Back to Journals » Psychology Research and Behavior Management » Volume 14
Prevalence and Associated Factors of Depression among Patients with HIV/AIDS in Lahore, Pakistan: Cross-Sectional Study
Authors Junaid K , Ali H , Khan AA, Khan TA, Khan AM, Khan A, Nazim R, Tahira K
Received 9 August 2020
Accepted for publication 13 October 2020
Published 3 February 2021 Volume 2021:14 Pages 77—84
DOI https://doi.org/10.2147/PRBM.S268099
Checked for plagiarism Yes
Review by Single anonymous peer review
Peer reviewer comments 2
Editor who approved publication: Professor Mei-Chun Cheung
Khunsa Junaid,1 Hassan Ali,2 Ali Akram Khan,3 Taimoor Akram Khan,4 Aabish Mehreen Khan,5 Amjad Khan,6 Rabia Nazim,7 Khadija Tahira8
1Department of Public Health, Institute of Social and Cultural Studies, University of Punjab, Lahore, Pakistan; 2Department of Public Health, Institute of Social and Cultural Studies, University of Punjab, Lahore, Pakistan; 3Department of Community Medicine, King Edward Medical University, Lahore, Pakistan; 4Department of Community Medicine, King Edward Medical University, Lahore, Pakistan; 5Department of Community Medicine, King Edward Medical University, Lahore, Pakistan; 6Department of Public Health, University of Haripur, Khyber Pakhtunkhwa, Pakistan; 7Department of Community Medicine, King Edward Medical University, Lahore, Pakistan; 8Department of Public Health, Institute of Social and Cultural Studies, University of Punjab, Lahore, Pakistan
Correspondence: Khunsa Junaid
Department of Public Health, Institute of Social and Cultural Studies, University of Punjab, Lahore, 75500, Pakistan
Email [email protected]
Background: Depression is defined as a psychiatric disorder characterized by depressed mood, lack of concentration, diminished energy, disturbed sleep, and low self-esteem. Depression is more prevalent in HIV/AIDS patients than the general population. There is no published study available that reveals the present status of depression among HIV patients in Pakistan. As such, the present study was conducted to determine the prevalence and associated factors of depression among HIV/AIDS patients attending the HIV clinic of Jinnah Hospital, Lahore, Pakistan.
Methods: A hospital-based cross-sectional study was carried out from February to March 2019 in Lahore. Data were collected from 158 HIV/AIDS patients using a pretested, standardized, structured interviewer-administered questionnaire. Nonprobability convenience sampling was used to recruit the study participants. Depression was evaluated using the Patient Health Questionnaire. SPSS version 23 was used to analyze the data. Binary logistic regression models were used to determine the various factors associated with depression. AORs with 95% CIs were used to assess the magnitude of associations between depression and associated factors.
Results: The mean age of the study participants was 35.03 years± 9.123. Prevalence of depression among HIV/AIDS patients was 32.2%. Living in a rural area (AOR 5.60, 95% CI 2.20, 14.15), fear of stigma and discrimination (AOR 3.505, 95% CI 1.364, 9.008), having worked abroad (AOR 3.017, 95% CI 1.134, 8.031), and history of substance abuse (AOR 4.147, 95% CI 1.673, 10.28) were significantly associated with depression.
Conclusion: The prevalence of depression among HIV/AIDS patients is very high in Pakistan. Therefore, it is suggested that guidelines formulated to screen and treat depression among HIV patients.
Keywords: depression, HIV/AIDS, convenience sampling, PHQ9 scale
Introduction
HIV is one of the most common causes of death and disability, particularly in low- and middle-income countries.1 According to a Joint United Nations Programme on HIV/AIDS 2020 report, approximately 38.9 million people were living with HIV, 25.4 million accessing antiretroviral therapy (ART), 1.7 million had recently become infected with HIV, and 690,000 had died due to AIDS-related illnesses worldwide.2 In Pakistan, a national HIV/AIDS-control program was launched in 1987, but since then HIV/AIDS cases have been increasing rapidly. By 2018, 160,000 people were living with HIV/AIDS in Pakistan, and among these only 10% were receiving ART.3 Increasing access to ART for people suffering from HIV/AIDS has resulted in a variety of benefits, such as delay in HIV-disease progression, prolonging life expectancy, and improving quality of life and mental well-being.4
Individuals with chronic health problems are at increased risk of detrimental mental health issues. Depression is common nowadays, affecting more than 350 million people worldwide. Globally, depression is the fourth–most important cause of disability, and its lifetime prevalence is about 3%–17%.5,6 Depression is defined as a psychiatric disorder characterized by depressed mood, lack of concentration, diminished energy, low self-esteem, disturbed sleep, low desire for food, and poor attentiveness. This interferes with everyday life and reduces the standard of living.5
The current evidence highlights that people who are infected with HIV/AIDS have increased prevalence of depression compared to the general population.7 According to recent data, there are approximately 121 million HIV/AIDS-infected individuals affected by depression globally.8 Studies carried out in various countries on the prevalence of depression among HIV-infected patients showed 29.4% prevalence in Brazil,9 18.6% in India,10 48.6% in Ethiopia,11 53.8% in South Africa,12 and 71.9% in China.13 Mental health issues associated with HIV/AIDS decrease the likelihood of receiving ART and deteriorate ART compliance, resulting in increased viral load and decreased CD4 cell count.5,7 Depression affects an individual’s capability to adhere to treatment for HIV/AIDS, resulting in reduced compliance with ART and HIV/AIDS disease progression.13,14 Various sociodemographic and clinical factors, such as low income, being female, poor compliance with ART, multiple visits for clinical appointments in a month, low educational status, age (40–49 years), and HIV/AIDS stage III and IV are significantly associated with depression among HIV-positive patients.6,10,11
Based on diverse study findings, the prevalence of depressive symptoms among people living with HIV/AIDS is very high. Therefore, it is necessary to recognize depression in HIV- infected patients for appropriate and well-timed management. Distressingly, in Pakistan medical services for HIV/AIDS patients focus mainly on physical symptoms of the disease and frequently overlook psychological symptoms, and consequently depression remains undiagnosed and undertreated. This is because of the fact that potential mental health services are not incorporated into the ART-services program. Very few studies regarding assessment of depression among HIV-infected patients in South Asia have been done. There have been no studies revealing the present status of depression among HIV-infected patients in Pakistan. As such, this study aimed to determine prevalence and associated factors of depression among HIV-infected patients attending the HIV clinic of Jinnah Hospital, Lahore, Pakistan. Results from this study will provide information for formulating and incorporating empirically based mental health–promotion and mental health disease–prevention programs.
Methods
Study Design, Setting, and Period
A hospital-based analytical cross-sectional study was conducted from February to March 2019 at Jinnah Hospital, Lahore. This HIV clinic operates from Monday to Saturday and serves approximately 15–20 patients per day.
Study Participants
The study population consisted of male and female HIV-infected patients aged ≥18 years, were positive on ELISA for HIV antibodies, had received ART, had the ability to speak Urdu (national language of Pakistan) or English, had soundness of mind, and were willing to be included in the study. HIV-infected patients who were critically ill, had head trauma, or had other medical diseases unrelated to HIV, such as malignancy, renal failure, and chronic hepatitis, determined on clinical examination were excluded from the study.
Sample Size and Sampling Technique
The sample size was calculated by using a single population–proportion formula 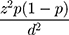 . Considering the estimated prevalence of depression among HIV-infected patients to be 18.6%10 with a 6% margin of error at 95% confidence, the final sample size calculatedwas 158. Nonprobability convenience sampling was used for this study.
. Considering the estimated prevalence of depression among HIV-infected patients to be 18.6%10 with a 6% margin of error at 95% confidence, the final sample size calculatedwas 158. Nonprobability convenience sampling was used for this study.
Data Collection and Instruments
Data were collected using a pretested structured interviewer-administered questionnaire, which contained four parts. The first part consisted of sociodemographic characteristics (age, occupation, sex, education, marital status, monthly family income, residential status, and religion), and the second part consisted of clinical and psychosocial characteristics of HIV-infected patients (disclosure of HIV status, availability of a social support network, HIV/AIDS stage, fear of stigma and discrimination, having worked abroad, CD4 cell count (cells/mm3), family history of depression, history of substance abuse, risk factors for HIV transmission, and history of psychiatric illness). The third part of the questionnaire consisted of a modified four-item version of the Simplified Medication Adherence Questionnaire (SMAQ), which was used to quantify medication nonadherence. The scoring plan of the four-item SMAQ was yes = 1 and no = 0. To present a range of scores of 0–4, scores on the SMAQ were summed.15 For the purposes of data analysis, total scores were dichotomized, with scores 1–4 representing nonadherence to medication and a score of 0 adherence to medication.
The fourth part of the questionnaire was the Patient Health Questionnaire (PHQ9), which was used to assess the presence of depression among HIV-infected patients. This uses a Likert-like scale consisting of nine questions about signs and symptoms that are categorized into four response options ranging from 0 (not at all) to 3 (nearly every day), with a total score ranging from 0 to 27 points. A total score ≤4 was considered normal, 5–9 mild depression, 10–14 moderate depression, 15–19 moderately severe depression, and 20–27 severe depression.11,14 The PHQ9 is commonly used to screen symptoms of depression in health-care settings in Pakistan. The scale uses a cutoff score of ≥10 for diagnosis of depression. In the current study, PHQ9 scores were further dichotomized into ≤10 (absence of depression) and ≥10 (presence of depression). A study conducted in Pakistan showed sensitivity and specificity of the PHQ9 with a cutoff of ≥10 to be 94.7% and 88.9%, respectively.16
Data Processing and Analysis
SPSS version 23 was used to analyze the data. Means ± SD were calculated for continuous data, and frequency summaries (counts and percentages) and χ2 tests for categorical data. To identify the association between each independent variable and outcome variable, binary logistic regression was performed. Variables that showed significant association on binary logistic regression based on p-value (≤0.20) were selected for inclusion in multivariate binary logistic regression analysis using the backward stepwise method to control for possible effects of confounders. Goodness of fit for the final model was assessed using the Hosmer–Lemeshow test. All statistical tests performed were two-tailed, and p<0.05 was considered statistically significant. AORs with 95% CIs were calculated to find magnitude of associations. AORs that did not include the value 1 in the 95% CI were considered statistically significant.
Ethical Considerations
Ethical clearance was obtained from the local Ethics Committee of Jinnah Hospital, Lahore (code 46th/ERB). The current study also followed the Declaration of Helsinki’s ethical principles for medical research involving human subjects. An approval letter for data collection was also obtained from the project director of the Punjab AIDS Control Program, Lahore. Patients were informed about the purpose, procedure, risks, and benefits of the study and assured about the confidentiality of the data. We obtained informed verbal consent for each participant before data collection. The process for obtaining informed verbal consent was approved by the Ethics Committee of Jinnah Hospital. Patients were also given the option to withdraw from the study at any point during the interview if they did not feel comfortable with proceeding. Codes were used in place of names and other identifying information.
Results
Sociodemographic Characteristics
A total of 158 study participants were included in the study. The mean±SD age of the respondents was 35.03±9.123 years. Among the participants, 95 (60.1%) HIV-infected patients were aged <40 years, 139 (88.0%) were male, 89 (56.3%) were illiterate, 93 (58.9%) were married, 101 (63.9%) were employed, 83 (52.5%) had a monthly family income <Rs20,000, 97 (61.4%) were living in urban regions, and 151 (95.6%) were Muslims (Table 1).
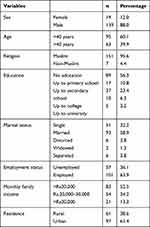 |
Table 1 Sociodemographic Characteristics of HIV-Infected Patients (n=158) |
Prevalence of Depression
Depressive symptoms were measured using the PHQ9. Based on the cutoff point of ≥10, the overall prevalence of depression was 51 (32.2%). Regarding severity of depression, 30 (18.9%) participants had moderate depression (PHQ9 score 10–14), nine (5.69%) moderately severe depression (PHQ9 score 15–19), and 12 (7.59%) severe depression (PHQ9 score 20–27).
Clinical and Psychosocial Characteristics
Among the 158 study participants, 77 (48.7%) had not disclosed their HIV status, 61 (38.6%) had a social support network, and 99 (62.7%) had a fear of stigma and discrimination in the community. In addition, 112 (70.9%) had stage I HIV/AIDS, 38 (24.1%) had worked abroad, 77 (48.7%) had CD4 cell counts <500 cells/mm3, 63 (39.9%) had no family history of depression, and 89 (56.3%) had a history of substance abuse. The results of the present study also revealed that 112 (70.9%) study participants were nonadherent to treatment and only 46 (29.1%) adherent. A large proportion of participants were heterosexual (64, 40.9%) and intravenous drug users 62, 39.2%). Only 49 (31.0%) participants had a history of psychiatric illness (Table 2).
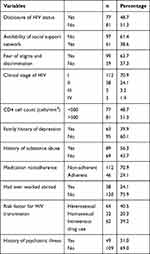 |
Table 2 Frequency Distribution of Clinical and Psychosocial Characteristics of HIV Patients (n=158) |
The results of the present study revealed that there was a statistically significant association between non-adherence to HIV medication and depression (p=0.001, Table 3).
 |
Table 3 Prevalence of Depression Among HIV Patients by Medication Nonadherence (n=158) |
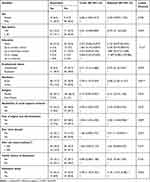 |
Table 4 Factors Associated with Depression Among HIV Patients (n=158) |
Factors Associated with Depression
Sex, age, education, employment status, residence, religion, availability of social support, fear of stigma and discrimination, having worked abroad, CD4 cell count, family history of depression, and substance abuse that fulfilled the criterion of p≤0.20 significance level on bivariate logistic regression analysis were considered for multivariate logistic regression analysis. After adjustment for all confounders, rural residence, fear of stigma and discrimination, having worked abroad, and history of substance abuse were significantly associated with depression (p<0.05).
The odds of developing depression among HIV-infected patients living in rural areas were 5.60 times those of HIV-infected patients living in urban areas (AOR 5.60,95% CI 2.20–14.15). The odds of developing depression were high among HIV-infected patients with a history of fear of stigma and discrimination in the community compared to those without a history of fear of stigma and discrimination in the community (AOR 3.505, 95% CI 1.364–9.008). The odds of developing depression were also high among HIV-infected patients with a history of working abroad than those without history of working abroad (AOR 3.017, 95% CI 1.134–8.031). The odds of developing depression among HIV-infected patients with a history of substance abuse were 4.14 times those of HIV-infected patients without history of substance abuse (AOR 4.147, 95% CI 1.673–10.28) (Table 4).
Discussion
This hospital-based cross-sectional study was carried out to evaluate prevalence and associated factors of depression among HIV-infected patients at Jinnah Hospital, Lahore using the PHQ9. The overall prevalence of depression among HIV-infected patients was 32.2%. Studies conducted at Ethiopia, South Africa, and China have reported prevalence of 48.6%, 53.8%, and 71.9%, respectively, among HIV-infected patients.11–13 On the other hand, studies conducted in Botswana, Brazil, and India have reported lower prevalence, ie, 31.4%, 29.4%, and 18.6%, respectively.9,10,17 Possible causes for this discrepancy may be variation in study design, sociocultural factors, sample size, and difference in depression-diagnosis tools.
The results of the present study revealed that there was a statistically significant association between HIV-medication nonadherence and depression on bivariate χ2 analysis. This finding is in line with another study conducted in India.10 The reason for this is that poor adherence to ART worsens quality of life among HIV-infected patients and consequently results in poor mental health. Additionally, timely recognition and management of depression goes a long way in enhancing the quality of life of HIV-infected patients. However, the association between HIV-medication nonadherence and depression lost its significance on multivariate regression analysis. Depression was found to be significantly associated with age. This finding is in line with the study in Ethiopia.11 In the current study, depression was also found to be significantly associated with employment status. As employment helps in income production and leads to social sustainability, economic growth, and a sense of self-worth in a person, that is why various other studies have also reported depression more common among unemployed patients.10,17
The odds of developing depression among HIV-infected patients living in rural areas were higher than HIV-infected patients living in urban areas. This finding is in line with the studies in Botswana and India.10,17 Individuals residing in rural areas belong to lower socioeconomic classes and do not have the availability of high-quality medical services that affect an individual’s psychological state. In our study, patients with a history of fear of stigma and discrimination in the community developed depressive symptoms more frequently than those without. This finding is similar to results of previous studies conducted in South Africa and Ethiopia.8,11 It may be noted that having HIV, which is a persistent long-term illness, is likely to increase levels of stigma, disgrace, and discrimination in society, and thus HIV-infected patients may prefer to live alone to avoid social stigma that leads to increased depressive symptoms.
The odds of developing depression were higher among those patients who had a history of substance abuse. This finding is consistent with those of studies carried out in Ethiopia.6,11 This may be because HIV-infected patients take up substance abuse to deal with distress and stigma related to HIV. Substance abuse in turn leads to depression and worsens the condition. Removal of dependence on substance abuse needs active interventions at various levels. In our study, the odds of developing depression were also high among those patients who had a history of working abroad. This finding is similar to those of previous studies conducted in India.18,19 This may be due to the fact that HIV-infected patients living outside their motherland feel more lonely because of lack of family and social support, which are very important in an illness like HIV/AIDS.
Strengths and Limitations
To the best of our knowledge, this is first study conducted in Lahore, Pakistan to highlight the presence of depression among HIV-infected patients using the PHQ9 and describe the various factors associated with depression. Another strength of the present study is a single observer (the self), which excludes observer bias. The measurement of depression had high construct validity, because a well-validated instrument was used. There are a few limitations that should be considered when interpreting the findings. Because of the small sample and collection of data from a single HIV center in Lahore, we cannot generalize its results to the whole population. Another limitation might have been interviewer administration of the PHQ9, as the patients may have been unwilling to describe mental health issues to an interviewer because of dread of stigmatization. Furthermore, due to the cross-sectional nature of the study design, we were not able to find a cause–effect relationship.
Conclusion
The prevalence of depressive symptoms among HIV-infected patients is high in Lahore, Pakistan — 32.2%. Rural residence, fear of stigma and discrimination, history of substance abuse, having worked abroad, age, and employment status were the most significant factors associated with depression among HIV-infected patients. Moreover, depression among HIV-positive patients remains underdiagnosed and undertreated and needs additional research. Therefore, the Ministry of Health should give more attention to HIV-infected patients with depressive symptoms and formulate guidelines to screen and treat depression. Additional research on risk factors of depression and anxiety should be carried out to reinforce and broaden these findings.
Data-Sharing Statement
The data sets used and/or analyzed during the current study can be obtained from the corresponding author on a reasonable request.
Acknowledgments
The authors would like to thank the study participants and facilitators who made the study possible. The authors received no support or funding for this report.
Disclosure
The authors report no conflicts of interest in this work.
References
1. Organization WH. HIV/AIDS and Mental Health: 2009. World Health Organization; 2008.
2. The global AIDS & HIVS statistics: 2020 fact sheet. United Nation Acquired Immunodeficiency Syndrome (UNAIDS) Website. Available from: https://www.unaids.org/en/resources/fact-sheet.Accessed.
3. The Pakistan AIDS & HIVS statistics: 2019 factsheet. United Nation Acquired Immunodeficiency Syndrome (UNAIDS) Website. Available from: https://www.unaids.org/en/regionscountries/countries/pakistan.
4. Ford N, Migone C, Calmy A, et al. Benefits and risks of rapid initiation of antiretroviral therapy. AIDS. 2018;32(1):17–23. doi:10.1097/QAD.0000000000001671
5. Organization WH. Mental Health Action Plan 2013–2020: 2013 Update. World Health Organization; 2013.
6. Tesfaw G, Ayano G, Awoke T, et al. Prevalence and correlates of depression and anxiety among patients with HIV on-follow up at Alert Hospital, Addis Ababa, Ethiopia. BMC Psychiatry. 2016;16(1):368. doi:10.1186/s12888-016-1037-9
7. L’akoa RM, Noubiap JJ, Fang Y, Ntone FE, Kuaban C. Prevalence and correlates of depressive symptoms in HIV-positive patients: a cross-sectional study among newly diagnosed patients in Yaoundé, Cameroon. BMC Psychiatry. 2013;13(1):228. doi:10.1186/1471-244X-13-228
8. Pappin M, Edwin Wouters E, Booysen F. Anxiety and depression amongst patients enrolled in a public sector anti retroviral treatment programme in South Africa: a cross-sectional study. BMC Public Health. 2012;12(1):244. doi:10.1186/1471-2458-12-244
9. Castrighini C, Gir E, Neves L, Reis R, Galvão M, Hayashido M. Depression and self-esteem of patients positive for HIV/AIDS in an inland city of Brazil. Retro Virol. 2010;7(Suppl 1):66.
10. Shukla M, Agarwal M, Singh JV, Tripathi AK, Srivastava AK, Singh VK. Predictors of depression among people living with HIV/AIDS on antiretroviral therapy attending tertiary care hospitals in the Capital of Uttar Pradesh: A cross-sectional study. Indian J Soc Psychiatry. 2017;33(1):159–164. doi:10.4103/0971-9962.209200
11. Duko B, Geja E, Zewude M, Mekonen S. Prevalence and associated factors of depression among patients with HIV/AIDS in Hawassa, Ethiopia, cross-sectional study. Ann Gen Psychiatry. 2018;17(1):45. doi:10.1186/s12991-018-0215-1
12. Van Copenhagen B, Duvenage HS. Prevalence of depression in people living with HIV and AIDS at the kalafong provincial tertiary hospital antiretroviral clinics. Afr J Psychiatr. 2019;25(1):1175. doi:10.4102/sajpsychiatry.v25i0
13. Su X, Lau J, Mak W, et al. Prevalence and associated factors of depression among people living with HIV in two cities in China. J Affect Disord. 2013;149(1–3):108–115. doi:10.1016/j.jad.2013.01.011
14. Eshetu DA, Woldeyohannes SM, Alemayehu M, Techane GN, Tegegne MT, Dagne K. Prevalence of depression and associated factors among HIV/AIDS Patients attending ART Clinic at Debrebirhan referral hospital, North Showa, Amhara Region, Ethiopia. Am J Community Psychol. 2014;2(6):101–108.
15. Knobel H, Alonso J, Casado J, et al. Validation of a simplified medication adherence questionnaire in a large cohort of HIV-infected patients: the GEEMA Study. AIDS. 2002;16(4):605–613. doi:10.1097/00002030-200203080-00012
16. Gallis JA, Maselko J, O’Donnell K, et al. Criterion-related validity and reliability of the Urdu version of the patient health questionnaire in a sample of community-based pregnant women in Pakistan. PeerJ. 2018;6(1):e5185. doi:10.7717/peerj.5185
17. Gupta R, Dandu M, Packel L, et al. Depression and HIV in Botswana: a population-based study on gender-specific socio economic and behavioral correlates. PLoS One. 2010;5(1):e14252. doi:10.1371/journal.pone.0014252.t001
18. Bhatia MS, Munjal S. Prevalence of depression in people living with HIV/AIDS undergoing ART and factors associated with it. J Clin Diagn Res. 2014;8(10):1–4. doi:10.7860/JCDR/2014/7725.4927
19. Rueda S, Mitra S, Chen S, et al. Examining the associations between HIV-related stigma and health outcomes in people living with HIV/AIDS: a series of meta-analyses. BMJ Open. 2016;6(7):e011453. doi:10.1136/bmjopen-2016-011453
 © 2021 The Author(s). This work is published and licensed by Dove Medical Press Limited. The full terms of this license are available at https://www.dovepress.com/terms.php and incorporate the Creative Commons Attribution - Non Commercial (unported, v3.0) License.
By accessing the work you hereby accept the Terms. Non-commercial uses of the work are permitted without any further permission from Dove Medical Press Limited, provided the work is properly attributed. For permission for commercial use of this work, please see paragraphs 4.2 and 5 of our Terms.
© 2021 The Author(s). This work is published and licensed by Dove Medical Press Limited. The full terms of this license are available at https://www.dovepress.com/terms.php and incorporate the Creative Commons Attribution - Non Commercial (unported, v3.0) License.
By accessing the work you hereby accept the Terms. Non-commercial uses of the work are permitted without any further permission from Dove Medical Press Limited, provided the work is properly attributed. For permission for commercial use of this work, please see paragraphs 4.2 and 5 of our Terms.
