Back to Journals » Advances in Medical Education and Practice » Volume 7
Resource-oriented coaching for reduction of examination-related stress in medical students: an exploratory randomized controlled trial
Received 12 April 2016
Accepted for publication 7 June 2016
Published 22 August 2016 Volume 2016:7 Pages 497—504
DOI https://doi.org/10.2147/AMEP.S110424
Checked for plagiarism Yes
Review by Single anonymous peer review
Peer reviewer comments 2
Editor who approved publication: Dr Md Anwarul Azim Majumder
Thomas Kötter,1 Frank Niebuhr2
1Institute of Social Medicine and Epidemiology, 2Institute of Family Medicine, University of Lübeck, Lübeck, Germany
Introduction: The years spent in acquiring medical education is considered a stressful period in the life of many students. Students whose mental health deteriorates during this long period of study are less likely to become empathic and productive physicians. In addition to other specific stressors, academic examinations seem to further induce medical school-related stress and anxiety. Combined group and individual resource-oriented coaching early in medical education might reduce examination-related stress and anxiety and, consequently, enhance academic performance. Good quality evidence, however, remains scarce. In this study, therefore, we explored the question of whether coaching affects examination-related stress and health in medical students.
Methods: We conducted a randomized controlled trial. Students who registered for the first medical academic examination in August 2014 at the University of Lübeck were recruited and randomized into three groups. The intervention groups 1 and 2 received a 1-hour psychoeducative seminar. Group 1 additionally received two 1-hour sessions of individual coaching during examination preparation. Group 3 served as a control group. We compared changes in self-rated general health (measured by a single item), anxiety and depression (measured by the hospital anxiety and depression scale), as well as medical school stress (measured by the perceived medical school stress instrument). In order to further investigate the influence of group allocation on perceived medical school stress, we conducted a linear regression analysis.
Results: We saw a significant deterioration of general health and an increase in anxiety and depression scores in medical students while preparing for an examination. We found a small, but statistically significant, effect of group allocation on the development of perceived medical school stress. However, we could not differentiate between the effects of group coaching only and group coaching in combination with two sessions of individual coaching.
Conclusion: The health of medical students deteriorated while preparing for an examination. Short-term resource-oriented coaching might be an effective means of reducing medical school stress in candidates preparing for an examination.
Keywords: education, medical, undergraduate, students, medical, stress, psychological, health promotion, resilience, psychological, counseling
A Letter to the Editor has been received and published for this article
Corrigendum for this paper has been published.
Introduction
There is ample evidence that the years spent in acquiring medical education is a stressful and difficult period in the life of many students.1 Starting at a good level,2 the health and well-being of medical students seems to deteriorate throughout their education,3 resulting in high rates of, for example, burnout and depression by the time of graduation4 and residency.5,6 Burnt out medical students and residents, however, seem less likely to be(come) empathetic and productive physicians.7,8 In addition to the individual burden, it is thus considered a systemic problem.9
Academic examinations seem to further provoke medical school-related stress and anxiety.10 Leading to a vicious circle, examination-related stress and anxiety may impair the academic performance of susceptible future doctors.11 There is evidence that female medical students are more prone to examination-related stress and anxiety.12,13 Since in many countries, to date, the majority of medical students are females; this finding is particularly important.14 The large amount of content to be learnt for an examination, the self-expectation to perform well, concern about poor marks, the long duration of periods of assessment, and a lack of exercise are among other factors associated with examination-related stress and anxiety.15,16
In her meta-analysis of the results of anxiety-reduction programs, Ergene17 concluded that: “individually conducted programs, along with programs that combined individual and group counseling formats, produced the greatest changes”. In order to break the vicious circle of examination-related stress and anxiety, and impaired academic performance early in medical education, combined group and individual resource-oriented coaching may pose a promising solution.18,19 Shiralkar et al conclude in their systematic review of stress management programs for medical students that more methodological rigor is required for related studies in order to more precisely identify which elements of such programs might be the most promising.20
Therefore, we explored the following questions by means of a randomized controlled trial:
- Does resource-oriented coaching influence examination-related stress in medical students?
- Does resource-oriented coaching influence general and mental health of medical students preparing for examination?
Materials and methods
We conducted a three-armed randomized controlled trial.
Participant recruitment and setting
All students who registered for the first medical examination in August 2014 at the University of Lübeck, a small public university with a focus on medicine and life sciences, were eligible to participate. We approached potentially eligible students in an anatomy refresher (“Anatomy in 5 days”21) in the middle of the summer semester. Students were preliminarily enrolled on a voluntary basis. Those who did not fulfill the criteria for registration for the first medical examination by mid-July, or refused to register for other reasons, were then excluded.
Interventions
Students in the intervention groups (groups 1 and 2) received a 1-hour psychoeducative seminar. During this seminar, a psychologist addressed issues, such as emotional reactions toward stressors, unconscious persistence of unprocessed negative emotions, and the relationship of the procession of stressful events and sleep. At the end of the seminar, all participants were surveyed using a paper–pencil questionnaire (t1).
Students in group 1 received two 1-hour sessions of manual-based individual coaching by trained psychologists and physicians within an interval of 2 weeks. The coaching was based on the so-called wingwave® (Besser Siegmund Institut, Hamburg, Germany) method. wingwave uses a finger-strength test derived from the Bi-Digital-O-Ring-Test for the determination of unconscious stressors following a standardized protocol.22 In order to process identified stressors, elements of eye movement desensitization and reprocession, and neurolinguistic programming techniques were applied.22,23 In several sessions ahead of the study period, four experienced wingwave coaches developed coaching techniques specifically for medical students in the examination preparation phase and wrote a standardized manual. As this coaching was not primarily designed to identify and treat deficits but to foster individual stress-management resources (“resilience” as defined by Zautra et al),24 we labeled the intervention “resource-oriented coaching”.25 During the first coaching session, students in group 1 received a universal serial bus memory stick containing hemisphere-stimulating music26 and were instructed on how to use it.
Following the psychoeducative seminar, students in group 2 received a universal serial bus memory stick containing hemisphere-stimulating music26 and an instruction sheet explaining how to use it.
Students in groups 1 and 2 were instructed to listen to the 20-minute piece of electronic music twice daily, before and during learning.
Students in group 3 served as control subjects and did not receive any intervention (“treatment as usual”). They were surveyed at the time of the psychoeducative seminar using a web survey containing the same questions as the paper–pencil survey in the treatment groups (t1).
To reduce potential dropout rates, the participants received a book voucher worth 5 Euro per completed questionnaire.
Randomization and allocation concealment
After preliminary enrolment, we randomly allocated participants to the treatment (groups 1 and 2) or control group (group 3) using a computer-generated random numbers table (randomization 1). By inviting those participants in the treatment group to participate in the psychoeducative seminar (described earlier), the students were immediately informed of their allocation to either control or treatment group. In a second step, the participants in the treatment group were randomly allocated to treatment groups 1 and 2 (randomization 2). This allocation was concealed by means of sealed, opaque envelopes until the end of the psychoeducative seminar and the t1 survey.
The participants, coaches, and the involved researcher were not blinded hereafter.
Measures
In addition to the information gathered about participants’ age and sex, outcome measures were chosen that would capture the possible intervention effects on different aspects of psychological health, including perceived study stress, self-rated general health, and mental health.
Outcomes were measured at two different points in time (after randomization 1 and the 1-hour psychoeducative seminar but before the examination preparation phase [t1] and directly before the examination [t2]). All outcome measures were used in numerous studies among medical students, as recommended by Shiralkar et al.20
Self-rated general health was measured by a single item (“How would you describe your health in general?”) to be answered on a five-point Likert scale from “very good” to “very poor”.27 Single item self-rated health has been found to be a predictor for several health outcomes in previous studies, including mortality.28
In order to measure mental health, we used the Hospital Anxiety and Depression Scale (HADS).29 The HADS was initially developed for clinical populations but has been widely used among students in general and medical students in particular.2,30,31 It comprises 14 items for two subscales. Each of the two subscales relates to anxiety and depression, and consists of seven items, which obtain responses on a four-point Likert scale, ranging from 0= mostly, to 3= not at all. Possible subscale scores range from 0 to 21. We used the German version (HADS-D), published by Herrmann-Lingen et al in 1995 and available in the third edition.32
We measured perceived medical school stress using the Perceived Medical School Stress (PMSS) scale in the German language (PMSS-D).33 This instrument was originally developed by Vitaliano et al in 198434 and has been translated into different languages and cultures and comprises 13 items in the German version. Each item can be answered on a five-point Likert scale (1= I strongly disagree; 5= I strongly agree). PMSS results have been linked to physical and mental well-being33 and have predictive validity for mental health problems in medical professionals 4 years after graduation.35 Shiralkar et al recommend using the PMSS as a standard measure for the evaluation of medical school stress management programs.20
Additionally, we collected qualitative data using focus groups and qualitative interviews. The qualitative analyses were designed to gain insight into the effective constituents of the intervention and to ask about adverse events. These results will be published separately.
Planned sample size
With 39 students per group, the trial would have been powered to detect medium-to-large effect sizes (d=0.65) for the difference in PMSS (standard deviation [SD] 7.8),33 using a two-tailed test, α =0.05 and an 80% power level. This number was determined using G*Power.36 In order to allow for a 10% dropout, the target sample size for the trial was 43 students per group (intervention groups 1 and 2 and control group 3).
Statistical methods
We substituted missing values following the rules provided in the handbooks for the instruments, that is, through interpolation where tolerable. We then excluded incomplete data sets. After a plausibility check, cases from the t1 and t2 surveys were matched using a self-generated pseudonym. We then excluded incomplete data sets. Data were missing from the responses of five students in the intervention group and seven in the control group, respectively. The last-observation-carried-forward method of imputation was chosen because this is a conservative method used in instances in which there is an equal dropout rate in the intervention and the control group.37 Intention-to-treat and per-protocol analyses yielded very similar results and we therefore present only the former. We used two-tailed t-tests to compare means of continuous variables. Where the assumptions for parametric tests were violated, we used the Mann–Whitney U tests. Results are reported as mean (M) ± standard deviation (SD). Cohen’s d was used to calculate the size of the treatment effect. We considered values of 0.2 small, 0.5 medium, and 0.8 large effect sizes. For methodological characteristics of the linear regression analysis, see the respective subsection of the “Results” section. All analyses were conducted using IBM SPSS Statistics version 22.0 (IBM Corporation, Armonk, NY, USA).
Ethical considerations
This trial is reported following the Consolidated Standards of Reporting Trials criteria.38 The trial was approved by the Ethics Committee of the University of Lübeck (File reference 14-098) and registered with the German Clinical Trials Register (DRKS00006349) before the time of first participant enrolment.39 All participants provided written informed consent.
Deviations from the trial protocol
Due of an unexpected shortfall in the sample size (n=24 students did not pass a test necessary to fulfill the examination admission requirements, Figure 1), we decided to combine both intervention groups for the quantitative analyses.
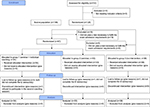  | Figure 1 Participant flow. Note: Outcome measured directly before the examination [t2]. |
Results
Baseline characteristics
Table 1 displays baseline characteristics for all participants included. Overall, 35 male and 70 female students (M =24.2 years, SD =2.6) with an age range between 19 and 32 years participated in this study (66% of the whole class). The study participants were 0.5 years younger and the percentage of females was higher when compared to the whole class. We had a lower percentage of male participants in the coaching group and participants in this group were 0.5 years older (Table 1). The participant flow for the trial is shown in Figure 1.
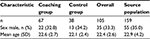  | Table 1 Baseline sociodemographic characteristics Abbreviations: SD, standard deviation. |
Outcomes
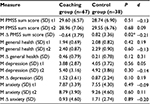
For the whole study population, regardless of allocation to treatment or control, we saw a statistically significant deterioration of general health (1.99 to 2.36; P<0.01) with a medium effect size (d=−0.64) between t1 and t2 (Table 2). Also for the whole group, we saw statistically significant increases of depression (3.94 to 5.23; P<0.01; d=0.47) and anxiety (7.75 to 8.96; P<0.01; d=0.33) levels during this period. Perceived medical school stress remained at about the same level in the whole study population (29.29 to 29.17, P=0.75).
For the development of general health, depression and anxiety during the study period, we found no statistically significant differences between the groups. However, perceived medical school stress decreased in the coaching group (from 29.60 to 28.96; Δ=−0.64) and increased in the control group (from 28.74 to 29.55; Δ=0.82). This difference is statistically significant (P<0.05), yet the effect size is small (d=−0.21).
Linear regression analysis
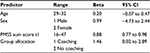
In order to further investigate the influence of group allocation on the PMSS score, we conducted a linear regression analysis controlling for sex, age, and the PMSS t1 sum score. We built the model by stepwise forward inclusion with a criterion of P<0.05 for the inclusion and P>0.10 for the exclusion of effects.
Linear regression confirmed group allocation to be a statistically significant predictor of perceived medical school stress immediately prior to the first medical examination (Table 3).
Discussion
The aim of this randomized controlled trial was to investigate the efficacy of short-term individual resource-oriented coaching on examination-related stress. We found a small, but statistically significant effect on the development of perceived medical school stress in the coaching group(s). However, due to the shortfall in the number of participants, we are not able to differentiate between the effects of group coaching only versus group coaching accompanied by two sessions of individual coaching.
To our knowledge, our study is the first to investigate not only the efficacy of resource-oriented coaching in the preparation phase before a medical academic examination, but also, at the same time, to take a closer look at the development of general and mental health while preparing for the examination.
For the whole study population, regardless of allocation to treatment or not, we saw a deterioration of general health and a rise of depression and anxiety levels during a relatively short time period of just over 3 weeks. Perceived medical school stress did not increase in the whole study population, which might have been caused by the identified effect of coaching on this variable, since it did increase in the control group (P=0.14, Table 3). These observational findings show the significant level of stress induced by examination has a measurable negative impact on not only the mental, but also the general health of the medical students. Examination stress has been identified as an important reason for the deterioration of medical students’ health throughout their education.10 Reducing the number of examinations and enhancing their design in order to mainly test knowledge and not primarily induce stress might thus be a promising starting point for health promotion in medical school students.40
When looking at the development of perceived medical school stress more closely, we saw a statistically significant difference between the t2−t1 Δ of the groups and a similar significant prediction of the PMSS t2-score by group allocation. Given the small effect size and absolute differences, we have to interpret this finding with caution. What we can say is that it might indicate the efficacy of a resource-oriented coaching program for candidates preparing for medical academic examination. This has been shown to be the case for other stress management techniques in a number of quantitative and qualitative studies.41–43 However, it remains unclear whether the stress-reducing efficacy of the interventions employed in this and other studies stems from certain methodological components or it can merely be seen as an unspecific effect of support during the examination preparation phase.
Strengths and limitations
Unfortunately, due to a merging of the intended two coaching groups, we were not able to decide whether group coaching alone or group coaching combined with sessions of individual coaching is the more promising approach to reduce perceived medical school stress while preparing for examination. Also, as group allocation was not concealed; t1 measures were completed after randomization; and the students, coaches, and investigators were not blinded, the differences between the groups at both t1 and t2 might have been influenced by a certain amount of frustration in the control group in not having received coaching. The 1-hour psychoeducative seminar might also have had an influence on the intervention groups’ t1 score. However, we did not find any statistically significant differences between the groups at t1. Furthermore, it seems less likely that surveying the intervention group after the seminar led to an overestimation of the observed effect (or type I error) compared with an underestimation (or type II error). The randomized controlled design of our study can, nevertheless, be seen as a major strength when compared to other existing studies in this field, which are preponderantly nonrandomized and do not include control groups at all.20,44 The risk of selection bias can hence be estimated as low. Outcomes were determined in the same way in all groups bearing a low risk of social desirability by using a web survey completed at home.45 The low dropout rate makes attrition bias due to incomplete outcome data unlikely.
Implications for research and practice
Future studies in this setting have to be designed to anticipate a higher dropout rate in order to avoid any power problems. Avoiding potential frustration through not receiving an intervention might be possible by employing a waiting-list-control design. It might prove helpful to identify students “in need of coaching” and recruit them for future, similar studies in order to depict a more realistic scenario (as students without a subjective need are less likely to benefit from such an intervention). In order to identify method-specific effects, and especially effective components of stress management programs, comparative mixed methods studies employing different kinds of interventions are required.
Our results show an urgent need for accompanying health promoting measures during the medical academic examination preparation phase. This should be of interest to universities in order for them to help prevent any avoidable examination-related health deterioration by paying for, or at least subsiding, appropriate measures, including, for example, individual short-term resource-oriented coaching as used in our study.
Conclusion
We saw a significant deterioration of general health and increasing anxiety and depression scores in medical students while preparing for examination. Our findings point to short-term resource-oriented coaching being effective in reducing medical school-stress in candidates preparing for examination, whereas the stress level increased in control subjects.
Acknowledgments
We would like to thank Cora Besser-Siegmund, Harry Siegmund, and Gabi Ertel for being a great coaching team and Sophia-Marie Saftien for her superb help during the coaching days. We also wish to thank the Lübeck Medical School, especially Jürgen Westermann, for supporting and funding this study. We would like to thank Angelika and Michael Hüppe for their input regarding design and analysis questions.
Disclosure
FN is a certified wingwave® coach and acted as one of the coaches in the present study. The authors declare no additional conflicts of interest in this work.
References
Dyrbye LN, Thomas MR, Shanafelt TD. Systematic review of depression, anxiety, and other indicators of psychological distress among U.S. and Canadian medical students. Acad Med. 2006;81(4):354–373. | ||
Kötter T, Tautphäus Y, Scherer M, Voltmer E. Health-promoting factors in medical students and students of science, technology, engineering, and mathematics: design and baseline results of a comparative longitudinal study. BMC Med Educ. 2014;14:135. | ||
Voltmer E, Kötter T, Spahn C. Perceived medical school stress and the development of behavior and experience patterns in German medical students. Med Teach. 2012;34(10):840–847. | ||
Koehl-Hackert N, Schultz J-H, Nikendei C, Möltner A, Gedrose B, van den Bussche H, Jünger J. Belastet in den Beruf – Empathie und Burnout bei Medizinstudierenden am Ende des Praktischen Jahres [Burdened into the job – final-year students’ empathy and burnout]. Z Evid Fortbild Qual Gesundhwes. 2012;106(2):116–124. | ||
Goldhagen BE, Kingsolver K, Stinnett SS, Rosdahl JA. Stress and burnout in residents: impact of mindfulness-based resilience training. Adv Med Educ Pract. 2015;6:525–532. | ||
Mata DA, Ramos MA, Bansal N, et al. Prevalence of depression and depressive symptoms among resident physicians: a systematic review and meta-analysis. JAMA. 2015;314(22):2373–2383. | ||
Wallace JE, Lemaire JB, Ghali WA. Physician wellness: a missing quality indicator. Lancet. 2009;374(9702):1714–1721. | ||
Dewa CS, Loong D, Bonato S, Thanh NX, Jacobs P. How does burnout affect physician productivity? A systematic literature review. BMC Health Serv Res. 2014;14:325. | ||
American Academy of Family Physicians (AAFP). Physician burnout (position paper) – AAFP policies. Available from: http://bit.ly/1CcVG09. Accessed August 2, 2016. | ||
Lyndon MP, Strom JM, Alyami HM, et al. The relationship between academic assessment and psychological distress among medical students: a systematic review. Perspect Med Educ. 2014;3(6):405–418. | ||
Frierson HT, Hoban JD. The effects of acute test anxiety on NBME Part I performance. J Natl Med Assoc. 1992;84(8):686–689. | ||
Farooqi YN, Ghani R, Spielberger CD. Gender differences in test anxiety and academic performance of medical students. Int J Psychol Behav Sci. 2012;2(2):38–43. | ||
Colbert-Getz JM, Fleishman C, Jung J, Shilkofski N. How do gender and anxiety affect students’ self-assessment and actual performance on a high-stakes clinical skills examination? Acad Med. 2013;88(1):44–48. | ||
General Medical Council. The state of medical education and practice in the UK report; 2014. Available from: http://bit.ly/1zYDJTK. Accessed August 2, 2016. | ||
Hashmat S, Hashmat M, Amanullah F, Aziz S. Factors causing exam anxiety in medical students. J Pak Med Assoc. 2008;58(4):167–170. | ||
Yusoff MS. Associations of pass-fail outcomes with psychological health of first-year medical students in a Malaysian medical school. Sultan Qaboos Univ Med J. 2013;13(1):107–114. | ||
Ergene T. Effective interventions on test anxiety reduction a meta-analysis. School Psychol Int. 2003;24(3):313–328. | ||
Gale AC, Gilbert J, Watson A. Life coaching to manage trainee underperformance. Med Educ. 2014;48(5):539. | ||
Wild K, Scholz M, Ropohl A, Bräuer L, Paulsen F, Burger PHM. Strategies against burnout and anxiety in medical education – implementation and evaluation of a new course on relaxation techniques (Relacs) for medical students. PLoS One. 2014;9(12):e114967. | ||
Shiralkar MT, Harris TB, Eddins-Folensbee FF, Coverdale JH. A systematic review of stress-management programs for medical students. Acad Psychiatry. 2013;37(3):158–164. | ||
Gebert A, Al-Samir K, Westermann J. Wie kann die Effizienz der Examensvorbereitung im Medizinstudium verbessert werden? Analyse eines Anatomierepetitoriums über drei Jahre [How to improve the efficiency of exam preparation in the study of medicine? Analysis of a repetition course in anatomy during three years]. Med Ausbild. 2002;19:35–37. | ||
Rathschlag M, Memmert D. Reducing anxiety and enhancing physical performance by using an advanced version of EMDR: a pilot study. Brain Behav. 2014;4(3):348–355. | ||
Besser-Siegmund C, Siegmund H. Achieve success through wingwave coaching. Available from: http://bit.ly/1zKhS19. Accessed August 2, 2016. | ||
Zautra AJ, Hall JS, Murray KE. Resilience – a new definition of health for people and communities. In: Handbook of Adult Resilience. New York, NY: Guilford Publications; 2012:4–7. | ||
World Health Organization. Ottawa Charter for Health Promotion. Geneva: WHO; 1986. Available from: http://bit.ly/1uBBtiy. Accessed August 2, 2016. | ||
Walk at the beach. Available from: http://bit.ly/1WmTJtW. Accessed August 2, 2016. | ||
World Health Organization. Health Interview Surveys. Towards International Harmonization. Geneva: WHO. Available from: http://bit.ly/1uIUvle. Accessed August 2, 2016. | ||
DeSalvo KB, Bloser N, Reynolds K, He J, Muntner P. Mortality prediction with a single general self-rated health question. A meta-analysis. J Gen Intern Med. 2006;21(3):267–275. | ||
Zigmond AS, Snaith RP. The hospital anxiety and depression scale. Acta Psychiatr Scand. 1983;67(6):361–370. | ||
Woolf K, Cave J, McManus IC, Dacre JE. “It gives you an understanding you can’t get from any book”. The relationship between medical students’ and doctors’ personal illness experiences and their performance: a qualitative and quantitative study. BMC Med Educ. 2007;7:50. | ||
Quince TA, Wood DF, Parker RA, Benson J. Prevalence and persistence of depression among undergraduate medical students: a longitudinal study at one UK medical school. BMJ Open. 2012;2(4):pii:e001519. | ||
Herrmann-Lingen C, Buss U, Snaith RP. Hospital Anxiety and Depression Scale – Deutsche Version. 3. Auflage. Bern: Huber; 2011. | ||
Kötter T, Voltmer E. Measurement of specific medical school stress: translation of the “perceived medical school stress instrument” to the German language. GMS Z Med Ausbild. 2013;30(2):Doc22. | ||
Vitaliano PP, Russo J, Carr JE, Heerwagen JH. Medical school pressures and their relationship to anxiety. J Nerv Ment Dis. 1984;172(12):730–736. | ||
Chew-Graham CA, Rogers A, Yassin N. “I wouldn’t want it on my CV or their records”: medical students’ experiences of help-seeking for mental health problems. Med Educ. 2003;37(10):873–880. | ||
Faul F, Erdfelder E, Lang AG, Buchner A. G*Power 3: a flexible statistical power analysis program for the social, behavioral, and biomedical sciences. Behav Res Methods. 2007;39(2):175–191. | ||
Lane P. Handling drop-out in longitudinal clinical trials: a comparison of the LOCF and MMRM approaches. Pharm Stat. 2008;7(2):93–106. | ||
Moher D, Hopewell S, Schulz KF, et al. CONSORT 2010 Explanation and Elaboration: Updated guidelines for reporting parallel group randomised trials. J Clin Epidemiol. 2010;63(8):e1–37. | ||
Kötter T. Individual short-term coaching against exam-related stress – trial registry entry. Available from: http://bit.ly/1GxnsZs. Accessed August 2, 2016. | ||
Kötter T, Pohontsch NJ, Voltmer E. Stressors and starting points for health-promoting interventions in medical school from the students’ perspective: a qualitative study. Perspect Med Educ. 2015;4(3):128–135. | ||
Simard AA, Henry M. Impact of a short yoga intervention on medical students’ health: a pilot study. Med Teach. 2009;31(10):950–952. | ||
Dayalan H, Subramanian S, Elango T. Psychological well-being in medical students during exam stress-influence of short-term practice of mind sound technology. Indian J Med Sci. 2010;64(11):501–507. | ||
Pereira MA, Barbosa MA. Teaching strategies for coping with stress – the perceptions of medical students. BMC Med Educ. 2013;13(1):50. | ||
Shapiro SL, Shapiro DE, Schwartz GE. Stress management in medical education: a review of the literature. Acad Med. 2000;75(7):748–759. | ||
Joinson A. Social desirability, anonymity, and Internet-based questionnaires. Behav Res Methods Instrum Comput. 1999;31(3):433–438. |
 © 2016 The Author(s). This work is published and licensed by Dove Medical Press Limited. The full terms of this license are available at https://www.dovepress.com/terms.php and incorporate the Creative Commons Attribution - Non Commercial (unported, v3.0) License.
By accessing the work you hereby accept the Terms. Non-commercial uses of the work are permitted without any further permission from Dove Medical Press Limited, provided the work is properly attributed. For permission for commercial use of this work, please see paragraphs 4.2 and 5 of our Terms.
© 2016 The Author(s). This work is published and licensed by Dove Medical Press Limited. The full terms of this license are available at https://www.dovepress.com/terms.php and incorporate the Creative Commons Attribution - Non Commercial (unported, v3.0) License.
By accessing the work you hereby accept the Terms. Non-commercial uses of the work are permitted without any further permission from Dove Medical Press Limited, provided the work is properly attributed. For permission for commercial use of this work, please see paragraphs 4.2 and 5 of our Terms.