Back to Journals » Infection and Drug Resistance » Volume 12
Next-generation-sequencing technology used for the detection of Mycoplasma hominis in renal cyst fluid: a case report
Authors Xiao N , Gai W, Hu WG, Li JX, Zhang Y, Zhao XY
Received 18 December 2018
Accepted for publication 5 April 2019
Published 23 May 2019 Volume 2019:12 Pages 1073—1079
DOI https://doi.org/10.2147/IDR.S198678
Checked for plagiarism Yes
Review by Single anonymous peer review
Peer reviewer comments 2
Editor who approved publication: Professor Suresh Antony
Nan Xiao,1 Wei Gai,2 Wei-Guo Hu,1 Jian-Xing Li,1 Yan Zhang,2 Xiu-Ying Zhao1
1Department of Clinical Laboratory, Beijing Tsinghua Changgung Hospital, School of Clinical Medicine, Tsinghua University, Beijing, People’s Republic of China; 2National Engineering Research Center for Beijing Biochip Technology, Beijing, People’s Republic of China
Background: Mycoplasma is an opportunistic pathogen causing both urogenital and extragenital infections. The lack of cell wall renders Mycoplasma difficult to culture and identify with ordinary methods. Next-generation sequencing (NGS) is a new technology helping a lot in the diagnosis of infective diseases. In this case, NGS played a key role in the diagnosis of Mycoplasma infection.
Case presentation: A mid-aged man suffering from renal cyst underwent cyst incision followed by invasive treatments to eliminate hematoma caused by renal artery hemorrhage. After the cyst incision operation, the patient had a persistent high temperature. The persistent increase of blood neutrophile granulocyte count and C-reaction protein suggested an unresolved infection. The empirically chosen anti-infective agents were meropenem and linezolid since the ordinary bacterial cultures of surgical site drainage and blood yielded a negative result. At postoperation day (POD) 17, NGS result of his drainage clearly indicated the pathogen was Mycoplasma hominis. At POD 24, the drug sensitivity test showed resistance to quinolones, clarithromycin and erythromycin, but intermediate to azithromycin. Since then, the antimicrobial agents were changed into azithromycin and kept unchanged until the patient was fully recovered and discharged at POD 39.
Conclusion: When the ordinary laboratory diagnostic methods failed, NGS diagnosis could reduce the hospitalization expenses and shorten the lengths of hospital stay.
Keywords: NGS, Mycoplasma, renal cyst, infection
Introduction
Mycoplasma species are often isolated from genitourinary system from healthy adults and sometimes cause upper genitourinary tract infection.1 It is also reported being isolated from several different categories of extragenital infections.2 The growth of untypical bacterial pathogens such as Mycoplasma needs special growth media3 or commercially available kits.4,5 Next-generation sequencing (NGS) is a powerful new technology to uncover the identity of pathogens which was difficult to be identified by traditional methods.6 In this case, NGS helps to diagnose the infection of Mycoplasma hominis (M. hominis) in a renal cyst and hematoma of a patient without immunosuppression.
Case presentation
Medical history and preliminary diagnosis
A 54-year-old male patient with Han nationality was presented in the Department of Urology of a tertiary hospital, because of a cyst in the right kidney. The cyst was found 5 years ago during a physical examination, and it was left untreated until recently it became obviously bigger. The patient reported a past history of hypertension for 2 years, whose highest record was 140/90 mmHg. He had taken bisoprolol 2.5 mg qd for treatment. No history of other disorders was reported.
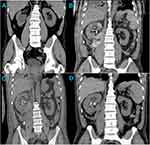
The preoperation computed tomography (CT) showed that the middle and low pole of the right kidney had elliptical cystic which had low density with clear border and no enhancement. And there was also an adrenal nodular hyperplasia presented in the left adrenal (Figure 1A). And the patient also had a ++++ leukocyte esterase urinalysis result which equaled ≥500 WBC/mL. The diagnoses of the patient were 1) acquired renal cyst, 2) benign adrenal tumors, 3) hypertension, 4) urinary tract infection.
Surgical operations
The patient undertook a selective operation during which surgeons performed a renal cyst incision with flexible ureteroscope. After general anesthesia, Storz ureteroscope was placed through the urethra. According to preoperative CT image localization, laser (1.0 J × 20 Hz) was used to incise the mucosal wall of the bulging collecting system. There were loose tissues and no clear cyst wall. Ultrasound-guided puncture of right kidney cyst was performed. The incision was about 1.5 cm without bleeding. Double-J tube and catheter were indwelled after the operation.
At postoperation day (POD) 2, patient suffered from abdominal distension and pain, with the drop of blood pressure and hemoglobin. Bedside color Doppler ultrasonography showed that a moderate echo mass was in front of psoas major muscle about 5 cm from the lower pole of right kidney. Renal artery embolization was performed successfully under local anesthesia, and renal artery branch hemorrhage was found during the operation (Figure 1B).
Three days later (POD 5), the patient’s hemoglobin was 79 g/L. He suffered from tachycardia and atrial fibrillation. Four units of suspended red blood cell and 400 mL plasma were transfused. Since the symptom of cardiac and pulmonary insufficiency caused by abdominal distention, diaphragmatic elevation and compression of the lungs cannot be relieved, the patient undertook the removal of the retroperitoneal hematoma. After the operation, he was moved to intensify care unit (ICU).
Course of the disease after operations
Because of the renal artery hemorrhage and the damage of the right renal structure, the patient suffered from perirenal and retroperitoneal hematoma. The efficient drainage helped with the reducoin of the hematoma and suspected urinary fistula. Four times of CT results before and after the invasive operations are shown in Figure 1. However, since the cyst incision operation, the inflammatory markers were high, which included body temperature, blood neutrophile granulocyte count (NEUT) and C-reaction protein, suggesting an infection statue of the patient (Figure 2).
 | Figure 2 Blood neutrophile granulocyte count (NEUT 108/L), C-reaction protein (CRP mg/L) and body temperatures from before-operation-day (BOD) 1 to POD 37. |
The steadily high levels of inflammatory markers necessitated anti-infective agents. The timeline of the invasive operations, symptoms and anti-infective medicine prescriptions is shown in Figure 3. At POD 3–4, cefimazole was prescribed when the patient was in the urology ward. When he was moved to ICU, the drug was changed into cefoperazone/sulbactam for 3 days. Nevertheless, the cephalosporin prescripts seemed not helpful to his symptoms. At POD 8–17, meropenem and linezolid were used instead of cephalosporin. The symptoms and CT results gradually improved (Figure 1C). During these days, all the bacteria cultures of drainage and blood yielded a negative result. However, some pin-point colonies were detected on the Columbia blood agar (CBA) plate and chocolate agar (Figure 4). The Gram stain failed to reveal any identifiable shapes of a typical bacterium. And the identity of the colonies could not be resolved with commonly used bacterial identification methods available in our laboratory. By the time, meropenem and linezolid seemed effective since his condition gradually improved though the infective pathogens were unknown. At POD 14, the drainage was sent for next-generation-sequencing (NGS). The result showed a M. hominis infection (Table 1, Figure 5), which was reported to the attending doctor at POD 17. The anti-infective agents were changed empirically to fosfomycin and levofloxacin. And the prescript was changed to azithromycin after the sensitivity test result was reported. It was kept the same until the inflammatory markers regained their normal levels and CT results showed this treatment was effective (Figure 1D). The patient was fully recovered and discharged at POD 39.
 | Table 1 NGS result |
 | Figure 3 The timeline of this case with the times of invasive operation, symptoms and the prescripts of anti-infective agents. |
 | Figure 4 The coverage profile and phylogenetic tree of the M. hominis strain X. |
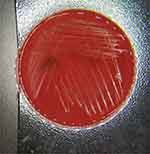 | Figure 5 The pin-point colonies grew on CBA plate. |
After been discharged from the hospital, the patient was called to come back to do a CT scan as follow-up evaluation. He simply dismissed the requirement and did not come back so far.
The NGS result and anti-infective drug sensitivity result
The result of NGS showed that the most prominent pathogen was M. hominis which had the highest reads count and the estimated copy number and designed as M. hominis strain X (Table 1). The genomic sequence of the strain X was reconstructed. According to the sequence of strain X and the data download from NCBI BLAST, a phylogenetic tree was constructed with maximum likelihood method by MEGA 7.0. The phylogenetic tree used HF559394.1 Mycoplasma cynos C142 as outgroup. The closest strain to strain X was CP009652.1 M. hominis ATCC 27545 and CP011538.1 M. hominis strain sprout (Figure 4).
The anti-infective drug sensitivity test was done with M. hominis IST (BioMerieux, France), which is a widely applied commercial Mycoplasma culture, detecting and drug sensitivity test kit with satisfying sensitivity and specificity4,5. The result is show in Table 2. And the strain X had resistance to quinolones, clarithromycin and erythromycin. The sensitivity to azithromycin was intermediate.
 | Table 2 Anti-infective drug sensitivity result |
Discussion and conclusion
Mycoplasma species lack a cell wall and grow relatively slowly. M. hominis appears as an amorphous mass when being Gram-stained, and its identification and anti-infective agent sensitivity test with routine culture methods are difficult.7 The M. hominis is frequently isolated from the lower genitourinary system from healthy adults and is sometimes responsible for infections of the upper genitourinary tract.1 Asymptomatic carriage of this bacterium is common, and the majority of individuals do not develop any disease.8 Some researchers believed it had some debatable negative effect on men fertility.9 The M. hominis is also reported being isolated from extragenital infection. Categories of such infections include septicemia, joint infections, central nervous system infections, respiratory tract infections and wound infections2. It was reported as a likely pathogen causing a hematoma or perinephric abscess in renal transplantation receipts.7,10–12 Nevertheless, sometimes normal people could suffer from hematoma and abscess caused by M. hominis infection.13
The patient in this case was basically a middle-aged man who had no obvious underlying disease leading to a possible immunosuppressive statue. He suffered from a renal cyst in right kidney. After the cyst was incised, renal artery hemorrhage occurred and he underwent two extrainvasive operations to stop the bleeding and eliminate the hematoma. Since he reported having hypertension for 2 years, we suspect it was the possible cause of the renal artery bleeding. He experienced a long-term fever indicting infection but without any culture finding. The culture media used for routine bacterial culture in our laboratory included CBA, MacConkey agar and chocolate agar, neither of which is the suitable growth media for Mycoplasma. The identity of the pin-point colonies was a frustrating myth which could not be solved by the routine methods available in our lab, including BioMerieux Compact II (France) and MALDI-TOF (Bruker, Germany). The NGS helped us uncover this finding and rendered it possible to do Mycoplasma drug sensitivity test.
The drug sensitivity test showed that the M. hominis strain X was resistant to most macrolide agents and quinolones. The drug sensitivity pattern was similar to previous reports.14,15 Although the drug sensitivity test showed that the tetracycline was senitive, the notorious side effects of tetracycline on young patients16 render the usage of this medicine very limited in China. Since the sensitivity to azithromycin was intermediate in this case, it was chosen as a single drug prescript. And it was proved to be effective. Before that, the physicians in ICU tried their luck with meropenem and linezolid. Since M. hominis was reported sensitive to linezolid,17 we speculate that linezolid maybe the real effective agent which cured the severe infection. This case also indicates that we should pay attention to Mycoplasma infection of patients undergoing renal cyst incision or other surgeries.
In this case, it was the NGS that helped with the diagnosis of the infection. Before the explicit pathogen and corresponding drug sensitivity were reported, the empirical antibiotics were applied including cephalosporins, meropenem and linezolid. Such prescripts lasted for about 2 weeks and costed up to more than $2000, not mention the expenses generated from the elongated hospital stay. Although the cost of NGS was higher than the routine bacterial culture and identification, it could certainly save a lot of money costed by useless medication and shorten the hospitalization time.
Ethics approval and consent to participate
According to the Declaration of Helsinki and International ethical guidelines for biomedical research involving human subjects, the ethics committee of Beijing Tsinghua Changgung hospital supervised the treatment and operation of the patient reported in this case report. The committee approved the study procedure. The reference number of the approval is 18149-0-01. The patient was fully aware of the data obtained from him was used in this study. He signed the informed consent and provided a written informed consent for the case details to be published.
Abbreviations list
NGS, next-generation sequencing technology; OD, operation day; POD, postoperation day; D-J tube, Double-J tube; NEUT, blood neutrophile granulocyte count; CRP, C-reaction protein; CBA, Columbia blood agar; M. hominis, Mycoplasma hominis.
Availability of data and material
The sequence of the M. hominis strain has been submitted to NCBI Blast. This data set will be available within dates in the link https://www.ncbi.nlm.nih.gov/bioproject/507519. All the related data was presented in the manuscript.
Disclosure
The authors report no conflicts of interest in this work.
References
1. Legg JM, Titus TT, Chambers I, Wilkinson R, Koerner RJ, Gould FK. Hematoma infection with Mycoplasma hominis following transplant nephrectomy. Clin Microbiol Infect. 2000;6:619–621.
2. Madoff S, Hooper DC. Nongenitourinary infections caused by Mycoplasma hominis in adults. Rev Infect Dis. 1988;10:602–613. doi:10.1093/clinids/10.3.602
3. Kenny GE, Balows A, Hausler WJ
4. D’Inzeo T, De Angelis G, Fiori B, et al. Comparison of Mycoplasma IES, Mycofast Revolution and Mycoplasma IST2 to detect genital mycoplasmas in clinical samples. J Infect Dev Ctries. 2017;11:98–101. doi:10.3855/jidc.8039
5. Clegg A, Passey M, Yoannes M, Michael A. High rates of genital mycoplasma infection in the highlands of Papua New Guinea determined both by culture and by a commercial detection kit. J Clin Microbiol. 1997;5:197–200.
6. Wilson MR, Naccache SN, Samayoa E, et al. Actionable diagnosis of neuroleptospirosis by next-generation sequencing. N Engl J Med. 2014;370:2408–2417. doi:10.1056/NEJMoa1401268
7. Taylor-Robinson D, Mandell GL, Bennett JE, Dolin R. Ureaplasma urealyticum and Mycoplasma hominis. In: Principles and Practice of Infectious Diseases. New York: Churchill Livingstone. 1995:1713–1717.
8. Horner P, Donders G, Cusini M, Gomberg M, Jensen JS, Unemo M. Should we be testing for urogenital Mycoplasma hominis, Ureaplasma parvum and Ureaplasma urealyticum in men and women? – a position statement from the European STI Guidelines Editorial Board. J Eur Acad Dermatol Venereol. 2018. doi:10.1111/jdv.15146
9. Stojanov M, Baud D, Greub G, Vulliemoz N. Male infertility: the intracellular bacterial hypothesis. New Microbes New Infect. 2018;22(26):37–41. doi:10.1016/j.nmni.2017.12.005
10. Camara B, Mouzin M, Ribes D, et al. Perihepatitis and perinephric abscess due to Mycoplasma hominis in a kidney transplant patient. Exp Clin Transplant. 2007;5:708–709.
11. Orange GV, Jones M, Henderson IS. Wound and perinephric haematomata infection with Mycoplasma hominis in a renal transplant recipient. Nephrol Dial Transplant. 1993;8:1395–1396.
12. Gerber L, Gaspert A, Braghetti A, et al. Ureaplasma and Mycoplasma in kidney allograft recipients-A case series and review of the literature. Transpl Infect Dis;2018:e12937. doi:10.1111/tid.12937.
13. Koshiba H, Koshiba A, Daimon Y, Noguchi T, Iwasaku K, Kitawaki J. Hematoma and abscess formation caused by Mycoplasma hominis following cesarean section. Int J Womens Health. 2011;3:15–18. doi:10.2147/IJWH.S16703
14. Redelinghuys MJ, Ehlers MM, Dreyer AW, Lombaard HA, Kock MM. Antimicrobial susceptibility patterns of Ureaplasma species and Mycoplasma hominis in pregnant women. BMC Infect Dis. 2014;14:171. doi:10.1186/1471-2334-14-171
15. Azizmohammadi S, Azizmohammadi S. Antimicrobial susceptibility patterns of Ureaplasma urealyticum and Mycoplasma hominis isolated from pregnant women. Iran Red Crescent Med J. 2015;17:e17211. doi:10.5812/ircmj.23191v2
16. Dorval J, Demers PP. Side effects of tetracyclines in pediatrics. Laval Med. 1968;39(10):939–954.
17. Kenny GE, Cartwright FD. Susceptibilities of Mycoplasma hominis, M. pneumoniae, and Ureaplasma urealyticum to GAR-936, dalfopristin, dirithromycin, evernimicin, gatifloxacin, linezolid, moxifloxacin, quinupristin-dalfopristin, and telithromycin compared to their susceptibilities to reference macrolides, tetracyclines, and quinolones. Antimicrob Agents Chemother. 2001;45:2604–2608.
 © 2019 The Author(s). This work is published and licensed by Dove Medical Press Limited. The full terms of this license are available at https://www.dovepress.com/terms.php and incorporate the Creative Commons Attribution - Non Commercial (unported, v3.0) License.
By accessing the work you hereby accept the Terms. Non-commercial uses of the work are permitted without any further permission from Dove Medical Press Limited, provided the work is properly attributed. For permission for commercial use of this work, please see paragraphs 4.2 and 5 of our Terms.
© 2019 The Author(s). This work is published and licensed by Dove Medical Press Limited. The full terms of this license are available at https://www.dovepress.com/terms.php and incorporate the Creative Commons Attribution - Non Commercial (unported, v3.0) License.
By accessing the work you hereby accept the Terms. Non-commercial uses of the work are permitted without any further permission from Dove Medical Press Limited, provided the work is properly attributed. For permission for commercial use of this work, please see paragraphs 4.2 and 5 of our Terms.