Back to Journals » International Journal of Women's Health » Volume 6
Prevalence and perinatal mortality associated with preterm births in a tertiary medical center in South East Nigeria
Authors Iyoke CA , Lawani OL, Ezugwu EC, Ilechukwu G, Nkwo PO, Mba SG, Asinobi IN
Received 4 August 2014
Accepted for publication 23 August 2014
Published 17 October 2014 Volume 2014:6 Pages 881—888
DOI https://doi.org/10.2147/IJWH.S72229
Checked for plagiarism Yes
Review by Single anonymous peer review
Peer reviewer comments 2
Editor who approved publication: Professor Elie Al-Chaer
Chukwuemeka Anthony Iyoke,1 Osaheni Lucky Lawani,2 Euzebus Chinonye Ezugwu,1 Gideon Ilechukwu,3 Peter Onubiwe Nkwo,1 Sunday Gabriel Mba,1 Isaac Nwabueze Asinobi4
1Department of Obstetrics and Gynaecology, University of Nigeria Teaching Hospital, Ituku-Ozalla, Enugu, Nigeria; 2Department of Obstetrics and Gynaecology, Federal Teaching Hospital, Abakaliki, Nigeria; 3Department of Paediatrics, Whiston Hospital, St Helen's and Knowsley Teaching Hospitals NHS Trust, Prescot, Lancashire, UK; 4Department of Paediatrics, University of Nigeria Teaching Hospital, Ituku-Ozalla, Enugu, Nigeria
Background: Preterm birth is a high risk condition associated with significant mortality and morbidity in the perinatal, neonatal, and childhood periods, and even in adulthood. Knowledge of the epidemiology of preterm births is necessary for planning appropriate maternal and fetal care.
Objective: The objective of this study was to determine the prevalence, pattern, and perinatal mortality associated with preterm births at the University of Nigeria Teaching Hospital, Enugu, South East Nigeria.
Methods: This was a review of prospectively collected routine delivery data involving preterm deliveries that occurred between 1 January 2009 and 31 December 2013. Data analysis involved descriptive and inferential statistics at 95% level of confidence using SPSS version 17.0 for Windows.
Results: There were 3,760 live births over the 5-year study period out of which 636 were preterm births, giving a prevalence rate of 16.9%. Spontaneous preterm births occurred in approximately 57% of preterm births while provider-initiated births occurred in 43%. The mean gestational age at preterm deliveries was 32.6±3.2 weeks while the mean birth weight was 2.0±0.8 kilograms. Approximately 89% of preterm births involved singleton pregnancies. Sixty-eight percent of preterm births were moderate to late preterm. The male:female ratio of preterm babies born during the period was 1.2:1. The adjusted perinatal mortality rate for preterm babies in the study center was 46.1% (236/512). The stillbirth rate for preterm babies was 22.0% (149/678) and the adjusted early neonatal death rate was 24.0% (87/363).
Conclusion: The prevalence of preterm births and associated perinatal mortality were high which may be a reflection of suboptimal prenatal and newborn care. An urgent improvement in prenatal and newborn care is therefore needed in the study center in order to improve the capacity to prevent or abate preterm labor, and preterm premature rupture of membranes; and to reduce avoidable stillbirths. Further upgrading of personnel and facilities in the newborn special care unit is also required to minimize early neonatal deaths.
Keywords: preterm birth, prevalence, mortality, pattern, Nigeria
Introduction
Globally, preterm birth is a major clinical problem associated with significant mortality and morbidity in the perinatal, neonatal, and childhood periods and even in adulthood.1–5 It is a major cause of long-term loss of human potential among survivors.6 In fact, the global concern about the burden of preterm birth has resulted in November 7th being earmarked as World Prematurity Day.7 Increasing preterm birth could significantly militate against the achievement of Millennium Development Goal 4.8 Perhaps in response to this threat, a goal to reduce preterm-specific mortality by 50% by 2025 has been set in the World Health Organization’s (WHO) “Born Too Soon” report.6
Preterm birth has been defined by WHO as any live birth before 37 completed weeks of gestation or fewer than 259 days since the first day of a woman’s last menstrual period.3,6,9 The point in pregnancy when the delivery of a fetus is counted as birth rather than abortion differs across countries.3 It depends on the perceived fetal age of viability, which is based on the availability of modern neonatal care facilities and expertise.10 In developing countries like Nigeria, the legal fetal age of viability is 28 weeks.8 However, below this gestational age, births involving babies with signs of life after 22 weeks are also taken as deliveries.
Preterm births have been categorized based on clinical presentation into: spontaneous preterm births (which comprise those following spontaneous preterm labor with or without preterm premature rupture of membranes) and provider-initiated preterm births.5,6 Globally, about 15 million babies are born preterm annually, representing 11.1% of all live births.5,6,11,12 However, the preterm birth rate varies from one place to another depending inter alia on the method of gestational age assessment and the perceived fetal age of viability.3,9 However, it has been reported to be increasing globally.3,9,13–15 South Asia and sub-Saharan Africa are the regions responsible for 60% of global preterm births.6,16 Reports from some African countries have shown overall preterm birth rate ranging from 11.1% to 57%.4,12
Improved care of preterm babies has resulted in reduced mortality in developed countries.2,11 This is not so in developing countries where the management of preterm birth babies is fraught with difficulties arising from scarcity of resources typified by poorly-equipped specialized newborn care units.12 Consequently, the burden of the complications and mortality from preterm births remains a significant potential challenge to newborn health in resource-poor settings like ours. Currently, there is scant literature on the epidemiology of preterm births in South East Nigeria to guide efforts at preventing and/or managing preterm births. The aims of this study were to determine the prevalence and pattern of, and perinatal mortality associated with preterm births at the University of Nigeria Teaching Hospital, Enugu, South East Nigeria.
Methods
Study center
The study was carried out at the University of Nigeria Teaching Hospital (UNTH), Enugu. There are ten clinical departments in UNTH, two of which are Obstetrics/Gynaecology department and Paediatrics department. The Paediatrics department has a specialized neonatology unit, the Newborn Special Care Unit (NBSCU), which is a neonatal intensive care unit located within the labor ward complex. The two departments render 24-hour obstetric and neonatal services. UNTH serves as a referral hospital to other health facilities mainly within Enugu State and less from the neighboring states of Abia, Ebonyi, Anambra, and Imo. Consequently, the maternity and neonatology units of the UNTH also receive pregnant women and/or newborn babies from across Enugu and the neighboring states.
Study design
This was a retrospective review of prospectively collected routine delivery data on preterm births.
Study period
The study covered the period between 1 January 2009 and 31 December 2013.
Sampling
The delivery database of the UNTH was reviewed and all births that occurred between 2009 and 2013 were examined. All women who delivered between gestational ages 28 weeks and 36 weeks plus 6 days whose records were available were selected. In addition, those who delivered babies below 28 weeks old whose babies had signs of life during study period were also included. The delivery and case records of selected patients were retrieved for data collection. The women were included if the date of the last menstrual period was reliably documented and/or there was ultrasound confirmation of gestational age. Similarly, the NBSCU database was reviewed and all the preterm babies who were delivered at the UNTH were identified and their case records were retrieved.
Data collection
Data extraction was done by two of the authors (CAI and INA) and two other trained research assistants who were of the rank of registrars (one each from the departments of Obstetrics/ Gynaecology and Paediatrics). The data were abstracted from the delivery database, mothers’ clinical case notes, NBSCU database, and the babies’ case notes. Data abstracted included maternal age, booking status, parity, educational status, occupation, previous gynecological and obstetric history, antenatal history, intrapartum events, gestational age at delivery, first- and fifth-minute Apgar scores, fetal sex, NBSCU admission, perinatal complications, and causes of perinatal deaths. The information extracted was entered into a structured pro forma which was divided into sections which included maternal socio-demographic data, obstetric history, prenatal interventions/treatment, intrapartum findings, and neonatal outcome.
Data analysis
The statistical analysis was carried out using Statistical Package for Social Sciences (SPSS) version 17.0 for Windows (SPSS Inc., Chicago, IL, USA) and Microsoft Excel software (Microsoft Corporation, Redmond, WA, USA). Classifications of preterm births and low birth weight were based on the WHO sub-categorization of preterm births and low birth weight.17 Provider-initiated preterm birth was defined as birth due to elective induction of preterm labor or due to preterm cesarean section before the onset of labor. Frequencies, means, and proportions of variables were computed. The association between categorical variables was determined using chi-square test or Fisher’s exact test where appropriate. For the estimation of perinatal mortality rate and early neonatal mortality rate, only the records of babies admitted into the NBSCU could be accessed and were therefore used: mortality data on preterm babies who were not admitted into the NBSCU were not available. Adjusted perinatal and early neonatal mortality rates were therefore computed.
To determine the variables that predicted perinatal death, a bivariate logistic regression analysis was done. Only variables significantly associated with perinatal death on bivariate analysis were included in logistic regression models. The Hosmer–Lemeshow goodness-of-fit test was done to determine the fitness of the data to the logistic regression model. The results were reported as adjusted odds ratios and 95% confidence intervals. For all analyses, P-value ≤0.05 was considered significant.
Ethical consideration
Ethical approval for the study was obtained from the Research Ethics Committee of the UNTH.
Results
Prevalence of preterm births
There were 3,760 live births over the 5-year study period out of which 636 involved preterm deliveries giving a preterm birth rate of 16.9% (169 preterm births per 1,000 live births). The records of 592 preterm births were available and were analyzed. Overall, spontaneous preterm births occurred in approximately 57% of preterm births while provider-initiated births occurred in 43%. Preterm premature rupture of membranes preceded delivery in 15.2% (91/592) of preterm births. Table 1 shows the yearly distribution of preterm births. The preterm birth rate increased from 9.8% in 2009 to 17.1% in 2013 after peaking at 23% in 2012. Figure 1 is a line graph to illustrate the trends in the preterm birth rates while Figure 2 is a stacked bar chart showing the trend in the proportion of preterm births due to provider-initiated births. The proportion of preterm births due to provider-initiated births increased about 4-fold between 2009 and 2013.
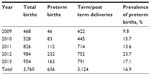  | Table 1 Yearly distribution of births at the University of Nigeria Teaching Hospital, Enugu, from 2009–2013 |
  | Figure 1 Trend in the prevalence of preterm births at University of Nigeria Teaching Hospital, Enugu, 2009–2013. |
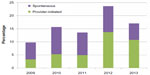  | Figure 2 Trend in the proportion of preterm births due to provider-initiated births among preterm births at the University of Nigeria Teaching Hospital, Enugu, 2009–2013. |
Pattern of preterm births
Table 2 shows the characteristics of women who had preterm deliveries. The mean age of mothers of preterm babies was 30.3±5.3 years and mean parity was 2.6±1.8. The mean postpartum blood loss was 363.1±279.1 mL (range 50–2,000 mL).
  | Table 2 Characteristics of women who delivered premature babies from 2009–2013 at the University of Nigeria Teaching Hospital, Enugu |
Table 3 summarizes the characteristics of preterm babies. The mean gestational age at preterm deliveries was 32.6±3.2 weeks while the mean birth weight was 2.0±0.8 kilograms. Approximately 89% of preterm births involved singleton pregnancies and 68% of preterm births were moderate to late preterm occurring from 32 weeks gestational age to 36 weeks, 6 days. The male:female ratio of preterm babies born during the period was 1.2:1. Approximately 69% of preterm babies had either low birth weight, very low birth weight, or extreme low birth weight. The distribution of the birth weights of preterm babies based on gestational age is shown in Table 4.
  | Table 3 Characteristics of preterm babies born at the University of Nigeria Teaching Hospital, Enugu, from 2009-2013 |
  | Table 4 Distribution of birth weights of premature babies according to gestational age of birth at the University of Nigeria Teaching Hospital, Enugu, from 2009-2013 |
Perinatal mortality associated with preterm births
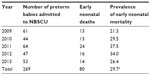
There were 149 stillbirths during the study period while 87 early neonatal deaths occurred among 363 preterm babies admitted to the NBSCU. The adjusted perinatal mortality rate was 46.1% (236/512) of total births.
Stillbirths
The stillbirth rate for preterm deliveries was 22.0% (149/678) of total births. Fresh stillbirth occurred in 86% (128/149) of stillbirths. Approximately 26% of singleton deliveries were still-born compared to 22% of twins. Table 5 shows the distribution of stillbirths according to gestational ages. There were no stillbirths among triplets and quadruplet preterm births. Table 6 shows a bivariate analysis of sociodemographic factors associated with stillbirth. Year of study, gestational age group, birth weight group, mode of delivery, and appropriateness of weight in relation to gestational age were all significantly associated with preterm stillbirths. Table 7 summarizes the logistic regression model to determine factors that predicted preterm stillbirths. Only route of delivery and gestational age group had significant predictive effect. Compared to babies born between 32–36+6 weeks, babies born between 28–31+6 weeks were two-and-a-half times more likely to be stillborn, while babies born at less than 28 weeks were three times more likely to be stillborn. Similarly, compared to those born by cesarean section, those born vaginally were six times more likely to be stillborn.
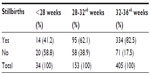  | Table 5 Distribution of stillbirths based on gestational age |
  | Table 6 Association of preterm stillbirth with maternal-fetal characteristics among preterm deliveries at University of Nigeria Teaching Hospital, Enugu, 2009–2013 |
Early neonatal deaths
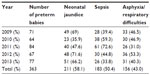
The early neonatal mortality rate for preterm babies born at the UNTH who were admitted to the NBSCU during the study period was 24.0% (87/363), and this excludes early neonatal mortality among preterm babies who were not admitted into the NBSCU. Table 8 shows the prevalence of early neonatal deaths among preterm babies during the study period. Approximately 86% (12/14) of liveborn extremely preterm babies died in the early neonatal period compared to 50.5% of very preterm babies (48/95). Table 9 shows the commonest complications of prematurity across the years of study. Jaundice (58.1%), sepsis (50.4%), and respiratory difficulties (43.0%) were the commonest complications of preterm births among preterm babies admitted to the NBSCU.
Discussion
A hospital-based maternity review of preterm deliveries was an appropriate study design to determine the prevalence and trend of preterm births and perinatal deaths: a population-based register of preterm births and stillbirths does not exist in our area. Studies based on admissions to newborn intensive care units would have excluded stillbirths and preterm births that did not require intensive care admissions: estimates from such studies would hardly be representative of all preterm births. In another vein, among the few maternity-based studies on preterm births in Nigeria, most addressed determinants of preterm births: we found no study which evaluated perinatal mortality associated with preterm births.18–21 This is the first study on the perinatal mortality associated with preterm births in this city.
Our study showed that the prevalence of preterm births during the study period was higher than the 12% reported by Mokuolu et al at Ilorin, Nigeria19 and the 8.5% reported by Etuk et al from Calabar, Nigeria.21 It is also higher than the less than 15% national preterm birth rate estimated by the WHO for Nigeria in the “Born Too Soon” report.6 The higher incidence rate recorded in this study compared to the two hospital-based studies from other parts of Nigeria may be due to differences in study design. Despite the fact that these studies were also based on maternity ward deliveries, the study in Calabar focused on factors influencing the incidence of preterm births and detailed characterization of preterm births was not given: it was therefore difficult to determine whether the study included multiple births. The study by Mokuolu et al19 was a prospective study of a very short duration of 9 months: it was also not reported whether multiple pregnancies were included or not. The discrepancy between our report and the WHO quoted national prevalence of preterm births in Nigeria may be due to the hospital-based nature of this study, which was likely to reflect referral bias.
This study also found a rising trend in the prevalence of preterm births during the study period. Although we found no previous study on the trends in preterm deliveries in Nigeria, the rising trend suggested by this study is in line with the global trend reported by the WHO on the incidence of preterm births.17 Besides, although the study showed rises in both spontaneous and provider-initiated preterm births, it was striking that there was a much greater increase in the provider-initiated preterm births. This rise in provider-initiated preterm births could be a reflection of an emerging trend in obstetric care in the hospital. The recent upgrading of the NBSCU of the hospital which resulted in increased capacity to salvage preterm babies may have given obstetricians greater confidence in initiating preterm births as a way of managing obstetric cases with high risk of intrauterine fetal death.
The high and rising trend in preterm births in this study contrasts with the pattern in the industrialized world. A recent report from Europe showed that many countries maintained or had reduced rates of singleton preterm births over the last 15 years, thereby challenging the widespread belief that preterm birth rates are rising globally.22 And although the US has incidence rates of preterm births in double digits like most developing countries, the rates are lower than in most developing countries and a steady decline in the incidence of preterm births in the US has been reported in the last 5 years.23
This study also found a high perinatal mortality rate which was almost twice the rate obtained in a study of perinatal mortality rate among the general pediatric population in the same hospital 7 years ago.24 Although the complications of prematurity would be expected to worsen perinatal mortality among preterm babies, the high perinatal mortality rate in this study underlies the enormity of human wastage associated with preterm births in developing countries. In contrast, recent reports from the UK suggest a rise in the survival of preterm babies.25
With respect to preterm stillbirths, this study found a stillbirth rate that was much higher than the 17.3% global stillbirth rate among preterm babies in the WHO “Born Too Soon” report.6 Although the high stillbirth rate in this study may be due to referral bias or the hospital-based design of this study, it draws attention to the need to take a closer look at stillbirths in this area. The authors found no study on preterm stillbirths in this area. Such a study is now needed to determine the possible modifiable factors promoting stillbirths. This will facilitate any intervention to minimize the occurrence of preterm stillbirths in this area. The fact that the odds of preterm stillbirth in this study increased with decreasing gestational age and with vaginal deliveries may be due to the fact that complications that are incompatible with life are likely to lead to fetal demise before term and the fact that obstetricians are more likely to allow vaginal birth for intrauterine fetal death or in situations where fetal survival after delivery was unlikely.
Another finding in this study is the proportion of preterm babies (6%) born before 28 weeks with signs of life. This could be one more reason why improvement in newborn intensive care units is urgently needed to facilitate the salvage of these babies. Besides, with the improvement in the salvage rate of preterm babies, this finding may indicate a foreseeable need to lower the legal definition of what constitutes birth as opposed to miscarriage in Nigeria. This is because sticking to 28 weeks may no longer be tenable with increasing birth and survival of babies born before 28 weeks gestational age.
The strengths of this study include the use of comprehensive hospital delivery data, as opposed to newborn admissions only for the determination of the prevalence of preterm births. The weaknesses include the hospital-based nature of the study in a country where most deliveries occur outside of health facilities. This may suggest that the prevalence rate of preterm deliveries could be substantially different from the prevalence in the general population. The fact that complicated obstetric cases are referred to this hospital could lead to a referral bias leading to over-estimation of preterm births and deaths.
We conclude that this study found a higher than the national average in the prevalence of preterm births and stillbirths, yielding a very high perinatal mortality rate among preterm births. These may, in part, be a reflection of suboptimal prenatal and newborn care. An urgent improvement in prenatal and newborn care is therefore needed in the study center in order to improve the capacity to prevent or abate preterm labor, and preterm premature rupture of membranes; and to reduce stillbirths from treatable causes such as malaria and bacterial infections. Further upgrading of personnel and facilities in the NBSCU is also required to minimize early neonatal deaths.
Disclosure
The authors have no conflict of interest in this study.
References
Oloyede OAO. Specialized antenatal clinics for women with a pregnancy at high risk of preterm birth (excluding multiple pregnancy) to improve maternal and infant outcomes. RHL The WHO Reproductive Health Library; Geneva: World Health Organisation. | |
Simmons LE, Rubens CE, Darmstadt GL, Gravett MG. Preventing preterm birth and neonatal mortality: Exploring the epidemiology, causes, and interventions. Semin Perinatol. 2010;34(6):408–415. | |
Lumley J. Defining the problem: the epidemiology of preterm birth. BJOG. 2003;110(Suppl 20):3–7. | |
Nkyekyer K, Enweonu-Laryea C, Boafor T. Singleton preterm births in Korle Bu Teaching Hospital, Accra, Ghana-origins and outcomes. Ghana Med J. 2006;40(3):93–98. | |
Vogee JP, Lee AC, Souza JP. Maternal morbidity and preterm birth in 22 low- and middle-income countries: a secondary analysis of the WHO global survey data set. BMC Pregnancy Childbirth. 2014;14:56. | |
Blencowe H, Cousens S, Chou D, et al. Born Too Soon: The global epidemiology of 15 million preterm births. Reprod Health. 2013; 10(Suppl 1):S2. | |
No authors listed. Delivery action on preterm births. Lancet. 2013; 382(9905):1610. | |
Lawn JE, Cousens S, Zupan J, Lancet Neonatal Survival Steering Team. 4 million neonatal deaths: When? Where? Why? Lancet. 2005;365(9462):891–900. | |
Beck S, Wojdyla D, Say L, et al. The worldwide incidence of preterm birth: a systematic review of maternal mortality and morbidity. Bull World Health Organ. 2010;88(1):31–38. | |
Bukar M, Geidam AD. Complications of unsafe abortion. In: Ebeigbe PN, editor. Foundations of Clinical Gynaecology in the Tropics. Benin City: Fodah Global Ultimate Limited; 2012:246–256. | |
Chang HH, Larson J, Blencowe H, et al. Preventing preterm births: trends and potential reductions with current interventions in 39 very high human development index countries. Lancet. 2013;381(9862):223–234. | |
Chiabi A, Mah EM, Mvondo N, et al. Risk factors for premature births: a cross-sectional analysis of hospital records in a Cameroonian health facility. Afr J Reprod Health. 2013;17(4):77–83. | |
Goldenberg RL, Culhane JF, Iams JD, Romero R. Epidemiology and causes of preterm birth. Lancet. 2008;371(9606):75–84. | |
Plunkett J, Muglia LJ. Genetic contributions to preterm birth: implications from epidemiological and genetic association studies. Ann Med. 2008;40(3):167–179. | |
Menon R. Spontaneous preterm birth, a clinical dilemma: etiologic, pathophysiologic and genetic heterogeneities and racial disparity. Acta Obstetrica Gynecol Scand. 2008;87(6):590–600. | |
Blencowe H, Cousens S, Oestergaard MZ, et al. National, regional and worldwide estimates of preterm birth rates in the year 2010 with time trends since1990 for selected countries: a systematic analysis and implication. Lancet. 2012;379(9832):2162–2172. | |
World Health Organization [homepage on the Internet]. Preterm birth Fact sheet No 363. Available from: http://www.who.int/mediacentre/factsheets/fs363/en/. Accessed September 10, 2014. | |
Onankpa BO, Isezuo K. Pattern of Preterm Delivery and Their Outcome in a Tertiary Hospital. International Journal of Health Sciences and Research. 2014;4(3):59–65. | |
Mokuolu OA, Suleiman BM, Adesiyun OO, Adeniyi A. Prevalence and determinants of pre-term deliveries in the University of Ilorin Teaching Hospital, Ilorin, Nigeria. Pediatr Rep. 2010;(1)2:e3. | |
Kunle-Olowu OE, Peterside O, Adeyemi OO. Prevalence and Outcome of Preterm admissions at the Neonatal Unit of a Tertiary Health Centre in Southern Nigeria. Open Journal of Pediatrics. 2014;4:67–75. | |
Etuk SJ, Etuk IS, Oyo-Ita AE. Factors influencing the incidence of pre-term birth in Calabar, Nigeria. Niger J Physiol Sci. 2005;20(1–2):63–68. | |
Zeitlin J, Szamotulska K, Drewniak N, et al. Preterm birth time trends in Europe: a study of 19 countries. BJOG. 2013;120(11):1356–1365. | |
March of Dimes Foundation. 2013 Premature Birth Report Card. Available from: http://www.marchofdimes.com/materials/premature-birth-report-card-united-states.pdf. Accessed June 30, 2014. | |
Adimora GN, Odetunde IO. Perinatal mortality in University of Nigeria Teaching Hospital (UNTH) Enugu at the end of the last millennium. Niger J Clin Pract. 2007;10(1):19–23. | |
Costeloe KL, Hennessy EM, Haider S, Stacey F, Marlow N, Draper ES. Short term outcomes after extreme preterm birth in England: comparison of two birth cohorts in 1995 and 2006 (the EPICure studies). BMJ. 2012;345:e7976. |
 © 2014 The Author(s). This work is published and licensed by Dove Medical Press Limited. The full terms of this license are available at https://www.dovepress.com/terms.php and incorporate the Creative Commons Attribution - Non Commercial (unported, v3.0) License.
By accessing the work you hereby accept the Terms. Non-commercial uses of the work are permitted without any further permission from Dove Medical Press Limited, provided the work is properly attributed. For permission for commercial use of this work, please see paragraphs 4.2 and 5 of our Terms.
© 2014 The Author(s). This work is published and licensed by Dove Medical Press Limited. The full terms of this license are available at https://www.dovepress.com/terms.php and incorporate the Creative Commons Attribution - Non Commercial (unported, v3.0) License.
By accessing the work you hereby accept the Terms. Non-commercial uses of the work are permitted without any further permission from Dove Medical Press Limited, provided the work is properly attributed. For permission for commercial use of this work, please see paragraphs 4.2 and 5 of our Terms.