Back to Journals » Journal of Multidisciplinary Healthcare » Volume 13
Radiography Advanced Practice in the United Arab Emirates: The Perceptions and Readiness of Mammographers
Authors Abuzaid MM , Hamad W, Elshami W , Tekin H , Ali W, Khayal S
Received 4 June 2020
Accepted for publication 20 July 2020
Published 5 August 2020 Volume 2020:13 Pages 753—758
DOI https://doi.org/10.2147/JMDH.S262579
Checked for plagiarism Yes
Review by Single anonymous peer review
Peer reviewer comments 2
Editor who approved publication: Dr Scott Fraser
Mohamed M Abuzaid,1 Wijdan Hamad,1 Wiam Elshami,1 Huseyin Tekin,1 Wadah Ali,2 Simaa Khayal3
1Medical Diagnostic Imaging Department, College of Health Sciences, University of Sharjah, Sharjah, United Arab Emirates; 2Department of Medical Imaging, College of Health Sciences, Gulf Medical University, Ajman, United Arab Emirates; 3Independent Researcher, Dublin, Ireland
Correspondence: Mohamed M Abuzaid P.O. Box 27272, Sharjah, United Arab Emirates
Tel +971-6-5057572
Email [email protected]
Introduction: This study is a part of an effort to determine the challenges faced by the United Arab Emirates (UAE) radiographers towards role extension and advanced practice. It reflects the current practice and challenges facing role extension compared to international advancement. The study aimed to assess the radiographers who worked at mammography screening perception and readiness to accept role extension and advanced practice in mammography.
Methods: A cross-sectional descriptive study using an online survey was conducted among radiographers who practice mammography. The survey captured demographics, qualifications, professional education, future development plans, interest in role extension, and incentive to pursue the mammography profession.
Results: Forty-five radiographers were invited to participate in the study the response rate was 71% (n=32), 34.4 (11%) were UAE nationals with the remainder being expats. The majority were young between 25 and 45 years old (84.4%), 81.3% hold a BSc qualification. 56.3% completed a post-qualification training specialized mammography certificate. 81% of the participants showed interest in role extension after appropriate education, training, and supervision by radiologists.
Conclusion: This study reports on the perceptions and readiness of radiographers on advanced practice within breast-screening centers. The results show acceptance and support after proper training, clear career pathway, and licensing body recognition. The role of the radiographer in the UAE is still growing.
Keywords: advanced practice, radiography, radiographers, mammography, professional practice
Introduction
The role extension and advanced practice by radiographers in the field of mammography screening widely discussed and implemented in different health-care systems globally.1–9 In the UK, radiographer advanced practice is recognized in image interpretation for more than 40 years and over 20 years in mammography image interpretation.1,10,11 The use of advanced practitioners in the UK greatly improved health-care services and reporting turnaround times.11
Many countries such as the USA and some European countries have developed specialized practice positions with different scopes of practice, including image interpretation. In 2012, the Australian Inter-Professional Advisory Team (IPAT) released a paper proposing that the Australian Institute of Radiography (AIR) develops a structure for Advanced Practitioner status within the radiography profession. The experienced practitioner will also be able to perform some of the tasks normally performed by radiologists; this would help to relieve the workload of the radiologists. Whereas in the field of mammography screening, some of the skills defined advanced practice positions as possible in advanced practice roles include: image commenting, and interventional techniques (biopsies and hook wire localizations).12
In 2013, a study in role extension for Australian radiographers indicated that Australian radiographers working in Breast Screen programs had shown interest in role extension.6,13 In South Africa, 2016, an article stated that additionally trained mammographers could be employed as first readers of mammogram images, monitoring, and assuring the quality of protocols in place to minimize inaccuracies, which may cause undetected cancers.14
In addition, the literature indicated that radiologist shortages could be resolved if radiographers (also known as radiology technologists) or mid-level practitioners (physician assistants or nurse practitioners) were able to interpret mammograms and serve as first readers, thus assessing the existence or absence of suspicious images in cases that require further evaluation by radiologists.15 Since 2008, legislation in Denmark has mandated a national breast-screening plan. The Danish mammography screening system has a shortage of radiologists, which is partially solved by integrating of radiographers advanced practice in image interpretation of mammography screening images.14
The role of a radiographer is evolving and expanding globally, and the successful development among radiographers in other countries simulates a discussion about possibilities of a similar development in UAE as the UAE is not traditionally linked with promoting radiographers’ role change. This study is a part of a project studying the radiography practice transition in UAE.16,17
In the UAE, a radiographer’s role is concentrated mainly in the production of mammogram images: which are interpreted by a radiologist. In screening mammography systems, they are following the American college of radiology guidelines, which state that the image interpretation is conducted by two radiologists.18 This double-reading routine means that breast-screening programs are heavily dependent on a number of radiologists available in a health-care institute.
Radiographers undergraduate curriculum in the UAE were primarily prepared the profession to focus on image acquisitions in different image modalities with great concentration on patient care, radiation protection and radiation safety.16
The national breast-screening program in UAE aims to maximize the number of cancers detected and to decrease the number of recall rates. Therefore, this study initiates the discussion to identify possibilities to step forward towards involving radiographers in the image interpretation process. In addition, it aims to highlight the potential of radiographers’ development in the UAE and to investigate their perception attitudes toward role extension.
Materials and Methods
Study Design
A descriptive cross-sectional study using an online survey was conducted among radiographers working in mammography screening centers in the UAE.
Ethical Approval
An ethical approval obtained from the Research Ethics committee at the University of Sharjah. Participants signed an online consent form before starting the online survey to approve their participation in the study.
Instrument and Data Collection
The online survey consisted of closed-ended questions that captured the participants’ demographics, qualifications, country in which their terminal degree, experience in was obtained, general radiography and mammography practice, professional development plan, role extension interests, and incentives for choosing the mammography profession. Respondents were given options to choose extended work activities list they would like to perform, and the incentives would make specializing in mammography more attractive to them.
Radiographers who practice screening mammography in the “Northern Emirates,” the five emirates located in the North of the country, were invited to participate in the study. The survey was administered between September and December 2019. The survey link built-in “Google Form,” accompanied by the objective of the study and consent form, was sent directly to the radiographers’ by the research assistant. The survey collects no personal information, and participants were able to withdraw at any stage of the study. The withdraw or uncompleted survey excluded from the results.
S. Moran investigated the willingness of radiographers to accept new role extension responsibilities in mammography in Australia and gave permission to use the survey in this study.6 The survey was piloted to determine the participants’ understanding of questions, validity, and reliability of the contents by three senior radiographers. The comments and suggestions were used to improve the survey understandability based on the working nature in UAE.
Sample Size
It was difficult to determine the actual number of radiographers who undertake screening mammography role. Out of 272 radiographers registered in Ministry of Health and Prevention (MOHAP), the sample size was estimated to be 45 mammographers working at mammography screening centers.19
Inclusion and Exclusion Criteria
Data were obtained from radiographers who practiced mammography in their clinical site and were willing to participate during the study period.
Radiographers who did not submit the survey in the timeframe were excluded.
Statistical Analysis
Data analysis was conducted using the Statistical Package for Social Sciences (SPSS) Version 25®, and graphs were created using Microsoft Office Excel 2016®.
Results
The study was conducted among radiographers working at mammography screening centers in (MOHAP). Together with the participant’s demographic characteristics (part 1), thoughts and Scope of role Extension (part 2), and incentives and justifications for choosing mammography (Part 3).
Part One: Demographics and Participant’s Characteristics
A survey return rate of 71% (n=32) was returned from the invited population (n=45). Table 1 shows participant age, experience, and qualifications. The majority of participants considered young aged between 25 and 35 years old (n=21, 65.6%) (n=6, 18.8%) between 36 and 45 years old and 20 (62.6%) radiographers have experience more than 10 years. In terms of qualification (n=26), 81.3% completed a Bachelor’s degree (B.Sc.) in radiography, and (n=3), 9.4% held a master’s degree (M.Sc.) and (n=3), 9.4% are still possessing diploma qualifications. Of the total participants, 65.6% (n=21) were non-Emirati. A total of 34.4% (n=11) classified themselves as mammographers, whilst the rest of the participants identified themselves as radiographers. The results showed that 56.3% (n=18) of the participants completed a specialized mammography certificate after their terminal degree.
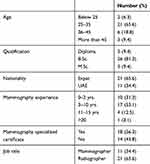 |
Table 1 Participants’ Characteristics |
Part Two: Thoughts and Scope of Role Extension
The survey defined the role extension based on the Australian and UK experience in the involvement of radiographers in six categories: 1) image interpretation; 2) core biopsies and localization; 3) administrative tasks, 4) Ultrasound assessment; 5) discussion of normal mammography results and others which include 6) research activity, QA, tutoring, and patient education. The participants were able to select multiple responses from the given options. Generally, the majority of the participants (81%) showed an interest in extending their role after appropriate preparation to improve their knowledge and clinical skills. The response to the question “which area you would like to have role extension in the future?”, image interpretation showed the highest level of interest (70%) followed by ultrasound (20%) and core biopsies and localization (10%) Table 2.
 |
Table 2 Role Extensions Area of Interests |
In regards to future education, the participants responded that they have a personal education plan (n=28, 87.2%). Out of them, 23 participants stated that their education plan is organized in coordination with their workplace. The participants’ answers to the question “What is the type of post-qualification education you prefer for mammography role extension?”. The majority of the participants (n=17, 53%) were interested in having a post-graduate certificate (Pg.Cer) in mammography.
Part Three: Incentives and Justifications for Choosing Mammography
The survey provided four possible incentives and justifications that make role extension and specializing in mammography more attractive to them (Table 3). The greatest perceived incentive to the participants was the nature of the job (56%) and personal and self-satisfaction (55%).
 |
Table 3 Incentives and Justification for Choosing Mammography Profession |
Discussion
Due to the low number of local scientific studies on the radiographer role extension, this study can shape the literature for future opportunities. The discussion of role extension in UAE can utilize the radiographers’ skills for potential effectiveness and efficient use of human resources.
This study aimed to understand the radiographer’s perceptions and willingness toward role extension in mammography practice. The integration of role extension in radiology practice proves to bridge the gap between an image taken and receiving of the final report due to the number of radiologists, workload, an increased number of patients and images.
Participation in image interpretation and breast ultrasound identified as essential elements in radiologist workload reduction and patient outcome improvement. The radiographers would feel confident to undertake extra views and complete the exam instead of waiting for the radiologist decision can reduce recall rate and, highly, improve patient satisfaction.
The result reflected the low number of radiographer who trained to perform duties other than mammography image production, this include; ultrasound assessment; image interpretation, and core biopsies. The author’s opinion that mammographers were occupied with high workload and job description restrictions. Most of the participants show definite basic qualifications or professional development with a desire to perform role extension after proper training and supervised practice by radiologists. Formal training and qualification supported by higher academic institutes, professional bodies, and workplaces will be welcomed and have great support from the mammographer to practice role extension. Such training will reduce the issues related to medico-legal and personal responsibilities.
Supervised role extension duties by radiologists will improve the confidence to provide independent image interpretation or ultrasound assessment. In Australia, the confidence level to practice role extension for mammographers with no formal training increased when they ensure that appropriate supervision and support provided by radiologists. In the UK; the high confidence of advanced mammographer practitioners is due to long experiences, proper training, and trust by some health organizations as first or second readers.5,13 The mammographer advance practitioner shows a clear understanding of their role extension is not going to replace the radiologists rather than creating a cooperative and interrelated work team.
Job satisfaction and nature of the job were the highest priority for the mammographer to select it as a profession and to extend their practice role. These two factors considered essential elements to increase the quality of practice and will lead to better utilization of human resources as well as building young Emirati professional leaders in health-care systems.
A discussion for the development of the UAE health-care system in relation to the cost, human resources, and building of Emirati health-care professionals should be raised and supported by research-based evidence. A linkage between the licensing system, professional body, and stakeholders is important to support the quality of care. This approach would be a potential opportunity for the UAE to pursue the development of the radiography profession; it will challenge the system advancements to be amongst international experience, for example, in Australia and the UK.
Conclusions
As mentioned earlier, this study is a part of a research effort to establish radiographer’s knowledge,17,20 practice21,23 and education16,24,25 assessment in UAE. A well-designed training program should not be underestimated and it will strength the radiographer’s skills and bring the practice to a higher level.
Radiographer role extension in the field of mammography can be designed in phases starting with needs assessment and acceptance studies, development of advance education and training program, implementation, career pathway development, and evaluation for improvement.
The advanced practitioner, especially at the screening centers, can play a role as the first image interpreter, selecting positive-negative cases, ultrasound assessment, and extra views requisitions.
Disclosure
The authors report no conflicts of interest for this work.
References
1. Milner RC, Snaith B. Are reporting radiographers fulfilling the role of advanced practitioner? Radiography. 2017;23(1):48–54. doi:10.1016/j.radi.2016.09.001
2. Henderson I, Mathers SA, McConnell J, Minnoch D. Advanced and extended scope practice of radiographers: the Scottish perspective. Radiography. 2016;22(2):185–193. doi:10.1016/j.radi.2015.12.002
3. Kelly J, Hogg P, Henwood S. The role of a consultant breast radiographer: A description and a reflection. Radiography. 2008;14(SUPPL. 1):2–10. doi:10.1016/j.radi.2008.10.003
4. Moran S, Warren-Forward H. The diagnostic accuracy of radiographers assessing screening mammograms: A systematic review. Radiography. 2016;22(2):137–146. doi:10.1016/j.radi.2015.09.008
5. Moran S, Warren-Forward H. Can Australian radiographers assess screening mammograms accurately? Biennial follow-up from a four year prospective study and lesion analysis. Radiography. 2016;22(3):e201–6. doi:10.1016/j.radi.2016.02.007
6. Moran S, Warren-Forward H. Assessment of the willingness of radiographers in mammography to accept new responsibilities in role extension: part one quantitative analysis. Radiography. 2011;17(4):270–274. doi:10.1016/j.radi.2011.06.003
7. Warren-Forward HM, Taylor J. Barriers and incentives for choosing to specialise in mammography: qualitative analysis. Radiography. 2017;23(1):32–37. doi:10.1016/j.radi.2016.07.009
8. Warren-Forward HM. Barriers and incentives for choosing to specialise in mammography a survey of Australian undergraduate diagnostic radiography students. Radiography. 2018;6–11.
9. Moran S, Warren-Forward H. The Australian BreastScreen workforce: a snapshot. J Med Radiat Sci. 2012;59(1):26–30.
10. Rees Z. Consultant breast radiographers: where are we now? An evaluation of the current role of the consultant breast radiographer. Radiography. 2014;20(2):121–125doi:10.1016/j.radi.2013.12.005
11. Deane L, Robinson L, England A. An investigation into the perceived value of the College of Radiographers voluntary accreditation scheme for advanced and consultant practitioners in breast imaging. Radiography. 2019;25(3):207–213. doi:10.1016/j.radi.2019.01.004
12. Moran S, Warren-Forward H. Can Australian radiographers assess screening mammograms accurately? First stage results from a four year prospective study. Radiography. 2016;22(2):e106–11. doi:10.1016/j.radi.2015.11.005
13. Moran S, Taylor JK, Warren-Forward H. Assessment of the willingness of Australian radiographers in mammography to accept new responsibilities in role extension: part two qualitative analysis. Radiography. 2013;19(2):130–136. doi:10.1016/j.radi.2012.12.006
14. Amanda LOUW. A Training Programme to Support an Extended Scope of Practice for South African Mammographers. University of Johannesburg; 2017.
15. Torres-Mejía G, Smith RA, de la Luz Carranza-flores M, et al. Radiographers supporting radiologists in the interpretation of screening mammography: A viable strategy to meet the shortage in the number of radiologists. BMC Cancer. 2015;15(1):1–12. doi:10.1186/s12885-015-1399-2
16. Abuzaid MM, Elshami W, McConnell J, Baird M. Changing the model of radiography practice in the UAE: A snapshot of a profession in transition. Radiography. 2020.
17. Abuzaid MM, Elshami W, Noorajan Z, Khayal S, Sulieman A. Assessment of the professional practice knowledge of computed tomography preceptors. Eur J Radiol Open. 2020;7.
18. The National Cancer Screening Initiative Committee. The national guidelines for breast cancer screening and diagnosis [internet]. 2014. Available from: www.mohap.gov.ae.
19. Elshami W, Abuzaid M, Piersson AD, et al. Occupational dose and radiation protection practice in UAE: a retrospective cross-sectional cohort study (2002–2016). Radiat Prot Dosimetry. 2019;187(4):426–437. doi:10.1093/rpd/ncz184
20. Elshami W, Elamrdi A, Alyafie S, Abuzaid M. Continuing professional development in radiography: practice, attitude and barriers. Int J Med Res Heal Sci. 2016;5(1):68.
21. Abuzaid MM, Elshami W, Hasan H. Knowledge and adherence to radiation protection among healthcare workers at operation theater. Asian J Sci Res. 2018;12(1):54–59. doi:10.3923/ajsr.2019.54.59
22. Abuzaid MM, Elshami W, Shawki M, Salama D. Assessment of compliance to radiation safety and protection at the radiology department. Int J Radiat Res. 2019;17:3.
23. Abuzaid MM, Saad R, Elshami W, Alyafei S. The effect of digital imaging on radiography work practice. Int J Sci Technol Res. 2015;4(07). Internet www.ijstr.org. Available from
24. Abuzaid M, Elshami W Integrating of scenario-based simulation into radiology education to improve critical thinking skills. Reports Med Imaging. 9. 17–22. doi:10.2147/RMI.S110343.
25. Abuzaid MM, Elshami W, Stevens LDAB. Perceptions of E-Portfolio use in lifelong learning and professional development among radiology professionals [internet]. Curr Med Imaging Rev. 2017;13:1–7. doi:10.2174/1573405613666170105153425
 © 2020 The Author(s). This work is published and licensed by Dove Medical Press Limited. The full terms of this license are available at https://www.dovepress.com/terms.php and incorporate the Creative Commons Attribution - Non Commercial (unported, v3.0) License.
By accessing the work you hereby accept the Terms. Non-commercial uses of the work are permitted without any further permission from Dove Medical Press Limited, provided the work is properly attributed. For permission for commercial use of this work, please see paragraphs 4.2 and 5 of our Terms.
© 2020 The Author(s). This work is published and licensed by Dove Medical Press Limited. The full terms of this license are available at https://www.dovepress.com/terms.php and incorporate the Creative Commons Attribution - Non Commercial (unported, v3.0) License.
By accessing the work you hereby accept the Terms. Non-commercial uses of the work are permitted without any further permission from Dove Medical Press Limited, provided the work is properly attributed. For permission for commercial use of this work, please see paragraphs 4.2 and 5 of our Terms.
