Back to Journals » Neuropsychiatric Disease and Treatment » Volume 18
Radiological Features for Outcomes of MOGAD in Children: A Cohort in Southwest China
Authors Fan X , Li Q, Li T, He X, Feng C, Qin B , Xu Y, He L
Received 27 April 2022
Accepted for publication 17 August 2022
Published 26 August 2022 Volume 2022:18 Pages 1875—1884
DOI https://doi.org/10.2147/NDT.S372446
Checked for plagiarism Yes
Review by Single anonymous peer review
Peer reviewer comments 2
Editor who approved publication: Dr Yuping Ning
Xiao Fan,1 Qi Li,2 Tingsong Li,3 Xiaoyan He,4 Chuan Feng,1 Bin Qin,1 Ye Xu,1 Ling He1
1Department of Radiology, the Children’s Hospital of Chongqing Medical University, National Clinical Research Center for Child Health and Disorders, Ministry of Education Key Laboratory of Child Development and Disorders, Chongqing, People’s Republic of China; 2Department of Radiology, the First Affiliated Hospital of Chongqing Medical University, Chongqing, People’s Republic of China; 3Department of Neurology, the Children’s Hospital of Chongqing Medical University, National Clinical Research Center for Child Health and Disorders, Ministry of Education Key Laboratory of Child Development and Disorders, Chongqing, People’s Republic of China; 4Center for Clinical Molecular Medicine, the Children’s Hospital of Chongqing Medical University, National Clinical Research Center for Child Health and Disorders, Ministry of Education Key Laboratory of Child Development and Disorders, Chongqing, People’s Republic of China
Correspondence: Ling He, Department of Radiology, the Children’s Hospital of Chongqing Medical University, No. 136 Zhongshan Er Road, Yuzhong District, Chongqing, People’s Republic of China, Tel +86 13983399138, Email [email protected]
Background: Studies suggested that myelin oligodendrocyte glycoprotein antibody-associated disorders (MOGAD) are an isolated group of diseases that are different from multiple sclerosis (MS) and neuromyelitis optica spectrum disorders (NMOSD). The proportion of individuals with MOGAD is higher among children. However, limited data are available on autoimmune antibodies and neuroimaging features in children with MOGAD.
Methods: This study retrospectively reviewed 42 children with MOGAD. The clinical, neuroradiological, and cerebrospinal fluid data were compared according to courses and radiological results.
Results: Of the 42 patients, 28 suffered a monophasic course and 14 had a relapsing course. During the follow-up magnetic resonance imaging (MRI), 21 patients had a well-resolved brain condition and another 21 patients showed slight improvement with marked residuals. Most patients with relapse had cortical lesions and a leukodystrophy-like MRI pattern (all p < 0.05). Children with poor radiological outcomes have confluent and hazy lesions that involve both cortexes, white matter lesion of > 2 cm, and a leukodystrophy-like pattern, as well as cerebral lesions with T1 hypointensity or enhancement and spinal lesions (all p < 0.05). The multivariable logistic regression analysis used the aforementioned differential features and showed cerebral enhancement and a leukodystrophy-like pattern as the most effective variations associated with poor radiological outcomes of MOGAD with an area under the curve of 0.875.
Conclusion: MOGAD in children have some radiological features suggestive of clinical courses and radiological outcomes. A good understanding of these differential features can help to give early warnings of disease recurrence or poor radiological improvement and develop subsequent therapeutic strategies.
Keywords: myelin oligodendrocyte glycoprotein, encephalomyelitis, magnetic resonance imaging, demyelination, central nervous system
Introduction
Myelin oligodendrocyte glycoprotein (MOG) is a membrane protein that is expressed by oligodendrocyte cell surfaces and outermost myelin sheath surfaces. Recent studies suggested the role of immunoglobulin G serum antibodies on myelin oligodendrocyte glycoprotein (MOG-IgG) that is detected using a cell-based assay in (mostly recurrent) optic neuritis (ON), acute disseminated encephalomyelitis (ADEM)-like presentations, and myelitis, rather than classic multiple sclerosis (MS).1,2 Some neurological and radiological characteristics overlap, but MOG-IgG is now considered to denote a disease entity in its own right, distinct from classic MS and anti-aquaporin-4 (AQP4)-IgG-positive neuromyelitis optica spectrum disorders (NMOSD), which is currently often referred to as MOG antibody-associated disorders (MOGAD).3–5 A review of 61 studies reveals that MOGAD occurs in various age groups, generally ADEM-like or optic-spinal, and that the proportion of individuals with MOGAD is higher among children (40%) than among mixed cohorts (29%) and adults (22%).6
This study summarized a pediatric cohort with MOGAD and obtained an overview of its clinical phenotypes and corresponding radiological features to determine if any typical radiological features can help estimate the outcomes of the affected children.
Methods
Population
A total of 42 patients in this series were under the care of the Children’s Hospital of Chongqing Medical University (the biggest pediatric institution in Southwest China and one of the National Centers for Children’s Health in China) from January 2018 to December 2019. MOGAD is diagnosed following the Consensus of Chinese Experts.7 All children with MOG-IgG detected in their serum were included using a validated live cell-based assay with full-length human antigenic substrates at the China branch of Euroimmun Medical Diagnostic Laboratory (EUROIMMUN AG, Lübeck, Germany), and the initial samples were obtained before the anti-inflammatory therapy. Serum follow-up MOG samples were tested on 31 children.
The Ethics Committee of the Children’s Hospital of Chongqing Medical University approved this study (No.2017-83). This retrospective study complies with the Declaration of Helsinki. A parent or legal guardian provided informed consent on behalf of the patients. Clinical and radiological data were blindly and respectively reviewed by two experienced neurologists (T Li and X He) and two neuroradiologists (X Fan and Q Li). The consensus was reached through discussion if disagreements occur.
Clinical Data
The literature reported that the involved MOGAD indices were determined and recorded as follows: disease courses (monophasic and relapsing), Epstein–Barr virus (EBV) infection, cerebrospinal fluid (CSF) studies (cell count and oligoclonal bands [OCBs]), other demyelinating antibodies (AQP4-IgG and anti-myelin basic protein [MBP] antibody), and visually evoked potential, as well as clinical phenotypes at the onset. Considering the overlapping symptoms of MS and NMOSD, clinical phenotypes were divided into the following six subtypes: (a) ON, (b) ADEM, (c) myelitis, (d) seizures, (e) ataxia, and (f) area postrema syndrome. ADEM is diagnosed based on the International Pediatric MS Study Group recommendations, including the first polyfocal, clinical central nervous system (CNS) event with a presumed inflammatory demyelinating cause, encephalopathy that cannot be explained by fever, systemic illness or postictal symptoms, and an abnormal brain magnetic resonance imaging (MRI) during the acute phase compatible with ADEM and not indicative of another CNS disease.8
Blinded Radiological Analysis
All MRI examinations were assessed, including the following sequences: T1 and T2-axial, fluid-attenuated inversion recovery-axial, T2 sagittal, and T1 with a contrast medium (0.2 mL/kg, Omniscan, GE, USA) on axial, sagittal, and coronal views. A total of 26 patients continued to undergo spinal MRI a week after the onset, with sagittal and axial images on T1 and T2; however, only 10 finished the contrast-enhanced examination. Among 42 children, 19 underwent MRI using scanners with a field strength of 1.5 T (Signa Horizon Lx; General Electric Medical System, Milwaukee, WI, USA) and 23 using a 3.0 T scanner (Philips, Achieva 3T, Netherlands).
MR images of patients at the onset were reviewed, and the lesion distribution was recorded as follows: confluent and hazy lesions that involve both the cortex and white matter, cortical lesion, sharply demarcated white matter lesion (WML) of >2 cm, WML of <2 cm, and none or nonspecific lesion in the hemispheres, as well as lesions in the basal ganglia, thalamus, brainstem, cerebellum, and cerebellar peduncle. Additionally, enhancement, symmetrical distribution, and lesion located in the spinal cord were also recorded. Moreover, some specific features related to typical MS were estimated, such as T1 hypointensity, Dawson fingers, and tumefactive demyelinating lesions (TDLs), besides a leukodystrophy-like MRI pattern, one special feature suggesting poor outcomes. A leukodystrophy-like pattern is defined as extensive and confluent white matter abnormalities, with a largely symmetric distribution.9
A follow-up brain MRI is available for all included patients. Only 14 patients underwent spinal scanning due to previous lesions or suspected additional lesions. The initial and follow-up MR images were compared and categorized into the following four subgroups to assess the outcomes of MOGAD using MRI: (a) complete resolution (no abnormality), (b) minor residuals (greatly improved [<10% of the lesions remained]), (c) moderate residuals (mildly improved [10–50% of the lesions remained]), and (d) marked residuals (multiple abnormal signals [≥50% of the lesions remained], or atrophy).
All data on clinical outcomes (monophasic or relapsing course) and neuroradiological results (from complete resolution to marked residuals) were compared to determine the correlation between the initial clinical and neuroradiological characteristics and outcomes in pediatric patients with MOGAD.
Statistical Analysis
The Statistical Package for the Social Sciences statistical software package was used for statistical analyses (SPSS, version 19.0 for Windows; IBM; NY, USA). First, the Kolmogorov–Smirnov analysis was used to test the normality of continuous variables. Normally distributed quantitative data were expressed as mean ± standard deviation and analyzed using the two-independent samples Student’s t-test, whereas nonnormally distributed data were presented as median ± interquartile range and assessed using the Mann–Whitney U-test. Categorical variables were expressed as numbers and percentages and evaluated using the Chi-square test. A two-sided p-value of <0.05 was considered to be significantly different. Clinical and cerebral MRI features that significantly differed between the two groups were used to identify the most effective variations to predict poor improvement on MRI. The final regression model was selected using the forward condition method, and the area under the receiver operating characteristic curve (AUC), accuracy, sensitivity, and specificity was used to evaluate its diagnostic performance.
Results
Patients
A total of 42 children diagnosed with MOGAD (23 females) were estimated, with a mean age of 94.67 ± 31.79 months (range, 19–146 months) and a median MRI follow-up length of 5.5 months (range, 21 days to 28.5 months). The MOG-IgG titers in serum ranged from 1:32 to 1:320, with the cut-off value 1:32 (1:32 n = 29, 1:100 n = 10, 1:320 n = 3). MOG-IgG was detected in the CSF samples of 32 patients (titers range: 1:10–1:320), seven were negative, and three patients refused the test. None of them had AQP4 or MBP antibodies in the serum or CSF. Only two patients had OCBs with weak positive in their CSF samples (one was monophasic course and another was relapsed), eight patients refused to test OCBs, and the rest of the 32 patients were negative for OCBs in their CSF and serum samples. Generally, 28 pediatric patients suffered a monophasic course, whereas 14 had relapsed. During the last follow-up MRI, seven patients had completely resolved status and 14 had minor brain residues. Conversely, only nine patients had a slightly improved status and 12 had radiologically marked residuals. Regarding the statistical requirement, the former two subgroups were combined as the good improvement group (n = 21) and the other two subgroups were categorized into the poor improvement group (n = 21). All patients received persistent treatment with prednisolone and regular tapering under the professional guidance of a specialist neurologist in our institution.
Among 42 patients with MOGAD, 23 (54.8%) experienced an ADEM-like attack at onset, which was the most frequent, followed by 11 (26.2%) with ON (6 with bilateral ON) and 10 (23.8%) with myelitis. Surprisingly, 9 (21.4%) children had seizures, which was the only symptom in five patients. Ataxia occurred in only 4 (9.5%) patients. None of MOGAD manifested area postrema syndrome. Combined symptoms were manifested in 11 patients (7 with ADEM-like attack and myelitis, two with ADEM-like attack, myelitis, and ON, and four with ADEM-like attack and seizures). The MRI revealed the most common lesions in the thalamus (n = 23), followed by WML of <2 cm (n = 21), BA (n = 21), and the cortex (n = 20).
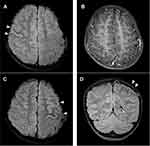
Then, the clinical phenotypes and corresponding radiological features were compared between different courses and radiological results, which are summarized in Tables 1 and 2. No significant differences were observed in age, gender, clinical, and CSF data between different disease courses or between radiological results (all p > 0.05). Only cell counting was positive for CSF testing, so the data were recorded. The MRI revealed the majority of pediatric patients with a relapsing course to have cortical lesions (Figure 1) and a leukodystrophy-like pattern (all p < 0.05). Other neuroradiological features had no significant differences between the courses (all p > 0.05).
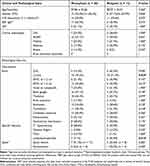 |
Table 1 Comparison of the Clinical and Corresponding Radiological Data Between Different Courses |
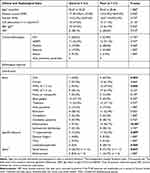 |
Table 2 Comparison of the Clinical and Corresponding Radiological Data Between Different Radiological Outcomes |
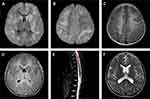
Regarding radiological outcomes, children with poor improvement (Figure 2) have confluent and hazy lesions that involve both the cortex and white matter, WML of >2 cm, and a leukodystrophy-like pattern (all p < 0.05). Moreover, cerebral lesions with T1 hypointensity or enhancement were significantly different between these two groups (all p < 0.05). Patients with poor radiological improvement were more likely to have spinal cord lesions than those with good improvement although few patients had the spinal cord data (n = 26) (p = 0.045).
Multiparametric Logistic Regression Analysis
Multiparametric analysis showed that cerebral enhancement and a leukodystrophy-like pattern were the most effective variations for predicting poor improvement for the model with clinical and cerebral MRI findings that significantly differed between the two radiological groups, with a diagnostic accuracy of 85.7%. The logistic regression function (P = 1/(1 + e (1.558–3.062 * cerebral enhancement–21.601 * leukodystrophy-like pattern))) obtained an AUC of 0.875 (95% confidence interval: 0.762–0.989; p < 0.001). We use a cut-off p-value of ≥0.496 for predicting poor improvement, with sensitivity and specificity of 81.0% and 90.5%, respectively.
Discussion
MOG is exclusively expressed in the CNS on the outermost surface of the myelin sheath and oligodendrocyte plasma membrane.10 MOG is a minor constituent of myelin, but its expression at the myelin sheath surface makes it accessible to antibodies and a candidate for CNS-targeted autoimmune responses in different species. The associated pathology is mediated by T cells and complement-fixing antibodies.6,11 MOGAD are rare, with a higher incidence in pediatric compared to adult patients, presented with various clinical phenotypes and associated radiological features.12 This study first compared the clinical and MRI features of 42 pediatric patients with MOGAD for different clinical and radiological outcomes, and then developed and validated a multivariable logistic regression model for predicting poor radiological outcomes. This retrospective analysis produced several major findings.
The clinical data from the pediatric series of MOGAD in Southwest China revealed it to slightly affect more girls (n = 23) than boys, with a median age of 7 years. Pediatric patients with high and persisting MOG-IgG titers were reported with a tendency to relapse.13 The titer was not included in the discussion, due to the low MOG-IgG titer (range: 1:32–1:320) in our series. None of them had AQP4 or MBP antibodies in the serum or CSF. We did not calculate the predictive OCB values because of inadequate cases (n = 2, weak positive). Our study revealed no significant difference was found in EBV infection for courses and radiological outcomes. The observation of intrathecal OCBs and the remote EBV infection confirmed previous findings.14–16 ADEM-like presentation at the onset of this younger-aged cohort was the most common clinical phenotype, which is consistent with recent observations that the clinical presentation of MOGAD changes with age.17 Approximately two-thirds of our patients experienced a monophasic course, which conforms to the recognition that MOGAD is a benign, non-MS demyelinating CNS disease. Some studies declare that recurrence is common in MOGAD. Most relapses occur in the early months after the onset of attack.17,18 Our institute started to conduct the MOG-IgG test by cell-based assay at the end of 2017, the MRI follow-up period ranged from 21 days to 28.5 months (median, 5.5 months), and nine children were followed up for <3 months; therefore, a relapse might be too early for these cases in our cohort. The literature has reported that irregular treatment or drug withdrawal can lead to relapse. Standard treatment was conducted among the children in this study since MOGAD diagnosis. All of them received persistent treatment with prednisolone and regular tapering to lower the risk of recurrence,19 which means therapy is less likely to result in a relapse.
This study aimed to determine the association between the disease courses and radiological outcomes and radiological features at the initial onset, which could give some clues for MOGAD in children from a neuroradiology perspective, although this is not a large cohort. After all, MRI is one of the main follow-up examinations.
The clinical outcomes revealed cortical lesions and a leukodystrophy-like pattern on MRI, which might suggest a relapsing course in children. Cortical involvement in imaging and presenting with seizures are categorized as a special MOGAD type, mainly in case reports on both children and adults from Japan or Europe.20–26 Patients with this presentation from Japan experienced different courses, but all of the European patients (from Spain and the United Kingdom) suffered a relapsing course. Of 18 patients with MOGAD with cortical involvement, 13 (72.2%) were reported in a mixed cohort from Shanghai, China, and cortical encephalitis was thought to be an important clinical MOGAD phenotype.27 Therefore, if a child presented with seizures and cortical encephalitis is depicted on MRI, clinicians should consider performing the MOG-IgG test and be aware of the risk of recurrence if the antibody is positive, although the mechanism remained unclear. Additionally, a leukodystrophy-like MRI pattern plays a role in the subsequent recurrence based on our observation. This finding is coherent with Hacohen et al’s study;9 however, the affected children with these extensive MRI presentations were younger (range, 1.7–6 years) than those in our cohort (range, 1.6–12.1 years). Thus, the immune damage mediated by MOG antibody disease could cause a wide range and severe myelin damage during childhood, even with the axonal loss, resulting in poor clinical outcomes.28 Doctors should be alert to this imaging pattern.
The radiological results revealed an equal good proportion and poor improvement (n = 21). Factors involved in poor neurological results in our study include confluent and hazy lesions that involve both the cortex and white matter, WML of >2 cm, and leukodystrophy-like patterns. These characteristics confirm the results of previous studies that MOG antibodies can induce extensive myelin damage and axonal loss.9,28 A recent study that used lesion volumetric analysis suggested that grey matter atrophy could be driven by the white matter bundle disruption projecting into the deep grey matter structures,29 which leads to poor radiological outcomes. It is also consistent with the most recent findings of MOGAD meeting MS diagnostic criteria by Fadda et al.30 Generally, MS is a chronic demyelinating disease in which the majority of patients suffer a progressive course. Hence, patients with MOGAD who meet the MS diagnostic criteria might experience a poorer outcome. Thus, should the radiologist recommend a follow-up MRI although no additional clinical manifestations show up when extensive white matter involvement is observed in patients suspected of MOGAD? Interestingly, future studies should assess whether relapsing patients with greater residual lesion load might predict a worse outcome, and thus require more aggressive therapy than those with lesion recovery. Likewise, cerebral lesions with T1 hypointensity were found to be more common in patients with poor recovery on MRI. T1 hypointensity is one of the typical features of MS.31,32 However, this imaging finding is consistent with histological observations in adults with fulminant episodes and MOG-IgG, depicting a so-called pattern II MS with demyelination and the presence of complement activation.33 Cerebral enhancement is also an imaging feature, which is more frequently observed in patients with MOGAD with poor radiological results. Previous radiological and pathological studies confirmed that enhancement demonstrates acute inflammatory reaction, causing blood–brain barrier (BBB) damage. This may explain the poor MRI results due to irreversible changes following BBB damage. Furthermore, spinal cord scanning is recommended if available, as abnormality implies the possibility of future residuals on imaging. Observations in adults or smaller pediatric cohorts have found some spinal cord imaging features that favor MOGAD diagnoses, such as the H-sign and leptomeningeal enhancement, and have shown few children experienced residual neurological deficits.34–37 These conflicting results among studies may be attributed to sampling size differences. Detailed imaging features will be further observed in a larger cohort.
Multivariable logistic regression analysis indicated that cerebral enhancement and a leukodystrophy-like pattern were the independent predictors of poor radiological outcomes of MOGAD. This model obtained an AUC, sensitivity, specificity, and accuracy of 0.875, 81.0%, 90.5%, and 85.7%, respectively, for predicting poor radiological outcomes of MOGAD.
This study has several limitations. This was a single-center, cross-sectional study with retrospective data collection. Our institution is highly specialized and serves as a national referral center. Therefore, only severe MOGAD cases may be encountered. Additionally, the radiological outcome measurement is subjective, and a few cases may be in the early disease stages due to a short follow-up time. Larger cohorts of milder cases and longer follow-up periods will be needed to further validate this observation.
Conclusion
Our findings demonstrate that MOGAD in children has some radiological features that suggest clinical courses and radiological outcomes. A good understanding of these differential features can give an early warning of disease recurrence or poor radiological improvement and develop subsequent therapeutic strategies.
Ethics Approval
The Ethics Committee of the Children’s Hospital of Chongqing Medical University approved this study (No.2017-83). This retrospective study complies with the Declaration of Helsinki.
Consent to Participate
A parent or legal guardian provided informed consent on behalf of the patients.
Author Contributions
All authors made a significant contribution to the work reported, whether that is in the conception, study design, execution, acquisition of data, analysis and interpretation, or in all these areas; took part in drafting, revising or critically reviewing the article; gave final approval of the version to be published; have agreed on the journal to which the article has been submitted; and agree to be accountable for all aspects of the work.
Funding
This work was supported by the Clinical New Technology Project in the Children’s Hospital of Chongqing Medical University [grant number 202026].
Disclosure
The authors declare that they have no conflict of interest.
References
1. Satukijchai C, Mariano R, Messina S, et al. Factors associated with relapse and treatment of myelin oligodendrocyte glycoprotein antibody-associated disease in the United Kingdom. JAMA Netw Open. 2022;5(1):e2142780. doi:10.1001/jamanetworkopen.2021.42780
2. Fadda G, Banwell B, Waters P, et al. Silent new brain MRI lesions in children with MOG-antibody associated disease. Ann Neurol. 2021;89(2):408–413. doi:10.1002/ana.25957
3. Reindl M, Jarius S, Rostasy K, et al. Myelin oligodendrocyte glycoprotein antibodies: how clinically useful are they? Curr Opin Neurol. 2017;30(3):295–301. doi:10.1097/WCO.0000000000000446
4. Zamvil SS, Slavin AJ. Does MOG Ig-positive AQP4-seronegative opticospinal inflammatory disease justify a diagnosis of NMO spectrum disorder? Neurol Neuroimmunol Neuroinflamm. 2015;2(1):e62. doi:10.1212/NXI.0000000000000062
5. Hohlfeld R, Dornmair K, Meinl E, et al. The search for the target antigens of multiple sclerosis, part 2: CD8+ T cells, B cells, and antibodies in the focus of reverse-translational research. Lancet Neurol. 2016;15(3):317–331. doi:10.1016/S1474-4422(15)00313-0
6. Reindl M, Waters P. Myelin oligodendrocyte glycoprotein antibodies in neurological disease. Nat Rev Neurol. 2019;15(2):89–102. doi:10.1038/s41582-018-0112-x
7. Immunology N B O T C S O. Chinese expert consensus on diagnosis and treatment of MOG-IgG associated disorders. Chin J Neuroimmunol Neurol. 2020;27(2):86–94.
8. Krupp LB, Tardieu M, Amato MP, et al. International Pediatric Multiple Sclerosis Study Group criteria for pediatric multiple sclerosis and immune-mediated central nervous system demyelinating disorders: revisions to the 2007 definitions. Multiple Sclerosis. 2013;19(10):1261–1267. doi:10.1177/1352458513484547
9. Hacohen Y, Rossor T, Mankad K, et al. ‘Leukodystrophy-like’ phenotype in children with myelin oligodendrocyte glycoprotein antibody-associated disease. Dev Med Child Neurol. 2018;60(4):417–423. doi:10.1111/dmcn.13649
10. Gardinier MV, Amiguet P, Linington C, et al. Myelin/oligodendrocyte glycoprotein is a unique member of the immunoglobulin superfamily. J Neurosci Res. 1992;33(1):177–187. doi:10.1002/jnr.490330123
11. Mader S, Gredler V, Schanda K, et al. Complement activating antibodies to myelin oligodendrocyte glycoprotein in neuromyelitis optica and related disorders. J Neuroinflammation. 2011;8. doi:10.1186/1742-2094-8-184
12. Bruijstens AL, Lechner C, Flet-Berliac L, et al. E.U. paediatric MOG consortium consensus: part 1 - classification of clinical phenotypes of paediatric myelin oligodendrocyte glycoprotein antibody-associated disorders. Eur J Paediatr Neurol. 2020;29:2–13.
13. Pröbstel AK, Dornmair K, Bittner R, et al. Antibodies to MOG are transient in childhood acute disseminated encephalomyelitis. Neurology. 2011;77(6):580–588. doi:10.1212/WNL.0b013e318228c0b1
14. Tintore M, Rovira À, Río J, et al. Defining high, medium and low impact prognostic factors for developing multiple sclerosis. Brain. 2015;138(Pt 7):1863–1874. doi:10.1093/brain/awv105
15. Balfour HH, Sifakis F, Sliman JA, et al. Age-specific prevalence of Epstein-Barr virus infection among individuals aged 6–19 years in the United States and factors affecting its acquisition. J Infect Dis. 2013;208(8):1286–1293. doi:10.1093/infdis/jit321
16. Hacohen Y, Mankad K, Chong WK, et al. Diagnostic algorithm for relapsing acquired demyelinating syndromes in children. Neurology. 2017;89(3):269–278. doi:10.1212/WNL.0000000000004117
17. Jurynczyk M, Messina S, Woodhall MR, et al. Clinical presentation and prognosis in MOG-antibody disease: a UK study. Brain. 2017;140(12):3128–3138. doi:10.1093/brain/awx276
18. Cobo-Calvo A, Ruiz A, Maillart E, et al. Clinical spectrum and prognostic value of CNS MOG autoimmunity in adults: the MOGADOR study. Neurology. 2018;90(21):e1858–e69. doi:10.1212/WNL.0000000000005560
19. Juryńczyk M, Jacob A, Fujihara K, et al. Myelin oligodendrocyte glycoprotein (MOG) antibody-associated disease: practical considerations. Pract Neurol. 2019;19(3):187–195. doi:10.1136/practneurol-2017-001787
20. Hino-Fukuyo N, Haginoya K, Nakashima I, et al. Clinical features and long-term outcome of a group of Japanese children with inflammatory central nervous system disorders and seropositivity to myelin-oligodendrocyte glycoprotein antibodies. Brain Dev. 2015;37(9):849–852. doi:10.1016/j.braindev.2015.02.006
21. Tsuburaya RS, Miki N, Tanaka K, et al. Anti-myelin oligodendrocyte glycoprotein (MOG) antibodies in a Japanese boy with recurrent optic neuritis. Brain Dev. 2015;37(1):145–148. doi:10.1016/j.braindev.2014.02.002
22. Ramberger M, Bsteh G, Schanda K, et al. NMDA receptor antibodies: a rare association in inflammatory demyelinating diseases. Neurol Neuroimmunol Neuroinflamm. 2015;2(5):e141. doi:10.1212/NXI.0000000000000141
23. Titulaer MJ, Höftberger R, Iizuka T, et al. Overlapping demyelinating syndromes and anti–N-methyl-D-aspartate receptor encephalitis. Ann Neurol. 2014;75(3):411–428. doi:10.1002/ana.24117
24. Ogawa R, Nakashima I, Takahashi T, et al. MOG antibody-positive, benign, unilateral, cerebral cortical encephalitis with epilepsy. Neurol Neuroimmunol Neuroinflamm. 2017;4(2):e322. doi:10.1212/NXI.0000000000000322
25. Fujimori J, Takai Y, Nakashima I, et al. Bilateral frontal cortex encephalitis and paraparesis in a patient with anti-MOG antibodies. J Neurol Neurosurg Psychiatry. 2017;88(6):534–536. doi:10.1136/jnnp-2016-315094
26. Hamid SHM, Whittam D, Saviour M, et al. Seizures and encephalitis in myelin oligodendrocyte glycoprotein IgG disease vs aquaporin 4 IgG disease. JAMA Neurol. 2018;75(1):65–71. doi:10.1001/jamaneurol.2017.3196
27. Wang L, Zhangbao J, Zhou L, et al. Encephalitis is an important clinical component of myelin oligodendrocyte glycoprotein antibody associated demyelination: a single-center cohort study in Shanghai, China. Eur J Neurol. 2019;26(1):168–174. doi:10.1111/ene.13790
28. Nave KA. Myelination and support of axonal integrity by glia. Nature. 2010;468(7321):244–252. doi:10.1038/nature09614
29. Messina S, Mariano R, Roca-Fernandez A, et al. Contrasting the brain imaging features of MOG-antibody disease, with AQP4-antibody NMOSD and multiple sclerosis. Multiple Sclerosis. 2022;28(2):217–227. doi:10.1177/13524585211018987
30. Fadda G, Waters P, Woodhall M, et al. Serum MOG-IgG in children meeting multiple sclerosis diagnostic criteria. Multiple Sclerosis. 2022;13524585221093789. doi:10.1177/13524585221093789
31. Jurynczyk M, Geraldes R, Probert F, et al. Distinct brain imaging characteristics of autoantibody-mediated CNS conditions and multiple sclerosis. Brain. 2017;140(3):617–627. doi:10.1093/brain/aww350
32. Patel J, Pires A, Derman A, et al. Development and validation of a simple and practical method for differentiating MS from other neuroinflammatory disorders based on lesion distribution on brain MRI. J Clin Neurosci. 2022;101:32–36. doi:10.1016/j.jocn.2022.04.035
33. Jarius S, Metz I, König FB, et al. Screening for MOG-IgG and 27 other anti-glial and anti-neuronal autoantibodies in ‘pattern II multiple sclerosis’ and brain biopsy findings in a MOG-IgG-positive case. Multiple Sclerosis. 2016;22(12):1541–1549. doi:10.1177/1352458515622986
34. Baumann M, Grams A, Djurdjevic T, et al. MRI of the first event in pediatric acquired demyelinating syndromes with antibodies to myelin oligodendrocyte glycoprotein. J Neurol. 2018;265(4):845–855. doi:10.1007/s00415-018-8781-3
35. Tantsis EM, Prelog K, Alper G, et al. Magnetic resonance imaging in enterovirus-71, myelin oligodendrocyte glycoprotein antibody, aquaporin-4 antibody, and multiple sclerosis-associated myelitis in children. Dev Med Child Neurol. 2019;61(9):1108–1116. doi:10.1111/dmcn.14114
36. Dubey D, Pittock SJ, Krecke KN, et al. Clinical, radiologic, and prognostic features of myelitis associated with myelin oligodendrocyte glycoprotein autoantibody. JAMA Neurol. 2019;76(3):301–309. doi:10.1001/jamaneurol.2018.4053
37. Fadda G, Alves CA, O’mahony J, et al. Comparison of spinal cord magnetic resonance imaging features among children with acquired demyelinating syndromes. JAMA Netw Open. 2021;4(10):e2128871. doi:10.1001/jamanetworkopen.2021.28871
 © 2022 The Author(s). This work is published and licensed by Dove Medical Press Limited. The full terms of this license are available at https://www.dovepress.com/terms.php and incorporate the Creative Commons Attribution - Non Commercial (unported, v3.0) License.
By accessing the work you hereby accept the Terms. Non-commercial uses of the work are permitted without any further permission from Dove Medical Press Limited, provided the work is properly attributed. For permission for commercial use of this work, please see paragraphs 4.2 and 5 of our Terms.
© 2022 The Author(s). This work is published and licensed by Dove Medical Press Limited. The full terms of this license are available at https://www.dovepress.com/terms.php and incorporate the Creative Commons Attribution - Non Commercial (unported, v3.0) License.
By accessing the work you hereby accept the Terms. Non-commercial uses of the work are permitted without any further permission from Dove Medical Press Limited, provided the work is properly attributed. For permission for commercial use of this work, please see paragraphs 4.2 and 5 of our Terms.