Back to Journals » International Journal of General Medicine » Volume 14
Influence of KDR Genetic Variation on the Efficacy and Safety of Patients with Chemotherapy Refractory Metastatic CRC Who Received Apatinib Treatment
Received 13 January 2021
Accepted for publication 22 February 2021
Published 25 March 2021 Volume 2021:14 Pages 1041—1055
DOI https://doi.org/10.2147/IJGM.S300968
Checked for plagiarism Yes
Review by Single anonymous peer review
Peer reviewer comments 2
Editor who approved publication: Dr Scott Fraser
Ming Bai,1,* Zhi-Guo Li,2,* Yi Ba1
1Department of Gastrointestinal Oncology, Affiliated Tumor Hospital of Tianjin Medical University, Tianjin Medical University Cancer Institute and Hospital, National Clinical Research Center for Cancer, Tianjin’s Clinical Research Center for Cancer, Key Laboratory of Cancer Prevention and Therapy, Tianjin, People’s Republic of China; 2Department of Minimally Invasive Digestive Surgery, Shanxi Cancer Hospital, Taiyuan, People’s Republic of China
*These authors contributed equally to this work
Correspondence: Yi Ba
Department of Gastrointestinal Oncology, Affiliated Tumor Hospital of Tianjin Medical University, 1 Middle Huanhu Road, Tianjin, People’s Republic of China
Tel +86 18622221230
Email [email protected]
Background: The aim of the present study was to investigate the influence of kinase insert domain containing receptor (KDR) genetic variation on the efficacy of treatment and safety of patients with chemotherapy-refractory metastatic colorectal cancer (CRC) receiving apatinib.
Methods: A total of 108 patients with chemotherapy refractory metastatic CRC who were treated with apatinib participated in this study retrospectively. Efficacy of the patients’ treatment was evaluated. Prognosis was carried out and safety profile was documented, respectively. Blood specimens and peripheral blood mononuclear cells (PBMC) of the patients were obtained for the analysis of genetic variation and KDR gene mRNA expression, respectively. The association between genotype status and clinical outcomes was presented.
Results: Objective response rate (ORR) and disease control rate (DCR) of the 108 patients with metastatic CRC receiving apatinib treatment were 5.6% and 69.4%, respectively. Survival analysis results exhibited that the median progression-free survival (PFS) and overall survival (OS) of the 108 patients with metastatic CRC was 3.6 months (95% confidence interval (CI): 3.03– 4.17 months) and 8.9 months (95% CI: 7.57– 10.23 months), respectively. Subsequently, the analysis of KDR genetic variation indicated that rs2071559 was of clinical significance. The minor allele frequency of rs2071559 was 0.22 and the genotype status corresponded with Hardy-Weinberg equilibrium (P=0.949). Prognosis analysis in a dominant inheritance manner through the combination of patients with TC and CC genotype showed that the median PFS of patients with TT genotype and TC/CC genotype was 4.1 and 3.0 months, respectively (P=0.012). Furthermore, the median OS of patients with the two genotypes was 10.5 and 6.1 months, respectively (P=0.007). Additionally, multivariate Cox regression analysis of OS showed that TC/CC genotype was an independent factor for OS (Hazard ratio (HR)=0.65, P=0.021). Interestingly, mRNA expression analysis suggested that the mRNA expression of KDR in PBMC differed significantly according to rs2071559 genotype status (P< 0.001).
Conclusion: Apatinib demonstrated a potentially superior clinical outcome for patients with chemotherapy-refractory metastatic CRC. KDR polymorphism rs2071559 could be used as a potential biomarker for the prognosis evaluation of patients with CRC receiving apatinib therapy.
Keywords: colorectal cancer, apatinib, kinase insert domain containing receptor, genetic variation, biomarker, clinical outcome, safety
Introduction
Colorectal cancer (CRC) is one of the most common malignancies and the leading cause of cancer-related death all over the world, and is characterized by the somatic mutations of the gene in critical pathways.1 It is estimated that annually there are approximately 1.8 million new cases and 0.86 million new deaths globally.2 Currently, there are approximately 375,000 new cases and 191,000 new deaths in China annually.3 A previous study exhibited that approximately 20% of the newly diagnosed patients presented with metastases and about 30% of patients with stage ІІ/ш who underwent surgical resection would experience recurrence within 5 years .4 As a result, the estimated patients with CRC of metastatic disease were approximately 187,000 each year in China.5 Therefore, numerous patients lost the opportunity for surgical resection and had to receive the fluorouracil-based double regimen as first-line chemotherapy treatment.6 Although immunotherapy has made significant breakthroughs in a number of tumors in recent years, it had been proved that only patients with highly unstable microsatellites (MSI-H) have the potentialto benefit from immunotherapy in metastatic CRC.7 The research breakthrough of targeted drugs in metastatic CRC is relatively limited currently, and is mainly concentrated on anti-EGFR cetuximab and anti-VEGF bevacizumab therapy.8 The first-line conventional chemotherapy regimen combined with EGFR antibody or VEGF antibody could prolong the median overall survival (OS) to approximately 30 months.9 Unfortunately, most of the patients experience disease progression after two or more lines of systemic treatment and a substantial proportion of patients were able to keep a relatively superior performance status after previous standard chemotherapy.10 Consequently, it was necessary to urgently investigate the potentially effective treatment options as subsequent line therapy.
To our knowledge, antiangiogenic targeted drugs have played an important role as the subsequent line treatment for patients with metastatic CRC.11 Regorafenib and fruquintinib were recommended as the subsequent line treatment for patients with metastatic CRC who were refractory to standard first-line and second-line therapy.12,13 As each is an antiangiogenic small molecular tyrosine kinase inhibitor (TKI), regorafenib and fruquintinib mainly targeted VEGFR1-3, FGFR and PDGFR, and were licensed in China since 2017 and 2018, respectively.14 However, owing to the unavailability of regorafenib and fruquintinib in China at a certain time, considerable exploratory studies evaluated other vascular epidermal growth factor receptor (VEGFR) inhibitors with similar mechanism to regorafenib or fruquintinib as the subsequent line treatment of metastatic CRC which failed after at least two lines of previous chemotherapy treatment.15 Apatinib was developed by Adrenchen Laboratories and approved as a subsequent line regimen for advanced or metastatic gastric cancer by cFDA in October 2014.16 Considerable researchdemonstrated that apatinib exhibited encouraging anti-tumor activity with tolerable toxicity in lung cancer and CRC.15,17,18 Interestingly, as far as we know, the overall response of antiangiogenic TKI was generally low clinically. In the treatment of metastatic CRC, the objective response rate (ORR) of apatinib,10 regorafenib19 and fruquintinib20 monotherapy was 8.3%, 4.4% and 4.7%, respectively. The conclusion of these studies highlighted that great individual differences existed regarding the efficacy of apatinib. Consequently, predictive biomarkers were needed to distinguish patients who would be most likely to benefit from antiangiogenic TKI therapy. However, the useful biomarkers were mainly focused on adverse reactions attributed to VEGF-TKIs, such as hypertension and hand-foot syndrome.21 These biomarkers, of course, were limited to post-treatment occurrences. Biomarkers for pre-treatment were also needed clinically. Interestingly, a recently published exploratory research exhibited that polymorphism 4397T>C in kinase insert domain containing receptor (KDR) gene could be a potential biomarker to predict the prognosis of patients with non-squamous non-small cell lung cancer who received apatinib treatment.22 As the important target of apatinib, KDR gene is located on chromosome 4q12 and contains 30 exons. Another previous study suggested that rs2071559 of VEGFR2 gene was of clinical significance to predict the efficacy in patients with epithelial ovarian carcinoma (EOC) treated with apatinib.23 In conclusion, these data demonstrated the potential predictive value of KDR gene for efficacy in patients receiving apatinib treatment.
However, no potential polymorphism biomarkers were available to predict the efficacy and safety of apatinib for patients with chemotherapy-refractory metastatic CRC. In consequence, the present study was to investigate the influence of KDR genetic variation on the efficacy and safety of apatinib for patients with chemotherapy-refractory metastatic CRC.
Patients and Methods
Patients Enrollment and Study Design
Given that apatinib was licensed in China since October 2014, a considerable number of patients with CRC have been treated with apatinib therapy clinically, so this study was designed as a real-world retrospective analysis. The protocol of the present study was approved by the ethics committee of Affiliated Tumor Hospital of Tianjin Medical University, and was conducted in accordance with the Declaration of Helsinki and Good Clinical Practice guidelines.
In detail, patients with CRC who failed after at least two lines of previous chemotherapy regimens in the Department of Gastrointestinal Oncology of Affiliated Tumor Hospital of Tianjin Medical University from January 2015 to March 2020 were included in this study consecutively. The main inclusion criteria included: (a) histologically or cytologically diagnosed adenocarcinoma in the colon or rectum; (b) age ≥18 years; (c) pathological stage of IV; (d) Eastern Cooperative Oncology Group (ECOG) performance status score ≤2 ; (e) apatinib was administered for patients who had failed after at least two lines of previous systemic chemotherapy regimens; (f) at least one measurable target lesion according to response evaluation criteria in solid tumors (RECIST 1.1) to document the tumor response and the patients were evaluated for at least one measurement.24 Primary exclusion criteria were: (a) pathological type of mucinous adenocarcinoma; (b) previous exposure to apatinib. However, pervious bevacizumab or other antiangiogenic TKI administration at any line was permitted; (c) concomitant with another tumor or serious diseases based on the decision of the investigator; (d) data for efficacy assessment were not available. The flow chart of our retrospective study is illustrated in Figure 1. Eventually, a total of 108 patients with metastatic CRC was enrolled. The primary analysis of the present study was the efficacy of treatment and safety of patients with chemotherapy refractory metastatic CRC who received apatinib treatment according to KDR gene polymorphism status.
Administration of Apatinib and Assessment of Efficacy and Safety
Apatinib was administered orally at an initial dosage of 500 mg or 250 mg per day, half an hour after meals with warm water and continuously for 28 days until disease progression or treatment became intolerable. The dosage of 500 mg or 250 mg depended on each doctor’s decision according to the physical condition of each patient. The dosage of apatinib was adjusted based on the hematological or non-hematological toxicity during the treatment. The treatment could be permanently discontinued in the event of severe adverse reactions.
The efficacy was assessed according to RECIST 1.1 criteria. The comparison of target lesions was assessed every two cycles or as necessary if significant symptoms with evidence of progression appeared. Adverse reactions during treatment were evaluated using Common Terminology Criteria for Adverse Events (CTCAE) 4.03 version to document hematological and non-hematological events that might be drug-related.25
With regard to the follow-up protocol, each patient was followed up from the onset of enrollment. Firstly, the patients were evaluated during the hospitalization period when they received apatinib treatment. Demographic characteristics, previous treatment regimens, response status, adverse reactions and progression status of the patient could be clearly obtained through the electronic medical record system. Secondly, the subsequent follow-up was mainly carried out by telephone. Each subject was followed up every months following the apatinib treatment for progression and survival status. The last follow-up date of this study was November 30, 2020.
Collection of Peripheral Blood Specimen and Genotyping of KDR Gene Polymorphism
Peripheral blood specimens of each patient were collected (approximately 4 mL). The genomic DNA was extracted using phenol chloroform method and then stored at −20°C for subsequent analysis.
Given that the previous study showed that 4397T>C (rs2071559) was of clinical significance among patients with NSCLC,22 rs2071559 was included in our analysis. Additionally, other single nucleotide polymorphisms were collected in the NCBI database with minor allele frequency (MAF) >10% among the Chinese population. The polymorphisms included were rs2071559, rs2305948, rs11941492 and rs1870377. We carried out the preliminary correlation analysis between the four polymorphisms’ genotype status and prognosis first, and the results are shown in Table 1. Of the four polymorphisms analyzed, only rs2071559 had a significant association with prognosis. Consequently, the subsequent analysis of this study was focused on the rs2071559 polymorphism.
 |
Table 1 The Four Polymorphisms Included in This Study and the Preliminary Analysis Between Genotypes Status and Prognosis |
The rs2071559 polymorphism of KDR gene was genotyped using restriction fragment length polymorphism polymerase chain reaction (PCR-RFLP). First, the PCR product including this polymorphism was amplified . The forward primer was 5ʹ-TCACTAGGGCTCTTCGTTGG-3ʹ, the reverse primer was 5ʹ-GAAGCGGATACTCAGCCAAG-3ʹ according to the previous study.23 The size of the amplified products was 271 bp, a total of 2 μL amplified products were digested using the restriction enzyme BsmI (Thermo Fisher Scientific, USA). The genotypes of the polymorphism were distinguished through the size of PCR bands as follows: TT genotype (one 271 bp band); CC genotype (one 108 bp band and one 163 bp band); TC genotype (one 271 bp band, one 108 bp band and one 163 bp band). Randomly selected genotyping results of rs2071559 were validated using ionization-time-of-flight mass spectrometry (Sequenom, SanDiego, CA). The two genotyping approaches reached 100% agreement.
Collection of PBMC Specimens and Analysis of KDR Gene mRNA Expression
Given that polymorphism is an inherited germline mutation rather than a somatic mutation, we collected the PBMC specimens instead of cancer tissue specimens to explore the potential association between polymorphism and mRNA expression. Consequently, the matched PBMC specimens were obtained from 81 randomly selected samples from the 108 patients with CRC initially. However, 6 patients failed the extraction of PBMC specimens and 9 specimens failed for the RNA extraction. Finally, a total of 66 specimens were available for mRNA experimentation and preserved in liquid nitrogen. Subsequently, total RNA samples were extracted using Trizol reagents (Takara, Biotechnology, Dalian, China) according to the manufacturer’s instruction and stored at −80°C for mRNA expression analysis.
A total of 500 ng RNA extracted from the PBMC specimens was used as the templates for reverse-transcription polymerase chain reaction to prepare the first-strand of cDNA using the PrimeScript RT reagent Kit. Relative quantitative analysis of KDR gene mRNA expression was performed using the LightCycler® 480 with SYBR Premix EX Taq system. The forward primer of KDR gene was 5ʹ-ATGCAGAGCAAGGTGCTGC-3ʹ, the reverse primer was 5ʹ- TTAAACAGGAGGAGAGCTCAGTG-3ʹ according to the previous work.22 Amplification systemcomprised 10 µL SYBR Premix EX Taq, 0.2 µL of each primer (20 µM), 7.6 µL double distilled water (ddH2O) and 2 µL cDNA. KDR mRNA expression was detected by comparative Ct (2−ΔΔCt). GAPDH mRNA expression was used as an endogenous control.
Statistical Analysis
All of the variables were statistically analyzed using the statistical analysis software SPSS version 25.0 (IBM, USA). Hardy-Weinberg equilibrium test was performed for the rs2071559 genotypes using χ2 test. The significance of proportion variables and continuous variables according to polymorphism genotype status was performed using χ2 test and the Mann–Whitney U non-parametric test, respectively. With regard to the efficacy of apatinib, ORR was the proportion of complete response (CR) plus partial response (PR) in the total evaluated patients. DCR was calculated according to the percentage of CR plus PR and stable disease (SD).
With regard to the prognosis, progression-free survival (PFS) was defined as the duration from the onset of apatinib treatment to disease progression or death, whichever occurred first. Overall survival (OS) was defined as the duration from the onset of apatinib treatment to death of the patient from any cause.26 For those who were still receiving apatinib treatment or alive, survival end points were censored at the date of cut-off. The final cut-off date was November 30, 2020. The primary analysis was performed on the association between rs2071559 genotype status and PFS. Kaplan-Meier survival curves were generated using Stata version 14.0 to compare the differences in PFS and OS according to rs2071559 genotype status with Log rank test. Multivariate Cox regression analysis was performed for PFS and OS. P<0.05 was denoted as statistical significance.
Results
Baseline Characteristics of the 108 Patients with Metastatic CRC According to Genotype Status of rs2071559
The baseline characteristics of the 108 patients with metastatic CRC are shown in Table 2. The median age of subjects enrolled was 58 (27–81) years old; 63 (58.3%) patients were male and 45 (41.7%) were female. ECOG 0–1 score was noted in 61 (56.5%) patients. Additionally, right-sided colon cancer and left-sided CRC was observed in 37 and 71 patients, respectively. Seventy-three patients were recorded with liver metastases from CRC and lung metastases were reported in 31 patients. A total of 35 patients had undergone R0 resection previously, 37 patients had undergone non-R0 resection previously. Moreover, 69 patients had received two lines of treatment and ≥3 lines of therapy was observed in 39 patients. The proportion was similar among patients with or without a history of targeted drugs therapy. Interestingly, 9 patients had received immunotherapy previously. Apatinib was administered at an initial dosage of 250 mg and 500 mg in 42 and 66 patients, respectively.
 |
Table 2 Baseline Characteristics of the 108 Patients with Metastatic CRC According to Genotype Status of rs2071559 Polymorphism |
Rs2071559 was of clinical significance in the subsequent analysis. The prevalence of rs2071559 in the 108 patients with CRC were: TT genotype 66 cases (61.1%), TC genotype 37 cases (34.3%) and CC genotype 5 cases (4.6%). Therefore, the minor allele frequency of rs2071559 was 0.22, which corresponded with Hardy-Weinberg equilibrium (P=0.949). Given that the frequency of CC genotype was relatively rare, CC and TC genotypes were merged in a dominant inheritance manner. As shown in Table 2, patients with TT and TC/CC genotypes were well balanced with similar distribution of baseline characteristics.
Influence of KDR Gene Polymorphism on the Clinical Outcomes of 108 Patients with CRC
The best overall response of each enrolled patient was recorded and analyzed during apatinib treatment. Efficacy of apatinib among patients with CRC included complete response (CR) in 0 patient, partial response (PR) in 6 patients, stable disease (SD) in 69 patients and progressive disease (PD) in 33 patients according to RECIST version 1.1. Consequently, ORR of the 108 patients with metastatic CRC was 5.6%, disease control rate (DCR) was 69.4%. The waterfall plot for the best percentage change in target lesion according to genotype status of rs2071559 polymorphism is shown in Figure 2. The ORR of patients with TT genotype and TC/CC genotype was 6.1% and 4.8% (P=0.774), respectively; the DCR of patients with TT genotype and TC/CC genotype was 74.2% and 61.9% (P=0.175), respectively. Interestingly, cavity in the target lesion was noted in our study. The MRI changes of the lung target lesion in one patient who was treated after 4 cycles of apatinib are shown in Figure 3. The efficacy in this patient receiving apatinib treatment was remarkable, an obvious cavity in the target lesion was observed dramatically.
 |
Figure 2 Waterfall plot for the best percentage change in target lesion size of the 108 patients with chemotherapy-refractory metastatic CRC according to KDR rs2071559 genotype status. |
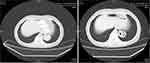 |
Figure 3 The MRI scan changes of target lesions in colorectal cancer patients with lung metastases after 4 cycles of apatinib treatment. |
With regard to the prognosis, the median follow-up duration of all the patients from the time of enrollment to the date of cut-off was 8.5 months (follow-up range: 0.3–24 months). As illustrated in Figure 4, the median PFS of the 108 patients with metastatic CRC receiving apatinib monotherapy was 3.6 months (95% confidence interval (CI): 3.03–4.17 months). Furthermore, overall survival was also carried out in this study. As shown in Figure 4, the median OS of the 108 patients with metastatic CRC was 8.9 months (95% CI: 7.57–10.23 months).
 |
Figure 4 The progression-free survival and overall survival of the 108 patients with chemotherapy-refractory metastatic CRC. |
As shown in Table 1, only rs2071559 was of clinical significance. Figure 5 shows that the median PFS of the patients with TT and TC/CC genotype of rs2071559 polymorphism was 4.1 and 3.0 months respectively, which was statistically significant (χ2=6.31, P=0.012). Additionally, in terms of the association between rs2071559 genotype status and OS, as illustrated in Figure 6, the median OS of the patients with TT and TC/CC genotype of the rs2071559 polymorphism was 10.5 and 6.1 months, respectively. This difference was statistically significant (χ2=7.24, P=0.007).
 |
Figure 5 The progression-free survival of the 108 patients with chemotherapy-refractory metastatic CRC according to KDR rs2071559 genotype status. |
 |
Figure 6 The overall survival of the 108 patients with chemotherapy-refractory metastatic CRC according to KDR rs2071559 genotype status. |
Furthermore, a multivariate Cox regression model was constructed to identify the independent significance of rs2071559 polymorphism. Multivariate analysis was performed after univariate analysis. As illustrated in Table 3, OS of the 108 patients with metastatic CRC according to baseline characteristics and polymorphism was analyzed first. Interestingly, only age, ECOG score, tumor location and rs2071559 polymorphism were found to be of statistical significance in the univariate analysis, which was included in the multivariate analysis. However, it should be noted that patients with two lines of previous treatment had a trend for superior OS compared with those with ≥3 lines of previous treatment, even though the difference was not statistically significant. In consequence, line of previous treatment was included in multivariate analysis as well. As shown in Table 3, after the multivariate adjustment, the statistically significant influence was still confirmed of KDR rs2071559 polymorphism on OS. Therefore, this conclusion demonstrated that rs2071559 polymorphism was an independent factor for OS (hazard ratio (HR)=0.65, P=0.021). Additionally, as indicated in Table 3, age (HR=0.82, P=0.040), ECOG score (HR=0.76, P=0.024) and tumor location (HR=1.38, P=0.017) were also independent factors for OS, respectively.
 |
Table 3 Overall Survival of the 108 Patients with Metastatic CRC According to Baseline Characteristics and Polymorphism in Univariate and Multivariate Analysis |
Association Analysis Between KDR rs2071559 Polymorphism and Safety Profile of Patients with Metastatic CRC
Safety profile was an important aspect to evaluate the clinical application of apatinib in patients with metastatic CRC, especially the initial dosage of 500 mg and 250 mg. No grade 5 adverse reactions were observed in our study. As illustrated in Figure 7, the common adverse reactions related to apatinib treatment in the 108 patients with metastatic CRC mainly manifested as hypertension, hand-foot syndrome (HFS), nausea and vomiting, fatigue, leukopenia, diarrhea, appetite decrease, AST/ALT elevation, proteinuria and oral mucositis. The incidence was 44 cases (40.7%), 41 cases (38.0%), 38 cases (35.2%), 31 cases (28.7%), 26 cases (24.1%), 19 cases (17.6%), 15 cases (13.9%), 11 cases (10.2%), 8 cases (7.4%)and 6 cases (5.6%), respectively. Additionally, the grade ≥3 adverse reactions were noted in hypertension 16 cases (14.8%), HFS 9 cases (8.3%), nausea and vomiting 6 cases (5.6%), leukopenia 4 cases (3.7%), proteinuria 3 cases (2.8%)and AST/ALT elevation 2 cases (1.9%). With regard to the association between rs2071559 genotype status and safety profile, unfortunately, no significant correlation was noted between the adverse reactions of the 108 patients and rs2071559 genotype status (P>0.05).
 |
Figure 7 The safety profile of patients with chemotherapy refractory metastatic CRC receiving apatinib monotherapy. |
Detection of KDR Gene mRNA Expression According to rs2071559 Genotype Status
As described in the Method section, a total of 66 patients were available for KDR mRNA expression analysis. Of the 66 specimens included in this study, the prevalence of KDR rs2071559 polymorphism was as follows: TT genotype 40 cases (60.6%), TC genotype 23 cases (34.9%), CC genotype 3 cases (4.5%), the minor allele frequency was 0.22, the distribution of the three genotypes was in accordance with Hardy-Weinberg equilibrium as well (P=0.894). And the genotype frequency was comparable with the genotype distribution frequency in the 108 patients with metastatic CRC. Consequently, TC and CC genotypes were merged during the subsequent analysis. As illustrated in Figure 8, compared with TT genotype, patients with TC/CC genotype demonstrated higher relative expression of KDR mRNA in PBMC specimens compared with patients with TT genotype (3.96±0.456 vs 2.70±0.661), which was statistically significant (t=8.598, P<0.001).
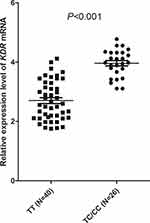 |
Figure 8 Relative mRNA expression level of KDR gene according to KDR rs2071559 genotype status. |
Discussion
To our knowledge, the present retrospective study highlighted the real-world evidence regarding the clinical outcome and safety of apatinib monotherapy in the treatment of patients with chemotherapy-refractory metastatic CRC. Simultaneously, polymorphism analysis in this study suggested that patients with TC/CC genotype of rs2071559 was associated with worse PFS and OS. The clinical outcomes of patients with metastatic CRC who were treated with apatinib could be impacted by KDR rs2071559 polymorphism through mediating KDR mRNA expression.
As a highly heterogeneous digestive system malignancy, metastatic CRC has been sensitive to fluorouracil-based first-line chemotherapy for the past several decades.27 Despite a high rate of response to the fluorouracil-based first-line therapy, patients with metastatic CRC almost always relapsed eventually.28 ORR of the subsequent line treatment was disappointing and great individual differences were observed for the efficacy and prognosis of patients with chemotherapy refractory metastatic CRC clinically.29 To the best of our knowledge, single nucleotide polymorphism was the third generation of molecular markers of genetic variation and contributed to the differences in susceptibility of cancer and diversity to drug response.30,31 Gratifyingly, there were considerable studies focusing on polymorphisms which could predict the efficacy and safety of metastatic CRC at present: JS Su and colleagues found in 2020 that the prognosis of patients with R0 resection CRC who received capecitabine-based adjuvant chemotherapy in real world may be influenced by PD-L1 901T>C polymorphism through mediation of the mRNA expression of PD-L1.32 Mitsukuni Suenaga and colleagues reported in 2020 that RPA2 polymorphism rs7356 might serve as a predictive and prognostic marker of oxaliplatin responsiveness in a RAS status-dependent manner in mCRC patients receiving FOLFOXIRI combined with bevacizumab regimens.33 The work of Ryuma Tokunaga and colleagues suggested that CD39 polymorphism rs11188513 in the adenosine pathway could influence the clinical outcomes of patients with metastatic CRC who were treated with FOLFIRI plus bevacizumab treatment.34 Mitsukuni Suenaga and colleagues investigated the gene polymorphism in the CCL5/CCR5 pathway in metastatic CRC receiving regorafenib treatment and the conclusion indicated that genetic variants rs1634517 and rs1130371 in the CCL5/CCR5 pathway could serve as prognostic markers and might predict severe hand-foot skin reaction in mCRC patients receiving regorafenib therapy.35 In conclusion, these above works demonstrated the potential predictive value of pharmacogenomics in the clinical outcomes and safety of patients with CRC.
Although our study was designed as a retrospective analysis, the clinical outcomes of patients with chemotherapy-refractory metastatic CRC receiving apatinib treatment were evaluated simultaneously. ORR of the 108 patients with CRC who received apatinib treatment was 5.6%, DCR was 69.4%, the median PFS was 3.6 months, which were slightly inferior to the prospective clinical trial of apatinib in metastatic CRC initiated by F Wang and colleagues in 2020 (ORR=8.3%, DCR=68.8% and mPFS=4.8 months) and the phase ІІ clinical trial initiated by XF Chen and colleagues in 2019 (mPFS=3.9 months).10,15 We speculated that the discrepancy could be attributed to the retrospective design of our study. Management of the patients in retrospective study was not sufficient and normative compared with a well-designed phase ІІ clinical trial, which was demonstrated in the other retrospective study of apatinib in metastatic CRC (ORR=3.7%, DCR=70.4% and mPFS=2.0 months).36 Additionally, it should be noted that the proportion of patients with ECOG 2 score in our study was higher than that in the phase ІІ study (43.5% vs 35.4%). To our knowledge, the previous research had suggested that higher ECOG score was associated with worse prognosis among patients with metastatic CRC.36,37 Furthermore, the results of Cox regression analysis in our study demonstrated that patients with higher ECOG 2 score were associated with worse OS, which was in concert with the results of the previous study.38 On the other hand, OS was also performed in our study. Interestingly, the median OS of the 108 patients with metastatic CRC receiving apatinib treatment was 8.9 months, which was relatively longer than that reported in the phase ІІ clinical trial initiated by XF Chen and colleagues (median OS=7.9 months). We speculated that the reason could be attributed to the continuous license of immunotherapy drugs (pembrolizumab and nivolumab) and targeted drug (regorafenib and fruquintinib) that could be effective as the subsequent line treatment for patients with metastatic CRC in China since 2018.19,20,39 Especially, fruquintinib became a new standard therapy as third-line and subsequent-line treatment in the FRESCO clinical trial for patients with metastatic CRC in China.40 Therefore, immunotherapy and fruquintinib or regorafenib were available for patients with chemotherapy refractory metastatic CRC to use after the progression of apatinib as the subsequent-line treatment, which could contribute to survival benefits for the patients continuously.41
With regard to the KDR gene polymorphism analysis, to our knowledge, our study was the first study concentrating on the association between the clinical outcome of patients with metastatic CRC receiving apatinib treatment and KDR gene polymorphism analysis in Chinese population. Interestingly, a recent study initiated by YD Wang and colleagues explored the clinical outcomes and safety of apatinib for patients with advanced non-squamous NSCLC who progressed after standard therapy and analysis of the KDR gene polymorphism.22 Results of the study demonstrated that patients with TC/CC genotype of KDR rs2071559 polymorphism were associated with worse prognosis, which demonstrated the potential predictive significance of this polymorphism in the clinical outcomes of patients with NSCLC who received apatinib treatment. Additionally, another exploratory study included 105 patients with metastatic osteosarcoma to investigate the influence of VEGFR2 gene polymorphism on the efficacy and safety of apatinib for patients with metastatic osteosarcoma who progressed after standard therapy.42 The results suggested that the clinical outcomes of apatinib might be influenced by the rs2071559 polymorphism. All the conclusions of the two previous studies were consistent with the results of our study to some extent. These findings demonstrated that rs2071559 polymorphism of KDR gene could play a certain role in apatinib disposition and treatment. Additionally, a previous study recruited a total of 118 patients with advanced epithelial ovarian carcinoma who received apatinib treatment. The peripheral blood and peripheral blood mononuclear cell (PBMC) specimens from these patients with EOC were collected to perform the genotyping of the genetic polymorphism and assess the mRNA expression of VEGFR2, respectively. The results demonstrated that patients with TC/CC genotype of rs2071559 had a worse PFS and OS compared with those with TT genotype, which was consistent with the conclusion in our study. On the other hand, the results of a recent study initiated by Ivana Sullivan and colleague were in line with that in our study as well.43 A total of 170 patients with metastatic NSCLC who were treated with first-line platinum-based chemotherapy were included in their study and the results found that VEGFA rs2010963 and VEGFR2 rs2071559 were significantly associated with OS. Specifically, patients with rs2071559 major genotype were associated with better prognosis, which was consistent with our results to some extent. Besides, a recent phase III trial of adjuvant sunitinib in patients with high-risk renal cell carcinoma demonstrated that longer DFS was observed with sunitinib versus placebo for VEGFR2 rs2071559 TT patients and the stratification analysis based on the rs2071559 genotype results showed that the median DFS was longer in the patients with TT genotype than the total patients that received sunitinib treatment,44 which was consistent with our study. From the above, KDR rs2071559 was of clinical significance as a biomarker for the prediction of the patients with metastatic CRC receiving apatinib monotherapy.
Additionally, a total of 66 randomly selected PBMC specimens were also included in our mRNA expression analysis. The results suggested that the mRNA expression of KDR gene was significantly higher in patients with CT/TT genotype. To our knowledge, KDR was the receptor with the strongest binding ability to VEGF-A and played an important role in angiogenesis. The protein expression level of KDR conferred a crucial role in the process of tumor proliferation and metastasis.45 Previous studies demonstrated that higher levels of KDR expression in tumor cells were associated with a greater chance for tumor cells to regenerate blood vessels and relapse or metastasize.46,47 Consequently, some of the relevant exploratory studies demonstrated that patients with higher expression levels of KDR conferred a worse PFS and OS in non-small cell lung cancer48 and gastric cancer,49 respectively. These results were consistent with our results to some extent. From the above, KDR rs2071559 polymorphism could be used as an independent biomarker for the prediction of patients with chemotherapy refractory metastatic CRC receiving apatinib monotherapy.
The common adverse reactions of patients with CRC receiving apatinib treatment were hypertension, hand-foot syndrome (HFS), nausea and vomiting, fatigue and leukopenia, which were similar with those of the previous retrospective studies of apatinib in metastatic CRC.37,50 No adverse reactions were newly detected during the study, which indicated that apatinib at an initial dosage of 250 mg or 500 mg could be safe for the patients. Additionally, the correlation analysis between polymorphism and adverse reactions failed to show a significant difference. This result demonstrated that the rs2071559 polymorphism did not contribute to pharmacokinetics of apatinib disposition.
In conclusion, the prognosis significance according to rs2071559 polymorphism status was interpreted appropriately, in that we thought our study was of potential clinical significance for the prognosis assessment of patients with chemotherapy refractory metastatic CRC receiving apatinib monotherapy. However, the conclusion should be confirmed and validated in large-scale prospective clinical trials in the further.
Ethical Approval
All procedures performed in studies involving human participants were in accordance with the ethical standards of the ethics committee of Affiliated Tumor Hospital of Tianjin Medical University and with the 1964 Helsinki Declaration and its later amendments or comparable ethical standards.
Informed Consent
Informed consent was obtained from all individual participants included in the study.
Acknowledgments
This work was supported by grants from the National Natural Science Foundation of China (Nos. 81772629, 81802363, 81702431, 81702437, 81772843, 81974374) and the Demonstrative Research Platform of Clinical Evaluation Technology for New Anticancer Drugs (No. 2018ZX09201015). This work was also supported by the Tianjin Science Foundation (Nos. 18JCQNJC81900, 18JCYBJC92000, 18JCYBJC25400, 16PTSYJC00170, 18JCYBJC92900) and the Science & Technology Development Fund of the Tianjin Education Commission for Higher Education (2018KJ046, 2017KJ227). Key Research and Development (R&D) Projects of Shanxi Province (201803D31167).
Disclosure
The authors declare that there are no conflicts of interest in this work.
References
1. Grolleman JE, Díaz-Gay M, Franch-Expósito S, Castellví-Bel S, de Voer RM. Somatic mutational signatures in polyposis and colorectal cancer. Mol Aspects Med. 2019:69;62–72. doi:10.1016/j.mam.2019.05.002
2. Bray F, Ferlay J, Soerjomataram I, et al. Global cancer statistics 2018: GLOBOCAN estimates of incidence and mortality worldwide for 36 cancers in 185 countries. CA Cancer J Clin. 2018;68(6):394–424. doi:10.3322/caac.21492
3. Chen W, Zheng R, Baade PD, et al. Cancer statistics in China, 2015. CA Cancer J Clin. 2016;66(2):115–132. doi:10.3322/caac.21338
4. Shah MA, Renfro LA, Allegra CJ, et al. Impact of patient factors on recurrence risk and time dependency of oxaliplatin benefit in patients with colon cancer: analysis from modern-era adjuvant studies in the adjuvant colon cancer end points (ACCENT) database. J Clin Oncol. 2016;34(8):843–853. doi:10.1200/jco.2015.63.0558
5. Ge Y, Lei S, Cai B, et al. Incidence and prognosis of pulmonary metastasis in colorectal cancer: a population-based study. Int J Colorectal Dis. 2020;35(2):223–232. doi:10.1007/s00384-019-03434-8
6. McQuade RM, Stojanovska V, Bornstein JC, Nurgali K. Colorectal Cancer Chemotherapy: the Evolution of Treatment and New Approaches. Curr Med Chem. 2017;24(15):1537–1557. doi:10.2174/0929867324666170111152436
7. Tintelnot J, Stein A. Immunotherapy in colorectal cancer: available clinical evidence, challenges and novel approaches. World J Gastroenterol. 2019;25(29):3920–3928. doi:10.3748/wjg.v25.i29.3920
8. Xie YH, Chen YX, Fang JY. Comprehensive review of targeted therapy for colorectal cancer. Signal Transduct Target Ther. 2020;5(1):22. doi:10.1038/s41392-020-0116-z
9. Venook AP, Niedzwiecki D, Lenz HJ, et al. Effect of first-line chemotherapy combined with cetuximab or bevacizumab on overall survival in patients with kras wild-type advanced or metastatic colorectal cancer: a randomized clinical trial. JAMA. 2017;317(23):2392–2401. doi:10.1001/jama.2017.7105
10. Wang F, Yuan X, Jia J, et al. Apatinib monotherapy for chemotherapy-refractory metastatic colorectal cancer: a multi-centre, Single-Arm, Prospective Study. Sci Rep. 2020;10(1):6058. doi:10.1038/s41598-020-62961-5
11. Yin L, Li J, Ma D, Li D, Sun Y. Angiogenesis in primary colorectal cancer and matched metastatic tissues: biological and clinical implications for anti-angiogenic therapies. Oncol Lett. 2020;19(5):3558–3566. doi:10.3892/ol.2020.11450
12. Zhang Y, Zou JY, Wang Z, Wang Y. Fruquintinib: a novel antivascular endothelial growth factor receptor tyrosine kinase inhibitor for the treatment of metastatic colorectal cancer. Cancer Manag Res. 2019:11;7787–7803. doi:10.2147/cmar.s215533
13. Dhillon S. Regorafenib: a Review in Metastatic Colorectal Cancer. Drugs. 2018;78(11):1133–1144. doi:10.1007/s40265-018-0938-y
14. Zhang Q, Wang Q, Wang X, et al. Regorafenib, TAS-102, or fruquintinib for metastatic colorectal cancer: any difference in randomized trials? Int J Colorectal Dis. 2020;35(2):295–306. doi:10.1007/s00384-019-03477-x
15. Chen X, Qiu T, Zhu Y, et al. A Single-Arm, Phase II Study of Apatinib in Refractory Metastatic Colorectal Cancer. Oncologist. 2019;24(7):883–e407. doi:10.1634/theoncologist.2019-0164
16. Li J, Qin S, Xu J, et al. Randomized, double-blind, placebo-controlled Phase III trial of apatinib in patients with chemotherapy-refractory advanced or metastatic adenocarcinoma of the stomach or gastroesophageal junction. J Clin Oncol. 2016;34(13):1448–1454. doi:10.1200/jco.2015.63.5995
17. Xu Y, Huang Z, Lu H, et al. Apatinib in patients with extensive-stage small-cell lung cancer after second-line or third-line chemotherapy: a Phase II, single-arm, multicentre, prospective study. Br J Cancer. 2019;121(8):640–646. doi:10.1038/s41416-019-0583-6
18. Wu F, Zhang S, Xiong A, et al. A Phase II clinical trial of apatinib in pretreated advanced non-squamous non-small-cell lung cancer. Clin Lung Cancer. 2018;19(6):e831–e842. doi:10.1016/j.cllc.2018.06.002
19. Li J, Qin S, Xu R, et al. Regorafenib plus best supportive care versus placebo plus best supportive care in Asian patients with previously treated metastatic colorectal cancer (CONCUR): a randomised, double-blind, placebo-controlled, Phase 3 trial. Lancet Oncol. 2015;16(6):619–629. doi:10.1016/s1470-2045(15)70156-7
20. Li J, Qin S, Xu RH, et al. Effect of Fruquintinib vs placebo on overall survival in patients with previously treated metastatic colorectal cancer: the FRESCO Randomized Clinical Trial. JAMA. 2018;319(24):2486–2496. doi:10.1001/jama.2018.7855
21. Fan M, Zhang J, Wang Z, et al. Phosphorylated VEGFR2 and hypertension: potential biomarkers to indicate VEGF-dependency of advanced breast cancer in anti-angiogenic therapy. Breast Cancer Res Treat. 2014;143(1):141–151. doi:10.1007/s10549-013-2793-6
22. Song ZZ, Zhao LF, Zuo J, et al. Clinical outcomes and safety of apatinib mesylate in the treatment of advanced non-squamous non-small cell lung cancer in patients who progressed after standard therapy and analysis of the KDR Gene Polymorphism. Onco Targets Ther. 2020:13;603–613. doi:10.2147/ott.s222985
23. Yan Z, Gu YY, Hu XD, et al. Clinical outcomes and safety of apatinib monotherapy in the treatment of patients with advanced epithelial ovarian carcinoma who progressed after standard regimens and the analysis of the VEGFR2 polymorphism. Oncol Lett. 2020;20(3):3035–3045. doi:10.3892/ol.2020.11857
24. Eisenhauer EA, Therasse P, Bogaerts J, et al. New response evaluation criteria in solid tumours: revised RECIST guideline (version 1.1). Eur J Cancer. 2009;45(2):228–247. doi:10.1016/j.ejca.2008.10.026
25. Miller TP, Fisher BT, Getz KD, et al. Unintended consequences of evolution of the common terminology criteria for adverse events. Pediatr Blood Cancer. 2019:e27747. doi:10.1002/pbc.27747
26. Wu D, Nie J, Hu W, et al. A phase II study of anlotinib in 45 patients with relapsed small cell lung cancer. Int J Cancer. 2020. doi:10.1002/ijc.33161
27. Chionh F, Lau D, Yeung Y, Price T, Tebbutt N. Oral versus intravenous fluoropyrimidines for colorectal cancer. Cochrane Database Syst Rev. 2017;7(7):Cd008398. doi:10.1002/14651858.CD008398.pub2
28. Sanz-Garcia E, Grasselli J, Argiles G, Elez ME, Tabernero J. Current and advancing treatments for metastatic colorectal cancer. Expert Opin Biol Ther. 2016;16(1):93–110. doi:10.1517/14712598.2016.1108405
29. Riechelmann R, Grothey A. Antiangiogenic therapy for refractory colorectal cancer: current options and future strategies. Adv Med Oncol. 2017;9(2):106–126. doi:10.1177/1758834016676703
30. Canavese M, Ngo DT, Maddern GJ, et al. Biology and therapeutic implications of VEGF-A splice isoforms and single-nucleotide polymorphisms in colorectal cancer. Int J Cancer. 2017;140(10):2183–2191. doi:10.1002/ijc.30567
31. Al-Shaheri FN, Al-Shami KM, Gamal EH, Mahasneh AA, Ayoub NM. Association of DNA repair gene polymorphisms with colorectal cancer risk and treatment outcomes. Exp Mol Pathol. 2020:113;104364. doi:10.1016/j.yexmp.2019.104364
32. Su J, Dai B, Yuan W, et al. The influence of PD-L1 genetic variation on the prognosis of R0 resection colorectal cancer patients received capecitabine-based adjuvant chemotherapy: a long-term follow-up, real-world retrospective study. Cancer Chemother Pharmacol. 2020;85(5):969–978. doi:10.1007/s00280-020-04069-1
33. Suenaga M, Schirripa M, Cao S, et al. Single nucleotide polymorphisms in miRNA binding sites of nucleotide excision repair-related genes predict clinical benefit of oxaliplatin in folfoxiri plus bevacizumab: analysis of the tribe trial. Cancers. 2020;12:7. doi:10.3390/cancers12071742
34. Tokunaga R, Cao S, Naseem M, et al. Prognostic effect of adenosine-related genetic variants in metastatic colorectal cancer treated with bevacizumab-based chemotherapy. Clin Colorectal Cancer. 2019;18(1):e8–e19. doi:10.1016/j.clcc.2018.09.003
35. Suenaga M, Schirripa M, Cao S, et al. Gene Polymorphisms in the CCL5/CCR5 pathway as a genetic biomarker for outcome and hand-foot skin reaction in metastatic colorectal cancer patients treated with regorafenib. Clin Colorectal Cancer. 2018;17(2):e395–e414. doi:10.1016/j.clcc.2018.02.010
36. Liao X, Li H, Liu Z, et al. Clinical efficacy and safety of apatinib in patients with advanced colorectal cancer as the late-line treatment. Medicine. 2018;97(50):e13635. doi:10.1097/md.0000000000013635
37. Gou M, Si H, Zhang Y, et al. Efficacy and safety of apatinib in patients with previously treated metastatic colorectal cancer: a real-world retrospective study. Sci Rep. 2018;8(1):4602. doi:10.1038/s41598-018-22302-z
38. Novakova-Jiresova A, Kopeckova K, Boublikova L, et al. Regorafenib for metastatic colorectal cancer: an analysis of a registry-based cohort of 555 patients. Cancer Manag Res. 2020:12;5365–5372. doi:10.2147/cmar.s255332
39. Franke AJ, Skelton WP, Starr JS, et al. Immunotherapy for Colorectal Cancer: a Review of Current and Novel Therapeutic Approaches. J Natl Cancer Inst. 2019;111(11):1131–1141. doi:10.1093/jnci/djz093
40. Ganesh K, Stadler ZK, Cercek A, et al. Immunotherapy in colorectal cancer: rationale, challenges and potential. Nat Rev Gastroenterol Hepatol. 2019;16(6):361–375. doi:10.1038/s41575-019-0126-x
41. Rawla P, Barsouk A, Hadjinicolaou AV, Barsouk A. Immunotherapies and Targeted Therapies in the Treatment of Metastatic Colorectal Cancer. Med Sci. 2019;7:8. doi:10.3390/medsci7080083
42. Liu JY, Zhu BR, Wang YD, Sun X. The efficacy and safety of Apatinib mesylate in the treatment of metastatic osteosarcoma patients who progressed after standard therapy and the VEGFR2 gene polymorphism analysis. Int J Clin Oncol. 2020;25(6):1195–1205. doi:10.1007/s10147-020-01644-7
43. Sullivan I, Riera P, Andres M, et al. Prognostic effect of VEGF gene variants in metastatic non-small-cell lung cancer patients. Angiogenesis. 2019. doi:10.1007/s10456-019-09668-y
44. George DJ, Martini JF, Staehler M, et al. Phase III trial of adjuvant sunitinib in patients with high-risk renal cell carcinoma: exploratory pharmacogenomic analysis. Clin Cancer Res. 2019;25(4):1165–1173. doi:10.1158/1078-0432.ccr-18-1724
45. Cho HD, Moon KD, Park KH, Lee YS, Seo KI. Effects of auriculasin on vascular endothelial growth factor (VEGF)-induced angiogenesis via regulation of VEGF receptor 2 signaling pathways in vitro and in vivo. Food Chem Toxicol. 2018:121;612–621. doi:10.1016/j.fct.2018.09.025
46. Lu Y, Xu Q, Zuo Y, et al. Isoprenaline/beta2-AR activates Plexin-A1/VEGFR2 signals via VEGF secretion in gastric cancer cells to promote tumor angiogenesis. BMC Cancer. 2017;17(1):875. doi:10.1186/s12885-017-3894-0
47. Jinesh GG, Manyam GC, Mmeje CO, Baggerly KA, Kamat AM. Surface PD-L1, E-cadherin, CD24, and VEGFR2 as markers of epithelial cancer stem cells associated with rapid tumorigenesis. Sci Rep. 2017;7(1):9602. doi:10.1038/s41598-017-08796-z
48. Ding M, Liu L, Hu C, et al. Expression of VEGFR2 and NRP-1 in non-small cell lung cancer and their clinical significance. Chin J Cancer Res. 2014;26(6):669–677. doi:10.3978/j.issn.1000-9604.2014.12.04
49. Zhu X, Wang Y, Xue W, et al. The VEGFR-2 protein and the VEGFR-2 rs1870377 A>T genetic polymorphism are prognostic factors for gastric cancer. Cancer Biol Ther. 2019;20(4):497–504. doi:10.1080/15384047.2018.1537575
50. Liang L, Wang L, Zhu P, et al. A pilot study of apatinib as third-line treatment in patients with heavily treated metastatic colorectal cancer. Clin Colorectal Cancer. 2018;17(3):e443–e449. doi:10.1016/j.clcc.2018.02.011
 © 2021 The Author(s). This work is published and licensed by Dove Medical Press Limited. The full terms of this license are available at https://www.dovepress.com/terms.php and incorporate the Creative Commons Attribution - Non Commercial (unported, v3.0) License.
By accessing the work you hereby accept the Terms. Non-commercial uses of the work are permitted without any further permission from Dove Medical Press Limited, provided the work is properly attributed. For permission for commercial use of this work, please see paragraphs 4.2 and 5 of our Terms.
© 2021 The Author(s). This work is published and licensed by Dove Medical Press Limited. The full terms of this license are available at https://www.dovepress.com/terms.php and incorporate the Creative Commons Attribution - Non Commercial (unported, v3.0) License.
By accessing the work you hereby accept the Terms. Non-commercial uses of the work are permitted without any further permission from Dove Medical Press Limited, provided the work is properly attributed. For permission for commercial use of this work, please see paragraphs 4.2 and 5 of our Terms.

