Back to Journals » International Journal of Nanomedicine » Volume 17
Nanomedicine: An Emerging Novel Therapeutic Strategy for Hemorrhagic Stroke
Authors Xu Y , Chen A, Wu J, Wan Y, You M, Gu X, Guo H, Tan S, He Q, Hu B
Received 8 January 2022
Accepted for publication 11 April 2022
Published 2 May 2022 Volume 2022:17 Pages 1927—1950
DOI https://doi.org/10.2147/IJN.S357598
Checked for plagiarism Yes
Review by Single anonymous peer review
Peer reviewer comments 3
Editor who approved publication: Prof. Dr. Anderson Oliveira Lobo
Yating Xu,* Anqi Chen,* Jiehong Wu,* Yan Wan, Mingfeng You, Xinmei Gu, Hongxiu Guo, Sengwei Tan, Quanwei He, Bo Hu
Department of Neurology, Union Hospital, Tongji Medical College, Huazhong University of Science and Technology, Wuhan, 430022, People’s Republic of China
*These authors contributed equally to this work
Correspondence: Bo Hu; Quanwei He, Department of Neurology, Union Hospital, Tongji Medical College, Huazhong University of Science and Technology, Wuhan, 430022, People’s Republic of China, Tel +86-27-87542857, Fax +86-27-87547063, Email [email protected]; [email protected]
Abstract: Hemorrhagic stroke is one of the most devastating diseases worldwide due to a high rate of disability and mortality with few effective treatments. Recent advances in nanomedicines to promote hemostasis, drug delivery, neuroprotection, and nerve regeneration may provide insight into hemorrhagic stroke treatment. In this review, we first view the pathophysiology and conventional therapeutics of hemorrhagic stroke. Second, we comprehensively summarize the current nanomedicines applied in hemorrhagic stroke, including inorganic nanomaterials, polymer-based nanomaterials, lipid-based nanomaterials, self-assembling peptide-based hydrogel, exosomes, and gel systems. Finally, the challenges, opportunities, and future perspectives of nanomedicines for hemorrhagic stroke are discussed. Thus, this review promotes greater exploration of effective therapies for hemorrhagic stroke with nanomedicines.
Keywords: hemorrhagic stroke, nanomedicine, therapy, subarachnoid hemorrhage, intracerebral hemorrhage
Introduction
A hemorrhagic stroke occurs when a blood vessel rupture resulting in bleeding into the brain. It can be divided into two types, namely intracerebral hemorrhage (ICH)—bleeding within the brain parenchyma—and subarachnoid hemorrhage (SAH)—bleeding within the subarachnoid space.1 Hemorrhagic stroke accounts for 10–20% of all strokes and results in 40% of stroke-related deaths, which has drawn research attention due to its high mortality rate.2 The mortality rate of hemorrhagic strokes is 25–30% in high-income countries and 30–48% in low- to middle-income countries.3 The effective treatments for hemorrhagic strokes are scarce leading to poor clinical outcomes and heavy social burden. Supportive therapy, hemostatic therapy, surgery, complication prevention, and rehabilitation treatment are conventional therapeutic strategies for hemorrhagic strokes.4 However, the clinical benefits of hemostatic therapy or surgery for hematoma removal are controversial.5–7 Moreover, many pharmacological agents failed to improve the prognosis of hemorrhagic strokes in clinical trials due to their short half-life periods, poor specificity of biodistribution, and inability to cross the blood-brain barrier (BBB).8,9
Since its conception in 1959, nanotechnology has opened a new area of study that involves creating and applying systems or materials at the nanometer-scale, known as nanoparticles (NPs). The application of nanotechnology in medicine (ie, nanomedicine) offers an exciting prospect for the diagnosis and treatment of many diseases.10 The advantages of nanomedicine have made it an ideal candidate to improve disease treatment. NPs can ameliorate the pharmacological and pharmacokinetic patterns of conventional drugs or achieve targeted delivery by acting as drug carriers.11 Many kinds of nanomedicines, including metal NPs, graphene oxide, hydrophilic carbon clusters, polymeric NPs, polymeric micelles, liposomes, lipid nanocapsules, nanoemulsions, self-assembly peptide based hydrogel, gel systems, and exosomes have been applied in hemorrhagic stroke therapy. Recent advances in nanomedicines concerning their promotion of hemostasis, neuroprotection, complication prevention, and nerve regeneration, provide new ideas for hemorrhagic stroke treatment.
In this review, we have provided an overview of the hemorrhagic stroke-associated brain injury mechanism, the conventional diagnosis and therapy methods, as well as their challenges. We also summarized the application of nanomedicines in the field of hemorrhagic stroke therapy (Figure 1). Finally, we addressed the challenges, opportunities, and future perspectives of nanomedicines for hemorrhagic strokes.
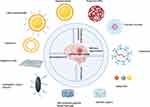 |
Figure 1 The nanomaterials used for therapy of hemorrhagic stroke. Created with Biorender.com. Abbreviation: NPs, nanoparticles. |
Pathophysiology of Hemorrhagic Stroke
Hemorrhagic stroke induces a series of adverse events that cause primary and secondary brain injury. Primary brain injury results from mass effect and mechanical disruption from extravasated blood, while secondary brain injury results from toxic biochemical and metabolic effects in response to extravasated blood components. The pathophysiology of hemorrhagic stroke is summarized in Figure 2.
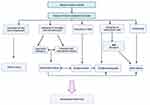 |
Figure 2 The pathophysiology of hemorrhagic stroke. Created with Biorender.com. Abbreviations: ICP, intracranial pressure; ROS, reactive oxygen species. |
Primary Brain Injury
As extravasated blood enters the brain parenchyma or/and subarachnoid space, it immediately increases the intracranial pressure (ICP), which may lead to arterial compression resulting in intracerebral ischemia. In ICH, the initial hematoma and hematoma expansion can result in mechanical compression of the peri-hematoma structures.
Secondary Brain Injury
Edema and BBB Disruption
Peri-hematoma edema, intra-hematoma edema, and global edema occurring after ICH and SAH are associated with poor clinical outcomes and could cause more severe secondary injuries.12,13 Blood components, such as thrombin, hemoglobin, and its degradation products, can lead to brain edema through BBB disruption and toxic effects. Meanwhile, neuro-inflammation after hemorrhagic stroke is responsible for initiating both vasogenic edema through BBB disruption and cellular edema through toxic effects on the cells. Ischemic injury, dysfunction of autoregulation, and clot retraction are also associated with brain edema after hemorrhagic stroke.
As mentioned above, degradation products of blood, inflammatory factors, and vasoactive substances are responsible for BBB disruption after hemorrhagic stroke since they can lead to endothelial death.14,15 Matrix metallopeptidase (MMP) is also related to BBB disruption after hemorrhagic stroke due to its ability to degrade the extracellular matrix of the cerebral microvascular basal lamina.
Oxidative Stress
Oxidative stress (OS) refers to the overproduction of free radicals, mainly reactive oxygen species (ROS). OS in hemorrhagic stroke results from mitochondrial dysfunction, blood cell decomposition products (iron ions and heme), inflammatory cell infiltration and activation, activation of many peroxidases, and disruption of the anti-oxidative system after hemorrhagic stroke.16,17 Excessive production of free radicals after hemorrhagic stroke is associated with neuronal damage, brain injury, and inflammatory responses.
Inflammation
The degradation products of red blood cells, overproduction of free radicals, and pathways secondary to endothelial injury are responsible for inflammation after hemorrhagic stroke.18 Substantial evidence indicates an inflammatory response after hemorrhagic stroke, including activation of microglial cells and recruitment of other inflammatory cells, such as neutrophils and macrophages.19 An increase in inflammatory mediators, including tumor necrosis factor, adhesion molecules, and matrix metalloproteinases, is also monitored after hemorrhagic stroke.19 The inflammatory response results in inflammation-related injuries, including BBB injury, edema, cell death, and vasospasm.
Cerebral Vasospasm
Cerebral vasospasm (CVS) has its onset on day 3 after SAH, peaks at day 7, and usually lasts for 2–3 weeks.20 CVS after SAH is a severe complication and associated with poor clinical outcomes.20 CVS usually results from overexpression of endothelin and hypoxia inducible factor-1, inflammation, overproduction of ROS, and endothelial cell apoptosis after SAH.21
Conventional Therapies for Hemorrhagic Stroke Treatment and Their Challenges
The conventional therapies for hemorrhagic strokes include general therapy, hemostatic therapy, surgery, complication prevention, and rehabilitation treatment.4
General therapy includes air protection, blood pressure (BP) management, and glycemic control.22,23 The use of these general therapies is recommended in a balanced manner. For instance, many patients with hemorrhagic stroke undergo endotracheal intubation for stroke intervention; however, the use of endotracheal intubation is subject to the risk of complications. For BP management, high BP is associated with the risk of hematoma expansion, aneurysmal rupture, and rebleeding, while hypotension may increase the risk of ischemia. Therefore, BP management should also consider risk assessment. For glycemic control, both hyperglycemia and hypoglycemia are associated with worse outcomes, such as CVS, higher short-term mortality, and hematoma expansion. Thus, blood glucose should be maintained at an appropriate level.
Hemostatic therapy is used to control the expansion of hematoma.24 The use of prothrombin complex concentrates, vitamin K, recombinant activated factor VII, and fresh frozen plasma is recommended. Nevertheless, one Phase III randomized trial found no clinical benefit of hemostatic therapy in patients without coagulation disorder.6 Therefore, current hemostasis should focus on patients with coagulopathy.
Various complications occur after hemorrhagic stroke, including cerebral edema, increased ICP, hydrocephalus, epileptic seizures, and CVS. Some of these complications can be deadly. Therefore, managing these complications is of great importance. Elevated ICP is commonly seen in patients with hemorrhagic stroke. It can be managed by simply elevating the head of the bed, analgesia, and sedation, or using mannitol, hypertonic saline, and neuromuscular paralysis.25 Concerning seizure prophylaxis, the guidelines recommend that anti-epileptic drugs (AEDs) should be used in patients with ICH presenting with clinical seizures or electrographic seizures. Routine AED administration is recommended for patients with SAH, especially for those with risk factors of developing onset seizures. Commonly used AEDs include levetiracetam, valproate, and fosphenytoin. Furthermore, CVS is a deadly complication of SAH. The most widely used prevention measure is the oral administration of nimodipine (NM) immediately after SAH. “Triple-H therapy”, which means hypervolemia by volume expansion, hypertension with BP augmentation, and hemodilution for reducing blood viscosity, is recommended after an incidence of CVS.26
Surgical evacuation is used in patients with ICH to decrease the mass effect and secondary injury caused by hematoma. Brainstem compression, neurological deterioration, and hydrocephalus due to ventricular obstruction are frequently used as indicators for emergent surgical intervention in patients with ICH.27 In patients with SAH, emergency surgery of endovascular coiling or surgical clipping is needed to stop the bleeding from a ruptured aneurysm.28
Despite the benefit of conventional therapies, many challenges arise in managing hemorrhagic strokes. First, although the pathophysiology of hemorrhagic stroke has been studied for years, no pharmacological agents are clinically available to effectively treat hemorrhagic stroke, especially by targeting the secondary injury after hemorrhagic stroke. Many clinical trials targeting neuro-inflammation, iron overload, and neuron injury after hemorrhagic stroke have failed to improve the prognosis of hemorrhagic stroke. Second, systemic administration of some drugs (eg, nimodipine), will lead to unwanted adverse effects since it can affect non-targeting sites. Hence, site-specific delivery of drugs is urgently needed. Another problem is that some therapeutic agents fail to reach the brain due to their short half-life and inability to cross the BBB. Thus, promoting a longer circulation half-life and trans-endothelial transport can help increase the therapeutic effects of drugs in hemorrhagic stroke.
Nanomedicines for the Treatment of Hemorrhagic Stroke
The use of nanomedicine is widely investigated in the field of hemorrhagic stroke therapy. Nano-dimensional particles can be used as drug carriers to encapsulate both hydrophilic and hydrophobic drugs to improve their solubility and stability. The surface of NPs can be modified with targeting ligands to aid the homing of drug-loaded carriers at the hemorrhagic site. The use of stimuli-responsive drug nanocarriers also enables the controlled release of drugs at the target sites. Small size and surface modification of drug-loaded NPs impart properties to permeate the BBB. Moreover, some inorganic and polymeric NPs with ROS depletion and iron chelation abilities have also been developed to attenuate secondary injury caused by iron overload and oxidative stress. Nanofiber-based scaffolds are also used in the field of nerve regeneration and hemostasis. Table 1 contains a detailed summary of nano-inventions used for hemorrhagic strokes. By improving pharmaceutical properties including solubility, stability, half-life period, and site-specific accumulation, nanomaterials can reduce the required dose and increase the interval between dosing compared with conventional medications. By achieving site-specific delivery, stimuli-responsive release, and improved BBB penetrability, nanomedicine can also increase drug accumulation in hemorrhagic stroke sites and reduce unwanted distribution to improve therapeutic efficacy while reducing adverse effects of pharmaceutical products. In addition, nanomaterials have led to the emergence of new treatments (eg, nerve regeneration therapy for hemorrhagic stroke) filling a gap not addressed by conventional therapies. Some nanomaterials have inherent therapeutic effects (eg, cerium oxide NPs), offering new therapeutic mechanisms beyond conventional therapies for hemorrhagic stroke.
 |  |  |  |
Table 1 Nanomedicines for Hemorrhagic Stroke Therapy |
Inorganic Nanomaterials
Inorganic nanomaterials including cerium oxide NPs, selenium (Se)-NPs, iron oxide NPs, polyethylene glycol (PEG) functionalized hydrophilic carbon clusters (PEG-HCCs), and graphene oxide nanosheets can be used for combating hemorrhagic stroke.29–35 Cerium oxide NPs, Se-NPs, and PEG-HCCs have been shown to exert neural protective effects by scavenging ROS.31–34 Furthermore, graphene oxide nanosheets were used to deliver neuroprotectant for neuroprotective therapy.29 Iron oxide NPs have been used in combination with stem cell therapy for neuroprotection.35
Metal NPs
Cerium oxide NPs may offer a new approach for neuroprotection after hemorrhagic stroke due to their ROS scavenging properties. Cerium oxide NPs have two co-existing oxidative states (3+ and 4+) in transition which participate in ROS decomposition.36 Ceria NPs have been widely used in the therapy of brain diseases with high levels of OS, such as ischemic stroke, Alzheimer’s disease (AD), and Parkinson’s disease (PD).37–39 Jeong et al synthesized uniform, 3 nm, water-dispersed, biocompatible, ceria NPs with aminocaproic acid coating (BA-CeNPs) and modified the NPs with PEG for better biocompatibility.32 The BA-CeNPs exhibited potent ability to reduce OS and cytotoxicity in RAW264.7 macrophages. After the intravenous administration of NPs one hour post-SAH, the rats exhibited less neuronal death, brain edema, neuronal inflammatory response, and better long-term clinical outcome. Accumulated ROS can activate the immune cells, and ceria NPs can reduce inflammation-associated injury by scavenging ROS. Cha et al developed lipid-coated magnetic mesoporous silica NPs doped with ceria NPs (LMCs) for theragnosis of ICH.33 LMCs consist of mesoporous silica NPs coated by lipid bilayers, which are loaded with large amounts of ceria NPs in the pores of their walls for ROS scavenging, and iron oxide NPs in their cores for magnetic resonance imaging (MRI) contrast. After intracerebral injection of LMCs, they were found to be recruited throughout the peri-hematoma area and accumulated in the intracellular space of active microglia/macrophages, indicating successful recruitment of LMCs to the target area and cells to accentuate the inflammatory response in the ICH models. Taking advantage of the iron oxide NPs in LMCs, researchers successfully achieved enhanced imaging of the peri-hematoma area using serial T2-weighted MRI. The injection of LMCs reduced neuronal inflammation and inflammatory cell infiltration after ICH. By attenuating neuro-inflammation after ICH, LMCs reduced brain edema and promoted a better neurological outcome. Furthermore, Zheng et al developed ceria NPs modified with PEG (PEG-CeNP) and demonstrated that PEG-CeNP treatment attenuates demyelination and white matter injury after ICH by ROS scavenging.31
Since Se is incorporated as selenocysteine in anti-oxidant enzymes, such as glutathione peroxidase, thioredoxin reductase, and selenoprotein P, where it acts as the redox center of these enzymes, Se-NPs are widely used in anti-oxidant therapy.40 Yang et al developed a porous Se and SiO2 nanocomposite (Se@SiO2), which has the ability of controlled Se release to guarantee the beneficial effects and reduce the toxicity of Se.34 An in vitro test proved that Se@SiO2 protected the neuroblastoma cell line SH- SY5Y from hemin-induced apoptosis by reducing the intracellular ROS level. Also, the intra-peritoneal injection of Se@SiO2 in ICH mice reduced the ROS level, cell apoptosis, and brain edema, as well as improved the BBB integrity compared with that in vehicle-treated ICH mice.
Ferrimagnetic iron oxide nanocubes (FIONs) can also be used for targeted drug delivery with the external magnetic field guidance or fictionalized with targeting moieties.41 Ming et al synthesized FIONs to label human embryonic stem cell-derived spherical neural masses (SNMs), which are known to have efficient differentiation ability.35 Researchers created an external magnetic field by adopting a magnet attached to the hamlet after injecting FION-labeled SNMs into the ICH models. They found that the guidance of the external magnetic field significantly increased the targeted delivery of FION-labeled SNMs, leading to reduced swelling, inflammatory response, and brain atrophy, and improved neurological function recovery after ICH.
Carbon-Based Nanomaterials
Carbon-based nanomaterials used in disease therapy and diagnosis include graphene, graphene oxide, nanodiamonds, carbon nanotubes, and carbon nanofibers. PEG-HCCs are a newly developed anti-oxidant, which can eliminate ROS in vitro and in vivo.42 Recently, Dharmalingam et al applied PEG-HCCs in the therapy of ICH.30 They found that PEG-HCCs significantly reduced ROS accumulation and genome damage induced by hemin, leading to reduced senescence phenotype. However, although PEG-HCC therapy reduced the senescence after exposure to hemin, it could increase the sensitivity to iron-mediated ferroptosis, since senescent cells were resistant to iron-mediated ferroptosis. Therefore, they developed PEG-HCCs covalently conjugated with well-known iron-chelating agent deferoxamine (DEF-HCC-PEG). DEF-HCC-PEG exhibited better efficiency in preventing hemin-induced genome damage, iron-induced ferroptosis and cell death than either DEF or PEG-HCCs alone (Figure 3). Graphene is a two-dimensional, one-atom-thick nanosheet with a large specific surface area ideal as a drug nanocarrier.43 As an oxidized form of graphene, graphene oxide has an oxygen-containing group on the surface which enables water dispersibility and easy modification.44 Yang et al synthesized a pirfenidone-loaded functionalized graphene oxide (pirfenidone-FGO) nanosheet with Tat and methoxy polyethylene glycol (mPEG).29 The functionalized nanosheet contributes to better BBB bypassing ability and stability in the blood circulation of pirfenidone. Pirfenidone-FGO also exhibits high efficiency of drug release in an acidic environment, which enables effective treatment of acidic inflammatory lesions after SAH. The researchers demonstrated that injection of pirfenidone-FGO significantly reduced the gray matter lesion and brain edema after SAH.
 |
Figure 3 ICH treatment with DEF-HCC-PEG. (A) The mechanism of DEF-PEG-HCC in combating ICH. Hemin can lead to senescence of neurons by inducing nuclear and mitochondrial DNA damage. Although PEG-HCC therapy can reduce senescence and DNA damage after exposure to hemin, it simultaneously increases iron-mediated ferroptosis. In contrast, DEF-HCC-PEG can prevent ferroptosis, DNA damage, and senescence with simultaneous iron chelation and ROS scavenging ability. (B) PEG-HCC-DEF restores the viability of hemin-treated neurons beyond that of PEG-HCC or DEF alone. The cultured neurons were treated with 5 μM hemin and received corresponding drugs. Total cell death was measured by MTT assay. (C) DEF-PEG-HCC exhibited higher efficiency in preventing hemin-induced DNA damage. The cultured neurons were treated with 5 μM of hemin and received corresponding drugs. IB was used to measure the level of γH2AX and p-53BP1 as biomarkers of genome damage. The histogram shows the quantitation results of IB. (D and E) The IB quantitation result of (D) GPX4 or (E) MDA levels in cultured neurons treated with 100 μM FeSO4 and in the presence or absence of hemin, PEG-HCC, DEF, or DEF-HCC-PEG. The reduction of GPX4 or increase of MDA levels can be markers of ferroptosis, respectively. Results are represented as mean ± SEM from three independent experiments. Significant differences: *p < 0.01; **p < 0.05. Reprinted with permission from American Chemical Society: ACS Nano, Pervasive Genomic Damage in Experimental Intracerebral Hemorrhage: Therapeutic Potential of a Mechanistic-Based Carbon Nanoparticle, Dharmalingam P, Talakatta G, Mitra J et al. Copyright 2020 American Chemical Society.30 Abbreviations: DEF, deferoxamine; IB, immunoblotting; ICH, intracerebral hemorrhage; MDA, malondialdehyde; PEG, polyethylene glycol; PEG-HCCs, polyethylene glycol functionalized hydrophilic carbon clusters; ROS, reactive oxygen species; SEM, standard error of mean. |
Polymer-Based Nanomaterials
Polymer-based nanomaterials are used for neuroprotection by optimizing pharmacological properties or improving the site-specific delivery of neuroprotectants and genes including resveratrol (Res), curcumin, rosuvastatin, dauricine (DRC), astaxanthin (ATX), neurotrophin-3 (NT-3).45–51 Polymer-based nanomaterials with ROS scavenging and iron chelation properties are also used for neuroprotection of hemorrhagic stroke.52,53 Polymer-based nanomaterials prevented complications after SAH by improving targeted delivery of the calcitonin gene-related peptide (CGRP) gene.54
Biodegradable polymeric NPs are one of the most widely used nanocarriers due to their low toxicity, good biocompatibility, biodegradability, high encapsulation efficiency, and sustained release ability.55 Encapsulating drugs with biodegradable polymeric NPs improve their solubility, bioavailability, and retention time.55 Poly(lactic-co-glycolic acid) (PLGA)-based NPs are one of the most widely used polymeric nanocarriers for drug therapy. Furthermore, the US Food and Drug Administration has granted approval for PLGA in human use.56 Mo et al developed PLGA NPs to improve the brain delivery and therapeutic efficacy of Res, which has been used as a neuroprotectant in many neurological diseases.48 The group demonstrated that Res NPs have higher permeability to cross physiological barriers, better oral absorption, and higher accumulation level in the brain, and exhibit a prolonged sustained release profile. Oral administration of Res NPs showed significant neuroprotection effects in the ICH mouse models. Curcumin, an extract from the plant Curcuma longa, can act as a candidate for hemorrhagic stroke therapy due to its anti-inflammatory and anti-oxidative effects. Curcumin-capsulated PLGA NPs have been successfully developed. They exhibited enhanced efficiencies for anti-neuronal apoptosis and anti-inflammation, inhibiting BBB disruption, hindering OS, as well as reducing glutamate in the cerebrospinal fluid (CSF) after SAH.45,46 Poly y(ε-caprolactone) (PCL) is a biodegradable polymer widely used in medical devices and tissue engineering.57 PEGylation of PCL results in amphiphilic PEG-PCL copolymer, which has been widely applied in drug delivery.58 In a recent study, PEG-PCL formed nanomicelles with a hydrophobic core to encapsulate rosuvastatin, a drug effective in inhibiting the inflammatory reaction after ICH.51 Rosuvastatin-loaded nanomicelles significantly improved the solubility and extended the half-life of rosuvastatin, thereby allowing for administration at a lower dose and frequency to reduce toxicity and improve the curative effect. Oral administration of the rosuvastatin-loaded nanomicelles relieved the inflammatory response in the ICH mouse models compared with those only receiving free rosuvastatin treatment.
In addition to drug delivery, polymeric NPs can be used for therapeutic intracellular gene delivery.59 It was demonstrated that poly(butyl cyanoacrylate) (PBCA)-NPs could act as effective vectors to deliver macromolecules to the injured brain and as a non-viral system for gene delivery.60,61 Chung et al developed PBCA NPs to transport plasmid NT-3, as an essential neurogenesis regulator, containing hormone response element (HRE) with a cytomegalovirus (cmv) promoter for neuroprotective effects in ICH rats.49 Intravenous injection of PBCA NP/cmv NT-3-HRE complexes significantly increased the expression of NT-3 in the brain tissue and exhibited anti-apoptotic effects and neuron protection after ICH. Gelatin NPs are biodegradable, biocompatible, non-toxic, and low-cost nanocarriers widely used for gene delivery.62 CGRP is a potent arterial and venous vasodilator used for the relief of CVS after SAH. Tat peptide-decorated gelatin-siloxane (Tat-GS) NPs were developed to transfer the CGRP gene for the treatment of CVS after SAH.54 The Tat-GS NP-loading CGRP plasmid successfully increased the CGRP expression level in vitro and in vivo and attenuated the neurological outcomes and CVS after SAH.
Polymeric NPs capable of controlled release and targeted drug delivery were also developed for the treatment of hemorrhagic stroke. Recently, metal ion-responsive DRC-loaded micelles (DPM) based on O-dodecyl p-methylene-bisphosphonic calix[4]arene for DRC delivery were successfully developed for ICH therapy.47 DRC is a drug isolated from traditional Chinese herbal medicine, which has properties of anti-neuronal apoptosis and endoplasmic reticulum stress relief. The DPM remained stable in the absence of ferrous ions and exhibited a ferrous ion-dependent DRC release profile in the in vitro drug release test, as shown in Figure 4A. The treatment of ICH animals with micelles attenuated the neurological deficits, BBB damage, apoptosis, ferroptosis, and neuro-inflammation after ICH47 (Figure 4). ATX is a neuroprotectant with anti-oxidative, anti-inflammatory, and anti-apoptotic properties. You et al developed transferrin functionalized PEG-encapsulated ATX-NPs for targeted delivery of ATX to neurons since transferrin receptors are highly expressed in the neuronal membrane.50 They demonstrated that transferrin functionalized ATX-NPs accumulated more significantly in primary cultured neurons than those without transferrin, and exhibited better neuroprotective efficiency compared with free ATX after exposure to oxygenated hemoglobin.
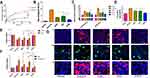 |
Figure 4 The treatment of ICH animals with micelles attenuated the neurological deficits, BBB damage, apoptosis, ferroptosis, and neuro-inflammation after ICH. (A) The DRC release profile of DPM in the presence or absence of 5 mM Fe2+. The results of (B) modified neurological severity score assessment, (C) brain water content measurement, (D) Evans blue extravasation assay, (E) Western blot of GPX-4 and Bcl-2, (F) Western blot of Bax and caspase-3, and (G) immunostaining of (a) Iba-1, (b) GFAP, as well as (c) MPO in each group. Craniotomy was used to set up the sham group. The ICH groups were set up by autologous whole blood double infusion in mice treated with vehicle (0.9% saline), free DRC, blank micelles (PM), or DPM. The mice were assessed 24 h after drug administration. Higher brain water content and Evans blue leakage are used as markers of BBB disruption. The depletion of GPX-4 is a marker of ferroptosis. The lower level of Bcl-2/Bax ratio and a higher level of caspase-3 indicate apoptosis. Iba-1, GFAP, and MPO are specifically expressed in microglia, astrocytes, and neutrophils, respectively. Values are presented as mean ± SD. *p < 0.05 was considered as statistically significant. Reprinted with permission from Springer Nature: Journal of Nanobiotechnology, Metal ion-responsive nanocarrier derived from phosphorated calix[4]arenes for delivering dauricine specifically to sites of brain injury in a mouse model of intracerebral hemorrhage, Li M, Liu G, Wang K et al. Copyright © 2020, The Author(s)..47 Abbreviations: BBB, blood-brain barrier; DPM, DRC-loaded micelles; DRC, dauricine; ICH, intracerebral hemorrhage; SD, standard deviation. |
More recently, NPs constituents of polymers with ROS scavenging and iron chelation abilities, were also developed to overcome the iron toxicity and ROS destruction after ICH.52,53 Zhu et al developed dual-functional nanoscavengers composed of DEF units and catechol moieties, with the former acting as iron chelators and the latter as ROS scavengers, as shown in Figure 5A.53 They demonstrated that the NPs exhibited efficient iron and ROS depletion capacity in cells and significantly attenuated the iron overload and OS caused by ICH in vivo (Figure 5). Redox polymers containing nitroxide radicals, which can act as ROS scavengers, were successfully developed and self-assembled into NPs.53 Moreover, redox polymer self-assembled NPs with nitroxide radicals in the core showed great ROS depletion ability in an ICH rat model.
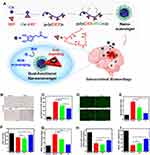 |
Figure 5 Dual-function nanoscavenger targeting iron chelation and ROS scavenging for hemorrhagic stroke therapy. (A) Dual-functional nanoscavenger consists of DEF units and Cat moieties. The results of (B) iron staining, (C) total iron content measurement, (D) ROS staining, (E) ROS level measured by flow cytometry, (F) SOD measurement, (G) MDA measurement, (H) total GSH content measurement, and (I) brain cell viability measurement in each group. ICH mouse model was set up by collagenase injection. Each group received saline, free DEF (50 mg/kg), or P3 nanoscavenger (50 mg/kg equivalent DEF) twice a day. The normal group received no intervention. The mice were sacrificed on the 4th day for evaluation. P3 refers to poly(DEF-PEG0.42)8. Values are presented as mean ± SD. Significant differences: *p < 0.05, **p < 0.01, and ***p < 0.001. Adapted with permission from American Chemical Society: ACS Appl Mater Interfaces, Efficient Iron and ROS Nanoscavengers for Brain Protection after Intracerebral Hemorrhage, Fang Zhu, Liu Zi, Peng Yang et al. Copyright 2021 American Chemical Society.52 Abbreviations: Cat, catechol; DEF, deferoxamine; MDA, malondialdehyde; PEG, polyethylene glycol; ROS, reactive oxygen species; SD, standard deviation; SOD, Superoxide dismutase. |
Lipid-Based NPs
Lipid-based NPs including liposomes, nanoemulsions, and lipid nanocapsules (LNCs) are used for drug delivery to relieve complications and achieve neuroprotection effects after hemorrhagic stroke. Lipid-based NPs were used to encapsulate neuroprotectants including β‐caryophyllene, xenon (Xe), curcumin, and quercetin (QU) to optimize their pharmacological properties and achieve controlled release.63–66 Lipid-based NPs have also been used to deliver fasudil, nitric oxide, and NM to prevent CVS after hemorrhagic stroke.67–69
Liposomes are vesicular carriers consisting of amphipathic lipid bilayers. The use of liposomes in the treatment of cerebral hemorrhage has been widely investigated, since liposomes have some desirable properties, such as low toxicity and good encapsulation properties for both hydrophilic and hydrophobic drugs.70 Takanashi et al developed liposomal fasudil which proved effective and safe as an intra-thecal treatment in preventing CVS after SAH.67 Another recent study also successfully used liposomes to deliver β‐caryophyllene, which has anti-inflammatory and anti-apoptotic effects in attenuating neurovascular unit damage after SAH in rats.65 However, intravenously injected liposomes can absorb plasma proteins, leading to rapid clearance of liposomes by the reticuloendothelial system.71 Surface modification with PEG can prolong the circulation time of liposomes by suppressing protein absorption.72 Miao et al developed PEGylated echogenic liposomes containing Xe, a well-known neuroprotectant, to attenuate early brain injury after SAH.66 Injection of Xe-containing echogenic liposomes with 1-MHz continuous wave ultrasound to trigger Xe release significantly reduced the SAH-induced neurological defects and mortality. Nitric oxide-loaded PEGylated echogenic liposomes with ultrasound-controlled nitric oxide release capacity have also been successfully developed for the treatment of CVS following SAH.69
Nanoemulsions are biphasic dispersion of two immiscible liquids either oil–in–water or water–in–oil stabilized by an amphiphilic surfactant. Nanoemulsions exhibited various advantages as drug nanocarriers, including enhanced semi-permeable membrane transport, ability to improve drug solubility and bioavailability, high stability, and increased interfacial area.73,74 Marques et al developed nanoemulsions to load curcumin for the therapy of ICH rats.64 They demonstrated that intra-peritoneal administration of nanoemulsified curcumin exhibited better neuron protection, anti-oxidant ability, and less adverse effects compared with free curcumin in Wistar rats after ICH. Galho et al synthesized nanoemulsions to deliver QU for the treatment of ICH in rats.63 QU is known for its strong anti-oxidant activity, but its application is limited due to its high lipophilicity. The nanomusiflied QU exhibits better bioavailability and anti-oxidant capacity than free QU. Therefore, treating the ICH rats with nanoemulsified QU resulted in better neurological outcomes and smaller hematoma volume.
LNCs are a type of lipid-based nanocarrier consisting of an oily core surrounded by a membrane made from a mixture of lecithin and a PEGylated surfactant. LNCs are prepared by an organic solvent free phase-inversion method which adds to their safety.75 Moreover, LNCs exhibit remarkably high stability and high efficiency for lipophilic drug encapsulation making them an ideal drug nanocarrier.76 Mohsen et al developed optimized LNCs with small particle size, narrow size distribution, high drug payload and stability, as well as a sustained drug release profile by using the solvent-free phase inversion technique.68 Researchers used LNCs to deliver NM, an FDA-approved drug for treating SAH-induced vasospasm via intranasal administration. The intranasally administered NM LNCs can deliver the same amount of NM in the brain tissue with a lower peak plasma concentration and a slower rate of elimination compared with the intravenously administered NM solution, which contributes to minimized cardiovascular side effects and a better curative effect of NM.
Self-Assembling Peptide-Based Hydrogel
Self-assembling peptide-based hydrogels offer a nanofiber scaffold for nerve regeneration after hemorrhagic stroke.77,78 It also blocks the ruptured vessels after hemorrhagic stroke for hemostasis therapy.79 Self-assembling peptides are biomedical materials that can form different structures by non-covalent interactions in response to different physical conditions.80 They have been widely investigated in the field of nerve regeneration as a therapy for stroke, spinal cord injury repair, traumatic brain injury, and ICH.79,81 Furthermore, a self-assembling peptide-based scaffold offers the following virtues for its application: 1) since a nanofiber scaffold is a kind of nanomaterial with enormous nanopores, it is investigated as a drug carrier to achieve sustained drug release; 2) it can act as an extracellular matrix (ECM) mimic for tissue cell culture, tissue repair, and tissue engineering; 3) hemostatic ability; and 4) high biocompatibility with low immunogenicity.
One of the most widely used self-assembling peptides is RADA16-I (Ac-RADARADARADARADA-CONH2; R, arginine; A, alanine; D, aspartate) which contains repeats of the hydrophilic and hydrophobic amino acid RADA peptide. Under an aqueous acidic environment, RADA16-I appears to be able to flow with high viscosity and can become a hydrogel structure in body fluids.82 It has been demonstrated that RADA16-I can provide a scaffold for neuronal cells to grow, repairing spinal cord injury, and attenuating injured optical pathways.83–85 In a rat ICH model, Sang et al demonstrated that local delivery of RADA16-I following hematoma aspiration significantly reduced brain edema, cerebral inflammation, apoptosis, and cavity volume, as well as attenuated functional deficits compared with the hematoma aspiration only group.77 After four weeks, they found that the RADA16-I hydrogel formed a tight interaction with the surrounding brain tissue. Meanwhile, axons and cells were found in the brain tissue near the hydrogel. However, few nerve fibers or cells were found in the grafted hydrogel, which might have resulted from the acidity of RADA16-I. To overcome this limitation, another group of researchers modified RADA16-I with bioactive short peptide motifs to develop RADA16 MIX, which consists of RADA16-RGD (Ac-RADARADARADARADA-DGDRGDS; G, glycine) and RADA16-IKVAV (Ac-RADARADARADARADA-ARIKVAV; I, Isoleucine; K, lysine; V, valine; V, valine).78 The pH value of RADA16 MIX is about 7.2, which is close to our physiological condition. RADA16-RGD is known to promote cell adhesion in a 3D cell culture.86 Furthermore, IKVAV is proven to promote neurite outgrowth and cell differentiation into neurons.87 They found that intra-lesion injection of RADA16 MIX solution after hematoma aspiration in ICH mice contributed to greater cell survival, less neuron inflammatory response, and better functional recovery compared with the RADA16-I injection. Several nerve fibers were found inside the grafted RADA16 MIX and cytoplasmic apophysis existed around the boundary of the RADA16 MIX, while no fibers were found inside RADA16-I. This indicated that the RADA16 Mix could act as a matrix for nerve fiber regeneration.
Elastin-like polypeptide (ELP) is a kind of self-assembling peptide with thermo-sensitive responsiveness. ELP becomes insoluble above a specific temperature called transition temperature and conversely soluble below the transition temperature. An Arg–Gly–Asp (RGD)-peptide-containing ELP fusion protein (REP) was developed to improve the cell adhesion ability. Park et al treated ICH rats by administration of cold REP through the internal carotid artery assuming that REP will assemble into gel-like aggregates and block the ruptured vessel at body temperature.79 They observed that REP exhibited improved brain endothelial cell adhesion ability and injected REP specifically located at the lesion site without occlusion of any intact microvessels. They also observed that administration of REP significantly reduced the hematoma volume, prevented the blood component leakage, and consequently reduced the inflammatory response.
Other Types of Nanomedicines for Hemorrhagic Stroke
This section introduces exosomes and gel systems. Exosomes played a neuroprotective role in hemorrhagic strokes since exosomes contain neuroprotective proteins and miRNAs.88,89 Gel systems can be used for in site delivery of bone marrow stromal cells (BMSCs) and epidermal growth factor (EGF) and provide a matrix for cell growth, thus promoting nerve regeneration after hemorrhagic stroke.90,91 Gel systems can also promote neuroprotection effects by delivering deferoxamine mesylate (DFO) or nicardipine hydrochloride (NCD).92,93 Gel systems with anti-inflammatory and hemostatic effects were used for neuroprotection and hemostatic therapy after hemorrhagic stroke.94,95
Exosomes are extracellular vesicles secreted by different cell types that have been used as carriers for drugs and different types of molecules (mRNA, miRNA, and protein).96 Otero-Ortega et al used proteomics analysis to identify protein in exosomes derived from mesenchymal stem cells (MSCs). They found that the exosomes contain various proteins involved in the process of brain repair function.88 ICH rat models with tail vein administration of MSCs-derived exosomes have exhibited improved functional recovery, reduced lesion size and white matter injury, increased tract connectivity, and axonal sprouting. miR-133b has been proven to be a neuroprotectant in many brain diseases, such as spinal cord injury and ischemic stroke. Shen et al used exosomes derived from miR-133b transferred MSCs, which contained enriched miR-133b.89 The injection of miR-133b enriched exosomes significantly reduced apoptosis and neurodegeneration induced by ICH.
Gel systems have been used for nasal, topical, and transdermal drug delivery for many years.97 In the field of hemorrhagic stroke therapy, it has been used in combination with nanomaterials. NCD has neuroprotective effects in ICH due to its anti-inflammatory properties. However, the low BBB penetration ability and short plasma half-life limit its bioavailability for oral administration. Guo et al prepared an intranasal gel made of blending hyaluronan and methylcellulose (HAMC) to reduce the systematic exposure by intranasal drug delivery and to enhance the residence time of the drug with mucoadhesive properties of the gelling drug delivery system.93 The HAMC gel was coated with a positively charged polymethylmethacrylate (PMMA) film on one side and loaded with positively charged NCD-encapsulated NPs to achieve charge-driven oriented drug migration to the nasal mucosa. In vivo tests proved that the NP-loaded gel improved drug delivery to the brain tissue, prolonged the retention time, and reduced the side effects caused by intranasal drug delivery on the lungs. The application of NPs and HAMC gel composites also attenuates brain injury after ICH by relieving the mass effect and exhibiting anti-apoptosis properties. BMSCs transplantation therapy has been widely used in tissue repair due to its high proliferative capacity. However, the transplant survival of BMSCs is limited by the microenvironment. For example, iron overload which is common in many hemorrhagic injuries can induce damage to transplanted BMSCs. Gong et al developed a core-shell hydrogel to enhance the efficiency of BMSC transplantation by preventing iron overload.90 The shell hydrogel is made of low-molecular-weight keratin (LMWK) and encapsulated with minocycline hydrochloride (MH) as an iron chelator. The core hydrogel is made of high-molecular-weight keratin (HMWK) hydrogel loaded with BMSCs and PLGA NPs encapsulating the EGF and basic fibroblast growth factor (bFGF). The core-shell hydrogel protects BMSCs by absorbing iron quickly and reducing the iron overload by MH. The PLGA NPs exhibited a sustained release of bFGF, and EGF provided a condition suitable for long-term growth and differentiation of BMSCs in vivo. The injection of the core-shell hydrogel collectively improved the transplant survival; significantly reduced the iron deposition area, brain atrophy, and brain edema; and improved neurological recovery after ICH. Gelatin and keratin-based gel systems have also been developed for hemorrhagic stroke therapy. They have been developed to deliver EGF and DFO for neuron regeneration and iron chelation after ICH.91,92 Recently, researchers have developed injectable gelatin hydrogel which can suppress neuroinflammation after ICH through regulation the polarization of immune cells by RGD-integrin interaction. Injection of the gelatin hydrogel reduced inflammation and attenuated neurological deficits after ICH.94 Keratin-based hydrogel with hemostatic effect have also successfully been applied in ICH therapy.95
Conclusion and Future Perspectives
In recent years, nanomedicines have been applied to the field of hemorrhagic stroke therapy since they not only improve the therapeutic effect of conventional drugs but also provide a possibility for attenuating secondary injury and regenerative therapy. Despite major progress made in nanomedicine research, many problems still need to be resolved before their implementation in clinical practice. A list of advantages and disadvantages of the main nanomaterials for hemorrhagic stroke therapy is presented in Table 2. In addition, the use of nanomedicines for hemorrhagic stroke therapy lacks clinical trials essential for developing new drugs. Some of the major challenges faced in the transition from preclinical to clinical trials include the heterogeneity of clinical conditions and animal models, difficulties in controlling biodistribution, problems in large-scale and reproducible synthesis, and obstacles in high-throughput NP optimization.98 Significant efforts are needed for promoting clinical trials of nano-intervention in hemorrhagic stroke. It is expected that the advantage of nanomedicines for hemorrhagic stroke therapy demonstrated by pre-clinical trials will provoke clinical trials in this field.
 |
Table 2 List of Advantages and Disadvantages for Nanomedicines Used in Hemorrhagic Stroke |
There are many preclinical models of hemorrhagic stroke, including autologous whole blood infusion, collagenase injection, cisterna magna blood injection, and endovascular perforation. Each of these mimics some aspects of the pathophysiological process after hemorrhagic stroke but differs from clinical conditions in other features.99–102 Therefore, in studying nanomedicine for intracerebral hemorrhage, it is important to select an appropriate model with potential translational purpose. A summary of the advantages and disadvantages of each model is presented in Table 3. Moreover, different models of hemorrhagic strokes lead to a different time-course and severity of BBB disruption which in turn affects the accumulation of NPs. The previous study showed that autologous whole blood infusion-induced BBB disruption peaked at day 5, while collagenase-induced BBB disruption peaked at day 3.103 Compared with autologous whole blood infusion-induced ICH, collagenase injection-induced ICH exhibits a more severe BBB disruption at an earlier stage.103 The BBB disruption in endovascular perforation started 30 min after SAH, lasted for one week, and peaked at 3 and 72 h after surgery.104 In the case of cisterna magna blood injection, the BBB opening started 36 h after SAH, peaked at 48 h, and lasted for 3 days.105 Compared with cisterna magna blood injection, endovascular perforation exhibits an earlier and longer BBB disruption after SAH. Therefore, the collagenase injection and endovascular perforation models of hemorrhagic stroke lead to higher BBB penetration and accumulation of NPs in the brain. The time of administration of NP-based therapeutics should therefore be optimized according to the time of the BBB opening in different models.
 |
Table 3 Advantages or Disadvantages of Preclinical Models for Mimicking Hemorrhagic Stroke in Humans |
The use of nanomedicines also results in potential toxicity and deposition, since the toxicology and degradation processes of many materials are not well known.106 Therefore, clinical use of nanomaterials in hemorrhagic stroke requires further analysis of the safety issues. To avoid the issue of deposition, NPs with hydrodynamic diameters below 6 nm are being promoted for better renal clearance or alternative materials are being designed for intravenous injection with full biodegradability and recyclability by the mononuclear phagocytic system.107,108
The intravenous injection of NPs may activate the platelets or other factors involved in blood coagulation, leading to blood clotting.109 Moreover, intravenously injected NPs may be rapidly cleared from the bloodstream by circulating phagocytic cells and macrophages.110 Biomimetic NPs, which are derived from cellular membranes, provide a solution to this problem. Since they are “invisible” to the phagocytic system and coagulation system, they can prevent thrombogenicity and have a prolonged circulation time.111
Inflammation is an important process involved in secondary injury from hemorrhagic stroke. Targeting inflammation offers new perspectives for developing new nanomedicines. As mentioned above, inflammation after hemorrhagic stroke is featured by infiltration of blood-derived leukocytes and macrophages, activation of resident microglia and astrocytes, and the release of inflammation mediators. Using inflammatory cell membrane-derived nanovesicles can be an effective way to achieve targeted delivery by targeting active endothelial cells after hemorrhagic stroke. In a recent study, neutrophil membrane-derived nanovesicles successfully delivered therapeutics in ischemic stroke.112 Nanomaterials that are responsive to the inflammatory environment, such as to enzymes and pH, offer another direction for designing nanomedicines for hemorrhagic stroke. Neutrophils, which result in brain tissue damage by producing ROS, releasing pro-inflammatory proteases, and disrupting the BBB integrity, can be a valuable target for nanomedicines used in hemorrhagic stroke. Recently, a study in ischemic stroke proved that doxorubicin-loaded albumin protein-formed NPs could induce neutrophil apoptosis, thus preventing brain injury.113
Theragnostic nanomaterials that contain therapeutic drugs and imaging agents to achieve the diagnosis and therapies in single NP platforms are another exciting application of nanomedicine in hemorrhagic stroke. For instance, NPs that contain both cerium NPs and iron oxide NPs successfully achieved concurrent therapy and imaging of ICH.33 It is imperative to develop more theragnostic nanomaterials for concomitant early diagnosis and therapy of hemorrhagic strokes in the future.
NPs with the ability of targeted delivery and controlled release is another direction of designing nanomedicines for hemorrhagic stroke. Ultrasound responsive and iron ion sensitive NPs have been developed for targeted delivery of therapeutics to the hemorrhagic site.66 Recently, an increasing number of stimuli-responsive nanomaterials have been developed. The application of exogenous stimuli-responsive nanocarriers (ie, a magnetic field, ultrasound, light, or electric signal) and endogenous stimuli-responsive nanocarriers (ie, pH, enzyme, or ROS) to hemorrhagic strokes can be attractive since they achieve drug delivery in spatial- and temporal- controlled fashions.114 Moreover, after hemorrhagic stroke, the expressions of many receptors on the BBB are up-regulated, which offers an opportunity for targeted delivery of nanomedicines. Modifying NPs with ligands possessing strong specificity and affinity for these receptors enables the accumulation of NPs at the hemorrhagic site.
Nanomedicines offers a new way for hemorrhagic therapy. However, studies of the application of nanomedicines are still in their infancy and clinical trials involving nano-intervention for hemorrhagic stroke are urgently needed. The animal models used in preclinical experiments should be aligned with appropriate translational research aims. More in-depth studies are needed to focus on the safety of nanomedicines. Biomimetic NPs, NPs targeting inflammation, theragnostic nanomaterials, and NPs with targeted delivery may offer promising directions for designing new nanomedicines for hemorrhagic stroke in the future.
Acknowledgments
This work is supported by the National Key Research& Development Program of China No.2018YFC1312200 to Bo Hu), National Natural Science Foundation of China (No. 82071335 to Quanwei He, No. 82090044 to Bo Hu, No. 82090044 to Bo Hu, No. 81901214 to Yan Wan, No. 82001271 to Jiehong Wu). The author has no other relevant affiliations or financial involvement with any organization or entity with a financial interest in or financial conflict with the subject matter or materials discussed in the manuscript apart from those disclosed.
Disclosure
The authors report no conflicts of interest in this work.
References
1. Smith SD, Eskey CJ. Hemorrhagic stroke. Radiol Clin North Am. 2011;49(1):27–45. doi:10.1016/j.rcl.2010.07.011
2. Yang Q, Tong X, Schieb L, et al. Vital signs: recent trends in stroke death rates—United States, 2000–2015. Morb Mortal Wkly Rep. 2017;66(35):933. doi:10.15585/mmwr.mm6635e1
3. Chen S, Zeng L, Hu Z. Progressing haemorrhagic stroke: categories, causes, mechanisms and managements. J Neurol. 2014;261(11):2061–2078. doi:10.1007/s00415-014-7291-1
4. Caceres JA, Goldstein JN. Intracranial hemorrhage. Emerg Med Clin North Am. 2012;30(3):771–794. doi:10.1016/j.emc.2012.06.003
5. Mendelow AD, Gregson BA, Fernandes HM, et al. Early surgery versus initial conservative treatment in patients with spontaneous supratentorial intracerebral haematomas in the International Surgical Trial in Intracerebral Haemorrhage (STICH): a randomised trial. Lancet. 2005;365(9457):387–397. doi:10.1016/S0140-6736(05)70233-6
6. Mayer SA, Brun NC, Begtrup K, et al. Efficacy and safety of recombinant activated factor VII for acute intracerebral hemorrhage. N Engl J Med. 2008;358(20):2127–2137. doi:10.1056/NEJMoa0707534
7. Post R, Germans MR, Tjerkstra MA, et al. Ultra-early tranexamic acid after subarachnoid haemorrhage (ULTRA): a randomised controlled trial. Lancet. 2021;397(10269):112–118. doi:10.1016/S0140-6736(20)32518-6
8. Vergouwen MD, Meijers JC, Geskus RB, et al. Biologic effects of simvastatin in patients with aneurysmal subarachnoid hemorrhage: a double-blind, placebo-controlled randomized trial. J Cereb Blood Flow Metab. 2009;29(8):1444–1453. doi:10.1038/jcbfm.2009.59
9. Selim M, Foster LD, Moy CS, et al. Deferoxamine mesylate in patients with intracerebral haemorrhage (i-DEF): a multicentre, randomised, placebo-controlled, double-blind Phase 2 trial. Lancet Neurol. 2019;18(5):428–438. doi:10.1016/S1474-4422(19)30069-9
10. Dilnawaz F, Acharya S, Sahoo SK. Recent trends of nanomedicinal approaches in clinics. Int J Pharm. 2018;538(1–2):263–278. doi:10.1016/j.ijpharm.2018.01.016
11. Su S, Kang P. Recent advances in nanocarrier-assisted therapeutics delivery systems. Pharmaceutics. 2020;12(9):837. doi:10.3390/pharmaceutics12090837
12. Zheng H, Chen C, Zhang J, Hu Z. Mechanism and therapy of brain edema after intracerebral hemorrhage. Cerebrovasc Dis. 2016;42(3–4):155–169. doi:10.1159/000445170
13. Hayman EG, Wessell A, Gerzanich V, Sheth KN, Simard JM. Mechanisms of global cerebral edema formation in aneurysmal subarachnoid hemorrhage. Neurocrit Care. 2017;26(2):301–310. doi:10.1007/s12028-016-0354-7
14. Keep RF, Andjelkovic AV, Xiang J, et al. Brain endothelial cell junctions after cerebral hemorrhage: changes, mechanisms and therapeutic targets. J Cereb Blood Flow Metab. 2018;38(8):1255–1275. doi:10.1177/0271678X18774666
15. Chen S, Xu P, Fang Y, Lenahan C. The updated role of the blood brain barrier in subarachnoid hemorrhage: from basic and clinical studies. Curr Neuropharmacol. 2020;18(12):1266–1278. doi:10.2174/1570159X18666200914161231
16. Hu X, Tao C, Gan Q, Zheng J, Li H, You C. Oxidative stress in intracerebral hemorrhage: sources, mechanisms, and therapeutic targets. Oxid Med Cell Longev. 2016;2016:3215391. doi:10.1155/2016/3215391
17. Ayer R, Zhang JH. Oxidative stress in subarachnoid haemorrhage: significance in acute brain injury and vasospasm. In: Acta Neurochir Suppl. Springer; 2008:33–41.
18. Khey KMW, Huard A, Mahmoud SH. Inflammatory pathways following subarachnoid hemorrhage. Cell Mol Neurobiol. 2020;40(5):675–693. doi:10.1007/s10571-019-00767-4
19. Zhang Z, Zhang Z, Lu H, Yang Q, Wu H, Wang J. Microglial polarization and inflammatory mediators after intracerebral hemorrhage. Mol Neurobiol. 2017;54(3):1874–1886. doi:10.1007/s12035-016-9785-6
20. van Lieshout JH, Dibue-Adjei M, Cornelius JF, et al. An introduction to the pathophysiology of aneurysmal subarachnoid hemorrhage. Neurosurg Rev. 2018;41(4):917–930. doi:10.1007/s10143-017-0827-y
21. Ciurea A, Palade C, Voinescu D, Nica D. Subarachnoid hemorrhage and cerebral vasospasm–literature review. J Med Life. 2013;6(2):120.
22. Cordonnier C, Demchuk A, Ziai W, Anderson CS. Intracerebral haemorrhage: current approaches to acute management. Lancet. 2018;392(10154):1257–1268. doi:10.1016/S0140-6736(18)31878-6
23. Sharma D. Perioperative management of aneurysmal subarachnoid hemorrhage. Anesthesiology. 2020;133(6):1283–1305. doi:10.1097/ALN.0000000000003558
24. Liu‐DeRyke X, Rhoney D. Hemostatic therapy for the treatment of intracranial hemorrhage. Pharmacotherapy. 2008;28(4):485–495. doi:10.1592/phco.28.4.485
25. Marcolini E, Stretz C, DeWitt KM. Intracranial hemorrhage and intracranial hypertension. Emerg Med Clin North Am. 2019;37(3):529–544. doi:10.1016/j.emc.2019.04.001
26. Rajajee V, Pandey AS, Williamson CA. Subarachnoid hemorrhage and therapy formerly known as “Triple-H”-new directions. World Neurosurg. 2019;127:500–501. doi:10.1016/j.wneu.2019.04.212
27. Chakravarthi SS, Lyons L, Orozco AR, et al. Combined decompressive hemicraniectomy and port-based minimally invasive parafascicular surgery for the treatment of subcortical intracerebral hemorrhage: case series, technical note, and review of literature. World Neurosurg. 2021;146:e1226–e1235. doi:10.1016/j.wneu.2020.11.130
28. Zipfel GJ. Ultra-early surgery for aneurysmal subarachnoid hemorrhage. J Neurosurg. 2015;122(2):381–382. doi:10.3171/2014.8.JNS141613
29. Yang L, Wang F, Han H, Yang L, Zhang G, Fan Z. Functionalized graphene oxide as a drug carrier for loading pirfenidone in treatment of subarachnoid hemorrhage. Colloids Surf B Biointerfaces. 2015;129:21–29. doi:10.1016/j.colsurfb.2015.03.022
30. Dharmalingam P, Talakatta G, Mitra J, et al. Pervasive genomic damage in experimental intracerebral hemorrhage: therapeutic potential of a mechanistic-based carbon nanoparticle. ACS Nano. 2020;14(3):2827–2846. doi:10.1021/acsnano.9b05821
31. Zheng J, Lu J, Mei S, et al. Ceria nanoparticles ameliorate white matter injury after intracerebral hemorrhage: microglia-astrocyte involvement in remyelination. J Neuroinflammation. 2021;18(1):43. doi:10.1186/s12974-021-02101-6
32. Jeong HG, Cha BG, Kang DW, et al. Ceria nanoparticles synthesized with aminocaproic acid for the treatment of subarachnoid hemorrhage. Stroke. 2018;49(12):3030–3038. doi:10.1161/STROKEAHA.118.022631
33. Cha BG, Jeong H-G, Kang D-W, et al. Customized lipid-coated magnetic mesoporous silica nanoparticle doped with ceria nanoparticles for theragnosis of intracerebral hemorrhage. Nano Res. 2018;11(7):3582–3592. doi:10.1007/s12274-017-1924-5
34. Yang Y, Deng G, Wang P, et al. A selenium nanocomposite protects the mouse brain from oxidative injury following intracerebral hemorrhage. Int J Nanomedicine. 2021;16:775–788. doi:10.2147/IJN.S293681
35. Kang MK, Kim TJ, Kim YJ, et al. Targeted delivery of iron oxide nanoparticle-loaded human embryonic stem cell-derived spherical neural masses for treating intracerebral hemorrhage. Int J Mol Sci. 2020;21(10):3658.
36. Xu C, Qu X. Cerium oxide nanoparticle: a remarkably versatile rare earth nanomaterial for biological applications. NPG Asia Materials. 2014;6(3):e90–e90. doi:10.1038/am.2013.88
37. Kim CK, Kim T, Choi IY, et al. Ceria nanoparticles that can protect against ischemic stroke. Angew Chem Int Ed Engl. 2012;51(44):11039–11043. doi:10.1002/anie.201203780
38. Kwon HJ, Cha MY, Kim D, et al. Mitochondria-targeting ceria nanoparticles as antioxidants for alzheimer’s disease. ACS Nano. 2016;10(2):2860–2870. doi:10.1021/acsnano.5b08045
39. Kwon HJ, Kim D, Seo K, et al. Ceria nanoparticle systems for selective scavenging of mitochondrial, intracellular, and extracellular reactive oxygen species in parkinson’s disease. Angew Chem Int Ed Engl. 2018;57(30):9408–9412. doi:10.1002/anie.201805052
40. Zachara BA. Selenium and selenium-dependent antioxidants in chronic kidney disease. Adv Clin Chem. 2015;68:131–151.
41. Estelrich J, Escribano E, Queralt J, Busquets MA. Iron oxide nanoparticles for magnetically-guided and magnetically-responsive drug delivery. Int J Mol Sci. 2015;16(4):8070–8101. doi:10.3390/ijms16048070
42. Samuel EL, Duong MT, Bitner BR, Marcano DC, Tour JM, Kent TA. Hydrophilic carbon clusters as therapeutic, high-capacity antioxidants. Trends Biotechnol. 2014;32(10):501–505. doi:10.1016/j.tibtech.2014.08.005
43. Liu J, Cui L, Losic D. Graphene and graphene oxide as new nanocarriers for drug delivery applications. Acta Biomater. 2013;9(12):9243–9257. doi:10.1016/j.actbio.2013.08.016
44. Kiew SF, Kiew LV, Lee HB, Imae T, Chung LY. Assessing biocompatibility of graphene oxide-based nanocarriers: a review. J Control Release. 2016;226:217–228. doi:10.1016/j.jconrel.2016.02.015
45. Chang CZ, Wu SC, Lin CL, Kwan AL. Curcumin, encapsulated in nano-sized PLGA, down-regulates nuclear factor kappaB (p65) and subarachnoid hemorrhage induced early brain injury in a rat model. Brain Res. 2015;1608:215–224. doi:10.1016/j.brainres.2015.02.039
46. Zhang Z-Y, Jiang M, Fang J, et al. Enhanced therapeutic potential of nano-curcumin against subarachnoid hemorrhage-induced blood–brain barrier disruption through inhibition of inflammatory response and oxidative stress. Mol Neurobiol. 2017;54(1):1–14. doi:10.1007/s12035-015-9635-y
47. Li M, Liu G, Wang K, et al. Metal ion-responsive nanocarrier derived from phosphonated calix[4]arenes for delivering dauricine specifically to sites of brain injury in a mouse model of intracerebral hemorrhage. J Nanobiotechnology. 2020;18(1):61. doi:10.1186/s12951-020-00616-3
48. Mo Y, Duan L, Yang Y, et al. Nanoparticles improved resveratrol brain delivery and its therapeutic efficacy against intracerebral hemorrhage. Nanoscale. 2021;13(6):3827–3840. doi:10.1039/D0NR06249A
49. Chung CY, Yang JT, Kuo YC. Polybutylcyanoacrylate nanoparticles for delivering hormone response element-conjugated neurotrophin-3 to the brain of intracerebral hemorrhagic rats. Biomaterials. 2013;34(37):9717–9727. doi:10.1016/j.biomaterials.2013.08.083
50. You ZQ, Wu Q, Zhou XM, et al. Receptor-mediated delivery of astaxanthin-loaded nanoparticles to neurons: an enhanced potential for subarachnoid hemorrhage treatment. Front Neurosci. 2019;13:989. doi:10.3389/fnins.2019.00989
51. Zi L, Zhou W, Xu J, et al. Rosuvastatin nanomicelles target neuroinflammation and improve neurological deficit in a mouse model of intracerebral hemorrhage. Int J Nanomedicine. 2021;16:2933–2947. doi:10.2147/IJN.S294916
52. Zhu F, Zi L, Yang P, et al. Efficient Iron and ROS nanoscavengers for brain protection after intracerebral hemorrhage. ACS Appl Mater Interfaces. 2021;13(8):9729–9738. doi:10.1021/acsami.1c00491
53. Chonpathompikunlert P, Fan C-H, Ozaki Y, Yoshitomi T, Yeh C-K, Nagasaki Y. Redox nanoparticle treatment protects against neurological deficit in focused ultrasound-induced intracerebral hemorrhage. Nanomedicine. 2012;7(7):1029–1043. doi:10.2217/nnm.12.2
54. Tian XH, Wang ZG, Meng H, et al. Tat peptide-decorated gelatin-siloxane nanoparticles for delivery of CGRP transgene in treatment of cerebral vasospasm. Int J Nanomedicine. 2013;8:865–876. doi:10.2147/IJN.S39951
55. El-Say KM, El-Sawy HS. Polymeric nanoparticles: promising platform for drug delivery. Int J Pharm. 2017;528(1–2):675–691. doi:10.1016/j.ijpharm.2017.06.052
56. Danhier F, Ansorena E, Silva JM, Coco R, Le Breton A, Preat V. PLGA-based nanoparticles: an overview of biomedical applications. J Control Release. 2012;161(2):505–522. doi:10.1016/j.jconrel.2012.01.043
57. Dash TK, Konkimalla VB. Poly-small je, Ukrainian-caprolactone based formulations for drug delivery and tissue engineering: a review. J Control Release. 2012;158(1):15–33.
58. Grossen P, Witzigmann D, Sieber S, Huwyler J. PEG-PCL-based nanomedicines: a biodegradable drug delivery system and its application. J Control Release. 2017;260:46–60. doi:10.1016/j.jconrel.2017.05.028
59. Li Y, Gao J, Zhang C, et al. Stimuli-responsive polymeric nanocarriers for efficient gene delivery. Top Curr Chem. 2017;375(2):27. doi:10.1007/s41061-017-0119-6
60. Duan J, Zhang Y, Chen W, et al. Cationic polybutyl cyanoacrylate nanoparticles for DNA delivery. J Biomed Biotechnol. 2009;2009:149254. doi:10.1155/2009/149254
61. Lin Y, Pan Y, Shi Y, Huang X, Jia N, Jiang JY. Delivery of large molecules via poly(butyl cyanoacrylate) nanoparticles into the injured rat brain. Nanotechnology. 2012;23(16):165101. doi:10.1088/0957-4484/23/16/165101
62. Madkhali O, Mekhail G, Wettig SD. Modified gelatin nanoparticles for gene delivery. Int J Pharm. 2019;554:224–234. doi:10.1016/j.ijpharm.2018.11.001
63. Galho AR, Cordeiro MF, Ribeiro SA, et al. Protective role of free and quercetin-loaded nanoemulsion against damage induced by intracerebral haemorrhage in rats. Nanotechnology. 2016;27(17):175101. doi:10.1088/0957-4484/27/17/175101
64. Marques MS, Cordeiro MF, Marinho MAG, et al. Curcumin-loaded nanoemulsion improves haemorrhagic stroke recovery in wistar rats. Brain Res. 2020;1746:147007. doi:10.1016/j.brainres.2020.147007
65. Wang F, Teng Z, Liu D, Wang Y, Lou J, Dong Z. beta-caryophyllene liposomes attenuate neurovascular unit damage after subarachnoid hemorrhage in rats. Neurochem Res. 2020;45(8):1758–1768. doi:10.1007/s11064-020-03037-8
66. Miao YF, Peng T, Moody MR, et al. Delivery of xenon-containing echogenic liposomes inhibits early brain injury following subarachnoid hemorrhage. Sci Rep. 2018;8(1):450. doi:10.1038/s41598-017-18914-6
67. Takanashi Y, Ishida T, Meguro T, Kiwada H, Zhang JH, Yamamoto I. Efficacy of intrathecal liposomal fasudil for experimental cerebral vasospasm after subarachnoid hemorrhage. Neurosurgery. 2001;48(4):894–901. doi:10.1097/00006123-200104000-00041
68. Mohsen K, Azzazy HME, Allam NK, Basalious EB. Intranasal lipid nanocapsules for systemic delivery of nimodipine into the brain: in vitro optimization and in vivo pharmacokinetic study. Mater Sci Eng C Mater Biol Appl. 2020;116:111236. doi:10.1016/j.msec.2020.111236
69. Kim H, Britton GL, Peng T, Holland CK, McPherson DD, Huang SL. Nitric oxide-loaded echogenic liposomes for treatment of vasospasm following subarachnoid hemorrhage. Int J Nanomedicine. 2014;9:155–165. doi:10.2147/IJN.S48856
70. Allen TM, Cullis PR. Liposomal drug delivery systems: from concept to clinical applications. Adv Drug Deliv Rev. 2013;65(1):36–48. doi:10.1016/j.addr.2012.09.037
71. Ishida T, Harashima H, Kiwada H. Liposome clearance. Biosci Rep. 2002;22(2):197–224. doi:10.1023/A:1020134521778
72. Yan X, Scherphof GL, Kamps JA. Liposome opsonization. J Liposome Res. 2005;15(1–2):109–139. doi:10.1081/LPR-64971
73. Hosny KM, Khallaf RA, Asfour HZ, et al. Development and optimization of cinnamon oil nanoemulgel for enhancement of solubility and evaluation of antibacterial, antifungal and analgesic effects against oral microbiota. Pharmaceutics. 2021;13(7):1008. doi:10.3390/pharmaceutics13071008
74. Jaromin A, Parapini S, Basilico N, et al. Azacarbazole n-3 and n-6 polyunsaturated fatty acids ethyl esters nanoemulsion with enhanced efficacy against Plasmodium falciparum. Bioact Mater. 2021;6(4):1163–1174. doi:10.1016/j.bioactmat.2020.10.004
75. Nel J, Desmet CM, Driesschaert B, Saulnier P, Lemaire L, Gallez B. Preparation and evaluation of trityl-loaded lipid nanocapsules as oxygen sensors for electron paramagnetic resonance oximetry. Int J Pharm. 2019;554:87–92. doi:10.1016/j.ijpharm.2018.11.007
76. Moura RP, Pacheco C, Pego AP, Des Rieux A, Sarmento B. Lipid nanocapsules to enhance drug bioavailability to the central nervous system. J Control Release. 2020;322:390–400. doi:10.1016/j.jconrel.2020.03.042
77. Sang LY, Liang YX, Li Y, et al. A self-assembling nanomaterial reduces acute brain injury and enhances functional recovery in a rat model of intracerebral hemorrhage. Nanomedicine. 2015;11(3):611–620. doi:10.1016/j.nano.2014.05.012
78. Zhang N, Luo Y, He L, Zhou L, Wu W. A self-assembly peptide nanofibrous scaffold reduces inflammatory response and promotes functional recovery in a mouse model of intracerebral hemorrhage. Nanomedicine. 2016;12(5):1205–1217. doi:10.1016/j.nano.2015.12.387
79. Park J, Kim JY, Choi SK, et al. Thermo-sensitive assembly of the biomaterial REP reduces hematoma volume following collagenase-induced intracerebral hemorrhage in rats. Nanomedicine. 2017;13(6):1853–1862. doi:10.1016/j.nano.2017.04.001
80. Gelain F, Luo Z, Zhang S. Self-assembling peptide EAK16 and RADA16 nanofiber scaffold hydrogel. Chem Rev. 2020;120(24):13434–13460. doi:10.1021/acs.chemrev.0c00690
81. Somaa FA, Wang TY, Niclis JC, et al. Peptide-based scaffolds support human cortical progenitor graft integration to reduce atrophy and promote functional repair in a model of stroke. Cell Rep. 2017;20(8):1964–1977. doi:10.1016/j.celrep.2017.07.069
82. Yokoi H, Kinoshita T, Zhang S. Dynamic reassembly of peptide RADA16 nanofiber scaffold. Proc Natl Acad Sci U S A. 2005;102(24):8414–8419. doi:10.1073/pnas.0407843102
83. Ellis-Behnke RG, Liang YX, You SW, et al. Nano neuro knitting: peptide nanofiber scaffold for brain repair and axon regeneration with functional return of vision. Proc Natl Acad Sci U S A. 2006;103(13):5054–5059. doi:10.1073/pnas.0600559103
84. Guo J, Su H, Zeng Y, et al. Reknitting the injured spinal cord by self-assembling peptide nanofiber scaffold. Nanomedicine. 2007;3(4):311–321. doi:10.1016/j.nano.2007.09.003
85. Holmes TC, de Lacalle S, Su X, Liu G, Rich A, Zhang S. Extensive neurite outgrowth and active synapse formation on self-assembling peptide scaffolds. Proc Natl Acad Sci. 2000;97(12):6728–6733. doi:10.1073/pnas.97.12.6728
86. Cao H, Liu T, Chew SY. The application of nanofibrous scaffolds in neural tissue engineering. Adv Drug Deliv Rev. 2009;61(12):1055–1064. doi:10.1016/j.addr.2009.07.009
87. Kam L, Shain W, Turner J, Bizios R. Axonal outgrowth of hippocampal neurons on micro-scale networks of polylysine-conjugated laminin. Biomaterials. 2001;22(10):1049–1054. doi:10.1016/S0142-9612(00)00352-5
88. Otero-Ortega L, Gomez de Frutos MC, Laso-Garcia F, et al. Exosomes promote restoration after an experimental animal model of intracerebral hemorrhage. J Cereb Blood Flow Metab. 2018;38(5):767–779. doi:10.1177/0271678X17708917
89. Shen H, Yao X, Li H, et al. Role of exosomes derived from miR-133b modified MSCs in an experimental rat model of intracerebral hemorrhage. J Mol Neurosci. 2018;64(3):421–430. doi:10.1007/s12031-018-1041-2
90. Gong Y, Wang Y, Qu Q, et al. Nanoparticle encapsulated core-shell hydrogel for on-site BMSCs delivery protects from iron overload and enhances functional recovery. J Control Release. 2020;320:381–391. doi:10.1016/j.jconrel.2020.01.029
91. Lim TC, Mandeville E, Weng D, et al. Hydrogel-based therapy for brain repair after intracerebral hemorrhage. Transl Stroke Res. 2020;11(3):412–417. doi:10.1007/s12975-019-00721-y
92. Zhu Q, Gong Y, Guo T, et al. Thermo-sensitive keratin hydrogel against iron-induced brain injury after experimental intracerebral hemorrhage. Int J Pharm. 2019;566:342–351. doi:10.1016/j.ijpharm.2019.05.076
93. Guo T, Guo Y, Gong Y, et al. An enhanced charge-driven intranasal delivery of nicardipine attenuates brain injury after intracerebral hemorrhage. Int J Pharm. 2019;566:46–56. doi:10.1016/j.ijpharm.2019.05.050
94. Xu J, Duan Z, Qi X, et al. Injectable gelatin hydrogel suppresses inflammation and enhances functional recovery in a mouse model of intracerebral hemorrhage. Front Bioeng Biotechnol. 2020;8:785. doi:10.3389/fbioe.2020.00785
95. He Y, Qu Q, Luo T, et al. Human hair keratin hydrogels alleviate rebleeding after intracerebral hemorrhage in a rat model. ACS Biomater Sci Eng. 2019;5(2):1113–1122. doi:10.1021/acsbiomaterials.8b01609
96. Liao W, Du Y, Zhang C, et al. Exosomes: the next generation of endogenous nanomaterials for advanced drug delivery and therapy. Acta Biomater. 2019;86:1–14. doi:10.1016/j.actbio.2018.12.045
97. Karavasili C, Fatouros DG. Smart materials: in situ gel-forming systems for nasal delivery. Drug Discov Today. 2016;21(1):157–166. doi:10.1016/j.drudis.2015.10.016
98. Anselmo AC, Mitragotri S. Nanoparticles in the clinic. Bioeng Transl Med. 2016;1(1):10–29. doi:10.1002/btm2.10003
99. Pedard M, El Amki M, Lefevre-Scelles A, Compere V, Castel H. Double direct injection of blood into the cisterna magna as a model of subarachnoid hemorrhage. J Vis Exp. 2020;162:e61322.
100. Kirkman MA, Allan SM, Parry-Jones AR. Experimental intracerebral hemorrhage: avoiding pitfalls in translational research. J Cereb Blood Flow Metab. 2011;31(11):2135–2151. doi:10.1038/jcbfm.2011.124
101. James ML, Warner DS, Laskowitz DT. Preclinical models of intracerebral hemorrhage: a translational perspective. Neurocrit Care. 2008;9(1):139–152. doi:10.1007/s12028-007-9030-2
102. Sehba FA. The rat endovascular perforation model of subarachnoid hemorrhage. Acta Neurochir Suppl. 2015;120:321–324. doi:10.1007/978-3-319-04981-6_55
103. Jia P, He J, Li Z, et al. Profiling of blood-brain barrier disruption in mouse intracerebral hemorrhage models: collagenase injection vs. autologous arterial whole blood infusion. Front Cell Neurosci. 2021;15:699736. doi:10.3389/fncel.2021.699736
104. Li Z, Liang G, Ma T, et al. Blood-brain barrier permeability change and regulation mechanism after subarachnoid hemorrhage. Metab Brain Dis. 2015;30(2):597–603. doi:10.1007/s11011-014-9609-1
105. Germano A, d’Avella D, Imperatore C, Caruso G, Tomasello F. Time-course of blood-brain barrier permeability changes after experimental subarachnoid haemorrhage. Acta neurochirurgica. 2000;142(5):575–581. doi:10.1007/s007010050472
106. Wu D, Ma Y, Cao Y, Zhang T. Mitochondrial toxicity of nanomaterials. Sci Total Environ. 2020;702:134994. doi:10.1016/j.scitotenv.2019.134994
107. Croissant JG, Fatieiev Y, Khashab NM. Degradability and clearance of silicon, organosilica, silsesquioxane, silica mixed oxide, and mesoporous silica nanoparticles. Adv Mater. 2017;29(9). doi:10.1002/adma.201604634
108. Bonnard T, Jayapadman A, Putri JA, et al. Low-fouling and biodegradable protein-based particles for thrombus imaging. ACS Nano. 2018;12(7):6988–6996. doi:10.1021/acsnano.8b02588
109. Starsich FH, Herrmann IK, Pratsinis SE. Nanoparticles for biomedicine: coagulation during synthesis and applications. Annu Rev Chem Biomol Eng. 2019;10:155–174. doi:10.1146/annurev-chembioeng-060718-030203
110. Bourquin J, Milosevic A, Hauser D, et al. Biodistribution, clearance, and long-term fate of clinically relevant nanomaterials. Adv Mater. 2018;30(19):e1704307. doi:10.1002/adma.201704307
111. Luk BT, Zhang L. Cell membrane-camouflaged nanoparticles for drug delivery. J Control Release. 2015;220:600–607. doi:10.1016/j.jconrel.2015.07.019
112. Dong X, Gao J, Zhang CY, Hayworth C, Frank M, Wang Z. Neutrophil membrane-derived nanovesicles alleviate inflammation to protect mouse brain injury from ischemic stroke. ACS Nano. 2019;13(2):1272–1283. doi:10.1021/acsnano.8b06572
113. Zhang CY, Dong X, Gao J, Lin W, Liu Z, Wang Z. Nanoparticle-induced neutrophil apoptosis increases survival in sepsis and alleviates neurological damage in stroke. Sci Adv. 2019;5(11):eaax7964. doi:10.1126/sciadv.aax7964
114. Mi P. Stimuli-responsive nanocarriers for drug delivery, tumor imaging, therapy and theranostics. Theranostics. 2020;10(10):4557–4588. doi:10.7150/thno.38069
 © 2022 The Author(s). This work is published and licensed by Dove Medical Press Limited. The
full terms of this license are available at https://www.dovepress.com/terms.php
and incorporate the Creative Commons Attribution
- Non Commercial (unported, v3.0) License.
By accessing the work you hereby accept the Terms. Non-commercial uses of the work are permitted
without any further permission from Dove Medical Press Limited, provided the work is properly
attributed. For permission for commercial use of this work, please see paragraphs 4.2 and 5 of our Terms.
© 2022 The Author(s). This work is published and licensed by Dove Medical Press Limited. The
full terms of this license are available at https://www.dovepress.com/terms.php
and incorporate the Creative Commons Attribution
- Non Commercial (unported, v3.0) License.
By accessing the work you hereby accept the Terms. Non-commercial uses of the work are permitted
without any further permission from Dove Medical Press Limited, provided the work is properly
attributed. For permission for commercial use of this work, please see paragraphs 4.2 and 5 of our Terms.
