Back to Journals » Journal of Hepatocellular Carcinoma » Volume 8
Recurrence of Hepatocellular Carcinoma After Liver Transplantation is Associated with Episodes of Acute Rejections
Authors Gül-Klein S , Kästner A, Haber PK, Krenzien F, Wabitsch S, Krannich A, Andreou A, Eurich D, Tacke F , Horst D, Pratschke J, Schmelzle M
Received 18 November 2020
Accepted for publication 21 January 2021
Published 18 March 2021 Volume 2021:8 Pages 133—143
DOI https://doi.org/10.2147/JHC.S292010
Checked for plagiarism Yes
Review by Single anonymous peer review
Peer reviewer comments 3
Editor who approved publication: Dr Ahmed Kaseb
Safak Gül-Klein,1 Anika Kästner,1 Philipp Konstantin Haber,1 Felix Krenzien,1 Simon Wabitsch,1 Alexander Krannich,2 Andreas Andreou,3 Dennis Eurich,1 Frank Tacke,4 David Horst,5 Johann Pratschke,1 Moritz Schmelzle1
1Department of Surgery, Campus Charité Mitte, Campus Virchow-Klinikum, Charité—Universitätsmedizin Berlin, Berlin, Germany; 2Clinical Study Center, Clinical Trial Office, Charité—Universitätsmedizin Berlin, Berlin, Germany; 3Division of Acute Care Surgery, Department of Visceral Surgery and Medicine, Inselspital, Bern University Hospital, Bern, Switzerland; 4Department of Hepatology/Gastroenterology, Charité—Universitätsmedizin Berlin, Berlin, Germany; 5Institute of Pathology, Charité—Universitätsmedizin Berlin, Berlin, Germany
Correspondence: Safak Gül-Klein
Department of Surgery, Campus Charité Mitte, Campus Virchow-Klinikum, Charité—Universitätsmedizin Berlin, Augustenburger Platz 1, Berlin, 13353, Germany
Email [email protected]
Purpose: The impact of acute rejection (AR) after liver transplantation (LT) for hepatocellular carcinoma (HCC) on patient outcome is uncertain. This aim of this study is to investigate whether AR is associated with HCC relapse and overall survival.
Patients and Methods: Patients undergoing LT for HCC between 2001 and 2015 were retrospectively analyzed with regard to histopathological proven AR within the median time until recurrence. Cox’s regression analysis was conducted revealing risk factors for HCC recurrence.
Results: HCC recurred in 47 of 252 analyzed patients with a median time to recurrence of 20 months. Patients with AR (28.6%) had a significantly higher frequency of recurrence compared to patients without AR (13.0%, p=0.002). Multiple Cox regression analyses identified AR within 20 months to be an independent risk factor for HCC recurrence both as dichotomized (HR=2.91, 95%CI: 1.30– 6.53; p=0.009) and as a continuous variable (HR=1.81, 95%CI: 1.28– 2.54; p=0.001). HCC recurrence and AR were associated with higher grades of liver fibrosis one year after LT, when compared to patients without AR (p=0.019).
Conclusion: Our results demonstrate an association of AR with HCC recurrence after LT with implications for intervals of monitoring in tumor surveillance. Graft fibrosis and immune mechanisms are potentially related and causal interactions are worth further investigation.
Keywords: histology, protocol liver biopsy, graft fibrosis, immunological mechanisms, predictors of tumor relapse
Introduction
The World Health Organization (WHO) reported hepatocellular carcinoma (HCC) to be the sixth most commonly diagnosed cancer and the fourth leading cause of cancer deaths worldwide in 2018.1 Potentially curative treatment strategies for HCC include liver transplantation (LT), liver resection (LR) and ablation. Among these options, LT is considered as first-line option for patients fulfilling benchmark criteria, especially for patients, in unsuitable condition for LR.2 Excellent long-term outcomes are achieved in selected HCC patients by LT as well as by LR with five-year survival rates between 60% and 70%.3–7 However, recurrent disease remains an persisting problem after LT with rates ranging from 9% to 16%.8,9 A first peak of intrahepatic recurrence—considered to be due to metastatic spread—is typically seen within the first 24 months after LR, whereas a second peak is postulated to be associated with de novo tumors in fibrotic grafts.10
Several oncological predictors for HCC recurrence are well known, eg vascular invasion, degree of differentiation, tumor size, number of nodules and satellites.8,11–15 During the past years different studies suggested some non-oncological risk factors in association with HCC recurrence, such as age, prolonged cold ischemia time (CIT; >10 h) and warm ischemia time (WIT; >50 min) as well as blood transfusion.16–21 Of note, biomarkers seem to play a key role in liver inflammation and ultimately tumor recurrence, such as being able to predict outcomes after LT.22 Particularly the neutrophil lymphocyte ratio (NLR) measured in the peripheral blood was found to be of importance in predicting outcome in several malignancies, including HCC. Several studies found that preoperative elevated NLR is associated with high risk of recurrence and death in patients with HCC undergoing LT.8,23–25
The incidence of acute rejection (AR) varies from 10% to 64% and its implications on patient outcomes after LT remains controversial.26–30 Toso et al stated that a history of AR is associated with a better postrecurrence survival after LT possibly linked to anticancer immunity.30 In contrast, other authors reported significantly increased risk of graft failure, mortality, and graft failure-related death regardless of primary liver disease but in association with AR.29 There is increasing evidence for the importance of immune responses in HCC; however, potential implications of AR on tumor recurrence after LT remain uncertain. Consequently, the aim of this study was to investigate associations between episodes of AR and HCC recurrence after LT.
Patients and Methods
Study Population
We analyzed all patients undergoing LT for HCC at the Department of Surgery, Campus Virchow-Klinikum, Charité—Universitätsmedizin Berlin between February 2001 and September 2015. Exclusion criteria were living donor LT (n=16), need for re-LT (n=22) or death within the median time to recurrence (20 months, n=38) and lost to follow-up (n=2).
The study focused on biopsy-proven AR after LT as potential risk factor for HCC recurrence. For this purpose, all liver biopsies were analyzed including routinely performed per protocol biopsies after LT as well as non-routinely performed biopsies for suspected AR. Episodes of AR occurring within the median time until HCC recurrence (20 months) were considered. HCC recurrence was defined as any tumor burden independent of the site, eg hepatic recurrence or distant metastases. Charité Local Ethics Committee approved data analysis (EA2/150/13). Medical records were reviewed based on the ethics vote of the IRB without an additional consent from the patients studied. First, all patients signed their informed consent to review their medical records at the time of liver transplantation. However, the retrospective study design was also causally related to this as a period of more than 13 years was studied, during which patients died. The privacy of all patients studied was kept confidential by anonymizing the data and following the Declaration of Helsinki. The owners of the data set are the authors of the study and they have collected the data through a retrospective evaluation. All organs were donated voluntarily with written informed consent and this was conducted in accordance with the Declaration of Istanbul.
Data Collection
Preoperative demographic characteristics and clinical variables included recipient and donor age at time of LT, recipient sex, body mass index (BMI) (in kg/m2), etiology of chronic liver disease, laboratory studies (alpha-fetoprotein (AFP) ≤200 µg/L vs >200 µg/L, NLR ≤4 vs >4, waiting time for LT ≤120 days vs >120 days, model of end-stage liver disease (MELD) score, beyond MILAN criteria (yes vs no) and bridging therapies to LT including LR, radiofrequency ablation (RFA) or transcatheter arterial chemoembolization (TACE) (yes vs no). Analyzed perioperative risk factors were CIT (>10 h) and WIT (>50 min). Oncological factors evaluated in the study were tumor size (>5 cm), >3 tumor nodules, bilobar HCC, T >2, vascular invasion and poor differentiation (G >2) in the explanted recipient liver (according to TNM classification at time of LT).
For patients undergoing LT with hepatitis C virus (HCV) viremia at time of transplant, duration of viremia after transplantation, type of HCV treatment (interferon, IFN; ribavirin, RBV; direct acting antiviral drugs, DAA) received post-LT and incidence of HCV recurrence were documented.
Immunosuppression
Standard immunosuppression (IS) regimens in our patient cohort consisted of calcineurin inhibitor (CNI)-based IS (FK506 rather than cyclosporine A; CyA) and low-dose steroid usage, with adjustments on an individual basis. Steroids were routinely tapered and stopped within three months after LT. Combination with antimetabolites as mycophenolate mofetil (MMF) were indicated on an individual basis, eg due to reduced renal function.
Baseline IS was reported in case of continuous application of at least three months in the first year after LT (median of values collected at 1, 3, 6, 9 and 12 months). In addition, usage of mammalian target of rapamycin inhibitors (mTORi—sirolimus, everolimus) was reported before diagnosis of recurrent disease or until last available follow-up (in the no recurrence group).
Post-LT Aftercare
The standardized performed aftercare included per protocol liver biopsies, laboratory AFP level measurement and sonographic examination of liver parenchyma in regard to steatosis, fibrosis and suspicious lesions after six months, 1, 3, 5, 7, 10, and 13 years post-LT. In case of suspected HCC recurrence, CT and/or MRI was performed. Recurrent disease was confirmed by radiological imaging in combination with elevated AFP levels or histopathological confirmation either by biopsy or partial resection.
Histopathology
Expert pathologists routinely analyzed liver biopsies. Paraffin-embedded liver biopsies were stained with H&E, Masson–Golder, iron and periodic-Schiff reagent. Histopathologic evaluation of liver tissue focused on signs of AR, as well as the presence and grading of fibrosis, median inflammation grades (hepatitis), steatosis, and cholangitis. Fibrosis was staged using a scale by Desmet et al (0: absent, 1: mild without septa, 2: moderate with few septa, 3: numerous septa without cirrhosis and 4: cirrhosis).31 Inflammation grades were assessed according to the classification by Desmet et al (0: none, 1: minimal, 2: mild, 3: moderate and 4: severe).31
Diagnosis and Therapy of AR
All ARs were histopathologically proven. No humoral rejections were included in this study. Common indications for non-protocol liver biopsy were elevated liver enzymes, cholestasis or liver dysfunction. The grading of severity of AR was classified according to Banff criteria and stratified as mild (score <5), moderate (5–6), and severe (7–9).32,33 According to histologically proven AR and clinical findings, treatment was initiated. Intravenous application of steroids represented the standard treatment of AR (methylprednisolone of 500 mg over three days). Moreover, dosage of CyA or FK506 was increased or MMF was added on an individual basis.
Statistical Analysis
For univariate analysis, continuous variables were reported as median (range), and categorical data as counts and percentages. Comparison of categorical data was performed, by using Pearson’s chi-squared test or Fisher's exact test. Mann–Whitney U-test or Student’s t test were used for continuous variables. OS and HCC recurrence rates were calculated by using Kaplan–Meier survival analysis with the log rank test for between-group comparison. Time until tumor recurrence was defined as the date of LT until tumor recurrence and censored at date of last available follow-up or death from nontumor-related causes. A sub-analysis was used to identify differences between patients with and without recurrent disease in regard to occurrence of AR. Therefore patients were divided into AR and no AR groups and again divided into HCC recurrence and no HCC recurrence. In addition, patients with HCC recurrence were separated into early (within 24 months) and late recurrence (>24 months) and compared within these groups. A subgroup analysis for HCV patients only was performed (see Supplemental Table 1).
To evaluate the association between potential risk factors for HCC recurrence, we conducted a multiple Cox proportional hazard regression with variables that were significant on the univariate analysis (p<0.05). Cox proportional regression analysis was used to develop a multiple model adjusting for the combined effects of pretransplant AFP >200 µg/L (yes vs no), preoperative NLR >4 (yes vs no), beyond MILAN (yes vs no), bilobar HCC expression (yes vs no), T grade >2 (yes vs no), grading >2 (yes vs no), and AR after LT (yes vs no) (model 1) or frequency of AR within 20 months (model 2). HRs were presented with 95%CI.
The statistical significance was set at p-value <0.05. All statistical analysis was performed using IBM SPSS Statistics version 22.
Results
Of 330 patients undergoing LT for HCC, 252 patients fulfilled the defined criteria and were subsequently analyzed (Figure 1). The main underlying etiology for chronic liver disease was alcoholic liver disease (n=107, 42.5%), followed by chronic HCV (n=83, 32.9%). During a mean follow-up time of 94.5±47.5 months, 47 patients (18.7%) developed recurrent disease. Of those one, two, three, and five-year recurrence rates were 21.3% (n=10), 57.4% (n=27), 70.2% (n=33), and 83.0% (n=39), respectively, with a median time until recurrence of 20 months (range: 5–108). Eight patients (17.0%) developed HCC recurrence in the liver graft, 16 patients (34.0%) had extrahepatic metastases and 23 patients (48.9%) had intra- and extrahepatic recurrence.
Histopathological proven AR occurred in 91 patients (36.1%) within the first 20 months after LT. The frequency of disease recurrence was significantly higher in patients with AR (28.6%) compared to patients without AR (13.0%, p=0.002). AR episodes within the first 20 months were more frequent in patients with HCC recurrence, when compared to patients without HCC recurrence (p=0.001, Figure 1). Furthermore, there was a tendency toward more frequent ARs within the first 30 days after LT in the HCC recurrence group (p=0.137, Figure 1). Of patients with AR, those with recurrent disease revealed significantly more episodes of AR (p=0.014) and were characterized by significantly higher grades of fibrosis one year after LT when compared to patients without recurrence (p=0.019). When comparing patients with and without AR, CIT >10 h were less frequent, whereas hepatitis was more frequent in patients with AR (Table 1).
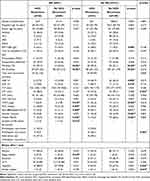 |
Table 1 Patient Characteristics and Perioperative Outcomes Compared Between Patients with Acute Rejection (AR) and without AR (No AR) Within 20 Months |
With regard to immunosuppression, there was no difference between the percentage of FK506 and CyA baseline usage (FK506: AR, n=85, 93.4%; no AR, n=150, 93.2%; p=0.942; CyA: AR, n=5, 5.5%; no AR, n=10, 6.2%, p=0.817) or between FK506 trough levels in patients with and without rejection (AR: 7.0, 1.3–12.3; no AR: 7.1, 1.0–13.5; p=0.711). Furthermore, there were no correlations between FK506 level and number of rejections (Spearman, r=–0.39; p=0.546). Correspondingly, no difference between percentage of FK506 usage on the one hand and recurrence on the other hand was found (no HCC recurrence, n=190, 92.7%; HCC recurrence, n=45, 95.7%, p=0.450). Usage of mTORi before HCC recurrence was also comparable between all groups (sirolimus: AR, n=18, 19.8%; no AR, n=28, 17.4%, p=0.637; everolimus: AR, n=5, 5.5%; no AR, n=13, 8.1%, p=0.445). Patients with recurrent disease received in 61.5% steroid bolus for first AR and patients without HCC recurrence in 61.9% of the cases (p=0.397). Only MMF was administered slightly more frequently in the group with rejections as opposed to the group without rejections (AR, n=55, 60.4%; no AR, n=65, 40.4%, p=0.002). Clinical and oncological features as well as histopathologic biopsy parameters are shown in Table 1 and therapy regimens for patients with AR are listed in Table 2.
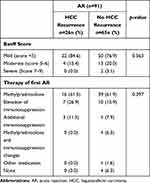 |
Table 2 Therapy of First AR Compared Between HCC Recurrence and No HCC Recurrence |
When comparing patients with early and late recurrent disease no significant differences with regard to preoperative and postoperative course as well as histopathologic features were found (Table 3). There was a tendency toward higher preoperative AFP levels in early HCC recurrence patients (p=0.067), whereas late recurrence tended toward prolonged cold ischemia times (p=0.078). Out of 47 patients with recurrent disease 33 (70.2%) were histologically proven, whereas 14 cases were radiologically confirmed in combination with elevated AFP levels with a median of 7063 µg/L.
 |
Table 3 Patient Characteristics and Perioperative Outcomes Compared Between Patients with Early HCC Recurrence and Late HCC Recurrence |
Risk Factor Analysis for HCC Recurrence
In univariate analysis, AFP >200 µg/L, NLR >4, HCC beyond MILAN, tumor size >5 cm and >3 nodules, bilobar HCC, poor differentiation (G >2), T3 and T4 stage and vascular invasion were associated with tumor recurrence (Table 4). AR within the first 20 months after LT were associated with recurrent disease as a continuous variable (HR=1.78, 95%CI: 1.35–2.35, p<0.001) as well as a dichotomized variable (HR=2.39, 95%CI: 1.34–4.25, p=0.003). Therefore, two Cox regression models were established: model 1 with AR as a dichotomized variable (yes vs no) and model 2 with AR as a a continuous variable (number of AR events) (Table 4).
 |
Table 4 Model 1 (AR as a Dichotomized Variable) and Model 2 (AR as a Continuous Variable): Analysis of Risk Factors for HCC Recurrence After OLT |
Statistically significant risk factors on univariate analysis were considered in multiple Cox analyses. Instead of taking tumor size, number, and vascularisation into account, the T stage was used.
AR within 20 months as a dichotomized variable (HR=2.91, 95%CI: 1.30–6.53, p=0.009) and as a continuous variable (HR=1.81, 95%CI: 1.28–2.54, p=0.001) were found to be statistically significant predictors for HCC-recurrence after LT. Other factors associated with HCC recurrence were baseline NLR >4, T3 or T4 stage of the tumor and bilobar HCC.
Discussion
Herein we report on the association between histopathological proven AR and HCC recurrence after LT for HCC. We showed that the occurrence of AR within the first 20 months after LT is an independent risk factor for HCC recurrence. While reported incidence rates of AR after LT vary, the 36.1% incidence we observed is generally in accordance with other studies.26–28,34 It has been described that younger recipient age, lack of renal impairment, higher aspartate aminotransferase (AST) levels, fewer human leukocyte antibody (HLA)-DR matches, longer cold ischemia times, and older donors were independently associated with an increased incidence of AR.27 Other reports on AR after LT discuss biliary complications as a potential cause and summarize that most ARs respond to bolus corticosteroid therapy.28 Our study revealed that overall mortality and survival regardless of the occurrence of AR was comparable in patients without recurrent disease.29
We hypothesize that the interplay of three key factors eventually determines the relationship between AR and tumor recurrence:
First, associations between immunosuppression and the risk of tumor recurrence after LT for HCC have been demonstrated previously.35 In our study cohort baseline FK506 usage during the first year post-LT was comparable between patients with and without HCC recurrence. This point is important because one could have imagined that associated number of rejections had more to do with the tailored immunosuppressive games in HCC patients at high oncological risk than with HCC recurrence itself. Of note, there were no correlations between FK506 level and number of rejections, respectively. MMF was indeed administered slightly more frequently in the group with rejections as opposed to the group without rejections, however, the clinical relevance is considered low in relation to the available literature.36,37 With regard to the use of mTORi before HCC recurrence, also no differences were found between both groups. This is important to emphasize, as it excludes a bias of antiproliferative immunosuppression on tumor recurrence.
Lai et al recently reported for the first time on the association between higher overall incidence of HCC recurrence and treatment of AR with steroid boluses.38 They hypothesized that the usage of steroid boluses to manage AR and exposure to longstanding immunosuppression after AR treatment promotes HCC recurrence.38 Based on our descriptive data, we cannot confirm or exclude causal links of steroid pulse therapy in episodes of AR and the risk of tumor recurrence. Interestingly, 65% of their matched control group consisted of patients without occurrence of AR.38 Therefore, their hypothesis is not controversial to our assumption that AR itself as inflammatory immune response could be triggering oncogenesis. Nonetheless, our findings seem to elucidate possible links between modulating immune responses and HCC recurrence after LT. Furthermore, Decaens et al found histologically proven acute rejections to be associated with significantly worsened five-year HCC recurrence-free survival after LT.39
Second, AR might trigger the development of fibrosis in grafts through sustained sterile inflammation.40 In pediatric patients an association between antibody-mediated AR and progress of graft fibrosis leading to liver graft damage after LT was reported.41,42 Furthermore, development and severity grade of liver fibrosis after LT is discussed as a potential predictor for death and graft loss in recipients.43 The chronically inflamed environment may promote carcinogenesis and may contribute to the increased frequency of tumor recurrence. This is supported by the papers suggesting a subclass of HCC tumors is linked to markers of immune invasion.44 Furthermore, liver fibrosis might be a factor not only associated with late, but also early phase recurrence after curative liver treatment.10 Until today no reports on the correlation of AR related inflammation as potential stimulus for fibrosis and furthermore to HCC recurrence were found.
Third, our results suggest a potential immunological role of frequent AR on HCC recurrence. As Li et al already discussed, the inflammatory microenvironment may play critical roles on orchestrating cancer cells together with immune cells to facilitate tumor recurrence post-LT.23 Interestingly, Motomura et al reported preoperative higher IL17 levels to be significantly associated with higher NLR, leading to shorter recurrence free survival, whereas IL17 also seems to be associated with the prediction of AR after LT.23,45 Moreover, high expression of IL17 was identified to enhance the proliferation in HBV-related HCC.46,47 In order to develop new markers for early phase liver graft injury leading to late phase tumor recurrence, we are in need of an improved understanding of the interplay between liver ischemia and inflammatory markers (eg IL17). In this regard, the role of immunoregulatory cells should be taken under focus.48 Of note, in patients with AR, hepatitis was found more frequently one year after LT, possibly contributing to development of fibrosis and recurrent disease.
As described widely in literature, patients with HCV need to be taken under special focus, since first IFN therapy can lead to more frequent episodes of AR and second, distinction between AR and HCV recurrence might be crucial.49 Therefore, we conducted a sub-analysis for this cohort, identifying no differences in regard to HCV viremia at the time of LT, HCV viremia duration post-LT, HCV recurrence and therapy of HCV (data not shown).
Our patient cohort was homogeneous, with a minimum length of follow-up of 20 months, with a sufficient observation time and regular post-LT check-ups. However, the results cannot be fully interpreted without considering specific limitations. The exclusion of patients who died before 20 months may potentially create a selection bias. Nevertheless, as shown in our supplemental analysis, no differences were noticed regarding the main hypothesis, that AR is associated with HCC recurrence. Of note, the study period of over 14 years at a single center must be reported as limitation. Therefore, in the long-term, results should be verified in a prospective study to mitigate the biases associated with a single center retrospective design. Nevertheless, serious consideration should be placed on the presence and frequency of AR within the first 20 months after LT as an early clinical marker for HCC recurrence. Therefore, those patients should be taken under special surveillance with the question of HCC recurrence.
Conclusion
The occurrence and frequency of episodes of AR within 20 months after LT is associated with HCC recurrence. Our results have implications for monitoring and tumor surveillance after LT. Although we cannot prove causal links to graft fibrosis and immunological mechanisms, hypothesized interactions are worth further investigation.
Acknowledgments
We gratefully thank for the raw data from Michael Hippler-Benscheidt and Yinan Wu and Robert Röhle for the statistical support from Clinical Trial Office of the Charité—Universitätsmedizin Berlin. We acknowledge support from the German Research Foundation (DFG) and the Open Access Publication Fund of Charité—Universitätsmedizin Berlin for open access publication costs.
Authorship
All authors made a significant contribution to the work reported, whether that is in the conception, study design, execution, acquisition of data, analysis and interpretation, or in all these areas; took part in drafting, revising or critically reviewing the article; gave final approval of the version to be published; have agreed on the journal to which the article has been submitted; and agree to be accountable for all aspects of the work. All authors have approved the final article.
Funding
The authors received no funding for this analysis; (they received funding for open access publication costs only).
Disclosure
Dr Moritz Schmelzle reports personal fees from Merck Serono and financial support of scientific meetings and OR courses from Bayer AG, ERBE Elektromedizin, Amgen Inc., Johnson & Johnson, Takeda Pharm.,Olympus K.K., Medtronic GmbH, and Intuitive Surg. Inc., outside the submitted work. The authors report no other potential conflicts of interest in this work.
References
1. Bray F, Ferlay J, Soerjomataram I, Siegel RL, Torre LA, Jemal A. Global cancer statistics 2018: GLOBOCAN estimates of incidence and mortality worldwide for 36 cancers in 185 countries. CA Cancer J Clin. 2018;68(6):394–424. doi:10.3322/caac.21492
2. European Association for the Study of the Liver, European Organisation for Research and Treatment of Cancer. EASL–EORTC Clinical Practice Guidelines: management of hepatocellular carcinoma. J Hepatol. 2012;56(4):908–943.
3. Forner A, Llovet JM, Bruix J. Hepatocellular carcinoma. Lancet. 2012;379(9822):1245–1255. doi:10.1016/S0140-6736(11)61347-0
4. Pinna AD, Yang T, Mazzaferro V, et al. Liver transplantation and hepatic resection can achieve cure for hepatocellular carcinoma. Ann Surg. 2018;268(5):868–875. doi:10.1097/SLA.0000000000002889
5. Krenzien F, Schmelzle M, Struecker B, et al. Liver transplantation and liver resection for cirrhotic patients with hepatocellular carcinoma: comparison of long-term survivals. J Gastrointest Surg. 2018;22(5):840–848. doi:10.1007/s11605-018-3690-4
6. Benzing C, Krezdorn N, Hinz A, et al. Mental status in patients before and after liver transplantation. Ann Transplant. 2015;20:683–693. doi:10.12659/AOT.894916
7. Llovet JM, Burroughs A, Bruix J. Hepatocellular carcinoma. Lancet. 2003;362(9399):1907–1917. doi:10.1016/S0140-6736(03)14964-1
8. Halazun KJ, Najjar M, Abdelmessih RM, et al. Recurrence after liver transplantation for hepatocellular carcinoma: a new moral to the story. Ann Surg. 2017;265(3):557–564. doi:10.1097/SLA.0000000000001966
9. Bina Possatto M, de Ataíde EC, Fazzio Escanhoela CA, et al. Factors related to hepatocellular carcinoma recurrence after liver transplantation—a brazilian multicenter study. Transplant Proc. 2017;49(4):863–866. doi:10.1016/j.transproceed.2017.01.055
10. Imamura H, Matsuyama Y, Tanaka E, et al. Risk factors contributing to early and late phase intrahepatic recurrence of hepatocellular carcinoma after hepatectomy. J Hepatol. 2003;38(2):200–207. doi:10.1016/S0168-8278(02)00360-4
11. Del Pozo EP, Bellido CB, Matín MS, et al. Recurrent hepatocellular carcinoma after liver transplantation: analysis of risk factors. Transplant Proc. 2016;48(9):2990–2993. doi:10.1016/j.transproceed.2016.09.020
12. Andreou A, Bahra M, Schmelzle M, et al. Predictive factors for extrahepatic recurrence of hepatocellular carcinoma following liver transplantation. Clin Transplant. 2016;30(7):819–827. doi:10.1111/ctr.12755
13. Llovet JM, Schwartz M, Mazzaferro V. Resection and liver transplantation for hepatocellular carcinoma. Semin Liver Dis. 2005;25(02):181–200. doi:10.1055/s-2005-871198
14. Mehta N, Heimbach J, Harnois DM, et al. Validation of a Risk Estimation of Tumor Recurrence After Transplant (RETREAT) score for hepatocellular carcinoma recurrence after liver transplant. JAMA Oncol. 2017;3(4):493. doi:10.1001/jamaoncol.2016.5116
15. Guerrini GP, Pinelli D, Di Benedetto F, et al. Predictive value of nodule size and differentiation in HCC recurrence after liver transplantation. Surg Oncol. 2016;25(4):419–428. doi:10.1016/j.suronc.2015.09.003
16. Nagai S, Yoshida A, Facciuto M, et al. Ischemia time impacts recurrence of hepatocellular carcinoma after liver transplantation. Hepatology. 2015;61(3):895–904. doi:10.1002/hep.27358
17. Seehofer D, Öllinger R, Denecke T, et al. Blood transfusions and tumor biopsy may increase HCC recurrence rates after liver transplantation. J Transplant. 2017;2017:1–9. doi:10.1155/2017/9731095
18. Montano-Loza AJ, Mazurak VC, Ebadi M, et al. Visceral adiposity increases risk for hepatocellular carcinoma in male patients with cirrhosis and recurrence after liver transplant: Montano-Loza, Mazurak. Hepatology. 2018;67(3):914–923. doi:10.1002/hep.29578
19. Liu B, Teng F, Fu H, et al. Excessive intraoperative blood loss independently predicts recurrence of hepatocellular carcinoma after liver transplantation. BMC Gastroenterol. 2015;15(1). doi:10.1186/s12876-015-0364-5.
20. Samoylova ML, Dodge JL, Yao FY, Roberts JP. Time to transplantation as a predictor of hepatocellular carcinoma recurrence after liver transplantation: waiting time is associated with HCC recurrence after LT. Liver Transpl. 2014;20(8):937–944. doi:10.1002/lt.23902
21. Wiltberger G, Wu Y, Lange U, et al. Protective effects of coffee consumption following liver transplantation for hepatocellular carcinoma in cirrhosis: XXXX. Aliment Pharmacol Ther. 2019;49(6):779–788. doi:10.1111/apt.15089
22. Amado V, Rodríguez-Perálvarez M, Ferrín G, De la Mata M. Selecting patients with hepatocellular carcinoma for liver transplantation: incorporating tumor biology criteria. J Hepatocellular Carcinoma. 2018;6:1–10. doi:10.2147/JHC.S174549
23. Motomura T, Shirabe K, Mano Y, et al. Neutrophil–lymphocyte ratio reflects hepatocellular carcinoma recurrence after liver transplantation via inflammatory microenvironment. J Hepatol. 2013;58(1):58–64. doi:10.1016/j.jhep.2012.08.017
24. Halazun KJ, Hardy MA, Rana AA, et al. Negative impact of neutrophil-lymphocyte ratio on outcome after liver transplantation for hepatocellular carcinoma. Ann Surg. 2009;250(1):141–151. doi:10.1097/SLA.0b013e3181a77e59
25. Agopian VG, Morshedi MM, McWilliams J, et al. Complete pathologic response to pretransplant locoregional therapy for hepatocellular carcinoma defines cancer cure after liver transplantation: analysis of 501 consecutively treated patients. Ann Surg. 2015;262(3):536–545. doi:10.1097/SLA.0000000000001384
26. Choudhary NS, Saigal S, Bansal RK, Saraf N, Gautam D, Soin AS. Acute and chronic rejection after liver transplantation: what a clinician needs to know. J Clin Exp Hepatol. 2017;7(4):358–366. doi:10.1016/j.jceh.2017.10.003
27. Wiesner RH, Demetris AJ, Belle SH, et al. Acute hepatic allograft rejection: incidence, risk factors, and impact on outcome. Hepatology. 1998;28(3):638–645. doi:10.1002/hep.510280306
28. Dogan N, Hüsing-Kabar A, Schmidt HH, Cicinnati VR, Beckebaum S, Kabar I. Acute allograft rejection in liver transplant recipients: incidence, risk factors, treatment success, and impact on graft failure. J Int Med Res. 2018;46(9):3979–3990. doi:10.1177/0300060518785543
29. Levitsky J, Goldberg D, Smith AR, et al. Acute rejection increases risk of graft failure and death in recent liver transplant recipients. Clin Gastroenterol Hepatol. 2017;15(4):584–593.e2. doi:10.1016/j.cgh.2016.07.035
30. Toso C, Cader S, Mentha-Dugerdil A, et al. Factors predicting survival after post-transplant hepatocellular carcinoma recurrence. J Hepatobiliary Pancreat Sci. 2013;20(3):342–347. doi:10.1007/s00534-012-0528-4
31. Desmet VJ, Gerber M, Hoofnagle JH, Manns M, Scheuer PJ. Classification of chronic hepatitis: diagnosis, grading and staging. Hepatology. 1994;19(6):1513–1520. doi:10.1002/hep.1840190629
32. An international panel is comprised of, Demetrius AJ, Batts KP, Dhillon AP, et al. Banff schema for grading liver allograft rejection: an international consensus document. Hepatology. 1997;25(3):658–663.
33. Demetris AJ, Banff Working Group. Liver biopsy interpretation for causes of late liver allograft dysfunction. Hepatology. 2006;44(2):489–501. doi:10.1002/hep.21280
34. Kim KJ, Li B, Winer J, et al. Inhibition of vascular endothelial growth factor-induced angiogenesis suppresses tumour growth in vivo. Nature. 1993;362(6423):841–844. doi:10.1038/362841a0
35. Lerut J, Iesari S, Foguenne M, Lai Q. Hepatocellular cancer and recurrence after liver transplantation: what about the impact of immunosuppression? Transl Gastroenterol Hepatol. 2017;2(10):80. doi:10.21037/tgh.2017.09.06
36. Toso C, Kneteman N. Does mycophenolate mofetil reduce the risk of late acute rejection after liver transplantation? Nat Rev Gastroenterol Hepatol. 2006;3(12):664–665. doi:10.1038/ncpgasthep0662
37. Schmeding M, Kiessling A, Neuhaus R, et al. Mycophenolate mofetil monotherapy in liver transplantation: 5-year follow-up of a prospective randomized trial. Transplantation. 2011;92(8):923–929. doi:10.1097/TP.0b013e31822d880d
38. Lai Q, Iesari S, Finkenstedt A, et al. Hepatocellular carcinoma recurrence after acute liver allograft rejection treatment: a multicenter European experience. Hepatobiliary Pancreat Dis Int. 2019;18(6):517–524. doi:10.1016/j.hbpd.2019.05.006
39. Decaens T. Roudot-Thoraval F, Bresson-Hadni S. Role of immunosuppression and tumor differentiation in predicting recurrence after liver transplantation for hepatocellular carcinoma: a multicenter study of 412 patients. WJG. 2006;12(45):7319. doi:10.3748/wjg.v12.i45.7319
40. Londoño M-C, Souza LN, Lozano -J-J, et al. Molecular profiling of subclinical inflammatory lesions in long-term surviving adult liver transplant recipients. J Hepatol. 2018;69(3):626–634. doi:10.1016/j.jhep.2018.04.012
41. Tokodai K, Miyagi S, Nakanishi C, et al. Association of post-transplant donor-specific HLA antibody with liver graft fibrosis during long-term follow-up after pediatric liver transplantation. Pediatr Transplant. 2018;22(3):e13169. doi:10.1111/petr.13169
42. Kurowski PN. Immunological factors and liver fibrosis in pediatric liver transplant recipients. Ann Transpl. 2015;20:279–284. doi:10.12659/AOT.892544
43. Bhat M, Ghali P, Rollet-Kurhajec KC, et al. Serum fibrosis biomarkers predict death and graft loss in liver transplantation recipients: serum fibrosis biomarkers in LT recipients. Liver Transpl. 2015;21(11):1383–1394. doi:10.1002/lt.24217
44. Sia D, Jiao Y, Martinez-Quetglas I, et al. Identification of an immune-specific class of hepatocellular carcinoma, based on molecular features. Gastroenterology. 2017;153(3):812–826. doi:10.1053/j.gastro.2017.06.007
45. Millán O, Rafael-Valdivia L, San Segundo D, et al. Should IFN-γ, IL-17 and IL-2 be considered predictive biomarkers of acute rejection in liver and kidney transplant? Results of a multicentric study. Clini Immunol. 2014;154(2):141–154. doi:10.1016/j.clim.2014.07.007
46. Hu Z, Luo D, Wang D, Ma L, Zhao Y, Li L. IL-17 activates the IL-6/STAT3 signal pathway in the proliferation of hepatitis b virus-related hepatocellular carcinoma. Cell Physiol Biochem. 2017;43(6):2379–2390. doi:10.1159/000484390
47. Huang Y, Wang F, Wang Y, et al. Intrahepatic interleukin-17 + T cells and FoxP3 + regulatory T cells cooperate to promote development and affect the prognosis of hepatocellular carcinoma: IL-17 + T cells and FoxP3 + Tregs in HCC. J Gastroenterol Hepatol. 2014;29(4):851–859. doi:10.1111/jgh.12418
48. Cescon M. Liver transplantation for hepatocellular carcinoma: role of inflammatory and immunological state on recurrence and prognosis. WJG. 2013;19(48):9174. doi:10.3748/wjg.v19.i48.9174
49. Bonaccorsi-Riani E, Pennycuick A, Londoño M-C, et al. Molecular characterization of acute cellular rejection occurring during intentional immunosuppression withdrawal in liver transplantation: molecular characterization of rejection. Am J Transpl. 2016;16(2):484–496. doi:10.1111/ajt.13488
 © 2021 The Author(s). This work is published and licensed by Dove Medical Press Limited. The full terms of this license are available at https://www.dovepress.com/terms.php and incorporate the Creative Commons Attribution - Non Commercial (unported, v3.0) License.
By accessing the work you hereby accept the Terms. Non-commercial uses of the work are permitted without any further permission from Dove Medical Press Limited, provided the work is properly attributed. For permission for commercial use of this work, please see paragraphs 4.2 and 5 of our Terms.
© 2021 The Author(s). This work is published and licensed by Dove Medical Press Limited. The full terms of this license are available at https://www.dovepress.com/terms.php and incorporate the Creative Commons Attribution - Non Commercial (unported, v3.0) License.
By accessing the work you hereby accept the Terms. Non-commercial uses of the work are permitted without any further permission from Dove Medical Press Limited, provided the work is properly attributed. For permission for commercial use of this work, please see paragraphs 4.2 and 5 of our Terms.

