Back to Journals » International Journal of Women's Health » Volume 12
Postpartum Modern Contraceptive Utilization and Associated Factors Among Women Who Gave Birth in the Last 12 Months in Addis Zemen, South Gondar, Ethiopia: Community-Based Cross-Sectional Study
Authors Nibret Mihretie G , Simegn A, Dereje A, Gebrehana H , Getie A, Getnet B , Degu A
Received 18 September 2020
Accepted for publication 25 November 2020
Published 24 December 2020 Volume 2020:12 Pages 1241—1251
DOI https://doi.org/10.2147/IJWH.S282733
Checked for plagiarism Yes
Review by Single anonymous peer review
Peer reviewer comments 3
Editor who approved publication: Professor Elie Al-Chaer
Gedefaye Nibret Mihretie, Amare Simegn, Agernesh Dereje, Habtamu Gebrehana, Adanech Getie, Bekalu Getnet, Alemu Degu
Department of Midwifery, College of Health Sciences, Debre Tabor University, Debre Tabor, Ethiopia
Correspondence: Gedefaye Nibret Mihretie Tel +251918159217
Email [email protected]
Introduction: While family planning (FP) is important throughout an individual’s and couple’s reproductive life, postpartum family planning (PPFP) focuses on the prevention of unintended and closely spaced pregnancies through the first 12 months following childbirth. However, modern contraception utilization practice during the postpartum period is underemphasized in Ethiopia.
Objective: This study aimed to assess postpartum modern contraceptive utilization and associated factors among postpartum women in Addis Zemen, South Gondar, Ethiopia in 2019.
Methods: Community-based cross-sectional study was conducted from January 1 to February 30, 2019 on 402 women. Study subjects were selected by simple random sampling technique. The data were collected by a structured and pretested, face-to-face, interviewer-administered questionnaire, entered into EpiData 4.2 and analyzed by using SPSS 23 software. Bivariate and multivariable analyses were used to examine the association. Odds ratio, 95% confidence interval (CI) and P-value < 0.05 were used to determine the statistical association.
Results: The prevalence of postpartum family planning utilization was 54.7%. Maternal educational status (adjusted odd ratio (AOR)=2.99, 95% CI (1.72, 5.19)), menses return (AOR=4.76, 95% CI (3.03, 7.48)), less than four alive children (AOR=3.61, 95% CI (1.51, 4.51)), postnatal care follow-up (AOR=2.96, 95% CI (1.57, 5.57)), length of time after delivery (AOR=1.80, 95% CI (1.16, 2.79)) and knowledge (AOR=1.69, 95% CI (1.07, 2.66)) were significantly associated with postpartum modern contraceptive utilization.
Conclusion: The postpartum modern contraceptive utilization was low. Therefore, health care providers should strengthen the integration of family planning services with maternal and child health service, provide health information about timely use of contraceptives and improve postnatal care follow-up after giving birth.
Keywords: postpartum, modern contraceptive, utilization, reproductive age, Addis Zemen, Ethiopia
Introduction
Family planning is described as the ability of individuals and couples to achieve their desired number of children in a family when they have children, the age range between children, and the timing of their births by using contraceptive methods.1 Postpartum family planning is defined as women who have ever used any type of family planning method within the first twelve months after she gave birth.2
Among pregnancy and childbirth related maternal and child health problems globally, failure of vaginal birth after cesarean delivery, increased risks of childhood undernourishment, stunted growth and child mortality are correlated with closely spaced births.3 In developing countries, the risk of low birth weight, prematurity and child mortality was high among women who had consecutive, closely spaced birth intervals less than 24 months.4 Maternal contraceptive utilization can prevent 3.2 million out of 5.6 million under five deaths and 109,000 out of 155,000 (70%) maternal deaths. However, statistics from 57 countries from a demographic health study found that 62% of women had an unmet need for contraceptive utilization.5 If all unmet need for modern contraceptive methods were satisfied, maternal mortality would decrease by almost 1/3from current levels, and unplanned pregnancies and unsafe abortions would decrease by 89–92%.6
According to the World Health Organization’s recommendation, after a woman has given birth, she should stay for at least two years before the next pregnancy to reduce the risk of adverse maternal, pre-natal and infant outcome.7 In Ethiopia, maternal mortality is an important public health issue; 412 per 100,000 live births are dying as result of complications related to pregnancy and childbirth.8 Provision of contraceptive can reduce maternal mortality by reducing the number of pregnancies, the number of abortions, and the proportion of births at high risk.9
Closely spaced pregnancies within twelve months of delivery increase the risks of preterm birth, low birth weight and small-for-gestational-age babies, risk of child mortality will also increase.10 Evidence in Ethiopia shows that almost half (47%) of all pregnancies occur within a short birth interval of less than 24 months after the previous birth.11 Postpartum women are an important group because, even if they are breastfeeding, they may not recognize they are at risk of unintended pregnancy.12 Maternal health services such as regular immunization services are a continuum point of contact to provide family planning information and link women to postpartum family planning services.13
Studies have shown that the prevalence of postpartum family planning utilization in Aksum town 2017, Debre Berhane 2016 and Dessie Town 2016 were 48%, 41.6% and 44%,14–16 respectively.
Different cross-sectional-based studies showed that reproductive health characteristics like resumed menses, resumed sexual intercourse and fertility desire,17 mothers who received antenatal care service,18 women who gave birth with the assistance of a skilled birth attendant,19 maternal age, educational status,20 religious,21 poor economic status,22 and knowledge about contraceptive method23 were significant factors of postpartum family planning utilization (Figure 1). Even though introduction of contraceptive during the postpartum period is very crucial, less emphasis is given in the first year after birth. Therefore, assessing postpartum modern contraceptive methods utilization and identifying factors affecting their utilization are very vital in designing, implementing and monitoring effective maternal and child health intervention.
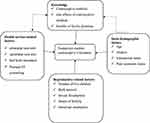 |
Figure 1 Conceptual framework for study done on postpartum modern contraceptive utilization and its associated factors among reproductive age women in Addis Zemen, South Gondar, Ethiopia, 2019. |
Method
Study Design
Community-based cross-sectional study was employed.
Study Setting
Addis Zemen is an administrative town of Libo Kemkem district which is located in South Gondar Zone 656 kilometers away from Addis Ababa, the capital city of Ethiopia. The town has an elevation of 2,216 meters above the sea level. The main source of income for Libo Kemkem wereda community is mixed agriculture. According to figures from the Central Statistical Agency in 2015, the estimated total population of the town is 42,983. The town has three kebeles (the smallest unit of the woreda) and 13,515 households. The town has one primary (district) hospital, one health center, and two private clinics. The total delivery within 2019 was 861 women.
Study Period
From January 1, 2019 to February 30, 2019.
Source and Study Population
All reproductive age (15–49) women who gave birth in the last 12 months and lived in Addis Zemen Town.
Sample Size Determination
A single population proportion formula was used to get the required sample size based on the following assumption by using: 95% confidence level, 5% margin of error and prevalence of postpartum family utilization planning (p=0.47).22 Then
n = z2 p (1-p)/d2); where z = level of confidence interval (1.96)2
Calculated sample size was: n = (1.96)2 * 0.47 (1–0.47)/(0.05)2, n = ~383
With 5% none respondent rate the final sample size was 402
Sampling Procedure
All three Kebeles of the town were included in this study. Then, sample frame was prepared in all selected kebeles to identify women who fulfill the inclusion criteria by having registered the birth date of the last child from family folders which was found from health extension workers. Based on the sample frame, house to house visit was conducted with their corresponding household identification number. Then, proportional to size allocation technique was employed to determine the study participants from each kebele.
Finally, reproductive age women whose last delivery was within the past one year prior to the study were selected using simple random sampling technique from the existing sampling frame. If the participant in the selected household was not present at the time of data collection, three revisits were made to interview the woman and if there were more than two participants in one household, one mother was selected by lottery method (Figure 2).
 |
Figure 2 Schematic representation of the sampling procedure among postpartum women in Addis Zemen Town, South Gondar Zone, Ethiopia, 2019. |
Variables
Dependent variable: postpartum modern contraceptive utilization (yes, no). Independent variables: socio demographic characteristics (age, marital status, educational status, religion, occupational status of the mother, husband educational status and occupation); reproductive and maternal health service use-related characteristics (parity, birth space, discuss with husband about postpartum family planning, previous history of contraceptive utilization, antenatal care follows up, postnatal care follows up, places of delivery, family planning counseling, birth attendants, menses return, length of time after delivery, pregnancy plan, want to have children for the future, resumed sexual intercourse); and knowledge on family planning (awareness of contraceptive use after birth, source of knowledge, source of FP, benefit of family planning).
Operational Definitions
Modern contraceptives: Sterilization (male and female), intrauterine devices, implants, oral contraceptives, condoms (male and female), injectables, emergency contraceptive pills and spermicidal agents26.
Postpartum period: the time from birth up to one year.27
Postpartum contraceptive utilization: women were considered as utilized when the women reported that she used any type of modern contraceptive method by herself or jointly with her husband from data collection time to the last 12 months after birth.14 The utilization was measured by mothers’ words by yes or no options for use (yes = 1, no = 0).
Knowledge of family planning: those participants who scored ≥50% considered “good knowledge” and <50% had ”poor knowledge” among knowledge question items.28
Data Collection Tools and Technique
A face to face, interviewer-based, structured questionnaire was used to collect the data. The questionnaire was first developed in English and translated to local language (Amharic) then back to English by language expertsto keep its consistency. Five health extension workers and two BSc midwives who were familiar with the local language and custom were recruited as data collectors and supervisors respectively. Training was given for data collectors and supervisors for two days on data collection procedures, interview techniques and confidentiality of the information obtained from the respondents. Finally, data collectors interviewed participants face to fac at home for 20–25 minutes.
Data Quality Assurance
Data quality was ensured during collection, entry and analysis. Before conducting the main study, pretest was carried out on 5% of the sample size and necessary modification has been made. The principal investigator and supervisors conducted a day-to-day on-site supervision during the whole period of data collection. At the end of each day, the questionnaires were reviewed and checked for completeness and accuracy by the supervisors and investigator. Then corrective discussion was undertaken by the research team members.
Data Analysis
After coding, the data were entered using Epi-data version 4.2 and then exported to SPSS version 23 software for analysis. Bivariate analysis was executed to examine crude association of predictors with postpartum contraceptive utilization. Finally, variables having p-values ≤0.2 on bivariate analysis were selected as candidates for multivariable analysis and then the independent effect of predictors on postpartum family planning utilization was determined. Odds ratio and 95% CI was used to measure the statistical association. P-values less than 0.05 were used to determine the statistical significance of the tests. Finally, the results were presented in texts, figure and tables.
Ethical Consideration
Ethical clearance for this study was obtained from ethical review committee of Debre Tabor University College of Health Sciences and supporting letter was written by department of midwifery to Addis Zemen Town health office. Informed consent for ≥ 18 year olds and assent for <18 years from their family was obtained after the purpose and objective of study was explained. To ensure confidentiality, names of respondents were replaced by code numbers.
Results
Socio-Economic and Demographic Characteristics of This Study
This study included a total of 402 postpartum child bearing age women with a response rate of 100%. All of the respondents (100%) were from urban area. The mean age of the study participants was 28.1 years (SD=±5.1). Majority of the respondents, 391 (97.3%),were Orthodox Christian followers and almost all (96.8%) of the respondents were married women (Table 1).
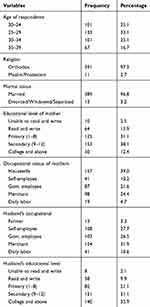 |
Table 1 Socio-Demographic Characteristics of Respondent at Addis Zemen Town, South Gondar, Ethiopia in June 2019 (n=402) |
Reproductive and Maternal Health Service Use-Related Characteristics of the Study Participants
Two hundred one (50.0%) participants had 2 to 4 children. Three hundred sixty-five (90.8%) of the respondents had at least one ANC service and 171 (42.5%) were counseled about family planning methods. Three hundred thirty-six (83.6%) respondents had planned pregnancy.
Among all women, 333 (82.2%) of them had no post-natal care. Among those who used postpartum contraceptive, 150 (80.2%) of the respondents got contraceptive from governmental institution. For 97.0% of the respondents were delivered at health institution where as 3.0% of them delivered at home. Three hundred eighty-eight (96.6%) deliveries were attended by midwives (Table 2).
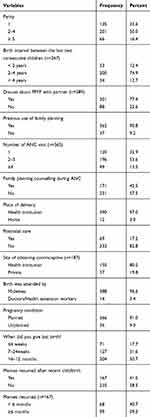 |
Table 2 Reproductive and Maternal Health Service Use-Related Characteristics of the Study Participants in Addis Zemen Town South Gondar, Northwest Ethiopia, 2019 (n=402) |
Knowledge About Postpartum Family Planning
The majority of participants (91.5%) had heard about modern contraceptive methods and more than half (62.2%) of them were knowledgeable about postpartum modern contraceptive (Table 3).
 |
Table 3 Knowledge and Discussion About Family Planning Among Postpartum Women in Addis Zemen Town South Gondar, Ethiopia in June 2019 (n=402) |
Contraceptive Use in Postpartum Period
Two hundred twenty (54.7%) respondents used modern postpartum contraceptive within the last twelve months after delivery. The most common contraceptive method used in this study was injectable which was 72.7%, followed by implants 10.9% (Figure 3).
 |
Figure 3 Methods used during postpartum period among respondents in Addis Zemen Town, South Gondar Zone, Ethiopia, in June 2019 (N=220). |
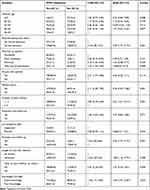
Factors Associated with Modern Postpartum Family Planning Utilization
First bi-variable logistic regression was conducted among different variables, only eleven variables with p-value of 0.2 or less were included in the multi-variable logistic regression. These variables were: maternal age, maternal educational status, maternal occupation, discuss with partner, menses return, number of alive children, antenatal care follow-up from last pregnancy, last pregnancy plan, postnatal care follow-up, the time interval between last birth to survey, fertility desire and knowledge.
As can be depicted from multivariable backward stepwise logistic regression, mothers with formal education, menses return after last birth, number of alive children ≤4, postnatal care follow-up, the time interval between last birth to survey and fertility desire were found to be significantly associated with postpartum family planning utilization.
Mothers with formal education were nearly 3 times (AOR=2.99, 95% CI (1.72, 5.19)), more likely to have postpartum modern contraceptive utilization as compared to those who had no formal education. The odds of having postpartum contraceptive utilization was higher among mothers whose menses was returned after last birth (AOR=4.76, 95% CI (3.03, 7.48)) than those who did not return the menses. Mothers who had less than four alive children were 3 times more likely to utilize modern contraceptive methods than their counterparts of mothers who had 5 or more alive children (AOR=3.61, 95% CI (1.51, 4.51)).
The odds of having modern contraceptive utilization among postpartum women were higher for mothers who had a history of postnatal care follow-up after last birth than those who did not have (AOR=2.96, 95% CI (1.57, 5.57)). Mothers who delivered before 6 months of the survey were nearly 2 times (AOR=1.80, 95% CI ((1.16, 2.79)), more likely to have postpartum contraceptive utilization as compared to those who gave birth within 6 months.
The odds of having postpartum utilization was higher among mothers who had good knowledge about postpartum modern contraceptive methods (AOR=1.69, 95% CI (1.07, 2.66)) than those who had poor knowledge. (Table 4).
Discussion
This study aimed to determine the prevalence of postpartum contraceptive utilization and identify factors that affect contraceptive utilization. The prevalence of postpartum contraceptive utilization was 54.7%, which was higher than studies conducted in Kenya (46%),29 Gondar Town (48.4%),21 Mexico (47%),30 Butajira (47%),21 Debre Birhan (41.6%),17 Nepal (32.8%),31 Oromia region (45.4%)32 and Uganda (28%).33 This disparity might be due to difference in study location, study residents and time period of the study. But this finding was also lower than study in Malawi (73%)23 and Addis Abeba (80.3%).32
In this study, the odds of having postpartum family planning utilization was higher among mothers who had no formal education as compared to their counterparts who attended formal education. Mothers who had formal education were 2.99 times more likely to utilize postpartum contraceptive as compared to mothers who had no formal education. This finding was supported by study conducted Uganda.33 This might be due to the fact that women with formal education are more likely to have better knowledge and decision-making ability for using modern contraceptives and other reproductive health services. Additionally, educated women might have better access of print media and social media that provide information about the benefit of postpartum family planning utilization.
In this study, mothers whose menses was resumed were 4.76 times more likely to use postpartum family planning utilization as compared to their counterparts who did not resume menses. This is consistent with a studies done in Gondar Town,21 Butajira,22 Nepal31 and Addis Abeba.32 This could be described by the fact that women who had resumed menses reflect themselves as susceptible to risk of unplanned pregnancy.
Women who had history of post-natal care service after the delivery of the last baby were more likely to experience postpartum family planning utilization practices than women who had no history of post-natal care service. This was supported by studies conducted in Butajira and Gida Ayana district Oromia region.22 This could be due to providing information during postnatal period about family planning by health care providers, help the women to agree and practice contraceptives utilization after delivery.
Maternal knowledge on postpartum contraceptive utilization was significantly associated with postpartum utilization. Mothers with good knowledge were 1.69 times more likely to initiate contraceptive utilization practices early as compared to those mothers who had poor knowledge. This finding was consistent with study conducted in Butajira.22 This might be due to the fact that mothers knowing the importance of postpartum family planning utilization and distinguishing the suggested time of starting postpartum family encourage mothers to initiate postpartum contraceptive utilization within one year after delivery.
Mothers who had less than four children were 2.61 times more likely to utilize postpartum contraceptive as compared to their counterparts. This finding was inversely related to the study conducted in Uganda.33 The reason for this might be due to younger women having relatively more knowledge about the time of postpartum contraceptive utilization because of exposure to social and print media as compared to older women.
The length of time after delivery was another factor which was significantly associated with postpartum utilization. Those mothers who had six months and above since the last birth were 1.8 times more likely to initiate postpartum contraceptive utilization practices as compared to those who were less than six months. This finding was consistent with study conducted in Addis Abeba32. This could be because as the duration of postpartum period increases sexual desire and activity also increase and then the women consider not using contraceptive in this time can expose to threat of unintended pregnancy.
Strength: the actual data were collected and community-based study design.
Limitation: memory bias might be introduced and this study’s focus on quantitative approach which could not address the “why” questions in detail.
Conclusion and Recommendation
The postpartum modern contraceptive utilization was low. Educational status of the mother, menses return, postnatal care follow-up, length of time after delivery and good knowledge about postpartum modern contraceptive method were significantly associated with postpartum modern contraceptive utilization. Therefore, health care providers should strengthen the integration of family planning services with maternal and child health services, provide health information about timely use of contraceptive and improve postnatal care follow-up after giving birth. Mixed quantitative and qualitative studies are better for further investigations to answer “why” questions.
Abbreviations
ANC, antenatal care; PPFP, postpartum family planning.
Data Sharing Statement
The data sets generated during this study are available from the corresponding author on reasonable request via email.
Acknowledgments
We are grateful to Debre Tabor University, College of Health Sciences for providing ethical clearance for this study. We would like to extend our thanks to Addis Zemen Town Health Office staff, study participants, supervisors and data collectors. This study was conducted in accordance with the Declaration of Helsinki. Addis Zemen Town Health Offices staffs support us by giving preliminary information. Participants, data collectors and supervisors were active participation and timely engaged data collection period.
Author Contributions
All authors contributed to data analysis, drafting or revising the article, have agreed on the journal to which the article will be submitted, gave final approval of the version to be published, and agree to be accountable for all aspects of the work.
Disclosure
The authors report no conflicts of interest for this work.
References
1. Bongaarts J, Cleland JC, Townsend J, Bertrand JT, Gupta MD. Family Planning Programs for the 21st Century: Rationale and Design. 2012.
2. World Health Organization. Programming Strategies for Postpartum Family Planning. 2013.
3. Kassebaum NJ, Bertozzi-Villa A, Coggeshall MS, et al. Global, regional, and national levels and causes of maternal mortality during 1990–2013: a systematic analysis for the global burden of disease study 2013. Lancet. 2014;384(9947):980–1004. doi:10.1016/S0140-6736(14)60696-6
4. Cleland J, Conde-Agudelo A, Peterson H, Ross J, Tsui A. Contraception and health. Lancet Ser. 2012;14:380.
5. Rossier C, Bradley SE, Ross J, Winfrey W. Reassessing unmet need for family planning in the postpartum period. Stud Fam Plann. 2015;46(4):355–367. doi:10.1111/j.1728-4465.2015.00037.x
6. Sundaram A, Vlassoff M, Bankole A, Remez L, Gebrehiwot Y. Benefits of meeting the contraceptive needs of Ethiopian women. Issues Brief (Alan Guttmacher Inst). 2010;1(1):1–8.
7. Garfield ME, Egan S, Temmermana M. It’s about time: WHO and partners release programming strategies for postpartum family planning. Glob J Health Sci. 2014;2(1).
8. CSACE I. Ethiopia Demographic and Health Survey 2016. Addis Ababa, Ethiopia, and Rockville, Maryland, USA: CSA and ICF; 2016.
9. Howie PW, McNEILLY AS, Houston MJ, Cook A, Boyle H. Fertility after childbirth: post‐partum ovulation and menstruation in bottle and breast feeding mothers. Clin Endocrinol (Oxf). 1982;17(4):323–332. doi:10.1111/j.1365-2265.1982.tb01597.x
10. USAID M. Family Planning Needs During the First Two Years Postpartum in the Ethiopia. WHO; 2005:13–15.
11. Borda MR, Winfrey W, McKaig C. Return to sexual activity and modern family planning use in the extended postpartum period: analysis of findings from seventeen countries. Afr J Reprod Health. 2010;14(4):75–80.
12. United states agency for international development/USAID. Maternal and Child Health Integrated Program; Family Planning Needs During the First Two-Year Postpartum Period in Ethiopia. 2012.
13. World health organization. Statement for Collective Action for Postpartum Family Planning. 2012.
14. Abraha TH, Teferra AS, Gelagay AA. Postpartum modern contraceptive use and associated factors in Northern Ethiopia: methodological Issues in this cross-sectional study. Epidemiol Health. 2017. doi:10.4178/epih.e2017019.r
15. Nigussie AT, Girma D, Tura G. Postpartum family planning utilization and associated factors among women who gave birth in the past 12 months, Kebribeyah Town, Somali Region, Eastern Ethiopia. J Womens Health. 2016;5(340):2167–2420.
16. Revanna R, Agadi N. Determinants of post-partum contraception practices in urban slums of central Karnataka, India. Indian J Community Health. 2016;28(3):280–285.
17. Demie T, Demissew T, Huluka T, Workineh F, Libanos H. Postpartum family planning utilization among postpartum women in public health institutions of Debre Berhan town, Ethiopia. J Womens Health Care. 2018;7(426):2167–2420. doi:10.4172/2167-0420.1000426
18. Tegegn M, Arefaynie M, Tiruye TY. Unmet need for modern contraceptives and associated factors among women in the extended postpartum period in Dessie town, Ethiopia. Contracept Reprod Med. 2017;2(1):21. doi:10.1186/s40834-017-0048-3
19. Eliason S, Baiden F, Quansah-Asare G, et al. Factors influencing the intention of women in rural Ghana to adopt postpartum family planning. Reprod Health. 2013;10(1):34. doi:10.1186/1742-4755-10-34
20. Mengesha ZB, Worku AG, Feleke SA. Contraceptive adoption in the extended postpartum period is low in Northwest Ethiopia. BMC Pregnancy Childbirth. 2015;15(160). doi:10.1186/s12884-015-0598-9
21. Abera Y, Mengesha ZB, Tessema GA. Postpartum contraceptive use in Gondar town, Northwest Ethiopia: a community based cross-sectional study. BMC Women’s Health. 2015;15(1):19. doi:10.1186/s12905-015-0178-1
22. Fantahun M. Assessment of Postpartum Contraceptive Adoption and Associated Factors in Butajira Health and Demographic Surveillance Site (HDSS). Southern Ethiopia: ADDIS ABABA UNIVERSITY; 2015.
23. Bwazi C, Maluwa A, Chimwaza A, Pindani M. Utilization of postpartum family planning services between six and twelve months of delivery at Ntchisi District Hospital, Malawi. Health. 2014;28:2014.
24. Demographic E. Health Survey Central Statistical Agency Addis Ababa. Ethiopia ICF International Calverton. Maryland, USA; 2011:180–186.
25. Teka TT, Feyissa TR, Melka AS, Bobo FT. Role of antenatal and postnatal care in contraceptive use during postpartum period in western Ethiopia: a cross sectional study. BMC Res Notes. 2018;11(1):581. doi:10.1186/s13104-018-3698-6
26. Hubacher D, Trussell J. A definition of modern contraceptive methods. Contraception. 2015;92(5):420–421. doi:10.1016/j.contraception.2015.08.008
27. Organization, W.H., WHO| family planning/contraception: fact sheet No 351; 2015. Available from: [
28. Gejo NG, Anshebo AA, Dinsa LH, Kabir R. Postpartum modern contraceptive use and associated factors in Hossana town. PLoS One. 2019;14(5):e0217167. doi:10.1371/journal.pone.0217167
29. Do M, Hotchkiss D. Relationships between antenatal and postnatal care and post-partum modern contraceptive use: evidence from population surveys in Kenya and Zambia. BMC Health Serv Res. 2013;13(1):6. doi:10.1186/1472-6963-13-6
30. Barber SL. Family planning advice and postpartum contraceptive use among low-income women in Mexico. Int Fam Plan Perspect. 2007;33(1):6–12. doi:10.1363/3300607
31. Joshi AK, Tiwari DP, Poudyal A, Shrestha N, Acharya U, Dhungana GP. Utilization of family planning methods among postpartum mothers in Kailali district, Nepal. Int J Womens Health. 2020;12:487. doi:10.2147/IJWH.S249044
32. Gebremedhin AY, Kebede Y, Gelagay AA, Habitu YA. Family planning use and its associated factors among women in the extended postpartum period in Addis Ababa, Ethiopia. Contracept Reprod Med. 2018;3(1):1. doi:10.1186/s40834-017-0054-5
33. Rutaremwa G, Kabagenyi A, Wandera SO, Jhamba T, Akiror E, Nviiri HL. Predictors of modern contraceptive use during the postpartum period among women in Uganda: a population-based cross-sectional study. BMC Public Health. 2015;15(1):262. doi:10.1186/s12889-015-1611-y
 © 2020 The Author(s). This work is published and licensed by Dove Medical Press Limited. The full terms of this license are available at https://www.dovepress.com/terms.php and incorporate the Creative Commons Attribution - Non Commercial (unported, v3.0) License.
By accessing the work you hereby accept the Terms. Non-commercial uses of the work are permitted without any further permission from Dove Medical Press Limited, provided the work is properly attributed. For permission for commercial use of this work, please see paragraphs 4.2 and 5 of our Terms.
© 2020 The Author(s). This work is published and licensed by Dove Medical Press Limited. The full terms of this license are available at https://www.dovepress.com/terms.php and incorporate the Creative Commons Attribution - Non Commercial (unported, v3.0) License.
By accessing the work you hereby accept the Terms. Non-commercial uses of the work are permitted without any further permission from Dove Medical Press Limited, provided the work is properly attributed. For permission for commercial use of this work, please see paragraphs 4.2 and 5 of our Terms.

