Back to Journals » Cancer Management and Research » Volume 12
Prognostic Significance of Preoperative Inflammatory Biomarkers and Traditional Clinical Parameters in Patients with Spinal Metastasis from Clear Cell Renal Cell Carcinoma: A Retrospective Study of 95 Patients in a Single Center
Authors Xu K, Li J, Hu M, Zhang H, Yang J, Gong H, Li B, Wan W, Xiao J
Received 24 August 2019
Accepted for publication 7 December 2019
Published 7 January 2020 Volume 2020:12 Pages 59—70
DOI https://doi.org/10.2147/CMAR.S228570
Checked for plagiarism Yes
Review by Single anonymous peer review
Peer reviewer comments 2
Editor who approved publication: Dr Eileen O'Reilly
Kehan Xu,1,* Jialin Li,1,* Mengzi Hu,2,* Hao Zhang,1 Jian Yang,1 Haiyi Gong,1 Bo Li,1 Wei Wan,1 Jianru Xiao1
1Department of Orthopedic Oncology, Changzheng Hospital, Second Military Medical University, Shanghai 200003, People’s Republic of China; 2Department of Orthopedics, Xuzhou Central Hospital, Xuzhou, Jiangsu 221009, People’s Republic of China
*These authors contributed equally to this work
Correspondence: Jianru Xiao; Wei Wan
Email [email protected]; [email protected]
Purpose: The purpose of this retrospective study was to identify preoperative inflammatory biomarkers and clinical parameters and evaluate their prognostic significance in patients with spinal metastasis from clear cell renal cell carcinoma (CCRCC).
Patients and methods: Correlations of overall survival (OS) with traditional clinical parameters and inflammatory indicators including the neutrophil–lymphocyte ratio (NLR), platelet–lymphocyte ratio (PLR), lymphocyte–monocyte ratio (LMR), albumin–globulin ratio (AGR), and C-reactive protein to albumin ratio (CRP/Alb ratio) were analyzed in 95 patients with spinal metastasis from CCRCA using the Kaplan–Meier method to identify potential prognostic factors. Factors with P values ≤ 0.1 were subjected to multivariate analysis by Cox regression analysis. P values ≤ 0.05 were considered statistically significant.
Results: The 95 patients included in this study were followed up by a mean of 48.8 months (median 51 months; range 6–132 months), during which 21 patients died, with a death rate of 22.1%. The statistical results indicated that patients with total piecemeal spondylectomy (TPS), targeted therapy, NLR < 3.8 and PLR < 206.9 had a significantly longer OS rate.
Conclusion: TPS and targeted therapy could significantly prolong the OS of patients with spinal metastasis from CCRCC. In addition, NLR and PLR are robust and convenient prognostic indicators that have a discriminatory ability superior to other inflammatory biomarkers.
Keywords: clear cell renal cell carcinoma, spinal metastasis, overall survival, prognosis, inflammatory biomarkers
Introduction
Prognostic significance of preoperative inflammatory biomarkers and traditional clinical parameters in patients with spinal metastasis from clear cell renal cell carcinoma: a retrospective study of 95 patients in a single center.
Clear cell renal cell carcinoma (CCRCC) is the most common subtype of renal cell carcinoma (RCC), accounting for approximately 70% of all RCC cases.1–3 Nearly 20–30% patients of CCRCC presented bone metastasis at the time of diagnosis, while 20% patients with localized CCRCC finally progressed into metastatic CCRCC, with the spine common site.4,5 Spinal metastasis causes malignant spinal cord compression (MSCC), defined as compression of the spinal cord or cord equina by metastatic or direct spread to the vertebrae that may cause neurological disability.6 MSCC exhibits paralysis, intractable pain, spinal instability, and hypercalcemia, increased morbidity and decreased quality of life of the patients.7,8 In our previous study,9 we reported surgical intervention and survival outcomes of 30 patients with spinal metastasis from CCRCC, in which the statistical results revealed that Tokuhashi score was the only independent prognostic indicator.9 However, the outcome obtained from that study is not convincing enough due to the small sample size. In addition, clinical practices have demonstrated that the conventional prognostic factors including sex, treatment history, surgical modality and Tomita score lack accuracy and adequacy in predicting the prognosis; therefore, more accessible and reliable prognostic indicators need to be explored to identify high-risk patients and allocate personalized treatment for the sake of improving the therapeutic and clinical outcome.
Increasing evidence has demonstrated that inflammatory mediators and cytokines produced by tumor inflammatory cells in the tumor microenvironment are important factors contributing to cancer progression by promoting proliferation, angiogenesis, and metastasis, reducing response to hormones and chemotherapeutic agents, and subverting adaptive immunity.10–14 Targeting of inflammatory pathways has been indicated as a novel way to further enhance the therapeutic efficacy.15,16 Therefore, preoperative inflammatory biomarkers may be potential prognostic factors for patients with spinal metastasis from CCRCC. Accordingly, serum white blood cells, neutrophils, lymphocytes, platelets and acute-phase proteins, such as C-reactive (CRP) protein and albumin (ALB), have been evaluated in different tumors and found to predict the prognosis and response to treatment.17,18 The appearance of Circulating tumor cells (CTCs) in the peripheral blood indicated active disease, proliferation, and metastatic potency, and is followed by genomic analyses that provide data in terms of the tumor biology and real-time monitoring of the therapeutic efficacy.19 Given the association between inflammatory response and tumor progression, the prognostic significance of several preoperative inflammatory biomarkers has been suggested, including the neutrophil/lymphocyte ratio (NLR), platelet/lymphocyte ratio (PLR), lymphocyte/monocyte ratio (LMR), ALB/globulin ratio (AGR), and CRP/ALB ratio (CAR). However, to the best of our knowledge, no publications in the medical literature have taken inflammatory factors as prognostic predictors of patients with spinal metastasis from CCRCC.
The aim of the present retrospective study was to evaluate the prognostic significance of several preoperative inflammatory biomarkers including the NLR, PLR, LMR, AGR, and CAR by comparing them with the conventional prognostic factors.
Materials and Methods
Patients
Medical records of 157 patients with spinal metastasis from CCRCC who received surgical treatment in our tumor center between August 2005 and September 2016 were analyzed retrospectively. This research project was examined and approved by the medical ethics committee of Changzheng hospital before commencing this study, and written informed consent was obtained from all patients or their legal guardians. The study was in compliance with the Declaration of Helsinki.
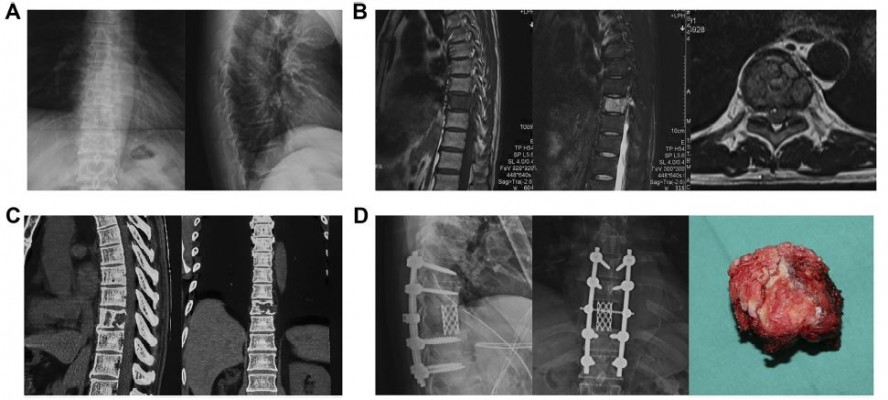
The inclusion criteria were as follows: 1) spinal metastasis from CCRCC confirmed by clinical manifestations, radiological presentations, and postoperative pathology; 2) patients who underwent surgical treatment in our tumor center; 3) patients had not taken anti-inflammatory medicines or received immunosuppressive therapy including recent steroid exposure, or with chronic inflammatory diseases including autoimmune diseases and infections before operation; 4) patients without receiving preoperative adjuvant therapy; and 5) the laboratory test results obtained before surgery. Finally, 95 patients who met with these inclusion criteria were enrolled in this study, and the flow diagram is shown in Figure 1. The material of a typical case underwent total en bloc spondylectomy (TES) is shown in Figure 2.
 |
Figure 1 Patient flow diagram. |
The clinical and operative notes, radiographic images, and pathological reports of all patients who received surgery in our department for RCC spinal metastases were reviewed retrospectively. The preoperative neurological status was evaluated according to the Frankel score.20 The spinal tumors were classified based on Tomita classification21 and Tokuhashi score.22 Only overall survival (OS) was considered as the endpoint in this study. Event times were defined as the interval from the date of surgery to death, or until September 2016 for living patients. All patients were followed up on an outpatient basis at 3, 6, and 12 months after surgical treatment, every 6 months for the second year, and then annually for life.
Statistical Method
X-tile 3.6.1 software 20 (Yale University, New Haven, CT, USA) was used to determine the optimal cut-off values for NLR, PLR, LMR, and CAR. Quantitative data are described by median (range), and qualitative data are described as counts and percentages. Statistical calculations were analyzed using SPSS version 19.0 (SPSS, Inc. Chicago, IL, USA). Univariate and multivariate analyses were used to identify the independent significant factors especially preoperative inflammatory biomarkers that could predict prognosis for OS. Log-rank tests were performed for univariate analysis, and Cox proportional hazards model was used for multivariate analysis. OS were calculated by the Kaplan–Meier method. Factors with P value ≤ 0.10 in univariate analysis were subjected to multivariate analysis. Factors with P values ≤ 0.05 in multivariate analysis were considered statistically significant.
Results
Patients’ Baseline Characteristics and Optimal Cutoff Values of Inflammatory Biomarkers
The characteristics of all patients are detailed in Table 1. The population comprised 84 males and 11 females with a mean age of 54.2 years (median, 56 years; range, 16–75 years). The mean follow-up time was 48.8 months (median, 51 months; range, 6–132 months). Of the 95 included patients, 21 died during the postoperative follow-up period, with death rate of 22.1%. The mean duration from initial surgery to death was 17.9 months (median, 15 months; range, 6–45 months). Of these patients, 80 patients were admitted for primary spinal metastasis from CCRCC, and the remaining 15 patients underwent surgical treatment for recurrences.
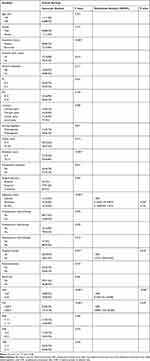 |
Table 1 Univariate and Multivariate Analysis of Clinical and Inflammatory Indicators for Overall Survival of Patients with Spinal Metastasis from CCRCC |
The optimal cut-off value of NLR, PLR, LMR, and CAR was determined by the X-tile program, which was 3.8, 206.9, 2.3, and 1.2, respectively (Figure 3). The log-rank value for NLR, PLR, LMR, and CAR was 63.5, 47.0, 51.0, and 8.2, respectively. According to the standard value reported by the Clinical Laboratory Department in Changzheng Hospital (Shanghai, China), the cut-off value for AGR was 1.5. Therefore, all patients were divided into two groups for further analysis (NLR<3.8 and NLR≥3.8; PLR<206.9 and PLR≥206.9; AGR<1.5 and AGR≥1.5; LMR<2.3 and LMR≥2.3; CAR<1.2 and CAR≥1.2).
Univariate and Multivariate Analyses of Prognostic Factors for OS
Twenty-one patients died during the follow-up period, thus the OS rate of patients with spinal metastasis from CCRCC was 77.9%, with a median OS of 57.6 months (range, 24–132 months). The results of univariate and multivariate analyses of possible prognostic factors are shown in Table 1. Univariate analysis revealed that significant difference was obtained in patients with treatment history (P < 0.001), Tokuhashi score (P < 0.001), resection mode (P < 0.001), targeted therapy (P = 0.001), NLR (P < 0.001), and PLR (P < 0.001).
All potential prognostic factors obtained by univariate analysis were extracted into Cox proportional hazard for multivariate analysis (Table 1). Patients who underwent TPS had longer OS than those who received TES or subtotal resection (TPS [HR, 0.319, P = 0.024] versus TES [HR, 0.196; P = 0.132]). Targeted therapy significantly increased chance of OS (HR, 3.471; P = 0.016). Patients with preoperative NLR < 3.8 had longer OS than those with preoperative NLR≥ 3.8 (HR, 8.332; P < 0.001). Simultaneously, preoperative PLR value≥206.9 significantly suggested poorer OS for patients with spinal metastasis from CCRCC (HR, 3.808; P = 0.010). The Kaplan–Meier curves of OS for resection mode, targeted therapy, NLR, and PLR are presented in Figure 4A–D. Therefore, resection mode, targeted therapy, NLR, and PLR were independent prognostic factors for OS.
 |
Figure 4 Kaplan–Meier curves of overall survival for (A) Resection mode, (B) Targeted therapy, (C) NLR, and (D) PLR. |
Clinical Management of Patients with Recurrent Spinal Metastasis from CCRCC
Based on the clinical manifestations and radiological presentations, 15 patients who received curettage in other hospitals were identified as having local recurrence of spinal lesions and chosen to undergo a second operation in our spinal tumor center. The characteristics of these recurrent patients are detailed in Tables 2 and 3. Interestingly, all patients were male with a mean age of 58.8 (43–68) years. The spinal lesions were classified by Tomita classification, and the condition of the patients was assessed by the Tokuhashi score. All spinal lesions were classified as Tomita IV-VI in accordance with Tomita classification. In three patients (Case # 10–12) with Tokuhashi score < 9, TPS or subtotal resection was performed TPS or subtotal resection under the robust request of patients or their guardians. Unfortunately, all of them died during the follow-up period. Case # 2 with the lesion classified as Tomita IV only received TES, and Case # 1 with the tumor evaluated as Tomita VI underwent TES and postoperative targeted therapy. All patients who received TES were alive during the follow-up period. TPS was performed in eight patients, three of whom (Case # 8,10,12) died of tumor recurrence, progression, and metastasis within 2 years, respectively. One patient (case # 10) dead 45 months after surgical treatment. Meanwhile, all patients (case # 9,11,13–15) who received subtotal resection died of tumor progression and metastasis. Case # 3 and Case # 7 received repeated operations for tumor recurrences in our spinal tumor center. To better understand the outcomes of different surgical methods, we conducted the Kaplan-Meier survival curve and Log-rank test and the result showed p value = 0.045 (Figure 5).
 |
Table 2 Clinical Management of Recurrent Patients with Spinal Metastasis from CCRCC |
 |
Table 3 Treatment Protocols and Outcomes of Recurrent Spinal Metastasis from CCRCC |
 |
Figure 5 Kaplan–Meier curves of overall survival of recurrent patients for resection mode. |
Discussion
To the best of our knowledge, this is the largest monocentric retrospective study regarding the prognostic significance of clinical factors and inflammatory biomarkers. About 30% CCRCC patients developed bone metastasis, especially in the spine.23
With the advance in surgical treatment, targeted therapy, and precise radiotherapy, the OS of spinal metastasis from CCRCC has improved remarkably in recent years.24–26
In this research, clinical factors and inflammatory biomarkers were analyzed to identify convenient and reliable prognostic biomarkers for identifying high-risk patients and improve the clinical outcome of spinal metastasis from CCRCC. Simultaneously, we attempted to find out answers to the following questions:
- Which parameters have the prognostic value for predicting OS for spinal metastasis from CCRCC?
- Do the inflammatory factors affect disease progression and OS?
- Do the widely used adjuvant therapies, such as adjuvant radiotherapy, intraoperative local treatment, and targeted therapy have a therapeutic effect?
The results obtained from this study suggest that resection mode, targeted therapy, NLR and PLR are significantly correlated with OS. Total resection is superior to subtotal resection for OS of patients with spinal metastasis from CCRCC. However, statistical analysis revealed that TPS could prolong the OS of patients compared with TES. With the development of targeted agents that inhibit the vascular endothelial grow factor (VEGF) and the mammalian target of rapamycin (mTOR) signal transduction pathways (7, 8), patients administered with targeted therapy had longer OS than those without it. Our finding demonstrated that NLR and PLR versus other indicators had a discriminatory ability as novel and promising inflammatory biomarkers.
Surgical treatment is the standard treatment based on Tomita classification for spinal metastasis with respect to preserving neurological functionality, relieving pain and promising prolonged survival.27–29 Petteys et al25 reported that resection and fixation provided pain relief and neurological stabilization in patients with spinal metastasis arising from RCC, and aggressive intervention was beneficial to younger patients. Tatsui et al6 also supported surgical treatment as aggressive intervention on the basis of identifying several factors influencing survival. Our former study suggested that surgical treatment was not the independent prognostic factor for patients with spinal metastasis from CCRCC, but the sample size of that study is small.9 In the present study, we for the first time demonstrated that TPS, rather than TES and subtotal resection, was the most beneficial surgical approach. As spinal metastatic lesions usually exhibit paraspinal extensions involving even the soft tissue, TES is not feasible. Extensive tumor resection may cause loss of stability of the spine, which was a major concern. This risk has been minimized by the anterior interbody fusion with or without instrumentation.30 Simultaneously, blood bleeding in the procedure of surgical treatment was high owing to rich blood supply in metastasis from RCC, which requires the surgeons to complete the operation as soon as possible. Subtotal resection produces tumor residuals, which is likely to cause local recurrence and tumor progression. In such a case, TPS seems the most suitable of the three surgical approaches.
Although chemotherapy and radiotherapy as adjuvant therapies have been applied to the treatment of spinal metastasis from CCRCC, the therapeutic outcome remains controversial.31 Tao et al32 reported that the combination of surgery with stereotactic body radiation therapy could offer patients with spinal metastatic a chance of durable tumor control with minimal toxicity. However, chemotherapy and postoperative radiotherapy are not significant prognostic factors for OS. With the understanding of molecular biology of RCC, several targeted agents inhibiting VEGF and mTOR signal transduction pathways such as Sunitinib, Sorafenib, Temsirolimus, and Pazopanib have been put into clinical practice.33–36 Meanwhile, statistical results in our study revealed that targeted therapy significantly prolonged the OS of patients with spinal metastasis from CCRCC. Increasing clinical evidence has proven that targeted therapy can downsize the tumor size, control tumor progression, and improve OS, in view of Sunitinib and Sorafenib as the first-line or second-line treatment.37,38 Furthermore, surgery in combination with targeted therapy is useful for patients with spinal metastasis from CCRCC in that it provides a new therapeutic strategy for such patients.
In addition, our results suggested that NLR and PLR could serve as reliable and novel inflammatory prognostic biomarkers superior to other indicators for spinal metastasis from CCRCC. The relationship between chronic inflammation and RCC has been investigated, and it is increasingly recognized that systemic inflammatory response plays a crucial role in RCC development and progression.39,40 However, there is no published information regarding the prognostic significance of preoperative inflammatory indicators for spinal metastasis from CCRCC. Zhun et al41 reported that a high preoperative PLR was correlated with poor prognosis in RCC patients, and Hu et al42 demonstrated that pre-operative NLR could be considered as a potential prognostic biomarker in RCC patients who underwent surgical resection. Recent studies43–45 have demonstrated that neutrophils interact with tumor cells via secretion of cytokines, thus promoting tumor development, lymphocytes mediate immunological destruction of cancer cells; and platelets serve as chemoattractants to promote migration of tumor cells. These inflammatory backgrounds at least theoretically support the use of several inflammatory biomarkers as prognostic indicators of spinal metastasis from CCRCC. Tokuhashi score and Tomita classification are known as the most popular prognostic scores for patients with spinal metastasis.21,22 In our previous study,9 we found that only the Tokuhashi score was an independent prognostic factor for patients with CCRCC. Pettey et al46 reported that Tokuhashi score could be used for selecting surgical patients with RCC spinal metastases, and maybe more relevant as compared with its effectiveness in patients with spinal metastases from other cancers. However, our results showed that the Tokuhashi score was not a suitable prognostic factor for OS. In our opinion, targeted therapy may be able to prolong the survival of patients with a low Tokuhashi score. In recurrent cases, nine of the 15 recurrent patients in our series died during the follow-up period, suggesting that local recurrence maybe an adverse prognostic factor for OS. Our subtype analysis suggested that TES significantly prolonged the OS of recurrent patients.
The present study has some limitations. First, this is a retrospective single-center study. In addition, the follow-up duration is not long enough. Finally, the study only focused on the OS of patients who underwent surgical treatment.
Conclusion
Our findings demonstrate that TPS and targeted therapy can significantly prolong the OS of patients with spinal metastasis from CCRCC. Besides, NLR and PLR are robust and convenient prognostic indicators whose discriminatory ability is superior to that of other preoperative inflammatory biomarkers. However, further multi-center studies are required to validate our results and conclusions.
Ethics Approval and Consent
All procedures involving human participants in this study were approved by the ethics committee of Changzheng Hospital (Shanghai, China), and written informed consent was obtained from all patients or their legal guardians. The study was in compliance with the Declaration of Helsinki. Patients or their legal guardians know of and approved the publication.
Disclosure
The authors report no funding and no conflicts of interest in this work.
References
1. Goodwin CR, Ahmed AK, Boone C, et al. The challenges of renal cell carcinoma metastatic to the spine: a systematic review of survival and treatment. Global Spine J. 2018;8(5):517–526. doi:10.1177/2192568217737777
2. Hirsch MS, Signoretti S, Dal Cin P. Adult renal cell carcinoma: a review of established entities from morphology to molecular genetics. Surg Pathol Clin. 2015;8(4):587–621. doi:10.1016/j.path.2015.09.003
3. Tan PH, Cheng L, Rioux-Leclercq N, et al. Renal tumors: diagnostic and prognostic biomarkers. Am J Surg Pathol. 2013;37(10):1518–1531. doi:10.1097/PAS.0b013e318299f12e
4. Guida A, Escudier B, Albiges L. Treating patients with renal cell carcinoma and bone metastases. Expert Rev Anticancer Ther. 2018;5:1–9.
5. Bianchi M, Sun M, Jeldres C, et al. Distribution of metastatic sites in renal cell carcinoma: a population-based analysis. Ann Oncol. 2012;23(4):973–980. doi:10.1093/annonc/mdr362
6. Boussios S, Cooke D, Hayward C, et al. Metastatic spinal cord compression: unraveling the diagnostic and therapeutic challenges. Anticancer Res. 2018;38(9):4987–4997. doi:10.21873/anticanres.12817
7. Higuchi T, Yamamoto N, Hayashi K, et al. Long-term patient survival after the surgical treatment of bone and soft-tissue metastases from renal cell carcinoma. Bone Joint J. 2018;100-B(9):1241–1248. doi:10.1302/0301-620X
8. Alamanda VK, Robinson MM, Kneisl JS, et al. Functional and survival outcomes in patients undergoing surgical treatment for metastatic disease of the spine. J Spine Surg. 2018;4(1):28–36. doi:10.21037/jss
9. Han S, Wang T, Jiang D, et al. Surgery and survival outcomes of 30 patients with neurological deficit due to clear cell renal cell carcinoma spinal metastases. Eur Spine J. 2015;24(8):1786–1791. doi:10.1007/s00586-015-3912-3
10. Diakos CI, Charles KA, McMillan DC, et al. Cancer-related inflammation and treatment effectiveness. Lancet Oncol. 2014;15(11):e493–e503. doi:10.1016/S1470-2045(14)70263-3
11. Candido J, Hagemann T. Cancer-related inflammation. J Clin Immunol. 2013;33(Supply 1):S79–S84. doi:10.1007/s10875-012-9847-0
12. Hirahara N, Matsubara T, Kawahara D, et al. Prognostic significance of preoperative inflammatory response biomarkers in patients undergoing curative thoracoscopic esophagectomy for esophageal squamous cell carcinoma. Eur J Surg Oncol. 2017;43(2):493–501. doi:10.1016/j.ejso.2016.11.018
13. Cerón-Carrasco JP, Pérez-Sánchez H, Zúñiga J, et al. Antibodies as carrier molecules: encapsulating anti-inflammatory drugs inside herceptine. J Phys Chem B. 2018;122(7):2064–2072. doi:10.1021/acs.jpcb.7b10749
14. Diakos CI, Charles KA, McMillan DC, et al. Cancer-related inflammation and treatment effectiveness. Lancet Oncol. 2014;15:e493–e503. doi:10.1016/S1470-2045(14)70263-3
15. Xu K, Lou Y, Sun R, et al. Establishment of a nomogram-based model for predicting the prognostic value of inflammatory biomarkers and preoperative D-Dimer level in spinal Ewing’s sarcoma family tumors: a retrospective study of 83 patients. World Neurosurg. 2019;121(Suppl 1):e104–e112. doi:10.1007/s10875-012-9847-0
16. Savant SS, Sriramkumar S, O’Hagan HM. The role of inflammation and inflammatory mediators in the development, progression, metastasis, and chemoresistance of epithelial ovarian cancer. Cancers (Basel). 2018;10(8):E251. doi:10.3390/cancers10080251
17. de Vivar Chevez AR, Finke J, Bukowski R. The role of inflammation in kidney cancer. Adv Exp Med Biol. 2014;8:197–234. doi:10.1007/978-3-0348-0837-8_9
18. Lee CS, Ryan EJ, Doherty GA. Gastro-intestinal toxicity of chemotherapeutics in colorectal cancer: the role of inflammation. World J Gastroenterol. 2014;20(14):3751–3761. doi:10.3748/wjg.v20.i14.3751
19. Boussios S, Ozturk MA, Moschetta M, et al. The developing story of predictive biomarkers in colorectal cancer. J Pers Med. 2019;9(1):E12. doi:10.3390/jpm9010
20. Frankel HL, Hancock DO, Hyslop G, et al. The value of postural reduction in the initial management of closed injuries of the spine with paraplegia and tetraplegia. I. Paraplegia. 1969;7(3):179–192.
21. Tomita K, Kawahara N, Kobayashi T, et al. Surgical strategy for spinal metastases. Spine. 2001;26(3):298–306. doi:10.1097/00007632-200102010-00016
22. Tokuhashi Y, Matsuzaki H, Toriyama S, et al. Scoring system for the preoperative evaluation of metastatic spine tumor prognosis. Spine (Phila Pa 1976). 1990;15:1110–1113. doi:10.1097/00007632-199011010-00005
23. Ruatta F, Derosa L, Escudier B, et al. Prognosis of renal cell carcinoma with bone metastases: experience from a large cancer center. Eur J Cancer. 2018;107:79–85. doi:10.1016/j.ejca.2018.10.023
24. Miller JA, Balagamwala EH, Angelov L, et al. Spine stereotactic radiosurgery with concurrent tyrosine kinase inhibitors for metastatic renal cell carcinoma. J Neurosurg Spine. 2016;25(6):766–774. doi:10.3171/2016.4.SPINE16229
25. Petteys RJ, Spitz SM, Goodwin CR, et al. Factors associated with improved survival following surgery for renal cell carcinoma spinal metastases. Neurosurg Focus. 2016;41(2):E13. doi:10.3171/2016.5.FOCUS16145
26. Mosele GR, Caggiari G, Scarpa RM, et al. The treatment of vertebral metastases from renal cell carcinoma: a retrospective study. Minerva Urol Nefrol. 2017;69(2):166–172. doi:10.23736/S0393-2249.16.02809-5
27. Ma Y, He S, Liu T, et al. Quality of life of patients with spinal metastasis from cancer of unknown primary origin: a longitudinal study of surgical management combined with postoperative radiation therapy. J Bone Joint Surg Am. 2017;99(19):1629–1639. doi:10.2106/JBJS.16.00286
28. Kakutani K, Sakai Y, Maeno K, et al. Prospective cohort study of performance status and activities of daily living after surgery for spinal metastasis. Clin Spine Surg. 2017;30(8):E1026–E1032. doi:10.1097/BSD.0000000000000456
29. Toquart A, Graillon T, Mansouri N, et al. Management of spinal metastasis by minimal invasive surgery technique: surgical principles, indications: a literature review. Neurochirurgie. 2016;62(3):157–164. doi:10.1016/j.neuchi.2015.12.007
30. Boussios S, Hayward C, Cooke D, et al. Spinal ewing sarcoma debuting with cord compression: have we discovered the thread of ariadne? Anticancer Res. 2018;38(10):5589–5597. doi:10.21873/anticanres.12893
31. Stenman M, Sinclair G, Paavola P, et al. Overall survival after stereotactic radiotherapy or surgical metastasectomy in oligometastatic renal cell carcinoma patients treated at two Swedish centres 2005-2014. Radiother Oncol. 2018;127:501–506. doi:10.1016/j.radonc.2018.04.028
32. Tao R, Bishop AJ, Brownlee Z, et al. Stereotactic body radiation therapy for spinal metastases in the postoperative setting: a secondary analysis of mature phase 1-2 trials. Int J Radiat Oncol Biol Phys. 2016;95(5):1405–1413. doi:10.1016/j.ijrobp.2016.03.022
33. Staehler M, Motzer RJ, George DJ, et al. Adjuvant sunitinib in patients with high-risk renal cell carcinoma: safety, therapy management, and patient-reported outcomes in the S-TRAC trial. Ann Oncol. 2018;29(10):2098–2104. doi:10.1093/annonc/mdy329
34. Wang Q, Wu G, Che X, et al. Sorafenib induces renal cell carcinoma apoptosis via upregulating activating transcription factor 4. Pharmazie. 2018;73(3):156–160. doi:10.1691/ph.2018.7855
35. Satoh T, Koie T, Horiguchi H, et al. Longer recurrence-free survival in a patient with metastatic renal cell carcinoma treated with temsirolimus. Clin Case Rep. 2017;5(12):1950–1953. doi:10.1002/ccr3.1181
36. Méndez-Vidal MJ, Molina Á, Anido U, et al. Pazopanib: evidence review and clinical practice in the management of advanced renal cell carcinoma. BMC Pharmacol Toxicol. 2018;19(1):77. doi:10.1186/s40360-018-0264-8
37. Cai W, Huang J, Yuan Y, et al. Sunitinib or sorafenib as neoadjuvant therapy may not improve the survival outcomes of renal cell carcinoma with tumor thrombus. Urol Int. 2018;101:391–399. doi:10.1159/000492723
38. Maroun R, Mitrofan L, Benjamin L, et al. Real life patterns of care and progression free survival in metastatic renal cell carcinoma patients: retrospective analysis of cross-sectional data. BMC Cancer. 2018;18(1):214. doi:10.1186/s12885-018-4117-z
39. Mizuno R, Kimura G, Fukasawa S, et al. Angiogenic, inflammatory and immunologic markers in predicting response to sunitinib in metastatic renal cell carcinoma. Cancer Sci. 2017;108(9):1858–1863. doi:10.1111/cas.13320
40. Gu L, Ma X, Wang L, et al. Prognostic value of a systemic inflammatory response index in metastatic renal cell carcinoma and construction of a predictive model. Oncotarget. 2016;8(32):52094–52103. doi:10.18632/oncotarget.10626
41. Wang Z, Peng S, Wang A, et al. Platelet-lymphocyte ratio acts as an independent predictor of prognosis in patients with renal cell carcinoma. Clin Chim Acta. 2018;480:166–172. doi:10.1016/j.cca.2018.02.014
42. Hu H, Yao X, Xie X, et al. Prognostic value of preoperative NLR, dNLR, PLR and CRP in surgical renal cell carcinoma patients. World J Urol. 2017;35(2):261–270. doi:10.1007/s00345-016-1864-9
43. Swierczak A, Mouchemore KA, Hamilton JA, et al. Neutrophils: important contributors to tumor progression and metastasis. Cancer Metastasis Rev. 2015;34(4):735–751. doi:10.1007/s10555-015-9594-9
44. Lissoni P, Brivio F, Fumagalli L, et al. Efficacy of cancer chemotherapy in relation to the pretreatment number of lymphocytes in patients with metastatic solid tumors. Int J Biol Markers. 2004;19:135–140. doi:10.1177/172460080401900208
45. Ishikawa S, Miyashita T, Inokuchi M, et al. Platelets surrounding primary tumor cells are related to chemoresistance. Oncol Rep. 2016;36(6):787–794. doi:10.3892/or.2016.4898
46. Petteys RJ, Spitz SM, Rhee J, et al. Tokuhashi score is predictive of survival in a cohort of patients undergoing surgery for renal cell carcinoma spinal metastases. Eur Spine J. 2015;24(10):2142–2149. doi:10.1007/s00586-015-3862-9
 © 2020 The Author(s). This work is published and licensed by Dove Medical Press Limited. The full terms of this license are available at https://www.dovepress.com/terms.php and incorporate the Creative Commons Attribution - Non Commercial (unported, v3.0) License.
By accessing the work you hereby accept the Terms. Non-commercial uses of the work are permitted without any further permission from Dove Medical Press Limited, provided the work is properly attributed. For permission for commercial use of this work, please see paragraphs 4.2 and 5 of our Terms.
© 2020 The Author(s). This work is published and licensed by Dove Medical Press Limited. The full terms of this license are available at https://www.dovepress.com/terms.php and incorporate the Creative Commons Attribution - Non Commercial (unported, v3.0) License.
By accessing the work you hereby accept the Terms. Non-commercial uses of the work are permitted without any further permission from Dove Medical Press Limited, provided the work is properly attributed. For permission for commercial use of this work, please see paragraphs 4.2 and 5 of our Terms.