Back to Journals » Risk Management and Healthcare Policy » Volume 15
Reliability of Non-Contact Infrared Thermometers for Fever Screening Under COVID-19
Authors Lai F, Li X , Wang Q, Luo Y, Wang X, Huang X, Zhang J, Peng J, Wang Q, Fan L, Li W, Huo J, Liu T , Li Y, Lin Y, Yang X
Received 8 January 2022
Accepted for publication 3 March 2022
Published 10 March 2022 Volume 2022:15 Pages 447—456
DOI https://doi.org/10.2147/RMHP.S357567
Checked for plagiarism Yes
Review by Single anonymous peer review
Peer reviewer comments 2
Editor who approved publication: Professor Mecit Can Emre Simsekler
Fan Lai,1,* Xin Li,1,* Qi Wang,1,* Yingjuan Luo,1 Xin Wang,1 Xiuhua Huang,1 Jiajia Zhang,1 Jieru Peng,1 Qin Wang,1 Li Fan,1 Wen Li,1 Junrong Huo,1 Tianjiao Liu,1 Yalan Li,2 Yonghong Lin,1 Xiao Yang1
1Chengdu Women’s and Children’s Central Hospital, School of Medicine, University of Electronic Science and Technology of China, Chengdu, 611731, People’s Republic of China; 2The Fourth People’s Hospital of Chengdu, School of Medicine, University of Electronic Science and Technology of China, Chengdu, 611731, People’s Republic of China
*These authors contributed equally to this work
Correspondence: Xiao Yang; Yonghong Lin, Chengdu Women’s and Children’s Central Hospital, 1617 Riyue Avenue, Qingyang District, Chengdu, 611731, Sichuan, People’s Republic of China, Tel +86 13882288881 ; +86 13808031895, Email [email protected]; [email protected]
Purpose: Fever is one of the most typical clinical symptoms of coronavirus disease 2019 (COVID-19), and non-contact infrared thermometers (NCITs) are commonly used to screen for fever. However, there is a lack of authoritative data to define a “fever” when an NCIT is used and previous studies have shown that NCIT readings fluctuate widely depending on ambient temperatures and the body surface site screened. The aim of this study was to establish cut-off points for normal temperatures of different body sites (neck, forehead, temples, and wrist) and investigate the accuracy of NCITs at various ambient temperatures to improve the standardization and accuracy of fever screening.
Patients and Methods: A prospective investigation was conducted among 904 participants in the outpatient and emergency departments of Chengdu Women’s and Children’s Central Hospital. Body temperature was measured using NCITs and mercury axillary thermometers. A receiver operating characteristic curve was used to determine the accuracy of body temperature detection at the four body surface sites. Data on participant characteristics were also collected.
Results: Among the four surface sites, the neck temperature detection group had the highest accuracy. When the neck temperature was 37.35°C as the optimum fever diagnostic threshold, the sensitivity was 0.866. The optimum fever diagnostic thresholds for forehead, temporal, and wrist temperature were 36.65°C, 36.65°C, and 36.75°C, respectively. Moreover, triple neck temperature detection had the highest sensitivity, up to 0.998, whereas the sensitivity of triple wrist temperature detections was 0.949. Notably, the accuracy of NCITs significantly reduced when the temperature was lower than 18°C.
Conclusion: Neck temperature had the highest accuracy among the four NCIT temperature measurement sites, with an optimum fever diagnostic threshold of 37.35°C. Considering the findings reported in our study, we recommend triple neck temperature detection with NCITs as the fever screening standard for COVID-19.
Keywords: COVID-19, epidemiology, fever, infrared rays, mass screening
Introduction
The coronavirus disease 2019 (COVID-19) pandemic has spread rapidly worldwide and has become a major global public health event since the first case of COVID-19 was diagnosed in December 2019.1,2 China has effectively suppressed the spread of COVID-19 through active prevention and control. However, with the advent of the delta and omicron variants, the prevalence of COVID-19 presents a distinct upward trend.3–6 The delta variant has a 60% higher risk of community transmission than the ancestral alpha strain and can even cause asymptomatic infection in vaccinated patients.7–9 Omicron has numerous mutations with the potential to increase transmissibility, confer resistance to therapeutics, or partially escape infection- or vaccine-induced immunity.10,11 Considering that the current epidemic is sporadic and small-scale, which is different from the previous COVID-19 attacks, severe measures such as city-wide blockades or nationwide nucleic acid detection are not suitable However, routine screenings at entrances of crowd-gathering areas, especially hospitals, should still be conducted to screen out potentially infected individuals.
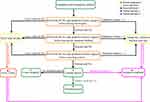
Although some COVID-19 cases are diagnosed with no obvious fever symptoms, fever is one of the most typical clinical symptoms of COVID-19, and occurs in more than 60% of all infectors, especially children and pregnant women.12–15 Since most COVID-19 infectors can be identified through early body temperature and epidemic history screening, temperature detection and epidemic history screening points were set at the entrance of all crowd-gathering areas in China to screen out possible infected persons. According to the regulations of the National Health Commission, triple body temperature and epidemic history screening were set up in outpatient and emergency departments.16 The flowchart of triple screening in the hospital is summarized in Figures 1 and 2.
Fever screening should follow the principles of rapid, accurate, and safe measurement.17–19 Non-contact infrared thermometers (NCITs) allow for rapid, wide-range body temperature measurement and are commonly used for body fever screening.20–24 However, there is a lack of authoritative data to define a “fever” when an NCIT is used, and several studies have reported that temperature measurements obtained from NCITs fluctuate widely. The different reference temperatures and fever thresholds were shown to be affected by different instruments, ambient temperatures, and body surface sites.25–27 Thus, it is essential to clarify the reliability of using NCITs for current routine body temperature detection.
Therefore, in the present study, we aimed to investigate the accuracy of NCITs for body temperature detection at four body surface sites and various ambient temperatures in outpatients. Additionally, we aimed to determine the optimum diagnostic threshold of fever at different body surface sites, standardize measurement sites, and unify fever reference standards to improve the standardization and accuracy of COVID-19 fever screening.
Patients and Methods
Study Design and Participants
This study was conducted between March 1 and April 30, 2021, and included outpatients and emergency patients who were willing to participate. The following patients were excluded from the study: those with unstable vital signs who needed to be rescued, those with mental illness or physical disability/disorder, and those whose body surface temperature could not be obtained (eg, because of antipyretic paste covering). The study was registered in the Chinese Clinical Trial Registry (No. ChiCTR2100049560) and was approved by the Ethics Committee of the Chengdu Women’s and Children’s Central Hospital (No. 202040). The study complies with the Declaration of Helsinki and written informed consent was obtained from all participants.
Data Collection
Participants’ sociodemographic data (age and sex) were collected using a standardized questionnaire (Supplementary Material). The data of patients’ preference of body temperature surface sites for temperature detection were collected from the questionnaire. Moreover, participants’ body temperature data were measured with NCITs (Model: JXB-178, measuring range 32.0°C–42.0°C, accuracy ±0.2°Cl Guangzhou Weierkang Medical Devices Co., Ltd) and mercury axillary thermometers (MATs; Model: CR.W11, Guangzhou Weierkang Medical Devices Co., Ltd) and were recorded immediately. All NCIT and MAT instruments were the same brand and signal, and each instrument was corrected before use. The ambient temperature was measured using an ambient temperature and humidity measuring instrument (WS2021, Tianjin Kehui Instrument Factory, China).
Body Temperature Data and Diagnostic Criteria
Before the study, all investigators received training on the use of NCITs and MATs, requirements for measuring sites and distances, measurement of ambient temperature and humidity, and data filling. Measuring body temperature strictly followed the triple temperature detections (level 1: hospital entrance; level 2: outpatient and emergency entrance; level 3: outpatient and emergency doctor consultation room). The distance from the hospital entrance to the Level 1 temperature detection point was approximately 400 m (approximately 5-min walk) (Figure 1), and the parking lot was located outside the hospital. NCITs were used in Levels 1 and 2, and NCITs and MATs were used in Level 3. Patients who were found to have body temperatures higher than 37.3°C in Levels 1 and 2 were immediately measured by MATs. Patients with an epidemic history of COVID-19 underwent nucleic acid testing, and their temperature was measured by MATs (Figure 2).
NCITs were used to detect the temperatures of the participants’ forehead, temple, neck, and wrist, 5 cm away from the body sites. NCIT measurements for the four body surface sites were compared with those obtained using MATs. Axillary temperature was considered a reference standard for three reasons. First, compared with NCITs, which are affected by different manufacturers, models, and the environment,28 measurements obtained using MATs are more consistent. Second, although some studies show that using MATs are time-consuming and that they do not have the highest sensitivity,29 it has been the mainstream method of body temperature measurement for a long time, especially in rural areas owing to its affordability and portability. Third, as oral temperature testing may increase the risk of COVID-19 and anal temperature is not suitable for large-scale body temperature detection, they were not used as screening standards. Fever was diagnosed when the temperature measured exceeded 37.3°C.29
Receiver Operating Characteristic (ROC) Curve
A ROC curve shows the trade-off between the sensitivity and specificity of fever screening.30 Body sites that yielded curves closer to the top-left corner indicated a better performance. The area under the ROC curve (AUC) was used as a criterion to measure the test’s discriminative ability, where the closer the AUC was to 1, the more efficient the fever screening test was. In this study, the cut-off value is the temperature diagnosed as fever. Patients whose body temperature is higher than the cut-off value are diagnosed as fever. Sensitivity was defined as the rate at which people were correctly identified as having fever. The Youden Index represents a summary measurement of the ROC curve for the accuracy of a diagnostic test with continuous endpoints.31 Youden index was used to determine the accuracy of body temperature measurements.
Statistical Methods
All statistical analyses were performed using SPSS version 25.0 (IBM, Armonk, NY, USA). Categorical variables are presented as counts and percentages, and continuous variables are presented as means and standard deviations. The ROC curve describes the accuracy of body temperature detection at the four body surface sites. All tests were two-tailed, and statistical significance was set at a p-value of <0.05.
Results
A total of 975 participants were initially recruited for this study. However, after excluding 71 participants who dropped out or whose complete data were lost, 904 participants were included in the final analysis. The descriptive data of the study participants are shown in Table 1. The mean age at recruitment was 29.63±6.30 years in adults and 3.71±3.25 years in children. In addition, 390 (46.1%) participants were male and 669 (74.0%) were children (<18 years old). Among the participants, 411 (45.5%) patients with axillary temperature of ≥37.3°C were diagnosed with fever. The ambient temperature was 14°C–29°C (mean: 19.8°C±3.72°C), and the humidity was 30–90%RH (mean: 55.60 ±11.60).
 |
Table 1 Description of the Participant Characteristics |
The temperatures measured at each body surface site were compared with the axillary temperature, and the results showed that the differences were statistically significant (p<0.001). The neck temperature was most consistent with and slightly higher than the axillary temperature, whereas the other body surface temperatures were lower than the axillary temperature (Table 1).
The accuracy of body temperature detection at the four body surface sites measured with NCITs was further analyzed using the ROC curve (Figure 3A). Among them, the neck temperature detection group had the largest AUC. When the neck temperature was 37.35°C as the optimum cut-off value, the highest Youden Index was 0.712, sensitivity was 0.866, and specificity was 0.846. The optimum cut-off values of forehead, temporal, and wrist temperatures were 36.65°C, 36.65°C, and 36.75°C, respectively, which were significantly lower than the axillary temperature. If 37.25°C is considered the diagnostic threshold of fever, the diagnostic sensitivity is 0.871, 0.496, 0.477, and 0.399 at the neck, forehead, temporal, and wrist sites, respectively (Table 2).
 |
Table 2 Description of the Accuracy of the NCITs on Four Body Surface Sites Measured with NCITs |
Considering that the ambient temperature may have a certain impact on NCIT measurements, the AUC of NCIT measurements at the four surface sites was described at various ambient temperatures (Figure 3B). Notably, AUC significantly reduced when the temperature was lower than 18°C and further decreased as the ambient temperature decreased during 14°C–18°C. However, the AUC of neck temperature (0.878) remained at a high at 14°C and remained basically above 0.9 when ambient temperature was 14°C–29°C.
Analysis of the triple temperature NCIT measurements revealed that the sensitivity of NCIT measurements at the four surface sites differed significantly (Table 3). The triple neck temperature detection had the highest sensitivity (up to 99.8%), whereas triple wrist temperature detection was only 94.9%.
 |
Table 3 Description of the Accuracy of NCITs on the Four Surface Sites by Triple Temperature Detection |
After analyzing participants’ opinions on the five temperature detection sites (Table 4), 236 (26.1%) participants preferred wrist temperature detection for convenience and 228 (25.2%) disliked axillary temperature detection, mainly because it was time-consuming. However, most participants (54.1%) were indifferent to the site of body temperature detection.
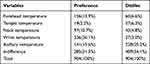 |
Table 4 Evaluation of Participants on the Five Temperature Detection Sites |
Discussion
This preliminary study investigated the accuracy of using NCITs for single and triple body temperature measurements at four body surface sites to improve the standardization and accuracy of COVID-19 fever screening.
Similar to previous studies, we found that body surface temperature measurements on the forehead, temple, and wrist were lower than that of the axillary temperature, whereas the neck temperature was slightly higher than the axillary temperature.32–35 These differences may be attributed to the temperature reduction caused by sweat on the forehead or temporal areas.36,37 Furthermore, the forehead and temple are typically exposed to ambient temperatures, whereas the neck is often concealed by the collar. The neck is also located near the carotid artery and is, thus, closer to the body’s core while the wrists are located at the extremities so that the blood supply provides far less heat than the neck. Given these influencing factors, it is predictable that the accuracy of NCIT measurements from the four surface sites differed, and that the sensitivity of neck temperature was significantly higher than that of the other three measurement sites.
Previous studies have reported that the ambient temperature has a certain impact on the accuracy of NCIT readings,21,37–40 which is consistent with our results. We found that the accuracy of NCIT measurements at the four surface sites was significantly reduced when the temperature was lower than 18°C, and further decreased as the ambient temperature dropped to 14°C. Nevertheless, the accuracy of neck temperature measurements was still maintained at a high level between 14°C and 29°C, possibly because the neck area was less affected by the external environment. Importantly, our findings also demonstrated that a single temperature measurement with an NCIT is insufficient for fever screening under COVID-19 because the highest sensitivity of a single measurement was just 0.866.
Similar to previous studies, we found that there were significant differences in the optimal diagnostic threshold of fever between different body surface sites.41,42 However, the optimal diagnostic thresholds of fever found in our study are different from previous studies. Wing P Chan et al found that when a tympanic temperature of 37.3°C or above was considered febrile, a corresponding cut-off value of 36.2°C when using an NCIT at the wrist was determined (0.864 sensitivity and 0.670 specificity).43 In fact, in our study, if 36.25°C is defined as the diagnostic standard of fever at wrist, the sensitivity is 0.830 and the specificity is 0.623, which are similar to their findings. At 36.25°C, the Youden index is 0.453 while that is 0.498 at 36.75°C. In order to compare the best diagnostic threshold of fever at four body surface sites, we selected the highest Youden value of each site for comparison. Of course, in fever screening, it is feasible to sacrifice some specificity for sensitivity. Appropriately reducing the diagnostic threshold of fever can improve the sensitivity of detecting fever patients and increasing the threshold can improve the specificity. For instance, 36.0°C was recommended as the fever diagnostic threshold of frontal temperature and 36.2°C and 37.5°C at wrist were taken in previous studies.20,44,45 Because of the differences in dressing habits and religious beliefs in different regions, as well as some individualized factors (such as physical disability and trauma), it is important to clarify the diagnostic threshold of fever at each body surface site. However, a considerable number of medical staff are unaware of this, and consider 37.3°C as the threshold for all fever screening methods; this lack of awareness is even more prevalent among non-medical staff. Therefore, standardized body temperature detection training for body temperature examiners is urgently needed, and our research group is currently conducting further research to investigate the understanding of fever diagnostic thresholds and the use of NCITs among body temperature examiners.
Under the regulations of the National Health Commission, Chinese hospitals were required to conduct a triple body temperature and epidemic history screening.16 In our study, we further tested the accuracy of this scheme. Triple neck temperature detection still had the highest sensitivity of 0.998, whereas the temporal and frontal temperatures had sensitivities of 0.994 and 0.990, respectively. Remarkably, the triple wrist temperature detection sensitivity was only 0.949, which is inconsistent with that in previous reports,20,46,47 questioning the accuracy of wrist temperature measurements for COVID-19 fever screening.
Due to the particularity of COVID-19, normalization management is necessary, which requires widespread participation and compliance. In the standardized questionnaire, we analyzed the participants’ views on the four temperature detection sites. A high proportion of participants (25.2%) disliked axillary temperature measurement, mainly because it was time-consuming. If the sensitivity of NCITs can be ensured, triple NCIT body temperature measurements could be a more rapid and convenient method of fever screening. Further exploration of measures for pandemic prevention and control is essential because it may aid preparation for the emergence of possible variant viruses or future virus pandemics.
The merit of our study is its large-scale and highly accurate data, which was confirmed by the same professional investigators and the same instruments. Additionally, the participants were followed up throughout the triple-measurement fever screening process, representing a relatively complete study design. Furthermore, our study had a large study population as it was conducted at one of the largest and most professional women’s and children’s hospitals in Southwest China that receives and treats women and children with fever on a daily basis.
Although this preliminary study contributes new knowledge on the use of single and triple NCIT measurements for accurate body temperature detection at the four body surface sites, it has several limitations. First, patients with hyperthermia (>40°C) did not participate in this study because of the severity of their condition. Therefore, the accuracy of NCIT measurements in patients with high fever requires further investigation. Second, during the study period, the ambient temperature range only fluctuated between 14°C and 29°C, and data beyond this range are lacking. Third, according to the epidemic prevention and control requirements of the National Health Commission, we only measured the temperature of these four common body surface sites, and the other sites considered to have high accuracy, such as the inner eye canthus and inner ear, have not been studied.48 Fourth, body temperature can be influenced by many factors. Although body surface sites, type of thermometer used, external environment and activities prior to measurement were controlled in this study, there are still some other influencing factors, such as circadian rhythm, age and ovulatory cycle, which were not included in the study design. A large-scale multi-center study including more participants, ambient temperatures, and body surface sites, is essential to better understand the accuracy of NCITs for single and triple temperature detection.
Conclusion
The neck was found to yield the most accurate NCIT temperature measurements among the four body sites, and the optimum fever diagnostic threshold was determined to be 37.35°C. However, single temperature measurement with an NCIT is insufficient for COVID-19 fever screening, we recommend triple neck temperature measurements with NCITs as a fever screening standard for COVID-19.
Abbreviations
BTD, body temperature detection; NCITs, non-contact infrared thermometers; MATs, mercury axillary thermometers; ROC, receiver operating characteristic; AUC, area under the curve; FT, forehead temperature; TT, temple temperature; NT, neck temperature; WT, wrist temperature; AT, axillary temperature; CI, confidence interval.
Data Sharing Statement
The data is available upon reasonable request to the corresponding author.
Acknowledgments
We thank the quarantined citizens, health workers, and all the other personnel in Chengdu who contributed to the prevention and control of COVID-19.
Author Contributions
All authors made a significant contribution to the work reported, whether that is in the conception, study design, execution, acquisition of data, analysis and interpretation, or in all these areas; took part in drafting, revising or critically reviewing the article; gave final approval of the version to be published; have agreed on the journal to which the article has been submitted; and agree to be accountable for all asects of the work.
Funding
Financial support of this work was provided by Chengdu Major Science and Technology Application Demonstration Project (No. 2021-YF09-00048-SN), Chengdu Municipal Medical Research Project (No. 2020216), and Chengdu Science and Technology Bureau (22ZDYF1597). The funding agencies did not have any role in the design of the study, collection, analysis, and interpretation of data, or in writing the manuscript.
Disclosure
The authors declare no conflicts of interest in this work.
References
1. Lu H, Stratton CW, Tang YW. The Wuhan SARS-CoV-2-What’s next for China. J Med Virol. 2020;92(6):546–547. doi:10.1002/jmv.25738
2. Ekstrom S, Andersson N, Lovquist A, et al. COVID-19 among young adults in Sweden: self-reported long-term symptoms and associated factors. Scand J Public Health. 2021;4:14034948211025425.
3. Mahase E. Covid-19: just a third of blood cancer patients had antibodies against delta variant after two vaccine doses, study finds. BMJ. 2021;375:n2623. doi:10.1136/bmj.n2623
4. Shiehzadegan S, Alaghemand N, Fox M, Venketaraman V. Analysis of the Delta Variant B.1.617.2 COVID-19. Clin Pract. 2021;11(4):778–784. doi:10.3390/clinpract11040093
5. Ferre VM, Peiffer-Smadja N, Visseaux B, Descamps D, Ghosn J, Charpentier C. Omicron SARS-CoV-2 variant: what we know and what we don’t. Anaesth Crit Care Pain Med. 2021;41(1):100998.
6. Thakur V, Ratho RK. OMICRON (B.1.1.529): a new SARS-CoV-2 variant of concern mounting worldwide fear. J Med Virol. 2021. doi:10.1002/jmv.27541
7. Hu K, Lin L, Liang Y, et al. COVID-19: risk factors for severe cases of the Delta variant. Aging (Albany NY). 2021;13:45.
8. Liu Y, Yang B, Liu L, Jilili M, Yang A. Occupational characteristics in the outbreak of the COVID-19 delta variant in Nanjing, China: rethinking the occupational health and safety vulnerability of essential workers. Int J Environ Res Public Health. 2021;18(20):65.
9. Christie B. Covid-19: vaccines are highly effective in preventing deaths from delta variant, study indicates. BMJ. 2021;375:n2582. doi:10.1136/bmj.n2582
10. Team CC-R. SARS-CoV-2 B.1.1.529 (Omicron) Variant - United States, December 1–8, 2021. MMWR Morb Mortal Wkly Rep. 2021;70(50):1731–1734.
11. Ai J, Zhang H, Zhang Y, et al. Omicron variant showed lower neutralizing sensitivity than other SARS-CoV-2 variants to immune sera elicited by vaccines after boost. Emerg Microbes Infect;2021. 1–24. doi:10.1080/22221751.2020.1868951
12. Cui X, Zhao Z, Zhang T, et al. A systematic review and meta-analysis of children with coronavirus disease 2019 (COVID-19). J Med Virol. 2021;93(2):1057–1069. doi:10.1002/jmv.26398
13. Perico L, Benigni A, Casiraghi F, Ng LFP, Renia L, Remuzzi G. Immunity, endothelial injury and complement-induced coagulopathy in COVID-19. Nat Rev Nephrol. 2021;17(1):46–64. doi:10.1038/s41581-020-00357-4
14. Gomez-Ochoa SA, Franco OH, Rojas LZ, et al. COVID-19 in health-care workers: a living systematic review and meta-analysis of prevalence, risk factors, clinical characteristics, and outcomes. Am J Epidemiol. 2021;190(1):161–175. doi:10.1093/aje/kwaa191
15. Roversi M, Raucci U, Pontrelli G, et al. Diagnosis of COVID-19 in children guided by lack of fever and exposure to SARS-CoV-2. Pediatr Res. 2021. doi:10.1038/s41390-021-01585-5
16. Li C, Tang L, Luo Y, et al. The prevention and control experience of maternal health care from Chengu, China during the COVID-19 epidemic. Risk Manag Healthc Policy. 2020;13:2213–2217. doi:10.2147/RMHP.S261821
17. Bassi A, Henry BM, Pighi L, Leone L, Lippi G. Evaluation of indoor hospital acclimatization of body temperature before COVID-19 fever screening. J Hosp Infect. 2021;112:127–128. doi:10.1016/j.jhin.2021.02.020
18. Zhang J, Liu S, Zhu B. Fever screening methods in public places during the COVID-19 pandemic. J Hosp Infect. 2021;109:123–124. doi:10.1016/j.jhin.2020.11.011
19. Buoite Stella A, Manganotti P, Furlanis G, Accardo A, Ajcevic M. Return to school in the COVID-19 era: considerations for temperature measurement. J Med Eng Technol. 2020;44(8):468–471. doi:10.1080/03091902.2020.1822941
20. Chen G, Xie J, Dai G, et al. Validity of the use of wrist and forehead temperatures in screening the general population for COVID-19: a Prospective Real-World Study. Iran J Public Health. 2020;49(Suppl 1):57–66. doi:10.18502/ijph.v49iS1.3670
21. Van den Bruel A, Verbakel J, Wang K, et al. Non-contact infrared thermometers compared with current approaches in primary care for children aged 5 years and under: a method comparison study. Health Technol Assess. 2020;24(53):1–28. doi:10.3310/hta24530
22. Aggarwal N, Garg M, Dwarakanathan V, et al. Diagnostic accuracy of non-contact infrared thermometers and thermal scanners: a systematic review and meta-analysis. J Travel Med. 2020;27(8). doi:10.1093/jtm/taaa193
23. Khan S, Saultry B, Adams S, et al. Comparative accuracy testing of non-contact infrared thermometers and temporal artery thermometers in an adult hospital setting. Am J Infect Control. 2021;49(5):597–602. doi:10.1016/j.ajic.2020.09.012
24. Foster J, Lloyd AB, Havenith G. Non-contact infrared assessment of human body temperature: the journal Temperature toolbox. Temperature (Austin). 2021;8(4):306–319. doi:10.1080/23328940.2021.1899546
25. Pang X, Zhu Z, Xu F, et al. Evaluation of control measures implemented in the severe acute respiratory syndrome outbreak in Beijing, 2003. JAMA. 2003;290(24):3215–3221. doi:10.1001/jama.290.24.3215
26. Bitar D, Goubar A, Desenclos JC. International travels and fever screening during epidemics: a literature review on the effectiveness and potential use of non-contact infrared thermometers. Euro Surveill. 2009;14(6). doi:10.2807/ese.14.06.19115-en
27. Sharif Nia H, Chong PP, Yiong Huak C, et al. Clinical accuracy and agreement between tympanic and forehead body temperature measurements for screening of patients with COVID-19. J Clin Nurs. 2021. doi:10.1111/jocn.16166
28. Pecoraro V, Petri D, Costantino G, et al. The diagnostic accuracy of digital, infrared and mercury-in-glass thermometers in measuring body temperature: a systematic review and network meta-analysis. Intern Emerg Med. 2021;16(4):1071–1083. doi:10.1007/s11739-020-02556-0
29. Kresch MJ. Axillary temperature as a screening test for fever in children. J Pediatr. 1984;104(4):596–599. doi:10.1016/S0022-3476(84)80558-2
30. Ruopp MD, Perkins NJ, Whitcomb BW, Schisterman EF. Youden Index and optimal cut-point estimated from observations affected by a lower limit of detection. Biom J. 2008;50(3):419–430. doi:10.1002/bimj.200710415
31. Youden WJ. Index for rating diagnostic tests. Cancer. 1950;3(1):32–35. doi:10.1002/1097-0142(1950)3:1<32::AID-CNCR2820030106>3.0.CO;2-3
32. Sener S, Karcioglu O, Eken C, Yaylaci S, Ozsarac M. Agreement between axillary, tympanic, and mid-forehead body temperature measurements in adult emergency department patients. Eur J Emerg Med. 2012;19(4):252–256. doi:10.1097/MEJ.0b013e32834c5841
33. Edling L, Carlsson R, Magnuson A, Holmberg H. [Forehead or axillary temperature measurement is not reliable. Methods and thermometers compared with rectal temperature measurement as a reference]. Lakartidningen. 2010;107(46):2888–2890. Swedish.
34. Shahat AM, Thundathil JC, Kastelic JP. Scrotal subcutaneous temperature is increased by scrotal insulation or whole-body heating, but not by scrotal neck insulation; however, all three heat-stress models decrease sperm quality in bulls and rams. J Therm Biol. 2021;100:103064. doi:10.1016/j.jtherbio.2021.103064
35. Liang M, Luo HX, Zhou P, Deng J. [A prospective randomized controlled study of the therapeutic effects of a self-developed novel low-temperature boric acid wet dressing on the face and neck wounds of patients with superficial burns]. Zhonghua Shao Shang Za Zhi. 2021;37(6):582–585. Chinese. doi:10.3760/cma.j.cn501120-20200820-00383
36. Lippi G, Henry BM, Leone L, Pighi L, Montagnana M. Variation of forehead temperature during routine working shift in hospital laboratory personnel: implications for SARS-CoV-2 screening. J Lifestyle Med. 2021;11(2):90–93. doi:10.15280/jlm.2021.11.2.90
37. Sullivan SJ, Seay N, Zhu L, et al. Performance characterization of non-contact infrared thermometers (NCITs) for forehead temperature measurement. Med Eng Phys. 2021;93:93–99. doi:10.1016/j.medengphy.2021.05.007
38. Chen Z, Wang H, Wang Y, Lin H, Zhu X, Wang Y. Use of non-contact infrared thermometers in rehabilitation patients: a randomized controlled study. J Int Med Res. 2021;49(1):300060520984617. doi:10.1177/0300060520984617
39. Erenberk U, Torun E, Ozkaya E, Uzuner S, Demir AD, Dundaroz R. Skin temperature measurement using an infrared thermometer on patients who have been exposed to cold. Pediatr Int. 2013;55(6):767–770. doi:10.1111/ped.12188
40. Hussain AS, Hussain HS, Betcher N, Behm R, Cagir B. Proper use of noncontact infrared thermometry for temperature screening during COVID-19. Sci Rep. 2021;11(1):11832. doi:10.1038/s41598-021-90100-1
41. Kasbekar R, Naz A, Marcos L, et al. Threshold for defining fever varies with age, especially in children: a multi-site diagnostic accuracy study. Nurs Open. 2021;8(5):2705–2721. doi:10.1002/nop2.831
42. Wright WF, Mulders-Manders CM, Auwaerter PG, Bleeker-Rovers CP. Fever of unknown origin (FUO) - A call for new research standards and updated clinical management. Am J Med. 2021;135:173–178. doi:10.1016/j.amjmed.2021.07.038
43. Chan WP, Kosik RO, Wang CJ. Considerations and a call to action for the use of noncontact forehead infrared handheld thermometers during the COVID-19 pandemic. J Glob Health. 2021;11:03023. doi:10.7189/jogh.11.03023
44. Holt SG, Yo JH, Karschimkus C, et al. Monitoring skin temperature at the wrist in hospitalised patients may assist in the detection of infection. Intern Med J. 2020;50(6):685–690. doi:10.1111/imj.14748
45. Chen HY, Chen A, Chen C. Investigation of the impact of infrared sensors on core body temperature monitoring by comparing measurement sites. Sensors (Basel). 2020;20(10). doi:10.3390/s20102885
46. Zhu TY, Rothenbuhler M, Hamvas G, et al. The accuracy of wrist skin temperature in detecting ovulation compared to basal body temperature: prospective comparative diagnostic accuracy study. J Med Internet Res. 2021;23(6):e20710. doi:10.2196/20710
47. Shan C, Hu J, Zou J, Zhang A. Wearable personal core body temperature measurement considering individual differences and dynamic tissue blood perfusion. IEEE J Biomed Health Inform. 2021;1. doi:10.1109/JBHI.2021.3124551
48. Budzan S, Wyzgolik R. Face and eyes localization algorithm in thermal images for temperature measurement of the inner canthus of the eyes. Infrared Phys Technol. 2013;60:225–234. doi:10.1016/j.infrared.2013.05.007
 © 2022 The Author(s). This work is published and licensed by Dove Medical Press Limited. The full terms of this license are available at https://www.dovepress.com/terms.php and incorporate the Creative Commons Attribution - Non Commercial (unported, v3.0) License.
By accessing the work you hereby accept the Terms. Non-commercial uses of the work are permitted without any further permission from Dove Medical Press Limited, provided the work is properly attributed. For permission for commercial use of this work, please see paragraphs 4.2 and 5 of our Terms.
© 2022 The Author(s). This work is published and licensed by Dove Medical Press Limited. The full terms of this license are available at https://www.dovepress.com/terms.php and incorporate the Creative Commons Attribution - Non Commercial (unported, v3.0) License.
By accessing the work you hereby accept the Terms. Non-commercial uses of the work are permitted without any further permission from Dove Medical Press Limited, provided the work is properly attributed. For permission for commercial use of this work, please see paragraphs 4.2 and 5 of our Terms.