Back to Journals » Adolescent Health, Medicine and Therapeutics » Volume 11
Pre-Transition Readiness in Adolescents and Young Adults with Four Chronic Medical Conditions in South East Nigeria – An African Perspective to Adolescent Transition
Authors Ayuk AC, Onukwuli VO, Obumneme-Anyim IN, Eze JN , Akubuilo UC, Mbanefo NR, Iloh KK , Ezenwosu OU, Odetunde IO , Okafor HU, Emodi IJ, Oguonu T
Received 14 November 2019
Accepted for publication 12 February 2020
Published 11 March 2020 Volume 2020:11 Pages 29—38
DOI https://doi.org/10.2147/AHMT.S238603
Checked for plagiarism Yes
Review by Single anonymous peer review
Peer reviewer comments 3
Editor who approved publication: Professor Alastair Sutcliffe
Adaeze C Ayuk, Vivian O Onukwuli, Ijeoma N Obumneme-Anyim, Joy N Eze, Uzoamaka C Akubuilo, Ngozi R Mbanefo, Kenechukwu K Iloh, Osita U Ezenwosu, Israel O Odetunde, Henrietta U Okafor, Ifeoma J Emodi, Tagbo Oguonu
College of Medicine University of Nigeria, University of Nigeria Teaching Hospital, Ituku Ozalla, Enugu, Nigeria
Correspondence: Adaeze C Ayuk
College of Medicine University of Nigeria, University of Nigeria Teaching Hospital, Ituku Ozalla, Enugu, Nigeria
Email [email protected]
Introduction: When a child reaches a certain age, he or she moves over to the adult physician. For this to maximally benefit the child, there has to be a process of equipping the child with skills required for taking on more responsibilities. Transitioning involves a process in which the adolescent with chronic illness is prepared ahead of time to enable them to eventually transfer to adult care with good outcomes. In high-income countries with well-organized health financing, the transitioning process begins as early as 12 years. In Africa, this process is not as organized and most hospitals would write a referral letter once the child turns 18 and transfer to adult clinic. In four of our chronic disease clinics (asthma, HIV, sickle cell anaemia and chronic kidney diseases) patients up to 24 years old are still attending the paediatric clinics. Understanding transition readiness among African adolescents remains a gap. Our findings will form a basis for informed practices for adolescent clinics in African countries.
Methods: This was a descriptive cross-sectional study of pre-transition readiness in adolescents and young adults with chronic illnesses attending four outpatient specialist clinics in a tertiary hospital in Enugu Nigeria. This was done using the validated STARx Questionnaire. Total scores were computed and scores nearer the upper limit of 90 were acceptable, while mean subdomain scores of 4 and above were considered as optimal level of transition readiness. Demographic and clinical data were also collected. Acceptability to move on to adult-oriented care was documented using binary response (yes/no). Cross tabulations were done, and likelihood ratios obtained for predictors of acceptability of transition. Significant value was set at p-value of ≤ 0.05.
Results: A total of 142 adolescents and young adults aged 12 to 24 years were studied. There were 38.0% (54), 24.6% (35), 22.5% (32) and 14.8% (21) from HIV, sickle cell anaemia, asthma and nephrology clinics, respectively. Their mean age was 15.6 years ± 2.4, and 48.6% (69) were male. The mean total transition readiness score was 56± 14 and this was not nearer the higher spectrum of total scores obtainable. Highest mean scores (3.7) occurred in the knowledge subdomain while least mean score (2) was noted in the use of medication reminders. The males had highest scores in the knowledge subdomain while the females were better informed about medication adherence and were more inquisitive about their chronic illness. Only about 37% (53) of the adolescents and young adults welcomed the idea of moving on to adult-care clinics. Children who had less frequent emergency hospital visits and better treatment outcome accepted the idea of transfer to adult care. Irrespective of the age all participants had suboptimal subdomain scores. High scores did not influence the participants’ choice to embrace transfer to adult care.
Conclusion: There is suboptimal transition readiness irrespective of the age. The older age groups were less willing to transfer to adult care. Better disease knowledge and better communication skills did not positively influence acceptability of transfer to adult care.
Keywords: adolescent, African, chronic, readiness, transition, transfer
Background
The chronicity of some medical conditions means that the disease occurs during the life span of the individual. Transitioning in children with chronic health conditions, from the paediatric to adult care is a planned and staged process that considers the various needs of the growing adolescents and young people with chronic medical conditions as they eventually transfer from child-centred to adult-oriented health-care systems.1,2 Having received care by a particular set of staff over years, the children are likely to be attached emotionally to their paediatrician and thus require readjusting to a new set of staff for continued care. While in adult-oriented care, the individual is further expected to take up more responsibility for self-care.International guidelines and authors had recommended that planning for the transition from adolescent to adult care should begin at the age of 12 years to allow enough time for developing a transition plan.3–5 This was supported by the American Academy of Pediatricians which described several activities designed to support transition beginning when a patient is 12 years old.6 The recommendation is that a transition plan should have been written for every child by 14 years of age as a critical step to improve the transition process to adult-oriented healthcare.7 These milestone ages correspond with commencement of puberty, which on the average is similar, but there may delay the transitioning process for the African adolescent who lags behind their Caucasian counterparts in cognitive development.8 More so, the adolescent stage is associated with a period of lack of identity and psychological peculiarities of not being sure if they are adults or still children, self-assertiveness, not like being told what to do, emotional tantrums and mood swings, alongside understanding their new body changes and physiological adjustments.9 All these may affect their transition readiness and their acceptability of the transfer process. Among African cultural practices includes that of having a deep-rooted respect for elders. The transition and transfer process may be more turbulent where because of this respect, an adolescent may be continually regarded as a child as long as the parents/elderly caregivers are still living, and this would occur even in the adult clinics. The adolescent who already feels uncomfortable when being seen amidst infants and younger children, may feel worse amongst the adult and elderly in the adult clinic. This occurrence is also attributable to over dependence on the parents who then continually see them as children. This is in contrast to what is obtainable in the western world where independence is encouraged at an earlier age and teenagers by 18 years are already prepared to live independent lives. There is therefore the need to understand within the African context, what aspects of transition readiness are required and need to be emphasized early, to adequately prepare the adolescents and young adults,10,11 for smooth continuum of care.
This study assessed readiness of transitioning and eventual transfer to adult care in adolescents and young adults with chronic health conditions (asthma, sickle cell anaemia, Human Immunodeficiency Virus (HIV) infection and chronic kidney diseases such as Nephrotic Syndrome. They were also asked if they accepted the idea of moving care (willingness to move to adult care) and what reasons affected their answers. The results from this study hopefully, will inform best practices for pre-transition counselling while preparing them for adult continuum of care in our setting and beyond. Our findings will also form a bed rock for informed practices when setting up adolescent clinics in our setting and similar African countries.
Methods
This was a descriptive cross-sectional study of adolescents and young adults with four chronic illnesses attending the four major outpatient paediatric specialist clinics at the University of Nigeria Teaching Hospital (UNTH), Ituku-Ozalla, Enugu, Nigeria. Prior to commencement, permission was obtained from the original developers of the study questionnaire in the University of North Carolina School of Medicine while ethical clearance was obtained from the Human Research and Ethics Committee of the University of Nigeria Teaching Hospital Ituku/Ozalla, Enugu, Nigeria. A signed written informed consent was also obtained from each participants and their parent or legal guardian. Proportionate sample size calculations were used to obtain sample sizes based on the number of children who were 12 years and above, who had been consistent in their respective clinics in the preceding year.12,13 Records from the four clinics were thus obtained and carefully studied and the number of children whose records showed a minimum of four outpatient visits in the preceding year were considered as consistent.14 These children were likely to have benefited appropriately from paediatric care and thus could give reliable data with regards to needs and gaps related to transitioning to adult care. Those who had less than four visits were excluded. The population was drawn from the total of 384 recorded adolescents and young adults that attended the 4 clinics in the preceding year. Based on their respective population in the clinics, we recruited consecutively the proportionate sample size required from the various clinics: 63, 39, 36 and 23 from, HIV, sickle cell anaemia, asthma, nephrology clinics, respectively. To collect data on transition readiness, the validated interviewer-administered Self-management and Transition to Adulthood with Treatment (STARx) questionnaire15–17 was pretested and found to have good internal consistency (Cronbach’s alpha 0.8), and was used via interviewer-administered survey.
The STARx questionnaire also has external validity meaning that it can be applied to make deductions outside the context of children with asthma, sickle cell, nephrotic syndrome and HIV disease as it has been applied across a wide range of several other chronic conditions and found to be a sound tool that informed decisions for those chronic conditions.15–20
The STARx questionnaire has a total of 18 questions with three subdomains. The subdomains contain nine questions on Self-Management methods which includes questions like: How easy or hard is it to take your medicines like you are supposed to? How easy or hard is it to take care of yourself? There were three questions on disease knowledge that asked: How much do you know about your illness? How much do you know about what will happen if you do not take your medicines? The third subdomain section had six questions on Communication skills which includes questions like: How easy or hard is it to talk to your doctor? How easy or hard is it to make a plan with your doctor to care for your health? How easy or hard do you think it would be for you to move to adult care? The answer options ranged from “I do not need to do this” to “I always do this” and a sixth option of “not needed for my care” (allowed for questions not applicable to an individual patient). These were graded on a Likert scale of 0 to 5 and each question worth a maximum score of 5 and minimum of 0. The zero score was given if that skill was not necessary for a particular question, score of 1 for not knowing how to perform the necessary skill, up to a maximum score of 5 where the participant performed that particular skill consistently. According to the number of questions asked, the maximum total score obtainable in the self-management subdomain was 45, for knowledge subdomain, 15; and for the communication skills a total score of 30. A mean subdomain readiness cut-off score of ≥4 was adopted as an acceptable readiness score and this was equivalent to respondents starting to perform necessary disease management skills for that subdomain, and required during adult continuum of care. This was similar to the cut-off points assigned as readiness cut-off by a similar validated tool, the Transition Readiness Assessment Questionnaire (TRAQ) which had good correlations with the STARx Questionnaire.21–23 Subdomain scores were combined to obtain the total scores with a possible maximum score of 90 and a possible minimum score of zero. Scores towards zero indicated that readiness for transition to adult care was lacking. The adolescents/young adults were thought to be sub-optimally ready if the total scores were not clearly nearer the upper 90 maximum score, and thus the specific subdomain where skills were lacking needed to be addressed.
Other data collected were gender, current age, age at disease onset, if caregivers had fully explained the respective disease status to the affected child (illness disclosure), parental socioeconomic status, hospital visit frequency, bill payment mode (out-of-pocket or health insurance). As a follow-up of the last question asked in the communication subdomain (How easy or hard do you think it would be for you to move to adult care?), a documentation on the participants’ acceptability of transfer to adult care (willingness to transit) was done. We also documented the possible reasons that may affect that decision and what age is the perceived ideal age for the African adolescent within the context of his/her culture. Beyond obtaining transition readiness score, this finding could help strengthen an adolescent counselling session for the African child and the reasons given serve as possible predictors for optimal or suboptimal transition readiness. These sub-analyses were important to this study to enable us contextually interpret and apply “an African perspective” to the findings from transition readiness scores. The respondents were thus required to answer “yes” or “no” to the acceptability of the transfer to adult care. Subsequently, they stated the reasons for their choices from listed options such as, “Yes” I am willing to transit because a) I am old enough to transit; b) I have overgrown coming to a paediatric clinic; c) I am not getting all the attention I need as an adolescent; d) I just want to change environment e) My doctor said I should move over; f) Others. Socio-economic status (SES) was determined using the level of education and type of vocation of parents and these were categorized into lower Class 3 (socioeconomic class [SEC] 4 and 5), middle Class 2 (SEC 2 and 3), and upper Class 1 (SEC 1), thus class I belonged to the highest, while class V belonged to the lowest economic cadre.24
Data Management and Analyses
Frequencies of the variables were done for initial descriptive statistics. The Shapiro–Wilk test was used to test for normality for continuous variables. Using the date of birth, participants current ages were further categorized into equal class intervals: 12 to ≤14 years, >14 to ≤17 and >17 years to fit into various developmental stages that may affect transition readiness.22 The mean total scores and mean subdomain scores for transition readiness and the various percentages representing acceptability of transfer to adult care were represented in prose form. Test of association and cross-tabulations of possible predictors of transition readiness between variables were done across groups using t-tests for numerical variables (e.g. current age, mean age at diagnosis, frequency of clinic attendance) and chi-square tests used when computing categorical variables (e.g. chronic health condition, gender, age group, illness disclosure to the child, health payment plan). Significant findings were represented in tables. Statistically, significant value was set at a p-value of <0.05.
Results
General Characteristics
Table 1 shows the adolescents and young adults between the ages of 12 and 24 years enrolled from HIV, sickle cell anaemia, asthma and nephrology clinics and comprised 38.0% (54), 24.6% (35), 22.5% (32) and 14.8% (21). Overall 48.6% (69) were male while 51.4% (73) were females. Ages of all participants and their SES were normally distributed. The mean age of all respondents was 15.6 years ± 2.4. Among all participants, 34.5% (49) were <14years old,45.1% (64) were >14 to <17 years old, while 20.4% (29) were>17years old. The distribution of the parental social classes: 15.5% (22), 30.3% (43), 26.1% (37), 19.0% (27) and 9.2% (13), respectively for social classes, I, II, III, IV and V. There were 89.4% (127) of study participants on self-paid health plan while 10.6% (15) were on some form of external health financing. Illness disclosure to the child had occurred in 81.0% (115). The mean age at diagnosis (all chronic cases combined) was 8.4 ± 4.8 years while the mean years of clinic attendance was 6.3 ± 5 years; with frequency of outpatient visits per year 5 ± 3.6 visits and inpatient admissions <1 per year.
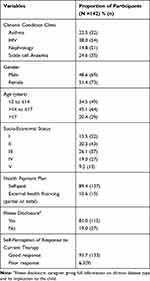 |
Table 1 Sociodemographic Characteristics of All Study Participants |
Transition Readiness Scores
The mean of total transition readiness scores for all participants was 59±14. The transition scores when assessed by the clinic type showed: asthma 59±14; HIV 59±23; nephrology 59±12 and sickle cell anaemia (SCA) clinic 58±15. When assessed by the various age categories, total mean scores of 59±14, 59±13 and 58±17 were, respectively, obtained in participants 12 to ≤14 years, >14 to ≤17 and >17 years old. Though not statistically significant, the lowest total score was obtained by the older age category. The children from upper social class had total score of 59±13; those from middle class 60±11, while those from lower SEC scored 59±14. The total transition readiness scores were not influenced by belonging to any specific social class, age category, gender, duration of ill-health, disclosure status or the clinic type attended.
Transition Readiness Subdomain Outcomes
Self-Management Methods
This subdomain included questions like How often did you need someone to remind you to take your medicines? How often did you use things like pillboxes, schedules, or alarm clocks to help you take your medicines when you were supposed to? How often did you use the internet, books or other guides to find out more about your illness? How often did you work with your doctor to take care of new health problems that came up? In this subdomain, the participants had a total score of 27 out of a possible score of 45 and a mean score of 3. The highest mean score of 5 was obtained from the question: “how often did you take your medications by yourself” and the lowest mean score of 2.3 obtained from the question “how often did you use things like pillboxes, schedules or alarm clocks to help you take your medicines”.
Knowledge Subdomain
These questions were included: How much do you know about your illness? How much do you know about taking care of your illness? How much do you know about what will happen if you do not take your medicines? In this subdomain, the participants had a total score of 11 out of a possible score of 15 and a mean score of 3.7. The highest mean score of 5 was obtained from the question pertaining to the knowledge of the consequences of missing prescribed medications, and the highest scores occurred in participants attending the HIV clinic.
Communication Subdomain
Some of the questions in this subdomain were: How easy or hard is it to talk to your doctor? How easy or hard is it to make a plan with your doctor to care for your health? How easy or hard is it to see your doctor by yourself? The participants had a total score of 20 out of a possible score of 30 and a mean score of 3.3. The lowest mean subdomain score 2, was obtained in two questions: whether they find it easy to make a plan with the doctor and whether they thought it would be easy to move to adult care.
Acceptability of Transferring to Adult-Oriented Care
The percentage of participants that welcomed the idea of transferring to adult care was 37.3% (53); while 62.7% (89) were unwilling to transfer to adult-oriented care, and this was more among the older age group, Table 2. Of those not willing to change carer, 71% said they did not want to change their paediatric doctor and also did not feel ready yet to transit to adult-oriented care, Table 3. Of the few willing to transfer to adult care, 43.3% wanted to do so because, they were old enough by their judgement. Children whose health were stable and were responding well to their current management without emergency hospital visits per year were more welcoming of the idea to move on to adult-oriented care; χ2=26.4; p= 0.02; LR= 30.6.
 |
Table 2 Acceptability Choices by Age with Regard to Transfer to Adult-Oriented Care Among African Adolescents/Young Adults with Chronic Illnesses |
 |
Table 3 Reasons Given for Acceptability Choices with Regards to Transfer to Adult-Oriented Care Among African Adolescents/Young Adults with Chronic Illnesses |
When these African adolescent participants were asked what the best age they would recommend as ideal to be transferred to adult care, they suggested 19.1±2.6 years.
Predictors of Transition Readiness and Acceptability of Transfer to Adult-Oriented Care
Influence of Specific Chronic Disease
For specific domain assessment, the self-management skills showed that among participants, those attending the HIV clinic, showed better skills in taking their medications unassisted. That notwithstanding, the idea of moving over to adult care was however still not acceptable to these children, p=0.015; LR 15.3, Table 4.
 |
Table 4 Self-Management Skill (Medication Intake) by Chronic Clinic Type and Willingness to Transfer Adult-Oriented Care |
Influence of Gender
When the communication skills domain was assessed, females fared better (high inquisitive skills mean score of 5), but the idea of moving over to adult care was however still not acceptable to these females (p 0.03), Table 5.
 |
Table 5 Communication Skills (Illness Inquisition) in Various Gender and Willingness to Transfer to Adult-Oriented Care |
Among males, those with high knowledge mean score of 5, did not also want to change existing care plan to move over to adult-oriented care, p=0.05, LR 12.1, Table 6.
 |
Table 6 Knowledge of Illness Score in Various Gender and Willingness to Transfer to Adult-Oriented Care |
Discussion
Transitioning from paediatric to adult care for adolescents with chronic health conditions is a planned process, even within cultural context. The adolescent is expected to take up more, if not full responsibility for self-care. Taking responsibility for self-care requires that the individual has adequate knowledge and experience about the specific chronic illness. Our study showed that females were more open to ask questions with good communication skills when compared to males. The African male may be seen with more ego and more reserved not ready to expose any lack of knowledge and this may affect his communication skills and ability to ask questions. Of note however, was that males who had more knowledge about their illness were still not embracing the idea of transitioning. A plausible explanation relates to the issue of confidentiality and stigmatization. As they become aware of their chronic condition as adolescents they may become less willing to have a new set of staff privy to their personal information. This is particularly true in a male African adolescent living with HIV, where his ego is at stake and the future of forming a nuclear family in the near future rests heavily on him and thus transfer to a new carer seen as a stranger, may not be a welcomed option.
This study documented low mean scores in communication skills but good scores on knowledge sub-domains. This was similarly observed in a study done among adolescents with sickle cell anaemia (SCA).16 Studies have reported the importance of having good communication skills and having good knowledge of medication intake before being considered as ready to be moved over to adult care.16,17 We noted that excellent communication skills alongside good knowledge of ones chronic illness did not translate to acceptability of change from paediatric care to adult-oriented care, because although females had better communication skills and were more open to ask questions, the knowledge acquired from the interaction did not positively affect their readiness to move over to adult care. This emphasizes the need to start on time to impart communication and interaction skills to children as this will be of great benefit to them even during the pre-transition stage.
Children attending the HIV clinic scored highly on the aspect of taking medications on their own without adult assistance. However, moving to adult-oriented care was still not acceptable to them. The high scores in this subdomain among children attending the HIV clinic may be related to awareness of the nature of their illness and consequences of missing medication. Adherence counselling is notably done routinely as part of the care package for the HIV infected adolescents attending our hospital. This, however, did not make them more likely to accept a move to adult care. This may also be related to the fear of stigmatization and breach of confidentiality.
Under self-care methods, all participants irrespective of the type of chronic illness, had their least scores in the use of reminders to take medications. Until their orientation is changed and they are taught better, use of medication counters and reminders may be perceived as a “white man practice.” This then results in further dependence on adult help with increased chances of forgetting to take their medication if adult help is not available. In a similar study,18 the most common reason in 50% of the participant for non-adherence was forgetfulness. The use of medication reminders, therefore, needs reinforcement during pre-transition counselling to help improve medication adherence outcomes.
Concerning health financing, some studies have reported availability of necessary funds and the health structure/medical payment plans of individual countries to predict transition readiness.1,2,10 Our study showed that majority of our participants paid out-of-pocket. In most African countries like Nigeria, the health insurance plans and packages are not as robust, thus assessment of influence of predictors such as payment plan showed that the bill payment plan neither influenced their transition readiness scores nor their acceptability to move to adult care. This is notwithstanding that our paediatric clinic costs and charges are much less compared to that of adult patients. Javalkara et al25 in USA, showed that significant predictors of transition readiness included age, gender, and higher SES. In contrast, our study and that of Jensen et al26 observed no significant influence of age, gender and social status on transition readiness. Lack of effect of sociodemographic factors in our study highlight the possible consequence of confidence developed over time by these children as they continued to bond with their Paediatricians, a bond that influenced their preference not to move on to adult care irrespective of the social status.
Participants with self-reported good response to their current management, had less emergency hospital visits, but this rather influenced them to be non-desirous of transfer to a new doctor. This probably reflects satisfaction with the “status quo” and preferring not to transit as has been suggested by other researchers.15,16
Benefits of well-managed transition include uninterrupted coordinated health care as well as reduced psychological fear and anxiety that may arise from meeting new doctors and learning new sets of instructions and taking care of oneself without much help anymore.25 In some studies, transition-related benefits expressed by adolescents that had moved on smoothly to adult care, included feeling of satisfaction in being treated as adults and having a sense of independence in adult-oriented care.26–28 This may have been impacted by possible early preparedness and telling the adolescents on time what to expect. Within our African cultural settings, with the inhibitory effect of respect for elders and not wanting to be quickly moved into same clinic with the elders, such organized and early process will be of great benefit. In the current study, more than 60% of participants did not want to change their current care set up. This included the “over-aged” clinic attendees who were already above the age of 18 years, and some who were up to 24 years. Similar to this, Huang et al27 in their cohort of children with three chronic diseases: cystic fibrosis, inflammatory bowel disease and type 1 diabetes also had children as old as 20 years still being attended to by paediatricians. In another study, up to 5% of the study population in a paediatric service were also noted to be between the ages of 22 to 23 years.26 This finding of older children still being seen in paediatric care may be improved if early initiation of transition is routinely practiced, with conscious efforts made at pre-transition preparations. In Nigeria, despite the cultural influence, the adult age of independence that accord some privileges like voting rights have remained at 18 years. This affects the age that the transitioning process is actively thought about and may have influenced our study participants suggesting 19 years as ideal age to transfer to adult care. This should not be so. Some guidelines6,28 have suggested ages as early as 12 to 14 years to move a child to adult care, but consensus opinion tend to rather adopt an individualized approach based on the transition readiness of each child.29 As seen also in other studies10,26,30 those who were not willing to move to adult-oriented care, expressed reasons related to strong paediatric staff (doctors and nurses) attachment. This highlights the need for early pre-transition preparations so that when it is time, it is a seamless transfer to adult-oriented care even within our African context.
Study Limitation
The study did not asses what effect pre-transition counselling may have on transition readiness. The inclusion of and comparison with caregiver/family opinion would have given a more holistic picture of adolescent transition in Africa and what other factors may affect the process. The study was a cross-sectional study, as a longitudinal design would be more informative on the complete transition process however we were able to assess the pre-transition readiness within the scope of our objective.
Conclusion
We emphasize that the transition process is totally different from a patient “transfer” to another clinic as may obtain in African settings. Transfer should occur only following a well-planned transitioning which requires a ready and pre-informed participation of the adolescent, their caregivers, and the health system. This study demonstrated a suboptimal readiness to transitioning among our African adolescent with chronic illnesses. The necessary skills required for adult-oriented care was lacking. Many did not accept the idea of moving on over to new carers even when the scores were appropriate for knowledge or communication skills. Use of medication reminders is low irrespective of chronic disease condition. The need to scale up adolescent transition programmes in Africa is recommended.
Disclosure
The authors report no conflicts of interest in this work.
References
1. Lam P-Y, Fitzgerald BB, Sawyer SM, et al. Young adults in children’s hospitals: why are they there? Med J Aust. 2005;182:381–384. doi:10.5694/j.1326-5377.2005.tb06755.x
2. Blum RW, Garell D, Hadgman CH, et al. Transition from child-centred to adult health-care systems for adolescents with chronic conditions. A position paper of the Society for Adolescent Medicine. J Adol Health. 1993;14:570–576. doi:10.1016/1054-139X(93)90143-D
3. Canadian Association of Paediatric Health Centres. National Transitions Community of Practice. A Guideline for Transition from Paediatric to Adult Health Care for Youth with Special Health Care Needs: A National Approach. Toronto (ON): Canadian Association of Paediatric Health Centres, Knowledge Exchange Network; 2016.
4. Young R, Dagnan D, Jahoda A. Leaving school: a comparison of the worries held by adolescents with and without intellectual disabilities. J Intellect Disabil Res. 2016;60(1):9–21. doi:10.1111/jir.12223
5. Ally S. Improving transition to adulthood for adolescents with intellectual and developmental disabilities. Can Fam Physician. 2018;64(Suppl 2):S37–S43.
6. White PH, Cooley WC. supporting the health care transition from adolescence to adulthood in the medical home. Pediatrics. 2018;142(5):e20182587. doi:10.1542/peds.2018-2587
7. Shaw TM, Delaet DE. Transition of adolescents to young adulthood for vulnerable populations. Pediatr Rev. 2010;31:497–507. doi:10.1542/pir.31-12-497
8. Rushton JP, Jensen AR. Thirty years of research on race differences in cognitive ability. Psychol Public Policy Law. 2005;11:235–294. doi:10.1037/1076-8971.11.2.235
9. Alderman EM, Breuner CC, committee on adolescence. Unique needs of the adolescent. Pediatrics. 2019;144(6):e20193150. doi:10.1542/peds.2019-3150
10. Prior M, McManus M, White P, Davidson L. Measuring the “Triple Aim” in transition care: a systematic review. Pediatrics. 2014;134:e1648–e1661. doi:10.1542/peds.2014-1704
11. Miles K, Edwards S, Clapson M. Transition from paediatric to adult services: experiences of HIV-positive adolescents; Psychological and Socio-medical Aspects of AIDS/HIV. AIDS Care. 2004;16(3):305–314. doi:10.1080/09540120410001665312
12. Whitley E, Ball J. Statistics review 4: sample size calculations. Crit Care. 2002;6(4):335–341. doi:10.1186/cc1521
13. Altman DG. Practical Statistics for Medical Research. London (UK): Chapman & Hall; 1991.
14. Kunutsor S, Walley J, Katabira E, et al. Clinic attendance for medication refills and medication adherence amongst an antiretroviral treatment cohort in Uganda: a prospective study. AIDS Res Treat. 2010;2010:872396. doi:10.1155/2010/872396
15. Gray WN, Resmini AR, Baker KD, et al. Concerns,barriers and recommendations to improve transition from pediatric to adult IB care: perspectives of patients, parents, and health professionals. Inflamm Bowel Dis. 2015;21:1641–1651. doi:10.1097/MIB.0000000000000419
16. Mennito S, Hletko P, Ebeling M, et al. Adolescents with sickle cell disease in a rural community: are they ready to transition to adulthood? South Med J. 2014;107:578–582. doi:10.14423/SMJ.0000000000000162
17. Withers AL, Green R. Transition for adolescents and young adults with asthma. Front Pediatr. 2019;7:301. doi:10.3389/fped.2019.00301
18. Straub DM, Tanner AE. Health-care transition from adolescent to adult services for young people with HIV. Lancet Child Adolesc Health. 2018;2:214–222. doi:10.1016/S2352-4642(18)30005-1
19. Ferris M, Cohen S, Haberman C, et al. Self-management and transition readiness assessment: development, reliability, and factor structure of the STARx questionnaire. J Pediatr Nurs. 2015;30(5):691–699.
20. Cohen SE, Hooper SR, Javalkar K, et al. Self-management and transition readiness assessment: concurrent, predictive and discriminant validation of the STARx questionnaire. J Pediatr Nurs. 2015;30(5):668–676.
21. Sawicki GS, Lukens-bull K, Yin X, et al. Measuring the transition readiness of youth with special healthcare needs: validation of the TRAQ—Transition Readiness Assessment Questionnaire with HIV. Lancet Child Adolesc Health. 2018;2:214–222.
22. Wood DL, Sawicki GS, Miller MD, et al. The transition readiness assessment questionnaire (TRAQ): its factor structure, reliability, and validity. AcadPediatr. 2014;14(4):415–422.
23. Transition readiness assessment questionnaire. Available from: www.etsu.edu/com/pediatrics/traq.
24. Ogunlesi AT, Dedeke IOF, Kuponiyi OT. Socio-economic classification of children attending specialist paediatric centres in Ogun State, Nigeria. Niger Med Pract. 2008;54:21–25.
25. Javalkara K, Johnson M, Kshirsagar AV, et al. Ecological factors predict transition readiness/self-management in youth with chronic conditions. J Adol Health. 2016;58(1):40–46. doi:10.1016/j.jadohealth.2015.09.013
26. Jensen PT, Paul GV, LaCount S, et al. Assessment of transition readiness in adolescents and young adults with chronic health conditions. Pediatr Rheumatol. 2017;15:70. doi:10.1186/s12969-017-0197-6
27. Huang JS, Terrones L, Tompane T, et al. Preparing Adolescents with chronic disease for transition to adult care: a technology program. Pediatrics. 2014;133:e1639–e1646. doi:10.1542/peds.2013-2830
28. Bolton-maggs PHB. Transition of care from paediatrics to adult services in hematology. Arch Dis Child. 2007;9(9):797–801. doi:10.1136/adc.2006.103804
29. American Academy of Pediatrics; American Academy of Family Physicians; American college of Physicians-American Society of Internal Medicine. A consensus statement on health care transitions for young adults with special health care needs. Pediatrics. 2002;110(6 pt 2):1304–1306.
30. Sobota A, Akinlonu A, Champigny M, et al. Self-reported transition readiness among young adults with Sickle Cell Disease. J Pediatr Hematol Oncol. 2014;36(5):389–394.
 © 2020 The Author(s). This work is published and licensed by Dove Medical Press Limited. The full terms of this license are available at https://www.dovepress.com/terms.php and incorporate the Creative Commons Attribution - Non Commercial (unported, v3.0) License.
By accessing the work you hereby accept the Terms. Non-commercial uses of the work are permitted without any further permission from Dove Medical Press Limited, provided the work is properly attributed. For permission for commercial use of this work, please see paragraphs 4.2 and 5 of our Terms.
© 2020 The Author(s). This work is published and licensed by Dove Medical Press Limited. The full terms of this license are available at https://www.dovepress.com/terms.php and incorporate the Creative Commons Attribution - Non Commercial (unported, v3.0) License.
By accessing the work you hereby accept the Terms. Non-commercial uses of the work are permitted without any further permission from Dove Medical Press Limited, provided the work is properly attributed. For permission for commercial use of this work, please see paragraphs 4.2 and 5 of our Terms.
