Back to Journals » Infection and Drug Resistance » Volume 13
Knowledge and Beliefs of Health Care Professionals Towards Antimicrobial Resistance in Hiwot Fana Specialized University Hospital, in Harar, Ethiopia
Authors Gebrehiwot Z, Tadiwos Y
Received 17 March 2020
Accepted for publication 16 June 2020
Published 30 June 2020 Volume 2020:13 Pages 2027—2035
DOI https://doi.org/10.2147/IDR.S254237
Checked for plagiarism Yes
Review by Single anonymous peer review
Peer reviewer comments 3
Editor who approved publication: Professor Suresh Antony
Zufan Gebrehiwot, Yohannes Tadiwos
School of Pharmacy, College of Health and Medical Sciences, Haramaya University, Harar, Ethiopia
Correspondence: Yohannes Tadiwos
School of Pharmacy, College of Health and Medical Sciences, Haramaya University, Harar, Ethiopia
Tel +251 912039585
Email [email protected]
Background: Antimicrobial resistance (AMR) results in treatment failure and spread of the infection, which will cause prolonged illness, increased mortality, and financial burdens. Some factors that are responsible for inappropriate use of antimicrobials include lack of expertise by health care professionals and problems in diagnosis.
Objective: To assess the knowledge and belief related to AMR among health care professionals in HFSUH in Harar, Ethiopia.
Methodology: A cross-sectional study was conducted on 153 physicians, nurses, and pharmacists from HFSUH, which were selected using stratified sampling with proportional allocation. Data were collected from March 1 to March 30, 2017, and were analyzed using the Statistical Package for Social Sciences (SPSS 20.0).
Results: Only 132 participants were willing to participate from the 153 health care providers; of whom, 35 (26.5%) were physicians, 86 (65.2%) were nurses, and 11 (8.3%) were pharmacists. MRSA was mentioned as the prominent resistant bacteria by 74.3% of the physician, 59.3% of the nurses, and 63.6% of the pharmacists. The majority consider the overuse of antibiotics, poor infection control, sub-standard antibiotic, and patients’ poor adherence as factors for AMR. AMR was considered a problem worldwide, country, and hospital level. Forty percent of the physicians, 32.6% of the nurses, and 63.6% of the pharmacists consider the patient influence on the prescriber as the cause; whereas, 31.4% of the physician, 48.8% nurses, and 36.4% of the pharmacists consider the failure of previous treatment as the major cause of unnecessary antimicrobial prescription.
Conclusion: The information the health care professionals have about the different resistant bacteria, on the different factors that cause unnecessary antibiotic prescription and on how to use susceptibility testing is low. All professionals should take regular AMR training and select antibiotics based on tests and minimize the risk of AMR.
Keywords: antimicrobial resistance, health care professionals, Hiwot Fana Specialized University Hospital
Introduction
Antibiotics that treat bacterial infection either kill the bacteria or prevent its multiplication.1 They are among the most important medicines ever discovered.2,3 They are used for combating bacterial infections thus reducing morbidity and mortality and have made the management of infectious disease easier.4,5 The lives of many have been saved because of their discovery in the early 1930.2
When a previously sensitive microorganism (some or all sub-populations of a microorganism) becomes resistant to an antimicrobial agent, antimicrobial resistance (AMR) happens.2,6 It develops because of a defense mechanism developed by the pathogen, such as gene alteration or acquiring resistant gene.7 Resistant microorganisms can withstand attack by antimicrobial, resulting in treatment failure and spread of the infection.8
Infections due to resistant microorganisms are a real threat since they cause prolonged illness, increased communicability, mortality, and financial burdens.4,9,10 It leads to longer and more expensive hospital stays, the use of second and third choice drugs, increasing treatment costs, and ultimately may lead to death.6 This global health problem11 also has a social, economic, and political impact.12 With a declining choice of antibiotics and with aggravation of AMR, we may enter into a “post-antibiotic” era.13,14 With this pace, by 2050 the problem of AMR might lead to the majority of death in the world, with a cost estimate of 100 trillion dollars.15
Factors that lead to the progression of AMR include inappropriate selection or misuse of antimicrobials, environmental contamination, inappropriate dosage regimen, self-medication, poor infection prevention, and poor drug quality.14,16 Some factors that are responsible for inappropriate use of antimicrobials include lack of expertise by health care professionals’, problems in diagnosis, and lack of knowledge by patients.4,17 In regards to health care professionals, factors that contribute to AMR development include lack of adequate or recent information regarding the usage of antimicrobials, lack of resources in the identification of a pathogen, and its susceptibility to antimicrobials, absence of guidelines in selecting the antimicrobials and poor antimicrobial stewardship.18 One way of combating resistance is to educate members of the public and health care professionals about AMR and assess their knowledge and practice regarding AMR.19 This involves changing the antimicrobial prescribing behavior and the use of antimicrobials by health professionals.20 Thus, assessing health care professionals’ knowledge and belief can be used as a baseline for a possible containment of AMR and also for framing antibiotic policy.17,21
Methodology
Study Design, Period and Setting
A cross-sectional study was carried out in Hiwot Fana Specialized University Hospital (HFSUH), Harar, Ethiopia, which is located 526 km east from Addis Ababa. Eligible physicians, pharmacists, and nurses were selected among the total physicians, pharmacists, and nurses working in HFSUH. The data were collected from March 1–30, 2017.
Source Population
The primary source populations for this study were all pharmacists, physicians, and nurses that were working in Harar town, Ethiopia.
Study Population
The sample populations for this study were those pharmacists, physicians, and nurses that were rendering service in HFSUH during the time of data collection.
Sample Size Determination
A single population proportion formula was used to calculate the sample size of 384. Then, a reduction formula was used since the number of those health care professionals working in HFSUH was 235 to obtain a reduced sample size of 146. Then, the final sample size of 153 was obtained after adding a 5% contingency.
Sampling Technique
Stratified sampling with proportional allocation was used to collect data from 42 physicians, 99 nurses’ and 12 pharmacists in this study, whose numbers were determined by proportionally allocating the professionals based on the final sample size and the number of physicians, nurses and pharmacists working in HFSUH.
Data Collection and Analysis
A self-administered questionnaire was used to collect information on the knowledge and belief of health care professionals, towards AMR. The questionnaire was developed by the first investigator by viewing other researches and was later modified. Before the actual study, the questionnaire was pretested on 5 health professionals. The collected data were checked for its completeness, accuracy, and clarity after the collection. Statistical Package for Social Sciences (SPSS) was used for the analysis of the collected data. A P-value of < 0.05 was considered statistically significant.
Result
Participants’ Profiles and Sources of Information on AMR
Only 132 participants were willing to participate in the study from the 153 health care providers; of whom, 35 (26.5%) were physicians, 86 (65.2%) were nurses, and 11 (8.3%) were pharmacists. The overall response rate of participants was 86.3%. The majority of the participants were male, 95 (72%), and were in the age group of 22–27, 97 (73.5%). Having recent information about AMR was mentioned by 74.3% of physicians, 47.7% of nurses, and 90.9% of pharmacists. Overall, 91.4% of physicians, 47.7% of nurses, and 36.4% pharmacists got information from relevant books. Other sources of information include the internet (for 16.3% of nurses and 27.3% of the pharmacists), and college or university courses and training (for 5.7% of the physician, 31.4% of the nurses, and 18.2% of the pharmacist). Regarding training, 74.3% of the physicians, 84.4% of the nurses, and 72.7% of the pharmacist responded that they did not attend training regarding AMR (Table 1).
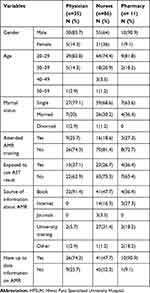 |
Table 1 Profiles of Health Care Professionals’ Working in HFSUH |
Knowledge About the Cause of AMR and Antibiotic-Resistant Bacteria
The factors that were considered by the health care providers for AMR occurrence were widespread or overuse of antibiotics (97.1% physician, 77.9% nurses and 100% pharmacist, p = 0.010), usage of broad-spectrum antibiotics (80% physician, 55.8% nurses and 81.8 pharmacists, p=0.019), poor hand washing (80% physicians, 81.4% nurses and 36.4% pharmacists, p=0.003). Hundred percent of the physicians and the pharmacists and 81.4% of the nurses considered bacterial mutations as the cause of AMR (p=0.008). Patients’ poor adherence to prescribed antibiotics was considered as a factor by 97% physician, 93% nurses, and 100% pharmacist. Hundred percent of physicians, 88.4% nurses, and 90.9% pharmacists consider poor infection control in hospitals as a factor for the spread of AMR. 100% of the physicians, 86% of nurses, and 90.9% of pharmacists say that substandard qualities of antibiotics promote AMR. Overall, more than 90% of the practitioners consider poor infection control in the hospital, sub-standard qualities of antibiotic and patients’ poor adherence as factors which promote AMR (Table 2).
 |
Table 2 Health Care Professionals’ Knowledge About the Causes of Antibiotic Resistance and Antibiotic-Resistant Bacteria in HFSUH |
From the different pathogens that are associated with drug resistance, methicillin-resistant staphylococcus aureus (MRSA) was mentioned as the prominent bacteria by the majority (74.3% of the physician, 59.3% of the nurses, and 63.6% of the pharmacists). MDR-TB was considered resistant by 22.9% of the physicians, 37.2% of the nurses, and 36.4% of the pharmacist. Pseudomonas aeruginosa was also considered by 2.9% of the physicians and 1.2% of the nurses. The practitioners consider self-prescription by the patients as the major factor for the development of AMR (80% of the physicians, 55.8% of the nurses, and 72.7% of the pharmacists) (Table 2).
Beliefs on Potential Intervention to Combat AMR
The majority of the professionals consider antimicrobial usage policy as very useful in combating AMR (80% of the physicians, 79.1% of the nurses, and 81.8% of the pharmacists). Only 1 nurse considers it as non-useful. More than half of the nurses (55.8%) and pharmacists (63.6%) consider the reduction of antibiotics at the outpatient setting as very useful whereas 40% of the physicians consider it only useful in combating AMR. Establishing national AMR surveillance was considered as a very useful step by 80% of the physician, by 79% of the nurses and by 81.8% of the pharmacist whereas establishing hospital infection control committee was considered as a very useful step by 77.1% of the physician, by 79.1% of the nurses and by 81.8% of the pharmacist. Developing institutional guidelines for antimicrobial use was considered very useful for 80% of the physician, 75.6% of the nurses, and 81.8% of the pharmacist. Education on antimicrobial therapy for prescribers was considered very useful by 74.3% of the physician, 79.1% of the nurses, and 81.8% of the pharmacist. On the other hand, establishing microbiology diagnostic services was considered very useful by 80% of the physician, by 67.4% of the nurses, and by 72.7% of the pharmacist (Table 3).
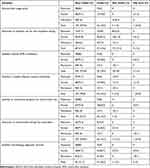 |
Table 3 Belief of Health Care Professionals’ Working in HFSUH on Potential Intervention to Combat AMR |
The Scope of AMR
The majority of the health practitioners strongly agree or agree that AMR is a worldwide problem (100% of the physician and pharmacists and 90.7% of the nurses). The majority of them also strongly agree or agree that AMR is a problem in Ethiopia, with 54.3% of the physicians, 61.6% of the nurses, and 63.6% of the pharmacist strongly agreeing to this fact. Whereas regarding AMR as a problem in the hospital, most of them (88.6% of the physicians, 100% of the pharmacists, and 86.1% of the nurses) strongly agree or agree with this fact (Table 4).
 |
Table 4 Percentage of Health Care Professionals’ Working in HFSUH Rating the Scope of AMR |
Table 5 shows the belief of health care professionals on the cause of inappropriate prescriptions. The majority of the respondents consider the patient influence on the prescriber and failure of previous treatment as the major cause of unnecessary antimicrobial prescription. 40% of the physicians and 63.6% of the pharmacists consider the patient influence on the prescriber as the cause whereas the 48.8% nurses consider a failure of previous treatment as the major cause of unnecessary antimicrobial prescription. Most of them also consider that unnecessary antibiotic is prescribed for upper respiratory tracts infections (57.1% of the physician, 43% of the nurses and 81.8% of the pharmacist, p=0.043) and unknown febrile illness (37.1% of the physicians and 38.4% of the nurses) (Table 5).
 |
Table 5 Belief of Health Care Professionals’ Working in HFSUH on Causes of Unnecessary Antibiotic Prescriptions |
Discussion
This study assesses the knowledge and belief regarding AMR and the antimicrobial usage of health care professionals (physicians, nurses, and pharmacists) working in HFSUH. The three practitioners were selected because of there great involvement in the usage of antimicrobials. The physicians and nurses are involved in prescribing and administration whereas the pharmacists’ role is the dispensing of antibiotics. In Ethiopia, because of resistant microorganisms, the number of antimicrobials being effective is becoming limited.6
In this study, the majority of health practitioners consider MRSA as resistant bacteria. The knowledge about MRSA is higher than studies conducted in Jordan (31.6% of the physicians, 33.6% of the nurses’ and 29.3% of the pharmacist)4 and in Amhara region (22.3% of physicians and 2.4% of nurses)20 but it is lesser than the study done in Ghanian Tertiary Hospital (98% of the physicians know about this bacteria).22 Pseudomonas aeruginosa as resistant bacteria was not considered by the majority of the health professionals in the current study. A similar result was observed in a study conducted in Khartoum (7.9% of the physicians).23 This result is lower than the result of the study conducted in Jordan (25.8% of the physicians and 28.2% of the pharmacists)4 Less than half of the health professionals considered MDR-TB as resistant bacteria and responded that they had training on AMR. So, the low level of training about AMR and the causative agents could also be one reason why most of the practitioners have a low understanding of the resistant bacteria other than MRSA.
Not being exposed to use the AST result could also be responsible for such a gap in knowledge regarding resistant bacteria. The majority of the health professionals were not exposed to use the AST result. In the absence of an AST, health care professionals resort to empiric treatment based on the symptom of the individual using broad-spectrum antibiotics. This will increase the risk of AMR since these antibiotics can affect the normal flora beside the infectious agent, weakening the defense of the host.14
One of the driving factors that was considered by the health care providers as driving force in AMR occurrence was widespread or overuse of antibiotics. This finding is higher than a study done in Khartoum (54.5% of the physicians).23 In the current study, the majority also consider poor infection control as a factor for the spread of AMR, which was also higher than the result obtained in Jordan (79.6%, 65.1%, and 64.3% of the physicians, pharmacists, and nurses, respectively).4 100% of the physicians, 86% of nurses, and 90.9% of pharmacists say that substandard qualities of antibiotics promote AMR. A lower result was obtained in a study done in Ghanian hospital (37.73% of the physicians).22 Another factor that was considered was patients’ poor adherence to prescribed antibiotics, which was considered as a factor by more than 90% of the health professionals in the current study. A slightly lower result was observed in a study done in India (89.65% of the physicians).24, 100% of the physicians and the pharmacists and 81.4% of the nurses considered bacterial mutations as the cause of AMR (p=0.008). This result was slightly higher than the study conducted in west Indies (84% of the physicians)25 This shows that the practitioners in the current study have a good knowledge regarding the cause of AMR when compared to other studies but with a slightly lower result (only 64.4% of the practitioners) was observed regarding usage of broad-spectrum antibiotics as a cause of AMR.
As a potential intervention to combat AMR, 95.4% consider establishing microbiology diagnostic services as very useful and/or useful which is higher than the study conducted in Addis Ababa (70.8% of the practitioners).8 In the current study, 100% of the physicians consider developing an institutional guideline for antimicrobial use as very useful or useful which is higher than a study done in Khartoum state hospital setting (75.4% of the physicians)23 and in a study done in West Indies (99% of the physicians).25 However, a lower amount of the physician (77.1%) considers the reduction of antibiotic use for outpatient settings as a means to combat AMR in the current study, which is almost similar to a study done in West Indies (81% of the physician).25 These results might be because practitioners have up-to-date information about AMR they obtain either from books or from the internet or university teaching they got.
Most of the respondents consider the patient influence on the prescriber and failure of previous treatment as the major cause of unnecessary antimicrobial prescription. Less than 10% of the health practitioners, on the other hand, consider critically or immuno-compromised patient and profit of the hospital as the cause for the unnecessary prescription. This result is lower than the study done in Amhara region, where 61% of the physicians and 53% of the nurses consider the patient influence on the prescriber, 90.2%, and 69.5% consider the failure of previous treatment, 52.3% of the physicians and 67.1% of the nurses consider critically or immuno-compromised patient and 35.6% of the physicians and 41% of the nurses consider profit of the hospital as the cause of unnecessary antimicrobial prescription.20 Such discrepancy might be because of the difference in the study area and also the number of hospitals utilized in the two studies and also because the study conducted in the Amhara region also involved private sectors, where unnecessary prescription use is commonly observed.
Regarding the awareness of the respondents on the scope of the AMR problem, most of the health care practitioners considered AMR as a problem across all three levels. A slightly lower result was observed with physicians regarding AMR as a worldwide problem in another study done in Khartoum (85.2% of the physicians),23 and in the Amhara region (82% of the physicians and 60% of the nurse).20 A slightly lower result (88.1% of the physicians and 89.9% of the nurses) however was also observed in the Amhara region regarding AMR as a problem in Ethiopia.20 This increased awareness of the health practitioners in the present study might be because the majority of them have up to date information which enables them to know the great extent of AMR problem worldwide or in Ethiopia. 88.6% of the physicians strongly agree or agree with AMR as a problem of the hospital they are working with. This is higher than the study done in Ghanaian tertiary care hospital (59.7% of the physicians).22 This could be due to malpractices or unnecessary antibiotic prescriptions they may observe during their work since the majority of them consider the influence of patients on prescribers and failure of treatment as a cause of unnecessary antibiotic prescription.
Conclusion
The pharmacists, physicians, and nurses working in HFSUH have information about MRSA, about perceived factors contributing to AMR development, potential intervention to combat AMR, cause of unnecessary antibiotic prescription, and scope of AMR. However, the information they have about the different resistant bacteria, on the different factors that cause unnecessary antibiotic prescription and on how to use AST is low and most of them have not taken training on AMR. The information gap present with the professional can be enhanced by training the professionals more about AMR. AST should be done before the use of antibiotics and the health care professionals should select the antibiotics based on these tests and minimize the risk of AMR.
Abbreviations
AMR, Antimicrobial Resistance; AST, Antimicrobial susceptibility test; HFSUH, Hiwot Fana Specialized University Hospital; SPSS, Statistical Package for Social Sciences.
Data Sharing Statement
The authors are willing to make the datasets available based on reasonable request.
Ethical Consideration
Haramaya University gave us ethical approval and clearance for conducting the study. HFSUH was asked for permission with a written letter by Haramaya University. Moreover, the questionnaire was given to pharmacist, physicians, and nurses based on written informed consent.
Acknowledgments
We would like to extend our deepest gratitude to all individuals who were involved in the research.
Author Contributions
All authors contributed to data analysis, drafting or revising the article, gave final approval of the version to be published, and agree to be accountable for all aspects of the work.
Disclosure
The authors declare that they have no competing interests.
References
1. Satish Kumar BP, Santhosh Y, Ahamed MG, Naveen MR. Survey on knowledge towards antibiotic among the nursing students. Int J Pharm Pharm Sci. 2011;3(2):227–229.
2. Lee Y, Wakabayashi M. Key informant interview on antimicrobial resistance (AMR) in some countries in the Western Pacific region. Global Health. 2013;9(1):34. doi:10.1186/1744-8603-9-34
3. Dhawal D, Sachdeva A. Knowledge, attitudes, and behavior towards antibiotic usage and its resistance among the general public of Shimla city a pilot study. Int J Com Health Med Res. 2015;1(1):9–16.
4. Alzoubi K, Ayoub N, Al-Sakaji S, Al-Azzami S, Mhaidat N, Masadeh M. Awareness of bacterial resistance among physicians, pharmacists, and nurses. Int J Occup Med Environ Health. 2009;22(4):363–372. doi:10.2478/v10001-009-0034-3
5. Pereko DD, Lubbe MS, Essack SY. Public knowledge, attitudes, and behavior towards antibiotic usage in Windhoek, Namibia. S Afr J Infect Dis. 2015;30(4):134–137. doi:10.1080/23120053.2015.1107290
6. Tafa B, Endale A, Bekele D. Paramedical staff knowledge and attitudes towards antimicrobial resistance in Dire Dawa, Ethiopia: a cross-sectional study. Ann Clin Microbiol Antimicrob. 2017;16(64):1–14. doi:10.1186/s12941-017-0241-x
7. Donyai P, Okafor S, Virgo R, Amin K, Nasr M. Messages about antibiotic resistance in different newspaper genres. Pharmacy. 2013;1(2):181–192. doi:10.3390/pharmacy1020181
8. Gemeda F, Gedif T. Assessment of antimicrobial resistance containment practices in selected public hospitals of Addis Ababa, Ethiopia (unpublished paper). Addis Ababa University, School of Pharmacy; 2014. Available from: http://etd.aau.edu.et/handle/123456789/865?show=full.
9. Ahmad A, Khan MU, Patel I, Maharaj S, Pandey S, Dhingra S. Knowledge, attitude, and practice of a B.Sc. Pharmacy students about antibiotics in Trinidad and Tobago. J Res Pharm Pract. 2015;4(1):37–41. doi:10.4103/2279-042X.150057
10. Kim SS, Moon S, Kim EJ. Public knowledge and attitudes regarding antibiotic use in South Korea. J Korean Acad Nurs. 2011;41(6):742–749. doi:10.4040/jkan.2011.41.6.742
11. Huang Y, Gu J, Zhang M, et al. Knowledge, attitude, and practice of antibiotics a questionnaire study among 2500 Chinese students. BMC Med Educ. 2013;13(163):1–9. doi:10.1186/1472-6920-13-163
12. Alzoubi K, Al-Azzam S, Alhusban A, et al. An audit on the knowledge, beliefs, and attitudes about the uses and side-effects of antibiotics among outpatients attending 2 teaching hospitals in Jordan. East Mediterr Health J. 2013;19(5):478–484. doi:10.26719/2013.19.5.478
13. Van Boeckel TP, Gandra S, Ashok A, et al. Global antibiotic consumption from 2000 to 2010: an analysis of national pharmaceutical sales data. Lancet Infect Dis. 2014;14(8):742–750. doi:10.1016/S1473-3099(14)70780-7
14. Ayukekbong JA, Ntemgwa M, Atabe AN. The threat of antimicrobial resistance in developing countries: causes and control strategies. Antimicrob Resist Infect Control. 2017;6(1):47. doi:10.1186/s13756-017-0208-x
15. Hayat K, Rosenthal M, Gillani AH, et al. Perspective of Pakistani physicians towards hospital antimicrobial stewardship programs: a multisite exploratory qualitative study. Int J Environ Res Public Health. 2019;16(9):1565. doi:10.3390/ijerph16091565
16. Castro-Sanchez E, Moore LS, Husson F, Holmes AH. What are the factors driving antimicrobial resistance? Perspectives from a public event in London, England. BMC Infect Dis. 2016;16(1):465. doi:10.1186/s12879-016-1810-x
17. Awad AI, Aboud EA, Singer AC. Knowledge, attitude and practice towards antibiotic use among the public in Kuwait. PLoS One. 2015;10(2):e0117910. doi:10.1371/journal.pone.0117910
18. WHO. Health workers’ education and training on antimicrobial resistance. Curricula guide; 2019. Available from: https://apps.who.int/iris/rest/bitstreams/1138914/retrieve.
19. Chaintarli K, Ingle SM, Bhattacharya A, Ashiru-Oredope D, Oliver I, Gobin M. Impact of a United Kingdom-wide campaign to tackle antimicrobial resistance on self-reported knowledge and behavior change. BMC Public Health. 2016;16(1):393. doi:10.1186/s12889-016-3057-2
20. Abera B, Kibret M, Mulu W. Knowledge and beliefs on antimicrobial resistance among physicians and nurses in hospitals in Amhara Region, Ethiopia. BMC Pharmacol Toxicol. 2014;15(26):1–7. doi:10.1186/2050-6511-15-26
21. Abbo LM, Cosgrove SE, Pottinger PS, et al. Medical students’ perceptions and knowledge about antimicrobial stewardship. How are we educating our future prescribers? Clin Infect Dis. 2013;57(5):631–638. doi:10.1093/cid/cit370
22. Labi AK, Obeng-Nkrumah N, Bjerrum S, Aryee NAA, Ofori-Adjei YA, Yawson AE. Physicians’ knowledge, attitudes, and perceptions concerning antibiotic resistance: a survey in a Ghanaian tertiary care hospital. BMC Health Serv Res. 2018;18(1):126. doi:10.1186/s12913-018-2899-y
23. Kheder SI. Physicians’ knowledge and perception of antimicrobial resistance a survey in khartoum state hospital settings. Br J Pharm Res. 2013;3(3):347–362. doi:10.9734/BJPR/2013/2117
24. Ridhorkar R, Nagdeo NV. Knowledge and beliefs on antimicrobial resistance among clinicians: step towards antibiotic stewardship. J Health Sci. 2018;8(1):4–11.
25. Tennant I, Nicholson A, Gordon-Strachan GM, Thoms C, Chin V, Didier MA. A survey of physicians’ knowledge and attitudes regarding antimicrobial resistance and antibiotic prescribing practices at the university hospital of the West Indies. West Indian Med J. 2010;59(2):165–170.
 © 2020 The Author(s). This work is published and licensed by Dove Medical Press Limited. The full terms of this license are available at https://www.dovepress.com/terms.php and incorporate the Creative Commons Attribution - Non Commercial (unported, v3.0) License.
By accessing the work you hereby accept the Terms. Non-commercial uses of the work are permitted without any further permission from Dove Medical Press Limited, provided the work is properly attributed. For permission for commercial use of this work, please see paragraphs 4.2 and 5 of our Terms.
© 2020 The Author(s). This work is published and licensed by Dove Medical Press Limited. The full terms of this license are available at https://www.dovepress.com/terms.php and incorporate the Creative Commons Attribution - Non Commercial (unported, v3.0) License.
By accessing the work you hereby accept the Terms. Non-commercial uses of the work are permitted without any further permission from Dove Medical Press Limited, provided the work is properly attributed. For permission for commercial use of this work, please see paragraphs 4.2 and 5 of our Terms.
