy was 1.98%. A retrospective study10 from China including 1,130 patients who underwent prostate biopsy demonstrated that the overall infectious complications rate was 4.25% after prostate biopsy. These infectious complications included 26 (2.30%) cases of urinary tract infection, 22 (1.95%) cases of fever, and no cases of sepsis. A 10-year single-center study11 in South China including 1,526 patients who underwent prostate biopsy revealed that the percentage of patients who developed febrile infection was 2.2%.
In this study, the rate of infectious complications following TRUSPB was 8.23% (99/1,203). Febrile urinary tract infections were the most common symptom in patients with infections (n=60), followed by prostatitis (n=14), fever (n=7), and severe sepsis (n=8). The risk factors for infectious complications and effective preventive strategies for dealing with infectious complications after TRUSPB were identified. Multivariate logistic regression analysis demonstrated that BMI, history of diabetes, and preoperative catheterization increased the risk of infection after prostate biopsy.
Our multivariate logistic regression analysis demonstrated that elevated BMI increased the risk of infectious complications after TRUSPB. Choi et al19 reported that 3.3% (39/1,195) of patients developed febrile urinary tract infections, and that BMI >25 kg/m2 was associated with this complication in univariate analysis. After adjusting for core number in the multivariate analysis, BMI >25 kg/m2 was still significantly correlated with febrile urinary tract infections in their study. Semins et al30 also reported that obese patients were more likely to be vulnerable to infection, as the obese were nearly five times more likely to be diagnosed with pyelonephritis than those with a BMI in the normal range. Wu et al11 reported that obesity (BMI >28 kg/m2) was an independent risk factor for post-biopsy infection (OR=3.383, 95% CI 1.327–8.626). In this study, we found that elevated BMI increased the risk of infectious complications after TRUSPB in Chinese patients (OR=2.339, 95% CI 2.029–2.697).
Although elevated BMI has been correlated as an increased risk factor for surgical infections in several surgical settings,31,32 the mechanisms whereby obesity contributes to increased infectious complications during prostate biopsy remain unknown. Diabetes is a known risk factor for infectious complications, and diabetic patients often present with an elevated BMI. Thus, diabetes may be treated as a confounder when determining the effects of obesity on infectious complications after TRUSPB. Prolonged hospital stays caused by difficulties in early ambulation after biopsy in obese patients may also contribute to the increased rate of infectious complications.33 Further studies are needed to validate whether a cause-and-effect relationship exists between elevated BMI and increased risk of infections. However, this finding should be used as guidance for urologists when treating obese patients.30
The increased risk of infectious complications following TRUSPB in diabetic patients has been observed in some centers.8,26 In this study, multivariate logistic regression analysis demonstrated that a history of diabetes increased the risk of infection after prostate biopsy. Consistent with previous studies, a history of diabetes was an independent risk factor for infection after prostate biopsy. Carignan et al8 reported a case-controlled study from a Canadian tertiary-care center that showed that diabetes was also an independent risk factor for infectious complications following prostate biopsy in a distinct geographic region. This finding was also demonstrated in a European randomized trial conducted by Loeb et al.29 Tsu et al34 reported that diabetes was associated with infection after TRUSPB. This was consistent with our study. However, a 10-year single-center study11 in the same region as our study revealed that diabetes was not an independent predictor of infection after TRUSPB, which was inconsistent with our study.
We also found correlations between infectious complications following TRUSPB and the use of preoperative catheterization. Preoperative catheterization increases the risk of introducing pathogenic microorganisms. In this study, the infection group included 23 patients (23.23%) who underwent preoperative catheterization, while only 149 patients (13.49%) underwent preoperative catheterization in non-infection group. Thus, there was a significant difference between the infection and non-infection groups, which was consistent with previous studies. Aus et al35 revealed that patients with preoperative catheterization were at a 2.3-fold increased risk of infection after prostate biopsy than those without preoperative catheterization. In this study, patients with preoperative catheterization showed a 2.303-fold increased risk of infection after prostate biopsy compared with those without preoperative catheterization. It has been reported that a catheter in the urinary tract may be treated as a foreign object that facilitates the proliferation of pathogenic microorganisms.36 Patients who underwent preoperative catheterization were often accompanied by urological diseases, including urinary retention, urinary incontinence, benign prostatic hyperplasia, and bladder calculi, which were significantly associated with a high risk of infectious complications after TRUSPB.
Choi et al19 reported on the incidence rate of infectious complications, and their data suggested that quinolone resistance has been increasing in recent years. Steensels et al37 also showed that quinolone-resistant infections after TRUSPB are on the rise. It has been reported that quinolones are the most frequently used prophylactic antibiotic before TRUSPB.8 To date, adequate studies of Chinese prostate cancer patients have not been conducted.11 A prospective study34 that enrolled 371 Chinese patients who underwent TRUSPB reported on the prevalence of fluoroquinolone-resistant bacteria and the relationship between microbiology and post-biopsy infection rates. This study also revealed that 150 (40.4%) Chinese patients had fluoroquinolone-resistant bacteria. Tsu et al34 reported a high prevalence of antimicrobial resistance (40.4%), although few patients (2.4%) developed infections (eight with fever and one with septic shock) after prostate biopsy. Furthermore, all infections were successfully managed with carbapenems. In this study, E. coli was the most frequent pathogen. Thus, alternative prophylactic agents should be preoperatively determined by rectal swab cultures for patients with a history of urinary infection and chronic prostatitis, to reduce the rate of infections after prostate biopsy. However, at our center, pre-biopsy rectal swab cultures38 are not routine for patients undergoing TRUSPB.
This study had several limitations. First, the sample size was limited by the low incidence of infectious complications after TRUSPB. Second, this was a retrospective study using data derived from a single center. Third, the conditions of blood-glucose control and diabetes treatments, and previous histories of quinolone use were not considered in this study. A large-scale, multicenter, prospective study is needed to confirm these results.
Conclusion
Our data show that BMI, history of diabetes, and preoperative catheterization are independent risk factors for infection after prostate biopsy.
Data sharing statement
All data generated or analyzed during this study are included in this published article.
Acknowledgments
This study was supported by Natural Science Foundation of Fujian Province (grant no. 2017J01197), the Youth Foundation of Health and Family Planning Commission of Fujian Province, China (grant no. 2017-1-58), the Funds for Creative Program of Health and Family Planning Commission of Fujian Province, China (grant no. 2016-CX-27), and the Joint Foundation of Fujian Province for Science and Technology Innovative Research Project (grant no. 2017Y9093).
Author contributions
YPW, XDL, and ZBK wrote the manuscript. SHC, PZC, and YW analyzed the results and revised the paper. JBH and XLS collected and analyzed clinical information on the patients. XYX, QSZ, and NX designed the study, analyzed the results, and revised the paper. All authors contributed toward data analysis, drafting and revising the paper and agree to be accountable for all aspects of the work.
Disclosure
The authors report no conflicts of interest in this work.
References
Siegel RL, Miller KD, Jemal A. Cancer statistics, 2016. CA Cancer J Clin. 2016;66(1):7–30. | ||
Center MM, Jemal A, Lortet-Tieulent J, et al. International variation in prostate cancer incidence and mortality rates. Eur Urol. 2012;61(6):1079–1092. | ||
Lu DD, Raman JD. Strategies for prevention of ultrasound-guided prostate biopsy infections. Infect Drug Resist. 2016;9:161–169. | ||
Loeb S, Vellekoop A, Ahmed HU, et al. Systematic review of complications of prostate biopsy. Eur Urol. 2013;64(6):876–892. | ||
Rosario DJ, Lane JA, Metcalfe C, et al. Short term outcomes of prostate biopsy in men tested for cancer by prostate specific antigen: prospective evaluation within ProtecT study. BMJ. 2012;344:d7894. | ||
Nam RK, Saskin R, Lee Y, et al. Increasing hospital admission rates for urological complications after transrectal ultrasound guided prostate biopsy. J Urol. 2013;189(1 Suppl):S12–S18. | ||
Loeb S, Carter HB, Berndt SI, Ricker W, Schaeffer EM. Complications after prostate biopsy: data from SEER-Medicare. J Urol. 2011;186(5):1830–1834. | ||
Carignan A, Roussy JF, Lapointe V, Valiquette L, Sabbagh R, Pépin J. Increasing risk of infectious complications after transrectal ultrasound-guided prostate biopsies: time to reassess antimicrobial prophylaxis? Eur Urol. 2012;62(3):453–459. | ||
Chiang BJ, Pu YS, Chung SD, et al. Quinolone prophylaxis in transrectal ultrasound guided prostate biopsy: an eight-year single center experience. ScientificWorldJournal. 2013;2013:452107. | ||
Zhang XH, Jia Y, Guo WH, et al. Clinical comparison of the efficacy of three different bowel preparation methods on the infectious complications following transrectal ultrasonography-guided prostate biopsy in nursing practice. J Clin Nurs. 2018;27(13-14):2583–2589. | ||
Wu X, Yu C, Li T, et al. Obesity was an independent risk factor for febrile infection after prostate biopsy: A 10-year single center study in South China. Medicine. 2018;97(1):e9549. | ||
Qiao LD, Chen S, Wang XF, et al. A multi-center, controlled, randomized, open-label clinical study of levofloxacin for preventing infection during the perioperative period of ultrasound-guided transrectal prostate biopsy. Eur J Clin Microbiol Infect Dis. 2016;35(11):1877–1881. | ||
Wang J, Wan B, Li C, et al. Diagnostic Yield and Complications Using a 20 Gauge Prostate Biopsy Needle versus a Standard 18 Gauge Needle: A Randomized Controlled Study. Urol J. 2015;12(5):2329–2333. | ||
Eruz ED, Yalci A, Ozden E, et al. Risk factors for infection development after transrectal prostate biopsy and the role of resistant bacteria in colonic flora. J Infect Dev Ctries. 2017;11(2):188–191. | ||
Williamson DA, Barrett LK, Rogers BA, Freeman JT, Hadway P, Paterson DL. Infectious complications following transrectal ultrasound-guided prostate biopsy: new challenges in the era of multidrug-resistant Escherichia coli. Clin Infect Dis. 2013;57(2):267–274. | ||
Shakir NA, Siddiqui MM, George AK, et al. Should Hypoechoic Lesions on Transrectal Ultrasound Be Sampled During Magnetic Resonance Imaging-targeted Prostate Biopsy? Urology. 2017;105:113–117. | ||
Na R, Ye D, Qi J, et al. Prostate health index significantly reduced unnecessary prostate biopsies in patients with PSA 2-10 ng/mL and PSA >10 ng/mL: Results from a Multicenter Study in China. Prostate. 2017;77(11):1221–1229. | ||
Whitson JM, Porten SP, Hilton JF, et al. The relationship between prostate specific antigen change and biopsy progression in patients on active surveillance for prostate cancer. J Urol. 2011;185(5):1656–1660. | ||
Choi JW, Kim TH, Chang IH, et al. Febrile urinary tract infection after prostate biopsy and quinolone resistance. Korean J Urol. 2014;55(10):660–664. | ||
Hashimoto T, Namiki K, Tanaka A, Shimodaira K, Gondo T, Tachibana M. Emphysematous cystitis following a transrectal needle guided biopsy of the prostate. BMC Infect Dis. 2012;12(1):322. | ||
Xu N, Xue XY, Li XD, Wei Y, Lin N. Meperidine relieves pain during transrectal ultrasound-guided prostate biopsy. Saudi Med J. 2014;35(5):454–459. | ||
Lai CY, Tian L, Schisterman EF. Exact confidence interval estimation for the Youden index and its corresponding optimal cut-point. Comput Stat Data Anal. 2012;56(5):1103–1114. | ||
Caminha TC, Ferreira HS, Costa NS, et al. Waist-to-height ratio is the best anthropometric predictor of hypertension: A population-based study with women from a state of northeast of Brazil. Medicine. 2017;96(2):e5874. | ||
Hasegawa T, Shimomura T, Yamada H, et al. Fatal septic shock caused by transrectal needle biopsy of the prostate; a case report. Kansenshogaku Zasshi. 2002;76(10):893–897. | ||
Batura D, Gopal Rao G. The national burden of infections after prostate biopsy in England and Wales: a wake-up call for better prevention. J Antimicrob Chemother. 2013;68(2):247–249. | ||
Simsir A, Kismali E, Mammadov R, Gunaydin G, Cal C. Is it possible to predict sepsis, the most serious complication in prostate biopsy? Urol Int. 2010;84(4):395–399. | ||
Wagenlehner FM, van Oostrum E, Tenke P, et al. Infective complications after prostate biopsy: outcome of the Global Prevalence Study of Infections in Urology (GPIU) 2010 and 2011, a prospective multinational multicentre prostate biopsy study. Eur Urol. 2013;63(3):521–527. | ||
Pinkhasov GI, Lin YK, Palmerola R, et al. Complications following prostate needle biopsy requiring hospital admission or emergency department visits - experience from 1000 consecutive cases. BJU Int. 2012;110(3):369–374. | ||
Loeb S, van den Heuvel S, Zhu X, Bangma CH, Schröder FH, Roobol MJ. Infectious complications and hospital admissions after prostate biopsy in a European randomized trial. Eur Urol. 2012;61(6):1110–1114. | ||
Semins MJ, Shore AD, Makary MA, Weiner J, Matlaga BR. The impact of obesity on urinary tract infection risk. Urology. 2012;79(2):266–269. | ||
Dotters-Katz SK, Feldman C, Puechl A, Grotegut CA, Heine RP. Risk factors for post-operative wound infection in the setting of chorioamnionitis and cesarean delivery. J Matern Fetal Neonatal Med. 2016;29(10):1541–1545. | ||
Sebastian A, Huddleston P, Kakar S, Habermann E, Wagie A, Nassr A. Risk factors for surgical site infection after posterior cervical spine surgery: an analysis of 5,441 patients from the ACS NSQIP 2005-2012. Spine J. 2016;16(4):504–509. | ||
Khan MN, Russo J, Spivack J, et al. Association of Body Mass Index With Infectious Complications in Free Tissue Transfer for Head and Neck Reconstructive Surgery. JAMA Otolaryngol Head Neck Surg. 2017;143(6):574–579. | ||
Tsu JH, Ma WK, Chan WK, et al. Prevalence and predictive factors of harboring fluoroquinolone-resistant and extended-spectrum β-lactamase-producing rectal flora in Hong Kong Chinese men undergoing transrectal ultrasound-guided prostate biopsy. Urology. 2015;85(1):15–22. | ||
Aus G, Ahlgren G, Bergdahl S, Hugosson J. Infection after transrectal core biopsies of the prostate--risk factors and antibiotic prophylaxis. Br J Urol. 1996;77(6):851–855. | ||
de Jesus CM, Corrêa LA, Padovani CR. Complications and risk factors in transrectal ultrasound-guided prostate biopsies. Sao Paulo Med J. 2006;124(4):198–202. | ||
Steensels D, Slabbaert K, de Wever L, Vermeersch P, van Poppel H, Verhaegen J. Fluoroquinolone-resistant E. coli in intestinal flora of patients undergoing transrectal ultrasound-guided prostate biopsy--should we reassess our practices for antibiotic prophylaxis? Clin Microbiol Infect. 2012;18(6):575–581. | ||
Taylor AK, Murphy AB. Preprostate Biopsy Rectal Culture and Postbiopsy Sepsis. Urol Clin North Am. 2015;42(4):449–458. |
 © 2018 The Author(s). This work is published and licensed by Dove Medical Press Limited. The full terms of this license are available at https://www.dovepress.com/terms.php and incorporate the Creative Commons Attribution - Non Commercial (unported, v3.0) License.
By accessing the work you hereby accept the Terms. Non-commercial uses of the work are permitted without any further permission from Dove Medical Press Limited, provided the work is properly attributed. For permission for commercial use of this work, please see paragraphs 4.2 and 5 of our Terms.
© 2018 The Author(s). This work is published and licensed by Dove Medical Press Limited. The full terms of this license are available at https://www.dovepress.com/terms.php and incorporate the Creative Commons Attribution - Non Commercial (unported, v3.0) License.
By accessing the work you hereby accept the Terms. Non-commercial uses of the work are permitted without any further permission from Dove Medical Press Limited, provided the work is properly attributed. For permission for commercial use of this work, please see paragraphs 4.2 and 5 of our Terms.

