Back to Journals » Diabetes, Metabolic Syndrome and Obesity » Volume 8
Interventions to improve long-term weight loss in patients following bariatric surgery: challenges and solutions
Authors McGrice M, Don Paul K
Received 25 December 2014
Accepted for publication 7 April 2015
Published 23 June 2015 Volume 2015:8 Pages 263—274
DOI https://doi.org/10.2147/DMSO.S57054
Checked for plagiarism Yes
Review by Single anonymous peer review
Peer reviewer comments 5
Editor who approved publication: Professor Ming-Hui Zou
Video abstract presented by Melanie McGrice
Views: 293
Melanie McGrice, Kathlene Don Paul
Nutrition Plus Enterprises, Melbourne, VIC, Australia
Abstract: Bariatric surgery aims to provide long-term weight loss and improvement in weight-related comorbidities. Unfortunately, some patients do not achieve predicted weight loss targets and many regain a portion of their lost weight within 2–10 years postsurgery. A review of the literature found that behavioral, dietary, psychological, physical, and medical considerations can all play a role in suboptimal long-term weight loss. Recommendations to optimize long-term weight loss include ensuring that the patient understands how the procedure works, preoperative and postoperative education sessions, tailored nutritional supplements, restraint with liquid kilojoules, pureed foods, grazing and eating out of the home, an average of 60 minutes of physical activity per day, and lifelong annual medical, psychological, and dietary assessments.
Keywords: weight, bariatric, surgery
Introduction
As the prevalence and burden of overweight and obesity increases globally, it is salient to develop and implement effective interventions for long-term weight loss. In 2008, statistics reported that global obesity had nearly doubled since 1980, with more than 1.4 billion adults identified as overweight, and approximately 200 million men and 200 million women being classified as obese.1 Overweight and obesity are associated with a range of noncommunicable diseases, which can result in significant morbidity. These health concerns can include type 2 diabetes, musculoskeletal complications, cardiovascular disease, some cancers, obstructive sleep apnea (OSA), infertility, negative emotional states, and an overall reduced quality of life.2,3 Therefore, the need for an effective intervention providing long-term weight loss is paramount to reduce the incidence of obesity-related health complications.
What is bariatric surgery and why should it be considered?
Bariatric surgery can be considered an effective and sustainable weight loss method in some patients. Bariatric procedures can be an appropriate weight loss option for patients with a body mass index (BMI) exceeding 40 kg/m2, individuals with a BMI between 35 and 40 who have developed diseases associated with obesity, and those who have been unsuccessful in losing weight through other weight loss strategies.2 The overall aim of bariatric procedures is to reduce the intake of food by physically restricting the gastric capacities of the body.2,4 Overall, bariatric surgery has been associated with significant weight loss, reductions in some weight-related comorbidities, and an increase in certain elements relating to quality of life, as compared to conventional treatments.2
There are a number of different types of bariatric surgery currently available to patients. The most common procedures are generally performed laparoscopically and include Roux-en-Y gastric bypass (RYGB), sleeve gastrectomy (SG), and laparoscopic adjustable gastric banding (LAGB). The RYGB is an irreversible procedure that involves the combination of restrictive and malabsorptive processes by constructing a small gastric pouch anastomosed to the distal part of the small intestine.2–4 The duodenum is attached further down the distal part of the intestines, creating a “Y”-like shape. Food bypasses the stomach as well as the proximal small bowel. The SG is an irreversible restrictive procedure involving the removal of a large portion of the stomach creating a “sleeve”-shaped tube. The surgery reduces the overall stomach size to around 25% of its original size.2–5 The LAGB procedure is a reversible surgery that involves restricting food intake by placing an inflatable silicone constricting band around the distal end of the fundus to make a smaller prestomach pouch.2,4,6 The band diameter can be altered by injecting or removing saline through a subcutaneous port to optimize restriction. These bariatric surgeries differ in technical procedure, outcome, and risk and, therefore, comprehensive consideration needs to be applied when choosing the more appropriate surgery for each patient. It is also important for the bariatric patient to have an understanding of the surgical procedure and the future implications to reduce the risk of complications and to improve overall weight loss.
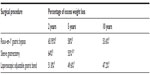
Long-term weight loss at 2, 5, and 10 years after bariatric surgery
Weight loss results vary between different bariatric procedures at 2 years, 5 years, and 10 years (Table 1). Results from a range of studies and systematic reviews were analyzed to approximate a mean percentage of weight loss after each bariatric procedure.
Successful weight loss post-bariatric surgery can be defined as the percentage of excess weight loss (%EWL), where
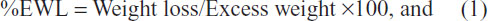
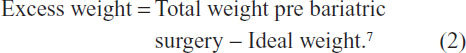
A successful postoperative outcome is generally considered to be a loss of greater than 50% EWL after 2 years.7
Although the overall goal of bariatric surgery is to achieve long-term weight loss, patients may face the challenge of regaining weight after surgery. Current research suggests weight regain is common 2–10 years after surgery with patients commonly regaining up to 15% of their initial body weight.11–13 Despite regaining a percentage of weight, most patients are still able to maintain a significant amount of weight loss of around 50% EWL.3 One longitudinal prospective study of over 700 patients found that weight regain was observed in over 50% of patients within 2 years of surgery, with the amount of weight regain being higher in the super-obese group.14
Challenges and solutions associated with long-term weight loss following bariatric surgery
Although bariatric surgery aims to provide patients with an effective and sustainable weight loss intervention, bariatric procedures are not a “miracle cure”. Silver et al15 found that 81% of patients surveyed were still trying to lose weight up to 4 years after surgery. To achieve optimal weight loss and health benefits, it is essential that bariatric patients are not neglected postsurgery, but undergo lifelong regular assessments and interventions as required. The potential challenges associated with each type of bariatric surgery need to be taken into consideration pre- and postsurgery to optimize long-term weight loss.
Weight regain tends to occur in a gradual and progressive manner,16 indicating the importance of regular long-term anthropometrical measurements and follow up.17 It is important to address any weight regain-related issues as soon as possible. It is therefore important for the patient to be supported by a multidisciplinary medical team to provide appropriate solutions to these challenges to ensure the safety and well-being of the patient is considered during the entire process.
The lack of implementation of behavioral strategies, suboptimal dietary intake, sedentary behavior, the physical side effects of surgery, and medical complications are common challenges that can contribute to possible weight regain or insufficient weight loss. Achieving sustainable weight loss following bariatric surgery can be challenging; however, provided with appropriate solutions to these challenges, a patient can successfully achieve and maintain weight loss.
Behavioral management
Research suggests that implementation of lifestyle changes is one of the key requirements for successful weight loss postbariatric surgery.18
Patient education
Significant dietary, psychological, and lifestyle changes are required postbariatric surgery. Pre- and postoperative education sessions provide the bariatric patient with practical knowledge, skills, and support to make the required changes and optimize weight. Research shows that the frequency of consultations is correlated with weight loss success, with a study by Dixon et al19 showing that patients who undertook a minimum of 12 consultations within the first 6 months of surgery achieved significantly better weight loss results postbariatric surgery. Furthermore, it is recommended that bariatric education be delivered by a multidisciplinary team of health professionals to ensure specialist advice.20 Digital communication methods such as social media, telephone consultations, and online education programs could be utilized to increase engagement with clients and minimize barriers such as time, distance, and cost.
Self-monitoring
Odom et al18 found that self-monitoring was one of the most protective strategies against weight regain postbariatric surgery. This is consistent with the literature for weight management within nonbariatric surgery communities, which shows that regular weigh-ins, food records, and exercise diaries are vital tools for avoiding weight regain.21 Encouraging bariatric patients to maintain a daily food intake journal is of particular value as, in addition to increasing the patient’s awareness of eating patterns, it also allows the bariatric dietitian to identify any high-risk areas, such as nutritional inadequacy, food intolerances, poor food choices, or food aversions – all of which may compromise weight loss and nutritional status.22
Dietary considerations
A primary cause of suboptimal weight loss postbariatric surgery is excessive energy intake.23 Although bariatric surgery is an effective tool for weight loss in many patients, the onus is on the patient to make major dietary changes, for which many may be inadequately prepared.24 Postoperative eating behaviors can be a major factor for the disparity in weight loss between procedures, as well as for overall long-term weight loss outcomes. This is particularly relevant for the LAGB and the RYGB.24 The bariatric patient may experience a number of nutrition and dietary challenges after the surgical procedure that can impact both short- and long-term weight loss.
Liquid kilojoules
High-calorie liquids, such as sweetened drinks, including commercial carbonated beverages, milkshakes, smoothies, cordials, and juices, are typically high in overall energy and low in nutritional composition. They provide minimal pressure in the stomach pouch; hence, they have little effect on satiety and can be appealing to patients after surgery to satisfy sweet cravings25 or to evade the negative symptoms of eating solid foods.24,25 Being so high in energy, high-calorie liquids make a significant contribution to energy intake and can perpetuate a positive energy balance and resultant weight regain.
A study of RYGB patients by Brolin et al24 found that more than half of their patients who lost less than 50% of their excess weight were found to excessively consume high-calorie liquids, illustrating that this is a major cause of inadequate weight loss. Studies have shown that the incidence of ingesting high-calorie liquids is even higher in patients who have undergone LAGB procedures, rather than RYGB or SG.24 This is thought to be due to the ease with which high-calorie liquids are tolerated postbanding, whereas physical restriction and fear of developing unpleasant symptoms associated with dumping syndrome limits the consumption of high-calorie liquids in some RYGB and SG patients.25
Alcohol can also be considered a high-calorie liquid due to its high-energy density; it can therefore pose a threat to successful long-term weight loss. Patients are advised to limit alcohol use after surgery, owing to excess caloric intake.23 Furthermore, research suggests that the metabolism of alcohol may be altered for patients post-RYGB, causing patients to become intoxicated more quickly with less alcohol, and they can take longer to return to sobriety than before surgery.26 If alcohol intake is not controlled, patients may be at an increased risk for alcohol dependency despite ingesting a smaller volume than what could be tolerated prior to surgery.23 A retrospective study found that 28.4% of bariatric patients reported evidence of alcohol dependence after surgery compared with 4.5% prior to surgery.23 It has been suggested that such high rates of alcohol intake can be in line with the “symptom substitution theory”, which states that the successful elimination of a particular symptom without treating the underlying cause will result in the appearance of a substitute symptom. As the surgery largely eliminates excessive eating, the consumption of high-calorie liquids, including alcohol, can take its place; meanwhile, the potential underlying psychopathology toward eating habits remains inadequately addressed.23
It is important for the medical team to evaluate a patient’s eating and drinking habits before surgery to identify patients’ predispositions to drinking high-calorie liquids, and to provide suitable recommendations for bariatric surgeries. For example, if a patient has a higher tendency for sweet drinks, then opting for a RYGB where the excess sugar may result in dumping symptoms may increase weight loss, yet simultaneously increase postoperative symptoms.25 Regular review with the dietetic team postoperatively will help to identify patients with excessive intakes of high-calorie liquids and line patients up with appropriate interventions to limit high-calorie liquid intake.
Pureed foods
After bariatric surgery, patients need to be guided through the process of reintroducing solid foods and texture progression, as this encourages greater satiety and enhanced nutritional composition. Patients can often be hesitant to progress to solid foods postoperatively for fear of weight gain, pain, nausea, or vomiting. Contrarily, staying on a pureed diet can jeopardize weight loss, as pureed foods do not provide as much satiety, particularly after LAGB. Table 2 provides an outline of the postoperative diet that bariatric surgery patients should follow postsurgery to prevent medical complications and physical side effects, and to improve overall long-term weight loss.
  | Table 2 Recommended foods for optimal long-term healthy eating postbariatric surgery |
Grazing
Grazing or excessive snacking is a common issue that affects many bariatric patients pre- and postoperatively, which can jeopardize long-term weight loss if not controlled. Grazing can be defined as the consumption of smaller amounts of food continuously over an extended period of time. Although bariatric surgery usually restricts the volume of food that can be consumed in one sitting, people who graze throughout the day can defeat the purpose of the surgery and result in consuming excessive kilojoules.29 Studies indicate that the prevalence of grazing following bariatric surgery is as high as 31%.29
Grazing is frequently triggered by social or psychological circumstances.30 These could include eating when stressed, bored, and/or emotional, and eating in association with other activities such as watching television, performing computer work, or attending social events.29,31 Interestingly, working around food has been determined as a primary risk factor for weight regain postbariatric surgery, presumably as a result of increased opportunity for snacking.32
Hunger can also be a precipitant for snacking, more so for LAGB patients, as the decreased ghrelin production seen in RYGB or SG reduces stimulation of the hunger center in the brain.33 For patients with a LAGB, it is prudent to monitor how much fluid is present in the band, as too much will cause excessive restriction. If the band is too tight, patients may be more likely to graze on smaller portions to minimize discomfort with eating or, if it is too loose, it can result in additional snacking as a result of hunger.
Patients who graze have higher caloric intakes and therefore report lower weight loss outcomes. In addition to suboptimal weight loss, research suggests that grazers are also more likely to have poorer mental health, as well as a higher risk of gastrointestinal symptoms.29 Patients who tend to snack excessively are more likely to present with a higher frequency of vomiting.34 It is important for patients to understand that regular vomiting postbariatric surgery is not, and should not, be the norm, and can cause nutritional deficiencies, dental caries, esophagitis, and gastric ulcers, which can further impact food choices and intake. Some patients incorrectly believe that as long as they are vomiting frequently, they will not gain weight. This is not the case, nor is it healthy.
It is most important for practitioners to educate bariatric patients regarding spacing out meals and snacks throughout the day. Having well-spaced, balanced meals will assist in inducing longer-term satiety; it will also allow for optimal nutritional adequacy and will prevent the overconsumption of kilojoules. The implementation and management of eating strategies is also vital to improve cognitive awareness of physical versus psychological hunger.31
Eating techniques
An additional challenge that bariatric patients will need to address to optimize weight loss is their eating techniques. Following bariatric surgery, patients require simple guidelines to assist them in adjusting to their new way of eating. It is essential that patients learn to eat slowly in a relaxed manner, avoiding distractions such as television, work, or reading, so that they are more attuned to their body’s signals and can determine when to stop eating, when they feel comfortable or satisfied, and how to avoid being full or overfull.27,28 Patients need to allow a period of 20–30 minutes for meal consumption, after which point they should discard the remainder of their meal.28 It is also beneficial to recommend eating from smaller sized crockery, such as entrÉe size or from a bread and butter plate, to help control portion sizes.20
Eating out of home
A study by Garcia et al35 found that a high consumption of fast food was one of the most common predisposing predictors of bariatric surgery. This was corroborated in a study by Mitchell et al,36 who found that in a pool of patients planning bariatric surgery, 50% of the patients ate fast food twice per week and ate at a restaurant four times per week. Although there is little evidence regarding rates of eating out of home postbariatric surgery, frequent intake of dining out and fast food could jeopardize weight loss. It is recommended that when eating out, patients choose entrée-sized mains, refrain from high-fat or sugar options, and avoid filling up on extras such as bread and high-energy drinks.
Protein intake
Adequate protein intake postbariatric surgery is essential for preserving lean muscle mass, increasing satiety, improving nutritional status, and maintaining weight loss.37,38 A study by Das et al39 found that resting energy expenditure decreased by 25% in patients post-RYGB. Suboptimal protein intake, resulting in muscle catabolism, is one of the primary influences for this. Furthermore, Faria et al40 found that individuals who make meals with a high glycemic load exhibited decreased weight loss.
It is recommended that protein consumption postbariatric surgery be similar to protein recommendations on other weight loss diets; however, the literature is divided about the amount of protein actually required.41 A meta-analysis by Krieger et al42 argues that protein intake during weight loss needs to be at a minimum of 1.05 g/kg of obesity-related adjusted weight to enable the retention of fat free mass. However, the nutrition guidelines by Mechanick et al20 report that protein intake postbariatric surgery should average between 60 and 120 g daily. Until a consensus can be reached, it seems prudent to encourage individuals to at least meet the recommended dietary intake (RDI) for protein. However, it is essential that practitioners use their clinical judgment to evaluate individual patient circumstances, with higher requirements needed for patients undertaking physical activity,43 wound healing,37 or gluconeogenesis.44
A reduction in protein synthesis starts with a major reduction in total energy intake following bariatric surgery. Although additional protein is often needed for gluconeogenesis, in addition to usual protein needs, protein intake is often reduced following bariatric surgery instead of increased due to a poor tolerance of protein-rich foods such as red meat.45 A study of LAGB patients 1 year postsurgery found that 32% of women were not meeting the recommended dietary intake (RDI) of 46 g per day for protein, and 64% of men were not meeting the RDI of 64 g per day.46
To ensure that patients are meeting their protein requirements postbariatric surgery, it is recommended that patients undergo regular assessments with a bariatric dietitian who can assess their needs and teach them how to meet their requirements. Some patients may need to use protein supplements to assist with meeting requirements postsurgery.22
Meeting vitamin and mineral requirements
An additional challenge that bariatric patients may experience postsurgery is meeting vitamin and mineral requirements. After surgery, nutritional deficiencies can occur as gastrointestinal modifications reduce dietary intake, which limits the actual availability of nutrients from food. Further to this, there is an element of malabsorption of key nutrients.47 Nutrient deficiencies can also occur due to frequent vomiting and/or poor patient compliance to the nutritional recommendations suggested by the bariatric dietitian.47
Deficiencies of iron; vitamin B12; folate; zinc; thiamine; calcium; vitamin D; fat-soluble vitamins A, D, E, and K; magnesium; selenium; copper; and phosphate are common postbariatric surgery.48 For patients post-RYGB or SG, vitamin B12 and iron deficiency is more likely due to a lack of acid and intrinsic factor in the stomach than food choices.33 Deficiencies of nutrients such as iron and vitamin B12 can result in fatigue that may then result in decreased levels of planned and incidental activity, and an increased reliance on higher calorie ready-made meals.49
Odom et al18 reports that “food urges” are one of the strongest predictors of weight regain postbariatric surgery. Food urges or cravings can be exacerbated by nutritional deficiencies, resulting in patients craving essential nutrients.18
Patients should take an appropriately approved multivitamin lifelong after bariatric surgery to help prevent micronutrient deficiencies. Due to the increased risk of nutritional deficiencies following bariatric procedures, it is recommended that the patient’s biochemistry or pathology is checked every 3–6 months postoperatively for the first 2 years and then monitored annually thereafter.20,22,50,51 This will minimize nutritional deficiencies causing fatigue, and minimize food cravings to improve long-term weight loss, as well as providing increased quality of life.
Physical activity
Physical activity and increased incidental exercise constitute an important long-term management strategy for weight loss after bariatric procedures. Physical activity can have a range of short- and long-term health benefits, including reducing the risk of coronary heart disease, hypertension, diabetes, stroke, some cancers, and depression, and helping to improve bone and functional health, energy balance, and weight control.52 It is also important for bariatric patients to increase their physical activity levels postsurgery to improve weight loss and maintain muscle mass, thus reducing the risk of weight regain. A low level of physical activity has been identified as a key predictor of weight regain postbariatric surgery.53
Research states that a minimum of 60 minutes of moderate to vigorous intensity physical activity is required daily – in one block, or it can also be separated – for long-term maintenance of significant weight loss.7 A study by Bond et al54 found that patients who increased their physical activity levels postsurgery lost more weight and reported an overall better quality of life compared with bariatric patients who remained inactive. Therefore, bariatric patients who are not already undertaking regular physical activity need to incorporate habitual physical activity behaviors into their everyday routines to achieve and then maintain substantial weight loss.
Psychological considerations
Mood disorders
Low self-esteem and/or depression have been found to be predictors of weight regain.18,53 Although the reason for this has not yet been identified, theories include an increase in emotional eating and reduced incidental activity. A study by Sousa et al55 found that body image concerns after weight loss surgery increased the risk of depression, leading to a loss of control over eating and a consequent weight regain. It is prudent to screen for depression, body image, and self-esteem issues, and engage these patients with additional support and resources to optimize weight loss postbariatric surgery.
Eating disorders
An increasing number of cases of eating disorders, including anorexia nervosa, bulimia nervosa, and eating disorders not otherwise specified, have been identified postbariatric surgery.56 A study by de Man Lapidoth et al57 concluded that patients who had undertaken bariatric surgery were more likely to develop eating disorders postoperatively than patients who had undergone traditional weight loss treatments. Eating disorders after weight loss surgery typically represent a continuation or recurrence of presurgical habits and patterns.31 Obesity and/or bariatric surgery may mask the side effects of eating disorders, making these conditions more difficult to diagnose. It is essential that health professionals are cognizant of this, and monitor the patient’s weight loss, eating behaviors, and mental state during review assessments.
Binge eating is an eating disorder that can be defined as eating substantially large amounts of food during short periods of time with a sense of loss of control.30 It is important to identify individuals diagnosed with binge eating disorder presurgery, as although weight loss surgery may physically prevent the ability to binge as one has done previously due to the reduction in stomach volume, the dynamics responsible typically persist.31 Despite not being about to tolerate a large volume of food, patients can develop the capacity to over-consume by excessively grazing throughout the day with persistent emotional distress,29,31 or to binge then purge. Maladaptive eating behaviors are high among patients diagnosed with binge eating during presurgical screening, and they result in a higher vomiting frequency after the surgery34 and subsequent weight gain. Kalarchian et al58 indicates that approximately 43% of bariatric patients have reported instances of loss of control at some point in the time after surgery, and that these patients tended to have poorer longer-term weight loss outcomes.
Contrarily, some patients will fail to consume sufficient calories and develop an intense fear of regaining weight.31 Feelings of dissatisfaction can result in refusal to maintain a normal weight, excessive preoccupation with weight and body image, an intense fear of gaining weight, and the use of restrictive and/or purging behaviors in an effort to gain control of weight management.31 Some patients report a fear of stretching the stomach pouch as the reason for extreme restrictive eating, and they tend to have an “all or nothing” attitude toward weight maintenance.31 This starving can lead to macro- and micronutrient deficiencies which, as described earlier, can lead to long-term weight regain.
Physical considerations
Bariatric surgery patients may experience physical side effects, such as maladaptive eating, return of hunger, eating disorders, and excessive skin after the procedure, which may directly or indirectly impact long-term weight loss. It is important for the multidisciplinary bariatric team to support patients through their weight loss journey to help prevent the possibility of these physical side effects from developing, and to improve their long-term weight loss outcomes.
Maladaptive eating
Failure to achieve anticipated results or acopia with physical changes is typically the stimuli for the onset of longer-term maladaptive eating postbariatric surgery.31 Brolin et al24 showed that the primary motivator to maladaptive eating is generally an aversion to vomiting.
Bariatric patients who engage in maladaptive eating generally avoid solid foods and eat softer, high-calorie foods such as chocolate, candy, and ice cream.30 A diet rich in these foods results in the patient consuming a higher calorie intake, particularly from carbohydrates and saturated fats. Foods such as soups, crackers, and cheese that melt in the mouth are also commonly consumed by maladaptive eaters as “meals”, as they are easier to swallow than solid foods.24 Overconsumption of softer and easy to eat foods provides inferior nutritional adequacy, as well as reduced gastric transit time, and therefore decreased satiety cues, which ultimately contribute to excessive energy intake and weight gain.
Burton and Brown59 have shown that post-LAGB satiety cues are induced by the activation of stretch receptors caused by “bouncing” of foods at the fundus of the stomach. When in the smaller stomach pouch formed by the band, solid foods, as opposed to foods of a more liquid consistency, bounce more times before passing through the band, providing more stimulation and greater satiety.
Maladaptive eating can also promote the development of food aversion, protein malnutrition, and vitamin and mineral deficiencies, which can affect longer-term weight management and quality of life.31 Prevention of maladaptive eating patterns should commence presurgery and continue in the months following surgery to reinforce healthy eating habits. Emphasis should be made to prevent the onset of gastrointestinal distress and weight regain through strategic dietary changes, such as eating slowly, portion control, and the use of cognitive behavioral strategies to encourage mindful eating.31 The most important strategy that can be utilized by health professionals is to educate patients regarding the need to increase the texture and consistency of their food so that they eat more solids. Not only will solid foods increase satiety by stimulating the stomach stretch receptors, but they also allow for greater variety, nutritional adequacy, and social acceptance of eating. Years of poor eating habits cannot be changed overnight postsurgery, and desensitization to satiety cues can be detrimental to long-term weight loss. Overall, it is essential that patients work in health care teams to prevent the occurrence of maladaptive eating behaviors and maintain a lifelong nutritious diet, and to not simply rely on weight loss alone to improve their life expectancy.
Excessive skin
A sometimes unforeseen complication of weight loss following bariatric surgery is that of excessive skin. After a person has experienced significant weight loss, excess skin and soft tissue redundancy of the trunk, buttocks, breasts, upper arms, and thighs can be obstructive to further weight loss.31,60 Excessive skin can result in musculoskeletal strain from increased tissue weight, and/or intertrigo, both of which can result in limiting both planned and incidental exercise. It is also important to consider the social impacts of having large and usually visible amounts of excessive skin, which may result in poor body image, self-esteem, and social acceptance, which can consequently result in a lack of willingness to participate in public activities such as social sports. This can result in an additional challenge for those trying to achieve weight maintenance.60 Sometimes, these negative impacts can affect social and mental health to a similar degree as prior to the surgery. Some patients resort to intentional weight gain by increasing calorie intake in an attempt to minimize redundant skin.31
More patients are making the decision to surgically remove the redundant skin to further their weight loss and to also improve their quality of life. Body recontouring surgery is generally performed after weight loss has been achieved and stabilized for at least 4–6 months. As a broad rule, this generally occurs 12–18 months postoperatively.60 The surgical team needs to discuss realistic goals, the surgical risk, and comorbidities with the patient before embarking on body contouring surgery. Factors such as the entire body circumference, skin tone and elasticity, sun exposure, smoking status, lean body mass, and muscle tone also need to be deliberated to determine appropriate outcomes. Surgery types generally include breast, thigh, lower body lift, abdominoplasty, face and neck lifts, as well as brachioplasty or arm lifts.61
Medical considerations
Depending on the bariatric procedure, a patient may experience medical complications that can lead to weight regain. These complications need to be continuously monitored to ensure the welfare of the patient is maintained to improve overall weight loss success.
Medical considerations after RYGB
Major postoperative complications, such as leakage, stricture, acute gastric dilatation, and staple failure can develop in the weeks following the RYGB procedure, but they generally are not common occurrences.20 Gastrointestinal anastomotic leakages, for example, have a reported incidence rate of between 1% and 5.1%.62 These complications may contribute to the complete failure of the procedure or the need for premature revision of the RYGB, resulting in limited weight loss and supplementary morbidity and mortality risk.63
More chronic complications include hernias, bowel obstruction, and delayed gastric emptying,20 and they can present months to years following surgery. Internal hernias can occur along different areas of the small bowel, generally at the site of any “limb” created by the bypass procedure.64 Hernias as well as adhesions may further develop into small bowel obstructions.65 Symptoms of these complications include intermittent, postprandial abdominal pain, nausea, and/or vomiting.65 Chronic complications can impede longer-term weight loss outcomes, as the patient may experience a decreased ability to exercise or may revert to maladaptive eating to minimize symptoms. Furthermore, there is the potential requirement for surgical intervention (hospital stints for hernia repair or bowel obstruction), which not only disturbs lifestyle, but which can impact weight loss.65
Medical considerations after SG
Major acute complications of the SG include hemorrhage and leakage along the staple line. As with the RYGB, if these major postoperative complications occur, urgent surgical intervention is required to repair the injury or revise the surgery. Such medical complications can cause substantial loss of lean muscle tissue if patients are not fed enterally or parenterally which, in turn, decreases the patient’s metabolic rate and may impede long-term weight loss outcomes.66
Longer-term medical complications that may affect the SG patient include gastroesophageal reflux disease (GERD) and stomach stretching. Studies indicate that post-SG, GERD is developed in approximately 20% of patients.33,67 Chronic GERD often influences dietary intake, and it may increase the likelihood of maladaptive eating.67 Furthermore, some patients turn to eating or drinking as a tool for symptom relief. Obviously, eating for symptom relief can lead to excess calorie intake and subsequent weight gain. GERD development can be attributed to altered gastric emptying, decreased gastric compliance resulting in increased intragastric pressure, as well as the anatomical changes in the angle of His.67 The angle of His is naturally a gastroesophageal-protective mechanism; however, it is initially blunted with the SG procedure. If this angle restores itself over time, patients generally report an improvement in GERD.67 If GERD does not resolve naturally, the use of medications, as well as dietetic intervention and education regarding food choices and eating strategies, should be adopted to best manage symptoms.
Stomach stretching is a significant cause of weight regain post-SG; however, there is a paucity of long-term clinical evidence to describe the rates of occurrence. The stomach may stretch and dilate over time, lessening the restrictive and early satiating effects of the SG, thus allowing the patient to ingest larger quantities of food and consequently regain weight.33 Investigations into stomach dilatation suggest that the stretching forms a new fundus, which counteracts the intentions of the sleeve.33 Studies suggest that creating a smaller stomach bougie size may result in greater weight loss and may prevent later stretch of the sleeve;68 otherwise, surgery may be considered to resleeve or convert to RYGB.33
Medical considerations after LAGB
Attractive benefits of the LAGB are that it has lower rates of nutritional deficiencies and mortality risks than other types of bariatric surgery, and there is the possibility of reversibility, while still having the potential for significant long-term weight loss.67 However, a study by Aarts et al69 found that 100% of patients who had their band removed regained the weight.
Furthermore, the band itself can be the cause of complications that can negatively affect long-term weight loss.20 Pouch dilatation, band migration, slippage of the stomach through the band, as well as issues arising from the port, such as leakage, infection, and dislocation are common complications seen longer-term postband insertion.70 Such complications can usually be treated laparoscopically, but this generally requires minimal fluid in the band, resulting in the level of restriction and satiety being decreased.70 Consequently, these complications can often result in significant weight regain. In the case of pouch dilatation, it results in decreased satiety and allows the patient to ingest a greater amount of food, which can lead to weight regain. For optimal results, the patient and health care team need to provide regular reviews to monitor the “health” of the band, such as placement, fluid capacity, and port access.
Gastric erosion of the band through the stomach wall is a more serious complication that requires the band to be completely removed, thereby increasing the risk of significant weight regain. Symptoms include fever, chills, and epigastric pain, which additionally impact on the patient’s dietary intake and physical activity levels prior to removal. Another LAGB may be reinserted after a period of recovery, or there may be the need for revisional bariatric surgery; however, this interim period (generally a few months) often results in weight regain.70
Although only occurring in a minority of cases, some patients may react negatively to the band being in situ. This is generally referred to as psychological intolerance to the band and arises as patients become averse to the concept of a foreign body being inside their person. Treatment involves complete band removal, and the patient and surgeon may then decide to revise the bariatric surgery to RYGB or SG.71 If the patient wants no further bariatric intervention, the weight loss assistance that the band could potentially provide disappears with its removal.
Dixon and O’Brien72 have shown that in people previously suffering with GERD and/or esophagitis, LAGB insertion can improve their symptoms. Explanations put forth include the narrowing of the esophagogastric junction, reconstitution of the angle of His, and the band itself acts as an antireflux mechanism.72 Longer-term follow up, however, indicates that GERD can develop in the years after LAGB insertion in approximately 20.5% of patients,67 potentially due to pouch dilatation or stomach herniation, slippage of the band, accumulation of acid, and/or disordered esophageal motility.73 Depending on its severity, GERD symptoms such as regurgitation, nausea, and/or heartburn can impact longer-term weight loss, as patients may alter their eating habits, turning to grazing, using food to medicate symptoms, and/or maladaptive eating. In extreme cases, some patients may even choose to remove the band as a result of debilitating GERD symptoms.73
Historically, the RYGB procedure has been preferred if revision surgery is required, either due to medical complications as a result of the band, or inadequate weight loss;63 however, SG surgeries are also emerging as a potential option as a secondary surgery post-LAGB.66 It should be known that the revision of previous bariatric procedures carries a higher risk of leakage, reported to be as high as 19%.63
As with all bariatric surgeries, the need for check-ups with the medical team in the weeks to years following the procedure is a requirement for the early diagnosis and resolution of structural or acute complications. Rectifying these complications may allow the patient the best chance of avoiding surgical failure or surgery revision and, therefore, of achieving maximum weight loss. Regular longer-term reviews with the health care team, including surgical and dietetic professions, will aid in potentially identifying more medical complications, as well as being able to implement suitable dietary interventions best suited for optimal recovery without weight regain.
Other medical conditions
Weight regain or suboptimal weight loss may also be a result of an underlying medical condition such as undiagnosed thyroid problems, Cushing’s syndrome, leptin deficiency, or OSA. A long-term observational study by Collen et al74 found that bariatric patients with OSA experienced significantly more weight loss success if they continued to utilize their continuous positive airway pressure machines as prescribed than those who did not. Medications that affect weight gain, such as insulin, steroids, and antipsychotics, can also have an impact on weight loss success, even after weight loss surgery. Subsequently, it is imperative for the health care team to consider conventional medical causes of the weight regain, branding the surgery as a “failure”.
Conclusion
Long-term weight loss in patients following bariatric surgery requires regular and supportive management by qualified health professionals. Based on the literature reviewed, our principal recommendations to optimize long-term weight loss include:
- ensuring that the patient understands how the procedure works;
- offering pre- and postoperative education sessions;
- ensuring the patient utilizes self-monitoring strategies;
- tailoring nutritional supplements;
- restraining liquid calories, pureed foods, grazing, and eating out of home;
- engaging in an average of 60 minutes of physical activity per day; and
- conducting lifelong annual medical, psychological, and dietary assessments.
Disclosure
The authors report no conflicts of interest in this work.
References
World Health Organization [webpage on the Internet]. Obesity and overweight. Geneva, Switzerland: World Health Organization; 2014. Available from: http://www.who.int/mediacentre/factsheets/fs311/en/. Accessed October 28, 2014. | |
Colquitt JL, Pickett K, Loveman E, Frampton GK. Surgery for weight loss in adults. Cochrane Database Syst Rev. 2014;8:CD003641. | |
Khwaja HA, Bonanomi G. Bariatric surgery: techniques, outcomes and complications. Trends in Anaesthesia and Critical Care. 2010;21(1):31–38. | |
National Health and Medical Research Council. Clinical practice guidelines for the management of overweight and obesity in adults, adolescents and children in Australia. National Health and Medical Research Council. 2013:204. | |
Jaunoo SS, Southall PJ. Bariatric surgery. Int J Surg. 2010;8(2):86–89. | |
Neff KJ, Olbers T, le Roux CW. Bariatric surgery: the challenges with candidate selection, individualizing treatment and clinical outcomes. BMC Med. 2013;11:8. | |
Ames GE, Patel RH, Ames SC, Lynch SA. Weight loss surgery: patients who regain. Obesity and Weight Management. 2009;5(4):154–161. | |
Puzziferri N, Roshek TB, Mayo HG, Gallagher R, Belle SH, Livingston EH. Long-term follow-up after bariatric surgery: a systematic review. JAMA. 2014;312(9):934–942. | |
O’Brien PE, MacDonald L, Anderson M, Brennan L, Brown WA. Long-term outcomes after bariatric surgery: fifteen-year follow-up of adjustable gastric banding and a systematic review of the bariatric surgical literature. Ann Surg. 2013;257(1):87–94. | |
Bohdjalian A, Langer FB, Shakeri-Leidenmühler S, et al. Sleeve gastrectomy as sole and definitive bariatric procedure: 5-year results for weight loss and ghrelin. Obes Surg. 2010;20(5):535–540. | |
O’Brien PE, McPhail T, Chaston TB, Dixon JB. Systematic review of medium-term weight loss after bariatric operations. Obes Surg. 2006;16(8):1032–1040. | |
Christou NV, Look D, Maclean LD. Weight gain after short- and long-limb gastric bypass in patients followed for longer than 10 years. Ann Surg. 2006;244(5):734–740. | |
Sjöström L, Lindroos AK, Peltonen M, et al; Swedish Obese Subjects Study Scientific Group. Lifestyle, diabetes, and cardiovascular risk factors 10 years after bariatric surgery. N Engl J Med. 2004;351(26):2683–2693. | |
Magro DO, Geloneze B, Delfini R, Pareja BC, Callejas F, Pareja JC. Long-term weight regain after gastric bypass: a 5-year prospective study. Obes Surg. 2008;18(6):648–651. | |
Silver HJ, Torquati A, Jensen GL, Richards WO. Weight, dietary and physical activity behaviors two years after gastric bypass. Obes Surg. 2006;16(7):859–864. | |
Shah M, Simha V, Garg A. Review: long-term impact of bariatric surgery on body weight, comorbidities, and nutritional status. J Clin Endocrinol Metab. 2006;91(11):4223–4231. | |
Wing RR, Tate DF, Gorin AA, Raynor HA, Fava JL. A self-regulation program for maintenance of weight loss. N Engl J Med. 2006;355(15):1563–1571. | |
Odom J, Zalesin KC, Washington TL, et al. Behavioral predictors of weight regain after bariatric surgery. Obes Surg. 2010;20(3):349–356. | |
Dixon JB, Laurie CP, Anderson ML, Hayden MJ, Dixon ME, O’Brien PE. Motivation, readiness to change, and weight loss following adjustable gastric band surgery. Obesity (Silver Spring). 2009; 17(4):698–705. | |
Mechanick JI, Kushner RF, Sugerman HJ, et al. American Association of Clinical Endocrinologists, The Obesity Society, and American Society for Metabolic and Bariatric Surgery Medical Guidelines for Clinical Practice for the perioperative nutritional, metabolic, and nonsurgical support of the bariatric surgery patient. Surg Obes Relat Dis. 2008;4(5 Suppl):S109–S184. | |
Soliah LA. The seven secrets of successful weight loss. Today’s Dietician. 2008;10(7):50. | |
Allis L, Blankenship J, Buffington C, Furtado M, Parrott J; Allied Health Sciences Section Ad Hoc Nutrition Committee. ASMBS Allied Health Nutritional Guidelines for the surgical weight loss patient. Surg Obes Relat Dis. 2008;4(5 Suppl):S73–S108. | |
Conason A, Teixeira J, Hsu CH, Puma L, Knafo D, Geliebter A. Substance use following bariatric weight loss surgery. JAMA Surg. 2013;148(2):145–150. | |
Brolin RE, Robertson LB, Kenler HA, Cody RP. Weight loss and dietary intake after vertical banded gastroplasty and Roux-en-Y gastric bypass. Ann Surg. 1994;220(6):782–790. | |
Sugerman HJ, Starkey JV, Birkenhauer R. A randomized prospective trial of gastric bypass versus vertical banded gastroplasty for morbid obesity and their effects on sweets versus non-sweets eaters. Ann Surg. 1987;205(6):613–624. | |
King WC, Chen JY, Mitchell JE, et al. Prevalence of alcohol use disorders before and after bariatric surgery. JAMA. 2012;307(23):2516–2525. | |
Parkes E. Nutritional management of patients after bariatric surgery. Am J Med Sci. 2006;331(4):207–213. | |
Dietitians Association of Australia. DAA Best Practice Guidelines for the Treatment of Overweight and Obesity in Adults. Canberra, Australia: Dietitians Association of Australia; 2005. | |
Colles SL, Dixon JB, O’Brien PE. Grazing and loss of control related to eating: two high-risk factors following bariatric surgery. Obesity (Silver Spring). 2008;16(3):615–622. | |
White MA, Kalarchian MA, Masheb RM, Marcus MD, Grilo CM. Loss of control over eating predicts outcomes in bariatric surgery patients: a prospective, 24-month follow-up study. J Clin Psychiatry. 2010;71(2):175–184. | |
Rusch MD, Andris D. Maladaptive eating patterns after weight-loss surgery. Nutr Clin Pract. 2007;22(1):41–49. | |
Bastos EC, Barbosa EM, Soriano GM, dos Santos EA, Vasconcelos SM. Determinants of weight regain after bariatric surgery. Arq Bras Cir Dig. 2013;26 Suppl 1:26–32. | |
Himpens J, Dobbeleir J, Peeters G. Long-term results of laparoscopic sleeve gastrectomy for obesity. Ann Surg. 2010;252(2):319–324. | |
Busetto L, Valente P, Pisent C, et al. Eating pattern in the first year following adjustable silicone gastric banding (ASGB) for morbid obesity. Int J Obes Relat Metab Disord. 1996;20(6):539–546. | |
Garcia G, Sunil TS, Hinojosa P. The fast food and obesity link: consumption patterns and severity of obesity. Obes Surg. 2012;22(5):810–818. | |
Mitchell JE, King WC, Courcoulas A, et al. Eating behavior and eating disorders in adults before bariatric surgery. Int J Eat Disord. 2015;48(2):215–222. | |
Agha-Mohammadi S, Hurwitz DJ. Nutritional deficiency of post-bariatric surgery body contouring patients: what every plastic surgeon should know. Plast Reconstr Surg. 2008;122(2):604–613. | |
Faria SL, de Oliveira Kelly E, Lins RD, Faria OP. Nutritional management of weight regain after bariatric surgery. Obes Surg. 2010;20(2):135–139. | |
Das SK, Roberts SB, McCrory MA, et al. Long-term changes in energy expenditure and body composition after massive weight loss induced by gastric bypass surgery. Am J Clin Nutr. 2003;78(1):22–30. | |
Faria SL, Faria OP, Lopes TC, Galvão MV, de Oliveira Kelly E, Ito MK. Relation between carbohydrate intake and weight loss after bariatric surgery. Obes Surg. 2009;19(6):708–716. | |
Dixon JB, O’Brien PE. Bariatric surgery provides unparalleled metabolic benefits. Obes Surg. 2007;17(2):193–194. | |
Krieger JW, Sitren HS, Daniels MJ, Langkamp-Henken B. Effects of variation in protein and carbohydrate intake on body mass and composition during energy restriction: a meta-regression 1. Am J Clin Nutr. 2006;83(2):260–274. | |
Aguirre N, van Loon LJ, Baar K. The role of amino acids in skeletal muscle adaptation to exercise. Nestle Nutr Inst Workshop Ser. 2013;76:85–102. | |
Dixon JB, O’Brien PE, Playfair J, et al. Adjustable gastric banding and conventional therapy for type 2 diabetes: a randomized controlled trial. JAMA. 2008;299(3):316–323. | |
Salgado W Jr, Modotti C, Nonino CB, Ceneviva R. Anemia and iron deficiency before and after bariatric surgery. Surg Obes Relat Dis. 2014; 10(1):49–54. | |
McGrice MA, Porter JA. What are gastric banding patients eating one year post-surgery? Obes Surg. 2012;22(12):1855–1858. | |
Isom KA, Andromalos L, Ariagno M, et al. Nutrition and metabolic support recommendations for the bariatric patient. Nutr Clin Pract. 2014;29(6):718–739. | |
McGrice MA, Porter JA. The micronutrient intake profile of a multicentre cohort of Australian LAGB patients. Obes Surg. 2014;24(3):400–404. | |
Aktas G, Alcelik A, Yalcin A, et al. Treatment of iron deficiency anemia induces weight loss and improves metabolic parameters. Clin Ter. 2014; 165(2):e87–e89. | |
Pournaras DJ, le Roux CW. After bariatric surgery, what vitamins should be measured and what supplements should be given? Clin Endocrinol (Oxf). 2009;71(3):322–325. | |
Yeager SF. Role of the dietician in a multidisciplinary bariatric program. Bariatric Nursing and Surgical Patient Care. 2008;3(2):107–116. | |
World Health Organization [webpage on the Internet]. Global strategy on diet, physical activity and health: physical activity. Geneva, Switzerland: World Health Organization; 2014. Available from: http://www.who.int/dietphysicalactivity/pa/en/. Accessed December 22, 2014. | |
Livhits M, Mercado C, Yermilov I, et al. Patient behaviors associated with weight regain after laparoscopic gastric bypass. Obes Res Clin Pract. 2011;5(3):e169–e266. | |
Bond DS, Evans RK, Wolfe LG, et al. Impact of self-reported physical activity participation on proportion of excess weight loss and BMI among gastric bypass surgery patients. Am Surg. 2004;70(9):811–814. | |
Sousa P, Bastos AP, Venâncio C, et al. [Understanding depressive symptoms after bariatric surgery: the role of weight, eating and body image]. Acta Med Port. 2014;27(4):450–457. Portuguese. | |
Segal A, Kinoshita Kussunoki D, Larino MA. Post-surgical refusal to eat: anorexia nervosa, bulimia nervosa or a new eating disorder? A case series. Obes Surg. 2004;14(3):353–360. | |
de Man Lapidoth J, Ghaderi A, Norring C. A comparison of eating disorders among patients receiving surgical vs non-surgical weight-loss treatments. Obes Surg. 2008;18(6):715–720. | |
Kalarchian MA, Marcus MD, Wilson GT, Labouvie EW, Brolin RE, LaMarca LB. Binge eating among gastric bypass patients at long-term follow-up. Obes Surg. 2002;12(2):270–275. | |
Burton PR, Brown WA. The mechanism of weight loss with laparoscopic adjustable gastric banding: induction of satiety not restriction. Int J Obes (Lond). 2011;35 Suppl 3:S26–S30. | |
Chandawarkar RY. Body contouring following massive weight loss resulting from bariatric surgery. Adv Psychosom Med. 2006;27:61–72. | |
Modolin M, Cintra W Jr, Gobbi CI, Ferreira MC. Circumferential abdominoplasty for sequential treatment after morbid obesity. Obes Surg. 2003;13(1):95–100. | |
Marshall JS, Srivastava A, Gupta SK, Rossi TR, DeBord JR. Roux-en-Y gastric bypass leak complications. Arch Surg. 2003;138(5):520–523; discussion 523–524. | |
Schwartz RW, Strodel WE, Simpson WS, Griffen WO. Gastric bypass revision: lessons learned from 920 cases. Surgery. 1988;104(4):806–812. | |
Tucker ON, Escalante-Tattersfield T, Szomstein S, Rosenthal RJ. The ABC System: a simplified classification system for small bowel obstruction after laparoscopic Roux-en-Y gastric bypass. Obes Surg. 2007;17(12):1549–1554. | |
Garza E, Kuhn J, Arnold D, Nicholson W, Reddy S, McCarty T. Internal hernias after laparoscopic Roux-en-Y gastric bypass. Am J Surg. 2004;188(6):796–800. | |
Lalor PF, Tucker ON, Szomstein S, Rosenthal RJ. Complications after laparoscopic sleeve gastrectomy. Surg Obes Relat Dis. 2008;4(1):33–38. | |
Himpens J, Dapri G, Cadière GB. A prospective randomized study between laparoscopic gastric binding and laparoscopic isolated sleeve gastrectomy: results after 1 and 3 years. Obes Surg. 2006;16(11):1450–1456. | |
Shi X, Karmali S, Sharma AM, Birch DW. A review of laparoscopic sleeve gastrectomy for morbid obesity. Obes Surg. 2010;20(8):1171–1177. | |
Aarts EO, Dogan K, Koehestanie P, Janssen IM, Berends FJ. What happens after gastric band removal without additional bariatric surgery? Surg Obes Relat Dis. 2014;10(6):1092–1096. | |
Niville E, Dams A, Vlasselaers J. Lap-Band erosion: incidence and treatment. Obes Surg. 2001;11(6):744–747. | |
Favretti F, Cadière GB, Segato G, et al. Laparoscopic banding: selection and technique in 830 patients. Obes Surg. 2002;12(3):385–390. | |
Dixon JB, O’Brien PE. Gastroesophageal reflux in obesity: the effect of lap-band placement. Obes Surg. 1999;9(6):527–531. | |
de Jong JR, van Ramshorst B, Timmer R, Gooszen HG, Smout AJ. The influence of laparoscopic adjustable gastric binding on gastroesophageal reflux. Obes Surg. 2004;14(3):399–406. | |
Collen J, Lettieri CJ, Eliasson A. Postoperative CPAP use impacts long-term weight loss following bariatric surgery. J Clin Sleep Med. 2015;11(3):213–217. |
 © 2015 The Author(s). This work is published and licensed by Dove Medical Press Limited. The full terms of this license are available at https://www.dovepress.com/terms.php and incorporate the Creative Commons Attribution - Non Commercial (unported, v3.0) License.
By accessing the work you hereby accept the Terms. Non-commercial uses of the work are permitted without any further permission from Dove Medical Press Limited, provided the work is properly attributed. For permission for commercial use of this work, please see paragraphs 4.2 and 5 of our Terms.
© 2015 The Author(s). This work is published and licensed by Dove Medical Press Limited. The full terms of this license are available at https://www.dovepress.com/terms.php and incorporate the Creative Commons Attribution - Non Commercial (unported, v3.0) License.
By accessing the work you hereby accept the Terms. Non-commercial uses of the work are permitted without any further permission from Dove Medical Press Limited, provided the work is properly attributed. For permission for commercial use of this work, please see paragraphs 4.2 and 5 of our Terms.