Back to Journals » International Journal of Women's Health » Volume 14
Knowledge and Perceptions of Chinese Female College Students Towards HIV/AIDS: A Qualitative Analysis
Received 17 May 2022
Accepted for publication 25 August 2022
Published 7 September 2022 Volume 2022:14 Pages 1267—1280
DOI https://doi.org/10.2147/IJWH.S374976
Checked for plagiarism Yes
Review by Single anonymous peer review
Peer reviewer comments 2
Editor who approved publication: Professor Elie Al-Chaer
Mengying Qiu,1 Yijin Wu2
1School of English Studies, Sichuan International Studies University, Chongqing, 400031, People’s Republic of China; 2School of Translation Studies, Qufu Normal University, Rizhao, 276825, People’s Republic of China
Correspondence: Yijin Wu, School of Translation Studies, Qufu Normal University, No. 5, Yantai Road, Donggang District, Rizhao, Shandong, 250100, People’s Republic of China, Tel/Fax +86 531 88377118, Email [email protected]
Objective: This study aims to explore knowledge and perceptions of Chinese female college students towards HIV/AIDS.
Design, Method, Participants and Setting: A purposive sampling method was used to recruit participants. Twenty female participants studying at a college located in Chongqing, Southwest China, were involved in the study. Semi-structured interviews were used to collect data. The face-to-face interview data were recorded and analyzed using the method of qualitative inductive content analysis.
Results: Five themes were identified from the data of transcribed interviews: HIV transmission routes (sexual transmission; blood transmission; mother-to-child transmission), sources of HIV/AIDS knowledge (education; mass media), AIDS prevention measures (avoiding sexual activity; establishing sense of self-protection; avoiding blood contact), attitudes towards PLWHA (treating all PLWHA equally; showing sympathy for the innocent PLWHA; discriminating against the immoral PLWHA), and suggested solutions to combat AIDS (assistance provided by governments; what health professionals can contribute; mobilization of social power; university intervention).
Conclusion: More efforts should be made to strengthen the HIV/AIDS education for female college students of non-medical majors in Southwest China. Accurate knowledge of HIV/AIDS and the right attitudes towards people living with HIV/AIDS (PLWHA) should be the foci of HIV/AIDS education for this population. In order to better cater future sex education in colleges to the requirements of female college students, educators and lawmakers may benefit from gaining a deeper grasp of their perspectives on HIV/AIDS.
Keywords: HIV/AIDS, female college students, China, qualitative content analysis
Introduction
The Acquired Immune Deficiency Syndrome (AIDS), caused by human immunodeficiency virus (HIV), is a kind of malignant infectious disease with extremely high mortality rate.1 HIV attacks the human body’s immune system, gradually causing the infected person less resistant to various diseases and eventually leading to death.2 So far, there has been no effective vaccine to prevent it and no effective treatment for the disease.3 HIV/AIDS persists to be a major concern in the domain of public health worldwide.
Young people are one of the populations that are affected by the HIV epidemic.4 Women and girls take up 48% of new HIV infections worldwide and the impact of AIDS is particularly noticeable among adolescent girls and young women.5 There is a growing concern with respect to HIV/AIDS knowledge, attitude and behavior among female college students in Asia and the US. Female college students in Japan and Bangladesh had high level of knowledge concerning HIV/AIDS.6,7 However, a survey showed female students from a university in Saudi Arabia had low awareness of HIV/AIDS knowledge.8 Investigations into American female college students of Hispanic and black ethnicities revealed that female college students sought HIV prevention information online or from particular forms of media, changing their attitudes towards HIV.9–12 They became more likely to get tested for HIV11 and adopt self-protective behaviors.12 A number of studies have found that female college students were vulnerable to HIV infection due to gender inequality and insufficient sexual education.13–15
AIDS has become the leading cause of death in China.16 In China, the HIV transmission route was mainly heterosexual contact.17 During 2007–2018, the overall rates of new diagnosis of HIV/AIDS increased 2.18 times among Chinese women.18 Sexual activity, including high-risk sexual behavior such as unprotected commercial sex, has become commonplace among Chinese female college students.13 However, studies on Chinese female college students’ knowledge and perceptions regarding HIV/AIDS are limited. Therefore, we aim to probe into the HIV/AIDS knowledge and perceptions of female college students with a qualitative approach to generate insights into HIV/AIDS intervention in college education. Qualitative health research examines cultural perception of disease and responses to illness19 and the focus is to describe or explore the individual experiences and perspectives.20 A qualitative study will be implicative to professionals when developing educational and behavior change interventions in university settings.21
Methods
Study Design
This study employed a qualitative method using semi-structured interviews22 to investigate knowledge and perceptions of Chinese female college students towards HIV/AIDS. During November, 2020 and February, 2021, face-to-face interviews were conducted to explore the knowledge and perceptions of Chinese female college students towards HIV/AIDS. Based on the interview data, this study provided detailed descriptions of knowledge and perceptions of Chinese university students regarding the HIV/AIDS. The method of qualitative inductive content analysis20,23 was used to describe views of Chinese female college students on HIV/AIDS. Results were presented in accordance with the consolidated criteria for reporting qualitative research (CO-REQ).24
Sampling Procedure and Participants
Purposive sampling was used to recruit participants. Twenty female students from a university located in Chongqing, Southwest China, were involved in this study. Although the first author and the 20 participants were from the same university, the first author was not acquainted with the 20 participants before the recruitment. Prior to the interview, the first author spent three weeks to get to know those 20 participants about their basic information and to explain the research objectives and ethical issues to the participants. Table 1 illustrated the demographic characteristics of participants. Variations in age, area of origin, and academic major among participants were taken into account to reach diversity in their knowledge and perceptions of AIDS. Their ages ranged from 19 to 23, with 18 English majors, one international politics major and one diplomacy major. Five of them were sophomores, ten seniors and five juniors. The freshmen were excluded due to their much later start of the school year. Fifteen (75%, N=20) participants’ hometowns were located in Western China, five (25%, N=20) in Eastern China. Seven of them (35%, N=20) were from rural areas and the rest (65%, N=20) were from urban areas.
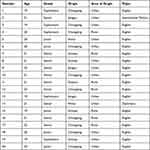 |
Table 1 Participant Demographic Data |
Interview and Procedure
Recruitment and interviews were conducted by the first author in Chinese during November, 2020 and February, 2021 at a university located in the city of Chongqing, Southwest China. The interview guideline was modified after a pilot interview designed to fit the research objectives. The modified interview guide questions for each participant were listed in Table 2. Interview questions focused on ways to gain knowledge on HIV/AIDS, preventive measures, attitudes towards HIV/AIDS, assistance to people living with HIV/AIDS and HIV/AIDS education intervention. These questions were all open-ended to allow the participants to offer adequate exploration of each interview guide. The interview continued until no new data were generated. The average duration of the interviews for the present study is 31 minutes.
 |
Table 2 Interview Guide |
Data Analysis
Prior to analysis, the data of interviews were audio recorded and all transcribed verbatim in Chinese. Content analysis, frequently employed in qualitative research, was first used to examine religious hymns, newspaper and magazine articles, advertisements, and political speeches in the 19th century.20 Based on textual material, content analysis uses systematic coding and categorization to identify trends and patterns in the words used to provide a profound understanding of the participants’ experiences and perspectives regarding the research topic.25 There are two methods used in the analysis process: inductive and deductive content analysis. In this study, we used an inductive content analysis method. If there is not enough former knowledge about the phenomenon or if this knowledge is fragmented, the inductive approach is recommended.26 Hence, inductive content analysis has no pre-set theoretical framework. Rather, inductive content analysis by means of coding and categorizing is performed to create theories from the data.
Constant comparative method27 was used to spot, categorize, scrutinize and verify emerging themes to achieve data saturation.28,29 The analysis primarily included five steps. Firstly, all researchers independently checked the transcribed data repetitively by looking over the transcripts while carefully listening to the audio data to obtain a general understanding of the meaning conveyed. Next, significant meaning units were independently identified by each researcher as open codes in the data reduction process. Then, those meaningful units were rephrased in more condensed ones into description close to the original written text of the transcripts until sub-themes were produced. In the fourth step, sub-themes were organized into themes. Finally, the main themes were created and described. The authors of this study independently returned to the raw interview data, determined what themes were identified from the data and then compared and contrasted all the themes until consensus was reached in order to ensure consistency in coding30 and establish trustworthiness.
Trustworthiness
Credibility, dependability, confirmability, authenticity and transferability were used to determine the trustworthiness of the findings.20,31 Accordingly, the following measures were taken to ensure the trustworthiness: (1) ensuring all sections of the study design available for review by all researchers; (2) employing purposive sampling to obtain the participant group; (3) keeping a record of reflection on prior discussions and opinions about the research; (4) permitting open peer review for decisions made, as a means of the audit trail. Researchers regularly (once a week) kept records to track processes and decision-making throughout the analytical procedure; (5) ensuring the value of agreement rates in intercoder reliability was over 80% by all researchers.32
Ethical Considerations
The study complies with the Declaration of Helsinki and was approved by the ethics committee of Qufu Normal University (QFNUN2021-01). All methods were performed in accordance with the relevant guidelines and regulations. The research objectives and its voluntary nature were explained to participants in advance. All participants were informed of the study procedures and notified that the interview would be audio-recorded and would not affect their academic performance. Written informed consent, including publication of anonymized responses, was obtained from all participants prior to the face-to-face interview. Confidentiality was guaranteed by listing numbers instead of names (eg Participant 1= P1) and participants’ self-identification content was excluded from the transcripts.
Results
Five themes were identified through the detailed analysis of the transcribed interviews, that is, HIV transmission routes, sources of HIV/AIDS knowledge, AIDS prevention measures, attitudes towards PLWHA, and suggested solutions to combat AIDS, as shown in Table 3.
 |
Table 3 Key Themes and Subthemes |
Theme 1: HIV Transmission Routes
Most participants had a good understanding of the major routes of HIV transmission, among which the most frequently mentioned three were sexual transmission, blood transmission and mother-to-child transmission. Sexual transmission is “the main mode of transmission” (P3, P4) and “more likely occur between gays” (P20). Participants also mentioned three sub-routes of blood transmission. The first is via blood contact with the wound of an AIDS patient, as P3 described, “If you have a bleeding wound, you may get the disease when you touch the wound of an AIDS patient.” The second is “through sharing pinholes in blood donation” as P4 described. The third is sharing the pinholes when taking drugs, as P19 reported,
I heard that drug abusers are sharing a syringe together, and this may also lead to the spread of the virus of AIDS.
Compared with sexual and blood transmission, mother-to-child transmission was “the least likely for college students” (P13). In addition, P12 stated,
The teacher emphasized that the virus would not be transmitted via saliva, so I knew that the virus would not be transmitted through saliva.
Theme 2: Sources of HIV/AIDS Knowledge
Education and mass media are the two major sources for participants to gain access to HIV/AIDS knowledge: (1) education, including school education and family education; (2) mass media, including printed and digitalized media.
Education
School education was the primary source for participants to learn about HIV/AIDS.
I began to know about AIDS mainly through biology courses in junior high or senior high and came to know more about it in universities through relevant elective courses or lectures [P1]
In addition to the courses, P4 said,
I received the information of AIDS through campus publicity such as banners, billboards, posters and pamphlets.
Some participants mentioned they also learnt about HIV/AIDS from their parents who sometimes would tell them sexual knowledge, including HIV/AIDS. Their parents, however, were not proactive in telling them more about AIDS, which was just mentioned in passing at their convenience without going into further details.
My parents shared the news story relevant to AIDS with only an oblique reference of the word “rape”, of which the meaning was left for me to figure out. [P19]
Mass Media
Rather than proactively seeking HIV-related information, the participants knew about HIV/AIDS as a byproduct of reading news and books or watching TV/films. Some participants incidentally learned about HIV/AIDS from traditional forms of media such as books, films and TV series. P17 reported,
I remembered that I read a book Insight by Chai Jing, a female journalist. The book mentioned AIDS in one unit about a gay man she interviewed quite long ago when less is known about AIDS.
In addition to books, P13 mentioned she acquired HIV/AIDS-related knowledge from films and TV series by chance,
I remember there is a film called the Grand Budapest Hotel or something like that. I learned from the film that cures for AIDS may be relatively scarce. Now, I’m watching the American TV series called Deadly Woman, in one episode where there is a gay man and he seems to have AIDS, and his face is blotched.
Some participants reported that they incidentally read online news with AIDS-related titles by browsing the website Baidu (the world’s biggest Chinese-language search engine).
Inadvertently, I see news related to AIDS with an eye-catching title, but often I won’t click it to learn more since such news often suggests negative information. [P12]
Theme 3: AIDS Prevention Measures
Three sub-themes were identified from participants’ knowledge about AIDS prevention measures: (1) avoiding sexual activity; (2) establishing a sense of self-protection; and (3) avoiding blood contact.
Avoiding Sexual Activity
Avoiding sexual activity before marriage was the baseline of morality, which could eliminate the risk of getting sexually transmitted HIV. As P2 remarked,
To keep distance means I won’t have sex with a boy before marriage. I’m not sure whether he is healthy or an HIV-infected person. He may be sexually active and may have a good number of sexual partners, which is also dangerous.
P19 disclosed that she had never been in a relationship, let along sexual intercourse, thus sparing herself from being sexually infected with HIV,
If college students are looking for their sexual partners, consider the safety issues first. For me, I may never have such sexual behavior so easily.
P5 pointed out college students lacked both sexual knowledge and parental supervision, so their behavior may become undisciplined. She suggested, “don’t check in a hotel to have sex with strangers.”
Establishing a Sense of Self-Protection
Some participants thought nowadays college students are more open to sex, so it was acceptable for them to have sex but they could, in various forms, protect themselves from being infected from HIV. P3 stated,
Firstly, keep personal hygiene. If you want to have sex, be sure to take preventive measures, for instance, to wear a condom. Secondly, if done without any preventive measures, it is strongly suggested to go to the hospital to have an HIV test, don’t feel shame to do so. Otherwise, you may spread the virus to another sexual partner.
P4 further suggested not go to places such as discos or night clubs where good and evil people mixed up, and said,
If you leave your table for a short while, then your drink will probably be poisoned and you are thus in a dangerous situation in which you are likely to be raped, but you don’t know if the man who poisoned the drink is living with HIV/AIDS or not.
Another proposed way to self-protect was to keep chastity and be cautious with strangers when hanging out.
Keep away from blind date apps such as Tantan or MOMO where there may be AIDS patients seeking a one-night stand. [P18]
Avoiding Blood Contact
Some participants reported that since blood is one of the HIV transmission routes, preventing HIV infection can be said to avoid blood infection, so they suggested students should be careful with blood in a number of situations. P5 mentioned one occasion that may run the risk of blood infection was blood donation and said,
If college students want to donate blood, they should go to qualified medical institutions, because used needles will probably be recycled in small clinics where the sanitary conditions are unqualified and the recycled needles might carry HIV.
Blood infection may also be occasioned by “getting tattoos or doing plastic surgeries” (P11). P19 said another way for blood contact was the drug,
One of the ways to stay away from HIV was to stay away from drugs, because I heard drug abusers are sharing a syringe together, which might also lead to the spread of the virus.
Additionally, P8 mentioned,
If students who are in a relationship start cohabitation, it is suggested not to share toothbrush or razors with their partners.
Theme 4: Attitudes Towards PLWHA
Participants revealed mixed attitudes towards PLWHA, including equal treatment to all PLWHA, bias against and sympathy for specific groups of PLWHA.
Treating All PLWHA Equally
Some participants stated that AIDS patients should be treated equally regardless of their sexes or sexual orientations. P15 noted, “AIDS patients, men or women, should be treated as ordinary people who do not have AIDS.” P14 noted this disease is more common in gay men, so we should not discriminate against their disease, nor their sexual orientations, but respect them:
I think that everyone has certain kind of sexual orientation, behavior and personality that God has given him. I think they shouldn’t be discriminated against since the world is inherently diverse and tolerant of differences. [P14]
However, equal treatment does not mean obsessive concern, according to P15,
We should not give them too much care, or look at them in a special way, because I think this will instead create a psychological burden for them. They will feel that they are different from others, being isolated and marginalized.
Showing Sympathy for the Innocent PLWHA
Many participants noted that the bias against PLWHA was often associated with the stereotype that PLWHA were definitely infected via sexual transmission. However, considering how the virus is transmitted, some participants also pointed out that PLWHA may have infected the virus unknowingly or through other means out of sex, and they showed their sympathy to this group of PLWHA. As P17 described,
If the virus was infected via mother-to-child transmission, then they were born to be infected … In fact, most of the time I think they are very pitiful and innocent. In such a case, they should not be discriminated against, I think.
P3 held similar view,
We should not downgrade the impression of a person as soon as we know he has got HIV, but display more understanding and compassion rather than discrimination, because we know that although AIDS patients may run the risk of HIV transmission, they may probably not suffer from the virus via sexually transmitted diseases.
If AIDS patients got infected with HIV without knowing it, then people should feel pathetic for them, as P19 shared a story she heard,
A police officer with a wound in his hand fought against a gangster with HIV, the gangster intentionally cut the officer’s hand with a knife and pressed his bleeding hand close to the policeman’s wound. And then the police officer would be very much likely to get infected and if so, we cannot discriminate against the police officer.
Discriminating Against the Immoral PLWHA
Some participants revealed their discrimination; however, it was not against all PLWHA but restricted to specific groups of them who had intentional wrongdoings and were irresponsible for their behaviors. The negative attitude towards treatment was one of the reasons for discrimination, as P4 remarked,
Just imagine, if a person with HIV knows he has got infected and he is also a drug abuser with a strong drug addiction, but he doesn’t take any measures for drug rehabilitation, against which should be discriminated.
Malicious harm was another cause for some participants’ discrimination. As P10 noted,
If an AIDS patient retaliates against the society or deliberately infects others by spreading the virus, then I think this person should be discriminated against and will be further denounced.
Theme 5: Suggested Solutions to Combat AIDS
Participants provided possible AIDS-combatting solutions, focusing on reducing stigma and discrimination against HIV/AIDS. Governments and societies were suggested to offer media, legal and financial support, medical and health institutions were encouraged to provide technical and emotional support, and schools were expected to take the educational intervention.
Assistance Provided by Governments
Participants shared their opinions on what assistance governments can provide, including introducing HIV/AIDS knowledge and proper attitudes towards PLWHA, giving policy guidance on laws concerning the legitimate rights of PLWHA, and increasing investments to ensure better and affordable treatment for PLWHA.
Many participants agreed that the greatest assistance that governments can provide was transmitting knowledge of AIDS to larger groups of the public. In addition, P20 suggested that
A proper attitude towards AIDS should also be facilitated, because governments have long tried on the advocacy work of AIDS, laying stress on its prevention and control, but little is observed on the promotion of zero-discrimination awareness.
Macro guidance on treatment policies and laws pertaining to AIDS patients’ rights and interests were proposed as well. Governments were suggested to offer legal protection to the patients, as P14 remarked,
As far as the government is concerned, it can provide immediate assistance by improving the legislation system for them. By doing so, at least AIDS patients have acquired legal dignity and rights. Under such protection, they are not being discriminated against or disrespected, to some extent.
Another assistance by governments was increasing investment on medical research and development.
People feel fearful for AIDS due to the lack of vaccine to cure it. If the government gives more investments to research institutions to solve this problem, I think, the fear for AIDS will be lessened and thus the discrimination will also be reduced. [P10]
What Health Professionals Can Contribute
Participants concluded the efforts to end the epidemic provided by medical and health institutions are primarily twofold: (1) privacy protection for patients and (2) medical service improvement.
Participants thought healthcare providers should not treat AIDS patients differently from other patients. The top priority for health professionals was to abide by their professional ethics, and they should, to the participants’ knowledge, keep the secrets of AIDS patients. P4 emphasized,
I think the most important thing for medical institutions is to protect the privacy of these AIDS patients, because these patients may be reluctant to let others know about their experiences and after all, many people have bias towards this disease.
According to the participants, the motivation to improve medical service was first to provide better medicine to relieve AIDS patients’ distress and then to meet their psychological and emotional needs. P4 suggested,
I think that the hospital should set up an AIDS center, and then provide them with comprehensive, professional and sustainable medical treatment.
P9 further remarked,
Since AIDS patients’ pains are both physical and emotional, the treatment should include not only physical treatment, but also psychological counseling, which reduces their pains and prolongs their lifespan.
Mobilization of Social Power
A variety of measures taken by societies, domestic or overseas, can help to fight against HIV/AIDS. The most frequently mentioned forms of assistance were fund-raising, volunteer activities, and support from international communities.
Participants proposed both traditional and novel ways for fund-raising. P1 suggested, “the direct way is a call for donations of money and goods to AIDS patients.” P15 described “step donation” as a new and popular way for fund-raising in China. She stated,
On your smart phones, you can upload the steps you walk every day onto apps such as WeChat. With a cumulation of the steps you can invite large charity companies to help convert the number of steps into money to be donated. This has already been done to help out those poor people living in mountainous areas. And now I think the beneficiaries can also be expanded to the AIDS group.
Many participants also suggested volunteers should regularly organize social activities for the patients to treat PLWHA like ordinary people. P3 proposed,
Psychological assistance can be provided by our social workers in the community, or by some voluntary groups, special medical organizations. For example, they can regularly pay visits to the AIDS patients, comfort them, or give them financial support, and provide them with jobs or opportunities to have communication with other AIDS patients.
Some participants pointed out treating AIDS needs international cooperation from both public and private organizations. P11 said,
The only international organization I know is the Red Ribbon. If we just rely on the Red Ribbon or larger state-owned organizations, then it won’t have a substantial effort. So, I think we should mobilize some private charity organizations to help PLWHA.
University Intervention
Most of the participants suggested the universities should strengthen (1) the prevention of HIV/AIDS with a focus on offering practical and high-quality health education courses and (2) the control of HIV/AIDS with an emphasis on cultivating students’ awareness of sexual safety precautions.
According to some participants, schools should provide comprehensive sexuality education, including HIV/AIDS courses. Many of the participants demanded the courses provided by the school should be compulsory. As P15 explained,
If it is an optional lecture, then fewer people would go, … if fewer people go to the lectures, then it won’t contribute to reducing the discrimination towards HIV/AIDS.
Participants thought nowadays college students hold more open attitudes towards sex, so schools are responsible for the availability of HIV self-testing and contraception products as preventive measures. As P5 said,
At the lobby of the teaching building, I saw the vending machine selling the HIV self-testing kit. The school should ensure students can have easy access to rapid HIV self-testing for safety purposes and the vending machine settings in our campus should be regularly examined to ensure current testing availability. Actually, this has already been done by the school as one preventive measure. Also, I think the school should also ensure the availability of contraception products.
Participants considered it practical for them to engage in extracurricular activities in an array of forms to fight against AIDS, including (1) quiz shows on HIV/AIDS knowledge, (2) speech contests with HIV/AIDS themes, and (3) student community activities. In addition, P2 emphasized animation created on social apps as a novel way in recruiting students in the participation of doing AIDS publicity campaign:
In WeChat, tweets with animation generated by H5, a technology frequently used, can make the reading experience more interesting, because I think it would be very passive for students to finish questionnaires. Instead, the same data or information on a questionnaire can be displayed with animated pictures via WeChat.
Discussion
The study found that participants had a good understanding of HIV transmission routes. In addition to the transmission routes, they also gained other knowledge about HIV/AIDS, through school education, mass media and parenting. Participants showed both biased and unbiased attitudes towards PLWHA and proposed a number of solutions intervened by different agencies to combat AIDS with a focus on reducing stigma towards PLWHA.
Results showed that most participants demonstrated their basic knowledge of the primary transmission modes of HIV, which confirmed the existing findings about Chinese college students’ HIV/AIDS knowledge.33–35 However, the participants seldom continued to tell more details about their knowledge of HIV/AIDS, especially high-risk sexual conducts of AIDS. Similar findings were obtained in prior investigations1,36 which reported that Chinese students who majored in medicine displayed richer knowledge on the HIV/AIDS than those who majored in humanities and social sciences. A study on the HIV-related knowledge and perceptions among American undergraduates showed similar result that students who majored in health and kinesiology were more knowledgeable about HIV than those who majored in physical sciences, mathematics, engineering, and business or education, humanities, and social sciences.21 We suggest that awareness about HIV/AIDS among female college students who majored in non-medical sciences still needs to be strengthened in the future.
This study showed participants’ HIV/AIDS education was accomplished by school courses and they hoped schools could provide comprehensive sexuality education. This coincides with the finding that 60.3% of the Chinese female college students hoped that in the future they can acquire health education knowledge from lectures delivered by health professionals or elective courses provided by schools.37
In addition to schools and the Internet, parenting was also a source of HIV/AIDS knowledge for the participants. Similar to a finding from a study conducted on Chinese college students in both China and the US, family education as a means of gaining HIV/AIDS knowledge was far less frequently observed.38 With respect to the contents of parental communication on HIV precaution, discrepancy is found between participants in this study and American black female college students with sexual experiences. As the results show, participants’ parents were inclined to tell them the sexual knowledge in a vague manner, emphasizing the negative consequences of HIV infection and unwilling to go to details. However, American female students who were sexually active had open conversations about HIV/STD (sexually transmitted diseases) knowledge with their parents.39 This contrast could be attributed to the factor that the participants and their American counterparts have different ways to enhance their contraceptive awareness regarding their different sexual behavior statuses. Many of the participants self-disclosed they had never been in a relationship, let alone being sexually active. Moreover, research has shown that Chinese families are unwilling to discuss sexual behavior.40 While in the US, the rate of sexually active female college students was reported to be much higher than that of China13 and quite a number of them had multiple sexual partners, which rendered them more susceptible to HIV, and they proactively exchange information about sex, including STD diseases such as AIDS, from their communication with parents, peers or friends.9
The results highlight the importance of re-examination of public and individual beliefs and understandings about HIV/AIDS. Findings of this study demonstrated participants had complicated perceptions towards PLWHA: some participants did not discriminate against AIDS patients and they showed sympathy for them, while other participants still had bias against AIDS patients, which is supported by studies that reported college students’ prejudice against AIDS group remained widespread.41,42 Our study found there was no significant difference in discrimination between students of rural and urban origins, different from a study which reported that college students from the rural areas of China tended to have more discrimination than those from the urban areas of China.13 This difference may stem from the purposive sampling of this study. Nonetheless, a study conducted on Chinese female college students revealed that their attitudes toward AIDS patients did not change significantly after health education intervention, and they still had antipathy to AIDS patients.37 The reason may be that the health education focused on the knowledge of reproductive health and the basic knowledge of AIDS, but neglected the knowledge of the correct attitude toward AIDS patients. The stigma will remain as an obstacle to realizing the goal of zero-discrimination, as one of the 2021–2026 goals of UNAIDS.5 The primary focus for effective health education is to raise students’ awareness and change their attitudes, thus maintaining a proper belief in a change of behavior.43 Good-quality health education can enhance students’ knowledge on HIV/AIDS, develop their positive attitudes towards PLWHA and reduce their HIV-and AIDS-related discrimination and stigma.44 Therefore, continued efforts in reducing the discrimination and stigma towards PLWHA are needed in future school-based comprehensive sexual education.
This study generates implementation insights into combating AIDS from the perspective of female college students. They have proposed quite specific policies that need intervention by different agencies aiming at reducing the negative attitudes towards HIV/AIDS and PLWHA. A study has investigated into service providers’ perspectives of HIV/AIDS stigma reduction intervention.45 However, little has been known about college students’ solutions on HIV/AIDS stigma reduction. The participants proposed detailed stigma reduction measures intervened by not only health service providers and governments, but also college students themselves.
Participants reported that China has made great advances in fighting against AIDS. The opinion accords with the finding from one study stating that China has achieved significant strides in combating HIV, implementing laws and regulations to enhance the well-being of PLWHA and offer prevention services to both individuals and communities.46 For example, the idea of a comprehensive care cascade was first introduced in the 2018 Chinese National Guidelines for HIV/AIDS Diagnosis and Treatment, which promotes coupling of diagnosis with treatment and management services within HIV care centers and engagement of a coordinated, multidisciplinary team to ensure the provision of comprehensive care.47 It is essential to alleviate the stigma against PLWHA; however, as the participants suggested, undue attention to PLWHA would give this population psychological burden and consequently undermine their well-being. Therefore, the study suggests lawmakers should be cautious in laying down and enforcing regulations that neither make AIDS patients feel that they receive discrimination nor make them feel overly concerned.
“Step donation”, the novel practice participants proposed, is launched on smartphone apps such as WeChat or Alipay and has been proven to be practical in fund-raising for poverty alleviation in China. Presumably, this can also be applied to fund-raising for AIDS treatment in China and to other countries, especially those with high HIV incidence. Insufficiency of investments was also observed by participants. It is noteworthy that HIV investment target for 2020 was not met. A 17% increase in investment in HIV treatment can result in a 35% increase in treatment coverage by 2025.5 To sum up, it is suggested to increase investment in treatment for people with AIDS, entitling them with legal rights in various settings. We believe those novel suggestions proposed by participants may contribute to producing positive and desirable outcomes for PLWHA in the future.
The findings highlighted the active roles of young people as participants engaging in an array of activities fighting against AIDS. The youths can have active involvement in initiating activities like filming and uploading short videos for HIV/AIDS prevention via multiple digital platforms of social media such as WeChat and Weibo in HIV/AIDS education intervention. This may serve as a means of peer education on sexual health program. A recent study has demonstrated that WeChat is effective to increase HIV-and AIDS-related knowledge, improve attitudes and reduce stigma and it shows the potential to implement WeChat educational intervention to college students because they have wide access to digital products.44 Mobile-based health interventions via a variety of social media platforms have recently been burgeoning in health education research.48 Public media contribute significantly to enhancing the HIV awareness and it is indispensable in HIV prevention among young adults.49 In China, mass media are one of the influential forces to scale up the efforts over the timing and course of HIV control by bringing news of HIV to the attention of the public and policymakers.50 As the results show, media are passive channel for students to gain HIV/AIDS knowledge. However, by promoting short videos for HIV prevention purposes on their smart phones or other digital devices, or by donating steps as ways of fund-raising via social apps such as WeChat, the college students can transform the passivity into initiative in the peer education of HIV/AIDS. To reduce stigma towards people with HIV/AIDS is still an essential part in educating college students. Thus, new media can be considered as a new way of peer-led college-based HIV/AIDS education to facilitate the elimination of the bias against PLWHA. This will be an integral component of the strenuous efforts to scale up effective HIV prevention intervention and education.
Strengths and Limitations
A qualitative inductive content analysis is employed to explore female college students’ knowledge and perceptions of HIV/AIDS. Face-to-face interviews provide the opportunity to obtain sufficient in-depth information with respect to the female youths’ perspectives on combating HIV/AIDS, including novel practices such as step donation as one means of fund-raising for PLWHA. The strength of content analysis reveals the complexity of individual mixed feelings towards HIV/AIDS, which cannot be obtained by means of numerical data and statistical techniques. Limitations include the study’s transferability that limits it to specific geographic and cultural context and the retrospective nature of the interviews compared with quantitative studies.
Conclusion
This study showed female college students gained a good understanding of HIV transmission routes but their awareness about HIV/AIDS was lower than that of medical majors. More efforts should be intensified in intervening the HIV/AIDS education on female college students of non-medical majors in areas with lower levels of economy and education. Correct knowledge of HIV/AIDS and non-discriminatory attitudes towards people living with HIV/AIDS (PLWHA) should be the foci of college-based HIV/AIDS education. To reduce HIV-related stigma, college students are suggested to have active involvement in HIV/AIDS prevention campaign via a variety of means. In order to better cater future sex education in colleges to the requirements of female college students, educators and lawmakers may benefit from gaining a deeper grasp of their perspectives on HIV/AIDS.
Abbreviations
HIV, human immunodeficiency virus; AIDS, Acquired Immune Deficiency Syndrome; UNAIDS, Joint United Nations Programme on HIV/AIDS; PLWHA, people living with HIV/AIDS; STD, sexually transmitted diseases.
Data Sharing Statement
The data analyzed during the current study are not publicly available due its sensitivity but are available from the corresponding author on reasonable request.
Consent for Publication
All participants have given consent for publication. Written informed consent, including publication of anonymized responses, was obtained from all study participants.
Acknowledgments
We would like to thank all the female college students for their participation.
Author Contributions
All authors made a significant contribution to the work reported, whether that is in the conception, study design, execution, acquisition of data, analysis and interpretation, or in all these areas; took part in drafting, revising or critically reviewing the article; gave final approval of the version to be published; have agreed on the journal to which the article has been submitted; and agree to be accountable for all aspects of the work.
Funding
This work was supported by Sichuan International Studies University [grant number 5001/222117016], [grant number 0202/676021], [grant number 5051/300501001].
Disclosure
The authors declare that they have no competing interests.
References
1. Sun X, Fan L, Chang C, Shi Y. HIV/AIDS related perception and behavior: a comparative study among college students of different majors in China. Int J Nurs Sci. 2020;7:S74–S79. doi:10.1016/j.ijnss.2020.07.010
2. Ellenberg SS, Morris JS. AIDS and COVID: a tale of two pandemics and the role of statisticians. Stat Med. 2021;40(11):2499–2510. doi:10.1002/sim.8936
3. Teng T, Shao Y. Scientific approaches to AIDS prevention and control in China. Adv Dent Res. 2011;23(1):10–12. doi:10.1177/0022034511398871
4. Tseng Y, Cheng C, Kuo S, Hou W, Chan T, Chou F. Safe sexual behaviors intention among female youth: the construction on extended theory of planned behavior. J Adv Nurs. 2020;76(3):814–823. doi:10.1111/jan.14277
5. Joint United Nations Programme on HIV/AIDS (UNAIDS). End inequalities, end AIDS: global AIDS strategy 2021–2026; 2020. Available from: https://www.unaids.org/sites/default/files/media_asset/global-AIDS-strategy-2021-2026_en.pdf.
6. Maswanya E, Moji K, Aoyagi K, et al. Knowledge and attitudes toward AIDS among female college students in Nagasaki, Japan. Health Educ Res. 2000;15(1):5–11. doi:10.1093/her/15.1.5
7. Mou S, Bhuiya F, Islam SS. Knowledge and perceptions of sexually transmitted diseases, HIV/AIDS, and reproductive health among female students in Dhaka, Bangladesh. Int J Adv Med Health Res. 2015;2(1):9. doi:10.4103/2349-4220.159118
8. Zaini R, Anjum F. Awareness of HIV/AIDS among female students attending college of applied medical sciences at Taif University. Int J Lab Med Res. 2015;1(1). doi:10.15344/2455-4006/2015/104
9. Chandler R, Canty-Mitchell J, Kip KE, et al. College women’s preferred HIV prevention message mediums: mass media versus interpersonal relationships. J Assoc Nurs AIDS Care. 2013;24(6):491–502. doi:10.1016/j.jana.2012.09.001
10. Cobb Payton F, Kvasny L, Kiwanuka-Tondo J. Online HIV prevention information: how black female college students are seeking and perceiving. Internet Res. 2014;24(4):520–542. doi:10.1108/IntR-09-2013-0193
11. Jones SG, Jones R, Fenkl EA, Lacroix-Williams L, Simon S, Chadwell K. Acceptability of the “Love, Sex, & Choices” HIV prevention intervention by Hispanic female college students. Hisp Health Care Int. 2021;19(2):112–117. doi:10.1177/1540415320976644
12. Kvasny L, Payton FC. Managing hypervisibility in the HIV prevention information-seeking practices of black female college students. J Assoc Info Sci Technol. 2018;69(6):798–806. doi:10.1002/asi.24001
13. Chen M, Liao Y, Liu J, et al. Comparison of sexual knowledge, attitude, and behavior between female Chinese college students from urban areas and rural areas: a hidden challenge for HIV/AIDS control in China. Biomed Res Int. 2016;2016:1–10. doi:10.1155/2016/8175921
14. Higgins LT, Sun C. Gender, social background and sexual attitudes among Chinese students. Cult Health Sex. 2007;9(1):31–42. doi:10.1080/13691050600963914
15. McCoy SI, Watts CH, Padian NS. Preventing HIV infection: turning the tide for young women. Lancet. 2010;376(9749):1281–1282. doi:10.1016/S0140-6736(10)61309-8
16. Disease Control Bureau of National Health Commission of the People’s Republic of China. An overview of 2019 national notifiable diseases. Chin J Viral Dis. 2020;10(4):245. in Chinese.
17. Lönn E, Sahlholm K, Maimaiti R, Abdukarim K, Andersson R. A traditional society in change encounters HIV/AIDS: knowledge, attitudes, and risk behavior among students in northwestern China. AIDS Patient Care St. 2007;21(1):48–56. doi:10.1089/apc.2006.0063
18. Zhang Y, Cai C, Wang X, et al. Disproportionate increase of new diagnosis of HIV/AIDS infection by sex and age — China, 2007−2018. China CDC Weekly. 2020;2(5):69–74. doi:10.46234/ccdcw2020.020
19. Morse J. What is qualitative health research? In: Denzin NK, Lincoln YS, editors. The SAGE Handbook of Qualitative Research.
20. Kyngäs H, Mikkonen K, Kääriäinen M. The Application of Content Analysis in Nursing Science Research. Switzerland: Springer; 2020.
21. Smith ML, La Place LL, Menn M, Wilson KL. HIV-related knowledge and perceptions by academic major: implications for university interventions. Front Public Health. 2014;2:1–18. doi:10.3389/fpubh.2014.00018
22. Kallio H, Pietilä AM, Johnson M, Kangasniemi M. Systematic methodological review: developing a framework for a qualitative semi-structured interview guide. J Adv Nurs. 2016;72(12):2954–2965. doi:10.1111/jan.13031
23. Krippendorff KH. Content Analysis: An Introduction to Its Methodology. Thousand Oaks, CA: Sage; 2004.
24. Tong A, Sainsbury P, Craig J. Consolidated criteria for reporting qualitative research (COREQ): a 32-Item checklist for interviews and focus groups. Int J Qual Health Care. 2007;19(6):349–357. doi:10.1093/intqhc/mzm042
25. Vaismoradi M, Turunen H, Bondas T. Content analysis and thematic analysis: implications for conducting a qualitative descriptive study: qualitative descriptive study. Nurs Health Sci. 2013;15(3):398–405. doi:10.1111/nhs.12048
26. Elo S, Kyngäs H. The qualitative content analysis process. J Adv Nurs. 2008;62(1):107–115. doi:10.1111/j.1365-2648.2007.04569.x
27. Strauss AL, Corbin JM. Basics of Qualitative Research: Techniques and Procedures for Developing Grounded Theory.
28. Vanderhaeghen B, Bossuyt I, Menten J, et al. What is good advance care planning according to hospitalized palliative patients and their families? An explorative study. J Palliat Care. 2020;35(4):236–242. doi:10.1177/0825859720938583
29. Whitehead K, Ala-Leppilampi K, Lee B, et al. Factors that determine the experience of transition to an inpatient palliative care unit for patients and caregivers: a qualitative study. J Palliat Care. 2022:082585972211050. doi:10.1177/08258597221105001
30. Zhang Q, Wu Y, Li M, et al. Epidemic prevention during work resumption: a case study of one Chinese company’s experience. Front Public Health. 2021;8:596332. doi:10.3389/fpubh.2020.596332
31. Lincoln YS, Guba EG. Naturalistic Inquiry. Beverly Hills, Calif: Sage Publications; 1985.
32. Burla L, Knierim B, Barth J, Liewald K, Duetz M, Abel T. From text to codings: intercoder reliability assessment in qualitative content analysis. Nurs Res. 2008;57(2):113–117. doi:10.1097/01.NNR.0000313482.33917.7d
33. Liu C, Bai Q, Zhao H, Zhang Q, Wen Y. Investigation of college students’ cognitive degree of AIDS and analysis of health education countermeasures. Chin J Nurs Pract Res. 2020;17(10):22–25. doi:10.3969/j.issn.1672-9676.2020.10.008
34. Lyu J, Shen X, Hesketh T. Sexual knowledge, attitudes and behaviours among undergraduate students in China—implications for sex education. IJERPH. 2020;17(18):6716. doi:10.3390/ijerph17186716
35. Zhang L, Yu H, Luo H, et al. HIV/AIDS-Related knowledge and attitudes among Chinese college students and associated factors: a cross-sectional study. Front Public Health. 2022;9:804626. doi:10.3389/fpubh.2021.804626
36. Albrektsson M, Alm L, Tan X, Andersson R. HIV/AIDS awareness, attitudes and risk. behavior among university students in Wuhan, China. Open AIDS J. 2009;3:55–62. doi:10.2174/1874613600903010055
37. Yang L, Li F, Ma Y, Zhao X. Cognition status of acquired immune deficiency syndrome of female college students and intervention effects. Chin J Woman Child Health Res. 2017;28(3):243–245. doi:10.3969/j.issn.1673-5293.2017.03.008
38. Tung W-C, Cook DM, Lu M, Yang W. HIV knowledge and behavior among Chinese college students in China and the United States. West J Nurs Res. 2013;35(9):1171–1183. doi:10.1177/0193945913486201
39. Chandler R, Anstey EH, Ross H, Morrison-Beedy D. Perceptions of black college women on barriers to HIV-Risk reduction and their HIV prevention intervention needs. J Assoc Nurs AIDS Care. 2016;27(4):392–403. doi:10.1016/j.jana.2016.01.004
40. Wang X, Jin Y, Tian M, et al. Safe-sex behavioral intention of Chinese college students: examining the effect of sexual knowledge using the theory of planned behavior. Front Psychol. 2022;13:805371. doi:10.3389/fpsyg.2022.805371
41. Wang L, Luo T, Pei HL, Wh F, Dai JH. Research progress on university students’ AIDS discrimination and exclusion. Occup Health. 2019;22:3162–3168. doi:10.13329/j.cnki.zyyjk.2019.0846
42. Ruan F, Fu G, Zhou M, et al. Application of the Chinese version of Zelaya’s HIV-related stigma scale to undergraduates in mainland China. BMC Public Health. 2019;19(1):1708. doi:10.1186/s12889-019-8054-9
43. Dadipoor S, Ghaffari M, Safari-Moradabadi A. University students and AIDS: a systematic review of knowledge, attitudes towards AIDS in Iran. Int J Adolesc Youth. 2020;25(1):861–871. doi:10.1080/02673843.2020.1758173
44. Zha P, Mahat G, Qureshi R, et al. Utilising a WeChat intervention to improve HIV and AIDS education among college students in China. Health Educ J. 2021;80(8):1002–1013. doi:10.1177/00178969211023084
45. Wu S, Li L, Wu Z, et al. A brief HIV stigma reduction intervention for service providers in China. AIDS Patient Care STDS. 2008;22(6):513–520. doi:10.1089/apc.2007.0198
46. Wu Z, Chen J, Scott SR, McGoogan JM. History of the HIV epidemic in China. Curr HIV/AIDS Rep. 2019;16(6):458–466. doi:10.1007/s11904-019-00471-4
47. Cao W, Hsieh E, Li T. Optimizing treatment for adults with HIV/AIDS in China: successes over two decades and remaining challenges. Curr HIV/AIDS Rep. 2020;17(1):26–34. doi:10.1007/s11904-019-00478-x
48. Guo Y, Hong YA, Qiao J, et al. Run4Love, a mHealth (WeChat-based) intervention to improve mental health of people living with HIV: a randomized controlled trial protocol. BMC Public Health. 2018;18(1):793. doi:10.1186/s12889-018-5693-1
49. Dehghani B, Dehghani A, Sarvari J. Knowledge and awareness regarding Hepatitis B, Hepatitis C, and Human Immunodeficiency Viruses among college students: a report from Iran. Int Q Community Health Educ. 2020;41(1):15–23. doi:10.1177/0272684X19896727
50. Wu Z, Sullivan SG, Wang Y, Rotheram-Borus MJ, Detels R. Evolution of China’s response to HIV/AIDS. Lancet. 2007;369(9562):679–690. doi:10.1016/S0140-6736(07)60315-8
 © 2022 The Author(s). This work is published and licensed by Dove Medical Press Limited. The full terms of this license are available at https://www.dovepress.com/terms.php and incorporate the Creative Commons Attribution - Non Commercial (unported, v3.0) License.
By accessing the work you hereby accept the Terms. Non-commercial uses of the work are permitted without any further permission from Dove Medical Press Limited, provided the work is properly attributed. For permission for commercial use of this work, please see paragraphs 4.2 and 5 of our Terms.
© 2022 The Author(s). This work is published and licensed by Dove Medical Press Limited. The full terms of this license are available at https://www.dovepress.com/terms.php and incorporate the Creative Commons Attribution - Non Commercial (unported, v3.0) License.
By accessing the work you hereby accept the Terms. Non-commercial uses of the work are permitted without any further permission from Dove Medical Press Limited, provided the work is properly attributed. For permission for commercial use of this work, please see paragraphs 4.2 and 5 of our Terms.
