Back to Journals » Neuropsychiatric Disease and Treatment » Volume 11
Predictors of premature discontinuation of outpatient treatment after discharge of patients with posttraumatic stress disorder
Authors Wang HR, Woo YS, Jun T, Bahk W
Received 26 November 2014
Accepted for publication 6 January 2015
Published 20 March 2015 Volume 2015:11 Pages 787—792
DOI https://doi.org/10.2147/NDT.S78212
Checked for plagiarism Yes
Review by Single anonymous peer review
Peer reviewer comments 3
Editor who approved publication: Professor Wai Kwong Tang
Hee Ryung Wang, Young Sup Woo, Tae-Youn Jun, Won-Myong Bahk
Department of Psychiatry, College of Medicine, The Catholic University of Korea, Seoul, Korea
Objective: This study aimed to examine the sociodemographic and disease-related variables associated with the premature discontinuation of psychiatric outpatient treatment after discharge among patients with noncombat-related posttraumatic stress disorder.
Methods: We retrospectively reviewed the medical records of patients who were discharged with a diagnosis of posttraumatic stress disorder.
Results: Fifty-five percent of subjects (57/104) prematurely discontinued outpatient treatment within 6 months of discharge. Comparing sociodemographic variables between the 6-month non-follow-up group and 6-month follow-up group, there were no variables that differed between the two groups. However, comparing disease-related variables, the 6-month follow-up group showed a longer hospitalization duration and higher Global Assessment of Function score at discharge. The logistic regression analysis showed that a shorter duration of hospitalization predicted premature discontinuation of outpatient treatment within 6 months of discharge.
Conclusion: The duration of psychiatric hospitalization for posttraumatic stress disorder appeared to influence the premature discontinuation of outpatient treatment after discharge.
Keywords: posttraumatic stress disorder, discontinuation, compliance, predictor
Introduction
Posttraumatic stress disorder (PTSD) is a common psychiatric disorder that is characterized by re-experience, hyperarousal, and avoidance.1 It has long been categorized as an anxiety disorder, however, in the fifth edition of the Diagnostic and Statistical Manual of Mental Disorders (DSM-5), it was included under a new classification termed, “Trauma- and Stressor-Related Dsiorder”.1 It is well known that PTSD is associated with significant social, interpersonal, and occupational problems.2,3 PTSD is also associated with a chronic course and a high rate of psychiatric and medical comorbidities.2,4
Since the introduction of selective serotonin reuptake inhibitors, their efficacy for the treatment of PTSD has been well demonstrated in many studies.2,5,6 In addition, newer treatment strategies including atypical antipsychotic agents have also been shown to be effective in various clinical trials.7–9 Despite this advance in pharmacotherapy for PTSD, poor treatment adherence to pharmacotherapy for PTSD is a critical issue that psychiatrists continue to face in clinical practice.10,11
Premature discontinuation of pharmacotherapy for PTSD has been associated with increased relapse rates12,13 and poor psychosocial outcomes, such as symptom aggravation, increased mortality, and increased health care use.14,15 Thus, treatment guidelines recommend medication therapy for PTSD for 6 to 12 months.1,16,17
So far, relatively few studies have investigated the predictors for treatment adherence or premature treatment discontinuation for this population compared to other psychiatric populations, such as those with major depressive disorder, bipolar disorder or schizophrenia.10,18 Furthermore, the majority of studies regarding treatment adherence among the PTSD population has focused on combat-related PTSD.19–23 Several studies have shown that combat-related PTSD differs from noncombat-related PTSD in treatment response and disease-related characteristics.24–30 Thus, we aimed to evaluate the predictors of premature discontinuation of psychiatric outpatient treatment after discharge from psychiatric hospitalization for noncombat-related PTSD using a retrospective chart review.
Methods
Study population
Subjects were patients who were diagnosed with PTSD based on the DSM-IV31 and discharged after psychiatric inpatient treatment at the Department of Psychiatry, Yeouido St Mary’s Hospital from 2003 to 2012. Subjects who were admitted for a legal psychiatric evaluation and not for treatment for PTSD were excluded. Those who were referred to another hospital within a year after discharge and those who participated in clinical trials during the 1-year period after discharge were also excluded. This study was approved by the Institutional Review Board of Yeouido St Mary’s Hospital in Korea. Informed consent was waived by the Institutional Review Board because this study was a retrospective chart review study.
Study methods
A retrospective chart review of the medical records of the PTSD patients who met the selection criteria was performed. We divided patients into the “6-month follow-up group” and the “6-month non-follow-up group” according to whether they regularly attended scheduled outpatient appointments for more than 6 months after discharge at least bi-monthly, or not. We defined “regular attendance to the scheduled outpatient appointments” as attending the outpatient clinic within 15 days of scheduled appointments calculated based on the number of days of the last prescription.
Two authors (HRW and WMB) independently extracted data on disease-related and sociodemographic variables from retrospective chart reviews using a predefined data extraction form. Sociodemographic variables examined were sex, age, occupation, educational years, socioeconomic status, and marital status. Disease-related variables investigated were duration of PTSD, age at first onset, duration of index hospitalization, family history of psychiatric disease, type of admission, number of previous hospitalizations for psychiatric conditions, a history of previous psychiatric treatment within 3 months prior to index hospitalization, Global Assessment of Function (GAF) scores32 at admission and at discharge, and treatment pattern prescribed at discharge.
Data analysis
Sociodemographic variables and disease-related variables were compared between the 6-month follow-up group and the 6-month non-follow-up group. For continuous variables, independent t-tests were used to analyze the differences between the two groups. For categorical variables, chi-square statistics were used. Multivariable logistic regression analysis was carried out to identify predictors of premature discontinuation of outpatient treatment. All tests used were two-tailed, and a P-value that was lower than 0.05 was considered statistically significant. Two authors (WMB and HRW) conducted data analysis using the Statistical Package for the Social Sciences (SPSS) software.
Results
Differences in sociodemographic variables between the 6-month follow-up group and the 6-month non-follow-up group
A total of 104 patients met the selection criteria and were included in the analysis. All patients had noncombat-related PTSD and 92 developed PTSD symptoms after traffic accidents. Among the 104 patients, 57 (54.8%) prematurely discontinued their outpatient treatment within 6 months after discharge. By comparing sociodemographic variables, no variables were found to differ between the two groups (Table 1).
  | Table 1 Differences in sociodemographic variables between the 6-month follow-up group and the 6-month non-follow-up group |
Differences in disease-related variables between the 6-month follow-up group and the 6-month non-follow-up group
The 6-month follow-up group showed a longer duration of index hospitalization than the 6-months non-follow-up group (37.3±23.6 days vs 27.0±17.6 days, F=1.671, P=0.012). The 6-month follow-up group also showed higher GAF scores at discharge than the 6-month non-follow-up group (60.2±7.4 vs 57.5±6.1, F=0.234, P=0.045) (Table 2).
Comparison of treatment patterns prescribed at discharge between the 6-month follow-up group and the 6-month non-follow-up group
The most common treatment pattern prescribed at discharge was combination therapy, used in 66.3% (69/104) of the subjects. Combination therapy included a combination of an antipsychotic agent and mood stabilizer, a combination of an antipsychotic agent and antidepressant, a combination of an antipsychotic agent, mood stabilizer, and antidepressant, a combination of a mood stabilizer and antidepressant, or a combination of two or more antidepressants from different classes. The second most common treatment pattern at discharge was antidepressant monotherapy, used in 29.8% (31/104) of the subjects. The comparison in treatment pattern did not significantly differ between the two groups. However, the 6-month non-follow-up group was more likely to be prescribed antidepressant monotherapy than the 6-month follow-up group (35.1% [20/57] vs 23.4% [11/47]). Whereas, the 6-month follow-up group was more likely to be prescribed combination therapy (76.6% [36/47] vs 57.9% [33/57]) (Table 3). The most common regimen of antidepressant monotherapy in the 6-month non-follow-up group was paroxetine monotherapy, with a mean dose of 33.9 mg/day. The most common combination therapy in the 6-month follow-up group was a combination of an antidepressant and an atypical antipsychotic. In this group, the most commonly used atypical antipsychotic was quetiapine, with a mean dose of 185.7 mg/day, and the most commonly used antidepressant was paroxetine, with a mean dose of 41.5 mg/day.
Impact of sociodemographic and disease-related variables on premature discontinuation within 6 months after discharge
To identify the predictors for premature discontinuation, we carried out multivariable logistic regression analysis. We entered two variables including GAF score at discharge and duration of hospitalization that were found to be significant on the independent t-test as dependent variables, and we entered the other two variables including age and sex as confounding variables.
The multivariable logistic regression analysis showed that premature discontinuation of outpatient treatment within 6 months after discharge was predicted by a shorter hospital stay duration (odds ratio =1.026, 95% confidence interval =1.003–1.050, P=0.024) (Table 4).
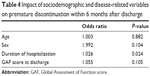  | Table 4 Impact of sociodemographic and disease-related variables on premature discontinuation within 6 months after discharge |
Discussion
As we expected, the premature discontinuation of outpatient treatment was common among the patients with noncombat-related PTSD. Only 45% of subjects continued their outpatient treatment for more than 6 months after discharge. We cannot directly compare this finding with the rates of continuity of outpatient treatment in other studies because no previous study has adopted the same definition of continuity of care of outpatient treatment used in this study (defined as regularly attending the scheduled outpatient visits, at least every other month, for more than 6 months post discharge). However, considering that consensus treatment recommendations typically require 6 to 12 months of pharmacotherapy for PTSD,12,16 this low continuity rate is a big challenge in clinical practice.
In our study, the 6-month follow-up group had higher GAF scores at discharge than the 6-month non-follow-up group. Several studies have examined the relationship between psychosocial functioning and the continuity of outpatient care among patients with psychiatric illness. Bindman et al33 prospectively followed 100 patients who had a prior history of two or more psychiatric hospitalizations due to their serious mental illness for 20 months. They found that a lower psychosocial functioning as assessed by the GAF score was associated with poor continuity of care.33 In Kreyenbuhl et al’s review,34 low social functioning was consistently associated with premature disengagement from psychiatric treatment among patients with schizophrenia and other serious mental illnesses. We believe that patients with a higher GAF score in this study might comply well with their scheduled outpatient appointments by regularly attending their timely outpatient visits due to their better functioning and this may have resulted in a lower rate of premature discontinuation.
In this study, the 6-month follow-up group showed a longer duration of index hospitalization. Furthermore, a shorter hospital stay was found to be a significant predictor of premature discontinuation. However, we were unable to find any studies that have investigated the relationship between duration of inpatient stay and treatment adherence after discharge among the noncombat-related PTSD populations. However, this finding is in line with some previous studies regarding predictors of poor treatment compliance among other psychiatric disorders. Stein et al35 investigated the influence of various variables on treatment compliance with timely psychiatric aftercare among Medicaid-enrolled patients after psychiatric hospitalization. They reported that a longer inpatient stay was a significant predictor of timely psychiatric aftercare.35 Axelrod and Wetzler36 also reported that the patients who stayed longer for psychiatric inpatient treatment were more likely to comply well with psychiatric aftercare during 6 months after discharge. However, Boyer et al37 reported different findings. They examined the risk factors for premature discontinuation of psychiatric outpatient treatment after hospitalization among 229 subjects with a primary diagnosis of psychiatric diseases. They found that the patients who received psychiatric inpatient treatment for a shorter period were more likely to attend their scheduled outpatient appointments after discharge.37 We think that the PTSD patients who stayed longer may have a relatively long enough time to receive adequate discharge plans and to have a discussion about future treatment with their psychiatrists or physicians, and this may explain the lower rate of premature discontinuation. In addition, we think that those who stayed longer had more opportunities to experience good treatment response, which was reflected in higher GAF scores at discharge, and this better experience perceived by the patients during hospitalization may result in better treatment compliance after discharge.
Even though the difference between the two groups did not reach statistical significance (P=0.070), there was a tendency for the 6-month non-follow-up group to more likely be prescribed antidepressant monotherapy and the 6-month follow-up group were more likely to be prescribed combination therapy. This finding was similar to that of Lockwood et al’s study.10 Lockwood et al10 investigated medication adherence following discharge among veterans who received a PTSD residential rehabilitation program. They found that only 34% of veterans included in their study were adherent to the psychotropic medication during the first year after discharge. They also found that subjects who were prescribed a higher number of medications were more adherent to treatment. They explained this relationship in the view of disease severity and patients’ perceived need for medication. Those who had a higher number of medications were more likely to have severe PTSD symptoms and thus, feel the necessity of taking medication more than those who had fewer medications. Another explanation is that the subjects who took more medications were more likely to receive frequent monitoring for their drug and this frequent monitoring would result in better adherence.10 However, in our retrospective data there was not sufficient information on the disease severity measured by validated instruments of PTSD, to explain our findings in terms of clinical severity. Instead, considering the higher GAF scores at discharge among the 6-month follow-up group, we think it is possible that better treatment perceived by the patients following combination therapy rather than antidepressant monotherapy might have led to a lower premature discontinuation rate after discharge. In addition, we hypothesize that the reason that this finding was not statistically significant was due to the small sample size in our study. To draw a definitive conclusion regarding the relationship between treatment compliance and treatment pattern, larger studies will be needed.
In this study, we identified the predictor of premature discontinuation of outpatient treatment after discharge, defined by the degree of patient’s compliance with the scheduled outpatient visits. This study has several limitations. First, this study used a retrospective chart review method; we could gather only the subjects’ information available in the medical records. Thus, we could not evaluate the effect of other variables on premature discontinuation that are known to be predictors in previous studies such as PTSD symptom severity measured by validated instruments, the doctor-patient relationship, and medication-related side effects. Additionally, because of limited information available in medical records, we were unable to evaluate the effects of physical conditions related to the trauma leading to PTSD, the presence of psychiatric comorbidity, and the presence of medical or surgical treatment the patients were concurrently receiving with psychiatric outpatient treatment on premature discontinuation. Second, our sample was of PTSD patients who were hospitalized at a university hospital and the sample size was relatively small. Thus, generalizing our results to the whole PTSD population does not seem appropriate.
Because PTSD has a chronic course, high rates of comorbidity and poor psychosocial outcomes,2,38 continuity of care that can enhance adherence to psychotropic medication is very important. Thus, identifying risk factors for premature discontinuation is critical because this can lead to targeted and more intensive interventions for a high risk group. Thus, we hope that future studies with larger sample sizes utilizing prospective designs will confirm the relationship between various sociodemographic or disease-related factors and continuity of treatment among this population.
Disclosure
The authors have no conflicts of interest to disclose.
References
American Psychiatric Association. Diagnostic and Statistical Manual of Mental Disorders. Fifth Edition. DSM-5. Washington, DC: American Psychiatric Association. 2013. | ||
Ipser JC, Seedat S, Stein DJ. Pharmacotherapy for prevention of post-traumatic stress disorder. Cochrane Database of Systematic Reviews. 2006(4):CD006239. | ||
Zatzick DF, Marmar CR, Weiss DS, et al. Posttraumatic stress disorder and functioning and quality of life outcomes in a nationally representative sample of male Vietnam veterans. Am J Psychiatry. 1997;154(12): 1690–1695. | ||
Ferrada-Noli M, Asberg M, Ormstad K, Lundin T, Sundbom E. Suicidal behavior after severe trauma. Part 1: PTSD diagnoses, psychiatric comorbidity, and assessments of suicidal behavior. J Trauma Stress. 1998;11(1):103–112. | ||
Pivac N, Kozaric-Kovacic D. Pharmacotherapy of treatment-resistant combat-related posttraumatic stress disorder with psychotic features. Croat Med J. 2006;47(3):440–451. | ||
Berger W, Mendlowicz MV, Marques-Portella C, et al. Pharmacologic alternatives to antidepressants in posttraumatic stress disorder: a systematic review. Prog Neuropsychopharmacol Biol Psychiatry. 2009;33(2): 169–180. | ||
Ahearn EP, Mussey M, Johnson C, Krohn A, Krahn D. Quetiapine as an adjunctive treatment for post-traumatic stress disorder: an 8-week open-label study. Int Clin Psychopharmacol. 2006;21(1):29–33. | ||
Berger W, Portella CM, Fontenelle LF, Kinrys G, Mendlowicz MV. Antipsychotics, anticonvulsants, antiadrenergic agents and other drugs: What to do when posttraumatic stress disorder does not respond to selective serotonin reuptake inhibitors? Revista Brasileira de Psiquiatria. 2007;29(Suppl 2):S61–S65. | ||
Carey P, Suliman S, Ganesan K, Seedat S, Stein DJ. Olanzapine monotherapy in posttraumatic stress disorder: efficacy in a randomized, double-blind, placebo-controlled study. Hum Psychopharmacol. 2012; 27(4):386–391. | ||
Lockwood A, Steinke DT, Botts SR. Medication adherence and its effect on relapse among patients discharged from a Veterans Affairs posttraumatic stress disorder treatment program. Ann Pharmacother. 2009;43(7):1227–1232. | ||
Kronish IM, Edmondson D, Li Y, Cohen BE. Post-traumatic stress disorder and medication adherence: results from the Mind Your Heart study. J Psychiatr Res. 2012;46(12):1595–1599. | ||
Davidson J, Pearlstein T, Londborg P, et al. Efficacy of sertraline in preventing relapse of posttraumatic stress disorder: results of a 28-week double-blind, placebo-controlled study. Am J Psychiatry. 2001;158(12):1974–1981. | ||
Martenyi F, Brown EB, Zhang H, Koke SC, Prakash A. Fluoxetine v. placebo in prevention of relapse in post-traumatic stress disorder. Br J Psychiatry. 2002;181:315–320. | ||
Melfi CA, Chawla AJ, Croghan TW, Hanna MP, Kennedy S, Sredl K. The effects of adherence to antidepressant treatment guidelines on relapse and recurrence of depression. Arch Gen Psychiatry. 1998;55(12): 1128–1132. | ||
Osterberg L, Blaschke T. Adherence to medication. N Engl J Med. 2005;353(5):487–497. | ||
No authors listed. The expert consensus guideline series. Treatment of Posttraumatic Stress Disorder. The Expert Consensus Panels for PTSD. J Clin Psychiatry. 1999;60 Suppl 16:3–76. | ||
National Institute for Health and Clinical Excellence [homepage on the Internet]. London: Post-traumatic stress disorder (PTSD): The management of PTSD in adults and children in primary and secondary care; 2005. Available from: https://www.nice.org.uk/guidance/cg26. Accessed February 4, 2015. | ||
Stein MB, Cantrell CR, Sokol MC, Eaddy MT, Shah MB. Antidepressant adherence and medical resource use among managed care patients with anxiety disorders. Psychiatr Serv. 2006;57(5):673–680. | ||
Greenberg GA, Rosenheck RA, Fontana A. Continuity of care and clinical effectiveness: treatment of posttraumatic stress disorder in the Department of Veterans Affairs. J Behav Health Serv Res. 2003;30(2):202–214. | ||
Greenberg GA, Fontana A, Rosenheck RA. Continuity and intensity of care among women receiving outpatient care for PTSD. Psychiatr Q. 2004;75(2):165–181. | ||
Huggins JM, Brown JN, Capehart B, Townsend ML, Legge J, Melnyk SD. Medication adherence in combat veterans with traumatic brain injury. Am J Health Syst Pharm. 2011;68(3):254–258. | ||
Lu MW, Duckart JP, O’Malley JP, Dobscha SK. Correlates of utilization of PTSD specialty treatment among recently diagnosed veterans at the VA. Psychiatr Serv. 2011;62(8):943–949. | ||
Elhai JD, Reeves AN. Predictors of Mental Health and Medical Service Use in Veterans Presenting With Combat-Related Posttraumatic Stress Disorder. Psychological Services. 2004;1(2):111–119. | ||
Hertzberg MA, Feldman ME, Beckham JC, Kudler HS, Davidson JR. Lack of efficacy for fluoxetine in PTSD: a placebo controlled trial in combat veterans. Ann Clin Psychiatry. 2000;12(2):101–105. | ||
van der Kolk BA, Dreyfuss D, Michaels M, et al. Fluoxetine in posttraumatic stress disorder. J Clin Psychiatry. 1994;55(12):517–522. | ||
Zohar J, Amital D, Miodownik C, et al. Double-blind placebo-controlled pilot study of sertraline in military veterans with posttraumatic stress disorder. J Clin Psychopharmacol. 2002;22(2):190–195. | ||
Brinker M, Westermeyer J, Thuras P, Canive J. Severity of combat-related posttraumatic stress disorder versus noncombat-related posttraumatic stress disorder: a community-based study in American Indian and Hispanic veterans. J Nerv Ment Dis. 2007;195(8):655–661. | ||
Breslau N, Davis GC. Posttraumatic stress disorder: the etiologic specificity of wartime stressors. Am J Psychiatry. 1987;144(5):578–583. | ||
Laufer RS, Brett E, Gallops MS. Dimensions of posttraumatic stress disorder among Vietnam veterans. J Nerv Ment Dis. 1985;173(9):538–545. | ||
Woodward SH, Leskin GA, Sheikh JI. Movement during sleep: associations with posttraumatic stress disorder, nightmares, and comorbid panic disorder. Sleep. 2002;25(6):681–688. | ||
American Psychiatric Association. Diagnostic and Statistical Manual of Mental Disorders. Fifth Edition (DSM-IV). Washington, DC: American Psychiatric Association; 1994. | ||
American Psychiatric Association. Diagnostic and Statistical Manual of Mental Disorders. Washington, DC: American Psychiatric Association; 2000. | ||
Bindman J, Johnson S, Szmukler G, et al. Continuity of care and clinical outcome: a prospective cohort study. Soc Psychiatry Psychiatr Epidemiol. 2000;35(6):242–247. | ||
Kreyenbuhl J, Nossel IR, Dixon LB. Disengagement from mental health treatment among individuals with schizophrenia and strategies for facilitating connections to care: a review of the literature. Schizophr Bull. 2009;35(4):696–703. | ||
Stein BD, Kogan JN, Sorbero MJ, Thompson W, Hutchinson SL. Predictors of timely follow-up care among medicaid-enrolled adults after psychiatric hospitalization. Psychiatr Serv. 2007;58(12):1563–1569. | ||
Axelrod S, Wetzler S. Factors associated with better compliance with psychiatric aftercare. Hosp Community Psychiatry. 1989;40(4):397–401. | ||
Boyer CA, McAlpine DD, Pottick KJ, Olfson M. Identifying risk factors and key strategies in linkage to outpatient psychiatric care. Am J Psychiatry. 2000;157(10):1592–1598. | ||
Rapaport MH, Endicott J, Clary CM. Posttraumatic stress disorder and quality of life: results across 64 weeks of sertraline treatment. J Clin Psychiatry. 2002;63(1):59–65. |
 © 2015 The Author(s). This work is published and licensed by Dove Medical Press Limited. The
full terms of this license are available at https://www.dovepress.com/terms.php
and incorporate the Creative Commons Attribution
- Non Commercial (unported, v3.0) License.
By accessing the work you hereby accept the Terms. Non-commercial uses of the work are permitted
without any further permission from Dove Medical Press Limited, provided the work is properly
attributed. For permission for commercial use of this work, please see paragraphs 4.2 and 5 of our Terms.
© 2015 The Author(s). This work is published and licensed by Dove Medical Press Limited. The
full terms of this license are available at https://www.dovepress.com/terms.php
and incorporate the Creative Commons Attribution
- Non Commercial (unported, v3.0) License.
By accessing the work you hereby accept the Terms. Non-commercial uses of the work are permitted
without any further permission from Dove Medical Press Limited, provided the work is properly
attributed. For permission for commercial use of this work, please see paragraphs 4.2 and 5 of our Terms.


