Back to Journals » International Journal of General Medicine » Volume 14
Pulmonary Barotrauma in COVID-19 Patients: Invasive versus Noninvasive Positive Pressure Ventilation
Authors Hamouri S , Samrah SM , Albawaih O , Saleh Z , Smadi MM , Alhazymeh A, Syaj S
Received 8 April 2021
Accepted for publication 6 May 2021
Published 24 May 2021 Volume 2021:14 Pages 2017—2032
DOI https://doi.org/10.2147/IJGM.S314155
Checked for plagiarism Yes
Review by Single anonymous peer review
Peer reviewer comments 2
Editor who approved publication: Dr Scott Fraser
Shadi Hamouri,1 Shaher M Samrah,2 Omar Albawaih,1 Zidan Saleh,2 Mahmoud M Smadi,3 Ahmad Alhazymeh,1 Sebawe Syaj1
1Department of General Surgery and Urology, Faculty of Medicine, Jordan University of Science and Technology, King Abdullah University Hospital, Irbid, 22110, Jordan; 2Department of Internal Medicine, Faculty of Medicine, Jordan University of Science and Technology, King Abdullah University Hospital, Irbid, 22110, Jordan; 3Department of Mathematics and Statistics, Faculty of Science and Art, Jordan University of Science and Technology, Irbid, 22110, Jordan
Correspondence: Shadi Hamouri
Department of General Surgery and Urology, Faculty of Medicine, Jordan University of Science and Technology, King Abdullah University Hospital, P. O. Box 3030, Irbid, 22110, Jordan
Tel +962 79 6266693
Fax +962-2-7095010
Email [email protected]
Purpose: This study aims to determine the incidence and outcome of COVID-19 patients who required positive pressure ventilation (PPV) and subsequently developed pulmonary barotrauma (PBT). Also, to investigate the risk factors and predictors of these complications to better understand the disease pathogenesis.
Patients and Methods: This retrospective analysis enrolled all adult COVID-19 patients admitted through the period from October 1, 2020, to December 31, 2020. All patients who received any form of PPV were included. Patients were then divided into two groups based on PBT development, including subcutaneous emphysema, pneumothorax, and pneumomediastinum. Medical records of all patients were reviewed. Patients’ demographics, laboratory data on admission, respiratory support modes, surgical interventions, and outcomes were collected and analyzed.
Results: In the specified period, 1095 patients were hospitalized due to COVID-19 illness. A total of 239 (21.8%) of all admitted patients received PPV. PBT accounted for 21.3% (51/239) of the study cohort. While both groups were equally exposed to the same modes of PPV, receiving invasive ventilation significantly correlated with decreased PBT odds (OR = 0.891; 95% CI, 0.803– 0.988; p=0.029). PBT patients were significantly younger (p< 0.001). Diabetes mellitus was found to have a protective effect on developing PBT (OR = 0.867; 95% CI, 0.782– 0.962), while PO2/FIO2 ratio was inversely associated with higher odds of developing PBT in both univariate and multivariate analyses (p=0.03 and p=0.019, respectively).
Conclusion: COVID-19-infected patients are at a higher risk of developing PBT. Invasive positive pressure ventilation was associated with less PBT compared to noninvasive ventilation and delaying intubation does not seem to reduce the risk of pulmonary barotrauma.
Keywords: COVID-19, pulmonary barotrauma, pneumothorax, pneumomediastinum, positive pressure ventilation, adult respiratory distress syndrome
Introduction
In late December 2019, mysterious reported cases of “unknown pneumonia” were noticed in Wuhan, China.1 It was found to be caused by a novel coronavirus called Severe Acute Respiratory Syndrome Coronavirus 2 (SARS-CoV-2).1 SARS-CoV-2 belongs to the beta-coronavirus family, which includes the virus responsible for Severe Acute Respiratory Syndromes (SARS) and Middle East Respiratory Syndromes (MERS) (SARS-CoV and MERS-CoV, respectively).1,2 SARS-CoV-2 appears to share the same human cell receptors as SARS-CoV,1,2 which appear to cause multiple systems infection in some animals and mainly respiratory tract infections in humans, such as SARS and MERS.3,4 While most COVID-19-infected patients will have no or mild symptoms, few might progress to severe pneumonia, Acute respiratory distress syndrome (ARDS), or multiple organ failure.5 Hypoxemic respiratory failure and ARDS associated with COVID-19 has a variable case fatality rate (2–13%), with a mortality rate reaching up to 15% in cases requiring mechanical ventilation.6–8 Both pneumothorax (PNX) and pneumomediastinum (PMD) are known complications of mechanical ventilation.4,9 Retrospective studies of patients with COVID-19 have suggested that pneumothorax might occur in 1% of those requiring hospital admission, 2% of patients requiring intensive care unit (ICU) admission, and 1% of patients dying from the infection.5,9,10 More recently, 15% of ventilated patients developed pulmonary barotrauma (PBT), including subcutaneous emphysema, PNX, and PMD.11
To our knowledge, the current literature describing subcutaneous emphysema, PNX, and PMD related to COVID-19 infection consists primarily of case series and single case reports. This observational case–control study describes subcutaneous emphysema, PNX, and PMD complications in patients with COVID-19 disease who required positive pressure ventilation (PPV). The aim is to determine these patients’ incidence and outcome and investigate the risk factors and predictors of these complications to understand better the disease pathogenesis leading to these complications.
Patients and Methods
Study Design and Setting
This study is a single-center observational case–control study conducted at King Abdullah University Hospital (KAUH), the main tertiary hospital serving the north of Jordan. The hospital serves a population exceeding 2 million. Ethical approval was obtained from the Institutional Review Board (IRB) of the hospital, committed to the scientific research policy at Jordan University of Science and Technology (JUST) and KAUH. The ethics committee approved a waiver of consent from individual patients due to the study’s retrospective nature. All the data was anonymized. Patients’ confidentiality was protected following Declaration of Helsinki provisions.
Inclusion Criteria and Ventilation Protocol
All adult patients (age ≥ 18) who were tested positive for COVID-19 infection by Polymerase Chain Reaction (PCR) nasal swab test and were admitted to the hospital wards and critical care units due to COVID-19 complications through the period from October 1, 2020, to December 31, 2020, were enrolled. All patients who developed any element of PBT (PNX, PMD, or subcutaneous emphysema) and those who received any form of PPV either by using Non-Invasive Positive Pressure Ventilation (NIPPV) such as continuous positive airway pressure (CPAP) or bi-level positive airway pressure (BiPAP) and those who required Invasive positive pressure Ventilation (IPPV), were included.
All patients requiring IPPV were managed according to lung-protective ventilation strategies using low tidal volume (Vt) between 4 and 8 mL/kg predicted body weight, using a volume-limited assist control mode and initial Positive End Expiratory Pressure (PEEP) of 5 cm H2O and titrate up gradually to improve oxygenation while targeting plateau pressure (Pplat) of <30 cm H2O to limit lung injury. All IPPV and patients requiring higher oxygen requirements while on NIPPV were transferred to a critical care unit for close monitoring. Only patients requiring intermittent NIPPV were kept on the floor or intermediate care units according to their clinical condition and their oxygen and pressure support requirements. Except for honoring patients’ refusal to receive IPPV, all patients were considered for IPPV support when indicated regardless of their underlying comorbidities. According to our hospital sedation and muscle relaxant protocol, sedation medications used in patients with ARDS included benzodiazepines such as Lorazepam (1–10 mg/hour) or Midazolam (2–10 mg/hour) infusions in combination with a potent analgesic such as Fentanyl, Remifentanil, or Morphine. Muscle relaxants if needed were only used in addition to sedation and analgesics infusions to ensure patient synchronization with the ventilator. This sedation protocol applies to patients receiving IPPV. On the other hand, patients receiving NIPPV, the use of sedatives or analgesics were avoided and were only given minimum doses as needed basis for comfort.
Procedure
Clinical and laboratory data were collected retrospectively by reviewing the medical records of the patients. Age, sex, body mass index (BMI), smoking history, chronic medical illnesses, and history of underlying lung disease, presenting symptoms, laboratory values on admission, respiratory support modes, ventilator settings at the time of the barotrauma event, surgical interventions, and outcomes (death or discharge) were collected. All data were collected according to a standardized protocol to minimize recorder bias. Imaging was reviewed for all patients throughout their admission. PBT was radiologically identified at the time of the event by the ordering physician and consulted pulmonologist with the confirmation of a radiologist. All Chest X-Rays and reports were reviewed by both the thoracic surgeon and pulmonologist study authors while collecting the study data.
Data Analysis
All patients who received any form of PPV were divided into two groups, the first group is the group of patients who developed any form of PBT, and the second (control) group consists of all patients who did not develop PBT (NPBT). We used frequencies and percentages to represent patients’ distribution across categories and means/medians for continuous variables with standard deviations and ranges as spread measures. Chi-square test was used to compare frequencies and Fisher’s exact test in case of low cell counts. The Student’s t-test was used for differences between means, and the Wilcoxon rank-sum test in cases of variables that lacked a normal distribution was examined by visual histograms and confirmed by the Shapiro–Wilk test. All tests were two-tailed, and a p-value of less than 0.05 was considered statistically significant. Odds ratios were calculated as an effect measure to compare the odds of having PBT. Additionally, a multiple regression model was calculated to predict PBT using independent variables including mode of ventilation, age, comorbidities such as hypertension, diabetes mellitus (DM), chronic kidney disease, laboratory measurements such as ferritin, urea, lactate dehydrogenase, D-dimer, platelet, neutrophil and lymphocyte counts, X-ray findings (unilateral/bilateral), and respiratory parameters including PCO2, and PO2/FIO2 ratio. All statistical analyses were done using R statistical language (version 4.0.4).12
Results
Sample Characteristics
A total of 1095 patients were diagnosed and hospitalized with COVID-19 during the study period. Two hundred and thirty-nine (21.8%) of all admitted patients received PPV during their hospital stay and were divided into two groups. The first group (PBT group) included 51 (21.3%) patients who developed elements of PBT (PNX, PMD, or subcutaneous emphysema) after receiving any form of PPV. The second group (NPBT group) consisted of 188 (78.7%) patients who also received any form of PPV but did not develop PBT. Out of 239 patients who received PPV, 112 patients received IPPV (47%), 17 patients developed PBT. On the other hand, 127 patients received NIPPV (53%). Out of those who received NIPPV, 60 patients received BiPAP, and 67 patients received CPAP, out of which 15 and 19 patients developed PBT, respectively (Figure 1). The mean age of patients was 66.1 (± 13.6) years, 61.1% of patients were males, 35.1% of them were smokers, and mean body mass index (BMI) was 30.2 (± 6.93). Shortness of breath was the most common presenting symptom (83.7%), followed by dry cough (71.5%) and fever (68.2%). Out of 239 patients, 165 had hypertension (69.0%), 119 had DM (49.8%), 53 had ischemic heart disease (22.2%), and other patients had heart failure, chronic kidney disease, active malignancy, chronic obstructive pulmonary disease (COPD), and asthma (Table 1). The overall mortality rate of 1095 admitted COVID-19 patients was 21.1%. The mortality rate of patients who received either forms of PPV was 87.9%, which is higher than of patients who did not receive PPV (2.6%). The highest mortality rate from COVID-19 infection was found among patients who developed PBT (90.2%). The mean length of hospital stay was 13 days (± 8.73 days). When comparing both groups, patients who developed PBT-related complications were significantly younger, with a mean age difference of 6.9 years (p=0.002) (Figure 2). The male-female ratio was about 1:1, with no difference in mean body mass index (BMI) between the two groups. About 38.3% of the NPBT group were smokers, while 23.5% of those who developed PBT were smokers (p=0.069). We found no difference in the frequencies of presenting symptoms. NPBT group had higher rates of comorbidities such as hypertension (72.3% vs 56.9%, p=0.041), DM (54.3% vs 33.3%, p=0.012), and chronic kidney disease (16.0% vs 5.9%, p=0.045). No difference in mortality was observed between PBT and NPBT groups (p=0.739). A sub-analysis of the patients’ characteristics who received IPPV vs NIPPV was performed (Table 2). Patients who received NIPPV are significantly younger (p=0.046), and the death rate in patients receiving IPPV is higher (p <0.001). Other findings showed no clinically significant difference in the patients’ demographics, explaining the lower barotrauma rate in the IPPV group.
 |
Table 1 Patients' Demographics |
 |
Table 2 Patients’ Demographics; Invasive Positive Pressure Ventilation vs Non-Invasive Positive Pressure Ventilation |
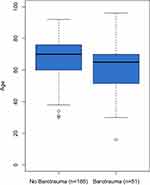 |
Figure 2 Side-by-side box of age for the two groups. |
Laboratory Results
As described in Table 3. NPBT group had high mean serum urea level (mean difference = 2.94 mmol/L, p=0.009) and higher serum creatinine levels (mean difference = 56.1 µg/dl, p < 0.001) than PBT patients. On the other hand, PBT group had higher levels of ferritin (mean difference = 118 ng/mL, p=0.07), but using Wilcoxon median test yields a significant difference in ferritin medians, p-value=0.019, lactate dehydrogenase levels (mean difference = 180 U/L, p=0.013), D-dimer levels (mean difference = 1.49, p=0.05) and higher white blood cell count (mean difference = 1.8*103 /µL, p=0.038) than the control group. There was no difference in neutrophils, lymphocytes, platelets, and blood levels of hemoglobin, C-reactive protein, creatinine kinase, and troponin between the two groups (Table 3). Nonetheless, using Wilcoxon median test, a significant difference in medians in neutrophils count was detected in the PBT group (p-value=0.024).
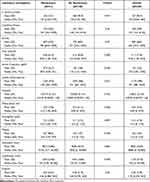 |
Table 3 Laboratory Investigations and Results |
Barotrauma and Mechanical Ventilation
Out of a total of 51 patients who experienced PBT, 17 patients had PBT while receiving IPPV support, while 19 patients were on CPAP support, and 15 were on BiPAP support (Figure 1). PBT manifested as PNX, PMD, or subcutaneous emphysema, as one or combination of more than one. A total of 23 patients of the PBT group manifested as PNX (45.1%), 25 patients developed PMD (49.0%), and 23 patients developed subcutaneous emphysema (45.1%) (Figure 3). The timeline of events for individuals who experienced PBT is illustrated in Figure 4.
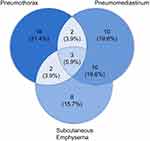 |
Figure 3 Venn diagram showing distribution of patients having different scenarios of barotrauma. |
Most PBT patients were treated with a chest tube (76.5%), with a drain size of either 24 or 28 French (Fr). The insertion site was in the right, left, or bilateral for 16, 12, and 10 patients, respectively (Table 4).
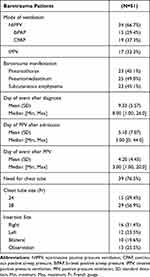 |
Table 4 Pulmonary Barotrauma Group; Mode of Ventilation, Complication, and Management |
Although both groups were exposed to the same PPV modes, receiving IPPV therapy was significantly correlated with decreased PBT odds (OR = 0.891; 95% CI, 0.803–0.988; p=0.029). Interestingly, NIPPV caused more PBT (34/51, 56%) than IPPV (17/51, 33.3%). Out of a total of 112 patients who required IPPV, 17 patients developed PBT (33.3%), while 27% (34/127) of patients who required NIPPV support, either BiPAP or CPAP, developed PBT (Table 5). The duration between the time of admission to the PPV support was not significantly different between the two groups. There was no difference in the mean tidal volume/ideal body weight, but the mean respiratory rate was higher in the NPBT group (1.8 breaths per minute, p=0.01), and although PaO2/FIO2 was significantly low in both groups, it was significantly lower in the PBT group (mean difference = 17.7, p=0.002). There was no difference in PCO2 (p=0.13). There was no significant difference or effect seen in the inspiratory positive airway pressure (IPAP), pressure support, positive end-expiratory pressure (PEEP), or fraction of inspired O2 on PBT development.
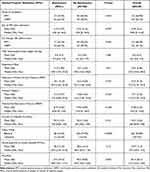 |
Table 5 Comparison Between Pulmonary Barotrauma and Control Group Ventilation Modes and Settings |
Radiological Findings
We have evaluated chest X-Ray findings for all PBT patients. Thirty-eight patients (74.5%) had bilateral lung involvement with diffuse infiltrates, 7 (13.7%) patients had left lung involvement, and 6 (11.8%) patients had right lung involvement. Chest tubes were inserted in the same side of the infiltrate in 4/10 patients, while on the opposite involvement side in 6/10 patients. For patients with bilateral infiltrates findings, chest tubes were inserted in the right side for nine patients, in the left side for nine patients, and bilaterally in 9 patients (Table 6). The location of X-ray findings was distributed equally in pneumomediastinum and subcutaneous emphysema patients, but pneumothorax patients had more tendency to be shown on the left (p=0.023).
 |
Table 6 Chest X-Ray Findings and Their Relation to the Pulmonary Barotrauma |
Predictors of Barotrauma
Logistic regression was carried out on variables that had a notable difference between PBT and NPBT patients, in addition to variables that were considered clinically significant. A significant regression equation was found using 15 variables and 140 degrees of freedom (p<0.0001), with an R2 measure of 27.1% and an adjusted-R2 measure of 19.3% (Table 7). In univariate analysis, PBT group patients were significantly younger (p<0.001), and this effect remains in multivariate analysis (p=0.038). DM was found to reduce the odds for developing PBT (OR = 0.867; 95% CI, 0.782–0.962). This effect persisted even after adjusting for age and other possible predictors in multivariate analysis (OR = 0.839; 95% CI, 0.725–0.970). While chronic kidney disease showed a significant effect in univariate analysis using chi-square test (p-value=0.045) but did not have significant effect in multivariate analyses, hypertension had an effect in the univariate analysis only (OR = 0.886; 95% CIs, 0.791–0.991; p=0.034). Lymphocyte count was found to have a significant effect in multivariate analysis (p=0.038). Other laboratory findings, including urea levels and lactate dehydrogenase, had significant adverse effects on PBT in univariate analysis but not in the multivariate analysis.
 |
Table 7 Logistic Regression Analysis of the Predictors of Barotrauma |
Other laboratory findings, including ferritin, D-dimer, platelet, and neutrophil counts, did not significantly predict PBT in either analysis. As for radiological findings, unilateral findings were significantly associated with PBT occurrence (OR=1.822; 95% CI, 1.274–2.606; p=0.003), but we did not find any significance for it in multiple regression. Lower PO2/FIO2 was associated with higher odds of developing PBT in both univariate and multivariate analyses (p=0.03 and p=0.019, respectively). PCO2 had no significant effects in either analysis. To further examine DM’s protective effect, we ran an additional model that does not include the diabetes variable. R2 measure was reduced from 27.1% to 24.2% and adjusted-R2 decreased from 19.3% to 16.3%. Finally, we compared this model against the original model using an ANOVA F-test, and it showed a significant difference (F = 5.70; p=0.018). Predictors of barotrauma are demonstrated in Figure 5.
Discussion
This observational study reports PBT in 60 patients out of 1095 SARS-CoV-2 infected hospitalized adults during the study period. To our knowledge, this is the largest study population of PBT in SARS-CoV-2 infection from a single center and one of few to describe associated risk factors in these patients. The overall incidence of PBT in our study of the SARS-CoV-2 population was about 5.5%. Most of the affected patients (85%) developed PBT while receiving PPV support, an incidence of 21.3%. A total of 9 cases developed spontaneous PNX, PMD, or subcutaneous emphysema out of 856 of SARS-CoV-2 admitted patients who did not require any form of PPV with an overall incidence of 1.0%. Multiple studies have reported PNX in association with COVID-19 pneumonia. The most extensive published retrospective case series included 71 patients with PBT from 16 centers by Martinelli et al reported incidence of about 25% of intubated patients developed PNX or PMD,13 which is similar to the incidence observed in our cohort. On the other hand, multiple case series studies reported a 10–14% incidence of PBT in mechanically ventilated ARDS patients infected with COVID-19.11,14–16
In our study, the incidence of PBT was higher in patients who received NIPPV than IPPV (34/127,26.8% vs 17/112,15.2%, respectively, p= 0.043). More patients from PBT group received NIPPV than IPPV (66.7% and 33.3%, respectively), compared to the NPBT group (50.5% and 49.5%, respectively). Our study is the largest and the second to report a higher incidence of PNX in patients who received NIPPV in comparison to IPPV support. Jones et al reported Seven out of eight patients (87.5%) in the barotrauma group had received NIPPV as the initial mode of advanced respiratory support, compared with 27 of 75 (36.0%) in the non-barotrauma group (p=0.007).17 Applying the universally accepted ARDS Network guidelines to ventilate ARDS patients using a protective-ventilation approach based on reducing the tidal volume to about 6 mL·kg−1 of ideal body weight and maintaining the airway plateau pressure below 30 cmH2O has helped to reduce the incidence of PBT significantly.18–20 Rates of NIPPV-associated barotrauma are not known but are reportedly rare in COVID-19 related ARDS.17,21,22 However, in NIPPV, the tidal volumes and transpulmonary pressure are dependent on the patient’s spontaneous respiratory effort, which may result in highly variable and fluctuant transpulmonary pressures that cannot be limited or controlled,23,24 which may result in self-inflicted PBT in patients with ARDS. Higher incidence of PBT in NIPPV might be also attributed to the limited use of sedation and muscle relaxant in NIPPV group compared to IPPV which might have impacted patient-ventilator desynchrony, and subsequently higher risk of developing PBT. This supports the importance of maintaining patient-ventilator synchrony to lower the risk of PBT. There is no agreement on using CPAP and NIPPV in severe COVID-19,25 but it has been promoted in some guidelines.26,27 Belletti et al evaluated predictors of PNX/PMD in mechanically ventilated COVID-19 patients and concluded that delayed intubation was an independent predictor of PNX/PMD development.28 In that study, the group who developed PBT had a longer time from symptoms onset to intubation than the group who did not develop PBT (13 vs 10 days, p=0.004). This higher incidence of PBT in NIPPV, as well as the reported cases of spontaneous PNX, may support that the underlying cause of PNX/PMD is due to an underlying virus-induced mechanism as part of the natural course/sequela of the SARS-CoV-2 disease rather than a mechanical PPV-induced complication caused by high transpulmonary pressure. This theory is also supported by the observation of overall higher incidence of PNX/PMD in COVID-19 related ARDS in comparison to non-COVID-19 ARDS. Lemmers et al observed a seven-fold increase in PBT in COVID-19 ARDS with a PMD incidence of 13% in COVID-19 ARDS versus 1.9% in non-COVID-19 ARDS.14 The reported incidence of PNX/PMD in non-COVID-19 ARDS is ranging between 3% and 15%.29–32 Spontaneous pneumothorax was also reported as a complication of the SARS caused by SARS-CoV-1 with an incidence of 1.7% in hospitalized patients.33
Many clinical and laboratory variables have been investigated in our cohort, looking for predictors associated with a higher risk of developing PBT in patients receiving PPV. Interestingly, the group who developed PBT were younger and with fewer comorbidities. Except for the higher prevalence of DM and better PO2/FIO2 ratio observed in the NPBT group, there was no significant difference observed in the other factors between the two groups to predict the risk of developing PBT in patients receiving PPV. A lower PO2/FIO2 ratio usually indicates a greater extent of lung injury or ARDS, thus raising the risk of PNX/PMD. Many studies have well-described DM as a risk factor for developing severe pneumonia in COVID-19-infected patients.34–38 Patients with type 2 DM were more likely to develop complications, more intensive care unit admissions, and death from COVID-19.
On the other hand, in an observational study from France, 1317 patients with DM were hospitalized with COVID-19. Neither long-term glycemic control nor routine therapies were associated with COVID-19 severity, intubation, and death.39 Up to our knowledge, no studies to date have described the effect of pre-existing DM in developing PBT in patients with SARS-CoV-2 infection. A meta-analysis study done by Ji et al looking into the effect of DM on the risk and mortality of acute lung injury/ARDS reviewed 14 studies and found no effect of having a pre-existing DM on the risk and mortality of ALI/ARDS.40 DM may play an essential role in the immune system and, consequently, contribute to a reduced overall inflammatory response with the attenuation of cytokine release and the reduction of neutrophil migration.41,42 This blunted inflammatory response might help reduce the rate of inflammation associated with SARS-CoV-2 infection. The mechanism is yet to be explained, but this may add on to the support of a possible immunomodulated response on the pathogenesis of developing PNX/PMD in patients infected with SARS-CoV-2.
The laboratory findings indicated significantly higher levels of urea and creatinine in the NPBT group. This finding can be explained by the higher incidence of chronic kidney disease compared to PBT group (16%vs 5.9%, respectively). Additionally, although not statistically significant, the smoking rate in the PBT group seems to be less than the NPBT group (23.5% vs 38.3%, respectively). Smoking is usually associated with chronic obstructive pulmonary disease (COPD)/emphysema which places patients at a higher risk of PNX while on PPV. Tindle et al described that nicotine and cigarette smoke have been reported to decrease levels of angiotensin-converting enzyme 2 (ACEII).43 Moreover, it may modulate COVID-19 disease severity through the cholinergic anti-inflammatory pathway, inhibiting macrophage-driven hyper-inflammation and platelet reactivity, thus reducing the cellular injury and severity of the disease.43 Nevertheless, it is suggested that smoking may confer some protective effect against the development of COVID-19 infection but might be associated with worse disease outcome once acquired.44
Chest radiograph of most SARS-CoV-2 patients who required PPV revealed diffuse lung involvement with equal bilateral infiltrates distribution. Most patients had diffuse and equally distributed bilateral infiltrates (38/51, 74.5%). Out of patients who developed PBT, 13 had a preferential unilateral lung involvement with one side involved with more infiltrates than the other; the chest tube was placed more in the opposite to the side with worse infiltrates (7/13, 54%) than of the same side (3/13, 23%). No apparent reason to explain this observation in our study. An assumption is that the lung areas with more infiltrates are stiffer and probably more resistant to developing PBT than areas with less infiltrate involvement. One important finding is that the tendency to follow conservative measures rather than proceeding with interventional measures and chest tube insertion was much more in patients with bilateral infiltrates (11/38, 29%) than with preferential infiltrates (2/13, 15%).
The mean time to develop PBT in our cohort was about nine days from diagnosis and about four days after the placement on any form of PPV. This finding is similar to the study by Edwards et al in which PNX/PMD occurred in less than four days from the start of mechanical ventilation.16 Multiple studies indicated that PNX usually develops at a relatively late stage (3–8 weeks) after the onset of symptoms.45,46 In a study by Capaccione et al, the time from intubation to PNX event was 14.9 days which is similar to that described by Belletti et al, in which the time from intubation to PNX was 14 days.15,28 Most patients who developed PBT in our study died (88%). The occurrence of PBT did not change the overall outcome of our study population. Multiple studies reported PBT to attribute to increased mortality in patients with COVID-19 infection, whether spontaneous or iatrogenic, due to PPV, both invasive and noninvasive.47,48 The mortality rate reported by Belletti et al was 61% in patients who developed PNX/PMD, higher than those who did not have PNX/PMD (39%, p=0.04).28 Abdallat et al described a case series of 25 patients with COVID-19 infection who developed PBT with a mortality rate of 64%.49 Martinelli et al indicated that although post-PNX survival was lower in patients receiving IPPV than patients who were not intubated, no significant difference was found between patients receiving IPPV or those not receiving IPPV ventilation. That lead to a conclusion that COVID-19 infection-related PNX did not seem to be an independent marker of poor prognosis,13,50 which is similar to our study. Multiple factors are thought to be contributing to the high overall mortality rate of SARS-CoV-2 patients in our cohort. First, the higher degree of severity in the patients and the hospital’s nature as the primary referral center accepts more severe cases with a more complicated course or advanced disease stage and frequently with significant comorbidities. The other main contributing factor is the overwhelmingly large number of admitted and accumulated patients in a short time frame with limited human resources and strict technical availability.
Our study has involved a relatively large number of patients reported in a single tertiary center. Nonetheless, our finding has its limitations that include the following: First, being a single-center observation, this will restrict the generalization of the results and findings. Secondly, our protocol in managing SARS-CoV-2 patients in our hospital does not include a computer tomography (CT) investigation. The absence of the CT from the investigation protocol may result in underestimating the barotrauma cases, especially mild pneumomediastinum or anterior pneumothoraxes that are not clinically apparent or difficult to be seen on the chest radiograph; moreover, the presence of necrotizing infections that may predispose for PNX is underestimated.
Conclusion
Our cohort study results highlighted and supported that COVID-19 ARDS infected patients are at a higher risk of developing PBT than non-COVID-19 ARDS. There is an added risk of developing PBT in patients receiving NIPPV compared to IPPV and avoiding intubation does not seem to reduce the risk of PBT and PNX/PMD development. These findings are essential to consider when placing a management protocol of COVID-19 ARDS.
Ethics Approval and Consent to Participate
Ethical approval was obtained from the Institutional Review Board (IRB) of the hospital, committed to the scientific research policy at Jordan University of Science and Technology (JUST) and KAUH. This study was conducted following the 1975 Helsinki declaration, as revised in 2008 and its later amendments or comparable ethical standards.
Consent for Publication
The ethics committee approved a waiver of consent from individual patients due to the study’s retrospective nature.
Funding
There is no funding to report.
Disclosure
The authors declare that they have no conflicts of interest and no financial disclosures.
References
1. Petrosillo N, Viceconte G, Ergonul O, Ippolito G, Petersen E. COVID-19, SARS and MERS: are they closely related? Clin Microbiol Infect. 2020;26(6):729–734. doi:10.1016/j.cmi.2020.03.026
2. Prompetchara E, Ketloy C, Palaga T. Immune responses in COVID-19 and potential vaccines: lessons learned from SARS and MERS epidemic. Asian Pacific J Allergy Immunol. 2020;38(1):1–9. doi:10.12932/AP-200220-0772
3. Zaki AM, van Boheemen S, Bestebroer TM, Osterhaus ADME, Fouchier RAM. Isolation of a novel coronavirus from a man with pneumonia in Saudi Arabia. N Engl J Med. 2012;367(19):1814–1820. doi:10.1056/nejmoa1211721
4. Yin Y, Wunderink RG. MERS, SARS and other coronaviruses as causes of pneumonia. Respirology. 2018;23(2):130–137. doi:10.1111/resp.13196
5. Chen N, Zhou M, Dong X, et al. Epidemiological and clinical characteristics of 99 cases of 2019 novel coronavirus pneumonia in Wuhan, China: a descriptive study. Lancet. 2020;395(10223):507–513. doi:10.1016/S0140-6736(20)30211-7
6. Wu Z, McGoogan JM. Characteristics of and Important Lessons from the Coronavirus Disease 2019 (COVID-19) outbreak in China: summary of a report of 72314 cases from the Chinese center for disease control and prevention. JAMA - J Am Med Assoc. 2020;323(13):1239–1242. doi:10.1001/jama.2020.2648
7. Zhou F, Yu T, Du R, et al. Clinical course and risk factors for mortality of adult inpatients with COVID-19 in Wuhan, China: a retrospective cohort study. Lancet. 2020;395(10229):1054–1062. doi:10.1016/S0140-6736(20)30566-3
8. Goyal P, Choi JJ, Pinheiro LC, et al. Clinical Characteristics of Covid-19 in New York City. N Engl J Med. 2020;382(24):2372–2374. doi:10.1056/nejmc2010419
9. Jacobi A, Chung M, Bernheim A, Eber C. Portable chest X-ray in coronavirus disease-19 (COVID-19): a pictorial review. Clin Imaging. 2020;64:35. doi:10.1016/J.CLINIMAG.2020.04.001
10. Salehi S, Abedi A, Balakrishnan S, Gholamrezanezhad A. Coronavirus disease 2019 (COVID-19): a systematic review of imaging findings in 919 patients. Am J Roentgenol. 2020;215(1):87–93. doi:10.2214/AJR.20.23034
11. McGuinness G, Zhan C, Rosenberg N, et al. Increased incidence of barotrauma in patients with COVID-19 on invasive mechanical ventilation. Radiology. 2020;297(2):E252–E262. doi:10.1148/radiol.2020202352
12. Team R Core/R Foundation for Statistical Computing/. R: a Language and Environment for Statistical Computing. Available from: https://www.r-project.org.
13. Martinelli AW, Ingle T, Newman J, et al. COVID-19 and pneumothorax: a multicentre retrospective case series. Eur Respir J. 2020;56:5. doi:10.1183/13993003.02697-2020
14. Lemmers DHL, Abu Hilal M, Bnà C, et al. Pneumomediastinum and subcutaneous emphysema in COVID-19: barotrauma or lung frailty? ERJ Open Res. 2020;6(4):00385–02020. doi:10.1183/23120541.00385-2020
15. Capaccione KM, D’souza B, Leb J, et al. Pneumothorax rate in intubated patients with COVID-19. Acute Crit Care. 2020;36:1. doi:10.4266/acc.2020.00689
16. Edwards JA, Breitman I, Bienstock J, et al. Pulmonary barotrauma in mechanically ventilated coronavirus disease 2019 patients: a case series. Ann Med Surg. 2021;61:24–29. doi:10.1016/j.amsu.2020.11.054
17. Jones E, Gould A, Pillay TD, et al. Subcutaneous emphysema, pneumomediastinum, and pneumothorax in critically Ill patients with coronavirus Disease 2019: a retrospective cohort study. Crit Care Explor. 2020;2(9):e0210. doi:10.1097/cce.0000000000000210
18. Brower RG, Matthay MA, et al.; Acute Respiratory Distress Syndrome Network. Ventilation with lower tidal volumes as compared with traditional tidal volumes for acute lung injury and the acute respiratory distress syndrome. N Engl J Med. 2000;342(18):1301–1308. doi:10.1056/NEJM200005043421801.
19. Fan E, Del Sorbo L, Goligher EC, et al. An official American Thoracic Society/European Society of intensive care medicine/society of critical care medicine clinical practice guideline: mechanical ventilation in adult patients with acute respiratory distress syndrome. Am J Respir Crit Care Med. 2017;195(9):1253–1263. doi:10.1164/rccm.201703-0548ST
20. Slutsky AS, Ranieri VM. Ventilator-induced lung injury. N Engl J Med. 2013;369(22):2126–2136. doi:10.1056/NEJMra1208707
21. Carron M, Freo U, Bahammam AS, et al. Complications of non-invasive ventilation techniques: a comprehensive qualitative review of randomized trials. Br J Anaesth. 2013;110(6):896–914. doi:10.1093/bja/aet070
22. Mehta S, Hill NS. Noninvasive ventilation. Am J Respir Crit Care Med. 2001;163(2):540–577. doi:10.1164/ajrccm.163.2.9906116
23. Marini JJ, Gattinoni L. Management of COVID-19 respiratory distress. JAMA - J Am Med Assoc. 2020;323(22):2329–2330. doi:10.1001/jama.2020.6825
24. Brochard L, Slutsky A, Pesenti A. Mechanical ventilation to minimize progression of lung injury in acute respiratory failure. Am J Respir Crit Care Med. 2017;195(4):438–442. doi:10.1164/rccm.201605-1081CP
25. Arulkumaran N, Brealey D, Howell D, Singer M. Use of non-invasive ventilation for patients with COVID-19: a cause for concern? Lancet Respir Med. 2020;8(6):e45. doi:10.1016/S2213-2600(20)30181-8
26. World Health Organization.Clinical Management of COVID-19: Interim Guidance, 27 May 2020. World Health Organization; 2020. Available from: https://apps.who.int/iris/handle/10665/332196.License:CCBY-NC-SA3.0IGONoTitle.
27. NHS England, NHS Improvement. Specialty guides for patient management during the coronavirus pandemic Guidance for the role and use of non-invasive respiratory support in adult patients with coronavirus (confirmed or suspected). 2020. Available from: https://www.nice.org.uk/guidance/ng159.
28. Belletti A, Palumbo D, Zangrillo A, et al. Predictors of pneumothorax/pneumomediastinum in mechanically ventilated COVID-19 patients. J Cardiothorac Vasc Anesth. 2021. doi:10.1053/j.jvca.2021.02.008
29. Guérin C, Reignier J, Richard J-C, et al. Prone positioning in severe acute respiratory distress syndrome. N Engl J Med. 2013;368(23):2159–2168. doi:10.1056/nejmoa1214103
30. Villar J, Ferrando C, Martínez D, et al. Dexamethasone treatment for the acute respiratory distress syndrome: a multicentre, randomised controlled trial. Lancet Respir Med. 2020;8(3):267–276. doi:10.1016/S2213-2600(19)30417-5
31. Early neuromuscular blockade in the acute respiratory distress syndrome. N Engl J Med. 2019;380(21):1997–2008. doi:10.1056/nejmoa1901686
32. Anzueto A, Frutos–Vivar F, Esteban A, et al. Incidence, risk factors and outcome of barotrauma in mechanically ventilated patients. Intensive Care Med. 2004;30(4):612–619. doi:10.1007/s00134-004-2187-7
33. Sihoe ADL, Wong RHL, Lee ATH, et al. Severe acute respiratory syndrome complicated by spontaneous pneumothorax. Chest. 2004;125(6):2345–2351. doi:10.1378/chest.125.6.2345
34. Guo W, Li M, Dong Y, et al. Diabetes is a risk factor for the progression and prognosis of COVID-19. Diabetes Metab Res Rev. 2020;36:7. doi:10.1002/dmrr.3319
35. Bode B, Garrett V, Messler J, et al. Glycemic characteristics and clinical outcomes of COVID-19 patients hospitalized in the United States. J Diabetes Sci Technol. 2020;14(4):813–821. doi:10.1177/1932296820924469
36. Targher G, Mantovani A, Wang XB, et al. Patients with diabetes are at higher risk for severe illness from COVID-19. Diabetes Metab. 2020;46(4):335–337. doi:10.1016/j.diabet.2020.05.001
37. Shang J, Wang Q, Zhang H, et al. The relationship between diabetes mellitus and COVID-19 prognosis: a retrospective cohort study in Wuhan, China. Am J Med. 2021;134(1):e6–e14. doi:10.1016/j.amjmed.2020.05.033
38. Barron E, Bakhai C, Kar P, et al. Associations of type 1 and type 2 diabetes with COVID-19-related mortality in England: a whole-population study. Lancet Diabetes Endocrinol. 2020;8(10):813–822. doi:10.1016/S2213-8587(20)30272-2
39. Cariou B, Hadjadj S, Wargny M, et al. Phenotypic characteristics and prognosis of inpatients with COVID-19 and diabetes: the CORONADO study. Diabetologia. 2020;63(8):1500–1515. doi:10.1007/s00125-020-05180-x
40. Ji M, Chen M, Hong X, Chen T, Zhang N. The effect of diabetes on the risk and mortality of acute lung injury/acute respiratory distress syndrome. Medicine (Baltimore). 2019;98(13):e15095. doi:10.1097/MD.0000000000015095
41. Frank JA, Nuckton TJ, Matthay MA. Diabetes mellitus: a negative predictor for the development of acute respiratory distress syndrome from septic shock. Crit Care Med. 2000;28(7):2645–2646. doi:10.1097/00003246-200007000-00079
42. Spiller F, Carlos D, Souto FO, et al. α1-acid glycoprotein decreases neutrophil migration and increases susceptibility to sepsis in diabetic mice. Diabetes. 2012;61(6):1584–1591. doi:10.2337/db11-0825
43. Tindle HA, Newhouse PA, Freiberg MS. Beyond smoking cessation: investigating medicinal nicotine to prevent and treat COVID-19. Nicotine Tob Res. 2020;22(9):1669–1670. doi:10.1093/ntr/ntaa077
44. Landoni G, Moro M, Belletti A, et al. Recent exposure to smoking and COVID-19. Crit Care Resusc. 2020. http://www.ncbi.nlm.nih.gov/pubmed/32645763.
45. Hollingshead C, Hanrahan J. Spontaneous pneumothorax following COVID-19 pneumonia. IDCases. 2020;21. doi:10.1016/j.idcr.2020.e00868.
46. Horii T, Fujioka T, Takahashi M, et al. Late-onset pneumothorax in a COVID-19 patient treated with ventilation and ECMO: a case report and literature review. Radiol Case Reports. 2020;15(12):2560–2564. doi:10.1016/j.radcr.2020.09.036
47. McGuinness G, Zhan C, Rosenberg N, et al. Increased incidence of barotrauma in patients with COVID-19 on invasive mechanical ventilation. Radiology. 2020;297(2):E252–E262. doi:10.1148/RADIOL.2020202352
48. López Vega JM, Parra Gordo ML, Diez Tascón A, Ossaba Vélez S. Pneumomediastinum and spontaneous pneumothorax as an extrapulmonary complication of COVID-19 disease. Emerg Radiol. 2020;27(6):727–730. doi:10.1007/s10140-020-01806-0
49. Abdallat M, Khalil M, Al-awwa G, Kothuru R, La PC. Barotrauma in COVID-19 Patients. 2020;4:8–12.
50. Hameed M, Jamal W, Yousaf M, et al. Pneumothorax In Covid-19 Pneumonia: a case series. Respir Med Case Reports. 2020;31(October):101265. doi:10.1016/j.rmcr.2020.101265
 © 2021 The Author(s). This work is published and licensed by Dove Medical Press Limited. The full terms of this license are available at https://www.dovepress.com/terms.php and incorporate the Creative Commons Attribution - Non Commercial (unported, v3.0) License.
By accessing the work you hereby accept the Terms. Non-commercial uses of the work are permitted without any further permission from Dove Medical Press Limited, provided the work is properly attributed. For permission for commercial use of this work, please see paragraphs 4.2 and 5 of our Terms.
© 2021 The Author(s). This work is published and licensed by Dove Medical Press Limited. The full terms of this license are available at https://www.dovepress.com/terms.php and incorporate the Creative Commons Attribution - Non Commercial (unported, v3.0) License.
By accessing the work you hereby accept the Terms. Non-commercial uses of the work are permitted without any further permission from Dove Medical Press Limited, provided the work is properly attributed. For permission for commercial use of this work, please see paragraphs 4.2 and 5 of our Terms.



