Back to Journals » Cancer Management and Research » Volume 10
Prospective study of neoadjuvant chemoradiotherapy using intensity-modulated radiotherapy and 5 fluorouracil for locally advanced rectal cancer – toxicities and response assessment
Authors Simson DK, Mitra S, Ahlawat P, Saxena U , Kumar Sharma M, Rawat S, Singh H, Bansal B, Sripathi LK, Tanwar A
Received 18 May 2017
Accepted for publication 18 December 2017
Published 19 March 2018 Volume 2018:10 Pages 519—526
DOI https://doi.org/10.2147/CMAR.S142076
Checked for plagiarism Yes
Review by Single anonymous peer review
Peer reviewer comments 2
Editor who approved publication: Professor Lu-Zhe Sun
David K Simson,1 Swarupa Mitra,2 Parveen Ahlawat,2 Upasna Saxena,2 Manoj Kumar Sharma,2 Sheh Rawat,2 Harpreet Singh,1 Babita Bansal,1 Lalitha Kameshwari Sripathi,1 Aditi Tanwar2
1Department of Radiation Oncology, Action Cancer Hospital, New Delhi, India; 2Department of Radiation Oncology, Rajiv Gandhi Cancer Institute and Research Centre, New Delhi, India
Aims and objectives: The past 2 decades witnessed the strengthening of evidence favoring the role of neoadjuvant chemoradiation (CHRT) in the treatment of locally advanced rectal cancer. The study aims to evaluate the response and acute toxicities to neoadjuvant CHRT using intensity-modulated radiotherapy (IMRT) in the treatment of rectal cancer. Predictive factors to achieve pathological complete response (pCR) were analyzed, as a secondary endpoint.
Materials and methods: All consecutive patients who underwent IMRT as part of neoadjuvant CHRT in the treatment of rectal cancer between August 2014 and December 2016 at a tertiary cancer care center were accrued for the study. The cohort underwent CHRT with IMRT technique at a dose of 50.4 Gy in 28 fractions concurrent with continuous infusion of 5 fluorouracil during the first and the last 4 days of CHRT. Surgery was performed 6 weeks later and the pathological response to CHRT was noted.
Results: Forty-three subjects were accrued for the study. Radiation dermatitis and diarrhea were the only observed grade ≥3 acute toxicities. Sphincter preservation rate (SPR) was 43.3%. pCR was observed in 32.6%. Univariate and multivariate logistic regression showed that carcinoembryonic antigen was the only independent predictive factor to achieve pCR.
Conclusion: IMRT as part of neoadjuvant CHRT in the treatment of locally advanced rectal cancer is well tolerated and gives comparable results with respect to earlier studies in terms of pathological response and SPR. Further randomized controlled studies are needed to firmly state that IMRT is superior to 3-dimensional conformal radiotherapy.
Keywords: IMRT, rectal cancer, chemoradiation, neoadjuvant, response
Introduction
The past decade has seen preoperative concurrent chemoradiation (CHRT) followed by surgery 6 weeks later as the dominating trend in the management of carcinoma of the rectum.1 Despite the fact that there are benefits of preoperative radiotherapy, the toxicities associated with the conventional broad fields or improper radiation techniques at some places were of significant concern for the oncologists.2
The past 2 decades have also seen the emergence of intensity-modulated radiotherapy (IMRT) along with gradual replacement of conventional techniques. IMRT hails with advantages of lower doses delivered to the organs at risk (OARs) as it makes the dose cloud or isodose lines conform to the shape of the volume of interest. The reduced dose to OARs like small bowel and urinary bladder translates into decreased toxicities, both acute and late, as seen in studies involving pelvic malignancies such as cervical, endometrial, and prostate cancers.3–5 However, this is derived largely from prospective and retrospective data rather than planned randomized studies comparing IMRT vs conventional techniques.
Materials and methods
After the ethical board approval (Institutional Review Board, Rajiv Gandhi Cancer Hospital and Research Centre, Delhi, India) of the prospective observational study, all patients undergoing CHRT for locally advanced rectal cancers were evaluated for response and toxicity profile. All consecutive patients attending the radiation department of a tertiary care cancer hospital opting for IMRT technique between August 2014 and December 2016 were accrued for this study. Written informed consent was obtained from all the patients who participated in this study. The cohort underwent whole abdomen MRI with contrast and serum carcinoembryonic antigen (CEA) levels prior to the treatment.
Patients were immobilized with the help of orfit-ray™ (Orfit Industries, Wijnegem, Belgium) thermoplastic cast and CT simulation was performed with SOMATOM sensation open™ (Global Siemens Healthcare, Erlanger, Germany) in supine position. Contrast-enhanced CT scans were performed with 3 mm slice thickness along with bladder protocol (the patient is asked to void and then drink 700 mL water and the scan is performed on having the sensation to pass urine). Contouring was done using Varian Eclipse™ Version 10 (Varian Medical Systems, Palo Alto, CA, USA) according to the Radiation Therapy Oncology Group (RTOG) guidelines.6 Conventional fractionation IMRT was used (total dose of 50.4 Gy with daily fractions of 1.8 Gy, 5 days a week) along with concurrent chemotherapy with 5 fluorouracil (5FU) 1000 mg/m2 in continuous infusion during the first and last 4 days of radiation. Patients were assessed weekly for acute toxicities such as skin reactions, vomiting, cystitis, diarrhea, and hematological toxicities. RTOG scoring scale was used to grade acute toxicities.7
At 6 weeks post-CHRT, contrast MRI-based response evaluation was done using RECIST 1.1 criteria.8 Surgery – either low anterior resection (LAR) or abdominoperineal resection – was performed, and pathological response to neoadjuvant CHRT was graded according to the College of American Pathologist guidelines.9 The primary endpoint was to evaluate down-staging and pathological response to CHRT. The secondary endpoint was to find out factors predictive for pathological complete response (pCR) to CHRT.
Statistical analysis
The descriptive statistics for quantitative variables are presented using mean (with SD), while categorical variables are presented in frequencies along with respective percentages. To compare categorical variables, Chi-square test or Fisher’s exact test was used according to the nature of data. Univariate and multivariate logistic regression were used to identify the associated independent predictive factors to achieve pCR. A p-value <0.05 was considered statistically significant. All p-values reported are two-tailed. Statistical Package for the Social Sciences version 20.0 (IBM Corporation, Armonk, NY, USA) was used to carry out all statistical computations.
Results
Forty-three patients were treated with CHRT followed by surgery after 6 weeks. The pretreatment clinical characteristics have been tabulated in Table 1. The mean dose received by 95% of planning target volume was 50.17 ± 0.39 Gy. Mean volume of small bowel that received dose >45 Gy (SBV45 Gy) was 78.79 ± 48.38 cc, while mean volume of urinary bladder receiving >50 Gy was 24.73 ± 7.93%. Diarrhea and radiation dermatitis were the only observed grade ≥3 acute toxicities (Table 2). The relationship between diarrhea and SBV45 Gy has been depicted in Table 3. It was noted that acute diarrheal toxicity of grades ≥3 was experienced when the SBV45 Gy exceeded 120 cc.
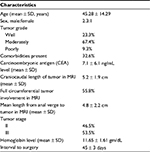  | Table 1 Pretreatment clinical characteristics |
  | Table 2 Acute toxicities |
  | Table 3 The relationship between grades of diarrhea and SBV45 Gy Abbreviation: SBV45, mean volume of small bowel that received dose >45 Gy. |
All patients underwent concurrent chemotherapy with continuous 5FU infusion. Chemotherapy dose reduction was done in 11.6% of patients during the second cycle in view of toxicities. Radiological response assessment with MRI at 6 weeks showed complete response [CR] in only one patient. Of the 30 lower rectal tumors (<5 cm from anal verge), 13 patients underwent LAR, and hence, sphincter preservation rate (SPR) was 43.3%. Pathological response assessment showed complete pathological response in 32.60%, moderate response in 30.20%, minimal response in 23.3%, and poor response in 14%. The details of down-staging (both “T” and “N” stages) have been tabulated in Tables 4 and 5. Univariate and multivariate logistic regression showed that pretreatment CEA level was the only independent predictive factor of pCR (Table 6). Additionally, a cutoff value of pretreatment CEA of ≤4.80 ng/mL (sensitivity – 71.4%; specificity – 75.9%) was derived using receiver operating characteristic (ROC) curve to predict pCR (Figure 1). Moreover, it was observed that the pretreatment CEA level was significantly associated with the length of the disease and overall clinical stage (Table 7). The outcomes of different CHRT studies using IMRT are summarized in Table 8.
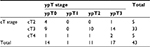  | Table 4 Pathological down-staging – T stage |
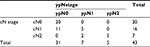  | Table 5 Pathological down-staging – N stage |
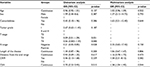  | Table 6 Univariate and multivariate analyses with pCR as a dependent variable Abbreviations: pCR, pathological complete response; CRM, circumferential resection margin; CEA, carcinoembryonic antigen. |
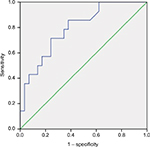  | Figure 1 Receiver operating characteristic curve showing the sensitivity and specificity of pretreatment carcinoembryonic antigen levels to achieve pathological complete response. |
Discussion
Clinical results of IMRT for rectal cancer as a part of CHRT have not been adequately documented worldwide. The studies mentioned in the literature are difficult to compare, as the protocols of both radiotherapy (total dose, boost technique, and dose per fraction) and chemotherapy vary between studies. The results of various studies using IMRT as part of CHRT are summarized in Table 8.
Grade ≥3 skin toxicities varied from 0.03% to 21% among different IMRT studies, compared to 12% in the present study (Table 8). Dermatitis was observed predominantly over the medial thigh and perineum. This occurred more in lesions of the lower rectum where doses were delivered up to or beyond the anal verge.
One of the advantages of IMRT over 3-dimensional conformal radiotherapy (3DCRT) lies in its ability to spare the small bowel. In a study conducted by Yang et al, the cases with grade ≥2 diarrhea were higher in rectal cancer patients who were treated with 3DCRT as part of CHRT in contrast to IMRT (32% vs 11%).27 Concurrently, RTOG 0822 (which was a Phase II trial using IMRT) did not result in significant difference in gastrointestinal toxicities.10 Nevertheless, this was a single-arm study, with IMRT as part of CHRT and the outcomes were compared with the results of RTOG 0247.30 Grade ≥3 diarrhea was experienced by 9.3% of the patients (4/43) in the present study, while the same has been reported between 1% and 18% among other IMRT studies (Table 8). It was noted that acute diarrheal toxicity grade ≥3 was experienced when the SBV45 Gy exceeded 120 cc. This is lower if compared to the QUANTEC guidelines, suggesting SBV45 Gy as 195 cc. This difference in the values could be a result of the variations in the ethnicity, contouring, planning, beam angles, and diets.
Compared to small bowel, urinary bladder has more tolerance toward radiation. Even though IMRT has more dosimetric avoidance of urinary bladder than 3DCRT, it is unlikely to reflect clinically. All patients in our study had only grade 1 cystitis. Except for one study conducted by Hernando-Requejo et al, showing grade ≥3 genitourinary (GU) toxicities of up to 5%, the remaining IMRT series failed to identify any grade ≥3 GU toxicities.12,16,18,25,26 Similarly, grade ≥3 hematological toxicities are less in almost all the IMRT studies, ranging between 0%–6%.14–17,22,24,26,28 Nonetheless, another study which is a Phase I trial using hypofractionated IMRT in rectal cancer showed 13% grade ≥3 anemia. This study was discontinued due to toxicities. Apart from two cases (4.7%) of neutropenia, no other grade ≥2 hematological toxicities were observed in the present study.
Despite toxicity reduction, sphincter preservation is another advantage of CHRT which converts abdominoperineal resection candidates to LAR ones. The German rectal cancer study demonstrated SPR of 39% in those who underwent preoperative CHRT by the conventional technique, while the present study showed 43.3%.1 Yet another study using IMRT by helical tomotherapy achieved an SPR of 85.2%.16
pCR rates range from 0%–50% among various IMRT studies.12,22,24,25,28 This wide range might be due to varying radiation doses, dose per fraction, chemotherapy regimen used, and certain factors of tumor biology are still unexplored and under research. Among these, Cubillo et al, who delivered equivalent 2 Gy per fraction (EQD2) of 60.4 Gy using the simultaneous integrated boost technique along with bevacizumab or cetuximab, achieved a pCR rate of 50%.13 As depicted in Table 8, only three studies have delivered EQD2 dose of 49.4 Gy (1.8 Gy per fraction to the tumor) without any boost.21,26,30 Of these, only one study has used 5FU or capecitabine and reported a pCR rate of 19.4%, compared to 32.6% in the present study.30
Predictors to achieve pCR have been extensively studied. A meta-analysis demonstrated interval to surgery as the independent variable to achieve the same.31 Another meta-analysis evaluated the role of pretreatment CEA level and concluded that a normal level of CEA predicted more pCR.32 The present study nevertheless kept one variable as a constant, as the interval to surgery was at a mean of 45 days with an SD of 3 days. The current study suggests that the independent predictive factor to achieve pCR is the pretreatment CEA level when surgery is performed at a mean interval of 45 days. Further, an ROC curve showed pretreatment CEA of ≤4.80 ng/mL (sensitivity – 71.4%; specificity – 75.9%) as a cutoff value to predict pCR (Figure 1). It was also noted that the rectal cancer patients with high pretreatment CEA levels (>5 ng/mL) demonstrated a significant association with increasing length of the disease and overall clinical stage (Table 7). Similarly, Filiz et al demonstrated a statistically significant correlation between preoperative serum CEA levels and overall clinical stage.33 However, the authors did not find any relationship with the length of the disease. The data from this study should be interpreted with caution as the number of patients was small.
Conclusion
IMRT as part of neoadjuvant CHRT in the treatment of locally advanced rectal cancer is well tolerated and gives comparable results with earlier studies in terms of pathological response, acute toxicities, and SPR. Pretreatment CEA turned out to be the independent predictor to achieve pCR when surgery was performed at a mean interval of 45 days. Further randomized controlled studies are needed to categorically state that IMRT is superior to 3DCRT.
Acknowledgment
The authors thank Dr DK Shukla (ICMR, Delhi) for his statistical analysis of this study.
Disclosure
The authors report no conflicts of interest in this work.
References
Sauer R, Becker H, Hohenberger W, et al. Preoperative versus postoperative chemoradiotherapy for rectal cancer. N Engl J Med. 2004;351(17):1731–1740. | ||
Bosset JF, Meneveau N, Pavy JJ. Les complications intestinales tardives de la radiothérapie adjuvante des cancers rectaux [Late intestinal complications of adjuvant radiotherapy of rectal cancers]. Cancer Radiother. 1997;1(6):770–774. French. | ||
Nutting CM, Convery DJ, Cosgrove VP, Rowbottom C, Padhani AR, Webb S, Dearnaley DP. Reduction of small and large bowel irradiation using an optimized intensity-modulated pelvic radiotherapy technique in patients with prostate cancer. Int J Radiat Oncol Biol Phys. 2000;48(3):649–656. | ||
Portelance L, Chao KS, Grigsby PW, Bennet H, Low D. Intensity-modulated radiation therapy (IMRT) reduces small bowel, rectum, and bladder doses in patients with cervical cancer receiving pelvic and para-aortic irradiation. Int J Radiat Oncol Biol Phys. 2001;51(1):261–266. | ||
Roeske JC, Lujan A, Rotmensch J, Waggoner SE, Yamada D, Mundt AJ. Intensity-modulated whole pelvic radiation therapy in patients with gynecologic malignancies. Int J Radiat Oncol Biol Phys. 2000;48(5):1613–1621. | ||
Myerson RJ, Garofalo MC, El Naqa I, et al. Elective clinical target volumes for conformal therapy in anorectal cancer: a radiation therapy oncology group consensus panel contouring atlas. Int J Radiat Oncol Biol Phys. 2009;74(3):824–830. | ||
Cox JD, Stetz J, Pajak TF. Toxicity criteria of the Radiation Therapy Oncology Group (RTOG) and the European Organization for Research and Treatment of Cancer (EORTC). Int J Radiat Oncol Biol Phys. 1995;31(5):1341–1346. | ||
Eisenhauer EA, Therasse P, Bogaerts J, et al. New response evaluation criteria in solid tumours: revised RECIST guideline (version 1.1). Eur J Cancer. 2008;45(2):228–247. | ||
Washington MK, Berlin J, Branton P, et al. Protocol for the examination of specimens from patients with primary carcinoma of the colon and rectum. Arch Pathol Lab Med. 2009;133(10):1539–1551. | ||
Hong TS, Moughan J, Garofalo MC, et al. NRG Oncology Radiation Therapy Oncology Group 0822: a Phase 2 study of preoperative chemoradiation therapy using intensity modulated radiation therapy in combination with capecitabine and oxaliplatin for patients with locally advanced rectal cancer. Int J Radiat Oncol Biol Phys. 2015;93(1):29–36. | ||
Engels B, Platteaux N, Van den Begin R, et al. Preoperative intensity-modulated and image-guided radiotherapy with a simultaneous integrated boost in locally advanced rectal cancer: report on late toxicity and outcome. Radiother Oncol. 2013;110(1):155–159. | ||
Hernando-Requejo O, Lopez M, Cubillo A, et al. Complete pathological responses in locally advanced rectal cancer after preoperative IMRT and integrated-boost chemoradiation. Strahlenther Onkol. 2014;190(6):515–520. | ||
Cubillo A, Hernando-Requejo O, Garcia-Garcia E, et al. A prospective pilot study of target-guided personalized chemotherapy with intensity-modulated radiotherapy in patients with early rectal cancer. Am J Clin Oncol. 2012;37(2):117–121. | ||
Zhu J, Liu F, Gu W, et al. Concomitant boost IMRT-based neoadjuvant chemoradiotherapy for clinical stage II/III rectal adenocarcinoma: results of a phase II study. Radiat Oncol. 2014;9:70. | ||
Zhu J, Lian P, Liu F, et al. Phase II trial of first-line chemoradiotherapy with intensity-modulated radiation therapy followed by chemotherapy for synchronous unresectable distant metastases rectal adenocarcinoma. Radiat Oncol. 2013;8:10. | ||
Huang MY, Chen CF, Huang CM, et al. Helical tomotherapy combined with capecitabine in the preoperative treatment of locally advanced rectal cancer. Biomed Res Int. 2014;2014:352083. | ||
Arbea L, Martinez-Monge R, Diaz-Gonzalez JA, et al. Four-week neoadjuvant intensity-modulated radiation therapy with concurrent capecitabine and oxaliplatin in locally advanced rectal cancer patients: a validation phase II trial. Int J Radiat Oncol Biol Phys. 2011;83(2):587–593. | ||
Aristu JJ, Arbea L, Rodriguez J, et al. Phase I-II trial of concurrent capecitabine and oxaliplatin with preoperative intensity-modulated radiotherapy in patients with locally advanced rectal cancer. Int J Radiat Oncol Biol Phys. 2008;71(3):748–755. | ||
Ballonoff A, Kavanagh B, McCarter M, et al. Preoperative capecitabine and accelerated intensity-modulated radiotherapy in locally advanced rectal cancer: a phase II trial. Am J Clin Oncol. 2008;31(3):264–270. | ||
Freedman GM, Meropol NJ, Sigurdson ER, et al. Phase I trial of preoperative hypofractionated intensity-modulated radiotherapy with incorporated boost and oral capecitabine in locally advanced rectal cancer. Int J Radiat Oncol Biol Phys. 2007;67(5):1389–1393. | ||
Gasent Blesa JM, Garde Noguera J, Laforga Canales JB, et al. Phase II trial of concomitant neoadjuvant chemotherapy with oxaliplatin and capecitabine and intensity-modulated radiotherapy (IMRT) in rectal cancer. J Gastrointest Cancer. 2012;43(4):553–561. | ||
Li JL, Ji JF, Cai Y, et al. Preoperative concomitant boost intensity-modulated radiotherapy with oral capecitabine in locally advanced mid-low rectal cancer: a phase II trial. Radiother Oncol. 2011;102(1):4–9. | ||
Richetti A, Fogliata A, Clivio A, et al. Neo-adjuvant chemo-radiation of rectal cancer with volumetric modulated arc therapy: summary of technical and dosimetric features and early clinical experience. Radiat Oncol. 2010;5:14. | ||
Zhu J, Gu W, Lian P, et al. A phase II trial of neoadjuvant IMRT-based chemoradiotherapy followed by one cycle of capecitabine for stage II/III rectal adenocarcinoma. Radiat Oncol. 2013;8:130. | ||
Parekh A, Truong MT, Pashtan I, et al. Acute gastrointestinal toxicity and tumor response with preoperative intensity modulated radiation therapy for rectal cancer. Gastrointest Cancer Res. 2013;6(5–6):137–143. | ||
Jabbour SK, Patel S, Herman JM, et al. Intensity-modulated radiation therapy for rectal carcinoma can reduce treatment breaks and emergency department visits. Int J Surg Oncol. 2012;2012:891067. | ||
Yang TJ, Oh JH, Son CH, Apte A, Deasy JO, Wu A, Goodman KA. Predictors of acute gastrointestinal toxicity during pelvic chemoradiotherapy in patients with rectal cancer. Gastrointest Cancer Res. 2013;6(5–6):129–136. | ||
Samuelian JM, Callister MD, Ashman JB, Young-Fadok TM, Borad MJ, Gunderson LL. Reduced acute bowel toxicity in patients treated with intensity-modulated radiotherapy for rectal cancer. Int J Radiat Oncol Biol Phys. 2012;82(5):1981–1987. | ||
Ng SY, Colborn KL, Cambridge L, Hajj, C, Yang TJ, Wu AJ, Goodman AK. Acute toxicity with intensity modulated radiotherapy versus 3-dimensional conformal radiotherapy during preoperative chemoradiation for locally advanced rectal cancer. Radiother Oncol. 2016;121(2):252–257. | ||
Wong SJ, Winter K, Meropol NJ, et al. Radiation Therapy Oncology Group 0247: a randomized Phase II study of neoadjuvant capecitabine and irinotecan or capecitabine and oxaliplatin with concurrent radiotherapy for patients with locally advanced rectal cancer. Int J Radiat Oncol Biol Phys. 2012;82(4):1367–1375. | ||
Petrelli F, Sgroi G, Sarti E, Barni S. Increasing the interval between neoadjuvant chemoradiotherapy and surgery in rectal cancer: a meta-analysis of published studies. Ann Surg. 2016;263(3):458–464. | ||
Yu H, Chen W, Cai Y, et al. Pretreatment serum CEA as a predictive biomarker for the response to neoadjuvant chemoradiotherapy: a meta-analysis in rectal cancer. J Carcinog Mutagen. 2015;6:237. | ||
Filiz AI, Sucullu I, Kurt Y, Karakas DO, Gulec B, Akin ML. Persistent high postoperative carcinoembryonic antigen in colorectal cancer patients – is it important? Clinics (Sao Paulo). 2009;64(4):287–294. |
 © 2018 The Author(s). This work is published and licensed by Dove Medical Press Limited. The full terms of this license are available at https://www.dovepress.com/terms.php and incorporate the Creative Commons Attribution - Non Commercial (unported, v3.0) License.
By accessing the work you hereby accept the Terms. Non-commercial uses of the work are permitted without any further permission from Dove Medical Press Limited, provided the work is properly attributed. For permission for commercial use of this work, please see paragraphs 4.2 and 5 of our Terms.
© 2018 The Author(s). This work is published and licensed by Dove Medical Press Limited. The full terms of this license are available at https://www.dovepress.com/terms.php and incorporate the Creative Commons Attribution - Non Commercial (unported, v3.0) License.
By accessing the work you hereby accept the Terms. Non-commercial uses of the work are permitted without any further permission from Dove Medical Press Limited, provided the work is properly attributed. For permission for commercial use of this work, please see paragraphs 4.2 and 5 of our Terms.


