Back to Journals » International Journal of Chronic Obstructive Pulmonary Disease » Volume 11 » Issue 1
Peripheral blood eosinophils: a surrogate marker for airway eosinophilia in stable COPD
Authors Negewo N, McDonald V ![]() , Baines K
, Baines K ![]() , Wark P
, Wark P ![]() , Simpson J
, Simpson J ![]() , Jones P
, Jones P ![]() , Gibson P
, Gibson P
Received 11 November 2015
Accepted for publication 7 March 2016
Published 1 July 2016 Volume 2016:11(1) Pages 1495—1504
DOI https://doi.org/10.2147/COPD.S100338
Checked for plagiarism Yes
Review by Single anonymous peer review
Peer reviewer comments 4
Editor who approved publication: Prof. Dr. Richard Russell
Netsanet A Negewo,1,2 Vanessa M McDonald,1–4 Katherine J Baines,1,2 Peter AB Wark,1–3 Jodie L Simpson,1,2 Paul W Jones,5 Peter G Gibson1–3
1Priority Research Centre for Healthy Lungs, Faculty of Health and Medicine, The University of Newcastle, Callaghan, NSW, Australia; 2Hunter Medical Research Institute, Faculty of Health and Medicine, The University of Newcastle, Callaghan, NSW, Australia; 3Department of Respiratory and Sleep Medicine, John Hunter Hospital, Newcastle, NSW, Australia; 4School of Nursing and Midwifery, Faculty of Health and Medicine, The University of Newcastle, Callaghan, NSW, Australia; 5Institute for Infection and Immunity, St George’s, University of London, London, UK
Introduction: Sputum eosinophilia occurs in approximately one-third of stable chronic obstructive pulmonary disease (COPD) patients and can predict exacerbation risk and response to corticosteroid treatments. Sputum induction, however, requires expertise, may not always be successful, and does not provide point-of-care results. Easily applicable diagnostic markers that can predict sputum eosinophilia in stable COPD patients have the potential to progress COPD management. This study investigated the correlation and predictive relationship between peripheral blood and sputum eosinophils. It also examined the repeatability of blood eosinophil counts.
Methods: Stable COPD patients (n=141) were classified as eosinophilic or noneosinophilic based on their sputum cell counts (≥3%), and a cross-sectional analysis was conducted comparing their demographics, clinical characteristics, and blood cell counts. Receiver operating characteristic curve analysis was used to assess the predictive ability of blood eosinophils for sputum eosinophilia. Intraclass correlation coefficient was used to examine the repeatability of blood eosinophil counts.
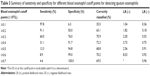
Results: Blood eosinophil counts were significantly higher in patients with sputum eosinophilia (n=45) compared to those without (0.3×109/L vs 0.15×109/L; P<0.0001). Blood eosinophils correlated with both the percentage (ρ=0.535; P<0.0001) and number of sputum eosinophils (ρ=0.473; P<0.0001). Absolute blood eosinophil count was predictive of sputum eosinophilia (area under the curve =0.76, 95% confidence interval [CI] =0.67–0.84; P<0.0001). At a threshold of ≥0.3×109/L (specificity =76%, sensitivity =60%, and positive likelihood ratio =2.5), peripheral blood eosinophil counts enabled identification of the presence or absence of sputum eosinophilia in 71% of the cases. A threshold of ≥0.4×109/L had similar classifying ability but better specificity (91.7%) and higher positive likelihood ratio (3.7). In contrast, ≥0.2×109/L offered a better sensitivity (91.1%) for ruling out sputum eosinophilia. There was a good agreement between two measurements of blood eosinophil count over a median of 28 days (intraclass correlation coefficient =0.8; 95% CI =0.66–0.88; P<0.0001).
Conclusion: Peripheral blood eosinophil counts can help identify the presence or absence of sputum eosinophilia in stable COPD patients with a reasonable degree of accuracy.
Keywords: sputum eosinophilia, diagnostic accuracy, chronic obstructive pulmonary disease, stability of eosinophil counts
Introduction
Airway eosinophilia, a hallmark feature of asthma, is now a recognized inflammatory pattern in chronic obstructive pulmonary disease (COPD).1–3 Eosinophilic COPD, defined as sputum eosinophils ≥3%, is reported during acute exacerbations in up to 28% of cases,4 and interestingly, in periods of disease stability, it is seen in approximately 34%5 (or 38%6) of COPD patients. Airway eosinophilia is a reliable predictor of responsiveness to inhaled and oral corticosteroid therapies in COPD.6–9
The detection and measurement of airway eosinophilia mostly require the assessment of induced sputum.2 Although sputum induction is considered a direct and reliable method of assessing airway inflammation, it has a number of limitations.10,11 In addition to being unsuitable for point-of-care testing, it requires expertise and may not be always successful (failure rate of up to 30%).10,11 Due to these reasons, the search for minimally invasive and easily applicable diagnostic tools that can predict sputum eosinophilia in COPD and asthma has intensified.4,10,12–15 The use of peripheral blood cell counts as a potential alternative is attracting profound interest owing to its ease of application in clinical practice. The ability of blood eosinophils to predict sputum eosinophilia in patients with asthma has been reported, with promising results.15–18 In COPD, however, very few studies have addressed this, particularly during clinical stability. A recent report in 20 COPD patients and 21 healthy controls has demonstrated the association between bronchial and blood eosinophil counts.19 Studies have also shown the potential ability of blood eosinophils to serve as a marker of response to corticosteroid treatments in exacerbating20 and stable21,22 COPD patients. The clinical characteristics of nonexacerbating COPD patients with persistently elevated levels of blood eosinophils (≥2%) and their longitudinal changes during a follow-up period of 3 years have also been investigated.3 Nevertheless, studies examining the utility of blood eosinophils in detecting sputum eosinophilia in stable COPD are still lacking.
In this study, we hypothesized that peripheral blood eosinophils can serve as a promising surrogate marker for sputum eosinophilia in stable COPD. To test this hypothesis, a cross-sectional analytical study of 141 stable COPD patients was conducted with the aim of investigating the correlation and predictive relationship between peripheral blood and sputum eosinophils. In addition, the stability of peripheral blood eosinophil counts between two measurements over a median period of 28 days was examined.
Methods
Study design
A cross-sectional analytical study was conducted involving 141 patients with stable COPD (Figure 1). The data for 71 participants were obtained from our previously published studies.5,23,24 The remaining 70 participants were recruited from the respiratory ambulatory care clinics at John Hunter Hospital (Newcastle, Australia), the clinical research databases of the Priority Research Centre for Asthma and Respiratory Disease at the University of Newcastle and the Hunter Medical Research Institute (Newcastle, Australia), and through community advertisement. All participants provided written informed consent, and ethics approval was obtained from the Human Ethics Research Committees of the Hunter New England Local Health District (12/12/12/3.06) and the University of Newcastle (H-2013-0010).
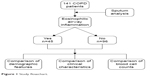  | Figure 1 Study flowchart. |
Study participants
Adults (n=141) with stable COPD and paired blood and sputum cell counts, which were obtained from samples collected during the same visit, were included. COPD diagnosis was confirmed by incompletely reversible airflow limitation (postbronchodilator forced expiratory volume in 1 second [FEV1] <80% predicted and FEV1 to forced vital capacity [FVC] ratio of <0.7). Stable COPD was defined as no increase in bronchodilator use, no use of oral corticosteroids or antibiotics, no unscheduled doctor’s visit, or no hospitalization due to COPD in the past 4 weeks. Participants were assessed for demographic features, lung function, airway and peripheral blood inflammatory cell counts, smoking history, body mass index, preceding year exacerbation history, medical history, dyspnea (modified Medical Research Council [mMRC]),25 comorbidities (Charlson Comorbidity Index),26 and health-related quality of life (St George Respiratory Questionnaire).27 The BODEx (body mass index, airflow obstruction, dyspnea, severe exacerbation) index was also calculated.28
Spirometry
Airflow limitation was assessed using spirometry (Medgraphics, CPFS/D™ USB Spirometer, BreezeSuite v7.1, MGC Diagnostics, Saint Paul, MN, USA) to measure pre- and postbronchodilator FEV1, FVC, and FEV1/FVC according to the standards of the American Thoracic Society.29 The third National Health and Nutrition Examination Survey reference equations were used to calculate percent predicted.30
Sputum induction and analysis
Sputum was induced using nebulized 4.5% saline in participants whose FEV1 was ≥1 L, using our previously described methods.31 In those with FEV1 <1 L, 0.9% saline was used. Lower respiratory sputum portions were selected and dispersed using dithiothreitol, and total cell count viability was performed. Cytospins were prepared, stained (May-Grunwald–Giemsa), and a differential cell count was obtained from 400 nonsquamous cells. Sputum samples obtained from all participants had squamous cell contamination less than 80% and were deemed adequate for further analysis.32 We defined eosinophilic COPD as sputum eosinophil count of ≥3%.33
Blood collection and analysis
Peripheral venous blood was collected into Vacutainer® tubes (BD Worldwide, North Ryde, NSW, Australia). Full blood counts were performed using standardized methods on a Beckman Coulter LH series analyzer (Beckman Coulter Ltd, Brea, CA, USA), through Hunter Area Pathology Service (Newcastle, Australia). The stability of peripheral blood eosinophils between two measurements, approximately 28 days apart, was evaluated in 46 participants who had repeated measurements of blood cell counts.
Statistical analysis
Data were analyzed using Stata 13 (Stata Corporation, College Station, TX, USA). Results are reported as mean ± standard deviation (SD) for normally distributed data and as median and interquartile range for nonparametric data. Student’s t-test was used for comparisons of normally distributed data, and Wilcoxon rank sum test was used for skewed data. Comparison of categorical data was done using Fisher’s exact test. Spearman’s rank correlation coefficient was used to examine the association between absolute blood cell counts/ratios and sputum eosinophils. Receiver operating characteristic (ROC) curves were generated, and the area under the curve (AUC) was calculated to assess the predictive relationship between blood and sputum eosinophils. Intraclass correlation coefficient and Bland–Altman plot were used to determine the agreement between two measurements of blood eosinophil counts. All results were reported as significant when P<0.05.
Results
Clinical characteristics
Table 1 presents the demographics and clinical characteristics of the 141 participants. Participants had a mean (SD) age of 69.8±7.7 years and mean postbronchodilator predicted FEV1 of 57.5%±17.9%. There were 89 (63.1%) males. Most of the participants (116, 82.3%) were ex-smokers with median pack-years of 37.5 (13.8, 62.5). In terms of GOLD (Global Initiative for Chronic Obstructive Lung Disease) grades, 11 (7.8%) patients were in GOLD I, 74 (52.5%) in GOLD II, 45 (31.9%) in GOLD III, and 11 (7.8%) in GOLD IV. With regard to the GOLD quadrants, using mMRC for symptom assessment, approximately half (53.9%) of the participants were in Quadrant D and 24.8% in Quadrant B. Over half (52.5%) were “frequent exacerbators”, having had two or more exacerbations in the past 12 months. Most (128, 90.8%) of the participants were prescribed maintenance inhaled corticosteroids (ICS) or ICS and long-acting β2 agonist (LABA) combination therapy (ICS/LABA), and of these, 102 (72.3% of the total population) participants were also taking long-acting muscarinic antagonists (LAMA).
Eosinophilic airway inflammation (sputum eosinophil count ≥3%) was present in 45 (31.9%) participants. Clinical characteristics were similar between those with sputum eosinophilia and those without, except for higher BODEx score (P=0.003) and more frequent high level of breathlessness (mMRC ≥2) (P=0.01) in the latter.
Peripheral blood cell counts/ratios
Both the absolute number and percentage proportion of blood eosinophils were significantly higher in eosinophilic COPD compared with noneosinophilic COPD (0.30×109/L vs 0.15×109/L, P<0.0001 and 3.95% vs 2.07%, P<0.0001, respectively) (Table 2, Figure 2A). Noneosinophilic participants had significantly elevated blood neutrophil counts compared with the eosinophilic group (5.3×109/L vs 4.6×109/L, P=0.02). There was no difference in blood lymphocytes (P=0.84) and total white blood cell counts (P=0.32) between the two groups. Participants with sputum eosinophilia had significantly higher blood eosinophil/neutrophil ratio (ENR) and eosinophil/lymphocyte ratio (ELR), whereas those without had significantly higher neutrophil/lymphocyte ratio (Table 2, Figure 2B–D).
Correlation between blood and sputum eosinophils
A significant correlation was found between blood eosinophil counts and the proportion (ρ=0.535; P<0.0001) (Figure 3A) and number of sputum eosinophils (ρ=0.473; P<0.0001) (Figure 3B). Similarly, percentage sputum eosinophils correlated reasonably well with both blood ELR (ρ=0.488; P<0.0001) and blood ENR (ρ=0.592; P<0.0001). No significant association was observed between percentage sputum neutrophils and blood neutrophil/lymphocyte ratio (ρ=0.0287; P=0.7355).
Receiver operating characteristic (ROC) curve analysis
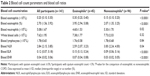
Absolute blood eosinophil count was predictive of sputum eosinophilia with AUC of 0.76 (95% confidence interval [CI] =0.67–0.84; P<0.0001) (Figure 4). Percentage blood eosinophils, blood ELR, and blood ENR were also predictive of sputum eosinophilia with AUCs of 0.80 (95% CI =0.73–0.86), 0.74 (95% CI =0.65–0.83), and 0.81 (95% CI =0.73–0.89), respectively. The sensitivities and specificities of different cutoff points of absolute blood eosinophil counts were evaluated together with their ability to correctly classify patients (Table 3). A summary of sensitivity and specificity for percentage blood eosinophils and blood ENR of different cutoff points is provided in the Supplementary material (Tables S1 and S2). The absolute blood eosinophil count threshold that balanced sensitivity and specificity on the ROC curve was found to be ≥0.3×109/L (300/μL), with a sensitivity of 60%, specificity of 76%, and a positive likelihood ratio of 2.5. At this cutoff point, blood eosinophil counts enabled the correct identification of the presence or absence of sputum eosinophilia in 71 cases out of 100. A higher cutoff point of ≥0.4×109/L (400/μL) gave a greater specificity (91.7%), a higher positive likelihood ratio (3.7), and an essentially similar classifying ability. In contrast, a higher degree of sensitivity (91.1%) was achieved at a peripheral blood eosinophil cutoff point of 0.2×109/L (200/μL).
Based on the peripheral blood eosinophil threshold of ≥0.3×109/L, 76% of the noneosinophilic participants (73 out of 96) would be correctly characterized as not having sputum eosinophilia (true negatives) while the remaining 24% as false positives. On the other hand, 60% of the eosinophilic participants (27 out of 45) would be accurately identified as having sputum eosinophilia (true positives) while the remaining 40% as false negatives. Two-by-two contingency tables for the blood eosinophil cutoff points of ≥0.2×109/L and ≥0.4×109/L are provided in the Supplementary material (Tables S3 and S4).
Clinical characteristics of participants classified by blood eosinophil counts
Blood eosinophilia (blood eosinophil count ≥0.4×109/L) was present in 22 (15.6%) participants (Table 4). Patients with blood eosinophilia had a higher postbronchodilator FEV1% predicted and a lower BODEx score compared to those without (<0.4×109/L). All other clinical parameters were similar between the two groups. There were no differences in blood eosinophil counts between males and females (0.2 [0.1, 0.3] ×109/L and 0.2 [0.1, 0.3] ×109/L; P=0.9087), ex-smokers and never smokers (0.2 [0.1, 0.3] ×109/L and 0.2 [0.1, 0.3] ×109/L; P=0.8848), frequent and nonfrequent exacerbators (0.2 [0.1, 0.3] ×109/L and 0.2 [0.1, 0.3] ×109/L; P=0.96), or between patients taking ICS(/LABA) and those who did not (0.2 [0.1, 0.3] ×109/L and 0.1 [0.1, 0.2] ×109/L; P=0.221).
Stability study
This study also assessed the stability of peripheral blood eosinophil counts in those participants who had repeated measurements of blood cell counts obtained from blood samples collected at two visits spaced a median of 28 (22.5, 35.5) days apart (n=46). There was a good agreement between the two measurements, with an intraclass correlation coefficient of 0.8 (95% CI =0.66–0.88; P<0.0001). The bias of measurement was negligible (0.002±0.13 [×109/L]), with equal scatter around the bias line, indicating no systematic measurement bias (Figure 5).
Discussion
This study, which assessed the ability of peripheral blood eosinophils for detecting sputum eosinophilia in stable COPD, had three main findings. First, peripheral blood eosinophil count was shown to distinguish patients with sputum eosinophilia from those without, thereby indicating its potential use as a diagnostic biomarker for eosinophilic COPD. Second, we have shown that blood eosinophil counts and their ratios (ELR and ENR) are elevated in eosinophilic COPD and correlate reasonably well with sputum eosinophilia. Third, blood eosinophil counts between two measurements over a median period of 28 days were found to be stable.
The diagnostic performance of peripheral blood eosinophils in identifying eosinophilic airway inflammation in mild, moderate, and severe asthma has been previously investigated.13–18,34 Studies examining the potential utility of blood eosinophils in COPD, particularly during stable conditions, are however few.3,19–21 One study in COPD has shown that peripheral percentage blood eosinophil count (>2%) can serve as a sensitive biomarker to determine sputum eosinophilia (>3%) during exacerbations (AUC 0.85 [95% CI =0.78–0.93], sensitivity =90%, specificity =60%).4 This AUC result is similar to our present AUC result in stable COPD.
As noted by Korevaar et al,14 optimal cutoff points for diagnostic biomarkers of airway eosinophilia selected by balancing sensitivity and specificity on a ROC curve may not be clinically applicable, given that their sensitivity and/or specificity is often suboptimal compared to that of reference standard tests, such as bronchoalveolar lavage and sputum induction. From the clinical point of view, the choice of a cutoff point is also partly determined by the clinical question. In view of this, we have evaluated the sensitivity and specificity of blood eosinophil counts at different cutoff points (Table 3). According to our data, in patients with stable COPD, peripheral blood eosinophil counts can help correctly identify the presence or absence of sputum eosinophilia in 71 cases out of 100 at cutoff points of ≥0.3×109/L or ≥0.4×109/L. Nevertheless, the higher cutoff point had a higher positive predictive value (PPV) (number of true positives/[number of true positive + number of false positives]) and a much better specificity to rule in sputum eosinophilia. This implies that patients with blood eosinophil counts above the threshold of 0.4×109/L would most likely have COPD with eosinophilic airway inflammation. Akin to the suggestion of Fowler et al,17 such patients may not necessarily need to undergo induction of sputum for the assessment of airway eosinophilia. Patients with blood eosinophil count of <0.4×109/L may however need further assessment because the proportion of false negatives at the cutoff point of 0.4×109/L is high (~69%). As a matter of interest, a similar blood eosinophil cutoff point of ≥0.45×109/L has been reported to help correctly identify sputum eosinophilia in patients with severe asthma with a specificity of 97%, sensitivity of 49.3%, and PPV of 89.2.17 Another recent study has also reported a blood eosinophil cutoff point of ≥0.41×109/L (specificity of 95%, sensitivity of 36%, and PPV of 79) for detecting sputum eosinophilia in a population of asthmatic patients of different phenotypes.15
For a clinician who wants to rule out sputum eosinophilia, on the other hand, a peripheral blood eosinophil cutoff point with a high sensitivity would be of interest. Based on our results, patients are unlikely to have sputum eosinophilia if their blood eosinophil count is below 0.2×109/L because the sensitivity at the cutoff point of 0.2×109/L is 91.1%.
It is interesting to note that in our study, there was discordance between sputum and blood eosinophils in approximately 40% of the patients with eosinophilic COPD at a peripheral blood eosinophil cutoff point of 0.3×109/L. This observation is similar to that of a recent study in patients with uncontrolled asthma where one-third of the participants exhibited discordance between blood and sputum eosinophils.35 In order to gain a better insight into our true-positive (27 patients) and false-negative (18 patients) cohorts, their demographic features, clinical characteristics, and sputum cell counts were compared. The results nevertheless revealed no significant difference between the two groups (Table S5). However, it should be highlighted that this analysis may have been underpowered due to small sample size.
Plausible causes for the discordance between sputum and blood eosinophils may include the imbalance between the production and subsequent clearance of eosinophils by airway macrophages36 and variations in the process of recruitment of eosinophils into the airways.35 The fact that only a proportion of the eosinophilic COPD patients had blood eosinophilia may suggest the involvement of more than one distinct biological mechanisms underlying eosinophilic airway inflammation within this COPD phenotype.37 As in the case of asthma, Th2 cytokines could be responsible for inflammation in eosinophilic COPD.37 Nevertheless, eosinophilic airway inflammation in the absence of elevated levels of Th2 has also been reported in some COPD patients.38 One potential mechanism for the non-Th2 eosinophilic inflammation in COPD could be the epithelial-innate lymphoid cell type 2 (ILC2) pathway, which has been suggested to play a similar role in severe nonallergic asthma.39 Obviously, further investigation is warranted to understand the mechanism underlying the different endotypes of the eosinophilic COPD phenotype.
Our data demonstrated that blood eosinophils and their ratios (ELR and ENR) were elevated in patients with sputum eosinophilia compared with those without. Absolute blood eosinophil counts correlated reasonably well with both the absolute sputum counts and percentage sputum eosinophils, which is in agreement with the findings of Wagener et al,18 Zhang et al,16 and Fowler et al17 in asthma, but not with those of Hastie et al34 and Amorim et al.40 In accordance with a previous finding in asthma,16 in our study, both blood ENR and ELR also correlated with percentage sputum eosinophils and were predictive of eosinophilic COPD with AUCs of 0.81 and 0.74, respectively. Recently, Khatry et al41 have suggested that ratios of blood cell types, such as ELR and ENR, may minimize variations associated with measurement, sample processing, and therapies and yield a more accurate diagnostic performance over actual blood cell counts. This certainly will be a topical issue for future studies in COPD.
According to Price et al,42 blood eosinophilia (defined as ≥0.5×109/L) occurs in 10% of stable COPD patients and is associated with higher rate of exacerbations, particularly in nonsmokers receiving maintenance therapy. Elevated levels of blood eosinophils in COPD patients have also been associated with increased risk of mortality from exacerbations.43 Nevertheless, our analysis indicated no significant difference in blood eosinophil counts between frequent and nonfrequent exacerbators. Similarly, there was no difference in the number of severe exacerbations in the past 12 months between patients with blood eosinophilia (≥0.4×109/L) and those without (<0.4×109/L). It is worth noting here that up to 90% of our study population was using either ICS/LABA alone or in combination with LAMA, which are known to reduce the risk of exacerbation. All things considered, the aforementioned discrepancies may possibly be due to differences in the characteristics of study populations.
In our study, the stability of peripheral blood eosinophil counts between two measurements over a median period of 28 days was found to be acceptable. This implies that a single measurement of blood eosinophil count may provide indicative information about eosinophilic airway inflammation status in stable COPD. The stability of peripheral blood eosinophil counts in repeated measurements in COPD population has been reported in other studies as well.20,21
Conclusion
In this study, we found a predictive relationship between blood and sputum eosinophils in stable COPD. Peripheral blood eosinophils were stable between two measurements, suggesting that a single blood eosinophil count may potentially serve as a reliable marker for eosinophilic COPD. A potential limitation of this study may be the fact that we did not have bronchoalveolar lavage or endobronchial biopsy samples for the assessment of airway eosinophilia.
The clinical relevance of our work lies in the fact that a simple blood test may allow the clinician to positively diagnose eosinophilic COPD. In relation to this, the question of when to use ICS in COPD is of high clinical importance. Biomarkers that allow for the identification of patients who are most likely to respond to ICS, and consequently minimize harm arising from inappropriate treatment, have the potential to significantly progress COPD management. In this regard, it will be interesting and a worthwhile endeavor to examine ICS response at different blood eosinophil thresholds in future prospective studies.
Acknowledgments
This study was supported by National Health and Medical Research Council (NHMRC), Australia, Grant ID: 1045230 (PGG, VMM, JLS, PABW); Ramaciotti Foundation (VMM); Lung Foundation of Australia (VMM); National Health and Medical Research Council (NHMRC), Australia, Grant ID: 455508 (2007–2010); and Priority Research Centre for Asthma and Respiratory Diseases PhD Scholarship and Emlyn and Jennie Thomas Postgraduate Medical Research Scholarship through the Hunter Medical Research Institute (NAN). The authors wish to acknowledge Kelly Steel, Amber Smith, Hayley Lunn, Penny Baines, Gabrielle LeBrocq, Brooke Emmett, Clare Powell, and Hayley Candler for their role in data collection; Kellie Fakes, Bridgette Donati, and Michelle Gleeson for their role in sample processing; and Heather Powell for statistical advice.
Disclosure
VMM has received grants from Ramaciotti Foundation, NHMRC, Lung Foundation of Australia during the conduct of the study; personal fees and honoraria for education and advisory boards from Menarini and personal fees from GSK, Novartis, and Astra Zeneca outside this work. KJB reports research fellowship from The Thoracic Society of Australia and New Zealand/National Asthma council. PGG is supported by a NHMRC practitioner fellowship and has received speakers fees from GlaxoSmithKline, Boehringer Ingelheim, AstraZeneca, and Novartis outside this work. PWJ reports being employed as a global medical expert by GSK. The authors report no other conflicts of interest in this work.
References
Saha S, Brightling CE. Eosinophilic airway inflammation in COPD. Int J Chron Obstruct Pulmon Dis. 2006;1(1):39–47. | ||
Brightling CE. Clinical applications of induced sputum. Chest. 2006;129(5):1344–1348. | ||
Singh D, Kolsum U, Brightling CE, Locantore N, Agusti A, Tal-Singer R; for ECLIPSE investigators. Eosinophilic inflammation in COPD: prevalence and clinical characteristics. Eur Respir J. 2014;44(6):1697–1700. | ||
Bafadhel M, McKenna S, Terry S, et al. Acute exacerbations of chronic obstructive pulmonary disease: identification of biologic clusters and their biomarkers. Am J Respir Crit Care Med. 2011;184(6): 662–671. | ||
McDonald VM, Higgins I, Wood LG, Gibson PG. Multidimensional assessment and tailored interventions for COPD: respiratory utopia or common sense? Thorax. 2013;68(7):691–694. | ||
Leigh R, Pizzichini MM, Morris MM, Maltais F, Hargreave FE, Pizzichini E. Stable COPD: predicting benefit from high-dose inhaled corticosteroid treatment. Eur Respir J. 2006;27(5):964–971. | ||
Brightling CE, Monteiro W, Ward R, et al. Sputum eosinophilia and short-term response to prednisolone in chronic obstructive pulmonary disease: a randomised controlled trial. Lancet. 2000;356(9240):1480–1485. | ||
Brightling CE, McKenna S, Hargadon B, et al. Sputum eosinophilia and the short term response to inhaled mometasone in chronic obstructive pulmonary disease. Thorax. 2005;60(3):193–198. | ||
Pizzichini E, Pizzichini MM, Gibson P, et al. Sputum eosinophilia predicts benefit from prednisone in smokers with chronic obstructive bronchitis. Am J Respir Crit Care Med. 1998;158(5 Pt 1): 1511–1517. | ||
Pavord ID, Bafadhel M. Exhaled nitric oxide and blood eosinophilia: independent markers of preventable risk. J Allergy Clin Immunol. 2013;132(4):828–829. | ||
Baines KJ, Pavord ID, Gibson PG. The role of biomarkers in the management of airways disease. Int J Tuberc Lung Dis. 2014;18(11): 1264–1268. | ||
Pavord ID, Gibson PG. Inflammometry: the current state of play. Thorax. 2012;67(3):191–192. | ||
Yap E, Chua WM, Jayaram L, Zeng I, Vandal AC, Garrett J. Can we predict sputum eosinophilia from clinical assessment in patients referred to an adult asthma clinic? Intern Med J. 2013;43(1):46–52. | ||
Korevaar DA, Westerhof GA, Wang J, et al. Diagnostic accuracy of minimally invasive markers for detection of airway eosinophilia in asthma: a systematic review and meta-analysis. Lancet Respir Med. 2015;3(4):290–300. | ||
Westerhof GA, Korevaar DA, Amelink M, et al. Biomarkers to identify sputum eosinophilia in different adult asthma phenotypes. Eur Respir J. 2015;46(3):688–696. | ||
Zhang XY, Simpson JL, Powell H, et al. Full blood count parameters for the detection of asthma inflammatory phenotypes. Clin Exp Allergy. 2014;44(9):1137–1145. | ||
Fowler SJ, Tavernier G, Niven R. High blood eosinophil counts predict sputum eosinophilia in patients with severe asthma. J Allergy Clin Immunol. 2015;135(3):822–824.e822. | ||
Wagener AH, de Nijs SB, Lutter R, et al. External validation of blood eosinophils, FE (NO) and serum periostin as surrogates for sputum eosinophils in asthma. Thorax. 2015;70(2):115–120. | ||
Eltboli O, Mistry V, Barker B, Brightling CE. Relationship between blood and bronchial submucosal eosinophilia and reticular basement membrane thickening in chronic obstructive pulmonary disease. Respirology. 2015;20(4):667–670. | ||
Bafadhel M, McKenna S, Terry S, et al. Blood eosinophils to direct corticosteroid treatment of exacerbations of chronic obstructive pulmonary disease: a randomized placebo-controlled trial. Am J Respir Crit Care Med. 2012;186(1):48–55. | ||
Pascoe S, Locantore N, Dransfield MT, Barnes NC, Pavord ID. Blood eosinophil counts, exacerbations, and response to the addition of inhaled fluticasone furoate to vilanterol in patients with chronic obstructive pulmonary disease: a secondary analysis of data from two parallel randomised controlled trials. Lancet Respir Med. 2015;3(6):435–442. | ||
Siddiqui SH, Guasconi A, Vestbo J, et al. Blood eosinophils: a biomarker of response to extrafine beclomethasone/formoterol in chronic obstructive pulmonary disease. Am J Respir Crit Care Med. 2015;192(4):523–525. | ||
Simpson JL, Powell H, Baines KJ, et al. The effect of azithromycin in adults with stable neutrophilic COPD: a double blind randomised, placebo controlled trial. PLoS One. 2014;9(8):e105609. | ||
McDonald V, Gibson PG, Scott H, et al. Should we treat obesity in COPD? The effects of diet and exercise training. Respirology. 2016; doi:10.1111/resp.12746. | ||
Bestall JC, Paul EA, Garrod R, Garnham R, Jones PW, Wedzicha JA. Usefulness of the Medical Research Council (MRC) dyspnoea scale as a measure of disability in patients with chronic obstructive pulmonary disease. Thorax. 1999;54(7):581–586. | ||
Charlson ME, Pompei P, Ales KL, MacKenzie CR. A new method of classifying prognostic comorbidity in longitudinal studies: development and validation. J Chronic Dis. 1987;40(5):373–383. | ||
Jones PW, Quirk FH, Baveystock CM, Littlejohns P. A self-complete measure of health status for chronic airflow limitation. The St George’s respiratory questionnaire. Am Rev Respir Dis. 1992;145(6):1321–1327. | ||
Soler-Cataluna JJ, Martinez-Garcia MA, Sanchez LS, Tordera MP, Sanchez PR. Severe exacerbations and BODE index: two independent risk factors for death in male COPD patients. Respir Med. 2009;103(5):692–699. | ||
Standardization of Spirometry, 1994 Update. American Thoracic Society. Am J Respir Crit Care Med. 1995;152(3):1107–1136. | ||
Hankinson JL, Odencrantz JR, Fedan KB. Spirometric reference values from a sample of the general US population. Am J Respir Crit Care Med. 1999;159(1):179–187. | ||
Gibson PG, Wlodarczyk JW, Hensley MJ, et al. Epidemiological association of airway inflammation with asthma symptoms and airway hyperresponsiveness in childhood. Am J Respir Crit Care Med. 1998;158(1):36–41. | ||
Fahy JV, Boushey HA, Lazarus SC, et al. Safety and reproducibility of sputum induction in asthmatic subjects in a multicenter study. Am J Respir Crit Care Med. 2001;163(6):1470–1475. | ||
Pavord ID, Brightling CE, Woltmann G, Wardlaw AJ. Non-eosinophilic corticosteroid unresponsive asthma. Lancet. 1999;353(9171):2213–2214. | ||
Hastie AT, Moore WC, Li H, et al. Biomarker surrogates do not accurately predict sputum eosinophil and neutrophil percentages in asthmatic subjects. J Allergy Clin Immunol. 2013;132(1):72–80. | ||
Schleich FN, Chevremont A, Paulus V, et al. Importance of concomitant local and systemic eosinophilia in uncontrolled asthma. Eur Respir J. 2014;44(1):97–108. | ||
Kulkarni NS, Hollins F, Sutcliffe A, et al. Eosinophil protein in airway macrophages: a novel biomarker of eosinophilic inflammation in patients with asthma. J Allergy Clin Immunol. 2010;126(1):61–69.e63. | ||
Woodruff PG, Agusti A, Roche N, Singh D, Martinez FJ. Current concepts in targeting chronic obstructive pulmonary disease pharmacotherapy: making progress towards personalised management. Lancet. 2015;385(9979):1789–1798. | ||
Ghebre MA, Bafadhel M, Desai D, et al. Biological clustering supports both “Dutch” and “British” hypotheses of asthma and chronic obstructive pulmonary disease. J Allergy Clin Immunol. 2015;135(1):63–72.e10. | ||
Brusselle G, Bracke K. Targeting immune pathways for therapy in asthma and chronic obstructive pulmonary disease. Ann Am Thorac Soc. 2014;11(Suppl 5):S322–S328. | ||
Amorim MM, Fernandes PB, Caetano LB, Dracoulakis S, Santoro IL, Fernandes AL. Nasal lavage is better than blood count in predicting sputum eosinophilia. Clin Exp Allergy. 2015;45(5):1006–1008. | ||
Khatry DB, Gossage DL, Geba GP, et al. Discriminating sputum-eosinophilic asthma: accuracy of cutoffs in blood eosinophil measurements versus a composite index, ELEN. J Allergy Clin Immunol. 2015;136(3):812–814.e812. | ||
Price D, Rigazio A, Postma D, et al. Blood eosinophilia and the number of exacerbations in COPD patients [abstract]. ERJ. 2014;44(Suppl 58):4416. | ||
Hospers JJ, Schouten JP, Weiss ST, Rijcken B, Postma DS. Asthma attacks with eosinophilia predict mortality from chronic obstructive pulmonary disease in a general population sample. Am J Respir Crit Care Med. 1999;160(6):1869–1874. |
 © 2016 The Author(s). This work is published and licensed by Dove Medical Press Limited. The
full terms of this license are available at https://www.dovepress.com/terms
and incorporate the Creative Commons Attribution
- Non Commercial (unported, 3.0) License.
By accessing the work you hereby accept the Terms. Non-commercial uses of the work are permitted
without any further permission from Dove Medical Press Limited, provided the work is properly
attributed. For permission for commercial use of this work, please see paragraphs 4.2 and 5 of our Terms.
© 2016 The Author(s). This work is published and licensed by Dove Medical Press Limited. The
full terms of this license are available at https://www.dovepress.com/terms
and incorporate the Creative Commons Attribution
- Non Commercial (unported, 3.0) License.
By accessing the work you hereby accept the Terms. Non-commercial uses of the work are permitted
without any further permission from Dove Medical Press Limited, provided the work is properly
attributed. For permission for commercial use of this work, please see paragraphs 4.2 and 5 of our Terms.








